Professional Documents
Culture Documents
Stroke: Causes, Incidence, and Risk Factors
Uploaded by
idno1008Original Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Stroke: Causes, Incidence, and Risk Factors
Uploaded by
idno1008Copyright:
Available Formats
Stroke
A stroke is an interruption of the blood supply to any part of the brain. A stroke is sometimes called a "brain attack."
Causes, incidence, and risk factors
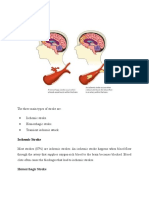
A stroke happens when blood flow to a part of the brain is interrupted because a blood vessel in the brain is blocked or bursts open. If blood flow is stopped for longer than a few seconds, the brain cannot get blood and oxygen. Brain cells can die, causing permanent damage. There are two major types of stroke: ischemic stroke and hemorrhagic stroke. ISCHEMIC STROKE Ischemic stroke occurs when a blood vessel that supplies blood to the brain is blocked by a blood clot. This may happen in two ways: A clot may form in an artery that is already very narrow. This is called a thrombus. If it completely blocks the artery, it is called a thrombotic stroke. A clot may break off from another place in the blood vessels of the brain, or some other part of the body, and travel up to the brain to block a smaller artery. This is called an embolism. It causes an embolic stroke. Ischemic strokes may result from clogged arteries, a condition called atherosclerosis. This may affect the arteries within the brain or the arteries in the neck that carry blood to the brain. Fat, cholesterol, and other substances collect on the wall of the arteries, forming a sticky substance called plaque. Over time, the plaque builds up. This often makes it hard for blood to flow properly, which can cause the blood to clot. Ischemic strokes may also be caused by blood clots that form in the heart or other parts of the body. These clots travel through the blood and can get stuck in the small arteries of the brain. This is known as a cerebral embolism. Certain drugs and medical conditions can make your blood more likely to clot and raise your risk for ischemic stroke. A common cause of ischemic stroke in people under age 40 is carotid dissection, or a tear in the lining of the carotid artery. The tear lets blood flow between the layers of the carotid artery. This causes narrowing of the carotid artery that is not due to plaque buildup. Some ischemic strokes start out without any bleeding, and then bleeding into the damaged area occurs. HEMORRHAGIC STROKE Hemorrhagic stroke occurs when a blood vessel in part of the brain becomes weak and bursts open, causing blood to leak into the brain. Some people have defects in the blood vessels of the brain that make this more likely. The flow of blood that occurs after the blood vessel ruptures damages brain cells.
STROKE RISKS High blood pressure is the number one risk factor for strokes. The following also increase your risk for stroke: Atrial fibrillation Diabetes Family history of stroke Heart disease High cholesterol Increasing age
Certain medications make blood clots more likely, and therefore increase your chances for a stroke. Birth control pills can increase the chances of having blood clots, especially in woman who smoke and who are older than 35. Men have more strokes than women. However, women have a higher risk of stroke during pregnancy and in the weeks immediately after pregnancy. The following can increase the risk of bleeding into the brain, which makes you more likely to have a stroke: Alcohol use Bleeding disorders Cocaine use Head injury
For more information see: Stroke risk factors and prevention
Symptoms
The symptoms of stroke depend on what part of the brain is damaged. In some cases, a person may not even be aware that he or she has had a stroke. Symptoms usually develop suddenly and without warning, or they may occur on and off for the first day or two. Symptoms are usually most severe when the stroke first happens, but they may slowly get worse. A headache may occur, especially if the stroke is caused by bleeding in the brain. The headache: Starts suddenly and may be severe Occurs when lying flat Wakes you up from sleep Gets worse when you change positions or when you bend, strain, or cough
Other symptoms depend on the severity of the stroke and what part of the brain is affected. Symptoms may include: Change in alertness (including sleepiness, unconsciousness, and coma) Changes in hearing Changes in taste
Clumsiness Confusion or loss of memory Difficulty swallowing Difficulty writing or reading Dizziness or abnormal sensation of movement (vertigo) Lack of control over the bladder or bowels Loss of balance Loss of coordination Muscle weakness in the face, arm, or leg (usually just on one side) Numbness or tingling on one side of the body Personality, mood, or emotional changes Problems with eyesight, including decreased vision, double vision, or total loss of vision Sensation changes that affect touch and the ability to feel pain, pressure, different temperatures, or other stimuli Trouble speaking or understanding others who are speaking Trouble walking
Signs and tests
A complete physical and neurological exam should be performed. Your doctor will: Check for problems with vision, movement, sensation, reflexes, understanding, and speaking. Your doctor and nurses will repeat this exam over time to see if your stroke is getting worse or is improving. Listen for an abnormal sound, called a "bruit," when using a stethoscope to listen to the carotid arteries in the neck. A bruit is caused by turbulent blood flow. Check and assess your blood pressure, which may be high. Tests can help your doctor determine the type, location, and cause of the stroke and rule out other disorders that may be responsible for the symptoms. A CT scan of the brain is often done soon after symptoms of a stroke begin. An MRI scan of the brain may be done instead or afterwards. Magnetic resonance angiography (MRA) or CT angiography may be done to check for abnormal blood vessels in the brain that may have caused the stroke. Echocardiogram may be done if the stroke could have been caused by a blood clot from the heart. Carotid duplex (a type of ultrasound exam) can show if narrowing of the neck arteries (carotid stenosis) led to the stroke. An angiogram of the head can reveal which blood vessel is blocked or bleeding, and help your doctor decide if the artery can be reopened using a thin tube. Laboratory tests will include a complete blood count (CBC), bleeding time, and blood clotting tests (prothrombin time or partial thromboplastin time). They will also check your blood cholesterol and sugar. Electrocardiogram (ECG) and heart rhythm monitoring can help determine if an irregular heartbeat (such as atrial fibrillation) caused the stroke. A spinal tap (cerebrospinal fluid exam) may also be done.
Treatment
A stroke is a medical emergency. Immediate treatment can save lives and reduce disability. Call 911 or your local emergency number or seek immediate medical care at the first signs of a stroke. It is very important for people who are having stroke symptoms to get to a hospital as quickly as possible. If the stroke is caused by a blood clot, a clot-busting drug may be given to dissolve the clot. Most of the time, patients must reach a hospital within 3 hours after symptoms begin. Some people may be able to receive these drugs for up to 4 - 5 hours after symptoms begin. Treatment depends on the severity and cause of the stroke. A hospital stay is required for most strokes. TREATMENT IN THE HOSPITAL Clot-busting drugs (thrombolytic therapy) may be used if the stroke is caused by a blood clot. Such medicine breaks up blood clots and helps restore blood flow to the damaged area. However, not everyone can receive this type of medicine. For these drugs to work, a person must be seen and treatment must begin within 3 hours of when the symptoms first started. A CT scan must be done to see whether the stroke is from a clot or from bleeding. If the stroke is caused by bleeding rather than clotting, clot-busting drugs (thrombolytics) can cause more bleeding. Other treatments depend on the cause of the stroke: Blood thinners such as heparin or warfarin (Coumadin) may be used to treat strokes due to blood clots. Aspirin or clopidogrel (Plavix) may also be used. Other medications may be needed to control other symptoms, including high blood pressure. Painkillers may be given to control severe headache. In some situations, a special stroke team and skilled radiologists may be able to use angiography to highlight the clogged blood vessel and open it up. For hemorrhagic stroke, surgery is often required to remove blood from around the brain and to repair damaged blood vessels. Surgery on the carotid artery may be needed. See also: Carotid artery disease Carotid artery surgery
Nutrients and fluids may be necessary, especially if the person has swallowing difficulties. These may be given through a vein (intravenously) or a feeding tube in the stomach (gastrostomy tube). Swallowing difficulties may be temporary or permanent. Physical therapy, occupational therapy, speech therapy, and swallowing therapy will all begin in the hospital. LONG-TERM TREATMENT
The goal of treatment after a stroke is to help the patient recover as much function as possible and prevent future strokes. The recovery time and need for long-term treatment differs from person to person. Problems moving, thinking, and talking often improve in the weeks to months after a stroke. A number of people who have had a stroke will still continue to improve in the months or years after the stroke. See: Stroke recovery for information about: Bladder and bowel problems Living at home rather than a nursing facility Muscle and nerve problems Speech problems Stroke rehabilitation Swallowing and eating problems Thinking and memory problems
Support Groups
Additional support and resources are available from the American Stroke Association -www.strokeassociation.org.
Expectations (prognosis)
The outlook depends on the type of stroke, how much brain tissue is damaged, what body functions have been affected, and how quickly treatment is received. Recovery may occur completely, or there may be some permanent loss of function. Over half of the people who have a stroke are able to function independently at home. If treatment with clot-busting drugs is successful, the symptoms of a stroke may completely go away. However, patients do not often arrive at the hospital soon enough to receive these drugs, or there are complicating medical conditions that prevent their use. People who have an ischemic stroke (stroke due to a blood clot) have a better chance of surviving than those who have a hemorrhagic stroke (stroke due bleeding in the brain). The risk for a second stroke is highest over the first few weeks or months after the first stroke and then begins to lessen.
Complications
Breathing food into the airway (aspiration) Decreased life span Difficulty communicating Fractures Malnutrition Muscle spasticity Permanent loss of brain functions Permanent loss of movement or sensation in one or more parts of the body
sores
Problems due to loss of mobility, including joint contractures and pressure Reduced ability to function or care for self Reduced social interactions Side effects of medications
Calling your health care provider
Stroke is a medical emergency that requires immediate treatment. Call your local emergency number (such as 911) if someone has symptoms of a stroke.
Prevention
To help prevent a stroke: Avoid fatty foods. Follow a healthy, low-fat diet. Do not drink more than 1 to 2 alcoholic drinks a day. Exercise regularly: 30 minutes a day if you are not overweight; 60 - 90 minutes a day if you are overweight. Get your blood pressure checked every 1 - 2 years, especially if high blood pressure runs in your family. Have your cholesterol checked. If you are at high risk for stroke, your LDL "bad" cholesterol should be lower than 100 mg/dL. Your doctor may recommend that you try to reduce your LDL cholesterol to 70 mg/dL. Follow your doctor's treatment recommendations if you have high blood pressure, diabetes, high cholesterol, and heart disease. Quit smoking. Aspirin therapy (81 mg a day or 100 mg every other day) is recommended for stroke prevention in all men who have stroke risk factors, and in women under age 65 who are at risk for stroke, as long as the benefits outweigh the risks. It should be considered for women over age 65 only if their blood pressure is controlled and the benefit is greater than the risk of gastrointestinal bleeding and brain hemorrhage. Ask your doctor if aspirin is right for you. Your doctor may also recommend aspirin therapy or another blood thinner if you have had a transient ischemic attack (TIA) or stroke in the past, or if you currently have: Congestive heart failure Irregular heartbeat (such as atrial fibrillation) Mechanical heart valve Other risk factors for stroke
A type of surgery called carotid endarterectomy may help prevent new strokes from occurring in persons with large blockages in their neck arteries. See also: Stroke risk factors and prevention
You might also like
- BBB EcgDocument33 pagesBBB EcgLokbre YoasNo ratings yet
- StrokeDocument25 pagesStrokeDedeNo ratings yet
- STROKE: Handbook with activities, exercises and mental challengesFrom EverandSTROKE: Handbook with activities, exercises and mental challengesNo ratings yet
- ArtherosclerosisDocument23 pagesArtherosclerosistanyagargNo ratings yet
- Brain Attack: StrokeDocument49 pagesBrain Attack: Strokeceudmd3d100% (1)
- Coronary Heart DiseaseDocument11 pagesCoronary Heart DiseaseZaryna TohNo ratings yet
- A Simple Guide to Stroke, (Cerebrovascular Infarction) Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Stroke, (Cerebrovascular Infarction) Diagnosis, Treatment and Related ConditionsNo ratings yet
- Patofisiologi Jantung: Fika EkayantiDocument59 pagesPatofisiologi Jantung: Fika EkayantiMaytaravikaHasan100% (1)
- Dental Management of The Medically Compromised Patient 8Th Ed by Little - Test BankDocument12 pagesDental Management of The Medically Compromised Patient 8Th Ed by Little - Test Bankkritisarena100% (1)
- StrokeDocument38 pagesStrokedyingangel_09100% (1)
- Cor Pulmonale Lesson PlanDocument49 pagesCor Pulmonale Lesson PlanRadha Sri50% (2)
- Stroke: Causes, Incidence, and Risk FactorsDocument9 pagesStroke: Causes, Incidence, and Risk Factorsthona_shirleneNo ratings yet
- 9-Strokes-29-06-2022 (29-Jun-2022) Material - I - 29-06-2022 - StrokeDocument14 pages9-Strokes-29-06-2022 (29-Jun-2022) Material - I - 29-06-2022 - Strokefiseha tadesseNo ratings yet
- What Is A Stroke?: Ischemic Stroke (Most Common Type) - This Type of Stroke Happens When Blood Is Blocked FromDocument13 pagesWhat Is A Stroke?: Ischemic Stroke (Most Common Type) - This Type of Stroke Happens When Blood Is Blocked FromDhulara IdNo ratings yet
- Stroke Causes: SkullDocument10 pagesStroke Causes: SkullMohd Farid Bin RosliNo ratings yet
- Stroke (Cerebrovascular Accident)Document3 pagesStroke (Cerebrovascular Accident)AlqrawyNo ratings yet
- Clinical Pharmacy-III: Understanding Stroke Symptoms, Types, Treatments & PreventionDocument21 pagesClinical Pharmacy-III: Understanding Stroke Symptoms, Types, Treatments & PreventionUmair MazharNo ratings yet
- Stroke: Prodi S1 Keperawatan Fakultas Kesehatan Universitas Wiraraja Sumenep 2016Document16 pagesStroke: Prodi S1 Keperawatan Fakultas Kesehatan Universitas Wiraraja Sumenep 2016Agus ZyapoetraaNo ratings yet
- Types of StrokeDocument12 pagesTypes of Strokefakher adnanNo ratings yet
- Cerebrovascular DiseaseDocument29 pagesCerebrovascular DiseaseKamsha UyNo ratings yet
- Understanding Strokes: Causes, Symptoms, and TreatmentDocument6 pagesUnderstanding Strokes: Causes, Symptoms, and TreatmentshaitabliganNo ratings yet
- CVA: Causes, Symptoms, Risk Factors & TreatmentDocument21 pagesCVA: Causes, Symptoms, Risk Factors & TreatmentAya EyadNo ratings yet
- StrokeDocument11 pagesStrokemakioedesemiNo ratings yet
- CARDIOVASCULAR DISEASE AND DIABETES PRESENTATIONDocument38 pagesCARDIOVASCULAR DISEASE AND DIABETES PRESENTATIONYu QingNo ratings yet
- Explaining StrokeDocument20 pagesExplaining StrokeChrisTine M. MoralesNo ratings yet
- What Is A StrokeDocument5 pagesWhat Is A StrokeLintsuNo ratings yet
- A Stroke RecoveryDocument2 pagesA Stroke Recoverymanjukumard2007No ratings yet
- By. ScribdDocument3 pagesBy. Scribdchreazy__021906No ratings yet
- ThrombosisDocument29 pagesThrombosistaanviruliislamNo ratings yet
- What is stroke? Everything you need to knowDocument6 pagesWhat is stroke? Everything you need to knowY. Beatrice AbigailNo ratings yet
- Types, Symptoms, Diagnosis and Treatment of StrokesDocument6 pagesTypes, Symptoms, Diagnosis and Treatment of StrokesAlfrien Ivanovich LarchsonNo ratings yet
- Types and Symptoms of StrokesDocument4 pagesTypes and Symptoms of StrokesRobby BanjarNo ratings yet
- Stroke 1Document7 pagesStroke 1mildred alidonNo ratings yet
- Blood Clot in The BrainDocument3 pagesBlood Clot in The BrainHarsh KananiNo ratings yet
- CVABDocument4 pagesCVABRobby BanjarNo ratings yet
- Brain Attack Day OneDocument48 pagesBrain Attack Day Onewisnu baskoroNo ratings yet
- Stroke: Trouble With Speaking and UnderstandingDocument23 pagesStroke: Trouble With Speaking and UnderstandingrosalindaNo ratings yet
- 5 CS and 5 RSDocument54 pages5 CS and 5 RSKristine CatariningNo ratings yet
- FAST signs and symptoms of strokeDocument16 pagesFAST signs and symptoms of strokeSandra Flores GaciasNo ratings yet
- Hem Stroke DefDocument5 pagesHem Stroke DefFate Ann Candle DagutaoNo ratings yet
- The Pathophysiology of Ischemic Strokes Is Widely Known. Ischemic Strokes Are TheDocument7 pagesThe Pathophysiology of Ischemic Strokes Is Widely Known. Ischemic Strokes Are Theprnczb13No ratings yet
- Stroke, Meningitis, and Trauma Management ContactDocument61 pagesStroke, Meningitis, and Trauma Management ContactUmar MukhtarNo ratings yet
- What Is A Coronary Angiogram?: HeartDocument2 pagesWhat Is A Coronary Angiogram?: HeartSagargn SagarNo ratings yet
- Cardivascular Deseases and Diabetes MellitusDocument38 pagesCardivascular Deseases and Diabetes MellitusSyafiqah SabriNo ratings yet
- REPORTDocument34 pagesREPORTClaire GidoNo ratings yet
- Clinical DiscussionDocument18 pagesClinical DiscussionKia MojicaNo ratings yet
- Cerebrovascular DiseaseDocument2 pagesCerebrovascular Diseaseapi-3717941No ratings yet
- Ucm 309725Document2 pagesUcm 309725haryatikennitaNo ratings yet
- Physiological Monitoring and Arterial DiseasesDocument100 pagesPhysiological Monitoring and Arterial DiseasesZllison Mae Teodoro MangabatNo ratings yet
- Ischemic StrokeDocument49 pagesIschemic StrokeMirna Ayu Permata SariNo ratings yet
- Stroke (Cerebrovascular Accident) : AtheromaDocument5 pagesStroke (Cerebrovascular Accident) : AtheromaIan MatatulaNo ratings yet
- DR NzooloDocument21 pagesDR NzooloJohn chrisant Mwansa the future presdoNo ratings yet
- Myocardial Infarction: Alternative NamesDocument5 pagesMyocardial Infarction: Alternative NamesKhalid Mahmud ArifinNo ratings yet
- Ischaemic Stroke GuideDocument12 pagesIschaemic Stroke Guidefatii.seedNo ratings yet
- Razonable Complete2.0 I.T Era - PPTX FinalDocument14 pagesRazonable Complete2.0 I.T Era - PPTX FinalJohn PiocoNo ratings yet
- Cerebrovascular Disease: Kelompok 6Document21 pagesCerebrovascular Disease: Kelompok 6Glen Jacobs SumadihardjaNo ratings yet
- Causes, Symptoms and Diagnosis of StrokeDocument7 pagesCauses, Symptoms and Diagnosis of StrokeRose SalviejoNo ratings yet
- 130416what Is A StrokeDocument17 pages130416what Is A StrokeAnand SarvaiyaNo ratings yet
- #9 Cerebrovascular AccidentDocument26 pages#9 Cerebrovascular AccidentRiyubi BianNo ratings yet
- Causes, Symptoms & Types of Cerebral InfarctionDocument2 pagesCauses, Symptoms & Types of Cerebral InfarctionMarie Aurora Gielbert MarianoNo ratings yet
- Cerebrovascular AccidentDocument1 pageCerebrovascular Accidentgeohanna_mariefNo ratings yet
- Cerebrovascular AccidentDocument2 pagesCerebrovascular AccidentAdrian PunongbayanNo ratings yet
- Stroke & Its TypesDocument30 pagesStroke & Its TypesSaher MatloobNo ratings yet
- To Whom It May ConcernDocument1 pageTo Whom It May Concernidno1008No ratings yet
- Singapore Business Visa Application Bangladesh BangladeshDocument6 pagesSingapore Business Visa Application Bangladesh Bangladeshidno1008No ratings yet
- New Drugs For Epilepsy Mangement 1Document48 pagesNew Drugs For Epilepsy Mangement 1idno1008No ratings yet
- Medication Should Not Be Used in MGDocument1 pageMedication Should Not Be Used in MGidno1008No ratings yet
- Patient Information On LOW BACK PAINDocument8 pagesPatient Information On LOW BACK PAINidno1008No ratings yet
- Farzana ApuDocument1 pageFarzana Apuidno1008No ratings yet
- Pathogenesis, Diagnosis and Treatment of Rasmussen EncephalitisDocument20 pagesPathogenesis, Diagnosis and Treatment of Rasmussen Encephalitisidno1008No ratings yet
- Rokeya Begum MEds.Document2 pagesRokeya Begum MEds.idno1008No ratings yet
- Rescued Document 2Document1 pageRescued Document 2idno1008No ratings yet
- One Stop Academic ActivitiesDocument1 pageOne Stop Academic Activitiesidno1008No ratings yet
- Musa IbrahimDocument3 pagesMusa Ibrahimidno1008No ratings yet
- Neurology AlimDocument38 pagesNeurology Alimidno1008No ratings yet
- Epilepsy Newspaper ArticleDocument10 pagesEpilepsy Newspaper Articleidno1008No ratings yet
- Letter of IntroductionDocument3 pagesLetter of Introductionidno1008No ratings yet
- Dr. ShahriarDocument1 pageDr. Shahriaridno1008No ratings yet
- EEG1Document13 pagesEEG1idno1008No ratings yet
- Department of NeuromedicineDocument4 pagesDepartment of Neuromedicineidno1008No ratings yet
- EEG Sedation For ChildrenDocument1 pageEEG Sedation For Childrenidno1008No ratings yet
- Daily StarDocument3 pagesDaily Staridno1008No ratings yet
- CIDPDocument21 pagesCIDPidno1008No ratings yet
- Aseptic Meningiti1Document18 pagesAseptic Meningiti1idno1008No ratings yet
- Bangladesh Gets The Glimpse of Defeat Depending On AshrafulDocument1 pageBangladesh Gets The Glimpse of Defeat Depending On Ashrafulidno1008No ratings yet
- Activities of Neuromedicine DepartmentDocument2 pagesActivities of Neuromedicine Departmentidno1008No ratings yet
- Autism Presentation (Final)Document48 pagesAutism Presentation (Final)idno1008No ratings yet
- Approach To The Patient With Epilepsy in The Outpatient DepartmentDocument13 pagesApproach To The Patient With Epilepsy in The Outpatient Departmentidno1008No ratings yet
- What To Do, When Aed Not WorkingDocument6 pagesWhat To Do, When Aed Not Workingidno1008No ratings yet
- Aseptic MeningitisDocument24 pagesAseptic Meningitisidno1008100% (1)
- Admin Protocol AhdDocument1 pageAdmin Protocol Ahdidno1008No ratings yet
- Academic Activities of Neurology DeptDocument1 pageAcademic Activities of Neurology Deptidno1008No ratings yet
- What To Do, When Gbs PT Fails To Respond To TreatmentDocument4 pagesWhat To Do, When Gbs PT Fails To Respond To Treatmentidno1008No ratings yet
- Kami Kagina, Gulpiyada Lang Siya Nadulaan Kusog Kag Gapukol Iya Hambalanon, Kag Nagakiwi Iya Nga Itsura." As VerbalizedDocument4 pagesKami Kagina, Gulpiyada Lang Siya Nadulaan Kusog Kag Gapukol Iya Hambalanon, Kag Nagakiwi Iya Nga Itsura." As VerbalizedKoleen Lhyte T. UYNo ratings yet
- ACLS Pharmacology GuideDocument5 pagesACLS Pharmacology GuideKim Still ChunnNo ratings yet
- Burger Allen Exercises PDFDocument122 pagesBurger Allen Exercises PDFlucky 116No ratings yet
- Diagnosa PRBDocument12 pagesDiagnosa PRBSAEHANNo ratings yet
- Intrinsic Conduction System of Heart: Setting The Basic RhythmDocument3 pagesIntrinsic Conduction System of Heart: Setting The Basic RhythmDeniebev'z OrillosNo ratings yet
- b4 Organisation in Animals Exam QsDocument30 pagesb4 Organisation in Animals Exam QsDarius “FlawlessStreak” OpreaNo ratings yet
- Analysis of Electrocardiograph Ecg Signal For The Detection of Abnormalities Using MatlabDocument4 pagesAnalysis of Electrocardiograph Ecg Signal For The Detection of Abnormalities Using MatlabHarshit JainNo ratings yet
- Atrial Fibrillation - Geeky MedicsDocument10 pagesAtrial Fibrillation - Geeky MedicsJahangir AlamNo ratings yet
- CatheterizationDocument2 pagesCatheterizationElishah CaprichoNo ratings yet
- ECMO (Extracorporeal Membrane Oxygenation)Document22 pagesECMO (Extracorporeal Membrane Oxygenation)dhivya singhNo ratings yet
- The Egyptian Heart Journal: Ahmed Elshazly, Hazem Khorshid, Hany Hanna, Ammar AliDocument3 pagesThe Egyptian Heart Journal: Ahmed Elshazly, Hazem Khorshid, Hany Hanna, Ammar AliImran TarmiziNo ratings yet
- IsdnDocument5 pagesIsdnWidya JelitaNo ratings yet
- 2008.clin Chem - RantnerDocument7 pages2008.clin Chem - RantnertwkangNo ratings yet
- Case Report Buerger DiseaseDocument36 pagesCase Report Buerger DiseaseKhaeruz Zahra67% (3)
- Shock in Children TutorialDocument37 pagesShock in Children TutorialSsenyonga DominicNo ratings yet
- Lesson 1: Overview and Principles of Resuscitation: Neonatal Resuscitation Program Slide Presentation KitDocument32 pagesLesson 1: Overview and Principles of Resuscitation: Neonatal Resuscitation Program Slide Presentation KitChauthiran AgamudaiyarNo ratings yet
- Anandhi ResumeDocument7 pagesAnandhi ResumeAnonymous rMa4DVY5J2No ratings yet
- High Blood PressureDocument9 pagesHigh Blood PressureshashidharanNo ratings yet
- DR Sandeep - EISENMENGER SYNDROMEDocument81 pagesDR Sandeep - EISENMENGER SYNDROMEAlexandrescuNo ratings yet
- EcgDocument29 pagesEcgSouvikDattaNo ratings yet
- Presented By: Bhawna Joshi Msc. Nursing 1 YearDocument52 pagesPresented By: Bhawna Joshi Msc. Nursing 1 YearBhawna JoshiNo ratings yet
- The Homocysteine and Stroke SeverityDocument28 pagesThe Homocysteine and Stroke Severitynesya_fanniaNo ratings yet
- Articulo COVID 19Document9 pagesArticulo COVID 19Omaira TovarNo ratings yet
- Hemorrhagic StrokeDocument2 pagesHemorrhagic StrokeMuhammad Anwar AnsoriNo ratings yet
- Cencus Thrombo Baru 2020Document14 pagesCencus Thrombo Baru 2020Wan ooNo ratings yet
- Sympathomimetics in VeterinaryDocument9 pagesSympathomimetics in Veterinaryjose pNo ratings yet