Professional Documents
Culture Documents
Radiografía Tórax: Signo de Westermark
Radiografía Tórax: Signo de Westermark
Uploaded by
TreXx GaMeROriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Radiografía Tórax: Signo de Westermark
Radiografía Tórax: Signo de Westermark
Uploaded by
TreXx GaMeRCopyright:
Available Formats
Radiografía Tórax
domingo, 27 de febrero de 2022 09:38 a. m.
▪ Confirm that the study associated with the right patient and has been performed on the right date. Signo de Westermark
▪ Therefore, when reviewing any chest radiograph it is vital to ascertain if there are previous studies available. Hiperclaridad pulmonar, generalmente en las
bases, por reducción del flujo sanguíneo distal al
Technical Aspects vaso ocluido, local o general.
▪ Confirm the satisfactory quality of any chest radiograph:
○ Rotation: Satisfactory chest radiograph should have no rotation. This is confirmed by ensuring that the
medial borders of the clavicle are equidistant from the spinous processes.
In the case of rotation, one side of the radiograph becomes darker than the other. This phenomenon is
known as "Increased Transradiancy".
May misinterpret this difference in transradiancy as pathology.
For example, the darker side may represent a pneumothorax or pulmonary embolism (Westermark sign).
In addition, the lighter side may be misinterpreted as a pleural fluid collection or air space consolidation
○ Inspiration: Also important to ensure that the patient has made a good inspiratory effort, confirmed by
ascertaining that there are ten ribs visible posteriorly.
Poor inspiratory effort, the pulmonary vessels become more prominent and an erroneous diagnosis of
cardiac failure.
○ Penetration: is less relevant nowadays.
▪ These two technical factors are so important, because, failure to ensure the correct standard can mimic life-
threatening pathology.
System for Reviewing the Chest Radiograph
▪ Having confirmed that the patient’s details are correct and that the radiograph is technically satisfactory, proceed
to reviewing the chest radiograph in a systematic order.
AP or PA Orientation?
▪ PA (posteroanterior) standard film has no annotative marking on it.
▪ Not to begin a report with reference to ‘PA’ or ‘AP’, vocalise the following introductory:
▪ “This is a frontal chest radiograph of an adult patient”.
▪ Secondly, and if appropriate, one adds a second line, “Both breast shadows are present”, a failure to recognise a
second breast shadow suggests an underlining diagnosis of mastectomy and, therefore, should prompt a
systematic review for evidence of breast cancer and its sequelae.
Heart Size
▪ Tansverse diameter of the heart should not exceed 50% of the maximum transverse diameter of the chest on a PA
radiograph-> Cardiothoracic Ratio.
▪ AP there is a magnification factor of approximately 20%. Gross cardiomegaly should be easily distinguishable
from a slightly magnified normal heart. It is, not correct to infer that the heart size cannot be assessed using an
AP study.
Pulmonary Vascularity
▪ When describe ‘pulmonary vascularity’, we are discussing pulmonary venous vascularity, a shorthand for the
absence or presence of cardiac failure.
▪ Enlarged pulmonary arteries, as for example, in a left to right cardiac shunt, is given a specific designation:
Pulmonary Plethora.
▪ Pulmonary vascularity is normal? There are elementary rules:
1. Pulmonary venous vessels should not be discretely visible in the outer third of the lung fields.
2. 90% of the pulmonary vascular structures are appreciated at the mid and lower zones.
3. When pulmonary vascularity increases, for example, with Heart Failure, increased vascular conspicuity is
apparent at the apices. This is known as Equivalence or Upper Zone Diversion (cephalisation of the
pulmonary veins).
4. Kerley B lines seen at the costophrenic angles and lateral chest walls are not specific to Cardiac Failure "Cefalización de las Venas Pulmonares"
and represent the manifestation of enlargement of the interlobular septa of the secondary pulmonary
lobules, in other words, interstitial lung diseases will produce precisely the same appearance.
5. Angel or Bat Wings. These are seen in the most severe form of cardiac failure, pulmonary oedema, and
are very rare.
Lung Fields
▪ The Silhouette Sign: only three densities are visible on any radiograph, bone, air and soft tissue.
▪ If the normal silhouette disappears, it implies that the adjoining area has now transmuted into the same density as
its neighbouring structure, usually indicating lobar consolidation.
▪ The location of the consolidation, is to know which lobe of each lung lies adjacent to the heart and
hemidiaphragms. "Signo de las Alas de Murcielago"
Review Areas Signo de Chilaiditi
Primer Parcial página 1
▪ The location of the consolidation, is to know which lobe of each lung lies adjacent to the heart and
hemidiaphragms. "Signo de las Alas de Murcielago"
Review Areas Signo de Chilaiditi
Interposición de intestino entre el hígado y el
1. Sub diaphragmatic region hemidiafragma derecho.
▪ Pneumoperitoneum, in the absence of recent surgery, often denotes a life-threatening pathology. Es más frecuente en varones (relación 4:1) y
▪ On erect chest radiograph there should be no free gas present under the diaphragm. generalmente es un hallazgo casual. Su causa es
▪ Even very small quantities of free gas can be confidently seen under the right hemidiaphragm and this should desconocida.Es asintomático.
represent an essential review area. En caso de asociarse a sintomatología se denomina
síndrome de Chilaiditi (digestivos: vómitos,
2. The Lung Apices. anorexia, estreñimiento y distensión abdominal).
▪ A particularly the case in the older patient where there is asymmetrical calcification of the costochondral
junctions. This age-related calcification can mimic a neoplasm, if there is diagnostic uncertainty the solution is to
request a supplementary Apical View, s allows visualisation of the lung apices without the complication of
overlapping bony structures, occasionally it will confirm quite a sizable mass lesion.
3. Trachea
▪ The ascertainment that it is midline is essential.
▪ The commonest neck mass to displace the trachea is a thyroid mass, which will displace it to the contralateral
side or within the chest, a tension pneumothorax, while collapse or atelectasis of a lobe will draw the trachea
towards the side of the abnormality.
4. The Hilum
▪ Hilar point represent the intersection of the pulmonary arteries and veins.
▪ Left hilar point normally lies higher than the right, the hila should always be equal in size and density.
5. The Aorto-pulmonary Window
▪ If one traces the edge of the aortic knuckle inferiorly, the next convexity is that of the pulmonary artery.
▪ Between the two there is a concavity. There should be nothing within this aorto-pulmonary bay.
▪ Malignant lymphadenopathy associated with a neoplasm can manifest within this window.
6. Bones
▪ There is a technique known as ‘high kilovoltage’ (kV), was developed to permit improved evaluation of the
chest organs, but the conspicuity of bone decreases.
▪ Identification of any rib fracture should prompt the immediate radiological exclusion of pneumothorax.
▪ Bone review effectively is performed for two reasons:
1. Trauma: exclude fractures or dislocations, particularly at shoulder level.
2. Neoplasia: exclude infiltration and destruction particularly in metastatic disease and myeloma.
▪ El rendimiento diagnóstico más alto es revisar los huesos que no se ven a través de una neblina de tejido
pulmonar y vasos pulmonares. Por lo tanto, las articulaciones de los hombros, las clavículas laterales y las
costillas inferiores (que recubren el hígado y el bazo) brindan una mejor precisión diagnóstica para la enfermedad
ósea infiltrante.
Common Pathologies
Cardiac Failure
▪ Following criteria will help formulate a diagnosis of cardiac failure:
1. Increased cardiothoracic ratio
2. Increased (venous) pulmonary vascularity
3. Kerley B lines
4. Pleural Effusions
5. Bat or Angel Wings
Lobar Consolidation
▪ Needs understanding of the silhouette principle.
▪ All one must do is confirm which silhouette is missing, the appropriate pulmonary lobe can then be identified:
○ Left lower lobe: Left hemidiaphragm
Primer Parcial página 2
○ Left lower lobe: Left hemidiaphragm
○ Right lower lobe: Right hemidiaphragm
○ Right heart border: Right middle lobe
○ Left heart border: Lingula (Porción inferior del lóbulo superior del pulmón izquierdo).
▪ Consolidation in the upper lobes follows:
○ On the right, the lung is demarcated by the transverse or minor fissure, consolidation above, and
terminating at, the minor fissure indicates right upper lobe consolidation.
○ Consolidation below, and terminating at, the transverse fissure, delineates the right middle lobe.
○ Consolidation of the left upper lobe tends to produce a fuzzy ‘veiling’ effect with consequent reduced
conspicuity of the aortic knuckle’s silhouette.
Pneumothorax
▪ Divided into the Simple and Tension Pneumothorax.
▪ The tension pneumothorax is diagnosed radiologically when the mediastinum is displaced to the contralateral
side and there is inferior displacement of the ipsilateral hemidiaphragm, accompanying clinical distress.
▪ Also is seen as the separation of lung edge from the chest wall, is maximal on expiration because of the increased
interpleural pressure, if there is a clinical suspicion of pneumothorax it is worth requesting an Expiratory View.
▪ An artifact that may occur in infant chest radiographs and adult nonPA chest studies.
"Skin Fold", represents the interposition of skin between the patient’s back and the X-ray cassette, can look like
a pneumothorax but the pulmonary vessels are seen to cross the ‘lung edge’ indicating that there is no
pneumothorax, also within its clinical context.
▪ Diagnosis of pneumothorax in the supine patient can be problematic, lung edge may not be appreciable. "Skin Fold"
▪ In these patients, costophrenic angle may be replaced with a "‘sausage-shaped’ Deep Sulcus Sign".
Pleural Effusions
▪ Chest radiograph is relatively insensitive.
▪ Typical appearances on an erect radiograph are an area of Increased Density with a Meniscus rising up the lateral
chest wall, that reflects the negative intrapleural pressure of fluid within the pleural space.
▪ A horizontal fluid level within the chest, suggests a hydropneumothorax with air in the pleural space.
▪ If the mediastinum is not displaced in pleural effusion, indicates underlying collapse of ipsilateral lung segment
or lobe.
▪ Diagnosis can be problematic in supine patient, the likely diagnostic sign will be difference in transradiancy.
▪ Important that the visualised difference in transradiancy in not the result of a malrotated chest radiograph.
Lines and Tubes
1. The Nasogastric Tube
▪ Penalty for commencing nasogastric feeding when the tube is misplaced within in the bronchus can be very high.
▪ Correctly placed has vertical orientation within the chest and pass below the diaphragm, projected over the left
upper quadrant of the abdomen, lie within the gastric atrium.
▪ Commonest misplaced nasogastric tube is within the right or left lower lobe bronchus.
2. The Central Venous Line
▪ Should lie at the junction of the superior vena cava and the right atrium, always ensure there is no associated
pneumothorax.
3. The Endotracheal Tube
▪ Lie above the level of the tracheal bifurcation or carina.
▪ The problem with a chest tube tip at the carina itself is that with respiration it will slide into the right main
Primer Parcial página 3
3. The Endotracheal Tube
▪ Lie above the level of the tracheal bifurcation or carina.
▪ The problem with a chest tube tip at the carina itself is that with respiration it will slide into the right main
bronchus obstructing the left and potentially causing left lung collapse.
4. The Aortic Balloon Pump
▪ Lies within the descending thoracic aorta.
▪ The upper or cranial end of the balloon is marked with a small radio opaque marker. Below this marker there is a
10 cm balloon.
▪ The balloon should lie between the left subclavian artery and the renal arteries, in order not to obstruct either.
▪ Ascertain that the radio opaque marker is not higher than the aortic knuckle.
▪ If the marker is identified at the mid thoracic aortic level, it suggests that the balloon may occlude the renal and
splanchnic ostia.
Primer Parcial página 4
You might also like
- Ebook Developing Human 9Th Edition Moore Test Bank Full Chapter PDFDocument30 pagesEbook Developing Human 9Th Edition Moore Test Bank Full Chapter PDFStacieSharpnocje89% (9)
- Test Bank For Essentials of Cardiopulmonary Physical Therapy 4th Edition by Ellen Hillegass Isbn 9780323430548Document36 pagesTest Bank For Essentials of Cardiopulmonary Physical Therapy 4th Edition by Ellen Hillegass Isbn 9780323430548potassicdaywomanslqia100% (28)
- Chest X-Ray CXR InterpretationDocument13 pagesChest X-Ray CXR InterpretationduncanNo ratings yet
- Chest X-Ray Interpretation A Structured Approach Radiology OSCEDocument1 pageChest X-Ray Interpretation A Structured Approach Radiology OSCEValentina SepúlvedaNo ratings yet
- Chest X-Ray: Confirm DetailsDocument14 pagesChest X-Ray: Confirm DetailsNosheen HafeezNo ratings yet
- DR Hamdi's Cases 52.compressedDocument159 pagesDR Hamdi's Cases 52.compressedSlm BngshNo ratings yet
- Plain Chest X RayDocument154 pagesPlain Chest X RaySamuel Gamadey100% (3)
- Interpreting The Chest Radio Graph Friendly)Document9 pagesInterpreting The Chest Radio Graph Friendly)Vagner BorgesNo ratings yet
- Chest Radiograph Signs Suggestive of Pericardial DiseaseDocument5 pagesChest Radiograph Signs Suggestive of Pericardial DiseasedriveNo ratings yet
- Neonatal Chest X-Ray-2019Document11 pagesNeonatal Chest X-Ray-2019madhu rathoreNo ratings yet
- Interpretation of Chest Imaging1Document91 pagesInterpretation of Chest Imaging1Brooke TurnerNo ratings yet
- Basic Chest Imaging and Heart FailureDocument57 pagesBasic Chest Imaging and Heart FailureKiaa auliaNo ratings yet
- Chest İmagi̇ngDocument83 pagesChest İmagi̇ngHamza EljoeidiNo ratings yet
- Diagnostic Imaging - 8 - Radiological Pathology - Lung Pathologies and Radiology in Specific Cases - Prof - Dr.i̇smet TAMERDocument35 pagesDiagnostic Imaging - 8 - Radiological Pathology - Lung Pathologies and Radiology in Specific Cases - Prof - Dr.i̇smet TAMERAly MssreNo ratings yet
- Normal Chest RadiographDocument108 pagesNormal Chest RadiographVenu Madhav100% (1)
- Radiology AssignmentDocument27 pagesRadiology AssignmentRoyce GonzagaNo ratings yet
- Neonatal Chest X Ray 2019Document11 pagesNeonatal Chest X Ray 2019Ahmad ApriansahNo ratings yet
- Topic 20. X-RayDocument4 pagesTopic 20. X-RayMadeline WanhartNo ratings yet
- The Radiology Assistant - Basic InterpretationDocument67 pagesThe Radiology Assistant - Basic InterpretationMaria LimaNo ratings yet
- Cardiovascular System ExaminationDocument20 pagesCardiovascular System ExaminationAditya CherukuriNo ratings yet
- Interpretasi Foto DadaDocument137 pagesInterpretasi Foto DadaRofi Irman100% (1)
- Respiratory Exam DetailedDocument12 pagesRespiratory Exam DetailedAshiniNo ratings yet
- Pericardial EffusionDocument3 pagesPericardial EffusionNita Hurek100% (1)
- CXR Interpretation WriteupDocument32 pagesCXR Interpretation WriteupArhanNo ratings yet
- Chest X-Ray IntDocument355 pagesChest X-Ray Intpk.bhayanaNo ratings yet
- Congenital Heart Disease: Kriti Puri, MD Hugh D. Allen, MD Athar M. Qureshi, MDDocument30 pagesCongenital Heart Disease: Kriti Puri, MD Hugh D. Allen, MD Athar M. Qureshi, MDhari ilman toniNo ratings yet
- Interpretando RX PediatricoDocument10 pagesInterpretando RX PediatricosuzukishareNo ratings yet
- in The Given Chest X-Ray, Normal Cardiothoracic Ratio IsDocument63 pagesin The Given Chest X-Ray, Normal Cardiothoracic Ratio Is李建明No ratings yet
- PICTURES All in This PDFDocument597 pagesPICTURES All in This PDFHai Sheikh100% (1)
- Chest AssessmentDocument5 pagesChest Assessmentرحاب المريNo ratings yet
- How To Read A CXRDocument12 pagesHow To Read A CXRReTti Ria MustikaNo ratings yet
- Chest X Ray - zp162335Document48 pagesChest X Ray - zp162335Kushmakar VarshneyNo ratings yet
- Auntminnie SignsDocument56 pagesAuntminnie SignsHey ReelNo ratings yet
- Cara Baca Foto ThoraxDocument23 pagesCara Baca Foto ThoraxNofilia Citra CandraNo ratings yet
- Clinical Case 01-09-22Document9 pagesClinical Case 01-09-22api-626421480No ratings yet
- Coarctation of AortaDocument40 pagesCoarctation of Aortaaalok1903No ratings yet
- 01 - PediatricsDocument74 pages01 - Pediatricscore radiologyNo ratings yet
- Radiological Investigation of Chest. The Radiological Semiotics of The Chest PathologyDocument169 pagesRadiological Investigation of Chest. The Radiological Semiotics of The Chest PathologyВладимир КурпаянидиNo ratings yet
- Accuracy of The Physical Examination in Evaluating Pleural EffusionDocument7 pagesAccuracy of The Physical Examination in Evaluating Pleural EffusionTeresa MontesNo ratings yet
- Imaging Findings in Cardiac Tamponade With Emphasis On CT: Education ExhibitDocument17 pagesImaging Findings in Cardiac Tamponade With Emphasis On CT: Education ExhibitPari Pengda BaliNo ratings yet
- Early Primary Repair of Tetralogy of Fallot: Richard A. JonasDocument9 pagesEarly Primary Repair of Tetralogy of Fallot: Richard A. JonasResiden KardiologiNo ratings yet
- Cleveland Clinic Journal of Medicine 2005Document12 pagesCleveland Clinic Journal of Medicine 2005melianasulistioNo ratings yet
- CXR InterpretationDocument3 pagesCXR InterpretationNairobipaeds Madakitari WatotoNo ratings yet
- Radiology 111Document51 pagesRadiology 111Sherika A. BurgessNo ratings yet
- Radiologi KardiovaskularDocument59 pagesRadiologi KardiovaskularNhaNa HikmAtulNo ratings yet
- Pleural PathologiesDocument34 pagesPleural PathologiesAshwani RamawatNo ratings yet
- Interpreting Chestxray and AirwayDocument127 pagesInterpreting Chestxray and Airwayrigo montejoNo ratings yet
- Chest X-RaysDocument39 pagesChest X-RaysDian Oktaria SafitriNo ratings yet
- CVS Exam (RCT)Document7 pagesCVS Exam (RCT)kenners100% (11)
- Examen RadiologicDocument101 pagesExamen RadiologicAndreea GuraliucNo ratings yet
- How To Read X-RayDocument8 pagesHow To Read X-RayPeterson Wachira HscNo ratings yet
- Chest X-Ray GuideDocument26 pagesChest X-Ray GuideRizky Ayu WirdaningsiNo ratings yet
- Chest Imaging in Children February 2023Document67 pagesChest Imaging in Children February 2023Chua Kai XiangNo ratings yet
- C.tscan Pathology by FaisalDocument82 pagesC.tscan Pathology by FaisaldrmalikarifNo ratings yet
- Cardiac Surgical Operative AtlasFrom EverandCardiac Surgical Operative AtlasThorsten WahlersNo ratings yet
- Difficult Acute Cholecystitis: Treatment and Technical IssuesFrom EverandDifficult Acute Cholecystitis: Treatment and Technical IssuesNo ratings yet
- Chest X-ray Interpretation for Radiographers, Nurses and Allied Health ProfessionalsFrom EverandChest X-ray Interpretation for Radiographers, Nurses and Allied Health ProfessionalsNo ratings yet
- Dr. S.K. Haldar's Lectures On Industrial Health For AFIH Students - Occu. Lung Dis Asbestosis Silicosis ByssinosisDocument26 pagesDr. S.K. Haldar's Lectures On Industrial Health For AFIH Students - Occu. Lung Dis Asbestosis Silicosis ByssinosisDr. Prakash Kulkarni100% (2)
- Judicial Affidavit HomicideDocument6 pagesJudicial Affidavit HomicideDonnel BustamanteNo ratings yet
- Hilar EnlargementDocument19 pagesHilar EnlargementGriggrogGingerNo ratings yet
- Talc Chemical PleurodesisDocument4 pagesTalc Chemical Pleurodesismastan shaikNo ratings yet
- Kinesiología y Sus AlcancesDocument16 pagesKinesiología y Sus AlcancesEzequiel SosaNo ratings yet
- Chest TubesDocument5 pagesChest TubesCristian Odany Lopez GregorioNo ratings yet
- 2011 Krok Bank SurgeryDocument31 pages2011 Krok Bank SurgeryRahul PatilNo ratings yet
- Respiratory MCQDocument10 pagesRespiratory MCQSyeda Aroosa Abbas Naqvi100% (1)
- Pleural EffusionDocument259 pagesPleural EffusionAjay G BellamNo ratings yet
- Mechanical Ventilator: Nur Aina Athiraa Binti Azman Wan Sabrina Binti Wan Safuan Azkiyyah Wahida Binti DzulkifliDocument35 pagesMechanical Ventilator: Nur Aina Athiraa Binti Azman Wan Sabrina Binti Wan Safuan Azkiyyah Wahida Binti DzulkifliJia HuiNo ratings yet
- Art 3A10.1007 2Fs00259 013 2535 3 PDFDocument477 pagesArt 3A10.1007 2Fs00259 013 2535 3 PDFHerryAsu-songkoNo ratings yet
- Daftar PustakaDocument2 pagesDaftar PustakaRosintchi MirsalNo ratings yet
- Chapter SixDocument182 pagesChapter Sixtadele10No ratings yet
- Pleural Effusion in A Patient With End-Stage Renal Disease - PMCDocument5 pagesPleural Effusion in A Patient With End-Stage Renal Disease - PMCCasemix rsudwaledNo ratings yet
- Chest Wall, Lung, MediastinumDocument124 pagesChest Wall, Lung, MediastinumKenn BrillanteNo ratings yet
- Radiological Diagnostics of Respiratory SystemDocument70 pagesRadiological Diagnostics of Respiratory SystemVAISHALI CHOUDHARYNo ratings yet
- 11 ArijitD Medicine BibliographyDocument9 pages11 ArijitD Medicine BibliographyLakshya J BasumataryNo ratings yet
- Chest Drain ManagementDocument7 pagesChest Drain ManagementanuzNo ratings yet
- Discharge Plan Patient Teaching Pleural Effusion CastleDocument6 pagesDischarge Plan Patient Teaching Pleural Effusion Castleapi-341263362100% (2)
- Tindakan TorakosentesisDocument15 pagesTindakan TorakosentesisSheilla ElfiraNo ratings yet
- IIII: United States PatentDocument7 pagesIIII: United States PatentJuan Pablo PérezNo ratings yet
- Tube IcomptDocument2 pagesTube IcomptAlessioNavarraNo ratings yet
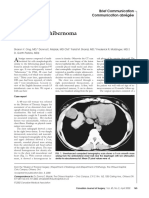
- Intrathoracic Hibernoma: Brief Communication Communication AbrégéeDocument2 pagesIntrathoracic Hibernoma: Brief Communication Communication AbrégéeM Ali AdrianNo ratings yet
- Perfusion BookDocument127 pagesPerfusion Bookreader100% (1)
- Lung BiopsyDocument8 pagesLung BiopsySiya PatilNo ratings yet
- Mis Cases Decision Making Wih Application Software 4th Edition Miller Solutions ManualDocument25 pagesMis Cases Decision Making Wih Application Software 4th Edition Miller Solutions ManualDestinyHardymaps100% (52)
- Nursing Pediatric Case StudyDocument9 pagesNursing Pediatric Case StudyKJay Solijon100% (1)
- Chest Tube ThoracostomyDocument5 pagesChest Tube ThoracostomyChristine AduvisoNo ratings yet