Professional Documents
Culture Documents
TTS Overview
Uploaded by
Faishal HanifCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
TTS Overview
Uploaded by
Faishal HanifCopyright:
Available Formats
Open Access
Austin Journal of Musculoskeletal Disorders
Case Report
Tarsal Tunnel Syndrome: An Overview
Ellison T1 and Saxena S1*
Department of Family Medicine, Creighton University
School of Medicine, USA
1
*Corresponding author: Saxena S, Department of
Family Medicine, Creighton University, 601 N 30th ST,
STE 6720, Omaha, NE 68131, USA
Received: April 30, 2015; Accepted: June 24, 2015;
Published: June 25, 2015
Abstract
Tarsal tunnel syndrome is an uncommon condition which can be painfully
debilitating. This clinical diagnosis is often enhanced by electro diagnostic tests.
Causes are both extrinsic and intrinsic. Initial treatment is usually non-operative,
but at times surgical intervention is indicated at the outset. The surgery is
difficult and the literature suggests patient selection is crucial for positive
surgical outcomes. Surgical success rates are highest when cause is extrinsic
and surgery is performed within 12 months of symptom onset.
Introduction
Tarsal Tunnel Syndrome (TTS) is a type of compression
neuropathy where the tibial nerve is compressed within the tarsal
tunnel running along the inside of the ankle into the foot. Tarsal
Tunnel Syndrome (TTS) is an uncommon condition that can become
debilitating as a result of progressive pain. With TTS, pain originates
in the ankle from entrapment of the posterior tibial nerve or its medial,
lateral or calcaneal branches in the proximal and/or distal tarsal
tunnel [1,2]. The flexor retinaculum serves as the roof of the fibroosseous tunnel connecting the medial malleolus to the calcaneous
while the medial aspect of the talus, calcaneum and distal tibia form
the floor [2,3]. The tarsal tunnel is posterior and inferior to the medial
malleolus and holds, from medial to lateral, the tibialis posterior
tendon, the flexor digitroumlongus tendon, the posterior tibial artery
and vein, the posterior tibial nerve and the flexor hallucislongus
tendon [1,4].The posterior tibial nerve can become compressed at the
tarsal tunnel leading to proximal TTS [5]. Calcaneal branches from
the posterior tibial nerve penetrate the flexor retinaculum to provide
sensation to the posterior and medial heel [1-5]. Ninety-five percent
of the time, the posterior tibial nerve bifurcates into the medial and
lateral planter nerves distal to the tunnel [1]. The medial and lateral
plantar nerves then enter their own distal tunnels [1,6]. Compression
of either the proximal or distal tunnels can lead to TTS causing pain
and hypoesthesia involving the heel and plantar surfaces of the foot
[1,6]. Due to low incidence along with variations in pain, sensory and
motor deficits, TTS can be difficult to diagnose. If TTS is suspected,
differential diagnoses such as chronic plantar fasciitis with distal TTS
or lumbar radiculopathy should be considered [1]. A variety of tests
performed on physical exam as well as imaging studies improve the
detection and diagnosis of TTS.
waking her at night [3]. She expressed concern over losing the ability
to golf, or even walk, if the pain and numbness continued to progress.
On exam, no obvious ankle deformity, such as hindfoot varus
or valgus, was appreciated. Ankle erythema and edema were absent.
Point tenderness over the soft spot on the medial border of the
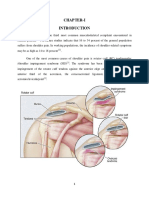
abductor hallucis was present (Figure 1) [5]. There was a positive
Valleix test (pain on deep palpation of the tarsal tunnel) as well as
arch tenderness [9]. Neurological examination revealed positive
Tinels sign and decreased two-point discrimination on the plantar
surface of the foot.
Etiology
Repetitive actions of dorsiflexion and plantar flexion during
activities such as sprinting and jumping can lead to increased tunnel
pressures and subsequent irritation. As walking, running and jumping
rarely result in tarsal tunnel irritation, many patients diagnosed with
TTS have either intrinsic or extrinsic factors predisposing them to
TTS [7]. Intrinsic factors may include tendonopathies, osteophytes,
anatomical anomalies and space occupying lesions such as accessory
muscles, ganglia or lipomas [1,4].Takakura et al. report ganglia
to be the most common space occupying lesions in proximal TTS
[10]. Intrinsic factors in the distal tarsal tunnel can lead to traction
neuritis. For example, the weakening of the plantar fascia can result
in stretching of the lateral plantar nerve, impinging it at the soft spot
as it turns into the distal foot over the flexor digitorum brevis [2,5]. In
Classic Presentation
A 42-year-old female presented with pain and burning of three
months duration in her left ankle and sole. She reported increasing
discomfort now interfering with her recreational golfing [7]. She
denied recent or past ankle trauma. Pain was localized posterior and
inferior to her medial malleolus and she complained of numbness
along her posterior and medial heel radiating to the plantar surface of
the foot [8]. She denied pain upon first step, but reported intensifying
pain with activity and after burn or lengthened time for pain
dissipation post activity [2]. More recently, pain has occurred at rest,
Austin J Musculoskelet Disord - Volume 2 Issue 3 - 2015
ISSN : 2381-8948 | www.austinpublishinggroup.com
Saxena et al. All rights are reserved
Figure 1: Point tenderness over the soft spot on the medial border of the
abductor hallucis.
Citation: Ellison T and Saxena S. Tarsal Tunnel Syndrome: An Overview. Austin J Musculoskelet Disord.
2015;2(3): 1022.
Saxena S
Austin Publishing Group
However, Yalcinkaya et al. report use of EMG and NCS is crucial,
especially in separating TTS from lumbar radiculopathy [9]. False
negative electro diagnostic studies are not uncommon and, for best
results, should be used to support the physical exam [1-9].
Treatment
Figure 2: In the dorsiflexion-eversion test, the foot is dorsiflexed, everted and
held for 10-15 seconds.
a recent case report, an abnormal branch of the posterior tibial artery
penetrated the posterior tibial nerve leading to a vascular leash. The
artery created traction on the nerve leading to neuropathy and TTS.
This and other idiopathic intrinsic factors reduce operative success
rates [8]. Extrinsic factors may include trauma, foot malformations,
constrictive footwear, edema and iatrogenic TTS [1,4]. Hindfoot
varus or valgus malformations can create increased pressures in the
tarsal tunnel leading to TTS. Unfortunately, surgical correction of
Hindfoot varus, or a lateral calcaneal osteotomy, can lead to acute
iatrogenic TTS requiring immediate surgical release [11]. Despite the
differing etiologies, studies suggest TTS causes can be identified 6080% of the time with proper diagnostic imaging [1,4,8].
Diagnosis
The diagnosis of TTS is clinical. The Tinel, dorsiflexion-eversion
and Valleix tests all increase the sensitivity and specificity of the
physical exam. Tinels test, tapping repeatedly on the soft spot to elicit
symptoms of pain and/or hypoesthesia, has a reported sensitivity of
92%, specificity of 100% and a positive predictive value of 85% [3,9].
In the dorsiflexion-eversion test, the foot is dorsiflexed, everted
and held for 10-15 seconds (Figure 2). A positive test elicits TTS
symptoms. Kinoshita et al. studied the sensitivity and specificity
of the dorsiflexion-eversion test in 37 patients with TTS against 50
controls. The dorsiflexion-eversion test had a sensitivity of 97% as
43/44 TTS patients were clinically positive and a specificity of 100%
as 0/50 controls tested positive [12]. In addition to physical exam,
other diagnostic modalities include x-ray, MRI, Magnetic Resonance
Neurography (MRN), ultrasound (US) and electro diagnostic
studies such as electromyography (EMG) and Nerve Conduction
Studies (NCS). X-rays should be taken to rule out fracture and an
MRI has high sensitivity for space occupying lesions [2]. As MRN
has a sensitivity of 77-100% for detecting nerve irritation, it can
be especially useful in the setting of recurrent TTS [5,9]. A 2010
case report found US provided direct visualization of a ganglion
compressing the nerve and adequately localized the lesion for surgical
removal [13]. EMG and NCS use is controversial. Dellon reports
repetitive micro-trauma in normal activity can cause EMG and NCS
abnormalities in asymptomatic individuals, thus making it difficult
for these electro diagnostics to separate life events from true TTS [3].
Submit your Manuscript | www.austinpublishinggroup.com
Non-operative treatment of TTS consists of activity modification,
medications such as systemic NSAIDs and gabapentin, nerve
mobilization exercises, night splints and orthotic inserts [1,2]. Gould
recommends custom orthotics with specific channels to relieve
pressure on the medial and lateral plantar nerves [2]. Other less
established non-operative treatments include massage, taping and
stretching [1]. Nerve irritants, such as hot or cold compress and
vibrations, should be avoided [2]. Kavlak and Uygur studied nerve
mobilization exercises as an adjunctive non-opperative treatment.
The exercises altered the sensory components of TTS by reducing
Tinels sign and improving two-point discrimination, but had no
positive impact on strength or range of motion [6].While nonoperative care is usually considered to be conservative care, at times
surgical intervention can be the more conservative treatment [2].
For example, competitive athletes wishing to return to competition
may benefit from immediate surgical intervention, rather than initial
non-operative treatment. Kinoshita et al. studied 15 competitive
athletes, all of whom failed non-operative management and
required surgery to return to competition [7]. However, when not
treating competitive athletes, Gould suggests initial treatment be
non-operative unless there are indications for immediate surgery
including general neuropathy and radiculopathy on initial exam [2].
Operative intervention, however, usually follows failed non-operative
care. Operative intervention is difficult with varying success rates. The
surgery begins with a curved medial incision over the tarsal tunnel
followed by the complete release of the posterior tibial nerve at the
tarsal tunnel as well as the release of its lateral and medial plantar
branches [1-9]. Reichert et al. report a 71% surgical success rate
while other studies report success rates ranging broadly from 4496% [4].Yalcinkaya et al. attribute such high failure rates to incorrect
diagnosis, unidentified space occupying lesions, surgeon error
with inadequate release of all branches, operative re-bleeding with
subsequent adhesive neuritis as wells as idiopathic causes [9].Above
all, surgical success rates rely heavily on patient selection [1-10].
Discussion
Gould et al. suggest most patients suffering from TTS should
complete a trial of the non-operative treatments discussed above.
Upon completion of six weeks of non-operative treatment, physician
reassessment of the syndrome should be made. If the patient shows
symptom improvement, non-operative interventions should
continue. However, in the absence of improvement with patient
compliance with non-operative treatments, surgery is recommended
[2]. Patients with positive Tinels sign, space occupying lesions, less
than 12 months of symptoms and early mobilization are the best
surgical candidates [1-7]. Reichert et al. reported 87% of study patients
with a positive Tinels sign had good or very good surgical results
[4]. Furthermore, the most predictable positive surgical outcomes
occur when a space occupying lesion is identified and removed.
Surgical success is further improved with rapid intervention with the
best surgical results achieved when surgery was performed within
Austin J Musculoskelet Disord 2(3): id1022 (2015) - Page - 02
Saxena S
Austin Publishing Group
1 year, and preferably within 6 months, from onset of symptoms
[1-4]. Intraneural fibrosis leading to permanent nerve damage has
been suggested as the reason early intervention increases surgical
success [4-10]. Finally, early post-surgical mobilization also resulted
in successful surgical outcomes as early movement promotes nerve
gliding through the tarsal tunnel and decreased adhesions at the
surgical site [3,9]. Symptoms of 12 or more months, idiopathic factors
and rare anatomical abnormalities, such as a vascular leash, result in
the worst surgical outcomes [4,8].
Conclusion
TTS can be painfully debilitating. This clinical diagnosis is
enhanced with imaging and may be further supported by electro
diagnostic tests. Initial treatment is usually non-operative, but at
times, surgical intervention is indicated at the outset. The surgery
is difficult and the literature suggests patient selection is crucial for
positive surgical outcomes. Further, surgical success rates are highest
when surgery is performed within 12 months of symptom onset.
References
1. Ahmad M, Tsang K, Mackenney PJ, Adedapo AO. Tarsal tunnel syndrome: A
literature review. Foot Ankle Surg. 2012; 18:149-152.
2. Gould JS. Tarsal tunnel syndrome. Foot Ankle Clin. 2011; 16: 275-286.
3. Dellon AL. The four medial ankle tunnels: a critical review of perceptions of
tarsal tunnel syndrome and neuropathy. Neurosurg Clin N Am. 2008; 19: 629648.
Austin J Musculoskelet Disord - Volume 2 Issue 3 - 2015
ISSN : 2381-8948 | www.austinpublishinggroup.com
Saxena et al. All rights are reserved
Submit your Manuscript | www.austinpublishinggroup.com
4. Reichert P, Zimmer K2, Wnukiewicz W2, Kuliski S2, Mazurek P2, Gosk
J2. Results of surgical treatment of tarsal tunnel syndrome. Foot Ankle Surg.
2015; 21: 26-29.
5. Gould JS1. Recurrent tarsal tunnel syndrome. Foot Ankle Clin. 2014; 19: 451467.
6. Kavlak Y, Uygur F. Effects of nerve mobilization exercise as an adjunct
to the conservative treatment for patients with tarsal tunnel syndrome. J
Manipulative Physiol Ther. 2011; 34: 441-448.
7. Kinoshita M, Okuda R, Yasuda T, Abe M. Tarsal tunnel syndrome in athletes.
Am J Sports Med. 2006; 34: 1307-1312.
8. Kosiyatrakul A, Luenam S2, Phisitkul P3. Tarsal tunnel syndrome associated
with a perforating branch from posterior tibial artery: a case report. Foot Ankle
Surg. 2015; 21: e21-22.
9. Yalcinkaya M, Ozer UE2, Yalcin MB2, Bagatur AE3. Neurolysis for failed
tarsal tunnel surgery. J Foot Ankle Surg. 2014; 53: 794-798.
10. Takakura Y, Kitada C, Sugimoto K, Tanaka Y, Tamai S. Tarsal tunnel
syndrome. Causes and results of operative treatment. J Bone Joint Surg Br.
1991; 73: 125-128.
11. Walls RJ, Chan JY2, Ellis SJ2. A case of acute tarsal tunnel syndrome
following lateralizing calcaneal osteotomy. Foot Ankle Surg. 2015; 21: e1-5.
12. Kinoshita M, Okuda R, Morikawa J, Jotoku T, Abe M. The dorsiflexioneversion test for diagnosis of tarsal tunnel syndrome. J Bone Joint Surg Am.
2001; 83-83A: 1835-1839.
13. Therimadasamy AK, Seet RC, Kagda YH, Wilder-Smith EP. Combination
of ultrasound and nerve conduction studies in the diagnosis of tarsal tunnel
syndrome. Neurol India. 2011; 59: 296-297.
Citation: Ellison T and Saxena S. Tarsal Tunnel Syndrome: An Overview. Austin J Musculoskelet Disord.
2015;2(3): 1022.
Austin J Musculoskelet Disord 2(3): id1022 (2015) - Page - 03
You might also like
- Naspub PDFDocument12 pagesNaspub PDFAbdillah AziziNo ratings yet
- New Perspectives On Neurogenic Thoracic Outlet SyndromeDocument10 pagesNew Perspectives On Neurogenic Thoracic Outlet SyndromeMourning_WoodNo ratings yet
- Entrapmentneuropathiesof Theupperextremity: Christopher T. Doughty,, Michael P. BowleyDocument14 pagesEntrapmentneuropathiesof Theupperextremity: Christopher T. Doughty,, Michael P. BowleydwiNo ratings yet
- Carpal Tunnel Syndrome - Clinical Manifestations and Diagnosis - UpToDateDocument19 pagesCarpal Tunnel Syndrome - Clinical Manifestations and Diagnosis - UpToDatefarhatullahsialNo ratings yet
- Carpal Tunnel Syndrome (CTS) Is When Symptoms Occur Due ToDocument8 pagesCarpal Tunnel Syndrome (CTS) Is When Symptoms Occur Due ToGio Vano NaihonamNo ratings yet
- Diagnosis and Management of The PainfulDocument32 pagesDiagnosis and Management of The PainfulDeanNo ratings yet
- Achilles TendinopathyDocument42 pagesAchilles TendinopathyAlberto GallariniNo ratings yet
- NDS in TTSDocument8 pagesNDS in TTSCornerstone OrganizationNo ratings yet
- The Triple Compression Stress Test For Diagnosis of Tarsal Tunnel SyndromeDocument4 pagesThe Triple Compression Stress Test For Diagnosis of Tarsal Tunnel SyndromeSemut BarbarNo ratings yet
- Tarsal Tunnel Syndrome - Physiopedia, Universal Access To Physiotherapy KnowledgeDocument9 pagesTarsal Tunnel Syndrome - Physiopedia, Universal Access To Physiotherapy KnowledgeMuhammad Sahrul PatunruNo ratings yet
- Carpal Tunnel SyndromeDocument2 pagesCarpal Tunnel SyndromeHejar A.No ratings yet
- Physiotherapy Management for Tennis Elbow Provides Pain Relief and Improved Muscle StrengthDocument12 pagesPhysiotherapy Management for Tennis Elbow Provides Pain Relief and Improved Muscle Strengthririn rahmayeniNo ratings yet
- Results of Surgical TreatmentDocument4 pagesResults of Surgical TreatmentChristine Yohana SianturiNo ratings yet
- Sesek NORA Paper 2003Document12 pagesSesek NORA Paper 2003damarliNo ratings yet
- Cumulative Trauma InjuriesDocument4 pagesCumulative Trauma InjuriesSanchita SumanNo ratings yet
- Tarsal Tunnel Syndrome:: A Clinical Management GuidelineDocument2 pagesTarsal Tunnel Syndrome:: A Clinical Management GuidelineAnna FaNo ratings yet
- Entrapment Neuropathies Conversion-GateDocument76 pagesEntrapment Neuropathies Conversion-GateRam ReddyNo ratings yet
- Strain Counter-Strain PDFDocument7 pagesStrain Counter-Strain PDFCarlosCarpinteroRubioNo ratings yet
- 2014 The Pain of Tendinopathy - Physiological or PathophysiologicalDocument15 pages2014 The Pain of Tendinopathy - Physiological or PathophysiologicalDavid Alejandro Cavieres AcuñaNo ratings yet
- Carpal Tunnel Syndrome - A ReviewDocument10 pagesCarpal Tunnel Syndrome - A ReviewkenthepaNo ratings yet
- Sensors: Neurological Tremor: Sensors, Signal Processing and Emerging ApplicationsDocument24 pagesSensors: Neurological Tremor: Sensors, Signal Processing and Emerging ApplicationsMuhammad Ali JoharNo ratings yet
- Effects of Tendon An Nerve Gliding Exercises and Instructions in Activities of Daily Livin Following Endoscopic Carpal Tunnel ReleaseDocument7 pagesEffects of Tendon An Nerve Gliding Exercises and Instructions in Activities of Daily Livin Following Endoscopic Carpal Tunnel ReleaseYimena JoyNo ratings yet
- Ntos Update FinalDocument8 pagesNtos Update FinalMisa AjversonNo ratings yet
- Carpal tunnel syndrome symptoms and causesDocument15 pagesCarpal tunnel syndrome symptoms and causesMalueth AnguiNo ratings yet
- Dislocation of the Temporomandibular Joint: A Guide to Diagnosis and ManagementFrom EverandDislocation of the Temporomandibular Joint: A Guide to Diagnosis and ManagementNigel Shaun MatthewsNo ratings yet
- Carpal Tunnel SyndromeDocument37 pagesCarpal Tunnel SyndromePramadya Vardhani MustafizaNo ratings yet
- Thoracic Outlet SyndromeDocument13 pagesThoracic Outlet SyndromeNada AymanNo ratings yet
- Restore Scapula Control for Thoracic Outlet SyndromeDocument10 pagesRestore Scapula Control for Thoracic Outlet Syndromercastello20No ratings yet
- 02.elbow PainDocument62 pages02.elbow PainKhushboo IkramNo ratings yet
- Carpal Tunnel Syndrome InforDocument5 pagesCarpal Tunnel Syndrome InforAnonymous uTEAEbugNo ratings yet
- Protocol AchillesTendinosisDocument11 pagesProtocol AchillesTendinosisPhooi Yee LauNo ratings yet
- Chapter 8 - Clinical Examination of The ElbowDocument3 pagesChapter 8 - Clinical Examination of The ElbowkenthepaNo ratings yet
- Conf 06 Ron Phelan TMJDocument14 pagesConf 06 Ron Phelan TMJtugurlanNo ratings yet
- Herniated Nucleus Pulposus TreatmentDocument19 pagesHerniated Nucleus Pulposus Treatmentvicky174No ratings yet
- ESWT and TTSDocument7 pagesESWT and TTSCornerstone OrganizationNo ratings yet
- Naskah PublikasiDocument10 pagesNaskah PublikasiJoses DimesNo ratings yet
- Effects of Transcutaneous Electrical Nerve Stimulation On Pain Pain Sensitivity and Function in People With Knee Osteoarthritis. A Randomized Controlled TrialDocument14 pagesEffects of Transcutaneous Electrical Nerve Stimulation On Pain Pain Sensitivity and Function in People With Knee Osteoarthritis. A Randomized Controlled TrialLorena Rico ArtigasNo ratings yet
- IVDP & Spinal SurgeriesDocument7 pagesIVDP & Spinal Surgeriesbbpanicker67% (3)
- Mechanisms of TENSDocument13 pagesMechanisms of TENSOana Budugan0% (1)
- Neuro DynamicsDocument12 pagesNeuro Dynamicsimamhanzala389No ratings yet
- Ultrasound and clinically guided Injection techniques on the musculoskeletal systemFrom EverandUltrasound and clinically guided Injection techniques on the musculoskeletal systemNo ratings yet
- HNPDocument7 pagesHNPLyka Mae Imbat - Pacnis100% (1)
- Ringkasan TBR TTSDocument3 pagesRingkasan TBR TTSbeirnesNo ratings yet
- Acupuntura para La RodillaDocument9 pagesAcupuntura para La Rodillaoscarin123456789No ratings yet
- Trigger FingerDocument13 pagesTrigger FingerEspers BluesNo ratings yet
- MANAGEMENT OF PHYSIOTHERAPY IN ISCHIALGIA SINISTRA DUE TO HERNIA NUCLEUS PULPOSUS (HNP) AT PKU MUHAMMADIYAH HOSPITAL YOGYAKARTADocument15 pagesMANAGEMENT OF PHYSIOTHERAPY IN ISCHIALGIA SINISTRA DUE TO HERNIA NUCLEUS PULPOSUS (HNP) AT PKU MUHAMMADIYAH HOSPITAL YOGYAKARTAharrylukitoNo ratings yet
- Naskah PublikasiDocument15 pagesNaskah PublikasiSuci AisyahNo ratings yet
- Leg Ankle Orthopaedic Conditions FinalDocument26 pagesLeg Ankle Orthopaedic Conditions Finalangel bolfriNo ratings yet
- Lumbar Disk HerniationDocument6 pagesLumbar Disk HerniationSyarifah Nadya ArfadNo ratings yet
- Spinous Process Tenderness Syndrome - A Newly Discovered DisorderDocument2 pagesSpinous Process Tenderness Syndrome - A Newly Discovered DisorderMichele MarengoNo ratings yet
- Carpal Tunnnel Syndrome: EtiologyDocument3 pagesCarpal Tunnnel Syndrome: EtiologyEga FlorenceNo ratings yet
- Extracorporeal Shock Wave Therapy For Sacroiliac Joint Pain: A Prospective, Randomized, Sham-Controlled Short-Term TrialDocument7 pagesExtracorporeal Shock Wave Therapy For Sacroiliac Joint Pain: A Prospective, Randomized, Sham-Controlled Short-Term TrialLizeth Tatiana Ortiz PalominoNo ratings yet
- Effectiveness of Eccentric Exercise in Tennis Elbow - A Single CaseDocument2 pagesEffectiveness of Eccentric Exercise in Tennis Elbow - A Single Caseirfan setiadiNo ratings yet
- Obstetrics & Gynaecology Unit Seminar Presented byDocument37 pagesObstetrics & Gynaecology Unit Seminar Presented byNana BabalolaNo ratings yet
- Joint Contractures Dr. JalalinDocument16 pagesJoint Contractures Dr. JalalinRestya FitrianiNo ratings yet
- Diagnosing Pronator SyndromeDocument6 pagesDiagnosing Pronator SyndromeMplusWNo ratings yet
- Knardahl 1998Document7 pagesKnardahl 1998Nurul AzizahNo ratings yet
- Carpal Tunnel SyndromeDocument19 pagesCarpal Tunnel Syndromekln.cheran100% (2)
- RCT ThesisDocument42 pagesRCT ThesismohiiieNo ratings yet
- Explaining Stroke 101Document29 pagesExplaining Stroke 101Christopher AdhisasmitaNo ratings yet
- Exercises for older people - NHSDocument14 pagesExercises for older people - NHSFaishal HanifNo ratings yet
- PsikiatriDocument8 pagesPsikiatriFaishal HanifNo ratings yet
- Management of Dyslipidemia in Adults - American Family PhysicianDocument9 pagesManagement of Dyslipidemia in Adults - American Family PhysicianFaishal HanifNo ratings yet
- PsikiatriDocument9 pagesPsikiatriFaishal HanifNo ratings yet
- Manajemen Hipoglikemia Nhs PDFDocument28 pagesManajemen Hipoglikemia Nhs PDFFaishal HanifNo ratings yet
- Language Development and Deaf Children 2012 v2 1Document6 pagesLanguage Development and Deaf Children 2012 v2 1Faishal HanifNo ratings yet
- Stroke PDFDocument15 pagesStroke PDFFaishal HanifNo ratings yet
- Buku Pedoman Nasional Penanggulangan TBCDocument131 pagesBuku Pedoman Nasional Penanggulangan TBCHasrapriliana Hersya100% (1)
- ASD Best Practice2002 PDFDocument193 pagesASD Best Practice2002 PDFNST MtzNo ratings yet
- Twins and Speech Delay PDFDocument11 pagesTwins and Speech Delay PDFFaishal HanifNo ratings yet
- FIGOCEDocument11 pagesFIGOCEAldwin TanuwijayaNo ratings yet
- Posterior TtsDocument6 pagesPosterior TtsFaishal HanifNo ratings yet
- Vbac StatementDocument48 pagesVbac StatementFaishal HanifNo ratings yet
- IUGR New Concepts - AJOG ReviewDocument13 pagesIUGR New Concepts - AJOG ReviewHanarisha Putri AzkiaNo ratings yet
- 8 CPG DyslipidemiaDocument10 pages8 CPG DyslipidemiaFaishal HanifNo ratings yet
- Eighth Joint National Committee JNC 8Document14 pagesEighth Joint National Committee JNC 8caluca1987No ratings yet
- Alcoholic KetoacidosisDocument3 pagesAlcoholic KetoacidosisFaishal HanifNo ratings yet
- TTS OverviewDocument3 pagesTTS OverviewFaishal HanifNo ratings yet
- Peroneal PalsyDocument7 pagesPeroneal PalsyriswanfebriantoNo ratings yet
- 8 CPG DyslipidemiaDocument10 pages8 CPG DyslipidemiaFaishal HanifNo ratings yet
- Tunnel: Thrsal SyndromeDocument3 pagesTunnel: Thrsal Syndromesatyagraha84No ratings yet
- Fisioterapi Pada CTSDocument2 pagesFisioterapi Pada CTSFaishal HanifNo ratings yet