Professional Documents
Culture Documents
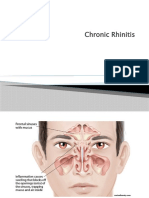
Chronic Nasal Conditions Guide
Uploaded by
Mohaaz Abdi0 ratings0% found this document useful (0 votes)
15 views15 pagesOriginal Title
Chronic Catarrhal Rhinitis
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
15 views15 pagesChronic Nasal Conditions Guide
Uploaded by
Mohaaz AbdiCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 15
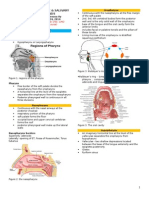
Chronic catarrhal rhinitis
Chronic catarrhal rhinitis
develops as a result of repeated acute rhinitis.
Prolonged congestive hyperemia of the nasal
mucosa caused by alcoholism, chronic disease
of the cardiovascular system, and kidneys
predisposes to the development of chronic
rhinitis. In these diseases, hereditary
preconditions, developmental defects,
violations of normal anatomical relationships,
causing difficulty in nasal breathing, are
significant. Chronic rhinitis also develops as a
secondary disease in the pathology of the
nasopharynx and paranasal sinuses.
Clinic
The symptoms of chronic catarrhal rhinitis are
generally similar to those of acute rhinitis, but are
much less intense. The patient complains of nasal
discharge of a mucous or mucopurulent nature.
Difficulty in nasal breathing increases (as does nasal
discharge) in the cold. Often there is an alternating
congestion in one of the halves of the nose. With
rhinoscopy, diffuse hyperemia of the mucous
membrane is determined, often with a cyanotic
shade. The inferior turbinates are moderately
swollen, narrowing the lumen of the common nasal
passage. Chronic catarrhal rhinitis may be
accompanied by hyposmia. A possible transition of
catarrhal inflammation from the nasal cavity to the
mucous membrane of the auditory tube with the
subsequent development of tubo-otitis
Diagnosis The diagnosis of the disease is established
on the basis of complaints, anamnesis, anterior and
posterior rhinoscopy. Differential diagnosis To
distinguish catarrhal chronic rhinitis from
hypertrophic, anemization of the mucous membrane is
performed with vasoconstrictor agents. A noticeable
contraction of the mucous membrane of the turbinates
indicates the absence of true hypertrophy
characteristic of hypertrophic rhinitis. Differential
diagnosis between false and true hypertrophy can be
performed using a bell-shaped probe.
In the case of false hypertrophy, the probe more easily
bends the mucous membrane to the bone wall. With
true hypertrophy, compacted tissue is determined,
which does not lend itself well to pressure exerted on
it.
Treatment
It is necessary to eliminate the unfavorable
factors that cause the development of chronic
rhinitis. It is useful to stay in a dry warm climate,
hydro and balneotherapy is indicated. Local
treatment consists in the use of antibacterial and
astringent drugs in the form of a 3-5% solution
of protargol (collargol), 0.25 - 0.5% solution of
zinc sulfate, 2% salicylic ointment, etc. UHF is
prescribed to the area nose, endonasally UFO
(tube-quartz). The prognosis is usually good.
Chronic hypertrophic rhinitis
The causes of hypertrophic rhinitis are the same as those
of catarrhal.
Clinic
Hypertrophic rhinitis is characterized by persistent nasal
congestion. Complicates nasal breathing and profuse
mucous and mucopurulent discharge. Due to obturation of
the olfactory gap, hyposmia occurs and then anosmia.
Subsequently, as a result of atrophy of the olfactory cells,
essential (irreversible) anosmia may occur. The timbre of
the voice in patients becomes nasal. As a result of the
compression of the lymph gaps by the fibrous tissue, the
lymph outflow from the cranial cavity is disrupted, which
causes the appearance of a feeling of heaviness in the
head, disability and sleep disturbance.
Treatment
Treatment of hypertrophic rhinitis is
predominantly surgical. If there is bone
hypertrophy of the turbinates, one of the
options for submucosal intervention is
performed. With limited hypertrophy of the
anterior and posterior ends of the inferior
turbinates or their lower edge, these areas
are excised (conchotomy).
conchotomy
Atrophic rhinitis (Ozaena)
Etiology
Hereditary factors: the disease runs in families.
Endocrine imbalance: the disease tends to start at
puberty and mostly involves females.
Racial factors: whites are more susceptible than
natives of equatorial Africa.
Nutritional deficiency: vitamins A or D, or iron.
Infection: Klebsiella ozaena.
Autoimmune factors: viral infection or some other
unidentified insult may trigger antigenicity of the
nasal mucosa.
Clinic
Nasal obstruction despite the roomy nasal cavity,
which can be caused either by the obstruction
produced by the discharge in the nose, or as a result
of sensory loss due to atrophy of nerves in the nose,
so the patient is unaware of the air flow.
Nasal discharge: greenish crusts with foul smelling,
though the patients may not be aware of this, because
the associated merciful anosmia.
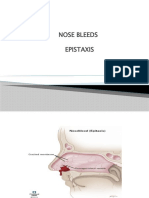
Epistaxis, may occur when the dried discharge (crusts)
are removed.
Hyposmia. Atrophic nasal mucosa and turbinates.
The nasal cavities become roomy and are filled with
foul smelling crusts.
treatment
Medical treatment:
Nasal irrigation and removal of crusts using alkaline
nasal solutions.
25% glucose in glycerin can be applied to the nasal
mucosa to inhibit the growth of proteolytic organisms
which produce foul smell.
Local antibiotic spray.
Estradiol spray for regeneration of seromucinous
glands.
Oral potassium iodide for liquefaction of secretion.
Placental extract injected in the submucosa.
Iron and vitamin A.
Surgical interventions:
Aims at narrowing of nasal cavity till the
mucosa regenerates.
Young's operation: Closure of the nasal cavity
affected with atrophic rhinitis by creating
mucocutaneous flaps (6m-2y). (Obsolete)
Submucosal augmentation using bone,
cartilage, or Teflon paste.
You might also like
- Acute and Chronic RhinitisDocument25 pagesAcute and Chronic RhinitisagniajolandaNo ratings yet
- Nasal Polyposis Slides 08042Document48 pagesNasal Polyposis Slides 08042Muhamad RizauddinNo ratings yet
- Nasal Obstruction BookDocument7 pagesNasal Obstruction BookChatradhar ChoudhuryNo ratings yet
- SinusitisDocument44 pagesSinusitisAmosNo ratings yet
- Treatment of Maxillary SinusitisDocument15 pagesTreatment of Maxillary SinusitisRabina PantaNo ratings yet
- OzaenaDocument4 pagesOzaenaArdi PratamaNo ratings yet
- Sistem Respirasi Sesak Napas: Problem Based LearningDocument61 pagesSistem Respirasi Sesak Napas: Problem Based LearningAkbar IskandarNo ratings yet
- Prof. DR .Mohamed Talaat EL - GhonemyDocument33 pagesProf. DR .Mohamed Talaat EL - Ghonemyadel madanyNo ratings yet
- 18 Tonsil, Adenoid Notes Cumming Abd Key Topics (New Moe)Document7 pages18 Tonsil, Adenoid Notes Cumming Abd Key Topics (New Moe)osamaeNo ratings yet
- Upper Respiratory AlterationDocument34 pagesUpper Respiratory AlterationJulia ManaloNo ratings yet
- Chronic Inflammation of Nose Leading to AtrophyDocument30 pagesChronic Inflammation of Nose Leading to AtrophysaleeNo ratings yet
- RespiratorydiseaseDocument13 pagesRespiratorydiseaseAJPEDO LIFENo ratings yet
- SINUSITISDocument45 pagesSINUSITISDevi DaryaningsihNo ratings yet
- Adenotonsillar Diseases DrbugnahDocument37 pagesAdenotonsillar Diseases DrbugnahDr.Sherif Bugnah100% (8)
- Pharyngeal Abscesses, Tonsillar and Adenoid InfectionsDocument36 pagesPharyngeal Abscesses, Tonsillar and Adenoid InfectionsRon Christian Neil RodriguezNo ratings yet
- Throat Pharynx Adenoids ENT LecturesDocument33 pagesThroat Pharynx Adenoids ENT LecturesRaju GangadharanNo ratings yet
- File 18584Document12 pagesFile 18584Mohammed MuthanaNo ratings yet
- Atrophic RhinitisDocument29 pagesAtrophic RhinitisProfit StreetNo ratings yet
- Respiratory Disorders ExplainedDocument89 pagesRespiratory Disorders ExplainedSyed MaazNo ratings yet
- PhysicsDocument29 pagesPhysicsPiryanka KumariNo ratings yet
- Maxillary SinusDocument43 pagesMaxillary SinusAli FalihNo ratings yet
- Maxillary SinusitisDocument28 pagesMaxillary SinusitisSumaNo ratings yet
- Li LBM 1 THT KL (Nallury)Document9 pagesLi LBM 1 THT KL (Nallury)Nallury Rizqi100% (1)
- Odontogenic Maxillary Sinusitis. Etiology, Anatomy, Pathogenesis, Classification, Clinical Picture, Diagnostics, Treatment and ComplicationsDocument36 pagesOdontogenic Maxillary Sinusitis. Etiology, Anatomy, Pathogenesis, Classification, Clinical Picture, Diagnostics, Treatment and ComplicationsАлександр ВолошанNo ratings yet
- NCM 113 Upper Respiratory DiseaseDocument68 pagesNCM 113 Upper Respiratory DiseaseJerah Aceron SatorreNo ratings yet
- Disorder of NoseDocument31 pagesDisorder of NoseSumit YadavNo ratings yet
- RHINOSINUSITIS: AN OVERVIEW OF PHYSIOLOGY, PATHOLOGY, CLINICAL PRESENTATION AND COMPLICATIONSDocument58 pagesRHINOSINUSITIS: AN OVERVIEW OF PHYSIOLOGY, PATHOLOGY, CLINICAL PRESENTATION AND COMPLICATIONSAnnisa AsdisyahNo ratings yet
- Tonsillectomy 200829131303Document102 pagesTonsillectomy 200829131303deptanaesaiimsgkpNo ratings yet
- Common Diseases of PharynxDocument72 pagesCommon Diseases of PharynxPinak DeNo ratings yet
- EPISTAXIS-bleeding From The Nose (Most Common) Etiology (Cause)Document34 pagesEPISTAXIS-bleeding From The Nose (Most Common) Etiology (Cause)Julliza Joy PandiNo ratings yet
- 1.0 Upper Airway InfectionsDocument45 pages1.0 Upper Airway InfectionsMariahNo ratings yet
- Disorder of ThroatDocument21 pagesDisorder of ThroatSumit YadavNo ratings yet
- 1.acute PharyngitisDocument88 pages1.acute PharyngitisIhsan Hanif0% (1)
- Chapter 22 Management of Patients With Upper Respiratory Tract DisordersDocument7 pagesChapter 22 Management of Patients With Upper Respiratory Tract DisordersPeej Reyes100% (2)
- Disorders of Middle EarDocument32 pagesDisorders of Middle EarAhmad fayazNo ratings yet
- Respiratorio PerrosDocument4 pagesRespiratorio PerrosErnesto Enriquez PozosNo ratings yet
- The Pharynx and Salivary GlandsDocument21 pagesThe Pharynx and Salivary GlandsAce Ashley BaronNo ratings yet
- EpistaxisDocument9 pagesEpistaxisAswathy RCNo ratings yet
- Acute and Chronic Upper Airway ConditionsDocument22 pagesAcute and Chronic Upper Airway ConditionsyuddNo ratings yet
- Lectures PPS Sinusitis - PpsDocument32 pagesLectures PPS Sinusitis - PpsAlfonso Molina RamirezNo ratings yet
- Diseases - of - The - Tonsil 2023Document41 pagesDiseases - of - The - Tonsil 2023dr MohammedNo ratings yet
- Upper Respiratory Infections: Symptoms and TreatmentsDocument45 pagesUpper Respiratory Infections: Symptoms and TreatmentsNatasha Abdulla100% (2)
- Definition: Anatomy:: Little's AreaDocument5 pagesDefinition: Anatomy:: Little's AreaFransisca YustikaNo ratings yet
- Laryngitis and Upper Airway ObstructionDocument9 pagesLaryngitis and Upper Airway Obstructionjonna casumpangNo ratings yet
- Anesthesia For Tonsillectomy: Aau-Chs School of AnesthesiaDocument54 pagesAnesthesia For Tonsillectomy: Aau-Chs School of AnesthesiaagatakassaNo ratings yet
- Uworld ENT NotesDocument4 pagesUworld ENT Notes808kailuaNo ratings yet
- Pediatric Nasopharyngeal Mass: Causes and ManagementDocument79 pagesPediatric Nasopharyngeal Mass: Causes and ManagementShahnawazNo ratings yet
- 14 Respiratory InfectionsDocument16 pages14 Respiratory InfectionsEsteban PrietoNo ratings yet
- Sinusitis 2 - New1Document48 pagesSinusitis 2 - New1neferpitouhoeNo ratings yet
- 2 RHINOLOGY SinusDocument87 pages2 RHINOLOGY SinusWai Kwong ChiuNo ratings yet
- Acute laryngitis causes, symptoms and treatmentDocument18 pagesAcute laryngitis causes, symptoms and treatmentROXTA RAHULNo ratings yet
- Anatomy Head Neck EMRCS MCQDocument23 pagesAnatomy Head Neck EMRCS MCQTowhid HasanNo ratings yet
- Retropharyngeal Abscess ReportDocument49 pagesRetropharyngeal Abscess ReportAyen FornollesNo ratings yet
- Chronic RhinosinusitisDocument8 pagesChronic RhinosinusitisYunardi Singgo100% (1)
- ASTHMADocument29 pagesASTHMAashoaib0313No ratings yet
- Acute Sinusitis Types and TreatmentsDocument11 pagesAcute Sinusitis Types and Treatmentsعبدالله فائز غلامNo ratings yet
- Class 2: 1. Signs and Symptoms of That Disease in Your PatientDocument4 pagesClass 2: 1. Signs and Symptoms of That Disease in Your Patientaayush upadhyayNo ratings yet
- Eent Mcq 266qzDocument13 pagesEent Mcq 266qzCosbyNo ratings yet
- A Review of Nasal Polyposis Arranged by Henni Juniati Siregar 71160891595Document20 pagesA Review of Nasal Polyposis Arranged by Henni Juniati Siregar 71160891595Divta AnimassariNo ratings yet
- Medical Mnemonic Sketches : Pulmonary DiseasesFrom EverandMedical Mnemonic Sketches : Pulmonary DiseasesNo ratings yet
- Recommendations For The Collection of Forensic Specimens Jul 22Document7 pagesRecommendations For The Collection of Forensic Specimens Jul 22Mohaaz AbdiNo ratings yet
- FME Form Suspect FSSC July 2021Document3 pagesFME Form Suspect FSSC July 2021Mohaaz AbdiNo ratings yet
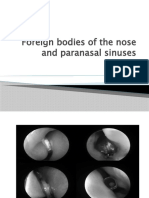
- Foreign Bodies of The Nose and Paranasal SinusesDocument8 pagesForeign Bodies of The Nose and Paranasal SinusesMohaaz AbdiNo ratings yet
- FME Form Complainant FSSC July 2021Document4 pagesFME Form Complainant FSSC July 2021Mohaaz AbdiNo ratings yet
- How to Stop a NosebleedDocument15 pagesHow to Stop a NosebleedMohaaz AbdiNo ratings yet
- RhinitisDocument15 pagesRhinitisMohaaz AbdiNo ratings yet
- EthmoiditisDocument11 pagesEthmoiditisMohaaz AbdiNo ratings yet
- OphthalmologyDocument21 pagesOphthalmologyPeterNo ratings yet
- BlidnessDocument13 pagesBlidnessMohaaz AbdiNo ratings yet
- CF Lecture 2Document8 pagesCF Lecture 2Maha KhanNo ratings yet
- Unfolding: By: Prof. Dr. Hardik Khamar M.D. (Hom.)Document6 pagesUnfolding: By: Prof. Dr. Hardik Khamar M.D. (Hom.)HomeoDr Babar AminNo ratings yet
- Communicable Disease ReviewerDocument18 pagesCommunicable Disease ReviewerMicah Jonah Elicaño100% (1)
- ENS Guide To Diagnosis & Management (v2 - 09.2016)Document37 pagesENS Guide To Diagnosis & Management (v2 - 09.2016)Renato Mondani0% (1)
- Day 15 - NCM-109 Children With Alteration in Oxygenation (A)Document50 pagesDay 15 - NCM-109 Children With Alteration in Oxygenation (A)Sheena Patricia ArasulaNo ratings yet
- Respiratory System 1Document186 pagesRespiratory System 1Ivann Chan MunarNo ratings yet
- Msds K2cro4 PDFDocument6 pagesMsds K2cro4 PDFAnonymous U0RczPNo ratings yet
- Acebrofilina PozziDocument10 pagesAcebrofilina PozziAgencia FaroNo ratings yet
- Respiratory DisordersDocument48 pagesRespiratory DisordersJean Cabigao100% (1)
- DR Raymond Bernard, Sex Desire ExplainedDocument3 pagesDR Raymond Bernard, Sex Desire ExplainedMeșterul ManoleNo ratings yet
- Acupressure PointsDocument15 pagesAcupressure PointsVeda Thakkar100% (2)
- Osha Training Toolbox Talk:: Biological Hazards - Common Signs and Symptoms of InfectionDocument3 pagesOsha Training Toolbox Talk:: Biological Hazards - Common Signs and Symptoms of InfectionMuhammad AwaisNo ratings yet
- Haematoxylon.: Action and Therapy.-A Mild, Unirritating Astringent and TonicDocument22 pagesHaematoxylon.: Action and Therapy.-A Mild, Unirritating Astringent and TonicDr Rushen Singh100% (1)
- Chronic Obstructive Pulmonary Disease Bronchitis Nursing Care PlansDocument10 pagesChronic Obstructive Pulmonary Disease Bronchitis Nursing Care Planscy belNo ratings yet
- Nursing ExamDocument11 pagesNursing ExamGunan DwynethNo ratings yet
- Antitussives and MucolyticsDocument1 pageAntitussives and MucolyticsArvin Bernardo QuejadaNo ratings yet
- Fish Diseases and Disorders Vol 1 - Protozoan and Metazoan InfectionsDocument801 pagesFish Diseases and Disorders Vol 1 - Protozoan and Metazoan Infectionsclaudiousdecastro100% (1)
- Biology 10 00095Document37 pagesBiology 10 00095Dayana CheriyanNo ratings yet
- Maxillary Sinus Anatomy and PathologyDocument15 pagesMaxillary Sinus Anatomy and PathologyRini RahmawulandariNo ratings yet
- Introduction To The Immune Response and InflammationDocument16 pagesIntroduction To The Immune Response and InflammationAlyssaGrandeMontimorNo ratings yet
- Arum TriphylumDocument13 pagesArum TriphylumShubhanshi BhasinNo ratings yet
- Promoting Activity Tolerance in a Patient with CoughDocument3 pagesPromoting Activity Tolerance in a Patient with CoughitsmeayaNo ratings yet
- Chapter 10 - Pathogens and ImmunityDocument79 pagesChapter 10 - Pathogens and ImmunityKareem DmourNo ratings yet
- New Microsoft Word DocumentDocument26 pagesNew Microsoft Word DocumentimtiazbscNo ratings yet
- Types of ImmunityDocument35 pagesTypes of ImmunityKailash NagarNo ratings yet
- Health Benefits of Guava JuiceDocument41 pagesHealth Benefits of Guava JuiceAiman IlhamNo ratings yet
- XAT-2008 1: Xavier Admission Test Practice PaperDocument27 pagesXAT-2008 1: Xavier Admission Test Practice PaperVenugopal ShettyNo ratings yet
- General Biology 2: Quarter 4: Week 4 - Module 1D PDocument25 pagesGeneral Biology 2: Quarter 4: Week 4 - Module 1D PSyrine Myles Sullivan100% (1)
- Cystic Fibrosis With Case StudyDocument27 pagesCystic Fibrosis With Case StudyAviva Tuteja100% (1)
- Nasal Irrigation - RachanonDocument2 pagesNasal Irrigation - RachanonShakritnat SakonNo ratings yet