Professional Documents
Culture Documents
KDI Dr. Henry
Uploaded by
Adhytya Pratama Ahmadi0 ratings0% found this document useful (0 votes)
23 views12 pagesslide MCVU
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentslide MCVU
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
23 views12 pagesKDI Dr. Henry
Uploaded by
Adhytya Pratama Ahmadislide MCVU
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 12
Jamaluddin, MD, FIHA
Bimo Bintoro, MD, FIHA
Henry S. Sauala, MD
Adhytya Pratama, MD
INTRODUCTION
Case
A 45 years-old gentleman visiting ED with chief complaint
of chest pain 14 hours prior to admission. The pain
characteristic was consistent to MI.
The night before, he initially sought no medical attention
and rest at his home. Afterwards in the morning, the pain
was felt again with the scale of 8/10+ dyspnea, and his wife
took him to ED. Risk Factor: Active Smoker, Dyslipidemia.
PEx:
110/60 mmHg; 100 bpm; 22x/m; 36,9OC
Gallop S3 (+), Rales: --+/--+; JVD R+3
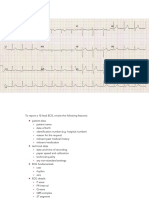
ED EKG
His ECG showed anterior extensive MI, MI algorithm
activated.
Working Dx: Acute anterior STEMI late onset Killip 2,
Acute HF
Rx: Aspirin 160mg (chewed), Clopidogrel 300mg,
ISDN 5 mg SL, simvaStatin 40mg orally
We continued with anticoagulation by giving
Fondaparinux.
We decided to perform fibrinolysis with 1.5 millions IU
of intravenous Streptokinase. In the process there were
bigeminy VPC, no other major complications of lytics
were observed. Afterwards the pain was decreasing to
4/10 and ECG evolved to Q waves.
Then in his next 24 hours, the pain was resolved to
0/10.
The third day of hospitalization, the echo was
evaluated.
1-H post lytics EKG
TTE
echo showed LVEF of 46% with RWMA according to
his infarcted areas.
and he was discharged home with dual antiplatelet,
statin, furosemide, ACE-I, and beta blocker.
Discussions
Though no mortality benefit was demonstrated in the
LATE and EMERAS trials when fibrinolytic was routinely
administered to patients between 12-24 hours, we believe
that it is still reasonable to consider fibrinolytic therapy
when PCI is not available for appropriate patients with
clinical and/or electrocardiographic evidence of ongoing
ischemia within 12 to 24 hours of symptoms onset and a
large area of myocardium at risk.
Persistent chest pain after the onset of symptoms correlates
with a higher incidence of collateral of anterograde flow in
the infarct zone and is therefore a marker for viable
myocardium that might be salvaged.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Critical Care Calculations Study GuideDocument6 pagesCritical Care Calculations Study GuideAja Blue100% (2)
- Basic Airway ManagementDocument98 pagesBasic Airway ManagementRani Salsabilah100% (1)
- Proceeding Book 27th AsmihaDocument14 pagesProceeding Book 27th AsmihaAdhytya Pratama AhmadiNo ratings yet
- Trivial INA ACCDocument2 pagesTrivial INA ACCAdhytya Pratama AhmadiNo ratings yet
- Permissive HypotensionDocument7 pagesPermissive HypotensionAdhytya Pratama AhmadiNo ratings yet
- Airborne Transmission of Severe Acute Respiratory Syndrome Coronavirus-2 To Healthcare Workers: A Narrative ReviewDocument10 pagesAirborne Transmission of Severe Acute Respiratory Syndrome Coronavirus-2 To Healthcare Workers: A Narrative ReviewAdhytya Pratama AhmadiNo ratings yet
- Format Isian TPP 2019Document4 pagesFormat Isian TPP 2019Adhytya Pratama AhmadiNo ratings yet
- Final KDI-Adhytya EditDocument15 pagesFinal KDI-Adhytya EditAdhytya Pratama AhmadiNo ratings yet
- Cek List Pre Angio ABDocument4 pagesCek List Pre Angio ABAdhytya Pratama AhmadiNo ratings yet
- EKGDocument53 pagesEKGAdhytya Pratama AhmadiNo ratings yet
- Slide PPT MMMDocument17 pagesSlide PPT MMMAdhytya Pratama AhmadiNo ratings yet
- VASDocument12 pagesVASAdhytya Pratama AhmadiNo ratings yet
- EKGDocument53 pagesEKGAdhytya Pratama AhmadiNo ratings yet
- 3 Daftar PustakaDocument2 pages3 Daftar PustakaAdhytya Pratama AhmadiNo ratings yet
- LM Thrombus Presenting with Stable AnginaDocument1 pageLM Thrombus Presenting with Stable AnginaAdhytya Pratama AhmadiNo ratings yet
- Uricase: Catalogue No. URIC-70-1701 and 70-1701-01 E.C. Number 1.7.3.3Document3 pagesUricase: Catalogue No. URIC-70-1701 and 70-1701-01 E.C. Number 1.7.3.3Adhytya Pratama AhmadiNo ratings yet
- Principles of Primary Health Care Ikm-Ikk 2016Document5,683 pagesPrinciples of Primary Health Care Ikm-Ikk 2016Adhytya Pratama AhmadiNo ratings yet
- Skill Lab Carcinoma MammaeDocument50 pagesSkill Lab Carcinoma MammaeAdhytya Pratama AhmadiNo ratings yet
- Jaundice in The Adult PatientDocument11 pagesJaundice in The Adult PatientAdhytya Pratama AhmadiNo ratings yet
- Morning Report BedahDocument21 pagesMorning Report BedahAdhytya Pratama AhmadiNo ratings yet
- House of IdeasDocument10 pagesHouse of IdeasAdhytya Pratama AhmadiNo ratings yet
- The IdleDocument33 pagesThe IdleAdhytya Pratama AhmadiNo ratings yet
- Jaundice in The Adult PatientDocument11 pagesJaundice in The Adult PatientAdhytya Pratama AhmadiNo ratings yet