Professional Documents
Culture Documents
Lymph Full
Uploaded by
mayada elmakkiOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Lymph Full
Uploaded by
mayada elmakkiCopyright:
Available Formats
Lymphoscintigraphic Mapping in Melanoma and Breast
Cancer
Madelene A. Young
Cuyahoga Community College, Parma, Ohio
CE credit: For CE credit, you can access the test for this article, as well as additional JNMT CE tests, online at https://www.snmmilearningcenter.org.
Complete the test online no later than December 2023. Your online test will be scored immediately. You may make 3 attempts to pass the test and must
answer 80% of the questions correctly to receive 1.0 CEH (Continuing Education Hour) credit. SNMMI members will have their CEH credit added to their VOICE
transcript automatically; nonmembers will be able to print out a CE certificate upon successfully completing the test. The online test is free to SNMMI members;
nonmembers must pay $15.00 by credit card when logging onto the website to take the test.
The SLN is the nodal site of potential micrometastasis.
In determining the best options for lymphoscintigraphy, inves- SLNs are the main focus of lymphoscintigraphy because
tigators have tried many different radiopharmaceuticals and these nodes indicate where malignant cells will spread first.
protocols. There are varying opinions on the best route of ad- This knowledge defines the route of potential treatment and
ministration, timing for delayed images, and radiopharmaceuti-
the prognosis for melanoma patients. The presence of re-
cal. Debate around which radiopharmaceutical is best arises
from the requirement that it clear from healthy lymph channels gional lymph node involvement is the single most impor-
quickly enough to reveal the SLN. This paper reviews and com- tant prognostic factor. Assessing how far the tracer has
pares 9 recognized publications on lymphoscintigraphy, illus- traveled also indicates how far the malignancy has traveled.
trates the different preferences regarding the procedure, and SLNs are the first draining node in the lymphatic chain.
describes the generally accepted protocols for the best way These chains are normal free-flowing channels throughout
to locate the sentinel lymph node. Detailed explanations are
the entire body. By identifying the SLN, or where the
given for the variable involvement of the sentinel lymph node
and the variations in disease stage seen with different protocols.
lymph fluid travels first in the body, one can map the route
All discrepancies between protocols are supported with evidence of the malignancy. The presence of an SLN on lymphoscin-
such as positive results or false-positive results. On reading this tigraphy images does not indicate that a malignancy has
paper, you will be able to form an opinion on the best protocols been found. But by locating this node, surgeons can remove
and radiopharmaceuticals and learn why lymphoscintigraphy is a it and send a sample to be tested for malignancy.
crucial tool in improving a patient’s prognosis. Lymphoscintigraphy assesses obstruction, flow, and ma-
Key Words: sentinel lymph node; lymph node mapping; lignancy in lymph nodes. The theory of lymph node mapping
melanoma entails injecting a radioactive tracer and performing imaging
J Nucl Med Technol 2020; 48:311–314 to follow the route of the tracer, determine where it builds up,
DOI: 10.2967/jnmt.120.246918 and see how far it can travel. Lymphoscintigraphy relies on
the SLN and lymphatic channels in the individual patient.
There are thousands of cellular and physical differences
between human beings. Malignancies that travel in lymph
L ymphoscintigraphy is used to track how malignant
cells travel in lymph channels throughout the body. The
channels are among the most dangerous, and the exact
placement of every SLN varies between individuals. Re-
gionally, lymph nodes are typically found in standard areas
lymph vessels that carry malignant cells follow patterns
from patient to patient. This standardized, regional flow
and trails yet are still unique to each type of malignancy.
gives the familiar patterns in which SLNs are commonly
Different radiopharmaceuticals and techniques impact
found; however, discovery of abnormal SLNs is not unusual.
how adequately we can locate the sentinel lymph node
(SLN). CLASSIFICATION OF MELANOMA
Melanoma, a common cancer, begins in the pigmented
(dark) cells in the skin called melanocytes. More than
Received Apr. 9, 2020; revision accepted Jul. 9, 2020. 70,000 patients are diagnosed with—and over 9,000 die
For correspondence or reprints contact: Madelene A. Young, Department
of Nuclear Medicine, Cuyahoga Community College, West Campus, Parma,
from—melanoma yearly (1). Malignant melanoma is clas-
OH 44130. sified as superficial spreading, nodular, lentigo maligna, or
E-mail: madeleneyoung108@gmail.com
Published online Sep. 4, 2020.
acral lentiginous (1). In Table 1 these subtypes are shown
COPYRIGHT © 2020 by the Society of Nuclear Medicine and Molecular Imaging. according to their growth patterns and potential for spread.
LYMPHOSCINTIGRAPHIC MAPPING • Young 311
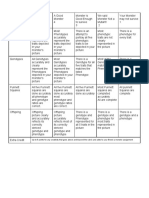
TABLE 1
Differences in Melanoma Subtypes, Their Impact on the Body, and Who Is Most at Risk
Subtype Incidence Location Growth pattern Metastasis potential Sex most at risk
Superficial spreading 70% Non–weight-bearing Slow and radial Low Women
surfaces of foot
Nodular 15%–30% Non–weight-bearing Rapid and vertical High Men
surfaces of foot
Lentigo maligna 4%–10% Anterior lower leg in Slow and radial Low Women
women; head and
trunk in men
Acral lentiginous 2%–8% Palms, soles, nail beds Radial at first, High Women
then vertical
Each subtype follows a different metastatic spreading syringes; these 4 injections surround the lesion. The acquisi-
pattern. tion parameters depend on the region of interest (ROI). The
camera is placed over the ROI and acquires a dynamic image
MELANOMA IMAGING TECHNIQUES for 30–60 min (6). Static images, in both axillary and inguinal
Many variables impact the quality of lymphoscintigraphic views, of the ROI and of any visualized lymph nodes are taken
findings for melanoma. Its location and type, preparation of the for 5–10 min. Images of the head and neck should be both
radiopharmaceutical, injection technique, and image views are anterior and posterior. Additional views, such as oblique, can
crucial to the quality and consistency of the findings. The be acquired as needed, or SPECT images can be obtained. The
radiopharmaceutical injection relies on the lymphatic system’s location of the SLN is marked on the skin. It is not advisable
ability to transport large molecules from the interstitial spaces to acquire images at more than 15 h after injection (6). Figure
back to the vascular system (2). Differences in molecule size 1 shows an example of lymph node localization in the groin;
present different challenges, such as lymphatic response time. the melanoma is in the thigh region.
Responses that are too quick cannot be captured on a nuclear Additional options in the standardized protocol include
using a transmission source, such as 57Co, to delineate the
image. Responses that are too slow make it difficult to find an
body contour of the patient. Radioactive markers may also
SLN.
be used as reference points to provide more anatomic in-
The ideal imaging agents for lymphoscintigraphy of cuta-
formation. Anatomic reference points are subject to inter-
neous melanoma clear rapidly from the injection site into the
pretation; however, when a transmission source is included,
lymphatic system, expose the patient to only a low radiation
the body contour is illuminated. The effect is similar to that
dose, are retained well within the lymph nodes, and have the
of a SPECT image, in that it provides more than just counts
correct particle size (depending on targeted findings). per image; the contour of the body is visible and can help
Two main types of tracers are used: macromolecules and guide interpretations. Usually, patients undergo surgery after
colloidal suspensions. Small particles (,100 nm) clear from lymphoscintigraphy procedures. This transmission-source
the interstitial spaces, whereas larger particles (.500 nm) body-contour image can be referenced by the surgeon to
tend to remain at the injection site (3). 99mTc-labeled col- confirm the target lymph node.
loids clear more slowly from the injection site than macro-
molecules and do not show lymphatic vessels in great detail CLASSIFICATION OF BREAST LESIONS
(4). However, colloidal suspensions are trapped much more
Malignant breast lesions are classified into 5 groups. (B-
effectively in lymph nodes, making them more suitable for
Coding System; established by the NHS Breast Cancer
lymph node mapping (4). Because the amount of radioactivity
Screening Program). B1 is normal tissue that does not require
injected into the patient is microscopic (,37 MBq [1 mCi]),
the radiation dose to the patient is often considered insignifi-
cant (5). Regardless of the tracer used, the injection technique
is crucial. Injection of too large a quantity may slow uptake of
the radiopharmaceutical and contaminate the patient’s skin.
Different tracers have different uptake times. Uptake time is
also impacted by the quality of the injection.
The standardized protocol of the Society of Nuclear
Medicine and Molecular Imaging for melanoma lympho-
scintigraphy (6) uses 99mTc-labeled filtered sulfur colloid
FIGURE 1. Leg melanoma with visualized node in groin. This
or 99mTc-tilmanocept (Lymphoseek; Cardinal Health). The image shows localization of SLN in groin area when injection is
target dose is 15 MBq (0.5 mCi), administered intradermally performed at thigh. Image provides idea of generalized regions
or subcutaneously. The dose is divided equally among 4 in which lymph nodes are frequently found.
312 JOURNAL OF NUCLEAR MEDICINE TECHNOLOGY • Vol. 48 • No. 4 • December 2020
further diagnostic testing. B2 is benign lesions that have been followed in preoperative and postoperative scans, 85% of
biopsied and have completed diagnostic testing. B3 is lesions patients have consistency between the two, identifying the
with potential for malignancy, including papillary lesions, scar same SLN. Differing protocols may lead to false identifi-
tissue, and classic lobular neoplasia; biopsy is necessary cation or a missed malignant node.
for B3 lesions to determine further action. B4 is malignancy, The definition of an abnormality also varies among institu-
or invasive carcinoma, that has been confirmed through biopsy tions, thus affecting staging, treatment plan, and prognosis. If
and diagnostic imaging. B5 lesions are malignant in situ, in- images are taken at 0, 30, 120, and 240 min at one institution
vasive and employ unequivocal malignant process; additional but at 0, 60, and 240 min at another location (both protocols
organs and systems are often involved when B5 lesions are are widely used), comparison between patient images will be
confirmed. misleading. The radiopharmaceuticals used should also be
standardized. If one institution scans with smaller particles
BREAST IMAGING TECHNIQUES
and another with larger particles, the smaller particles will
Similar to lymphoscintigraphy imaging of melanoma, appear to travel farther than the larger ones. Use of the wrong
lymphoscintigraphy imaging of the breast uses many particle size can give a false-negative if large particles
different protocols, which lead to differing results. The ra- remain at the injection site, leading physicians to believe the
diopharmaceuticals used are the same as for melanoma malignant cells are not likely to spread.
lymphoscintigraphy: 99mTc-labeled filtered sulfur colloid Nissenkorn compared the use of whole-body lympho-
or 99mTc-tilmanocept. The dose administered is also about scintigraphy, lymphangiography, and CT to evaluate for
the same, ranging from 15 MBq (0.5 mCi) to 35 MBq (1.0 mCi). metastasis. A correct diagnosis was made in 61.5% of patients,
Injections should be subareolar or peritumoral, surrounding whereas 23.1% had false-positive results. False-positive results
the ROI. In the standardized protocol of the Society of Nuclear were twice as common for lymphoscintigraphy as for
Medicine and Molecular Imaging (7), the acquisition includes lymphangiography and CT (9). This result demonstrates
a 30-min dynamic image and static images from 10–15 min that even within the same health-care facility, lymphoscin-
per view. The tracer is to be administered 0.25–3 h before tigraphy procedures can be inconsistent.
surgery, and no imaging should be performed 15 h post The standardization of lymphoscintigraphy protocols
injection (8). will advance this modality to the point that it may surpass
The imaging findings are usually confined to the other modalities. If physicians can compare studies that are
axillary area. Figure 2 illustrates images showing an performed according to the same protocol worldwide, more
SLN in the axilla. The depth of the lymph node is what patients will receive accurate treatment and preventative
makes this study more difficult to read. Even if SLNs are measures.
clearly seen to be in the axillary region, the reading phy-
sician cannot pinpoint the lymph node for excision if the PRACTICAL USES FOR LYMPHOSCINTIGRAPHY
body contour is not visible. Figure 3 illustrates images that
Lymphoscintigraphy is also a preoperative tool. The
were obtained using a transmission source and show the
images can identify and localize lymph node involvement
body contour.
before nodovenous shunt procedures, SLN biopsies, and
DOWNSIDES TO LYMPHOSCINTIGRAPHY lymph node dissection. SLN biopsy is the most commonly
used procedure in conjunction with lymphoscintigraphy.
Although lymphoscintigraphy clearly has many uses and
Early-stage abnormalities may also be detected in unsus-
benefits, such as tracking cancer before it has spread
pected areas when comparing the whole-body images with
beyond borders, the lack of a standardized protocol hinders
specific regions defined by lymphoscintigraphy images.
its full potential. Since lymphatics are unpredictable, it is
Lymphedema patients are also the subject of a large percentage
imperative that the same protocol be used when lympho-
of lymphoscintigraphy studies. Assessment of lymphatic drain-
scintigraphy is repeated in a patient. Postoperative scans are
done at the 3- to 6-mo mark. If the same protocol is age pinpoints where the channels are not draining properly.
This malfunction causes a buildup of fluid, which is often
painful. Lymphedema is very treatable or can be managed to
a functional state once the ROI is defined (8). Knowledge of
the ROI through lymphoscintigraphy can be used to repair
specific sites rather than treating the entire affected area.
Imaging technique is also crucial, considering the views
taken are to be compared before and after therapy or
surgery. Lymphoscintigraphy has improved the accuracy of
melanoma staging using SPECT/CT and PET/CT. Many of
FIGURE 2. Breast lesion with visualized lymph node in axilla.
the lymphatic drainage routes assessed by lymphoscintigraphy
Compare with Figure 3 to see benefits of using transmission and SPECT/CT correspond to sites of lymph node metastases.
source when imaging SLNs. The acquisitions differ in timing, position, and field of view.
LYMPHOSCINTIGRAPHIC MAPPING • Young 313
For example, although the use of
99mTc-labeled filtered sulfur colloid
allows tracking of melanoma and
breast cancer, the use of a different
tracer might enable tracking of other
types of malignancy. The field of lym-
phoscintigraphy is advancing every day,
yet inconsistency in protocols may hinder
its future potential.
DISCLOSURE
No potential conflict of interest rele-
vant to this article was reported.
ACKNOWLEDGMENT
I thank Catherine Bloor, BS, RT
(N), and James Fisher BS, CNMT,
RSO, for supporting this research.
FIGURE 3. Breast lesion lymphoscintigraphy with 57Co transmission source (7). This
image shows how transmission source can be effective tool when trying to relate
internal node to external site on body. By showing body outline, image makes it REFERENCES
easier to mark node for surgery. A 5 SLN from lateral view; B and C 5 other 1. Weiss J, Bertz J, Jung EG. Malignant melanoma in
significant nodes, from anterior view, in ROI. These nodes may also be removed for southern Germany: different predictive value of risk
biopsy. factors for melanoma subtypes. Dermatologica.
1991;183:109–113.
2. Yudd AP, Kempf JS, Goydos JS, Stahl TJ, Feinstein RS.
Flood sources are used to define the body contour, allowing Use of sentinel node lymphoscintigraphy in malignant melanoma. Radiographics.
depiction of more centrally located lymph nodes and delineation 1999;19:343–353.
3. Perissinotti A, Rietbergen DD, Vidal-Sicart S, Riera AA, Olmos RAV. Melanoma &
of the nodes from the lymphatic channels. nuclear medicine: new insights & advances. Melanoma Manag. 2018;5:MMT06.
Internationally, lymphoscintigraphy is being performed 4. Melanoma. SNMMI website. http://www.snmmi.org/AboutSNMMI/Content.aspx?
at thousands of institutions using hundreds of protocols. The ItemNumber5995. Accessed September 28, 2020.
5. Kaplan WD, Davis MA, Rose CM. A comparison of two technetium-99m-labeled
resulting inconsistency between images makes comparisons radiopharmaceuticals for lymphoscintigraphy: concise communication. J Nucl
unreliable. Standardizing the protocol for such a widely used Med. 1979;20:933–937.
imaging modality would enable physicians to consult similar 6. Alazraki N, Glass EC, Castronovo F, Olmos RA, Podoloff D; Society of Nuclear
Medicine. Procedure guideline for lymphoscintigraphy and the use of intraoper-
cases when diagnosing and treating melanoma patients. ative gamma probe for sentinel lymph node localization in melanoma of interme-
diate thickness 1.0. J Nucl Med. 2002;43:1414–1418.
7. Giammarile F, Alazraki N, Aarsvold J; Society of Nuclear Medicine. The EANM
THE FUTURE POTENTIAL OF LYMPHOSCINTIGRAPHY and SNMMI practice guideline for lymphoscintigraphy and sentinel node locali-
The many protocols used in lymphoscintigraphy, and the zation in breast cancer. Eur J Nucl Med Mol Imaging. 2013; 40:1932–1947.
8. Kalawat TC, Chittoria RK, Reddy PK, Suneetha B, Narayan R, Ravi P. Role of
vast diversity among patients, affect outcomes. Standard- lymphoscintigraphy in diagnosis and management of patients with leg swelling of
izing and refining protocols among institutions that share unclear etiology. Indian J Nucl Med. 2012;27:226–230.
images would allow for more accurate diagnoses. Lympho- 9. Nissenkorn I, Winkler H, Servadio C, et al. A comparative evaluation of lympho-
scintigraphy versus lymphangiography and computerized tomography scanning in
scintigraphy is a widely available modality that has the diagnosis of lymph node metastases in advanced bladder cancer. J Urol. 1986;136:
capacity to embrace the use of other radiopharmaceuticals. 825–827.
314 JOURNAL OF NUCLEAR MEDICINE TECHNOLOGY • Vol. 48 • No. 4 • December 2020
You might also like
- Salivary Gland Cancer: From Diagnosis to Tailored TreatmentFrom EverandSalivary Gland Cancer: From Diagnosis to Tailored TreatmentLisa LicitraNo ratings yet
- REVIEW. Keywords - Sentinel Lymph Node, Lymphatic Mapping, Breast Cancer, Esophageal Cancer, Less Invasive SurgeryDocument18 pagesREVIEW. Keywords - Sentinel Lymph Node, Lymphatic Mapping, Breast Cancer, Esophageal Cancer, Less Invasive SurgeryMDNo ratings yet
- Sentinel Lymph Node (SLN) Biopsy PDFDocument5 pagesSentinel Lymph Node (SLN) Biopsy PDFMDNo ratings yet
- 2021 Article 827Document39 pages2021 Article 827Ahmad TaufikNo ratings yet
- 10 REV 6767 IngDocument9 pages10 REV 6767 IngDaniel StaniloaieNo ratings yet
- Garbe2007 PDFDocument7 pagesGarbe2007 PDFArsen NitNo ratings yet
- EANM Lymphoscintigraphy GuidelinesDocument17 pagesEANM Lymphoscintigraphy Guidelinesayodeji78No ratings yet
- The Histogenesis and Biologic Behavior of Primary Human Malignant Melanomas of The Skin1Document23 pagesThe Histogenesis and Biologic Behavior of Primary Human Malignant Melanomas of The Skin1Lenutza LenutaNo ratings yet
- Malignant Melanoma Diagnosis & Treatment (2018 - 10 - 02 00 - 06 - 35 UTC)Document4 pagesMalignant Melanoma Diagnosis & Treatment (2018 - 10 - 02 00 - 06 - 35 UTC)Alexander EnnesNo ratings yet
- Pathology Clinic Nasopharyngeal CarcinomaDocument2 pagesPathology Clinic Nasopharyngeal CarcinomaTukang Gali KuburNo ratings yet
- Jurnal Lipoma Inggris 1Document9 pagesJurnal Lipoma Inggris 1Yunawan Dwi PuspoNo ratings yet
- Primary Excision Margins, Sentinel Lymph Node Biopsy, and Completion Lymph Node Dissection in Cutaneous MelanomaDocument10 pagesPrimary Excision Margins, Sentinel Lymph Node Biopsy, and Completion Lymph Node Dissection in Cutaneous MelanomaAndrés Faúndez TeránNo ratings yet
- Sentinel Lymph Node Biopsy in Breast Cancer - A Technical and Clinical AppraisalDocument7 pagesSentinel Lymph Node Biopsy in Breast Cancer - A Technical and Clinical AppraisalIris LanNo ratings yet
- Sentinel Lymph Node Mapping in High-Grade Endometrial CancerDocument13 pagesSentinel Lymph Node Mapping in High-Grade Endometrial CancerZaniru Raúl Marín MartínezNo ratings yet
- Thesis IntroductionDocument155 pagesThesis IntroductionSravani PeddagangannagariNo ratings yet
- Axillary Lymph Node Dissection in Patients With Micrometastasis in Sentinel Lymph Node New Predilections.Document12 pagesAxillary Lymph Node Dissection in Patients With Micrometastasis in Sentinel Lymph Node New Predilections.Mathew UsfNo ratings yet
- Basic Plastic + Skin CancerDocument29 pagesBasic Plastic + Skin CancermitaNo ratings yet
- Veterinary Oncology, A Short TextbookDocument6 pagesVeterinary Oncology, A Short TextbookMacarena Beatriz Piña ValenciaNo ratings yet
- Assessment of Sentinel Lymph Node Biopsy Vs Lymphadenectomy For Intermediate - and High-Grade Endometrial Cancer StagingDocument8 pagesAssessment of Sentinel Lymph Node Biopsy Vs Lymphadenectomy For Intermediate - and High-Grade Endometrial Cancer StagingEzequiel GonzalezNo ratings yet
- Artikel NPC Inggris CadanganDocument4 pagesArtikel NPC Inggris CadanganwidyalimNo ratings yet
- Thyroidcancer: Ultrasound Imaging and Fine-Needle Aspiration BiopsyDocument21 pagesThyroidcancer: Ultrasound Imaging and Fine-Needle Aspiration BiopsyPedro Gómez RNo ratings yet
- Cellular AberrationDocument83 pagesCellular AberrationA. Lizette PabloNo ratings yet
- Mengenal Gambaran Lesi Jinak, Ganas Dan Metastasis Pada Nodus Limfa Leher Menggunakan UltrasonografiDocument11 pagesMengenal Gambaran Lesi Jinak, Ganas Dan Metastasis Pada Nodus Limfa Leher Menggunakan UltrasonografiSilvia EmyNo ratings yet
- Cutaneous Melanoma - Guidelines For Diagnostics and Therapy in 2016Document17 pagesCutaneous Melanoma - Guidelines For Diagnostics and Therapy in 2016Dyerik LilingNo ratings yet
- Cytogenetic Analysis in The Diagnosis of Acute Leukemia: Sverre Heim, FelixDocument9 pagesCytogenetic Analysis in The Diagnosis of Acute Leukemia: Sverre Heim, FelixEnas KharbotlyNo ratings yet
- Managing Malignant Melanoma: Learning Objectives: After Reading This Article, The Participant Should Be AbleDocument15 pagesManaging Malignant Melanoma: Learning Objectives: After Reading This Article, The Participant Should Be AbleDian Ariska SNo ratings yet
- Applications and Safety of Sentinel Lymph Node Biopsy in Endometrial CancerDocument19 pagesApplications and Safety of Sentinel Lymph Node Biopsy in Endometrial CancerEzequiel GonzalezNo ratings yet
- Atypical Melanoma Mimicking A Vascular Tumor: Clinical and Dermoscopic FindingsDocument6 pagesAtypical Melanoma Mimicking A Vascular Tumor: Clinical and Dermoscopic FindingsIJAR JOURNALNo ratings yet
- Melanoma - PregradoDocument8 pagesMelanoma - PregradoDaniela DuránNo ratings yet
- Surgical Treatment of Melanoma: Acta Chirurgiae Plasticae April 2018Document8 pagesSurgical Treatment of Melanoma: Acta Chirurgiae Plasticae April 2018alexandru_andreaNo ratings yet
- Ijss Nov Oa28Document5 pagesIjss Nov Oa28Irsanti sasmitaNo ratings yet
- Lymphedema: Classification, Diagnosis and Therapy: Vascular Medicine 1998 3: 145-156Document12 pagesLymphedema: Classification, Diagnosis and Therapy: Vascular Medicine 1998 3: 145-156Vladislav KotovNo ratings yet
- Detection of Melanoma CellsDocument8 pagesDetection of Melanoma CellsLoredana VoiculescuNo ratings yet
- NE0PLASIADocument28 pagesNE0PLASIADaniel SutantoNo ratings yet
- MilanDocument21 pagesMilanJose Daniel Garcia AlatorreNo ratings yet
- Lymphedema Classification, Diagnosis, TherapyDocument12 pagesLymphedema Classification, Diagnosis, Therapymaevy dwiNo ratings yet
- FNAC Axillary 2012bDocument7 pagesFNAC Axillary 2012bDima PathNo ratings yet
- Management of Small Renal MassDocument5 pagesManagement of Small Renal MassAung Ko HtetNo ratings yet
- SC - Ultrasound Evaluation of Neck Lymph NodesDocument9 pagesSC - Ultrasound Evaluation of Neck Lymph NodesMihaela DragomirNo ratings yet
- Pemeriksaan Penunjang Onkologi Pada MataDocument29 pagesPemeriksaan Penunjang Onkologi Pada MatamazidahzulfaNo ratings yet
- Carcinogenesis CervicalDocument6 pagesCarcinogenesis Cervicalluz carmen herrera trilloNo ratings yet
- Update On Nasopharyngeal Carcinoma: Ó Humana 2007Document6 pagesUpdate On Nasopharyngeal Carcinoma: Ó Humana 2007Zakia AjaNo ratings yet
- MRI of The Central Lymphatic System Indications,.5Document6 pagesMRI of The Central Lymphatic System Indications,.5csánchez_167No ratings yet
- Anal Melanoma: Marc Singer, M.D. and Matthew G. Mutch, M.DDocument10 pagesAnal Melanoma: Marc Singer, M.D. and Matthew G. Mutch, M.DbkiriazovNo ratings yet
- Clinocopathological Features and Prognosis of Patients With de Novo Versus Nevus Associated Melanoma in TaiwanDocument16 pagesClinocopathological Features and Prognosis of Patients With de Novo Versus Nevus Associated Melanoma in Taiwanira nurinaNo ratings yet
- ClinCancerInvestigJ 2016 5 1 15 172029Document5 pagesClinCancerInvestigJ 2016 5 1 15 172029Yashwanth GowdaNo ratings yet
- Lymph Nodes Normal and MalignantDocument12 pagesLymph Nodes Normal and MalignantMagzNo ratings yet
- Sheet 11 PDFDocument16 pagesSheet 11 PDFHanin AbukhiaraNo ratings yet
- Alkuwari 2008Document5 pagesAlkuwari 2008ayuNo ratings yet
- 2020 - LN Imaging Breast CR - Concurrent Diagnostic Tools - MarinoDocument12 pages2020 - LN Imaging Breast CR - Concurrent Diagnostic Tools - MarinoГаянэ АллахвердянNo ratings yet
- 1 s2.0 S0002939419300625 Main PDFDocument9 pages1 s2.0 S0002939419300625 Main PDFAsti DwiningsihNo ratings yet
- The Small Fatal Choroidal Melanoma Study. A Survey by The European Ophthalmic Oncology GroupDocument9 pagesThe Small Fatal Choroidal Melanoma Study. A Survey by The European Ophthalmic Oncology GroupAsti DwiningsihNo ratings yet
- PathwaysoflymphaticspreadDocument31 pagesPathwaysoflymphaticspreadZaniru Raúl Marín MartínezNo ratings yet
- Conjunctival Pigmented LesionsDocument0 pagesConjunctival Pigmented LesionsBhartendu Agarwal0% (1)
- Lcnec Versus SCLCDocument76 pagesLcnec Versus SCLCnurul hidayahNo ratings yet
- Non-Odontogenic Tumors of Epithelial Tissue Origin: Guided By-Presented byDocument93 pagesNon-Odontogenic Tumors of Epithelial Tissue Origin: Guided By-Presented byrajaniNo ratings yet
- 1 s2.0 S0378603X13001253 MainDocument8 pages1 s2.0 S0378603X13001253 MainMoh Hidayat ThahaNo ratings yet
- Cutaneous Melanoma: Atypical Variants and PresentationsDocument6 pagesCutaneous Melanoma: Atypical Variants and PresentationsMoet Moet KhineNo ratings yet
- Atypical Spitz Tumors: A Diagnostic ChallengeDocument8 pagesAtypical Spitz Tumors: A Diagnostic ChallengeCristi PopescuNo ratings yet
- Topic Viii NeoplasiaDocument6 pagesTopic Viii NeoplasiaMarinelle TumanguilNo ratings yet
- PWSMTS Full Test - 01 - Test PaperDocument9 pagesPWSMTS Full Test - 01 - Test PaperPranav kr. PrasadNo ratings yet
- 1741 - Long Span Structures ReportDocument5 pages1741 - Long Span Structures ReportHuzefa SayyedNo ratings yet
- Non Destructive TestingDocument9 pagesNon Destructive TestingAhmed KhanNo ratings yet
- Breed A Monster RubricDocument1 pageBreed A Monster Rubricapi-495151215No ratings yet
- Pathe Projector Pathe Baby User ManualDocument23 pagesPathe Projector Pathe Baby User ManualzakskenNo ratings yet
- Rabies CaseDocument3 pagesRabies CaseanastasiaNo ratings yet
- IELTS Reading Skills & StrategiesDocument4 pagesIELTS Reading Skills & StrategiesThinn Thinn Oo100% (1)
- HFWB - 170224 - Floor StandingDocument2 pagesHFWB - 170224 - Floor StandingAkilaJosephNo ratings yet
- Electrical DrivesDocument1 pageElectrical DriveschaitanayNo ratings yet
- ABHYANGADocument2 pagesABHYANGASandeep NairNo ratings yet
- Tutorial 8: Pre-Tensioned Bolts: Laurence MarksDocument5 pagesTutorial 8: Pre-Tensioned Bolts: Laurence Marksgurpinder Singh DhaliwalNo ratings yet
- Chapter 03 Two Dimensional Problems in Elasticity - Ugural, FensterDocument50 pagesChapter 03 Two Dimensional Problems in Elasticity - Ugural, Fensteracanerk100% (6)
- LG 47ld450-Ua Chassis La01bDocument71 pagesLG 47ld450-Ua Chassis La01belrudo11100% (1)
- Capgemini TestsDocument50 pagesCapgemini TestsObli Narasimha RajanNo ratings yet
- The Anatomy and Physiology of The Stomach: Ian R. Daniels and William H. AllumDocument21 pagesThe Anatomy and Physiology of The Stomach: Ian R. Daniels and William H. Allummutia aNo ratings yet
- 005 - Romulan Warbird (D'Deridex)Document20 pages005 - Romulan Warbird (D'Deridex)Fabien Weissgerber100% (1)
- Bosvark ZL08F Front-End Loader: Key FeaturesDocument2 pagesBosvark ZL08F Front-End Loader: Key FeaturesJaco Coetzer100% (1)
- en Volvo D49Document84 pagesen Volvo D49Lucas MarquesNo ratings yet
- 21 Lesson For 21st CenturyDocument16 pages21 Lesson For 21st CenturySamia GhafoorNo ratings yet
- Work From Home Project: Peshawar Model SchoolDocument4 pagesWork From Home Project: Peshawar Model SchoolShabir RizwanNo ratings yet
- Benign Bone Tumours LectureDocument11 pagesBenign Bone Tumours Lecturekyliever100% (1)
- EMD Tools1Document55 pagesEMD Tools1Vladimir ArsicNo ratings yet
- Compound Plamar GanglionDocument4 pagesCompound Plamar Ganglionchinmayghaisas100% (2)
- Evaluation of PV-Wind Hybrid Energy System For A Small IslandDocument3 pagesEvaluation of PV-Wind Hybrid Energy System For A Small Islandhamza malikNo ratings yet
- The First Two Years of Operational Experience With The Sikorsky S-61Document6 pagesThe First Two Years of Operational Experience With The Sikorsky S-61Floyd PriceNo ratings yet
- Works) : SABS 1200Document10 pagesWorks) : SABS 1200Palesa TshetlanyaneNo ratings yet
- 2019 Iran PPRDocument10 pages2019 Iran PPRFareena FatimaNo ratings yet
- Abnormal Lie in PregnancyDocument2 pagesAbnormal Lie in PregnancyAlexander EnnesNo ratings yet
- HSE TerminologyDocument6 pagesHSE TerminologyZeshanNo ratings yet
- ASC - General - Purpose - Capacitor For HallsensorDocument19 pagesASC - General - Purpose - Capacitor For HallsensorLusiNo ratings yet
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (5)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (39)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 4 out of 5 stars4/5 (5)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 4.5 out of 5 stars4.5/5 (84)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)From EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Rating: 3 out of 5 stars3/5 (1)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (404)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeRating: 2 out of 5 stars2/5 (1)
- The Twentysomething Treatment: A Revolutionary Remedy for an Uncertain AgeFrom EverandThe Twentysomething Treatment: A Revolutionary Remedy for an Uncertain AgeRating: 4.5 out of 5 stars4.5/5 (3)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (44)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (267)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (170)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- I Shouldn't Feel This Way: Name What’s Hard, Tame Your Guilt, and Transform Self-Sabotage into Brave ActionFrom EverandI Shouldn't Feel This Way: Name What’s Hard, Tame Your Guilt, and Transform Self-Sabotage into Brave ActionNo ratings yet
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (46)
- Critical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsFrom EverandCritical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsRating: 4.5 out of 5 stars4.5/5 (39)
- The Fun Habit: How the Pursuit of Joy and Wonder Can Change Your LifeFrom EverandThe Fun Habit: How the Pursuit of Joy and Wonder Can Change Your LifeRating: 4.5 out of 5 stars4.5/5 (19)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesFrom EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesRating: 4.5 out of 5 stars4.5/5 (1412)
- Summary: How to Be an Adult in Relationships: The Five Keys to Mindful Loving by David Richo: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: How to Be an Adult in Relationships: The Five Keys to Mindful Loving by David Richo: Key Takeaways, Summary & Analysis IncludedRating: 4 out of 5 stars4/5 (11)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingFrom EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingRating: 4 out of 5 stars4/5 (1138)
- The Story of Philosophy: The Lives and Opinions of the Greater PhilosophersFrom EverandThe Story of Philosophy: The Lives and Opinions of the Greater PhilosophersNo ratings yet