Professional Documents
Culture Documents
اورثوبيديك محاضرة 4 دكتور اكرم هيثم
Uploaded by
2020033390 ratings0% found this document useful (0 votes)
3 views44 pagesOriginal Title
اورثوبيديك_محاضرة_4_دكتور_اكرم_هيثم
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
3 views44 pagesاورثوبيديك محاضرة 4 دكتور اكرم هيثم
Uploaded by
202003339Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 44
Metabolic bone diseases
Management And PT Implications
Your Assignment
Read a scientific paper and present a resume/summary, in no more
than a page (500 words)
Related to orthopaedics or orthopaedic PT
Last 5 years
Open access journal, conference, academic essay…
Sent to us via Email, no handwriting.
Title
Introduction
Material
Methods
Results
Discussion
Conclusion
General bone diseases
metabolic and endocrinal diseases
• The main bone functions, support,
protection and leverage, deal carefully
with diseased bones…
• Normal control of mineral content (and
bone composition)
• Bones as mineral reservoir, which
constitutes around 50% of the total bone
mass
• The continuous flux of minerals to and
from bones mediated by local factors
and hormones and implemented by
cellular activity
Normal bone structure
Normal bone structure
• Stages of bone formation:
Osteoid= the unmineralised
bone
Woven bones= newly
formed bones
Lamellar bones= mature
bones
• Types of lamellar bones:
1. Cortical (compact) bones
2. Cancellous bones,
Normal bone structure
• The cotical bone:
Dense and strong, found where
support matters, as in shafts of long
bones and the subchondral plates
Arranged in osteons (haversian
systems) containing haversian canals
having bd vessels and lymphatics
and surrounded by densly packed
concectric lamellae of bone.
Haversian canals are connected to
both the periosteal and endosteal
surfaces by the small Volkmann’s
canals
Normal bone structure
• The cancellous bone
More porous, found near long bone
ends and in the vertebrae, made
up of trabeculae in sheets like
honey comb appearance and
arranged according to the
mechanical needs. Being weaker,
the effects of metabolic diseases
appear 1st in trabecular bones
Normal bone structure
• Blood supply to bones is really
rich. Vessels in the Haversian
canals form an anastomotic
network between the
medullary and periosteal blood
supply.
• Periosteal coverage and
enosteal lining occur in fully
formed bones. The deepest
layer of the former is a bone
forming layer besides its blood
supply role
Normal bone structure
• Bone cells and its functions:
Osteoblasts are cocerned with
bone formation and
osteclast activation
Osteoclasts are concerned with
bone resorption
Osteocytes are concerned with
communication and
providing information about
stresses
Bone development and growth
• Endochondral ossification, increasing mainly
length
Bone development and growth
• Intramembranous
ossification
increasing mainly
width
• Bone modelling and
remodeling
Normal bone structure
• Wolff’s law, intensity increases for areas of
stress
• Age related changes in bones for men and
women
Mineral exchange and Ca metabolism
• Bone turnover and mineral exchange, new bone
replaces old bone throughout life
• Ca metabolism, daily intake, absorption and
excretion, and the factors affecting that process.
• Phosphorous and vitamin D
• PTH, the fine regulator of Ca metabolism
• Calcitonin, the counterpart of PTH
Mineral exchange and Ca metabolism
Mineral exchange and Ca metabolism
• Other factors controlling Ca metabolism:
1. Estrogen
2. Adrenal corticosteroids
3. Local factors like insulin-like growth factor,
transforming growth factor, interleukin-1
prostaglandins and bone morphogenetic proteins
4. Mechanical factors like loss of wt, lack of exercise,
ms weakness prolonged bed rest and limb
immobilization = osteoporosis
Metabolic bone diseases
• Depletion of bone tissue manifested as:
1. Quantitative diminution of bone mass,
osteoporosis
2. Poorly mineralised osteoid, osteomalacia
3. Excessive bone resorption and increased PTH,
osteitis fibrosa
Beware while dealing with diseased bones
Metabolic bone diseases
• Common feature is the bad quality bones, be
very careful while doing physiotherapy for
those pts
• General clinical assessment
• Measurement of bone mass
• Biochemical testing
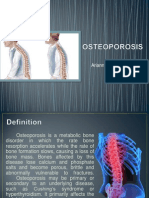
Osteoporosis
• Osteoporosis is quantitative loss of bone mass
• Osteopenia and osteoporosis
• Postmenopausal osteoporosis, high and low
turnover osteoporosis
• Risk factors for osteoporosis, like white race, family
history, early onset menopause, early hysterectomy,
lack of exercise and smoking and alcohol
Osteoporosis
Clinical picture:
Back pain and
generalised bone aches,
kyphos deformity, history
of fractures.
X ray shows diminished
bone density as well as
DEXA scan
Osteoporosis
• Prevention and treatment
Identify high risk groups, DEXA screening, adequate
Ca and vit D intake, stop smoking and alcohol
1. Hormonal replacement, many side effects
2. Bisphosphonates, best R modality now
3. Denosumab, newer approach
4. Management of fractures accordingly
Osteoporosis
• Secondary osteoporosis
1. Hypercortisonim
2. Thyrotoxicosis
3. Alcohol abuse
4. Multiple myeloma and carcinomatosis
5. Disuse
6. Others, like rheumatoid arthritis
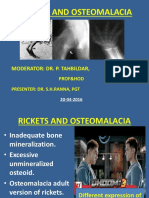
Rickets and osteomalacia
• Inadequate mineralization of bone
• Deformed joints and widened metaphysis in
children
• Soft indentable and easy fracturing bones in adults
Vitamin D deficiency rickets
• Used to be common in cold
areas(no sun rays)
• Clinically:
1. Craniotabes
2. Cupping(broadening) of the
epiphyses, distal radius, ankles
for physeal overgrowth
3. Rachitic rosary
4. Lateral indentation of the
chest(Harrison’s sulcus)
Vitamin D deficiency rickets
• X ray: thickening and widening of the
epiphyses, distortion of the metaphyses and
bow legs
Vitamin D deficiency rickets
• Biochemical investigations:
1. Serum ca and p and 25 HCC low
2. Alkaline phosphatase high
3. Urinary ca excretion low
• Treatment: vitamin D administration+ ca
supplement
Osteomalacia
• Defects anywhere in the metabolic pathway of
vitamin D
• Clinical picture insidious bone pains or ms
weakness probably for years, may present
with a stress fracture or insufficiency fracture
(to minor traumatic incidents).
• X ray generalized rarefaction, old poorly heald
fractures
Osteomalacia
Osteomalacia
• Investigations: as in rickets
• Biopsy may be needed
• After diagnosis of osteomalacia, we re-
investigate to know the cause, like
malabsorption synd, liver or kidney disease…
• Treatment :
Treatment of the cause
Supplementation with sufficient doses of Ca and
vitamin D
Hyperparathyroidism
• Over secretion of
parathormone
hormone from the
parathyroid gld
• Occurs 1ry, 2ry or
trtiary
• The cardinal feature is
elevated serum Ca and
parathyroid hormone
Hyperparathyroidism
pathology
• Ca absorption from the intestines as well as
Ca reabsorption from the kidneys are both
increased
• Ca is mobilised out of its bone storage
excessively leading to adverse effects on the
bones in the form of rarefaction and porosis
and on the kidneys in the form of stones,
nephrocalcinosis, infections
• Soft tissue calcifications can occur elsewhere
Hyperparathyroidism
pathology
• In severe cases, bones have cystic changes
and fibrous replacement, osteitis fibrosa
cystica
• Hge and giant cell reaction within the fibrous
stroma may give rise to brownish tu. Like
masses whose liquification leads to fluid filled
cysts, brown tu.
Hyperparathyroidism
C/P
• Middle aged females
• Symptoms of hypercalcaemia like anorexia, N&V,
abdominal pains, depression, fatigue and ms
weakness.
• Symptoms of renal disease
• Chondrocalcinosis
• Bone pains and pathological fractures
• X rays:
Subperiosteal cortical
resorption of the
middle phalanges is
most pathognomonic
generalised
osteoporosis
Vertebral collapse
Cortical erosions and
cyst formation
• Lab work:
Elevated s. Ca and PTH
and reduced s. P
Hyperparathyroidism
Treatment
• Conservative in mild
cases, adequate
hydration and decrease
Ca intake
• Treatment of associated
pathological fractures if
any
• Operative in severe
cases,
parathyroidectomy
Osteits fibrosa cystica
Renal osteodystrophy
• Bone weakness associated
with chronic renal disease
• Elevated s. P, and
defective vit D metabolism
leads to diminished s. Ca
• Children more affected,
stunted growth
• Treatment of renal dis vit
D replacement, then
correctin of deformitirs
Scurvy
• Defeciency of vit C leads to defective collagen and
consequently defective osteid formation
• Results in bone weakness and bleeding tendency
• X ray shows marked porotic changes, the ring sign
• Treatment is by vit C replacement
Paget’s disease
• Enlarged and thickened
bones with brittle internal
architecture
• Prevalent in the west and
reason is unknown
• Stage of resorption
(vascular), liable for
deformities and stage of
excess formation, liable for
pathological fractures
Paget’s disease
c/p
• More in older age
• Common in pelvis and tibia
• May remain dormant for many
years
• Deformities of the spine and the
legs give the classic picture
• Occasional dull and constant
pains
• Commonly present with
pathological fractures
• X ray appearance is characteristic.
• S. alkaline phosphatase raised
while s Ca and P are normal
Paget’s disease
complications
• Fractures
• Nerve compression
• Malignant transformation
into osteosarcoma
• Hypercalcaemia
• Cardiac failure
Paget’s disease
Treatment
• Treatment : antiresorptive
medicines like calcitonin and
bisphosphonates for symptomatic
pts.
• ORIF for fractures ”not an easy job”
• Surgical excision for ostesarcoma
(prognosis is bad)
Endocrine • The endocrine system has
disorders direct effect of growth and
maintenance of the skeletal
system
• Hypopituitarism in childhood
leads to obesity and
weakness of the physes,
slipping of the proximal
epiphysis while in adults
leads to osteoporosis
• Hyperthyroidism may give
rise to porotic manifestations.
Hypercortisonism
• Hypercortisonism (cushing’s
syndrome) excess secretion of
glucocorticoids leads to
porotic manifestations of
bones by stimulating bone
resorption and inhibiting
bone formation.
• Delayed healing, little
purchase for internal fixation
devices, high infection
incidence and avascular
necrosis are important
features of the disease
Hypercortisonism
• Treatment with corisone
has the same effects
• Ca and vit D supplements
may improve the condition
You might also like
- 03 Bone Non-Neoplastic Part-1Document52 pages03 Bone Non-Neoplastic Part-1dryunusaqNo ratings yet
- Osteoporosis PowerpointDocument45 pagesOsteoporosis PowerpointAgustina Anggraeni Purnomo100% (1)
- Metabolic Bone Diseases in ChildrenDocument44 pagesMetabolic Bone Diseases in ChildrenPartha GanesanNo ratings yet
- BBB Month 28 Workout PlanDocument11 pagesBBB Month 28 Workout Planluniblue100% (1)
- Serious Strength Training BompaDocument8 pagesSerious Strength Training BompaJosé Manuel Chicote100% (4)
- ACL Case StudyDocument14 pagesACL Case StudyKate Crizia VillafuerteNo ratings yet
- Essential Joint MovementsDocument52 pagesEssential Joint MovementsKhairul Hanan100% (5)
- Osteomalacia, Rickets, OsteoporosisDocument38 pagesOsteomalacia, Rickets, OsteoporosisalkalicharanNo ratings yet
- Endocrine and Metabolic DisordersDocument21 pagesEndocrine and Metabolic DisordersAyeshaNo ratings yet
- Rickets and Osteomalacia: Moderator: Dr. P. TahbildarDocument43 pagesRickets and Osteomalacia: Moderator: Dr. P. TahbildarNorman RiyadiNo ratings yet
- Rickets and Osteomalacia: Moderator: Dr. P. TahbildarDocument43 pagesRickets and Osteomalacia: Moderator: Dr. P. TahbildarNorman RiyadiNo ratings yet
- Bone PathologyDocument78 pagesBone Pathologyanupama menonNo ratings yet
- OsteoporosisDocument20 pagesOsteoporosisAishath Samha HussainNo ratings yet
- Osteoporosis & OsteomalaciaDocument29 pagesOsteoporosis & OsteomalaciaKeith OmwoyoNo ratings yet
- Kano State College of Nursing and Midwifery: BY Maimuna Sulaiman Ahmad RN, RM, BNSCDocument11 pagesKano State College of Nursing and Midwifery: BY Maimuna Sulaiman Ahmad RN, RM, BNSCMuhammad Daha SanusiNo ratings yet
- Metabolic Bone DisordersDocument24 pagesMetabolic Bone Disordersbpt20% (1)
- Kelainan Metabolik Dan Endokrin Oleh Dr. RonaldDocument48 pagesKelainan Metabolik Dan Endokrin Oleh Dr. RonaldOdilia Maria RahalusNo ratings yet
- Anatomy - Physiology of The Skeletal SystemDocument22 pagesAnatomy - Physiology of The Skeletal SystemMunish DograNo ratings yet
- An Overview: Feb 7, 2007: RicketsDocument22 pagesAn Overview: Feb 7, 2007: RicketsAustine OsaweNo ratings yet
- In The Name of GodDocument46 pagesIn The Name of GodGalaxyNo ratings yet
- Laboratory Finding in Metabolic Bone Disease and AutoimuneDocument58 pagesLaboratory Finding in Metabolic Bone Disease and AutoimuneRikaNo ratings yet
- Chapter 9Document13 pagesChapter 9Zaky DavidiaNo ratings yet
- Metabolic Bone Diseases: Dr. R.C.JindalDocument73 pagesMetabolic Bone Diseases: Dr. R.C.JindalpriyankNo ratings yet
- Book Reading and Metabolic Bone DisordersDocument25 pagesBook Reading and Metabolic Bone DisordersFrancisco GaniNo ratings yet
- Skeletal System: Bones, Joints, and HomeostasisDocument59 pagesSkeletal System: Bones, Joints, and HomeostasisaldiNo ratings yet
- Systemic Diseases Manifested in The JawsDocument25 pagesSystemic Diseases Manifested in The JawsTeguh Caninus100% (1)
- Musculoskeletal Disease Teaching MaterialsDocument150 pagesMusculoskeletal Disease Teaching Materialsghina zalmihNo ratings yet
- Patho - 4th Asessment - Metabolic Bone Disease - 2007Document39 pagesPatho - 4th Asessment - Metabolic Bone Disease - 2007api-3703352100% (1)
- Metabolic & Endocrine DisordersDocument113 pagesMetabolic & Endocrine DisordersEka Yoga WiratamaNo ratings yet
- 7 PathophysiologyDocument1 page7 PathophysiologyKizzel MacapazNo ratings yet
- Pathologicalfractures 170201065538Document54 pagesPathologicalfractures 170201065538manan shroffNo ratings yet
- OsteomalaciaDocument5 pagesOsteomalaciaLorebell100% (5)
- Osteomalacia: Softening of Bones Due to Defective MineralizationDocument38 pagesOsteomalacia: Softening of Bones Due to Defective MineralizationAji PrimaNo ratings yet
- Osteoporosis diagnosis and treatment overviewDocument27 pagesOsteoporosis diagnosis and treatment overviewShoban RajNo ratings yet
- Orthopedics BoneDisordersDocument20 pagesOrthopedics BoneDisordersannapanna1No ratings yet
- Osteomyelitis Metabolic Bone DisordersDocument36 pagesOsteomyelitis Metabolic Bone DisordersVishesh JainNo ratings yet
- Metabolic Bone Disease & Bone Markers - SlidesDocument46 pagesMetabolic Bone Disease & Bone Markers - Slidesmonday125100% (1)
- Rickets and OsteomalaciaDocument22 pagesRickets and Osteomalaciajoe BouGhazaliNo ratings yet
- Metabolic Jaw DiseasesDocument55 pagesMetabolic Jaw DiseasesoladunniNo ratings yet
- OmrDocument36 pagesOmrGayathri MenonNo ratings yet
- OsteoporosisDocument15 pagesOsteoporosisCamille Marie ReyesNo ratings yet
- Osteoporosis: University of Health Sciences Faculty of Medicine Im Bunthoeun 2016Document17 pagesOsteoporosis: University of Health Sciences Faculty of Medicine Im Bunthoeun 2016Moni RethNo ratings yet
- Musculoskeletal PathophysiologyDocument72 pagesMusculoskeletal PathophysiologyMartyarini BudiNo ratings yet
- Lec 3 2010 02 6Document8 pagesLec 3 2010 02 6Ras WhoknowsmeNo ratings yet
- Bone and Joints 2Document38 pagesBone and Joints 2Eryn HooverNo ratings yet
- Metabolic Bone Disorders: Osteoporosis and ManagementDocument35 pagesMetabolic Bone Disorders: Osteoporosis and Managementkelemwork WaleNo ratings yet
- Osteoporosis: Davin PannaaustenDocument23 pagesOsteoporosis: Davin PannaaustenDavinPannaaustenNo ratings yet
- Nutrional Bone Disorder.Document21 pagesNutrional Bone Disorder.Sharafudheen KaNo ratings yet
- Pagets DiseaseDocument62 pagesPagets DiseaseKush PathakNo ratings yet
- Osteomalacia, Rickets, Osteoporosis and Parathyroid DisordersDocument48 pagesOsteomalacia, Rickets, Osteoporosis and Parathyroid DisordersHimanshu NarangNo ratings yet
- Bone Pathology: Osteoporosis, Osteomalacia, Osteopetrosis, Paget's Disease & TumorsDocument25 pagesBone Pathology: Osteoporosis, Osteomalacia, Osteopetrosis, Paget's Disease & TumorsDoodNo ratings yet
- Bone Tissue: Supportive Connective Tissue: CellsDocument52 pagesBone Tissue: Supportive Connective Tissue: CellsCalin PopaNo ratings yet
- MuscolskeletalDocument74 pagesMuscolskeletalsamar yousif mohamedNo ratings yet
- Osteoporosis: The Silent Bone DiseaseDocument15 pagesOsteoporosis: The Silent Bone Diseaseعبدالرحمن علىNo ratings yet
- Rickets: Causes, Symptoms, Diagnosis and TreatmentDocument49 pagesRickets: Causes, Symptoms, Diagnosis and TreatmentMis Bah100% (1)
- Musculoskeletal Disorders Part 1 Metabolic Bone Disorders.Document84 pagesMusculoskeletal Disorders Part 1 Metabolic Bone Disorders.Carmela Lacsa DomocmatNo ratings yet
- Bone Markers Univ West APC Feb 2013Document82 pagesBone Markers Univ West APC Feb 2013monday125No ratings yet
- Regulation of Intracellular Calcium HomeostasisDocument27 pagesRegulation of Intracellular Calcium HomeostasisArumpaavai PugazhiniNo ratings yet
- OsteopetrosisDocument14 pagesOsteopetrosisMaha JabeenNo ratings yet
- 7 - Metabolic and Endocrine Bone DisordersDocument16 pages7 - Metabolic and Endocrine Bone DisordersYoga PribadiNo ratings yet
- Paget Disease of Bone, A Simple Guide to the Condition, Treatment and Related DiseasesFrom EverandPaget Disease of Bone, A Simple Guide to the Condition, Treatment and Related DiseasesNo ratings yet
- The Slim Book of Health Pearls: Symptoms Never to IgnoreFrom EverandThe Slim Book of Health Pearls: Symptoms Never to IgnoreNo ratings yet
- Clinical Signs in Humans and Animals Associated with Minerals, Trace Elements and Rare Earth ElementsFrom EverandClinical Signs in Humans and Animals Associated with Minerals, Trace Elements and Rare Earth ElementsNo ratings yet
- Physics of Bones and JointsDocument5 pagesPhysics of Bones and JointsAnonymous x62KIL4xNo ratings yet
- 2-HEAD AND NECK PrintDocument30 pages2-HEAD AND NECK Printsaddam hussain100% (1)
- Dr. K.B.Sudhikumar Prof. & HOD Dept. of Salyatantra, GAC, TripunithuraDocument69 pagesDr. K.B.Sudhikumar Prof. & HOD Dept. of Salyatantra, GAC, Tripunithuraapi-73271717No ratings yet
- Morning Stretch #1: Courtesy of Getty ImagesDocument5 pagesMorning Stretch #1: Courtesy of Getty ImagesVipul SinghNo ratings yet
- Veritas Health Lower Back Exercise GuideDocument5 pagesVeritas Health Lower Back Exercise GuidecasimiroamadoNo ratings yet
- Ankle Syndesmosis and Pilon FracturesDocument6 pagesAnkle Syndesmosis and Pilon Fractures姚立喬No ratings yet
- Eular Us Course Modulo 5 Tornozelo e PeDocument44 pagesEular Us Course Modulo 5 Tornozelo e PeGustavo Bernardo DamascenoNo ratings yet
- 16 - Face (FF)Document57 pages16 - Face (FF)checkmateNo ratings yet
- ACL Reconstruction With Bio-TransFix® T3Document6 pagesACL Reconstruction With Bio-TransFix® T3Gustavo Enrique Matson Carballo100% (1)
- Principle of Fracture Management: Dr. Miawa RobertDocument63 pagesPrinciple of Fracture Management: Dr. Miawa Robertkajojo joyNo ratings yet
- Diagnosis & Procedural Coding For PodiatryDocument45 pagesDiagnosis & Procedural Coding For PodiatrydarienDPM100% (1)
- Fundamental Starting PositionDocument28 pagesFundamental Starting PositionShobhit SainiNo ratings yet
- Hershey Board Certification Review Outline Study Guide: Jonathan M. Singer, D.P.MDocument9 pagesHershey Board Certification Review Outline Study Guide: Jonathan M. Singer, D.P.MpoddataNo ratings yet
- Calisthenics Workout ProgramDocument9 pagesCalisthenics Workout ProgramDanielNo ratings yet
- Blood Supply of Lower LimbDocument27 pagesBlood Supply of Lower LimbabdullahNo ratings yet
- Outcome of Wearing High Heel Shoes in Young GenerationDocument16 pagesOutcome of Wearing High Heel Shoes in Young GenerationCureusNo ratings yet
- AFO Prescription - Measurement - Casting - Rectification & Fitting ICRCDocument58 pagesAFO Prescription - Measurement - Casting - Rectification & Fitting ICRCEmna Laabidi100% (1)
- PM 070 E0Document23 pagesPM 070 E0Radu HarliscaNo ratings yet
- UCBL LectureDocument29 pagesUCBL Lectureergosadia658No ratings yet
- Bones and Skeletal Tissue Matching QuestionsDocument10 pagesBones and Skeletal Tissue Matching Questionsjinni0926No ratings yet
- MUSCULAR-SYSTEM-TRANS-WEEK-1Document9 pagesMUSCULAR-SYSTEM-TRANS-WEEK-1olaya.xyzanigaia.bsnNo ratings yet
- Clinical Orthopaedic Rehabilitation Brotzmanpdf Eb PDFDocument1 pageClinical Orthopaedic Rehabilitation Brotzmanpdf Eb PDFMarie BaptisteNo ratings yet
- CT TractionDocument3 pagesCT TractionLaira CañeteNo ratings yet
- Spinal Disorders - Study GuideDocument183 pagesSpinal Disorders - Study Guidetechsupport24712365No ratings yet
- Zach Roys Powerbuilding Program For Men MASTERDocument51 pagesZach Roys Powerbuilding Program For Men MASTERStandaardStanNo ratings yet
- Spondylosis, Cervical and LumbarDocument1 pageSpondylosis, Cervical and LumbarLuis HerreraNo ratings yet