100% found this document useful (9 votes)
4K views5 pagesCardiovascular Drug Classifications
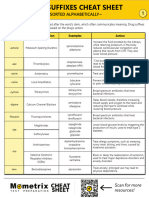
This document summarizes several classes of cardiovascular medications including their mechanisms of action, examples, uses in treating various cardiac conditions, monitoring parameters, and potential side effects. ACE inhibitors work by decreasing the conversion of angiotensin I to angiotensin II and are used to treat hypertension, heart failure, and arrhythmias. Beta blockers decrease heart rate and conduction and are used for hypertension, angina, arrhythmias. Calcium channel blockers decrease conduction and are used for hypertension, angina, and arrhythmias.
Uploaded by
Nichole ColettaCopyright
© © All Rights Reserved
We take content rights seriously. If you suspect this is your content, claim it here.
Available Formats
Download as PDF, TXT or read online on Scribd
Topics covered
- ACE inhibitors,
- Beta blockers,
- K+ channel blockers,
- Cardiotonics,
- Direct vasodilators,
- Statin drugs,
- Antiplatelet,
- Anticoagulation,
- Anticholinergic,
- Heart failure
100% found this document useful (9 votes)
4K views5 pagesCardiovascular Drug Classifications
This document summarizes several classes of cardiovascular medications including their mechanisms of action, examples, uses in treating various cardiac conditions, monitoring parameters, and potential side effects. ACE inhibitors work by decreasing the conversion of angiotensin I to angiotensin II and are used to treat hypertension, heart failure, and arrhythmias. Beta blockers decrease heart rate and conduction and are used for hypertension, angina, arrhythmias. Calcium channel blockers decrease conduction and are used for hypertension, angina, and arrhythmias.
Uploaded by
Nichole ColettaCopyright
© © All Rights Reserved
We take content rights seriously. If you suspect this is your content, claim it here.
Available Formats
Download as PDF, TXT or read online on Scribd
Topics covered
- ACE inhibitors,
- Beta blockers,
- K+ channel blockers,
- Cardiotonics,
- Direct vasodilators,
- Statin drugs,
- Antiplatelet,
- Anticoagulation,
- Anticholinergic,
- Heart failure