Professional Documents
Culture Documents
MS Respi Disorder
Uploaded by
secondacvalo1230 ratings0% found this document useful (0 votes)
5 views10 pagesThis document discusses various respiratory diseases including their risk factors, signs and symptoms, assessment, diagnosis, and treatment. It covers upper respiratory tract infections caused by viruses like the common cold. It also discusses rhinitis, rhinosinusitis, acute and chronic pharyngitis, tonsillitis, and adenoiditis. For each condition, it provides details on potential causes, clinical presentation, evaluation methods, and medical and nursing management approaches.
Original Description:
Original Title
MS-RESPI-DISORDER
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document discusses various respiratory diseases including their risk factors, signs and symptoms, assessment, diagnosis, and treatment. It covers upper respiratory tract infections caused by viruses like the common cold. It also discusses rhinitis, rhinosinusitis, acute and chronic pharyngitis, tonsillitis, and adenoiditis. For each condition, it provides details on potential causes, clinical presentation, evaluation methods, and medical and nursing management approaches.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
5 views10 pagesMS Respi Disorder
Uploaded by
secondacvalo123This document discusses various respiratory diseases including their risk factors, signs and symptoms, assessment, diagnosis, and treatment. It covers upper respiratory tract infections caused by viruses like the common cold. It also discusses rhinitis, rhinosinusitis, acute and chronic pharyngitis, tonsillitis, and adenoiditis. For each condition, it provides details on potential causes, clinical presentation, evaluation methods, and medical and nursing management approaches.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 10
Responses to Alterations in ❖ Purulent with bacterial ▪ subacute (4 to 12
rhinitis weeks), and
oxygenation and ventilation ❖ Sneezing ▪ chronic (more than 12
❖ Pruritus of the nose roof weeks
RISK FACTORS FOR RESPIRATORY of the mouth, throat, ▪ ABRS
DISEASE eyes and ears ▪ AVRS
➢ Smoking ❖ Headache ▪ Follows viral URI, or
➢ Use of chewing tobacco ❖ rhinosinusitis unresolved viral or
➢ Allergies bacterial infection
➢ Frequent respiratory Medical Management: ▪ Drainage obstruction
illnesses - depends on the cause ▪ Deviated septum,
➢ Chest injury - Hx and Physical Examination - hypertrophied
➢ Surgery Pharmacologic management: turbinates, spurs or nasal
➢ Exposure to chemicals & - allergic and nonallergic polyps, tumors or sinus
environmental pollutants — antihistamines and infection
➢ Family history of corticosteroids nasal sprays ▪ Suppurative process
infectious disease - Dimetapp ▪ Purulent discharge
➢ Geographic residence
& travel to foreign Viral Rhinitis/ Common Cold Assessment and Diagnostic
countries ▪ most common and self- Findings
limited -history and physical examination
- head and neck, nose, ears,
Management of Patients with ▪ Rhinoviruses- most
common teeth, sinuses, pharynx, and chest
URTD - Tenderness of the sinuses
▪ Coronavirus, adenovirus,
Upper Airway Infections/ URI RSV, - Transillumination
➢ Most common cause of ▪ influenza, parainfluenza Medical Management
illness ▪ Location varies - ✓ Antibiotics- to shrink the
➢ Acute or chronic? nasal mucosa, relieve
➢ Common cold (viral S/Sx: pain, and treat infection
rhinitis) - CA: viruses ❖ low-grade fever,
➢ Affect : •nasal cavity ❖ nasal congestion, Nursing Management
•sinuses rhinorrhea and nasal - Educating Patients About Self-
Incidence rate: 2 to 4 times per discharge, Care
year ❖ halitosis, sneezing, - Report symptoms of
❖ tearing watery eyes, complications
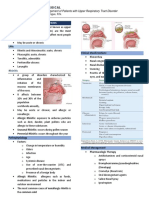
Rhinitis “scratchy” or sore - periorbital edema
throat, - severe pain on palpation
▪ inflammation and
❖ general malaise, - methods to promote drainage
irritation of the mucous
❖ chills, and often of the
membrane of the nose
headache and muscle sinuses
▪ Acute or chronic?
aches. - avoid swimming, diving, and air
▪ Allergic or nonallergic?
❖ Cough travel
▪ Seasonal or perennial?
❖ the virus exacerbates during the acute infection
Risk factors:
herpes simplex, - fever, severe headache, and
▪ Change in temperature
❖ cold sore nuchal
and humidity
rigidity—-potential complications
▪ Odors
▪ Infection; age; systemic Medical Management
disease; use of OTC -symptomatic therapy Acute Pharyngitis
-adequate fluid intake, rest, ▪ sudden painful
Allergens: prevention inflammation of the
Indoor of chilling pharynx
- dust mite feces -use of expectorants as needed ▪ adenovirus, influenza
- Dog dander -Warm salt-water gargles soothe virus,
- Cat dander the sore throat, ▪ Epstein–Barr virus, and
- Cockroach droppings - nonsteroidal antiinflammatory herpes
- Molds drugs (NSAIDs), such as aspirin or ▪ simplex virus - Bacterial
Outdoor ibuprofen,relieve aches and infection
- trees pains. ▪ GABHS
- Weeds - Antihistamines
- Grasses
-Molds Rhinosinusitis
▪ sinusitis
Signs/Symptoms: ▪ inflammation of the
❖ rhinorrhea paranasal S/Sx:
❖ nasal congestion ▪ sinuses and nasal cavity • fiery-red pharyngeal
❖ Nasal discharge ▪ acute (less than 4 membrane and tonsils,
weeks),
• Swollen lymphoid • mucus that collects in • Trismus- inability to open
follicles flecked with the throat and can be the mouth
white-purple exudate expelled by coughing, • Drooling
• enlarged and tender • difficulty swallowing. • Intense pain
cervical lymph nodes, • intermittent postnasal • Rancid breath
and no cough. drip • raspy voice
• Fever (higher than *A sore throat that is worse with • odynophagia- pain in
38.3°C swallowing in the absence of swallowing
• malaise, and sore throat pharyngitis- thyroiditis • dysphagia- discomfort in
swallowing
Assessment and Diagnostic Medical Management • otalgia-ear pain
Findings ❖ relieving symptoms
▪ Rapid antigen detection ❖ avoiding exposure to Assessment and Diagnostic
testing irritants Findings
▪ (RADT) ❖ correcting any upper • aspiration
▪ swabs that collect respiratory, pulmonary, • Intraoral ultrasound
specimens gastrointestinal, or • transcutaneous cervical
▪ from the posterior cardiac condition—--- ultrasound
pharynx and tonsil chronic cough.
▪ Negative results should Medical Management
be confirmed- culture Tonsillitis and Adenoiditis • Antimicrobial agents
• bacterial pathogens • penicillin
Medical Management include GABHS • corticosteroid therapy
▪ Viral pharyngitis- S/Sx:
supportive measures ➢ sore throat, fever, Surgical Management
▪ Bacterial pharyngitis- snoring, and difficulty • Needle aspiration
antimicrobial agents- swallowing • Incision and drainage
Penicillin V potassium ➢ Enlarged adenoids • Tonsillectomy
▪ Nutritional Therapy-liquid ➢ mouth breathing,
or soft diet earache, Nursing Management
➢ draining ears, , ✓ patient requires
Nursing Management bronchitis, foul-smelling intubation
✓ supportive measures breath, voice ✓ Cricothyroidotomy
✓ Watch out!!- dyspnea, impairment, and noisy ✓ Tracheotomy
drooling, inability to respiration ✓ Gentle gargling after the
swallow, and inability to procedure with a cool
fully open the mouth Assessment and Diagnostic normal saline gargle
Findings? Medical Management? ✓ The patient must be
Chronic Pharyngitis Nursing Management? upright and
• persistent inflammation Postoperative Care ✓ clearly expectorate
of the pharynx risk of hemorrhage forward.
Risk factors Position? ✓ patient requires
• dusty surroundings, ice collar to the neck - intubation
• use their voice to excess, Complications? ✓ Cricothyroidotomy
• suffer from chronic - fever, throat pain, ear pain, and ✓ Tracheotomy
cough, habitually use bleeding ✓ Gentle gargling after the
alcohol- tobacco procedure with a cool
Peritonsillar Abscess normal saline gargle
There are three types of chronic ▪ Quinsy- pus filled ✓ 1 or 2 hours for 24 to 36
pharyngitis: ▪ common major hours
Hypertrophic—char. by general suppurative ✓ The patient must be
thickening and congestion of the ▪ complication of sore upright and clearly
pharyngeal mucous membrane throat expectorate forward
Atrophic—probably a late stage ▪ 20 to 40 years ✓ Adequate fluid intake
of the first type (the membrane is ▪ collection of purulent
thin, whitish, glistening, and at exudate
times wrinkled) ▪ tonsillar capsule and the
Chronic granular—char. by surrounding tissues,
numerous swollen lymph follicles ▪ soft palate
on the pharyngeal wall ▪ acute tonsillar infection
▪ local cellulitis and Laryngitis
abscess Risk
S/Sx. ▪ voice abuse or exposure
• constant sense of S/Sx. to dust, chemicals,
irritation • severe sore throat smoke, and other
• fullness in the throat • fever, t pollutants or as part of a
URI
▪ gastroesophageal reflux Ventilation-Perfusion ▪ Macroatelectasis- affect
▪ Reflux laryngitis segment of a lung loss of
Relationships
▪ Pathogens? – segmental, lobar or
● Gas exchange relies on overall lung volume
S/sx: adequate perfusion of the alveoli. (visible on xray)
➢ hoarseness or aphonia ✓ Normally, the volume in
and severe cough the conducting airways, Pathophysiology
such as the trachea and ➢ nonobstructive
Medical Management bronchioles, do not atelectasis-caused by
resting the voice, participate in gas post op complications-
avoiding irritants (including exchange. reduced ventilation
smoking), resting, ● anatomical dead space ➢ obstructive atelectasis-
inhaling cool steam or an aerosol. ✓ because these obstruction in the
structures are not passage of air going to
Nursing Management designed for gas alveoli : blockage that
rest the voice and to maintain a exchange obstructs passage of air
well humidified environment ● Alveolar dead space unit to and from the alveoli -
✓ when an alveolus is not most common type.
NURSING PROCESS???? perfused ➢ reabsorption of gas
1. Assessment — enumerate!! (obstructed/collapsed), ➢ no additional air can
2. Diagnosis? Based on priority air did not arrive in enter into the alveoli
3. Planning alveolus. ➢ affected portion of the
4. Nursing Intervention ✓ because no gas lung becomes airless
a. MAINTAINING A PATENT exchange is occurring ➢ alveoli collapse:
AIRWAY ✓ ventilation exceeds obstructive
b. PROMOTING COMFORT perfusion
c. PROMOTING ■ pulmonary embolism- has dead Causes;
COMMUNICATION space ❖ foreign body, tumor
d. ENCOURAGING FLUID INTAKE ■ pulmonary infarct. ❖ altered breathing
e. MONITORING AND MANAGING patterns
POTENTIAL COMPLICATIONS ● shunt unit ❖ retained secretions,
✓ when an alveolus is pain,
inadequately ventilated ❖ alterations in small
Pulmonary Volumes and
in the presence of airway function,
Capacities perfusion (there’s a ❖ prolonged supine
1. Total Lung Capacity (TLC) supply of blood, but positioning,
✓ Max vol the lungs can alveolus is not ❖ increased abdominal
hold- 6000 mL ✓ perfusion exceeds pressure,
2. Tidal Volume (VT) ventilation ❖ reduced lung volumes
✓ Volume of one ■ pneumonia caused by:
inhalation/exhalation ■ atelectasis. Musculoskeletal,
cycle - 500 mL neurologic disorders,
3. Functional residual volume ● Silent unit restrictive defects
(FRC) ✓ when ventilation and ❖ specific surgical
✓ Vol remaining in the perfusion are impaired procedures (e.g., upper
lungs after a normal ✓ severe ARDS or abdominal, thoracic, or
exhalation- 2400mL pneumothorax open heart surgery
4. Inspiratory capacity (VT +IRV)- (respiratory
3600mL emergencies)- fatal
compressive atelectasis
5. Inspiratory Reserve Volume
(IRV) Management of Patients with ➢ restricts normal lung
✓ Volume of air one is able Chest and Lower Respiratory Tract expansion on inspiration:
to inhale in addition to Disorders possible cause, post op-
the VT- 3100mL prolong supine position
6. Residual Volume (RV) ➢ pressure can be
ATELECTASIS
✓ Volume of air that produced by fluid
▪ closure or collapse of accumulation
remains in the lungs alveoli
following forced -pleural space —-pleural effusion
▪ chest x-ray findings - (fluid accumulation)
expiration beyond acute or chronic
normal (ERV)-1200mL -air in the pleural space leads to
Can be developed by: pneumothorax
7. Vital CApacity ▪ postoperative setting
✓ Sum of ERV, VT and IRV- -blood in the pleural space leads
▪ COPD to Hemothorax
4800mL ▪ Lung cancer- -pericardial area pericardial
malignancies effusion
Respiration (Diffusion) ▪ Microatelectasis -certain
area of alveoli.
Clinical Manifestations
➢ insidious- develops - It measures volumetric spontaneously
slowly. displacement on the device breathing patient.
➢ increasing dyspnea, 2. Flow-oriented devices ✓ Increases the amount
cough, and sputum - It provides only an indirect of air remaining in the
production. indicator of the patient’s inspired lungs at the end of
➢ lobar atelectasis, one volume expiration.
lobe is affected (worse) ✓ Fewer complications
➢ marked respiratory Management than PEEP.
distress • improve ventilation and ✓ Ordered as 5–10 cm
➢ tachycardia, remove secretions: turn H2O
tachypnea, pleural patient, early
➢ pain, and central ambulation, instruct pt. Acute Tracheobronchitis
cyanosis( not enough deep breathing ▪ acute inflammation of
air)- caused by exercises the mucous membranes
hypoxemia • In patients who do not of the trachea
➢ Orthopnea- difficulty in respond to first-line ▪ bronchial tree
breathing while laying measures or who cannot ▪ airway is affected
(sitting best position to perform deep-breathing
relieve) exercises: PEEP( mech Pathophysiology
➢ chronic atelectasis? – vent) help alveoli ➢ Streptococcus
manifestation: pt, • simple mask pneumoniae
having probs with • one-way valve system ➢ Haemophilus influenzae
ventilation of alveoli, risk provides varying ➢ Mycoplasma
for pulmonary infection amounts of expiratory pneumoniae.
➢ Friction happen- pleurisy resistance, usually 10 to ➢ fungal infection
15 cm H2O (e.g.,Aspergillus)
Assessment and Diagnostic • CPAP ➢ sputum culture sensitivity
Findings ● Positive End-Expiratory Pressure ➢ inhalation of physical-
➢ Chest x-ray- best way to (PEEP): person to person (talk,
diagnose ✓ Increases oxygenation sneeze)
✓ patchy infiltrates or by increasing functional ➢ chemical irritants, gases,
consolidated areas residual capacity (FRC). or other air
✓ pulse oximetry (SpO2) - ✓ Keeps alveoli inflated contaminants
<90% after expiration. ➢ ventilatorassociated
✓ partial pressure of ✓ Can use lower O2 trachea bronchitis-
arterial oxygen (PaO2) concentrations with commonly cause by
✓ Below Normal PEEP;decreases risk of fungal infection
3 hall mark signs: O2 toxicity. Ordered as
• Decrease O2 sat- cause 5–10 cm H2O Clinical Manifestation
by hypoxemia ● Low-flow O2 Therapy • dry, irritating cough
• Marked tachypnea ✓ Simple masks • expectorates a scanty
• Difficulty in breathing ✓ allow for higher FiO2 but amount of mucoid
precise calculation of sputum
Prevention of collapse Alveoli FiO2 is again • sternal soreness
• frequent turning dependent on the • coughing
• early mobilization( patient’s respiratory • fever or chills
specially for patient pattern.
• night sweats, headache
after surgery) ✓ Flow rates administered
• General malaise
• teach strategies to via simple masks range
• short of breath- late
expand the lungs (deep from 8 to 12 LPM.
signs
breathing exercises) ● Non-rebreather masks
• noisy inspiration and
- at least every 2 hours - manage -dependent on patients
expiration (inspiratory
secretions : directed cough breathing, effort
stridor and expiratory
• Suctioning ✓ have valves over the
wheeze)
• aerosol nebulizer ports that allow exhaled
• produce purulent (pus-
treatments/ MDI air to escape but
filled) sputum
• chest physiotherapy: prevent room air from
• blood-streaked
postural drainage and being inhaled.
✓ This mask is capable of secretion
chest percussion
• incentive spirometry; delivering up to 100%
O2. Medical Management
bronchoscopy- use to ❖ Antibiotics
check for collapse of ● Continuous Positive Airway
Pressure (CPAP): ❖ Antihistamines- not
alveoli usually given because
✓ Maintains positive
pressure throughout the secretions may become
Incentive Spirometry dry
1. Volume –oriented devices respiratory cycle of a
❖ Suctioning and
bronchoscopy
❖ endotracheal marcescens,Pseudomon
intubation- last resort as aeruginosa, Risk Factors??
❖ acute respiratory failure methicillin-sensitive or Clinical Manifestations
methicillin-resistant • sudden onset of chills,
Nursing Management Staphylococcus aureus rapidly rising fever
➢ increased fluid intake (MRSA), and S. • pleuritic chest pain that
➢ directed coughing to pneumoniae is aggravated by deep
remove secretions 4. Ventilator-associated breathing and coughing
➢ Rest and activity pneumonia (VAP) • streptococcal
balance ➢ A type of HAP that (pneumococcal)
develops ≥48 hours after pneumonia
Pneumonia endotracheal tube • headache, low-grade
▪ inflammation of the lung intubation fever, pleuritic pain,
parenchyma myalgia, rash, and
▪ Pneumonitis Pneumonia in the pharyngitis
▪ Restrict lung Immunocompromised Host - • mucoid or
Classification Pneumocystis pneumonia (PCP) mucopurulent sputum
1. Community-Acquired ➢ Pneumocystis jiroveci • cheeks are flushed and
Pneumonia (CAP) ➢ fungal pneumonias the lips and nail beds
✓ Acquired in community ➢ Mycobacterium • demonstrate central
setting or within the first tuberculosis cyanosis
48 hours after Aspiration Pneumonia • late sign of poor
hospitalization or ➢ pulmonary oxygenation
institutionalization consequences resulting [hypoxemia]
✓ Causative agents? from entry of • Orthopnea (orthopneic
endogenous or position, inclined
2. Health care–associated exogenous substances position)
pneumonia (HCAP) into the lower airway. • Poor appetite,
✓ Pneumonia occurring in diaphoretic and tires
a non hospitalized Pathophysiology easily
patient with extensive ❖ normal flora present in • Rusty, blood-tinged
health care contact patients whose sputum
with one or more of the resistance has been • streptococcal
following: altered (pneumococcal),
✓ Hospitalization for ≥2 ❖ Oropharynx staphylococcal, and
days in an acute care ❖ often have an acute or Klebsiella pneumonia
facility within 90 days of chronic underlying • Crackles- fluid
infection disease that impairs host accumulation in kung
✓ Residence in a nursing defenses tissue
home or long-term care ❖ bloodborne organisms • consolidation of lung
facility ❖ affects both ventilation tissue- xray result (white
✓ Antibiotic therapy, and diffusion- churva)
chemotherapy, or oxygenation is affected • tactile fremitus
wound care within 30 ❖ Exudate- excess mucous • vocal vibration
days of current infection production detected on palpation,
H ❖ oxygen and carbon
• percussion dullness,
✓ Hemodialysis treatment dioxide- O2 down
• bronchial breath sounds,
at a hospital or clinic CarbD, increases- leads
- egophony, when
✓ Home infusion therapy to respi acidosis
auscultated, the spoken
or home wound care ❖ White blood cells –
“E” becomes a loud,
✓ Family member with neutrophils
nasal-sounding “A”
infection due to ❖ Decreased ventilation-
• whispered pectoriloquy
multidrug-resistant decrease O2 entering
• whispered sounds are
bacteria alveoli
easily auscultated
❖ Decreased alveolar O2
through the chest wall -
3. Hospital-acquired pneumonia tension
consolidation
(HAP) ❖ Bronchospasm-
✓ Pneumonia occurring narrowing of bronchi
Assessment and Diagnostic
≥48 hours after hospital ❖ Hypoventilation- affect
Findings
admission that did not ventilation perfusion
✓ history (particularly of a
appear to be ❖ V/Q mismatch - Venous
recent respiratory tract
incubating at the time blood (ventilation and
infection)
of admission perfusion no longer
✓ physical examination
➢ Enterobacter species, sustaining the need of
✓ chest x-ray
Escherichia coli, H. the body)
✓ blood culture
influenzae, Klebsiella ❖ Poorly oxygenated -
(bloodstream
species, Proteus, Serratia hypoxemia
invasion[bacteremia] ❖ talking, coughing, • sputum culture for acid-
occurs frequently) sneezing, laughing, or fast bacilli
✓ sputum examination? singing. • complete history
✓ rinse the mouth with ❖ Larger droplets settle • physical examination
water to minimize ❖ smaller droplets remain • tuberculin skin test
contamination by suspended in the air and • chest x-ray
normal oral flora, are inhaled by a • Assessment
✓ breathe deeply several susceptible person • Physical examination
times, cough deeply, • Chest X-ray
and (4) expectorate the Pathophysiology • Multinodular infiltrates
raised sputum into a • Mycobacterium with calcification in
sterile container • Alveoli upper lobes
• Lymph system and • Sputum cultures
Pharmacologic Therapy - blood stream • Acid-fast smear
Antibiotic • Kidneys, bones, cerebral • Negative after 3 months
➢ culture and sensitivity. cortex - Inflammatory of treatment - Mantoux
➢ ceftriaxone (Rocephin), reaction test
➢ ampicillin/sulbactam • Phagocytes (neutrophils • Reliable test
(Unasyn), and macrophages • Positive reaction?
➢ levofloxacin (Levaquin), • TB-specific lymphocytes • Active disease
➢ ertapenem (Invanz) lyse - Exudate • Previous exposure—
➢ cephalosporin or • Alveoli inactive
ceftazidime (Fortaz) • bronchopneumonia • Assessment - PPD test
➢ antipseudomonal • 2 to 10 weeks • Positive
carbapenem
• 10mm or more--- 48 to
➢ piperacillin/tazobactam Risk factors 72 hours after injection
(Zosyn) plus • Close contact For pts. With HIV 5 mm
antipseudomonal • Immunocompromised or greater – Positive
fluoroquinolone status • QuantiFERON-TB Gold
➢ aminoglycoside plus • Substance abuse test
linezolid (Zyvox) or • Poverty • A blood analysis test by
vancomycin (Vancocin) • Preexisting Medical an enzyme-linked
condition Travel to immunosorbent assay
NURSING PROCESS countries with high TB • A sensitive and rapid
1. Assessment cases test (results can be
2. Diagnosis • Institutionalization available in 24 hours)
3. Planning • Living condition that assists in diagnosing
4. Nursing Interventions • Health Worker the client
a. Improving airway
b. Promoting rest and conserving Prevention? (CDC) Pharmacologic Management
energy ❖ Early identification and - Rifamipicin (Rifampin
c. Fluid intake treatment of persons - Isoniazid (INH)
d. Nutrition with active TB - Pyrazinamide (PZA)
e. Education ❖ Prevention of spread of - Ethambutol
f. Monitoring of complications infectious droplet nuclei - Streptomycin
delirium- older patient by source control
methods and by Nursing Management
Pulmonary Tuberculosis reduction of microbial ✓ Promoting Airway
▪ infectious disease that contamination of indoor Clearance
primarily affects the lung air ✓ Promoting Adherence
parenchyma ❖ Initiate AFB isolation to Treatment Regimen
▪ meninges, kidneys, precautions - ✓ Promoting Activity and
bones, and lymph nodes Surveillance for TB Adequate Nutrition
▪ M. tuberculosis -is an transmission ✓ Preventing Transmission
acid-fast aerobic rod of Tuberculosis Infection
that grows slowly and is Clinical Manifestations
sensitive to heat and ❖ low-grade fever,
cough, night sweats, Lung Abscess
ultraviolet light
fatigue, and weight loss ▪ lung abscess is a
Transmission and Risk Factors ❖ Hemoptysis localized collection of
❖ spreads from person to pus caused by microbial
person by airborne infection
transmission ▪ caused by anaerobic
❖ An infected person Assessment and Diagnostic bacteria (doesn’t need
releases droplet nuclei Findings any oxygen to stay)
(usually particles 1 to 5 • positive skin test enters lung by aspiration
mcm in diameter) • blood test
▪ chest x-ray ▪ grating or creaking
demonstrates a cavity sound Pleurisy
of atleast 2 cm in lungs ▪ Crackles - chest x-ray • inflammation of both
(hole, pus, exudates) wtf ▪ infiltrate with an air–fluid layers of the pleurae
level - sputum culture • Complication of;
Risk Factors: ▪ fiberoptic bronchoscopy pneumonia or an upper
• impaired cough reflexes ▪ computed tomography respiratory tract
• swallowing difficulties (CT) scan infection, TB, or collagen
• CNS disorders disease; after trauma to
• drug addiction Bronchoscopy the chest, pulmonary
• Alcoholism ❖ direct inspection and infarction, or PE
• esophageal disease examination of the • primary or metastatic
• compromised immune larynx, trachea, and cancer; and after
function bronchi through either a thoracotomy
• patients without teeth flexible fiberoptic
• nasogastric tube bronchoscope or a rigid Clinical Manifestations
feedings bronchoscope • pleuritic pain
• altered state of • severe, sharp, knifelike
consciousness 1. to visualize tissues and pain
determine the nature, location, • Intensifies during
Pathophysiology and extent of the pathologic inspiration
• complication of process • deep breath, coughing,
bacterial pneumonia 2. to collect secretions for analysis or sneezing
• aspiration of oral and to obtain
anaerobes into the lung. a tissue sample for diagnosis Assessment and Diagnostic
• The site of the lung 3. to determine whether a tumor Findings
abscess is related to can be resected • pleural friction rub
gravity surgically • chest x-rays, sputum
• Initially the cavity in the 4. to diagnose sources of analysis,
lung may or may not hemoptysis. • thoracentesis
extend directly into a • pleural fluid for
bronchus Medical Management examination
• the abscess becomes ❖ postural drainage and Medical Management
surrounded, or chest • discover the underlying
encapsulated, by a wall ❖ physiotherapy condition
of fibrous tissue ❖ percutaneous chest
• causing the pleurisy
• extend until it reaches catheter
• to relieve the pain
the lumen of a bronchus ❖ long-term drainage of
• monitored for signs and
or the pleural space the abscess. - Surgical
symptoms of pleural
• respiratory tract, the intervention is rare
effusion
pleural cavity, or both o but pulmonary
• shortness of breath,
• If bronchus? resection
pain,
• purulent contents are (lobectomy)
• Prescribed analgesic
expectorated o massive
agents and topical
continuously in the form hemoptysis
applications of heat or
of sputum o if there is little
cold
• if Pleura- empyema or no response
• NSAIDs
• If Both—-- to medical
bronchopleural fistula management.
Nursing Management
❖ enhance comfort- such
Clinical Manifestations Medical Management
as turning frequently
❖ fever • IV antimicrobial therapy
onto the affected side—
❖ productive cough with • clindamycin (Cleocin),
To splint the chest wall
moderate to copious ampicillin-sulbactam
and reduce the
amounts of foul-smelling (Unasyn) or
stretching of the
❖ bloody sputum carbapenem
pleurae.
❖ Leukocytosis -use the hands or a
❖ Pleurisy Nursing Management
pillow
❖ Dyspnea • administers antibiotics
-splint the rib cage while
❖ Weakness • Chest physiotherapy
coughing
❖ anorexia, and weight • Health education
loss • deep-breathing and
Pleural Effusion
coughing exercises
Assessment and Diagnostic • proper nutritional intake ▪ collection of fluid in the
Findings • high in protein and pleural space
▪ Physical Examination calories ▪ secondary to other
▪ pleural friction rub • emotional support, diseases.
▪ pleural space fluid? 5 to ▪ abnormal accumulation
15 ml Chest Drainage Systems of fluid in the lung tissue,
▪ Complication of; ➢ suction source- create the alveolar space, or
-heart failure, TB, negative pressure and both
pneumonia, pulmonary promote drainage of ▪ severe, life-threatening
infections, nephrotic fluid and removal of air. condition
syndrome, connective -20 cm H2O ▪ damage of the
tissue disease, PE and -bubbling appears in the pulmonary capillary
neoplastic tumors suction chamber lining
➢ collection chamber for
Pathophysiology pleural drainage -
❖ accumulate in the reservoir for fluid Risk Factors
pleural space draining • direct injury
•clear fluid ➢ water seal chamber • chest trauma, aspiration,
•Bloody -mechanism to prevent and smoke inhalation
•Purulent air from reentering the • hematogenous injury
Transudate- filtrate of plasma that chest with inhalation • sepsis, pancreatitis,
moves across intact capillarywalls multiple transfusions,
❖ heart failure. and cardiopulmonary
Empyema
Exudate- extravasation of fluid bypass
into tissues or a cavity ▪ accumulation of thick,
•bacterial products or tumors purulent fluid within the
pleural space
Chronic Obstructive Pulmonary
Clinical Manifestations ▪ complications of
bacterial pneumonia or Disease
❖ fever, chills, and pleuritic
chest pain lung abscess. ➢ preventable and
❖ a malignant effusion ▪ penetrating chest treatable slowly
❖ dyspnea, difficulty lying trauma progressive respiratory
flat, and coughing - ▪ hematogenous infection disease of airflow
of the pleural space, obstruction
Assessment and Diagnostic ▪ nonbacterial infections ➢ airflow limitation or
Findings ▪ iatrogenic causes (after obstruction in COPD is
• Physical examination thoracic surgery or not fully reversible
thoracentesis) ➢ emphysema and
• decreased or absent
breath sounds chronic bronchitis
Clinical Manifestations Risk Factors:
• decreased fremitus
• acute respiratory • cigarette smoking-
• dull, flat sound on
infection or pneumonia destroys the ability of
percussion
• fever, night sweats, lung to clean up respi
• Tracheal deviation
pleural pain, cough, tract)
• chest x-ray
dyspnea, anorexia, • Passive smoking
-lies on the affected side
weight loss • Tobacco
chest CT, and
thoracentesis • Age
Assessment and Diagnostic • Occupational exposure
Findings • Genetic abnormalities—
Thoracentesis ▪ Physical Assessment alpha1-antitrypsin
➢ aspiration of fluid and air ▪ decreased or absent (kulang ng alpha-1,
from the pleural space breath sounds which this is important in
diagnostic or therapeutic?? ▪ dullness on chest respi tract to fight
percussion foreign bodies-
Medical Management ▪ decreased fremitus deficient=magkaka
❖ to discover the ▪ thoracentesis COPD)
underlying cause
❖ to prevent Medical Management Pathophysiology
reaccumulation of fluid ❖ Needle aspiration ▪ symptomatic during the
❖ to relieve discomfort, (thoracentesis) middle adult years
dyspnea, and ❖ Tube thoracostomy ▪ airflow limitation is both
respiratorycompromise progressive and
Nursing Management associated with the
Nursing Management ✓ instructs the patient in lungs’ abnormal
✓ supporting the medical lung-expanding inflammatory response
regimen ✓ breathing exercises to to noxious particles or
✓ prepares and positions restore normal gases (exposur)
the patient for respiratory function ▪ body’s attempts to
thoracentesis repair changes and
✓ chest tube Pulmonary Edema narrowing can occur in
management the airways (instead of
(Noncardiogenic)
✓ Pain management -
patent, obstructive can the acinus (sa tubing ✓ Monitoring and
happen -2 mm lang) (hyperextended Managing Potential
▪ goblet cells (will ang lobular) Complications
enlarged) and enlarged ▪ chronic hypoxemia,
submucosal glands hypercapnia, Bronchiectasis
(enlarged= additional polycythemia ▪ Chronic but irreversible
mucous plug, mas mag ▪ right-sided heart failure dilation of the bronchi
babara) and bronchiole
▪ hypersecretion of mucus Complication ▪ destruction of muscles
(chronic air limitation) Cor pulmonale- increase pressure and elastic connective
in pulmonary artery. tissue
Chronic Bronchitis (COPD) ▪ right-sided heart failure ▪ dilation of the bronchi
• presence of cough and brought on by long-term and bronchus
sputum production for high blood pressure in (reproduction of
at least 3 months in the pulmonary arteries mucous)
each of 2 consecutive (accumulation of fluid)
years ▪ dependent edema Risk factors
• smoke or other ▪ distended neck veins ➢ respiratory infections
environmental pollutants ▪ pain in the region of the (pneumonia, TB)
• hypersecretion of mucus liver (because of fluid ➢ CF (cystic fibrosis)| own
• Bronchial walls accumulation) immune system tries to
thickened |hypertension in the liver destroy connective
• narrowing the bronchial can occur if last longer,, tissue that leads to
lumen chariz| rebound effect dilation of bronchi and
can also occur bronchus. (also produce
Emphysema (COPD) mucous, excess)
Assessment and Diagnostic ➢ rheumatic and other
• impaired oxygen and
Findings systemic diseases
carbon dioxide
-PFT ➢ primary ciliary
exchange
- Spirometry dysfunction
• results from destruction
- FEV1 to forced vital capacity ➢ Tuberculosis
of the walls of
(FVC) (affected, bumababa- and ➢ mmunodeficiency
overdistended alveoli (in
patient can have an air flow disorders
the alveoli)
limitation=obstructive airway)
• pathologic term that
Pathophysiology
describes an abnormal
Medical Management - damages the bronchial wall
distention of the
- promoting smoking cessation - loss of its supporting structure -
airspaces – Alveoli
prescribing medications: thick sputum obstructs the
• bronchodilators bronchi.
Manifestation: Barrel chest
• Corticosteroid-
• Hypoxemia can
formoterol/budesonide
increase pulmonary
(Symbicort) Clinical Manifestations
artery pressures leads to
salmeterol/fluticasone - chronic cough
pulmonary hypertension
(Advair) - production of purulent sputum in
• Hypercapnia- excessive copious amounts
• managing
carbon dioxide in the - hemoptysis (blood in sputum)
exacerbations
lungs that results to
• Providing supplemental
respiratory acidosis Assessment and Diagnostic
oxygen therapy as
indicated. Findings
panlobular (panacinar) - prolonged history of productive,
▪ destruction of the Management chronic cough, with sputum
respiratory bronchiole, ✓ Breathing Exercises consistently negative for tubercle
alveolar duct, and ✓ Activity Pacing Bacilli
alveolus ✓ Self-Care Activities
▪ hyperinflated ✓ Physical Conditioning Medical Management
(hyperexpanded) chest ✓ Oxygen Therapy • promote bronchial
▪ marked dyspnea on ✓ Nutritional Therapy drainage (chest
exertion percussion, chest
▪ weight loss Nursing Management physiotherapy- improve
▪ expiration becomes ✓ Achieving Airway removal of secretion)
active Clearance (orthopnic • clear excessive
position) secretions from the
centrilobular (centroacinar) ✓ Improving Breathing affected portion of the
▪ in the center of the Patterns lungs
secondary lobule, ✓ Improving Activity • prevent or control
preserving the Tolerance infection
peripheral portions of
• Bronchoscopy Chest • atelectasis well as needed changes
physiotherapy in ventilator or oxygen
Assessment and Diagnostic settings.
Findings
Asthma (distinct condition) ❖ determine that episodic Normal Values
➢ heterogeneous disease, symptoms of airflow
usually characterized by obstruction
chronic airway ❖ positive family history
inflammation (cause by ❖ environmental factors
triggering factors: ❖ seasonal changes, high
allergens, food, pollen counts, mold, pet
environmental dander, climate
pollutants, genetic changes
predisposition) ❖ occupation-related
➢ airway chemicals
hyperresponsiveness, ❖ Eosinophilia
mucosal edema, and ❖ IgE
mucus production ❖ allergy
(appears because of
triggering factors) Medical Management
Pharmacologic Therapy
Pathophysiology 1. quickrelief medications
➢ When allergen triggers a. immediate treatment of
inflammatory process, it asthma symptoms
will now react to 3: b. Short-acting beta2-adrenergic
increase airway agonists
reaction, airway i. Albuterol, Proventil, Ventolin c.
limitation (because it ipratropium [Atrovent])
triggers mucosal edema
and mucus production, 2. exacerbations and long-acting
narrowed airway= medications
wheezing sounds, a. To achieve and maintain
coughing, dyspnea, control of persistent asthma
chest tightness b. Corticosteroids
c. Long-acting beta2-agonists
Clinical Manifestations (LABA)
▪ Coughing i. Theophylline ii. Salmeterol
▪ Chest tightness iii. formoterol
▪ Diaphoresis (sweating)
▪ Tachycardia Nursing Management
▪ Hypoxemia (low O2) 1. assesses the patient’s
▪ Restless respiratory status
▪ Irritation a. breath sounds, peak flow, pulse
▪ Anxiety oximetry, and vital signs.
▪ Hyperventilation – CO2 2. Obtains a history of allergic
decreases reactions to medications before
▪ Wheezing sound administering medications.
Note: asthma attack happens 3. Identifies medications the
night or early in the morning (it is patient is taking.
because of the change of 4. Administers medications as
temperature| lumalamig) prescribed and
monitors the patient’s responses
Initial Manifestation: to those medications.
Hypocapnia- decrease in 5. Administers fluids if the patient is
alveolar and blood carbon dehydrated
dioxide level below normal range.
Respiratory Alkalosis-( Arterial Blood Gases (ABG)
hyperventilation) ❖ An ABG directly
measures the pH of the
blood, along with the
Complications: partial pressure of O2,
• can be progressive and CO2, bicarbonate ion,
recurrent leads to status and saturation of Hgb.
asthmaticus, life ❖ When these values are
threatening. abnormal, they can be
• Respiratory failure significant clues to
• Pneumonia respiratory problems as
You might also like
- Breath Sounds Incredibly EasyDocument4 pagesBreath Sounds Incredibly EasyMatthew Ryan100% (3)
- UntitledDocument6 pagesUntitledFritz Angelo BullonNo ratings yet
- ENT Emergency: James Paul O'NeillDocument43 pagesENT Emergency: James Paul O'NeillkylieverNo ratings yet
- Laryngeal Diseases: Laryngitis, Vocal Cord Nodules / Polyps, Carcinoma LarynxDocument52 pagesLaryngeal Diseases: Laryngitis, Vocal Cord Nodules / Polyps, Carcinoma LarynxjialeongNo ratings yet
- Airway Emergencies: ORL PostingDocument58 pagesAirway Emergencies: ORL PostingKimberlyLaw95No ratings yet
- DDs of Fever With RashDocument18 pagesDDs of Fever With RashEBNo ratings yet
- Adeno TonsillitisDocument65 pagesAdeno TonsillitisdrtpkNo ratings yet
- Respiratory Disorders in PediatricsDocument11 pagesRespiratory Disorders in PediatricsMateo Geoff100% (1)
- Lower Respiratory Tract InfectionsDocument14 pagesLower Respiratory Tract InfectionsEric EpahNo ratings yet
- Upper Respiratory DiseasesDocument113 pagesUpper Respiratory DiseasesVictor StevenNo ratings yet
- Flash CardDocument2 pagesFlash CardRoy CabuenasNo ratings yet
- MS 1 Chap 22Document9 pagesMS 1 Chap 22Louise Lorraine TaculodNo ratings yet
- Nursing Care of Clients With Upper Airway or Respiratory DisordersDocument6 pagesNursing Care of Clients With Upper Airway or Respiratory DisordersVinzii DrtNo ratings yet
- ARIs CME2Document50 pagesARIs CME2JunaidahMubarakAliNo ratings yet
- Laryngitis: Yanti NurrokhmawatiDocument73 pagesLaryngitis: Yanti NurrokhmawatiArief FakhrizalNo ratings yet
- Microbial Disease On Respiratory SystemDocument9 pagesMicrobial Disease On Respiratory SystemrishellemaepilonesNo ratings yet
- Nose Ears Throat CoughDocument82 pagesNose Ears Throat CoughHassan El HajjNo ratings yet
- Introduction To Pharmacy Practice and Simulation: PHAR456Document82 pagesIntroduction To Pharmacy Practice and Simulation: PHAR456Hassan El HajjNo ratings yet
- Sore Throat, Earache, and Upper Respiratory SymptomsDocument15 pagesSore Throat, Earache, and Upper Respiratory SymptomsMel PajantoyNo ratings yet
- 1 NR 602 Quiz 3 Study Guide: Respiratory InfectionsDocument12 pages1 NR 602 Quiz 3 Study Guide: Respiratory InfectionsLinda FieldsNo ratings yet
- Nursing Care of Clients With Upper Airway or Respiratory DisordersDocument6 pagesNursing Care of Clients With Upper Airway or Respiratory DisordersLuna MarieNo ratings yet
- WD LaryngitisDocument80 pagesWD LaryngitisArief FakhrizalNo ratings yet
- Understanding of Rhinosinusitis: Complication and Implication of Rhinosinusitis Daily PracticeDocument43 pagesUnderstanding of Rhinosinusitis: Complication and Implication of Rhinosinusitis Daily PracticeYunita Indah PalupiNo ratings yet
- Throat PowerpointDocument29 pagesThroat Powerpointminci sensei100% (8)
- Acute Respiratory Tarct Infection in ChildrenDocument4 pagesAcute Respiratory Tarct Infection in ChildrenDoc AchondoNo ratings yet
- URTIDocument41 pagesURTIGetaneh LiknawNo ratings yet
- Upper Respiratory Tract InfectionsDocument71 pagesUpper Respiratory Tract InfectionsRasha Al MousaNo ratings yet
- MEDSURGDocument7 pagesMEDSURGVal FielNo ratings yet
- Respiratory DisordersDocument15 pagesRespiratory DisordersStephanie LeeNo ratings yet
- Week 12 Learning ObjectivesDocument10 pagesWeek 12 Learning ObjectivesCamryn NewellNo ratings yet
- MK CoryzaDocument3 pagesMK CoryzaMoses Jr KazevuNo ratings yet
- Respi Patho 1Document111 pagesRespi Patho 1Quolette ConstanteNo ratings yet
- 5 2-DeanDocument7 pages5 2-Deanfiel borataNo ratings yet
- Week 1 3 Management of Patients With Problems in Respiratory SystemDocument22 pagesWeek 1 3 Management of Patients With Problems in Respiratory SystemKIANA LOUISE ROMANONo ratings yet
- Pediatric Infectious DiseasesDocument6 pagesPediatric Infectious DiseasesZllison Mae Teodoro MangabatNo ratings yet
- Ent Badi PDFDocument42 pagesEnt Badi PDFsandeepNo ratings yet
- Sore ThroatDocument41 pagesSore ThroatWongHN100% (1)
- PharyngitisDocument27 pagesPharyngitisSubhada GosaviNo ratings yet
- Presenter: clerk 2 蘇雋淋 Date: 2022/03/11Document39 pagesPresenter: clerk 2 蘇雋淋 Date: 2022/03/11s0501120醫學系No ratings yet
- Acute NasopharyngitisDocument13 pagesAcute Nasopharyngitisjyoti kunduNo ratings yet
- Upper Respiratory AlterationDocument34 pagesUpper Respiratory AlterationJulia ManaloNo ratings yet
- Curs FaringeDocument49 pagesCurs FaringeAdi SitaruNo ratings yet
- PharyngitisDocument54 pagesPharyngitisDr Sravya M VNo ratings yet
- Ipm-3 EpitelDocument58 pagesIpm-3 EpitelVonny MariaNo ratings yet
- Chapter 30: Nursing Care of Patients With Upper Respiratory Tract DisordersDocument4 pagesChapter 30: Nursing Care of Patients With Upper Respiratory Tract DisordersPaige Nicole GauthreauxNo ratings yet
- Management of Common Ear Nose & Throat Problems: Professor Khalid H MahidaDocument65 pagesManagement of Common Ear Nose & Throat Problems: Professor Khalid H MahidaFurqan MirzaNo ratings yet
- Pharyngitis: Dr.M.KarimiDocument60 pagesPharyngitis: Dr.M.KarimiJessa AdenigNo ratings yet
- Rhino SinusitisDocument30 pagesRhino SinusitisTheSekKuNo ratings yet
- File 000Document48 pagesFile 000nasarcedaNo ratings yet
- Common Viral Infec - Part 2Document13 pagesCommon Viral Infec - Part 2d99452727No ratings yet
- g1b Asthma PDFDocument75 pagesg1b Asthma PDFAniq Zahran MasomNo ratings yet
- Laryngitis: Wahyu Priatmoko 1301 1207 0197 Ilman Fathony 1301 1207 007Document74 pagesLaryngitis: Wahyu Priatmoko 1301 1207 0197 Ilman Fathony 1301 1207 007Arief FakhrizalNo ratings yet
- Pediatric Upper Respiratory Tract DisordersDocument5 pagesPediatric Upper Respiratory Tract DisordersANGELTHERESE CANDIANo ratings yet
- Ent Case ReportDocument36 pagesEnt Case ReportCal MJNo ratings yet
- Kawasaki Disease CaseDocument64 pagesKawasaki Disease CaseRon Christian Neil RodriguezNo ratings yet
- 3 Upper RespiDocument81 pages3 Upper RespiRizza TadeoNo ratings yet
- Throat DisorderDocument46 pagesThroat DisorderKpj KpjNo ratings yet
- Management of Patients With Upper Respiratory Tract DisordersDocument93 pagesManagement of Patients With Upper Respiratory Tract DisordersErica Clerigo LandichoNo ratings yet
- A Topic Presentation ON: Emerging Communicable DiseasesDocument52 pagesA Topic Presentation ON: Emerging Communicable DiseasesGiri SivaNo ratings yet
- Sore Throat: Introduction To ComplaintDocument8 pagesSore Throat: Introduction To Complaintnorma ocanaNo ratings yet
- Infeksi Saluran Pernafasan Atas Blok 17 PSPDDocument48 pagesInfeksi Saluran Pernafasan Atas Blok 17 PSPDFahmiNo ratings yet
- Maklumat Vaksinasi: Vaccination DetailsDocument1 pageMaklumat Vaksinasi: Vaccination DetailsFahrin ZikriNo ratings yet
- Medical Management For PneumoniaDocument2 pagesMedical Management For PneumoniaSue Elaine100% (1)
- MSN Unit 8Document2 pagesMSN Unit 8tarangini mauryaNo ratings yet
- Acute Bronchitis: Bjorn BuhagiarDocument4 pagesAcute Bronchitis: Bjorn Buhagiaryulita kesumaNo ratings yet
- Jurnal Ilmiah Maksitek ISSN. 2655-4399 Vol. 5 No. 4 Desember 2020Document6 pagesJurnal Ilmiah Maksitek ISSN. 2655-4399 Vol. 5 No. 4 Desember 2020MasithaNo ratings yet
- CH 010 Croup in ChildrenDocument7 pagesCH 010 Croup in ChildrenDr Sonali KadeliNo ratings yet
- Cough - AMBOSSDocument12 pagesCough - AMBOSSAmira AlmutairiNo ratings yet
- Influenza: Flu "Influenza" Definition, Symptoms, Causes, Treatment, PreventionDocument3 pagesInfluenza: Flu "Influenza" Definition, Symptoms, Causes, Treatment, PreventionYusuf Rony LosongNo ratings yet
- Overview of Covid 19 in Nigeria.Document10 pagesOverview of Covid 19 in Nigeria.KRUSU ISAACNo ratings yet
- Signs and Symptoms: Acute Respiratory Distress SyndromeDocument14 pagesSigns and Symptoms: Acute Respiratory Distress SyndromeMichelle LopezNo ratings yet
- PcapDocument13 pagesPcapManjuNo ratings yet
- Cold vs. Flu vs. Allergies vs. COVID-19Document1 pageCold vs. Flu vs. Allergies vs. COVID-19prabuNo ratings yet
- Chest Trauma: Prof. Anjum Sohail Ansari H.O.D Surgery Cims, BahawalpurDocument37 pagesChest Trauma: Prof. Anjum Sohail Ansari H.O.D Surgery Cims, BahawalpurAmnaNo ratings yet
- CASE Pneumonia EnglishDocument35 pagesCASE Pneumonia EnglishDhiya Ul AzkaNo ratings yet
- Artikel KKN 15 - A.rizal Dwiki RivaldhyDocument17 pagesArtikel KKN 15 - A.rizal Dwiki RivaldhyArizal RivaldhyNo ratings yet
- Chest, Abdomen and RheumatologyDocument142 pagesChest, Abdomen and RheumatologyAhmed JaoadNo ratings yet
- Diagnosis and Management of COPD A Case StudyDocument4 pagesDiagnosis and Management of COPD A Case StudyZairenee QuizanaNo ratings yet
- Respiratory System SummaryDocument6 pagesRespiratory System SummaryKiara GovenderNo ratings yet
- Respiratory SoundsDocument2 pagesRespiratory SoundsMuhammad NaeemjakNo ratings yet
- NIV Algorithm Final Version Jan 2020Document3 pagesNIV Algorithm Final Version Jan 2020AmalNo ratings yet
- AdmissionLogBook 10192019Document24 pagesAdmissionLogBook 10192019Jessa Beth SantiagoNo ratings yet
- FEU Review Pre Board Exam 2016 PathophysioDocument8 pagesFEU Review Pre Board Exam 2016 PathophysioDharlyn MungcalNo ratings yet
- HRCTDocument82 pagesHRCTmahmod omerNo ratings yet
- Physical Education 12 Pneumonia: To Be Reported By: Alawi, Lhamiah M. Casano, Diana Elizabeth C. Kinoshita, Ryou GDocument21 pagesPhysical Education 12 Pneumonia: To Be Reported By: Alawi, Lhamiah M. Casano, Diana Elizabeth C. Kinoshita, Ryou GRyou KinoshitaNo ratings yet
- Lets Talk About Coronavirus Reading Comprehension Exercises TestsDocument3 pagesLets Talk About Coronavirus Reading Comprehension Exercises TestsEka BabunidzeNo ratings yet
- 1 Topic 1 - Differential Diagnosis of Pneumonia in Children. Complications of Pneumonia ... (PDFDrive)Document164 pages1 Topic 1 - Differential Diagnosis of Pneumonia in Children. Complications of Pneumonia ... (PDFDrive)Dara PitraNo ratings yet
- BMJ Avian FluDocument49 pagesBMJ Avian Flualiakbar178No ratings yet
- First Aid '20: Osmosis VideosDocument55 pagesFirst Aid '20: Osmosis VideosJulien ClaireNo ratings yet