Professional Documents
Culture Documents
Necrosis
Uploaded by
Sivaani ChidambaramOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Necrosis
Uploaded by
Sivaani ChidambaramCopyright:
Available Formats
Definition:
Necrosis is spectrum of morphological changes that follow cell death in living tissues resulting from
denaturation of intracellular proteins or degradative action of enzymes on irreversibly injured cell.
The hallmark of necrosis is loss of integrity of cell membrane.
Types of necrosis:
1. Coagualative necrosis:
a. Most common type.
b. Caused due to sudden cessation blood flow in organs like the heart,kidney and spleen.
c. Seen in myocardial infarction.
2. Liquefactive necrosis: Seen in brain
3. Caseous necrosis: most commonly seen when cell death is attributed to Mycobacterium
tuberculosis.
4. Fibrinoid necrosis: seen in immune reactions involving blood vessels.
5. Fat necrosis: seen in breast and pancreas.
6. Gangrenous necrosis:
a. It is of two types: Dry gangrene and wet gangrene.
b. Dry gangrene seen in lower limbs
c. Wet gangrene is seen when the overlying gangrenous tissue is devitalized, bacterial
infection is superimposed.
Morphology of caseous necrosis
Caseous necrosis is encountered most often in foci of tuberculous infection
The term “caseous” (cheeselike) is derived from the friable white appearance of the area of necrosis
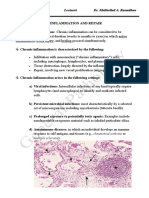
On microscopic examination, the necrotic area appears as a collection of fragmented or lysed cells and
amorphous granular debris enclosed within a distinctive inflammatory border; this appearance is
characteristic of a focus of inflammation known as a granuloma.
A granuloma is a focus of chronic inflammation consisting of a microscopic aggregation of macrophages
that are transformed into epithelium-like cells, surrounded by a collar of mononuclear leukocytes,
principally lymphocytes and occasionally plasma cells.
In the usual hematoxylin and eosin–stained tissue sections, the epithelioid cells have a pale pink granular
cytoplasm with indistinct cell boundaries, often appearing to merge into one another. The nucleus is less
dense than that of a lymphocyte, is oval or elongate, and may show folding of the nuclear membrane.
Frequently, epithelioid cells fuse to form giant cells in the periphery or sometimes in the center of
granulomas.
You might also like
- ++ GP - 02 - NecrosisDocument53 pages++ GP - 02 - Necrosissam adam ChalhoubNo ratings yet
- A Simple Guide to Mucocutaneous Lymph Node Syndrome (Kawasaki Disease), Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Mucocutaneous Lymph Node Syndrome (Kawasaki Disease), Diagnosis, Treatment and Related ConditionsNo ratings yet
- Cell Death: Apoptotic Bodies Which Are Phagocytised by Neighbouring Phagocytes. Apoptosis Is Not AssociatedDocument5 pagesCell Death: Apoptotic Bodies Which Are Phagocytised by Neighbouring Phagocytes. Apoptosis Is Not AssociatedIsak ShatikaNo ratings yet
- Necrosis and Degeneration - Copy)Document41 pagesNecrosis and Degeneration - Copy)Saubie Aslamiah100% (2)
- UntitledDocument170 pagesUntitledMarie GdlNo ratings yet
- NecrosisDocument12 pagesNecrosisAneeza AhmadNo ratings yet
- Types of Cell Injury. Apoptosis NecrosisDocument28 pagesTypes of Cell Injury. Apoptosis NecrosisAsmaNo ratings yet
- Necrosis - Gen. PathologyDocument16 pagesNecrosis - Gen. PathologyMohamed FaizalNo ratings yet
- Necrosis and Its Types: DefinitionDocument7 pagesNecrosis and Its Types: DefinitionHussen AliNo ratings yet
- NecrosisDocument31 pagesNecrosisMuhammad izazNo ratings yet
- Session 06-Cell DeathDocument39 pagesSession 06-Cell Deathkasper mkNo ratings yet
- 3 NecrosisDocument28 pages3 NecrosisSuman MahmoodNo ratings yet
- Apoptosis, Necrosis and AutophagyDocument18 pagesApoptosis, Necrosis and AutophagyFazal haqNo ratings yet
- Necrosis Is The Death of Tissue in A LivingDocument80 pagesNecrosis Is The Death of Tissue in A Livingsame_jish100% (1)
- Necrosis & ApoptosisDocument6 pagesNecrosis & ApoptosisshabeebakpNo ratings yet
- Necrosis: Erbil Polytechnic University Erbil Health Technical College MLT Department Third Stage Group CDocument13 pagesNecrosis: Erbil Polytechnic University Erbil Health Technical College MLT Department Third Stage Group CRayan JabbarNo ratings yet
- SHS 301 Lect-4Document65 pagesSHS 301 Lect-4moral seekersNo ratings yet
- Dr. Ranjita Singh Department of PathologyDocument19 pagesDr. Ranjita Singh Department of PathologyMohan Prasad GuptaNo ratings yet
- Inflammation and Neoplasia NecrosisDocument6 pagesInflammation and Neoplasia NecrosisTapitNo ratings yet
- Exercise 10 EcrosisDocument10 pagesExercise 10 EcrosismikeeNo ratings yet
- Necrosisgangreneandapoptosis 150918022114 Lva1 App6891 PDFDocument51 pagesNecrosisgangreneandapoptosis 150918022114 Lva1 App6891 PDFArTurNo ratings yet
- 2 Cellular Response To Injury 2Document35 pages2 Cellular Response To Injury 2Alex XanderNo ratings yet
- Master Plan Patho!Document94 pagesMaster Plan Patho!chiarastanziola01No ratings yet
- Morphology of Irreversible Cell InjuryDocument17 pagesMorphology of Irreversible Cell Injurysnehagpt100% (1)
- SHS 301 Lect-4Document63 pagesSHS 301 Lect-4AAZEEN ALINo ratings yet
- Necrosis and Types of NecrosisDocument2 pagesNecrosis and Types of NecrosisHisham NesemNo ratings yet
- Necrosis NotesDocument3 pagesNecrosis Notesjerad19No ratings yet
- Pathology Slides in English (Little Bit Bulgarian Too:)Document89 pagesPathology Slides in English (Little Bit Bulgarian Too:)Fırat Güllü94% (16)
- PATHOLOGY Week 1Document9 pagesPATHOLOGY Week 1RANA MOHAMMED HAMOOD AL-HADEQNo ratings yet
- NecrosisDocument17 pagesNecrosisIrah Birung LorenzoNo ratings yet
- LKLKLDocument3 pagesLKLKLKaye SnppyNo ratings yet
- NecrosisDocument17 pagesNecrosisArooma KhalidNo ratings yet
- علم الامراض Lec 3Document5 pagesعلم الامراض Lec 3ttrteNo ratings yet
- Necrosis and ApoptosisDocument18 pagesNecrosis and ApoptosisMasum ShahriarNo ratings yet
- م 4Document10 pagesم 4Najwa AbdualgaderNo ratings yet
- 1 - Cell Injury and DeathDocument4 pages1 - Cell Injury and DeathALNAKINo ratings yet
- Cell Injury 2Document56 pagesCell Injury 2hangoverNo ratings yet
- Necrosis: Anmc General Pathology Lecture Series Cell, Cell Injury, Cell Death, and AdaptationsDocument73 pagesNecrosis: Anmc General Pathology Lecture Series Cell, Cell Injury, Cell Death, and AdaptationsHussain Ali Abbas KhanNo ratings yet
- Cell Injury, Adaptation, and DEATHDocument31 pagesCell Injury, Adaptation, and DEATHagungNo ratings yet
- III. Irreversible Cell Injury (Cell Death)Document42 pagesIII. Irreversible Cell Injury (Cell Death)Manal ElnemrNo ratings yet
- Pathology For Dentistry Lect 6Document5 pagesPathology For Dentistry Lect 6Mohamad AladdinNo ratings yet
- Lec5 Sem1 FMweek2 20150102Document6 pagesLec5 Sem1 FMweek2 20150102Uloko ChristopherNo ratings yet
- Irreversible Cell Injury and Cell DeathDocument38 pagesIrreversible Cell Injury and Cell DeathPradeep100% (2)
- Glomerular Diseases: Ass - Prof. Rihab Al-Mudhaffer Kufa University Department of Pathology and Forensic MedicineDocument37 pagesGlomerular Diseases: Ass - Prof. Rihab Al-Mudhaffer Kufa University Department of Pathology and Forensic MedicineAli HusseinNo ratings yet
- Circulating KineticsDocument82 pagesCirculating KineticsJilycamae COSMODNo ratings yet
- Cell IjuryDocument133 pagesCell IjuryMd. Zayed ZamanNo ratings yet
- Effusion Cytology-2022Document82 pagesEffusion Cytology-2022Boy blueNo ratings yet
- Renal Biopsy Pathology 2011Document10 pagesRenal Biopsy Pathology 2011AnamNo ratings yet
- Cell InjuryDocument86 pagesCell InjuryMaharani SaraswatiNo ratings yet
- Resumen Necrosis 1Document2 pagesResumen Necrosis 1FRANCO GARCIA ZENAIDONo ratings yet
- Necrosis (From TheDocument6 pagesNecrosis (From TheSnapeSnapeNo ratings yet
- Review Paper: I. Explain Briefly The Following TermDocument6 pagesReview Paper: I. Explain Briefly The Following Termapi-19916399No ratings yet
- Cell Injury - UpdatedDocument33 pagesCell Injury - UpdatedMohammadLatifNo ratings yet
- 03 - Pathology CELL INJURY L2 Medical Sept. 2019Document34 pages03 - Pathology CELL INJURY L2 Medical Sept. 2019Saman ArshadNo ratings yet
- Pathos (Suffering) Logos: Pathology Is The Study of The Causes and Effects ofDocument70 pagesPathos (Suffering) Logos: Pathology Is The Study of The Causes and Effects ofahmed mokhtar100% (1)
- Patho 4Document9 pagesPatho 4ambiliNo ratings yet
- Patho 2Document72 pagesPatho 2Mohammed Amen FaresNo ratings yet
- Robbin'S and Cotran'S: Pathologic Basis of DiseaseDocument6 pagesRobbin'S and Cotran'S: Pathologic Basis of Diseasenge257No ratings yet
- Cell InjuryDocument53 pagesCell InjuryRick Ghosh (Shreyam)No ratings yet
- Head Injury - FMDocument3 pagesHead Injury - FMSivaani ChidambaramNo ratings yet
- Microbiology POL ChartsDocument14 pagesMicrobiology POL ChartsSivaani ChidambaramNo ratings yet
- Microbiology Must To Read For UniversityDocument8 pagesMicrobiology Must To Read For UniversitySivaani ChidambaramNo ratings yet
- AI and Human - Efficient Together.!Document3 pagesAI and Human - Efficient Together.!Sivaani ChidambaramNo ratings yet
- University Practical List of Examination SpecimensDocument4 pagesUniversity Practical List of Examination SpecimensSivaani ChidambaramNo ratings yet
- Slides PointsDocument13 pagesSlides PointsSivaani ChidambaramNo ratings yet
- URINE EXMN With AnswersDocument12 pagesURINE EXMN With AnswersSivaani ChidambaramNo ratings yet
- Peripheral Smear Preparation and StainingDocument7 pagesPeripheral Smear Preparation and StainingSivaani ChidambaramNo ratings yet
- Micro Paper IIDocument1 pageMicro Paper IISivaani ChidambaramNo ratings yet
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)
- 10% Human: How Your Body's Microbes Hold the Key to Health and HappinessFrom Everand10% Human: How Your Body's Microbes Hold the Key to Health and HappinessRating: 4 out of 5 stars4/5 (33)
- The Ancestor's Tale: A Pilgrimage to the Dawn of EvolutionFrom EverandThe Ancestor's Tale: A Pilgrimage to the Dawn of EvolutionRating: 4 out of 5 stars4/5 (811)
- A Brief History of Intelligence: Evolution, AI, and the Five Breakthroughs That Made Our BrainsFrom EverandA Brief History of Intelligence: Evolution, AI, and the Five Breakthroughs That Made Our BrainsRating: 4 out of 5 stars4/5 (5)
- Tales from Both Sides of the Brain: A Life in NeuroscienceFrom EverandTales from Both Sides of the Brain: A Life in NeuroscienceRating: 3 out of 5 stars3/5 (18)
- Gut: the new and revised Sunday Times bestsellerFrom EverandGut: the new and revised Sunday Times bestsellerRating: 4 out of 5 stars4/5 (392)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- Gut: The Inside Story of Our Body's Most Underrated Organ (Revised Edition)From EverandGut: The Inside Story of Our Body's Most Underrated Organ (Revised Edition)Rating: 4 out of 5 stars4/5 (378)
- The Other Side of Normal: How Biology Is Providing the Clues to Unlock the Secrets of Normal and Abnormal BehaviorFrom EverandThe Other Side of Normal: How Biology Is Providing the Clues to Unlock the Secrets of Normal and Abnormal BehaviorNo ratings yet
- The Molecule of More: How a Single Chemical in Your Brain Drives Love, Sex, and Creativity--and Will Determine the Fate of the Human RaceFrom EverandThe Molecule of More: How a Single Chemical in Your Brain Drives Love, Sex, and Creativity--and Will Determine the Fate of the Human RaceRating: 4.5 out of 5 stars4.5/5 (516)
- Undeniable: How Biology Confirms Our Intuition That Life Is DesignedFrom EverandUndeniable: How Biology Confirms Our Intuition That Life Is DesignedRating: 4 out of 5 stars4/5 (11)
- A Series of Fortunate Events: Chance and the Making of the Planet, Life, and YouFrom EverandA Series of Fortunate Events: Chance and the Making of the Planet, Life, and YouRating: 4.5 out of 5 stars4.5/5 (62)
- All That Remains: A Renowned Forensic Scientist on Death, Mortality, and Solving CrimesFrom EverandAll That Remains: A Renowned Forensic Scientist on Death, Mortality, and Solving CrimesRating: 4.5 out of 5 stars4.5/5 (397)
- Good Without God: What a Billion Nonreligious People Do BelieveFrom EverandGood Without God: What a Billion Nonreligious People Do BelieveRating: 4 out of 5 stars4/5 (66)
- Buddha's Brain: The Practical Neuroscience of Happiness, Love & WisdomFrom EverandBuddha's Brain: The Practical Neuroscience of Happiness, Love & WisdomRating: 4 out of 5 stars4/5 (215)
- This Is Your Brain On Parasites: How Tiny Creatures Manipulate Our Behavior and Shape SocietyFrom EverandThis Is Your Brain On Parasites: How Tiny Creatures Manipulate Our Behavior and Shape SocietyRating: 3.5 out of 5 stars3.5/5 (31)
- Fast Asleep: Improve Brain Function, Lose Weight, Boost Your Mood, Reduce Stress, and Become a Better SleeperFrom EverandFast Asleep: Improve Brain Function, Lose Weight, Boost Your Mood, Reduce Stress, and Become a Better SleeperRating: 4.5 out of 5 stars4.5/5 (15)
- Who's in Charge?: Free Will and the Science of the BrainFrom EverandWho's in Charge?: Free Will and the Science of the BrainRating: 4 out of 5 stars4/5 (65)
- The Consciousness Instinct: Unraveling the Mystery of How the Brain Makes the MindFrom EverandThe Consciousness Instinct: Unraveling the Mystery of How the Brain Makes the MindRating: 4.5 out of 5 stars4.5/5 (93)
- The Invention of Tomorrow: A Natural History of ForesightFrom EverandThe Invention of Tomorrow: A Natural History of ForesightRating: 4.5 out of 5 stars4.5/5 (5)
- Crypt: Life, Death and Disease in the Middle Ages and BeyondFrom EverandCrypt: Life, Death and Disease in the Middle Ages and BeyondRating: 4 out of 5 stars4/5 (4)
- The Lives of Bees: The Untold Story of the Honey Bee in the WildFrom EverandThe Lives of Bees: The Untold Story of the Honey Bee in the WildRating: 4.5 out of 5 stars4.5/5 (44)
- Inside of a Dog: What Dogs See, Smell, and KnowFrom EverandInside of a Dog: What Dogs See, Smell, and KnowRating: 4 out of 5 stars4/5 (390)
- Wayfinding: The Science and Mystery of How Humans Navigate the WorldFrom EverandWayfinding: The Science and Mystery of How Humans Navigate the WorldRating: 4.5 out of 5 stars4.5/5 (18)