Professional Documents
Culture Documents
Acs Nstemi Pathway
Acs Nstemi Pathway
Uploaded by
TPROriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Acs Nstemi Pathway
Acs Nstemi Pathway
Uploaded by
TPRCopyright:
Available Formats
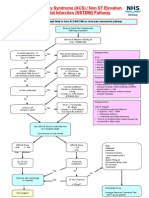
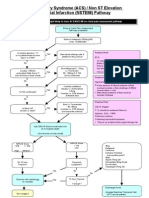
Acute Coronary Syndrome (ACS) / Non ST Elevation
Myocardial Infarction (NSTEMI) Pathway
Eligibility: Patients thought likely to have ACS/NSTEMI on chest pain assessment pathway
Ensure Chest Pain Assessment
Pathway completed
Start s/c Dalteparin 120U/kg bd
(max. 10,000units)2
Is random glucose > 11 Practice Point
Yes Start insulin sliding scale in
or is patient known to have addition to this protocol
type I or II DM? ECG
On admission
Within 24 hours
No
Prior to discharge
Any time symptomatic
Give Metoprolol 5 - 15mg Clinical changes
Is pulse > 65/min i.v. PLUS start
Yes
and patient Killip Score I? 50 - 100mg p.o. tds
(Use formula on back sheet) (to be continued)
Practice Point
No Hypotension (Systolic BP < 90)
In the absence of clinical evidence of fluid
Consider additional overload consider a fluid challenge of 250ml
Yes dose(s) i.v. Diamorphine normal saline i.v. stat
Is Pain continuing?
2.5mg With clinical evidence of fluid overload
Consider i.v. GTN infusion consider inotropes
at titrated dose
No
Practice Point
Give i.v. Furosemide
Is there LVF 40 - 80mg Use of Oxygen
Yes
(known or new)? Consider i.v. GTN infusion O2 should be continued if there is:
(see separate protocol) o Hypoxia - SaO2 < 90%
o Pulmonary oedema
o Continuing myocardial ischaemia
There is no evidence that oxygen therapy has
any benefit in other cases
Use GRACE Score to estimate risk
of in hospital death
(Use formula on back sheet)
GRACE Score GRACE Score Stop
> 9% 1 - 9% < 1% Dalteparin
Low Continue
High Medium -blocker if started
(see practice point1)
Start
Aspirin 75mg od
Do 12 hour Recurrent Simvastatin 40mg nocte
Troponin I symptoms? Do not start
Clopidogrel
Yes No
No
Discuss with cardiology
re: transfer Yes 12 hour Troponin
I
> 0.5g/l ?
Discharge home
Go to page 2 Arrange Exercise Tolerance Test
(ETT) as out-patient
Acute Coronary Syndrome (ACS) / NSTEMI Pathway
Patient discussed
with cardiologists
at ARI
Patient awaiting transfer Declined or not suitable for
transfer
Start Start
Aspirin 75mg od Aspirin 75mg od
Clopidogrel 75mg od Clopidogrel 75mg od
Simvastatin 40mg nocte Simvastatin 40mg nocte
Continue Continue
s/c Dalteparin 120U/kg bd s/c Dalteparin 120U/kg bd
(max. 10,000 U) (max. 10,000 U) for duration
-blocker (see practice point1) of admission
-blocker (see practice point1)
Consider starting Tirofiban
infusion (only after discussion Within 36 hours add
with cardiologists) p.o. Ramipril 1.25mg - 2.5mg od
See separate protocol (dose to be titrated up)
Yes
Is pain ongoing Consider additional dose(s) Optimise anti-anginal therapy
i.v. Diamorphine 2.5mg
No Consider i.v. GTN infusion at
titrated dose
Within 48 hours change
Metoprolol to Atenolol
Within 36 hours add (Metoprolol 50mg tds =
p.o. Ramipril 1.25 - 2.5mg od Atenolol 50mg od)
(dose to be titrated up)
Aim to discharge when symptom
free after one week
Transfer patient to ARI CCU
with letter and any relevant
investigation results (blood Refer to cardiac nurses for
results, ECGs etc) cardiac rehab programme
GP should aim to titrate Ramipril
to 10mg od or max. tolerated
dose
Clopidogrel should be
continued for 3 months
1
Practice Point
-Blockers
-blockers not without problems. Check no contraindications
No strong evidence for any particular one - appears to be class effect. Atenolol, having od dosage, will aid compliance
Start with Metoprolol but if no problems change to Atenolol within 48 hours
-blockers should be withheld in patients with LV failure/pulmonary oedema. Subsequent cautious addition of highly selective -blocker (e.g.
carvidolol) is of proven benefit.
2
Practice Point
Dalteparin in Renal Impairment
Dalteparin (and other LMW heparins) are excreted mainly by the kidneys . LMW heparins, having smaller molecular size, bind less to
plasma proteins, platelets and endothelium and so have greater bioavailablity
Unfractionated heparins ( e.g. heparin sodium) are excreted mainly by the liver
In patients with a creatinine of > 200mmol/L heparin sodium should be used.
o Prophylactic dose is 5000units sc twice daily (but use Dalteparin 2500units once daily if heparin sodium is unavailable)
o Treatment doses are administered as a continuous infusion of heparin sodium with 6-8 hourly APTT monitoring (target ratio usually 2 -
2.5)
In patients with a creatinine of 130 - 200mmol/L consult BNF to calculate Dalteparin dose reductions both for treatment and prophylactic
doses
Acute Coronary Syndrome (ACS) / NSTEMI Pathway
Killip Score
Used to assess degree of acute cardiac failure
Excluded if pre-hospital cardiac arrest
Killip Score
I No clinical signs of heart failure
II Crackles, S3 gallop and elevated jugular venous pressure
III Frank pulmonary oedema
IV Cardiogenic shock - hypotension (systolic < 90mmHg) and evidence of peripheral vasoconstriction (oliguria, cyanosis, sweating)
GRACE Score (Global Registry of Acute Coronary Events)
Used to assess risk of in-hospital death in ACS
1. Find Points for Each Predictive Factor:
Serum
Killip SBP Heart Rate Age
Points Points Points Points Creatinine Points
Score mm Hg Beats/min years
mol/l
I 0 80 58 50 0 30 0 0 - 34 1
II 20 80 - 99 53 50 - 69 3 30 - 39 8 35 - 70 4
III 39 100 - 119 43 70 - 89 9 40 - 49 25 71 - 105 7
IV 59 120 - 139 34 90 - 109 15 50 - 59 41 106 - 140 10
140 - 159 24 110 - 149 24 60 - 69 58 141 - 176 13
160 - 199 10 150 - 199 38 70 - 79 75 177 - 353 21
200 0 200 46 80 - 89 91 353 28
90 100
Other Risk Factors Points
Cardiac Arrest at Admission 39
ST-Segment Deviation 28
Elevated Cardiac Enzyme Levels 14
2. Sum Points for All Predictive Factors:
Killip + Systolic + Heart + Age + Creatinine + Cardiac + ST + Elevated = TOTAL
Class BP Rate Level Arrest at Segment Cardiac POINTS
Admission Deviation Enzymes
3. Look Up Risk Corresponding to Total Points:
Total Points
60 70 80 90 100 110 120 130 140 150 160 170 180 190 200 210 220 230 240 250
Probability
of In-
Hospital 0.2 0.3 0.4 0.6 0.8 1.1 1.6 2.1 2.9 3.9 5.4 7.3 9.8 13 18 23 29 36 44 52
Death, %
For example, a patient has Killip class II, SBP of 100mm Hg, heart rate of 100 beats/min, is 65 years of age, has serum creatinine level of 1mg/dL, did
not have a cardiac arrest at admission but did have ST-segment deviation and elevated enzyme levels.
His score would be: 20+53+15+58+7+0+28+14=196
This person would have about a 16% risk of having an in-hospital death.
Similarly, a patient with Killip class I, SBP of 80mm Hg, heart rate of 60 beats/min, is 55 years of age, has serum creatinine level of 0.4, and no risk
factors would have the following score:
0+58+3+41+1=103, which gives approximately a 0.9% risk of having an in-hospital death.
Definitions
Acute MI: symptoms ? consistent with cardiac ischaemia within 24 hours of presentation with a rise in Troponin I
Unstable Angina: symptoms consistent with cardiac ischaemia within 24 hours of hospital admission with no rise in Troponin I
AND at least one of:
1 Hx MI cardiac arrest, angina or ischaemic CCF
2 Hx of positive ETT
3 Documented cardiac catheterisation of 50% stenosis and 1 coronary artery
4 Hx of angioplasty with CABG
5 ECG transient ST elevation 1mm in 3 continuous chest leads, St depression 1mm, new T wave inversion 1mm, pseudonormaligatin of
previously inverted T
You might also like
- Pathophysiology of Rheumatic Heart DiseaseDocument3 pagesPathophysiology of Rheumatic Heart DiseaseXtiaR85% (13)
- Loser WalkthroughDocument17 pagesLoser WalkthroughFuckNo ratings yet
- Smoking QuestionnaireDocument13 pagesSmoking QuestionnaireNeric Ico Magleo100% (1)
- Psych Case Study 1Document3 pagesPsych Case Study 1Aibonez Shelton- Johnson100% (1)
- Cardiology Case 1Document2 pagesCardiology Case 1vil62650% (2)
- Powerpoint: Disorders of The EsophagusDocument65 pagesPowerpoint: Disorders of The Esophagusj.doe.hex_8782% (11)
- Kdoqi PDFDocument164 pagesKdoqi PDFcindyrely100% (1)
- 12 Week Shred - Dieting - Low Carbohydrate Diet PDFDocument37 pages12 Week Shred - Dieting - Low Carbohydrate Diet PDFonslaughtilus0% (1)
- Philip Manfield-Split Self - Split Object - Understanding and Treating Borderline, Narcissistic, and Schizoid Disorders-Jason Aronson Inc. (1992) PDFDocument392 pagesPhilip Manfield-Split Self - Split Object - Understanding and Treating Borderline, Narcissistic, and Schizoid Disorders-Jason Aronson Inc. (1992) PDFCristina Mitroi83% (6)
- JSA For Concrete WorkDocument6 pagesJSA For Concrete Worklê ngọc tùng0% (1)
- Acs Nstemi PathwayDocument3 pagesAcs Nstemi PathwayAliey's SKeplek NgeNersNo ratings yet
- Bagi Percakapan EnglishDocument4 pagesBagi Percakapan EnglishFatimatuz ZahroNo ratings yet
- Acute Tubular NecrosisDocument15 pagesAcute Tubular NecrosisDeepak patelNo ratings yet
- Reteplase (MIRel)Document23 pagesReteplase (MIRel)Jhoann JamanilaNo ratings yet
- Acute Liver Failure-1Document40 pagesAcute Liver Failure-1elizabethNo ratings yet
- 22 Ventricular Septal DefectDocument26 pages22 Ventricular Septal Defectdhiraj parmarNo ratings yet
- Heart FailureDocument4 pagesHeart FailureDane WrightNo ratings yet
- Calcium GluconateDocument1 pageCalcium GluconateDilip SenthNo ratings yet
- Obstructive JaundiceDocument69 pagesObstructive JaundiceAbdirazak HassanNo ratings yet
- Sick Sinus Syndrome 1Document23 pagesSick Sinus Syndrome 1Salman HabeebNo ratings yet
- Clinical Examination of Genitourinary SystemDocument43 pagesClinical Examination of Genitourinary SystemKeamina .aNo ratings yet
- CASE PRESENTATION ON U AnginaDocument40 pagesCASE PRESENTATION ON U AnginaSafoora RafeeqNo ratings yet
- Cerebrovascular Accident (CVA)Document71 pagesCerebrovascular Accident (CVA)nur muizzah afifah hussinNo ratings yet
- Nephrolithiasis AnatomyDocument3 pagesNephrolithiasis AnatomyKevin Ker Campaner MerillesNo ratings yet
- GLOMERULONEPHRITIS (Bright's Disease)Document8 pagesGLOMERULONEPHRITIS (Bright's Disease)Anjitha K. JNo ratings yet
- Eisenmenger SyndromeDocument41 pagesEisenmenger SyndromeJennifer DixonNo ratings yet
- Acute Tubular Necrosis 2Document19 pagesAcute Tubular Necrosis 2Sangeeta BSRNo ratings yet
- Esophageal Varices Week 4 T2T3Document37 pagesEsophageal Varices Week 4 T2T3liewhuilianNo ratings yet
- Steps To Perform A Blood TransfusionDocument1 pageSteps To Perform A Blood Transfusionzepoli_zepoly6232No ratings yet
- 11 Nursing Management in Uterine (Endometrial) CancerDocument17 pages11 Nursing Management in Uterine (Endometrial) Cancerclaire yowsNo ratings yet
- Angina PectorisDocument17 pagesAngina PectorisRacel HernandezNo ratings yet
- Acute Miocard InfarkDocument32 pagesAcute Miocard InfarkhansNo ratings yet
- Dialysis Round Work Plan 2022 - للطلابDocument16 pagesDialysis Round Work Plan 2022 - للطلابAhmed SalahNo ratings yet
- Hypertrophic CardiomyopathyDocument2 pagesHypertrophic CardiomyopathyMichelle KwokNo ratings yet
- Dr. Sunatrio - Management Hypovolemic ShockDocument59 pagesDr. Sunatrio - Management Hypovolemic ShockArga Putra SaboeNo ratings yet
- Management of Sepsis, Surviving Sepsis Campaign GuidelinesDocument76 pagesManagement of Sepsis, Surviving Sepsis Campaign GuidelinesMohammad Ali100% (1)
- Administrative Applications in Nursing 09Document23 pagesAdministrative Applications in Nursing 09ramroum18No ratings yet
- Acute Coronary SyndromeDocument21 pagesAcute Coronary SyndromeSofia Andi100% (2)
- Renal CalculiDocument9 pagesRenal Calculimehreen.alina35No ratings yet
- Pedal EdemaDocument45 pagesPedal Edemafirdaushassan2112No ratings yet
- Topic / Organ-System:: 1. General Data/InformationDocument5 pagesTopic / Organ-System:: 1. General Data/InformationDan Angelo MatiasNo ratings yet
- Basal Bolus InsulinDMT22009Document92 pagesBasal Bolus InsulinDMT22009scribdNo ratings yet
- Kidney TransplantDocument11 pagesKidney TransplantPrincess Xzmae RamirezNo ratings yet
- Bone Marrow BiopsyDocument28 pagesBone Marrow BiopsyAmeer MattaNo ratings yet
- Example Case StudyDocument7 pagesExample Case StudyTerrena Lyn BlackmanNo ratings yet
- Acute CholecystitisDocument19 pagesAcute Cholecystitisapi-3815243100% (2)
- Peripheral Arterial DiseaseDocument40 pagesPeripheral Arterial Diseaseuseofforcelaw100% (1)
- NCLEX Midterm HandoutDocument17 pagesNCLEX Midterm Handoutjomel magalonaNo ratings yet
- Chest Physiotherapy For Mechanical Ventilation PatientDocument6 pagesChest Physiotherapy For Mechanical Ventilation PatientAkshay BangadNo ratings yet
- PericarditisDocument45 pagesPericarditisBrenda WardshoneNo ratings yet
- Product Information Avil Product NamesDocument4 pagesProduct Information Avil Product Namesindyanexpress100% (1)
- Av Fistula CreationDocument3 pagesAv Fistula CreationJianNo ratings yet
- 13.24 Abdominal-InjuryDocument42 pages13.24 Abdominal-InjuryMuhammad FajarNo ratings yet
- Periampullary TumorsDocument30 pagesPeriampullary TumorsAsif.N.IqbalNo ratings yet
- DKA Study GroupDocument24 pagesDKA Study GroupAqila MumtazNo ratings yet
- Cardiogenic ShockDocument82 pagesCardiogenic ShockLenin Zavaleta RodriguezNo ratings yet
- Deep Vein Thrombosis (DVT) : Education For NursesDocument26 pagesDeep Vein Thrombosis (DVT) : Education For NursesVashNo ratings yet
- Cardiomyopathy My LectureDocument33 pagesCardiomyopathy My LectureAbraha HailuNo ratings yet
- AnginaDocument17 pagesAnginaGaming ModeNo ratings yet
- Cholangitis and Cholecystitis (DR - Dr. Hery Djagat Purnomo, SpPD-KGEH)Document47 pagesCholangitis and Cholecystitis (DR - Dr. Hery Djagat Purnomo, SpPD-KGEH)Aditya SahidNo ratings yet
- ShockDocument24 pagesShockYaacub IbrahimNo ratings yet
- CHC-PC-0033: Procedure Number Version NosDocument7 pagesCHC-PC-0033: Procedure Number Version NosQari Ramadhan AminNo ratings yet
- CCU HandoverDocument9 pagesCCU Handoverapi-192342497No ratings yet
- Chest Pain Protocol in EDDocument3 pagesChest Pain Protocol in EDshahidchaudharyNo ratings yet
- 6 - Fahad Class 6 Cardiac AnesthesiaDocument18 pages6 - Fahad Class 6 Cardiac AnesthesiaOne ClickNo ratings yet
- Chest Pain ProtocolDocument4 pagesChest Pain ProtocolArul ShanmugamNo ratings yet
- Acute Coronary Syndromes 2015Document26 pagesAcute Coronary Syndromes 2015prototypeallhellNo ratings yet
- ACS NSTEMI Clinical PathwayDocument3 pagesACS NSTEMI Clinical PathwayXtiaRNo ratings yet
- FNCP - HPNDocument7 pagesFNCP - HPNXtiaRNo ratings yet
- Revenue Budget: Description Detail AmountDocument1 pageRevenue Budget: Description Detail AmountXtiaRNo ratings yet
- CMO 09 s2007Document55 pagesCMO 09 s2007XtiaRNo ratings yet
- Ebook John Murtaghs General Practice Companion Handbook PDF Full Chapter PDFDocument67 pagesEbook John Murtaghs General Practice Companion Handbook PDF Full Chapter PDFroberto.duncan209100% (33)
- Acute EpiglottitisDocument12 pagesAcute EpiglottitisDr. Sarthak MishraNo ratings yet
- Balantidium ColiDocument5 pagesBalantidium Coliglorya barbessNo ratings yet
- Wa0002.Document9 pagesWa0002.SojiNo ratings yet
- Bone Parasite 1e v1Document2 pagesBone Parasite 1e v1shaunNo ratings yet
- The Management of Polycystic Ovary Syndrome: Vincenza Bruni, Metella Dei, Valentina Pontello, and Paolo VangelistiDocument15 pagesThe Management of Polycystic Ovary Syndrome: Vincenza Bruni, Metella Dei, Valentina Pontello, and Paolo VangelistiDaniela UrreaNo ratings yet
- Jurnal Psikososial Kebudayaan Dalam KeperawatanDocument9 pagesJurnal Psikososial Kebudayaan Dalam KeperawatanApri AnnurNo ratings yet
- English 3 w5Document6 pagesEnglish 3 w5Almie Adarayan BrosotoNo ratings yet
- Konsep Asuhan Keperawatan Keluarga TM. IIIDocument27 pagesKonsep Asuhan Keperawatan Keluarga TM. IIImichaelNo ratings yet
- Candido Gen Bio W5 6Document2 pagesCandido Gen Bio W5 6Joash Nimrod CandidoNo ratings yet
- Supplements Guide: Human Growth HormoneDocument3 pagesSupplements Guide: Human Growth HormoneBrett WhittingNo ratings yet
- Otitis Media Nurisng Care PlanDocument11 pagesOtitis Media Nurisng Care PlanRnspeakcom100% (1)
- First WHO Global Forum On Medical DevicesDocument76 pagesFirst WHO Global Forum On Medical DevicesWolaé Mathurin Edmond AmegandjinNo ratings yet
- Rural OutreachDocument35 pagesRural OutreachPriyanshu Agrawal100% (1)
- Prelim Activity 1 - Health TeachingsDocument2 pagesPrelim Activity 1 - Health TeachingsNICOLE MAGLAQUINo ratings yet
- Thehistoryofneurocritical Careasasubspecialty: Kristi Tempro,, Cherylee W.J. ChangDocument15 pagesThehistoryofneurocritical Careasasubspecialty: Kristi Tempro,, Cherylee W.J. ChangJonathan Mendoza V.No ratings yet
- Construction Project Manager Healthcare in San Antonio TX Resume Joseph ShumateDocument2 pagesConstruction Project Manager Healthcare in San Antonio TX Resume Joseph ShumateJosephShumate100% (1)
- Dermatomycological Profile of Patients in A Tertiary Care Hospital of Western MaharashtraDocument2 pagesDermatomycological Profile of Patients in A Tertiary Care Hospital of Western MaharashtraApple IdeaNo ratings yet
- Dr. Ahmed Curriculum 2019Document9 pagesDr. Ahmed Curriculum 2019Dr.Ahmed AlnoumanNo ratings yet
- 4 November 2004 DR - Supparearg DisayabutrDocument38 pages4 November 2004 DR - Supparearg DisayabutrDonnaya KrajangwittayaNo ratings yet
- 2012 Atypical Antipsychotic, A Nightmarish ProblemDocument1 page2012 Atypical Antipsychotic, A Nightmarish ProblemDiego HormacheaNo ratings yet
- Bai Thuyet Trinh Thi Cuoi HKDocument3 pagesBai Thuyet Trinh Thi Cuoi HKlee hoangNo ratings yet
- Child Poverty Uk DissertationDocument7 pagesChild Poverty Uk DissertationWillSomeoneWriteMyPaperForMeUK100% (1)
- Efektifitas Penggunaan Metode Smart Energy (REIKI) Sebagai Alternatif Preventif Hyperglikemia Pasien Diabetes Melitus Tipe 2Document14 pagesEfektifitas Penggunaan Metode Smart Energy (REIKI) Sebagai Alternatif Preventif Hyperglikemia Pasien Diabetes Melitus Tipe 2Dea ameliaNo ratings yet