Professional Documents
Culture Documents
Dialyzer Reuse For Dialysis
Uploaded by
AndriKusuma100%(3)100% found this document useful (3 votes)
3K views25 pagesOriginal Title
Dialyzer reuse for dialysis PPT.pptx
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
100%(3)100% found this document useful (3 votes)
3K views25 pagesDialyzer Reuse For Dialysis
Uploaded by
AndriKusumaCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 25
DIALYZER REUSE FOR DIALYSIS
Patients on hemodialysis are often surprised to
learn that the complex dialysis machine next to
them on the dialysis floor isnt the device thats
cleaning their blood of excess wastes and fluid.
Instead, a filter, called a dialyzer that is about a
foot long, encased in plastic and inserted into a
holder on the front or side of the dialysis
machine, is actually doing the work of cleaning
the blood. The dialysis machine supports the
work of the dialyzer with pumps, heaters, safety
monitors and alarms.
Dialyzer reuse has been practiced in the
United States since the early 1960s.
Patients who choose to reuse their dialyzers
are given an individual dialyzer that they will
continue to use for the number of times
specified by their doctor or until it is no longer
efficient.
Patients do not share dialyzers; each
patient has his or her own.
What is a dialyzer and how is
it reused?
A dialyzer is often referred to as an artificial
kidney. Its function is to remove the excess
wastes and fluid from the blood, when the
patients kidneys can no longer perform that
task.
Dialyzers are made of a thin, fibrous material.
The fibers form a semipermeable membrane,
which allows smaller particles and liquids to pass
through. The dialyzer is encased in a sealed
plastic cylinder about a foot long and
approximately two to three inches in diameter
with openings at the top and bottom.
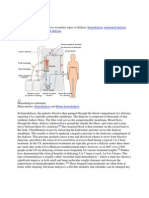
During treatment dialysate (dialysis solution)
and your blood flow through the dialyzer (but
they never touch).
Fresh dialysate from the machine enters your
dialyzer through one opening and blood
enters through the other. Wastes are filtered
out of your blood into the dialysate. Dialysate
containing waste products leaves the dialyzer
and is washed down the drain, while the
cleaned blood goes back into your body.
There are different sizes of dialyzers. These
sizes are related to the blood volume that will
go through them, which depends on the
patient's size and weight. Your kidney doctor
will prescribe the right-sized dialyzer for you.
Dialyzers can remain functional after more than
one use, which is why many facilities reuse them.
Dialyzers are reused for a certain number of
times or until it no longer works efficiently,
whichever comes first.
Each doctor sets his or her own policy for the
maximum number of reuses. Some dialysis
facilities do not reuse dialyzers, and patients at
those facilities are given new dialyzers for each
hemodialysis session.
Patients are given the choice of whether or
not to reuse their dialyzers.
Facilities that reuse must follow strict
guidelines to ensure the reused dialyzers are
labeled with the patients name, cleaned
properly, sterilized and working so the
patient can have an optimal dialysis
treatment.
How is reuse performed?
Patients only reuse their own dialyzer, meaning
that no other patient has or will ever use it.
Dialyzers are never shared between patients.
After your dialysis session is complete, a facility
member (either your renal nurse or a patient care
technician) will take you off the dialysis machine
and seal your dialyzer, which is labeled with your
name, in a plastic bag.
The dialyzer is then sent to a reuse technician
who will follow strict procedures to make sure
your dialyzer is clean, sterile and in good working
condition before you use it again.
The reuse technician will first do a visual
inspection of the dialyzer for blood or fiber
clots. The technician will also note the
number of times the dialyzer has been used.
If the dialyzer is due to be replaced, the
technician will replace it with a new one in the
size prescribed by the physician. If the
dialyzer can be reused, the technician will
place it into the reuse machine to start the
cleaning process.
Reprocessing technique
The major steps in dialyzer reprocessing are
rinsing, cleaning, measuring dialyzer
performance, disinfecting/sterilizing, and
removing germicides
Cleaning
Water, A prolonged rinse with
reverse-osmosis water followed
by reverse ultrafiltration has
been shown to be an effective
means of cleaning dialyzers
without the addition of
chemicals.
Cleaning
Bleach. Sodium hypochlorite (bleach), diluted
to 0.6% or less, dissolves proteinaceous
deposits that may occlude fibers. Bleach
increases albumin losses in high-flux cellulose
triacetate (CT 190) and
polysulfonepolyvinylpyrrolidone (F80B)
dialyzers. Albumin losses are generally not
clinically significant unless bleach is used on
high-flux membranes with exceptionally high
water permeability.
The reuse machine cleans the dialyzer using
water treated with reverse osmosis. This
water is highly purified and cleans the
dialyzer without leaving traces of particles
and chemicals.
After cleaning, the machine performs a
pressure test and blood volume test.
The pressure test checks for any holes in the
dialyzer. The blood volume test ensures that the
dialyzers capacity is above 80% of the dialyzers
stated size.
If there are any holes in the dialyzer, or if the
blood volume is less than 80% of the dialyzers
size, it is replaced with a new one. If any
problems are detected during the reuse test, the
reuse machine indicators let the reuse technician
know, and the dialyzer is disposed of in the
proper manner.
After the reuse machine has cleaned and
tested the dialyzer, it will then be filled with
disinfectant and stored for at least 11 hours.
Just before the patients next dialysis
treatment, the dialyzer is rinsed with saline
solution until all disinfectant is removed.
A test is performed to make sure no
disinfectant is left in the dialyzer. Once it is
tested, the dialyzer is ready to use for the
dialysis treatment.
Is reuse safe?
Various studies have examined the issue of
reuse. These studies have found that the
mortality rate between patients who reuse
dialyzers and patients who do not was the
same.
Dialysis facilities that reuse dialyzers must follow
strict guidelines set forth by the Association for
the Advancement of Medical Instrumentation
(AAMI). The AAMI guidelines make provisions for
patient safety, among them:
A dialyzer must be clearly labeled with the patients
name and only used for the same patient.
A dialyzer must be tested after each use to make sure
it is working properly.
A dialyzer must be tested after rinsing for any traces of
disinfectant that may remain.
Patients must be monitored for any reactions due to
reuse.
Does reuse affect dialysis
outcomes?
Different factors can affect your Kt/V and
URR (urea reduction ratio), standard
measures of how effective your dialysis
treatments are. Although reuse may affect
Kt/V and URR levels, following the correct
standards of reuse for monitoring fiber
volumes and testing the reuse dialyzers
makes this a rare issue.
What are the advantages of
reuse?
Reuse can be helpful to the patient and to the
planet.
Patient advantages of reuse Since each dialyzer is
inspected by a reuse technician, the technician can
note any blood clots in the dialyzer and alert a renal
nurse. Blood clots could mean you are not getting
enough heparin, which is a medicine given before
and throughout hemodialysis. Heparin thins the
blood to allow it to pass easily through the dialyzer
and prevent it from clotting, which would reduce the
dialyzers ability to remove wastes and fluid. Blood
clots in the dialyzer may make your dialysis session
less effective and can lower your Kt/V.
Environmental advantages of reuse Dialyzer
reuse helps to reduce negative environmental
consequences in several ways. On average, it
only takes 9.6 reuse dialyzers to treat one
patient for one year, versus an average of 153
single-use dialyzers. The reuse of all dialyzers in a
single year would eliminate the production of up
to 46 million dialyzers and reduce the amount of
medical waste ending up in landfills by more
than 62 million pounds.
Dialyzer reuse also reduces the amount of harmful
toxins created by waste processing. In order to be
properly disposed of, dialyzers first have to go
through a decontamination process requiring they
either be incinerated or microwaved before being
sent to landfills.
When dialyzers are incinerated, the process
produces emissions and ash that have negative
health effects on the surrounding communities.
While the microwave process does not produce
harmful toxins, it does nothing to reduce the amount
of medical waste that ends up in landfills.
By choosing dialyzer reuse, you can
dramatically reduce the negative impact on
the environment. Dialyzer reuse reduces your
carbon footprint, helps relieve America of its
dependence on crude oil, sends less non-
biodegradable waste to landfills and
ultimately benefits the dialysis patient by
keeping costs lower without compromising
clinical outcomes.
What are the disadvantages of
reuse?
If proper procedures are followed for
inspecting, cleaning and disinfecting your
dialyzer, you should have no problems. If the
reuse procedure is not followed properly you
may have problems with your Kt/V levels or a
physical reaction. However, these problems
are rare, and because you are being closely
monitored during treatment, if these issues
arise, they can be resolved quickly.
HATUR NUHUN
You might also like
- HemodialysisDocument28 pagesHemodialysischarlenetan18100% (6)
- DialysisDocument25 pagesDialysisDivya Sridharan100% (4)
- How Haemodialysis WorksDocument19 pagesHow Haemodialysis WorksMaxence KouessiNo ratings yet
- HEMODIALYSISDocument7 pagesHEMODIALYSISClarisse ReyesNo ratings yet
- Renal Replacement Therapies: Hemodialysis and Peritoneal DialysisDocument86 pagesRenal Replacement Therapies: Hemodialysis and Peritoneal DialysisSabita Tripathi100% (2)
- Hemodialysi S: Ariane Jake C. Fernandez, RN, MSNDocument37 pagesHemodialysi S: Ariane Jake C. Fernandez, RN, MSNMicah Alexis Candelario100% (3)
- Hemodialysis, Phosphorus and Calcium, Peritoneal DialysisDocument29 pagesHemodialysis, Phosphorus and Calcium, Peritoneal DialysisTrizha MaeNo ratings yet
- Dialysis PrescriptionDocument23 pagesDialysis PrescriptionMercy Juliana Jacqualine100% (1)
- DialysisDocument34 pagesDialysisdaisy100% (2)
- Care For Hemodialysis Patients: Pre, During, Post Dialysis CareDocument18 pagesCare For Hemodialysis Patients: Pre, During, Post Dialysis CareHemanth PrakashNo ratings yet
- Anticoagulation On DialysisDocument52 pagesAnticoagulation On DialysisFey100% (1)
- Myths of Dialysis: Understanding Treatment OptionsDocument26 pagesMyths of Dialysis: Understanding Treatment OptionsSijo Muthukad M100% (1)
- Dialysis PresentationDocument21 pagesDialysis PresentationRon Anderson100% (1)
- DIALYSISDocument6 pagesDIALYSISJobelle AcenaNo ratings yet
- DialysisDocument5 pagesDialysisAnusha Verghese100% (1)
- Diabetic NephropathyDocument21 pagesDiabetic NephropathyNugroho HarsonoNo ratings yet
- KDOQI Clinical Practice Guideline Hemodialysis Update - Public Review Draft FINAL - 20150204 PDFDocument78 pagesKDOQI Clinical Practice Guideline Hemodialysis Update - Public Review Draft FINAL - 20150204 PDFศักดิ์ชัย พูนศรีเจริญกุลNo ratings yet
- TypesDocument3 pagesTypesProser Faith TabaculdeNo ratings yet
- Dialysis: Acute Dialysis Is Indicated When There Is A High and Rising Level of SerumDocument19 pagesDialysis: Acute Dialysis Is Indicated When There Is A High and Rising Level of SerumMJ Amarillo100% (1)
- HemodialysisDocument19 pagesHemodialysisK.R.Raguram88% (26)
- Hemodialysis Delivery SystemDocument6 pagesHemodialysis Delivery SystemShemae Quilacio100% (2)
- Renal Replacement TherapyDocument50 pagesRenal Replacement TherapyMalueth Angui100% (1)
- Dialysis BasicsDocument23 pagesDialysis Basicsdidik_sugiarto_2100% (1)
- Peritoneal Dialysis SeminarDocument25 pagesPeritoneal Dialysis SeminardrresmiajithNo ratings yet
- DIALYSIS ReportingDocument10 pagesDIALYSIS ReportingGlenelyn Grace InfanteNo ratings yet
- Complications of DialysisDocument7 pagesComplications of DialysisDilessandro PieroNo ratings yet
- Dialysis Notes 1Document3 pagesDialysis Notes 1SarahSigrid87% (23)
- Renal NursinglDocument36 pagesRenal NursinglgireeshsachinNo ratings yet
- 5 - Cleaning and Disinfection of Dialysis Water Equipment - Final - 2012Document7 pages5 - Cleaning and Disinfection of Dialysis Water Equipment - Final - 2012Denisse Ro100% (1)
- Haemo DialysisDocument52 pagesHaemo DialysisPam Atienza MagtibayNo ratings yet
- Renal TransplantationDocument33 pagesRenal TransplantationRohini Rai100% (1)
- BloodDocument49 pagesBloodvruttika parmar100% (3)
- Peritoneal DialysisDocument56 pagesPeritoneal DialysisVanet100% (1)
- DIALYSIS ProcedureDocument8 pagesDIALYSIS ProcedureRaman SamraoNo ratings yet
- Anti DiureticsDocument16 pagesAnti DiureticsPuneethgowda.G.K Puneeth50% (2)
- Top Dialysis Training CentersDocument6 pagesTop Dialysis Training CenterssakuraleeshaoranNo ratings yet
- DIALYSISDocument51 pagesDIALYSISEdwin Jose S100% (1)
- DialyzerDocument10 pagesDialyzerfatima rasheedNo ratings yet
- Dialysis Notes: Types, Indications, and ComplicationsDocument3 pagesDialysis Notes: Types, Indications, and ComplicationsLucelle ArellanoNo ratings yet
- Notes Liver CirrhosisDocument10 pagesNotes Liver CirrhosisSanthu SuNo ratings yet
- Eye Banking OphthalmologyDocument21 pagesEye Banking Ophthalmologyvivekrajbhilai5850100% (2)
- Infusing Total Parenteral Nutrition (TPN) - 1Document16 pagesInfusing Total Parenteral Nutrition (TPN) - 1Jan Federick BantayNo ratings yet
- Nursing Management Objective-NDocument3 pagesNursing Management Objective-NRajaNo ratings yet
- Guidelines for administering RituximabDocument9 pagesGuidelines for administering RituximabMonica MonikaNo ratings yet
- Essential Blood Bank ServicesDocument21 pagesEssential Blood Bank ServicesPriti Thakur100% (3)
- Infection Control Protocol in IcuDocument63 pagesInfection Control Protocol in IcuindraNo ratings yet
- Core Curriculum for Dialysis NursesDocument7 pagesCore Curriculum for Dialysis Nursesgreen_archerNo ratings yet
- Testing Specimen For Sugar & Nursing ResponsibilitiesDocument11 pagesTesting Specimen For Sugar & Nursing ResponsibilitiesrnrmmanphdNo ratings yet
- Guidelines For Patients On Chronic Haemodialysis Programme QehbDocument33 pagesGuidelines For Patients On Chronic Haemodialysis Programme QehbRhys Espinosa100% (2)
- Dialyzer: by Daniel V Dialysis LecturerDocument52 pagesDialyzer: by Daniel V Dialysis LecturerDani Dany100% (2)
- Fluids and Electrolytes NCM 101Document142 pagesFluids and Electrolytes NCM 101France John Evangelista Torres100% (2)
- Hemodialysis Adequacy DwiDocument27 pagesHemodialysis Adequacy Dwiryo_ninukNo ratings yet
- Haemodialysis in ChildrenDocument38 pagesHaemodialysis in ChildrenValliammalShanmugam75% (8)
- The Icn Code of Ethics For NursesDocument17 pagesThe Icn Code of Ethics For NursesSanjay Kumar Sanju100% (1)
- DACUM Competency Profile For Hemodialysis TechnicianDocument5 pagesDACUM Competency Profile For Hemodialysis Technicianmanishbabu100% (1)
- Hemodialysis and Peritoneal DialysisDocument57 pagesHemodialysis and Peritoneal Dialysisirene joy91% (11)
- Dialysis: Edna Co RN ManDocument37 pagesDialysis: Edna Co RN ManMary Shine GonidaNo ratings yet
- B.Reprocessing of DialyzerDocument4 pagesB.Reprocessing of DialyzerKyara Mara Gabrielle AnditNo ratings yet
- What You Should Know About Dialyzer Reuse: A Guide For Hemodialysis Patients and Their FamiliesDocument8 pagesWhat You Should Know About Dialyzer Reuse: A Guide For Hemodialysis Patients and Their FamiliesDewiyanti TodingNo ratings yet
- HemaDocument10 pagesHemaハンター ジェイソンNo ratings yet
- Acute N Chronic Complication of HD - YennyDocument77 pagesAcute N Chronic Complication of HD - YennyAndriKusumaNo ratings yet
- Anticoagulant TherapyDocument47 pagesAnticoagulant TherapyAndriKusuma75% (4)
- DialysisDocument14 pagesDialysisAndriKusumaNo ratings yet
- Dialyzer Reuse For DialysisDocument25 pagesDialyzer Reuse For DialysisAndriKusuma100% (3)
- Dialyzer Reuse For DialysisDocument25 pagesDialyzer Reuse For DialysisAndriKusuma100% (3)
- Medication Safety Anticoagulation ManagementDocument39 pagesMedication Safety Anticoagulation ManagementAndriKusumaNo ratings yet
- Acute N Chronic Complication of HD - YennyDocument77 pagesAcute N Chronic Complication of HD - YennyAndriKusumaNo ratings yet
- Anticoagulant TherapyDocument47 pagesAnticoagulant TherapyAndriKusuma75% (4)
- Composition and Regulation of Body FluidsDocument32 pagesComposition and Regulation of Body FluidsAndriKusumaNo ratings yet
- CAPD Pelatihan, 15 April 2011Document66 pagesCAPD Pelatihan, 15 April 2011AndriKusumaNo ratings yet