Professional Documents
Culture Documents
Lec 3 Heart Failure
Uploaded by
Delete Account0 ratings0% found this document useful (0 votes)
17 views25 pagesOriginal Title
Lec 3 Heart Failure (1)
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
17 views25 pagesLec 3 Heart Failure
Uploaded by
Delete AccountCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 25
Heart Failure
Heart failure describes
the clinical syndrome that
develops when the heart
cannot maintain
adequate output
The heart cannot meet
the functional need of the
body
In mild to moderate forms
of heart failure, symptoms
occur only when the
metabolic demand
increases during exercise
or some other form of
stress.
In severe heart failure,
symptoms may be
present at rest.
Epidemiology
Heart failure predominantly affects the elderly;
the prevalence rises from 1%in those aged50–
59years to over10%in those aged 80–89years.
In the UK ,most patients admitted to hospital
with heart failure are more than70years old.
untreated heart failure generally carries a poor
prognosis; approximately50%of patients with
severe heart failure due to left ventricular
dysfunction will die within2years.
An accurate diagnosis is important because
treatment of the underlying cause may reverse
heart failure or prevent its progression.
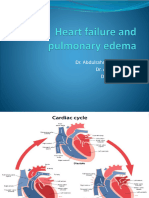
Cardiac Physiology
Frank-starling Mechanism
The Frank-Starling law of
the heart states that as
the ventricular volume
increases and stretches
the myocardial muscle
fibers, the stroke volume
increases, up to its
maximum capacity. After
that point, increasing
volume increases
pulmonary capillary
pressure (and pulmonary
congestion), without
increasing the stroke
volume or cardiac
output..
causes of heart failure
1. Coronary artery disease.
Narrowed arteries may
limit your heart's supply
of oxygen-rich blood,
resulting in weakened
heart muscle.
2. Heart attack.
3. Heart valve disease.
4. High blood pressure.
5. Irregular heartbeats.
6. Congenital heart
disease.
7. Diabetes.
FB5'F (F6H-J)
'D/E
6JB 'DFA3 'D'67,'9J
Acute and chronic heart failure
left and right heart failure signs and symptoms
Investigations
1.ECG
Determine the etiology( Ischemic Heart Disease,
Valvular heart disease, Cardiomyopathy).
Assess the severity( measuring the ejection
fraction EF >55%)
Follow up response to treatment.
2.chest X-ray
3.Urea, creatinine, electrolytes( Na , K, Mg)
4.Hemoglobin , PCV.
5.Thyroid function test.
6.Brain natriuretic peptide (BNP) is elevated in heart
failure and can be used as a screening test in
breathless patients and those with edema
Stage of Heart failure
Management of Acute heart failure
Acute heart failure with pulmonary oedema is a
medical emergency that should be treated urgently.
The patient should initially be kept rested, with
continuous monitoring of cardiac rhythm, BP and
pulse oximetry.
IV opiates can be of value in distressed patients but
must be used sparingly, as they may cause
respiratory depression
inotropic agents such as dobutamine (2.5–10
μg/kg/min) may be required to augment cardiac
output, particularly in hypotensive patients.
Insertion of an intra-aortic balloon pump may be
beneficial in patients with acute cardiogenic
pulmonary oedema and shock.
Management of chronic heart failure:
1- diuretics:
urinary sodium and water excretion
reduction in blood plasma volume
reduces preload
improves pulmonary and systemic venous congestion.
reduce Afterload
2-Mineralocorticoid receptor antagonists, such as
spironolactone is potassium-sparing diuretics ( may cause
Hyperkalemia).
3- Angiotensin-converting enzyme inhibitors ( ACE-inhibitors)
4- Angiotensin receptor blockers ARBs
5- Vasodilators
Venodilators, such as nitrates, reduce preload
arterial dilators, such as hydralazine, reduce Afterload.
Management of chronic heart
failure:
6- Beta-adrenoceptor blockers:
increase ejection fraction
improve symptoms
reduce the frequency of hospitalization
reduce mortality in patients with chronic heart
failure.
7- Digoxin
can be used to provide rate control in patients with
heart failure and atrial fibrillation.
8- Amiodarone
This is a potent anti-arrhythmic drug that has little
negative inotropic effect and may be valuable in
patients with poor left ventricular function.
Management of chronic heart failure:
Non-pharmacological treatments
Implantable cardiac defibrillators
Resynchronization devices
These devices are indicated in
patients with symptomatic In patients with marked intraventricular
ventricular arrhythmias and heart conduction delay, the LV and RV are paced
failure simultaneously to generate a more
coordinated LV contraction
Non-pharmacological treatments
Coronary revascularization Cardiac transplantation
Non-pharmacological treatments
Ventricular assist devices
complications of Heart failure
1. Renal failure.
2. Hypokalaemia.
3. Hyperkalaemia.
4. Hyponatraemia- It is a poor prognostic sign.
5. Impaired liver function.
6. Thromboembolism ( DVT )
7. Atrial and ventricular arrhythmias, electrolyte
changes (e.g. Hypokalaemia, hypomagnesaemia),
underlying structural heart disease, pro-arrhythmic
effects of increased circulating catecholamines ,
drugs (e.g. Digoxin)
You might also like
- Nursing Care Plan For Insufficient Breastmilk NCPDocument2 pagesNursing Care Plan For Insufficient Breastmilk NCPderic100% (17)
- MCAT MiniTest EbookDocument36 pagesMCAT MiniTest Ebookgood0% (2)
- Usmle Pharmacology Quiz Multiple ChoiceDocument42 pagesUsmle Pharmacology Quiz Multiple ChoiceSamer Khodor83% (6)
- Heart Failure: Low Output HF High Output HFDocument7 pagesHeart Failure: Low Output HF High Output HFJake BurrNo ratings yet
- Basic Science OITE ReviewDocument91 pagesBasic Science OITE ReviewICH KhuyNo ratings yet
- Pathophysiology of CholecystitisDocument2 pagesPathophysiology of CholecystitisAnonymous gDp7y3Cl86% (21)
- HF DeaDocument53 pagesHF DeaSyifa Mahmud Syukran AkbarNo ratings yet
- Cardiac Failure: Dr. Abdul Ghani WaseemDocument33 pagesCardiac Failure: Dr. Abdul Ghani WaseemFarwaNo ratings yet
- Systolic Dysfunction:: Types of Heart FailureDocument13 pagesSystolic Dysfunction:: Types of Heart FailureElisabeth F. OjhaNo ratings yet
- Heart Failure and ShockDocument34 pagesHeart Failure and Shockfrenee aradanasNo ratings yet
- Heart Failure in ChildrenDocument47 pagesHeart Failure in ChildrenDr.P.NatarajanNo ratings yet
- Acute Heart FailureDocument18 pagesAcute Heart FailureGeorge GeorgeNo ratings yet
- Cardiovascular DisordersDocument38 pagesCardiovascular Disordersmark100% (4)
- Heart Failure IntroductionDocument12 pagesHeart Failure IntroductionJasper VictoryNo ratings yet
- Treating Heart Failure: Current Guidelines for Pharmacological ManagementDocument11 pagesTreating Heart Failure: Current Guidelines for Pharmacological ManagementKareem SaeedNo ratings yet
- Chronic Heart FailureDocument11 pagesChronic Heart FailurelaydyNo ratings yet
- Tutorial KMB1 - 3C5 - Senin 18 Oktober 2021.id - enDocument8 pagesTutorial KMB1 - 3C5 - Senin 18 Oktober 2021.id - enNamulondo Mwajib BogereNo ratings yet
- Management of Heart Failure: DR Ambakederemo TE Consultant Physician/cardiologist NduthDocument71 pagesManagement of Heart Failure: DR Ambakederemo TE Consultant Physician/cardiologist NduthPrincewill SeiyefaNo ratings yet
- Mrs RockhartDocument4 pagesMrs RockhartClark BaldwinNo ratings yet
- Unit 2 Heart Failure: StructureDocument29 pagesUnit 2 Heart Failure: StructurebtaleraNo ratings yet
- High output heart failure: a reviewDocument7 pagesHigh output heart failure: a reviewChanvira Aria CandrayanaNo ratings yet
- Pedal EdemaDocument45 pagesPedal Edemafirdaushassan2112No ratings yet
- Pharmacology II Sovan Sarkar 186012111012Document14 pagesPharmacology II Sovan Sarkar 186012111012Sovan SarkarNo ratings yet
- Heart Failure: Causes, Symptoms, and TreatmentDocument36 pagesHeart Failure: Causes, Symptoms, and TreatmentnathanNo ratings yet
- Heart Failure and Pulmonary EdemaDocument60 pagesHeart Failure and Pulmonary EdemaYosra —No ratings yet
- Heart FailureDocument13 pagesHeart Failuremildred alidon100% (2)
- Heart Failure New SlidesDocument41 pagesHeart Failure New SlidesjawadNo ratings yet
- In Partial Fulfillment of The Requirements in Medical Ward RotationDocument5 pagesIn Partial Fulfillment of The Requirements in Medical Ward RotationEiz CabreraNo ratings yet
- Chapter 33 HypertensionDocument5 pagesChapter 33 HypertensiongytmbiuiNo ratings yet
- Congestive Heart Failure (CHF) : BY Miss. S. D. Ajetrao Assistant Professor ADCDP, AshtaDocument16 pagesCongestive Heart Failure (CHF) : BY Miss. S. D. Ajetrao Assistant Professor ADCDP, AshtaChandraprakash JadhavNo ratings yet
- Drugs Used in Heart Failure: Pharmacology (2) PHAR 342Document19 pagesDrugs Used in Heart Failure: Pharmacology (2) PHAR 342Dana HamarshehNo ratings yet
- Nursing Study GuideDocument21 pagesNursing Study GuideYanahNo ratings yet
- Nur 111 Session 7 Sas 1Document8 pagesNur 111 Session 7 Sas 1Zzimply Tri Sha UmaliNo ratings yet
- Heart Failure: Presentation by Dr. Tooba ShahbazDocument30 pagesHeart Failure: Presentation by Dr. Tooba ShahbazTooba ShahbazNo ratings yet
- Heart FailureDocument39 pagesHeart FailureMuhammad AsifNo ratings yet
- Gagal JantungDocument101 pagesGagal JantungAde Fitriyani LubisNo ratings yet
- СердечнаяDocument70 pagesСердечнаяDaniel FunkNo ratings yet
- Signs and SymptomsDocument16 pagesSigns and SymptomsRose AnnNo ratings yet
- HHFFDocument56 pagesHHFFNesru Ahmed AkkichuNo ratings yet
- What Is Cardiogenic Shock?Document3 pagesWhat Is Cardiogenic Shock?nipheyy dananNo ratings yet
- Cardiac Failure & Myocardial Infarction GuideDocument6 pagesCardiac Failure & Myocardial Infarction GuideDaniel GeduquioNo ratings yet
- LAS 4 Drugs For HypertensionDocument28 pagesLAS 4 Drugs For HypertensionMuhammad Haroon RazaNo ratings yet
- Heart Failure: DR Kaem Shir AliDocument24 pagesHeart Failure: DR Kaem Shir AliMwanja MosesNo ratings yet
- Heart FailureDocument8 pagesHeart FailureSophia MarieNo ratings yet
- Cardaic ArrestDocument17 pagesCardaic ArrestM Farhad KhaniNo ratings yet
- Broken Heart Syndrome: DiagnosticsDocument25 pagesBroken Heart Syndrome: DiagnosticsOlga Goryacheva100% (1)
- Lec 2 Heart Failure, Angina and Arryth2Document19 pagesLec 2 Heart Failure, Angina and Arryth2Adel AlomarNo ratings yet
- Heart FailureDocument28 pagesHeart FailureNabeel ShahzadNo ratings yet
- Cardiac FailureDocument63 pagesCardiac FailureNina OaipNo ratings yet
- ThiroidDocument9 pagesThiroidAhmed EmadNo ratings yet
- Update: Review and Update On Inotropes and VasopressorsDocument9 pagesUpdate: Review and Update On Inotropes and VasopressorsMaryam JamilahNo ratings yet
- Heart To HeartDocument110 pagesHeart To HeartmahyorwaNo ratings yet
- Ipd - KardiologiDocument116 pagesIpd - KardiologiWynda MuljonoNo ratings yet
- Congestive Cardiac Failure Causes, Symptoms & TreatmentDocument24 pagesCongestive Cardiac Failure Causes, Symptoms & TreatmentFarheen KhanNo ratings yet
- Heart FailureDocument17 pagesHeart FailureIsna IndahNo ratings yet
- The Heart-1Document30 pagesThe Heart-1Ebuka AniNo ratings yet
- Cardiac Failure: by Dr. Osman BukhariDocument48 pagesCardiac Failure: by Dr. Osman BukhariIrfandy Chairi Sulaiman LubisNo ratings yet
- Cardiogenic Shock Causes and TreatmentDocument5 pagesCardiogenic Shock Causes and Treatmental-obinay shereenNo ratings yet
- Comprehensive Study of Beta BlockersDocument40 pagesComprehensive Study of Beta Blockersapi-369859880% (5)
- Heart FailureDocument9 pagesHeart Failuregmqkxq6wshNo ratings yet
- CHF NanananananananannaDocument19 pagesCHF NanananananananannaKhairatul Laila INo ratings yet
- Congestive Heart Failure ReportDocument6 pagesCongestive Heart Failure ReportSunshine_Bacla_4275100% (1)
- ArrthymiasDocument11 pagesArrthymiasSyafiq AbeNo ratings yet
- Manage Cardiac EmergenciesDocument56 pagesManage Cardiac Emergencies21rayhanf100% (1)
- Atrial Fibrillation A Simple Guide to The Condition, Treatment And Related DiseasesFrom EverandAtrial Fibrillation A Simple Guide to The Condition, Treatment And Related DiseasesRating: 4 out of 5 stars4/5 (1)
- 1 Metabolic Response To InjuryDocument15 pages1 Metabolic Response To InjuryDelete AccountNo ratings yet
- Stats About Employee Feedback 160511221043Document17 pagesStats About Employee Feedback 160511221043Delete AccountNo ratings yet
- X-Rays Final ExamDocument32 pagesX-Rays Final ExamDelete AccountNo ratings yet
- Red Complex Polymicrobial Conglomerate in Oral FloDocument7 pagesRed Complex Polymicrobial Conglomerate in Oral FloDelete AccountNo ratings yet
- Tiroiditis Subakut PDFDocument8 pagesTiroiditis Subakut PDFAdeh MahardikaNo ratings yet
- Activity Sheet For Lab 2 On Gram's StainingDocument5 pagesActivity Sheet For Lab 2 On Gram's Stainingfranyce thomasNo ratings yet
- Hba1C: A Review of Non-Glycaemic Variables: Leon Campbell, Tessa Pepper, Kate ShipmanDocument8 pagesHba1C: A Review of Non-Glycaemic Variables: Leon Campbell, Tessa Pepper, Kate ShipmanDerison MarsinovaNo ratings yet
- Anatomy Catalogue 2017 PDFDocument4 pagesAnatomy Catalogue 2017 PDFujala singhNo ratings yet
- NovorapidDocument16 pagesNovorapidRADITA MAULASARINo ratings yet
- PCODDocument18 pagesPCODsandeepv08No ratings yet
- GAD65Ab Prevalence in Children with T1DMDocument5 pagesGAD65Ab Prevalence in Children with T1DMAdrian KhomanNo ratings yet
- CBSE Class 8 Science Chapter 10 Reaching The Age of Adolescence Objective QuestionsDocument10 pagesCBSE Class 8 Science Chapter 10 Reaching The Age of Adolescence Objective Questionsg c lallNo ratings yet
- Tutorial - Metabolism and Fatigue (Student Notes)Document2 pagesTutorial - Metabolism and Fatigue (Student Notes)Ronak SinaeiNo ratings yet
- Journal Club-Stage 4 NB - Presented by TANVIRDocument15 pagesJournal Club-Stage 4 NB - Presented by TANVIRTanvir AhammedNo ratings yet
- Reactivos Pictus 700Document4 pagesReactivos Pictus 700Marco Antonio Sandoval NinaNo ratings yet
- Fisiologi Sistem Pencernaan: Kristanti, DRDocument64 pagesFisiologi Sistem Pencernaan: Kristanti, DRFeny Maharani100% (1)
- Pi AminolebanDocument1 pagePi AminolebanPatricia DalanNo ratings yet
- Non-Alcoholic Fatty Liver Disease (NAFLD) : A Review of Epidemiology, Risk Factors, Diagnosis and ManagementDocument16 pagesNon-Alcoholic Fatty Liver Disease (NAFLD) : A Review of Epidemiology, Risk Factors, Diagnosis and Managementdekatria 2020No ratings yet
- Drug Levothyroxine SodiumDocument2 pagesDrug Levothyroxine SodiumSrkocher0% (1)
- 11 Series TNCDocument32 pages11 Series TNCPoonam Yadav roll no.53No ratings yet
- Hipertiroidismo en GatosDocument20 pagesHipertiroidismo en GatosBrenda GómezNo ratings yet
- Best Practice & Research Clinical Obstetrics and GynaecologyDocument12 pagesBest Practice & Research Clinical Obstetrics and GynaecologyMariana HernandezNo ratings yet
- The Digestive SystemDocument4 pagesThe Digestive SystemAngelica Carrillo-Contreras100% (1)
- Autoimmune Disorders: CausesDocument2 pagesAutoimmune Disorders: CausesMaxNo ratings yet
- CrossWards USMLE Step 2 Board Review PDFDocument210 pagesCrossWards USMLE Step 2 Board Review PDFICH KhuyNo ratings yet
- Skenario F Blok 23Document71 pagesSkenario F Blok 23Fatimah Shellya ShahabNo ratings yet
- Differences in Uric Acid Levels Between Perimenopausal and Menopausal WomenDocument4 pagesDifferences in Uric Acid Levels Between Perimenopausal and Menopausal Womenria kartini panjaitanNo ratings yet
- Maternal Blood Folate Status During Early Pregnancy and Occurrence of Autism Spectrum Disorder in Offspring A Study of 62 Serum BiomarkersDocument15 pagesMaternal Blood Folate Status During Early Pregnancy and Occurrence of Autism Spectrum Disorder in Offspring A Study of 62 Serum BiomarkersmaxNo ratings yet
- Edexcel International GCSE (9-1) Biology Student Book-58Document1 pageEdexcel International GCSE (9-1) Biology Student Book-58Mominul HaqueNo ratings yet