Professional Documents
Culture Documents
Oral Manifestations of Viral Infections: CPD Article
Oral Manifestations of Viral Infections: CPD Article
Uploaded by
Henry KeefeOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Oral Manifestations of Viral Infections: CPD Article
Oral Manifestations of Viral Infections: CPD Article
Uploaded by
Henry KeefeCopyright:
Available Formats
CPD Article
Oral manifestations of
viral infections
Van Heerden WFP, BChD, MChD (Oral Path), FC Path (SA) Oral Path, PhD, DSc
Department of Oral Pathology and Oral Biology, University of Pretoria
Correspondence to: Prof Willie van Heerden, e-mail: wvheerd@medic.up.ac.za
Abstract
Examination of the oral cavity is an integral part of every clinical examination. The clinical presentation of various viral
conditions is discussed in this article and will provide the family practitioner with an up to date guide to better diagnosis
and management.
SA Fam Pract 2006;48(8): 20-24
Introduction
Viral infections of the oral mucosa are
frequently encountered in general practice. The clinical diagnosis of these lesions can sometimes be confusing due
to similar clinical presentations. The
clinical presentation, diagnosis and
appropriate management of common
viral infections of the oral mucosa are
discussed.
Herpes simplex virus
Primary herpetic gingivostomatitis
The infection that accompanies primary
herpetic gingivostomatitis is usually
subclinical in early childhood and only a
small percentage of patients develop an
acute primary infection. This usually occurs in older children and consists of fever, malaise, headache, cervical lymphadenopathy and a vesiculo-ulcerative
eruption on the peri-oral skin, vermilion
or any intra-oral mucosal surface.1 The
vesicles, which are 2 to 3 mm in diameter, rupture, leaving painful ulcers
that heal without scarring after seven to
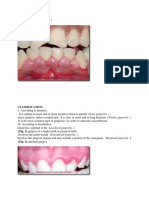
ten days. The gingivae are swollen and
reddish due to a general inflammation
(see Figure 1). The virus then migrates
to the trigeminal ganglion, where it remains latent. In more affluent countries
with better living conditions and less
overcrowding, many young adults do
not acquire the infection during childhood. They are at risk of developing a
symptomatic infection as an adult, usually presenting as a pharyngotonsillitis,
with constitutional symptoms of fever,
malaise and headaches. In the case of
cervical lymphadenopathy, the vesicles
and ulcers on the tonsils and posterior
20
pharynx can resemble infectious mononucleosis or a streptococcal sore
throat infection. Primary infection in an
immunocompromised adult can be life
threatening, with disseminated disease,
or it may present with extensive nonhealing oral ulceration.2
Figure 2: Herpes labialis, consisting of a
cluster of vesicles on the vermillion (arrow).
Figure 1: Primary herpetic gingivostomatitis
resulting in painful erythematous palatal gingivae (arrows).
Secondary herpes labialis
Around 15 to 30% of the community is
affected by episodes of secondary herpes simplex lesions (herpes labialis).
Common colds, influenza, fever, UV
exposure, menstruation, emotional upset, stress and anxiety predispose the
patient to recurrent infection, as these
cause reactivation of the virus, which
subsequently migrates along one of
the sensory divisions of the trigeminal
nerve. The lesions are most often seen
at the mucocutaneous junction of the
lip or peri-oral skin (see Figure 2). A
burning sensation usually precedes
the development of a small cluster of
vesicles. These vesicles enlarge, coalesce, ulcerate and become crusted
before healing within 10 days.
Diagnosis and management
The clinical features are usually sufficient to diagnose these conditions. The
differential diagnosis of primary herpetic gingivostomatitis includes recurrent
aphthous ulceration, which forms ulcers
on non-keratinised oral mucosa without
a vesicle phase.
There currently is no drug available
to prevent the migration of the herpes
virus to the trigeminal ganglion after
primary infection. Acyclovir is a potent
drug and may be life saving for herpetic encephalitis and disseminated infection, especially in those individuals who
are immuno-compromised. It will accelerate healing if used sufficiently early in
the disease stage. Bed rest, fluids and
a soft diet, with antipyretics for fever,
are recommended for primary herpetic gingivostomatitis. Preventative therapy, such as using sun block, is the
management of choice for herpes labialis, while antiviral drugs such as acyclovir are only useful if applied at the
prodromal stage before the development of vesicles.3 Patients must be
discouraged from touching the lesions
SA Fam Pract 2006:48(8)
CPD Article
in order to reduce the risk of spreading the infection to other sites. Systemic acyclovir may be used for immunocompromised individuals.1
Varicella-zoster virus
Chickenpox (varicella) results from primary infection, while reactivation of the
virus is known as herpes zoster (shingles). Intra-oral vesicles of varicella,
when present, are seen on the tongue,
buccal mucosa, gingival, palate and
oropharynx. They generally are not
very painful. Following the primary
infection, the virus is transported via
the sensory nerves to the dorsal spinal
ganglia or trigeminal ganglion, where it
remains latent.
A number of predisposing factors
can lead to a recurrence of the infection
in the tissue supplied by the sensory
nerve. Conditions leading to herpes
zoster are usually those that cause immunosuppression, such as cytotoxic
drugs, radiation, internal malignancies,
malnutrition, old age, and alcohol and
substance abuse. Occasionally, dental
manipulation in a localised area can
lead to reoccurrence. The first signs of
herpes zoster are pain and tenderness
in the dermatome corresponding to the
affected sensory ganglion. In the head
and neck area, vesicles form on one
side of the face or in the oral mucosa
in one of the divisions of N. trigeminus.
These unilateral vesicles form clusters
with areas of surrounding erythema,
ending abruptly in the midline (see
Figure 3). The vesicles ulcerate and
form pustules within three to four days.
A crust lesion then forms, and healing
takes place within seven to ten days.
These lesions often heal with scarring
and areas of hypo/hyperpigmentation
may be seen. When the N. facialis
and N. auditorius are involved (via the
geniculate ganglion), facial paralysis,
vesicles on the external ear, tinnitus,
deafness and vertigo may follow. This
is known as Ramsay-Hunt syndrome.4
Figure 3: Herpes zoster, presenting with
multiple ulcers on the palate. Note the
abrupt ending of the ulcers at the midline
(arrow).
22
Spontaneous bone necrosis of the
mandible, occurring during an acute
attack of herpes zoster, has been seen
in immunocompromised patients.5 The
patients present with the unilateral vesicles of herpes zoster, with subsequent
unilateral exfoliation of the teeth in the
necrotic mandible (see Figure 4).
Figure 5: Herpangina, presenting with
multiple ulcers on the soft palate, uvula and
fauces.
Figure 4: Unilateral necrosis of the mandible (arrow) in an HIV-positive man with a
CD4 count of less than 200.
A residual complication of herpes zoster
is post-herpetic neuralgia. It occurs in
10% of patients with herpes zoster and
affects the trigeminal nerve, most commonly the ophthalmic division. There is
persistent, unilateral pain in the affected
area. A history of previous skin lesions
and possible scarring may aid in the diagnosis. The pain is not paroxysmal, as
is seen in trigeminal neuralgia, although
it may be just as severe.
Diagnosis and management
The clinical picture is often distinctive.
Herpes zoster may be confused with
recurrent Herpes simplex virus infection. Herpes zoster has a longer duration, a more severe prodromal phase,
unilateral vesicles and ulceration, with
abrupt ending at the midline and postherpetic neuralgia.
The treatment is supportive and
symptomatic, with topical or systemic
antipruritics and analgesics that do not
contain aspirin. A high dose of oral acyclovir (800 mg five times daily for seven
days) is recommended for treating both
primary and recurrent infections in immunocompromised patients.6
Coxsackie virus
Herpangina
Herpangina affects children, mainly
during summer, and is characterised
by a sudden onset of malaise, fever
and a sore throat. Patients present
with vesicles, ulcerations, and diffuse
erythema on the soft palate, fauces
and tonsillar areas (see Figure 5). The
systemic symptoms settle in two to three
days and the ulcers heal in seven to ten
days.
Hand, foot and mouth disease
Hand, foot and mouth disease is most
commonly seen amongst children aged
one to five years. In 75% of cases it
presents with an eruption of vesicles
on the palms of the hands and on the
feet. Occasional vesicles may also be
found on the proximal extremities and
buttocks. There are also vesicles in the
anterior part of the mouth (see Figure
6). An associated low-grade fever and
malaise are usually present.
Diagnosis and management
The clinical features of Coxsackie virus
are distinctive. The distribution of the
lesions of herpangina differentiates it
from primary herpetic gingivostomatitis,
which affects the gingivae, whereas
herpangina is an oropharyngitis. The
systemic symptoms differentiate it from
recurrent aphthous ulceration. The vesicles also help to distinguish herpangina from streptococcal pharyngitis.
In the case of hand, foot and mouth
disease, the cutaneous vesicles can
resemble chickenpox; however, in
chickenpox the vesicles usually start
on the face and trunk and then spread
to the extremities. Involvement of the
palms and soles is rare in chickenpox
infections. Oral lesions are also rare in
chickenpox.
Herpangina and hand, foot and
mouth disease are self-limiting, of short
duration and need no treatment. Symptomatic treatment is indicated in very
painful cases of herpangina, in which
case non-aspirin antipyretics and topical anaesthetics can be used.
Human papillomavirus
Focal epithelial hyperplasia (Hecks
disease)
Hecks disease presents with multiple
asymptomatic, slightly elevated, mucosa-coloured, smooth-surfaced nodules that occur on the labial or buccal
mucosa gingivae or tongue of children
(see Figure 7). Individual lesions tend
to be small (0.3 to 1 cm), but they frequently cluster and coalesce, giving the
SA Fam Pract 2006:48(8)
CPD Article
mucosa a cobblestone or fissured surface. Most lesions are found in children,
although they occasionally can be
found in older age groups. They usually
regress spontaneously with age.
Figure 6: Patient with hand, foot and mouth
disease, presenting with (A) intra-oral ulcerations (arrow) secondary to vesicles, with
(B) small vesicles on his palm and fingers
(arrows) and (C) a vesicle on the toe (arrow)
is clearly visible.
Squamous cell papilloma and verruca vulgaris
Squamous papilloma is a slow-growing, solitary, painless, cauliflower-like
lesion with branched finger-like processes (see Figure 8). It can occur at
any age, but is most commonly diagnosed in the age group 30 to 50 years.
It may initially grow rapidly, but seldom
grows beyond 5 mm in diameter. Although any site of the oral cavity may
be affected, the tongue, lips and soft
palate are common locations. The lesion will range from reddish to white,
depending on the degree of surface
keratinisation.
Verruca vulgaris is a very common
childhood infection. Oral lesions usually
arise from autoinoculation, most commonly on the labial mucosa, tongue and
gingiva. It presents as a slow-growing,
painless, exophytic lesion that consists
of sharp, finger-like processes.
Condyloma accuminatum
Condyloma accuminatum is usually
present on the genitals, although it may
be found in the oral cavity. Oral lesions
are predominantly transmitted through
oral-genital sexual contact. It consists of
multiple cauliflower-like lesions, some of
which are larger than 0.5 cm. They may
become as large as 3 cm in size. The
most common intra-oral sites are the
labial mucosa and the lingual frenum
and soft palate.
Diagnosis and management
No treatment is usually required for
focal epithelial hyperplasia, as the nodules undergo spontaneous regression during puberty. Lesions that cause
SA Fam Pract 2006:48(8)
aesthetic problems or are chronically
injured can be removed surgically.
It is often impossible to distinguish
between verruca vulgaris and squamous cell papilloma of the oral mucosa. Excision of both lesions is the treatment of choice.
Condyloma accuminatum should
not be confused with focal epithelial
hyperplasia. It may be difficult to distinguish from squamous cell papilloma,
which is usually single and not larger
than 0.5 cm. Excision is the treatment of
choice. The presence of these lesions
in children should raise the possibility
of sexual abuse, although on rare occasions they may be transmitted by nonsexual contact.7
tous maculopapular skin rash. The
incidence of measles has decreased
dramatically in many communities due
to successful vaccination programs
although it has re-emerged in unvaccinated children, mostly amongst children of poor rural communities. Following an incubation period of 10 to 12
days, a prodromal phase consisting
of fever, malaise, conjunctivitis, cough
and coryza is seen. This is followed
by a generalized exanthematous skin
rash. The oral manifestation of measles
is known as Kopliks spots. These occur early in the course of the infection
and often precede the skin rash by 1
to 2 days. Kopliks spots are white-red
macules on that appear on the buccal and labial mucosa (see Figure 9).
These macules represent foci of epithelial necrosis.8
Figure 9: Kopliks spots on the labial mucosa present as numerous small macules
(arrows).
Figure 7: Focal epithelial hyperplasia at the
mucosa of the corner of the mouth, consisting of multiple, slightly elevated, mucosacoloured nodules.
Diagnosis and management
Diagnosis is based on the clinical
features and history. Laboratory confirmation is possible for atypical cases.
Supportive therapy including bed rest,
fluids, adequate diet and non-aspirin
antipyretics are recommended for
symptomatic relief.
Human immunodeficiency virus
Although no oral lesions are found as
a direct result of HIV infection itself, a
range of HIV-associated oral lesions,
some with a viral aetiology, have been
described.
Figure 8: Squamous papilloma presenting
as a single cauliflower-like lesion (arrow) on
the lingual frenum in an adult.
Measles
Measles, a paramyxovirus infection,
is most commonly seen in children as
an acute febrile illness and erythema-
Oral hairy leukoplakia
This presents as a white, vertically corrugated, non-removable lesion on the
lateral or ventral margin of the tongue
(see Figure 10). The surface might
be non-corrugated if it is seen on the
inferior surface of the tongue or in the
buccal mucosa. This lesion is caused
by the Epstein-Barr virus and has no
premalignant potential. It has also
been reported in HIV-negative persons
23
CPD Article
in association with immunosuppresive
therapy. It must be differentiated from
chronic hyperplastic candidiasis or
leukoplakia (a potentially malignant lesion). A biopsy must be performed to
establish a reliable diag-nosis. Once
the diagnosis has been made, no treatment for the lesion is necessary.
Kaposis sarcoma
Kaposis sarcoma is characterised by
erythematous or violaceous plaquelike lesions that develop into tumorous growths over time (see Figure 11).
These larger lesions may become ulcerated and painful and may interfere
with function. Kaposis sarcoma is predominantly seen in the palate or on the
attached gingivae, but can appear on
other mucosal sites. It has been demonstrated that Kaposis sarcoma is
caused by infection with human herpes virus 8. The clinical diagnosis
should be confirmed by biopsy, as
several other lesions may have similar clinical presentations. This is especially true for early lesions that may
have similar clinical features as vascular malformations, bacillary angiomatosis and even well differentiated angiosarcoma. A variety of treatment options are available varying from intralesional injection of chemotherapeutic or
sclerosing agents to surgery or radiation. Regression of Kaposis sarcoma
has been reported in patients receiving
combination antiretroviral therapy.
in appropriate patient care. Persistent lesions, especially if ulcerated, should be
biopsied to exclude the possibility of a
non-infective, more serious aetiology. Biopsies or other laboratory investigations
should also be performed if a clinical
diagnosis can not be established. This is
especially true in the setting of HIV/AIDS
that can influence the typical clinical features of viral infections.
Figure 10: Oral hairy leukoplakia on the
lateral border of the tongue, with extension onto the smooth ventral aspect of the
tongue (arrow).
See CPD Questionnaire, page 44
P This article has been peer reviewed
References
Figure 11: Kaposis sarcoma of the palate
(arrows) in (A) the early plaque stage and in
(B) the more advanced tumorous phase on
the gingiva (arrows).
Conclusion
Examination of the oral cavity should
routinely be performed as the oral
mucosa is often the first site affected
by viral infections. A thorough medical history together with a detailed
examination will result in an accurate
diagnosis for the majority of viral lesions affecting the oral cavity, resulting
1. McCullough MJ, Savage NW. Oral viral
infections and the therapeutic use of antiviral
agents in dentistry. Aust Dent J 2005;50:S31-5.
2. Schubert MM. Oral manifestations of viral
infections in immunocompromised patients.
Curr Opin Dent 1991;1:384-97.
3. Raborn GW, Grace MG. Recurrent herpes
simplex labialis: selected therapeutic options.
J Can Dent Assoc 2003;69:498-503.
4. Sweeney CJ, Gilden DH. Ramsay-Hunt
syndrome. J Neurol Neurosurg Psychiatry
2001;71:149-54.
5. Van Heerden WF, McEachen SE, Boy SC.
Alveolar bone necrosis and tooth exfoliation
secondary to herpes zoster in the setting of
HIV/AIDS. Aids 2005;19:2183-4.
6. Reusser P. Management of viral infections in
immunocompromised cancer patients. Swiss
Med Wkly 2002;132:374-8.
7. Kui LL, Xiu HZ, Ning LY. Condyloma
acuminatum and human papilloma virus
infection in the oral mucosa of children. Pediatr
Dent 2003;25:149-53.
8. Neville BD, Damm DD, Allen CM, Bouquot JE.
Oral and Maxillofacial Pathology, 2nd ed. WB
Saunders Co, Philadelphia 2002.
ATROVENT 20 HFA : The first CFC-free Ipratropium Bromide
Boehringer-Ingelheim is proud to announce the launch of the new ATROVENT 20 HFA metered dose inhaler
which will replace the existing ATROVENT 40 inhaler once stocks are
depleted.
The availability of ATROVENT 20 HFA
is in line with Boehringer-Ingelheims
commitment to provide effective and
affordable alternatives to CFC-containing
inhalers.
ATROVENT 20 HFA is indicated for
the relief of symptoms associated with
asthma and COPD. Each 20 l metered
dose (puff) contains 0,021 mg ipratropium bromide and it will be necessary
to adjust the patients dosage accordingly.
24
Patients using ATROVENT 20 HFA for
the first time might notice that the taste
is slightly different from that of the CFCcontaining ATROVENT 40 metered
dose inhaler. This is due to the limited
amount of alcohol needed to dissolve
the active ingredients. Patients should
be made aware of this when changing
from one formulation to the other.
ATROVENT 20 HFAs introduction
highlights
Boehringer-Ingelheims
commitment to provide high quality,
research-based, affordable products to
the healthcare market in South Africa.
For further information please contact
Cumi Pretorius on (011) 348 2400
or email pretoriusc@jnb.boehringeringelheim.com
SA Fam Pract 2006:48(8)
You might also like
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (844)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5811)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1092)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- 10 Essential Guitar Scales For BeginnersDocument10 pages10 Essential Guitar Scales For Beginnerstep kosal100% (1)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Mise en Scene (Inc Lighting)Document41 pagesMise en Scene (Inc Lighting)Dee WatsonNo ratings yet
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Douay Rheims 1610 BibleDocument2,872 pagesDouay Rheims 1610 BibleOrthodox Voices100% (3)
- 6th Central Pay Commission Salary CalculatorDocument15 pages6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- Restorative Dentistry Board QSDocument67 pagesRestorative Dentistry Board QSDonto83% (6)
- EndoDocument61 pagesEndodeenm100% (2)
- Gingival InflammationDocument12 pagesGingival InflammationdeenmNo ratings yet
- RPD Review QuestionsDocument85 pagesRPD Review Questionsdeenm67% (3)
- Spanish Football Federation Soccer Camps in Madrid, SpainDocument7 pagesSpanish Football Federation Soccer Camps in Madrid, SpainKerine HeronNo ratings yet
- BLRDocument7 pagesBLRNityanad ChoudharyNo ratings yet
- Jacky - S Electronics Uae2018Document1 pageJacky - S Electronics Uae2018dyeaayaser5No ratings yet
- 2016 Anesthesia Use GuidelinesDocument12 pages2016 Anesthesia Use GuidelinesdeenmNo ratings yet
- Oral Squamous Cell CarcinomaDocument10 pagesOral Squamous Cell CarcinomadeenmNo ratings yet
- Plaque FluidDocument7 pagesPlaque FluiddeenmNo ratings yet
- 63.a Child With A Swollen FaceDocument4 pages63.a Child With A Swollen FacedeenmNo ratings yet
- Self Study Intraoral Anatomy RadiologyDocument80 pagesSelf Study Intraoral Anatomy RadiologydeenmNo ratings yet
- 21.trauma To An Immature IncisorDocument4 pages21.trauma To An Immature IncisordeenmNo ratings yet
- Teeth Eruption and Calcification ChartDocument1 pageTeeth Eruption and Calcification ChartdeenmNo ratings yet
- Endo PerioDocument2 pagesEndo PerioMohammed OmoshNo ratings yet
- Capital Punishment in The PhilippinesDocument27 pagesCapital Punishment in The PhilippinesLaine KimNo ratings yet
- Interior Design SyllabusDocument5 pagesInterior Design SyllabusNupur BhadraNo ratings yet
- An Overview On Biological Effect of Trace-Element in Substituted Calcium PhosphateDocument4 pagesAn Overview On Biological Effect of Trace-Element in Substituted Calcium PhosphateSaiful FirdausNo ratings yet
- Utah State Football Signing Class of 2016Document9 pagesUtah State Football Signing Class of 2016WordofgreenNo ratings yet
- Herbert W Armstrong Library and ArchivesDocument4 pagesHerbert W Armstrong Library and ArchivesTim KitchenNo ratings yet
- Subsquid Testnet Coinlist CoDocument9 pagesSubsquid Testnet Coinlist Cojejemeyy100% (1)
- Annexure-123. (B.Sc. (H) Microbiology)Document125 pagesAnnexure-123. (B.Sc. (H) Microbiology)revathidadam55555No ratings yet
- Past Papers IGCSE 2023 21Document8 pagesPast Papers IGCSE 2023 21David ThydetNo ratings yet
- Binomial Distribution Basics - 1Document3 pagesBinomial Distribution Basics - 1manjushreeNo ratings yet
- LBT .No VAT .No. Dealer NameDocument303 pagesLBT .No VAT .No. Dealer NameShashi SukenkarNo ratings yet
- What Are The 25 Consonant SoundsDocument3 pagesWhat Are The 25 Consonant SoundsvidyapostNo ratings yet
- Project Currency Converter JavaDocument16 pagesProject Currency Converter JavaHARESH.SNo ratings yet
- Technical CollegesDocument228 pagesTechnical CollegesRupak TiwariNo ratings yet
- ABE - Law Summary RA.8559Document2 pagesABE - Law Summary RA.8559Jefrey M. ButilNo ratings yet
- X-Final Syllabus 2018-19Document159 pagesX-Final Syllabus 2018-19Huba ZehraNo ratings yet
- Full Merchant Shipping Act Plus AmendmentsDocument245 pagesFull Merchant Shipping Act Plus AmendmentsVaishnavi JayakumarNo ratings yet
- Chapter 3 - Rules On Gross Gift (Notes)Document11 pagesChapter 3 - Rules On Gross Gift (Notes)Angela Denisse FranciscoNo ratings yet
- Dinacell LoadweigherDocument24 pagesDinacell LoadweigherkieranNo ratings yet
- Affidavit For Change of Color Thru Mechanic - SampleDocument2 pagesAffidavit For Change of Color Thru Mechanic - SampleDaisy Jean CaballesNo ratings yet
- History of State Bank of IndiaDocument5 pagesHistory of State Bank of IndiaanilllllNo ratings yet
- Cascading New Knowledge and The Teacher Tote Video TranscriptDocument2 pagesCascading New Knowledge and The Teacher Tote Video TranscriptEllaine Krizha CulalicNo ratings yet
- T1752 Bid TabDocument17 pagesT1752 Bid TabBakhtiar KianiNo ratings yet
- ADM - Masonry - Q1 - M2Document23 pagesADM - Masonry - Q1 - M2joanduermeNo ratings yet
- Lab Act 11Document8 pagesLab Act 11angelica sherinnNo ratings yet