Professional Documents
Culture Documents
Obstruction E
Uploaded by
Corina MunteanuCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Obstruction E
Uploaded by
Corina MunteanuCopyright:
Available Formats
INTESTINAL OBSTRUCTION
Intestinal obstruction presents a clinical syndrome, in which a complete arrest or
serious impairment to the passage of intestinal contents is happened. Obstructions can be
complete, meaning that the lumen is totally occluded, or incomplete, meaning that the
lumen is narrowed but permits distal passage of some fluid and air. Also is known as
ileus (from Greek language eileos - twisted). Obstruction presents 3,5-9% from all the
patients with the acute abdomen (M.Cuzin, 1994).
I. ETIOLOGY AND PATHOGENESIS
Intestinal obstruction is multifactorial syndrome. The common causes of mechanical
obstruction are anatomical and pathological features of the intestinal tract, such as atresia,
adhesions, bands, foreign bodies (including gallstones), fecaliths impaction, malrotated gut
accompanied with high motility;
a)
Sex men suffer 1 - 2 folds more frequently;
b)
Age 70% of patients are 40 years and older;
c)
Physical effort with increasing of the intra-abdominal pressure;
d)
Seasons more often it happens in summer and autumn, and depends on food
quality.
II. PATHOPHYSIOLOGY OF INTESTINAL OBSTRUCTION
When a loop of bowel becomes obstructed, intestinal gas and fluid accumulate. The
quality of symptoms and complications development depends on luminal volume, bacterial
proliferation, and alterations in motility and perfusion.
Experimental studies indicated that the source of gaseous distention in cases of
obstruction was swallowed air (70% of total volume) and gas produced by activity of
microorganisms (30% of volume). Fluid accumulates intraluminally in intestinal obstruction
too. Intestinal intra-luminal pressure gradually increases due to distention of the lumen by
gas and fluids. When intra-luminal pressures achieves 10-15 cm H 2O the venous
circulation is compromised. On the level of intra-luminal pressures of 30-40 cm H 2O
capillary collapse occurs. Experimental studies and clinical investigations demonstrated
that elevation of luminal pressures above 20 cm H 2O inhibits absorption and stimulates
secretion of salt and water into the lumen proximal to an obstruction, in intestinal wall and
peritoneal cavity. Only intra-luminal above the obstruction accumulates 8-10 liters of fluid
within 24 hours period. This space, which sequesters a fluid is named 3 rd sector (Rondall)
and include intra-luminal, parietal and peritoneal spaces. Organisms loss of salt and
water is accomplished by vomiting, particularly in the small bowel obstruction. Due to
massive loss of fluid from intra-cellular and extra-cellular spaces, dehydration and arterial
blood hypotension are developed. The clinical signs of dehydration [di:haidreision] are:
thirst [Oa:st], dry skin, arterial blood hypotension, tachycardia. Massive losses of Na
stimulates produces of aldosteron, that detains Na and Cl in organism, but majors
elimination of K. Laboratory findings in this stage of obstruction are: increased Ht,
hypokalemia, hyponatremia. Hypokalemia is associated with weakness, muscular
hypotension, cardiovascular disturbances, decreasing of the intestinal motility. In closedloop obstruction, luminal pressures can exceed 5060 cm H 2O and may provoke an
arterial ischemia of the bowel wall. Since this moment the intestinal wall becomes
permeable for microorganisms and bacterial endotoxins. Simultaneously with hydrosaline
imbalances, the considerable alteration of protein metabolisms occurs in the bowel
obstruction. The protein secretion in bowel lumen and wall, and peritoneal cavity increases
abnormally. Another mechanisms of protein loss is the increasing cellular metabolism. The
metabolic acidosis gradually develops. The proteins destroy goes to delivery of the large
amount of the intracellular K. Hyperkalemia is manifested by coronary disturbances
(arrhythmia, palpitation).
III. CLASSIFICATION
For clinical purposes, intestinal obstruction is divided into:
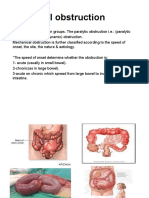
1. MECHANICAL OBSTRUCTION
2. DYNAMICAL OBSTRUCTION
Mechanical obstruction is divided in two types:
1. Strangulating, in which arterial and venous flow of a bowel segment (within its
mesentery or within the bowel wall) is cut off. The strangulating obstruction more
frequently affects small bowel, than colon. As example may serve: volvulus, hernias
(external or internal) with strangulation.
2. Simple, in which there is no interference with blood supply usually caused by
obstacle to intestinal passage, without ischemical changes. Obstacle may be located:
INTRALUMINAL (that blocks the lumen of bowel): foreign body, gallstone, fecaliths,
parasites- ascaris, bezoars.
INTRAMURAL (situated in the intestinal wall): congenital atresia or stenosis, inflammatory
process (such as Crohns disease, diverticulitis), benign or malignant tumor, postoperative
stenosis.
EXTRINSIC (cause is situated out of bowel, but provokes obstruction by outer
compression): adhesions, external mass effect (abscess, carcinomatosis, pancreatic
pseudocyst).
3. Combined, in which ischemia and luminal obturation are happened simultaneously:
intussusception, adhesions.
Dynamical obstruction. May be divided in two groups in dependence on its
mechanisms:
Spastic ileus occurs in different intoxication (including professional intoxication with
lead, by ascaris endotoxins, hysteria, asthma.
Paralytic ileus occurs more frequently and may be caused by variable etiology criteria.
Adynamic ileus is most often associated with intra- or retroperitoneal infection. Ileus
may be produced by mesenteric ischemia, by arterial or venous injury, by
retroperitoneal or intra-abdominal hematomas, after intra-abdominal surgery, in
association with renal or thoracic disease or injuries, and by metabolic disturbances.
a) Metabolic paralytic ileus caused by metabolic disturbances (hypokalemia, in
association with renal or endocrine disease - diabetic ketoacidosis, and uremia).
b) Reflex ileus initiates due to irritation of sympathetic nerves. May appear in
pleurisy or pneumonia, ribs fracture and other thoracic injuries, spinal column
fractures, retroperitoneal hematomas, renal colic, coronary diseases, pancreatic
diseases.
c) Adynamic ileus, caused by nervous and psychic disturbances, named as
neurogen ileus and psychogen ileus.
d) Toxic ileus, caused by different intoxication, such as: some professional
intoxication, endotoxic shock, excessive use of medicaments: anti-Parkinsonian
drugs, nicotine, analgesics, ganglions blockers.
e) Adynamic postoperative ileus, or postoperative paresis. The intestinal motility
disturbances appear following abdominal surgery are largely a result of
abdominal or retro-peritoneal manipulations.
The intestinal obstruction also is divided in dependence on its level:
The superior (proximal) intestinal obstruction, in jejuno-ileum (small bowel),
The inferior (distal) intestinal obstruction, in the large bowel.
And in dependence of origin of the intestinal obstruction:
congenital obstruction
acquired obstruction.
IV. SYMPTOMS AND SIGNS
Variability of the symptoms according to the site and cause of the obstruction must be
emphasized. It is generally true that the higher intestinal obstruction provides more severe
symptoms: severe abdominal pain, persistent vomiting, general status is worth. Colon
obstruction is usually accompanied by varying levels of pain, with massive abdominal
distention, and constipation, but general status remains well for a long time. The
mechanism of obstruction is also important. So, strangulation obstruction of the small or
large intestine is accompanied by symptoms and signs that suggest early necrosis of the
loop with violent pain, decreasing urine output, fever, tachycardia and shock. The
symptoms pain, vomiting, constipation and abdominal distention are less evidenced in
simple obstruction.
Pain is the most common symptom of the intestinal obstruction. Pain is often very
severe from the onset.
The spasmodic pain in simple obstruction is due to the
peristalsis of the intestine trying to overcome the obstruction. When the pain starting
with cramps becomes severe and steady, strangulation must be suspected.
Vomiting the second characteristic feature. Vomiting appears early with small bowel
and late with large bowel obstruction. In obstructive vomiting, first the stomach contents
are expelled, then green bilious material appears and, if the obstruction in some way
down to small intestine, the color of the vomit changes to yellow or greenish-brown and
becomes feculent. Hemathemesis is the serious prognostic sign, usually indicating
strangulating obstruction, accomplished by severe lesions.
Constipation is the important symptom of intestinal obstruction, but not always evident
at first, because the gut below the stoppage can empty itself, particularly in high small
bowel obstruction and incomplete ileus.
Physical examination provides the following crucial symptoms:
a) Special search must be made for abdominal scars. Besides it, three important signs
are evident: abdominal distention, hyperactive peristalsis and abdominal asymmetry.
Abdominal distension may be localized and diffuse. Initially distention is situated
immediately above the obstruction and produces an abdominal asymmetry. In the volvulus
of the sigmoid colon an asymmetric distension is occupied left part of abdomen (Bayers
sign). Considerable distention of the cecum is known as Bouverets sign and may be
helpful for diagnosis of low colic obstruction. No distention is present in high duodenaljejunal obstruction, and the abdomen remains flat.
Peristalsis. Hyperactive, high-pitched peristalsis with rushes coinciding with cramps
is typical. Initially, the peristaltic wave can be seen in a certain point, in the site of
obstruction (Knigs sign). Peristalsis disappears in advanced period of the intestinal
obstruction.
b) Percussion of the abdomen give the following data:
-
Generalized abdominal tympani;
tympani above asymmetric site - (Wahls sign);
obscure of the liver dullness, caused by distension of the large bowel (Celoditis
sign);
provoked plash, diffuse or local situated (Sclearovs sign);
shiftable dullness in lateral parts of the abdomen, caused by peritoneal fluid in
the advanced intestinal obstruction.
c) Palpation.
-
Careful search must be made for sites of external hernias;
Localization of pain, usually above the site of affected intestinal loop;
Rigidity of the abdominal wall in the case of local peritonitis round an
strangulated section of bowel. In the absence of strangulation, the abdomen is
not tender;
Sometimes, a mass corresponding to the site of the obstructing tumor, may be
palpable.
e)
Auscultation of the abdomen reveals the following abnormalities:
-
Intestinal sounds are loud and sometimes may be hear on the distance
Schlanghes sign, is characteristics for initial period of obstruction;
Auscultation reveals a silent abdomen with cardiac and respiratory sounds
(Mondors sign), characteristics for loop necrosis and advanced peritonitis.
f)
Rectal examination is necessary in all cases of the intestinal obstruction and may
reveal rectal stenosis, rectal tumor, fecaliths. In volvulus of the sigmoid colon the rectal
ampulla is empty and enlarged (Hochwag-Grecovs sign).
V. DIAGNOSIS.
Diagnosis usually is confirmed by the abdominal x-ray, which should be taken in
upright positions.
Fluid levels in the gut can be seen in upright films Kloibers sign. Distended loops
may be absent with an obstruction of the upper jejunum. In the small bowel obstruction
a typical series of multiple air-fluid levels located at different areas. Small bowel loops
usually appear in the central part of abdomen, whereas in the case of large bowel
obstruction bowel loops are few with appearance in the laterals abdominal parts;
In gallstone intestinal obstruction the abdominal film rarely shows the stone, but free air
in billiary tree due to cholecysto-duodenal fistula is usually seen;
In volvulus of the sigmoid colon the proximal colon is considered dilated when it
reaches 8 to 10 cm, such as bicycle camera;
In questionable cases of small bowel obstruction, barium can be given orally;
however, barium by mouth is contraindicated if obstruction is believed to be in the colon.
Schwarz has proposed this procedure for the first time in 1911. Normally, after 3-4 hours
after ingestion the barium achieves into the cecum. If the contrast remains more than 4-5
hours in the small bowel, a proximal intestinal obstruction must be suspected.
A barium enema usually is used to rule out colonic lesions, such as tumor, volvulus or
intussusception, as well as a level of bowel obturation.
Laboratory
examination.
Hypoproteinemia,
hemoconcentration,
hypokalemia,
hyponatremia, hypochloremia, metabolic acidosis are typical findings on the laboratory
examination. Hyperleucocytosis (15,000 20,000) usually indicates strangulation or
infarction of the bowel.
VI. DIFFERENTIAL DIAGNOSIS
The most difficult is differentiation between mechanical and dynamical ileus. The
main symptoms for diagnosis of mechanical obstruction are: conditions of ileus
appearance, quality of pain, abdominal distention, early vomiting, increased peristalsis.
Radiological examination shows a multiple air-fluid levels (Kloibers sign). In the dynamic
ileus a patient may experience discomfort and distention as swallowed air fills loops that
do not have effective peristalsis. Plain films of the abdomen reveal gas in segments of
both the small and large bowel. The flow of contrast to the large bowel excludes the
diagnosis of bowel obstruction.
VII. TREATMENT
The restoration of the normal intestinal passage by removing of the ileus cause is the
main purpose of surgical intervention in intestinal obstruction. The preoperative
preparation is necessary. It includes:
a) Decreasing and prevention of the intestinal distension;
b) Correction of metabolic and electrolyte imbalances.
Moreover, these two measures must be done continuously before, within and after
surgery.
Nasogastric decompression is indicated in all cases. The nasogastric tube serves to
prevent distal passage of swallowed air, reduces intestinal distention and minimizes the
discomfort of refluxing intestinal content. The nasogastric tube is removed only after full
restoration of the intestinal transit. The large bowel is cleaned of its contents by enema.
Continuous epidural block with lidocaine may be helpful.
Initial management includes resuscitation and correction of underlying metabolic or
electrolyte imbalances by intravenous administration of lactated Ringer's solution, glucose
solution, normal saline solution in 2-3 liters of volume and plasma transfusion. This
preoperative management has a duration of 3-4 hours. The effectiveness of the
preoperative treatment must be appreciated by normalization of the central venous
pressure, urine output, correction of respiratory and circulatory disturbances.
However, the management differs considerably, when patient is hospitalized with
strangulating obstruction: his general status is bed with hemodynamical instability, with
presence of free fluid in the peritoneal cavity, hyperleucocytosis. Because of this, the
preoperative management is short-term and begins with resuscitation. Intravenous line is
helpful and perfusion of dextrans solution, fluids and electrolytes are started immediately.
Perfusion is made under permanent control of a central venous pressure. An urethral
catheter is necessary to monitor urinary output.
VIII. SURGICAL TREATMENT
The most preferable is medial incision and general anesthesia.
Inspection of the peritoneal cavity should begin from the ileo-cecal part. In the case
of cecal distention cause of obstruction should be found in the large bowel. When the
cecum is normal cause of obstruction is situated proximally, in the small bowel.
The surgical procedure depends on obstruction cause and viability of the bowel. After
that obstruction cause is removed (detorsion of volvulus, desinvagination, destrangulation
of hernia, cut of adhesions) viability of the bowel should be assessed. If bowel is viable its
color is rose, peristalsis is visible, and pulsation of mesenteric vessels is determined.
When bowel ischemia is suspected two measures of the intestinal resuscitation must be
undertaken: (1) a wet surgical towel with hot (+40C) saline solution
is put round of
affected loop; (2) mesentery of the bowel is infiltrated with 0,5% novocaine solution. After
15 - 20 minutes of observation a viability of the suspected intestinal loop is assessed
again.
If bowel necrosis is found, the affected segment is resected with restoration of
intestinal integrity by side-to-side or end-to-end entero-entero anastomosis. If advanced
peritonitis is present, operation is finished with enterostomy or colostomy.
In obturation obstruction a gallstone, bezoars or ascaris can be removed through
enterotomy. In the gallstone intestinal obstruction, treatment consists of lithotomy;
cholecystectomy done either simultaneously or later.
Obstructing cancers of the colon usually can be treated by a single-stage resection
and anastomosis. Other choices include a tumor resection with sigmoid colostomy for leftside obstruction (Hartmanns procedure) and anastomosis is delayed to a later date or
simple colostomy for unresectable obstructing tumor.
In the majority of cases the intraoperative decompression of the intestinal tract is
necessary. This may be done by nasogastric tube placing, simple intubation using a long
intestinal tube (Miller-Abbotts tube), enterotomy, or through the proximal loop of resected
intestine.
Treatment in the postoperative period has a following aims:
-
Gastric and intestinal decompression;
Correction of homeostatic imbalances;
Restoration of peristalsis;
Prevention of the postoperative complications.
Intestinal decompression in the postoperative period provides be nasogastric tube,
long intestinal tube, placed intraoperatively beyond the anastomosis, or tube, placed in
colon through the rectum.
Moreover for early restoration of peristalsis, the postoperative treatment should
include prozerin, ubretid, hypertonic saline solution intravenous, and enemas, which also
stimulate intestinal movements.
Correction of fluid volume and electrolyte imbalances provides by intravenous
administration of lactated Ringer's solution, glucose solution, normal saline solution, and
plasma or albumin transfusion in 2-3 liters of volume daily. The effectiveness of the
treatment is appreciated by pulse rate, ABP (arterial blood pressure), central venous
pressure, Ht, ionogram and blood pH, urine output, peristalsis.
In order to prevent a complications, such as pneumonia, thrombosis, wound and
intra-abdominal sepsis, special therapy sometimes is necessary: dezagregantii dextrans
(rheopoliglucin), anticoagulation therapy (heparin 5.000 UN x 4 times daily, fraxiparin),
antibiotics, early activation of patient.
IX. CLINICAL FORMS
1.
VOLVULUS OF THE SIGMOID COLON. The most common site for volvulus
is the sigmoid colon, accounting for 65% of cases. The term volvulus indicates that a loop
of bowel is twisted more than 180 degrees about the axis of its mesentery. By definition, a
volvulus is a form of closed-loop obstruction of the colon. Volvulus often has an abrupt
onset. Volvulus of the sigmoid colon is associated with abdominal distention and, usually,
severe pain located in the left abdominal part. In the volvulus of the sigmoid colon an
asymmetric distension is occupied left part of abdomen (Bayers sign). Constipation is
observed from the onset, whereas vomiting appears later. On rectal examination the rectal
ampulla is empty and enlarged (Hochwag-Grecovs sign).
The diagnosis is based on the radiographic examination and barium enema.
The treatment of choice is surgery. If the bowel is viable, detorsion of the volvulus
and fixation of the affected loop to prevent twisting is indicated (procedure Gaghen-Torn).
If the patient presents with peritoneal signs and bowel necrosis is found, the affected
segment is resected and a primary anastomosis or colostomy is done.
2.
INTUSSUSCEPTION. An intussusception (or invagination) occurs when one
segment of bowel telescopes into an adjacent segment, resulting in obstruction and
ischemic injury to the intussuscepting segment. About 70% of intussusception cases occur
in infants and children. May be caused by polyps, enterocolitis, ascaris, Meckels
diverticolum, tumors and others. Three types of intussusception are recognized: enteric,
enterocolic, and colic. In the most frequent enterocolic form, the ileum telescopes into the
colon.
Colicky pain and a presence of a tumor are the two main symptoms. The another
usual signs are: vomiting, constipation, passage of blood and mucus per anus, shock and
abdominal distention.
Radiographic features of intussusception are not specific. Plain films reveal evidence
of partial or complete obstruction.
The only effective treatment in adults is surgery. There are rare cases, when
operation can be limited by disinvagination. The most common is intestinal resection,
performed by right hemicolectomy or segmental resection of the bowel. Sometimes, in the
presence of advanced peritonitis, enterostomy or colostomy is indicated.
3.
ADHESIONS. Peritoneal adhesions account for more than half of small
bowel obstruction cases. Abdominal procedures such as appendectomy, hysterectomy,
cholecystectomy, gastrectomy are common previous operations to adhesive obstruction.
10
Histologic examination of chronic adhesions reveals foreign-body reaction, usually to talc,
intestinal content, or suture.
Simple adhesive obstruction is distinguished from most other forms of obstruction by
its capacity to resolve without surgical intervention. A history of a laparotomy simply
provides a reasonable basis for expectant management of patients in whom it is not yet
possible to diagnose a complete obstruction.
The most reasonable approach to reducing adhesion formation includes careful
hemostasis, gentle surgical technique, and removal of foreign material from the peritoneal
cavity. It is also possible that the use of monofilament sutures for fascial closure and
avoidance of closure of the peritoneum as a separate layer lower the formation of
adhesions between viscera and the abdominal wall.
You might also like
- Intestinal Obstruction: EpidemiologyDocument11 pagesIntestinal Obstruction: EpidemiologyBereket temesgenNo ratings yet
- Intestinal ObstructionDocument157 pagesIntestinal ObstructionOmar SuleimanNo ratings yet
- Intestinal ObstructionDocument9 pagesIntestinal ObstructionMuhammad Fuad Jaafar100% (1)
- Obstruction EDocument87 pagesObstruction ETimbur IgorNo ratings yet
- K26 Ileus ObsDocument18 pagesK26 Ileus ObsmitrajoeNo ratings yet
- 58.intestinal ObstructionDocument18 pages58.intestinal ObstructionAdenegan Adesola RaymondNo ratings yet
- Ashok Intestinal OostructionDocument92 pagesAshok Intestinal OostructionAshok Shinde0% (1)
- Bowel Obstruction Vs IleusDocument62 pagesBowel Obstruction Vs IleusSandra SuryariniNo ratings yet
- Intestinal ObstructionDocument12 pagesIntestinal ObstructionPrincewill SeiyefaNo ratings yet
- MODULE 2 - Diseases and MalfunctionsDocument47 pagesMODULE 2 - Diseases and MalfunctionsVicKy AmaliaNo ratings yet
- 9 Intestinal ObstructionDocument7 pages9 Intestinal ObstructionMAH pedNo ratings yet
- Intestinal Obstruction PDFDocument7 pagesIntestinal Obstruction PDFmist73No ratings yet
- INTESTINAL OBSTRUCTION AND PERITONITIS - Docx Version 1.ru - enDocument11 pagesINTESTINAL OBSTRUCTION AND PERITONITIS - Docx Version 1.ru - enAina OlajumokeNo ratings yet
- Equine Colic (Adult Horses) : EtiologyDocument22 pagesEquine Colic (Adult Horses) : EtiologyroonyNo ratings yet
- Small Bowel Obstruction &post Operative IleusDocument62 pagesSmall Bowel Obstruction &post Operative IleusMamanya Fadhil HaniNo ratings yet
- Intestinal ObstructionDocument12 pagesIntestinal ObstructionBheru LalNo ratings yet
- Pathology (Digestive System)Document20 pagesPathology (Digestive System)chepie villalonNo ratings yet
- Intestinal ObstructionDocument48 pagesIntestinal ObstructionMahmoud AbuAwadNo ratings yet
- Intestinal Obstruction: Yohannes TDocument34 pagesIntestinal Obstruction: Yohannes TVincent Ser100% (1)
- Acute Intestinal ObstructionDocument3 pagesAcute Intestinal Obstructionoddone_outNo ratings yet
- Intestinal ObstructionDocument21 pagesIntestinal ObstructionBheru LalNo ratings yet
- PeritonitisDocument14 pagesPeritonitisAyad IdresNo ratings yet
- ILEUS AND PERITONITIS AnglDocument51 pagesILEUS AND PERITONITIS Anglutami nahdyaNo ratings yet
- Intestinal ObstructionDocument9 pagesIntestinal ObstructionHamss AhmedNo ratings yet
- Acute Intestinal Obstruction...Document42 pagesAcute Intestinal Obstruction...Ali100% (2)
- Bowel ObstructionDocument36 pagesBowel ObstructionResti Fratiwi FitriNo ratings yet
- INR (International Normalized Ratio) : Rigler's SignDocument11 pagesINR (International Normalized Ratio) : Rigler's SignLee Zheng CongNo ratings yet
- GI Notes For Exam 3Document4 pagesGI Notes For Exam 3cathyNo ratings yet
- Askep Ileus Paralitik PDFDocument12 pagesAskep Ileus Paralitik PDFniaNo ratings yet
- გაუვალობაDocument37 pagesგაუვალობაMalak A MahadeenNo ratings yet
- Mechanical Causes of Intestinal ObstructionDocument5 pagesMechanical Causes of Intestinal ObstructionKimberly Subade MandilagNo ratings yet
- Large Bowel Obstruction by Nic MDocument42 pagesLarge Bowel Obstruction by Nic MRisky OpponentNo ratings yet
- Abdomen Examination General Inspection Clinical SignsDocument16 pagesAbdomen Examination General Inspection Clinical SignsJerry GohNo ratings yet
- Small Bowel: Alaa MaaliDocument78 pagesSmall Bowel: Alaa MaaliHalima AssiNo ratings yet
- Paralytic Ileus: Prepared By: Laurence A. Adena, ManDocument43 pagesParalytic Ileus: Prepared By: Laurence A. Adena, ManJanah Beado PagayNo ratings yet
- INTESTINAL OBSTRUC PremierDocument52 pagesINTESTINAL OBSTRUC Premierapi-19641337No ratings yet
- Topic: Cholecystitis: IntroductionDocument11 pagesTopic: Cholecystitis: IntroductionSyarafina AzmanNo ratings yet
- Patofisiologi Digestive (2015)Document65 pagesPatofisiologi Digestive (2015)IndriNo ratings yet
- Gastrointestinal SystemDocument5 pagesGastrointestinal SystemTaylor NicholNo ratings yet
- Bowel ObstructionDocument8 pagesBowel ObstructionJils SureshNo ratings yet
- RP RPDocument6 pagesRP RPEliezah RodriguezNo ratings yet
- Anatomy Atresia, Volvulus, Meckel's Diverticulum: BowelDocument45 pagesAnatomy Atresia, Volvulus, Meckel's Diverticulum: BowelkedokterankeluargaNo ratings yet
- Ileus PutriDocument17 pagesIleus PutriSukir LiboNo ratings yet
- 2013 Surgery ReviewDocument5 pages2013 Surgery ReviewHaslinNo ratings yet
- Lecture 7 Intussusception 2016Document8 pagesLecture 7 Intussusception 2016Nuukelo ShimbomeNo ratings yet
- Intestinal Obstruction ChikaDocument45 pagesIntestinal Obstruction ChikarohitNo ratings yet
- Intestinal ObstructionDocument15 pagesIntestinal ObstructionEmmeline Dycangchon-GarmaNo ratings yet
- Small and Large Bowel Obstruction (1) - 1Document91 pagesSmall and Large Bowel Obstruction (1) - 1dagimb bekeleNo ratings yet
- Case 5 - Pancreatitis-1Document4 pagesCase 5 - Pancreatitis-1ngNo ratings yet
- What Is Intestinal ObstructionDocument5 pagesWhat Is Intestinal ObstructionmatrixtrinityNo ratings yet
- Intestinal Obstruction FinalDocument10 pagesIntestinal Obstruction FinalAmlan jyoti thanapatiNo ratings yet
- Intestinal Diseases: Gastrointestinal shengjing Hospital of Medical youwei kou (寇有为)Document80 pagesIntestinal Diseases: Gastrointestinal shengjing Hospital of Medical youwei kou (寇有为)Abhirami AnilNo ratings yet
- Cholecystitis: Causes and PathologyDocument12 pagesCholecystitis: Causes and PathologySher KhanNo ratings yet
- Curs 4 Gastro IDocument23 pagesCurs 4 Gastro In bNo ratings yet
- Intestinal ObstructionDocument42 pagesIntestinal ObstructionSaurabh SharmaNo ratings yet
- Intestinal Obstruction: By: Dr. Wasfi M SalaytaDocument16 pagesIntestinal Obstruction: By: Dr. Wasfi M SalaytayayaNo ratings yet
- Chronic Diarrhoea SaqlainDocument116 pagesChronic Diarrhoea SaqlainMohammed SaqlainNo ratings yet
- Intestinal Obstruction AditiDocument67 pagesIntestinal Obstruction Aditiaditi BahugunaNo ratings yet
- Intestinal Obstruction Halel Khaled Al-WardDocument10 pagesIntestinal Obstruction Halel Khaled Al-Wardمنيب سالمNo ratings yet
- Example: Write Sentences To Give Advice. Use The Verb and The Information in Parenthesis. (1.25 Points)Document2 pagesExample: Write Sentences To Give Advice. Use The Verb and The Information in Parenthesis. (1.25 Points)Robert Jesús Guerrero GilerNo ratings yet
- Angelman Syndrome - Identification and ManagementDocument10 pagesAngelman Syndrome - Identification and ManagementFajar YuniftiadiNo ratings yet
- Referral Letter To Specialist From GPDocument74 pagesReferral Letter To Specialist From GPyazz80% (5)
- TSS 30 - Application Form - SODocument4 pagesTSS 30 - Application Form - SOkemvanNo ratings yet
- SES Presentation FinalDocument65 pagesSES Presentation FinalCurtis YehNo ratings yet
- 2005 Proverbs TOM SchizophreniaDocument7 pages2005 Proverbs TOM SchizophreniaKatsiaryna HurbikNo ratings yet
- Seminar and Topic ObjectivesDocument2 pagesSeminar and Topic ObjectivesNeyo KatalbasNo ratings yet
- PARCO Project HSE Closing ReportDocument22 pagesPARCO Project HSE Closing ReportHabib UllahNo ratings yet
- Phys Ther 2012 Macedo 363 77Document18 pagesPhys Ther 2012 Macedo 363 77Anang FajarNo ratings yet
- Assisting For Endotracheal IntubationDocument16 pagesAssisting For Endotracheal IntubationSREEDEVI T SURESH100% (1)
- XA6 - Emergency Provision Workbook 2020 v0 - 5 - CKDocument35 pagesXA6 - Emergency Provision Workbook 2020 v0 - 5 - CKguyNo ratings yet
- Health Beliefs and PracticesDocument7 pagesHealth Beliefs and Practicesapi-283426681No ratings yet
- The Myths and Truths About Transcendental MeditationDocument11 pagesThe Myths and Truths About Transcendental MeditationMeditation Fix100% (2)
- Nitroimidazole Wps OfficeDocument10 pagesNitroimidazole Wps OfficeCamelle DiniayNo ratings yet
- NCP For PostpartumDocument1 pageNCP For PostpartumMary Hope BacutaNo ratings yet
- Risk Assessment - GardenDocument2 pagesRisk Assessment - GardenOlivia BrookesNo ratings yet
- About The Author-James Herriot: A Triumph of Surgery Chapter - 1 Footprint Without FeetDocument4 pagesAbout The Author-James Herriot: A Triumph of Surgery Chapter - 1 Footprint Without FeetSunil rathi100% (3)
- SHARON SCHULTZ, ET AL. v. JANOS GUOTH, M.D. AND KHALED F. RABIE, M.D. (Parish of Rapides)Document18 pagesSHARON SCHULTZ, ET AL. v. JANOS GUOTH, M.D. AND KHALED F. RABIE, M.D. (Parish of Rapides)wstNo ratings yet
- APDSA SRC Submitssion FormDocument2 pagesAPDSA SRC Submitssion FormDevi 吴姗姗 GunawanNo ratings yet
- Ateneo de Zamboanga University: Course Outline (Second Semester) ZOO 208Document1 pageAteneo de Zamboanga University: Course Outline (Second Semester) ZOO 208Almira AhamadNo ratings yet
- Interval TrainingDocument24 pagesInterval TrainingRukmantaraNo ratings yet
- MFDS FAQsDocument2 pagesMFDS FAQsSuhesh HydrosNo ratings yet
- Validity and Reliability Study of The Turkish Version of Ego Identity Process QuestionairreDocument6 pagesValidity and Reliability Study of The Turkish Version of Ego Identity Process QuestionairreSergio F. GonzalezNo ratings yet
- Dinup BSBMGT605Document41 pagesDinup BSBMGT605fhc munna100% (1)
- AH1N1 PPT PresentationDocument28 pagesAH1N1 PPT PresentationIna Isabela CostiboloNo ratings yet
- The Brain, PT 2 - Neuroscience and BehaviorDocument2 pagesThe Brain, PT 2 - Neuroscience and BehaviorprtemnNo ratings yet
- Daftar PustakaDocument2 pagesDaftar PustakaNi Made Ayu DwipayantiNo ratings yet
- Physical Fitness Test Individual Score CardDocument12 pagesPhysical Fitness Test Individual Score CardJunessa TadinaNo ratings yet
- National Health Policy in India: Dr. Kanupriya ChaturvediDocument38 pagesNational Health Policy in India: Dr. Kanupriya ChaturvediRadhakrishnan TherivilaNo ratings yet
- Worm The Game Edit of Wildbow'sDocument16 pagesWorm The Game Edit of Wildbow'sLuke AjemNo ratings yet