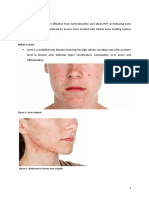
Allergic Disease in
Dermatology
Nyoman Suryawati
Bagian/ SMF IKKK FK UNUD
�Allergic disease in dermatology
Atopic Dermatitis
Contact dermatitis
Irritant Contact
Dermatitis
Allergic Contact
Dermatitis
�Atopic Dermatitis (AD)
The word "dermatitis" means inflammation of the skin.
Atopic dermatitis (AD) or atopic eczema is a chronically
relapsing, pruritic, exanthematous dermatosis of
uncertain etiology that is characterized primarily by an
allergic diathesis as well as erythema, oozing, crusting,
excoriations, lichenification, and dehydration of
involved skin surfaces.
"Atopic" refers to diseases that are hereditary, tend to
run in families, and often occur together.
These diseases include asthma, hay fever, and atopic
dermatitis. In atopic dermatitis, the skin becomes
extremely itchy and inflamed, causing redness,
swelling, cracking, weeping, crusting, and scaling.
�Atopic Dermatitis (AD)
JAAD 2003
A chronic inflammatory pruritic skin
disease which occurs most frequently in
children but can occur in adults and follows
a relapsing course. It is often associated
with elevated serum IgE levels and a
personal or family history of Type I
allergies, allergic rhinitis and asthma.
�Atopic Dermatitis (AD)
Epidemiology
In the western : prevalence has been estimated at
approximately 10%, up to a 20%
Overall, males and females are affected with equal
incidence
Seasonal variation does play a role in the
prevalence, with
Exacerbations occurring primarily in the winter.
Genetic predisposition has not been identified,
there usually is a
family history of either atopic
eczema, asthma, or seasonal allergic rhinitis
�Atopic Dermatitis (AD)
Etiology
The etiology of AD has not been fully
elucidated, suggested that both genetic and
environmental factors
AD in children is approximately 60% one
affected parent
80% two affected parents.
It also has been reported that nearly 40% of
patients have at least one first degree relative
who has AD.
�Atopic Dermatitis (AD)
Prevalence
Doubled or tripled in industrialized countries
during the past three decades;
15 to 30% of children and 2 to 10% of adults are
affected.
Atopic dermatitis frequently starts in early infancy
(earlyonset atopic dermatitis). in adults (lateonset atopic
dermatitis).
A total of 45% of all cases of atopic dermatitis
begin within
during the
years of age.
the first 6 months of life, 60% begin
first year, and 85% begin before 5
Up to 70% of these children have a spontaneous
remission before adolescence
�Atopic Dermatitis (AD)
Environmental factors :
Contact irritants and allergens,
Climate,
Sweating,
Aeroallergens,
house dust mite (Dermatophagoides
pteronyssinus),
molds, pollen, and dander
Microbial organisms,
Certain foods: eggs, meat, milk, soy, nuts, fish,
shellfish, and wheat
Stress/psyche,
�Factors Influencing the Development of Atopy and Allergic Inflammation
Mediated by Th2 Cells (Atopic Allergic Disease). The induction of atopy is
dependent on interactions between genes and the environment. The
induction of atopic allergic disease may require further interactions
between defects in the target organ and various environmental triggers.
FceRIb denotes the gene for the b chain of the high-affinity receptor for
IgE.
���Atopic Dermatitis (AD)
Hyperactive Th2 subset Thelper cells (associated with
promotion of IgE production from B lymphocytes,
differentiation of CD-4 T lymphocytes, suppression of
Th1 cell activities,
stimulation of proliferation,
and differentiation of B lymphocytes)
Increased levels of serum IgE
Upregulation of IL-4
Downregulation of IFN-gamma
Increased eosinophils
Elevated levels of IgE activated mast cells
Disturbances in fatty acid metabolism/deficiencies of
omega-6 fatty acids in plasma, adipose tissues, and
formed blood elements
���Th1/Th2 Paradigm
Cell-mediated immunity
IL-2
Th1
IL-12
TNF
IFN
IL-10
Th0
Humoral immunity
IL-4
IL-12, IFN
IL-4
Th2
IL-5
IL-10
�Current Model of Acute/Chronic Atopic Dermatitis
�Atopic Dermatitis (AD)
The natural history of the illness may
be described under the different age
groups:
1. Infancy : 2 mo 2 yr
2. Childhood
3. Adolescence and adulthood
�Atopic Dermatitis (AD)
Infantile atopic dermatitis
Face, cheeks, chin, extensor
surfaces, scalp, neck, wrists
Erythematous patches
Diaper area is spared
Resolves by 18 months, or
goes on to Childhood Atopic
Dermatitis
�Atopic Dermatitis (AD)
Childhood Atopic Dermatitis
Lesions less exudative
Dry, scaling papular lesions, with
lichenification
Areas of perspiration
Antecubital and popliteal areas, neck,
Under tight clothing
Wrists, eyelids, face
Worse in the winter
Hypopigmented due to repeated trauma
�Atopic Dermatitis (AD)
Adolescence Atopic Dermatitis
Pruritic, localized, erythematous,
scaly, papular patches
Antecubital and popliteal fossae,
neck, forehead, periorbital skin,
hands
8-10% of adults with atopic
dermatitis develop cataracts
�Acute Stage
Pruritic, erythmatous, excoriated
papules with extensive serous
exudate superimposed on a
background of erythema
Chronic Stage
Repeated excorations and
trauma lead to chronic
lescharacterized by thickened
plaques with increased marking
ions (lichenification) and dry,
fibrotic papules
�Kriteria Diagnosis
Hanifin & Lobitz
Hanifin & Rajka
Svenson
William
Kriteria Hanifin & Rajka (modifikasi, 1990)
Kriteria Mayor ( 3 dari 4)
1.
2.
3.
4.
Pruritus
Morfologi & distribusi yang khas
Kronik- residif
Stigmata atopik dalam keluarga
�Kriteria Minor ( 3 atau lebih)
1.
3.
5.
7.
9.
11.
13.
15.
17.
19.
Xerosis
Hiperlinearitas palmar
Ig E meningkat
Kheilitis
Mudah terjadi infeksi
Pitiriasis alba
White dermographism
Uji kulit positif
Kepucatan wajah
Faktor emosi
2.
Fisura periaurikuler
4. Keratosia pilaris
6. Dermatitis tanga
8. Dermatitis Scalp
10. Keratosis pilaris
12. Dermatitis niple
14. Katarak/keratok
16. Garis Dennie-Mo
18. Awitan dini
20. Tanda Hertog
�Treatment Guidelines for Atopic
Dermatitis
Bath oil soaks, at least once daily
Creams or mild, unscented soaps for washing
Moisturizers applied after bath oil soak and
throughout the day
For mild flare, mild (class VI or VII) corticosteroid to
affected areas twice daily
For severe eczema, short term (no more than 2 wk)
of medium- to high-potency topical corticosteroids
(class III through V)
except on face or in skin folds
Oral antibiotics for widespread, infected, flaring
eczema
� Topical antimicrobials, including mupirocin,
bacitracin, 3%
precipitated sulfur in petrolatum, 3%
iodochlorohydroxyquin, and 1% hydrocortisone,
applied
twice daily for infected eczema of the
trunk and extremities
Intranasal mupirocin twice daily for 10 days to
eliminate Staphylococcus aureus carrier status
Topical antifungal preparations in addition to class
VII
corticosteroid for flaring eczema of the face
Baby shampoo or antifungal shampoo for flaring
eczema of the
scalp
Antihistamines for pruritis
Clip fingernails short; add cotton mittens at night to
reduce
excoriations
Eliminate precipitating environmental factors
��Contact dermatitis refers to dermatitis caused by skin contact with
an environmental agent.
Contact dermatitis (CD) is an altered state of skin reactivity induced by
exposure to an external agent.
According to the mechanism of elicitation, the following types of
contact reactions may be distinguished:
1. allergic contact dermatitis (ACD),
2. irritant contact dermatitis (ICD),
3. phototoxic and photoallergic contact dermatitis, and
4. immediate type contact reactions.
�Chemicals or physical agents damage the surface of the skin faster
than the skin is able to repair the damage.
well demarcated with a glazed surface but there may be redness,
itching, swelling, blistering and scaling of the damaged area.
Amount and strength of the irritant
Length and frequency of exposure (eg. short heavy exposure or
repeated/prolonged low exposure)
Skin susceptibility (eg. thick, thin, oily, dry, very fair, previously
damaged skin or pre-existing atopic tendency)
Environmental factors (eg. high or low temperature or
humidity)
� ICD may affect anyone, given sufficient exposure to irritants, but
those with atopic dermatitis are particularly susceptible.
80% of cases of occupational hand dermatitis are due to irritants
The inflammation process in irritant contact dermatitis is not
mediated through an immunologic mechanism. Irritant contact
dermatitis is more common (70-80 %) than allergic
contact
dermatitis (20-30 %).
�a. Acute irritant contact dermatitis
Strong irritants e.g. concentrated acids, alkalis or solvents
The skin structures are damaged directly by the irritant.
The cause of acute irritant contact dermatitis is often obvious.
b. Cumulative irritant contact dermatitis
This type caused by repeated skin contact with weak irritants.
The duration between first exposure to the irritant and the
appearance of derniatitis varies from weeks to years, depending on the
nature of the irritant, frequency of contact,
and host susceptibility.
Cumulative insult dermatitis is exemplified by the chronic
hand dermatitis caused by detergents among dishwashers and
housewives, and by cutting fluid dermatitis among
metalworkers.
��Treatment
The management of ICD can be divided into treating the active case and
prevention. Topical corticosteroids, soap substitutes, and emollients are
widely accepted as the treatment of established contact dermatitis.
Second line treatments such as topical PUVA, azathioprine, and
cyclosporin are probably widely used for steroid resistant chronic hand
dermatitis.
�Allergic contact dermatitisis (ACD) an immunologic inflammatory
reaction of the skin due to contact with an allergen.
Different substances have different sensitizing potential, and there is
individual susceptibility to sensitization by an allergen.
�Type IV (Delayed or Cell-Mediated)
Hypersensitivity
Inflammation due to contact with certain
antigens occurs after 12-24 hours
Result from the interactions of antigen,
antigen-presenting cells, and T cells
Delay in this response reflects the time it
takes
for macrophages and T cells to
migrate to
and proliferate at the site of
the antigen
�Mechanism of Type IV
Hypersensitivities
���Sensitization is the first phase of ACD and involves penetration of low
molecular weight contact allergens into the skin for the first time where
they interact with proteins. The consequence of this step is the activation of
the innate immune system which leads to skin inflammation. This is an
essential step in the sensitization process as it results in the activation of
dendritic cells (DC). The activated epidermal Langerhans cells and the
dermal DC upregulate co-stimulatory molecules required for T cell activation
and chemokine receptors required for DC emigration from the skin to the
�Treatment ACD
The only available etiologic treatment of ACD is
elimination of the contact allergen.
Systemic
Antihistamine
Corticosteroid
Topical
Acute phase (papulo-vesiculo, oozing) wet
bandage
solutio NaCl 0,9 %
Chronic phase topical steroid
�mmon causes of allergic contact dermatitis
Nickel
Chromate
Cosmetics and skin care products
Drug dermatitis
Plant dermatitis
�Clinical Features
Major subjective symptoms
History of sufficient exposure to a cutaneous irritant
Onset of symptoms within minutes to hours of exposure in simple
acute irritant contact dermatitis.
The onset of signs and symptoms may be delayed by weeks in
cummulative irritant contact dermatitis.
Pain, burning, stinging or discomfort exceeding pruritus early in the
clinical course