Professional Documents
Culture Documents
Abdominal Cavity
Uploaded by
tanishapatel10050 ratings0% found this document useful (0 votes)
3 views78 pagesCopyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
3 views78 pagesAbdominal Cavity
Uploaded by
tanishapatel1005Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 78
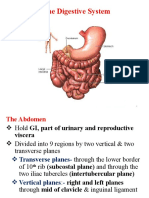
ABDOMINAL CAVITY:
GENERAL
ARRANGEMENT OF
ABDOMINAL VISCERA,
PERITONEUM
ANISA Z. SADAIN, MD, FPSCRS
July 13, 2023
Scope: • Quadrants and Regions of the
Abdominal Cavity
• General arrangement of the Abdominal
Viscera
• Peritoneum
• Peritoneal Nerve Supply and Function
• Clinical Notes
• Embryology
Quadrants and
Regions of the
Abdominal
Cavity
Four Quadrants of the Abdominal Cavity
• Right upper quadrant.
• Left upper quadrant.
• Right lower quadrant.
• Left lower quadrant.
Nine Regions of the Abdominal Cavity
General
Arrangement of
the Abdominal
Viscera
General Arrangement of the Abdominal
Viscera
The esophagus connects the pharynx with the
stomach.
The stomach occupies the left upper
quadrant, epigastric, and umbilical area
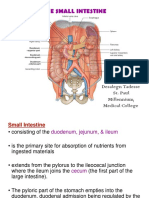
The duodenum of the small intestine is
situated in the epigastric and umbilical area
The jejunum occupies the upper left part,
while the ileum occupies the lower right part
of the abdominal cavity and the pelvic cavity.
• The large Intestine arches around and encloses
the coils of the small intestine.
• The liver occupies the upper part of the
abdominal cavity. The gallbladder adheres to
the undersurface of the right lobe of the liver.
General Arrangement of the Abdominal
Viscera
The pancreas stretches obliquely
across the posterior abdominal wall
in the epigastric region.
The spleen occupies the left upper
part of the abdomen.
The kidneys lie high up on the
posterior abdominal wall.
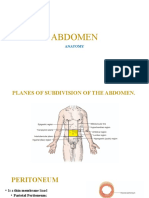
PERITONEUM
Peritoneum
• a thin serous membrane that lines the
walls of the abdominal and pelvic
cavities and clothes the viscera
• parietal peritoneum - lines the walls
of the abdominopelvic cavity
• visceral peritoneum - covers the
organs
• extraperitoneal tissue - lies between
the parietal peritoneum and the fascial
lining of the abdominal and pelvic
walls.
Peritoneum
• peritoneal cavity - potential space
between the parietal and visceral layers
• It is the largest cavity in the body and is
divided into two parts:
• the greater sac - main compartment
and extends from the diaphragm
down into the pelvis
• the lesser sac - smaller and lies
behind the stomach.
• secretes a small amount of serous fluid
(peritoneal fluid), which lubricates the
surfaces of the peritoneum and allows
free movement between viscera.
Peritoneum
• The greater and lesser sacs are in free
communication with one another through an oval
window called the opening of the lesser sac
(epiploic foramen/foramen of Winslow)
Peritoneum
Intraperitoneal & Retroperitoneal
Relationships
• lntraperitoneal organs - is almost
totally covered with visceral
peritoneum. They are attached to other
organs or the abdominal wall by
peritoneal bridges (omenta,
mesenteries, ligaments)
• The stomach, jejunum, ileum, and
spleen.
• Retroperitoneal organs - lie behind
the peritoneum and are only partially
covered with visceral peritoneum.
• The pancreas, ascending and
descending parts of the colon
Peritoneal Ligaments
• Peritoneal ligaments are two-layered folds
of the peritoneum that connect solid
viscera to the abdominal walls
• Liver connects to the diaphragm by the
falciform ligament, the coronary
ligament, and the right and left
triangular ligaments
Peritoneal Ligaments: Liver
Peritoneal Ligaments:
Spleen & Stomach
Omenta
• Omenta are two-layered folds of
peritoneum that connect the stomach
to another viscus
• greater omentum - connects the
greater curvature of the stomach to the
transverse colon
• lesser omentum - suspends the lesser
curvature of the stomach and the
proximal duodenum from the fissure
of the ligamentum venosum and the
porta hepatis on the undersurface of
the liver
• gastrosplenic omentum (ligament)
connects the stomach to the hilum of
the spleen
Omenta
Omenta
Mesenteries
• Mesenteries are two-layered folds of the peritoneum connecting parts
of the intestines to the posterior abdominal wall
• mesentery of the small intestine, the transverse mesocolon, and the
sigmoid mesocolon
Mesenteries
Peritoneal Bridges
• peritoneal ligaments, omenta,
and mesenteries serve as bridges
that permit blood, lymph vessels,
and nerves to reach the viscera.
Lesser Sac
(Omental Bursa)
• lies behind the stomach and the
lesser omentum
• extends upward as far as the
diaphragm and downward
between the layers of the greater
omentum
• Left margin of sac: the spleen,
the gastrosplenic omentum, and
the splenorenal ligament
• Right margin of sac: opens into
the greater sac through the
opening of the lesser sac
(epiploic foramen)
Lesser Sac
• Epiploic foramen/Foramen of Winslow
boundaries:
• Anteriorly: free border of the lesser
omentum, the bile duct, the hepatic
artery, and the portal vein
• Posteriorly: inferior vena cava
• Superiorly: caudate process of the
caudate lobe of the liver
• lnferiorly: first part of the duodenum
Abdominal Cavity
• Roof: diaphragm (also forms the upper
parts of the lateral and posterior walls)
• Floor: It is absent inferiorly as the
abdominal cavity communicates with the
pelvic cavity at the pelvic brim.
• The peritoneal cavity is divided Into an
upper part within the abdomen and a lower
part In the pelvis. The abdominal part is
further subdivided by the many peritoneal
reflections into important recesses and
spaces, which, in turn, are continued into
the paracolic gutters
Abdominal Recesses
• small pockets or fossae in
the peritoneal cavity, which are
bounded by folds of peritoneum
Abdominal Recesses
• Duodenal Recesses - close to the
duodenojejunal junction: (4)
• superior duodenal recess
• inferior duodenal recess
• paraduodenal recess
• retroduodenal recess
Abdominal Recesses
• Cecal Recesses - close to the cecum: (3)
• superior ileocecal recess
• inferior ileocecal recess
• retrocecal recess
Abdominal Recesses
Abdominal Recesses
• Intersigmoid recess - situated at
the apex of the inverted, V-shaped
root of the sigmoid mesocolon
Subphrenic Spaces
• The right and left anterior subphrenic
spaces lie between the diaphragm and the
liver, on each side of the falciform
ligament
• The right posterior subphrenic space lies
between the right lobe of the liver, the
right kidney, and the right colic flexure
• The right extraperitoneal space lies
between the layers of the coronary
ligament and is therefore situated between
the liver and the diaphragm.
Paracolic gutters
• lie on the lateral and medial
sides of the ascending and
descending colons
Subphrenic Space &
Paracolic gutters
Peritoneal Nerve Supply
Parietal peritoneum (somatic nerve
innervation)
• sensitive to pain, temperature, touch, pressure
• Lower six thoracic and first lumbar nerve
- supply the parietal peritoneum lining the
anterior abdominal wall
• Phrenic nerves
- supply the central part of the diaphragmatic
peritoneum
• Lower six thoracic nerves
- Supply the peripheral diaphragmatic
peritoneum
• Obturator nerve, a branch of the lumbar plexus
- supplies parietal peritoneum in the pelvis
Peritoneal Nerve Supply
Visceral peritoneum (visceral afferent
innervation)
• sensitive only to stretch and tearing
• Visceral afferent nerves supply the
viscera and also travel in mesenteries.
• Overdistension of a viscus leads to the
sensation of pain. The mesenteries of
the small and large Intestines are
sensitive to mechanical stretching.
Peritoneal Functions
Peritoneal Fluid Peritoneal Folds
• is pale yellow & viscid, containing leukocytes • suspends the various organs within the
• secreted by the peritoneum and ensures that peritoneal cavity and serve as avenues
the mobile viscera glide easily on one another for conveying the blood vessels,
lymphatics, and nerves to these organs.
• Intraperitoneal movement of fluid toward the
diaphragm appears to be continuous and there • Large amounts of fat are stored in the
it is quickly absorbed into the subperitoneal peritoneal ligaments and mesenteries,
lymphatic capillaries and especially in the greater omentum
Peritoneal circulation: watershed regions in
the peritoneal cavity that are areas of fluid
stasis:
• Ileocolic region
• Root of the sigmoid mesentery
CLINICAL NOTES
Peritoneum &
Peritoneal Cavity
• Peritoneal Fluid Movement
• Ascitis - excessive accumulation of peritoneal
fluid within the peritoneal cavity. It can occur
secondary to:
• hepatic cirrhosis (portal venous congestion)
• malignant disease
• congestive heart failure (systemic venous
congestion)
• In a thin patient, as much as 1500 mL has to
accumulate before ascites can be recognized
clinically.
• Paracentesis - the withdrawal of peritoneal fluid
from the peritoneal cavity
Peritoneum & Peritoneal Cavity
Peritoneal Infection/Peritonitis
• Spontaneous bacterial peritonitis
• Secodnary peritonitis: enter the
peritoneal cavity through several
routes:
• from the interior of the GI tract
and gallbladder
• through the anterior abdominal
wall
• via the uterine tubes in females
(gonococcal peritonitis or
pneumococcal peritonitis)
• from the blood
Peritoneum & Peritoneal Cavity
Peritoneal Infection/ Abscess
• Collection of infected peritoneal fluid in
one of the subphrenic spaces is often
accompanied by infection of the pleural
cavity localized pus in a pleural
space (empyema) with a subphrenic
abscess
• Spread from the peritoneum to the
pleura via the diaphragmatic lymph
vessels.
• Subphrenic abscess/blood under
diaphragm pain over the shoulder
Peritoneum & Peritoneal Cavity
Peritoneal Infection/ Abscess
• sit patient up in bed with the back at a 45◦ angle
infected peritoneal fluid gravitates downward
into the pelvic cavity (rate of toxin absorption is
slow)
Greater Omentum
Localization of infection:
• “abdominal policeman”
• Poorly developed during the first 2 years
of life
• Infection is often localized to a small area
of the peritoneal cavity, thus saving the
patient from a serious diffuse peritonitis
(ie. appendicitis)
Greater Omentum
Hernia Plug:
• can plug the neck of a hernial sac and
prevent the entrance of coils of small
intestine
Greater Omentum
Greater Omentum used in Surgery:
• Surgeons sometimes use the omentum
to buttress an intestinal anastomosis, in
the closure of a perforated gastric or
duodenal ulcer or in fistula repairs.
Omental patching
in dudoenal or
gastric ulcer
Omentum used to buttress an
anastomosis in the esophagus
Omentum used in fistula repair
Greater Omentum
Torsion:
• The greater omentum may undergo
torsion, and if extensive, the blood
supply to a part of It may be cut off,
causing necrosis.
Abdominal Pain
• Abdominal peritoneal pain
• Pelvic peritoneal pain
• Referred visceral pain
Abdominal Peritoneal Pain
• Abdominal pain originating from the
parietal peritoneum is somatic and can be
precisely localized and is usually severe
• The lower six thoracic nerves and the first
lumbar nerve supply the parietal
peritoneum lining the anterior abdominal
wall
• An inflamed parietal peritoneum is
extremely sensitive to stretch.
Abdominal Peritoneal Pain
• To diagnose peritonitis:
pressure is applied to the
abdominal wall over the
site of the inflammation.
The pressure is then
removed by suddenly
withdrawing the finger
abdominal wall rebounds
extreme local pain
“rebound tenderness”
Pelvic Peritoneal Pain
• The parietal peritoneum in the
pelvis can be palpated by means of
a pelvic (rectal or vaginal)
examination
• An Inflamed appendix may hang
down into the pelvis and irritate the
parietal peritoneum there.
• Pelvic examination can detect
extreme tenderness of the parietal
peritoneum on the right side
Referred Visceral Pain
• Stretch caused by
overdistension of a viscus or
pulling on a mesentery gives
rise to the sensation of pain,
which is commonly referred to
a characteristic site in the skin.
• GI tract arises embryonically as
a midline structure and receives
a bilateral nerve supply, pain
may be referred to the midline
Peritoneal Dialysis
• a treatment for kidney failure that uses the
peritoneum to filter the blood inside the body
• A watery solution, the dialysate, is introduced
through a catheter through a small midline
incision through the anterior abdominal wall
below the umbilicus.
Peritoneal Dialysis
• The products of metabolism, such as urea,
diffuse through the peritoneal lining cells
from the blood vessels into the dialysate and
are removed from the patient
Internal Abdominal Hernia
• Occasionally, a loop of intestine enters
a peritoneal pouch or recess (eg. the
lesser sac of the duodenal recess) and
becomes strangulated at the edges of
the recess
• Uncommon
• Can be congenital or acquired
Internal Abdominal Hernia
• strangulating SBO, that occurs
after a closed-loop obstruction
• Most common: Paraduodenal
hernias, foramen of Winslow
hernias
EMBRYOLOG
Y NOTES
Peritoneum and Peritoneal Cavity
Development
• By the end of the 4th week of embryonic
development, the intraembryonic coelomic
cavity has been formed by folding of the
embryonic disc.
• The intraembryonic coelomic cavity is lined
by mesoderm which encloses the primitive
gut and forms the peritoneum.
• The outer or somatic mesoderm, lining
the cavity, forms the parietal layer (lining
the peritoneal cavity)
• The inner or splanchnic mesoderm forms
the visceral layer (covering abdominal
organs).
Peritoneum and Peritoneal Cavity
Development
Peritoneum and Peritoneal Cavity
Development
• Early in development, the peritoneal
cavity is divided into right and left
halves by a central partition formed by
the dorsal mesentery, the gut, and the
small ventral mesentery. However, the
ventral mesentery extends only for a
short distance along the gut so that the
right and left halves of the peritoneal
cavity are in free communication.
Peritoneal Ligaments and Mesenteries
Formation
• The peritoneal ligaments are
developed from the ventral and dorsal
mesenteries.
• The ventral mesentery is formed from
the mesoderm of the septum
transversum (derived from the cervical
somites, which migrate downward).
• The ventral mesentery forms:
• the falciform ligament
• the lesser omentum
• the coronary and the triangular ligaments
of the liver.
Peritoneal Ligaments and Mesenteries
Formation
• The dorsal mesentery is formed from
the fusion of the splanchnopleuric
mesoderm on the two sides of the
embryo. It extends from the posterior
abdominal wall to the posterior border
of the abdominal part of the gut
• The dorsal mesentery forms:
• the gastrophrenic ligament
• the gastrosplenic omentum
• the splenorenal ligament
• the greater omentum
• the mesenteries of the small and large
intestines.
Lesser and Greater Sac Formation
• The extensive growth of the
right lobe of the liver pulls
the ventral mesentery to the
right and causes rotation of
the stomach and duodenum
• The remaining part of the
peritoneal cavity, which is
not included In the lesser sac,
would become the greater sac
Greater Omentum Formation
• The spleen is developed in the upper part of
the dorsal mesentery, and the greater
omentum is formed as a result of the rapid
and extensive growth of the dorsal mesentery
caudal to the spleen. To begin with, the
greater omentum extends from the greater
curvature of the stomach to the posterior
abdominal wall superior to the transverse
mesocolon
• Later, the posterior layer of the omentum
fuses with the transverse mesocolon.
• The inferior recess of the lesser sac extends
inferiorly between the anterior and the
posterior layers of the greater omentum.
- END OF LECTURE -
1. What is the communication between the lesser sac and
greater sac called?
2. What is the abdominal policeman?
3. What is another name of the lesser omentum?
4. Name one viscera/organ
contained in each region
5. Name the following structures:
6. Name a few functions of the peritoneum
7. Name 2 ligaments from each
major peritoneal ligament:
You might also like
- Peritoneum, Peritoneal Cavity, and Diaphragm 11-6-15-1Document67 pagesPeritoneum, Peritoneal Cavity, and Diaphragm 11-6-15-1Deny ShajiniNo ratings yet
- ANAT 221 - PeritoneumDocument22 pagesANAT 221 - PeritoneumWisdom IkechukwuNo ratings yet
- 1 Abdominal VisceraDocument45 pages1 Abdominal VisceraMero HamedNo ratings yet
- Abdomen.: Moore, Keith. Clinically Oriented Anatomy. Seventh Edition. Lippincott Williams & Wilkins. Baltimore. 2014Document58 pagesAbdomen.: Moore, Keith. Clinically Oriented Anatomy. Seventh Edition. Lippincott Williams & Wilkins. Baltimore. 2014Paola Solarte ChicaizaNo ratings yet
- Peritoneum - Dr. QuratulainDocument40 pagesPeritoneum - Dr. QuratulainWajahat FaizNo ratings yet
- Abdominal AnatomyDocument39 pagesAbdominal AnatomyRahul MandhanNo ratings yet
- Anatomy of PeritoneumDocument61 pagesAnatomy of PeritoneumFirdaus SeptiawanNo ratings yet
- The Abdominal Cavity, The Peritoneum & The Peritoneal CavityDocument62 pagesThe Abdominal Cavity, The Peritoneum & The Peritoneal CavityAidos BolatovNo ratings yet
- Abdomen - Esophagus To ColonDocument42 pagesAbdomen - Esophagus To ColonBibek GajmerNo ratings yet
- Small IntestineDocument34 pagesSmall IntestineIAMSANWAR019170100% (1)
- Gi AnatomyDocument67 pagesGi AnatomyasyanadhikaryNo ratings yet
- Anatomy of The Abdomen (6) : - Abdominal Esophagus - Stomach - Small Intestine - Large IntestineDocument34 pagesAnatomy of The Abdomen (6) : - Abdominal Esophagus - Stomach - Small Intestine - Large IntestineBilal YimamNo ratings yet
- Stomach Anatomy in 40 CharactersDocument29 pagesStomach Anatomy in 40 CharactersSupriti Verma Bhatnagar100% (1)
- Clinical Embriology and Anatomy of Gi Tract Part1Document44 pagesClinical Embriology and Anatomy of Gi Tract Part1trianaamalia100% (1)
- Duodenum and PancreaslectureDocument35 pagesDuodenum and PancreaslectureChigozie GeraldNo ratings yet
- PeritoneumDocument39 pagesPeritoneumtuhinsinghNo ratings yet
- Surgical Anatomy of PeritoneumDocument63 pagesSurgical Anatomy of PeritoneumSuvarna RajNo ratings yet
- Large IntestineDocument29 pagesLarge IntestineOlaifa victorNo ratings yet
- Ana SGD 15Document67 pagesAna SGD 15Bea ManzanoNo ratings yet
- Digestive SystemDocument64 pagesDigestive SystemAyro Business CenterNo ratings yet
- Abdomen AnatomyDocument9 pagesAbdomen AnatomyPhan Hoàng SơnNo ratings yet
- Clinical Embriology and Anatomy of Gi Tract Part1Document43 pagesClinical Embriology and Anatomy of Gi Tract Part1Luna LitamiNo ratings yet
- Digestive System EmbryologyDocument104 pagesDigestive System EmbryologyAlistair WalkerNo ratings yet
- Digestive System OverviewDocument90 pagesDigestive System OverviewDiazNo ratings yet
- StomachDocument24 pagesStomachHarini KarthikeyanNo ratings yet
- The Small Intestine-1Document38 pagesThe Small Intestine-1ChiderahNo ratings yet
- 4rd Lecture - AbdomenDocument26 pages4rd Lecture - AbdomenZainab Jamal SiddiquiNo ratings yet
- The PERITONEUMDocument27 pagesThe PERITONEUMEniola abdullahi AduagbaNo ratings yet
- ANATOMY OF SMALL AND LARGE INTESTINEDocument38 pagesANATOMY OF SMALL AND LARGE INTESTINERakaNo ratings yet
- Large Intestine Functions and AnatomyDocument34 pagesLarge Intestine Functions and AnatomySastiy MutiadesieNo ratings yet
- GIT Cont 071628Document51 pagesGIT Cont 071628Olatomide OlaniranNo ratings yet
- Small IntestineDocument16 pagesSmall IntestineShimmering MoonNo ratings yet
- Development of the Gastrointestinal SystemDocument88 pagesDevelopment of the Gastrointestinal SystemBindiya MangarNo ratings yet
- Gross Anatomy LiverDocument51 pagesGross Anatomy LiverDeny ShajiniNo ratings yet
- Anat 221-Large IntestineDocument21 pagesAnat 221-Large IntestineWisdom IkechukwuNo ratings yet
- Anterior Abdominal Wall Lecture - Nov2015Document75 pagesAnterior Abdominal Wall Lecture - Nov2015Nithin0% (1)
- GasterDocument179 pagesGasterAraka Patriota100% (1)
- Anatomy of the Stomach and DuodenumDocument179 pagesAnatomy of the Stomach and DuodenumHaraka NabdaNo ratings yet
- Pelvic Cavity: Prep by Lect: S Hasssn AskariDocument32 pagesPelvic Cavity: Prep by Lect: S Hasssn AskariShimmering MoonNo ratings yet
- Med II GIT 2 Peritoneum Aug 23Document24 pagesMed II GIT 2 Peritoneum Aug 23Suhayb CumarNo ratings yet
- Anatomy of GIT For PCII Students..Document106 pagesAnatomy of GIT For PCII Students..AMANUEL HABTEWOLDNo ratings yet
- Stomach: DR Kavitha M Kjiar (Savli)Document52 pagesStomach: DR Kavitha M Kjiar (Savli)Dhaval Chauhan0% (1)
- Anatomy Stomach & Duodenum: by Mekonnen.A (R1)Document46 pagesAnatomy Stomach & Duodenum: by Mekonnen.A (R1)Tsega WesenNo ratings yet
- Peritoneum & Peritoneal Cavity PresentationDocument59 pagesPeritoneum & Peritoneal Cavity Presentationsaint thuggerNo ratings yet
- Peritonem A ND Peritonealcavity PDFDocument62 pagesPeritonem A ND Peritonealcavity PDFKarem MaaliNo ratings yet
- Anatomy of DuodenumDocument23 pagesAnatomy of DuodenumEngki AdityaNo ratings yet
- 4 The Stomach and The Abdominal EsophagusDocument43 pages4 The Stomach and The Abdominal EsophagusAbdullah HaroonNo ratings yet
- Gastrointestinal AnatomyDocument70 pagesGastrointestinal AnatomyNatasya Ryani PurbaNo ratings yet
- By Prof. Saeed Abuel MakaremDocument25 pagesBy Prof. Saeed Abuel MakaremmahardikaNo ratings yet
- Physiology of Lower GI TractDocument180 pagesPhysiology of Lower GI TractIcarus WingsNo ratings yet
- MD Anatomy Guide to the StomachDocument58 pagesMD Anatomy Guide to the StomachSkinny tuberNo ratings yet
- Pancreas AnatomDocument50 pagesPancreas Anatomhabtsh habshaNo ratings yet
- Anatomy of Liver and Pancreas by Kazim AliDocument32 pagesAnatomy of Liver and Pancreas by Kazim AliAhmad KhanNo ratings yet
- 7) Anatomy of OMENTUMDocument22 pages7) Anatomy of OMENTUMGoodone OneNo ratings yet
- Anatomy of The EsophagusDocument14 pagesAnatomy of The EsophagusroselynroukayaNo ratings yet
- The StomachDocument3 pagesThe StomachAhmad BdeirNo ratings yet
- Dr. Meidona - Development of Gastrointestinal System PDFDocument54 pagesDr. Meidona - Development of Gastrointestinal System PDFwkwkwkhhhhNo ratings yet
- Small Intestine MMCDocument65 pagesSmall Intestine MMCWorku KifleNo ratings yet
- ANATOMI SISTEM PENCERNAAN by Dr. RifalDocument97 pagesANATOMI SISTEM PENCERNAAN by Dr. RifalSusi ErawatiNo ratings yet
- Intestinal Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandIntestinal Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- TISSUESDocument19 pagesTISSUESHARETASREE GANESANNo ratings yet
- CCNDocument39 pagesCCNMann TSha100% (1)
- GR 10 Life Sciences IEB 3 in 1 Extracts PDFDocument16 pagesGR 10 Life Sciences IEB 3 in 1 Extracts PDFteeNo ratings yet
- Pineal Gland or EpiphysisDocument5 pagesPineal Gland or EpiphysisPanche BozhikovNo ratings yet
- Marma and Marma TherapyDocument14 pagesMarma and Marma TherapysunithaNo ratings yet
- Muscular System Chapter 10 SummaryDocument6 pagesMuscular System Chapter 10 SummaryKYLA LORENZ BALUMANo ratings yet
- Biology Standard XII Human Reproduction WorksheetDocument10 pagesBiology Standard XII Human Reproduction WorksheetPriya SinghNo ratings yet
- Placenta and Fetal Membrane-6614Document45 pagesPlacenta and Fetal Membrane-6614Incredible DivineNo ratings yet
- NCM 108 - Nursing Care During Normal Pregnancy and Care of The Developing FetusDocument5 pagesNCM 108 - Nursing Care During Normal Pregnancy and Care of The Developing FetusKristine BartsNo ratings yet
- BIOCHEMISTRY EXAMDocument7 pagesBIOCHEMISTRY EXAMchristinejoanNo ratings yet
- Levels of Organization PPT - 1314Document9 pagesLevels of Organization PPT - 1314HafserhNo ratings yet
- Structural Organisation in Animals Mind MapDocument3 pagesStructural Organisation in Animals Mind MapAstha AgrawalNo ratings yet
- Water Vascular System of AsteriasDocument3 pagesWater Vascular System of AsteriasCyanDes50% (2)
- Evidences of Evolution Activity SheetsDocument8 pagesEvidences of Evolution Activity SheetsVena Grace MendezNo ratings yet
- Biokemistri Volume 32, Number 1Document95 pagesBiokemistri Volume 32, Number 1Clement BewajiNo ratings yet
- Roitt'S Essential Immunology 12Th Edition (All Mcqs With Answers)Document100 pagesRoitt'S Essential Immunology 12Th Edition (All Mcqs With Answers)Kiran Krupa100% (6)
- Antiadrenergic Drugs 23.07.018 PDFDocument23 pagesAntiadrenergic Drugs 23.07.018 PDFHitesh karnNo ratings yet
- Knruhs 2022 1ST Proff Regular - 240111 - 005627Document12 pagesKnruhs 2022 1ST Proff Regular - 240111 - 005627ranjanavnish142No ratings yet
- Understanding Sars-Cov-2-Induced Systemic Amyloidosis: BiorxivDocument4 pagesUnderstanding Sars-Cov-2-Induced Systemic Amyloidosis: BiorxivAntonisNo ratings yet
- Sheehan's Syndrome PathophysiologyDocument2 pagesSheehan's Syndrome PathophysiologyirismgallNo ratings yet
- Shivering and Neuraxial AnesthesiaDocument12 pagesShivering and Neuraxial AnesthesiaKarla Albert ReyesNo ratings yet
- ER Farmer Organophosphate Poisoning TreatmentDocument4 pagesER Farmer Organophosphate Poisoning TreatmentjuanNo ratings yet
- Bio X Control and Coordination AssignmentDocument2 pagesBio X Control and Coordination AssignmentdevanshiNo ratings yet
- Physical Science Report (Glenn Trono)Document17 pagesPhysical Science Report (Glenn Trono)Glenn TronoNo ratings yet
- CH 8 BOOK PDFDocument22 pagesCH 8 BOOK PDFAshlye LunaNo ratings yet
- AMORC Index Degrees 5 and 6Document48 pagesAMORC Index Degrees 5 and 6Alois HaasNo ratings yet
- Physiology RAASDocument3 pagesPhysiology RAASAulia Mahya FaradisaNo ratings yet
- Student Exploration: Cell Structure: Vocabulary: Cell Membrane, Cell Wall, Centriole, Chloroplast, Cytoplasm, EndoplasmicDocument5 pagesStudent Exploration: Cell Structure: Vocabulary: Cell Membrane, Cell Wall, Centriole, Chloroplast, Cytoplasm, EndoplasmicDhyanesh K.B100% (1)
- Psychology Paper 1 TZ1 HLSL MarkschemeDocument10 pagesPsychology Paper 1 TZ1 HLSL MarkschemeWanna One HatsuneNo ratings yet
- Jurnal UtamaDocument9 pagesJurnal UtamarekaNo ratings yet