Professional Documents
Culture Documents
PN21 Health and Healing - Pre-Class Activities - Test 2 PDF
Uploaded by
Rachel HomesOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
PN21 Health and Healing - Pre-Class Activities - Test 2 PDF
Uploaded by
Rachel HomesCopyright:
Available Formats
PN2 Health and Healing Test #2
Unit 2: Package 6 Antonio Colangelo (COPD)
About Antonio Colangelo:
72 year old
male
Italian
has been admitted to acute care medical unit from ER accompanied with his wife
admitting dx: COPD
Observations:
often speaks to his wife in a loud and what appears to the nurse to be an angry manner during nursing hx (as a
nurse - question this behaviour: hard of hearing; frustration over disease, etc?)
Hx:
worked with asbestos (***read up on) for many years before his retirement seven years ago
smoked for 40 years a package of cigarettes/day; quit 5 years ago
reveals that he has taken puffer for his bad chest (client teaching on why he is taking puffers and proper use;
what do you mean by bad chest?)
indicates that he has been SOBOE for several years
frequent productive cough and recently feet have been swelling to the point that his shoes have become
uncomfortable to wear
Need to know:
medications and why he has been prescribed the meds
types of tests he has had to dx his condition
precipitating factors (stress, anger, exertion, environmental factors)
support systems in place; what is lacking (allows nurse to make referrals; direct toward resources)
understanding of disease (directs client teaching)
Overview:
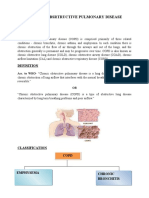
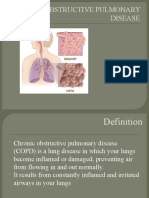
COPD: a respiratory disorder largely caused by smoking; characterized by progressive, partially reversible airflow
obstruction, systemic manifestations, and increasing frequency and severity of exacerbations (Lewis, 2010). Inability to
exhale.
Chronic Bronchitis: the presence of chronic productive cough for 3 months in a 2 successive years in a client in whom
other causes of chronic cough have been excluded (Lewis, 2010).
Emphysema: an abnormal and permanent enlargement of the airspaces distal to the terminal bronchioles, accompanied
by destruction of their walls and without obvious fibrosis (Lewis, 2010).
Pathophysiology:
COPD
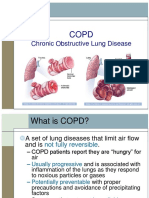
What's It's Comprised Of? Usually Chronic Bronchitis and/or Emphysema. Many COPD sufferers may also have
an asthma component.
Chronic Bronchitis affects the lining inside your bronchial tubes. They get irritated and fill with mucus resulting
in a wet cough. The mucus plugs or blocks the tubes marking it harder for you to breathe.
With emphysema the tiny hair like air sacs called "alveoli" get irritated and stiff making it hard to transfer
oxygen and carbon dioxide. The end result is shortness of breath.
What Does It Do? It blocks and narrows the airways and inflames the lungs causing obstruction.
What Are the Symptoms or Characteristics? The common characteristics of COPD is trouble breathing (shortness of
breath aka SOB) and/or a cough lasting 3 or more months. You may have noticed you have to stop and catch your breath
more, or perhaps you don't exercise as much because you've always thought you were "out of shape". Perhaps you are, or
you were, a smoker and you have developed what many refer to as a "smoker's cough".
Chronic Bronchitis: pathological changes in the lung consist of:
hyperplasia of mucus-secreting glands in the trachea and bronchi
increases in goblet cells
disappearance of cilia
PN2 Health and Healing Test #2
chronic inflammatory changes and narrowing of small airways
o
chronic inflammation is the primary pathological mechanism involved in causing the changes
characteristic of chronic bronchitis; it causes vasodilation, congestion and mucosal edema.
o
hyperplasia, inflammatory swelling, and excess thick mucus cause narrowing of the airway lumen and
result in diminished airflow.
altered function of alveolar macrophages, leading to increased bronchial infections
Hypoxemia and hypercapnia develop more frequently in chronic bronchitis than in emphysema. Diminished respiratory
drive with a tendency to hypoventilate and retain CO2 result in many areas of the lung to be not ventilated causing a
diffusion of O2 to occur.
Coughing is stimulated by retained mucus that cannot adequately be removed because of the decrease in cilia and
mucociliary activity. Bronchospasm may also develop adding to the airway resistance, resulting in further increased work
of breathing and impaired gas exchange.
Emphysema: structural changes in emphysema include:
hyperinflation of alveoli
destruction of alveolar walls
destruction of alveolar capillary walls
narrowed, indirect, small airways
loss of lung elasticity
There are two types of emphysema:
Centrilobular:
primary involvement is the central part of the lobule. Respiratory bronchioles enlarge, the walls are destroyed and
the bronchioles become confluent.
Panlobular:
involves distension and destruction of the whole lobule (usually in persons with AAT [a1-antitrypsin]
deficiency). Respiratory bronchioles, alveolar ducts and sacs, and alveoli are affected. There is a progressive loss
of lung tissue and decreased alveolar-capillary surface areas and in some bullae (large cystic areas) develop.
Differences between chronic bronchitis and emphysema
Bronchitis
inflammation, or irritation, in the bronchioles of the
lungs
this irritation causes an increased amount of heavy
mucus in the lungs that over time, interferes with
breathing
body responds to this mucus by producing a cough in
an attempt to clear the airways
mucus is so abundant and thick, it is often difficult
for a person with chronic bronchitis to expel it
thick mucus makes perfect habitat for bacteria
Manifestations
Onset
Cough
General Appearance
Auscultation
Emphysema
permanent enlargement of the airways in lungs
it is accompanied by destruction of the walls of the
alveoli
when the alveoli are destroyed, it makes it difficult
for the person with emphysema to breathe
gradual onset
Chronic Bronchitis
- 3 months to 2 consecutive years
with symptoms
- chronic productive cough (constant
cough)
- SOB
- coughing
- spitting up of sputum/phlegm
- stridor
- crackles
Emphysema
- gradual onset
- minimal cough with none/small
amount of sputum
- SOB
- wheezing
- chest breathing
- barrel shaped chest
- fatigue
- weight loss
- swollen fingers (clubbing)
- no adventitious sounds auscultated
PN2 Health and Healing Test #2
IncidencePrevalence of COPD in Canada: (http://www.copdcanada.ca/women_and_copd.htm)
COPD is currently the 4th leading cause of death.
In Canada, COPD is the fourth most common cause of hospitalization among men and the sixth most
common cause of hospitalization among women.
Affects women more than men.
o
Men's numbers for COPD are dropping, women's are increasing.
According to Canada's Public Health Agency, 4.8 % of women over 35 suffer from COPD, compared to 4.3% of
the males.
Risk Factors:
cigarette smoking
occupational chemicals and dust
infection
heredity
Complications:
Cor Pulmonale:
o
Hypertrophy of the right side of the heart, with or without heart failure, resulting from pulmonary
hypertension.
Acute Exacerbations of COPD:
o
(AECOPD) acute exacerbations are the most frequent cause of medical visits, hospitalizations, and death
for people with COPD.
o
AECOPD is a sustained worsening of dyspnea, cough or sputum production leading to an increased use
of maintenance medications or supplementation with additional medications.
Acute Respiratory Failure:
o
AECOPD is the most common event leading to acute respiratory failure in COPD.
Depression, Anxiety and Panic:
o
People with COPD experience higher rates of depression, anxiety and panic.
o
Rates of depression range from: 20-50% and is related to disease severity.
Clinical Manifestations:
cough
sputum production
dyspnea
history of smoking or exposure
prolonged expiratory phase of respiration, wheezes of decreased breath sounds
hypoxemia (over time)
Symptoms: (Med-Surg)
anorexia, weight loss or gain, early satiety, difficulty eating
decreased level of activity and ability to perform ADL`s
constipation, gas bloating
headache, loss of memory, inability to concentrate
fatigue, insomnia, depression, anxiety, panic
Mr. Colangelo: clinical manifestations
dyspnea on exertion
productive cough
peripheral edema
Mr. Colangelo: risk factors
worked with asbestos
smoked a package of cigarettes a day for 40 years
environment
o
(Hamilton has more risk factors; air quality or farming areas at higher risk)
PN2 Health and Healing Test #2
Doctors orders for Mr. Colangelo are as follow:
1. Furosemide 40 mg PO daily
2. Salbutamol 1 cc in 1 cc normal saline via nebulizer q4h PRN
3. Advair 250 mcg. 1 puff BID
4. sputum for C&S and then begin Ampicillin 500 mg IV q6h
5. oxygen 3 L via nasal prongs
6. vital signs and oxygen saturation q4h
7. weigh daily
8. NAS diet
9. IV NS lock
10. arterial blood gasses stat
11. CBC, electrolyte, BUN, creatinine
12. Pulmonary Functioning Test
Pulmonary function testing:
Is performed to assess lung function and determine the degree of damage to the lungs.
Tests can be used for screening for the existence of lung diseases determining the patient's condition prior to
surgery to assess the risk of respiratory complications after surgery.
Evaluating the ability for a patient to be weaned from a ventilator.
Assessing the progression of lung disease and the effectiveness of treatment.
The most common test is the spirometry which requires patient, after all air has been expelled, to inhale deeply.
o This manoeuvre is then followed by a rapid exhalation so that all the air is exhausted from the lungs.
How to Prepare for the Test
Do not eat a heavy meal before the test.
Do not smoke, drink caffeine, or use bronchodilators for 4 - 6 hours before the test.
You may have to breathe in medication before the test.
Forced vital capacity (FVC):
The amount of air which can be forcibly exhaled from the lungs after taking the deepest breath possible.
Forced expiratory volume in the first second (FEV1):
The amount of air which can be forcibly exhaled from the lungs in the first second of a forced exhalation.
ABG: (http://nursingcrib.com/medical-laboratory-diagnostic-test/arterial-blood-gas-analysis/)
Purpose
To evaluate the efficiency of pulmonary gas exchange and function of kidneys.
To assess the integrity of the ventilatory control system.
To determine the acid/base level of the blood.
To monitor respiratory therapy.
Procedure
Patient Preparation
1. Explain the arterial blood gas analysis evaluates how well the lungs are delivering the oxygen to the blood and
eliminating carbon dioxide.
2. Tell the patient that the test requires a blood sample.
3. Explain to the patient, who will perform the arterial puncture, when it will occur, and where the puncture site will
be; radial, brachial, or femoral artery.
4. Inform the patient that he may not need to restrict food and fluids.
5. Instruct the patient to breathe normally during the test, and warn him that he may experience a brief cramping or
throbbing pain at the puncture site.
Implementation
1. Use a heparinized blood gas syringe to draw the sample.
2. Perform an arterial puncture or draw blood from an arterial line.
3. Eliminate air from the sample, place it on ice immediately, and prepare to transport for analysis. Sample on ice
must be analysed with in 1 hour.
4. Note the flow rate of oxygen therapy and method of delivery.
5. Note the patients rectal temperature.
PN2 Health and Healing Test #2
Nursing Interventions
1. After applying pressure to the puncture site for 3 to 5 minutes and when bleeding has stopped, tape a gauze pad
firmly over it.
2. If the puncture site is on the arm, dont tape the entire circumference because this may restrict circulation.
3. If the patient is receiving anticoagulants or has a coagulopathy, apply pressure to the puncture site longer than 5
minutes if necessary.
4. Monitor vital signs and observe for signs of circulatory impairment.
Interpretation
Normal Results
Resource: Hamilton Health Sciences (HHSC)
Benefits of oxygen therapy:
Administering supplemental O2 raises the partial pressure of O2 (PO2) in inspired air. O2 is usually
administered to treat hypoxemia caused by respiratory disorders such as COPD, AECOPD, cor pulmonale,
pneumonia, atelectasis, and lung cancer.
Supplemental oxygen helps prevent heart failure in people with severe lung disease, improves sleep, mood,
mental alertness and stamina and allows individuals to carry out normal, everyday functions.
(90% O2 sats is acceptable for COPD patients); dont give more than O2 reading of 90% when giving Oxygen
Therapy
Mr. Colangelo limited to 3Lmin. Why?
low O2 triggers COPD patients to breath (in healthy individual, CO2 triggers the patient to breath)
chronic retainers of CO2 b/c chemoreceptors desensitized to CO2
giving O2 tells pt they dont have to breath
if you give too much O2 (3L/minute) it will tell Mr. Colangelos body to stop breathing and cause a toxic buildup of CO2 in the blood which can be fatal
Procedure for obtaining a sputum sample for C&S:
Sterile specimen cup:
o
Have the patient drink plenty of fluids on the evening before the day of the test to boost sputum
production, have patient rinse mouth with water so that the sputum isnt contaminated with bacteria.
o
Have patient deep breath and cough, expectorating sputum into sterile container.
o
Continue until you`ve collected 15mL of sputum.
o
Send specimen for testing, do not refrigerate.
Nasotracheal suctioning:
o
First assess the patient's cardiac and respiratory status to be sure he can tolerate procedure. Instruct
patient to slightly tilt head back.
o
Dip tip of catheter into lubricant and carefully put it into one of nares.
o
When tip of catheter reaches the back of throat, the patient may cough.
o
As pt coughs, quickly but gently advance the catheter into trachea.
o
Instruct patient to take several deep breaths through the mouth to ease insertion.
o
Have pt give a deep cough, and apply suction at a pressure of 100 150 mm Hg for five to 10 seconds.
Reason for obtaining specimen prior to commencing ampicillin?
The ampicillin would alter the results of the pulmonary function test.
PN2 Health and Healing Test #2
Medications Ordered
Drug Name
Mechanism of Action
potent, locally acting
Advair
(fluticasone +
anti-inflammatory and
salmeterol)
immune modifier
/relaxes the smooth
muscles in the airway,
Classification:
corticosteroid/
resulting in
bronchodilator
bronchodilation
ampicillin
Classification:
anti-infective
aminopenicillins
bind to bacterial cell
wall, resulting in cell
death
salbutamol
(Ventolin)
via *nebulizer
Classification:
bronchodilators
adrenergics
relaxes the smooth
muscles in the airway,
resulting in
bronchodilation
pt taking to relieve
and prevent
bronchospasms in
COPD
Adverse Effects
headache
tremors
palpitations
tachycardia
abdominal pain
cough
seizures
pseudomembra
nous colitis
diarrhea
rashes
anaphylaxis
serum sickness
nervousness
restlessness
tremor
paradoxical
bronchospasm
(excessive use
of inhalers)
chest pain
palpitations
Nursing ResponsibilitiesHealth Teaching
may cause serum and urine glucose
should not be discontinued abruptly
monitor respiratory status and lung sounds
use only as prescribe; risk for oral infection
shake well before using
use BID
use 30-60 minutes before activity
caution pt not to use Advair for acute
symptoms; use bronchodilator for relief of
acute attacks
administer on an empty stomach 1hr before
or 2hr after meals with a full glass of water
may causeAST, ALT
may cause false-positive direct Coomb`s
test and urinary glucose
pt to notify Dr. if fever and diarrhea occur
do not take with oral contraceptives
assess lung sounds, pulse, BP
note amount, colour, character of sputum
observer for paradoxical bronchospasm
(wheezing); if condition occurs,
hold/discontinue medication
Nursing Diagnosis - research 3 and create individualized nursing care plan for Mr. Colangelo
Nursing Diagnosis
Interventions & Rationale
Ineffective airway
clearance r/t to expiratory
airflow obstruction,
ineffective cough, increased
mucous production,
decreased cilia, infection in
airway AEB by wheezes and
dyspnea (COPD)
Impaired gas exchange r/t
alveolar hypoventilation
AEB by headache on
awakening, abnormal PaCO2
45 mmHg and SaO2 < 90%
Disturbed sleep pattern r/t
dyspnea, depression, anxiety,
hypoxemia, and/or
hypercapnia, medication side
effects AEB insomnia,
lethargy, fatigue,
restlessness, irritability
orthopnea, or paroxysmal
nocturnal dyspnea
Facilitate deep breathing by sitting pt up to maximize use of diaphragm and
prolong expiratory phase.
Ensure adequate hydration (oral intake approx. 2-3Ld, humidified ambient air) to
liquefy secretions for easier expectoration.
Teach effective cough techniques to minimize airway collapse and enhance airway
clearance.
Assist with inhaled bronchodilator administration to facilitate clearance of retained
secretions.
Monitor respiratory and oxygenation status to assess need for intervention.
Teach pursed-lip breathing to prolong expiratory phase and slow respiratory rate.
Assist patient to assume position of comfort to maximize respiratory excursion.
Administer and teach appropriate use of bronchodilators to open airway.
Administer O2 when appropriate.
Identify usual sleep habits and elicit reasons for difficulty sleeping to provide
baseline data.
Monitor patients sleep pattern, and note physical circumstances that interrupt sleep
so appropriate interventions can be initiated.
Encourage exercise and activity during daylight hours to improve sleep at night.
Identify patient-specific methods of relaxation, and teach patient relaxation
methods to foster sleep.
Instruct patient in maintaining an environment conductive to rest.
Observe for signs and symptoms of sleep apnea such as frequent awakenings at
night, excessive daytime sleepiness, or snoring or gasping for air so appropriate
diagnostic testsinterventions can be initiated.
Teach avoidance of alcoholic beverages, caffeine products or other stimulants
before bedtime to reduce interference with sleep.
PN2 Health and Healing Test #2
After a few days in hospital, Mr. Colangelo seems to be improving, however, on the third day after his admission, you
learn that he has considerable increase in his ankle edema, his cough has increased and he has some inspiratory crackles
and expiratory wheezes throughout both lungs. After doing a complete cardiorespiratory assessment, you notice the
doctor; who suspecting Cor Pulmonale:
A Registered Nurse now has assumed primary responsibility for MR. Colangelos care. You will be working
collaboratively with the RN to provide comprehensive care for this client.
New orders are as follows:
1. stat chest x-ray
2. Furosemide 120 mg IV stat
3. increase daily Furosemide to 60 mg PO daily
4. Potassium Chloride (Slow K 8mEq) 2 tabs PO BID
5. vital signs q2h
6. Digoxin 0.5 mg IV stat followed by 0.25mg X2 q8h and then Digoxin 0.25mg PO daily
7. insert an indwelling catheter stat
8. measure urinary output q2h
Cor Pulmonale:
Late manifestation of COPD with poor prognosis; approximately 40% of patients will get cor pulmonale
Hypertrophy of the right side of the heart, with/without heart failure, resulting from pulmonary hypertension
Pulmonary hypertension is caused primarily by constriction of the pulmonary vessels in response to alveolar
hypoxia, with acidosis further potentiating the vasoconstriction
S&S
o
exertional dyspnea
o
chronic productive cough; wheezing respirations
o
swelling of ankles/feet (peripheral edema)
o
tachypnea
o
tachycardia
o
decreased cardiac output
Cardiorespiratory Assessment:
Subjective Data:
Present health: assess experience of dyspnea (with activity and at rest) and cough. If cough is productive
determine colour, consistency, and quantity of secretions
Past health history: long-term exposure to chemical pollution, respiratory irritants, occupational fumes, and
dust; history and frequency of respiratory infections; previous hospitalizations related to breathing and cardiac
problems; smoking exposure (pack-years, exposure to secondary smoke), personal and family history of
respiratory and cardiac conditions
Medications: use and duration of supplemental O2, bronchodilators, anticholinergics, corticosteroids, antibiotics,
OTC drugs, complementary therapies; effectiveness of bronchodilators and experience of side effects
Objective Data:
General:
height, weight, BMI, distress, increased work of breathing, use of compensatory mechanisms for breathing,
anxiety, depression, LOC
Integumentary:
cyanosis, poor skin turgor, thin skin, easy bruising, peripheral edema
Respiratory:
rapid, shallow breathing; accessory muscle use; inability to speak; prolonged expiratory phase; pursed-lip
breathing; wheezing, crackles, diminished breath sounds; chest excursion and diaphragmatic movement; dull
chest sounds on percussion, dyspnea, pulse oximetry
Cardiovascular:
tachycardia, dysrhythmias, jugular vein distension, right-sided S3 (cor pulmonale), edema
Gastrointestinal:
ascites, hepatomegaly (cor pulmonale)
Musculoskeletal:
muscle atrophy, anterior-posterior diameter (barrel-chest)
PN2 Health and Healing Test #2
Orthopneic Position
form of dyspnea in which the pt can breathe comfortably only when standing or sitting erect
Nursing Responsibilities
o
daily weight to assess hydration status
o
measuring intake and output
o
when: weigh in the morning
o
how: standing position
o
why: to prevent risk factors by weight gain such as HTN
o
If pt gains 1 Kg, add 1000mL of fluid
o
when charting, it is important to document pt weight gain/loss
o
DAR chart
Why has the RN assumed primary responsibility for the case of Mr. Colangelo?
Both nurses and employers make client assignment decisions based on the characteristics of the nurse, client
population and environment.
The three factor framework (College of Nurses of Ontario) takes into account the nurses knowledge, skill and
judgment; the clients health condition, care needs and situation; as well as the environment in which the care is
being provided, including the specific supports it provides.
Mr. Colangelos care has become highly complex:
o
multiple issues which are overlapping
o
requires frequent monitoring and/or reassessment b/c condition is fluctuating
o
client is at risk for negative outcome
o
may not me enough supports in place (such as a social worker or family involvement)
Drug Name
furosemide
(Lasik)
Classification:
diuretic
loop diuretic
potassium
chloride (Slow
K)
Classification:
electrolyte
replacement
digoxin
(Lanoxin;
Digitalis)
Classification:
antiarrhythmic,
inotropic
digitalis
glycosides
Action
Inhibits reabsorption
of sodium + chloride
by causing sodium to
be excreted in the
urinewhere salt
goes, water follows
Pt has edema
For treatment/
prevention of
potassium depletion
Digoxin depletes
potassium; furosemide
can deplete potassium
reduces contractions
of the heart therefore
better O2 distribution
tx for cor pulmonale
(hypertrophy of right
sided heart
with/without HF;
increases contraction
of the heart thus better
O2 distribution
Adverse Effects
dehydration
hypokalemia
hyponatremia
hypovolemia
orthostatic
hypotension
arrhythmias
abdominal pain
diarrhea
flatulence
nausea
vomiting
arrhythmias
bradycardia
anorexia
nausea
vomiting
fatigue
Nursing ResponsibilitiesHealth Teaching
monitor electrolytes, renal and hepatic
function, serum glucose
caution pt to change positions slowly to
minimize orthostatic hypotension
give early in the day to prevent nocturia
measure and record weight for fluid
change and report loss/gain; >1.5KG day
assess for hypokalemia
assess for hyperkalemia
monitor serum potassium, renal function,
serum bicarbonate, pH
instruct pt not to use salt substitutes
containing potassium
monitor apical pulse for 1 full min; do not
administer if <60bpm in adults; teach pt
to monitor own pulse at home daily and
report abnormal to physician stat
evaluate serum electrolyte levels
(especially potassium, magnesium, and
calcium) and renal and hepatic functions
monitor for signs of toxicity and teach pt
symptoms:
o
abdominal pain
o
GI upset
o
visual disturbances
o
bradycardia
o
arrhythmias
risk for falls in elderly
adhere to medication regimen at all times;
dont double dose
encourage pt to carry identification
describing disease process and medication
regimen
PN2 Health and Healing Test #2
Discharge health teaching and health promotion:
Overall goals for a patient with COPD include:
The prevention of disease progression
The patient being able to perform ADLs
Relief from breathlessness and other respiratory symptoms
Improvement in exercise tolerance
The prevention and treatment of exacerbations
Improved overall quality of life
The reduction in premature mortality
RNAOs best practice guideline helping people quit smoking is available at
http://rnao.ca/bpg/guidelines/integrating-smoking-cessation-daily-nursing-practice
avoiding or controlling exposure to occupational and environmental pollutants and irritants
good handwashing techniques, avoid sharing food and drinks, keep hands away from their nose, mouth and ears
influenza and pneumococcal pneumonia vaccinations are recommended
Patient and Family Teaching Guide:
Non-pharmacological Therapy:
Breathing exercises:
o
Pursed-lip breathing
o
Diaphragmatic breathing
o
Controlled huff coughing
Relaxation techniques
Energy conservation techniques
Regular exercise
Smoking cessation
Medications:
Anticholinergics
Corticosteroids
Antibiotics
2-adrenergic agonists
methylxanthines
review medication schedule for indications for use and watch for side effects
flu shot annually
Correct use of inhalation devices:
Metered-dose inhalers with and without spacers
Dry powder inhalers
Rinse mouth out after inhalers
Use bronchodilator first, then corticosteroid (5 minutes between each inhaler; and 2 minutes between each puff of
same inhaler)
Clean outside of inhalers with warm water and allow to air dry
keep track of inhalers on MDI
Home Oxygen:
Explain need for O2
Explain equipment and rationale for use
Guide for home O2 and ambulatory use
Care of oxygen equipment
Psychosocial and Emotional issues:
Concerns about interpersonal relationships: dependency, intimacy
Depression
Anxiety and panic
Support and rehabilitation groups
COPD Management plan:
Focus on self-management
Need for a written self-management plan
PN2 Health and Healing Test #2
10
Monitoring signs and symptoms
Reporting changes in symptoms
Causes of flare-ups
Recognition of signs and symptoms of respiration infection, heart failure
Yearly follow-up
Healthy Nutrition:
Potassium enriched (due to loss via medications: Diuretics and Digoxin); Dietician ordered diet if on Slow K (to
prevent excess potassium intake/hyperkalemia)
Na restricted
cold foods best
5-6 small meals/day
avoid gassy foods
increased protein
Increased fluid: 3L/day to liquefy secretions between meals
Lifestyle:
rest before meals
use Ventolin before meals
walk
smoking cessation
conserve energy
use bronchodilator before sex (prophylaxis)
sex when breathing is easiest
refrain from strenuous activity of meals
dont assume dominate position
dont prolong foreplay
End-of-Life and Advance planning:
Identify concerns and preferences for end of life
Support problem solving, decision making, and planning
Mr. Colangelos COPD developed in part because of his cigarette smoking habit of 40 years and a nursing colleague
comments that she feels that Mr. Colangelo brought the disease on himself.
How do you feel about the comment? How would you respond to your colleague?
the nurse needs to keep her personal judgments, values, and beliefs separate from her job
was also brought on by exposure to asbestos via his job
there wasnt education about the dangers of smoking 45 years ago
smoking use to be an accepted practice; smoking was promoted in the media
the nurse should focus on the achievement of the patient quitting over 5 years ago
smoking is extremely addictive
PN2 Health and Healing Test #2
11
Unit 2 Package 7: Jessie Sinclair
(Diabetes/ CRF/Stroke/Afib)
Overview
About Jessie Sinclair:
72 year old female
aboriginal - 1st nation from Cayuga nation
window past 4 years
lives alone
1 daughter with 3 children (busy); lives in same town
Observations:
daughter and family constantly at her side; creating difficulty because they are constantly asking questions;
daughter doesnt want dialysis because mother has too much to deal with already
Hx:
HTN (past 15 years)
Diabetes Type 1 (past 15 years)
Atrial Fib (one episode, 5 years ago)
recent dx of chronic renal failure (renal insufficiency stage) r/t diabetic neuropathy
Family Hx -mother and 2 siblings: stroke; diabetes; HTN
Need to know:
S&S of:
o
Kidney (chronic)
o
HTN
o
Stroke
o
Diabetes
Tests to have done
o
CT scan/Cerebral Angiogram - look up nursing considerations
Tests to interpret
o
Blood work:
BUN
Creatinine
CBC
Platelets
Fasting BG
Electrolytes
Lipids
HbgA1C
Medications
o
Humulin R - sliding scale
o
Humulin 30/70 - 26 units QAM
o
Novolin R ge Toronto
o
Novolin 30/70
Recall Pathophysiology of Diabetes
a multisystem disease related to abnormal insulin secretion, impaired insulin action, or both
primarily a disorder of glucose metabolism related to absent or insufficient insulin supply or poor
utilization of the insulin that is available
Type 1
o
progressive destruction of pancreatic beta cells due to an autoimmune process
Type 2
o
insulin resistance - insulin receptors unresponsive to action of insulin, insufficient in number, or both
o
decreased insulin production over time - inappropriate glucose production by the liver
o
marked decrease in the ability of the pancreas to produce insulin
Incidence/prevalence of Diabetes within the First Nation people in Canada
First Nations, Inuit, and Metis are 3-5 times more likely than the general population to develop type 2 diabetes
PN2 Health and Healing Test #2
12
Clinical Manifestations of Type 1 and Type 2 Diabetes
Type 1 - 5-10% of diabetes
Characteristics
- most often occurs in people under 20
Age of Onset
- (peak onset 11-13yrs juvenile)
- lean body type
Typical Body Weight
- genetic disposition
Etiology/Risk Factors
- Gender: Male
Exposure to environmental factors (ex.
viral infections; pesticides)
- Autoimmune (Type A)
- Nonautoimmune (Type B)
- progressive destruction of pancreatic
Pathophysiology
beta cells due to an autoimmune and
genetic process in susceptible
individuals
- absent or minimal insulin production
- T cells are attacking beta cells; thereby
destroying the pancreas cells
- thirst (polydipsia)
Symptoms
- polyuria (frequent urination)
- polyphagia (excessive hunger)
- fatigue
- changes in visual acuity
- hx of recent and sudden weight loss
***S&S abrupt, but actual disease
process may be present for several years
- nutrition therapy essential
Treatment
***see below for more
- insulin required on a permanent basis
detail on treatment
Hypoglycemia
Anxiety, restlessness, nervousness, tremor
tingling in hands, feet, lips, or tongue
chills, cold sweats, cool, pale skin
confusion, difficulty in concentration
drowsiness, nightmares or trouble sleeping
excessive hunger, headache, irritability
nausea
tachycardia
weakness, unsteady gait
Interventions:
Conscious?
15 g of glucose in the form of glucose tablets
15 mL (3 teaspoons) or 3 packets of table sugar
dissolved in water
175 mL (3/4 cup) of juice or regular soft drink
6 Life Savers (1=2.5 g of carbohydrate)
15 mL (1 tablespoon) of honey
Unconscious?
IV glucose (50%) or glucagon
Wait 10 to 15 minutes, then check your blood
glucose again. If it is still low:
Treat again
If next meal is more than one hour away, or pt is
going to be active, eat a snack, such as a halfsandwich or cheese and crackers (something with
15 grams of carbohydrate and a protein source.)
Type 2 - 90% of diabetes
- usually occurs in people over 40 years
- 80-90% are overweight at time of dx
- obesity; lack of exercise; high fat foods
- increased BP, Fat levels
- ethnicity (Japanese, Native, African, Hispanic
- Gender: Female
- hyperlipidemia
- stress, gestational DM
insulin resistance - insulin receptors are
unresponsive to the action of insulin,
insufficient in number, or both
decreased insulin production over time inappropriate glucose production by the liver
Impaired use of glucose by the cells
- frequently none
- fatigue
- recurrent infections
- prolonged wound healing
- visual acuity changes
- painful peripheral neuropathy in the feet
- overweight
- gradual onset
- lifestyle change: diet and exercise
- oral hyperglycaemic agents usually beneficial
Hyperglycemia
3 Ps:
polyuria
polyphagia
polydipsia
confusion, drowsiness
flushed, dry skin
fruit-like breath odour
rapid, deep breathing (Kussmaul resps from acidosis)
acidosis
Interventions:
There are some specific algorithms used to manage
complications knowns as DKA and HHNKS in adults
and children.
Key principles involve the following:
o
Fluid rehydration to restore normal ECFV and
tissue perfusion
o
Correction of hyperglycemia by addressing
absolute or relative insulin deficiency
o
Resolution of ketoacidosis usually occurs
within insulin therapy and fluid rehydration
requires physicians attention
continuance of OHA or insulin as ordered; may need to
increase in dose (via IV infusion)
check blood glucose frequently; check urine for
ketones; record results
hourly drinking of fluids (flush glucose from blood)
IV fluids may be necessary
PN2 Health and Healing Test #2
13
Effect Diabetes can have on Mrs. Sinclairs neurologic, sensory, cardiovascular, renal, integumentary,
musculoskeletal and immune system (Med-Surg, 2010, p. 1364-1369)
Neurological
loss of sensation; muscular atrophy; weakness; decreased reflexes; pain; numbness and tingling (paresthesia)
loss of sensation, especially in feet/extremities which can lead to undetected injury and infection
Sensory
Retinopathy
Neuropathy
Nephropathy
decreased vision, smell, taste
diminished thirst
Cardiovascular
HTN due to fluid overload in intravascular because glucose acts as a sponge pulling water
CAD due to walls thickening; sclerosis - become blocked or occluded by plaque build-up/or damaged due to
damaging effects of high glucose in the blood
macrovascular damage to medium-large vessels leads to CAD because of scarring
microvascular changes in capillary beds - affect kidneys and retina
Renal
Nearly of all have chronic kidney disease and of those require dialysis/transplants
50% with Diabetes have chronic kidney problems
Microalbuminuria is an early sign of nephropathy
kidneys filtration mechanism is stressed allowing protein to leak into the urine
Integumentary
loss of pain perception
increased risk for infection; skin breakdown; slow to heal
dry
damage r/t insulin injections (lipodystrophy)
Musculoskeletal
muscle atrophy r/t sedentary lifestyle
earlier dx may effect bone growth; effects osteocyte activity
general aches and pains
Immune
poor circulation due to angiopathy (blood vessel disease) which can delay or prevent the immune response
impairment of WBC, particularly the neutrophils and monocytes
peripheral neuropathy (main delay detection of infection)
PN2 Health and Healing Test #2
14
Microvascular and Macrovascular complications of Diabetes
Micro
complications from thickening of blood vessels in response to conditions of chronic hyperglycemia
Mostly affects:
o
Eyes - Retinopathy: damage of blood vessels in retina
o
Kidneys - Nephropathy: damage to small blood vessels that supply the glomeruli of the kidney
o
Nerves - Neuropathy: nerve damage usually in the peripheral areas
Macro
Includes:
o
Cerebrovascular Disease
o
Cardiovascular Disease
o
Peripheral Vascular Ischemia
Define the following lab tests and results which would indicate diabetes is not well controlled: (Med-Surg. p. 1331;
CDA)
FPG normal: 4-6
Oral glucose tolerance: <11.1 mmol/L at 30 and 60 min,
and <7.8 mmol/L at 120 min
A1C normal: 4-6%; increased value indicates Diabetes is not well
controlled
Random normal: <11.1 mmol/L
Urine for Protein
help evaluate and monitor kidney function, and to help detect and diagnose early kidney damage and disease
the dipstick primarily measures albumin, the 24-hour urine protein test also may be ordered if a doctor suspects
that proteins other than albumin are being released
Serum cholesterol and triglyceride levels
close association between elevated levels of these parameters and the risk of arteriosclerosis/atherosclerosis later
leading to cardiovascular disease
Ophthalmologist to assess vision
check for signs of retinopathy
PN2 Health and Healing Test #2
15
Drug Therapy: Oral Antihyperglycemic Agents (OHAs) - Type 2 Diabetes
are not insulin, but they work to improve the mechanism by which insulin and glucose are produced and
used by the body
they encompass all of the oral medications for the management of blood glucose control
for any of the OHAs to be affective, the client must have some circulating endogenous insulin
Drug Name
metformin
Glucophage
Glucophage
XR
Classification:
oral antihyperglycemic
agent
biguanide
Route: Oral
Peak: 2-2.5 hrs
Duration: 10-16 hr
glyburide
(Diabeta)
Classification:
oral anti-hyperglycemic
agents
sulfonylureas
Micronized
Route - Oral
Onset - 1 hr
Peak - 2-3 hr
Duration - 12-24 hr
Nonmicronized
Route - Oral
Onset - 2-4 hr
Peak - 4 hr
Duration - 12-24 hr
Mechanism of
Action
inhibits hepatic
glucose
production
increases
peripheral
sensitivity to
insulin and
inhibits GI
absorption of
glucose
decreased glucose
in blood
adjunct to diet to
lower blood
glucose with:
Type 2 Diabetes
stimulates release
of insulin from
beta cells;
decrease
glycogenolysis
and
gluconeogenesis;
glimipramide may
improve
insensitivity in
tissues
adjunct to diet to
lower blood
glucose with:
Type 2 Diabetes
Adverse Effects
CNS:
Drowsiness
Tinnitus
Fatigue
Asthenia
Nervousness
Tremor
Insomnia
CV
Increased risk of CV
mortality
Endocrine
Hypoglycemia
lactic acidosis
GI
GI disturbances (not
constipation)
Metallic taste
Heme
Leukopenia
Thrombocytopenia
Anemia
Hypersensitivity
Allergic skin
reaction
Eczema
Pruritus
Erythema
Urticaria
Photosensitivity
Fever
Eosinophilia
Jaundice
Other
Blurred vision
*** assess for hypoglycemia at peak action of drug
Nursing ResponsibilitiesHealth Teaching
Assessment
risk of severe lactic acidosis; monitor
patient, and treat any suspicions of lactic
acidosis
monitor urine or serum glucose levels
frequently to determine effectiveness of
drug and dosage
Labs:
o Monitor CBC (baseline, q3mo)
during treatment
o Liver function tests (AST, LDH)
and renal tests (BUN, creatinine)
periodically during treatment
o Glucose
o A1c
Administration
give drug before breakfast
o if severe GI upset occurs, dose may
be divided and given before meals
assess for hypoglycemia at peak times
o sweating
o weakness
o dizziness
o anxiety
o tremors
o hunger
Health teaching
do not discontinue this medication
without consulting your health care
provider
teach how to monitor blood for glucose
and ketones as prescribed
swallow extended-release tablets whole
o do not cut, crush, or chew
do not use this drug during pregnancy
report fever, sore throat, unusual bleeding
or bruising, rash, dark urine, lightcoloured stools, hypoglycemic or
hyperglycemic reactions
avoid alcohol while using this drug
Surgery:
o
product should be discontinued
temporarily for surgical
procedures when patient is NPO,
or if contrast media is used;
resume when patient is eating
PN2 Health and Healing Test #2
16
*Insulins differ in regard to onset, peak action, and duration; can be used to tailor treatment to the clients specific
patterns of blood glucose levels, lifestyle, eating and activity.
Types of insulin approved for use in Canada and qualify to be on CPNRE Licensing Exam
Insulin type/action (appearance)
Brand names (generic in brackets)
Dosing Schedule
Rapid-acting analogue (clear)
Onset: 10-15 minutes
Peak: 60-90 minutes
Duration: 3-5 hours
Apidra (insulin glulisine)
Humalog (insulin lispro)
NovoRapid (insulin aspart)
Usually taken right before eating,
or to lower high blood glucose
Short-acting (clear)
Onset: 30 minutes
Peak: 2-3 hours
Duration: 6.5 hours
Humulin-R
Novolinge Toronto
Taken about 30 minutes before
eating, or to lower high blood
glucose
Intermediate-acting (cloudy)
Onset: 1-3 hours
Peak: 5-8 hours
Duration: up to 18 hours
Humulin-N
Novolinge NPH
Often taken at bedtime, or twice a
day (morning and bedtime)
Long-acting analogue (clear and
colourless)
Onset: 90 minutes
Peak: none
Duration: up to 24 hours (Lantus
24 hours, Levemir 16-24 hours)
Lantus (insulin glargine)
Levemir (insulin detemir)
Usually taken once or twice a day
Premixed (cloudy)
PREMIXED REGULAR INSULIN - NPH Depends on the combination
A single vial or cartridge contains Humulin (30/70)
a fixed ratio of insulin (the
Novolinge (30/70, 40/60, 50/50)
numbers refer to the percent of
PREMIXED INSULIN ANALOGUES
rapid- or fast-acting insulin to the Humalog Mix25 and Mix50
percent of intermediate-acting
NovoMix 30
insulin)
(Highlighted are drugs from package so try to learn)
Drug Name
Novolin 30/70
Adverse Effects
Endo:
HYPOGLYCEMIA.
Nursing ResponsibilitiesHealth Teaching
Assessment
Assess periodically for symptoms of hypoglycemia
and hyperglycemia
Local: erythema, lipodystrophy,
Monitor body weight periodically. Changes may
pruritus, swelling.
necessitate changes in insulin dose.
Toxicity and Overdose: Overdose is manifested by
Misc.: ALLERGIC REACTIONS
symptoms of hypoglycemia. Mild hypoglycemia
INCLUDING ANAPHYLAXIS.
may be treated by ingestion of oral glucose. Severe
Novolin R (ge
hypoglycemia is a life-threatening emergency;
Toronto)
treatment consists of IV glucose, glucagon, or
epinephrine.
Regular insulin
Health Teaching
Patients with DM should carry a source of sugar
Given according to
(candy, glucose gel) and identification describing
sliding scale: QID
their disease and treatment regimen at all times.
***Lipodystrophy may occur if insulin is given cold or in repeated area by not repeating site rotation for each injection
(Med-Surg. p. 1345)
Why does Mrs. Sinclair now require insulin?
her diabetes is not controlled
her oral medications are not as effective when she is unstable
insulin is given when there is an infection (foot ulcer)
PN2 Health and Healing Test #2
17
What does the term sliding scale mean?
the amount of short-acting insulin may be varied depending on the patient's pre-prandial finger-stick glucose
sliding scale will be based on doctors orders
Would you give Humulin R if you were unable to find Novolin R? Why or why not?
No
Humulin is fake human insulin and Novolin is pig insulin think of cultures that dont eat pork
regardless the insulin's composition, we must NEVER interchange medication w/o an order
Explain why blood glucose testing is recommended to monitor glucose rather than urine testing
quick
cheap
effective
accurate
What health teaching regarding diet and exercise would assist Mrs. Sinclair in the management of her diabetes?
capillary blood glucose monitoring
exercise - moderate 3X/week for 20 minutes each
if on medications that can cause hypoglycemia, it is recommended that pt schedule exercise about 1 hour after a
meal, or have a 10-15 g carbohydrate snack before exercising
small carb snacks can be taken every 30 minutes during exercise to prevent hypoglycemia
pt should also carry fast acting source of carbohydrate such as juice, glucose tablets, or hard candies when
exercising
Identify 4 nursing diagnoses that are the most appropriate for Mrs. Sinclair; develop goals, interventions and
evaluation criteria
Nursing Diagnosis:
Ineffective Health maintenance r/t complexity of therapeutic regimen
Ineffective Health management
Non-compliance r/t restrictive lifestyle; changes in diet, medication, exercise
Imbalanced Nutrition: more than body requirements r/t excessive intake of nutrients
Ineffective peripheral tissue Perfusion r/t impaired arterial circulation
Powerlessness r/t perceived lack of personal control
Disturbed Sensory perception r/t ineffective tissue perfusion
Risk for unstable blood Glucose level
Risk for Infection: Risk factors: hyperglycemia, impaired healing, circulatory changes
Risk for Injury: Risk factors: hyperglycemia or hypoglycemia from failure to consume adequate calories, failure
to take insulin
Risk for impaired Skin integrity: Risk factors: loss of pain perception in extremities
Acute Pain r/t insulin injections, peripheral blood glucose testing
EXTRAS:
Ineffective Therapeutic Regime Management:
evaluate the amt of knowledge the pt has r/t the disease to determine extent of required teaching
discuss lifestyle changes that may be required & measures to prevent & minimize symptoms
review steps to prevent hyper/hypoglycemia & review insulin administration technique
encourage pt to actively participate & describe possible complications
plan individualized exercise program with patient
review community resources & DM control regime
Imbalanced Nutrition: More than Body Requirements:
assist pt to accommodate food preferences to the diet to increase chance of compliance
refer pt to dietitian and nutritionist to continue education
instruct pt how to monitor activity tolerance to prevent injury
assist pt to incorporate activity to life style because it is an integral part of management
monitor closely signs & symptoms of hyperglycemia to alert client to glucose-insulin imbalanced and act
anticipate situations in which insulin would be required
restrict exercise when blood glucose is > 14mmol specially when ketones are present, to decrease the body's
glucose requirement since there is no available glucose to the cells
PN2 Health and Healing Test #2
18
Risk for Injury:
assess foot for signs of neuropathy
provide info r/t neuropathy, injury, CVD, & the risk for ulceration & amputation to promote commitment
caution about potential source of injury (heat, cold, cutting corns/nails, chemicals, antiseptics, tape, barefoot,
open toe-shoes, ill-fitting shoes, tape)
instruct pt to inspect inside shoes daily to prevent injury that is not felt
monitor S&S of hyper/hypoglycemia and evaluate the knowledge of the pt in this regard to determine the level of
health teaching needed
instruct client t have simple carbs available in case of hypoglycemia
instruct pt to obtain & carry emergency identification
Risk for Peripheral Neurovascular Dysfunction:
perform peripheral vascular assessment
inspect skin for signs of ulcers, skin breakout, or necrosis
provide protection for extremities (foot board/bed cradle at bed side, well-fitted shoes, sheepskin under feet &
lower legs)
keep pt hydrate to lower blood viscosity
instruct pt to exercise as tolerated to maintain peripheral circulation
provide teaching r/t factors that interfere w. circulation (smoking, restrictive clotting, exposure to cold
temperature, crossing legs/feet)
execute proper foot care
Ambulatory & Home care:
Monitor Personal Hygiene
dental practices are necessary (daily brushing and flossing)
daily assessment of feet
if cuts scrapes, burns occur, monitoring + wash & apply non-irritating antiseptic ointment + monitoring (if not
healing within 24hrs = notify HC professional)
o
***creams not between the toes; promotes growth of bacteria leading to infection
assess for insulin therapy
Client/Family Teaching
if client participates in self-management of DM = better outcomes
o however, clients can encounter variety of physical, emotional, and socioeconomic barriers
explain about the disease process (pathology, etiology, pharmacology)
encourage physical activity (discuss importance of exercise when managing DM)
menu planning (educate client about well-balanced diet + benefits or counterproductive impact of a non-well
balanced diet)
encourage medication compliance (ensure client knows actions + methods of application of insulin) (account
limitations that client may have & discuss side effects)
teach how to monitor BG (how often + analyzing results + immediate actions)
promote risk reduction (ensure client understand symptoms of hypo/hyperglycemia + stress, appropriate foot care
+ instruct client about effects of stress and good coping mechanism)
facilitate and make client aware of the many different resources available to help adjust & answer common
question r/t DM
advise to carry medical identification when traveling
Foot Care
Foot ulcers develop in approximately 15% of individuals with diabetes and foot disorders are a leading cause
of hospitalization among this group.
o
85% of lower limb amputations in persons with diabetes are preceded by foot ulcers
The most important factors related to the development of foot ulcers are peripheral neuropathy, minor foot
trauma and foot deformities
o
Diabetic foot ulcers are complex and multi-factorial in nature, often involving ischemic and neuropathic
components, the latter of these two occurring within 10-15 years of diagnosis in 50% of diabetic pts
A person with diabetes should expect to be offered information about the following:
Self-care and monitoring of diabetes
The potential impact of diabetes on the feet
PN2 Health and Healing Test #2
19
Daily examination of feet for problems and when to seek advice from a healthcare professional
o e.g. if any color change, swelling, breaks in the skin, pain or numbness is found, or if self-care and
monitoring is not possible or difficult
Implications of loss of protective sensation
Possible consequences of neglecting the feet
Methods to help self-examination/monitoring (for example, the use of mirrors if mobility is limited
Hygiene (daily washing and careful drying)
Skin care (moisturizer use)
Nail care
Dangers associated with inappropriate mechanical and chemical skin removal
Footwear (the importance of well-fitting shoes and hosiery)
Injury prevention and the importance of not walking barefoot when reduced sensation is present
Annual foot exam by trained professional to assess for neuropathy and vascular disease
Prompt detection and management of any problems are important, thus the importance of seeking help as soon as
possible
All persons living with diabetes should have access to health care providers to help them (as needed) with the
following:
Foot inspection/examination and risk assessment
Nail care
Callus care
Skin care
Foot hygiene
Podiatric management
Pressure reduction to foot (off-loading)
Appropriate selection of protective footwear which includes:
o
commercially available shoes with proper design characteristics may be adequate for low-risk patients
o
added depth shoes should be recommended for high-risk patients who have sensory loss, vascular
insufficiency and/or mild to moderate foot deformity (a custom molded inlay may be added to these
shoes to further enhance pressure distribution)
o
custom molded shoes with custom inlays should be recommended for high-risk patients with advanced
deformity
PN2 Health and Healing Test #2
20
PN2 Health and Healing Test #2
21
Pathophysiology of stroke:
an interruption of the blood supply to any part of the brain
happens when a blood vessel in the brain is blocked or bursts open
There are two major types of stroke:
ischemic stroke
o
blood vessel that supplies blood to the brain is blocked by a blood clot
hemorrhagic stroke
o
blood vessel in part of the brain becomes weak and bursts open, causing blood to leak into the brain
Describe the risk factors for a stroke:
Modifiable:
Hypertension
Hyperlipidemia
Smoking
Diabetes Mellitus
Heart disease
o
Atrial fibrillation
o
Wall motion defects
Coronary artery disease (carotid artery disease)
Coagulation disorders
Obesity/inactivity
Heavy alcohol use
PN2 Health and Healing Test #2
22
Cocaine use
Asymptomatic carotid stenosis
Oral contraceptive use
Sickle cell disease
Sleep apnea
Non-Modifiable:
Age
Gender: More common in men than in women
Race: Black
Heredity
Clinical Manifestations of a stroke:
Motor Function:
Mobility
Respiratory function
Dysphagia
Gag reflex
Self-care abilities
Loss of skilled voluntary movement (akinesia)
Impairment of integration of movements
Alterations in muscle tone
Alterations in reflexes
o
Initial hyporeflexia (depressed reflexes) progresses to hyperreflexia (hyperactive reflexes) for most
clients
Communication:
Aphasia
o
Expressive aphasia (Brocas aphasia): difficulty in expressing thoughts through speech or writing
o
Receptive aphasia (Wernickes aphasia): difficulty understanding spoken or written language
o
Anomic or amnesia aphasia (lease severe): problems finding the correct names for specific objects,
people, places or events
o
Global aphasia: loss of all communication and receptive function.
Dysarthria
Affect:
Difficulty controlling emotions
o
Responses may be exaggerated or unpredictable
o
Depressing and feelings associated with changes in the body image and loss of function can make this
worse
Intellectual Function:
Both memory and judgement may be impaired
o
Left-brain damage:
Paralyzed right side: hemiplegia (paralysis of one side of the body)
Impaired speech
Impaired right left discrimination
Slow performance, cautions
Aware of deficits: depression, anxiety
Impaired comprehension related to language, math
o
Right-brain damage:
Paralyzed left side: hemiplegia
Left-sided neglect
Spatial perceptual deficits
Tends to deny or minimize problems
Rapid performance, short attention span
Impulsive; safety problems
Impaired judgement and time concepts
PN2 Health and Healing Test #2
23
Elimination:
Problems with urinary and bowel elimination occur initially and are temporary
Partial sensation for bladder filling remains; voluntary urination is present
Constipation is associated with immobility, weak abdominal muscles, dehydration and diminished response to
defecation reflex
Urinary and bowel elimination problems may also be related to inability to express needs
Atrial Fibrillation: why is it a risk factor for stroke?
The increased risk due to the fact that during atrial fibrillation, the heart's atria are not squeezing effectively.
o
Consequently, the blood tends to "pool" in the atria - and whenever blood flow is disrupted, blood
clotting can occur.
o
Clots that form in the atria can break loose eventually, and if the clots travel through the arteries to the
brain, a stroke results.
What drug would be prescribed for clients with atrial fibrillation to minimize the risk of stroke?
Heart rate medications
1. Beta blockers
These drugs help lower heart rate.
They do this by blocking the effects of epinephrine, also known as adrenaline.
Beta blockers are often given to people with Afib.
2. Calcium channel blockers
Calcium channel blockers also slow down the heart rate.
These drugs help relax the smooth muscle lining of the arteries.
They also keep the heart from absorbing calcium.
Calcium can strengthen the hearts contractions.
These actions mean that these drugs help relax the heart muscle and widen the arteries.
Only two calcium channel blockers are centrally acting.
o
This means that they help lower your heart rate.
o
Theyre often used to treat Afib.
o
These drugs include:
diltiazem hydrochloride (Cardizem)
Other calcium channel blockers are peripherally acting.
o
They also relax blood vessels, but they arent helpful for Afib heart rate problems.
3. Digitalis glycosides
This drug helps strengthen heart contractions.
Digoxin helps slow the speed of electrical activity from the atria to the ventricles.
This action helps control heart rate.
Heart rhythm medications
Afib is an electrical problem.
o
The hearts rhythm is controlled by electrical currents that follow a set path throughout the heart.
o
In Afib, electrical currents no longer follow that pattern.
o
Instead, chaotic electrical signals run throughout the atria.
o
This makes the heart quiver and beat erratically.
PN2 Health and Healing Test #2
24
Drugs that are specifically used to treat problems with heart rhythm are called antiarrhythmic drugs.
o
There are two basic types that help prevent recurring Afib episodes:
1. Sodium channel blockers
These drugs help control heart rhythm.
They do this by reducing how fast the heart muscle conducts electricity.
They focus on electrical activity in the sodium channels of the heart cells.
2. Potassium channel blockers
Like sodium channel blockers, potassium channel blockers also help control heart rhythm.
They slow down electrical conduction in the heart.
They do so by interfering with conduction that occurs through the potassium channels in the cells.
o
amiodarone (Cordarone, Pacerone)
Blood thinners
There are different types of blood thinners.
These drugs help prevent dangerous blood clots from forming.
They include antiplatelet drugs and anticoagulant drugs.
Blood thinners raise your risk of bleeding.
If your doctor gives you one of these drugs, theyll watch you closely for side effects during treatment.
1. Antiplatelet drugs
These drugs work by interfering with the action of platelets in your bloodstream.
Platelets are blood cells that help stop bleeding by bunching together and forming a clot.
o
aspirin
o
clopidogrel (Plavix)
2. Anticoagulants
These drugs work by extending the time it takes for your blood to clot.
If the doctor prescribes this drug, theyll monitor the patient closely to make sure the dosage is correct.
It can be tricky to keep blood at the correct thinning level, so the doctor needs to check often that the dosage is
accurate.
PO:
o
warfarin (Coumadin)
Injectable:
o
dalteparin (Fragmin)
http://www.healthline.com/health/living-with-atrial-fibrillation/medication-list#Bloodthinners4
Pathophysiology of Chronic Renal Failure: (Chronic Kidney Disease [CKD])
The presence of kidney damage or renal insufficiency that is unlikely to be reversed; it is present for a period
of 3 months or more and can be classified at one of the five stages, depending on level of severity based on
glomerular filtration rate (GFR).
Stages of Chronic Renal Failure:
Stage 1:
Kidney damage with normal or GFR; 90 mL/minute
Action: Diagnosis and treatment, treatment of co morbid conditions, CVD risk reduction
Stage 2:
Kidney damage with mild GFR; 60-89 mL/minute
Action: Estimation of progression
Stage 3:
Moderate GFR; 30-59 mL/minute
Action: evaluation and treatment of complications
Stage 4:
Severe GFR; 15-29 mL/minute
Action: preparation for renal replacement therapy
Stage 5: End-Stage Renal Disease (ESRD)
Kidney failure; <15 mL/minute (or dialysis)
Action: renal replacement therapy; RRT (if uremia present)
o
Dialysis modalities remain the most common renal replacement therapy because:
A lack of donated organs
Medical conditions that preclude transplantation
Personal reasons where an individual may decline transplantation as a treatment option
PN2 Health and Healing Test #2
25
Risk factors for CRF:
Modifiable:
Diabetes
High blood pressure (HTN)
Drug abuse
Inflammation
Overuse of pain killers and allergic reactions to antibiotics
Blockages
o
Scarring from infections or malformed lower urinary tract system
Non-Modifiable:
Ethnic groups:
o
Aboriginal: 6 times in Native North Americans with diabetes
o
Asian
o
South Asian
o
Pacific island
o
African-Caribbean
o
Hispanic
Premature birth
Age
Family history; genetics
Trauma or accident
Certain diseases
o
Systemic lupus erythematosus (connective tissue disease)
o
Sickle cell anemia
o
Cancer
o
AIDS
o
Hepatitis C
o
CHF
Clinical Manifestations of CRF:
As renal function progressively deteriorates, excretory, regulatory and endocrine function is lost, and these
effects are manifested in every body system, no matter what the underlying cause of the CRF is.
They are manifested in retained substances; including urea, creatinine, phenols, hormones, electrolytes and water.
Urinary:
Polyuria: results from inability of the kidneys to concentrate urine
Nocturia
Oliguria: as CRF worsens
Proteinuria, casts, pyuria and hematuria could be present of the client is still producing urine
Metabolic Disturbances:
Waste product accumulation:
o
Nitrogen waste products in advanced stages of CRF often manifest with symptoms of nausea, vomiting,
lethargy, fatigue, impaired thought processes, headaches
Altered carbohydrate metabolism:
o
Caused by impaired glucose use resulting from cellular insensitivity to the normal action of insulin
Elevated triglycerides:
o
Hyperinsulinemia stimulates hepatic production of triglycerides
o
Dyslipidemia
Electrolyte and Acid-Base Imbalances:
Potassium:
o
Hyperkalemia
Sodium:
o
May be normal or low in renal failure
Calcium and phosphate:
o
Hypocalcaemia
o
Phosphate excess
o
Alterations are associated with mineral metabolism disorders in CRF
PN2 Health and Healing Test #2
26
Magnesium:
o
Hypomagnesemia: only a problem if client is ingesting magnesium; milk of magnesia, magnesium
citrate, antacids containing magnesium
Metabolic acidosis:
o
Resulting from impaired ability of the kidneys to excrete the acid (hydrogen ions) load and from
defective reabsorption and regeneration of bicarbonate ions
Hematological:
Anemia:
o
Classified as normocytic, normochromic; due to production of the hormone erythropoietin by the
kidneys
Bleeding tendencies:
o
Most common cause of bleeding in uremia is a qualitative defect in platelet function
Infection:
o
Caused by changes in leukocyte function and altered immune response and function
Diminished inflammatory response
Lymphopenia, lymphoid tissue atrophy, antibody production and suppression of the delayed
hypersensitivity response
Increased incidence of cancer:
o
Lung, breast, uterus, colon, prostate and skin malignancies are most commonly found in those with renal
failure who have not had a transplant
Cardiovascular:
Leading cause of death in people with CRF
HTN
Atherosclerotic vascular disease
Left ventricular hypertrophy which can lead to pulmonary edema
CHF
Peripheral edema
Uremic pericarditis (inflammation of the pericardium)
Respiratory:
Pulmonary edema from fluid overload
Uremic pleuritis
Pleural effusion
Predisposition to respiratory infections
Kussmauls respirations (found in very advanced CRF because of acidosis)
Gastrointestinal:
Stomatitis with exudates and ulcerations
Metallic taste in mouth
Uremic fetor (a ruinous odour of the breath; urine smell on the breath)
Anorexia, nausea, and vomiting cause by irritation to the GI tract
Diarrhea may occur due to hyperkalemia and altered calcium metabolism
Neurological:
Depression of the CNS
o
Lethargy
o
Apathy
o
ability to concentrate
o
Fatigue
o
Irritability
o
Altered mental ability
Seizures (related to alterations in electrolyteslow sodium will cause seizures)
Coma
Peripheral neuropathy
Restless legs syndrome
PN2 Health and Healing Test #2
27
Musculoskeletal:
Osteoporosis (calcium taken from bone to correct hypocalcaemia)
Osteitis fibrosa cystica (resorption and replacement of calcified bone with fibrous tissue)
Osteomalacia (bone demineralization due to deficiency or impaired metabolism of vitamin D or phosphates)
Adynamic bone disorder (Loss of strength or vigor of bones)
Mixed osteodystrophy (Defective formation of bone)
Integumentary:
Yellow-grey discoloration of the skin
perspirations
Pruritus
Dry, brittle hair; may fall out
Thin, brittle, and rigid nails
Reproductive:
Infertility
libido
Women: levels of estrogen, progesterone and luteinizing hormone causing anovulation and menstrual changes
Men: loss of testicular consistency, testosterone levels and low sperm count
Endocrine:
Hypothyroidism
Psychological:
Personality and behavioural changes
Emotional lability
Withdrawal
Depression
Incidence/Prevalence of stoke and renal disease for First Nations Canadians vs. Non First Nations Canadians:
6 times in Native North Americans with diabetes
What risk factors does Mrs. Sinclair have for a stroke?
Aboriginal
CAD
Afib
Terms
Hemiparalysis: Paralysis of one side of the body
Expressive aphasia: Partial or total loss of the ability to express oneself, either through speech or writing
Receptive aphasia: Inability to understand written, spoken, or tactile speech symbols
Homonymous hemianopia: Loss of vision of the right or left halves of the visual field in both eyes
Nursing responsibilities/pre-post procedure care of:
CT scan:
Computer-assisted x-ray views of several levels or thin cross-sections of body parts are done to detect problems such as
hemorrhage, space-occupying lesions, cerebral edema, brain atrophy, and other abnormalities
Explain that the procedure is non-invasive ( if no contrast medium used)
Observe for allergic reaction and note puncture site (if contrast medium used)
Explain the appearance of the scanner
Instruct the client on the need to remain absolutely still during the procedure
Cerebral angiography:
Serial x-ray visualization of intracranial and extracranial blood vessels is performed to detect vascular lesions and tumours
of brain. Contract medium is used.
Explain that the client will have a hot flush of head and neck when contrast medium is injected
Explain the need to be absolutely still during the procedure
Monitor neurological and VS every 15-30 mins for the first 1 hrs, every hour for the next 4 hrs, then every 4 hrs
for the next 24 hrs
PN2 Health and Healing Test #2
28
Maintain pressure dressing and ice to injection site
Maintain bedrest until client is alert and VS are stable (4 hours)
Report any signs of change in neurological status
Further assessment before initiating feeding: (see below in blue)
Swallowing assessment (SLP)
Members of the health care team to have a swallowing assessment done:
The interdisciplinary dysphagia team includes:
Speech-language pathologist (SLP):
o
Plays a central role in screening, assessing, treating and managing dysphagia
Registered dietician (RD):
o
Plays a key role in assessing and monitoring clinical indicators of nutritional status
o
Recommends types and route of administration of external feeding and dietary components
Physician (MD):
o
Supervises the medical management, monitoring and managing pulmonary status and hydration, order
appropriate investigations, consulting RD and SLP about need for enteral and parenteral feeding
Registered Nurse (RN):
o
Key member based on central role of this discipline in patient care, which involves monitoring patient at
all times
Registered Practical Nurse (RPN):
o
Same as RN
Occupational Therapist (OT):
o
Traditionally responsible for ADLs, including meal preparation and pre-feeding activities
o
Determines types of adaptive equipment needed and ways to improve meal set-up and food transport to
the mouth
Physiotherapist (PT):
o
Can assist with optimal positioning for safe feeding and with implementing swallowing strategies that
direct the bolus away from the airway and facilitate safer swallowing
Best practices for feeding a client with dysphagia:
Diet modification is one of the most frequently used interventions to compensate for dysphagia.
Effective feeding techniques include the following:
Use a slow rate of presentation
Allow adequate time between bites of food
Control rate of intake by presenting a maximum of 1 teaspoon per bite
Place food on the strong side of mouth
Encourage the stroke survivor to take 2 or more swallows per bite, to clear residue and aid esophageal transit
Alternate liquids and solids, but never combine them in the same bite
Talk conversationally with stroke survivor during oral intake, but time responses so that the stroke survivor does
not reply with food/liquid in mouth
Advise stroke survivor of what food/liquid is being presented
Ask stroke survivor in which order food/liquid should be presented
Provide visual or verbal cues for opening mouth, chewing and swallowing
Reduce or eliminate talking by the stroke survivor during oral intake, but allow talking between bites
Check for pocketing and residue after feeding
Recommendations for medication administration:
Pills should be taken with water, one at a time
Pills should be crushed (verify with pharmacist that pill is crushable)
Pills should be cut in half (verify with pharmacist that pill can be cut)
Medication should be given as a liquid, possibly thickened (verify with pharmacist that medication can be
dispensed in liquid form and that it can be thickened using specific parameters)
Pills should be placed in a spoon of puree, such as applesauce or pudding
Pills should not be taken with water
PN2 Health and Healing Test #2
29
Implement safe feeding practices:
Observe the patient during feeding
Encourage strategies to improve eating behaviour to ensure adequate oral intake and effective feeding techniques
Use recommended medication administration methods
The environment in which the dysphagic patient is eating is highly important for safe feeding. This includes the
individuals physical status and environment, sensory input, the social aspect of meals and meal independence.
Types of food most appropriate for Mrs. Sinclair; with rationale:
Typical diet textures given to stroke survivors with dysphagia:
Mechanically chopped or minced semi-solids that require little chewing
o
Minced or ground foods: This food texture refers to soft solid foods that have been chopped to peasized particles and are moist enough to form a cohesive and easy-to-chew bolus. A ground/minced diet
allows the stroke survivor to eat with minimal chewing. Typical foods in this category include
shepherds pie and cottage cheese.
Pureed solids with homogeneous, very cohesive, pudding-like consistencies that require bolus control but no
chewing
o
Pureed foods: Pureed foods are smooth and homogenous, with a spoon-thick consistency. This food
texture includes mashed or blenderized foods with a dense, smooth consistency, such as yogurt,
applesauce or mashed potatoes. Pureed foods should never be lumpy or runny.
Thickened, slower-moving liquids that compensate for slower-moving swallowing muscles
o
Thickened fluids: The purpose of thickening liquids is to slow the time it takes for the fluid to move
through the mouth and esophagus, allow better control of the swallow, and decrease the risk of
aspiration pneumonia. The recommended thickness of thickened fluids varies, for example, from that of
nectar to honey, and is determined individually. It is important to note that the thickness of a liquid is
often temperature dependent; for example, ice cream is a puree when cold but a thin liquid at body
temperature. Thickened fluids reduce the risk of aspiration, but stroke survivors often find them
unappealing, increasing the risk of malnutrition and dehydration
***Need to avoid dry particulates, bread products, mixed consistencies, thin fluids and reflux-promoting foods.
Drugs
Drug Names
Desired Action
Adverse Effects
Nursing Responsibilities/ Health
Teaching
Hypoglycaemia
1. Assess for symptoms of
Humulin 30/70 Control of
(insulin:
hyperglycemia in Anaphylaxis
hypoglycemia
mixtures)
patients with type Erythema
2. Monitor body weight periodically
1 or type 2
Lipodystrophy
3. Lab tests: may cause serum
Classifications:
Antidiabetic
diabetes
Pruritus
inorganic phosphate, magnesium, and
Hormones
Lower blood
potassium levels
Pancreatics
glucose
4. Monitor blood glucose q6h
5. Overdose is manifested by symptoms
Peak: 30 min
of hypoglycaemia
Onset: 4-8 hr
6. Store insulin in the refrigerator
Duration: 24 hr
7. Do not interchange insulin without
consulting physician
Control of
Humulin R
8. Subcut: rotate injection site
(insulin: short
hyperglycemia in
9. Administer: into abdominal wall,
acting)
patients with type
thigh, or upper arm
1 or type 2
diabetes
Classification:
Antidiabetic Can be used to
Hormones
treat diabetic
Pancreatics
ketoacidosis
Treatment of
Peak: 30-60 min
hyperkalemia
Lower blood
Onset: 2-4 hr
glucose
Duration: 5-7 hr
- most common - life threatening - most important to know - lecture notes
PN2 Health and Healing Test #2
Drug Names
furosemide
(Lasix)
Desired Action
Classifications:
Diuretic
Loop
diuretic
Drug Names
atorvastatin
(Lipitor)
Classifications:
Lipid
lowering
agent
HMG-CoA
reductase
inhibitor
30
Inhibits
reabsorption of
sodium +
chloride by
causing sodium
to be excreted in
the urinewhere
salt goes, water
follows
Pt has edema
Adverse Effects
Desired Action
Adjunctive
management of
primary
hypercholesterol
emia and mixed
dyslipidemia
Primary
prevention of
coronary heart
disease
Dehydration
Hypokalemia
Hypovolemia
Hypotension
Dyspepsia
Aplastic anemia
Agranulocytosis
Nursing Responsibilities/Health
Teaching
1. Monitor BP and pulse and assess
potassium levels before/during admin
2. Lab Tests: Monitor electrolytes, renal
and hepatic function, serum glucose.
Commonly serum potassium. May
cause serum sodium, calcium,
magnesium. May also cause BUN,
glucose, creatinine, and uric acid
3. PO: May be taken with food or milk
to minimize gastric irritation
Adverse Effects
Abdominal cramps
Constipation
Diarrhea
Heartburn
Rashes
Myalgia (achy bones)
Rhabdomyolysis
Hypersensitivity
reactions: including
angioneurotic edema
1.
2.
3.
4.
Drug Names
aspirin (ASA)
Classifications:
Antiinflammatory
Non-opioid
analgesic
Anti-coagulant
Desired Action
Drug Names
lisinopril
(Zestril)
Desired Action
Classifications:
Anti-HTN
ACE
inhibitor
pain
fever
contraindicated
in children
inflammation
prevention/
prophylaxis of
thrombus/MI
Adverse Effects
Management of
HTN
Management of
heart failure
risk of MI
GI bleeding
Dyspepsia
Epigastric distress
Nausea
Tinnitus
Hepatoxicity
Allergic reaction:
including anaphylaxis
1.
2.
3.
4.
5.
Adverse Effects
Dizziness
Cough
Fatigue
Chest pain
Hypotension
headache
Angioedema
1.
2.
3.
4.
5.
6.
7.
Nursing Responsibilities/ Health
Teaching
Assess fluid status. Monitor daily
weight, intake and output ratios,
amount and location of edema
Lab Tests: Monitor electrolytes, renal
and hepatic function, serum glucose,.
Commonly serum potassium. May
cause serum sodium, calcium, and
magnesium concentrations. May also
cause BUN, serum glucose,
creatinine, and uric acid levels
PO: May be taken with food or milk
to GI irritation; dont take with
antacids
When to give: after dinner; liver
releases most cholesterol at night;
give at same time everyday
Nursing Responsibilities/ Health
Teaching
Give with milk or full glass of water
to GI irritation
Lab Tests: hepatic function, may
cause serum ALT, AST, alkaline
phosphatise; Hct levels periodically
Hold 1 week before surgery
Do not crush EC (enteric coated)
Assess for bleeding
Nursing Responsibilities/ Health
Teaching
Monitor BP and pulse frequently
Do not administer if BP 100/60
Lab Tests: May BUN, creatinine,
hyperkalemia
Pharmacist can compound an oral
suspension if client has dysphagia
Shake suspension before each use
Encourage client to change positions
slowly to minimize orthostatic
hypotension
Take with meals
PN2 Health and Healing Test #2
Drug Names
Vitamin D
Classifications:
Vitamins
Fat-soluble
vitamins
Drug Names
Therapeutic/Desired
Action
Treatment and
prevention of
deficiency states
Increases
absorption of
calcium
Therapeutic/Desired
Action
Treatment and
prevention of
hypocalcaemia
Relief of acid
indigestion or
heartburn
Treatment of
hyperphosphate
mia in end-stage
renal disease
31
Adverse Effects
Pancreatitis
Headache
Weakness
Constipation
Hypercalcemia
Nursing Responsibilities/ Health
Teaching
1. May be administered without regard
to food
2. Lab Tests: serum calcium,
phosphorus, and alkaline phosphatase
Avoid use of antacids with
magnesium
Important
Adverse/Undesirable Effects
Arrhythmias
Bradycardia
Constipation
Nausea
Vomiting
Hypercalciuria
Nursing Responsibilities/Health
Teaching
calcium
1. Chronic use with antacids in renal
carbonate
insufficiency may lead to milk-alkali
(Calcite)
syndrome
2. Excessive amounts may decrease the
effects of calcium channel blockers
Classifications:
mineral and
3. Assess for symptoms of
electrolyte
hypocalcaemia
replacement
4. Lab Tests: Monitor serum calcium or
ionized calcium, chloride, sodium,
potassium, magnesium, albumin, and
parathyroid hormone (PTH)
concentrations before and periodically
during therapy
5. Toxicity and Overdose: Assess
patient for nausea, vomiting, anorexia,
thirst, severe constipation, paralytic
ileus, and bradycardia
6. Do not administer enteric-coated
tablets within 1 hr of calcium
carbonate
- most common - life threatening - most important to know - lecture notes
Nursing Diagnoses most relevant for Mrs. Sinclair:
Nursing Diagnosis
Interventions & Rationale
Excess fluid volume related Monitor for increase in BP, peripheral edema and dyspnea which are indicators of fluid
to inability of kidneys to
excess.
excrete fluid and excess
Teach client how to maintain a low-sodium diet to help control edema and HTN.
fluid as evidence by edema
Teach client fluid control measures and importance of daily weights to help monitor and
and HTN.
control fluid and reduce HTN.
Assess for hypocalcaemia and hyperphosphatemia to determine degree of bone
Risk for injury (fracture)
related to alterations in the
demineralization and potential risk for injury.
absorption of calcium and
Administer calcium supplements, vitamin D, and phosphate binders as ordered to
the excretion of phosphate
prevent and/or treat the bone demineralization.
and altered vitamin D
Give calcium supplement or phosphate binder with meals to increase effectiveness.
metabolism.
Provide safe environment to reduce the risk of injury.
Assess skin for changes in colour, texture, turgor, and vascularity to provide
Impaired skin integrity
related to decrease in oil &
information for appropriate interventions.
sweat gland activity and
Inspect client for bruises and signs of infection to detect early signs of problems.
excess fluid as evidence by
Provide skin care with tepid water, bath oils, super-fatted soaps, or oatmeal to relieve
itching, bruising, edema and
itching and moisturize dry skin.
dry skin.
Risk for infection related to Assess for manifestations of infection that are local (pain on urination, hematuria,
suppressed immune system,
cloudy urine; redness, swelling, or draining in areas of skin breaks) and systemic (chills,
access sites, and
fever, tachycardia) to ensure early identification and treatment.
malnutrition secondary to
Maintain aseptic technique when performing invasive procedures to prevent the
uremia.
introduction of organisms.
Instruct client to avoid exposure to people with infections to decrease risk of infection.
PN2 Health and Healing Test #2
32
Lecture (lecture notes in blue throughout package)
Nursing Dx r/t Stroke and Diabetes
1. Risk for Aspiration r/t Stoke, Age, AEB difficulty swallowing pills; right sided hemiplegia; aphasia (difficulty
communicating trouble swallowing); pt is 72 years old
assess readiness to eat (LOC
position pt for feeding (high fowlers)
proper diet
assess whole time feeding; after feeding complete (pocketing?)
2. Risk for Skin Breakdown r/t decreased mobility, Diabetes, AEB Stroke (right-sided hemiplegia), FBG: 13.0, A1C:
10%
3. Risk for Injury r/t Stroke, Ineffective management of Diabetes, AEB right-sided hemiplegia, homonymous
hemianopia, FBG: 13.0, A1C: 10%
observe Q1H prn
remove obstacles
proper transfer techniques (right side is strong side)
assistive devices
4. Imbalance nutrition: less than body requirements r/t Stroke, Diet (?), AEB difficulty swallowing pills, client may not
like pureed diet
5. Risk for Infection r/t Diabetes, Immobility, Insertion Site for Diagnostics, Lab Values
Renal Diet
3 Ps to decrease
potassium
phosphorus
protein
1 C to increase
calcium
Low Potassium Diet
alfalfa sprouts
beans (green/yellow)
raw cabbage
cucumber
lettuce (all)
pepper (red and green)
apple sauce
cranberry sauce
relish
Renal replacement Tx
peritoneal dialysis (can do at home via catheter; health teaching: risk for infection; daily weight; dont want to
gain too much)
hemodialysis (shunt may go in up to a year before they may need it because of poor functioning/healing if wait
when ill; Q3Weekly for 6-8 hours)
kidney transplant (70% die before they can get a transplant)
Dialysis
Dialysis replacement of kidney function to sustain life
Salt and water removal (volume homeostasis)
o Ultrafiltration
Removal of uremic toxins, drugs
o Clearance
Metabolic processes
Acid-base balance lactate or bicarbonate buffer
Vit D, Calcium, Phosphorus homeostasis
Hormonal processes
Erythropoietin
Adequate preparation time for dialysis is 12 months:
medical
transplant assessment
PD catheter insertion
creation of AV fistula
psychosocial
know how to assess
income loss, work
travel arrangements
PN2 Health and Healing Test #2
33
Peritoneal Dialysis
Cycles
o
Infuse - Takes about 5-10 minutes to run the dialysate into the peritoneal cavity by gravity
o
Dwell - Dialysate stays in the peritoneal cavity up against the peritoneal membrane for 1.5-10 hours
o
Drain - Solution runs out by gravity takes about 20 minutes
Solution
o
Solutions contain dextrose (sugar) that is used as an osmotic agent
o
The dextrose pulls water molecules from the patients blood across the PD membrane into the PD cavity
o
The solutions come in 1.5%, 2.5%, and 4.5% dextrose strength
o
The higher the sugar the more fluid can be removed
o
Sterile
o
Usually 2 litre volume
o
Contains Lactate as a buffer- patient absorbs lactate and converts it to bicarb
o
Contains Na, Cl, Mg, Ca,
o
Note does not contain K or Phos
Hemodialysis
Patients dialyze:
o 3x weekly for approx. 4 hours
Vascular access: such as a fistula, graft or central venous catheter
Artificial kidney (dialyzer)
Dialysis monitoring machine
Test/Know
difference between peritoneal dialysis and hemodialysis
S&S of Chronic Renal Failure
3 Ps and 1 C
Nursing Care for Kidney Failure
o
Fluid restriction
monitor in and out
drink only when thirsty
consult dietician for amount permitted
o
Dietary restriction
decreased potassium, phosphorus, protein
increased calcium
o
Labs
Urea, Creatinine, CBC
o
Safety (Injury, Skin breakdown)
You might also like
- Case Study Orange CountyDocument3 pagesCase Study Orange CountyJobayer Islam Tunan100% (1)
- OMM Blurbs From ScottDocument3 pagesOMM Blurbs From ScottshadowlightfoxNo ratings yet
- C+F-Syringomyelia and Hydro My Elia in Dogs and CatsDocument9 pagesC+F-Syringomyelia and Hydro My Elia in Dogs and Catstaner_soysurenNo ratings yet
- Community Medicine Prep Manual for UndergradsDocument5 pagesCommunity Medicine Prep Manual for UndergradsSaumyaNo ratings yet
- Case Study 10: Diana Dichoso Navarete Talavera TibilloDocument25 pagesCase Study 10: Diana Dichoso Navarete Talavera TibilloDaniela DianaNo ratings yet
- VivitrolFactSheet PDFDocument5 pagesVivitrolFactSheet PDFwebmaster@drugpolicy.org100% (1)
- Breen, 2004, The Marketplace of Revolution, How Consumer Politics Shaped American IndependenceDocument401 pagesBreen, 2004, The Marketplace of Revolution, How Consumer Politics Shaped American IndependenceFelipe RochaNo ratings yet
- Mental HealthDocument4 pagesMental HealthAlvin Cabral100% (1)
- Big Five Personality Traits in "House M.D.", S01E09, DNRDocument6 pagesBig Five Personality Traits in "House M.D.", S01E09, DNRStarling HunterNo ratings yet
- Emergency Preliminary Injunctive Relief Requested Oral Argument RequestedDocument27 pagesEmergency Preliminary Injunctive Relief Requested Oral Argument RequestedAmerican Vaping AssociationNo ratings yet
- Beads of Privilege ActivityDocument2 pagesBeads of Privilege Activityapi-599435438No ratings yet
- Chapter 6Document44 pagesChapter 6Teddy Matthew AudleyNo ratings yet
- 1723 West GreenleafDocument2 pages1723 West GreenleafGapers BlockNo ratings yet
- 3E Skin ProtectionDocument4 pages3E Skin ProtectioncarolinangelicaNo ratings yet
- New Financial Products For An Aging PopulationDocument16 pagesNew Financial Products For An Aging PopulationsaminbdNo ratings yet
- (161121608101) - (42K08.1) - (LÊ THỊ PHAN ANH) - BaoCaoToanVanDocument114 pages(161121608101) - (42K08.1) - (LÊ THỊ PHAN ANH) - BaoCaoToanVanHieuhanh TruongNo ratings yet
- John Hopkins Community HealthDocument143 pagesJohn Hopkins Community HealthAndré Jason MendesNo ratings yet
- OSPF Single-Area Configuration GuideDocument24 pagesOSPF Single-Area Configuration GuideAmira JebaliNo ratings yet
- THUY HO THESIS Ambition and Ethics in Marketing FINALDocument44 pagesTHUY HO THESIS Ambition and Ethics in Marketing FINALMuhammad Dzaky Alfajr DirantonaNo ratings yet
- MEMS Application FormDocument1 pageMEMS Application FormdaridlaaNo ratings yet
- COPD, or Chronic Obstructive Pulmonary DiseaseDocument18 pagesCOPD, or Chronic Obstructive Pulmonary DiseaseemilliansNo ratings yet
- Copd 200412082048Document139 pagesCopd 200412082048Richard ArceNo ratings yet
- Chronic Obstructive Pulmonary Disease: National University College of Allied of Health Department of PharmacyDocument8 pagesChronic Obstructive Pulmonary Disease: National University College of Allied of Health Department of PharmacyVenus PolatrixNo ratings yet
- COPD Chronic Obstructive Pulmonary Disease REVISEDDocument37 pagesCOPD Chronic Obstructive Pulmonary Disease REVISEDSonny AgultoNo ratings yet
- Onchi & CopdDocument8 pagesOnchi & CopdAngellene GraceNo ratings yet
- Analisis Kasus COPD KMBDocument36 pagesAnalisis Kasus COPD KMBTHERESA SETIAWANNo ratings yet
- COPD AsthmaDocument16 pagesCOPD Asthma09172216507No ratings yet
- Scenario 5: Group 6Document51 pagesScenario 5: Group 6Gd SuarantaNo ratings yet
- COPD Treatment and ManagementDocument3 pagesCOPD Treatment and ManagementHydie Mae AlcabedosNo ratings yet
- Copd (Chronic Obstructive Pulmonary Disease)Document11 pagesCopd (Chronic Obstructive Pulmonary Disease)Catherine MetraNo ratings yet
- Chronic Obsrtructive Pulmonary DiseaseDocument11 pagesChronic Obsrtructive Pulmonary Diseasepreeti sharmaNo ratings yet
- CopdDocument4 pagesCopdapi-3739910100% (2)
- COPD Synopsis: Chronic Obstructive Pulmonary Disease (COPD)Document3 pagesCOPD Synopsis: Chronic Obstructive Pulmonary Disease (COPD)See my profile pictureNo ratings yet
- COPDDocument18 pagesCOPDMae CalicaNo ratings yet
- Chronic Obstructive Pulamonary DiseaseDocument12 pagesChronic Obstructive Pulamonary Diseaseanamika sharmaNo ratings yet
- Chronic Obstructive Pulmonary Disease (COPD)Document36 pagesChronic Obstructive Pulmonary Disease (COPD)GLORY MI SHANLEY CARUMBANo ratings yet
- COPD Asthma AssignmentDocument17 pagesCOPD Asthma AssignmentKhadija BakhtawarNo ratings yet
- COPDDocument52 pagesCOPDSoySauceNo ratings yet
- Nurul Anisha Bio COPDDocument17 pagesNurul Anisha Bio COPDtriplea_squad2851No ratings yet
- Case Presentation: Ablay-Andrade-Batario-Berbano-Bibera-Borja-Borres-Burns - Cabañero-Corsiga-Custodio - CuyegkengDocument122 pagesCase Presentation: Ablay-Andrade-Batario-Berbano-Bibera-Borja-Borres-Burns - Cabañero-Corsiga-Custodio - CuyegkengJustin Ahorro-Dionisio67% (3)
- Case Study For Chronic BronchitisDocument6 pagesCase Study For Chronic BronchitisGabbii CincoNo ratings yet
- COPD Case Pres2Document29 pagesCOPD Case Pres2Kelly Queenie Andres100% (1)
- PT Case: Copd Exacerbation: DedicationDocument10 pagesPT Case: Copd Exacerbation: DedicationDianaLopezBorjaNo ratings yet
- TB and Copd!Document9 pagesTB and Copd!RachnaNo ratings yet
- 7a COPDDocument45 pages7a COPDDerrick GramataNo ratings yet
- COPD Case PresentationDocument15 pagesCOPD Case PresentationBola Kwentua29% (7)
- NCLEX Review NotesDocument36 pagesNCLEX Review NotesKyla Patricia RibanoNo ratings yet
- COPD Guide: Symptoms, Causes, and TreatmentDocument30 pagesCOPD Guide: Symptoms, Causes, and TreatmentsalmanhabeebekNo ratings yet
- COPD Patient Information Version 3Document7 pagesCOPD Patient Information Version 3contehamosaNo ratings yet
- CopdDocument60 pagesCopdRizqy Shofianingrum100% (1)
- SL NO Content NODocument12 pagesSL NO Content NOPdianghunNo ratings yet
- Tina ThankachanDocument50 pagesTina ThankachanBharat JamodNo ratings yet
- Bronchitis 170709131740Document28 pagesBronchitis 170709131740Viji MNo ratings yet
- 2copd FinalDocument2 pages2copd FinaluikapuNo ratings yet
- Chronic Obstructive Pulmonary DiseaseDocument10 pagesChronic Obstructive Pulmonary DiseaseZinya RobinsonNo ratings yet
- Chronic B. 234Document4 pagesChronic B. 234Sheene Ainasthazia Diego AngNo ratings yet
- Chronic-Bronchitis MedBackDocument37 pagesChronic-Bronchitis MedBackclaire.deveraNo ratings yet
- CopdDocument54 pagesCopdHerty FeliciaNo ratings yet
- COPD Nursing Care GuideDocument16 pagesCOPD Nursing Care GuideJay-ar Zars0% (1)
- COPDDocument52 pagesCOPDswapnil3250No ratings yet