Professional Documents
Culture Documents
15-Kidney Pathology
Uploaded by
Rodriguez Vivanco Kevin Daniel0 ratings0% found this document useful (0 votes)
13 views32 pagesOriginal Title
15-Kidney pathology
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
13 views32 pages15-Kidney Pathology
Uploaded by
Rodriguez Vivanco Kevin DanielCopyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 32
Lecture Plan
The kidneys are essentially regulatory organs
which maintain the volume and composition of
body fluid by filtration of the blood and selective
reabsorption or secretion of filtered solutes.
The kidneys take their blood supply directly from
the aorta via the renal arteries; blood is returned to
the inferior vena cava via the renal veins
The kidneys are critical in regulating the internal
environment of the body.
Homeostasis:
Endocrine function:
Sodium/Volume;
Renin;
Water/Osmolarity;
Erythropoietin;
Asid/Base;
1,25 – Vitamin D
Electrolytes (K+, Ca++, Mg++, HPO4)
Hemodynamic regulation: Clearance:
Renin / Angiotensin / Aldosteron; Products of metabolism;
Sodium balance; Drugs and toxins;
Pressure natriuresis
Normal urine volume is 750 to 2000 ml per day.
Polyuria - increase the daily amount
of urine are usually caused by:
- absorption of edema, transudate, exudate;
- states after feverish;
- primary aldosteronism; Anuria - a lack of urine,
- hyperparathyroidism; less than 50 ml per day.
- nephrosclerosis; - acute renal failure;
- diabetes and diabetes insipidus - severe nephritis;
- meningitis (reflex);
Oliguria - a reduction of daily amount - poisoning;
of urine are usually caused by: - tetany;
- febrility; -blockage of the urinary tract
- heart disease; tumor or stone
- acute renal failure;
- nephrosclerosis.
Color of urine
Normally, urine is amber or straw-yellow color.
Changes in urine color is possible with a number of
physiological and pathological conditions.
Hyperhromuria is Hypohromuriya is physiological
physiological if it’s caused if it’s caused by polyuria as a
by oliguria as a result of limit result of increased drinking,
drinking, sweating, eating diuretics food.
carrots in the food.
Pathological hyperhromuria Pathological hypohromuriya is
is developed due to: developed due to:
- diarrhea; - diabetes;
- toxicoses;
- fever; - diabetes insipidus;
- vomiting; - nephrosclerosis.
- liver disease, heart disease;
- hemolytic state.
Normal urine is transparent. While standing in a vessel in it it's easy
to turbidity.
Turbidity of urine caused by crystals, cellular elements, bacteria,
mucus, and fat.
The reaction of the urine is normal when pH is 5,5-7,0.
Pathology of urine рН:
Acidic: Alkaline:
- diabetes (predkoma, coma); - haematuria;
- fevers; - after vomiting and diarrhea;
- starvation; -resorption of exudates,
- renal failure; transudate;
- tuberculosis of kidneys; - taking soda and mineral water;
- leukemia; - hyperhloremic acidosis;
- hypokalemic state - renal tubular acidosis;
(paradoxical aciduria) - chronic urinary tract infections
Qualitative changes of urine
Relative density of urine ranged from 1.010 to 1.025 in the adult.
Hyperstenuria - is the high Hypostenuria - is low relative
relative density of urine to ,030- density of urine. It indicates
1,034 and often can be caused by that concentrating function of
extra renal disturbances: the kidneys has lost:
-in the morning portion of -diabetes insipidus;
healthy individuals; -resorption of edema and
-in febrile patients; inflammatory infiltrates;
-a reduced amount of urine; -chronic pyelonephritis;
-with amyloid and lipoid -chronic nephritis;
nephrosis; -chronic renal failure;
-diabetes mellitus, glycosuria; -nephrosclerosis;
-hyperparathyroidism, etc. - glomerulonephritis.
Isostenuria - an absence of specific gravity‘s daily deviations. It
means that the diluting and concentrating functions of the
kidneys have both been lost:
-the latest stage of hronic renal failure;
-severe subacute and chronic nephritis.
Qualitative changes of urine
Pathological admixtures in urine
Proteinuria is defined as urinary protein excretion exceeding
150 mg/day.
The mechanism of proteinuria may be related to 2 aspects:
1. Molecular barrier injury: holes on glomerular basement
membrane (GBM) become larger, plasma protein can pass
through the GBM into the urine;
2. Charge barrier injury: loss of negative charge (glycoprotein)
within GBM, plasma protein (with negative charge) can pass
through the GBM into urine.
Proteinuria may be divided into two categories:
1. Nonpathological proteinuria - excessive protein excretion is
apparently not the result of a disease. The level of proteinuria is
generally less than 1 g/day and is never associated with edema.
1) Postural (orthostatic)
2) Febrile
3) Exercise-induced
2. Pathological proteinuria results from glomerular or tubular disorders.
It is characterized by persistent and severe intensity - more than 3.5
g/l.
1) Tubular:
Inherited - Cystinosis, Wilson disease, Lowe syndrome);
Acquired - Antibiotic-induced, Interstitial nephritis, Acute tubular
necrosis, Heavy metal poisoning);
2) Glomerular - nephrotic syndrome, idiopathic, mesangial proliferation,
focal sclerosis, glomerulonephritis, systemic diseases (lupus
erythematosus), drugs, hypertension, diabetes mellitus, hemolytic
uremic syndrome and other renal diseases.
Qualitative changes of urine
Haematuria is defined as appearance of RBC in urine
Common Causes of Glomerular Hematuria:
1. IgA nephropathy (Berger’s disease);
2. Thin glomerular basement membrane disease;
3. Hereditary nephritis (Alport’s syndrome). RENAL
Common Causes of Non-Glomerular Hematuria:
Upper Tract:
1. Urolithiasis;
URETERAL
2. Pyelonephritis;
3. Renal cell cancer;
4. Transitional cell carcinoma;
5. Urinary obstruction;
6. Benign hematuria
Lower Tract:
1. Bacterial cystitis;
BLADDER
2. Benign prostatic hyperplasia;
3. Transitional cell carcinoma; URETHRAL
4. Strenuous exercise (“marathon runner’s hematuria”);
5. Spurious hematuria (e.g. menses);
6. Instrumentation;
7. Benign hematuria
Haematuria is most usefully divided into:
Visible (macroscopic) haematuria (VH)
Non-visible (microscopic) haematuria (NVH) - is not visible to
the naked eye.
Macroscopic hematuria can be divided into three types:
Initial Hematuria - bleeding that occurs at the start of urination.
This could indicate a problem in the urethra in women or the
prostate (in men).
Total Hematuria - bleeding that occurs while urinating is known as
total hematuria. Men could experience total hematuria because
of an enlarged prostrate. In women, vaginal bleeding during
urination could be an indication of an infection in the bladder,
ureter or kidneys.
Terminal Hematuria - bleeding after urination in men and women.
Blood after urination in women is usually indicative of a
bladder infection. Men can also experience terminal hematuria
because of prostate diseases.
Qualitative changes of urine
Pathological admixtures in urine
Leukocyturia is the presence of leukocytes in urine
Usually, the WBC's in urine are granulocytes.
The common diseases that may result to the presence of leukocytes
in urine:
1. Urinary tract infection;
2. Cystitis – is the inflammation of the bladder (the infection has
made its way from the urethra to the bladder, spreading the
infection and damaging parts of the kidneys).
3. Pyelonephritis –is case, the infection has affected not only the
urethra and the bladder, but also the kidneys.
Qualitative changes of urine
Pathological admixtures in urine
Urinary casts are cylindrical aggregations of particulate matter that
form in the distal nephron.
The various types of casts that may be
classified as follows:
I. Acellular casts
Acellular casts II. Cellular casts
1. Hyaline casts - the most common type
of cast, Tamm-Horsfall mucoprotein
secreted from the tubular epithelial cells.
2. Granular casts -result either from the
breakdown of cellular casts, or the
inclusion of aggregates of plasma proteins.
3. Waxy casts - thought to represent the end product of cast
evolution, suggest the very low urine flow associated with severe,
longstanding kidney disease such as renal failure.
4. Fatty casts - formed by the breakdown of lipid rich epithelial cells,
these are hyaline casts with fat globule inclusions.
5. Pigment casts - formed by the adhesion of metabolic breakdown
products or drug pigments.
6. Crystal casts - though crystallized urinary solutes, such as
oxalates, urates, or sulfonamides, may become enmeshed within a
hyaline cast during its formation.
Qualitative changes of urine
Pathological admixtures in urine
Cellular casts
1. Red blood cell casts – are always pathologic, and is strongly
indicative of glomerular damage (glomerulonephritis, vasculitis,
lupus erythematosis, post-streptococcal glomerulonephritis or
Goodpasture’s syndrome). They are usually associated with
nephritic syndromes.
2. White blood cell casts - indicative of inflammation or
infection.
The presence of white blood cells within or upon casts strongly
suggests pyelonephritis, a direct infection of the kidney.
3. Bacterial casts - given their appearance in pyelonephritis,
these should be seen in association with loose bacteria, white
blood cells, and white blood cell casts.
4. Epithelial cell casts - formed via inclusion or adhering of
desquamated epithelial cells of the tubule lining (acute tubular
necrosis, toxic ingestion, such as from mercury, diethylene glycol,
or salicylate).
Qualitative changes of urine
Pathological admixtures in urine
Glycosuria - is the identification of glucose in urine.
In the urine of healthy human glucose is not detected in the urine
in clinical diagnostic laboratories.
Glucosuria depends on three factors:
1. Blood glucose concentration;
2. Glomerular filtrate kidney in 1 minute;
3. Amount reabsorbed in the tubules of glucose in 1 ml.
Glucosuria appears when blood glucose levels exceed 10 mmol/l –
the “renal threshold” or the glomerular clearance of glucose.
Causes of glycosuria:
1. Insulin deficiency;
2. Decline of renal function and / or liver;
3. Violation of the hormonal regulation of carbohydrate
metabolism;
4. Eating large amounts of carbohydrates
Clinical:
1. Primary - are caused by kidney pathology (acute diffuse proliferative
postinfectious GN, membranoproliferative GN, rapid progressive GN, lipoid
nephrosis, focal segmental sclerosis, membranous glomerulopathy, IgA
nephropathy, chronic glomerulonephritis);
2. Secondary - are caused by other organs and systems pathology or systemic
diseases: (SLE, diabetes mellitus, amyloidosis, Henoch-Schenlein purpura,
bacterial endocarditis);
3. Hereditary disorders - Alport syndrome, thin membrane disease etc.
Histopathological (patterns established on light microscopy):
Proliferative and nonproliferative variants are possible.
Membranous;
Mesangiocapillary;
Focal segmental glomerulosclerosis etc.
Etiological:
Inflammatory - the dominant aetiological agent for GN are bacteria, viruses,
parasites;
Noninflammatory – immunopathological;
Idiopathic.
In each of the clinical entities with glomerular proliferation,
the inflammation process leads to:
- decreased glomerular perfusion,
- retention of salt and water
- potential development of hypertension and edema.
Acute Poststreptococcal Glomerulonephritis (APSGN):
- is clearly the most frequent form of acute postinfectious
glomerulonephritis;
- the clinical syndrome is often regarded as the prototype of
the acute nephritic syndrome;
- Group A I²-hemolytic streptococcus serologic testing
confirms recent infection (pharyngitis or pyoderma).
APSGN is primarily a disease of school-age children (5 -
15 years) and is more common in boys.
Patients are usually afebrile with a latency period
following pharyngitis of 1 to 2 weeks and 3 to 6 weeks
after a skin infection.
The most common presenting features are edema and
gross hematuria. Essentially all the patients have
microhematuria. The urine often has a color, described as
smoky, cola-colored, or tea-colored.
Hypertension is common but is usually mild to moderate;
rarely, hypertensive encephalopathy has been reported.
Nephritic syndrome is a typical manifestation of APSGN.
Fewer than 5% of patients develop nephrotic syndrome
with significant proteinuria and a slightly depressed
serum albumin level.
Pathogenesis Streptococcal Infection
Immune Complexes Formation and
Depositions in Glomerular Basement Membrane (GBM)
Complement System Activated Low Serum Complement
Immune Injuries
Cellular Proliferation GBM Fracture
Capillary Lumen Narrowed Hematuria
Glomerular Blood Flow Decreased Proteinuria
Oliguria Glomerular Filtration Rate Distal Sodium Reabsorption
Decreased
Retention of Water and Sodium Odema
Blood Volume Hypertension
Nephritic Syndrome - is the acute onset of:
1. Hematuria - may be microscopic or macroscopic. Podocytes develop
large pores which allow blood and protein through.
2. Proteinuria - small amount, < 3.5 g/24 hr).
3. Hypertension is generally mild.
4. Oedema is usually mild and results from sodium and water
retention.
5. Oliguria (low urine volume <300ml/day due to renal function been
poor).
6. Red cell casts
Causes of Acute Nephritis:
I. Primary Glomerulonephritis - acute GN (post-streptococcal, non-
streptococcal, rapidly progressive GN, membrano-proliferative GN,
focal GN, IgA nephropathy).
II. Systemic Disease (SLE, polyarteritis nodosa, Wegener's
granulomatosis, Henoch-Schonlein purpura, cryoglobulinaemia).
Nephrotic syndrome - is a group of diseases having different
pathogenesis and characterized by clinical findings of:
1. Massive proteinuria (>3.5g in 24hrs, urine looks frothy), mostly
consists of loss of albumin.
2. Hypoalbuminemia (albumin is lost in the urine due to gaps in
podocytes allowing proteins to escape).
3. Oedema - is usually peripheral (swelling around ankles & eyes) due
to:
loss of albumin and intravascular oncotic pressure decreasing;
sodium and water retention (secondary hyperaldosteronism, but
osmotic pressure of blood is decreased);
increase of hydrodynamic intravascular pressure and vessels
permobility (fluid moves out of vessels);
4. Hyperlipidemia/hyperlipiduria is caused by:
1) Hypoproteinemia stimulates protein synthesis in the liver,
resulting in the overproduction of lipoproteins;
2) Lipid catabolism is decreased due to lower levels of lipoprotein
lipase.
Hyperlipiduria is due to hyperlipidemia.
I. Primary Glomerulonephritis:
Minimal change disease (most common in children);
Membranous GN (most common in adults);
Membranoproliferative GN;
Focal GN;
IgA Nephropathy
II. Systemic Disease (diabetes mellitus, amyloidosis, SLE)
III. Systemic Infections:
Viral infections (HBV, HCV, HIV);
Bacterial infections (Bacterial endocarditis, syphilis, leprosy);
Protozoa and parasites (P. falciparum malaria, filariasis)
IV. Hypersensitivity Reactions:
Drugs (penicillamine, tolbutamide, heroin addiction);
Bee stings, snake bite, poison ivy
V. Malignancy (carcinomas, myeloma, Hodgkin's disease)
VI. Pregnancy (toxaemia of pregnancy)
VII Circulator Disturbances (renal vein thrombosis, constrictive
pericarditis)
VIII. Hereditary Disease (Alport's disease, nail-patella syndrome)
Renal failure often refers to significant loss of renal
function.
When less than 10% of renal function remains, this is
termed end-stage renal failure (ESRF).
Renal failure may be:
- acute as usual is reversible process;
- chronic is termed end-stage renal failure (ESRF).
Acute renal failure (ARF) is an abrupt reduction in renal
function with elevation of Blood Urea Nitrogen (BUN) and
plasma creatinine levels, usually associated with oliguria
(urine output of less than 30 ml/hr or less than 400 ml/day),
although urine output may be normal or increased.
Acute renal failure commonly is classified as:
I. Pre-renal - is caused by impaired renal blood flow.
The GFR declines because of the decrease in filtration
pressure. Poor perfusion can result from hypotension,
renal vasoconstriction,, hypovolemia, hemorrhage,
or inadequate cardiac output.
II. Intra-renal - may result from pre-renal acute renal
failure (e.g., acute tubular necrosis or cortical necrosis)
or many other diseases, including acute glomerulonephritis,
malignant hypertension, disseminated intravascular
coagulation, and renal vasculitis.
III. Post-renal - usually occurs with bilaterally urinary tract
obstruction (e.g., bladder outlet obstruction,
prostatic hypertrophy, or bilateral ureteral
obstruction). Several hours of anuria with flank
pain followed by polyuria is a characteristic
finding. This type of renal failure can occur
after diagnostic catheterization of the ureters.
Sudden onset of oliguria (urine volume 20-200 mL/day).
Oliguria may not occur).
Proteinuria
Hematuria
Specific gravity of 1.010 -1.016.
Anorexia, nausea and vomiting
Lethargy
Elevation of blood pressure.
Signs of uremia: progressive increase in serum urea nitrogen,
creatinine, potassium, phosphate, sulfate; decrease in sodium,
calcium, bicarbonate.
Spontaneous recovery in a few days to 6 weeks.
Pathophysiology and Clinical manifestations of Uremic
syndrome
Uremia is a syndrome of renal failure and includes
elevated blood urea and creatinine levels accompanied by
fatigue, anorexia, nausea, vomiting, pruritus, and
neurologic changes. Usually develops when the creatinine
clearance falls to less than 10 mL/min.
Azotemia means increased serum urea levels and
frequently increased creatinine levels as well. Renal failure
causes azotemia.
Both azotemia and uremia indicate an accumulation of
nitrogenous waste products in the blood.
1. Retention of nitrogenous wastes
2. Increased intracellular Na+ and water
3. Decreased intracellular K+
4. Increased levels of bioactive substances normally cleared renally
(hormones)
5. Decreased levels of hormones and other mediators prodesed by
the kidney
6. Decrease basal body temperature
7. Diminished lipoprotein lipase activity
1. Skin manifestations - pruritus, uremic "frost", skin
2. Cardiac manifestations - uremic pericarditis
3. Neurological manifestations - peripheral neuropathy
4. Pulmonary complications - pneumonitis and
hemorrhage
5. Hematopoietic manifestations - anemia, bleeding
diathesis
6. Skeletal abnormalities - renal osteodystrophy
(secondary hyperparathyroidism)
7. Other metabolic imbalances
Thank you for your attention
You might also like
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (589)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5796)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1091)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- Herbal Medicine IntroDocument14 pagesHerbal Medicine IntrocryarNo ratings yet
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- Autopsy Life and Death - PoisonDocument3 pagesAutopsy Life and Death - PoisonJames DaurayNo ratings yet
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Urinary SystemDocument40 pagesUrinary Systemapi-87967494100% (3)
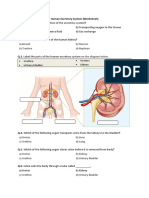
- Human Excretory SystemDocument2 pagesHuman Excretory SystemVio ElenaNo ratings yet
- Diploma ProspectusDocument16 pagesDiploma Prospectusanggun99No ratings yet
- Pathophysiology of Endocrine SystemDocument37 pagesPathophysiology of Endocrine SystemRodriguez Vivanco Kevin DanielNo ratings yet
- Congenital Anomalies of KidneDocument7 pagesCongenital Anomalies of KidneSanthosh.S.U100% (2)
- Ex, 2a, B, C, 3, 4a, B, Pages 50-51 (SB) 2a.: 1. Most Advertising in Ancient Times Was Word-Of-Mouth, That Is, PeopleDocument4 pagesEx, 2a, B, C, 3, 4a, B, Pages 50-51 (SB) 2a.: 1. Most Advertising in Ancient Times Was Word-Of-Mouth, That Is, PeopleRodriguez Vivanco Kevin DanielNo ratings yet
- Disappearing LanguagesDocument4 pagesDisappearing LanguagesRodriguez Vivanco Kevin DanielNo ratings yet
- Red Blood Cells PathologyDocument47 pagesRed Blood Cells PathologyRodriguez Vivanco Kevin DanielNo ratings yet
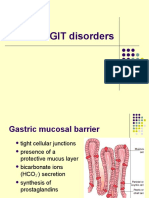
- 6 Krok GitDocument14 pages6 Krok GitRodriguez Vivanco Kevin DanielNo ratings yet
- 12-Blood Vessels PathologyDocument37 pages12-Blood Vessels PathologyRodriguez Vivanco Kevin DanielNo ratings yet
- Англ тести фармDocument138 pagesАнгл тести фармRodriguez Vivanco Kevin DanielNo ratings yet
- Pathphys ModuleDocument102 pagesPathphys ModuleRodriguez Vivanco Kevin DanielNo ratings yet
- 14-GIT and LiverDocument36 pages14-GIT and LiverRodriguez Vivanco Kevin DanielNo ratings yet
- 13 - Lung PathologyDocument38 pages13 - Lung PathologyRodriguez Vivanco Kevin DanielNo ratings yet
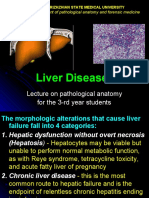
- Liver Diseases: Lecture On Pathological Anatomy For The 3-rd Year StudentsDocument27 pagesLiver Diseases: Lecture On Pathological Anatomy For The 3-rd Year StudentsRodriguez Vivanco Kevin DanielNo ratings yet
- Pathology of Pregnancy and Delivery: Lecture On Pathological Anatomy For The 3-rd Year StudentsDocument35 pagesPathology of Pregnancy and Delivery: Lecture On Pathological Anatomy For The 3-rd Year StudentsRodriguez Vivanco Kevin DanielNo ratings yet
- Endocrine Pathology: Lecture On Pathomorphology For 3-rd Year StudentsDocument44 pagesEndocrine Pathology: Lecture On Pathomorphology For 3-rd Year StudentsRodriguez Vivanco Kevin DanielNo ratings yet
- Example of Practical Work 3Document5 pagesExample of Practical Work 3Rodriguez Vivanco Kevin DanielNo ratings yet
- Tuberculosis:: - Classification - Morphology - Clinical FeaturesDocument28 pagesTuberculosis:: - Classification - Morphology - Clinical FeaturesRodriguez Vivanco Kevin DanielNo ratings yet
- Topic - Operation, AnesthesiaDocument5 pagesTopic - Operation, AnesthesiaRodriguez Vivanco Kevin DanielNo ratings yet
- Age PeriodsDocument12 pagesAge PeriodsRodriguez Vivanco Kevin DanielNo ratings yet
- Nursing Practice 2019Document87 pagesNursing Practice 2019Rodriguez Vivanco Kevin DanielNo ratings yet
- Nursing Care For Children With Urinary DisordersDocument55 pagesNursing Care For Children With Urinary DisordersTania Febria AzizahNo ratings yet
- Nursing Process DRUG ABUSEDocument24 pagesNursing Process DRUG ABUSEIris Caberte0% (1)
- Kelompok 2 - Tugas TT PT 6 - KODEFIKASI.Document3 pagesKelompok 2 - Tugas TT PT 6 - KODEFIKASI.Nalisa JasrinNo ratings yet
- Neurogenic BladderDocument11 pagesNeurogenic BladderRoy LiemNo ratings yet
- Interpretation of The eGFR Jul 07Document8 pagesInterpretation of The eGFR Jul 07Danielcc LeeNo ratings yet
- Unroanálisis Breve HistoriaDocument4 pagesUnroanálisis Breve HistoriaAndreaFonsecaNo ratings yet
- Interpretation of Urine DRDocument117 pagesInterpretation of Urine DRShanza AmaanNo ratings yet
- ReferensiDocument6 pagesReferensiLady AnnNo ratings yet
- Sign and Symptoms in Urology 1Document15 pagesSign and Symptoms in Urology 1Sri PertiwiNo ratings yet
- 62-Article Text-58-1-10-20190528 PDFDocument5 pages62-Article Text-58-1-10-20190528 PDFputri vinia /ilove cuteNo ratings yet
- Daftar Pustaka: Universitas Sumatera UtaraDocument3 pagesDaftar Pustaka: Universitas Sumatera UtaraAdisti ZakyatunnisaNo ratings yet
- Anna University - Bio Medical Engineering Syllabus Reg - 2017Document11 pagesAnna University - Bio Medical Engineering Syllabus Reg - 2017Haem Nahth50% (2)
- Biomarkers in Progressive Chronic Kidney Disease. Still A Long Way To GoDocument13 pagesBiomarkers in Progressive Chronic Kidney Disease. Still A Long Way To GoconstanzanazarethNo ratings yet
- Excretion in Humans Igcse BiologyDocument26 pagesExcretion in Humans Igcse BiologyThe PassionNo ratings yet
- Urinalysis in The Diagnosis of Kidney DiseaseDocument94 pagesUrinalysis in The Diagnosis of Kidney DiseasegibreilNo ratings yet
- NephrolithiasisDocument2 pagesNephrolithiasisDeepthiNo ratings yet
- Long-Term Safety and Efficacy of Psoas Bladder Hitch in Infants Aged Menor 12 Months With Unilateral Obstructive Megaureter. 2020. ENSAYO CLINICODocument8 pagesLong-Term Safety and Efficacy of Psoas Bladder Hitch in Infants Aged Menor 12 Months With Unilateral Obstructive Megaureter. 2020. ENSAYO CLINICOJulio GomezNo ratings yet
- Renal Embryology: Jason Ryan, MD, MPHDocument731 pagesRenal Embryology: Jason Ryan, MD, MPHFateh BoulounisNo ratings yet
- Chapter - 2: Basic Cell PhysiologyDocument72 pagesChapter - 2: Basic Cell Physiologyyash ingawaleNo ratings yet
- 11 Biology Chapter 20.Document4 pages11 Biology Chapter 20.jackieaj093No ratings yet
- Activity 6Document5 pagesActivity 6convekz100% (3)
- Urethroplasty, A Review of Indications, Techniques and OutcomesDocument5 pagesUrethroplasty, A Review of Indications, Techniques and OutcomesDKANo ratings yet
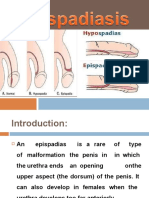
- EpispadiasisDocument12 pagesEpispadiasisvishnuNo ratings yet
- Education Program Curriculum: Academy of Life UnderwritingDocument6 pagesEducation Program Curriculum: Academy of Life Underwritingartlover30No ratings yet