Professional Documents
Culture Documents
The Histomorphological Study of Prostate Lesions
Uploaded by
IOSRjournalOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
The Histomorphological Study of Prostate Lesions
Uploaded by
IOSRjournalCopyright:
Available Formats
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS)
e-ISSN: 2279-0853, p-ISSN: 2279-0861.Volume 14, Issue 11 Ver. VIII (Nov. 2015), PP 85-89
www.iosrjournals.org
The histomorphological study of prostate lesions
Dr. Ashish Joshee, Dr. Kaushal C.L.Sharma
Institute- Department of Pathology, Geetanjali Medical College and Hospital, Udaipur
Corresponding author- Dr. Ashish Joshee
Abstract: With increasing life expectancy, increasing awareness and better health services lesions of prostate
has become a common specimen received for diagnostic of both benign and malignant lesions which may have a
very similar presentation but their management and prognosis is quite different. Most important investigation is
the biopsy of the prostate. A visual of features of the lesion gives best diagnosis. 122 prostate specimens were
studied over a period of 21 months and revealed most common lesion to be benign prostatic hyperplasia
routinely diagnosed on the commonest type of specimens obtained that were transuretheral resection of prostate
(TURP) with peak age of occurrence in 6th decade of life. Adenocarcinoma cases of Gleason grade 4 were
common also in same age range. Prostatic intraepithelial neoplasia lesions present a diagnostic challenge due to
them being a known precursor lesion of prostatic carcinoma. Histopathological diagnosis and grading plays a
definitive role in the management of prostatic cancer.
Keywords: prostate, benign hyperplasia of prostate, adenocarcinoma, Gleason grade, HGPIN
I.
Introduction-
Prostate is essential structure of the male reproductive system composed of glands and stroma and its
secretions forming 30-50 % of the seminal fluid volume.[1] With increasing life expectancy, increasing
awareness and better health services lesions of prostate has become a common specimen received for diagnostic
of both benign and malignant lesions. Most patients of benign lesions present with complaints related to
micturition and incontinence. The problem lies in the fact that malignant and benign lesions of prostate may
have a very similar presentation but their management and prognosis is quite different. Thus patients who have
been suffering from such symptoms should have themselves checked. A regular examination specifically
includes digital rectal examination (DRE) for an enlarged prostate apart from list up of the urinary complaints.
This DRE may not always be conclusive. A lab investigation that was previously linked to prostatic lesion is
prostate specific antigen levels whose increased levels were thought to be a good indicator. [2, 3] But its
significance is only complete when it is supported by histopathology. The most important investigation in such
cases is the biopsy of the prostate. Visually interpreting the features of the lesion gives best diagnosis. Knowing
the histological grade in malignant lesions helps in proper management. Thus diagnosis of prostatic lesions is
important both to the clinician and pathologist.
II. Material And Methods
The current study is a prospective study which includes data of cases from January 2014 to September
2015. The type of specimens received were transuretheral resection of prostate (TURP), transrectal ultrasound
(TRUS) guided trucut biopsy and cystoprostatectomy. The clinical data was collected from biopsy forms and
medical record department. The received specimens were fixed in 10% formalin and routine hematoxyline and
eosin staining was done. All the specimens were analysed as type of specimen, age of patient, microscopic
features and diagnosis. The 2002 W.H.O. classification was used to diagnose and classify prostate tumours. The
cases of adenocarcinoma were graded according to Gleason grading system.[4]
III. Results
In this study a total of 122 prostate specimens were studied which were received between January 2014
to September 2015 in the histopathology section of department of Pathology. Of the 122 specimens 81 (66 %)
were TURP specimens which were received as soft to firm grey white chips. Also 34 trucut biopsy specimens
(29%) were obtained as linear tissue strips, 0.3 to 1cm long.
DOI: 10.9790/0853-141188589
www.iosrjournals.org
85 | Page
The histomorphological study of prostate lesions
TYPES OF SPECIMEN
NUMBER
81
34
TURP
TRUS guided prostate biopsy Cystoprostatectomy
Table 1: Distribution of types of specimen received
The most common lesion diagnosed was benign prostatic hyperplasia in 79 cases with peak age of
occurrence in 6th decade of life. In the same age range maximum cases of the 30 adenocarcinoma cases were
seen. High grade prostatic intraepithelial neoplasia (HGPIN) was diagnosed in 8 cases.
Diagnosis
Benign prostatic hyperplasia
Adenocarcinoma
High grade prostatic intraepithelial neoplasia
Granulomatous prostatitis
Embryonal rhabdomyosarcoma
Small cell carcinoma
Number of cases
79
30
8
3
1
1
Percentage (%)
61
25
7
2
<1
<1
Table 2: Distribution of number of cases by diagnosis
Benign prostatic hyperplasia
On microscopy the glandular component is made up of nodules of small and large acini lined by basal
and secretory cells. Some gland show papillary infolding and projections and others that are dilated and cystic.
Stromal component often shows both fibrous and smooth muscle elements. Maximum cases were in age range
of 6th followed by 7th decade. Few cases also showed prostatitis.
Adenocarcinoma
Adenocarcinoma of prostate is the most common type of malignancy in the prostate and the glandular
pattern observed under low power microscope is important as it used for Gleason grading [4]. This grading
system has described 5 patterns; which are recognized as primary dominant pattern and the secondary (second
most dominant) structural patterns and given a grade from 1 to 5 with 1 being most differentiated and 5 the least
differentiated. These two grades are added together to obtain the Gleason score. The most common predominant
grades observed in this study were grade 4 and grade 3. No cases showed grades 1 and 2. The most common
score obtained was 7 in 13 cases of the total 30 adenocarcinoma cases.
Prostatic intraepithelial neoplasia
The diagnosis of prostatic intraepithelial neoplasia (PIN) is made when microscopically benign
prostatic acini or ducts are lined by cytologically atypical cells showing stratification and slight nuclear
enlargement.[5],[6],[7] In the current study 8 cases of PIN were diagnosed.
IV. Discussion
BPH and adenocarcinoma are the two most common conditions affecting prostate gland. In our study
TURP specimens were most common specimen received which was similar to that in studies conducted by
Shakya et al [8] and Mittal et al [9] indicating a similar diagnostic approach. In the present study, we had 61%
cases of BPH, 25% cases of adenocarcinoma and 7% case of HGPIN. The findings in our study are comparable
with those of Mittal et al [9], Mohammed et al [10] and Sharma et al [11].
DOI: 10.9790/0853-141188589
www.iosrjournals.org
86 | Page
The histomorphological study of prostate lesions
BPH is a condition where hyperplasia of both glandular and stromal components leading to an enlarged
prostate gland. The clinical incidence of this disease is only 8% during the fourth decade, but it reaches 50% in
the fifth decade and 75% in the eighth decade of life [12]. However, symptomatic BHP producing urinary
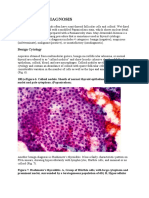
complaints and requiring surgical intervention is seen in only 5-10% of cases. Hyperplastic glands appear
cystically dilated with lining of two layers of cells, an inner columnar layer and an outer layer of cuboidal or
flattened epithelium (Figure 1). The nucleoli are inconspicuous. A continuous basal cell layer is seen
immediately above a basement membrane [13]. These glands often contain thickened secretions in their lumen
called corpora amylacea[14].
Fig 1. Benign hyperplasia of prostate (H&E X400)
In our study maximum cases of BPH were diagnosed in TURP specimens that are similar to Arora et al
[15]. This shows that TURP is still considered the gold standard for BPH cases. Maximum cases of BPH were
seen in the 61-69 years age group similar to Matapurkar et al[16]. Kim KB[17] et al had more cases in 8th
decade age group.
Chronic prostatitis is most commonly observed in nodular hyperplasia which was also seen by Kohnen
et al [18] in his study. But it is important to distinguish the true infectious processes of prostate from the
inconsequential mononuclear infiltrates often seen accompanying nodular hyperplasia [19]. In the current study
14 cases were diagnosed as chronic prostatitis where in microscopy showed presence of periglandular or
interglandular mononuclear cell infiltrate in the stroma, composed mainly of lymphocytes, few plasma cells and
histiocytes.
Granulomatous prostatitis can be clinically confused with prostatic carcinoma. The reported incidence
of granulomatous prostatitis is 0.36-4% [20],[21]. It is thought to represent an initially immune-mediated
process accompanied by a reaction to the prostatic secretions released from obstructed ducts [22, 23,24].
Histologically, an inflammatory reaction consisting of lymphocytes, macrophages, plasma cells and some giant
cells is seen. These granulomas are mostly centred in the lobules [25]. In the current study 2 cases of this
condition were seen.
PIN has been identified as a precursor lesion for prostatic carcinoma [26]. Currently conventional use
of the term PIN without qualification refers to only high grade PIN (HGPIN). The clinical importance of
recognising PIN is based on it being strongly associated with carcinoma of prostate. PIN has a high predictive
value as a marker for adenocarcinoma and its identification in biopsy specimens of the prostate should
necessitate a thorough search for invasive carcinoma [27]. PIN consists of architecturally benign large,
branching prostatic acini lined by cytologically atypical cells with prominent nucleoli [5].(Figure 2) In our
study 8 cases showed HGPIN features.
DOI: 10.9790/0853-141188589
www.iosrjournals.org
87 | Page
The histomorphological study of prostate lesions
Fig 2. High grade prostatic intraepithelial neoplasia (H&E X400)
Carcinoma of prostate is the second most common malignancy in men, second only to lung cancers
[28]. It is commonly seen in men above age of 50 years and it has age related increase in incidence, affecting
approximately 70% in men between the ages of 70 and 80 years [29]. Androgenic hormones play an important
role in occurrence of prostatic carcinoma [30]. A higher incidence has been seen in males with a first degree
relative being affected [31].
Microscopically in carcinoma there is only a single cell type without the basal layer. The pathological
diagnosis of carcinoma is indicated by crowded glands growing in haphazard fashion, large acini without
convolutions, fused glands, gland in gland, columns, cords and solid sheets. Nuclear enlargement with
prominent nucleoli is common (Figure 3). Adenocarcinoma accounted for 25% cases in our study. Maximum
numbers of our cases were in the 6 th decade. Sharma et al [11] had more cases in 7th decade.
Fig 3. Adenocarcinoma of prostate (H&E X400).
Adenocarcinomas were graded according to Gleasons system [2] by taking into account morphological
appearance of glandular cells and the glandular pattern. Most common predominant grades observed in this
study were grade 4 while none of the cases showed grades 1 and 2. The most common score obtained was 7 in
13 cases of adenocarcinoma. Vollmer [32] had score 6 most common whereas Brawn et al [33] had scores 6 &
7. Adenocarcinoma cases commonly show the presence of malignant glands within perineurial spaces [34].
This finding is a strong indicator of malignancy but is not pathognomonic[35]. It represents spread of glandular
tissue along planes of lesser resistance [36, 37]. Its presence in a needle biopsy specimen is a good predictor of
capsular invasion by the tumor [38]. Perineurial invasion was seen in 9 of the 30 carcinoma cases.
DOI: 10.9790/0853-141188589
www.iosrjournals.org
88 | Page
The histomorphological study of prostate lesions
V. Conclusion
TURP specimens were the most common type of specimen received for prostatic conditions. The
commonest age group affected by prostate lesions is the 6th decade of life and the most common lesion observed
is BPH followed by prostate adenocarcinoma. PIN lesions present an important diagnostic challenge as they are
a known precursor lesion of prostatic carcinoma. Histopathological diagnosis and grading plays a definitive role
in the management of prostatic cancer.
References
[1].
[2].
[3].
[4].
[5].
[6].
[7].
[8].
[9].
[10].
[11].
[12].
[13].
[14].
[15].
[16].
[17].
[18].
[19].
[20].
[21].
[22].
[23].
[24].
[25].
[26].
[27].
[28].
[29].
[30].
[31].
[32].
[33].
[34].
[35].
[36].
[37].
[38].
"Chemical composition of human semen and of the secretions of the prostate and seminal vehicles". Am J Physiol 136 (3): 467
473. 1942.
Thompson IM, Pauler DK, Goodman PJ, Tangen CM, Lucia MS, Parnes HL, Minasian LM, Ford LG, Lippman SM, Crawford ED,
Crowley JJ, Coltman CA (May 2004). "Prevalence of prostate cancer among men with a prostate-specific antigen level < or =4.0 ng
per milliliter". The New England Journal of Medicine 350 (22): 223946.
Crawford ED, Schutz MJ, Clejan S, Drago J, Resnick MI, Chodak GW, Gomella LG, Austenfeld M, Stone NN, Miles BJ (1992).
"The effect of digital rectal examination on prostate-specific antigen levels". Jama 267 (16): 22278.
Epstein JI, Allsbrook WCJr, Amin MB, Egevad LL. The 2005 International Society of Urological Pathology (ISUP) Consensus
Conference on Gleason Grading of Prostatic Carcinoma. Am J Surg Pathol 2005; 29(9):1228-1242.
McNeal JE, Bostwick DG. Intraductal dysplasia: a premalignant lesion of the prostate.Hum Pathol 1986;17:6471.
Bostwick DG, Brawer MK. Prostatic intra-epithelial neoplasia and earlyinvasion in prostate cancer. Cancer 1987;59:788794.
Drago JR, Mostofi FK, Lee F. Introductory remarks and workshop summay. Urol (Suppl)1989;34:23.
Shakya G, Malla S, Shakya KN. Salient and comorbid features in benign prostatic hyperplasia: A histopathological study of the
Prostate. Kathmandu Univ Med J. 2003; 2:104-109.
Mittal BV, Amin MB, Kinare SG. Spectrum of histological lesions in 185 consecutive prostatic specimens. J Postgrad Med 1989;
35:157.
Mohammed AZ, Alhasn SU, Edino ST, Ochicha O. Histopathological review of prostatic diseases in Kano, Nigeria. Niger Postgrad
Med J 2003; 10(1):1-5.
Sharma GC, Mathur SC, Sharma ML. Occult carcinoma in benign hypertrophy of prostate (Clinicopathological study of 100 cases).
Ind J Surg 1972 April: 152-155.
Bushman W: Etiology, epidemiology, and natural history of benign prostatic hyperplasia. Urol Clin N Am 36:403, 2009.
Rosai J Rosai and Ackerman's Surgical Pathology. 6th ed. London: Elsevier-Mosby; 2011;18:1289.
Smith MJ. Prostatic corpora amylacea. MonogrSurg Sci 1966, 3: 209265.
Arora AK, Agrawal R, Kumar P. Histopathological Spectrum of Prostatic Diseases. International Journal of advances in health
sciences 2015; 2(1): 94-100.
Matapurkar BG, Taneja OP. Incidence of carcinoma prostate. Ind J of Cancer 1969 Sept 172-182.
Kim KB, Kim KS. A Histopathological observation on 48 cases of benign prostatic hypertrophy. Korean J Urol 1982; 23(8):30.
Kohnen PW, Drach GW. Patterns of inflammation in prostatic hyperplasia: A histologic and bacterial study. J Urol 1979; 12:755
Theyer G, Kramer G, Assmann I, Sherwood E, Preinfalk W, Marberger M, Zechner O, Steiner GE. Phenotypic characterization of
infiltrating leukocytes in benign prostatic hyperplasia. Lab Invest 1992, 66: 96107.
Oppenheimer JR, Kahane H, Epstein JI. Granulomatous prostatitis on needle biopsy. Arch Path Lab Med 1997; 121(7):724-729.
Keuhnelian JG. Experiences with granulomatous prostatitis. J Urol 1964; 91:173.
Dhundee J, Maciver AG. An immunohistological study of granulomatous prostatitis. Histopathology 1991, 18: 435441.
Kelalis PP, Greene LF, Harrison EG Jr. Granulomatous prostatitis. A mimic of carcinoma of the prostate. JAMA 1965, 191: 111
113.
Uzoh CC, Uff JS, Okeke AA. Granulomatous prostatitis. BJU Int 2007, 99: 510512.
Peterson RO, Sesterhenn IA, Davis CJ, editors. Prostate. In: Urologic Pathology. Lippincott Williams and Wilkins; 2009. p. 451559.
Epstein JI. Precursor lesions to prostatic adenocarcinoma. Virchows Arch 2009, 454:116.
Deshmukh BD, Ramteerthakar NA, Sulhyan KR. Histopathological study of lesions of prostate - A five year study. Int J Health Sci
Res. 2014; 4(1):1-9.
"Prostate cancer statistics". Cancer Research UK. Retrieved 3 October 2014.
Hsing AW, Chokkalingam AP: Prostate cancer epidemiology. Front Biosci 11:1388, 2006.
Bostwick DG, Burke HB, Djakiew D, Euling S, Ho SM, Landolph J, Morrison H, Sonawane B, Shifflett T, Waters DJ, Timms B.
Human prostate cancer risk factors. Cancer 2004, 101:23712490.
Steinberg GD, Carter BS, Beaty TH, Childs B, Walsh PC (1990). "Family history and the risk of prostate cancer". Prostate 17 (4):
33747.
Vollmer RT. Prostatic cancer and chip specimen: complete versus partial sampling. Hum Pathol 1986; 17:285-290.
Brawn PN, Ayala AG, vonEschenbach AC, Hussey DH, Johnson DE. Histologic grading study of prostate adenocarcinoma: The
development of a new system and comparison with other methods- A preliminary study. Cancer 1982; 49:525-532.
Franks LM. Latent carcinoma of the prostate. JPathol Bacteriol 1954, 68: 603616.
Carstens PHB. Perineural glands in normal and hyperplastic prostates. J Urol 1980, 123:686688.
Hassan MO, Maksem J. The prostatic perineural space and its relation to tumor spread. Am J Surg Pathol 1980, 4: 143148.
Rodin AE, Larson DL, Roberts DK. Nature of perineural space invaded by prostatic carcinoma. Cancer 1967, 20: 17721779.
Bastacky SI, Walsh PC, Epstein JI. Relationship between perineural tumor invasion on needle biopsy and radical prostatectomy
capsular penetration in clinical stage B adenocarcinoma of the prostate. Am J Surg Pathol 1993, 17:336341.
DOI: 10.9790/0853-141188589
www.iosrjournals.org
89 | Page
You might also like
- Kinesics, Haptics and Proxemics: Aspects of Non - Verbal CommunicationDocument6 pagesKinesics, Haptics and Proxemics: Aspects of Non - Verbal CommunicationInternational Organization of Scientific Research (IOSR)No ratings yet
- File 1Document4 pagesFile 1Marsya Yulinesia LoppiesNo ratings yet
- Clinicopathological Study of Prostatic Biopsies: Abst TDocument4 pagesClinicopathological Study of Prostatic Biopsies: Abst TMata MataNo ratings yet
- Neuroendocrine Tumors Dr. WarsinggihDocument20 pagesNeuroendocrine Tumors Dr. WarsinggihAndi Eka Putra PerdanaNo ratings yet
- Philippine Journal of Gynecologic Oncology Volume 9 Number 1 2012Document48 pagesPhilippine Journal of Gynecologic Oncology Volume 9 Number 1 2012Dasha VeeNo ratings yet
- Jurnal Sitologi PDFDocument5 pagesJurnal Sitologi PDFIbnu Satria ApriansaNo ratings yet
- Diagnostic and Prognostic Markers For Gastrointestinal Stromal Tumors in NorwayDocument8 pagesDiagnostic and Prognostic Markers For Gastrointestinal Stromal Tumors in NorwayNengLukmanNo ratings yet
- 直肠类癌临床病理分析_李征Document3 pages直肠类癌临床病理分析_李征kuangzhu820No ratings yet
- Human Colonic TissuesDocument9 pagesHuman Colonic TissuesAnomar MRgNo ratings yet
- Cancer GuidelinesDocument17 pagesCancer GuidelinesJoni WitziNo ratings yet
- YagciDocument7 pagesYagciPatricia BezneaNo ratings yet
- Does Tumor Grade Influence The Rate of Lymph Node Metastasis in Apparent Early Stage Ovarian Cancer?Document4 pagesDoes Tumor Grade Influence The Rate of Lymph Node Metastasis in Apparent Early Stage Ovarian Cancer?Herry SasukeNo ratings yet
- Ijss Jan Oa08Document7 pagesIjss Jan Oa08IvanDwiKurniawanNo ratings yet
- 172 - 04 101 13 PDFDocument8 pages172 - 04 101 13 PDFAlexandrosNo ratings yet
- Rare Pancreatic Tumor Case ReportDocument3 pagesRare Pancreatic Tumor Case ReportcostachemfNo ratings yet
- Cummings Et Al-2014-The Journal of PathologyDocument9 pagesCummings Et Al-2014-The Journal of Pathologyalicia1990No ratings yet
- Clinical and Cytopathological Aspects in Phyllodes Tumors of The BreastDocument7 pagesClinical and Cytopathological Aspects in Phyllodes Tumors of The Breastreeves_coolNo ratings yet
- Yolk Sac Tumor Testis Suatu Laporan Kasus: Meta Zulyati OktoraDocument8 pagesYolk Sac Tumor Testis Suatu Laporan Kasus: Meta Zulyati OktorafreakNo ratings yet
- Urinary Tumor Markers For Bladder Cancer PDFDocument13 pagesUrinary Tumor Markers For Bladder Cancer PDFRaja SharmaNo ratings yet
- Analytic Hierarchy Process in An Online QuestionnaireDocument84 pagesAnalytic Hierarchy Process in An Online QuestionnaireUlianti UmurahNo ratings yet
- Multinodular Goiter-Diagnostic and Treatment Considerations: Thyroid DisordersDocument4 pagesMultinodular Goiter-Diagnostic and Treatment Considerations: Thyroid DisordersAchmad DainuriNo ratings yet
- RPB14150079015Document5 pagesRPB14150079015Ijupbs IjupbsNo ratings yet
- ESMOGuidelines Ann Oncol 2014Document10 pagesESMOGuidelines Ann Oncol 2014Vlad CiobanuNo ratings yet
- Carcinoid Tumor of The Appendix: A Case ReportDocument3 pagesCarcinoid Tumor of The Appendix: A Case ReportrywalkNo ratings yet
- Javali2018 en IdDocument10 pagesJavali2018 en IdDona Ratna SariNo ratings yet
- Diagnostics 13 01362Document10 pagesDiagnostics 13 01362ela.sofiaNo ratings yet
- EmerencyDocument3 pagesEmerencySehrish SiddiqueNo ratings yet
- Near-Infrared Raman Spectroscopy For TheDocument12 pagesNear-Infrared Raman Spectroscopy For TheAlberto Carlos Espinosa GaravitoNo ratings yet
- Solitary TumorDocument7 pagesSolitary TumorOla AzzahraNo ratings yet
- Diagnostic Accuracy Fine Needle Aspiration Cytology of Thyroid Gland LesionsDocument6 pagesDiagnostic Accuracy Fine Needle Aspiration Cytology of Thyroid Gland LesionsinventionjournalsNo ratings yet
- 10.1186@s13048 020 00619 6Document10 pages10.1186@s13048 020 00619 6Berry BancinNo ratings yet
- Song 2017Document8 pagesSong 2017Patricia BezneaNo ratings yet
- Benign Esophageal TumorsDocument24 pagesBenign Esophageal TumorsMikael Angeloo100% (1)
- Journal Obstructive JaundiceDocument8 pagesJournal Obstructive JaundiceHiLmy Zakiyah0% (1)
- The Thyroid Nodule: Clinical PracticeDocument8 pagesThe Thyroid Nodule: Clinical PracticeAkhdan AufaNo ratings yet
- Parotid Glands Tumours: Overview of A 10-Years Experience With 282 Patients, Focusing On 231 Benign Epithelial NeoplasmsDocument5 pagesParotid Glands Tumours: Overview of A 10-Years Experience With 282 Patients, Focusing On 231 Benign Epithelial NeoplasmsCeriaindriasariNo ratings yet
- 54 Raviswami EtalDocument3 pages54 Raviswami EtaleditorijmrhsNo ratings yet
- BiopsyDocument5 pagesBiopsyDavid YapNo ratings yet
- Testicular CancerDocument12 pagesTesticular Cancerghost_724No ratings yet
- Citologie-Fna Tiroida DocumentDocument10 pagesCitologie-Fna Tiroida DocumentMocanu RalucaNo ratings yet
- Adult Nursing 2 Teaching PlanDocument5 pagesAdult Nursing 2 Teaching PlanJerilee SoCute WattsNo ratings yet
- Malignant Transformation in An Ovarian Mature Cystic Teratoma: A Case ReportDocument4 pagesMalignant Transformation in An Ovarian Mature Cystic Teratoma: A Case ReportnajmulNo ratings yet
- En - 0120 9957 RCG 33 02 00134 PDFDocument10 pagesEn - 0120 9957 RCG 33 02 00134 PDFbernardo04061993No ratings yet
- ESMO Testicular CancerDocument8 pagesESMO Testicular CancerBernadetta ViaNo ratings yet
- A Review On The Accuracy of Bladder Cancer Detection MethodsDocument7 pagesA Review On The Accuracy of Bladder Cancer Detection MethodsrekanihlaNo ratings yet
- Epithelial To Mesenchymal Transition and Cell Biology of Molecular Regulation in Endometrial CarcinogenesisDocument17 pagesEpithelial To Mesenchymal Transition and Cell Biology of Molecular Regulation in Endometrial CarcinogenesisMelati HasnailNo ratings yet
- Localised Colon Cancer: ESMO Clinical Practice Guidelines For Diagnosis, Treatment and Follow-UpDocument15 pagesLocalised Colon Cancer: ESMO Clinical Practice Guidelines For Diagnosis, Treatment and Follow-UpDrogoman MarianNo ratings yet
- A Rare Case of The Urinary Bladder: Small Cell CarcinomaDocument3 pagesA Rare Case of The Urinary Bladder: Small Cell CarcinomaMuhammad MaulanaNo ratings yet
- NLR Marker for Papillary Thyroid MicrocarcinomasDocument6 pagesNLR Marker for Papillary Thyroid MicrocarcinomasagusNo ratings yet
- Patented Biomarkers For The Early Detection of Ovarian CancerDocument9 pagesPatented Biomarkers For The Early Detection of Ovarian CancerHanny TanzilNo ratings yet
- Molecular Profiling in Muscle-Invasive Bladder Cancer: More Than The Sum of Its PartsDocument11 pagesMolecular Profiling in Muscle-Invasive Bladder Cancer: More Than The Sum of Its PartsJoel ChávezdrumsNo ratings yet
- Histopathological Description of Testis Carcinoma and Therapy in Patients at Dr. Hasan Sadikin General Hospital During 2017-2020 REV 31 - 08Document15 pagesHistopathological Description of Testis Carcinoma and Therapy in Patients at Dr. Hasan Sadikin General Hospital During 2017-2020 REV 31 - 08Titus RheinhardoNo ratings yet
- Full TextDocument6 pagesFull Textpqp2303No ratings yet
- 1078 0432.CCR 14 0442.fullDocument12 pages1078 0432.CCR 14 0442.fullAndrea KamóNo ratings yet
- 45 Siddaganga EtalDocument4 pages45 Siddaganga EtaleditorijmrhsNo ratings yet
- Thyroid Diseases HistopathologyDocument6 pagesThyroid Diseases HistopathologyUmaieyaal AnnarajahNo ratings yet
- Ovarian Cysts and Tumors in Infancy and Childhood: Riginal RticleDocument4 pagesOvarian Cysts and Tumors in Infancy and Childhood: Riginal RticleIwan Budianto HadiNo ratings yet
- Rapid On-site Evaluation (ROSE): A Practical GuideFrom EverandRapid On-site Evaluation (ROSE): A Practical GuideGuoping CaiNo ratings yet
- Upper Tract Urothelial CarcinomaFrom EverandUpper Tract Urothelial CarcinomaShahrokh F. ShariatNo ratings yet
- Attitude and Perceptions of University Students in Zimbabwe Towards HomosexualityDocument5 pagesAttitude and Perceptions of University Students in Zimbabwe Towards HomosexualityInternational Organization of Scientific Research (IOSR)No ratings yet
- Socio-Ethical Impact of Turkish Dramas On Educated Females of Gujranwala-PakistanDocument7 pagesSocio-Ethical Impact of Turkish Dramas On Educated Females of Gujranwala-PakistanInternational Organization of Scientific Research (IOSR)No ratings yet
- "I Am Not Gay Says A Gay Christian." A Qualitative Study On Beliefs and Prejudices of Christians Towards Homosexuality in ZimbabweDocument5 pages"I Am Not Gay Says A Gay Christian." A Qualitative Study On Beliefs and Prejudices of Christians Towards Homosexuality in ZimbabweInternational Organization of Scientific Research (IOSR)No ratings yet
- Investigation of Unbelief and Faith in The Islam According To The Statement, Mr. Ahmed MoftizadehDocument4 pagesInvestigation of Unbelief and Faith in The Islam According To The Statement, Mr. Ahmed MoftizadehInternational Organization of Scientific Research (IOSR)No ratings yet
- A Review of Rural Local Government System in Zimbabwe From 1980 To 2014Document15 pagesA Review of Rural Local Government System in Zimbabwe From 1980 To 2014International Organization of Scientific Research (IOSR)No ratings yet
- An Evaluation of Lowell's Poem "The Quaker Graveyard in Nantucket" As A Pastoral ElegyDocument14 pagesAn Evaluation of Lowell's Poem "The Quaker Graveyard in Nantucket" As A Pastoral ElegyInternational Organization of Scientific Research (IOSR)No ratings yet
- Assessment of The Implementation of Federal Character in Nigeria.Document5 pagesAssessment of The Implementation of Federal Character in Nigeria.International Organization of Scientific Research (IOSR)No ratings yet
- The Role of Extrovert and Introvert Personality in Second Language AcquisitionDocument6 pagesThe Role of Extrovert and Introvert Personality in Second Language AcquisitionInternational Organization of Scientific Research (IOSR)No ratings yet
- Edward Albee and His Mother Characters: An Analysis of Selected PlaysDocument5 pagesEdward Albee and His Mother Characters: An Analysis of Selected PlaysInternational Organization of Scientific Research (IOSR)No ratings yet
- A Proposed Framework On Working With Parents of Children With Special Needs in SingaporeDocument7 pagesA Proposed Framework On Working With Parents of Children With Special Needs in SingaporeInternational Organization of Scientific Research (IOSR)No ratings yet
- Comparative Visual Analysis of Symbolic and Illegible Indus Valley Script With Other LanguagesDocument7 pagesComparative Visual Analysis of Symbolic and Illegible Indus Valley Script With Other LanguagesInternational Organization of Scientific Research (IOSR)No ratings yet
- Women Empowerment Through Open and Distance Learning in ZimbabweDocument8 pagesWomen Empowerment Through Open and Distance Learning in ZimbabweInternational Organization of Scientific Research (IOSR)No ratings yet
- Relationship Between Social Support and Self-Esteem of Adolescent GirlsDocument5 pagesRelationship Between Social Support and Self-Esteem of Adolescent GirlsInternational Organization of Scientific Research (IOSR)No ratings yet
- The Impact of Technologies On Society: A ReviewDocument5 pagesThe Impact of Technologies On Society: A ReviewInternational Organization of Scientific Research (IOSR)100% (1)
- Topic: Using Wiki To Improve Students' Academic Writing in English Collaboratively: A Case Study On Undergraduate Students in BangladeshDocument7 pagesTopic: Using Wiki To Improve Students' Academic Writing in English Collaboratively: A Case Study On Undergraduate Students in BangladeshInternational Organization of Scientific Research (IOSR)No ratings yet
- The Lute Against Doping in SportDocument5 pagesThe Lute Against Doping in SportInternational Organization of Scientific Research (IOSR)No ratings yet
- Importance of Mass Media in Communicating Health Messages: An AnalysisDocument6 pagesImportance of Mass Media in Communicating Health Messages: An AnalysisInternational Organization of Scientific Research (IOSR)No ratings yet
- Transforming People's Livelihoods Through Land Reform in A1 Resettlement Areas in Goromonzi District in ZimbabweDocument9 pagesTransforming People's Livelihoods Through Land Reform in A1 Resettlement Areas in Goromonzi District in ZimbabweInternational Organization of Scientific Research (IOSR)No ratings yet
- Role of Madarsa Education in Empowerment of Muslims in IndiaDocument6 pagesRole of Madarsa Education in Empowerment of Muslims in IndiaInternational Organization of Scientific Research (IOSR)No ratings yet
- Beowulf: A Folktale and History of Anglo-Saxon Life and CivilizationDocument3 pagesBeowulf: A Folktale and History of Anglo-Saxon Life and CivilizationInternational Organization of Scientific Research (IOSR)No ratings yet
- An Exploration On The Relationship Among Learners' Autonomy, Language Learning Strategies and Big-Five Personality TraitsDocument6 pagesAn Exploration On The Relationship Among Learners' Autonomy, Language Learning Strategies and Big-Five Personality TraitsInternational Organization of Scientific Research (IOSR)No ratings yet
- Classical Malay's Anthropomorphemic Metaphors in Essay of Hikajat AbdullahDocument9 pagesClassical Malay's Anthropomorphemic Metaphors in Essay of Hikajat AbdullahInternational Organization of Scientific Research (IOSR)No ratings yet
- Human Rights and Dalits: Different Strands in The DiscourseDocument5 pagesHuman Rights and Dalits: Different Strands in The DiscourseInternational Organization of Scientific Research (IOSR)No ratings yet
- Substance Use and Abuse Among Offenders Under Probation Supervision in Limuru Probation Station, KenyaDocument11 pagesSubstance Use and Abuse Among Offenders Under Probation Supervision in Limuru Probation Station, KenyaInternational Organization of Scientific Research (IOSR)No ratings yet
- Designing of Indo-Western Garments Influenced From Different Indian Classical Dance CostumesDocument5 pagesDesigning of Indo-Western Garments Influenced From Different Indian Classical Dance CostumesIOSRjournalNo ratings yet
- A Study On The Television Programmes Popularity Among Chennai Urban WomenDocument7 pagesA Study On The Television Programmes Popularity Among Chennai Urban WomenInternational Organization of Scientific Research (IOSR)No ratings yet
- Design Management, A Business Tools' Package of Corporate Organizations: Bangladesh ContextDocument6 pagesDesign Management, A Business Tools' Package of Corporate Organizations: Bangladesh ContextInternational Organization of Scientific Research (IOSR)No ratings yet
- Motivational Factors Influencing Littering in Harare's Central Business District (CBD), ZimbabweDocument8 pagesMotivational Factors Influencing Littering in Harare's Central Business District (CBD), ZimbabweInternational Organization of Scientific Research (IOSR)No ratings yet
- Micro Finance and Women - A Case Study of Villages Around Alibaug, District-Raigad, Maharashtra, IndiaDocument3 pagesMicro Finance and Women - A Case Study of Villages Around Alibaug, District-Raigad, Maharashtra, IndiaInternational Organization of Scientific Research (IOSR)No ratings yet
- Pathology Course Audit-3Document26 pagesPathology Course Audit-3Joana Marie PalatanNo ratings yet
- BDD Sylabus 2022-2023Document11 pagesBDD Sylabus 2022-2023Adway KNo ratings yet
- Aggc 2022 Manuscript 3Document2 pagesAggc 2022 Manuscript 3api-636941880No ratings yet
- Prostate Cancer - Risk Stratification and Choice of Initial Treatment - UpToDateDocument30 pagesProstate Cancer - Risk Stratification and Choice of Initial Treatment - UpToDateVictoria KeitelNo ratings yet
- Prostate CancerDocument12 pagesProstate CancerSaloni PatelNo ratings yet
- Prostate Cancer, Version 2.2019: NCCN Clinical Practice Guidelines in OncologyDocument27 pagesProstate Cancer, Version 2.2019: NCCN Clinical Practice Guidelines in OncologyHendik RiawanNo ratings yet
- Vadina 1Document38 pagesVadina 1api-3702141No ratings yet
- Miniguia de EstudosDocument6 pagesMiniguia de EstudosMaykom LiraNo ratings yet
- Prostate Cancer: Detection, Diagnosis and TreatmentDocument42 pagesProstate Cancer: Detection, Diagnosis and TreatmentMegawati Abubakar100% (1)
- Prostate EMEDICINEDocument14 pagesProstate EMEDICINESan Phạm ĐìnhNo ratings yet
- A Neutrosophic Cubic Hesitant Fuzzy Decision Support System, Application in The Diagnosis and Grading of Prostate CancerDocument20 pagesA Neutrosophic Cubic Hesitant Fuzzy Decision Support System, Application in The Diagnosis and Grading of Prostate CancerScience DirectNo ratings yet
- Carcinoma of Prostate: Dr. Saadat Hashmi Consultant UrologistDocument48 pagesCarcinoma of Prostate: Dr. Saadat Hashmi Consultant UrologistMuhammad ArsalNo ratings yet
- Prostate TumorsDocument17 pagesProstate TumorsElian Jesús JimenezNo ratings yet
- Genes Dev.-2010-Shen-1967-2000Document35 pagesGenes Dev.-2010-Shen-1967-2000Vanessa Anton MuñozNo ratings yet
- Prostate Cancer: Presented By, Denna Benny Roll. No:21 3 Year B. SC NursingDocument58 pagesProstate Cancer: Presented By, Denna Benny Roll. No:21 3 Year B. SC NursingSamuel LalNo ratings yet
- MD Final Year Exams May 2018 Systemic Pharmacology PaperDocument15 pagesMD Final Year Exams May 2018 Systemic Pharmacology PaperdentsavvyNo ratings yet
- PROSTATE CANCER PPT - OdpDocument20 pagesPROSTATE CANCER PPT - OdpCharissa Magistrado De LeonNo ratings yet
- CA Prostate by Dr. Musaib MushtaqDocument71 pagesCA Prostate by Dr. Musaib MushtaqDr. Musaib MushtaqNo ratings yet
- Study Protocol of A Randomised Controlled Trial of Prostate Radiotherapy in High-Risk and Node-Positive Disease Comparing Moderate and Extreme Hypofractionation (PRIME TRIAL)Document8 pagesStudy Protocol of A Randomised Controlled Trial of Prostate Radiotherapy in High-Risk and Node-Positive Disease Comparing Moderate and Extreme Hypofractionation (PRIME TRIAL)William trincaNo ratings yet
- Prostate CarcinomaDocument42 pagesProstate CarcinomaWhydia Wedha SutedjaNo ratings yet
- Haroon RashidDocument50 pagesHaroon RashidSaayk HabibNo ratings yet
- PSA Level and Gleason Score in Predicting The Stage of Newly Diagnosed Prostat CancerDocument6 pagesPSA Level and Gleason Score in Predicting The Stage of Newly Diagnosed Prostat CancergumNo ratings yet
- Prostate Cancer Between Prognosis and Adequate/proper TherapyDocument8 pagesProstate Cancer Between Prognosis and Adequate/proper TherapyGabriel NguyenNo ratings yet
- Nejmoa1113162 AppendixDocument35 pagesNejmoa1113162 AppendixayuannisahusnaNo ratings yet
- Artifi Cial Intelligence in Cancer Research and Precision MedicineDocument17 pagesArtifi Cial Intelligence in Cancer Research and Precision MedicineCristina ViaplanaNo ratings yet
- Prostate CancerDocument58 pagesProstate CancerIsaac MwangiNo ratings yet
- Urology: Diseases of The Genitourinary System: ProstateDocument41 pagesUrology: Diseases of The Genitourinary System: ProstatepetoeditNo ratings yet
- Advanced Prostate Cancer Guide 2009Document133 pagesAdvanced Prostate Cancer Guide 2009Mochammad Adam EldiNo ratings yet
- Portfolio Clinical Case Study 2Document29 pagesPortfolio Clinical Case Study 2api-277136509No ratings yet
- Ijsrp p11558Document5 pagesIjsrp p11558Zuhri mardiahNo ratings yet