Professional Documents
Culture Documents
برسثو محاضرة 4
Uploaded by
Abeer KhasawnehCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
برسثو محاضرة 4
Uploaded by
Abeer KhasawnehCopyright:
Available Formats
^^ - - , . : , , , . )) (( : ..
Biomechanics of RPD Biomechanical principles: 1. Support 2. Retention 3. Stability (Resistance form) The upper 3 points are related to complete and partial dentures 4. Maintaining dental, gingival and periodontal health: we need to protect the gingival and periodontal tissues and to protect teeth from caries. The principles that we applied on the complete denture are the same here, but with a little difference which is related to point 4 (Maintaining dental, gingival and Periodontal health) because RPD takes a lot of retention and support from the surrounding teeth, then if the teeth are compromise in any way, we will end with problems.
-1-
Forces in the oral cavity: 1. Functional/Normal : Mastication-chewing Gravity Tongue movements during speech: some say that the forces produced by speech are not significant. Others say those that have tongue movements during speaking resist the cheek movement. (Where the cheek movement inside, makes the tongue to push the teeth outside). Cheek pressure 2. Non-functional/they cause pathological & physiological problems Bruxism Clenching: it's a bruxism but with lateral movement. Nail biting Hard object biting- as seeds, pipe, instruments. Premature dental contact as: High fillings, crowns. Biting on hard food-rock Tongue thrust Harsh hygiene practices
Tolerance of dental structures: What is tolerance? When dental and oral tissues withstand these forces without physiologic or pathologic change. If these forces exceed the normal limits, they become potentially destructive. So the tolerance is: 1. Functional Tolerated well
-2-
Tooth and periodontal ligament distribute forces to the underlying alveolar bone. Can increase beyond tolerance point. 2. Non-functional Poorly tolerated. Cause tooth and periodontal tissue damage- occlusal trauma
On the long term cause dental wear and/or bone resorption.
So, if the forces exceed the ability of tolerance (how much tissue can tolerates/stands), they become potentially destructive which is considered as a pathological change. Let's imagine this situation where there will be a pathological change If we have a height filling or a height crown, there will be so much pain, which will cause edema, and it will end up with pulp death (irreversible pulpitis), then it will go into necrosis. So there will be: Pain edema pulpitis necrosis In RPD we will resist the normal forces. But why do we need to resist normal forces!? - For ex., The patient has 32 teeth, when he loses part of them, the other teeth will hold the occlusal forces of the missing teeth, So this extra force is a normal force, but because the number of teeth are smaller, the amount of forces on the remaining teeth are larger, (that's how normal forces sometimes cause trauma). So the 1st force that we have to resist is the natural forces that are coming from mastication or from regular using of the mouth, because of: 1. the number of teeth remaining.
-3-
The number of teeth is reduced, it becomes abnormal (abnormal for each individual tooth remaining). 2. The quality of RPD it self. RPD is removable not fixed, while the teeth are semi fixed, this contrast between something mobile and something solid in place, causes other types of forces.
So again, we will design RPD in away to resist these forces in order not to cause trauma.
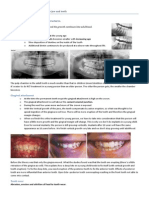
Here, we have a situation of "free end saddle":
Metal frame work
The canine here is holding the forces of all of the missing teeth. So, we utilize it and we design the rest of RPD to protect it from excessive forces.
-4-
How do forces become harmful? If they change from normal, by changing:
1. Magnitude: is the amount of the force, but loss of teeth
reduces the occlusal bearing surfaces-so same occlusion force but on less number of teeth.
2. Direction: tilted teeth direct the forces in an incorrect
direction. 3. Duration: is a single force and means how much you keep biting on your teeth, in chewing cycle your teeth touch each other in 0.3 sec only, so the duration of the force is 0.3sec. So, does the duration of biting differ? If you have RPD in your mouth will you be eating more?!! Actually, the duration is the same- chewing cycle tooth contact is 0.3 sec. 4. Frequency: how much do you eat; it might not differ if the patient does not alter his meals frequency. If RPD is present, it may change the amount and direction of force exerted on teeth and tissue. Un-wanted movement in RPD: The RPD are not rigidly connected to the teeth or tissues, which means they are subject to movement in response to functional loads. Gravity pulling upper RPD down. Sticky food pulling both upper and lower dentures away from their seating. Occlusal forces moving the distal extension bases towards tissue are subject to movement in response. So, we need to design the RPD in a way to resist these changes by: Distributing these forces on large number of teeth.
-5-
Trying to direct the force in a way that will be resistible vertically on the teeth and minimize the unwanted movements that happen because of the nature of the RPD. So, for protecting the tissue, we need to select RPD design and the location of its component and make sure that everything is in harmony with the occlusion.
As we know we have tooth support, tooth -mucosal support and mucosal support. BUT which one can be more harmful in the long term use? If the RPD is designed perfectly, it will not cause harm anyway.
If we have two teeth on bounded saddle, we will have the support, and the pressure will be directed to the two teeth. But when we have free end saddle, the pressure will be directed to one tooth mostly. And it's no longer how the teeth and the periodontal ligament in alveolar bone get the force, there is a residual ridge and over this residual ridge we have soft mucosa, and this soft mucosa can spring in and out (so we have minor movement). No matter how my RPD is good, the mucosa can spring in & out during mastication. This causes some accessory forces. So, these unwanted movement come from RPD itself in the way it's connected to the teeth, and we should not exceed the capability of supporting structure. But what about the long span bounded saddle (class 3 or 4) where the long span means the number of missing teeth is large-? Kennedy classification does not count the number of missing teeth, but in term of support if we have more than 4 teeth missing (although they are bounded by teeth on each side), they will cause some forces
-6-
to be exerted on the residual ridge itself. So, we have combinations sometime! We have tooth support and tooth tissue support for free end saddle, and mucosal support for temporary RPD! (Temporary RPD ONLY has a mucosal support). We can add to it combination when we have a long span class 3 or 4 because of the large number of missing teeth. So, we adapt it by major connector and rests, and these provide some types of resistance or support. We were talking about the direction of the force, and it changes by the type of leverage.
1- What is the type of saddle here? Free end saddle. 2-what is the type of support? Tooth -tissue support. 3-where does the unwanted movement happen? Under the distal extension.
-7-
There is some movement here, but what happens to this tooth after we wrap around it totally by C clasp? There will be a movement downward and upward, also we have a rest where we have a fulcrum, and this end of the clasp is engaged in the tooth, so whenever the free end saddle is moving, the clasp will do extraction to the tooth, because the clasp is located under the maximum bulge of the tooth.
Also, during mastication, the free end saddle will move, so the clasp will push the teeth upward because it engages under the undercut, this is the abnormal direction. The teeth can resist the vertical movement, but it can't resist the upward movement. And in similar way we can extract teeth. Suppose we want to extract a tooth, we hold the tooth and move it laterally. The tooth is bounded by periodontal ligament; this lateral movement has a medium resistance, so the lateral movement has moderate resistance. If you try to go inward, it will be pushed up. But if I hold the tooth, take it out and rotate it where these movements have the weakest resistance of the tooth, I can easily extract it. So, what shall you do as a dentist to extract a tooth? Use a special plaier hold the tooth move it laterally many times start to rotate it it will come out :D In other cases, if this tooth is in normal function and occlusion and the direction of the force has a problem, its PDL will begin breaking down in long term use & the tooth can be extracted.
-8-
Another case where we have such situation is when we have gravity & the gravity is pushing the upper denture downward. We have this I- bar & fulcrum here. If we change the fulcrum position what will happen??? It'll go inward but if the fulcrum is in the other side within I-bar on the upper side we might get extracted forces. Also according to the bound saddles, there might be some problems with sticky food, but what's the frequency of eating sticky food?? It's very low & we don't usually use them. If we have a small unwanted movement around the free end saddle, it will move up & down & it will also move slightly on the side way. We need to resist these side way movements and up & down movements so how do I resist them? - Avoid putting dentures in patients with periodontal disease (in which the teeth are already weakened). - Make sure that bone type and health of periodontal ligament are correct and the height of the bone on that tooth which I'm going to use is good. (if I don't have a lot of bone on that tooth, I don't use it as abutment & I move to the next tooth because I expect at any time that tooth will be extracted because it's already weak. Amount of rotation depends on: quality of those supporting tissues Bone type Health of periodontal tissue Bone height the accuracy of fitting surface extent of the denture base And the total functional load applied - Normal - increased.
-9-
Imagine a mouth without RPD& there is a week tooth, what will happen if I put RPD? It might cause a problem. So, we need to make sure that we don't place our denture, except in patients whose remaining teeth are healthy or at least controlled in terms of periodontal disease. Related to the accuracy of fitting tissue, do you think we'll have the same movement if this RPD is very good in fitting & adapting on the ridge? Actually, the more fit we have, the less movement will be. We try to extend the denture base as much as possible, so in free end saddle, we need to extend the denture as much as the tissue tolerates. And make sure that the load is normal.
A normal mouth tolerates extension up to border structures, so when we have a border structure like a cheek or buccal frenum, you can't extend the denture beyond it, because it'll be harmful for the patient, so this is why in free end saddle we try to extend the denture as much as possible.
support components-resist occlusal forces : 1. Rigid connectors Major connector. Promotes cross-arch force transmission (contributes to cross arch stability and support). Minor connectors. Transfer forces to and from abutment teeth. Ok! What about RPD itself, can we use very flexible RPDs?? No, it's preferred to have rigid RPDs & we use for definitive RPD the alloy (metal), so whenever the major connector is solid, it will help me to achieve the following: cross arch stability & support minor connectors
- 10 -
Maxillary major connector produces forces on the palate & this increases the coverage, this'll give more support so we avoid the teeth rather than putting the forces on it. 2. Maxillary major connectors incorporate horizontal hard palate coverage to provide muco-osseos support as required. 3. Direct retainer designs for control of forces minimize horizontal forces on abutment teeth. Usually, stress released designs are preferred. stress director attachment wrought wire clasps Remote rest & other conventional clasps. Split major connector. 4. Rests provide dento-alveolar support (to distribute forces & we try to make them as much as we can). Although adjacent (proximate) rests may provide efficient forces transmission to abutment teeth, remote rest clasp designs are often more desirable since they may decrease the favor into requiring force. Adequate tooth modification for rest seats promotes apically directed forces on abutment teeth. * Putting rests on other teeth
- 11 -
Un-wanted movement act as Levers in mechanics: 1. Class 1: the most famous unwanted movement is the movement of the distal extension of the free end saddle.
2. Gravity 3. Long span in bounded saddle has some movements in the mucosa. But when the denture moves, it has a way to move, this way is called Fulcrum line effect.
The fulcrum line: It's the center of rotation as the distal extension base moves toward the supporting tissue, when an occlusal load is applied.
The fulcrum line in free end saddles is the line passing behind the last rests. So, it's important to know the direction of denture movements. (We place it in the most distal direction to rests in the both sides.
- 12 -
But if we have 2 large edentulous areas, we may have 2 fulcrum lines, but usually the fulcrum line extends along the most distal rests. 5. Denture base extension provides muco-osseous support: Maximum soft tissue coverage is limited by movable tissues (i.e. snowshoe effect). Coverage of primary force hearing areas. i. Posterior maxillary ridge. ii. Buccal shelf. iii. Pear-shaped pad retromolar. 6. Impression procedures: the application of selective pressure records the soft tissue to promote support. Dual stage selective pressure impression (altered cast impression). Reline at delivery.
- 13 -
Altered cast technique impressions
we make sure that we use a very good impression material. We concentrate on: The method we take impressions by: we want to take a very accurate impression for this area. We call it altered cast technique: it means that I'm taking a very accurate impression over here do border molding take impression make our cast. Altered cast: it means that we have a cast at the first visit but we're going to change it.
So, this is the impression visit #2 (we'll see it later when we will take the bases), but when we have free end saddle, we have 2 impressions to do, especially if the free end saddle is large: the 1st impression is called primary impression & the 2nd impression is called altered cast technique impression.
- 14 -
Stability In complete dentures we were taking it from residual ridges. But in RPD there are other stuff that don't let the denture to go a side way. So the stability is provided by: 1. 2. 3. 4. 5. 6. 7. Any vertically placed components of RPD denture Minor connectors: to get sub- stability from them Proximal plates Reciprocating arms of clasps Lingual plates Rest seats designed as intra-coronal boxes (channel rest) Residual ridges as in complete dentures, so please revise the lecture in complete denture course. 8. get stability from the other side of the arch
But why do we go to the other side to get stability? The main reason, that if we don't get stability from other side, the RPD will be as a small piece, and because it's removable, there will be a chance for the patient to swallow it. And there are secondary reasons for that, like more support, distribution of forces and cross arch stabilization. Cross arch stabilization: it means that we are going to the other side, although there are no missing teeth but to get more stability.
- 15 -
How to reduce the unwanted movement? We mentioned some of them but let's see them in pictures:
1. Rather than putting half round clasp, we put something called Ibar clasp ( RPI system ), where we have guiding plane , rest and I-bar arm, this causes the least damaging when we have free end saddle . Or it's called PPA when it's coming from the mesial side not from the distal as a regular one. Using wrought wire bind the stainless steel wire more softly on tooth and will not do excessive forces on the tooth. If I do upward movement, the arm of I-bar will resist.
2. Sometimes, we use the stress breaking attachments (we will take them later).
- 16 -
3. Sometime we make such cut to make the metal more flexible, we call it stress breaking design.
Indirect retainer
4. Here, I didnt replace tooth #7, why? Because when I have smaller number of teeth, the amount of forces will be less unwanted movement will be less. Q: which one will cause more lever effect? - Free end saddle replaces 4,5,6 - Free end saddle replaces 4,5,6,7 - Free end saddle replaces 4,5,6,7,8 More replaced teeth lead to more unwanted movements, so the free end saddle which replaces 4, 5,6,7,8 will cause more lever effect.
- 17 -
5. Reduce lever by reducing FES distance by EXTRA indirect retainers placed as far from fulcrum line to resist the movement around the fulcrum line. Fulcrum line (glossary) 1. A theoretical line passing through the point around which a lever functions and at right angles to its path of movement 2: an imaginary line, connecting occlusal rests, Around which a partial removable dental prosthesis tends to rotate under masticatory forces. The determinants for the fulcrum line are usually the cross arch occlusal rests located adjacent to the tissue borne components
6. Put components of clasping and reciprocators closer to root area tooth alterations, lowering survey lines.
More far away from gingiva more unwanted movement. Q: Is it better for the tooth to put the clasp above or below the survey line? Below the survey line, because it is closer to the root. But when the maximum bulge is high survey line will be high, so we do tooth alteration, we try to grind from the tooth to
- 18 -
lower the survey line buccally. We do the same thing at the lingual side for the reciprocal arm of the clasp. 7. Cross arch stabilization. 8. Altered cast technique impressions, by eliminating any space between distal extension and the ridge. 9. The rest design.
The best rest directs the forces vertically to the tooth
Periodontal reactions related to RPD. 1. If you put the force in a correct direction, you can get the optimal health of PDL. 2. The use of RPDs leads to detrimental qualitative and quantitative changes in plaque. So use hygienic design of all components coming in contact with teeth or gingival tissue (the major connecter away from marginal gingiva, not touching it). 3. Maintain oral hygiene and keep recalling the patient on long term.
- 19 -
NOTE: not all of the slides are included in this script; there are some with extra pictures. So, you should go back to them!
THE END
: :
- 20 -
You might also like
- Prostho 9, Teeth SettingDocument15 pagesProstho 9, Teeth SettingJustDen09No ratings yet
- Nikitha AnchorageDocument116 pagesNikitha AnchorageMounika S100% (1)
- Management of Shallow VestibuleDocument4 pagesManagement of Shallow VestibuleNola SyairNo ratings yet
- Lec.9 Ortho. MovementDocument10 pagesLec.9 Ortho. MovementSaid SaidNo ratings yet
- ADEA EssaysDocument6 pagesADEA EssaysprasantiNo ratings yet
- Oet SpeakingDocument8 pagesOet SpeakingGouri Kalambi Gokarn100% (5)
- The Roth PrescriptionDocument7 pagesThe Roth PrescriptionsanjeetNo ratings yet
- A Simple Guide to Temporomandibular Joint Disorders, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Temporomandibular Joint Disorders, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Teeth Grinding (Bruxism), A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandTeeth Grinding (Bruxism), A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Anchorage: By, Ayesha Khan Ambreen ThobaniDocument33 pagesAnchorage: By, Ayesha Khan Ambreen ThobaniMaira HassanNo ratings yet
- Anchorage in OrthodonticsDocument127 pagesAnchorage in Orthodonticsmustafa_tambawala75% (4)
- Report On AnchorageDocument69 pagesReport On AnchorageHari KrishnaNo ratings yet
- Prostho Sheet 2Document31 pagesProstho Sheet 2Yomna NimerNo ratings yet
- Prostho 9Document20 pagesProstho 9junjiaNo ratings yet
- Prostho Lec - OverdenturesDocument14 pagesProstho Lec - Overdenturesdrgayen6042No ratings yet
- Prostho#8Document9 pagesProstho#8api-19840404No ratings yet
- Presnebdr M. Rkhaif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresnebdr M. Rkhaif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presnebdr M. Rukhaif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresnebdr M. Rukhaif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presnebdr M. Rkhaif Zaman Khan Department Oorthodontics and Dentofacial OrthopaedicsDocument21 pagesPresnebdr M. Rkhaif Zaman Khan Department Oorthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presnebdr M. Rkhaif Zaman Khan Department Oorthodouuuktukntics and Dentofacial OrthopaedicsDocument21 pagesPresnebdr M. Rkhaif Zaman Khan Department Oorthodouuuktukntics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presned BDR K. M. Rukhaif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresned BDR K. M. Rukhaif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presnted by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresnted by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presnted by DR K. M. Rukhsh Aif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresnted by DR K. M. Rukhsh Aif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presnted by Dr. K. M. Rukhsh Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresnted by Dr. K. M. Rukhsh Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Bite Forces and Bite PressureDocument7 pagesBite Forces and Bite PressureDrAmit PatilNo ratings yet
- Introduction To Removable Partial Denture IIDocument16 pagesIntroduction To Removable Partial Denture IIkilolopoNo ratings yet
- Space MGMT PPT 38Document81 pagesSpace MGMT PPT 38AbboodNo ratings yet
- Fixed AppliancesDocument16 pagesFixed AppliancesAmmar Aldawoodyeh100% (1)
- General Information About The Rapid Maxillary Expander: Dr's Ranu, Crowe & StankeviciusDocument4 pagesGeneral Information About The Rapid Maxillary Expander: Dr's Ranu, Crowe & StankeviciusSitti Nur QomariahNo ratings yet
- Bio329-Study Guide-4Document5 pagesBio329-Study Guide-4AsepDaryaNo ratings yet
- Revision Occlusion: Hazem MohamedDocument18 pagesRevision Occlusion: Hazem Mohamedasop06No ratings yet
- Maturational Changes in The Jaw and TeethDocument4 pagesMaturational Changes in The Jaw and TeethHayley WelshNo ratings yet
- Crown & BridgeDocument10 pagesCrown & Bridgeapi-19840404No ratings yet
- Q: Why Do Teeth Drift Mesially, Not Distally?Document8 pagesQ: Why Do Teeth Drift Mesially, Not Distally?Shazrin AhmadNo ratings yet
- Types of Dental ForcepsDocument10 pagesTypes of Dental Forcepspradyum doibaleNo ratings yet
- Presented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Presented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDocument21 pagesPresented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNo ratings yet
- Pedo V Script 1management of Developing OcclusionDocument12 pagesPedo V Script 1management of Developing OcclusionPrince AhmedNo ratings yet
- Penjangkaran: Yenny Yustisia Bag. Ortodonsia FKG UnejDocument47 pagesPenjangkaran: Yenny Yustisia Bag. Ortodonsia FKG UnejPrima D AndriNo ratings yet
- 1 - IntroductionDocument28 pages1 - IntroductionsamiyaNo ratings yet
- Oral Histo 9th Lec Pt2Document18 pagesOral Histo 9th Lec Pt2Khalid MortajaNo ratings yet
- Removable Partial DentureDocument72 pagesRemovable Partial DentureAyodele Oludare AyodejiNo ratings yet
- Occlusion IIDocument55 pagesOcclusion IIAnubhuti Gupta100% (2)
- Chpt-08 Ortho NotesDocument6 pagesChpt-08 Ortho NotesdaneshkumarytcNo ratings yet
- Periodontal & Bone Response To Normal Function: 16-4-2020 by DR - Anees MaweriDocument57 pagesPeriodontal & Bone Response To Normal Function: 16-4-2020 by DR - Anees MaweriAnees MaweriNo ratings yet
- Short Note OrthoDocument28 pagesShort Note Orthomhmdalbdyny764No ratings yet
- Dental Anatomy - Lecture 2Document9 pagesDental Anatomy - Lecture 2Mohamed Harun B. SanohNo ratings yet
- Tooth MovementDocument48 pagesTooth MovementSweta RajputNo ratings yet
- Ortho Intro #5 - Anchorage and HeadgearDocument5 pagesOrtho Intro #5 - Anchorage and HeadgearOrion KongNo ratings yet
- Development of Normal Occlusion Part 2 Copy 2Document49 pagesDevelopment of Normal Occlusion Part 2 Copy 2MSA universityNo ratings yet
- Anatomy of Edentouls Maxilla and MandibleDocument30 pagesAnatomy of Edentouls Maxilla and MandibleYazmine ElsayedNo ratings yet
- Fractured Tooth, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandFractured Tooth, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Oral PigmentationsDocument64 pagesOral PigmentationsAbeer KhasawnehNo ratings yet
- Final O.MDocument8 pagesFinal O.MAbeer KhasawnehNo ratings yet
- AseelDocument4 pagesAseelAbeer KhasawnehNo ratings yet
- 3 EditedDocument22 pages3 EditedAbeer KhasawnehNo ratings yet
- Prosthodontics: Physiology of The Cell Is Altered But It Goes Back To Be NormalDocument5 pagesProsthodontics: Physiology of The Cell Is Altered But It Goes Back To Be NormalAbeer KhasawnehNo ratings yet
- Lec2 Radiation PhysicsDocument12 pagesLec2 Radiation PhysicsSawsan Z. JwaiedNo ratings yet
- 041-مصطفي محود - رجل تحت الصفرDocument97 pages041-مصطفي محود - رجل تحت الصفرboshkashxp0% (1)
- Final Practical Exam InstructionsDocument1 pageFinal Practical Exam InstructionsAbeer KhasawnehNo ratings yet
- Anti NeoplasiaDocument17 pagesAnti NeoplasiaAbeer KhasawnehNo ratings yet
- Lecture 4, Methods of Measuring Periodontal DiseasesDocument9 pagesLecture 4, Methods of Measuring Periodontal DiseasesJustDen09No ratings yet
- General Pharmacology: Pharmacology of The BloodDocument30 pagesGeneral Pharmacology: Pharmacology of The BloodAbeer KhasawnehNo ratings yet
- Peri: Around Odont: Tooth Logous: Study Itis: Inflammation Principle FibersDocument6 pagesPeri: Around Odont: Tooth Logous: Study Itis: Inflammation Principle FibersBea YmsnNo ratings yet
- Segmented Arch or Continuous Arch Technique? A Rational ApproachDocument1 pageSegmented Arch or Continuous Arch Technique? A Rational ApproachSantos TicaNo ratings yet
- Current Perspectives On Use of Aloe Vera in DentistryDocument12 pagesCurrent Perspectives On Use of Aloe Vera in DentistrysevattapillaiNo ratings yet
- Partial Veneer Crown N' BioDocument6 pagesPartial Veneer Crown N' BioNoor HaiderNo ratings yet
- 19-A Natural Head Position Technique For Radiographic CephalometryDocument3 pages19-A Natural Head Position Technique For Radiographic CephalometryAlvaro ChacónNo ratings yet
- University of Sheffield Bachelor of Dental Surgery BrochureDocument12 pagesUniversity of Sheffield Bachelor of Dental Surgery BrochureYoussef MaharemNo ratings yet
- Dental Aesthetic and Self Confidence Among Filipino AdolescentsDocument9 pagesDental Aesthetic and Self Confidence Among Filipino Adolescentssumbu pendekNo ratings yet
- B - Cracked Tooth SyndromeDocument8 pagesB - Cracked Tooth SyndromeDavid TaylorNo ratings yet
- Perio PaperDocument9 pagesPerio Paperapi-391478637No ratings yet
- Registry RegisteredDocument141 pagesRegistry RegisteredKesiime EstherNo ratings yet
- Management of Oral Cancer (1) ...Document3 pagesManagement of Oral Cancer (1) ...Mircea IlieNo ratings yet
- Kunta Ar Soram J530205010 TaurodonsiaDocument3 pagesKunta Ar Soram J530205010 TaurodonsiaKunta ArsoramNo ratings yet
- Pitch, Roll, and Yaw: Describing The Spatial Orientation of Dentofacial TraitsDocument6 pagesPitch, Roll, and Yaw: Describing The Spatial Orientation of Dentofacial TraitssanjeetNo ratings yet
- 28 Pinho Dental Asymmetries PDFDocument7 pages28 Pinho Dental Asymmetries PDFDr. Naji ArandiNo ratings yet
- Pediatric Oral HealthDocument172 pagesPediatric Oral HealthArif HidayatNo ratings yet
- Controversies in Condylar Fracture Repair UntalanDocument35 pagesControversies in Condylar Fracture Repair UntalanFrederick Mars Untalan100% (1)
- Long-Term Radiologic Pulp Evaluation After Partial Pulpotomy in Young Permanent MolarsDocument9 pagesLong-Term Radiologic Pulp Evaluation After Partial Pulpotomy in Young Permanent MolarsAbdul Rahman AlmishhdanyNo ratings yet
- Maccabi Supplemental PlansDocument36 pagesMaccabi Supplemental PlansEnglishAccessibilityNo ratings yet
- Reciprocation Is Active When The Retainer Is Active Along The Retention Distance (TheDocument8 pagesReciprocation Is Active When The Retainer Is Active Along The Retention Distance (TheNour S. El ShayebNo ratings yet
- Gingival Overgrowth and Altered Passive Eruption in Adolescents Literature Review and Case ReportDocument8 pagesGingival Overgrowth and Altered Passive Eruption in Adolescents Literature Review and Case ReportAulia ElnisaNo ratings yet
- Jaringan Keras Dan Jaringan Pendukung Gigi". Penerbit BukuDocument6 pagesJaringan Keras Dan Jaringan Pendukung Gigi". Penerbit BukuStacia AnastashaNo ratings yet
- Entrevista BjornDocument11 pagesEntrevista BjornMirza GlusacNo ratings yet
- Anesthetic Considerations in Dental SpecialtiesDocument10 pagesAnesthetic Considerations in Dental SpecialtiesOmar FawazNo ratings yet
- TeledentistryDocument4 pagesTeledentistrypopat78100% (1)
- Sarezidento Programa 'Ortopediuli Stomatologia (Xangrzlivoba - 15 Tve) Tavi I. Zogadi Debulebebi Muxli 1. Programis Mizani Da AmocanebiDocument26 pagesSarezidento Programa 'Ortopediuli Stomatologia (Xangrzlivoba - 15 Tve) Tavi I. Zogadi Debulebebi Muxli 1. Programis Mizani Da AmocanebiLaSha BatnidzeNo ratings yet
- US Army Medical Course MD0510-200 - General Duties of The Dental SpecialistDocument75 pagesUS Army Medical Course MD0510-200 - General Duties of The Dental SpecialistGeorges100% (4)
- Organisational Change, Environmental and Ethical IssuesDocument20 pagesOrganisational Change, Environmental and Ethical IssuesCvetozar MilanovNo ratings yet