Professional Documents
Culture Documents
832 Inservicespectrumucl
Uploaded by
api-5190368660 ratings0% found this document useful (0 votes)
12 views16 pagesOriginal Title
832inservicespectrumucl
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
12 views16 pages832 Inservicespectrumucl
Uploaded by
api-519036866Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 16
Ulnar Collateral Ligament
Injury and Rehabilitation in the
Overhead Athlete
Alex Caudy, SPT
Background
• Elbow injuries (specifically UCL injuries) are becoming increasingly more
prevalent in the overhead athlete
• 193% increase in UCL reconstruction surgeries in the past 10 years 1
• A survey of 6135 professional baseball players was done seeking results on
how common UCL reconstructions were currently in the game. 2 It found
that amongst responding pitchers:
• 26% of major league pitchers reported having undergone a UCL reconstruction
• 19% of minor league pitchers reported having undergone a UCL reconstruction
• And pro baseball players are not the only ones being affected by this
“epidemic”. UCL reconstructions in individuals under 18 has been on the
rise as well 3
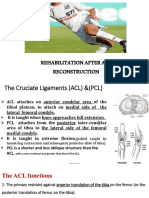
Anatomy
• Static Restraints
• Osseus hinge joint
• Medial joint capsule
• UCL
• UCL is composed of the anterior, posterior, and
transverse bundles
• Anterior band is primary restraint to valgus
forces (stabilizes from 30-90 deg of elbow
flexion)
• Posterior band stabilizes from 90-120 deg of
elbow flexion
• Dynamic Restraints
• Flexor Pronator Mass
• This is composed of FCU, FDS, and Pronator
Teres
Risk Factors for Young Overhead Athletes4,5
• Throwing when fatigued!!!
• High Velocity
• High pitching volume
• Throwing year round
• Poor throwing mechanics
• Warm weather climates
• Pitcher/catcher combination
Immediate Treatments
• Rest and Load Management
• Non-Operative Rehab
• Reconstruction
• Repair
Non-Operative Rehab for UCL Sprains
• Around 50% of individuals with UCL injury can be treated non-surgically and return to prior level of
function 6
• Rest and anti-inflammatories
• Often includes bracing for around 3-4 weeks, depending on the severity of the sprain
• To prevent valgus stress and to limit range of motion initially
• Non-painful ROM is progressed gradually
• Muscle strengthening
• Initially consists of isometrics
• Emphasis on wrist flexors and pronators (Flexor Pronator Mass provides dynamic support for UCL)
• Thrower’s Ten
• Often not throwing for 2-3 months
• Initiated after adequate strength testing and no pain
• Platelet Rich Plasma (PRP) Injections are common
• Enhances body’s healing response, platelets have growth factors
Operative (Reconstructions)7
• Modified Jobe (Figure 8 Method)-James Andrews, MD
• FPM is spared with modified technique; is just elevated to expose UCL and
sublime tubercle of ulna
• Subcutaneous ulnar nerve transposition from the cubital tunnel
• Utilizes a series of tunnels through the medial epicondyle of humerus and
sublime tubercle of ulna; graft is then passed through these in a figure 8
pattern
• Docking Procedure- David Altchek, MD
• FPM is divided through muscle splitting technique
• Usually no subcutaneous ulnar nerve transposition
• The graft is secured/docked with a bone bridge
Operative (Repairs)8
• Typically done in adolescent and young adults with good joint stability
• Require good tissue quality; typically done only with proximal or distal
insertion tears unless the mid-substance tear is minor
• Due to surgical advances, repairs are making a comeback…
• UCL Repair with Internal Brace
• Augmentation of the original ligament with a collagen dipped tape (internal brace) and
then anchored at the proximal and distal original UCL footprints
• Surgical dissection similar to Modified Jobe (FPM elevated to expose UCL, subcutaneous
ulnar nerve transposition only in patients presenting with existing neuro symptoms)
• Healing time significantly shorter than reconstruction!! (Return to play around 5 months
as opposed to about 12 months)
Rehabilitation Following Reconstructions
• Acute Phase (Weeks 0-4)-Phase 1
• Protect healing UCL with bracing
• Decrease pain and inflammation
• Gradually restore range of motion
• Prevent Muscular Disuse Atrophy
• Wrist/hand isometrics, UE isometrics, isotonics later in phase 1
• Scapular, glenohumeral, core, and lower extremity need to be considered
• Subacute Phase (Weeks 4-10)-Phase 2
• Continue ROM and stretching
• Discontinue brace about 6 weeks
• Isotonic strengthening
• Thrower’s Ten about week 5
• Continue Core and LE program
Rehabilitation Following Reconstructions
Cont.
• Advanced Phase (weeks 10-16)- Phase 3
• Continue ROM and stretching as needed
• Advanced Isotonic Program
• Advanced Thrower’s Ten
• Emphasis on eccentric control
• Incorporate Plyometrics
• Return to Activity Phase (week 16)- Phase 4
• Light stretching program
• Advanced thrower’s ten
• Plyometrics
• Begin interval Throwing Program at about 5-6 months; off mound beginning about 9 months
• Return to competitive throwing 12-18 months
Rehabilitation Following Repairs8
• Immediate Post-Op Phase (week 1)
• Protect healing tissue with brace, reduce pain and inflammation, retard
muscle atrophy, achieve full wrist ROM
• Controlled Mobility Phase (weeks 2-5)
• Gradually restore ROM, improve muscular strength and endurance, normalize
joint arthrokinematics
• Initiate Thrower’s Ten at week 3
• Intermediate Phase (weeks 6-8)
• Restore full elbow ROM, progress UE strength, continue with functional
progression
• DC brace at week 6, initiate advanced thrower’s 10, plyometrics, core
Rehabilitation Following Repairs cont. 8
• Advanced Phase (weeks 9-14)
• Advance strengthening exercises
• Initiate interval throwing program week 12 with progression to long toss
• Continue 1 and 2 hand plyometrics
• Return To Activity/Play Phase (weeks 14+)
• Progress long toss, flat ground pitching about weeks 16-20
• Return to mound activities about week 20
• Return to competition when ready at this point
Comparison of Timelines
• Thrower’s Ten initiated much faster with repair (week 3 vs 5)
• Both discontinue brace around week 6
• Advanced thrower’s ten initiated earlier with repair (week 6 vs 10-16)
• Plyometrics initiated earlier (weeks 6 vs 10-16)
• Interval throwing program initiated earlier (week 12 vs 5-6 months)
• Return to Play earlier (about 5 months vs at least 12 months)
Outcomes3
• 83% of pitchers included in a review by Cain et al. were able to return to
the same or higher level of competition in one year following UCL
reconstruction
• 76% of MLB, 73% of minor league, and 83% of high school athletes (total n=256) 3
• 70% of repairs returned to previous level of competition or higher3
• However, this sample size was much smaller
• This new internal brace technique is not really being used with professional
athletes yet as data collection continues
• According to Wilk et al. the results are showing promise for this new repair
technique however more research is needed before it becomes more common
with pro athletes. 8
Summary
• UCL injuries are becoming much more common in overhead athletes and these
injuries are starting to become prevalent at younger ages
• About half of UCL injuries can be treated non-surgically
• If surgery is opted for, then repair or reconstruction?
• Rehabilitation following repair follows a significantly more accelerated timeline
than that of reconstruction
• Outcomes following surgical UCL treatment and subsequent rehabilitation are
overall good to great
• More research is needed on internal brace repairs, but this could be a game
changer if integrated at the professional level due to its quick return to play
timeline
References
• 1. Hodgins JL, Vitale M, Arons RR, Ahmad CS. Epidemiology of medial ulnar collateral ligament reconstruction: a 10-year
studyin New York State. Am J Sports Med. 2016;44:729-734
• 2. Leland DP, Conte S, et al: Prevalence of Medial Ulnar Collateral Ligament Surgery in 6135 Current Professional
Baseball Players: A 2018 Update. Am J Sports Med. Orthop J Sports Med. 2019 Sep 25;7(9)
• 3. Cain EL, Andrews JR, Dugas JR, et al: Outcome of UCL Reconstruction of the Elbow in 1281 Athletes. Am J Sports Med.
2010 Dec;38(12):2426-34
• 4. Fleisig GS, Andrews JR: Prevention of elbow injuries in youth baseball pitchers. Sports Health. 2012 Sep;4(5):419-24.
• 5. Olsen II SM, Fleisig GS, et al: Risk factors for shoulder and elbow injuries in adolescent baseball pitchers. Am J Sports
Med. 2006 Jun;34(6):905-12.
• 6. Rettig AC, Sherrill C, Snead DS, Mendler JC, Mieling P. Nonoperative treatment of ulnar collateral ligament injuries in
throwing athletes. Am J Sports Med. 2001;29:15-1.
• 7. Looney AM, Fackler NP, Pianka MA, et al. No Difference in Complications Between Elbow Ulnar Collateral Ligament
Reconstruction With the Docking and Modified Jobe Techniques: A Systematic Review and Meta-analysis. Am J Sports
Med. 2021;3635465211023952.
• 8. Wilk KE, Arrigo CA, Bagwell MS, Rothermich MA, Dugas JR. Repair of the Ulnar Collateral Ligament of the Elbow:
Rehabilitation Following Internal Brace Surgery. J Orthop Sports Phys Ther. 2019;49(4):253-261.
You might also like
- Rehabilitation After Anterior Cruciate Ligament ReconstructionDocument62 pagesRehabilitation After Anterior Cruciate Ligament ReconstructionVladGrosuNo ratings yet
- نسخة light blue creative modern medical clinic presentationDocument33 pagesنسخة light blue creative modern medical clinic presentationFaresNo ratings yet
- Postertemplate 36 X 24Document1 pagePostertemplate 36 X 24api-300747065No ratings yet
- Hip Labral Repair PresentationDocument15 pagesHip Labral Repair Presentationapi-612728940No ratings yet
- Recent Advances in The Rehabilitation LCADocument19 pagesRecent Advances in The Rehabilitation LCAMiguel Andres Sepulveda CastroNo ratings yet
- ACL InjuryDocument42 pagesACL InjuryRishabh VermaNo ratings yet
- Rehabilitation of Traumatic Injuries To Knee/Ankle/FootDocument57 pagesRehabilitation of Traumatic Injuries To Knee/Ankle/FootStefan VladNo ratings yet
- Acl CaseDocument8 pagesAcl CaseLidia DebbyNo ratings yet
- Tratamiento Osteopático para Paciente Con Reconstrucción de LCADocument4 pagesTratamiento Osteopático para Paciente Con Reconstrucción de LCAAdolfo Esteban Soto MartinezNo ratings yet
- Avances LCA WilkDocument19 pagesAvances LCA WilkCarlos Martín De RosasNo ratings yet
- Anterior Cruciate Ligament Rekonstruction PhysioplusDocument13 pagesAnterior Cruciate Ligament Rekonstruction PhysioplusAde Dian KurniawanNo ratings yet
- Sport Traumatology-III Knee Complex-10Document26 pagesSport Traumatology-III Knee Complex-10kamran aliNo ratings yet
- Scapular DyskinesisDocument32 pagesScapular DyskinesisorthodoctorvinayNo ratings yet
- Knee Injuries Part 1Document38 pagesKnee Injuries Part 1meenoNo ratings yet
- Meniscus Injury: Khairul Nizam Abdul Rahman 4262143008Document22 pagesMeniscus Injury: Khairul Nizam Abdul Rahman 4262143008Soumashree MondalNo ratings yet
- Rehab AclDocument71 pagesRehab AclQuang TranNo ratings yet
- The Long-Term Effect of 2 PostoperativeDocument9 pagesThe Long-Term Effect of 2 Postoperativeahmed K.Abd el SaterNo ratings yet
- Trunk Stability by Calvin Morriss, PHD.: What Exactly Is Trunk Stability For A Rugby Player?Document9 pagesTrunk Stability by Calvin Morriss, PHD.: What Exactly Is Trunk Stability For A Rugby Player?Justice Man100% (1)
- Biomech Swimming ConditionsDocument23 pagesBiomech Swimming ConditionsSanjanaa ZadNo ratings yet
- Jeeth Case Study ASCADocument9 pagesJeeth Case Study ASCAJeeth DevaiahNo ratings yet
- ACL Reconstruction 2020Document39 pagesACL Reconstruction 2020محمد عقلNo ratings yet
- 27.08 - Arthroscopic Rotator Cuff RepairDocument24 pages27.08 - Arthroscopic Rotator Cuff RepairMoiz AliNo ratings yet
- Slow Guy Speed SchoolDocument77 pagesSlow Guy Speed SchoolOrestis AndreouNo ratings yet
- 5a4 PCLDocument6 pages5a4 PCLNyemas reda LedistiaNo ratings yet
- Rehabilitation Guidelines For Posterior Cruciate Ligament ReconstructionDocument6 pagesRehabilitation Guidelines For Posterior Cruciate Ligament ReconstructionMono MostafaNo ratings yet
- Scapular Stabilization ExercisesDocument2 pagesScapular Stabilization ExercisesnimitrisNo ratings yet
- Post-Op Shoulder 1Document49 pagesPost-Op Shoulder 1api-557944670No ratings yet
- Hall Poster MiniDocument1 pageHall Poster Miniapi-290917332No ratings yet
- Rehabilitation After Surgery of The Spinal Deformity: Presented byDocument40 pagesRehabilitation After Surgery of The Spinal Deformity: Presented byreskiNo ratings yet
- Qindeel - Fatima - 102 - Sports PT - AssignmentDocument16 pagesQindeel - Fatima - 102 - Sports PT - AssignmentQindeel FatimaNo ratings yet
- Posterior Tibialis Tendon Dysfunction (PTTD)Document11 pagesPosterior Tibialis Tendon Dysfunction (PTTD)bigpawn13No ratings yet
- Acute Anterior Shoulder Dislocation Physical Therapy ProtocolDocument4 pagesAcute Anterior Shoulder Dislocation Physical Therapy Protocolgermano87No ratings yet
- Rotator Cuff RepairDocument10 pagesRotator Cuff Repairapi-331169259No ratings yet
- Weight Lifting Day 1Document37 pagesWeight Lifting Day 1AdnanNo ratings yet
- Patellar Tendon Rupture and RehabilitationDocument4 pagesPatellar Tendon Rupture and RehabilitationdedsnetNo ratings yet
- Reab. CotoveloDocument29 pagesReab. CotoveloAugusto ManoelNo ratings yet
- Ox Ach Exere-Prescripn-slides SuppletDocument40 pagesOx Ach Exere-Prescripn-slides SuppletБаровић ЛукаNo ratings yet
- Hip InjuryDocument53 pagesHip InjuryDevsya DodiaNo ratings yet
- SH 1Document10 pagesSH 1ع الNo ratings yet
- Total Knee ReplacementDocument23 pagesTotal Knee ReplacementLeoNo ratings yet
- Qindeel Fatima 102 Sports PT AssignmentDocument16 pagesQindeel Fatima 102 Sports PT AssignmentQindeel FatimaNo ratings yet
- Progressive Systematic Functional Rehabilitation: Ameema, Hina, IfraDocument33 pagesProgressive Systematic Functional Rehabilitation: Ameema, Hina, Ifrakashmala afzalNo ratings yet
- Elbow Subluxation With Ucl and Triceps TearDocument27 pagesElbow Subluxation With Ucl and Triceps Tearapi-385570980No ratings yet
- Rehabilitasi Post Op Spine Surgery: Kobal Sangaji Dokter Spesialis Rehabilitasi Medik RS Awalbros PekanbaruDocument27 pagesRehabilitasi Post Op Spine Surgery: Kobal Sangaji Dokter Spesialis Rehabilitasi Medik RS Awalbros PekanbarukurniaNo ratings yet
- Total Knee Replacement ProtocolDocument4 pagesTotal Knee Replacement ProtocolSheel GuptaNo ratings yet
- Arthroscopic Shoulder Anterior Stabilisation Rehabilitation Protocol by TENDAYI MUTSOPOTSI MSc. ORTHO-MEDDocument8 pagesArthroscopic Shoulder Anterior Stabilisation Rehabilitation Protocol by TENDAYI MUTSOPOTSI MSc. ORTHO-MEDPhysiotherapy Care SpecialistsNo ratings yet
- Knee DislocationDocument39 pagesKnee Dislocationdr_s_ganesh100% (1)
- Knee Meniscus Repair 2008Document5 pagesKnee Meniscus Repair 2008drrajmptnNo ratings yet
- Short-Term Recovery From HipDocument4 pagesShort-Term Recovery From Hipdamien333No ratings yet
- Neurorehabilitasi Nyeri KronisDocument60 pagesNeurorehabilitasi Nyeri KronisWegrimel AriegaraNo ratings yet
- 15hip TotalHipArthroplastyDocument4 pages15hip TotalHipArthroplastyudaysravsNo ratings yet
- Final Case Report - HarrisDocument25 pagesFinal Case Report - Harrisapi-621459006No ratings yet
- Hip ArthroplastyDocument29 pagesHip ArthroplastyAmiraa IbrahiimmNo ratings yet
- Determinants RESISTED EX'SDocument24 pagesDeterminants RESISTED EX'Svenkata ramakrishnaiahNo ratings yet
- Rehabilitacion LCADocument44 pagesRehabilitacion LCAsebafigueroa94No ratings yet
- The Whartons' Strength Book: Lower Body: Total Stability for Upper Legs, Hips, Trunk, Lower Legs, Ankles, and FeetFrom EverandThe Whartons' Strength Book: Lower Body: Total Stability for Upper Legs, Hips, Trunk, Lower Legs, Ankles, and FeetRating: 3 out of 5 stars3/5 (3)
- Dynamic Stretching: The Revolutionary New Warm-up Method to Improve Power, Performance and Range of MotionFrom EverandDynamic Stretching: The Revolutionary New Warm-up Method to Improve Power, Performance and Range of MotionRating: 5 out of 5 stars5/5 (1)
- The Whartons' Strength Book: Upper Body: Total Stability for Shoulders, Neck, Arm, Wrist, and ElbowFrom EverandThe Whartons' Strength Book: Upper Body: Total Stability for Shoulders, Neck, Arm, Wrist, and ElbowRating: 5 out of 5 stars5/5 (1)
- FinalcasereportcaudyDocument30 pagesFinalcasereportcaudyapi-519036866No ratings yet
- 634 InservicetnkDocument12 pages634 Inservicetnkapi-519036866No ratings yet
- Gradereport 1Document1 pageGradereport 1api-512622549No ratings yet
- FirstclinicalcpipdfDocument4 pagesFirstclinicalcpipdfapi-519036866No ratings yet
- Third Year Goals For Physical Therapy SchoolDocument1 pageThird Year Goals For Physical Therapy Schoolapi-519036866No ratings yet
- FallcpiDocument4 pagesFallcpiapi-519036866No ratings yet
- Gradereport 2019-20 FallDocument1 pageGradereport 2019-20 Fallapi-468018392No ratings yet
- BlscertificationDocument1 pageBlscertificationapi-519036866No ratings yet
- Gradereport 3Document1 pageGradereport 3api-512622549No ratings yet
- CertificateofcompletionDocument1 pageCertificateofcompletionapi-519036866No ratings yet
- Citi Training CertificateDocument1 pageCiti Training Certificateapi-337927842No ratings yet
- 645 Group 1 LitreviewDocument11 pages645 Group 1 Litreviewapi-519036866No ratings yet
- Cprcertthrough 2022Document1 pageCprcertthrough 2022api-519036866No ratings yet
- DatastewardshipDocument1 pageDatastewardshipapi-519036866No ratings yet
- 617 ObstructivediseaseDocument12 pages617 Obstructivediseaseapi-519036866No ratings yet
- 661 ArticlereviewDocument4 pages661 Articlereviewapi-519036866No ratings yet
- Ptgoalsforyear 2Document1 pagePtgoalsforyear 2api-519036866No ratings yet
- Spring 2020 GradereportDocument1 pageSpring 2020 Gradereportapi-512417124No ratings yet
- Summeryear 1 GradesDocument1 pageSummeryear 1 Gradesapi-519036866No ratings yet
- Ptschoolpersonalgoalsyear 1Document1 pagePtschoolpersonalgoalsyear 1api-519036866No ratings yet
- PTH 725 Research ProposalDocument7 pagesPTH 725 Research Proposalapi-519036866No ratings yet
- Fall 2019 GradereportDocument1 pageFall 2019 Gradereportapi-512417124No ratings yet
- Definition of Terms: Service RadiusDocument11 pagesDefinition of Terms: Service RadiusSamuel ValentineNo ratings yet
- The Impact of Computer Based Test On Senior Secondary School StudentsDocument46 pagesThe Impact of Computer Based Test On Senior Secondary School StudentsOrlanshilay100% (18)
- CV Dr. ErwadiDocument3 pagesCV Dr. ErwadiErwadi ErwadiNo ratings yet
- Tanishqa Jogani - TAPMIDocument3 pagesTanishqa Jogani - TAPMITanishqa JoganiNo ratings yet
- Health Insurance COMPANYDocument6 pagesHealth Insurance COMPANYWajid MalikNo ratings yet
- Cervantes, Ralph Raymond G. (Persuasive Speech (PIECE) - SPEECH 1)Document8 pagesCervantes, Ralph Raymond G. (Persuasive Speech (PIECE) - SPEECH 1)Ralph Raymond CervantesNo ratings yet
- KI Health 75th FinalDocument127 pagesKI Health 75th FinalChandrimaChatterjeeNo ratings yet
- Defining - Mental - Health - and - Mental - Illness by Sharon Leighton and Nisha DograDocument13 pagesDefining - Mental - Health - and - Mental - Illness by Sharon Leighton and Nisha DograGeorgi Limonov100% (1)
- Focusing in Clinical Practice The Essence of Chang... - (Chapter 1 The Essence of Change)Document19 pagesFocusing in Clinical Practice The Essence of Chang... - (Chapter 1 The Essence of Change)lemvanderburgNo ratings yet
- Memorix Anatomy 2Document1 pageMemorix Anatomy 2Sreedhar Tirunagari100% (1)
- TSCC SheettDocument2 pagesTSCC Sheettadriana martorell0% (1)
- 4.iJGP - Case ReportDocument4 pages4.iJGP - Case Reportpalak GandhiNo ratings yet
- 5 INGREDIENTS - EbookDocument14 pages5 INGREDIENTS - EbookHeuler KretliNo ratings yet
- TemplateDocument15 pagesTemplateJogie DalumpinesNo ratings yet
- Cross-Regional Statement On "Infodemic" in The Context of COVID-19Document3 pagesCross-Regional Statement On "Infodemic" in The Context of COVID-19dbersotNo ratings yet
- Construction Site Housekeeping ChecklistDocument3 pagesConstruction Site Housekeeping ChecklistMuhammad Zarul Aziri Bin MaamurNo ratings yet
- MicroSilver BG PDFDocument16 pagesMicroSilver BG PDFBoblea LaviniaNo ratings yet
- Sample Disaster Emergency Preparedness ManualDocument32 pagesSample Disaster Emergency Preparedness ManualAnn PerezNo ratings yet
- Colisage ProduitsDocument6 pagesColisage ProduitsBerriche MohamedNo ratings yet
- Improve Your Medication Management Processes: Advisory ServicesDocument2 pagesImprove Your Medication Management Processes: Advisory ServicesSimarpreet KaurNo ratings yet
- Working at Heights Translab and PBDocument1 pageWorking at Heights Translab and PBCIDI Avida Towers VergeNo ratings yet
- The Problem and Background of The StudyDocument6 pagesThe Problem and Background of The StudyAileen ElegadoNo ratings yet
- Method of Statement For GroutingDocument7 pagesMethod of Statement For GroutingCezar DasiNo ratings yet
- PareidoliaDocument7 pagesPareidoliamariaNo ratings yet
- Parent Child RelationshipDocument8 pagesParent Child RelationshipHUSSAINA BANONo ratings yet
- NRP - Lesson 1 Foundation NRPDocument21 pagesNRP - Lesson 1 Foundation NRPShariti DeviNo ratings yet
- Medical EthicsDocument3 pagesMedical EthicsJona MagudsNo ratings yet
- Chapter 10Document38 pagesChapter 10chindypermataNo ratings yet
- Red Cross CPR Guidelines PDFDocument31 pagesRed Cross CPR Guidelines PDFandrewh3No ratings yet
- HDFC ERGO General Insurance Company Limited: Claim Form - Part ADocument7 pagesHDFC ERGO General Insurance Company Limited: Claim Form - Part AchakshuNo ratings yet