Professional Documents
Culture Documents
Diagnosis of Common, Benign Neonatal Dermatoses: Daniel Wallach, MD
Uploaded by
Desi RatnaningtyasOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Diagnosis of Common, Benign Neonatal Dermatoses: Daniel Wallach, MD
Uploaded by
Desi RatnaningtyasCopyright:
Available Formats
Diagnosis of Common, Benign
Neonatal Dermatoses
DANIEL WALLACH, MD
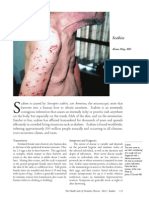
eonatal dermatology is a growing field of medical knowledge. Excellent, comprehensive reviews of this field have been published recently.1,2 This article deals with a number of benign,
cutaneous conditions that are frequently observed in
the newborn. These conditions are of no medical consequence; they have also been called nondiseases of the
newborn. It is, however, important to identify them
correctly to avoid parental concern as well as unnecessary diagnostic or therapeutic aggressive procedures.
Normal Neonatal Skin
Inasmuch as benign neonatal dermatoses may be considered variations from the normal, it is important to
describe in detail the appearance of the normal skin at
birth. The appearance of neonatal skin depends on the
maturity of the newborn. In full-term newborns (gestational age 37-40 weeks), the skin is pink or pink-light
brown in children of African ancestry. It is opaque, soft,
and velvety. In prematurs, the skin is thinner, lacking
the external keratinized layer, and may be gelatinous,
glistening, or translucent. In postterm newborns, desquamation is prominent.
The skin at birth is covered with a white, greasy
coating called vernix caseosa; it is abundant mainly in
infants born at full term. The vernix caseosa is mainly
made of lipids deriving from the epidermis and sebaceous secretions; it may cover the whole body or only
the back and skinfold areas. Vernix caseosa is thought
to represent a barrier between the fetal epidermis and
the amniotic fluid. The vernix caseosa dries out after a
few hours but is usually wiped out as routine neonatal
care; in case of fetal distress, the vernix is stained yellow
or brown by contact with the meconium.
Routine Skin Care of the Full-Term Newborn
Bathing in 37C water and gentle cleansing with clean
hands, using a nonmedicated, mild syndet bar or liquid
cleanser, is advisable.3,4 Massage of the skin with a
bland emollient is beneficial in prematures5; in full-term
From the Department of Dermatology, Hopital Tarnier-Cochin, Paris,
France.
Address correspondence to Daniel Wallach, MD, Department of Dermatology, Hopital Tarnier-Cochin, 89 rue dAssas, 75006 Paris, France.
E-mail address: dwallach@noos.fr
2003 by Elsevier Inc. All rights reserved.
360 Park Avenue South, New York, NY 10010
newborns, there is no medical reason to neither recommend nor forbid it. There are as yet no accepted guidelines for umbilical cord care. As a consequence, many
uncontrolled techniques are currently in use; cleansing
with an aqueous chlorhexidine solution appears to be
the best current recommendation.6
Regular use of disposable, absorbant diapers has
made diaper dermatitis much rarer than it was when
cloth diapers were used. Diapers must be changed as
often as necessary (about 10 times daily in a newborn),
as contact with the urine and feces is the main cause of
diaper dermatitis. In addition to gentle cleansing, application of a protective emollient or paste is useful as a
barrier to protect the skin in the diaper area. In case of
erythema, topical antifungals are often recommended
to prevent infection.
Physiologic Desquamation
Full-term newborns often exhibit a fine, diffuse scaling,
starting from the second day of life and lasting a few
days (Fig 1); this scaling may be reduced by the application of emollient creams. When intense, physiologic
desquamation may appear ichthyosiform, but the rare
neonatal ichthyoses are very different, exhibiting continuous scaling with an underlying erythematous skin.
In the peeling skin syndrome, large sheets of skin are
removed, and the condition is long-lasting.
Milia
Milia are tiny, epidermal inclusion cysts due to retention of keratin at the extremity of hair follicles; they
occur almost exclusively on the face, although at times
some may be seen on the genital areas. Milia may be
very numerous (Fig 2) but desquamate spontaneously,
and no intervention is indicated. Widespread or lasting
milia are part of rare developmental syndromes such as
orofacialdigital syndrome type I or Marie Unna hypotrichosis. Epsteins pearls are tiny, palatal cysts, similar
to milia.
Miliaria
Miliaria is the consequence of sweat retention in immature, impermeable eccrine ducts. Sweating in newborns
occurs only in term infants and must lead to the correction of excessive environmental temperature or re0738-081X/03/$see front matter
doi:10.1016/S0738-081X(03)00049-X
Clinics in Dermatology
2003;21:264 268
DIAGNOSIS OF COMMON BENIGN NEONATAL DERMATOSES
Figure 1. Physiologic desquamation in a newborn, gestational
age 40 weeks.
moval of clothing. Miliaria crystallina appears as tiny,
translucid vesicles; inflammation induces peripheral erythema, known as miliaria rubra (Fig 3); in case of
superinfection, miliaria becomes pustular.
Cutaneous Consequences of
hormonal transition
During the last weeks of gestation, the fetus receives
important hormonal influences from the mother and
the placenta. At birth, this influence ceases abruptly,
and this cessation transiently stimulates the neonatal
endocrine system. All this endocrine transition has
visible consequences on the skin.
265
Figure 3. Miliaria rubra.
sient hyperplasia seems to be unrelated to neonatal
acne.
Neonatal Acne
Neonatal acne is a consequence of transient neonatal
androgen excess; very rarely, it can be due to congenital
adrenal hyperplasia or to a gonadal or adrenal tumor.
Neonatal acne predominates on the cheeks. Although
papules, pustules, and small nodules may be more
visible, the specific lesion is the comedo (Fig 5). Except
in a few instances, neonatal acne resolves in few weeks;
topical antimicrobial therapy is usually prescribed.
Sebaceous Gland Hyperplasia
As a consequence of the influence of maternal androgens, the sebaceous glands on the nose and central face
are often enlarged, and the openings of the follicles
appear as pinpoint, yellowish papules (Fig 4). This tran-
Figure 2. Numerous milia.
Figure 4. Hyperplasia of the sebaceous glands of the nose.
Clinics in Dermatology
266 WALLACH
Figure 5. Acne neonatorum.
Pseudopuberty of the Newborn
This transient consequence of stimulation by sexual
hormones is seen in both sexes. In girls, one may see
hyperpigmentation of the linea alba and of the external
genitalia; edema of the labia majora; vaginal discharge,
usually whitish, rarely hemorrhagic (pseudomenses);
and hypertrophy of the mammary glands, with the
possibility of a milky secretion for a few days. Mastitis
and abscess can occur, especially in cases of inadequate
manipulation. In boys, genitalia may similarly appear
to be of abnormally large size during the neonatal
period.
Figure 6. Physiologic cutis marmorata.
2003;21:264 268
Figure 7. Erythema toxicum.
Consequences of Vascular Immaturity
The change from the intra-amniotic to the aerial environment implies dramatic modifications in vasomotor
tone; some instability of the cutaneous vascularization
in the neonatal period may be visible.
Normal Skin Color
Many pathologic conditions may alter skin color: circulatory or respiratory distress, anemia, polycythemia,
jaundice, and so forth. In the absence of any of these
conditions, normal skin color at birth is associated with
Figure 8. A florid pustulosis due to Malassezia on the face of a
healthy newborn. Topical antifungal therapy led to complete cure
in 3 days.
Clinics in Dermatology
2003;21:264 268
central erythema and peripheral cyanosis. Ethnic pigmentation is usually delayed.
Cutis Marmorata
Cutis marmorata (mottled skin) is a normal reaction to
cold in newborns, and it disappears with warming (Fig
6). Physiologic neonatal cutis marmorata must be differentiated from cutis marmorata telangiectatica congenita.7 In this rare vascular anomaly, mottling of the
skin is more marked, permanent, and associated with
areas of atrophy, ulceration, and other lesions. Systemic
malformations and mental retardation are rarely associated.
DIAGNOSIS OF COMMON BENIGN NEONATAL DERMATOSES
267
other neonatal pustuloses (Fig 8). The almost unique
location is the face (cheeks, forehead), but occasional
lesions may be seen on the neck, nape, or chest. The
main differential diagnosis is neonatal acne, but in this
condition, comedones are always present and lesions
are more durable. It is likely that many cases diagnosed
as neonatal acne were in fact Malassezia-induced pustulosis, also called neonatal cephalic pustulosis. Direct
microscopic examination shows Malassezia furfur, and
topical antifungals clear the eruption in a few days. The
spontaneous course is not known but is thought to be
self-limited.
Hair and Nail Conditions
Harlequin Color Change
Lanugo
The difference in skin coloration between the upper and
lower half of body may be seen during episodes lasting
a few minutes; it is the most spectacular manifestation
of neonatal vascular immaturity. Its observation is limited to the first days of life.
Lanugo is a vellus, unpigmented body hair. It is mainly
abundant in prematures (28-30 weeks gestational age);
the importance of lanugo is not predictive of later body
hair, which depends mainly on familial and ethnic patterns.
Erythema Toxicum
Scalp Hair Growth
Erythema toxicum is the most common of all neonatal
dermatoses. Its pathogenesis is unknown, and the word
toxicum does not indicate any toxicity. Erythema
toxicum occurs in about half of term neonates, and only
atypical forms attract dermatologic attention. It is not
present at birth, begins after the first day of life, and
usually lasts about 1 week. The lesions predominate on
the trunk and proximal parts of the limbs; they are
typically large (1-3 cm), erythematous macules and
papules; the center of the lesion is more elevated than
the periphery and at times, may be marked by a small
vesicle or even a pustule (Fig 7). Some lesions are
purely vesicular or pustular, lacking the erythematous
component. In these cases, one may need confirmation
of the diagnosis by showing the eosinophilic content of
the liquid lesions on Tzancks smear. There is also a
blood hypereosinophilia, the signification of which is
unknown.
Transient neonatal pustular melanosis, which is
more frequent in black newborns, is considered a variant of erythema toxicum,8 with hyperpigmented sequelar macules lasting for some weeks.
Most newborns have abundant terminal scalp hair; the
normal cycle of individual growth and fall is not yet
established, and synchronized telogen effluvium may
occur during the first months of life, followed by normal regrowth. A transient, occipital alopecia is frequent; it is probably favored by repeated rubbing on the
bed.
Neonatal Cephalic
(Malassezia-Induced) Pustulosis
A benign facial neonatal pustulosis induced by Malassezia species has recently been described9 and is probably
not rare.10 Malassezia-induced neonatal pustulosis usually starts between the ages of 7 and 30 days. It appears
as numerous, small, erythematous pustules on erythematous bases and in fact is clinically different from
Nails
The length of nails at birth is one of the indicators of the
duration of gestation, and postterm babies have long
nails. Newborn nails are usually small and soft, mainly
on the toes, and the surrounding skin may cover the
nails edges (pseudoingrown toenails). Except in cases
of scratching, nails must not be cut and in no instance
cut too short.
Nodular Fat Necrosis
Idiopathic panniculitis, known as nodular fat necrosis
of the newborn, is seen after difficult labor and delivery,
especially when the baby has suffered from hypoxia
and hypothermia; it also occurs in the absence of any
identifiable cause. Lesions are usually located on the
upper part of the posterior trunk. The buttocks, arms,
and legs may also be involved. Lesions are palpable as
subcutaneous, indurated masses; the overlying skin is
usually red. The main differential diagnosis is neonatal
sclerema, a diffuse induration of the skin occurring in
severely ill neonates. In contrast, babies with nodular
fat necrosis remain in good health. Nodular fat necrosis
heals in a few weeks; hypercalcemia has been reported
268 WALLACH
and must be prevented and monitored. Infection is very
rare.
References
1. Wagner AM, Hansen RC. Neonatal skin and skin disorders. In: Schachner LA, Hansen RC, editors. Pediatric
dermatology, 2nd edition. New York: Churchill Livingstone, 1995:236 46.
2. Eichenfield LF, Frieden IJ, Esterly NB. Textbook of neonatal dermatology. Philadelphia: Saunders, 2001.
3. Siegfried EC. Neonatal skin and skin care. Dermatol Clin
1998;16:43746.
4. Liou LW, Janniger CK. Skin care of the normal newborn.
Cutis 1997;59:1714.
5. Hoath SB, Narendran V. Adhesives and emollients in the
preterm infant. Semin Neonatol 2000;5:289 96.
Clinics in Dermatology
2003;21:264 268
6. Verber IG, Pagan FS. What cord care, if any? Arch Dis
Child 1993;68:594 6.
7. Picascia DD, Esterly NB. Cutis marmorata telangiectatica
congenita: report of 22 cases. J Am Acad Dermatol 1989;
20:1098 104.
8. Ferrandiz C, Coroleu W, Ribera M, et al. Sterile transient neonatal pustulosis is a precocious form of erythema toxicum neonatorum. Dermatology 1992;185:18
22.
9. Aractingi S, Cadranel S, Reygagne P, Wallach D. Pustulose ne o-natale induite par Malassezia furfur. Ann Dermatol Ve ne re ol 1991;118:856 8.
10. Bernier V, Weill FX, Hirigoyen V, et al. Skin colonization
by Malassezia species in neonates: a prospective study and
relationship with neonatal cephalic pustulosis. Arch Dermatol 2002;138:2158.
You might also like
- Neonatal Skin Disorders and The Emergency Medicine Physician PDFDocument10 pagesNeonatal Skin Disorders and The Emergency Medicine Physician PDFsamerdkhNo ratings yet
- Commonrashes in Neonates201205suDocument6 pagesCommonrashes in Neonates201205suDanielcc LeeNo ratings yet
- Pediatric Dermatology Lecture HandoutDocument62 pagesPediatric Dermatology Lecture Handoutskin_docNo ratings yet
- Disorders of Pigmentation 1Document56 pagesDisorders of Pigmentation 1Ahmed Noureldin AhmedNo ratings yet
- A Guide To Neonatal RashesDocument8 pagesA Guide To Neonatal RashesdragajojicNo ratings yet
- Paediatric DermatologyDocument12 pagesPaediatric DermatologyDuranka PereraNo ratings yet
- MCN NBDocument6 pagesMCN NBJudy BaguiwenNo ratings yet
- Pathophysiology and Impact of Acne Vulgaris (38 charactersDocument6 pagesPathophysiology and Impact of Acne Vulgaris (38 charactersPrajnamita Manindhya El FarahNo ratings yet
- Pediatric DermatosesDocument58 pagesPediatric DermatosesSajin AlexanderNo ratings yet
- Vitiligo: Refer ATDocument18 pagesVitiligo: Refer ATAndhika FrabesNo ratings yet
- The Mcmaster Pediatric Curriculum: at NightDocument39 pagesThe Mcmaster Pediatric Curriculum: at NightyumizoneNo ratings yet
- Eyelid Disorders - Diagnosis and Management - AAFPDocument15 pagesEyelid Disorders - Diagnosis and Management - AAFPMufassiraturrahmahNo ratings yet
- Derm Online Resource Pack PDFDocument81 pagesDerm Online Resource Pack PDFOlaNo ratings yet
- Common Paediatric Skin Conditions & BirthmarksDocument10 pagesCommon Paediatric Skin Conditions & Birthmarksdr.nadia sharifNo ratings yet
- Scabies Diagnosis and ManagementDocument5 pagesScabies Diagnosis and ManagementAbdul Rauf ZakariaNo ratings yet
- Meth Elab Topic N2Document19 pagesMeth Elab Topic N2Group M1869No ratings yet
- Genodermatosis: The IchthyosisDocument4 pagesGenodermatosis: The IchthyosisOman ArifNo ratings yet
- GENOVE, ERICKA IS-Module2Document11 pagesGENOVE, ERICKA IS-Module2Ericka GenoveNo ratings yet
- Psoriasis: Posted: 02 Aug 2010 11:18 PM PDTDocument5 pagesPsoriasis: Posted: 02 Aug 2010 11:18 PM PDTScamb TrekNo ratings yet
- 2021 - Neonatal Dermatology The Normal, The Common and The SeriousDocument14 pages2021 - Neonatal Dermatology The Normal, The Common and The SeriousnancyerlenNo ratings yet
- The Essential Role of Eyelids in Eye HealthDocument96 pagesThe Essential Role of Eyelids in Eye HealthArwa QishtaNo ratings yet
- Vesicular, Pustular, and Bullous Lesions in The Newborn and InfantDocument18 pagesVesicular, Pustular, and Bullous Lesions in The Newborn and InfantMirela Marina BlajNo ratings yet
- Psoriasis Case StudyDocument4 pagesPsoriasis Case StudyMIKAELLA BALUNANNo ratings yet
- Toacs 4Document211 pagesToacs 4Mobin Ur Rehman Khan100% (1)
- Pediatric and Adolescent Gynecology 2015Document25 pagesPediatric and Adolescent Gynecology 2015hasiNo ratings yet
- Robinson HC CT105003132Document5 pagesRobinson HC CT105003132Francesca BizzocoNo ratings yet
- DermatitisDocument61 pagesDermatitisAlex XanderNo ratings yet
- Neonatal Dermatology PDFDocument67 pagesNeonatal Dermatology PDFAlejananaNo ratings yet
- Atopic Dermatitis PresentsiDocument17 pagesAtopic Dermatitis PresentsianniNo ratings yet
- 5: Allergy and The Skin: Eczema and Chronic Urticaria: Mja Practice Essentials - AllergyDocument6 pages5: Allergy and The Skin: Eczema and Chronic Urticaria: Mja Practice Essentials - AllergyDavid PattersonNo ratings yet
- Derma Slides 2017Document268 pagesDerma Slides 2017Nadia AlmahalawiNo ratings yet
- Case Study IGDocument2 pagesCase Study IGCheha PaikNo ratings yet
- Dermatitis: Management: Diaper Differential andDocument4 pagesDermatitis: Management: Diaper Differential andRatna OktavianiNo ratings yet
- DermatitisDocument5 pagesDermatitisAzriatul Farahain Ahmad ZamiliNo ratings yet
- Nursing Management of Common Skin and Parasitic DiseasesDocument14 pagesNursing Management of Common Skin and Parasitic Diseasesyer tagalajNo ratings yet
- Skin and Parasitic DiseasesDocument14 pagesSkin and Parasitic DiseasesduapajNo ratings yet
- Birthmarks Identificationandmx201205ryanDocument4 pagesBirthmarks Identificationandmx201205ryanDanielcc LeeNo ratings yet
- ScabiesDocument4 pagesScabiesGenita Savitri EkandariNo ratings yet
- Skin Pigmentation + Hari DisorderDocument113 pagesSkin Pigmentation + Hari DisorderAfiqah So JasmiNo ratings yet
- Master Plan Onn Skin DisordersDocument5 pagesMaster Plan Onn Skin DisordersSakthi DeviNo ratings yet
- Eyelid inflammation guideDocument15 pagesEyelid inflammation guideLatoya ShopNo ratings yet
- ScienceDocument1 pageScienceni putu.comsurya dianaNo ratings yet
- Lupus ErythematosusDocument3 pagesLupus ErythematosusAMOS MELINo ratings yet
- Histology For JordanianDocument24 pagesHistology For JordanianKhaldoun AlmomaniNo ratings yet
- Tinea Versicolor: Pathophysiology, Etiology in <40 CharsDocument4 pagesTinea Versicolor: Pathophysiology, Etiology in <40 Charswahyuni taslimNo ratings yet
- Continuing Medical Education: Amanda M M Oakley MBCHB Fracp DiphealinfDocument4 pagesContinuing Medical Education: Amanda M M Oakley MBCHB Fracp DiphealinfCarol SantosNo ratings yet
- Atopic EczemaDocument8 pagesAtopic EczemaMohamed OmerNo ratings yet
- Nursing Management of Common Skin ConditionsDocument4 pagesNursing Management of Common Skin Conditionsstudyhard001No ratings yet
- Vitiligo (: UVB PhototherapyDocument5 pagesVitiligo (: UVB PhototherapyneeeeeeeeeeshaNo ratings yet
- Muallem 2006Document4 pagesMuallem 2006winda ayundariNo ratings yet
- Acne and Rosacea: AetiologyDocument7 pagesAcne and Rosacea: AetiologyananNo ratings yet
- Guide to Common Skin ConditionsDocument93 pagesGuide to Common Skin Conditionsneha100% (5)
- Acne Vulgaris Clinical FeaturesDocument22 pagesAcne Vulgaris Clinical FeaturesHanako AranillaNo ratings yet
- Jadotte Pityriasis AlbaDocument8 pagesJadotte Pityriasis Albapene asoyNo ratings yet
- Pityriasis AlbaDocument7 pagesPityriasis AlbaAri Kurniawan100% (1)
- Pityriasis Alba: Are You Confident of The Diagnosis?Document3 pagesPityriasis Alba: Are You Confident of The Diagnosis?freska ayu wardhaniNo ratings yet
- Sebaceous Cyst, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandSebaceous Cyst, A Simple Guide To The Condition, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Jurnal Stress OksidatifDocument8 pagesJurnal Stress OksidatifDesi RatnaningtyasNo ratings yet
- Antioxidants 06 00095Document11 pagesAntioxidants 06 00095Desi RatnaningtyasNo ratings yet
- Antioxidants 06 00095Document11 pagesAntioxidants 06 00095Desi RatnaningtyasNo ratings yet
- Patch Test DrugDocument9 pagesPatch Test DrugDesi RatnaningtyasNo ratings yet
- Patch Test DrugDocument9 pagesPatch Test DrugDesi RatnaningtyasNo ratings yet
- Correlation Serum Zink With AVDocument7 pagesCorrelation Serum Zink With AVwe sagara dewiNo ratings yet
- A Prospective Split Face Double Blinded Randomized Study of The Efficacy and Safety of A Fractional 1064 NM Q Switched ND YAG Laser For PhotoagingDocument7 pagesA Prospective Split Face Double Blinded Randomized Study of The Efficacy and Safety of A Fractional 1064 NM Q Switched ND YAG Laser For PhotoagingDesi RatnaningtyasNo ratings yet
- Section6 Psoriasis Guideline PDFDocument38 pagesSection6 Psoriasis Guideline PDFDesi RatnaningtyasNo ratings yet
- Adolescent Acne Treatment Options OverviewDocument3 pagesAdolescent Acne Treatment Options OverviewDesi RatnaningtyasNo ratings yet
- Nbuvb VS MTXDocument5 pagesNbuvb VS MTXDesi RatnaningtyasNo ratings yet
- Histo PA AspergilosisDocument34 pagesHisto PA AspergilosisDesi RatnaningtyasNo ratings yet
- Antioxidants 06 00095Document11 pagesAntioxidants 06 00095Desi RatnaningtyasNo ratings yet
- Efficacy Caspofungin in AspergilosisDocument9 pagesEfficacy Caspofungin in AspergilosisDesi RatnaningtyasNo ratings yet
- UV Radiation and Skin PDFDocument27 pagesUV Radiation and Skin PDFDesi RatnaningtyasNo ratings yet
- AspergillosisDocument34 pagesAspergillosisvilla88No ratings yet
- AspergillosisDocument34 pagesAspergillosisvilla88No ratings yet
- Angiogenic 1Document15 pagesAngiogenic 1Desi RatnaningtyasNo ratings yet
- Aspergillosis Among People Infected With Human Immunodeficiency VirusDocument5 pagesAspergillosis Among People Infected With Human Immunodeficiency VirusDesi RatnaningtyasNo ratings yet
- Aspergillosis PathologyDocument2 pagesAspergillosis PathologyDesi RatnaningtyasNo ratings yet
- Non Ablative LaserDocument12 pagesNon Ablative LaserDesi RatnaningtyasNo ratings yet
- Efficacy Caspofungin in AspergilosisDocument9 pagesEfficacy Caspofungin in AspergilosisDesi RatnaningtyasNo ratings yet
- Artigo Protetor SolarDocument10 pagesArtigo Protetor Solarprepre00No ratings yet
- MTX PsoriasisDocument16 pagesMTX PsoriasisDesi RatnaningtyasNo ratings yet
- VitiligoDocument5 pagesVitiligoDesi RatnaningtyasNo ratings yet
- Chua Et Al-2014-British Journal of DermatologyDocument8 pagesChua Et Al-2014-British Journal of DermatologyDesi RatnaningtyasNo ratings yet
- Fractional Q Switched MICHAEL H. GOLD1Document8 pagesFractional Q Switched MICHAEL H. GOLD1Desi RatnaningtyasNo ratings yet
- LepraDocument10 pagesLepraDesi RatnaningtyasNo ratings yet
- Management of Cutaneous ErythrasmaDocument11 pagesManagement of Cutaneous ErythrasmaDesi RatnaningtyasNo ratings yet
- NCM 116 Midterm PDFDocument130 pagesNCM 116 Midterm PDFPonciana PasanaNo ratings yet
- Metadichol® Vitamin D Inverse AgonistDocument45 pagesMetadichol® Vitamin D Inverse AgonistDr P.R. RaghavanNo ratings yet
- Progestins AND AntiprogestinsDocument41 pagesProgestins AND AntiprogestinsdrfatimarizNo ratings yet
- Chapter 08: Pharmacokinetics and Related Topics: OxfordDocument12 pagesChapter 08: Pharmacokinetics and Related Topics: OxfordPrince AroraNo ratings yet
- MusaedAlsayadi (GynaecologmcqsDr. Farouk Haseeb)Document65 pagesMusaedAlsayadi (GynaecologmcqsDr. Farouk Haseeb)a7332773No ratings yet
- XBHA2103 Human Anatomy and Physiology Capr14 (RS) (M) PDFDocument8 pagesXBHA2103 Human Anatomy and Physiology Capr14 (RS) (M) PDFbell mailNo ratings yet
- Acid Base Balance in ICU Summary 25122020Document8 pagesAcid Base Balance in ICU Summary 25122020Aya NassarNo ratings yet
- Basic Science OITE ReviewDocument91 pagesBasic Science OITE ReviewICH KhuyNo ratings yet
- Actividad Semana 1 - Anatomia y Fisiologia.Document7 pagesActividad Semana 1 - Anatomia y Fisiologia.Claribel Sarait Blanco GiilNo ratings yet
- Phys - Mcqs - Endocrine - Gastroenterology 123Document41 pagesPhys - Mcqs - Endocrine - Gastroenterology 123Syeda AlizaNo ratings yet
- HP - Supplement Guide - 9Document30 pagesHP - Supplement Guide - 9Jelena StojadinovNo ratings yet
- United States Patent: (10) Patent No .: US 10, 414, 831 B2 (45) Date of Patent: Sep - 17, 2019Document14 pagesUnited States Patent: (10) Patent No .: US 10, 414, 831 B2 (45) Date of Patent: Sep - 17, 2019Raf RafNo ratings yet
- GLP 1 R AgonistDocument8 pagesGLP 1 R AgonistHninNo ratings yet
- The Thyroid Reset Diet 3 ChaptersDocument71 pagesThe Thyroid Reset Diet 3 ChaptersjovaneticNo ratings yet
- Embryology (3) Development of The Male Reproductive OrgansDocument13 pagesEmbryology (3) Development of The Male Reproductive OrgansNazmul Hossain TayonNo ratings yet
- Educational Case: Pituitary Adenoma: Ayda Javanbakht, MD and George Zanazzi, MD, PHDDocument5 pagesEducational Case: Pituitary Adenoma: Ayda Javanbakht, MD and George Zanazzi, MD, PHDShromona ChakrabortyNo ratings yet
- Diabetic Patient's Biochemistry ReportDocument2 pagesDiabetic Patient's Biochemistry Reportgsm2008No ratings yet
- Multiple Effects of HormonesDocument35 pagesMultiple Effects of HormonesRokia GhariebNo ratings yet
- Baby Katzung Case 1 10Document15 pagesBaby Katzung Case 1 10Danielle Sabrina LimNo ratings yet
- Digestive System VOSMED RUTDocument29 pagesDigestive System VOSMED RUTRut H. P. EkasiwiNo ratings yet
- Analisis Hematologi Monyet Ekor PanjangDocument148 pagesAnalisis Hematologi Monyet Ekor PanjangIrfan Rian SaputraNo ratings yet
- IGCSE Homeostasis (Parts 1 and 2)Document19 pagesIGCSE Homeostasis (Parts 1 and 2)buhNo ratings yet
- Steroids HormonesDocument15 pagesSteroids HormonesZain Ul Abdin Mughal100% (1)
- Sedative & Hypnotics: Prof. Hanan Hagar Pharmacology Department Medical College King Saud UniversityDocument51 pagesSedative & Hypnotics: Prof. Hanan Hagar Pharmacology Department Medical College King Saud UniversityRose Ann Raquiza-PeranteNo ratings yet
- DAONIL® TabletsDocument3 pagesDAONIL® TabletsSayeed BalalaNo ratings yet
- NHS FPX 6004 Assessment 2 Policy ProposalDocument4 pagesNHS FPX 6004 Assessment 2 Policy Proposaljoohnsmith070No ratings yet
- Download ebook Endocrine Secrets Pdf full chapter pdfDocument67 pagesDownload ebook Endocrine Secrets Pdf full chapter pdfjason.green261100% (23)
- Experiment 9 - Hydrolysis of CarbohydratesDocument2 pagesExperiment 9 - Hydrolysis of CarbohydratesJuren LasagaNo ratings yet
- Bacterial Communities Associated With The Lichen SDocument7 pagesBacterial Communities Associated With The Lichen SAli Mariouni AlawieNo ratings yet
- Metabolism QuestionsDocument5 pagesMetabolism QuestionsErjus Hoxhaj100% (1)