Professional Documents
Culture Documents
Antimicrobial Therapy
Uploaded by
nishadi0 ratings0% found this document useful (0 votes)
2 views26 pagesCopyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
2 views26 pagesAntimicrobial Therapy
Uploaded by
nishadiCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 26
Antimicrobial Therapy
Principles of Antimicrobial Therapy
1. Make a diagnosis:
• As precisely as possible.
• Define the site of infection and the organism(s) responsible and their
sensitivity to drugs.
• All relevant biological samples should be taken before treatment.
Principles of Antimicrobial Therapy
2. Remove barriers to cure:
• Drain abscesses
• Replace infected IV cannula
• Clear blocked passages - respiratory, urinary
Principles of Antimicrobial Therapy
3. Decide the necessity of antimicrobials:
• Some of the acute infections are better managed symptomatically
than by antimicrobials e.g., Need of antibiotics for superficial wounds.
• Risks of adverse drug reactions
• Chronic wounds, chronic abscess or empyema respond poorly to
antibiotics alone.
Principles of Antimicrobial Therapy
4. Select the best drug:
• Consider the specificity – ideally the antimicrobial activity of the drug
should match that of the infecting organisms. Avoid broad spectrum
antibiotics – risk of resistance and opportunistic infections. At the
beginning – empirical/ best guess therapy.
• Consider the pharmacokinetic factors – the selected antibiotic should
reach the site of action in adequate amounts e.g., BBB, bones.
• Consider patient factors – allergies, renal/hepatic impairment.
Principles of Antimicrobial Therapy
5. Administering drugs:
• Optimum dose and frequency – inadequate dose may encourage
development of resistance.
• By the most appropriate route(s)
• Plasma concentration monitoring can be performed to optimize the
therapy and to reduce adverse drug reactions e.g., aminoglycosides,
Vancomycin.
Principles of Antimicrobial Therapy
6. Continuation of therapy:
• For most infections 5-7 days
• Longer for some infections in which relapse is possible long after the
apparent clinical cure e.g., Tuberculosis and infective endocarditis.
• Otherwise, prolonged therapy is to be avoided because it increase the
costs and the risks of adverse drug reactions.
Principles of Antimicrobial Therapy
7. Test for cure:
• Symptoms and signs disappear before organism has been eradicated
e.g., UTI.
• Microbiological culture must be done after the withdrawal of
antibiotics.
Concentration-dependent killing
• Show a significant increase in the rate of bacterial killing as the
concentration of antibiotic increases.
• Concentration-dependent killing is exhibited by once-a day bolus
infusions which achieves high peak levels favoring rapid killing of the
infecting pathogen.
• E.g., aminoglycosides, fluoroquinolones
Time-dependent killing
• Killing effect is best predicted by the time duration that the blood
concentrations of the antibiotic remain above the MIC.
• Increasing the concentration of antibiotic to higher the multiples of
the MIC does not significantly increase the rate of kill.
• E.g., Penicillin and Cephalosporins, Carbapenems
• Severe infections are best treated by continuous infusion of these
agents rather than by intermittent dosing.
Use of Antimicrobials
• Empirical therapy – Broad spectrum agent/s to cover all the likely
pathogens because the infecting organism(s) has not yet been
defined.
• Definitive therapy – Once the infecting microorganism is identified, a
narrow-spectrum, low-toxic agent can be used to complete the
course of treatment.
• Prophylactic therapy – Exposed to an agent and then to prevent
infection e.g., TB OR Following procedures likely to cause bacteremia
in susceptible people e.g., surgery.
• Combination Therapy – e.g., treatment of tuberculosis benefits from
drug combinations.
Combination Therapy
It is therapeutically advisable to treat patients with the single agent that is
most specific for the infecting organism. However, situations in which
combinations of drugs are employed do exist:
• To broaden the spectrum of antibacterial activity e.g., in a known mixed
infection etc.
• To obtain potentiation or synergy e.g., penicillin plus gentamicin.
• To enable reduction of the dose of one component and hence reduce the
risks of adverse drug reactions.
When a combination must be used blindly, it is theoretically preferable to
use two bacteriostatic or two bactericidal drugs, because a bacteriostatic
drug, by reducing multiplication, may protect the organism from a
bactericidal drug.
Complications of Antimicrobial Therapy
• Hypersensitivity e.g., Penicillin
• Direct toxicity e.g., aminoglycosides can cause ototoxicity
• Super infections – with broad-spectrum antimicrobials or
combinations of agents, can lead to alterations of the normal
microbial flora, permit the overgrowth of opportunistic organisms,
especially fungi.
• Resistance
• Masking of infections e.g., a course of penicillin adequate to cure
gonorrhea may prevent simultaneously infected syphilis from showing
primary and secondary stages.
To reduce the emergence of resistance
• Antibiotics Should use only when indicated
• Select most appropriate antibiotic
• Use the antibiotic for the total required duration
• Should not stop when symptoms disappear
• Use first line drugs whenever possible
Classification of Antimicrobials
According to the type of organism which they are active against:
• Antibacterial drugs
• Antiviral drugs
• Antifungal drugs
• Antiprotozoal drugs
• Anthelmintic drugs
Classification of Antimicrobials
According to the spectrum of activity:
• Narrow-spectrum antibiotics e.g., Isoniazid is active only against
mycobacteria
• Extended-spectrum antibiotics – antibiotics that are effective against
gram-positive organisms and also against a significant number of
gram-negative bacteria e.g., Ampicillin
• Broad-spectrum antibiotics – affect a wide variety of microbial species
e.g., tetracycline
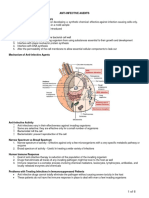
Classification of Antimicrobials
According to the site of
action:
• Interference with
breakdown and extension
of the cell wall
• Interference with plasma
membrane
• Inhibit protein synthesis
• Interference with nucleic
acid synthesis
• Interference with DNA or
RNA replication/ repair
Classification of Antimicrobials
According to the chemical structure:
• Beta lactams
• Macrolides
• Quinolones
• Tetracyclines
• Aminoglycosides
• Sulfonamides
Antibiotics
• Antibiotics are chemicals
that enter and stick to
important parts of the
bacterial cell and
interfere with its ability
to survive and multiply.
• These important parts
include proteins/sugars
in the bacterial wall or
important enzymes that
make new bacterial DNA
or proteins.
Classification of Antibiotics
Bacteriostatic:
• Those that act primarily by
arresting bacterial multiplication.
• E.g., sulfonamides, tetracyclines
and chloramphenicol
Bactericidal:
• Those which act primarily by
killing bacteria.
• E.g., beta lactams,
aminoglycosides, quinolones
Classification of Antibiotics
Classification of Antibiotics
Classification of Antibiotics
Classification of Antibiotics
You might also like
- Anti InfectivesDocument126 pagesAnti Infectiveseunice lachicaNo ratings yet
- Alprazolam Dosage, Uses, Side EffectsDocument2 pagesAlprazolam Dosage, Uses, Side EffectsKristi WrayNo ratings yet
- Antimicrobial AgentDocument30 pagesAntimicrobial AgentShardendu MishraNo ratings yet
- Pharmacology Unit 2 Antimicrobial DrugsDocument62 pagesPharmacology Unit 2 Antimicrobial DrugsAsif Ali LashariNo ratings yet
- Antibiotics Used in DentistryDocument17 pagesAntibiotics Used in Dentistrymegamarwa50% (2)
- CHEMOTHERAPY FOR TUBERCULOSISDocument49 pagesCHEMOTHERAPY FOR TUBERCULOSISJia YingNo ratings yet
- Antimicrobial DrugsDocument20 pagesAntimicrobial Drugsnadar shahNo ratings yet
- Amoxicillin Guide: Draw out your antibiotic weapon to defeat bacterial infections like pneumonia, STDs, urinary tract and skin infectionsFrom EverandAmoxicillin Guide: Draw out your antibiotic weapon to defeat bacterial infections like pneumonia, STDs, urinary tract and skin infectionsRating: 5 out of 5 stars5/5 (24)
- Principles of Antimicrobial TherapyDocument39 pagesPrinciples of Antimicrobial TherapyAsthree Nur AzizahNo ratings yet
- Edited: DR - Dairion Gatot M.Ked SP - PD-KHOMDocument57 pagesEdited: DR - Dairion Gatot M.Ked SP - PD-KHOMayuhati siregarNo ratings yet
- Anti MicrobialsDocument78 pagesAnti MicrobialsEmma Joel OtaiNo ratings yet
- Lecture 11 - Antimicrobial ChemotherapyDocument24 pagesLecture 11 - Antimicrobial Chemotherapyapi-3703352100% (2)
- Controlling Microbial Growth in Vivo Using Antimicrobial AgentsDocument30 pagesControlling Microbial Growth in Vivo Using Antimicrobial AgentsJen PanganibanNo ratings yet
- 1 Principles & Cell Wall Synthesis InhibitorsDocument94 pages1 Principles & Cell Wall Synthesis InhibitorsRjDNo ratings yet
- Unit-II Lecture-IV Antibiotics by ZebDocument84 pagesUnit-II Lecture-IV Antibiotics by ZebImad khanNo ratings yet
- Antibiotics 150406092448 Conversion Gate01Document76 pagesAntibiotics 150406092448 Conversion Gate01Dr.Aman SaxenaNo ratings yet
- Pharmacology IDocument202 pagesPharmacology ISalahadinNo ratings yet
- Agus AntibioticDocument78 pagesAgus AntibioticagusNo ratings yet
- Antimicrobial GeneralDocument18 pagesAntimicrobial Generalymeen9829No ratings yet
- 20-08-21 - T.Y - Ict 21-22 - Chap 1 - Chemotherapy - Basic Concepts and General PrinciplesDocument62 pages20-08-21 - T.Y - Ict 21-22 - Chap 1 - Chemotherapy - Basic Concepts and General PrinciplesRahul LakhaniNo ratings yet
- Week 4 Chemotherapeutic AgentsDocument339 pagesWeek 4 Chemotherapeutic AgentsLassie AbusadoNo ratings yet
- Empirical or Presumptive Anti-Infective Therapy Is BasedDocument11 pagesEmpirical or Presumptive Anti-Infective Therapy Is BasedCabdiNo ratings yet
- AntibioticsDocument49 pagesAntibioticsShriefElghazalyNo ratings yet
- ChemotherapeuticDocument71 pagesChemotherapeuticAginaya Rein0% (1)
- Microbial ResistanceDocument16 pagesMicrobial ResistanceDixa MeNo ratings yet
- Day 2 General Microbiology 12-1-2021Document150 pagesDay 2 General Microbiology 12-1-2021ShriefElghazalyNo ratings yet
- Antimicrobial Drugs History and MechanismsDocument76 pagesAntimicrobial Drugs History and MechanismsJann ClaudeNo ratings yet
- 22 Antibiotics 202333Document33 pages22 Antibiotics 202333محمد آل راشدNo ratings yet
- Basic Dental PharmacologyDocument152 pagesBasic Dental PharmacologyDr-Mohamed KandeelNo ratings yet
- PHARMACOLOGY AntibioticsDocument29 pagesPHARMACOLOGY AntibioticsBeck33ers5826100% (1)
- AntibioticsDocument70 pagesAntibioticsMunazza QuraishiNo ratings yet
- Understanding AntimicrobialsDocument11 pagesUnderstanding Antimicrobialscyrilperry1No ratings yet
- ID 6-Antimicrobial Policy 2022 Student EditionDocument30 pagesID 6-Antimicrobial Policy 2022 Student Edition白羽マイリフNo ratings yet
- Antobiotics I NotesDocument11 pagesAntobiotics I NotesBayan AlsaadiNo ratings yet
- SURGICAL AntibioticDocument58 pagesSURGICAL AntibioticdaNo ratings yet
- Antimicrobial DrugsDocument89 pagesAntimicrobial DrugsShahane AlisosoNo ratings yet
- Antimicrobial Agents 2021Document82 pagesAntimicrobial Agents 2021Aprilene Angel Balaque ZunegaNo ratings yet
- Module 3Document6 pagesModule 3richelleambrocio054No ratings yet
- L11 Antimicrobial DrugsDocument22 pagesL11 Antimicrobial DrugsSaadNo ratings yet
- Edited ANTIMICROBIAL AGENTS & SUSCEPTIBILITY TESTINGDocument18 pagesEdited ANTIMICROBIAL AGENTS & SUSCEPTIBILITY TESTINGSaid AbdelaNo ratings yet
- Principles of Anti-Microbial TherapyDocument34 pagesPrinciples of Anti-Microbial TherapyApurba Sarker ApuNo ratings yet
- Final Exam PointersDocument53 pagesFinal Exam PointersBelleNo ratings yet
- Antimicrobial AgentsDocument244 pagesAntimicrobial AgentsN Gv FcNo ratings yet
- Everything You Need to Know About Using Antibiotics in SurgeryDocument29 pagesEverything You Need to Know About Using Antibiotics in SurgeryRony RonyNo ratings yet
- Choosing the Right Antimicrobial AgentDocument53 pagesChoosing the Right Antimicrobial AgentEkanita DesianiNo ratings yet
- 5.1 Antimicrobial AgentsDocument22 pages5.1 Antimicrobial AgentsWong ShuanNo ratings yet
- Antimicrobial Agents NrsDocument24 pagesAntimicrobial Agents NrsSusmita BeheraNo ratings yet
- Use of Antibiotics 2017Document17 pagesUse of Antibiotics 2017bernard.triciaNo ratings yet
- K6. Penggunaan Antibiotik RasionalDocument32 pagesK6. Penggunaan Antibiotik RasionalAfdaliaNo ratings yet
- Pharma 14 To 23Document298 pagesPharma 14 To 23Loai Mohammed IssaNo ratings yet
- Introduction To Antimicrobials Page 1 of 6Document6 pagesIntroduction To Antimicrobials Page 1 of 6Hassan.shehriNo ratings yet
- ANTIMICROBIALS (Israjaved)Document23 pagesANTIMICROBIALS (Israjaved)Isra JavedNo ratings yet
- N-LEC5 - Chemotherapeutic Agents (General Considerations)Document33 pagesN-LEC5 - Chemotherapeutic Agents (General Considerations)geng gengNo ratings yet
- Universitas Sumatera Utara: School of MedicineDocument60 pagesUniversitas Sumatera Utara: School of MedicineedelinNo ratings yet
- Antimicrobial Pharmacology 9Document164 pagesAntimicrobial Pharmacology 9elias adugnaNo ratings yet
- Antimicrobial DrugsDocument63 pagesAntimicrobial DrugsMarianaBologanNo ratings yet
- ANTIBIOTICS23Document94 pagesANTIBIOTICS23RPMFA RPMFANo ratings yet
- AntimicrobialAgents PDFDocument34 pagesAntimicrobialAgents PDFIrawan RiyanNo ratings yet
- Everything You Need to Know About Chemotherapy in 40 CharactersDocument29 pagesEverything You Need to Know About Chemotherapy in 40 CharactersNABAKOOZA ELIZABETHNo ratings yet
- Antibiotics en NurseDocument118 pagesAntibiotics en Nurseabsolomon777No ratings yet
- General Aspects of AntimicrobialsDocument62 pagesGeneral Aspects of AntimicrobialsShree pharmacy 10th batchNo ratings yet
- Principles of Antimicrobial Therapy 2022Document33 pagesPrinciples of Antimicrobial Therapy 2022Puteri Nursyamimi Mohd SabilanNo ratings yet
- Drug StudyDocument19 pagesDrug StudyFrancis AngNo ratings yet
- Daftar Obat AB Januari 2019Document162 pagesDaftar Obat AB Januari 2019mannaria jayatiNo ratings yet
- 47 Antimycobacterial DrugsDocument77 pages47 Antimycobacterial DrugsKriziaoumo P. OrpiaNo ratings yet
- Biowaiver Monographs For Immediate-Release Solid Oral Dosage Forms: NifedipineDocument10 pagesBiowaiver Monographs For Immediate-Release Solid Oral Dosage Forms: Nifedipine9147Indah WulandariNo ratings yet
- EpinephrineDocument14 pagesEpinephrineAndriy SubieNo ratings yet
- Spesifikasi Agilia SP TIVA ID: Pt. Fresenius Kabi IndonesiaDocument1 pageSpesifikasi Agilia SP TIVA ID: Pt. Fresenius Kabi IndonesiaSajar BudiNo ratings yet
- SPIRIVA HandiHaler InstructionsDocument9 pagesSPIRIVA HandiHaler InstructionsElla Masliana DewiNo ratings yet
- FINALS NCM 106 Lesson 1 Part 1 Drugs Acting in The Central and Peripheral Nervous System Week 1Document4 pagesFINALS NCM 106 Lesson 1 Part 1 Drugs Acting in The Central and Peripheral Nervous System Week 1Rayanna MaligaNo ratings yet
- Actiivity No. 4 Functions and Responsibilities of Pharmacy and Therapeutics CommitteeDocument5 pagesActiivity No. 4 Functions and Responsibilities of Pharmacy and Therapeutics CommitteeJovet MontesNo ratings yet
- Schedule 4 Appendix D Drugs Prescribed Restricted Substances Pharmaceutical ServicesDocument8 pagesSchedule 4 Appendix D Drugs Prescribed Restricted Substances Pharmaceutical Servicesrohan NathNo ratings yet
- Prepared By: Murari Pavan M.Pharm (Pharmaceutics) Gautham College of PharmacyDocument22 pagesPrepared By: Murari Pavan M.Pharm (Pharmaceutics) Gautham College of PharmacyAshutosh LohumiNo ratings yet
- Pharmacy Training Book Topic GuideDocument355 pagesPharmacy Training Book Topic GuideHaneen HaneenNo ratings yet
- Passo A Passo "Management" Farmacoterapia Da Asma: Updated!Document1 pagePasso A Passo "Management" Farmacoterapia Da Asma: Updated!Eduardo PalmaNo ratings yet
- Inibizione Della Ciclossigenasi e Rischio Cardiovascolare: Farmaci Antinfiammatori Non Steroidei Tradizionali e Selettivi Per La Ciclossigenasi-2Document18 pagesInibizione Della Ciclossigenasi e Rischio Cardiovascolare: Farmaci Antinfiammatori Non Steroidei Tradizionali e Selettivi Per La Ciclossigenasi-2CeceNo ratings yet
- Vancomycin Data Sheet Highlights Treatment OptionsDocument13 pagesVancomycin Data Sheet Highlights Treatment OptionsAmanuel GirmayeNo ratings yet
- New Classes of Glaucoma MedicationsDocument8 pagesNew Classes of Glaucoma MedicationsMega Mulya Dwi FitriyaniNo ratings yet
- Bronchodilators Explained: Uses, Types, and Nursing ConsiderationsDocument12 pagesBronchodilators Explained: Uses, Types, and Nursing ConsiderationsDelyn Gamutan Millan100% (1)
- Data Obat LengkapDocument165 pagesData Obat Lengkapibnu an nafisNo ratings yet
- SedativesDocument4 pagesSedativesalghashm001No ratings yet
- The Lingua Franca of Pharmaceutical Brand Name ApproachDocument43 pagesThe Lingua Franca of Pharmaceutical Brand Name ApproachMd. Masum ChowdhuryNo ratings yet
- 1 Main SheetDocument1,196 pages1 Main SheetNaeem SheikhNo ratings yet
- COVID vaccination certificate issued in IndiaDocument1 pageCOVID vaccination certificate issued in IndiaMahendra Singh jat/meel/ChoudharyNo ratings yet
- Laporan Harian Bulanan Harian ApotekDocument56 pagesLaporan Harian Bulanan Harian ApotekyusiNo ratings yet
- Ranitidine 50mg - 2ml Solution For Injection and Infusion - (EMC) Print FriendlyDocument6 pagesRanitidine 50mg - 2ml Solution For Injection and Infusion - (EMC) Print FriendlyDewi Wara ShintaNo ratings yet
- Angela Dela Cruz-MunarrizDocument29 pagesAngela Dela Cruz-MunarrizangelaNo ratings yet
- DrugmedsDocument52 pagesDrugmedsshirleyNo ratings yet
- Ketorolac vs. TramadolDocument5 pagesKetorolac vs. TramadolRully Febri AnggoroNo ratings yet
- Nausea and Vomiting PDFDocument8 pagesNausea and Vomiting PDFRoosita Arbaane SafitriNo ratings yet