Professional Documents
Culture Documents
Peptic Ulcer Disease (Pud)
Uploaded by
nanjegovictoria0 ratings0% found this document useful (0 votes)
2 views19 pagesPeptic ulcer disease is caused by erosion of the gastrointestinal mucosa by gastric acid and pepsin, usually occurring in the stomach or duodenum. Ulcers are typically classified based on location and chronicity. Helicobacter pylori infection is the leading cause of peptic ulcers. Treatment involves antibiotic therapy to eradicate H. pylori along with acid suppression medications. Surgical intervention may be required for complications like bleeding, perforation or obstruction.
Original Description:
Surgery
Original Title
PEPTIC ULCER DISEASE (PUD)
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentPeptic ulcer disease is caused by erosion of the gastrointestinal mucosa by gastric acid and pepsin, usually occurring in the stomach or duodenum. Ulcers are typically classified based on location and chronicity. Helicobacter pylori infection is the leading cause of peptic ulcers. Treatment involves antibiotic therapy to eradicate H. pylori along with acid suppression medications. Surgical intervention may be required for complications like bleeding, perforation or obstruction.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
2 views19 pagesPeptic Ulcer Disease (Pud)
Uploaded by
nanjegovictoriaPeptic ulcer disease is caused by erosion of the gastrointestinal mucosa by gastric acid and pepsin, usually occurring in the stomach or duodenum. Ulcers are typically classified based on location and chronicity. Helicobacter pylori infection is the leading cause of peptic ulcers. Treatment involves antibiotic therapy to eradicate H. pylori along with acid suppression medications. Surgical intervention may be required for complications like bleeding, perforation or obstruction.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 19
CLINICAL CORRALATION
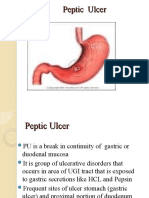
PEPTIC ULCER
•Is an erosion of the gastro intestinal
mucosa/sub-mucosa resulting from the digestive
action of HCI and pepsin
•A non – malignant ulcer in those parts of the
digestive tract in contact with gastric secretions.
Usually in the lower oesophagus, stomach,
duodenum and margin of gastrojejunal
anastomosis after surgical procedure.
Classification
• According to location:- gastric or duodenal
• According to degree of mucosal involvement (severity)
• Acute ulcer is associated with superficial erosion and
minimal inflammation. Its of short duration and resolves
quickly when the cause is identified and removed.
• Chronic Ulcer:- Is one of long duration, eroding throuth
the muscular wall with formation of firous tissue.
• Its present continuously for many months or
intermittently through out the person’s life time. Chronic
ulcer is at least 4 times as common as a cute ulcer.
AETIOLOGY
• Infection by Helicobacter pylori (70% of all
duodenal ulcers and 50% of gastric ulcers). It’s a
gram negative motile organism which sits just
behind the mucous layers of the stomach and
duodenum.
• It produces enzyme urase, which converts urea into
ammonia which is alkaline and combines the
hydrogen ions to ensures that environment is
alkaline and favourable for its survival.
• NH3 + H⁺ NH4⁺
• It also stimulates the gastric cells in the antrum of the
stomach to secrete gastrin which stimulates the parietal cells
to produce histamine which binds to his tamine receptors
and hence stimulate the H⁺K⁺-ATpase pump causing
secretion of H⁺ into the lumen of the stomach in exchange
for K⁺ that are secreted into the parietal cell.H+ later causes
destruction of the mucosa of the stomach
• The H⁺ Pylori also inhibits the D.Cells to release
somatostatin. Somatostatin antagonizes the action of gastrin,
this leads to excessive secretion of H⁺ by the un antagonised
gastrin cells therefore causing excessive destruction of the
mucosa.
K⁺ H⁺
ATP
K⁺ H⁺- K⁺- ATpase Pump
Drugs
• Nsaids e.g. Aspirin
They prevent production of prostaglandins necessary for
formation of the mucus in the stomach and duodenum and
production of bicarbonates.
Corticosteroids reduce the rate of mucosal renewal
Arachidonic acid
-Lipo-oxygenase
Phospholipids
-Cyclo-oxygenase NSAIDS
inhibit
Prostoglandins
• Stress – Increased amount of stress leads to
decrease in the production of prostaglandins
• Zollinger – Ellison syndrome. Symptoms,
include hypergastrineamia, severe peptic
ulceration from gastrinoma.
• Burns – cause stress e.g. curling uclers.
PATHOPHY SIOLOGY
• The integrity of the gastric mucosa is maintained when a
balance exists between the acid – secreting functions and
mucosal protective functions of the stomach and duodenum.
• The stomach is normally protected from autodigestion by
gastric mucosal barrier. When the barrier is broken, HCI
freely enters the mucosa and causes injury to the tissues.
This results in cellular destruction and inflammation. His
tamine is released from the damaged mucosa resulting in
vosodilation and increased in vasodilation and increased
capillary permeability.
• The release of histamine is then capable of stimulating
further secretion of acid and pepsin.
Clinical Presentation
• Gastric ulcer;
• Pain; dull epigastric, located near midline, gets worse on feeding
or relieved by vomiting
• Reflux of gastric, contents into esophagus causes heart burn,
cough from aspiration, expectoration of chyme
• Common in younger individuals others; Anorexia, nansea &
vomiting
• Hematemesis; vomiting of blood, coffee – ground emesis,
reflects slow bleeding; bright –red emesis implies rapid bleeding
• Melena
• Signs of anaemia i.e. Ulcer are bleeding
Summary
• Tripple therapy
• Omeprazole + Amoxicillin + Metronidazole 20mg od. 500mg 8⁰hly.
400mg 8⁰hly for at least 2 weeks
Diet
• eat 3 balanced meals a day
• eat slowly and chew food thoroughly
• do not over eat
• avoid any foods that increase discomfort e.g. fizzy drinks like soda,
fatty, oily food.
• Avoid bed time snacking because it increases night time acid secretion
• Stress reduction
• Surgical management
Indication
• Intractibility; failure of the ulcer to heal or
recurrence after therapy
• History of haemorrhage during RX
• Multiple ulcers
• Possible existence of malignant ulcer
• Gastric outlet obstruction
• Partial Gastrectomy with removal of the distal
2/3 of the stomach and anastomosis of gastric
stump to the duodenum is called
gastroduodenostomy (Billroth’s Operation)
• Gastro-jejunostomy (Billroth’s II operation)
• Vagotomy
Duodenal Ulcer
• Pain; epigastric location near midline, may
radiate around costal border to back.
• Pain is described as gnawing, burning, aching,
episodic in nature lasting between 30 mins to
2 hours. Worsened on starvation and relieved
by feedng
• Weight gain
• Common in elderly
Diagnosis
• History + physical examination
• Fibroptic endoscopy
• Upper GI barium contrast
• H- Pylori testing of blood, stool
• Urine, breath
• CBC, Biopsy, LFYs etc.
Management
• Medical regimen consists of adequate rest,
dietary modifications, medications,
elimination of smoking and long term follow
up.
Medication
• Anticids to neutralise free Hcl to prevent irritation
and permit mucosal healing e.g. magnesium
trisilicate either tablets or syrup
• Histamine (H₂) receptor blockers e.g. (cemetidine,
Ranitidine, famotidine.
• Proton pump inhibitor e.g. omeprazole lan soprazole
• Anti biotics e.g. amoxicillin, metrondozole,
clarithromycin
• Mucosal protective agents e.g. misoprosol
Complications of PUD
• Gastric outlet obstruction (Ulcers heal by
fibrosis) sign and symptoms include; vomiting
after feeds, food vomited even after 24 hours
is easily identified.
• Gastric perforation; common in the lesser
curvature of the stomach
Dsis: Usually known PUD patient
• Sudden on set of constant, generalised abdominal pain
• Shortness of breath (diaphragmatic irritation)
• Abdominal tenderness, rigidity, guarding
• Signs and symptoms of hypovolaemic shock
• Air under diaphragm on plain erect abdominal x-ray
(80% of cases)
• Positive fluid aspiration
• Gastric tumor; usually formed by chronic ulcers
• Bleeding;hematemesis
You might also like
- Alteration in Elimination BowelDocument140 pagesAlteration in Elimination BowelBayu Kxiikdx Lskd100% (1)
- Necrotizing Sialometaplasia of The Palate: A Case Report: Ashwarya Trivedi, Mysore K Sunil, Sonam Gupta, Shaveta GargDocument4 pagesNecrotizing Sialometaplasia of The Palate: A Case Report: Ashwarya Trivedi, Mysore K Sunil, Sonam Gupta, Shaveta Gargandrianiputri916No ratings yet
- Stomach &duodenumDocument89 pagesStomach &duodenumj6r4qvkrkzNo ratings yet
- Peptic UlcerDocument34 pagesPeptic UlcerAnjum AbbasiNo ratings yet
- Presentation On Gastric Ulcer-1Document37 pagesPresentation On Gastric Ulcer-1Roshan GhimireNo ratings yet
- Lecture 1part 2Document50 pagesLecture 1part 2mashe1No ratings yet
- Peptic UlcerDocument20 pagesPeptic UlcerSINDHOOR S MNo ratings yet
- GERDDocument20 pagesGERDSINDHOOR S MNo ratings yet
- Peptic Ulcer Disease: by Aniedu, UgochukwuDocument32 pagesPeptic Ulcer Disease: by Aniedu, UgochukwuManish Sapkota100% (1)
- Acute Gastritis CiciDocument43 pagesAcute Gastritis CiciDwi Rezky AmaliaNo ratings yet
- Gastrointestinal DrugsDocument29 pagesGastrointestinal DrugsSyed Ali Faizan NaqviNo ratings yet
- Disorders of Stomach and IntestineDocument64 pagesDisorders of Stomach and IntestineAyomide IgeNo ratings yet
- Gastroesophageal Reflux Disease Gerd 1Document62 pagesGastroesophageal Reflux Disease Gerd 1Kimverly Paredes GallanoNo ratings yet
- Peptic Ulcer Muhammad Aurangzeb Institute of Nursing Sciences Khyber Medical UniversityDocument28 pagesPeptic Ulcer Muhammad Aurangzeb Institute of Nursing Sciences Khyber Medical UniversityManish SapkotaNo ratings yet
- Student Copy of Gastrointestinal Problems SP 2010 IggyDocument80 pagesStudent Copy of Gastrointestinal Problems SP 2010 IggyJade CentinoNo ratings yet
- Pemicu 2: Mudita Dewi 405150016Document43 pagesPemicu 2: Mudita Dewi 405150016Mudita DewiNo ratings yet
- Esophagi T IsDocument30 pagesEsophagi T Iskanza MughalNo ratings yet
- 2 CARE OF CLIENTS GERD HIATAL HERNIA ACHALASIA PUD GI BLEEDING FinalDocument114 pages2 CARE OF CLIENTS GERD HIATAL HERNIA ACHALASIA PUD GI BLEEDING Finalevren yilmazNo ratings yet
- DIVERTICULOSISDocument23 pagesDIVERTICULOSISRashmita DahalNo ratings yet
- Gastrointestinal Bleeding: Dr. Isbandiyah, SPPD FK UmmDocument25 pagesGastrointestinal Bleeding: Dr. Isbandiyah, SPPD FK Ummikaummu amaliahNo ratings yet
- The Digestive System: and ItsDocument102 pagesThe Digestive System: and ItsRhea Andrea Uy100% (1)
- K11 Bedah EsofagusDocument37 pagesK11 Bedah EsofagusenriNo ratings yet
- Peptic Ulcer DiseaseDocument6 pagesPeptic Ulcer DiseaseNispap Harami RJNo ratings yet
- Bio 253 MidtermDocument17 pagesBio 253 MidtermJason ChuNo ratings yet
- Nur 322 Gi DisordersDocument113 pagesNur 322 Gi DisordersLovelights ZamoraNo ratings yet
- HIATAL HERNIA PPT Final PDFDocument49 pagesHIATAL HERNIA PPT Final PDFregysujit60% (5)
- Hiatal Hernia AchalasiaDocument22 pagesHiatal Hernia AchalasiaDhen MarcNo ratings yet
- Peptic Ulcer Disease: Dr. Haji Bahadar Pharmd, PHD Assistant Professor Khyber Medical University-PeshawarDocument24 pagesPeptic Ulcer Disease: Dr. Haji Bahadar Pharmd, PHD Assistant Professor Khyber Medical University-Peshawarms khan100% (1)
- Gi NclexDocument14 pagesGi NclexYoke W Khoo100% (3)
- Wa0016.Document176 pagesWa0016.Sreeja ReddyNo ratings yet
- Management of Upper GI BleedingDocument70 pagesManagement of Upper GI BleedingaboubakarylwabukobaNo ratings yet
- Digestive SystemDocument53 pagesDigestive SystemEra CaridoNo ratings yet
- Assessment and Management of Patients With Biliary DisorderDocument50 pagesAssessment and Management of Patients With Biliary DisorderZanida ZainonNo ratings yet
- INTESTINEDocument98 pagesINTESTINEDeepika LingamNo ratings yet
- Pancreatitis: Def Pancreatitis (Inflammation of The Pancreas) Is A Serious Disorder. The Most Basic Classification SystemDocument5 pagesPancreatitis: Def Pancreatitis (Inflammation of The Pancreas) Is A Serious Disorder. The Most Basic Classification SystemSanthu Su100% (2)
- GI SlidesDDM1Document39 pagesGI SlidesDDM1Anonymous d3qpXcm4xVNo ratings yet
- GIT 2021 Lect17Document49 pagesGIT 2021 Lect17Nikkole PhalulaNo ratings yet
- Pat GIT Diseases For Students - 1Document78 pagesPat GIT Diseases For Students - 1Carlo MaxiaNo ratings yet
- Problem 5 GIT Kelompok 16Document116 pagesProblem 5 GIT Kelompok 16Andreas AdiwinataNo ratings yet
- Gastroesophageal RefluxDocument20 pagesGastroesophageal Refluxtofan widyaNo ratings yet
- Gastric UlcerDocument31 pagesGastric UlcerMuhammadNo ratings yet
- Peptic Ulcer Nursing CareDocument5 pagesPeptic Ulcer Nursing CareFuad TalNo ratings yet
- GS DivisionDocument42 pagesGS DivisionDonald IDEDENo ratings yet
- Peptic Ulcer: Gastritis Gastroesophageal Reflux DiseaseDocument11 pagesPeptic Ulcer: Gastritis Gastroesophageal Reflux Diseasenickrulz10No ratings yet
- Gastro Intestinal SystemDocument9 pagesGastro Intestinal SystemJe Lyn100% (1)
- Gastritis: Medical AffairDocument11 pagesGastritis: Medical AffairKomal KhanNo ratings yet
- Gastro-Oesophageal RefluxDocument66 pagesGastro-Oesophageal Refluxsami khanNo ratings yet
- Biliary DisoderDocument50 pagesBiliary DisoderZanida ZainonNo ratings yet
- StomachDocument204 pagesStomachrajmv7No ratings yet
- Problem 2 Gastrointestinal System: Ryan Juliansyah 405130048 University of TarumanagaraDocument76 pagesProblem 2 Gastrointestinal System: Ryan Juliansyah 405130048 University of TarumanagaraRyan Juliansyah ZeinNo ratings yet
- "Gosh, Mrs. Doubtfire You Look Pale": Fire" in Television at The Emergency Departement You Worked ForDocument84 pages"Gosh, Mrs. Doubtfire You Look Pale": Fire" in Television at The Emergency Departement You Worked ForAngela Kristiana IntanNo ratings yet
- UNIT III Gastrointestinal DrugsDocument60 pagesUNIT III Gastrointestinal DrugsAahad AmeenNo ratings yet
- Nichols GI 09Document59 pagesNichols GI 09marviecute22No ratings yet
- 7.peptic Ulcer DiseaseDocument20 pages7.peptic Ulcer DiseaseHayat AL AKOUMNo ratings yet
- Crohn's Disease: GIT DisordersDocument8 pagesCrohn's Disease: GIT DisordersyeshweenNo ratings yet
- Disorders of The ColonDocument47 pagesDisorders of The ColonGieve BlasurcaNo ratings yet
- Diseases of The StomachDocument72 pagesDiseases of The StomachAMANUEL HABTEWOLDNo ratings yet
- AntiUlcer DrugsDocument8 pagesAntiUlcer DrugsGangadhar HariNo ratings yet
- Peptic UlcerDocument7 pagesPeptic UlcerNyakie MotlalaneNo ratings yet
- A Simple Guide to Gastritis and Related ConditionsFrom EverandA Simple Guide to Gastritis and Related ConditionsRating: 4.5 out of 5 stars4.5/5 (3)
- Pathfit 1Document9 pagesPathfit 1Minimi LovelyNo ratings yet
- Treatment of Hypernatremia in Adults - UpToDateDocument35 pagesTreatment of Hypernatremia in Adults - UpToDateJuLio Czar Carmona100% (1)
- Gordon'S Functional Health Patterns: University of San Jose - Recoletos School of Allied Medical Sciences NursingDocument2 pagesGordon'S Functional Health Patterns: University of San Jose - Recoletos School of Allied Medical Sciences NursingIvan A. EleginoNo ratings yet
- LRDocument6 pagesLRapi-582635800No ratings yet
- Patient Brochure Restylane Refyne USDocument9 pagesPatient Brochure Restylane Refyne USLavinia CristianNo ratings yet
- Case Files PedsDocument54 pagesCase Files PedsSam ZeezNo ratings yet
- Jama Zhou 2023 It 230012 1694198870.80806Document2 pagesJama Zhou 2023 It 230012 1694198870.80806William TapiaNo ratings yet
- Annex I Summary of Product CharacteristicsDocument60 pagesAnnex I Summary of Product CharacteristicsMadhu MitaNo ratings yet
- Differential Diagnosis of The Scalp Hair FolliculitisDocument8 pagesDifferential Diagnosis of The Scalp Hair FolliculitisandreinaviconNo ratings yet
- ENTREPRENEURSHIPDocument2 pagesENTREPRENEURSHIPkowie playsNo ratings yet
- WPTDay11 Cancer Fact Sheet C6 PDFDocument3 pagesWPTDay11 Cancer Fact Sheet C6 PDFDr. Krishna N. SharmaNo ratings yet
- Conservative Treatment For Meniscus RehabilitationDocument2 pagesConservative Treatment For Meniscus RehabilitationShahroz Khan100% (1)
- Sulfonamides: Miss Preeti Verma Assistant Professor Faculty of Pharmaceutical Sciences, Rama University, Kanpur, U.PDocument17 pagesSulfonamides: Miss Preeti Verma Assistant Professor Faculty of Pharmaceutical Sciences, Rama University, Kanpur, U.PYash SinghNo ratings yet
- Appendicitis ManuscriptDocument4 pagesAppendicitis Manuscriptkint manlangitNo ratings yet
- Multiple Associated Anomalies in Patients of Duodenal Atresia: A Case SeriesDocument2 pagesMultiple Associated Anomalies in Patients of Duodenal Atresia: A Case SeriesMuhammad Bilal MirzaNo ratings yet
- Kami Export - Philip Bolko - Kami Export - Hsantmyco07 Student WorksheetDocument6 pagesKami Export - Philip Bolko - Kami Export - Hsantmyco07 Student Worksheetphilip 6969No ratings yet
- Case Report ToxicologyDocument5 pagesCase Report ToxicologyschwanneNo ratings yet
- Personality Disorders Cluster ADocument7 pagesPersonality Disorders Cluster AKodhai NarayananNo ratings yet
- ctg نهائيDocument37 pagesctg نهائيdr.nahlla hellesNo ratings yet
- What Is A Blood TransfusionDocument6 pagesWhat Is A Blood TransfusionCarlo TolentinoNo ratings yet
- Brief Gelicart Colageno HidrolizadoDocument8 pagesBrief Gelicart Colageno HidrolizadoJenni KortezNo ratings yet
- Charles University Faculty of Physical Education and SportDocument140 pagesCharles University Faculty of Physical Education and SportPaulomds1991No ratings yet
- Ultrasonography TheDocument3 pagesUltrasonography TheNor-aina Edding AbubakarNo ratings yet
- 2surgical Nursing-Chronic Illness and Older AdultsDocument6 pages2surgical Nursing-Chronic Illness and Older AdultsGedie RocamoraNo ratings yet
- ORAL - 235 - Cindy Kesty - Laparoscopic Resection of Cornual Ectopic PrengnancyDocument10 pagesORAL - 235 - Cindy Kesty - Laparoscopic Resection of Cornual Ectopic Prengnancypb pogiNo ratings yet
- Case Analysis and Concept MapDocument2 pagesCase Analysis and Concept MapHoney Bitas Orias100% (1)
- Endocrine and Metabolic DisordersDocument21 pagesEndocrine and Metabolic DisordersAyeshaNo ratings yet
- Carcinoma Pancreas: Risk Factors: (A) Demographic FactorsDocument4 pagesCarcinoma Pancreas: Risk Factors: (A) Demographic FactorsSakthi Annamalai.cNo ratings yet
- Giant BullaeDocument43 pagesGiant Bullaefaishalanwar36No ratings yet