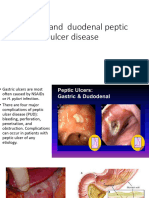
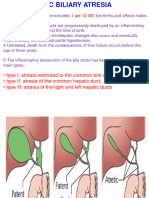
Professional Documents
Culture Documents
Management of Liver Abscess: Anita Dutta,, Sanjay Bandyopadhyay
Uploaded by
SMB8Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Management of Liver Abscess: Anita Dutta,, Sanjay Bandyopadhyay
Uploaded by
SMB8Copyright:
Available Formats
Management of Liver Abscess
9:4
Anita Dutta, Kishangunj, Sanjay Bandyopadhyay, Kolkata
INTRODUCTION
Liver is an important and vital organ of the body. This organ is subjected to numerous systemic
infections viral, bacterial and parasitic and lies at the distal end of the portal circulation; it is therefore
bathed with portal blood containing viruses, bacteria parasites, ova, products of digestion and other
antigens.1
Hepatic or liver abscesses are infectious, space-occupying lesions in the liver; the two most common
abscesses being pyogenic and amoebic. Pyogenic liver abscess (PLA) is a rare but potentially lethal
condition, with a reported incidence of 20 per 1,00,000 hospital admissions in a western population.2
Its severity depends on the source of the infection and the underlying condition of the patient. Amoebic
liver abscesses (ALA) are common in tropical regions mainly where Entamoeba histolytica is
endemic and is more prevalent in individuals (mostly young males) with suppressed cell mediated
immunity.3
In both the types of hepatic abscesses, right lobe of the liver is the most likely site of infection. The
clinical presentation of both the types may be elusive with combination of fever, right upper quadrant
pain and hepatomegaly with or without jaundice.
PYOGENIC LIVER ABSCESS (PLA)
Etiology
Over the past 50 years, there has been a major shift in the etiology of PLA. PLA may be of biliary,
portal, arterial, or traumatic origin (Table 1). Ascending infection of the biliary tree secondary to
obstruction is now the most identifiable cause of PLA. The etiology of biliary obstruction has some
geographic differences: in Western countries this scenario is common in patients with malignant
disease,4 while in Asia, gall stone disease and hepatolithiasis are more common.5 Between 15 to
55% patients in different series, no identifiable cause or source for PLA was found (hence called
cryptogenic).4-6 There is an increase in the median age of patients with PLA in recent years, that is
mostly responsible for increased severity and mortality in spite of advancement in antibiotic therapy.6,7
Clinical presentation:
Early symptoms during the onset of a PLA are non-specific and include malaise, nausea, anorexia and weight loss, headaches, myalgia, and arthralgia in most of the cases.
These prodromal symptoms may be present for many weeks before the appearance of more
specific symptoms, such as fever, chills and abdominal pain, although the pain is not always
localized to the right upper quadrant.
An abscess adjacent to the diaphragm may cause pleuritic type pain, cough and dyspnea, and
when this presentation is associated with the above-mentioned non-specific symptoms, it can
cause diagnostic difficulty.
Septic shock may occur in a few patients, especially in the setting of an obstructed biliary tree.
469
Medicine Update 2012 Vol. 22
Table 1: Common causes of pyogenic liver abscess
Hepatobiliary
Benign
Lithiasis
Cholecystitis
Biliary enteric anastomosis
Endoscopic biliary procedures
Percutaneous biliary procedures
Malignant
Common bile dust
Gall bladder
Ampulla
Head of pancreas
Portal
Fig. 1 : CT scan of liver showing multiple hypodense lesions
suggestive of pyogenic abscess
Benign
Diverticulitis
Anorectal suppuration
Pelvic suppuration
Postoperative sepsis
Intestinal perforation
Plain abdominal and chest radiographs are usually too
non-specific to be diagnostic.
Ultrasound (USG) is the imaging modality used in the
initial evaluation. The appearance on USG varies according to the stage of evolution of the abscess.8 Initially the abscess is hyperechoic and indistinct, but with
maturation and pus formation, it becomes hypoechoic
with a distinct margin. When the pus is very thick, a
fluid-containing lesion may be confused with a solid lesion on USG. USG has a sensitivity of 75% to 95%, but
has difficulty in detecting an abscess high in the dome of
the right hemiliver and especially multiple small PLAs.
By showing gallstones, dilated bile ducts, and hepatolithiasis, USG has the advantage of imaging underlying
biliary tract pathology.
A computed tomography (CT) scan is more accurate
than USG in the differentiation of PLA from other liver
lesions and is reported to have a sensitivity of approximately 95%.8 The portal venous phase using intravenous
contrast material gives the best differentiation between
the liver and the abscess, with the periphery of the PLA
having contrast enhancement as opposed to non-enhancement of the central portion (Figure 1).
Magnetic resonance imaging (MRI) does not seem to
have any advantage over CT or USG.
The spectrum of organisms that may be cultured in PLA
is listed in Table 2. E. coli is cultured most frequently in
Western series9,10 and Klebsiella in Asian series.6,7
Pancreatic abscess
Appendicitis
Inflammatory bowel disease
Malignant
Colonic cancer
Gastric cancer
Arterial
Endocarditis
Vascular sepsis
ENT infection
Dental infection
Traumatic
Benign
Open or closed abdominal trauma
Malignant
Chemoembolization
Percutaneous ethanol injection or radiofrequency
Cryptogenic
Although uncommon, some patients present with peritonitis after free rupture of an abscess into the peritoneal
cavity.
Diagnosis:
Laboratory investigations show an elevated white cell
count, anaemia, hypoalbuminemia, elevated transaminases and alkaline phosphatase. Hyperglycemia may be
the first indication that the patient is diabetic or there is
loss of control because of septic process.
Management of pyogenic liver abscess
(PLA)
The principles of treatment are to
470
Management of Liver Abscess
the same time.
Table 2: Spectrum of microorganisms causing pyogenic liver
abscess
Clinicians have questioned when should the primary treatment
be aspiration alone and when should a percutaneous catheter
drain be inserted. Percutaneous needle aspiration (PNA)
group has a high success rate and a shorter hospital stay,
but a large percentage requires second or third aspirations to
achieve success.12 When PNA fails, catheter drainage should
be performed.
Gram-negative aerobes
Escherichia Coli
Klebsiella pneumoniae
Pseudomonas aeruginosa
Proteus spp.
Citrobacter freundii
Streptococcus milleri
Primary treatment by percutaneous catheter drainage (PCD)
is performed when:
Staphylococcus aureus
Enterococcus spp.
The pus is too thick to be aspirated
The abscess is greater than 5 cm in diameter
Gram positive aerobes
Gram negative anaerobes
Bacteroides spp
The wall is thick and non-collapsible
Fusobacterium spp.
The PLA is multi-loculated
Gram positive anaerobes
The use of PCD is not precluded by the presence of multiple
abscess cavities, but this does necessitate the placement of
several catheters.10
Clostridium spp.
Peptostreptococcus spp.
Drain the pus,
Institute appropriate antibiotics, and
Deal with any underlying source of infection, if present.
The advances in USG and CT that provide earlier and more
accurate diagnosis also have enabled these modalities to
facilitate treatment through guided aspiration and drainage,
shifting management away from open surgery to minimally
invasive techniques. Percutaneous drainage combined with
antibiotics has become the first line and mainstay of treatment
for most PLAs.1
Antibiotics: Before obtaining positive cultures from blood or
pus, broad-spectrum antibiotics should be started to cover
Gram-negative and Gram-positive aerobes and anaerobes.
Initial therapy with amoxicillin, an aminoglycosides, and
metronidazole or a third generation cephalosporin and
metronidazole generally covers the causative organisms
most commonly found, although this regimen may be varied
according to geographic differences and antimicrobial
treatment policies.
Initially, antibiotics should be administered parenterally, and
after 2 weeks of systemic therapy, appropriate oral agents
may be used for a further 4 weeks.11 In patients with multiple
PLAs that are too small to drain, antibiotics may be the only
treatment possible. In addition, efforts must be made to
identify any underlying biliary obstruction, which needs to
be overcome for the antibiotic therapy to succeed.
Percutaneous procedures: Percutaneous drainage is performed
under USG or CT guidance. Aspiration of PLAs to confirm the
diagnosis and obtain pus for culture should be accompanied
by complete aspiration of the pus or insertion of a drain at
Although highly successful, PNA/ PCD fail in approximately
10% cases. Incomplete or unsuccessful drainage may result
from:
Catheter too small to drain the thick pus,
Position of catheter not conducive to adequate drainage,
Catheter removed prematurely
Thick fibrous encasing wall of PLA that is unable to collapse.
An abscess with biliary communication has been reported
to be treated as effectively by PCD as a non-communicating
abscess, although the continuous output of bile leads to a
prolonged period of abscess drainage.13
Surgical treatment: The only indication of primary surgical
treatment of PLAs is in patients with an initial presentation
with intraperitoneal rupture or in patients with multiple
abscesses above an obstructed system that cannot be
negotiated by non-operative means.14 Open operation is also
indicated when there is failure of non-operative treatment and
for complications of percutaneous drainage, such as bleeding
or intraperitoneal leakage of pus. Surgery is required to treat
any underlying causative disease if necessitated, particularly
those pertaining to hepatobiliary area.
The traditional principles of surgery are: to perform needle
aspiration before blunt puncture, finger explorations to break
down loculations, insertion of a large bore drainage tube
for adequate drainage and to maximize dependent drainage.
Postoperative irrigation and suction of the cavity via the
drainage tube is usually advantageous.
There have been isolated references to the use of hepatic
471
Medicine Update 2012 Vol. 22
resection in the treatment of PLAs.4,6,15
Recent travel to a tropical region
There is no single therapy that cures all cases. Antibiotics
combined with percutaneous aspiration (which may need to
be repeated) or PCD is successful in 90% of patients.1
Clinical features:
Approximately 20% have a past history of dysentery and
another 10% history of diarrhoea or dysentery at the time of
diagnosis.20
Prognosis: With modern treatments, the prognosis depends
more on the underlying etiology and co-morbid factors than
the PLA itself, although delay in presentation and diagnosis
contributes to a poor outcome.
The risk factors most commonly associated with mortality
include:6,9,16
Onset is usually abrupt with fever. Fever varies between
38 and 40C, frequently in spikes but sometimes persists for several days, with rigors and profuse sweating.
Pain in the upper abdomen, usually intense and constant,
radiating to the scapular region and right shoulder, increases with deep breathing or coughing, or when the
patient rests on the right side. In ALAs localized on the
left lobe, pain occurs on the left side and may radiate to
the left shoulder.
Septic shock,
Clinical jaundice
Coagulopathy
Leukocytosis
Diarrhoea and/or dysentery
Hypoalbuminemia
Nausea, vomiting and fatigue
Multiple abscesses
Anorexia, weight loss
Intraperitoneal rupture
Cough & dyspnoea
Malignancy (more in hepatopancreatobiliary malignancy than other malignant diseases)
On examination:
AMOEBIC LIVER ABSCESS (ALA)
Epidemiology:
Mild jaundice is quite common, but severe jaundice is
rare.
The cardinal sign of amoebic liver abscess is painful hepatomegaly. On palpation the liver is soft and smooth.
Localized tenderness in the region of the abscess, most
commonly at the lower right intercostal spaces, is frequently seen. Hepatomegaly may not be detected in patients with abscess at subdiaphragmatic location.
Movement of the right side of the chest and diaphragm
may be restricted with dullness on percussion.
ALA is the most common extra intestinal site of infection but
occurs in only less than 1% of E. histolytica infections.17 ALAs
are 3 to 10 times more common in men.18 Patients commonly
affected are between 20 to 40 years of age with residence in,
recent travel to or emigration from an endemic region.
ALA lesions are usually single and mostly found in the right
lobe of the liver. The incidence of ALA of the left lobe ranges
from 5% to 21%. The liver abscess has a thin capsular wall
with a necrotic centre composed of a thick fluid. Typically,
abscess fluid is odourless, resembling chocolate syrup or
anchovy paste in half, and bacteriologically sterile, although
secondary bacterial invasion may occur (in 15 to 20%). The
mortality rate has been estimated to be around 0.2-2.0% in
adults and up to 26% in children.1
Investigations:
Raised bilirubin, leukocytosis (75% cases) raised
transaminases and alkaline phosphatase (non-specific)
and raised markers of acute inflammation are usually
found in varying combination.
Fresh fecal sample may detect trophozoites containing
erythrocytes, preferably within 30 minutes of the passage of stool. Wet mount preparation should be made in
saline solution, in saline plus iodine, and in saline plus
methylene blue. Presence of erythrophagocytic trophozoites is strongly suggestive of invasive disease.
On aspiration, the amoebae are sparse in necrotic material from the centre of the abscess, but are more abundant on the marginal walls and are therefore more commonly found in the last portion of aspirated material.
Serology can be useful in the diagnosis of amoebiasis,
Risk Factors for ALA are:19
Alcoholism
Malignancy
HIV infection
Malnutrition
Corticosteroid use
Disorders of cell mediated immunity
Homosexual activity
472
Management of Liver Abscess
particularly in non-endemic areas (incidence of high
false positivity in endemic regions). Antibody response
is present in 85-95% of patients with invasive disease.
Indirect Haemagglutinin assays (IHA) is the most sensitive test (90%). Antibody may be negative in early infection and should be repeated 7 days later. IHA may
remain positive for up to 20 yrs and represent a previous infection.21 EIA (Enzyme-linked immunosorbent
assays) is the most commonly employed test and it usually become negative within 6-12 months.22 A negative
serology, however, does not exclude the diagnosis.
Straight X-ray of abdomen and thorax: May reveal elevation of the right hemidiaphragm, pleural reaction obscuring the right costophrenic angle.
USG: Typically reveals a round or oval hypoechoic area
which is contiguous to the liver capsule and without significant wall echoes (Figure 2). It may also show associated right pleural effusion or evidence of rupture.
CT scan of abdomen and MRI are sensitive studies for
demonstrating an abscess.
Polymerase chain reaction: also included in molecular
diagnosis of amebiasis.
Management of amoebic liver abscess
(ALA)
Four groups of treatment modalities are effective:
1. Drug therapy only
2. USG guided aspiration and drug
3. Percutaneous catheter drainage and drug
4. Laparatomy, drainage and drug
Medical therapy:
Fig. 2 : Showing ultrasonographic demonstration of an amoebic
liver abscess
Medical therapy may be instituted using either a single agent
or a combination of drugs for the extraluminal parasite (Table
3).
Table 3: Pharmacotherapy of E. histolytica infection in adults and children
Medication
Adult dosage
Pediatric dosage
Side Effects
Amoebicidal agents
1. Metronidazole
750 mg orally three times a day for 3050 mg/kg/d for 510 days orally Psychosis, seizures, Peripheral neu510 days;
in three divided doses;
ropathy and a metallic test
500 mg IV every 6 hours for 510 15 mg/kg IV load followed by 7.5 mg/
days
kg every 6 hours (maximum, 2250
mg/d)
2.
Chloroquine (base) (used as an 600 mg/d orally for 2 days, then 300 10 mg /kg of chloroquine base
alternative or adjuvant)
mg/d orally for 14 days
3.
Tinidazole (Preferable to Chlo- 2 gm/ day for 3-5 days
roquine)
Diarrhoea, abdominal cramps, cardiotoxicity, seizures and hypotension
Luminal agents
(Used to eradicate intestinal colonization after Amoebicidal treatment)
1.
Paromomycin
2. Iodoquinol
3.
25-30 mg/kg/d orally for 7 days in 25 mg/kg/d orally for 7 days in three Diarrhoea,
three divided doses
divided doses (maximum, 2 g/d)
650 mg orally three times a day for 3040 mg/kg/d for 20 days in three Contra indicated in patients with He20 days
divided doses (maximum, 2 g/d)
patic insufficiency or hypersensitivity
to Iodine
Diloxanide furoate (Indicated in 500 mg orally three times a day for 20 mg/kg/d in three divided doses
patients who fail to respond to 10 days
Iodoquinol and Paromomycin)
473
Medicine Update 2012 Vol. 22
Criteria for medical management
All non-complicated abscess
No features of rupture / impending rupture
No compression effect
Surgical mortality is, however, very high. Hence, in clinical
practice, it is only used when the cavity has ruptured into
adjacent viscera or body cavities.
Long term follow up of ALA patients:
Nitroimidazoles including metronidazole are effective in over
90%.23 Therapy should continue for at least 10 days. Relapses
have been reported with this duration and the drug may be
administered for up to 3 weeks. Single agent therapy with
metronidazole yields excellent results and the alternative toxic
drugs are indicated rarely and used probably in seriously ill
patients where the risk of failure of therapy is unacceptable.
The response to anti-amoebic drug is usually evident within
48 to 72 hours with the subsidence of toxemia.24
Aspiration or drainage of the abscess:
Routine aspiration of liver abscess is not indicated for
diagnostic or therapeutic purposes.25 A combination of USG
findings with a positive serology in the appropriate clinical
setting is adequate to start drug therapy.
Aspiration has been indicated in the following circumstances:26
Lack of clinical improvement in 48 to 72 hours
Left lobe abscess
Large abscess having impending rupture / compression
sign
Thin rim of liver tissue around the abscess (<10 mm)
Seronegative abscesses
Failure in the improvement following non-invasive
treatment after 4 to 5 days
Like PLA, percutaneous drainage is indicated when thick
collection is not getting aspirated by needle or there is failure
of USG-guided aspiration.
Antiamoebic therapy alone is as effective as routine needle
aspiration combined with antiamoebic therapy in the treatment
of patients with uncomplicated liver abscess.27
Surgical intervention:
Open surgical drainage is rarely indicated and may be required
in the setting of:28
large abscess with a poor yield on needle aspiration or
percutaneous drainage
clinical deterioration despite attempted needle aspiration
complicated ALA (like ruptured abscess in peritoneal
cavity with features of peritonitis)
complicated ALA (ruptured in the pleural cavity / pericardial cavity/ adjacent viscera)
After clinical cure, patients show few symptoms and
sonographic follow up demonstrates evidence of persistent
hypoechoic lesion. The mean time for the disappearance of
the sonographic abnormality is 6-9 months.29 Relapses are
very uncommon and the sonographic abnormality does not
warrant continued therapy.
The patterns of resolution seen on sonographic follow up
include:29 Type I: where complete disappearance of the cavity
occurs within 3 months (29.8%), Type II: a rapid reduction till
25% of the original cavity size and then a delayed resolution
(5.9%).
Factors influencing healing time include: the size of abscess
cavity at admission, hypoalbuminaemia and anaemia. The
type of clinical presentation, nature of therapy, number of
location of abscesses and time for clinical resolution pattern
of multiple liver abscesses is similar to solitary abscess. The
total abscess volume of all the cavities is the most important
factor that influences resolution time in multiple abscesses.
As clinical resolution does not correlate with ultrasonographic
resolution it is suggested that the results of the therapy should
be monitored by clinical criteria rather than USG.
Prognostic markers: Independent risk factors for mortality
in ALA are:30
bilirubin level > 3.5 mg/dl
encephalopathy,
volume of abscess cavity
hypoalbuminaemia (serum albumin <2.0 g/dl)
The duration of symptom and the type of treatment does not
influence mortality.
CONCLUSION
PLA and ALA have many features in common and diagnosis
is often delayed due to vague clinical symptoms resulting in
adverse outcomes. Because of the difficulty in differentiating
between these two types of abscesses initially, antiamoebic
therapy is usually recommended in addition to broad-spectrum
antibiotics.
Medical therapy alone is effective in most cases of ALA
while some form of intervention is usually needed or PLA.
Mortality is low with ALA compared with PLA. Abscesses
are slow to resolve. A multidisciplinary approach, including
a gastroenterologist, radiologist, surgeon, and laboratory, is
crucial for successful treatment of these curable infections.
474
Management of Liver Abscess
REFERENCES
1.
Branum G, et al. Hepatic abscess: changes in etiology, diagnosis
and management. Ann Surg 1990;212:655-62
2. Huang CJ, et al. Pyogenic hepatic abscess. Ann Surg 1996;
223:600-9.
3. Sharma MP, et al. Management of amoebic and pyogenic liver
abscess. Indian J Gastroenterol 2001; 20, supplement C33-36.
4.
Huang C, et al. Pyogenic hepatic abscess: changing trends over 42
years. Ann Surg 1996; 223:600-9.
5.
Chu KM, et al. Pyogenic liver abscess: an audit of experience over
the last decade. Arch Surg 1996; 131:148-52.
6.
Chou FF, et al. Single and multiple pyogenic liver abscesses: clinical course, etiology and results of treatment. World J Surg 1997;
21:384-9.
7.
Wong WM, et al. Pyogenic liver abscess: retrospective analysis
of 80 cases over a 10 year period. J Gastroenterol Hepatol 2002;
17:1001-7.
8.
Saini S. Imaging of the hepatobiliary tract. N Engl J Med 1997;
336:1889-94.
9.
Perez J, et al. Clinical course, treatment and multivariate analysis of risk factors for pyogenic liver abscess. Am J Surg 2001;
181:177-86.
10. Seeto R, et al. Pyogenic liver abscess: changes in etiology, management and outcome. Medicine 1996; 75:99-113.
11. Ng FH, et al. Sequential intravenous/oral antibiotics vs continuous
intravenous antibiotics in the treatment of pyogenic liver abscess.
Aliment Pharmacol Therap 2002; 16:1083-90.
12. Yu SC, et al. Treatment of pyogenic liver abscess: prospective randomized comparison of catheter drainage and needle aspiration.
Hepatology 2004; 39:932-8.
13. Bayraktar Y, et al. Percutaneous drainage of hepatic abscess: therapy does not differ for those with identifiable biliary fistula. Hepatogastroenterol 1996; 43:620-6.
14. Stain S, et al. Pyogenic liver abscess: modern treatment. Arch Surg
1991; 126:991-5.
15. Balasegaram M. Management of hepatic abscess. Curr Prob Surg
1981; 18:282-340.
16. Yeh TS, et al. Pyogenic liver abscess in patients with malignant
disease. Arch Surg 1998; 13:242-5.
17. Peters RS, et al. Amoebic liver disease. Ann Rev Med 1982;
32:161-74.
18. Maltz G, et al. Amoebic liver abscess: a 15-year experience. Am J
Gastroenterol 1991; 86:704-10.
19. Li E, et al. Protozoa: amoebiasis. Gastroenterol Clin North Am
1996; 25:471-92.
20. Hoffner RJ, et al. Common presentations of amoebic liver abscess.
Ann Emerg Med 1999; 34:351-5.
21. Ravdin JI. Amoebiasis. Clin Infect Dis 1995; 20:1453-64.
22. Sharma MP, et al. A simple and rapid dot-ELISA dipstick technique for detection of antibodies to Entamoeba histolyica in amoebic liver abscess. Indian J Med Res 1988; 88:409-15.
23. Sharma MP, et al. Management of amoebic liver abscess. Arch
Med Res 2000; 31:S4-5.
24. Thompson JE Jr, et al. amoebic liver abscess: a therapeutic approach. Rev Infect Dis 1985; 7:171-9.
25. Stanley SL Jr. Amoebiasis. Lancet 2003; 361:1025-34.
26. Ralls PW, et al. Sonographic findings in hepatic amoebic abscess.
Radiology 1982; 145:123-6.
27. Chavez-Tapia NC, et al. Image guided percutaneous procedure
plus metronidazole versus metronidazole alone for uncomplicated
amoebic liver abscess. Cochrane Data Syst Rev 209; 1:CD004886.
28. Sarda AK, et al. Intraperitoneal rupture of amoebic liver abscess.
Br J Surg 1989; 76:202-3.
29. Sharma MP, et al. Long term follow up of amoebic liver abscess:
clinical and ultrasound patterns of resolution. Trop Gastroenterol
1995; 16:24-8.
30. Sharma MP, et al. Prognostic markers in amoebic liver abscess: a
prospective study. Am J Gastroenterol 1996; 91:2584-8.
475
You might also like
- Lepsius R - Discoveries in Egypt, Ethiopia, and The Peninsula of Sinai in The Years 1842 To 1845 - 1853Document486 pagesLepsius R - Discoveries in Egypt, Ethiopia, and The Peninsula of Sinai in The Years 1842 To 1845 - 1853Keith JundeaconNo ratings yet
- Gallbladder EmpyemaDocument17 pagesGallbladder EmpyemaYayut 18No ratings yet
- CHOLEDocument25 pagesCHOLEJane TuazonNo ratings yet
- Set 3 COMP-2Document71 pagesSet 3 COMP-2Appu ayyalaNo ratings yet
- A Simple Guide to Blood in Stools, Related Diseases and Use in Disease DiagnosisFrom EverandA Simple Guide to Blood in Stools, Related Diseases and Use in Disease DiagnosisRating: 3 out of 5 stars3/5 (1)
- Urology MCQDocument16 pagesUrology MCQChristian Jara80% (5)
- HowToBuildAStockStrategy - Portfolio123Document36 pagesHowToBuildAStockStrategy - Portfolio123life_enjoy50% (2)
- Acute Cholecystitits, Choledocholithiasis and Acute CholangitisDocument16 pagesAcute Cholecystitits, Choledocholithiasis and Acute CholangitisKath de L'EnferNo ratings yet
- CholecystitisDocument12 pagesCholecystitisMariela HuertaNo ratings yet
- Peritonitis: Presentan: FAUZAN AKBAR YUSYAHADI - 12100118191Document21 pagesPeritonitis: Presentan: FAUZAN AKBAR YUSYAHADI - 12100118191Fauzan Fourro100% (1)
- Gall Bladder CarcinomaDocument29 pagesGall Bladder CarcinomaUsman FarooqNo ratings yet
- Biliary Diseases: Dr. Wu Yang Dept. of Surgery The First Affiliated Hospital of Zhengzhou UniversityDocument42 pagesBiliary Diseases: Dr. Wu Yang Dept. of Surgery The First Affiliated Hospital of Zhengzhou Universityapi-19916399No ratings yet
- Liver Cancer Pathophysiology: Predisposing FactorDocument3 pagesLiver Cancer Pathophysiology: Predisposing FactorTarantado100% (2)
- Painting Procedure JotunDocument9 pagesPainting Procedure Jotunspazzbgt100% (2)
- Liver AbsesDocument8 pagesLiver AbsesS FznsNo ratings yet
- Management of Liver Abscess: Anita Dutta,, Sanjay BandyopadhyayDocument7 pagesManagement of Liver Abscess: Anita Dutta,, Sanjay BandyopadhyayMuhammad Ahmad bin makruf syammakuNo ratings yet
- Liver Abscess DissertationDocument4 pagesLiver Abscess DissertationPayForAPaperAtlanta100% (1)
- Perez JyDocument3 pagesPerez JyBarudak Theris BadeurNo ratings yet
- Help Pedsurgeryafrica81Document7 pagesHelp Pedsurgeryafrica81tikaauliaNo ratings yet
- Empiema Kandung EmpeduDocument7 pagesEmpiema Kandung EmpeduHasya KinasihNo ratings yet
- There Are Many Potential Causes of Liver AbscessesDocument4 pagesThere Are Many Potential Causes of Liver AbscessesmarianmadhurNo ratings yet
- Today's: Diseases of The AlimentaryDocument3 pagesToday's: Diseases of The AlimentaryArix BakaNo ratings yet
- 2 Gastric and Duodenal Peptic Ulcer Disease 2Document35 pages2 Gastric and Duodenal Peptic Ulcer Disease 2rayNo ratings yet
- Ruptured Hepatic Abscess Mimicking Perforated ViscusDocument3 pagesRuptured Hepatic Abscess Mimicking Perforated ViscusMichu VuNo ratings yet
- 7cholestatic Liver DiseaseDocument9 pages7cholestatic Liver DiseaseDaniel Fernando LozanoNo ratings yet
- Liver AbscessDocument3 pagesLiver AbscessLyiuiu TranNo ratings yet
- Gallbladder PolypDocument28 pagesGallbladder PolypChristian LoyolaNo ratings yet
- Liver Fibrosis ProgressDocument9 pagesLiver Fibrosis ProgressTaufik Rizkian AsirNo ratings yet
- Gallbladder IIDocument22 pagesGallbladder IIAli SafaaNo ratings yet
- Literature Review of Liver AbscessDocument4 pagesLiterature Review of Liver Abscessc5ng67v1100% (1)
- What Is An Acute AbdomenDocument112 pagesWhat Is An Acute AbdomenLavasa SharmaNo ratings yet
- Open Access Textbook of General Surgery: Large Bowel Obstruction A BoutallDocument6 pagesOpen Access Textbook of General Surgery: Large Bowel Obstruction A BoutallDian FikriNo ratings yet
- Clinical Clerk Seminar Series: Approach To Gi BleedsDocument11 pagesClinical Clerk Seminar Series: Approach To Gi BleedsAngel_Liboon_388No ratings yet
- 1.7B AppendixDocument4 pages1.7B AppendixDulce Kriselda E. FaigmaniNo ratings yet
- Emergent Treatment of Acute Cholangitis andDocument10 pagesEmergent Treatment of Acute Cholangitis anddhimas satriaNo ratings yet
- Liver Abscess Modul 2Document3 pagesLiver Abscess Modul 2ras emil sazuraNo ratings yet
- Inflammatoray Bowel DiseaseDocument14 pagesInflammatoray Bowel DiseaseSadr AkrmNo ratings yet
- Colelitiasis SD MirizziDocument14 pagesColelitiasis SD MirizziPipex Del MorroNo ratings yet
- Amoebic Liver Abscess: Clinical MedicineDocument5 pagesAmoebic Liver Abscess: Clinical MedicineAizat KamalNo ratings yet
- Pathogens: Hepatic AbscessDocument8 pagesPathogens: Hepatic Abscessalberto cabelloNo ratings yet
- Histolytica Accounts For 10% of Cases.: Risk FactorsDocument4 pagesHistolytica Accounts For 10% of Cases.: Risk FactorsLadywill GamitNo ratings yet
- CholangitisDocument11 pagesCholangitisNilamsari KurniasihNo ratings yet
- Appendicitis, Acute: BackgroundDocument5 pagesAppendicitis, Acute: BackgroundIka YusniartiNo ratings yet
- Jaundice and Parasitic INFECTIONS Ibrahem Sayed Ibrahem 220521Document4 pagesJaundice and Parasitic INFECTIONS Ibrahem Sayed Ibrahem 220521Hend Qorani HassanNo ratings yet
- Uworld Summary NotesDocument6 pagesUworld Summary Notesnavneet mannNo ratings yet
- 260-Article Text-875-1-10-20220728Document4 pages260-Article Text-875-1-10-20220728hasan andrianNo ratings yet
- Ramnarine, 2017Document10 pagesRamnarine, 2017Areza Eka PermanaNo ratings yet
- CholangiocarcinomaDocument7 pagesCholangiocarcinomailovedaneNo ratings yet
- Cholecystitis FinalDocument57 pagesCholecystitis FinalRajendra DesaiNo ratings yet
- AppendicitisDocument14 pagesAppendicitisMary Joy BunuanNo ratings yet
- GALLBLADDERDocument16 pagesGALLBLADDERKadenceFreya-Charisse G PosadasBulintao100% (2)
- Maat 12 I 3 P 271 DDDDDocument5 pagesMaat 12 I 3 P 271 DDDDKacamata BagusNo ratings yet
- Jejunojejunal Intussusception As Initial Presentation of Coeliac Disease: A Case Report and Review of LiteratureDocument6 pagesJejunojejunal Intussusception As Initial Presentation of Coeliac Disease: A Case Report and Review of Literatureellya theresiaNo ratings yet
- Biliary CirrhosisDocument11 pagesBiliary CirrhosisradistryaNo ratings yet
- Acute Chronic PancreatitisDocument78 pagesAcute Chronic PancreatitisSirfaymons Sirfaymons Sirfaymons100% (1)
- Urinary RetentionDocument12 pagesUrinary RetentionPaula GomezNo ratings yet
- Help Pedsurgeryafrica80Document4 pagesHelp Pedsurgeryafrica80Thayalan SukumaranNo ratings yet
- Radiology Case Report - Splenic AbscessDocument6 pagesRadiology Case Report - Splenic AbscessAbeebNo ratings yet
- ML Diverticular Disease: Diagnosis and Treatment: Am Fam Physician. 2005 Oct 1 72 (7) :1229-1234Document8 pagesML Diverticular Disease: Diagnosis and Treatment: Am Fam Physician. 2005 Oct 1 72 (7) :1229-1234Zaky IbadurrahmanNo ratings yet
- Gastroenterology For General SurgeonsFrom EverandGastroenterology For General SurgeonsMatthias W. WichmannNo ratings yet
- Diseases of the Liver and Biliary TreeFrom EverandDiseases of the Liver and Biliary TreeAnnarosa FloreaniNo ratings yet
- Craap WorksheetDocument1 pageCraap Worksheetapi-288189987No ratings yet
- Sairam Vidyalaya: To Study The Collision of Two Balls in Two DmensionsDocument14 pagesSairam Vidyalaya: To Study The Collision of Two Balls in Two DmensionsAditya VenkatNo ratings yet
- Graphene-Based Conducting Inks 2Document3 pagesGraphene-Based Conducting Inks 2VishnuTejaChundiNo ratings yet
- Homeostasis and Rein Control: From Daisyworld To Active PerceptionDocument6 pagesHomeostasis and Rein Control: From Daisyworld To Active PerceptionVeronique PoenelleNo ratings yet
- General Deductions (Under Section 80) : Basic Rules Governing Deductions Under Sections 80C To 80UDocument67 pagesGeneral Deductions (Under Section 80) : Basic Rules Governing Deductions Under Sections 80C To 80UVENKATESAN DNo ratings yet
- 6 Trimble HD-GNSS White PaperDocument13 pages6 Trimble HD-GNSS White PaperpuputrahsetyoNo ratings yet
- Oleg A. Starykh, Andrey V. Chubukov and Alexander G. Abanov - Flat Spin-Wave Dispersion in A Triangular AntiferromagnetDocument4 pagesOleg A. Starykh, Andrey V. Chubukov and Alexander G. Abanov - Flat Spin-Wave Dispersion in A Triangular AntiferromagnetGravvolNo ratings yet
- Working in The Dark Understanding The Presuicide State of MindDocument8 pagesWorking in The Dark Understanding The Presuicide State of MindAntonia InaNo ratings yet
- Survey of Processes For High Temperature-High Pressure Gas Purification - OCR PDFDocument241 pagesSurvey of Processes For High Temperature-High Pressure Gas Purification - OCR PDFChristopher BrownNo ratings yet
- An Introduction To CCARDocument10 pagesAn Introduction To CCARRanit Banerjee100% (1)
- Jx6 Con Move Ba 30001 ManualDocument544 pagesJx6 Con Move Ba 30001 ManualPongsak KungsuwunNo ratings yet
- Engineering Assistant in Prasar Bharti 2013 Final Result PDFDocument27 pagesEngineering Assistant in Prasar Bharti 2013 Final Result PDFKiran Jot SinghNo ratings yet
- Design CakesDocument1 pageDesign CakesM-LamersNo ratings yet
- An Introduction To Mathematical ReasoninDocument3 pagesAn Introduction To Mathematical ReasoninGero Nimo100% (1)
- EVS Assignment Question by Vedant Nagpal Answer 03Document1 pageEVS Assignment Question by Vedant Nagpal Answer 03Vedant NagpalNo ratings yet
- Martin2019 Article BusinessAndTheEthicalImplicatiDocument11 pagesMartin2019 Article BusinessAndTheEthicalImplicatihippy dudeNo ratings yet
- Ca Foundation Law Sales of Goods Act Classwork 041021Document8 pagesCa Foundation Law Sales of Goods Act Classwork 041021Rakesh AgarwalNo ratings yet
- PresentasiDocument6 pagesPresentasiAfanda Dwi R R100% (1)
- K LP - All ItemsDocument11 pagesK LP - All ItemsRumesh RoshanNo ratings yet
- InglesDocument7 pagesInglesMica LetoNo ratings yet
- ChemistryDocument16 pagesChemistryShashank Dubey0% (1)
- Refresher Module - Surveying (Earthworks) : Methods of Calculating VolumeDocument2 pagesRefresher Module - Surveying (Earthworks) : Methods of Calculating VolumeOctavia BlakeNo ratings yet
- Terminating A Swap ContractDocument2 pagesTerminating A Swap Contractravi_nyseNo ratings yet
- Consti 4 PDFDocument110 pagesConsti 4 PDFRenceNo ratings yet
- Chrystal Chao Ci Xin'赵: Achievements Software SkillsDocument4 pagesChrystal Chao Ci Xin'赵: Achievements Software SkillsCHAO CI XINNo ratings yet
- Case Study 4aDocument16 pagesCase Study 4aAntonia RauNo ratings yet
- NSP/004/109 (OHI 9) Guidance On Anti-Climbing Devices, Safety Signs and Labels Required On Overhead Line SupportsDocument25 pagesNSP/004/109 (OHI 9) Guidance On Anti-Climbing Devices, Safety Signs and Labels Required On Overhead Line SupportsMuhammad BilalNo ratings yet