Professional Documents
Culture Documents
Respinursing 110215173709 Phpapp02 PDF
Respinursing 110215173709 Phpapp02 PDF
Uploaded by
zhai bambalanOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Respinursing 110215173709 Phpapp02 PDF
Respinursing 110215173709 Phpapp02 PDF
Uploaded by
zhai bambalanCopyright:
Available Formats
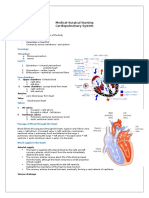
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
MEDICAL AND SURGICAL NURSING
Respiratory System
Lecturer: Mark Fredderick R. Abejo RN,MAN
MS
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
ANATOMY OF RESPIRATORY SYSTEM
2.
OXYGENATON: the dynamic interaction of gases in the body for
the purpose of delivering adequate oxygen essential for cellular
survival
3.
RESPIRATORY SYSTEM MAIN FUNCTION:
GAS EXCHANGE
I.
4.
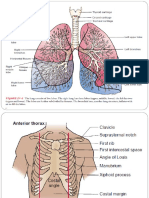
Upper Respiratory Tract
A. Functions
1. Filtering
2. Warming and moistening
3. Humidification
B. Parts
1. Nose - made up of framework of cartilages; divided
into R and L by the nasal septum.
2. Paranasal Sinuses includes four pair of bony
cavities that are lined with nasal mucosa and ciliated
epithelium.
3. Tubernate Bones ( Conchae )
4. Pharynx muscular passageway for both food and
air
Nasopharynx
Oropharynx
Laryngopharynx
5. Tonsils and Adenoids
6. Larynx voice production, coughing reflex
Made up of framework of:
Epiglottis valve that covers the opening
to the larynx during swallowing.
Glottis opening between the vocal cords
Hyoid bone u shaped bone in neck
Cricoid cartilage
Thyroid cartilage, forms the Adams apple
Arythenoid cartilage
Speech production and cough reflex
Vocal cords
7. Trachea - consists of cartilaginous rings
Passageway of air
Site of tracheostomy (4th-6th tracheal ring)
Bronchi
Lobar Bronchi: 3 R and 2 L
Segmental Bronchi: 10 R and 8 L
Subsegmental Bronchi
Bronchioles
Terminal Bronchioles
Respiratory Bronchioles, considered to be
the transitional passageways between the
conducting airways and the gas exchange
Alveoli
functional cellular units or gas-exchange
units of the lungs.
O2 and CO2 exchange takes place
Made up of about 300 million
TYPE 1 - provide structure to the alveoli
TYPE 2 - secrete SURFACTANT, reduces surface
tension; increases alveoli stability & prevents their
collapse
TYPE 3 alveolar cell macrophages, destroys
foreign material, such as bacteria
Lecithin
Sphingomyelin
L/S ratio indicates lung maturity
2:1 normal
1:2 immature lungs
PULMONARY CIRCULATION
Provides for reoxygenation of blood and release of CO2
PULMONARY ARTERIES, carry blood from
the heart to the lungs.
PULMONARY VEINS, is a large blood vessel
of the circulatory system that carries blood
from the lungs to the left atrium of the heart.
II. Lower respiratory tract
A. Function: facilitates gas exchange
B. Parts
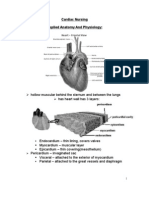
1. Lungs, are paired elastic structure enclosed in the
thoracic cage, which is an airtight chamber with
distensible walls.
Right 3 lobes, 10 segments
Left 2 lobes, 8 segments
Client post pneumonectomy affected side to promote expansion
Post lobectomy unaffected side to promote drainage
MS
RESPIRATORY MUSCLES
PRIMARY: diaphragm and external intercostal muscles
ACCESORY: sternocleidomastoid (elevated sternum),
the scalene muscles (anterior, middle and posterior
scalene) and the nasal alae
Pleural cavity
Parietal
Visceral
Pleural Fluid: prevents pleural friction rub
(as seen in pneumonia and pleural effusion)
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
PHYSIOLOGY OF RESPIRATORY SYSTEM
VENTILATION: The movement of air in and out of the airways.
The thoracic cavity is an air tight chamber. the floor of
this chamber is the diaphragm.
Inspiration: contraction of the diaphragm (movement of
this chamber floor downward) and contraction of the
external intercostal muscles increases the space in this
chamber. lowered intrathoracic pressure causes air to
enter through the airways and inflate the lungs.
Expiration: with relaxation, the diaphragm moves up and
intrathoracic pressure increases. this increased pressure
pushes air out of the lungs. expiration requires the elastic
recoil of the lungs.
Inspiration normally is 1/3 of the respiratory cycle and
expiration is 2/3.
Exchange of gases occurs because of differences in
partial pressures.
Oxygen diffuses from the air into the blood at the alveoli
to be transported to the cells of the body.
Carbon dioxide diffuses from the blood into the air at the
alveoli to be removed from the body.
NEUROCHEMICAL CONTROL
MEDULLA OBLONGATA respiratory center
initiates each breath by sending messages to primary
respiratory muscles over the phrenic nerve
has inspiration and expiration centers
PONS has 2 respiration centers that work with the
inspiration center to produce normal rate of breathing
1. PNEUMOTAXIC CENTER affects the inspiratory
effort by limiting the volume of air inspired
2. APNEUSTIC CENTER prolongs inhalation
NOTE: Chemoreceptors responds to changes in ph, increased
PaCO2 = increase RR
DRIVING FORCE FOR AIR FLOW
Airflow driven by the pressure difference between
atmosphere (barometric pressure) and inside the lungs
(intrapulmonary pressure).
RESPIRATORY EXAMINATION AND
ASSESSMENT
Background information
A. Abnormal patterns of breathing
1. Sleep Apnea
cessation of airflow for more than 10 seconds more
than 10 times a night during sleep
causes: obstructive (e.g. obesity with upper narrowing,
enlarged tonsils, pharyngeal soft tissue changes in
acromegaly or hypothyroidism)
2. Cheyne-Stokes
periods of apnoea alternating with periods of
hyperpnoae
pathophysiology: delay in medullary chemoreceptor
response to blood gas changes
causes
left ventricular failure
brain damage (e.g. trauma, cerebral,
haemorrhage)
high altitude
3. Kussmaul's (air hunger)
deep rapid respiration due to stimulation of respiratory
centre
causes: metabolic acidosis (e.g. diabetes mellitus,
chronic renal failure)
4. Hyperventilation
complications: alkalosis and tetany
causes: anxiety
5. Ataxic (Biot)
irregular in timing and deep
causes: brainstem damage
6. Apneustic
post-inspiratory pause in breathing
causes: brain (pontine) damage
AIRWAY RESISTANCE
Resistance is determined chiefly by the radius size of the
airway.
Causes of Increased Airway Resistance
1. Contraction of bronchial mucosa
2. Thickening of bronchial mucosa
3. Obstruction of the airway
4. Loss of lung elasticity
RESPIRATION
The process of gas exchange between atmospheric air
and the blood at the alveoli, and between the blood cells
and the cells of the body.
MS
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
- asthma
- carcinoma of bronchus
- left ventricular failure
- interstitial lung disease
- ACE inhibitors
Sputum
volume
type (purulent, mucoid, mucopurulent)
presence or absence of blood?
Stridor
croaking noise loudest on inspiration
is a sign that requires urgent attention
causes: (obstruction of larynx, trachea or large
broncus)
- acute onset (minutes)
inhaled foreign body
acute epiglottitis
anaphylaxis
toxic gas inhalation
- gradual onset (days, weeks)
laryngeal and pharyngeal tumours
crico-arytenoid rheumatoid arthritis
bilateral vocal cord palsy
tracheal carcinoma
paratracheal compression by lymph nodes
post-tracheostomy or intubation
granulomata
Hoarseness
causes include:
- laryngitis
- laryngeal nerve palsy associated with
carcinoma of lung
- laryngeal carcinoma
7. Paradoxical
the abdomen sucks with respiration (normally, it
pouches uotward due to diaphragmatic descent)
causes: diaphragmatic paralysis
B. Cyanosis
1. Refers to blue discoloration of skin and mucous
membranes , is due to presence of deoxygenated
haemoglobin in superficial blood vessels
2. Central cyanosis = abnromal amout of deoxygenated
haemoglobin in arteries and that blue discoloration is
present in parts of body with good circulation such as
tongue
3. Peripheral cyanosis = occurs when blood supply to a
certain part of body is reduced, and the tissue extracts
more oxygen from normal from the circulating blood, e.g.
lips in cold weather are often blue, but lips are spared
4. Causes of cyanosis
Central cyanosis
decreased arterial saturation
decreased concentration of inspired oxygen:
high altitude
lung disease: COPD with cor pulmoale,
massive pulmonary embolism
right to left cardiac shunt (cyanotic congenital
heart disease)
polycythaemia
haemoglobin abnromalities (rare):
methaemoglobinaemia, sulphaemoglobinaemia
Peripheral cyanosis
all causes of central cyanosis cause peripheral
cyanosis
exposure to cold
reduced cardiac output: left ventricular failure or
shock
arterial or venous obstruction
The Hands
Clubbing
commonly cause by respiratory disease (but NOT
emphysema or chronic bronchitis)
occasionally, clubbing is associated with hypertrophic
pulmonary osteoarthropathy (HPO)
characterised by periosteal inflammation at distal ends
of long bones, wrists, ankles, metacarpals and
metatarsals
sweelling and tenderness over wrists and other
involved areas
Position: patient sitting over edge of bed
General appearance
look for the following
Dyspnea
normal respiratory rate < 14 each minute
tachypnoea = rapid respiratory rate
are accessory muscles being used (sternomastoids,
platysma, strap muscles of neck) - characteristically,
the accessory muscles cause elevation of shoulders
with inspiration and aid respiration by increasing
chest expansion
Cyanosis
Character of cough
ask patient to cough several times
lack of usual explosive beginning may indicate
vocal cord paralysis (bovine cough)
muffled, wheezy ineffective cough suggests airflow
limitation
very loose productive cough suggests excessive
bronchial secretions due to:
- chronic bronchitis
- pneumonia
- bronchiectasis
dry irritating cough may occur with:
- chest infection
MS
Staining
staining of fingers - sign of cigarette smoking (caused by
tar, not nicotine)
Wasting and weakness
Pulse rate
Flapping tremor (asterixis) - unreliable sign
ask patient to dorsiflex wrists and spread out fingers, with
arms outstretched
flapping tremor may occur with severe carbon dioxide
retention (severe chronic airflow limitation)
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
The Face
Funnel chest (pectus excavatum)
developmental defect involving a localised depression
of lower end of sternum in severe cases, lung capacity
may be restricted
Eyes
Horner's syndrome? (constricted pupil, partial ptosis and
loss of sweating which can be due to apical lung tumour
compressing sympathetic nerves in neck)
Nose
polpys? (associated with asthma)
engorged turbinates? (various allergic conditions)
deviated septum? (nasal obstruction)
Mouth and tongue
look for central cyanosis
evidence of upper respiratory tract infection (a reddened
pharynx and tonsillar enlargement with or without a
coating of pus)
broken tooth - may predispose to lung abscess or
pneumonia
sinusitis is indicated by tenderness over the sinuses on
palpation
some patients with obstructive sleep apnoea will be obese
with a receding chin, a small pharynx and a short thick neck
Harrison's sulcus
innar depression of lower ribs just above costal margins
at site of attachment of diaphragm
causes:
severe asthma in childhood
rickets
Kyphosis , exaggerated forward curvature of spine
Scoliosis , lateral bowing
Kyphoscoliosis: causes:
idiopathic (80%)
secondary to poliomyelitis (inflammation involving
grey matter of cord)
(note: severe thoracic kyphoscoliosis may reduce lung
capacity and increase work of breathing)
Lesions of chest wall
scars - previous thoracic operations or chest drains for a
previous pneumothorax or pleural effusion
thoracoplasty (was once performed to remove TB, but
no longer is because of effective antituberculosis
chemotherapy) invovled removal of large number of
ribs on one side to achieve permanent collapse of
affected lung
erythema and thickening of skin may occur in
radiotherapy; there is a sharp demarcation between
abnormal and normal skin
Diffuse swelling of chest wall and neck
pathophysiology: air tracking from the lungs
causes:
pneumothorax
rupture of oesopahagus
Prominent veins
cause: superior vena caval obstruction
Asymmetry of chest wall movements
assess this by inspecting from behind patient, looking
down the clavicles during moderate respiration diminished movement indicates underlying lung disease
the affected side will showed delayed or decreased
movement
causes of reduced chest wall movements on one side are
localised:
localised pulmonary fibrosis
consolidation
collapse
pleural effusion
pneumothroax
causes of bilateral reduced chest wall movements are
diffuse:
chronic airflow limitation
diffuse pulmonary fibrosis
The Trachea
causes of tracheal displacement:
toward the side of the lung lesion
upper lobe collapse
upper lobe fibrosis
pneumonectomy
upper mediastinal masses, such as retrosternal goitre
tracheal tug (finger resting on trachea feels it move inferiorly
with each inspiration) is a sign of gross overexpansion of the
chest because of airflow obstruction
The Chest: inspection
Shape and symmetry of chest
Barrel shaped
anteroposterior (AP) diameter is increased compared
with lateral diameter
causes: hyperinflation due to asthma, emphysema
Pigeon chest (pectus carinatum)
localised prominence (outward bowing of sternum and
costal cartilages)
causes:
manifestation of chronic childhood illness (due to
repeated strong contractions of diaphragm while
thorax is still pliable)
rickets
MS
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
The Chest: palpation
cardiac dullness:
area of cardiac dullness is uaully present on left side of
chest
this may decrease in emphysema or asthma
chest expansion
place hands firmly on chest wall with fingers extending
around sides of chest (fugyre 4.5)
as patient takes a big breath in, the thumbs should move
symmetrically apart about 5 cm
reduced expansion on one side indicates a lesion on that
side
note: lower lobe expansion is tested here; upper lobe is
tested for on inspection (as above)
apex beat
(discussed in cardiac section)
for respiratory diseases:
displacement toward site of lesion - can be caused by:
collapse of lower lobe
localised pulmonary fibrosis
displacement away from site of lesion - can be caused
by:
pleural effusion
tension pneumothorax
apex beat is often impalpable in a chest which is
hyperexpanded secondary to chronic airflow limitation
vocal fremitus
palpate chest wall with palm of hand while patient repeats
"99"
front and back of chest are each palpated in 2 comparable
positions with palms; in this way differences in vibration on
chest wall can be detected
causes of change in vocal fremitus are the same as those for
vocal resonance (see later)
ribs
gently compress chest wall anteroposteriorly and laterally
localised pain suggests a rib fracture (may be secondary to
trauma or spontaneous as a result of tumour deposition or
bone disease)
The Chest: auscultation
breath sounds
introduction
one should use the diaphragm of stethoscope to listen
to breath sound in each area, comparing each side
remember to listen high up into the axillae
remember to use bell of stethoscope to listen to lung
from above the clavicles
quality of breath sounds
normal breat sounds
are heard with stethoscope over all parts of
chest, produced in airways rather than alveoli
(although once they had been thought to arise
from alveoli (vesicles) and are therefore called
vesicular sounds)
normal (vesicular) breath sounds are louder and
longer on inspiration than on expiration; and
there is no gap between the inspiratory and
expiratory sounds
bronchial breath sounds
turbulence in large airways is heard without
being filtered by the alveoli, and therefore
produce a different quality; they are heard over
the trachea normally, but not over the lungs
are audible throughout expiration, and often
there is a gap between inspiration and expiration
are heard over areas of consolidation since solid
lung conducts the sound of turbulence in main
airways to peripheral areas without filtering
causes include:
- lung consolidation (lobar pneumonia) common
- localised pulmonary fibrosis - uncommon
- pleural effusion (above the fluid) uncommon
- collapsed lung (e.g. adjacent to a pleural
effusion) - uncommon
amphoric sound = when breath sounds over a
large cavity have an exaggerated bronchial
quality)
intensity of breath sounds
causes of reduced breath sounds include:
chronic airflow limitation (especially
emphysema)
pleural effusion
pneumothorax
pneumonia
large neoplasm
pulmonary collapse
added (adventitious) sounds
two types of added sounds: continuous (wheezes) and
interrupted (crackles)
wheezes
may be heard in expiration or inspiration or both
pathophysiology of wheezes - airway narrowing
an inspiratory wheeze implies severe airway
narrowing
The Chest: percussion
with left hand on chest wall and fingers slightly separated and
aligned with ribs, the middle finger is pressed firmly against
the chest; pad of right middle finger is used to strike firmly the
middle phalanx of middle finger of left hand
percussion of symmetrical areas of:
anterior (chest)
posterior (back) (ask patient to move elbows forward
across the front of chest - this rotates the scapulae
anteriorly, i.e. moves it out of the way)
axillary region (side)
supraclavicular fossa
percussion over a solid structure (e.g. liver, consolidated lung)
produces a dull note
percusion over a fluid filled area (e.g. pleural effusion)
produces an extremely dull (stony dull) note
percussion over the normal lung produces a resonant note
percussion over a hollow structure (e.g. bowel, pneumothorax)
produces a hyperresonsant note
liver dullness:
upper level of liver dullness is determined by percussing
down the anterior cehst in mid-clavicular line
normally, upper level of liver dullness is 6th rib in right
mid-clavicular line
if chest is resonant below this level, it is a sign of
hyperinflation usually due to emphysema, asthma
MS
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
causes of wheezes include:
- asthma (often high pitched) - due to muscle
spasm, mucosal oedema, excessive
secretions
- chronic airflow diseases - due to mucosal
oedema and excessive secretions
- carcinoma causing bronchial obstruction tends to cause a localised wheeze which is
monophonic and does not clear with
coughing
crackles
some terms not to use include rales (low pitched
crackles) and creptitations (high pitched
crackles)
crackles are due to collapse of peripheral
airways on expiration and sudden opening on
inspiration
early inspiratory crackles
- suggests disease of small airways
- characteristic of chronic airflow limitation
- are only heard in early inspiration
late or paninspiratory crackles
- suggests disease confined to alveoli
- may be fine, medium or coarse
- fine crackles - typically caused by
pulmonary fibrosis
- medium crackles - typically caused by left
ventricular failure (due to presence of
alveolar fluid)
- coarse crackes - tend to change with
coughing; occur with any disease that leads
to retention of secretions; commonly occur
in bronchiectasis
pleural friction rub
when thickened, roughened pleural surfaces rub
together, a continuous or intermittent grating
sound may be heard
suggests pleurisy, which may be secondary to
pulmonary infarction or pnuemonia
pulmonary thromboembolism
marked obesity
sleep apnoea
severe kyphoscoliosis
The Abdomen
palpate liver for enlargement due to secondary deposits of
tumour from lung, or right heart failure
Other
Permberton's sign
ask patient to lift arms over head
look for development of facial plethora, inspiratory
stridor, non-pulsatile elevation of jugular venous
pressure
occurs in vena caval obstruction
Feet
inspect for oedema or cyanosis (clues of cor
pulmonale)
look for evidence of deep vein thrombosisd
Respiratory rate on exercise and positioning
patients complaining of dyspnoea should have their
respiratory rate measured at rest, at maximal tolerated
exertion and supine
if dyspnoea is not accompanied by tachypnoea when
a patient climbs stairs, one should consider
malingering
look for paradoxical inward motion of abdomen
during inspiration when patient is uspine (indicating
diaphragmatic paralysis)
Temperature: fever may accompany any acute or chronic
chest infection
DIAGNOSTIC EVALUATION
1. Skin Test: Mantoux Test or Tuberculin Skin Test
vocal resonanance
gives information about lungs' ability to transmit sounds
consolidated lung tends to transmit high frequencies so
that speech heard through stethoscope takes a bleeting
quality (aegophony); when a patient with aegophony says
"bee" it sounds like "bay"
listen over each part of chest as patient says "99"; over
consolidated lung, the numbers will become clearly
audible; over normal lung, the sound is muffled
whispering pectoriloquy - vocal resonance is increased to
such an extent that whispered speech is distinctly heard
This is used to determine if a person has been infected or
has been exposed to the TB bacillus.
This utilizes the PPD (Purified Protein Derivatives).
The PPD is injected intradermally usually in the inner
aspect of the lower forearm about 4 inches below the
elbow.
The test is read 48 to 72 hours after injection.
(+) Mantoux Test is induration of 10 mm or more.
But for HIV positive clients, induration of about 5 mm is
considered positive
Signifies exposure to Mycobacterium Tubercle bacilli
The Heart
lie patient at 45 degrees
measure jugular venous plse for right heart failure
examine preacordium; pay close attention to pulmonary
component of P2 (which is best heard at 2nd intercostal
space on left) and should not be louder than A2; if it is
louder, suspect pulmonary hypertension
cor pulmonale (also called pulmonary hypertensive heart
disease) may be due to:
chronic airflow limitation (emphysema)
pulmonary fibrosis
MS
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
2. Pulse Oximeter
Non-invasive method of continuously monitoring he
oxygen saturation of hemoglobin
A probe or sensor is attached to the fingertip, forehead,
earlobe or bridge of the nose
Sensor detects changes in O2 sat levels by monitoring
light signals generated by the oximeter and reflected by
the blood pulsing through the tissue at the probe
Normal SpO2 = 95% - 100%
< 85% - tissues are not receiving enough O2
Results unreliable in:
Cardiac arrest
Shock
Use of dyes or
vasoconstrictors
Severe anemia
High carbon
monoxide Level
Clear MRI images of lung airways during breathing.
6. Flouroscopy
Studies the lung and chest in motion
Involves the continuous observation of an image
reflected on a screen when exposed to radiation in the
manner of television screen that is activated by an
electrode beam.
Structures of different densities that intercept the X-ray
beam are visualized on the screen in silhouette
3. Chest X-ray
This is a NON-invasive procedure involving the use of xrays with minimal radiation.
The nurse instructs the patient to practice the on cue to
hold his breath and to do deep breathing
Instruct the client to remove metals from the chest.
Rule out pregnancy first.
7. Indirect Bronchography
A radiopaque medium is instilled directly into the
trachea and the bronchi and the outline of the entire
bronchial tree or selected areas may be visualized
through x-ray.
It reveals anomalies of the bronchial tree and is
important in the diagnosis of bronchiectasis.
5. Computed Tomography (CT Scan) and Magnetic Resonance
Imaging ( MRI )
The CT scan is a radiographic procedure that utilizes
x-ray machine.
The MRI uses magnetic field to record the H+ density of
the tissue.
It does NOT involve the use of radiation.
The contraindications for this procedure are the
following: patients with implanted pacemaker,
patients with metallic hip prosthesis or other metal
implants in the body.
Nursing interventions BEFORE Bronchogram
Secure written consent
Check for allergies to sea foods or iodine or
anesthesia
NPO for 6 to 8 hours
Pre-op meds: atropine SO4 and valium,
topical anesthesia sprayed; followed by local
anesthetic injected into larynx. The nurse must
have oxygen and anti spasmodic agents ready.
Nursing interventions AFTER Bronchogram
Side-lying position
NPO until cough and gag reflexes returned
Instruct the client to cough and deep breathe
client
8. Bronchoscopy
This is the direct inspection and observation of the
larynx, trachea and bronchi through a flexible or rigid
bronchoscope.
Passage of a lighted bronchoscope into the bronchial
tree for direct visualization of the trachea and the
tracheobronchial tree.
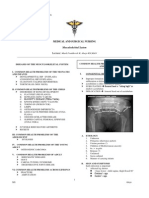
This chest CT scan shows a cross-section of a person
with bronchial cancer. The two dark areas are the lungs. The light
areas within the lungs represent the cancer.
MS
Diagnostic uses:
To examine tissues or collect secretions
To determine location or pathologic process
and collect specimen for biopsy
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
MS
To evaluate bleeding sites
To determine if a tumor can be resected
surgically
9. Lung Scan
Procedure using inhalation or I.V. injection of a
radioisotope, scans are taken with a scintillation camera.
Imaging of distribution and blood flow in the lungs.
(Measure blood perfusion)
Confirm pulmonary embolism or other blood- flow
abnormalities
Therapeutic uses
To Remove foreign objects from
tracheobronchial tree
To Excise lesions
To remove tenacious secretions obstructing the
tracheobronchial tree
To drain abscess
To treat post-operative atelectasis
Nursing interventions BEFORE Bronchoscopy
Informed consent/ permit needed
Explain procedure to the patient, tell him what
to expect, to help him cope with the unkown
Atropine (to diminish secretions) is
administered one hour before the procedure
About 30 minutes before bronchoscopy,
Valium is given to sedate patient and allay
anxiety.
Topical anesthesia is sprayed followed by
local anesthesia injected into the larynx
Instruct on NPO for 6-8 hours
Remove dentures, prostheses and contact lenses
The patient is placed supine with
hyperextended neck during the procedure
Nursing interventions BEFORE the procedure:
Allay the patients anxiety
Instruct the patient to Remain still during the
procedure
Nursing interventions AFTER the procedure
Check the catheter insertion site for bleeding
Assess for allergies to injected radioisotopes
Increase fluid intake, unless contraindicated.
10. Sputum Examination
Laboratory test
Indicated for microscopic examination of the sputum:
Gross appearance, Sputum C&S, AFB staining, and
for Cytologic examination/ Papanicolaou examination
Nursing interventions AFTER Bronchoscopy
Put the patient on Side lying position
Tell patient that the throat may feel sore with .
Check for the return of cough and gag reflex.
Check vasovagal response.
Watch for cyanosis, hypotension, tachycardia,
arrythmias, hemoptysis, and dyspnea. These
signs and symptoms indicate perforation of
bronchial tree. Refer the patient immediately!
Nursing interventions:
Early morning sputum specimen is to be
collected (suctioning or expectoration)
Rinse mouth with plain water
Use sterile container.
Sputum specimen for C&S is collected before
the first dose of anti-microbial therapy.
For AFB staining, collect sputum specimen for
three consecutive mornings.
11. Biopsy of the Lungs
Percutaneous removal of a small amount of lung tissue
For histologic evaluation
Transbronchoscopic biopsydone during bronchoscopy,
Percutaneous needle biopsy
Open lung biopsy
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
Nursing interventions BEFORE the procedure:
Withhold food and fluids
Place obtained written informed consent in the
patients chart.
LUNG CAPACITIES:
Functional Residual Capacity (ERV 1100 mL + RV 1200 mL =
2300 mL )
The volume of air that remains in the lungs after normal,
quiet exhalation
Inspiratory Capacity (TV 500 mL + IRV 3000 mL = 3500 mL )
The amount of air that a person can inspire maximally
after a normal expiration
Vital capacity (IRV 3000 mL + TV 500 mL + ERV 1100 mL =
4600 mL )
The maximum volume of air that can be exhaled after a
maximum inhalation
Reduced in COPD
Total Lung Capacity (IRV 3000 mL + TV 500 mL + ERV 1100
mL + RV 1200 mL = 5800 mL )
Total of all four volumes
Nursing interventions AFTER the procedure:
Observe the patient for signs of Pneumothorax
and air embolism
Check the patient for hemoptysis and
hemorrhage
Monitor and record vital signs
Check the insertion site for bleeding
Monitor for signs of respiratory distress
12. Lymph Node Biopsy
Scalene or cervicomediastinal
To assess metastasis of lung cancer
13. Pulmonary Function Test / Studies
Non-invasive test
Measurement of lung volume, ventilation, and diffusing
capacity
Nursing interventions:
Document bronchodilators or narcotics used
before testing
Allay the patients anxiety during the testing
14. Arterial Blood Gas
Laboratory test
Indicate respiratory functions
Assess the degree to which the lungs are able to provide
adequate oxygen and remove CO2
Assess the degree to which the kidneys are able to
reabsorb or excrete bicarbonate.
Assessment of arterial blood for tissue oxygenation,
ventilation, and acid-base status
Arterial puncture is performed on areas where good
pulses are palpable (radial, brachial, or femoral).
Radial artery is the most common site for withdrawal of
blood specimen
Nursing interventions:
Utilize a 10-ml. Pre-heparinized syringe to
prevent clotting of specimen
Soak specimen in a container with ice to
prevent hemolysis
If ABG monitoring will be done, do Allens
test to assess for adequacy of collateral
circulation of the hand (the ulnar arteries)
LUNG VOLUMES: (ITER)
Inspiratory reserve volume (3000 mL)
The maximum volume that can be inhaled following a
normal quiet inhalation.
Tidal volume (500 mL)
The volume of air inhaled and exhaled with normal quiet
breathing
Expiratory reserve volume (1100 mL)
The maximum volume that can be exhaled following the
normal quiet exhalation
Residual volume (1200 mL)
The volume of air that remains in the lungs after forceful
exhalation
MS
15. Pulmonary Angiography
This procedure takes X-ray pictures of the pulmonary
blood vessels (those in the lungs).
Because arteries and veins are not normally seen in an Xray, a contrast material is injected into one or more
arteries or veins so that they can be seen.
10
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
16. Ventilation - Perfusion Scan
Radioactive albumin injection is part of a nuclear scan
test that is performed to measure the supply of blood
through the lungs.
After the injection, the lungs are scanned to detect the
location of the radioactive particles as blood flows
through the lungs.
The ventilation scan is used to evaluate the ability of air
to reach all portions of the lungs. The perfusion scan
measures the supply of blood through the lungs.
A ventilation and perfusion scan is most often performed
to detect a pulmonary embolus. It is also used to evaluate
lung function in people with advanced pulmonary disease
such as COPD and to detect the presence of shunts
(abnormal circulation) in the pulmonary blood vessels.
RESPIRATORY CARE MODALITIES
1. Oxygen Therapy
Oxygen is a colorless, odorless, tasteless, and dry gas that
supports combustion
Man requires 21% oxygen from the environment in order
to survive
Indication: Hypoxemia
Signs of Hypoxemia
o Increased pulse rate
o Rapid, shallow respiration and dyspnea
o Increased restlessness or lightheadedness
o Flaring of nares
o Substernal or intercostals retractions
o Cyanosis
17. Thoracentesis
Procedure suing needle aspiration of intrapleural fluid or
air under local anesthesia
Specimen examination or removal of pleural fluid
Nursing intervention BEFORE Thoracentesis
Secure consent
Take initial vital signs
Instruct to remain still, avoid coughing during
insertion of the needle
Inform patient that pressure sensation will be
felt on insertion of needle
MS
Low flow oxygen provides partial oxygenation with patient
breathing a combination of supplemental oxygen and room air.
Low-flow administration devices:
o Nasal Cannula 24-45% 2-6 LPM
o Simple Face Mask 0-60% 5-8 LPM
o Partial Rebreathing Mask 60-90%
6-10 LPM
o Non-rebreathing Mask
95-100% 6-15 LPM
o Croupette
o Oxygen Tent
Nursing intervention DURING the procedure:
Reassess the patient
Place the patient in the proper position:
Upright or sitting on the edge of
the bed
Lying partially on the side,
partially on the back
High flow oxygen provides all necessary oxygenation, with
patients breathing only oxygen supplied from the mask and
exhaling through a one-way vent.
High flow administration devices
o Venturi Mask
24-40% 4-10 LPM
Preferred for clients with COPD because it
provides accurate amount of oxygen.
o Face Mask
o Oxygen Hood*
o Incubator / isolette*
Nursing interventions after Thoracentesis
Assess the patients respiratory status
Monitor vital signs frequently
Position the patient on the affected side, as
ordered, for at least 1 hour to seal the puncture
site
Turn on the unaffected side to prevent leakage
of fluid in the thoracic cavity
Check the puncture site for fluid leakage
Auscultate lungs to assess for pneumothorax
Monitor oxygen saturation (SaO2) levels
Bed rest
Check for expectoration of blood
Note: * can be used for both low and high flow administration
11
The nurse should prevent skin breakdown by checking
nares, nose and applying gauze or cotton as necessary
Ensure that COPD patients receive only LOW flow
oxygen because these persons respond to hypoxia, not
increased CO levels.
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
2. Tracheobronchial suctioning
Suction only when necessary not routinely
Use the smallest suction catheter if possible
Client should be in semi or high Fowlers position
Use sterile gloves, sterile suction catheter
Hyperventilate client with 100% oxygen before and
after suctioning
Insert catheter with gloved hand (3-5 length of catheter
insertion) without applying suction. Three passes of the
catheter is the maximum, with 10 seconds per pass.
Apply suction only during withdrawal of catheter
The suction pressure should be limited to less than 120
mmHg
When withdrawing catheter rotate while applying
intermittent suction
Suctioning should take only 10 seconds (maximum of 15
seconds)
Evaluate: clear breath sounds on auscultation of the chest.
Goals are removal of bronchial secretions, improved
ventilation, and increased efficiency of respiratory
muscles.
Postural drainage uses specific positions to use gravity to
assist in the removal of secretions.
Vibration loosens thick secretions by percussion or
vibration.
Breathing exercises and breathing retraining improve
ventilation and control of breathing and decrease the
work of breathing.
These are procedures for patients with respiratory
disorders like COPD, cystic fibrosis, lung abscess, and
pneumonia. The therapy is based on the fact that mucus
can be knocked or shaken from airways and helped to
drain from the lungs.
Postural drainage
Use of gravity to aid in the drainage of secretions.
Patient is placed in various positions to promote flow of
drainage from different lung segments using gravity.
Areas with secretions are placed higher than lung
segments to promote drainage.
Patient should maintain each position for 5-15 minutes
depending on tolerability.
3. Bronchial Hygiene Measures
Suctioning: oropharyngeal; nasopharyngeal
a. Steam inhalation
The purpose of steam inhalation are as follows:
- to liquefy mucous secretions
- to warm and humidify air
- to relieve edema of airways
- to soothe irritated airways
- to administer medication
It is a dependent nursing function
Inform the client and explain the purpose of the procedure
Place the client in Semi-Fowlers position
Cover the clients eyes with washcloth to prevent irritation
Check the electrical device before use
Place the steam inhalator in a flat, stable surface.
Place the spout 12 18 inches away from the clients nose or
adjust distance as necessary
CAUTION: avoid burns. Cover the chest with towel to
prevent burns due to dripping of condensate from the steam.
Assess for redness on the side of the face which indicates
first degree burns.
To be effective, render steam inhalation therapy for 15 20
minutes
Instruct the client to perform deep breathing and coughing
exercises after the procedure to facilitate expectoration of
mucous secretions.
Provide good oral hygiene after the procedure.
Do after-care of equipment.
Percussion
Produces energy wave that is transmitted through the
chest wall to the bronchi.
The chest is struck rhythmically with cupped hands over
the areas were secretions are located.
Avoid percussion over the spine, kidneys, breast or
incision and broken ribs. Areas should be percussed for
1-2 minutes
Vibration
Works similarly to percussion, where hands are placed on
clients chest and gently but firmly rapidly vibrate hands
against thoracic wall especially during clients exhalation.
This may help dislodge secretions and stimulate cough.
This should be done at least 5-7 times during patient
exhalation.
b. Aerosol inhalation
done among pediatric clients to administer brochodilators or
mucolytic-expectorants.
.
c. Medimist inhalation
done among adult clients to administer bronchodilators or
mucolytic-expectorants.
4. Chest Physiotheraphy ( CPT )
Includes postural drainage, chest percussion and vibration,
and breathing retraining. Effective coughing is also an
important component.
MS
12
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
Suctioning
Nursing Interventions in CPT
Verify doctors order
Assess areas of accumulation of mucus secretions.
Position to allow expectoration of mucus secretions
by gravity
Place client in each position for 5-10 to 15 minutes
Percussion and vibration done to loosen mucus
secretions
Change position gradually to prevent postural
hypotension
Client is encouraged to cough up and expectorate
sputum
Procedure is best done 60 to 90 minutes before
meals or in the morning upon awakening and at
bedtime.
Provide good oral care after the procedure
Types of Bottle Drainage
One-bottle system
The bottle serves as drainage and water-seal
Immerse tip of the tube in 2-3 cm of sterile NSS to
create water-seal.
Keep bottle at least 2-3 feet below the level of the
chest to allow drainage from the pleura by gravity.
Never raise the bottle above the level of the heart
to prevent reflux of air or fluid.
Assess for patency of the device
Observe for fluctuation of fluid along the tube. The
fluctuation synchronizes with the respiration.
Observe for intermittent bubbling of fluid;
continues bubbling means presence of air-leak
5. Incentive Spirometry
Types: volume and flow
Device ensures that a volume of air is inhaled and the
patient takes deep breaths.
Used to prevent or treat atelectasis
To enhance deep inhalation
Nursing care
Positioning of patient, teach and encourage use,
set realistic goals for the patient, and record the
results.
In the absence of fluctuation:
Suspect obstruction of the device
Assess the patient first, then if patient is stable
Check for kinks along tubing;
Milk tubing towards the bottle (If the hospital allows the
nurse to milk the tube)
If there is no obstruction, consider lung re-expansion;
(validated by chest x-ray)
Air vent should be open to air.
Two-bottle system
If not connected to the suction apparatus
The first bottle is drainage bottle;
The second bottle is water-seal bottle
Observe for fluctuation of fluid along the tube
(water-seal bottle or the second bottle) and
intermittent bubbling with each respiration.
6. Closed Chest Drainage ( Thoracostomy Tube )
Chest tube is used to drain fluid and air out of the
mediastinum or pleural space into a collection chamber
to help re-establish normal negative pressure for lung reexpansion.
Purposes
To remove air and/or fluids from the pleural space
To reestablish negative pressure and re-expand the
lungs
Procedure
The chest tube is inserted into the affected chest
wall at the level of 2nd to 3rd intercostals space to
release air or in the fourth intercostals space to
remove fluid.
MS
NOTE! IF connected to suction apparatus
1. The first bottle is the drainage and water-seal bottle;
2. The second bottle is suction control bottle.
3. Expect continuous bubbling in the suction control bottle;
4. Intermittent bubbling and fluctuation in the water-seal
5. Immerse tip of the tube in the first bottle in 2 to 3 cm of
sterile NSS
6. Immerse the tube of the suction control bottle in 10 to 20
cm of sterile NSS to stabilize the normal negative
pressure in the lungs.
7. This protects the pleura from trauma if the suction
pressure is inadvertently increased
13
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
Removal of chest tubedone by physician
The nurse Prepares:
Petrolatum Gauze
Suture removal kit
Sterile gauze
Adhesive tape
Place client in semi-Fowlers position
Instruct client to exhale deeply, then inhale and do
valsalva maneuver as the chest tube is removed.
Chest x-ray may be done after the chest tube is
removed
Asses for complications: subcutaneous emphysema;
respiratory distress
Three-bottle system
The first bottle is the drainage bottle;
The second bottle is water seal bottle
The third bottle is suction control bottle.
Observe for intermittent bubbling and
fluctuation with respiration in the water- seal
bottle
Continuous GENTLE bubbling in the suction
control bottle. These are the expected observations.
Suspect a leak if there is continuous bubbling in
the WATER seal bottle or if there is VIGOROUS
bubbling in the suction control bottle.
The nurse should look for the leak and report the
observation at once. Never clamp the tubing
unnecessarily.
7. Artificial Airway
a. Oral airways- these are shorter and often have a larger lumen.
They are used to prevent the tongue form falling backward.
If there is NO fluctuation in the water seal bottle, it may mean
TWO things
Either the lungs have expanded or the system is NOT
functioning appropriately.
In this situation, the nurse refers the observation to the
physician, who will order for an X-ray to confirm the
suspicion.
b. Nasal airways- these are longer and have smaller lumen Which
causes greater airway resistance
c. Tracheostomy- this is a temporary or permanent surgical
opening in the trachea. A tube is inserted to allow ventilation and
removal of secretions. It is indicated for emergency airway access
for many conditions. The nurse must maintain tracheostomy care
properly to prevent infection.
Important Nursing considerations
Encourage doing the following to promote drainage:
Deep breathing and coughing exercises
Turn to sides at regular basis
Ambulate
ROM exercise of arms
Mark the amount of drainage at regular intervals
Avoid frequent milking and clamping of the tube to
prevent tension pneumothorax
RESPIRATORY DISEASES AND
DISORDERS
What the nurse should do if:
If there is continuous bubbling:
The nurse obtains a toothless clamp
Close the chest tube at the point where it exits the chest
for a few seconds.
If bubbling in the water seal bottle stops, the leak is
likely in the lungs,
But if the bubbling continues, the leak is between the
clamp and the bottle chamber.
I.
Next, the nurse moves the clamp towards the bottle checking the
bubbling in the water seal bottle.
If bubbling stops, the leak is between the clamp
and the distal part including the bottle.
But if there is persistent bubbling, it means that the
drainage unit is leaking and the nurse must obtain
another set.
In the event that the water seal bottle breaks, the
nurse temporarily kinks the tube and must obtain a
receptacle or container with sterile water and
immerse the tubing.
She should obtain another set of sterile bottle as
replacement. She should NEVER CLAMP the tube
for a longer time to avoid tension pneumothorax.
In the event the tube accidentally is pulled out, the
nurse obtains vaselinized gauze and covers the
stoma.
She should immediately contact the physician.
MS
PNEUMONIA inflammation of the lung parenchyma
leading to pulmonary consolidation because alveoli is filled
with exudates
A.
14
ETIOLOGIC AGENTS
1. Streptococcus
pneumoniae
(pneumococcal
pneumonia)
2. Hemophilus influenzae (bronchopneumonia)
3. Klebsiella pneumoniae
4. Diplococcus pneumoniae
5. Escherichia coli
6. Pseudomonas aeruginosa
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
B.
HIGH RISK GROUPS
1. Children less than 5 yo
2. Elderly
C.
PREDISPOSING FACTORS
1. Smoking
2. Air pollution
3. Immunocompromised
(+) AIDS
Kaposis Sarcoma
Pneumocystis Carinii Pneumonia
DOC: Zidovudine (Retrovir)
Bronchogenic Ca
4. Prolonged immobility (hypostatic pneumonia)
5. Aspiration of food (aspiration pneumonia)
6. Over fatigue
D.
SIGNS AND SYMPTOMS
1. Productive cough, greenish to rusty
2. Dyspnea with prolong expiratory grunt
3. Fever, chills, anorexia, general body malaise
4. Cyanosis
5. Pleuritic friction rub
6. Rales/crackles on auscultation
7. Abdominal distention paralytic ileus
E.
DIAGNOSTICS
1. Sputum GS/CS confirmatory; type and sensitivity;
(+) to cultured microorganism
2. CXR (+) pulmonary consolidation
3. CBC
Elevated ESR (rate of erythropoeisis) N = 0.51.5% (compensatory mech to decreased O2)
Elevated WBC
4. ABG PO2 decreased (hypoxemia)
F.
MS
Usually, it is the upper lung areas which are
drained
Nursing management:
Monitor VS and BS
Best performed before meals/breakfast or
2-3 hours p.c. to prevent gastroesophageal
reflux or vomiting (pagkagising maraming
secretions diba? Nakukuha?)
Encourage DBE
Administer bronchodilators 15-30 minutes
before procedure
Stop if pt. cant tolerate the procedure
Provide oral care after procedure as it may
affect taste sensitivity
Contraindications:
Unstable VS
Hemoptysis
Increased ICP
Increased IOP (glaucoma)
12. Provide pt health teaching and d/c planning
Avoidance of precipitating factors
Prevention of complications
Atelectasis
Meningitis
Regular compliance to medications
Importance of ffup care
NURSING MANAGEMENT
1. Enforce CBR (consistent to all respi disorders)
2. Strict respiratory isolation
3. Administer medications as ordered
Broad spectrum antibiotics
Penicillin pneumococcal infections
Tetracycline
Macrolides
Azithromycin (OD x 3/days)
1. Too costly
2. Only se: ototoxicity transient
hearing loss
Anti-pyretics
Mucolytics/expectorants
4. Administer O2 inhalation as ordered
5. Force fluids to liquefy secretions
6. Institute pulmonary toilet measures to promote
expectoration of secretions
DBE,
Coughing
exercises,
CPT
(clapping/vibration), Turning and repositioning
7. Nebulize and suction PRN
8. Place client of semi-fowlers to high fowlers
9. Provide a comfortable and humid environment
10. Provide a dietary intake high in CHO, CHON,
Calories and Vit C
11. Assist in postural drainage
Patient is placed in various position to drain
secretions via force of gravity
II.
15
Tracheostomy usually done at bedside, 10-20 minutes
Stress test: 30 minutes
Mammography: 10-20 minutes
LARYNGOSPASM tracheostomy STAT
OR Tracheostomy: laryngeal, thyroid, neck CA
DIAPHRAGM primary muscle for respiration
INTERCOSTAL MUSCLES secondary muscle for respiration
ALVEOLI (Acinar cells) functional unit of the lungs; site for gas
exchange (via diffusion)
VENTILATION movement of air in and out of the lungs
RESPIRATION lungs to cells
Internal
External
RETROLENTAL FIBROPLASIA retinopathy/blindness in
immaturity d/t high O2 flow in pedia patients
PULMONARY TUBERCULOSIS (KOCHS DISEASE)
infection of the lung parenchyma caused by invasion of
mycobacterium tuberculosis or tubercle bacilli (gram negative,
acid fast, motile, aerobic, easily destroyed by heat/sunlight)
A.
PRECIPITATING FACTORS
1. Malnutrition
2. Overcrowding
3. Alcoholism: Depletes VIT B1 (thiamin) alcoholic
beriberi malnutrition
4. Physical and emotional stress
5. Ingestion of infected cattle with M. bovis
6. Virulence (degree of pathogenecity)
B.
MODE OF TRANSMISSION: Airborne droplet
infection
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
C.
D.
E.
MS
SIGNS AND SYMPTOMS
1. Productive cough (yellowish)
2. Low grade afternoon fever, night sweats
3. Dyspnea, anorexia, malaise, weight loss
4. Chest/back pain
5. Hemoptysis
DIAGNOSTICS
1. Skin testing
Mantoux test PPD
Induration width (within 48-72 h)
8-10 mm (DOH)
10-14 mm (WHO)
5 mm in AIDS patients is +
indicates previous exposure to tubercle
bacilli
2. Sputum AFB (+) tubercle bacilli
3. CXR (+) pulmo infiltrated due to caseous necrosis
4. CBC elevated WBC
Avoidance of precipitating factors : alcoholism,
overcrowding
Prevention of complications
Atelectasis
Military TB (extrapulmonary TB:
meningeal, Potts, adrenal glands, skin,
cornea)
Strict compliance to medications
Never double the dose! Continue taking
the meds if missed a day)
Diet modifications: increased CHON, CHO,
Calories, Vit C
Importance of ffup care
III. HISTOPLASMOSIS acute fungal infection caused by
inhalation of contaminated dust with Histoplasma capsulatum
from birds manure
A.
NURSING MANAGEMENT
1. Enforce CBR
2. Institute strict respiratory isolation
3. Administer O2 inhalation
4. Forced fluids
5. Encourage DBE and coughing
NO CLAPPING in chronic PTB d/t
hemoptysis may lead to hemorrhage
6. Nebulize and suction PRN
7. Provide comfortable and humid environment
8. Institute short course chemotherapy
Intensive phase
INH
SE: peripheral neuritis (increase vit
B6 or pyridoxine
Rifampicin
SE: red orange color of bodily
secretions
PZA
May be replaced with Ethambutol
(SE:
optic
neuritis)
if
(+)
hypersensitivity to drug
SE: allergic reactions; hepatotoxicity
and nephrotoxicity
1. Monitor liver enzymes
2. Monitor BUN and CREA
INH given for 4 months, PZA and
Rifampicin is given for 2 months, A.C. to
facilitate absorption
These 3 drugs are given simultaneously to
prevent development of resistance
Standard Regimen
Streptomycin injection (aminoglycosides)
Neomycin, Amikacin, Gentamycin
1. common SE: 8th CN damage
tinnitus hearing loss
ototoxicity
2. nephrotoxicity
a. BUN (N = 10-20)
b. CREA (N = 8-10)
9. Health teaching and d/c planning
PREDISPOSING FACTORS
Inhalation of contaminated dust
2.
SIGNS AND SYMPTOMS
PTB like symptoms
Productive cough
Fever, chills, anorexia, generalized body
malaise
Cyanosis
Chest and joint pains
Dyspnea
Hemoptysis
3.
DIAGNOSTICS
Histoplasmin skin test is (+)
ABG analysis reveals pO2 low
4.
NURSING MANAGEMENT
Enforce CBG
Administer meds as ordered
Antifungal agents
Amphotericin B (Fungizone) SE:
nephrotoxicity and hypokalemia
Monitor transaminases, BUN and
CREA
Corticosteroids
Anti-pyretics
Mucolytics/expectorants
Administer oxygen inhalation as ordered
Forced fluids
Nebulize and suction as necessary
Prevent complications
Bronchiectasis, atelectasis
Prevention of spread
Spraying of breeding places
Kill bird and owner! Hehe!
CHRONIC OBSTRUCTIVE PULMONARY DISEASES
1.
2.
3.
4.
16
Chronic Bronchitis
Bronchial Asthma
Bronchiectasis
Pulmonary Emphysema
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
I.
MS
CHRONIC BRONCHITIS (Blue Bloaters) Inflammation
of the bronchi due to hypertrophy or hyperplasia of goblet
mucous producing cells leading to narrowing of smaller
airways
A.
PREDISPOSING FACTORS
1. Smoking
2. Air pollution
B.
SIGNS AND SYMPTOMS
1. Consistent productive cough
2. Dyspnea on exertion with prolonged expiratory
grunt
3. Anorexia and generalized body malaise
4. Cyanosis
5. Scattered rales/rhonchi
6. Pulmonary hypertension
Peripheral edema
Cor pulmonale
C.
DIAGNOSTICS
1. ABG analysis: decreased PO2, increased PCO2,
respiratory acidosis; hypoxemia cyanosis
D.
NURSING MANAGEMENT
1. Enforce CBR
2. Administer medications as ordered
Bronchodilators
Antimicrobials
Corticosteroids
Mucolytics/expectorants
3. Low inflow O2 admin; high inflow will cause
respiratory arrest
4. Force fluids
5. Nebulize and suction client as needed
6. Provide comfortable and humid environment
7. Health teaching and d/c planning
avoidance of smoking
prevent complications
CO2 narcosis coma
Cor pulmonale
Pleural effusion
Pneumothorax
Regular adherence to meds
Importance of ffup care
II.
17
BRONCHIAL ASTHMA reversible inflammatory lung
condition caused by hypersensitivity to allergens leading to
narrowing of smaller airways
A.
PREDISPOSING FACTORS
1. Extrinsic (Atopic/Allergic Asthma)
Pollens, dust, fumes, smoke, fur, dander, lints
2. Intrinsic (Non-Atopic/Non-Allergic)
Drugs (aspirin, penicillin, B-blockers)
Foods (seafoods, eggs, chicken, chocolate)
Food additives (nitrates, nitrites)
Sudden change in temperature, humidity and
air pressure
Genetics
Physical and emotional stress
3. Mixed type combination of both
B.
SIGNS AND SYMPTOMS
1. Cough that is productive
2. Dyspnea
3. Wheezing on expiration
4. Tachycardia, palpitations and diaphoresis
5. Mild apprehension, restlessness
6. Cyanosis
C.
DIAGNOSTICS
1. PFT decreased vital lung capacity
2. ABG analysis PO2 decreased
D.
NURSING MANAGEMENT
1. Enforce CBR
2. Administer medications as ordered
Bronchodilators administer first to facilitate
absorption of corticosteroids
Inhalation
MDI
Corticosteroids
Mucolytics/expectorants
Mucomyst
Antihistamine
3. Administer oxygen inhalation as ordered
4. Forced fluids
5. Nebulize and suction patient as necessary
6. Encourage DBE and coughing
7. Provide a comfortable and humid environment
8. Health teaching and d/c planning
Avoidance of precipitating factors
Prevention of complications
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
Status asthmaticus
DOC: Epinephrine
Aminophylline drip
Emphysema
Regular adherence to medications
Importance of ffup care
D.
SURGERY
1. Segmental lobectomy
2. Pneumonectomy
Most feared complications
Atelectasis
Cardiac tamponade: muffled heart sounds,
pulsus paradoxus, HPN
E.
NURSING MANAGEMENT
1. Enforce CBR
2. Low inflow O2 admin; high inflow will cause
respiratory arrest
3. Administer medications as ordered
Bronchodilators
Antimicrobials
Corticosteroids
(5-10
minutes
after
bronchodilators)
Mucolytics/expectorants
4. Force fluids
5. Nebulize and suction client as needed
6. Provide comfortable and humid environment
7. Health teaching and d/c planning
Avoidance of smoking
Prevent complications
Atelectasis
CO2 narcosis coma
Cor pulmonale
Pleural effusion
Pneumothorax
Regular adherence to meds
Importance of ffup care
III. BRONCHIECTASIS permanent dilation of the bronchus
due to destruction of muscular and elastic tissue of the
alveolar walls (subject to surgery)
A.
MS
PREDISPOSING FACTORS
1. Recurrent lower respiratory tract infection
Histoplasmosis
2. Congenital disease
3. Presence of tumor
4. Chest trauma
B.
SIGNS AND SYMPTOMS
1. Consistent productive cough
2. Dyspnea
3. Presence of cyanosis
4. Rales and crackles
5. Hemoptysis
6. Anorexia and generalized body malaise
C.
DIAGNOSTICS
1. ABG analysis reveals low PO2
2. Bronchoscopy direct visualization of bronchi
lining using a fibroscope
Pre-op
Secure consent
Explain procedure
NPO 4-6 hours
Monitor VS and breath sounds
Post-operative
Feeding initiated upon return of gag reflex
Instruct client to avoid talking, coughing
and smoking as it may irritate respiratory
tract
Monitor for s/sx of frank or gross bleeding
Monitor for signs of laryngeal spasm
DOB and SOB prepare trache set
IV. PULMONARY EMPHYSEMA terminal and irreversible
stage of COPD characterized by :
Inelasticity of alveoli
Air trapping
Maldistribution of gasses (d/t increased air trapping)
Overdistention of thoracic cavity (Barrel chest)
compensatory mechanism increased AP diameter
18
Abejo
Medical and Surgical Nursing
Respiratory System Lecture Notes
Prepared by: Mark Fredderick R. Abejo RN,, MAN
RESTRICTIVE LUNG DISEASE
A.
B.
C.
D.
MS
PREDISPOSING FACTORS
1. Smoking
2. Air pollution
3. Hereditary: involves alpha-1 antitrypsin for
elastase production for recoil of the alveoli
4. Allergy
5. High risk group elderly degenerative
decreased vital lung capacity and thinning of
alveolar lobes
V.
SIGNS AND SYMPTOMS
1. Productive cough
2. Dyspnea at rest
3. Prolonged expiratory grunt
4. Resonance to hyperresonance
5. Decreased tactile fremitus
6. Decreased breath sounds ( if (-) BS lung collapse)
7. Barrel chest
8. Anorexia and generalized body malaise
9. Rales or crackles
10. Alar flaring
11. Pursed-lip breathing (to eliminate excess CO2)
PNEUMOTHORAX partial or complete collapse of the
lungs due to accumulation of air in pleural space
A.
TYPES
1. Spontaneous air enters pleural space without an
obvious cause
Ruptured blebs (alveolar filled sacs)
inflammatory lung conditions
2. Open air enters pleural space through an opening
in pleural wall (most common)
Gun shot wounds
Multiple stab wounds
3. Tension air enters pleural space during inspiration
and cannot escape leading to overdistention of the
thoracic cavity mediastinal shift to the affected
side (ie. Flail chest) paradoxical breathing
B.
PREDISPOSING FACTORS
1. Chest trauma
2. Inflammatory lung condition
3. tumors
SIGNS AND SYMPTOMS
1. Sudden sharp chest pain, dyspnea, cyanosis
2. Diminished breath sounds
3. Cool, moist skin
4. Mild restlessness and apprehension
5. Resonance to hyperresonance
C.
DIAGNOSTICS
1. ABG analysis reveal
Panlobular, centrilobular PO2 elevation and
PCO2 depression respiratory acidosis (blue
bloaters)
Panacinar/centriacinar PCO2 depression and
PO2 elevation (pink puffers hyperaxemia)
2. Pulmo function test decreased vital lung capacity
NURSING MANAGEMENT
1. Enforce CBR
2. Administer medications as ordered
Bronchodilators
Antimicrobials
Corticosteroids
Mucolytics/expectorants
3. Low inflow O2 admin; high inflow will cause
respiratory arrest and oxygen toxicity
4. Force fluids
5. Pulmonary toilet
6. Nebulize and suction client as needed
7. Institute PEEP in mechanical ventilation
PEEP positive end expiratory pressure
allows for maximum alveolar diffusion
prevent lung collapse
8. Provide comfortable and humid environment
9. Diet modifications: high calorie, CHON, CHO,
vitamins and minerals
10. Health teaching and d/c planning
Avoidance of smoking
Prevent complications
Atelectasis
CO2 narcosis coma
Cor pulmonale
Pleural effusion
Pneumothorax
Regular adherence to meds
Importance of ffup care
19
D.
DIAGNOSTICS
1. ABG analysis: PO2 decreased
2. CXR confirms collapse of lungs
E.
NURSING MANAGEMENT
1. Assist in endotracheal intubation
2. Assist in thoracentesis
3. Administer meds as ordered
Narcotic analgesics Morphine sulfate
Antibiotics
4. Assist in CTT to H20 sealed drainage
Abejo
You might also like
- Alternative Medicine and Wellness TechniquesDocument210 pagesAlternative Medicine and Wellness TechniquesDr. Peter Fritz Walter91% (11)
- Cardiac DrugsDocument10 pagesCardiac Drugssurviving nursing school100% (3)
- The Basics: A Comprehensive Outline of Nursing School ContentFrom EverandThe Basics: A Comprehensive Outline of Nursing School ContentRating: 5 out of 5 stars5/5 (3)
- Cardiac DrugsDocument5 pagesCardiac Drugseric100% (17)
- Lab ValuesDocument3 pagesLab Valuessurviving nursing school100% (1)
- Fluid and Electrolytes for Nursing StudentsFrom EverandFluid and Electrolytes for Nursing StudentsRating: 5 out of 5 stars5/5 (12)
- Anti Psychotic DrugsDocument2 pagesAnti Psychotic DrugsJohn Corpuz100% (1)
- Nursing Memory JoggersDocument2 pagesNursing Memory JoggersMarcus, RN96% (24)
- Fundamentals of NursingDocument8 pagesFundamentals of NursingFreeNursingNotes92% (13)
- Med SurgDocument62 pagesMed SurgJean Soriano98% (65)
- Respiratory Notes Sample ChapterDocument10 pagesRespiratory Notes Sample ChapterHitesh Deora75% (4)
- Cardiac AssessmentDocument7 pagesCardiac AssessmentBryan Mae H. Degorio75% (4)
- Adult III Cardiac Study GuideDocument15 pagesAdult III Cardiac Study GuideNursingSchoolNotes100% (6)
- Nursing Mnemonics: The Ultimate Tips and Notes For NursesFrom EverandNursing Mnemonics: The Ultimate Tips and Notes For NursesRating: 5 out of 5 stars5/5 (1)
- Cardiac DisordersDocument15 pagesCardiac Disordersgold_enriquez100% (3)
- Cardiovascular SystemDocument10 pagesCardiovascular Systemsurviving nursing school100% (2)
- Med Surg Study GuideDocument98 pagesMed Surg Study Guideprogramgrabber100% (23)
- Dimensional Analysis For Nursing StudentsFrom EverandDimensional Analysis For Nursing StudentsNo ratings yet
- Lower Respiratory Study SheetDocument13 pagesLower Respiratory Study SheetJune Rhoades100% (2)
- The 12-Lead Electrocardiogram for Nurses and Allied ProfessionalsFrom EverandThe 12-Lead Electrocardiogram for Nurses and Allied ProfessionalsNo ratings yet
- Medsurg Cardio Ana&PhysioDocument6 pagesMedsurg Cardio Ana&Physiorabsibala80% (10)
- Medical Surgical NursingDocument59 pagesMedical Surgical NursingChey Dianne Seriña100% (11)
- Cardiac Notes NursingDocument16 pagesCardiac Notes NursingYemaya8494% (17)
- Surviving the ICU: A Toolkit for the Critical Care NurseFrom EverandSurviving the ICU: A Toolkit for the Critical Care NurseNo ratings yet
- FLASH CardsDocument3 pagesFLASH Cardsclarheena100% (2)
- Cardionursing 110207023802 Phpapp01Document18 pagesCardionursing 110207023802 Phpapp01LudwigJayBarayuga100% (5)
- Musculoskeletal Note1Document34 pagesMusculoskeletal Note1FreeNursingNotes100% (4)
- A Handbook for Student Nurses, 201617 edition: Introducing key issues relevant for practiceFrom EverandA Handbook for Student Nurses, 201617 edition: Introducing key issues relevant for practiceRating: 4 out of 5 stars4/5 (1)
- Cardiac NursingDocument26 pagesCardiac Nursingjgcriste95% (20)
- Respiratory NCLEX Practice Test Part 1: Guillain-Barré SyndromeDocument20 pagesRespiratory NCLEX Practice Test Part 1: Guillain-Barré SyndromeHasan A AsFour100% (2)
- Respiratory DisordersDocument15 pagesRespiratory Disordersmnlstr100% (5)
- Neuro Study GuideDocument7 pagesNeuro Study GuideNursingSchoolNotes100% (2)
- Nursing Pharmacology Perfusion Study GuideDocument9 pagesNursing Pharmacology Perfusion Study GuideChelsea SmithNo ratings yet
- Medical Surgical Nursing PathophysiologyDocument23 pagesMedical Surgical Nursing Pathophysiologymarc joseph100% (2)
- Respiratory Care Review: An Intense Look at Respiratory Care Through Case StudiesFrom EverandRespiratory Care Review: An Intense Look at Respiratory Care Through Case StudiesNo ratings yet
- Gastrointestinal NursingDocument8 pagesGastrointestinal Nursingohsnapitslei90% (10)
- Numeracy and Clinical Calculations for Nurses, second editionFrom EverandNumeracy and Clinical Calculations for Nurses, second editionRating: 1 out of 5 stars1/5 (1)
- Assessment of Respiratory SystemDocument18 pagesAssessment of Respiratory SystemIbi Yulia Setyani100% (1)
- CRITICAL THINKING IN CLINICAL NURSING PRACTICE (RN): Passbooks Study GuideFrom EverandCRITICAL THINKING IN CLINICAL NURSING PRACTICE (RN): Passbooks Study GuideNo ratings yet
- Medical Surgical Nursing Cardio Vascular System ClassDocument15 pagesMedical Surgical Nursing Cardio Vascular System Classvallal100% (2)
- Cardiovascular Nursing Bullet Points I PDFDocument4 pagesCardiovascular Nursing Bullet Points I PDFKhalid Epping100% (3)
- Chart of Neuro DisordersDocument1 pageChart of Neuro DisordersNursingSchoolNotes100% (2)
- Nursing Respiratory SystemDocument254 pagesNursing Respiratory SystemWendy EvansNo ratings yet
- MEDICAL-SURGICAL NURSE: Passbooks Study GuideFrom EverandMEDICAL-SURGICAL NURSE: Passbooks Study GuideNo ratings yet
- Schaum's Outline of Critical Care Nursing: 250 Review QuestionsFrom EverandSchaum's Outline of Critical Care Nursing: 250 Review QuestionsRating: 5 out of 5 stars5/5 (1)
- Activity Intolerance NCPDocument7 pagesActivity Intolerance NCPMariquita BuenafeNo ratings yet
- Nclex TestDocument38 pagesNclex TestIke Agbor97% (33)
- Cardiac DisordersDocument38 pagesCardiac Disordersprototypeallhell100% (1)
- Sahaja Yoga Meditation PresentationDocument37 pagesSahaja Yoga Meditation Presentationpoonamt2001100% (5)
- Mus Culo SkeletalDocument16 pagesMus Culo Skeletalshenric16100% (2)
- 60 Item Exam On Cardiovascular DisordersDocument9 pages60 Item Exam On Cardiovascular DisordersAijem RyanNo ratings yet
- Nursing Fundamentals DeMYSTiFieD, Second EditionFrom EverandNursing Fundamentals DeMYSTiFieD, Second EditionRating: 2 out of 5 stars2/5 (2)
- Dialysis Inspection Tool 2014Document11 pagesDialysis Inspection Tool 2014Maek100% (1)
- NATIONAL COUNCIL LICENSURE EXAMINATION FOR REGISTERED NURSES (NCLEX-RN): Passbooks Study GuideFrom EverandNATIONAL COUNCIL LICENSURE EXAMINATION FOR REGISTERED NURSES (NCLEX-RN): Passbooks Study GuideNo ratings yet
- Evidence Based Nursing PracticeDocument21 pagesEvidence Based Nursing Practiceshenric16No ratings yet
- Fluid and ElectrolytesDocument13 pagesFluid and ElectrolytesHenry Philip93% (15)
- Palmer Complete Edited Royal PentagonDocument26 pagesPalmer Complete Edited Royal Pentagonshenric16100% (1)
- Ms Penta NotesDocument84 pagesMs Penta Notesshenric16No ratings yet
- Med Surge 2 - RESP SYSTEM NOTESDocument26 pagesMed Surge 2 - RESP SYSTEM NOTESlorrainenxumalo75% (4)
- Neuro OphthalmologyDocument114 pagesNeuro OphthalmologySurat TanprawateNo ratings yet
- Fundamentals of NursingDocument31 pagesFundamentals of NursingAngelica Soriano93% (14)
- Community Health Nursing Practice Questions With RationalesDocument15 pagesCommunity Health Nursing Practice Questions With RationalesFelice Lamzon Labrador100% (2)
- Community Health Nursing Practice Questions With RationalesDocument15 pagesCommunity Health Nursing Practice Questions With RationalesFelice Lamzon Labrador100% (2)
- Medical Surgical Nursing Review NotesDocument78 pagesMedical Surgical Nursing Review NotesLouie ParillaNo ratings yet
- The GastroDocument25 pagesThe Gastroangel_maui100% (7)
- Genito UrinarysystemDocument7 pagesGenito Urinarysystemshenric16No ratings yet
- Reviewer For NleDocument14 pagesReviewer For Nleshenric16No ratings yet
- Nursing Board Exam Test Drill 3Document2 pagesNursing Board Exam Test Drill 3Kira100% (15)
- Medicationpart1 110202192115 Phpapp02Document10 pagesMedicationpart1 110202192115 Phpapp02Jessamine Rochelle Reyes Esberto100% (1)
- Community Health NursingDocument49 pagesCommunity Health Nursingshenric16No ratings yet
- Community Health NursingDocument49 pagesCommunity Health Nursingshenric16No ratings yet
- 100 Item Comprehensive Exam With Answers and RationaleDocument21 pages100 Item Comprehensive Exam With Answers and RationaleAijem Ryan93% (15)
- Professional Adjustment Leadership Management and ResearchDocument10 pagesProfessional Adjustment Leadership Management and Researchshenric16100% (1)
- COMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuideFrom EverandCOMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuideNo ratings yet
- Fhsis Annual 2018Document496 pagesFhsis Annual 2018shenric16No ratings yet
- Uhc Irr DraftDocument107 pagesUhc Irr Draftshenric16No ratings yet
- Evidence Based Nursing PracticeDocument21 pagesEvidence Based Nursing Practiceshenric16No ratings yet
- Health Teaching PDFDocument1 pageHealth Teaching PDFshenric16No ratings yet
- Patient Positioning in The Operating RoomDocument33 pagesPatient Positioning in The Operating Roomshenric16No ratings yet
- Maternity Nursing ReviewDocument37 pagesMaternity Nursing Reviewshenric16No ratings yet
- Maternal Ob NotesDocument37 pagesMaternal Ob Notesshenric16No ratings yet
- Cognitive DisordersDocument2 pagesCognitive DisordersSherrizah Alexis Naag NavaNo ratings yet
- Nle - July 2011Document12 pagesNle - July 2011shenric16100% (1)
- Course Audit Professional AdjustmentDocument9 pagesCourse Audit Professional Adjustmentshenric16No ratings yet
- Maternal Ob NotesDocument37 pagesMaternal Ob Notesshenric16No ratings yet
- Pediatric Nursing Edison O Dangkeo RNDocument59 pagesPediatric Nursing Edison O Dangkeo RNshenric16100% (1)
- Final Outline Psychiatric NursingDocument52 pagesFinal Outline Psychiatric Nursingshenric16100% (1)
- Maternal and Child Health Nursing: KeepsDocument32 pagesMaternal and Child Health Nursing: Keepsshenric16No ratings yet
- Pattern Recognition in Pharmacokinetic Data Analysis PDFDocument17 pagesPattern Recognition in Pharmacokinetic Data Analysis PDFBagoes AsNo ratings yet
- Nsaid GuidelineDocument62 pagesNsaid GuidelineraffellaNo ratings yet
- Ercoli Et Al-2018-Journal of Clinical PeriodontologyDocument12 pagesErcoli Et Al-2018-Journal of Clinical PeriodontologyTeresa BeltranNo ratings yet
- Development of A Quality Assessment Instrument For Trials of Treatments For Depression and NeurosisDocument8 pagesDevelopment of A Quality Assessment Instrument For Trials of Treatments For Depression and NeurosisvNo ratings yet
- Chlorine Dioxide PDFDocument4 pagesChlorine Dioxide PDFSudhakar Rao100% (1)
- Presentator: Z. Chandra S. Harahap Supervisor: Prof. Dr. Bahagia Loebis, SP - KJ (K) Moderator: Dr. Vita Camellia, M.Ked, SP - KJDocument12 pagesPresentator: Z. Chandra S. Harahap Supervisor: Prof. Dr. Bahagia Loebis, SP - KJ (K) Moderator: Dr. Vita Camellia, M.Ked, SP - KJputrianabrsitompulNo ratings yet
- Hypokalaemic PERIODIC ParalysisDocument34 pagesHypokalaemic PERIODIC ParalysistukogustarilisaNo ratings yet
- Complex DesignsDocument10 pagesComplex Designsrabiafarooq51100% (1)
- Addiction TestDocument11 pagesAddiction TestAnonymous qm1BVDOHNo ratings yet
- Neurologic Diagnostic ProceduresDocument18 pagesNeurologic Diagnostic Procedureszarka wahid buxNo ratings yet
- Major Depressive Disorder in Adults 2016 (Philippines)Document29 pagesMajor Depressive Disorder in Adults 2016 (Philippines)Doroteo Jose StationNo ratings yet
- Ghora Ba 2016Document8 pagesGhora Ba 2016marlon GarcíaNo ratings yet
- Flank Pain, Anxiety...Document7 pagesFlank Pain, Anxiety...reneighdNo ratings yet
- Autoimmune Bullous DiseaseDocument10 pagesAutoimmune Bullous DiseaseSiti Habibah ZeinNo ratings yet
- ML 800 Drugs&Xenobioticsblood Conc.Document28 pagesML 800 Drugs&Xenobioticsblood Conc.Andreia AndreiutzaNo ratings yet
- CABRAL Diabetes Mellitus Case Presentation and DiscussionDocument9 pagesCABRAL Diabetes Mellitus Case Presentation and DiscussionCalingalan Hussin CaluangNo ratings yet
- Bulimia NervosaDocument17 pagesBulimia NervosaJheanAlphonsineT.Means100% (1)
- Nursing Care Plan GuideDocument1 pageNursing Care Plan GuideTracy100% (1)
- Psychiatric Disorders in Medical Practice: Specific SyndromesDocument14 pagesPsychiatric Disorders in Medical Practice: Specific SyndromesEduard TomițaNo ratings yet
- Mediterranean Diet ScoreDocument1 pageMediterranean Diet Scoregabriel01022010No ratings yet
- Hannah Leah DardenDocument3 pagesHannah Leah Dardenapi-243270092No ratings yet
- Nursing ResponsibilityDocument9 pagesNursing Responsibilityايام اول الشحيNo ratings yet
- Report of The Sixth Annual Meeting of The London Mesmeric Infirmary (1855)Document48 pagesReport of The Sixth Annual Meeting of The London Mesmeric Infirmary (1855)marcinlesniewiczNo ratings yet
- Contrast Poc Tool Anaphylaxis Wall ChartDocument1 pageContrast Poc Tool Anaphylaxis Wall Chartapi-358179847No ratings yet