Professional Documents
Culture Documents
Reviews: Non-Cardiogenic Pulmonary Edema
Reviews: Non-Cardiogenic Pulmonary Edema
Uploaded by
journaltranslateOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Reviews: Non-Cardiogenic Pulmonary Edema
Reviews: Non-Cardiogenic Pulmonary Edema
Uploaded by
journaltranslateCopyright:
Available Formats
Hellenic J Cardiol 44: 385-391, 2003
Reviews
Non-Cardiogenic Pulmonary Edema
NICHOLAOS S. KAKOUROS1, STAVROS N. KAKOUROS2
1
2
Key words:
Non-cardiogenic
pulmonary edema,
pulmonary edema
of unknown
pathogenesis,
ARDS.
Manuscript received:
May 30, 2002;
Accepted:
October 18, 2002.
Address:
Stavros N. Kakouros
26, N. Paritsi St.,
154 51, Athens, Greece
e-mail:
kakst@otenet.gr
Department of Cardiology, London Chest Hospital, London, UK
Department of Cardiology, Athens Chest Hospital, Sotiria, Athens, Greece
he barrier between pulmonary
capillaries and alveolar gas consists of a series of three anatomical layers with distinct structural characteristics. The cytoplasmic projections
of the capillary endothelial cells represent the first layer of this barrier and
overlap to form a continuous cytoplasmic
tube. At the overlapping junctions of
these cytoplasmic projections are clefts of
varying sizes (averaging approximately 4
nm in width), which provide communication between pulmonary capillaries and
the interstitial space (loose junctions).
The interstitial space represents the second layer and contains connective tissue, fibroblasts, macrophages, small
arteries, veins and lymphatic channels.
The third layer is the alveolar wall which
is continuous with the bronchial epithelium and is composed of large squamous cells with thin cytoplasmic projections. These projections overlap in a
similar way to the projections of capillary
endothelium. In contrast to the endothelial junctions, which allow for variable
continuity between capillaries and
interstitial space, the alveolar epithelial
clefts are obliterated by complete fusion
of the membranes of the adjacent cells,
so as to demand greater forces for their
disruption (tight junctions). The tightness
of these junctions helps to forestall
alveolar flooding, which represents the
final stage of pulmonary edema.
In other tissues there is normally a
continuous exchange of liquid and colloids
between the vascular bed and the interstitium. The lymphatics serve to continuously remove colloids and fluid from
the interstitial space to the systemic venous
circulation, so as to ensure that the volume
of interstitial space remains constant.
Pulmonary edema develops when the
movement of liquid from the blood vessels
to the interstitial space and in some instances to the alveoli exceeds the return of
liquid to the blood by way of the lymphatics. Whether initiated by an imbalance of
Starling forces or by primary damage to
the various components of the alveolarcapillary membrane, the sequence of liquid
exchange and accumulation in the lungs is
the same and can be represented as three
separate stages1.
In stage 1, there is an increase in transfer of liquid from blood capillaries to the
interstitial space. The pulmonary capillary
endothelial junctions are widened by an
increase in filtrative forces or by toxic damage of the membrane. Despite the
increased filtration, there is no increase in
interstitial volume because there is an
equal increase in lymphatic drainage.
When the filtered load from the pulmonary capillaries to the interstitial space is
increased beyond a limit, the lymphatics
cannot follow this rapid rhythm and liquid
and colloid begin to accumulate in the
more compliant interstitial compartment
surrounding bronchioles, arterioles and
venules (stage 2).
With further increase in filtered load,
the volume limits of the more compliant
(Hellenic Journal of Cardiology) HJC 385
N. Kakouros, S. Kakouros
spaces of the interstitial space are exceeded and the
liquid begins to accumulate in the less compliant
compartments of the interstitial space. The alveolarcapillary membrane is very thin and disrupts immediately, so that alveolar flooding occurs (stage 3).
This flooding decreases pulmonary oxygenation
which results in deterioration of left ventricular function. This mechanism leads to further increase of
pressure in the pulmonary capillaries and further
deterioration of pulmonary edema2.
Classification of pulmonary edema
The two most common forms of pulmonary edema are
those initiated by an imbalance of Starling forces
(Hydrostatic Pulmonary edema) and those initiated by
disruption of alveolar-capillary membrane (NCPE).
Less often, lymphatic insufficiency can be involved as a
predisposing factor (post lung transplant, lymphangitic
carcinomatosis, fibrosin lymphangitis). Irrespective of
the initiating event, the stage of alveolar flooding is
characterized to some degree by disruption of alveolar-capillary membrane1.
Cardiogenic pulmonary edema
Hydrostatic pulmonary edema is usually cardiogenic.
The usual causes of systolic and diastolic left ventricular dysfunction (coronary artery disease, myocarditis, cardiomyopathy, hypertension, congenital
heart diseases etc.) are responsible for the development of acute pulmonary edema. Usual triggering factors are acute ischemia, myocardial infarction,
rhythm or conduction abnormalities, high blood
pressure, infection, omission of drug intake, dietary
abuse, physical or psychological stress.
The normal pulmonary capillary pressure is about
8 mmHg. Due to the effect of gravity, hydrostatic pressure is greater from apex to base and this explains the
non- homogeneous blood perfusion to the lungs. Deviation from this gravity-dependant pattern has been
called vascular redistribution. Redistribution is due to
increased pulmonary venous pressure and is demonstrated by greater perfusion to the apex than to the
base of the lungs. This kind of redistribution is seen
after an acute attack of alveolar pulmonary edema or
in chronic situations with high left atrial pressure as
happens in mitral stenosis and congestive heart failure2.
Pulmonary edema will occur only when the
pulmonary capillary pressure rises to values exceeding the plasma colloid osmotic pressure, which is
386 HJC (Hellenic Journal of Cardiology)
approximately 28 mmHg in humans. Although pulmonary capillary pressure must be abnormally high
for the development of pulmonary edema, this
pressure may not correlate with the severity of pulmonary edema. The rate of increase in lung liquid at
any given elevation of capillary pressure is related to
the functional capacity of lymphatics and to variations in interstitial and pulmonary pressures1.
In patients with chronic heart failure lymphatics
are hypertrophied and lymph flow may exceed up to
twenty times the normal rate. This creates a safety
margin for compensation of increased hydrostatic
pressure and increased filtration. That is why patients with heart failure may have pulmonary artery
wedge pressure to 45 mmHg without being in pulmonary edema1,2. Experimental work showed that
the resection of over half the pulmonary capillary
bed has been required to produce pulmonary edema2.
Non-cardiogenic pulmonary edema
NCPE continues to represent an important cause of
morbidity and mortality with a large human and financial cost. Because of the resemblance of the clinical
picture to that seen with respiratory distress of the
neonate, NCPE has been referred to as the Adult
Respiratory Distress Syndrome (ARDS). In spite of
the great improvement in supportive therapy, mortality continues to exceed 50%. Early diagnosis is important for the management of this syndrome.
Many conditions are associated with pulmonary
edema that appears to be due to diffuse damage and
increased permeability of alveolar-capillary membrane. These conditions include infectious (bacterial,
viral, parasitic) septicemia, trauma and disseminated
intravascular coagulation. Also, shock lung in association with non-thoracic trauma, acute hemorrhagic
pancreatitis, inhalation of toxic gases (smoke, ozone,
cadmion, phosgene, chlorine, nitrogen dioxide), circulating foreign substances (snake venom, alloxan,
alpha-naphthyl thiourea) and endogenous vasoactive
substances (histamine, kinins). Burn, aspiration of
gastric contents, inhalation of foreign body, acute
radiation pneumonitis and drowning have been also
implicated in the development of pulmonary edema.
Special forms of non-cardiogenic pulmonary edema
Conditions considered as initiating mechanisms for
the development of NCPE are listed in the table that
follows.
Non-cardiogenic Pulmonary Edema
Table 1. Special forms of non-cardiogenic pulmonary edema.
Pharmaceutical
Narcotic overdose
Chemotherapy
Salicylate intoxication
Calcium antagonist overdose
Hydrochlorothiazide
Contrast fluids
High-altitutde
Neurogenic
Pulmonary embolism
Eclampsia
Post cardioversion
Post anaesthesia
Post cardiopulmonary bypass
Pharmaceutical
thogenesis. By distinction to drug-induced pulmonary pneumonitis that may lead to permanent
pulmonary fibrosis, NCPE is not fatal. It can be
reversed upon prompt recognition, immediate discontinuation of the offensive drug and intensive
supportive treatment with intravenous corticosteroids5.
Salicylate intoxication
Salicylate intoxication is frequently overlooked as a
cause of NCPE and altered mental status in adult
patients. Non-early diagnosis and treatment leads to
high morbidity and mortality. A high index of suspicion is necessary for early recognition and successful
treatment with hemodialysis and urinary alkalinization6,7.
Narcotic overdose
Pulmonary edema is usually a complication of
pharmaceutical intoxication with antidepressants,
opiates. It is a well-recognized complication of
heroin overdose and represents the most important
cardiopulmonary toxic effect of opiates overdosing.
It is usually a standard pathologic finding in fatal
cases and may be the result of intravenous, oral or
administration of the narcotic drug by inhalation.
The pathophysiologic feature of the syndrome is
increased permeability of pulmonary capillaries and
the normal or even low left atrial pressure. The mechanisms which are responsible for the endothelial
damage remain unclear.
In spite of the fact that pulmonary edema usually
appears shortly after heroin injection, it may appear
late, even 6 hours later3. Mechanical ventilation with
positive airway pressures (PEEP) offers great support
to patients2,4.
Chemotherapy
NCPE is a rare pulmonotoxic complication of anticancer therapy. It is less well recognizable than
pneumonitis and fibrosis. Chemotherapeutic agents
clearly associated with NCPE are cytarabine, gemcitabine, interleukin 2, as well as all-trans retinoid
acid in acute promyelocytic leukemia. The pathophysiology of lung injury in drug-induced NCPE,
remains unclear. There are indications suggesting
that both a direct cytotoxic insult to the lung epithelial cells and induction of a cytokine-triggered
inflammatory response may be involved in its pa-
Calcium antagonist overdose
NCPE has been reported after an overdose of diltiazem, nifedipine and verapamil. Multiple cellular
mechanisms appear to be responsible for the development of NCPE after overdoses of calcium
channel blockers. First, prostaglandins have been
shown to play an important role in maintaining
cellular integrity, especially during lung inflation.
The protective role of prostaglandins in cellular integrity is lost with excessive concentrations of calcium channel blockers (inhibition of prostacyclin
release). This leads to a leaky capillary syndrome.
Secondly, calcium channel blockers, cause systemic
precapillary vasodilation and peripheral edema due
to their effect on vascular smooth muscle. Finally, it
has been shown that the pulmonary vasodilatory
effect of calcium antagonists may lead to perfusionventilation mismatch and hypoxemia. Management
of these patients includes infusion of calcium and
catecholamines and correction of hyperglycemia8,9,10.
Hydrochlorothiazide use
Less than 40 cases of NCPE have been reported to be
associated with use of hydrochlorothiazide. Even a
single dose (50mg) may induce the syndrome, the
etiology of which remains unknown. It is suggested that
a possible involvement of an immunologic mechanism
is responsible for this adverse reaction. The reaction is
associated with granulocytic infiltration into the lungs
and IgG deposition in alveolar membranes. It is
reported good response to dopamine and steroids11.
(Hellenic Journal of Cardiology) HJC 387
N. Kakouros, S. Kakouros
Radiocontrast media
Fulminant NCPE has been reported several minutes
after intravenous administration of radiocontrast
media. The low pulmonarycapillary wedge pressure
and the high protein concentration in pulmonary
edema fluid indicated a NCPE related to increased
lung vascular permeability. The response is considered as allergic reaction and the possibility of its
occurrence is increased in patients with known immunologic abnormality12.
High-altitude
This uncommon type of NCPE occurs in young
people who have quickly ascended to altitudes above
2700m and who then engage in strenuous physical
exercise at that altitude, before they have become
acclimatized. The incidence of this illness is about
6.5 cases per 100 exposures in persons less than 21
years of age.
Although most patients have pulmonary hypertension, the pulmonary capillary wedge pressure is
normal. The direct effect of alveolar hypoxia on
increasing alveolar-capillary membrane permeability
is considered possible mechanism for the pathogenesis of NCPE13. Transient intravascular coagulation has also been implicated. Gradual ascent, allowing time for acclimatization and limiting physical
exertion for 2-3 days in high altitudes are thought to be
preventive14.
Reversal of this syndrome is rapid (in less than
48 hours) and certain by returning the patient to a
lower altitude and by administering a high inspiratory concentration of oxygen. When this is not available, treatment with nifedipine is recommended
until descent is possible14.
a Marathon and had pulmonary edema, the mean
plasma sodium level was 1213 mmol/l and oxygen
saturation was less than 70%. Electrocardiograms
and echocardiograms were normal and chest radiographs showed pulmonary edema with a normal
heart. Cardiac enzymes and pulmonary artery wedge
pressure were not elevated. Scanning of the brain
showed cerebral edema. Treatment includes intubation and mechanical ventilation with intravenous
administration of hypertonic sodium chloride (NaCl)
with such a rate of continuous infusion as to increase
plasma sodium levels by 10mmol/l in 12 hours. Pulmonary and cerebral edema resolve as the sodium
level increases15,16.
Pulmonary embolism
Pulmonary edema can occur after massive or multiple
smaller pulmonary embolisms and is most often
attributed to concomitant left ventricular dysfunction
due to hypoxemia and displacement of the interventricular septum to the left vetricular cavity by right
ventricular dilatation. There are data to suggest that
an increase in permeability of the alveolar-capillary
membrane also occurs. Thrombin generated by the
clotting process in association with the embolus causes
aggregation of platelets, complement activation and
leukostasis. The radiographic findings are relevant to
the severity of pulmonary edema and in 20% of the
cases there is a coexistent pneumonia17,18.
Eclampsia
Multiple factors such as cerebral dysfunction with
massive sympathetic discharge, hypervolemia, hypoalbuminemia and disseminated intravascular coagulation probably play a role in the pathogenesis19.
Neurogenic
It is suggested from experimental studies that sympathetic overactivity plays a key role in the pathogenesis of this disorder 15. Central nervous system
disorders ranging from head trauma to grand mal
seizures can be associated with acute pulmonary
edema, without detectable left ventricular disease.
Neurogenic pulmonary edema is often associated
with increased intracranial pressure and can be the
initial manifestation of hyponatremic encephalopathy with nausea and vomiting as it happens in
otherwise healthy Marathon runners16. In a study of
Marathon runners who collapsed after competing in
388 HJC (Hellenic Journal of Cardiology)
Post Cardioversion
The mechanism of pulmonary edema which occasionally occurs after cardioversion of tachyarrhythmias,
remains unknown. Ineffective left atrial function
after cardioversion, left ventricular dysfunction and
neurogenic mechanisms have all been suggested as
contributing factors20.
Post anaesthesia
In previously healthy subjects, pulmonary edema has
been found in the early post anaesthesia period with-
Non-cardiogenic Pulmonary Edema
out a clear relationship to fluid overload or any evidence of left ventricular dysfunction. The mechanism of this disorder is unknown but some cases
have been connected to the administration of naloxone. Upper airway obstruction due to laryngospasm
is considered the most possible mechanism causing
rapid changes in intrathoracic, alveolar and interstitial pressures, which recover within 48 hours after
proper intervention. Early diagnosis and management is lifesaving for the patient21,22.
Post cardiopulmonary bypass
NCPE is a rare adverse event that occurs in 0.2% of
cardiopulmonary bypass patients, with mortality
rates approaching 30%. Although all patients who
undergo cardiopulmonary bypass, have significant
heart disease, the development of edema has been
associated with normal left atrial pressures.
Alterations in surfactant due to prolonged collapse of the lung, with subsequent need to apply high
negative intrapleural pressures for reexpansion,
hypotension, hemorrhagic shock, transfusion of fresh
frozen plasma and packed red blood cells and possibly
drugs (amiodarone) may be responsible for the
pathogenesis.
Complement activation or direct pharmacologic
release of histamine by high concentrations of protamine (given for reversal of heparin anticoagulation), is the suspected cause. Cautious administration and accurate calculation of protamine doses
may prevent such an event 22,24,25. Treatment is supportive.
Differential diagnosis
The differentiation between hydrostatic (cardiogenic) and increased permeability edema (NCPE),
can usually be made through assessment of the clinical context in which it occurs and by means of
clinical and laboratory data. This approach may be
difficult as there is overlapping of pathogenetic mechanisms in the two forms. For example, the primary
hemodynamic event of cardiogenic pulmonary edema, that is increase in intravascular pressure, may
disrupt the capillary and alveolar membranes producing a NCPE. The basic differences between the two
forms of pulmonary edema are provided by history,
clinical examination and laboratory tests.
In NCPE, there is neither history of acute cardiac event nor underlying cardiac disease. In car-
diogenic pulmonary edema, clinical examination
reveals low flow state (cool periphery), S3 gallop,
cardiomegaly, jugular venous distention and wet
crackles.
NCPE is usually high flow state (warm periphery), with bounding pulses, no gallop, no jugular
venous distention and with dry crackles.
Concerning laboratory tests, in cardiogenic pulmonary edema, we may have ECG signs of ischemia or
infarction, raised cardiac enzymes and perihilar distribution of congestion in chest x-ray. Pulmonary
capillary wedge pressure exceeds 18mmHg and the ratio of pulmonary edema fluid protein to plasma protein concentration is less than 0.5. On the contrary in
NCPE, ECG and cardiac enzymes are usually normal,
on chest x-ray there is peripheral distribution of edema, pulmonary capillary wedge pressure is less than
18mmHg and the ratio of pulmonary edema fluid protein to plasma protein concentration is 0.7 or above.
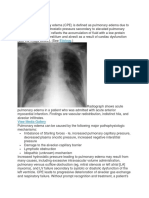
Chest x-ray findings usually appear late, at least
12 hours after the onset of cardiopulmonary symptoms. It is stated that the value of chest radiography
is limited in the differentiation of the two types of
pulmonary edema in severe cases. However, recent
studies have suggested that chest radiography can be
used to distinguish these types of pulmonary edema,
if careful attention is given to certain radiographic
features. In some studies, independent investigators
(thoracic radiologists), managed to distinguish NCPE
from cardiogenic with an accuracy of 91%. The distinguishing radiographic criteria of the two types of
pulmonary edema are listed below26-28:
1. In NCPE, the initial site of fluid accumulation is
the pulmonary interstitium including peribronchial cuffs and septal lines. This type of edema
appears predominantly as alveolar filling, since
the altered (disrupted) alveolar-capillary membrane allows for the direct accumulation in the
air spaces of fluid that is too proteinaceous to be
cleared via the interstitium. In contrast, in cardiogenic pulmonary edema filling of air spaces
(alveolar flooding) occurs when the interstitial
space is finally overwhelmed.
2. Kerley lines are never seen in increased permeability edema whereas they are a common finding in cardiogenic. The appearance of Kerley
lines in NCPE, indicates the coexistence of cardiogenic pulmonary edema.
3. Patchy or peripheral pattern of edema is relatively specific for NCPE. Air bronchograms are
frequently seen in patients with NCPE.
(Hellenic Journal of Cardiology) HJC 389
N. Kakouros, S. Kakouros
4. In cardiogenic pulmonary edema the distribution
of edema is central and pleural effusion usually
coexists.
5. In NCPE, cardiac size, vascular pedicle width
and pulmonary blood volume are usually normal. On the contrary, in cardiogenic pulmonary
edema cardiac size is increased, vascular pedicle
width is enlarged and there is inverted distribution of blood flow.
In the study of Milne et al27 in which radiography
was useful in distinguishing the type of pulmonary
edema, patients were not very ill and underwent radiography while positioned upright. In more severe
cases the distinguishing radiographic features are
neither sensitive nor specific and differentiation between the two types of edemas is more difficult28.
Management of non-cardiogenic pulmonary edema
At the time of initial injury and several hours thereafter, the patient may be free of respiratory symptoms
or signs. The earliest sign is an increase in respiratory
frequency followed shortly by dyspnea. Whatever the
underlying cause of pulmonary edema, analysis of
arterial blood to assess the type and degree of gas
exchange abnormality is necessary, followed by institution of appropriate inhalation therapeutic measures. Arterial blood gas measurement in the earlier
period will disclose a depressed PO2 and decreased
PCO2. At this point, oxygen given by mask or nasal
prongs, results in a significant increase in the arterial PO2.
Physical examination may be unremarkable,
although a few fine inspiratory rales may be audible.
With progression, the patient becomes cyanotic and
increasingly dyspneic and tachypneic. Rales are
more prominent and easily heard throughout both
lung fields along with regions of tubular breath
sounds. At this stage, hypoxemia cannot be corrected by the simple administration of oxygen, and
mechanical ventilatory assistance must be initiated
to provide adequate oxygenation of arterial blood.
Should this treatment be delayed, the combination
of increasing tachypnea and smaller tidal volume,
results in a rising PCO 2 and further fall in PO 2 to
fatal levels1.
When there is hypoxemia (PO 2 <60 mm Hg)
without hypercapnia, enrichment of the inspired gas
may suffice and can be given either by nasal prongs
or Venturi mask with reservoir, depending upon the
degree of oxygen enrichment required to elevate the
390 HJC (Hellenic Journal of Cardiology)
PO2 sufficiently. If PO2 cannot be maintained at or
near 60 mmHg despite inhalation of 100% 2 at 20
liters per minute, or if there is progressive hypercapnia, mechanical ventilation is necessary 29.
Mechanical ventilation
Mechanical ventilation is particularly useful in the
treatment of patients with NCPE. If hypoxemia is
not corrected by mechanical ventilation or if toxic
concentrations of oxygen are necessary for prolonged periods, further improvements in arterial oxygenation at the same inspired oxygen concentration
or equivalent levels of arterial oxygenation at lower
concentrations of oxygen can be achieved by increasing end-expiratory lung volumes by the addition
of positive end-expiratory pressure (PEEP)1.
In these conditions we usually apply PEEP at 520 cm H2O. The role of PEEP is to avoid collapse of
alveoli and to maintain their inflation throughout
the respiratory cycle. This actually increases FRC
and avoids the risk for further pulmonary injury29.
Although application of PEEP is effective improving
oxygenation in the majority of patients, it might pose
a risk for complications particularly when mechanical support is applied in an injured lung like in
NCPE.
Application of PEEP at very high pressures may
cause deterioration of alveolar edema, decrease
cardiac output and diminish pressure and renal
blood supply. An additional contribution may come
from greater pulmonary vascular resistance due to
increased lung volume. The result of increased right
ventricular afterload is a displacement of the interventricular septum to the left, which impedes left
ventricular diastolic filling30. Another complication
of PEEP is barotrauma, the incidence of which is
between 5-15% and it is presented as pneumomediastinum, pneumothorax and subcutaneous emphysema31.
Conclusion
Pulmonary edema is a generalized descriptive term
for the accumulation of fluid within the interstitial
and/or the alveolar spaces of the lungs. This accumulation of fluid has a cause that may be termed cardiogenic or non-cardiogenic. Pulmonary edema of
cardiogenic origin is usually due to failure of the left
side of the heart. Non-cardiogenic pulmonary edema
is a clinical syndrome characterized by simultaneous
Non-cardiogenic Pulmonary Edema
presence of severe hypoxemia, bilateral alveolar
infiltrates on chest radiograph and no evidence of
left atrial hypertension/congestive heart failure.
Prompt recognition of pulmonary edema is important to avoid life-threatening complications. The
aim of this review is to alert cardiologists, that besides known factors for the development of cardiogenic pulmonary edema, there are other significant mechanisms that cause NCPE. The reader
of this article should be able to identify the differences between cardiogenic pulmonary edema and
NCPE, to identify the most common causes of NCPE
and state the actions that are indicated in the care of
patients with NCPE.
References
1. Roland H, Ingram J, Braunwald E: Pulmonary edema: Cardiogenic and noncardiogenic. Pp.551-566, Volume 1. In Heart
Diseases by Braunwald, W.B. Saunders Co, Philadelphia,
1992.
2. Colice G: Detecting the presence and cause of pulmonary
edema. Postgratuade medicine 1993; 93: 161-166.
3. Steinberg A, Karliner J: The clinical spectrum of heroin pulmonary edema. Arch Intern Med 1968; 122: 122-125.
4. Dahlin K, Lastbon L, Ryrfeldt A: Acute lung failure induced
by tricyclic antidepressants. Toxicology & Applied Pharmacology 1997; 146: 309-316.
5. Briasoulis E, Pavlides N: Noncardiogenic pulmonary edema:
an unusual and serious complication of anticancer therapy.
Oncologist 2001; 6: 153-161.
6. Chalasani N, Roman J, Jurado R: Systemic inflammatory
response syndrome caused by chronic salicylate intoxication.
Southern Medical Journal 1996; 89: 479-482.
7. Cohen D, Post J, Ferroggiaro A, Perrone J, Foster M: Chronic
salicylism resulting in noncardiogenic pulmonary edema
requiring hemodialysis. Am Journal of kidney disease 2000;
36: 20.
8. Lam Y, Tse H, Lau C: Continuous calcium chloride infusion
for massive nifedipine overdose. Chest 2001; 119: 1280-1282.
9. Humbert V, Munn N, Hawkins R: Noncardiogenic pulmonary edema complicating massive diltiazem overdose. Chest
1991; 99: 258-260.
10. Leesar M, Martyn, Talley D, Frumin H: Noncardiogenic
pulmonary edema,complicating massive verapamil overdose. Chest 1994; 105: 606-607.
11. Bernal C, Patarca R: Hydrochlorothiazide-induced pulmonary edema and associated immunologic changes. Annals of
Pharmacotherapy 1999; 33: 172-174.
12. Vandenplas O, Hantson P, Dive A, Mahieu P: Fulminant
pulmonary edema following administration of radiocontrast
media. Acta Clinica Belgica 1990; 45: 334-339.
13. Ladner E, Schobersberger W, Sparr H, Pall H: High altitude
pulmonary edema at a medium height. Anaesthesist 1994;
43: 183-186.
14. Grisson C, Ziemmerman G, Whatley R: Endothelial selectins in acute mountain sickness and high-altitude pulmonary edema. Chest 1997; 112: 1572-1578.
15. Ayus J, Varon J, Arieff A: Hyponatremia, cerebral edema
and noncardiogenic pulmonary edema in marathon runners.
Annals of internal Medicine 2000; 132: 711-714.
16. Malik A: Mechanisms of neurogenic pulmonary edema. Circ
Res 1985; 57: 1-3.
17. Malik A, Tahamont M, Minnear F: Lung fluid and protein exchange after pulmonary vascular thrombosis. Chest 1982; 81:
451-454.
18. Johnson A, Malik A: Effect of defibrinogenation on lung
water accumulation after pulmonary microembolism in
dogs. J Appl Physiol 1980; 49: 841-844.
19. Rovinsky J, Guttmacher A: Medical, Surgical and Gynecologic complications of pregnancy. 2nd ed. Baltimore, Williams and Wilkins Co., 1965.
20. Goldbaum T, Bacos J, Lindsay J: Pulmonary edema following conversion of tachyarrythmia. Chest 1986; 89: 465.
21. Parquin F, Marchal M, Mehiri S, Herve P, Lescot B: Postpneumonectomy pulmonary edema. Analysis and risk
factors. European Journal of Cardio-Thoracic Surgery 1996;
10: 929-932.
22. Pararajasingam R, Nicholson M, Bell P, Sayers R: Noncardiogenic pulmonary edema in vascular surgery. European
Journal of vascular & Endovascular surgery 1999; 17: 93-105.
23. Urdaneta F, Lobato E, Kirby R, Horrow J: Noncardiogenic
pulmonary edema associated with protamine administration
during coronary artery bypass graft surgery. Journal of
Clinical Anesthesia 1999; 11: 675-681.
24. Brooks J: Noncardiogenic pulmonary edema immediately
following rapid protamine administration. Annals of Pharmacotherapy 1999; 33: 927-930.
25. Kindler C, Bircher A, Stulz P: Protamine-induced fulminating non-cardiogenic pulmonary edema following cardiopulmonary bypass. European Journal of Cardiothoracic Surgery 1996; 10: 463-466.
26. Kithreotis P: Noncardiogenic pulmonary edem a (ARDS).
Acute respiratory failure. Hellenic Respiratory Society
publications 2000; 452-458.
27. Milne N, Pistolesi M, Miniati M: The radiologic distinction
of cardiogenic and noncardiogenic edema. A.J.H Roentgenol 1985; 144: 879-894.
28. Aberle R, Wiener P, Webb R: Hydrostatic versus increased
permeability pulmonary edema. Diagnosis based on radiographic criteria in critically ill patients. Radiology 1988; 168: 73-75.
29. Andreadis N, Petty L: Adult respiratory distress syndrome: Problems and prognosis. Am Rev Resp Dis 1985; 132: 1344-1347.
30. Rizk W, Murray F: PEEP and pulmonary edema. Am J Med
1982; 72: 381-384.
31. Pepe P, Hudson D, Carrico J: Early application of PEEP in
patients at risk for the adult respiratory distress syndrome.
N Engl J Med 1984; 311: 281-284.
(Hellenic Journal of Cardiology) HJC 391
You might also like
- Pathophysiology of Cardiogenic Pulmonary EdemaDocument8 pagesPathophysiology of Cardiogenic Pulmonary EdemaLili Fiorela CRNo ratings yet
- Body Weight in TBDocument8 pagesBody Weight in TBNiar MarhaliNo ratings yet
- Noncardiogenic Pumonary EdemaDocument15 pagesNoncardiogenic Pumonary EdemaAnonymous OlS0WZwNo ratings yet
- Pulmonary Edema - StatPearls - NCBI BookshelfDocument7 pagesPulmonary Edema - StatPearls - NCBI BookshelfriyanasirNo ratings yet
- Noncardiogenic Pulmonary EdemaDocument19 pagesNoncardiogenic Pulmonary EdemaCláudio CalixtoNo ratings yet
- Acute Pulmonary OdemaDocument9 pagesAcute Pulmonary OdemaAnonymous ysrxggk21cNo ratings yet
- Pathophysiology of Cardiogenic Pulmonary Edema - UpToDateDocument9 pagesPathophysiology of Cardiogenic Pulmonary Edema - UpToDateRoberto López MataNo ratings yet
- Pathophysiology of Cardiogenic Pulmonary EdemaDocument13 pagesPathophysiology of Cardiogenic Pulmonary EdemaIrina DuceacNo ratings yet
- Pathophysiology of Cardiogenic Pulmonary Edema - UpToDateDocument14 pagesPathophysiology of Cardiogenic Pulmonary Edema - UpToDateStefani AtlleNo ratings yet
- Background: EtiologyDocument5 pagesBackground: Etiologylia lykimNo ratings yet
- Noncardiogenic Pulmonary EdemaDocument12 pagesNoncardiogenic Pulmonary EdemaIrina DuceacNo ratings yet
- Acute Pulmonary Edema - NEJMDocument4 pagesAcute Pulmonary Edema - NEJMSuzika Dewi0% (1)
- 3487 VJXHXVDocument13 pages3487 VJXHXVمحمد عقيليNo ratings yet
- Flash Pulmonary EdemaDocument11 pagesFlash Pulmonary EdemaEda SopNo ratings yet
- Pulmonary Embolism (PE) - Pulmonary Disorders - MSD Manual Professional EditionDocument25 pagesPulmonary Embolism (PE) - Pulmonary Disorders - MSD Manual Professional Editionpeterpavel112No ratings yet
- Cor Pulmonale An Overview 2003Document12 pagesCor Pulmonale An Overview 2003Ade Cahyo IslamiNo ratings yet
- Cor PulmonaleDocument14 pagesCor PulmonaleEvangelin MelvinNo ratings yet
- Pediatric Acute Respiratory Distress SyndromeDocument2 pagesPediatric Acute Respiratory Distress SyndromeTry Febriani SiregarNo ratings yet
- Lorraine B Ware Acute Pulmonary Edema 2005Document9 pagesLorraine B Ware Acute Pulmonary Edema 2005rdelgado3No ratings yet
- Pulmonary Infarction - Radiology Reference ArticleDocument7 pagesPulmonary Infarction - Radiology Reference ArticleHieu PhanNo ratings yet
- History and Physical Examination: EvaluationDocument3 pagesHistory and Physical Examination: EvaluationDore NanNo ratings yet
- Edema ParuDocument4 pagesEdema ParuSri BayaniNo ratings yet
- Pulmonary Edema: René P. Michel, Peter GoldbergDocument34 pagesPulmonary Edema: René P. Michel, Peter GoldbergNadya NovianiNo ratings yet
- Pathophysiology: Hypoxemic Respiratory FailureDocument6 pagesPathophysiology: Hypoxemic Respiratory FailurevidagurlNo ratings yet
- Go To:: Indications For Mechanical VentilationDocument25 pagesGo To:: Indications For Mechanical VentilationsakuraleeshaoranNo ratings yet
- ArdsDocument48 pagesArdsvmalik985No ratings yet
- Sclerodactyly, and Telangiectasis) Syndrome Accompany-: Cor PulmonaleDocument2 pagesSclerodactyly, and Telangiectasis) Syndrome Accompany-: Cor PulmonaledivinaNo ratings yet
- Cor PulmonaleDocument15 pagesCor PulmonaleRizky Zulfa Afrida100% (1)
- Pleural Disease in The Emergency Department - The ClinicsDocument25 pagesPleural Disease in The Emergency Department - The ClinicsEdgardo Vargas AlvarezNo ratings yet
- Acute Respiratory Distress SyndromeDocument9 pagesAcute Respiratory Distress SyndromeMatthew Ryan100% (2)
- Pulmonary Edema: Dr. Harsh Pandya R1 Under Guidance of DR - Nipa Nayak M.D. Asso. ProfDocument49 pagesPulmonary Edema: Dr. Harsh Pandya R1 Under Guidance of DR - Nipa Nayak M.D. Asso. ProfSef NengkoNo ratings yet
- Cor Pulmonale EmedicineDocument16 pagesCor Pulmonale EmedicineHengki Permana PutraNo ratings yet
- HAP Pulmonar 19Document106 pagesHAP Pulmonar 19jorge corolla montesNo ratings yet
- Kuliah 4 Oedem Paru PulmonaryedemaDocument43 pagesKuliah 4 Oedem Paru PulmonaryedematrianaamaliaNo ratings yet
- Copd and Cor PulmonalDocument14 pagesCopd and Cor PulmonalAldi RafaelNo ratings yet
- Acute Respiratory Failure 1Document7 pagesAcute Respiratory Failure 1Trish 0019No ratings yet
- Ards 2Document7 pagesArds 2LUCIBELLOT1No ratings yet
- Acute Respiratory Distress Syndrome - Background, Pathophysiology, EtiologyDocument5 pagesAcute Respiratory Distress Syndrome - Background, Pathophysiology, EtiologyARHNo ratings yet
- Lung PathologyDocument101 pagesLung Pathologyhm3398No ratings yet
- Pulmonary Edema: Dr. Harsh Pandya R1 Under Guidance of DR - Nipa Nayak M.D. Asso. ProfDocument49 pagesPulmonary Edema: Dr. Harsh Pandya R1 Under Guidance of DR - Nipa Nayak M.D. Asso. ProfKrisno ParammanganNo ratings yet
- Lung Head and NeckDocument26 pagesLung Head and Neckzeroun24100% (2)
- Pulmonary EmbolismDocument25 pagesPulmonary EmbolismRaymund VadilNo ratings yet
- Acute Respiratory Distress Syndrome: Epidemiology, Pathophysiology, Pathology, and Etiology in AdultsDocument30 pagesAcute Respiratory Distress Syndrome: Epidemiology, Pathophysiology, Pathology, and Etiology in Adultsmisabelgarciag18No ratings yet
- Acute Respiratory Distress SyndromeDocument36 pagesAcute Respiratory Distress Syndromedr9348345000No ratings yet
- Pathophysiology ARDSDocument2 pagesPathophysiology ARDSKim AmboyaNo ratings yet
- Cor Pulmonale by Prof. Dr. Rasheed Abd El Khalek M. DDocument45 pagesCor Pulmonale by Prof. Dr. Rasheed Abd El Khalek M. DvaishnaviNo ratings yet
- CHP 11 Cerebral Air EmbolismDocument8 pagesCHP 11 Cerebral Air EmbolismSrinivas GokulnathNo ratings yet
- Pleural Effusion in Adults-Etiology, Diagnosis, and Treatment (24.05.2019)Document10 pagesPleural Effusion in Adults-Etiology, Diagnosis, and Treatment (24.05.2019)lordiroh1No ratings yet
- Cor Pulmonale ReferensiDocument6 pagesCor Pulmonale ReferensiMiranty Aditya HadiniNo ratings yet
- Cor Pulmonale PresentationDocument17 pagesCor Pulmonale Presentationandi reskifaisNo ratings yet
- Diseases of The Respiratory SystemDocument71 pagesDiseases of The Respiratory SystemZafir SharifNo ratings yet
- The Vital Role of The Right Ventricle in The Pathogenesis of Acute Pulmonary EdemaDocument9 pagesThe Vital Role of The Right Ventricle in The Pathogenesis of Acute Pulmonary EdemaAngel LlanasNo ratings yet
- Causes and Treatment of Oedema in Patients With Heart FailureDocument16 pagesCauses and Treatment of Oedema in Patients With Heart FailureAndrés MorenoNo ratings yet
- Anglisht 2Document8 pagesAnglisht 2Ejona SuloNo ratings yet
- Cor Pulmonale - Introduction To Cor Pulmonale, Etiology and Pathophysiology of Cor Pulmonale, Epidemiology of Cor PulmonaleDocument18 pagesCor Pulmonale - Introduction To Cor Pulmonale, Etiology and Pathophysiology of Cor Pulmonale, Epidemiology of Cor PulmonaleRicky SpideyNo ratings yet
- NJCC 01 Review-MartinDocument7 pagesNJCC 01 Review-MartinCarlos Xavier Rivera RuedaNo ratings yet
- Persistent Pulmonary Hypertension of The NewbornDocument4 pagesPersistent Pulmonary Hypertension of The NewbornMarwa Adly100% (1)
- ARDS SLHDocument43 pagesARDS SLHYamto TlNo ratings yet
- Chronic Cor Pulmonale: General CardiologyDocument7 pagesChronic Cor Pulmonale: General CardiologyAnastasia Eka PuteriNo ratings yet
- Bilateral Massive Pulmonary Embolism Secondary To Decompression Sickness: A Case ReportDocument4 pagesBilateral Massive Pulmonary Embolism Secondary To Decompression Sickness: A Case ReportPatricio Toledo FuenzalidaNo ratings yet
- A Simple Guide to Pulmonary Infarction, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Pulmonary Infarction, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Glucocorticoid Effects On The Immune SystemDocument92 pagesGlucocorticoid Effects On The Immune SystemdarmariantoNo ratings yet
- TB ImmunotherapyDocument25 pagesTB ImmunotherapydarmariantoNo ratings yet
- Cancer Care Ontario's Symptom Management Guide-To-Practice Loss of AppetiteDocument31 pagesCancer Care Ontario's Symptom Management Guide-To-Practice Loss of AppetitedarmariantoNo ratings yet
- Anatomy of The Thorax (CT)Document7 pagesAnatomy of The Thorax (CT)darmariantoNo ratings yet
- Revisión DressDocument10 pagesRevisión Dressvintage20No ratings yet
- Immunomodulators For AsthmaDocument7 pagesImmunomodulators For AsthmadarmariantoNo ratings yet
- Immunity Against MycobacteriaDocument9 pagesImmunity Against MycobacteriadarmariantoNo ratings yet
- MS 1 Mastery TestDocument16 pagesMS 1 Mastery TestRika MaeNo ratings yet
- Clinical Manifestations and Diagnosis of Edema in AdultsDocument7 pagesClinical Manifestations and Diagnosis of Edema in AdultsOscar Castro CuaquiraNo ratings yet
- Emergency PDFDocument17 pagesEmergency PDFMrudu Ranjan TripathyNo ratings yet
- Cfu Med SurgDocument25 pagesCfu Med SurgCharlene Jacobe CornistaNo ratings yet
- Pulmonary Insufficiency:: Acute Respiratory Distress SyndromeDocument72 pagesPulmonary Insufficiency:: Acute Respiratory Distress SyndromeJannen CasasNo ratings yet
- GROUP 3 Hepatitis Cirrhosis Nursing CareDocument15 pagesGROUP 3 Hepatitis Cirrhosis Nursing CareMutia AmandaNo ratings yet
- PathoDocument2 pagesPathohrry stylesNo ratings yet
- Test Bank For Caring For Older Adults Holistically 5th Edition, MaryDocument28 pagesTest Bank For Caring For Older Adults Holistically 5th Edition, MaryILL108100% (1)
- COPD Case PresentationDocument50 pagesCOPD Case PresentationNaresh JeengarNo ratings yet
- Fisiologia Basica de La AlturaDocument12 pagesFisiologia Basica de La AlturaMARIA MARCELINA PACHECHO VARGASNo ratings yet
- Heart Failure: Dr.K.Sathish Kumar, MD (Hom) .Document11 pagesHeart Failure: Dr.K.Sathish Kumar, MD (Hom) .mnr hmcNo ratings yet
- Toxicology Case StudyDocument4 pagesToxicology Case Studyhazrat balindongNo ratings yet
- Inhalation InjuryDocument59 pagesInhalation InjuryElle LibalibNo ratings yet
- NCP: Gestational HTN - Preeclampsiaeclampsia - Hellp SyndromeDocument23 pagesNCP: Gestational HTN - Preeclampsiaeclampsia - Hellp SyndromeKath100% (2)
- Myocarditis Diagnosis AdultsDocument44 pagesMyocarditis Diagnosis AdultsGiga HasabiNo ratings yet
- YeDocument39 pagesYeRhea RaveloNo ratings yet
- Reexpansion Pulmonary Edema : UpdateDocument6 pagesReexpansion Pulmonary Edema : UpdateWenny EudensiaNo ratings yet
- Lecture 01 - CVSDocument45 pagesLecture 01 - CVSHeeb WardaNo ratings yet
- Acute Respiratory Failure Concept MapDocument1 pageAcute Respiratory Failure Concept Mapjenievysenerez100% (1)
- NCLEX QuestionsDocument27 pagesNCLEX QuestionsAngie MandeoyaNo ratings yet
- Clinical Case StudyDocument39 pagesClinical Case Studyapi-240895351No ratings yet
- Medical Surgical ComprehensiveDocument15 pagesMedical Surgical ComprehensiveMatt Lao DionelaNo ratings yet
- Symptoms of CvsDocument25 pagesSymptoms of CvsstudymedicNo ratings yet
- Cardio MnemonicsDocument21 pagesCardio MnemonicsAilene Ponce FillonNo ratings yet
- Heart Failure Clinical Presentation - History, Physical Examination, Predominant Right-Sided Heart FailureDocument9 pagesHeart Failure Clinical Presentation - History, Physical Examination, Predominant Right-Sided Heart FailureAizel ManiagoNo ratings yet
- HAADDocument52 pagesHAADElsayed AbdallahNo ratings yet
- Inistitutional Assessementknowledge Test For Comprhenssive NursingDocument19 pagesInistitutional Assessementknowledge Test For Comprhenssive NursingkassahunNo ratings yet
- VENTILATOR PREPARATION and SETTINGDocument22 pagesVENTILATOR PREPARATION and SETTINGArtha WigunaNo ratings yet
- Cerebral EdemaDocument15 pagesCerebral EdemaMae FlagerNo ratings yet