Professional Documents
Culture Documents
Soal 3 Diagnosis PK 1 Laten
Uploaded by
Made Surya0 ratings0% found this document useful (0 votes)
22 views12 pagesThis document contains a case study of a 27-year-old woman, gravida 1, at 39 weeks gestation presenting with contractions and vaginal bleeding since the night before. On examination, the fetal head is at station 3/5 with no abnormalities detected. The CTG tracing is categorized as Category 2 with moderate variability, accelerations seen twice in 20 minutes, slow and variable decelerations present. The diagnosis is latent phase 1 labor with possible fetal cord compression. The proposed treatment is to monitor for signs of cord compression, change maternal positioning, and prepare for possible resuscitation or expedited delivery if needed.
Original Description:
Original Title
SOAL 3 CTG
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document contains a case study of a 27-year-old woman, gravida 1, at 39 weeks gestation presenting with contractions and vaginal bleeding since the night before. On examination, the fetal head is at station 3/5 with no abnormalities detected. The CTG tracing is categorized as Category 2 with moderate variability, accelerations seen twice in 20 minutes, slow and variable decelerations present. The diagnosis is latent phase 1 labor with possible fetal cord compression. The proposed treatment is to monitor for signs of cord compression, change maternal positioning, and prepare for possible resuscitation or expedited delivery if needed.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
22 views12 pagesSoal 3 Diagnosis PK 1 Laten
Uploaded by
Made SuryaThis document contains a case study of a 27-year-old woman, gravida 1, at 39 weeks gestation presenting with contractions and vaginal bleeding since the night before. On examination, the fetal head is at station 3/5 with no abnormalities detected. The CTG tracing is categorized as Category 2 with moderate variability, accelerations seen twice in 20 minutes, slow and variable decelerations present. The diagnosis is latent phase 1 labor with possible fetal cord compression. The proposed treatment is to monitor for signs of cord compression, change maternal positioning, and prepare for possible resuscitation or expedited delivery if needed.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 12
SOAL 3
I Made Ngurah Surya
Jihan Bennovry
Soal No.3
buat diagnosis, perencanaan tatalaksana dan jelaskan
• Ny. P, 27 th, G1 hamil 39 minggu, janin presentasi kepala tunggal
hidup
• Mengeluh kontraksi dan keluar darah lender sejak semalam
• TBJ 3500 g, kepala 3/5, tidak ada kelainan morfologi mayor, tidak ada
lilitan tali pusat, plasenta di fundus, volume air ketuban normal
• VT: pembukaan 2 jari, porsio axial, kenyal, ketuban (+), kepala H II
• Hasil CTG sbb:
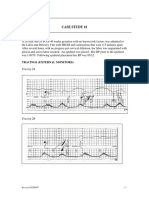
Interpretasi CTG
• Frekuensi Dasar: 130 dpm • Kontraksi uterus: 3-4x/10 menit
• Variabilitas: 20 dpm (normal) • Kekuatan: 40mmHg
• Akselerasi: 2x dalam 20 menit • Lamanya: 1.5 menit
• Deselerasi lambat • Relaksasi (+)
• Deselerasi variabel “shouldering • Ritme: reguler
sign” • Gerak janin: aktif 20x/10 menit
• Kesimpulan CTG kategori 2
Diagnosis
• PK 1 Laten pada G1 hamil 39 minggu, janin presentasi kepala tunggal
hidup
• Janin dengan kompresi tali pusat ec. ?
Tatalaksana
• Cari penyebab kompresi tali pusat
• Lakukan observasi dan evaluasi kembali secara berkala
• Resusitasi intrauterine dengan perubahan posisi ibu (lateral)
• Reposisi tali pusat jika tali pusat menumbung
• Pemberian oksigen pada ibu bila saturasi O2 bila ditemukan SpO2 ibu
turun
Variability refers to predominant baseline FHR pattern (marked, moderate, minimal, absent) during a 30-minute evaluation period, as defined by NICHD.
Marked variability is considered same as moderate variability for purposes of this algorithm.
Significant decelerations are defined as any of the following:
• Variable decelerations lasting longer than 60 seconds and reaching a nadir more than 60 bpm below baseline.
• Variable decelerations lasting longer than 60 seconds and reaching a nadir less than 60 bpm regardless of the baseline.
• Any late decelerations of any depth.
• Any prolonged deceleration, as defined by the NICHD. Due to the broad heterogeneity inherent in this definition, identification of a prolonged deceleration should prompt
discontinuation of the algorithm until the deceleration is resolved.
Application of algorithm may be initially delayed for up to 30 minutes while attempts are made to alleviate Category II pattern with conservative therapeutic interventions (eg,
correction of hypotension, position change, amnioinfusion, tocolysis, reduction or discontinuation of oxytocin).
Once a Category II FHR pattern is identified, FHR is evaluated and algorithm applied every 30 minutes.
Any significant change in FHR parameters should result in reapplication of algorithm.
For Category II FHR patterns in which algorithm suggests delivery is indicated, such delivery should ideally be initiated within 30 minutes of decision for cesarean.
If at any time tracing reverts to Category I status, or deteriorates for even a short time to Category III status, the algorithm no longer applies.
However, algorithm should be reinstituted if Category I pattern again reverts to Category II.
In fetus with extreme prematurity, neither significance of certain FHR patterns of concern in more mature fetus (eg, minimal variability) or ability of such fetuses to tolerate
intrapartum events leading to certain types of Category II patterns are well defined. This algorithm is not intended as guide to management of fetus with extreme prematurity.
Algorithm may be overridden at any time if, after evaluation of patient, physician believes it is in best interest of the fetus to intervene sooner.
You might also like
- Standard Operating Procedures HospitalDocument5 pagesStandard Operating Procedures HospitalCesar Francisco95% (37)
- Drug FormularyDocument112 pagesDrug FormularyKok Hui Diong100% (1)
- Case Report Uterine InversionDocument64 pagesCase Report Uterine InversionFelicia Yumita Winata100% (1)
- Soal 3 Diagnosis PK 1 LatenDocument12 pagesSoal 3 Diagnosis PK 1 LatenMade SuryaNo ratings yet
- Royal Hospital For Women: Clinical Policies, Procedures & Guidelines ManualDocument5 pagesRoyal Hospital For Women: Clinical Policies, Procedures & Guidelines ManualahmadsebastianakbarNo ratings yet
- Uterine Hyperstimulation, Management of - ABMU Maternity Guideline 2018Document7 pagesUterine Hyperstimulation, Management of - ABMU Maternity Guideline 2018Chintya MarcellinNo ratings yet
- Intrapartum Assessment: Jonelle Baloloy, MD MCMC Ob GyneDocument39 pagesIntrapartum Assessment: Jonelle Baloloy, MD MCMC Ob GyneJonelle baloloyNo ratings yet
- Kardiotokografi YBSDocument62 pagesKardiotokografi YBSUmmi RosmalasariNo ratings yet
- Fetal SurvillanceDocument26 pagesFetal SurvillanceBetelhem EjiguNo ratings yet
- Assessing Fetal Well-BeingDocument24 pagesAssessing Fetal Well-BeingMukesh ThakurNo ratings yet
- Nursing Care During Labor AND Birth: Group 3 - Ncma219RleDocument23 pagesNursing Care During Labor AND Birth: Group 3 - Ncma219Rlemonica mittiamNo ratings yet
- Intrapartum Fetal AssessmentDocument52 pagesIntrapartum Fetal AssessmentAditya TejabaswaraNo ratings yet
- Лекция, Аномалии Род Деятельности, Англ. -Document60 pagesЛекция, Аномалии Род Деятельности, Англ. -RamNo ratings yet
- Fetal Monitoring: Dr. Anjoo Agarwal Professor Dept of Obs & Gyn KGMU, LucknowDocument30 pagesFetal Monitoring: Dr. Anjoo Agarwal Professor Dept of Obs & Gyn KGMU, LucknowMay MardiahNo ratings yet
- O&g Hsajb ProtocolDocument69 pagesO&g Hsajb Protocol23-Chong Kar KinNo ratings yet
- Abnormal Cardiotohography in NewbornDocument37 pagesAbnormal Cardiotohography in NewbornAdityaRahaneNo ratings yet
- Fetal Monitoring GuideDocument15 pagesFetal Monitoring GuideMelodia Turqueza GandezaNo ratings yet
- 9fetal Well Being in PregnancyDocument10 pages9fetal Well Being in PregnancyuouoNo ratings yet
- Intrapartum Assessment: Factors That Affect Oxygenation During LaborDocument10 pagesIntrapartum Assessment: Factors That Affect Oxygenation During LabornicewanNo ratings yet
- Case Scenario: 1Document4 pagesCase Scenario: 1Artika MalaNo ratings yet
- Fetal Monitoring CTGDocument28 pagesFetal Monitoring CTGChuah Wei HongNo ratings yet
- CTG Algorithm 3jan08Document1 pageCTG Algorithm 3jan08TunnelssNo ratings yet
- RANZCOG CTG Guideline SummaryDocument23 pagesRANZCOG CTG Guideline SummaryAndi Farid ANo ratings yet
- Pregnant Woman with Uterine ProlapseDocument5 pagesPregnant Woman with Uterine ProlapseJashtine JingcoNo ratings yet
- Partograph and CTG Intrapartum Fetal MonitoringDocument56 pagesPartograph and CTG Intrapartum Fetal MonitoringPEÑAFLOR, Shealtiel Joy G.No ratings yet
- Abnormal LaborDocument114 pagesAbnormal LaborMohammad AlrefaiNo ratings yet
- Management of First Stage of LabourDocument55 pagesManagement of First Stage of LabourBharat ThapaNo ratings yet
- NST CSTDocument9 pagesNST CSTNadiya RashidNo ratings yet
- Ob Ati StudyDocument22 pagesOb Ati Studylpirman0580% (5)
- Antenatal Assessment of Fetal WellbeingDocument52 pagesAntenatal Assessment of Fetal Wellbeing6ixSideCreate MNo ratings yet
- Non-Invasive Fetal Surveillance Methods ExplainedDocument537 pagesNon-Invasive Fetal Surveillance Methods ExplainedMorita TakaNo ratings yet
- Normal Delivery Process and Fetal MonitoringDocument83 pagesNormal Delivery Process and Fetal MonitoringenriNo ratings yet
- Clinical Course and Management of First and SecondDocument66 pagesClinical Course and Management of First and SecondEkawali Sharma100% (1)
- Procedures ObgDocument12 pagesProcedures Obgraghuram reddyNo ratings yet
- CTG Interpretation and Response - 280720Document7 pagesCTG Interpretation and Response - 280720Yane Aulia YasminNo ratings yet
- Cardiotocography: Dr. Elise Johana Knoch 18 Januari 2017Document22 pagesCardiotocography: Dr. Elise Johana Knoch 18 Januari 2017Novita Rotua Sari SitumeangNo ratings yet
- Management of First Stage of Labour: Prepared By: Nirsuba Gurung Assistant Lecturer MsonDocument55 pagesManagement of First Stage of Labour: Prepared By: Nirsuba Gurung Assistant Lecturer MsonBharat ThapaNo ratings yet
- Antepartum Fetal Assessment 2018Document39 pagesAntepartum Fetal Assessment 2018amena mahmoudNo ratings yet
- Case Studies - Answers 1-4 PDFDocument11 pagesCase Studies - Answers 1-4 PDFAbbeygale GalanNo ratings yet
- OBG assessment of intra uterine fetal well beingDocument11 pagesOBG assessment of intra uterine fetal well beingshivaguruNo ratings yet
- Fetal Wellbeing AssessmentDocument67 pagesFetal Wellbeing AssessmentPaunami Dey50% (2)
- Partograph NextDocument50 pagesPartograph NextPrag GK Subedi0% (1)
- 1835 FHR MonitoringDocument47 pages1835 FHR MonitoringjackNo ratings yet
- Distosia: Dr. Kusuma Andriana SpogDocument63 pagesDistosia: Dr. Kusuma Andriana SpogAnisa WahyuniartiNo ratings yet
- 3. PARTOGRAMDocument30 pages3. PARTOGRAMMuwanga faizoNo ratings yet
- DR - Asirifi-Induction and Augmentation of Labour (Autosaved)Document19 pagesDR - Asirifi-Induction and Augmentation of Labour (Autosaved)Max ZealNo ratings yet
- Normal Labor, Partogram and Augmetation LatesttttDocument35 pagesNormal Labor, Partogram and Augmetation LatesttttnatyaNo ratings yet
- Normal Vs Abnormal Labour 2023Document52 pagesNormal Vs Abnormal Labour 2023Rohan Prem NairNo ratings yet
- Instruments and Medications in Labour Room & OtDocument40 pagesInstruments and Medications in Labour Room & OtIsaac TanNo ratings yet
- Stages of LabourDocument43 pagesStages of LabourhaisureshNo ratings yet
- Normal LaborDocument56 pagesNormal Laborحسام رياض عبد الحسين راضيNo ratings yet
- Normal Labor: Rumelle B. Reyes, M.D. Department of Obstretrics and Gynecology Eastern Visayas Regional Medical CenterDocument33 pagesNormal Labor: Rumelle B. Reyes, M.D. Department of Obstretrics and Gynecology Eastern Visayas Regional Medical CenterRumelle ReyesNo ratings yet
- Assessment of Fetal Wellbeing in Pregnancy Dr. Ban HadiDocument37 pagesAssessment of Fetal Wellbeing in Pregnancy Dr. Ban HadiKaram SaadNo ratings yet
- Antenatal AssessmentDocument84 pagesAntenatal AssessmentRitbano AhmedNo ratings yet
- NSO (Nipple Stimulation Contraction Stress Test) SANAANIDocument5 pagesNSO (Nipple Stimulation Contraction Stress Test) SANAANINur SetsuNo ratings yet
- ACOG Practice Bulletin 106, July 2009 - 1to11 by UPADDocument11 pagesACOG Practice Bulletin 106, July 2009 - 1to11 by UPADOwen AlbaNo ratings yet
- Safe Birth Planning (37Document22 pagesSafe Birth Planning (37dodoNo ratings yet
- Fetal CirculationDocument36 pagesFetal CirculationShfici AdanNo ratings yet
- 3 Month of Pregnancy Abortion 1st Daughter Twin Babies: Changes Felt by Patient Changes Observed by ExaminerDocument5 pages3 Month of Pregnancy Abortion 1st Daughter Twin Babies: Changes Felt by Patient Changes Observed by ExaminerEben Ezar Dela CruzNo ratings yet
- Menstrual Cycle Related Disorders: Volume 7: Frontiers in Gynecological EndocrinologyFrom EverandMenstrual Cycle Related Disorders: Volume 7: Frontiers in Gynecological EndocrinologySarah L. BergaNo ratings yet
- Length Tension Testing Book 2, Upper Quadrant: A Workbook of Manual Therapy TechniquesFrom EverandLength Tension Testing Book 2, Upper Quadrant: A Workbook of Manual Therapy TechniquesRating: 1 out of 5 stars1/5 (1)
- Antenatal CareDocument13 pagesAntenatal CareMade SuryaNo ratings yet
- Principles of Drug Use During LactationDocument18 pagesPrinciples of Drug Use During LactationMade SuryaNo ratings yet
- Pone.0113715 SlideDocument23 pagesPone.0113715 SlideMade SuryaNo ratings yet
- 2021 - Article - 3735 SlideDocument9 pages2021 - Article - 3735 SlideMade SuryaNo ratings yet
- 1471-0528.14400 SlideDocument6 pages1471-0528.14400 SlideMade SuryaNo ratings yet
- Bmjopen 2015 009189Document6 pagesBmjopen 2015 009189Made SuryaNo ratings yet
- Duration of The Second Stage of Labor in Multiparous Women: Maternal and Neonatal OutcomesDocument8 pagesDuration of The Second Stage of Labor in Multiparous Women: Maternal and Neonatal OutcomesMade SuryaNo ratings yet
- Management of Surgical Instruments With Radio Frequency Identification TagsDocument12 pagesManagement of Surgical Instruments With Radio Frequency Identification TagsMade SuryaNo ratings yet
- Basic Standard Procedure of Abdominal Hysterectomy: Part 1: Yuji Hiramatsu, MD, PHDDocument9 pagesBasic Standard Procedure of Abdominal Hysterectomy: Part 1: Yuji Hiramatsu, MD, PHDMade SuryaNo ratings yet
- An Audit of Sample Sizes For Pilot and Feasibility Trials Being Undertaken in The United Kingdom Registered in The United Kingdom Clinical Research Network DatabaseDocument6 pagesAn Audit of Sample Sizes For Pilot and Feasibility Trials Being Undertaken in The United Kingdom Registered in The United Kingdom Clinical Research Network DatabaseMade SuryaNo ratings yet
- Pathogenesis of Spontaneous Preterm BirthDocument39 pagesPathogenesis of Spontaneous Preterm BirthMade SuryaNo ratings yet
- Augmentation of Labour: Nabhan A, Boulvain MDocument8 pagesAugmentation of Labour: Nabhan A, Boulvain MMade SuryaNo ratings yet
- Estimating The Sample Size For A Pilot Randomised Trial To Minimise The Overall Trial Sample Size For The External Pilot and Main Trial For A Continuous Outcome VariableDocument17 pagesEstimating The Sample Size For A Pilot Randomised Trial To Minimise The Overall Trial Sample Size For The External Pilot and Main Trial For A Continuous Outcome VariableMade SuryaNo ratings yet
- A History of Surgery in The Instrument Tray: Eponymous Tools Used in Hand SurgeryDocument12 pagesA History of Surgery in The Instrument Tray: Eponymous Tools Used in Hand SurgeryMade SuryaNo ratings yet
- Basic Principle and Step-by-Step Procedure of Abdominal Hysterectomy: Part 2Document11 pagesBasic Principle and Step-by-Step Procedure of Abdominal Hysterectomy: Part 2Made SuryaNo ratings yet
- European Journal of Obstetrics & Gynecology and Reproductive BiologyDocument6 pagesEuropean Journal of Obstetrics & Gynecology and Reproductive BiologyMade SuryaNo ratings yet
- Resources, Conservation & Recycling: Full Length ArticleDocument8 pagesResources, Conservation & Recycling: Full Length ArticleMade SuryaNo ratings yet
- Guidelines For The Development of Research Proposals Following A Structured, Holistic Approach For A Research Proposal (SHARP)Document15 pagesGuidelines For The Development of Research Proposals Following A Structured, Holistic Approach For A Research Proposal (SHARP)Made SuryaNo ratings yet
- The American Journal of Surgery: Xiaodong (Phoenix) Chen, Alan Harzman, Amalia Cochran, E.Christopher EllisonDocument4 pagesThe American Journal of Surgery: Xiaodong (Phoenix) Chen, Alan Harzman, Amalia Cochran, E.Christopher EllisonMade SuryaNo ratings yet
- The New England Journal of MedicineDocument7 pagesThe New England Journal of MedicineMade SuryaNo ratings yet
- COVID-19 Plan Protect StaffDocument5 pagesCOVID-19 Plan Protect StaffArgie Corbo BrigolaNo ratings yet
- Comprehensive Hospital Strategic Plan ExampleDocument28 pagesComprehensive Hospital Strategic Plan ExampleEsteban R. Langlois100% (1)
- Malaria in ChildrenDocument19 pagesMalaria in ChildrenAngel Ellene MarcialNo ratings yet
- Communicable Disease AnswersDocument11 pagesCommunicable Disease AnswersRika MaeNo ratings yet
- Sjögren's SyndromeDocument18 pagesSjögren's Syndromezakaria dbanNo ratings yet
- Christopher Hammond - Homeopathy - An Illustrated Encyclopedia of Safe and Effective Remedies (Natural Ways To Health) (1995) - Libgen - LiDocument264 pagesChristopher Hammond - Homeopathy - An Illustrated Encyclopedia of Safe and Effective Remedies (Natural Ways To Health) (1995) - Libgen - LisengourabNo ratings yet
- Complementary therapy for reducing pain in gastritis patientsDocument28 pagesComplementary therapy for reducing pain in gastritis patientsYendy AftirandiNo ratings yet
- The Effect of Music Therapy On Pain Level in Infusion in Children 6-12 Years of Age at Harapan Dan Doa HospitalDocument9 pagesThe Effect of Music Therapy On Pain Level in Infusion in Children 6-12 Years of Age at Harapan Dan Doa Hospitalratna purnamasariNo ratings yet
- Choque HemorragicoDocument9 pagesChoque HemorragicoAna NevesNo ratings yet
- ADMINISTRATIVE SERVICES in HospitalDocument20 pagesADMINISTRATIVE SERVICES in HospitalSthitapragyan senapati100% (1)
- LAPORAN DATA KESAKITAN ICD XDocument5,181 pagesLAPORAN DATA KESAKITAN ICD XReyni ThasariNo ratings yet
- Health Declaration Form: (Buong Pangalan) (Petsa) (Oras) (Kasa/ukuyang Tirahan) : (Numero NG Telepono)Document1 pageHealth Declaration Form: (Buong Pangalan) (Petsa) (Oras) (Kasa/ukuyang Tirahan) : (Numero NG Telepono)NICOSAT CollegesNo ratings yet
- Measuring pulse and oxygen with a pulse oximeterDocument2 pagesMeasuring pulse and oxygen with a pulse oximeterPedro TelloNo ratings yet
- Pleural Effusion - ClinicalKeyDocument13 pagesPleural Effusion - ClinicalKeyWialda Dwi rodyahNo ratings yet
- Tanzania Health System Assessment 2010Document135 pagesTanzania Health System Assessment 2010Anney Mwakabonga100% (1)
- Fac Thrombolysis 2007Document36 pagesFac Thrombolysis 2007Tri Harjono0% (1)
- Swami SIVANANDA - Practice of Ayurveda DDocument170 pagesSwami SIVANANDA - Practice of Ayurveda Dthomas100% (1)
- Newborn AssessmentDocument6 pagesNewborn AssessmentSirine AjourNo ratings yet
- Study of Hemotologicalprofile and Serum Iron Indices in Chronic Kidney Disease in Tertiary Care CentreDocument5 pagesStudy of Hemotologicalprofile and Serum Iron Indices in Chronic Kidney Disease in Tertiary Care CentreIJAR JOURNALNo ratings yet
- Ene 14885Document12 pagesEne 14885mikeNo ratings yet
- Dementia Vs DeliriumDocument40 pagesDementia Vs DeliriumDr. Mushfique Imtiaz ChowdhuryNo ratings yet
- e-CHECK (XS) HELPDocument3 pagese-CHECK (XS) HELPImas NurhayatiNo ratings yet
- The Common ColdDocument3 pagesThe Common ColdLalan ArdyanNo ratings yet
- Career Test High School College Students Free Job Quiz Best TestsDocument2 pagesCareer Test High School College Students Free Job Quiz Best TestsShibaQLeapNo ratings yet
- Transes Tra-FundaDocument33 pagesTranses Tra-FundaJoshua DelantarNo ratings yet
- Cardiac Arrhythmias Guide - Causes, Symptoms and Treatment OptionsDocument5 pagesCardiac Arrhythmias Guide - Causes, Symptoms and Treatment OptionsaksinuNo ratings yet
- Sandaletal UpdateonITPDocument18 pagesSandaletal UpdateonITPMarcellia AngelinaNo ratings yet