Professional Documents
Culture Documents
How the female reproductive system works
Uploaded by
Joann Jacob0 ratings0% found this document useful (0 votes)
12 views29 pagesOriginal Title
Female Rep. system
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
12 views29 pagesHow the female reproductive system works
Uploaded by
Joann JacobCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 29
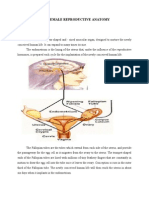
How does the female reproductive system work?
The female reproductive system provides several
functions. The ovaries produce the egg cells, called
the ova or oocytes. The oocytes are then transported to
the fallopian tube where fertilization by a sperm may
occur. The fertilized egg then moves to the uterus,
where the uterine lining has thickened in response to
the normal hormones of the reproductive cycle. Once
in the uterus, the fertilized egg can implant into
thickened uterine lining and continue to develop. If
implantation does not take place, the uterine lining is
shed as menstrual flow. In addition, the female
reproductive system produces female sex hormones
that maintain the reproductive cycle.
During menopause, the female reproductive system gradually
stops making the female hormones necessary for the
reproductive cycle to work. At this point, menstrual cycles can
become irregular and eventually stop. One year after menstrual
cycles stop, the woman is considered to be menopausal.
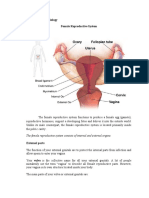
What parts make-up the female anatomy?
The female reproductive anatomy includes both external and
internal structures.
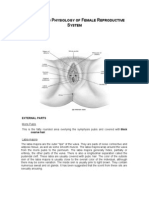
The function of the external female reproductive structures
(the genital) is twofold: To enable sperm to enter the body and
to protect the internal genital organs from infectious
organisms.
The main external structures of the female
reproductive system include:
LABIA MAJORA
The labia majora (“large lips”)
enclose and protect the other
external reproductive organs.
During puberty, hair growth occurs
on the skin of the labia majora,
which also contain sweat and oil-
secreting glands.
Labia minora
The labia minora (“small lips”) can have a variety
of sizes and shapes. They lie just inside the labia
majora, and surround the openings to the vagina
(the canal that joins the lower part of the uterus to
the outside of the body) and urethra (the tube that
carries urine from the bladder to the outside of the
body). This skin is very delicate and can become
easily irritated and swollen.
Bartholin’s glands
These glands are located next to the vaginal
opening on each side and produce a fluid
(mucus) secretion.
The Bartholin's glands (named after Thomas
Bartholin; also called Bartholin glands or
greater vestibular glands) are two pea sized
compound alveolar glands located slightly
posterior and to the left and right of the
opening of the vagina. They secrete mucus to
lubricate the vagina and are homologous to
bulbourethral glands in males.
Clitoris
The two labia minora meet at the
clitoris, a small, sensitive
protrusion that is comparable to
the penis in males. The clitoris is
covered by a fold of skin, called
the prepuce, which is similar to the
foreskin at the end of the penis.
Like the penis, the clitoris is very
sensitive to stimulation and can
become erect.
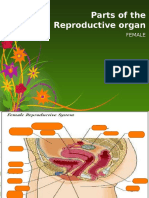
The internal reproductive organs include:
Vagina
The vagina is a canal that joins the cervix (the lower
part of uterus) to the outside of the body. It also is
known as the birth canal.
Uterus (womb)
The uterus is a hollow, pear-shaped
organ that is the home to a
developing fetus. The uterus is
divided into two parts: the cervix,
which is the lower part that opens
into the vagina, and the main body
of the uterus, called the corpus. The
corpus can easily expand to hold a
developing baby. A canal through
the cervix allows sperm to enter and
menstrual blood to exit.
Ovaries
The ovaries are small,
oval-shaped glands that are
located on either side of
the uterus. The ovaries
produce eggs and
hormones.
Fallopian tubes
These are narrow tubes that are attached to the
upper part of the uterus and serve as pathways
for the ova (egg cells) to travel from the ovaries
to the uterus. Fertilization of an egg by a sperm
normally occurs in the fallopian tubes. The
fertilized egg then moves to the uterus, where it
implants to the uterine lining.
What happens during the menstrual cycle?
Females of reproductive age (beginning anywhere from 11 to
16 years of age) experience cycles of hormonal activity that
repeat at about one-month intervals. Menstru means
"monthly” – leading to the term menstrual cycle. With every
cycle, a woman’s body prepares for a potential pregnancy,
whether or not that is the woman’s intention. The term
menstruation refers to the periodic shedding of the uterine
lining. Many women call the days that they notice vaginal
bleeding their “period,” “menstrual” or cycle.
The average menstrual cycle takes about 28 days and occurs in phases.
These phases include:
The follicular phase (development of the egg)
The ovulatory phase (release of the egg)
The luteal phase (hormone levels decrease if
the egg does not implant)
Follicular phase
The follicular phase starts on the first day of
menstruation and ends with ovulation. Prompted by
the hypothalamus, the pituitary gland releases follicle
stimulating hormone (FSH). This hormone stimulates
the ovary to produce around five to 20 follicles (tiny
nodules or cysts), which bead on the surface.
The follicular phase begins on the first day of menstrual
bleeding (day 1). But the main event in this phase is the
development of follicles in the ovaries.
At the beginning of the follicular phase, the lining of the
uterus (endometrium) is thick with fluids and nutrients
designed to nourish an embryo. If no egg has been
fertilized, estrogen and progesterone levels are low. As a
result, the top layers of the endometrium are shed, and
menstrual bleeding occurs.
About this time, the pituitary gland slightly increases
its production of follicle-stimulating hormone. This
hormone then stimulates the growth of 3 to 30
follicles. Each follicle contains an egg. Later in the
phase, as the level of this hormone decreases, only
one of these follicles (called the dominant follicle)
continues to grow. It soon begins to produce estrogen,
and the other stimulated follicles begin to break down.
The increasing estrogen also begins to prepare the
uterus and stimulates the luteinizing hormone surge.
On average, the follicular phase lasts about
13 or 14 days. Of the three phases, this
phase varies the most in length. It tends to
become shorter near menopause. This phase
ends when the level of luteinizing hormone
increases dramatically (surges). The surge
results in release of the egg (ovulation) and
marks the beginning of the next phase.
Ovulatory phase
The ovulatory phase begins with a surge in
luteinizing hormone and follicle-stimulating hormone
levels. Luteinizing hormone stimulates egg release
(ovulation), which usually occurs 16 to 32 hours after
the surge begins. The estrogen level decreases during
the surge, and the progesterone level starts to increase
The ovulatory phase begins when the level of luteinizing
hormone surges. Luteinizing hormone stimulates the dominant
follicle to bulge from the surface of the ovary and finally
rupture, releasing the egg. The level of follicle-stimulating
hormone increases to a lesser degree. The function of the
increase in follicle-stimulating hormone is not understood.
The ovulatory phase usually lasts 16 to 32 hours. It ends when
the egg is released, about 10 to 12 hours after the surge in the
level of luteinizing hormone. The egg can be fertilized for only
up to about 12 hours after its release.
The surge in luteinizing hormone can be
detected by measuring the level of this
hormone in urine. This measurement can be
used to determine when women are fertile.
Fertilization is more likely when sperm are
present in the reproductive tract before the
egg is released. Most pregnancies occur
when intercourse occurs within 3 days
before ovulation.
Around the time of ovulation, some women feel a dull
pain on one side of the lower abdomen. This pain is
known as mittelschmerz (literally, middle pain). The
pain may last for a few minutes to a few hours. The
pain is usually felt on the same side as the ovary that
released the egg, but the precise cause of the pain is
unknown. The pain may precede or follow the rupture
of the follicle and may not occur in all cycles.
Egg release does not alternate between the two ovaries
and appears to be random. If one ovary is removed, the
remaining ovary releases an egg every month.
The luteal phase
The luteal phase begins after ovulation. It lasts about 14 days
(unless fertilization occurs) and ends just before a menstrual
period.
In this phase, the ruptured follicle closes after releasing the
egg and forms a structure called a corpus luteum, which
produces increasing quantities of progesterone. The
progesterone produced by the corpus luteum does the
following:
Prepares the uterus in case an embryo is implanted
Causes the endometrium to thicken, filling with fluids and
nutrients to nourish a potential embryo
Causes the mucus in the cervix to thicken, so that sperm or
bacteria are less likely to enter the uterus
Causes body temperature to increase slightly during the luteal
phase and remain elevated until a menstrual period begins
(this increase in temperature can be used to estimate whether
ovulation has occurred)
During most of the luteal phase, the estrogen level is high.
Estrogen also stimulates the endometrium to thicken.
The increase in estrogen and progesterone levels causes milk
ducts in the breasts to widen (dilate). As a result, the breasts
may swell and become tender.
If the egg is not fertilized or if the fertilized egg does not
implant, the corpus luteum degenerates after 14 days, levels
of estrogen and progesterone decrease, and a new menstrual
cycle begins.
If the embryo is implanted, the cells around the developing
embryo begin to produce a hormone called human chorionic
gonadotropin. This hormone maintains the corpus luteum,
which continues to produce progesterone, until the growing
fetus can produce its own hormones. Pregnancy tests are
based on detecting an increase in the human chorionic
gonadotropin level.
How many eggs does a woman have?
During fetal life, there are about 6 million to 7 million
eggs. From this time, no new eggs are produced. At
birth, there are approximately 1 million eggs; and by
the time of puberty, only about 300,000 remain. Of
these, only 300 to 400 will be ovulated during a
woman's reproductive lifetime. Fertility can drop as a
woman ages due to decreasing number and quality of
the remaining eggs.
You might also like
- Parent and ChildDocument288 pagesParent and ChildMinisterNo ratings yet
- FEMALE REPRODUCTIVE ORGANSDocument5 pagesFEMALE REPRODUCTIVE ORGANSYanie ZsofNo ratings yet
- Reproductive System Powerpoint LectureDocument55 pagesReproductive System Powerpoint LectureJames DaurayNo ratings yet
- How to Read a CTGDocument12 pagesHow to Read a CTGyehezkieldward100% (1)
- The Menstrual Cycle PDFDocument6 pagesThe Menstrual Cycle PDFPerry Sin100% (1)
- Female Reproductive System ExplainedDocument17 pagesFemale Reproductive System ExplainedJasmaine RivoNo ratings yet
- Orgasmic Invocation by Rev Maskim XulDocument1 pageOrgasmic Invocation by Rev Maskim XulAnaYoshime11No ratings yet
- Exposing The Myth ofDocument7 pagesExposing The Myth ofnowayborngay0% (1)
- Processes of The Female Reproductive SystemDocument40 pagesProcesses of The Female Reproductive SystemPristine AlbayNo ratings yet
- Crop Science 1V Lecture NotesDocument167 pagesCrop Science 1V Lecture NotesJoann JacobNo ratings yet
- Western Schools of Philosophy: Idealism, Realism, PragmatismDocument94 pagesWestern Schools of Philosophy: Idealism, Realism, PragmatismJoann JacobNo ratings yet
- Western Schools of Philosophy: Idealism, Realism, PragmatismDocument94 pagesWestern Schools of Philosophy: Idealism, Realism, PragmatismJoann JacobNo ratings yet
- Cdi 5 PresentationDocument108 pagesCdi 5 PresentationJoann JacobNo ratings yet
- Human Reproduction in 12 WordsDocument16 pagesHuman Reproduction in 12 Wordsprince matamboNo ratings yet
- Reproductive SystemDocument89 pagesReproductive SystemIbrahim Mahmoud Ali100% (1)
- Female Reproductive System, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandFemale Reproductive System, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Anatomy and Physiology of Female Reproductive SystemDocument6 pagesAnatomy and Physiology of Female Reproductive SystemFarlyn Real MoralesNo ratings yet
- Parts of The Reproductive OrganDocument64 pagesParts of The Reproductive OrganFrancez Anne GuanzonNo ratings yet
- Preconception CareDocument30 pagesPreconception CareShani Jyothis100% (2)
- Sociology and EducationDocument16 pagesSociology and EducationJoann JacobNo ratings yet
- HORMONAL CYCLE EXPLAINEDDocument20 pagesHORMONAL CYCLE EXPLAINEDGunaNo ratings yet
- Attitudes Towards Profession, Teaching Strategies, Teacher Indirectness and Classroom PerformanceDocument24 pagesAttitudes Towards Profession, Teaching Strategies, Teacher Indirectness and Classroom PerformanceJoann Jacob100% (1)
- RPRHDocument39 pagesRPRHCassyDelaRosaNo ratings yet
- Antenatal PreparationDocument26 pagesAntenatal Preparationvaishali TMU studentNo ratings yet
- Abortion PP TDocument42 pagesAbortion PP TDivya ToppoNo ratings yet
- UNCLOS PresentationDocument24 pagesUNCLOS PresentationJoann JacobNo ratings yet
- Maternal and Child QuestionsDocument13 pagesMaternal and Child Questionsnursejoy100% (3)
- SG 10 Female Reproductive SystemDocument4 pagesSG 10 Female Reproductive SystemBernice OrtegaNo ratings yet
- The Female Reproductive System How Does The Female Reproductive System Work?Document4 pagesThe Female Reproductive System How Does The Female Reproductive System Work?Noella MenesesNo ratings yet
- The Female Reproductive System Is Designed To Carry Out Several FunctionsDocument2 pagesThe Female Reproductive System Is Designed To Carry Out Several FunctionsArdie MingayNo ratings yet
- Female Reproductive Anatomy and Menstrual Cycle ExplainedDocument3 pagesFemale Reproductive Anatomy and Menstrual Cycle ExplainedRinoa Raine PayumoNo ratings yet
- FEMALE-REPRODUCTIVE-SYSTEMDocument9 pagesFEMALE-REPRODUCTIVE-SYSTEMbyata pausanosNo ratings yet
- Your Guide to the Female Reproductive System Explained <40Document17 pagesYour Guide to the Female Reproductive System Explained <40Nas Rudy HamzahNo ratings yet
- Anatomy and Physiology of The Female Reproductive SystemDocument8 pagesAnatomy and Physiology of The Female Reproductive Systemaye ayENo ratings yet
- 07.writing - Membuat Bahan AjarDocument8 pages07.writing - Membuat Bahan AjarHanna HannaNo ratings yet
- Sexual and Reproductive Health RightsDocument44 pagesSexual and Reproductive Health RightsAYO NELSONNo ratings yet
- Dekey Biology ProjectDocument12 pagesDekey Biology ProjecttseringchondenmakhamNo ratings yet
- Intro To Pregnancy LVL 1Document34 pagesIntro To Pregnancy LVL 1Helene NketchouaNo ratings yet
- Female Reproductive SystemDocument6 pagesFemale Reproductive SystemRodelyn Dahay CalluengNo ratings yet
- What Is Reproduction?: Male Reproductive System GenesDocument4 pagesWhat Is Reproduction?: Male Reproductive System GenesPrada Maya AnggariNo ratings yet
- Female Reproductive SystemDocument4 pagesFemale Reproductive SystemDeepak VermaNo ratings yet
- Producing Gametes and the Menstrual CycleDocument7 pagesProducing Gametes and the Menstrual CycleRichard GrayNo ratings yet
- Female Reproductive SystemDocument4 pagesFemale Reproductive SystemDeepak VermaNo ratings yet
- Human Reproductive SystemDocument3 pagesHuman Reproductive SystemAltheaNo ratings yet
- What the Female Reproductive System Does (39Document11 pagesWhat the Female Reproductive System Does (39MarianaNo ratings yet
- Female Reproductive Anatomy GuideDocument9 pagesFemale Reproductive Anatomy GuidePinkeyinthecityNo ratings yet
- Female Reproductive SystemDocument7 pagesFemale Reproductive SystemKomail SrnNo ratings yet
- Anatomy and PhysiologyDocument5 pagesAnatomy and PhysiologytwicetrashNo ratings yet
- Female Reproductive System FunctionsDocument27 pagesFemale Reproductive System FunctionsbobNo ratings yet
- Vagina:: Female Reproductive System (Human), Details ..Document8 pagesVagina:: Female Reproductive System (Human), Details ..Giovanni CeneriniNo ratings yet
- Female Reproductive SystemDocument7 pagesFemale Reproductive SystemStudent NurseNo ratings yet
- Reproductive System: Renthel R. Cueto Bsabe - 1ADocument5 pagesReproductive System: Renthel R. Cueto Bsabe - 1ARenthel CuetoNo ratings yet
- How Does The Female Reproductive System Work?Document6 pagesHow Does The Female Reproductive System Work?Samlie BarengNo ratings yet
- Female Reproductive SystemDocument28 pagesFemale Reproductive System1-LUMALANG Ashley Anne A.No ratings yet
- Menstrual CycleDocument2 pagesMenstrual CycleWan SarimiNo ratings yet
- Menstrual Cycle Biology ProjectDocument4 pagesMenstrual Cycle Biology ProjectaddyNo ratings yet
- FemrepnotesDocument38 pagesFemrepnotesLibi FarrellNo ratings yet
- Reproduction & Growth CycleDocument96 pagesReproduction & Growth Cyclebiologi88No ratings yet
- The Menstrual Cycle TranskipDocument5 pagesThe Menstrual Cycle Transkiplen lehangNo ratings yet
- 10FRSDocument27 pages10FRSWakanda ForeverNo ratings yet
- 1 Normal Ob (Menstrual Cycle) : Glora P. de Leon, RN, RM, ManDocument75 pages1 Normal Ob (Menstrual Cycle) : Glora P. de Leon, RN, RM, ManJoan VillafrancaNo ratings yet
- Female Reproduction11Document4 pagesFemale Reproduction11Cyber.HNo ratings yet
- TranscriptDocument3 pagesTranscriptapi-400463992No ratings yet
- Reviewer in ScienceDocument24 pagesReviewer in ScienceBye Not thisNo ratings yet
- Terms and DefinitionsDocument4 pagesTerms and DefinitionsAdaha AngelNo ratings yet
- Anatomy and Physiology OvaryDocument6 pagesAnatomy and Physiology OvaryFretchell Aripal MontesNo ratings yet
- The Female Reproductive System Is A Group of Organs That Work Together To Enable ReproductionDocument5 pagesThe Female Reproductive System Is A Group of Organs That Work Together To Enable ReproductionNica Gobaliza EsquilonaNo ratings yet
- Reproductive Cycles in MammalsDocument9 pagesReproductive Cycles in MammalsSeemal shahidNo ratings yet
- The-Female-Repr-WPS-Office_011337Document17 pagesThe-Female-Repr-WPS-Office_011337tefzychiNo ratings yet
- Menstrual CycleDocument4 pagesMenstrual CycleIce-ice Valencia-SulaikNo ratings yet
- The Reproductive SystemDocument7 pagesThe Reproductive SystemAndri SusantoNo ratings yet
- Understanding the Menstrual CycleDocument2 pagesUnderstanding the Menstrual CycleShekinah MaeNo ratings yet
- Physiology of Female Reproductive System The Ovarian CycleDocument9 pagesPhysiology of Female Reproductive System The Ovarian CycleAmiraah MasriNo ratings yet
- Reproductive SystemDocument13 pagesReproductive SystemAlicia ValverdeNo ratings yet
- Sexual Reproduction in Humans PDF NotesDocument61 pagesSexual Reproduction in Humans PDF NotesANWESHA BALNo ratings yet
- Sci LectureDocument3 pagesSci LectureDenver Ghen V. GamutanNo ratings yet
- Climate Change Impact SolutionsDocument20 pagesClimate Change Impact SolutionsJoann JacobNo ratings yet
- TM 1 - SyllabusDocument12 pagesTM 1 - SyllabusJoann JacobNo ratings yet
- College of Agriculture and ForestryDocument17 pagesCollege of Agriculture and ForestryJoann JacobNo ratings yet
- Schoolcommunitypartnership 141021024403 Conversion Gate01Document31 pagesSchoolcommunitypartnership 141021024403 Conversion Gate01Joann JacobNo ratings yet
- CROP SCIENCE 1 Lab ActivityDocument4 pagesCROP SCIENCE 1 Lab ActivityJoann JacobNo ratings yet
- School Culture: Shaping Beliefs and PracticesDocument30 pagesSchool Culture: Shaping Beliefs and PracticesJoann JacobNo ratings yet
- Sexual SelfDocument11 pagesSexual SelfJoann JacobNo ratings yet
- Agri 15 Bsa Water MNG'T and IrrigationDocument27 pagesAgri 15 Bsa Water MNG'T and IrrigationJoann JacobNo ratings yet
- Sexual SelfDocument11 pagesSexual SelfJoann JacobNo ratings yet
- Theories of Learning: Pavlov, Skinner & BanduraDocument48 pagesTheories of Learning: Pavlov, Skinner & BanduraJoann JacobNo ratings yet
- United-Nations-Convention-on-the-Law-of-the-Sea - For MergeDocument16 pagesUnited-Nations-Convention-on-the-Law-of-the-Sea - For MergeJoann JacobNo ratings yet
- Understanding the Rizal Law Legislative ProcessDocument34 pagesUnderstanding the Rizal Law Legislative ProcessJoann JacobNo ratings yet
- Presented By: Raizza CorpuzDocument30 pagesPresented By: Raizza CorpuzJoann JacobNo ratings yet
- Relationship of Education and Psychology: Presented byDocument41 pagesRelationship of Education and Psychology: Presented byJoann JacobNo ratings yet
- Presented By: Raizza CorpuzDocument30 pagesPresented By: Raizza CorpuzJoann JacobNo ratings yet
- Relativism: A Presentation On Supporters and Dissenters by Zenon LysDocument18 pagesRelativism: A Presentation On Supporters and Dissenters by Zenon LysJoann JacobNo ratings yet
- The National Birth Center Study IIDocument12 pagesThe National Birth Center Study IIapi-38108107No ratings yet
- First Summative Test Science 5Document3 pagesFirst Summative Test Science 5Gil Arriola100% (2)
- Case Study (Summer)Document30 pagesCase Study (Summer)dave del rosarioNo ratings yet
- Men As Success Objects and Women As Sex ObjectsDocument6 pagesMen As Success Objects and Women As Sex ObjectsAvnika SethiNo ratings yet
- Understanding Reproductive Endocrinology UnderstandingDocument3 pagesUnderstanding Reproductive Endocrinology Understandingdivya maniNo ratings yet
- Pil 50 IDocument6 pagesPil 50 IKiran kumarNo ratings yet
- Kinship, marriage and household typesDocument3 pagesKinship, marriage and household typesDan Gabriel LacernaNo ratings yet
- Technical Notes Community Health NursingDocument8 pagesTechnical Notes Community Health NursingMary JoyNo ratings yet
- Vaginal Birth After Cesarean Delivery (VBAC) Definition/AbbreviationDocument3 pagesVaginal Birth After Cesarean Delivery (VBAC) Definition/AbbreviationCalvin TranNo ratings yet
- What Is The Process of Becoming A SurrogateDocument2 pagesWhat Is The Process of Becoming A SurrogateEva HospitalNo ratings yet
- Polygamy BrochureDocument2 pagesPolygamy BrochurecalvinhanggNo ratings yet
- Human Sexuality CSL650 Reaction PaperDocument9 pagesHuman Sexuality CSL650 Reaction PaperTe-Erika50% (2)
- Information About Uterine Fibroids From The Royal Free Hospital, London, UKDocument151 pagesInformation About Uterine Fibroids From The Royal Free Hospital, London, UKHarith NaharNo ratings yet
- Evaluation of Primigravida in Labour Using Modified WHO Partograph: Comparative Study of 100 CasesDocument6 pagesEvaluation of Primigravida in Labour Using Modified WHO Partograph: Comparative Study of 100 CasesShobhitNo ratings yet
- Menopause Daftar PustakaDocument3 pagesMenopause Daftar PustakaMuhammad Izzuddin Abdul JalilNo ratings yet
- MGM Bill Tri-Fold BrochureDocument2 pagesMGM Bill Tri-Fold BrochureMatthew Hess100% (1)
- TEAS, DHEA, CoQ10, and GH For Poor Ovarian Response Undergoing IVF-ET: A Systematic Review and Network Meta-AnalysisDocument12 pagesTEAS, DHEA, CoQ10, and GH For Poor Ovarian Response Undergoing IVF-ET: A Systematic Review and Network Meta-AnalysisiremcoskuntanNo ratings yet
- Anth 13 2 131 11 679 Mushtaq S TTDocument5 pagesAnth 13 2 131 11 679 Mushtaq S TTchie_8866No ratings yet
- Abstract Presentation: Anna Ravendran and Kate Burry of Family Planning New Zealand (SRHR in Rural Vanuatu: Knowledge, Access and Barriers)Document14 pagesAbstract Presentation: Anna Ravendran and Kate Burry of Family Planning New Zealand (SRHR in Rural Vanuatu: Knowledge, Access and Barriers)bobbyramakantNo ratings yet
- REPASO Parte3Document25 pagesREPASO Parte3B Mobile T5No ratings yet
- All India Institute of Medical Sciences Nagpur Department of Obstetrics and GynecologyDocument19 pagesAll India Institute of Medical Sciences Nagpur Department of Obstetrics and GynecologySugan GavaskarNo ratings yet