Professional Documents
Culture Documents
Karin Ananditya Fazri 30101407217: Pembimbing: DR, Dian Indah Setyorini, SP - THT-KL
Uploaded by
Vivie Tirany Soediro0 ratings0% found this document useful (0 votes)
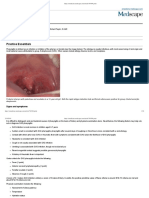
18 views31 pages1) Streptococcal acute pharyngitis is an inflammation of the throat that is commonly caused by Streptococcus pyogenes bacteria. While most cases are mild and self-limiting, S. pyogenes infection requires diagnosis and treatment to prevent potential post-infection complications.
2) Diagnosis involves throat culture or rapid antigen testing, and treatment of confirmed S. pyogenes infection consists of a 10-day course of penicillin or other antibiotics. Symptomatic relief can also be provided with anti-inflammatory or analgesic medications.
3) Future efforts aim to develop an effective vaccine against S. pyogenes to help prevent streptococcal pharyngitis and its associated risks.
Original Description:
Journal Reading
Original Title
Journal Reading
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document1) Streptococcal acute pharyngitis is an inflammation of the throat that is commonly caused by Streptococcus pyogenes bacteria. While most cases are mild and self-limiting, S. pyogenes infection requires diagnosis and treatment to prevent potential post-infection complications.
2) Diagnosis involves throat culture or rapid antigen testing, and treatment of confirmed S. pyogenes infection consists of a 10-day course of penicillin or other antibiotics. Symptomatic relief can also be provided with anti-inflammatory or analgesic medications.
3) Future efforts aim to develop an effective vaccine against S. pyogenes to help prevent streptococcal pharyngitis and its associated risks.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
18 views31 pagesKarin Ananditya Fazri 30101407217: Pembimbing: DR, Dian Indah Setyorini, SP - THT-KL
Uploaded by
Vivie Tirany Soediro1) Streptococcal acute pharyngitis is an inflammation of the throat that is commonly caused by Streptococcus pyogenes bacteria. While most cases are mild and self-limiting, S. pyogenes infection requires diagnosis and treatment to prevent potential post-infection complications.
2) Diagnosis involves throat culture or rapid antigen testing, and treatment of confirmed S. pyogenes infection consists of a 10-day course of penicillin or other antibiotics. Symptomatic relief can also be provided with anti-inflammatory or analgesic medications.
3) Future efforts aim to develop an effective vaccine against S. pyogenes to help prevent streptococcal pharyngitis and its associated risks.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 31
JOURNAL READING
STREPTOCOCCAL
ACUTE PHARYNGITIS
PEMBIMBING:
DR, DIAN INDAH SETYORINI, SP.THT-KL
Karin Ananditya Fazri
30101407217
Journal Identity
Title : Streptococcal Acute Pharyngitis
Author : Lais Martins Moreira Anjos, Mariana Barros
Marcondes, Mariana Ferreira Lima, Alessandro Lia Mondelli
and Marina Politi Okoshi
Publisher : Journal of Tropical Medicine of Brazil Society
Year Published : 2015
INTRODUCTION
Pharyngitis is the inflammation of the pharynx- the
word comes from Greek word pharynx meaning
“throat” and the suffix-it is meaning”inflammation
In most cases it is quite painful and it is the most
common cause of sore throat. If the inflammation
includes tonsillitis,it may be called
pharyngotonsilitis
Acute pharyngitis/tonsillitis, characterized by
inflammation of posterior pharynx and tonsils, is a
common condition observed in outpatients
seeking healthcare provision.
Its main symptoms are sore throat and fever.
Most cases of acute pharyngitis present a benign
course and resolve without antiinfective
treatment
Several viruses and bacteria can cause acute
pharyngitis. however, Streptococcus pyogenes
(also known as Lancefield group A β-hemolytic
streptococci) is the only agent that requires an
etiologic diagnosis and specific treatment
S. pyogenes is of major clinical importance
because it can trigger post-infection systemic
complications, acute rheumatic fever, and post-
streptococcal glomerulonephritis, which occur 1-
3 weeks after the pharynx infection.
epidemiology
In the United States of America, there are an
estimated 7 million cases of acute pharyngitis
diagnosed in children annually. S. pyogenes is
responsible for 5% to 30% of cases of acute
pharyngitis, and it is more frequent in children
than in adults
It is more common in children between 5 years
and 15 years
In Brazil, it is difficult to evaluate the incidence of
streptococcal infections; however, the Brazilian
Institute of Geography and Statistics (Rio de
Janeiro, Brazil) estimates that 10 million cases of
streptococcal infection occur annually.
OBJECTIVE
In this review, we present the cause and clinical
manifestations of acute pharyngitis, and the
diagnosis and treatment of streptococcal
pharyngitis.
ETIOLOGY
Viruses cause approximately 75% of pharyngitis cases. The
following viruses have been associated with acute
pharyngitis: rhinovirus, coronavirus, adenovirus, influenza
virus, parainfluenza virus, coxsackievirus, herpes simplex
virus, Epstein-Barr virus, cytomegalovirus, and human
immunodeficiency virus (HIV).
In addition to group A streptococci, several strains of
bacteria can cause acute pharyngitis such as group C
streptococci and group G streptococci, Fusobacterium
necrophorum, Arcanobacterium haemolyticum, Neisseria
gonorrhoeae, Treponema pallidum, Francisella tularensis,
Corynebacterium diphtheriae, Yersinia enterocolitica,
Yersinia pestis, Mycoplasma pneumoniae, Chlamydophila
psittaci, and mixed anaerobes
CLINICAL MANIFESTATION
Common manifestations of acute pharyngitis are fever and sore
throat with or without tonsillar erythema, swelling, exudate, or
ulcerations
In streptococcal infections, symptom onset is usually abrupt and
includes intense sore throat, fever, chills, malaise, headache,
tender and enlarged anterior cervical lymph nodes, and
pharyngeal or tonsillar exudate.
Palatal petechiae and scarlatiniform rash are highly specific, but
rarely present.
Cough, conjunctivitis, and diarrhea are uncommon in
streptococcal infection, and their presence suggests a viral
etiology
DIAGNOSIS
A diagnosis of pharyngitis is supported by the patient’s medical
history and by the physical examination. Previous exposure to
streptococcus or viral agents should be investigated.
However, infection caused by many other agents can be
clinically indistinguishable from streptococcal pharyngitis
The etiologic diagnosis is based on laboratory
tests. Throat culture is the gold standard for
diagnosing pharyngitis caused by streptococcus
and it has a sensitivity ranging between 90% and
95%.
Samples should be obtained by vigorously
swabbing the tonsils and the posterior pharynx.
If the result is negative, most patients should not
be administered antibiotic therapy.
However, when the result is positive, it does not
eliminate the possibility of chronic colonization
ALTERNATIVE
Rapid antigen detection tests have been used to
detect S. pyogenes directly from throat swabs within
minutes
These tests have a high specificity (89.7%-99.0%) and
variable sensitivity (55.0%-99.0%), depending on the
assay used and the probability of streptococcal
infection.
When results are positive, the rapid tests guide
treatment and dispense with the need for a throat
culture.
However, if results are negative, clinicians should
decide between performing a throat culture or
ruling out streptococcal infection, based on the
clinical evidence of S. pyogenes and their health
service guidelines
Although etiologic diagnosis of streptococcal
pharyngitis depends on the laboratory tests,
clinical scoring systems have been developed to
predict the risk of S. pyogenes infection.
The most commonly used scoring system is the
Centor score, which was first proposed in 1981
and modified in 2004 to include age in the risk
classification
The authors clinically estimated the risk of
streptococcal pharyngitis by using fever, cough,
tender anterior cervical adenopathy, tonsillar
swelling or exudate, and patient age data
The Centor score was recently validated in an
analysis of data collected from 206,870 patients
aged 3 years or more with a painful throat.
Several guidelines recommend the score as a
triage method
TREATMENT
There are recommendation discrepancies between
the European and North American guidelines for
acute pharyngitis treatment, both of which
emphasize the importance of reducing overall
antibiotic use to limit antibiotic resistance.
However, many physicians still prescribe antibiotics in
patients with pharyngitis without evidence of S.
pyogenes infection. Because most acute pharyngitis
cases are caused by viruses, antibiotic treatment is
completely useless. A recent report showed that
antibiotics were prescribed for up to 73% of adults
with acute pharyngitis. In fact, acute pharyngitis is a
major cause of inappropriate antibiotic use in
clinical practice
Narrow-spectrum penicillins are the first choice for
treatment because of the rarity of documented
resistance to penicillin by group A streptococcus
during pharyngitis treatment and because of their
low cost.
The recommended oral formulation is penicillin V. For
complete agent eradication, it is important to
emphasize that oral penicillin should be taken for 10
days, even if symptoms subside within a few days.
It is difficult for patients to maintain treatment for 10
days because of the drug’s poor palatability, the
need to take it several times a day, and the rapid
symptom resolution.
Because amoxicillin is reportedly equally effective
and has a better palatability, it is a suitable option
for children.
In patients with penicillin allergy, cephalosporins
can be an acceptable alternative, although a
primary hypersensitivity to cephalosporins can
occur. The macrolides are another option.
S. pyogenes resistance to erythromycin has
increased with increased macrolide use
A recent literature review shows that the
administration of new generation antibiotics such
as azithromycin for 3-6 days has comparable
efficacy as the standard 10-day course of oral
penicillin.
However, the authors of that review state that this
result must be interpreted with caution in areas
with a high incidence of rheumatic heart disease
Anti-inflammatory agents such as ibu profen,
ketoprofen, and diclofenac, or analgesic agents
such as paracetamol can reduce severe
symptoms and high fever.
Systemic corticosteroids should not be routinely
prescribed in acute pharyngitis. They can
however be considered in adult patients who
have more severe presentations (e.g., a score of
3-4 points in the Centor criteria)
In a recurrence of pharyngitis, a throat swab
culture or a rapid antigen detection test should
be performed. When test results are positive,
patients should be treated again. In these cases,
it is also recommended to detect and treat
healthy carriers among people from the same
residence
FUTURE PERSPECTIVES
Future perspectives on preventing streptococcal
pharyngitis, and more importantly systemic post-
infection complications include the development
of an anti-Streptococcus pyogenes vaccine.
Several decades ago, efforts to produce a
vaccine against S.pyogenes began, and different
models have been proposed.
There are currently several vaccine models, most
in preclinical studies. Recent experimental studies
have shown that a 55-residue peptide, called
StreptInCor, can be an effective and safe
vaccine for preventing S. pyogenes infection.
CONCLUSION
Acute pharyngitis/tonsillitis is a common health issue caused by
several viruses and bacteria.
S. Pyogenes is the only agent that requires an etiologic diagnosis
and specific treatment because of its potential to trigger systemic
postinfection complications.
A diagnosis of pharyngitis is supported by medical history and
physical examination.
The clinical Centor score has been used to predict the risk of
S.Pyogenes infection.
Throat culture is the gold standard for diagnosing streptococcal
pharyngitis.
Rapid antigen detection tests have been used to detect S.
pyogenes directly from throat swabs within minutes.
Narrow-spectrum penicillins are still the first choice for treating
pharyngitis and preventing acute rheumatic fever.
You might also like
- Streptococcal PharyngitisDocument33 pagesStreptococcal PharyngitisIkrimaikNo ratings yet
- Streptococcal PharyngitisDocument19 pagesStreptococcal PharyngitisBimasenaNo ratings yet
- 4 PDFDocument5 pages4 PDFFriskyShandy BadiNo ratings yet
- Pediatric Pharyngitis: Etiology and Management ApproachesDocument4 pagesPediatric Pharyngitis: Etiology and Management ApproachesshibghatullahNo ratings yet
- The Clinical Presentation of Fusobacterium-Positive and Streptococcal-Positive Pharyngitis in A University Health ClinicDocument10 pagesThe Clinical Presentation of Fusobacterium-Positive and Streptococcal-Positive Pharyngitis in A University Health ClinicAnonymous zSt6YuNo ratings yet
- Tonsillectomy and Adenoidectomy and Myringotomy With Tube InsertionDocument12 pagesTonsillectomy and Adenoidectomy and Myringotomy With Tube Insertionlolamusic90No ratings yet
- PharyngitisDocument20 pagesPharyngitisPutri ClaraNo ratings yet
- Strep Throat GuidelinesDocument13 pagesStrep Throat Guidelinessnowden1No ratings yet
- Pharyngitis: Approach To Diagnosis and TreatmentDocument9 pagesPharyngitis: Approach To Diagnosis and Treatmentraudhatul muttaqinNo ratings yet
- Acute PharyngitisDocument3 pagesAcute PharyngitisMohammed Taha Al-nuaimyNo ratings yet
- URTIDocument18 pagesURTIAfnan RajeNo ratings yet
- Journal Reading Tonsilitis Akut PDFDocument6 pagesJournal Reading Tonsilitis Akut PDFTaufiq HidayatNo ratings yet
- Treatment of Acute PharyngitisDocument4 pagesTreatment of Acute PharyngitisZafira Ananda RaishaNo ratings yet
- Acute Pharyngitis: Group #9Document32 pagesAcute Pharyngitis: Group #9Shad SimNo ratings yet
- Upper Respiratory Tract Infections.: DR Abdelmoniem Saeed MohammedDocument47 pagesUpper Respiratory Tract Infections.: DR Abdelmoniem Saeed MohammedYousef Al-AmeenNo ratings yet
- Diagnosis and Treatment of Chronic CoughFrom EverandDiagnosis and Treatment of Chronic CoughSang Heon ChoNo ratings yet
- Faringitis StreptococcusDocument16 pagesFaringitis StreptococcusnurNo ratings yet
- TOnsillitis in ChildrenDocument5 pagesTOnsillitis in ChildrenTibu DollNo ratings yet
- Pharyngitis: Approach To Diagnosis and TreatmentDocument7 pagesPharyngitis: Approach To Diagnosis and TreatmentRanny Ariana PutriNo ratings yet
- Pharyngitis: Approach To Diagnosis and TreatmentDocument7 pagesPharyngitis: Approach To Diagnosis and TreatmentVio LatteireNo ratings yet
- Streptococcal PharyngitisDocument13 pagesStreptococcal PharyngitisAndreas IoannouNo ratings yet
- Pharyngitis Case ReportDocument4 pagesPharyngitis Case ReportMelissa TiofanNo ratings yet
- Acute and Chronic Tonsillitis in ChildrenDocument5 pagesAcute and Chronic Tonsillitis in ChildrenKym DominguezNo ratings yet
- Streptococcal PharyngitisDocument28 pagesStreptococcal PharyngitissylviaNo ratings yet
- Antibioticoterapia Na Pneumonia Pediátrica 2006Document7 pagesAntibioticoterapia Na Pneumonia Pediátrica 2006Tainah__100% (1)
- Optimizing The Management of The Main Acute Infections in Pediatric ORL Tonsillitis, Sinusitis, Otitis MediaDocument8 pagesOptimizing The Management of The Main Acute Infections in Pediatric ORL Tonsillitis, Sinusitis, Otitis MediaummilhumairoNo ratings yet
- Rational Laboratory For Etiology of Acute TonsillopharyngitisDocument2 pagesRational Laboratory For Etiology of Acute Tonsillopharyngitislegion spamNo ratings yet
- Diagnosis and Treatment of BronchiectasisDocument12 pagesDiagnosis and Treatment of Bronchiectasisrichie_ciandraNo ratings yet
- Streptococcal Pharyngitis: Clinical PracticeDocument8 pagesStreptococcal Pharyngitis: Clinical PracticeMilagros DiazNo ratings yet
- 04 Acute Bronchitis and Pneumonia in ChildrenDocument58 pages04 Acute Bronchitis and Pneumonia in ChildrenMi PatelNo ratings yet
- Case Study On Otitis Media. Group 2 BSN2A MCNP, Penablanca, CagayanDocument27 pagesCase Study On Otitis Media. Group 2 BSN2A MCNP, Penablanca, CagayanJean nicole GaribayNo ratings yet
- SJAMS 611 4269 4274 CDocument6 pagesSJAMS 611 4269 4274 CKiki Celiana TiffanyNo ratings yet
- Nosocomial Pneumonia: Self AssessmentDocument10 pagesNosocomial Pneumonia: Self AssessmentZali AhmadNo ratings yet
- Pharyngitis: Signs and SymptomsDocument26 pagesPharyngitis: Signs and SymptomsCM NajitoNo ratings yet
- Community Acquired Pneumonia, A Case StudyDocument26 pagesCommunity Acquired Pneumonia, A Case StudyMenggay SanDiego57% (7)
- Accepted Manuscript: Paediatric Respiratory ReviewsDocument32 pagesAccepted Manuscript: Paediatric Respiratory ReviewslaurentiaNo ratings yet
- Microbial Diseases of The Respiratory SystemDocument6 pagesMicrobial Diseases of The Respiratory SystemJohn Daemer Halasan KinocNo ratings yet
- When It Is Not Just A Sore ThroatDocument2 pagesWhen It Is Not Just A Sore ThroatSundar RamanathanNo ratings yet
- Pediatric Community-Acquired Pneumonia: Nelson 20 EdDocument43 pagesPediatric Community-Acquired Pneumonia: Nelson 20 EdRazel Kinette AzotesNo ratings yet
- Influenza: Laboratory FindingsDocument6 pagesInfluenza: Laboratory FindingsAlya Putri KhairaniNo ratings yet
- Management of PharyngotonsylitisDocument6 pagesManagement of PharyngotonsylitisAmeenu Isah HasheemNo ratings yet
- Role of Usage of Antibiotics in Pharyngitis: A Prospective StudyDocument5 pagesRole of Usage of Antibiotics in Pharyngitis: A Prospective StudypinandhitaNo ratings yet
- Enteric Fever 2013Document3 pagesEnteric Fever 2013aminceloNo ratings yet
- History: Allergic RhinitisDocument8 pagesHistory: Allergic RhinitisEga AnisaNo ratings yet
- JR Farlar 3Document12 pagesJR Farlar 3Coryza Gabrie tanNo ratings yet
- Tonsil Lo Pharyngitis Is Acute Infection of The PharynxDocument35 pagesTonsil Lo Pharyngitis Is Acute Infection of The PharynxJay-ar Batara Soriano0% (1)
- Whooping Cough - Still A Challenge: Coqueluche - Ainda Um DesafioDocument3 pagesWhooping Cough - Still A Challenge: Coqueluche - Ainda Um DesafioStacey GarciaNo ratings yet
- Rhinopharyngeal Retrograde Clearance Induces Less Respiratory Effort and Fewer Adverse Effects in Comparison With Nasopharyngeal Aspiration in Infants With Acute Viral BronchiolitisDocument7 pagesRhinopharyngeal Retrograde Clearance Induces Less Respiratory Effort and Fewer Adverse Effects in Comparison With Nasopharyngeal Aspiration in Infants With Acute Viral Bronchiolitismariane bezerraNo ratings yet
- Present Advancement in The Diagnosis and Treatment of Typhoid FeverDocument7 pagesPresent Advancement in The Diagnosis and Treatment of Typhoid Feverelsa_imamNo ratings yet
- Pneumonia Term PaperDocument8 pagesPneumonia Term Paperc5qvf1q1100% (1)
- Pharyngitis (Strep Throat) : Group A Streptococcal (GAS) DiseaseDocument7 pagesPharyngitis (Strep Throat) : Group A Streptococcal (GAS) DiseasegiselNo ratings yet
- Acute Rhinosinusitis in AdultsDocument7 pagesAcute Rhinosinusitis in AdultsMelissa BerlianNo ratings yet
- PIIS1198743X14619686Document27 pagesPIIS1198743X14619686yosefNo ratings yet
- 13-10 Topic 7. Complicated PneumoniaDocument35 pages13-10 Topic 7. Complicated PneumoniaReza Ervanda ZilmiNo ratings yet
- Tratamiento RinosinusitisDocument10 pagesTratamiento RinosinusitisrrrocafuNo ratings yet
- Influenza vaccination: What does the scientific proof say?: Could it be more harmful than useful to vaccinate indiscriminately elderly people, pregnant women, children and health workers?From EverandInfluenza vaccination: What does the scientific proof say?: Could it be more harmful than useful to vaccinate indiscriminately elderly people, pregnant women, children and health workers?No ratings yet
- Clinically Relevant Mycoses: A Practical ApproachFrom EverandClinically Relevant Mycoses: A Practical ApproachElisabeth PresterlNo ratings yet
- Living on the Frontline of COVID-19 in MCO And CMCOFrom EverandLiving on the Frontline of COVID-19 in MCO And CMCONo ratings yet
- Update On Otitis Media - Prevention and TreatmentDocument10 pagesUpdate On Otitis Media - Prevention and TreatmentVivie Tirany SoediroNo ratings yet
- Jurnal ObsgynDocument11 pagesJurnal ObsgynVivie Tirany SoediroNo ratings yet
- Jurnal ObsgynDocument11 pagesJurnal ObsgynVivie Tirany SoediroNo ratings yet
- Mengapa Didapatkan Keluhan Sakit Kepala Dan Panas Tinggi?: LBM 5 Demam Dan KejangDocument14 pagesMengapa Didapatkan Keluhan Sakit Kepala Dan Panas Tinggi?: LBM 5 Demam Dan KejangVivie Tirany SoediroNo ratings yet
- Sexual Transmitted DiseasesDocument27 pagesSexual Transmitted DiseasesVivie Tirany SoediroNo ratings yet
- Fisiologi Saraf SensorikDocument48 pagesFisiologi Saraf SensorikVivie Tirany SoediroNo ratings yet
- Lilbm3 Modul KB Dan KependudukanDocument14 pagesLilbm3 Modul KB Dan KependudukanVivie Tirany SoediroNo ratings yet
- Hse BooksDocument20 pagesHse BooksLaurentia AgathaNo ratings yet
- CPG Management of EVALI 20211007Document48 pagesCPG Management of EVALI 20211007MrS D100% (1)
- Nutramigen Insurance Letter 1Document2 pagesNutramigen Insurance Letter 1Richard BakerNo ratings yet
- ACE Inhibitors - Blood HypertensionDocument2 pagesACE Inhibitors - Blood HypertensionErik SilvaNo ratings yet
- DM Screen - PortraitDocument5 pagesDM Screen - PortraitEsteban BernsNo ratings yet
- Peritoneal DialysisDocument26 pagesPeritoneal DialysisKath LeenNo ratings yet
- Ppok 2023 PDFDocument33 pagesPpok 2023 PDFBagas Trikuncoro BawonoNo ratings yet
- Learning Module in NCM 114 Pre FinalDocument77 pagesLearning Module in NCM 114 Pre FinalJohn Van Dave TaturoNo ratings yet
- The Polymeal PlanDocument3 pagesThe Polymeal PlanFrancisco Chacón Lozsán KonradyNo ratings yet
- Try This! Directions: Answer All The Necessary Information Needed in The Column Below. UseDocument10 pagesTry This! Directions: Answer All The Necessary Information Needed in The Column Below. UseChristine Joy Molina100% (1)
- Notes On Renal Function Tests by Dr. Ashish Jawarkar ContactDocument26 pagesNotes On Renal Function Tests by Dr. Ashish Jawarkar ContactChaht RojborwonwitayaNo ratings yet
- (GM) Epidemiology and Prevention (NonCommunicable Disease)Document41 pages(GM) Epidemiology and Prevention (NonCommunicable Disease)Astrid FausziaNo ratings yet
- ArdsDocument9 pagesArdsNoel Anthony BadajosNo ratings yet
- Prof TestDocument13 pagesProf TestOlive NNo ratings yet
- Community Health NursingDocument23 pagesCommunity Health NursingMimi Vee100% (1)
- NR 325 Neuro Worksheet 2Document6 pagesNR 325 Neuro Worksheet 2John Thomas100% (1)
- PT3 ELSA SampleDocument8 pagesPT3 ELSA Samplefattahjamal50% (2)
- TPNDocument37 pagesTPNSreya Sanil100% (7)
- Crying ChildDocument36 pagesCrying ChildAbhay BarnwalNo ratings yet
- Case of DiverticulitisDocument5 pagesCase of DiverticulitisFuture RN100% (1)
- Diabetic Ketoacidosis in Pregnancy: Diagnosis of DKADocument7 pagesDiabetic Ketoacidosis in Pregnancy: Diagnosis of DKA123someone123No ratings yet
- Art of Case Taking by Pierre SchmidtDocument18 pagesArt of Case Taking by Pierre SchmidtDr. Debprasad Das100% (1)
- Non Resolving Pneumonia: by DR - Lokesh.L.V Moderators DR Mohan - Rao AND DR UmamaheshwariDocument58 pagesNon Resolving Pneumonia: by DR - Lokesh.L.V Moderators DR Mohan - Rao AND DR Umamaheshwaridrlokesh100% (5)
- U.S. Coast Guard Personnel Casualty Addendum: Section I - Reporting Vessel/Facility Information - Casualty Date/TimeDocument2 pagesU.S. Coast Guard Personnel Casualty Addendum: Section I - Reporting Vessel/Facility Information - Casualty Date/TimeArslan JadoonNo ratings yet
- Rheumatoid ArthritisDocument54 pagesRheumatoid ArthritisGökhan SüzenNo ratings yet
- Problem Solving With AnswersDocument50 pagesProblem Solving With Answersapi-3814958No ratings yet
- GotaDocument17 pagesGotaAtelos EctasiaNo ratings yet
- Balantidium ColiDocument14 pagesBalantidium ColiSanjay Kumar100% (1)
- Ronaldo Conspiracy TheoryDocument2 pagesRonaldo Conspiracy TheoryjanNo ratings yet
- Homeopathy: Similia Similibus Curentur, or "Like Cures Like"Document20 pagesHomeopathy: Similia Similibus Curentur, or "Like Cures Like"AK KJNo ratings yet