Professional Documents
Culture Documents
T Wave / T Talas
Uploaded by
LidianaBeka0%(1)0% found this document useful (1 vote)
288 views14 pagesThis document describes abnormalities of the T wave seen on electrocardiograms. It discusses various types of T wave abnormalities including peaked, hyperacute, inverted, biphasic, 'camel hump', and flattened T waves. For each type of abnormality, it provides examples of common causes such as hyperkalemia, myocardial ischemia or infarction, bundle branch blocks, ventricular hypertrophy, pulmonary embolism, and electrolyte abnormalities. Each abnormality pattern is illustrated with example ECG tracings.
Original Description:
promene T talasa
Original Title
T wave / T talas
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document describes abnormalities of the T wave seen on electrocardiograms. It discusses various types of T wave abnormalities including peaked, hyperacute, inverted, biphasic, 'camel hump', and flattened T waves. For each type of abnormality, it provides examples of common causes such as hyperkalemia, myocardial ischemia or infarction, bundle branch blocks, ventricular hypertrophy, pulmonary embolism, and electrolyte abnormalities. Each abnormality pattern is illustrated with example ECG tracings.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0%(1)0% found this document useful (1 vote)
288 views14 pagesT Wave / T Talas
Uploaded by
LidianaBekaThis document describes abnormalities of the T wave seen on electrocardiograms. It discusses various types of T wave abnormalities including peaked, hyperacute, inverted, biphasic, 'camel hump', and flattened T waves. For each type of abnormality, it provides examples of common causes such as hyperkalemia, myocardial ischemia or infarction, bundle branch blocks, ventricular hypertrophy, pulmonary embolism, and electrolyte abnormalities. Each abnormality pattern is illustrated with example ECG tracings.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 14
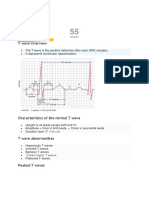
T wave
The T wave is the positive deflection after each QRS complex.
It represents ventricular repolarisation.
Characteristics of the normal T wave
Upright in all leads except aVR and V1
Amplitude < 5mm in limb leads, < 15mm in precordial leads
Duration (see QT interval)
T wave abnormalities
Hyperacute T waves
Inverted T waves
Biphasic T waves
Camel Hump T waves
Flattened T waves
Peaked T waves
Tall, narrow, symmetrically peaked T-waves are characteristically seen in hyperkalaemia.
Peaked T waves due to hyperkalaemia
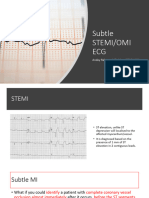
Hyperacute T waves
Broad, asymmetrically peaked or hyperacute T-waves are seen in the early stages of ST-elevation
MI (STEMI) and often precede the appearance of ST elevation and Q waves. They are also seen
with Prinzmetal angina.
Hyperacute T waves due to anterior STEMI
Loss of precordial T-wave balance
Loss of precordial T-wave imbalance occurs when the upright T wave is larger than that in V6. This
is a type of hyperacute T wave.
The normal T wave in V1 is inverted. An upright T wave in V1 is considered
abnormal especially if it is tall (TTV1), and especially if it is new (NTTV1).
This finding indicates a high likelihood of coronary artery disease, and when new
implies acute ischemia.
Inverted T waves
Inverted T waves are seen in the following conditions:
Normal finding in children
Persistent juvenile T wave pattern
Myocardial ischaemia and infarction
Bundle branch block
Ventricular hypertrophy (strain patterns)
Pulmonary embolism
Hypertrophic cardiomyopathy
Raised intracranial pressure
T wave inversion in lead III is a normal variant. New T-wave inversion (compared with prior
ECGs) is always abnormal. Pathological T wave inversion is usually symmetrical and deep
(>3mm).
Paediatric T waves
Inverted T-waves in the right precordial leads (V1-3) are a normal finding in children, representing
the dominance of right ventricular forces.
Normal pattern of T-wave inversions in a 2-year old boy
Persistent Juvenile T-wave Pattern
T-wave inversions in the right precordial leads may persist into adulthood and are most commonly
seen in young Afro-Caribbean women. Persistent juvenile T-waves are asymmetric, shallow
(<3mm) and usually limited to leads V1-3.
Persistent juvenile T-waves in an adult
Myocardial Ischaemia and Infarction
T-wave inversions due to myocardial ischaemia or infarction occur in contiguous leads based on the
anatomical location of the area of ischaemia/infarction:
Inferior = II, III, aVF
Lateral = I, aVL, V5-6
Anterior = V2-6
NOTE:
Dynamic T-wave inversions are seen with acute myocardial ischaemia.
Fixed T-wave inversions are seen following infarction, usually in association with
pathological Q waves.
Inferior T wave inversion due to acute ischaemia
Inferior T wave inversion with Q waves due to prior inferior MI
T wave inversion in the lateral leads due to acute ischaemia
Anterior T wave inversion with Q waves due to recent anterior MI
Bundle Branch Block
Left Bundle Branch Block
Left bundle branch block produces T-wave inversion in the lateral leads I, aVL and V5-6.
Lateral T wave inversion due to LBBB
Right Bundle Branch Block
Right bundle branch block produces T-wave inversion in the right precordial leads V1-3.
T-wave inversion in the right precordial leads due to RBBB
Ventricular Hypertrophy
Left Ventricular Hypertrophy
Left ventricular hypertrophy produces T-wave inversion in the lateral leads I, aVL, V5-6 (left
ventricular strain pattern), with a similar morphology to that seen in LBBB.
Lateral T wave inversion due to LVH
Right Ventricular Hypertrophy
Right ventricular hypertrophy produces T-wave inversion in the right precordial leads V1-3 (right
ventricular strain pattern) and also the inferior leads (II, III, aVF).
T wave inversion in the inferior and right precordial leads due to RVH
Pulmonary Embolism
Acute right heart strain (e.g. secondary to massive pulmonary embolism) produces a similar pattern
to RVH, with T-wave inversions in the right precordial (V1-3) and inferior (II, III, aVF) leads.
T wave inversion in the inferior and right precordial leads in a patient with bilateral PEs
Deep T wave inversion in V1-3 with RBBB in a patient with massive PE
Pulmonary embolism may also produce T-wave inversion in lead III as part of the S
I
Q
III
T
III
pattern
(S wave in lead I, Q wave in lead III, T-wave inversion in lead III).
SI QIII TIII pattern in acute PE
Hypertrophic Cardiomyopathy (HOCM)
HOCM is associated with deep T wave inversions in all the precordial leads.
T wave inversion in V1-6 due to HOCM
Raised intracranial pressure
Events causing a sudden rise in ICP (e.g. subarachnoid haemorrhage) produce widespread deep T-
wave inversions with a bizarre morphology.
Widespread deep T wave inversion due to SAH
Biphasic T waves
There are two main causes of biphasic T waves:
Myocardial ischaemia
Hypokalaemia
The two waves go in opposite directions:
Ischaemic T waves go up then down
Hypokalaemic T waves go down then up
Ischaemia
Biphasic T waves due to ischaemia
Hypokalaemia
Biphasic T waves due to hypokalaemia
Wellens Syndrome
Wellens syndrome is a pattern of inverted or biphasic T waves in V2-3 (in patients presenting with
ischaemic chest pain) that is highly specific for critical stenosis of the left anterior descending
artery.
There are two patterns of T-wave abnormality in Wellens syndrome:
Type 1 Wellens T-waves are deeply and symmetrically inverted
Type 2 Wellens T-waves are biphasic, with the initial deflection positive and the
terminal deflection negative
Wellens Type 1
Wellens Type 2
Camel hump T waves
This is a term used by the great ECG lecturer and Emergency Physician Amal Mattu to describe T-
waves that have a double peak or camel hump appearance.
There are two causes for camel hump T waves:
Prominent U waves fused to the end of the T wave, as seen in severe hypokalaemia
Hidden P waves embedded in the T wave, as seen in sinus tachycardia and various
types of heart block
Prominent U waves due to severe hypokalaemia
Hidden P waves in sinus tachycardia
Hidden P waves in marked 1st degree heart block
Hidden P waves in 2nd degree heart block with 2:1 conduction
Flattened T waves
Flattened T waves are a non-specific finding, but may represent ischaemia (if dynamic or in
contiguous leads) or electrolyte abnormality, e.g. hypokalaemia (if generalised).
Ischaemia
Dynamic T-wave flattening due to anterior ischaemia (above). T waves return to normal once the
ischaemia resolves (below).
Dynamic T wave flattening due to anterior ischaemia
T waves return to normal as ischaemia resolves
Hypokalaemia
Note generalised T-wave flattening with prominent U waves in the anterior leads (V2 and V3).
T wave flattening due to hypokalaemia
You might also like
- T WaveDocument15 pagesT WaveKay BristolNo ratings yet
- T WaveDocument15 pagesT WaveKay BristolNo ratings yet
- ECG NotesDocument85 pagesECG NotesMalcum TurnbullNo ratings yet
- ECG Master Class-3Document97 pagesECG Master Class-3Shohag ID CenterNo ratings yet
- ST-T Depression HannaDocument11 pagesST-T Depression Hannadrimran570No ratings yet
- T Wave PDFDocument6 pagesT Wave PDFgabernNo ratings yet
- УСПDocument50 pagesУСПAli Aborges Jr.No ratings yet
- Wellen EcgDocument9 pagesWellen EcgElokNo ratings yet
- EkgDocument3 pagesEkgMihaela GaidurNo ratings yet
- LITFL - Wellens SyndromeDocument8 pagesLITFL - Wellens Syndromesunil abrahamNo ratings yet
- ST Segment DepressiDocument16 pagesST Segment Depressiaya405No ratings yet
- ECG Master Class-1Document132 pagesECG Master Class-1Shohag ID Center100% (1)
- ABC of Clinical Electrocardiography - Introduction. II-Basic Terminology - PMCDocument11 pagesABC of Clinical Electrocardiography - Introduction. II-Basic Terminology - PMCRuban RichardNo ratings yet
- ST Segment DepressiDocument16 pagesST Segment DepressiHayaNo ratings yet
- 4-Subtle ECG in ACSDocument20 pages4-Subtle ECG in ACSyandraNo ratings yet
- Top 100 ECG CasesDocument212 pagesTop 100 ECG Casessoha.s.tumsa7No ratings yet
- Electrocardiograms in The Pediatric EDDocument69 pagesElectrocardiograms in The Pediatric EDbradsoboNo ratings yet
- Right Ventricular StrainDocument9 pagesRight Ventricular StrainhasaɴNo ratings yet
- ECG & ArrhythmiasDocument8 pagesECG & ArrhythmiasDr. SobanNo ratings yet
- ECG Made Easy - An Abnormal LookDocument46 pagesECG Made Easy - An Abnormal LookabdallahNo ratings yet
- Basic ECG and Arrhythmia FINALDocument16 pagesBasic ECG and Arrhythmia FINALCharlotte James100% (5)
- TH TH TH THDocument9 pagesTH TH TH THAlex PengNo ratings yet
- ECG DiscussionDocument33 pagesECG Discussionyrx8k8j9qyNo ratings yet
- XI. T Wave Abnormalities: Frank G. Yanowitz, MD Professor of Medicine University of Utah School of MedicineDocument1 pageXI. T Wave Abnormalities: Frank G. Yanowitz, MD Professor of Medicine University of Utah School of MedicineLwin Maung Maung ThikeNo ratings yet
- ST Segment and T Waves:: Ischemia, Infarction, Drug & Electrolyte EffectsDocument34 pagesST Segment and T Waves:: Ischemia, Infarction, Drug & Electrolyte EffectsHibba NasserNo ratings yet
- Thinking About Ecgs (Garcia)Document9 pagesThinking About Ecgs (Garcia)Filip IonescuNo ratings yet
- 15.2. ECG 2 (Chambers Enlargement)Document149 pages15.2. ECG 2 (Chambers Enlargement)mirabel IvanaliNo ratings yet
- ECGDocument6 pagesECGMatthew MackeyNo ratings yet
- Ekg PJKDocument113 pagesEkg PJKdevipuspaNo ratings yet
- ST - Elevation Myocardial InfarctionDocument25 pagesST - Elevation Myocardial InfarctionJo CanensNo ratings yet
- ECG Findings: Valvular Heart Disease Cardiomyopathies MyocarditisDocument30 pagesECG Findings: Valvular Heart Disease Cardiomyopathies MyocarditisensiNo ratings yet
- Wellens SyndromeDocument4 pagesWellens Syndromeqayyum consultantfpscNo ratings yet
- P Wave With A Broad ( 0.04 Sec or 1 Small Square) and Deeply Negative ( 1 MM) Terminal Part in V1 P Wave Duration 0.12 Sec in Leads I and / or IIDocument9 pagesP Wave With A Broad ( 0.04 Sec or 1 Small Square) and Deeply Negative ( 1 MM) Terminal Part in V1 P Wave Duration 0.12 Sec in Leads I and / or IIpisbolsagogulamanNo ratings yet
- EKG Interpretation: UNC Emergency Medicine Medical Student Lecture SeriesDocument58 pagesEKG Interpretation: UNC Emergency Medicine Medical Student Lecture SeriesRenn Karlo LindoNo ratings yet
- Lia TrapaidzeDocument32 pagesLia TrapaidzeShubham TanwarNo ratings yet
- EKG Interpretation: UNC Emergency Medicine Medical Student Lecture SeriesDocument58 pagesEKG Interpretation: UNC Emergency Medicine Medical Student Lecture SeriesDyah Ajeng PratiwiNo ratings yet
- EKG Interpretation: UNC Emergency Medicine Medical Student Lecture SeriesDocument58 pagesEKG Interpretation: UNC Emergency Medicine Medical Student Lecture SeriesWidya Surya AvantiNo ratings yet
- Ekg FastlaneDocument10 pagesEkg FastlaneAida UzunovicNo ratings yet
- Introduction To ECG: Presenter: Emiacu Kenneth Facilitator: Dr. Ssebuliba MosesDocument36 pagesIntroduction To ECG: Presenter: Emiacu Kenneth Facilitator: Dr. Ssebuliba MosesNinaNo ratings yet
- Stemi, Stemi Equivalents and STEMI Mimics: Kyaw Soe WinDocument114 pagesStemi, Stemi Equivalents and STEMI Mimics: Kyaw Soe WinYoung MilkNo ratings yet
- Normal Atria: o o o o o o oDocument5 pagesNormal Atria: o o o o o o oPoetraSyah اولياء 花火No ratings yet
- A Normal Adult 12Document8 pagesA Normal Adult 12el adikkzNo ratings yet
- 7InitialDraft 4Document8 pages7InitialDraft 4pigzeniNo ratings yet
- ECG TerminologyDocument66 pagesECG TerminologyblndfflNo ratings yet
- ECG NotesDocument7 pagesECG NotesShams NabeelNo ratings yet
- Physio 4.3-4.5Document4 pagesPhysio 4.3-4.5Raj BulaNo ratings yet
- EKG PJK Co AssDocument115 pagesEKG PJK Co AsssalmaNo ratings yet
- EKG Interpretation: UNS Cardiovascular Dept Medical Student Lecture SeriesDocument85 pagesEKG Interpretation: UNS Cardiovascular Dept Medical Student Lecture Seriesandina rosmalianti100% (1)
- T Wave & U WaveDocument4 pagesT Wave & U WavejthsNo ratings yet
- Stemi'Document25 pagesStemi'Kaviya RaviNo ratings yet
- 2 ECG HockstadDocument65 pages2 ECG HockstadAUH ICUNo ratings yet
- ECG - Doc 09Document11 pagesECG - Doc 09Rincy RajanNo ratings yet
- EKG+Mastery +ischemiaDocument6 pagesEKG+Mastery +ischemiamoussa medjahedNo ratings yet
- EKG+Mastery +ischemia PDFDocument6 pagesEKG+Mastery +ischemia PDFCatur Ari Intan PuspitasariNo ratings yet
- Anterior Myocardial InfarctionDocument14 pagesAnterior Myocardial InfarctionUtami HandayaniNo ratings yet
- Anatomy, Physiology & Conduction System of The HeartDocument122 pagesAnatomy, Physiology & Conduction System of The HeartShelly Lavenia Sambodo100% (1)
- EKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookFrom EverandEKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookNo ratings yet
- The Effect of Uterine Closure Technique On Cesarean Scar Niche Development After Multiple Cesarean DeliveriesDocument8 pagesThe Effect of Uterine Closure Technique On Cesarean Scar Niche Development After Multiple Cesarean DeliveriesWillans Eduardo Rosha HumerezNo ratings yet
- Prevalencia de Ulcera Gastrica en Caballos Con Colico EquinoDocument7 pagesPrevalencia de Ulcera Gastrica en Caballos Con Colico EquinoMaria Paula DuqueNo ratings yet
- What Is Gestational DiabetesDocument6 pagesWhat Is Gestational DiabetesLiza M. PurocNo ratings yet
- Office PDFDocument65 pagesOffice PDFSugar MusicNo ratings yet
- Systemic Absorption of Topically Administered DrugsDocument8 pagesSystemic Absorption of Topically Administered Drugstaner_soysuren100% (2)
- Final Profile Draft - Zach HelfantDocument5 pagesFinal Profile Draft - Zach Helfantapi-547420544No ratings yet
- Roleplay Persalinan Inggris Bu ShintaDocument4 pagesRoleplay Persalinan Inggris Bu ShintaDyta Noorfaiqoh MardlatillahNo ratings yet
- Managment of Sepsis and Septic ShockDocument2 pagesManagment of Sepsis and Septic ShockDavid Simon CruzNo ratings yet
- Jurnal NeuroDocument6 pagesJurnal NeuroSiti WahyuningsihNo ratings yet
- Revision MCQsDocument6 pagesRevision MCQswiamNo ratings yet
- COVID-19 Prevention PlanDocument12 pagesCOVID-19 Prevention PlanZubair KhanNo ratings yet
- Agaches Measuring The Skin Non-Invasive Investigations, Physiology, Normal Constants (Philippe Humbert, Ferial Fanian Etc.) (Z-Library)Document1,622 pagesAgaches Measuring The Skin Non-Invasive Investigations, Physiology, Normal Constants (Philippe Humbert, Ferial Fanian Etc.) (Z-Library)irina obrejaNo ratings yet
- Pterygium After Surgery JDocument6 pagesPterygium After Surgery JRayhan AlatasNo ratings yet
- 12 - 01 DR - Anang - Airway Management Basic AG FinalDocument41 pages12 - 01 DR - Anang - Airway Management Basic AG FinalmeirismaNo ratings yet
- Alcoholic Liver DiseasesDocument45 pagesAlcoholic Liver DiseasesSunith KanakuntlaNo ratings yet
- Developement of Wearable Therapy Device For Carpal Tunnel SyndromeDocument56 pagesDevelopement of Wearable Therapy Device For Carpal Tunnel SyndromeZulfadhli ZulkafliNo ratings yet
- ANTIJAMURDocument3 pagesANTIJAMURCharlesMahonoNo ratings yet
- Single Choice Questions in ORTHOPAEDICS Mahmood A Sulaiman: January 2019Document186 pagesSingle Choice Questions in ORTHOPAEDICS Mahmood A Sulaiman: January 2019Kiran Kumar100% (1)
- Pathological Anatomy IntroductionDocument9 pagesPathological Anatomy IntroductionRashid NawazNo ratings yet
- TLE 9 Organic Agri Q1 M5Document21 pagesTLE 9 Organic Agri Q1 M5Netchie BajeNo ratings yet
- PMLS (Mod 1-3)Document23 pagesPMLS (Mod 1-3)Ja NaeNo ratings yet
- Pediatrics Rapid RevisionDocument72 pagesPediatrics Rapid RevisionWorld MedclickzNo ratings yet
- Case Study An Older COVID-19 Patient in A Turkish IntensiveDocument7 pagesCase Study An Older COVID-19 Patient in A Turkish IntensiveAJENGNo ratings yet
- Philippine Orthopedic Center Hospital Services and Times of AvailabilityDocument2 pagesPhilippine Orthopedic Center Hospital Services and Times of AvailabilityJhay GoloNo ratings yet
- A Patient 'S Guide To Refractive SurgeryDocument7 pagesA Patient 'S Guide To Refractive SurgeryJon HinesNo ratings yet
- Drug Used in The Therapy of Shock.Document8 pagesDrug Used in The Therapy of Shock.Vennela100% (1)
- Bachelor of Science in Project and Facility Management With Honours MAY 2020Document17 pagesBachelor of Science in Project and Facility Management With Honours MAY 2020Suziah Baindis AngkimNo ratings yet
- National Filariasis Elimination ProgramDocument20 pagesNational Filariasis Elimination ProgramNaomi Cyden YapNo ratings yet
- Shadow Health Focused Exam Anxiety John LarsenDocument4 pagesShadow Health Focused Exam Anxiety John LarsenJaskaran KhakhNo ratings yet
- Kode ICD 10Document111 pagesKode ICD 10MarnitaNo ratings yet