Professional Documents
Culture Documents
Ajr 20 23108
Ajr 20 23108
Uploaded by
alameluOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Ajr 20 23108
Ajr 20 23108
Uploaded by
alameluCopyright:
Available Formats
Downloaded from www.ajronline.org by 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5 on 07/09/21 from IP address 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5. Copyright ARRS.
For personal use only; all rights reserved
Segmental Bowel Hypoenhancement on CT Predicts Ischemic
Mesenteric Laceration After Blunt Trauma
Alexis R. Boscak, MD1, Uttam K. Bodanapally, MD1, Tarek Elshourbagy, MBBCH2,
Kathirkamanathan Shanmuganathan, MD1,3
Gastrointestinal Imaging · Original Research
Keywords
abdominal injuries, blunt injuries, OBJECTIVE. The objectives of this study were to examine the performance of CT in
bucket-handle tears, MDCT, nonocclusive the diagnosis of ischemic mesenteric laceration after blunt trauma and to assess the pre-
mesenteric ischemia dictive value of various CT signs for this injury.
MATERIALS AND METHODS. In this retrospective study, consecutive patients with
Submitted: Mar 7, 2020 bowel and mesenteric injury diagnosed by CT or surgery from January 2011 through
Revision requested: May 7, 2020 December 2016 were analyzed. Two radiologists evaluated CT images for nine signs of
Revision received: May 18, 2020
bowel injury. The outcome evaluated was ischemic mesenteric laceration. Univariable
Accepted: Jun 17, 2020
First published online: Apr 28, 2021 analysis followed by logistic regression was performed.
RESULTS. The study included 147 patients (96 men and 51 women; median age, 35
The authors declare that they have no years; age range, 23–52 years). Thirty-three patients had surgically confirmed ischemic
disclosures relevant to the subject matter of mesenteric lacerations. CT signs that correlated with ischemic mesenteric laceration were
this article. abdominal wall injury, mesenteric contusion, free fluid, segmental bowel hypoenhance-
ment, and bowel hyperenhancement adjacent to a hypoenhancing segment. The regres-
Based on a presentation at the Radiological sion model developed after inclusion of clinical variables identified two predictors: seg-
Society of North America 2019 annual mental bowel hypoenhancement (adjusted odds ratio, 22.9 [95% CI, 7.9–66.2; p < .001] for
meeting, Chicago, IL. reviewer 1 and 20.7 [95% CI, 7.2–59.0; p < .001] for reviewer 2) and abdominal wall injury
(adjusted odds ratio, 5.26 [95% CI, 1.7–15.9; p = .003] for reviewer 1 and 5.3 [95% CI, 1.9–
15.0; p = .002] for reviewer 2), which yielded an AUC of 0.87 for predicting injury. For re-
viewer 1 and reviewer 2, the sensitivities of CT in detecting the injury were 72.3% (95% CI,
54.5–86.7%) and 78.8% (95% CI, 61.0–91.0%), respectively, whereas the specificities were
94.7% (95% CI, 88.9–98.0%), and 92.1% (95% CI, 85.5–96.3%), respectively.
CONCLUSION. CT has limited sensitivity but good specificity for detecting ischemic
mesenteric laceration, with segmental bowel hypoenhancement considered the most
predictive imaging sign.
Ischemic mesenteric laceration is a specific type of blunt bowel and mesenteric injury that
can be difficult to detect on CT [1]. It is also called bucket-handle mesenteric laceration, with
the term “bucket handle” describing a linear mesenteric tear coursing parallel to the bowel
and avulsing the terminal vascular supply, resulting in segmental bowel ischemia [2, 3]. The
affected bowel segment is immediately devascularized but is not otherwise injured, so bow-
el wall edema or hematoma is not an early feature of injury, and perforation is not present
(although necrosis may result in eventual perforation, if the injury goes undetected).
Diagnosis on CT remains a challenge, primarily because of the absence of typical find-
ings of blunt bowel injury. In a systematic literature review of 20 cases of ischemic mesen-
teric laceration, up to 58% of injuries were missed on initial workup; CT had poor sensitiv-
ity (45%), although its specificity was high (95%) [4]. A delay in diagnosing surgical bowel
injuries increases morbidity and mortality [5–7].
A mechanistic classification that discriminates ischemic from nonischemic bowel injuries
and a description of associated CT findings could aid in the appraisal of this specific injury by
Boscak et al.
Predicting Ischemic Mesenteric Laceration With CT
radiologists. Such classification broadly divides bowel and mesenteric injuries into ischemic
Gastrointestinal Imaging injuries caused by mesenteric laceration and nonischemic injuries such as perforation, con-
Original Research
tusion, intramural hematoma, or a combination of these injuries [8]. Ischemic bowel injuries
are categorized as the highest grade of blunt bowel injuries and/or mesenteric injuries, ac-
Boscak AR, Bodanapally UK, Elshourbagy TA, cording to the American Association for the Surgery of Trauma organ injury scale [9].
Shanmuganathan K
1
Department of Diagnostic Radiology and Nuclear Medicine, R Adams Cowley Shock Trauma Center, University of
doi.org/10.2214/AJR.20.23108 Maryland School of Medicine, 22 S Greene St, Baltimore, MD 21201. Address correspondence to U. K. Bodanapally
AJR 2021; 217:93–99 (ubodanapally@umm.edu).
ISSN-L 0361–803X/21/2171–93 Faculty of Medicine, Cairo University, Cairo, Egypt.
2
© American Roentgen Ray Society Deceased.
3
AJR:217, July 2021 www.ajronline.org | 93
Downloaded from www.ajronline.org by 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5 on 07/09/21 from IP address 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5. Copyright ARRS. For personal use only; all rights reserved
Boscak et al.
undergone laparotomy before CT, had not undergone abdomi-
Bowel injuries from No presurgical CT nopelvic CT within 6 hours of admission, had an inadequate CT
trauma registry (n = 371) (n = 108)
examination (defined as one for which contrast injection failed,
a nontrauma protocol was followed, or excessive motion or oth-
er artifact was observed), or had inadequate follow-up (defined
CT before laparotomy CT inadequate as the absence of a surgical note or, if nonsurgical, by a lack of
(n = 263) (n = 92) documentation at least 1 week after trauma). One author (a trau-
ma and emergency radiologist with 10 years of experience), who
did not perform study image interpretation, conducted reviews
CT adequate and per Inadequate follow-up of the trauma registry, electronic medical records, and radiology
protocol (n = 171) (n = 24) information system to select the study sample. A flowchart of the
patient selection process is presented in Figure 1.
Laparotomy
(n = 99) CT Protocol
Adequate follow-up: CT examinations conducted at admission to the hospital were
study sample (n = 147)
routinely performed in accordance with our institutional blunt
Nonoperative
management (n = 48) trauma admission protocol. Scans were obtained using 40- or 64-
MDCT scanners (Brilliance, Philips Healthcare). Enteric contrast
medium was not used. Administration of IV contrast material (100
Fig. 1—Flowchart of patient selection process. mL of iohexol; 350 mg I/mL [Omnipaque 350, GE Healthcare]) was
achieved by power injection of 60 mL at a rate of 6 mL/s, followed
The present study aimed to examine the performance of CT by 40 mL administered at a rate of 4 mL/s and then a 50-mL sa-
in the diagnosis of ischemic mesenteric laceration by use of such line flush. Arterial phase imaging of the abdomen and pelvis was
mechanistic classification and to assess the value of various CT performed after bolus tracking using a 120-HU trigger in the de-
signs in predicting this specific injury. scending thoracic aorta. The parameters that were used were
as follows: tube voltage, 120 kVp; tube current–exposure time
Materials and Methods product, 250 mAs; collimation, 0.625 mm; and reconstruction
Study Design with a 3-mm slice thickness and 3-mm intervals. Portal venous
This retrospective study was HIPAA compliant and was ap- phase imaging was performed only through the upper abdo-
proved by the institutional review board at the University of men during the early portion of the study. Because portal venous
Maryland School of Medicine. A waiver of informed consent phase images through the entire abdomen and pelvis were not
was provided. available for all study patients, only arterial phase images were
Consecutive patients who were admitted to our level I trauma used for review.
center from January 2011 through December 2016 were eligible
for inclusion. Inclusion criteria were age 18 years or older, blunt CT Image Interpretation and Definitions
force trauma, and diagnosis of bowel injury per the trauma reg- For each study patient, arterial phase CT images were loaded
istry (with both clinical CT and surgical diagnoses included). A re- to a dedicated study worklist on the PACS (AGFA IMPAX, AGFA
view of the electronic medical records and the radiology informa- Healthcare) by the same trauma and emergency radiologist who
tion system was performed to exclude those patients who had reviewed the trauma registry. The images were evaluated for a
TABLE 1: Unadjusted Analysis of CT Signs Predictive of Ischemic Mesenteric Lacerations for Both Reviewers
Reviewer 1 Reviewer 2
Variable Unadjusted OR (95% CI) p Unadjusted OR (95% CI) p
Abdominal wall injury 7.2 (2.8–17.9) < .001 a
6.2 (2.7–14.4) < .001a
Mesenteric contusion 7.0 (2.0–24.3) .002a 10.5 (2.4–46.0) .002a
Mesenteric vascular lesion 2.1 (0.7–6.7) .22 2.3 (0.8–6.4) .11
Pneumoperitoneum 1.6 (0.6–4.1) .32 1.5 (0.6–3.6) .38
Free fluid 7.8 (1.8–34.1) .007a 12.0 (1.6–91.0) .01a
Bowel wall thickening 2.0 (0.9–4.5) .08 1.2 (0.5–2.5) .70
Focal wall defect 1.8 (0.15–19.9) .65 2.4 (0.4–14.9) .34
Segmental hypoenhancement of bowel 27.7 (10.1–75.7) < .001a 22.7 (8.5–61.0) < .01a
Hyperenhancement of bowel adjacent to hypoenhancing segment 11.3 (1.1–112.0) .04a 6.6 (1.5–29.3) .01a
Note—OR = odds ratio.
a
Statistically significant.
94 AJR:217, July 2021
Downloaded from www.ajronline.org by 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5 on 07/09/21 from IP address 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5. Copyright ARRS. For personal use only; all rights reserved
Predicting Ischemic Mesenteric Laceration With CT
total of nine CT signs of blunt bowel and mesenteric injury as de- ment of bowel wall was defined as nonenhancement or hypoen-
scribed in the literature [10–13] (Table 1). CT studies were rated hancement of a segment of bowel loop (Figs. 2A, 2C, 3A, and 3B).
using a binary variable. Reviewer 1 (a trauma radiologist with 10 Hyperenhancement of bowel adjacent to a hypoenhancing seg-
years of experience) and reviewer 2 (a trauma radiologist with 25 ment was defined as relative segmental hyperenhancement ad-
years of experience) were instructed to identify all studies as hav- jacent to hypoenhancing segment.
ing positive or negative findings for each sign and the specific
diagnosis of ischemic mesenteric laceration. For CT diagnosis of Reference Standard
ischemic mesenteric laceration, discrepancies between the initial Laparotomy notes, discharge summaries, and records from fol-
assessments of the two reviewers were subsequently evaluated low-up clinic visits were used to determine the presence or ab-
in concert, and consensus was reached. Consensus review was sence of ischemic mesenteric laceration. Laparotomy findings
not performed for individual CT signs. were considered positive if mesenteric laceration was associat-
ed with adjacent segmental bowel ischemia. Patients with nega-
Study Term Definitions tive laparotomy findings or successful nonoperative management
Specific study definitions of CT findings of bowel and mes- (minimum postinjury follow-up, 1 week) were considered to have
enteric injury were established. Abdominal wall injury was de- findings negative for ischemic mesenteric laceration. At our study
fined as the presence on CT of seat belt sign (transverse and/or institution, management of patients with CT findings of nonsur-
diagonal contusions across the abdomen), traumatic abdominal gical bowel or mesenteric injury is usually formulated on an indi-
wall hernias (including lumbar hernias), and any abdominal wall vidual basis. Patients whose condition is stable and who have CT
contusions in patients who were not involved in a motor vehi- findings of nonsurgical injury or otherwise unexplained findings
cle collision (MVC) (Figs. 2A and 2B). Mesenteric contusion was of intraperitoneal free fluid are evaluated with follow-up CT per-
defined as mesenteric fat stranding with or without organized formed 4 to 6 hours after the initial CT examination or serial clin-
mesenteric hematoma (Figs. 2A–2C). Mesenteric vascular lesions ical examinations to identify radiologic or clinical deterioration.
were defined as vascular irregularity or beading (in milder forms
of injury) or active bleeding (in more severe injuries). Free fluid Statistical Analysis
was defined as unexplained intraperitoneal free fluid (a moder- Data for continuous variables are summarized as mean (± SD)
ate-to-large volume of pelvic fluid, a small volume of multifocal values for normally distributed variables and as median (first
fluid, interloop or intermesenteric fluid, or high-attenuation [≥ 15 quartile and third quartile) values for nonnormally distributed
HU] fluid) (Fig. 2C). Bowel wall thickening was defined as circum- variables. Categoric variables are summarized as counts and per-
ferential or eccentric bowel wall thickening. Although described centages. The effect of each CT predictive variable on ischemic
as wall thickness greater than 3 mm (for small bowel) or 5 mm mesenteric laceration without adjusting for other predictors was
(for large bowel) in the presence of adequate distention of the lu- determined, and the unadjusted odds ratio (OR) and correspond-
men, bowel wall thickening was rated subjectively in the present ing 95% CIs were calculated. Predictors for which p < .10 on un-
study, as in routine clinical practice. Segmental hypoenhance- adjusted analysis were incorporated into the logistic regression
Fig. 2—60-year-old man with right flank injury after
motorcycle crash.
A B A, Axial arterial phase CT image shows segmental
hypoenhancement of ileum (straight white
arrow), hyperenhancement of bowel adjacent to
hypoenhancing segment (curved arrow), mesenteric
contusion (red arrow), and abdominal wall injury
(subcutaneous soft-tissue contusion) (arrowhead).
B, Axial arterial phase CT image shows large area of
mesenteric contusion (arrows) and abdominal wall
injury (arrowhead).
C, Coronal arterial phase CT image shows segmental
hypoenhancement of ileum (thick white arrow), well-
defined demarcation between normally enhancing
segment and hypoenhancing segment (arrowheads),
mesenteric contusion (red arrow), and free fluid in
pelvic peritoneum (thin white arrow).
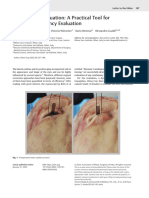
D, Intraoperative photograph of surgical specimen
shows large bucket-handle tear (arrows) with
devascularized ileum.
C D
AJR:217, July 2021 95
Downloaded from www.ajronline.org by 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5 on 07/09/21 from IP address 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5. Copyright ARRS. For personal use only; all rights reserved
Boscak et al.
Fig. 3—24-year-old man with abdominal injury after
motor vehicle collision.
A and B, Axial arterial phase CT images show
segmental hypoenhancement of ileum (arrow) and
sharp demarcation with enhancing wall (curved
arrow).
A B
model to select the best independent predictors. The final model increase in the odds of ischemic mesenteric laceration developing
for the diagnosis was developed using the backward elimination after an MVC (OR, 1.04; 95% CI, 0.4–2.7; p = .90) compared with in-
method based on Akaike information criterion. juries not associated with an MVC. A higher injury severity score
For the prediction model for the specific injury, ROC analy- (OR, 1.03; 95% CI, 0.99–1.06; p = .12) also showed no increased
sis was performed to assess the overall predictive ability of the OR. Laparotomy was performed for bowel injuries in 99 patients,
model using the ROC AUC and corresponding SE. Sensitivity and whereas nonoperative management was successful for 48 pa-
specificity analysis and interobserver agreement for the overall tients. A total of 33 patients had surgically proven ischemic mes-
ability of CT as well as individual CT variables in diagnosing isch- enteric lacerations. The right lower quadrant mesentery was the
emic mesenteric laceration were obtained from contingency ta- most common site of laceration, with 17 injuries resulting in ileal
bles. The kappa coefficient (κ) was used to measure interobserver devascularization, followed by jejunal mesentery (n = 8), the com-
agreement. Kappa results were interpreted as follows: ≤ 0 denot- bination of jejunal and ileal mesentery (n = 4), sigmoid mesocolon
ed no agreement; 0.01–0.2, none to slight agreement; 0.21–0.4, (n = 2), left mesocolon (n = 1), and transverse mesocolon (n = 1).
fair agreement; 0.41–0.6, moderate agreement; 0.61–0.8, sub-
stantial agreement; and 0.81–1.0, almost perfect agreement. All Unadjusted and Adjusted Association of CT Signs With
analyses were performed using commercially available statistical Ischemic Mesenteric Laceration
software (JMP 12 software, SAS Institute). Without adjustment for other factors, the CT signs that cor-
related with a higher incidence of mesenteric laceration were ab-
Results dominal wall injury (Figs. 2A and 2B) (OR, 7.1 [95% CI, 2.8–17.9; p <
The baseline clinical characteristics of the 147 patients in the .001] for reviewer 1 and 6.2 [95% CI, 2.7–14.4; p < .001] for reviewer
study sample (96 men and 51 women; median age, 35 years; age 2), mesenteric contusion (Figs. 2A–2C) (OR, 7.0 [95% CI, 2.0–24.3;
range, 23–52 years) are shown in Table 2. There was no significant p = .002] for reviewer 1 and 10.5 [95% CI, 2.4–46.0; p = .002] for re-
TABLE 2: Baseline Characteristics of Study Population
Patients With Ischemic Patients Without Ischemic
Characteristic Mesenteric Laceration (n = 33) Mesenteric Laceration (n = 114) All Patients (n = 147)
Age (y), median (Q1, Q3) 42 (25, 53.5) 34 (23, 52) 35 (23, 52)
Sex
Male 17 (11.6) 79 (53.7) 96 (65.3)
Female 16 (10.9) 35 (23.8) 51 (34.7)
ISS, median (Q1, Q3) 29 (19, 41) 26 (17, 36) 27 (17, 41)
Mechanism of injury
MVC 26 (17.7) 89 (60.5) 115 (78.2)
Fall 0 (0) 11 (7.5) 11 (7.5)
MCC 3 (2.0) 4 (2.7) 7 (4.8)
Pedestrian injuries 2 (1.4) 3 (2.0) 5 (3.4)
Industrial accidents 0 (0) 3 (2.0) 3 (2.0)
Assaults 0 (0) 2 (1.4) 2 (1.4)
Kicked by horse 1 (0.7) 1 (0.7) 2 (1.4)
ATV accident 0 (0) 1 (0.7) 1 (0.7)
Personal watercraft 1 (0.7) 0 (0) 1 (0.7)
Note—Except where otherwise indicated, data are number of patients (percentage of all 147 patients). Q1 = first quartile, Q3 = third quartile, ISS = injury severity score,
MVC = motor vehicle collision, MCC = motorcycle crash; ATV = all-terrain vehicle.
96 AJR:217, July 2021
Downloaded from www.ajronline.org by 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5 on 07/09/21 from IP address 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5. Copyright ARRS. For personal use only; all rights reserved
Predicting Ischemic Mesenteric Laceration With CT
TABLE 3: Sensitivity and Specificity of Overall CT Diagnosis and Individual CT Signs in the Diagnosis
of Ischemic Mesenteric Laceration Along With Interobserver Agreement
Reviewer 1 Reviewer 2
Sensitivity, % Specificity, % Sensitivity, % Specificity, % Interobserver Agreement,
Variable (95% CI) (95% CI) (95% CI) (95% CI) κ (95% CI)
CT diagnosis of ischemic mesenteric laceration 72.3 [24/33] 94.7 [108/114] 78.8 [26/33] 92.1 [105/114] 0.66 (0.52–0.81)
(54.5–86.7) (88.9–98.0) (61.0–91.0) (85.5–96.3)
Abdominal wall injury 78.8 [26/33] 65.8 [75/114] 63.6 [21/33] 78.1 [89/114] 0.7 (0.59–0.82)
(61.0–91.0) (56.3–74.4) (45.0–79.6) (69.3–85.3)
Mesenteric contusion 90.9 [30/33] 41.2 [47/114] 93.9 [31/33] 40.4 [46/114] 0.51 (0.36–0.66)
(75.7–98.0) (32.0– 50.8) (79.8–99.3) (31.3–50.0)
Mesenteric vascular lesion 15.1 [5/33] 92.1 [105/114] 21.2 [7/33] 89.5 [102/114] 0.63 (0.42–0.83)
(5.0–31.9) (85.5–96.3) (9.0–38.9) (82.3–94.4)
Pneumoperitoneum 24.2 [8/33] 83.3 [95/114] 27.3 [9/33] 79.8 [91/114] 0.81 (0.69–0.93)
(11.0–42.3) (75.2–89.7) (13.3–45.5) (71.3–86.8)
Free fluid 93.9 [31/33] 33.3 [38/114] 97.0 [32/33] 27.2 [31/114] 0.6 (0.45–0.75)
(79.8–99.3) (24.8–42.8) (84.2–99.9) (19.3–36.3)
Bowel wall thickening 63.6 [21/33] 53.5 [61/114] 48.5 [16/33] 55.3 [63/114] 0.42 (0.27–0.56)
(45.1–79.6) (43.9–62.9) (30.8–66.5) (45.6–64.6)
Focal wall defect 3.0 [1/33] 98.2 [112/114] 6.0 [2/33] 97.4 [111/114] 0.74 (0.4–1.0)
(0.1–15.8) (93.8–99.8) (0.7–20.2) (92.5–99.4)
Segmental hypoenhancement of bowel 72.7 [24/33] 91.2 [104/114] 78.8 [26/33] 86.0 [98/114] 0.61 (0.47–0.76)
(54.5–86.7) (84.5–95.7) (61.0–91.0) (78.2–91.8)
Hyperenhancement of bowel adjacent to 9.0 [3/33] 99.1 [113/114] 15.1 [5/33] 97.4 [111/114] 0.14 (−0.15 to 0.42)
hypoenhancing segment (1.9–24.3) (95.2–99.9) (5.1–31.9) (92.5–99.5)
Note—Except where otherwise indicated, data are percentage [number of CT-positive patients/number of patients with injury] for Sensitivity columns and [number of
CT-negative patients/number of patients without injury] for Specificity columns (95% CI). Kappa coefficient was interpreted as follows: values ≤ 0 indicated no agreement;
0.01–0.2, no to slight agreement; 0.21–0.4, fair agreement; 0.41–0.6, moderate agreement; 0.61–0.8, substantial agreement; and 0.81–1.0, almost perfect agreement.
viewer 2), free fluid (Fig. 2C) (OR, 7.8 [95% CI, 1.8–34.1; p = .007] for odds by four to five times (adjusted OR, 5.26 [95% CI, 1.7–15.9; p =
reviewer 1 and 12.0 [95% CI, 1.6–91.0; p = .01] for reviewer 2), seg- .003] for reviewer 1 and 5.3 [95% CI, 1.9–15.0; p = .002] for reviewer
mental bowel hypoenhancement (Figs. 2A, 2C, 3A, and 3B) (OR, 2). ROC analysis performed using the combination of the two CT
27.7 [95% CI, 10.1–75.7; p < .001] for reviewer 1 and 22.7 [95% CI, predictors yielded an AUC (standard error) of 0.87 (0.04) for both
8.5–61.0; p < .001] for reviewer 2), and bowel hyperenhancement reviewers 1 and 2 in identifying the injury.
adjacent to a hypoenhancing segment (Fig. 2A) (OR, 11.3 [95% CI,
1.1–112.0; p = .04] for reviewer 2 and 6.6 [95% CI, 1.5–29.3; p = .01] Sensitivity and Specificity of CT and Individual CT Signs in
for reviewer 2). There was no correlation with mesenteric vascu- Diagnosing of Ischemic Mesenteric Laceration
lar lesion, pneumoperitoneum, focal bowel wall defect, and bow- The overall sensitivity of CT in detecting the injury was 72.3%
el wall thickening. Age (OR, 0.99; 95% CI, 0.97–1.02; p < .60), sex (24/33; 95% CI, 54.5–86.7%) for reviewer 1 and 78.8% (26/33; 95%
(OR, 0.47; 95% CI, 0.21–1.00; p < .06), and mechanism of injury (OR, CI, 61.0–91.0%) for reviewer 2, whereas the specificity was 94.7%
1.04; 95% CI, 0.4–2.7; p < .93) were clinical variables that were not (108/114; 95% CI, 88.9–98.0%) for reviewer 1 and 92.1% (105/114;
correlated with a higher incidence of mesenteric laceration. Com- 95% CI, 85.5–96.3%) for reviewer 2, respectively. The overall sen-
plete details are provided in Table 1. sitivity of CT in diagnosing the injury improved to 81.8% (27/33;
Logistic regression analysis performed after inclusion of clini- 95% CI, 64.5–93.0%), and specificity improved to 98.2% (112/114;
cal and CT variables for which p < .10 identified two independent 95% CI, 93.8–99.8%) after the discrepant interpretations were
predictors with significance in identifying injury: segmental bow- reviewed together by the two radiologists and a final decision
el hypoenhancement (adjusted odds ratio, 22.9 [95% CI, 7.9–66.2; made based on consensus. Individual sensitivities and specifici-
p < .001] for reviewer 1 and 20.7 [95% CI, 7.2–59.0; p < .001] for ties of each CT signs are presented in Table 3.
reviewer 2) and abdominal wall injury (adjusted odds ratio, 5.26 The interobserver agreement between the two reviewers in
[95% CI, 1.7–15.9; p = .003] for reviewer 1 and 5.3 [95% CI, 1.9–15.0; detecting the ischemic mesenteric lacerations was reflected by a
p = .002] for reviewer 2), which yielded an AUC of 0.87 for predict- kappa coefficient of 0.66 (95% CI, 0.52–0.81). The degree of agree-
ing injury. On average, the finding of segmental bowel hypoen- ment for each of the CT signs is shown in Table 3. Of the 147 stud-
hancement increased the odds of ischemic mesenteric laceration ies reviewed, nine studies had no CT signs of bowel and mesen-
(Fig. 2D) by 20–22 times (adjusted OR, 22.9 [95% CI, 7.9–66.2; p < teric injury identified by reviewer 1, six studies had no such signs
.001] for reviewer 1 and 20.7 [95% CI, 7.2–59.0; p < .001] for review- identified by reviewer 2, and three studies had concordant find-
er 2). The presence of abdominal wall injury on CT increased the ings according to both reviewers.
AJR:217, July 2021 97
Downloaded from www.ajronline.org by 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5 on 07/09/21 from IP address 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5. Copyright ARRS. For personal use only; all rights reserved
Boscak et al.
Discussion of the difficulty of placing ROIs on relatively thin bowel walls.
The major findings from the present study are that segmental The abdominal wall injury CT sign in our study encompassed a
hypoenhancement of the bowel was the CT sign with the high- broad range of injuries (seat belt sign, traumatic abdominal wall
est OR for injury, segmental hypoenhancement of the bowel and hernias including lumbar hernias, and any abdominal wall con-
abdominal wall injury on CT were independent predictors of in- tusions). Evidence exists that characterization of seat belt sign
jury on regression analysis, and the sensitivity of CT in detecting in relation to the anterior superior iliac spine and the contusion
ischemic mesenteric laceration ranged from 72.3% (95% CI, 54.5– depth has a better ability to predict the need for abdominal sur-
86.7%) to 78.8% (95% CI, 61.0–91.0%), whereas specificity ranged gery, although the study did not specifically look at ischemic
from 94.7% (95% CI, 88.9–98.0%) to 92.1% (95% CI, 85.5–96.3%). mesenteric lacerations [17]. However, the present study did not
To our knowledge, this is the first study to report the accura- characterize abdominal wall injuries on the basis of their ana-
cy of CT in the specific diagnosis of ischemic mesenteric lacera- tomic relations and morphologic features; therefore, the best
tion. A previous study by Matsushima et al. [8] showed that the precision may not have been achieved.
incidence of ischemic mesenteric laceration was 39% in a sample The CT finding of segmental bowel hypoenhancement after
of 67 patients, which is in contrast to the incidence of 22% seen blunt trauma reflects focal interruption of vascular inflow, as a re-
in our study sample. This discrepancy might be due to the selec- sult of transection of terminal arteries at the site of mesenteric lac-
tion bias introduced in the earlier study, which resulted from the eration. The affected bowel segment parallels the mesenteric lacer-
narrow inclusion criteria that required laparotomy as the refer- ation, with abrupt transition from normal to abnormal bowel wall
ence standard. Our broader selection criterion resulted in the in- enhancement at the margins of injury. The associated phenom-
clusion of all patients with CT findings of bowel injury with both enon of relative bowel wall hyperenhancement adjacent to a hy-
laparotomy and clinical follow-up used as the reference stan- poenhancing segment may reflect inflammatory hyperemia (in-
dard. The inclusion of patients with unexplained intraperitoneal creased contrast inflow), venous congestion (decreased contrast
free fluid in the absence of solid organ injury likely helped min- outflow), a pathologic increase in endothelial permeability (intersti-
imize the probability of missed injuries because intraperitone- tial contrast accumulation), or a combination of these findings [18].
al free fluid is the CT sign with the highest reported sensitivity It is important to note that several classic CT signs of surgical
(range, 81–100%) for detecting bowel and mesenteric injuries [10, bowel and mesenteric injury are not strongly associated with isch-
12–14]. The same study also found no CT findings that differed emic mesenteric laceration. These include signs of direct bowel
significantly between ischemic injury and nonischemic injury [8]. trauma and perforation, such as bowel wall edema or thickening,
However, the present study found various CT signs to be more extraluminal gas, and focal bowel wall defect, which are not fea-
prevalent in ischemic mesenteric laceration, including abdomi- tures of ischemic mesenteric laceration in its early stages. Mes-
nal wall injury, mesenteric contusion, free fluid, segmental bowel enteric contusion may be present but is nonspecific. Mesenteric
hypoenhancement, and bowel hyperenhancement adjacent to a vascular lesions (including vascular beading and active bleeding)
hypoenhancing segment. are more specific but show very low sensitivity.
The most common mechanism of ischemic mesenteric lacera- In the present study, only arterial phase CT images were re-
tion, which is associated with use of a seat belt restraint, is a rap- viewed. To our knowledge, no published reports have compared
id deceleration force caused by a motor vehicle collision (MVC) the utility of arterial versus portal venous phase CT in bowel and
[1, 7]. Our results are consistent with those of prior reports, with mesenteric injury. However, previous studies that compared the
the highest number of injuries occurring after MVC, although the enhancement of ischemic versus nonischemic bowel segments
results also showed that there was no significant increase in the in nontraumatic disease have described a greater difference in
odds of injury after MVC. Mesenteric lacerations seem to result attenuation in the arterial phase, providing higher contrast and
from shearing forces at the junction of mobile and fixed bowel improving lesion conspicuity [19]. Extrapolating these findings,
segments, with the most common injury site involving the right we think that arterial phase imaging is adequate for evaluating
lower quadrant [2, 15, 16]. Similar results were obtained in the ischemic mesenteric laceration. There is no consensus regard-
present study, which noted that the most common site of inju- ing whole-body CT protocol in trauma patients. Studies have
ry was the right lower quadrant with ileal devascularization, fol- indicated that biphasic image acquisition is optimal for detect-
lowed by the jejunal mesentery and mesocolon. ing traumatic vascular lesions in the spleen [20, 21]. Such a pro-
The two CT signs (segmental hypoenhancement of the bowel tocol includes arterial phase imaging from the thoracic inlet to
and abdominal wall injury) that were the independent predic- the greater trochanters, to screen for vascular injuries, and portal
tors of injury had kappa values of 0.61 and 0.7 (indicating sub- venous phase imaging through the upper abdomen, to screen
stantial agreement), respectively. The present study relied on for solid organ injuries during peak parenchymal enhancement.
subjective assessment of bowel wall attenuation and did not for- However, the sensitivity of CT for some abnormalities, especially
mally quantify differential enhancement. Dual-energy CT may active bleeding, may be decreased if portal venous phase imag-
increase the sensitivity and diagnostic confidence in detecting ing is not extended through the injury site [12].
bowel wall hypoenhancement through the use of low-kiloelec- Based on the results of this study, the limitations of CT in the di-
tron-volt virtual monoenergetic images and iodine maps, by ac- agnosis of ischemic mesenteric laceration must be emphasized,
centuating the subtle enhancement differences [10]. Quantita- despite improved awareness of this injury among radiologists [1].
tive measurements of bowel wall enhancement (expressed as Because delayed surgical repair increases morbidity and mortal-
Hounsfield units) or iodine content are also possible on dual-en- ity, maximizing the accuracy of CT is essential to optimize out-
ergy CT iodine maps but can be extremely challenging because comes. Increased scrutiny for the predictive and associated CT
98 AJR:217, July 2021
Downloaded from www.ajronline.org by 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5 on 07/09/21 from IP address 2409:4062:4e09:1dbd:ede2:f369:f9bc:37d5. Copyright ARRS. For personal use only; all rights reserved
Predicting Ischemic Mesenteric Laceration With CT
signs described in the present study should improve the sensitiv- from 275,557 trauma admissions from the East multi-institutional trial.
ity and specificity of CT diagnosis. J Trauma 2003; 54:289–294
The present study has a number of limitations. It has a retro- 6. Fakhry SM, Watts DD, Luchette FA; EAST Multi-Institutional Hollow Viscus
spective single-center design, which introduces selection and in- Injury Research Group. Current diagnostic approaches lack sensitivity in
stitutional biases. The sample was limited to patients with bowel the diagnosis of perforated blunt small bowel injury: analysis from 275,557
injury who underwent CT followed by laparotomy or close clinical trauma admissions from the EAST multi-institutional HVI trial. J Trauma
follow-up; this was done to capture most patients with both sur- 2003; 54:295–306
gical and nonsurgical bowel injuries with the use of reliable ref- 7. Fakhry SM, Brownstein M, Watts DD, Baker CC, Oller D. Relatively short di-
erence standards. The study also had a variety of exclusion crite- agnostic delays (<8 hours) produce morbidity and mortality in blunt small
ria, as previously described, and it is of note that the study could bowel injury: an analysis of time to operative intervention in 198 patients
not include patients who underwent immediate laparotomy af- from a multicenter experience. J Trauma 2000; 48:408–414; discussion,
ter blunt trauma without presurgical CT. As such, the specificity 414–415
data from this nonrandom sample may not be generalizable to all 8. Matsushima K, Mangel PS, Schaefer EW, Frankel HL. Blunt hollow viscus
trauma patients. The study sample had a high incidence of bowel and mesenteric injury: still underrecognized. World J Surg 2013; 37:759–765
injury, likely introducing both attribution and availability biases 9. Moore EE, Cogbill TH, Malangoni MA, et al. Organ injury scaling. II. Pancre-
into CT interpretation, particularly because ischemic mesenter- as, duodenum, small bowel, colon, and rectum. J Trauma 1990; 30:1427–
ic laceration is a relatively uncommon injury. Finally, only arterial 1429
phase CT images were reviewed. The authors acknowledge that 10. Dattwyler M, Bodanapally UK, Shanmuganathan K. Blunt injury of the
CT protocols are diverse and that many centers do not routinely bowel and mesentery. Curr Radiol Rep 2018; 6:17
acquire arterial phase images through the abdomen and pelvis. 11. Choi AY, Bodanapally UK, Shapiro B, Patlas MN, Katz DS. Recent advances in
Our results do not establish diagnostic performance in the por- abdominal trauma computed tomography. Semin Roentgenol 2018;
tal venous phase, thereby limiting the applicability of our study. 53:178–186
12. Bates DD, Wasserman M, Malek A, et al. Multidetector CT of surgically prov-
Conclusion en blunt bowel and mesenteric injury. RadioGraphics 2017; 37:613–625
Ischemic mesenteric laceration presents a diagnostic chal- 13. Abdel-Aziz H, Dunham CM. Effectiveness of computed tomography scan-
lenge to radiologists interpreting CT images of the abdomen ning to detect blunt bowel and mesenteric injuries requiring surgical inter-
and pelvis obtained after blunt trauma. Increased attention to vention: a systematic literature review. Am J Surg 2019; 218:201–210
bowel wall hypoenhancement as a specific CT finding predic- 14. LeBedis CA, Anderson SW, Bates DD, et al. CT imaging signs of surgically
tive of this injury, knowledge of the association with abdominal proven bowel trauma. Emerg Radiol 2016; 23:213–219
wall injury, and awareness of the typical absence of several clas- 15. Fakhry SM, Allawi A, Ferguson PL, et al.; EAST small bowel perforation (SBP)
sic CT signs of blunt bowel and/or mesenteric injuries should Multi-Center Study Group. Blunt small bowel perforation (SBP): an Eastern
inform the interpretation of blunt trauma CT for patients at risk Association for the Surgery of Trauma multicenter update 15 years later. J
for this surgical lesion. Trauma Acute Care Surg 2019; 86:642–650
16. Hawkins AE, Mirvis SE. Evaluation of bowel and mesenteric injury: role of
Acknowledgment multidetector CT. Abdom Imaging 2003; 28:505–514
We thank Brigitte Pocta for editing the manuscript. 17. Johnson MC, Eastridge BJ. Redefining the abdominal seatbelt sign: en-
hanced CT imaging metrics improve injury prediction. Am J Surg 2017;
References 214:1175–1179
1. Extein JE, Allen BC, Shapiro ML, Jaffe TA. CT findings of traumatic buck- 18. Mirvis SE, Shanmuganathan K, Erb R. Diffuse small-bowel ischemia in hy-
et-handle mesenteric injuries. AJR 2017; 209:[web]W360–W364 potensive adults after blunt trauma (shock bowel): CT findings and clinical
2. Nosanov LB, Barthel ER, Pierce JR. Sigmoid perforation and bucket-handle significance. AJR 1994; 163:1375–1379
tear of the mesocolon after bicycle handlebar injury: a case report and re- 19. Ohira G, Shuto K, Kono T, et al. Utility of arterial phase of dynamic CT for
view of the literature. J Pediatr Surg 2011; 46:e33–e35 detection of intestinal ischemia associated with strangulation ileus. World
3. Dinatti LA, Meagher DP Jr, Martinez-Frontanilla LA. “Bucket handle” avul- J Radiol 2012; 4:450–454
sion of intestine in gastroschisis. J Pediatr Surg 1993; 28:840 20. Boscak AR, Shanmuganathan K, Mirvis SE, et al. Optimizing trauma multi-
4. Kordzadeh A, Melchionda V, Rhodes KM, Fletcher EO, Panayiotopolous YP. detector CT protocol for blunt splenic injury: need for arterial and portal
Blunt abdominal trauma and mesenteric avulsion: a systematic review. Eur venous phase scans. Radiology 2013; 268:79–88
J Trauma Emerg Surg 2016; 42:311–315 21. Uyeda JW, LeBedis CA, Penn DR, Soto JA, Anderson SW. Active hemorrhage
5. Watts DD, Fakhry SM; EAST Multi-Institutional Hollow Viscus Injury Re- and vascular injuries in splenic trauma: utility of the arterial phase in multi-
search Group. Incidence of hollow viscus injury in blunt trauma: an analysis detector CT. Radiology 2014; 270:99–106
AJR:217, July 2021 99
You might also like
- NIHSS Scoring: Coma Difficult or Confused TipsDocument1 pageNIHSS Scoring: Coma Difficult or Confused TipsDanielMahendra100% (1)
- ALZHEIMERSDocument16 pagesALZHEIMERSKathleen DiangoNo ratings yet
- ACLS HandoutsDocument4 pagesACLS HandoutshasanNo ratings yet
- Urban - Evaluation of The Combination of Strip Gingival Grafts and A Xenogeneic Collagen Matrix For The Treatment of Severe Mucogingival DefectsDocument7 pagesUrban - Evaluation of The Combination of Strip Gingival Grafts and A Xenogeneic Collagen Matrix For The Treatment of Severe Mucogingival DefectsEliza DraganNo ratings yet
- Pcos Purposal 1Document33 pagesPcos Purposal 1sushma shrestha0% (2)
- The Functional Anatomy of The Deep Facial Fat Compartments: A Detailed Imaging-Based InvestigationDocument11 pagesThe Functional Anatomy of The Deep Facial Fat Compartments: A Detailed Imaging-Based InvestigationFernanda RibeiroNo ratings yet
- Hand Book of Veterinary Internal MedicineDocument88 pagesHand Book of Veterinary Internal MedicineDanielle Fisher91% (11)
- M05 Writing Case Study 1 - BrandyDocument6 pagesM05 Writing Case Study 1 - BrandyMad MaximusNo ratings yet
- Gridhrasi Case PresentationDocument35 pagesGridhrasi Case PresentationAmogha Kulkarni100% (1)
- 0004-Table of Contents-V-Viii-9780702071546 PDFDocument4 pages0004-Table of Contents-V-Viii-9780702071546 PDFcont2chanduNo ratings yet
- Geriatric Optometry and Pediatric OptometryDocument2 pagesGeriatric Optometry and Pediatric OptometryRony MathewsNo ratings yet
- Pedersen Babu LymphaticsDocument10 pagesPedersen Babu Lymphaticsrandy22002No ratings yet
- Extein Et Al 2017 CT Findings of Traumatic Bucket Handle Mesenteric InjuriesDocument5 pagesExtein Et Al 2017 CT Findings of Traumatic Bucket Handle Mesenteric Injuries132 Naga VamsiNo ratings yet
- Outcome of 1000 Patients With Gastrointestinal.20Document11 pagesOutcome of 1000 Patients With Gastrointestinal.20drhusseinfaour3126No ratings yet
- Ankle and Foot Injuries:: Analysis of MDCT FindingsDocument8 pagesAnkle and Foot Injuries:: Analysis of MDCT FindingsraditNo ratings yet
- Dual-Targeted Synthetic Nanoparticles For Cardiovascular Diseases - ACS-AMIDocument11 pagesDual-Targeted Synthetic Nanoparticles For Cardiovascular Diseases - ACS-AMIBhabatosh Banik , Cotton University, AssamNo ratings yet
- CT-Derived Body Composition Assessment As A Prognostic ToolDocument10 pagesCT-Derived Body Composition Assessment As A Prognostic ToolWenwen NiNo ratings yet
- Dias Et Al 2013 The Effectiveness of Postoperative Physical Therapy Treatment in Patients Who Have UndergoneDocument17 pagesDias Et Al 2013 The Effectiveness of Postoperative Physical Therapy Treatment in Patients Who Have UndergoneDiogo MarquesNo ratings yet
- Imaging Analyses of Bone Tumors JBJSDocument11 pagesImaging Analyses of Bone Tumors JBJSVera VeraNo ratings yet
- Sainani 2009Document10 pagesSainani 2009Patricia BezneaNo ratings yet
- Fonc 11 631686Document11 pagesFonc 11 631686pasyaNo ratings yet
- Carlos Eduardo Torres Fuentes Arthroscopic AssistedDocument6 pagesCarlos Eduardo Torres Fuentes Arthroscopic AssistedJuan HoyosNo ratings yet
- Bcs Article RoleDocument15 pagesBcs Article RoleSowmya ANo ratings yet
- CV Ajr.19.22578Document10 pagesCV Ajr.19.22578Andi Wetenri PadaulengNo ratings yet
- Identifying The Anatomical Variations of The.20Document7 pagesIdentifying The Anatomical Variations of The.20FERNANDO ALVESNo ratings yet
- CT Predictors of Unfavorable Clinical Outcomes of Acute Right Colonic DiverticulitisDocument10 pagesCT Predictors of Unfavorable Clinical Outcomes of Acute Right Colonic DiverticulitisDiego Andres VasquezNo ratings yet
- Effect of Timing of ACL Reconstruction in Surgery and Development of Meniscal and Chondral LesionsDocument6 pagesEffect of Timing of ACL Reconstruction in Surgery and Development of Meniscal and Chondral LesionsPascha ParamurthiNo ratings yet
- Case Report Stensrud2012Document13 pagesCase Report Stensrud2012marcus souzaNo ratings yet
- Aesthetic and Functional Abdominoplasty .35Document9 pagesAesthetic and Functional Abdominoplasty .35Lucila MangasNo ratings yet
- Artigo Cientifico Dia 02-08Document10 pagesArtigo Cientifico Dia 02-08DOUGLAS LIEBELNo ratings yet
- Meniscus (Materi Fisio Beni)Document30 pagesMeniscus (Materi Fisio Beni)Atikah SaraswatiNo ratings yet
- Arthrodesis in The Charcot FooDocument6 pagesArthrodesis in The Charcot Foolatifa adluNo ratings yet
- Influence of Age On Healing Capacity of Acute Tears of The Anterior Cruciate Ligament Based On Magnetic Resonance Imaging AssessmentDocument6 pagesInfluence of Age On Healing Capacity of Acute Tears of The Anterior Cruciate Ligament Based On Magnetic Resonance Imaging Assessmentirfan.shaikh5995No ratings yet
- 16 STENSRUD A 12 Week Exercise Therapy Program in Middle Aged PatientsDocument13 pages16 STENSRUD A 12 Week Exercise Therapy Program in Middle Aged PatientsLuis MiguelNo ratings yet
- AICTE STTP Brochure On SHMDocument3 pagesAICTE STTP Brochure On SHMCF forumNo ratings yet
- 2022 Article 3346Document5 pages2022 Article 3346فرجني موغNo ratings yet
- Early Diagnostic Evaluation of Mandibular Symmetry.6Document6 pagesEarly Diagnostic Evaluation of Mandibular Symmetry.6Naliana LupascuNo ratings yet
- Anatomy of Ankle Syndesmotic Ligaments A Systematic Review of Cadaveric Studies Foot & Ankle SpecialistDocument10 pagesAnatomy of Ankle Syndesmotic Ligaments A Systematic Review of Cadaveric Studies Foot & Ankle SpecialistMarcus EstradaNo ratings yet
- Diagnostics 12 03064 v2Document31 pagesDiagnostics 12 03064 v2Kinga BazakNo ratings yet
- Pandi A Raj 2021Document8 pagesPandi A Raj 2021ShreerakshaNo ratings yet
- Kutkut 2011 Sinus WidthDocument5 pagesKutkut 2011 Sinus WidthLamis MagdyNo ratings yet
- Roles of Trauma CT and Cta in Salvaging Threateaned or Mangled ExtremityDocument18 pagesRoles of Trauma CT and Cta in Salvaging Threateaned or Mangled ExtremityJEAN CARLOS GALLO VALVERDENo ratings yet
- Lyon Et Al 2018 Computational Techniques For Ecg Analysis and Interpretation in Light of Their Contribution To MedicalDocument18 pagesLyon Et Al 2018 Computational Techniques For Ecg Analysis and Interpretation in Light of Their Contribution To MedicalPedro RigueiraNo ratings yet
- Solid Renal Masses: What The Numbers Tell Us: Stella K. Kang William C. Huang Pari V. Pandharipande Hersh ChandaranaDocument11 pagesSolid Renal Masses: What The Numbers Tell Us: Stella K. Kang William C. Huang Pari V. Pandharipande Hersh ChandaranaTạ Minh ZSNo ratings yet
- New Technique For Magnetic Compression Anastomosis.8Document10 pagesNew Technique For Magnetic Compression Anastomosis.8sjmc.surgeryresidentsNo ratings yet
- Canthopexy Evaluation - Anny SubillagaDocument2 pagesCanthopexy Evaluation - Anny SubillagaAnny SubillagaNo ratings yet
- Effect of Posterior Malleolus Fracture On.10Document6 pagesEffect of Posterior Malleolus Fracture On.10Charlie KorbaNo ratings yet
- Deep Bite Correction With An Anterior Bite Plate.13Document5 pagesDeep Bite Correction With An Anterior Bite Plate.13Umair AliNo ratings yet
- 10 2214@ajr 19 21486Document9 pages10 2214@ajr 19 21486Cinthya Añazco RomeroNo ratings yet
- Reconstruction Options and Outcomes For Acetabular Bone Loss in Revision Hip ArthroplastyDocument7 pagesReconstruction Options and Outcomes For Acetabular Bone Loss in Revision Hip ArthroplastyMohan DesaiNo ratings yet
- Monoarthritis Ellis 2019Document7 pagesMonoarthritis Ellis 2019castillojessNo ratings yet
- Clear Cell Renal Cell Carcinoma: Associations Between CT Features and Patient SurvivalDocument8 pagesClear Cell Renal Cell Carcinoma: Associations Between CT Features and Patient SurvivalBastian VizcarraNo ratings yet
- 10.1136@bjsports 2020 1028ggdjnDocument2 pages10.1136@bjsports 2020 1028ggdjnLukas ŽarnauskasNo ratings yet
- A Transfer Learning Method For Brain Tumor Classification Using EfficientNet-B3 ModelDocument6 pagesA Transfer Learning Method For Brain Tumor Classification Using EfficientNet-B3 Model李明No ratings yet
- ACSM Conference PosterDocument1 pageACSM Conference PosterAssad JarrahianNo ratings yet
- Yu Et Al 2014 Mri Features of Gastrointestinal Stromal TumorsDocument12 pagesYu Et Al 2014 Mri Features of Gastrointestinal Stromal TumorsRESIDENTES HNGAINo ratings yet
- Personal Use Only: Pneumatosis Intestinalis in Ulcerative ColitisDocument4 pagesPersonal Use Only: Pneumatosis Intestinalis in Ulcerative ColitiszixdiddyNo ratings yet
- Lei 2019Document7 pagesLei 2019LaRNo ratings yet
- Ajr 10 5540Document9 pagesAjr 10 5540Pepe pepe pepeNo ratings yet
- Ajr 2Document10 pagesAjr 2Fika FathiaNo ratings yet
- 2019 - Comparison of Bite Force in Patients After Treatment of Mandibular Fractures With 3-Dimensional Locking Miniplate and Standard MiniplatesDocument4 pages2019 - Comparison of Bite Force in Patients After Treatment of Mandibular Fractures With 3-Dimensional Locking Miniplate and Standard MiniplatesLeandro Nascimento Rodrigues dos santosNo ratings yet
- Eurheartj Intracoronary ImagingDocument20 pagesEurheartj Intracoronary ImagingDan PruneaNo ratings yet
- MINOCADocument10 pagesMINOCAmariana virguezNo ratings yet
- Radiology of Chest Wall MassesDocument11 pagesRadiology of Chest Wall MassesDevina BumiNo ratings yet
- 237-Texto Del Artículo, Manuscrito o Aportación A La Revista-1136-1!10!20220317Document14 pages237-Texto Del Artículo, Manuscrito o Aportación A La Revista-1136-1!10!20220317Rodrigo TompsonNo ratings yet
- Van Leeuwen Et Al 2013 Variations in Venous and Segmental Anatomy of The Liver Two and Three Dimensional MR Imaging inDocument9 pagesVan Leeuwen Et Al 2013 Variations in Venous and Segmental Anatomy of The Liver Two and Three Dimensional MR Imaging inUsateo TeoNo ratings yet
- ESC HF Pages 1 97 Halaman 9 50Document42 pagesESC HF Pages 1 97 Halaman 9 50Athea 88No ratings yet
- ORBIT PublicationDocument3 pagesORBIT PublicationVinathi MutyalaNo ratings yet
- Task 2 Case Notes: Brendan CrossDocument4 pagesTask 2 Case Notes: Brendan CrossFatma ArslanNo ratings yet
- EbolaviruspptDocument22 pagesEbolaviruspptAmna ShahidNo ratings yet
- Stepwise Approach To Continuous Glucose Monitoring Interpretation For Internists and Family PhysiciansDocument10 pagesStepwise Approach To Continuous Glucose Monitoring Interpretation For Internists and Family PhysiciansRafael Baybay100% (1)
- Cataract - GlaucomaDocument2 pagesCataract - GlaucomaggukNo ratings yet
- Kawasaki Disease: An Update: EpidemiologyDocument10 pagesKawasaki Disease: An Update: EpidemiologyEmma González de BaideNo ratings yet
- Rheumatoid Arthritis OsteoarthritisDocument33 pagesRheumatoid Arthritis OsteoarthritisTri Hastuti HendrayaniNo ratings yet
- Pakistan Kidney and Liver Institute & Research Centre (PKLI)Document1 pagePakistan Kidney and Liver Institute & Research Centre (PKLI)Waqas SaleemNo ratings yet
- Knowledge Regarding Prevention of Helminthic Disease Among School ChildrenDocument5 pagesKnowledge Regarding Prevention of Helminthic Disease Among School ChildrenIJAR JOURNALNo ratings yet
- Calcium Gluconate PDFDocument2 pagesCalcium Gluconate PDFDayan CabrigaNo ratings yet
- NifedipineDocument2 pagesNifedipineapi-3797941100% (3)
- 8 Plasma Derivatives ProductsDocument12 pages8 Plasma Derivatives ProductssayednourNo ratings yet
- Deep Vein ThrombosisDocument11 pagesDeep Vein ThrombosisTushar GhuleNo ratings yet
- Abdominal Compartment SyndromeDocument29 pagesAbdominal Compartment Syndromesgod34100% (1)
- BTB Template Er-IntakeDocument3 pagesBTB Template Er-IntakeBoy MadNo ratings yet
- Interpretation of Urine CulturesDocument29 pagesInterpretation of Urine Culturestummalapalli venkateswara raoNo ratings yet
- Hepatitis B Prevention and ControlDocument19 pagesHepatitis B Prevention and Controlcolltfrank100% (1)
- SYNOZ® - Kyeron 2Document1 pageSYNOZ® - Kyeron 2karamnader76No ratings yet
- Tetratology Hand OutsDocument1 pageTetratology Hand OutsAngielyn Montibon JesusNo ratings yet
- Medication: Expected Pharmacological Action Therapeutic UseDocument1 pageMedication: Expected Pharmacological Action Therapeutic UseAiyanna RankinsNo ratings yet
- Testicular TorsionDocument20 pagesTesticular TorsionnurisumirizqiNo ratings yet
- How To Institute The low-FODMAP DietDocument3 pagesHow To Institute The low-FODMAP DietanaNo ratings yet