Professional Documents
Culture Documents
Laparoscopic Vs Open Distal Pancreatectomy: A Single-Institution Comparative Study
Uploaded by
Hana YunikoOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Laparoscopic Vs Open Distal Pancreatectomy: A Single-Institution Comparative Study
Uploaded by
Hana YunikoCopyright:
Available Formats
PAPER
Laparoscopic vs Open Distal Pancreatectomy
A Single-Institution Comparative Study
Sandeep S. Vijan, MBBS; Kamran A. Ahmed, BS; William S. Harmsen, MS; Florencia G. Que, MD;
Kaye M. Reid-Lombardo, MD; David M. Nagorney, MD; John H. Donohue, MD;
Michael B. Farnell, MD; Michael L. Kendrick, MD
Hypothesis: Laparoscopic distal pancreatectomy (LDP) in meters squared) (mean, 27.4 vs 27.9; P=.44), or Ameri-
provides outcome advantages compared with open dis- can Society of Anesthesiologists score of 3 or higher (58%
tal pancreatectomy (ODP). vs 52%; P=.39). Tumor size was greater in the ODP group
than in the LDP group (mean, 4.0 vs 3.3 cm; P=.02). The
Design: Single-institutional, retrospective review from LDP group as compared with the ODP group demon-
January 1, 2004, to May 1, 2009. strated decreased blood loss (mean, 171 vs 519 mL;
P⬍.001) and shorter duration of hospital stay (mean, 6.1
Setting: Tertiary referral center. vs 8.6 days; P ⬍ .001). There were no differences be-
tween the LDP and ODP groups in operative time (mean,
Patients: Patients undergoing LDP (n = 100) were 214 vs 208 minutes; P =.50), pancreatic leak rate (17%
matched by age, pathologic diagnosis, and pancreatic vs 17%; P⬎.99), overall 30-day morbidity (34% vs 29%;
specimen length to a cohort undergoing ODP (n=100). P =.45), and 30-day mortality (3% vs 1%; P=.62).
Main Outcome Measures: Perioperative outcomes and Conclusions: The laparoscopic approach to distal pan-
overall 30-day morbidity and mortality. Univariate and createctomy appears to provide advantages of reduced
multivariate analyses were performed using logistic or blood loss and length of hospital stay in selected pa-
linear regression as appropriate. tients compared with the open approach. Overall com-
plication rates appear similar. Patient selection bias and
Results: Patients in the LDP group did not differ from limits of a retrospective analysis warrant prospective
those in the ODP group in age (mean, 59.0 vs 58.6 years; validation.
P=.85), sex (60% vs 50% female; P = .16), body mass in-
dex (calculated as weight in kilograms divided by height Arch Surg. 2010;145(7):616-621
W
ITH THE ADVANCES IN acceptance of laparoscopic distal pancre-
instrumentandvideo atectomy (LDP), several case series and
technology, laparo- comparative cohort studies have sug-
scopic approaches gested that laparoscopic approaches to
have gained favor in distal pancreatic resection provide simi-
many procedures and across most surgi- lar advantages that have been demon-
cal disciplines. These approaches have strated for other minimally invasive
demonstrated advantages over open ap- procedures.3-5 However, limitations of
proaches with regard to blood loss, op- selection bias, small sample size, and pool-
erative time, pain, wound morbidity, and ing of multi-institutional data have pre-
length of hospital stay in several proce- vented a meaningful comparative trial
dures. In addition to cholecystectomy, of LDP and open distal pancreatectomy
herniorrhaphy, colectomy, and bariatric (ODP). 6-9 We report a large, single-
Author Affiliations: Division of procedures, many advantages are also sug- institutional, comparative study of these
Gastroenterologic and General gested in solid organ resection such as that 2 approaches within a case-matched co-
Surgery (Drs Vijan, Que, of the liver and spleen.1,2 Laparoscopic pan- hort design, attempting to better eluci-
Reid-Lombardo, Nagorney,
creatic resection has been approached date the benefits of laparoscopy.
Donohue, Farnell, and
Kendrick and Mr Ahmed) and more cautiously and with less enthusi-
Department of Biostatistics and asm because of the retroperitoneal loca- METHODS
Epidemiology (Mr Harmsen), tion, proximity to major vasculature, and
Mayo Clinic, Rochester, propensity for postoperative complica- We conducted a retrospective review of all pa-
Minnesota. tions. Despite the apprehensive use and tients who underwent a distal pancreatec-
(REPRINTED) ARCH SURG/ VOL 145 (NO. 7), JULY 2010 WWW.ARCHSURG.COM
616
©2010 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ on 08/09/2019
tomy from January 1, 2004, to May 1, 2009, at our institution
(n=582).
All pancreatectomies were performed by experienced hepa-
topancreatic and biliary surgeons at a single institution. Fol-
lowing institutional review board approval, 100 patients un-
dergoing LDP were matched by patient age (±8 years), pathologic
diagnosis (benign vs malignant), and pancreatic specimen length
(±2 cm) to a cohort (n=100) undergoing ODP. For most, we
10 mm
were able to appropriately match cystic vs noncystic neo-
plasms and primary vs metastatic malignant neoplasms. The
hand-assisted technique was used selectively in 2 patients and
is included in the LDP group. 10
Clinicopathologic features were evaluated by comparing these mm
5 mm
10 mm
2 groups, and perioperative outcomes were sought. We re-
viewed each patient’s history for age, sex, body mass index (BMI; 2 cm
calculated as weight in kilograms divided by height in meters
10 mm
squared), American Society of Anesthesiology (ASA) score, pre-
vious abdominal surgery, pathologic diagnosis, tumor size, pan-
creatic specimen length, and concomitant operations. Specific
outcomes that were addressed included operative time (in min-
utes), operative blood loss (in milliliters), wound morbidity,
30-day major morbidity and mortality, pancreatic leak rate (in
percentage), and grade of leak (A, B, or C).
DEFINITIONS
Wound morbidity included superficial wound infections, sub-
cutaneous hematomas, and seromas. Major morbidity in-
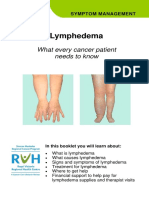
Figure. Trocar placement for laparoscopic distal pancreatectomy.
cluded pancreatic leak, intra-abdominal abscess, postopera-
Reproduced with permission from the Mayo Foundation for Medical
tive ileus, venous thromboembolism, cardiac ischemia or Education and Research. All rights reserved.
arrhythmias, reoperation, and any complication with a net effect
to significantly prolong hospital stay within 30 days from pan-
createctomy. gan resection or hernia repair, and specimen length. The ␣ level
Per International Study Group on Pancreatic Fistula10 rec- was set at .05 for statistical significance.
ommendations, pancreatic leak is defined as any measurable
volume of fluid output from a surgical or radiologically placed
drain on or after postoperative day 3 that has an amylase level OPERATIVE TECHNIQUE
3 times greater than the serum level. The presence of a peri-
pancreatic fluid collection on axial imaging with clinical sus- Although some intersurgeon variability exists, we perform LDP
picion for leak is included. in the following manner. Under general endotracheal anesthe-
Grade of pancreatic leak is also in accordance with Inter- sia, in the supine position, pneumoperitoneum is established
national Study Group on Pancreatic Fistula definitions. A grade through a 10/12 left subcostal trocar placed under direct vi-
A leak is one that has no major clinical effect on the patient’s sion using the Optiview system (Ethicon Endo-Surgery, Inc,
clinical course. Its management involves the use of oral anti- Cincinnati, Ohio). After initial abdominal exploration to rule
biotics and slow withdrawal of surgical drains. The patient is out peritoneal or visceral metastasis, a total of 3 additional 10/12
fed orally and remains clinically well. A grade B leak is one that trocars are placed. A 10-mm port in the infraumbilical loca-
entails manipulation of surgical drains or radiologic place- tion and 2 other 10-mm ports in the midclavicular lines, slightly
ment of a percutaneous drain into a peripancreatic fluid col- above the umbilical line on the left and slightly below on the
lection. Patients may or may not be kept withholding oral food right, are placed (Figure). The Harmonic Ace scalpel (Ethi-
and fluids and supported with enteral or parenteral feeds. These con Endo-Surgery, Inc) is used for most of the tissue dissec-
scenarios include hospital readmissions and delays in dis- tion. The gastrocolic ligament is transected and the lesser sac
charge. A grade C leak is one that involves major change in the is widely exposed. The mesocolon is dissected off the inferior
patient’s management. This may necessitate intensive care unit border of the pancreas and the pancreas is dissected off the ret-
monitoring, intravenous antibiotics, use of somatostatin ana- roperitoneum. The splenic vessels are dissected away from the
logues, and/or reoperation. There is typically evidence of clini- pancreas near the proposed site of pancreatic transection and
cal sepsis and resultant extended duration of hospital stay. an umbilical “shoestring” noose is placed around the pan-
creas. This is secured on the specimen side and is used for re-
traction during the remainder of the procedure. The pancre-
STATISTICAL ANALYSIS atic parenchyma is then divided with the harmonic scalpel
(preferred) or with an Endo GIA stapler (Autosuture, Nor-
Preoperative and clinicopathologic features were compared be- walk, Connecticut). If splenic preservation is indicated, the pan-
tween the LDP and ODP groups using a t test or 2 test as ap- creas is dissected off the splenic vessels; tributary vessels are
propriate. The outcomes of 30-day morbidity, major morbid- treated with the harmonic scalpel or clips. When simulta-
ity, pancreatic leak, mortality, operative blood loss (ⱕ350 mL neous splenectomy is being performed, the splenic artery and
vs ⬎350 mL), operative time (ⱕ5 hours vs ⬎5 hours), and hos- vein are ligated and divided or are transected with the Endo
pital length of stay (ⱕ7 days vs ⬎7 days) were assessed using GIA stapler. The pancreas is then retracted anteriorly and lat-
logistic regression. Multivariable models included group sta- erally with lateral dissection off the retroperitoneum. All peri-
tus, age, sex, BMI, ASA score (1 or 2 vs 3 or 4), additional or- pancreatic lymphatic tissue is taken en bloc with the speci-
(REPRINTED) ARCH SURG/ VOL 145 (NO. 7), JULY 2010 WWW.ARCHSURG.COM
617
©2010 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ on 08/09/2019
Table 1. Preoperative Features of Patients Undergoing Open Table 2. Clinicopathologic Features of Patients Undergoing
and Laparoscopic Distal Pancreatectomy Open and Laparoscopic Distal Pancreatectomy
ODP LDP P ODP LDP P
Variable (n = 100) (n = 100) Value Variable (n = 100) (n = 100) Value
Age, mean (SD), y 58.6 (15.2) 59.0 (17.3) .85 Additional organ resection or hernia 20 (20) 21 (21) .86
Female, No. (%) 50 (50) 60 (60) .16 repair, No. (%)
BMI, mean (SD) 27.9 (5.0) 27.4 (5.2) .44 Specimen length, mean (SD), cm 9.4 (3.2) 9.3 (3.4) .90
Prior abdominal surgery, No. (%) 30 (30) 44 (44) .04 Tumor size, mean (SD), cm 4.0 (2.9) 3.3 (1.9) .02
ASA score ⱖ3, No. (%) 52 (52) 58 (58) .39 Histologic diagnosis, No. (%) ⬎.99
Benign 77 (77) 77 (77) .31 a
Abbreviations: ASA, American Society of Anesthesiologists; BMI, body mass Pancreatitis 4 (4) 1 (1)
index (calculated as weight in kilograms divided by height in meters squared); Cystic 43 (43) 49 (49)
LDP, laparoscopic distal pancreatectomy; ODP, open distal pancreatectomy. Solid 30 (30) 27 (27)
Malignant 23 (23) 23 (23) ⬎.99 a
Primary 21 (21) 20 (20)
men. The short gastric vessels are divided with the harmonic Metastatic 2 (2) 3 (3)
scalpel, and the splenic attachments are lysed. The specimen
is then placed in an Endocatch II bag (Tyco Health Group, Au- Abbreviations: LDP, laparoscopic distal pancreatectomy; ODP, open distal
tosuture) and removed via the periumbilical trocar site, which pancreatectomy.
a Comparisons are between ODP and LDP groups by histologic diagnosis
is extended just enough to accommodate the specimen, typi- among patients with a benign diagnosis (P = .31) and among patients with a
cally 3 to 5 cm in length. The pancreatic stump is then treated malignant diagnosis (P ⬎ .99).
with the TissueLink device (TissueLink, Dover, New Hamp-
shire). Closed suction drains are used selectively.
The histologic diagnosis of benign vs malignant was
RESULTS not different between the 2 groups (Table 2). How-
ever, tumor size was greater in the ODP group than in
A total of 104 consecutive patients in the LDP group the LDP group (mean, 4.0 vs 3.3 cm; P = .02). Pancre-
were evaluated. In 4 cases, the procedure was converted atic adenocarcinoma represented the most common
to laparotomy due to extensive intra-abdominal adhe- malignant tumor in both the LDP group (n = 17) and
sions (n = 3) or bleeding (n = 1), yielding a 4% conver- the ODP group (n = 19), followed by neuroendocrine
sion rate. These patients were subsequently excluded carcinoma (LDP, n = 3; ODP, n = 2) and metastatic
from further analysis. renal cell carcinoma (LDP, n = 3; ODP, n = 2). Malig-
Preoperative features of all 200 patients are reported nant neoplasms were expected or biopsy proven pre-
in Table 1. Notably, the patients in the ODP group did operatively in all patients with adenocarcinoma. All
not differ from those in the LDP group in age (mean, 58.6 patients in both groups had an R0 resection per-
vs 59.0 years; P = .85), sex (50% vs 60% female; P =.16), formed, and there was no difference in the number of
BMI (mean, 27.9 vs 27.4; P = .44), or ASA score of 3 or lymph nodes harvested.
higher (52% vs 58%; P = .39). Previous abdominal op- Overall 30-day major morbidity was not different be-
erations were more common in the LDP group (44%) tween the LDP (34%) and ODP (29%) groups (odds ra-
compared with the ODP group (30%) (P = .04). tio=0.8; P =.45). Specifically, in the LDP vs ODP group,
Clinicopathologic features of patients are outlined in there was no difference in the wound morbidity (0% vs
Table 2. Of the 100 patients undergoing LDP, 25 5%; P=.06) or pancreatic leak rate (17% vs 17%; P⬎.99).
(25%) underwent a spleen-preserving pancreatectomy. In the LDP group, there were 2 grade A (2%), 14 grade B
This was accomplished only when a diagnosis of having (14%), and 1 grade C (1%) pancreatic leaks, while in the
a malignant neoplasm was not entertained preopera- ODP group, there were 1 grade A (1%) and 16 grade B
tively or intraoperatively. Twenty percent of the ODP (16%) pancreatic leaks.
group had simultaneous adjacent organ resection or The 30-day or in-hospital mortality rate was not sta-
hernia repair vs 21% of the LDP group (P = .86). Opera- tistically different between the LDP group (3 cases [3%])
tive drains were used in 82% of ODP cases and 36% of and the ODP group (1 case [1%]) (P = .62). Three pa-
LDP cases. tients in the LDP group died postoperatively of pulmo-
Univariate and multivariate analyses are reported in nary embolus (n=2) or complications of pancreatic leak
Table 3. For the LDP group as compared with the ODP (n=1), and 1 patient in the ODP group died of pulmo-
group, operative time was not different (mean, 214 vs nary embolus.
208 minutes; P=.50); however, blood loss was less (mean, The length of hospital stay was shorter in the LDP
171 vs 519 mL; P ⬍ .001). When outcome data were di- group (mean [SD], 6.1 [2.4] days) compared with the
chotomized, a patient in the ODP group relative to a pa- ODP group (mean [SD], 8.6 [5.9] days) (P⬍.001). A pa-
tient in the LDP group had increased odds of a blood vol- tient who underwent ODP relative to a patient who un-
ume loss greater than 350 mL (Table 3). This association derwent LDP had increased odds that their hospital stay
persisted in the multivariable models that also included would exceed 7 days (odds ratio=3.5; 95% confidence
the variables age, sex, BMI, ASA score (1 or 2 vs 3 or 4), interval, 1.8-6.8); this association remained significant
additional organ resection or hernia repair, and speci- in the multivariable model (odds ratio=3.9; 95% confi-
men length. dence interval, 2.0-7.8).
(REPRINTED) ARCH SURG/ VOL 145 (NO. 7), JULY 2010 WWW.ARCHSURG.COM
618
©2010 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ on 08/09/2019
Table 3. Univariate and Multivariable Analyses of Perioperative Outcome Measures of Patients
Undergoing Open and Laparoscopic Distal Pancreatectomy
Univariate Multivariable a
Patients,
Outcome No. (%) OR (95% CI) P Value OR (95% CI) P Value
Operative blood loss ⬎350 mL
ODP 52 (52) 9.8 (4.6-20.9) ⬍.001 10.6 (4.7-23.6) ⬍.001
LDP 10 (10)
Operative time ⬎3.5 h
ODP 40 (40) 0.8 (0.5-1.4) .47 0.7 (0.4-1.3) .30
LDP 45 (45)
Wound morbidity
ODP 5 (5) ⬁ .06 NA b NA
LDP 0
Major morbidity
ODP 29 (29) 0.8 (0.4-1.4) .45 0.8 (0.4-1.5) .48
LDP 34 (34)
Pancreatic leak
ODP 17 (17) 1.0 (0.5-2.1) ⬎.99 1.0 (0.4-2.1) .94
LDP 17 (17)
Mortality
ODP 1 (1) 0.3 (0.03-3.2) .62 NA b NA
LDP 3 (3)
Length of hospital stay ⬎7 d
ODP 42 (42) 3.5 (1.8-6.8) .002 3.9 (2.0-7.8) ⬍.001
LDP 17 (17)
Abbreviations: CI, confidence interval; LDP, laparoscopic distal pancreatectomy; NA, not applicable; ODP, open distal pancreatectomy; OR, odds ratio.
a Multivariable model included patient age, sex, body mass index, American Society of Anesthesiologists score (1 or 2 vs 3 or 4), additional organ resection or
hernia repair, and specimen length.
b Multivariable model not performed owing to low number of events.
COMMENT leak and differences in practice patterns with regard to
duration of hospital stay.
Despite the lack of level 1 evidence for LDP, more cen- The only other 2 comparative series to our knowl-
ters are adopting this technique. Current supporting evi- edge are by Velanovich11 and Teh et al.12 In both stud-
dence for this approach exists only in retrospective case ies, the LDP group again demonstrated a shorter hospi-
series6,8,9 and a few case-control studies.3,4,7 tal stay and lower overall morbidity. Unfortunately, both
Notable is the recent work of Kooby et al,3 a large multi- of these studies are small and underpowered, and the lat-
institutional case-control study in which 142 LDPs were ter is based on an unmatched cohort and is therefore most
compared with 200 ODPs. Patients were matched based susceptible to selection bias.
on age, pathologic findings, ASA criteria, and pancre- To our knowledge, our study is the largest single-
atic specimen length. Similar to our findings, Kooby and institution experience comparing LDP with ODP. While
colleagues documented a significant decrease in blood this study suggests that the laparoscopic approach re-
loss (mean [SD], 357 [497] mL) and hospital stay (mean duced blood loss and length of hospital stay, there are sev-
[SD], 5.9 [3.8] days) for patients undergoing LDP. How- eral limitations and outcomes that warrant further discus-
ever, operative time was not different between the 2 sion. The observed 30-day mortality rate was 3% in our LDP
groups, and there was no increase in major morbidity group and 1% in the ODP group. While this did not reach
(40%) or pancreatic leak rate (28%) with the laparo- statistical difference, the rate for LDP appears higher than
scopic approach; reported mortality was 0%. This study that reported by others.3,4,11,12 The 3 patient deaths in this
is limited by its multi-institutional, retrospective nature study were due to pulmonary embolism (n=2, confirmed
and the variability in experience of one center to an- by autopsy in one and clinically suspected in the other) and
other. Only 3 institutions in this study were considered uncontrolled pancreatic leak (n=1). Fatal pulmonary em-
high-volume centers, performing more than 30 LDPs per boli occurred in 2 patients who underwent LDP with sple-
year; the overall conversion rate to laparotomy was 13%. nectomy for malignancy, one with ductal adenocarci-
Eom et al4 also published case-matched analyses noma and the other with neuroendocrine carcinoma. Both
with 31 LDPs and 62 ODPs. Eom and colleagues re- had an initial uncomplicated course without evidence of
ported shorter hospital stay (11.5 days for LDP vs 13.5 pancreatic leak or deep venous thrombosis and were dis-
days for ODP) but no difference in operative time, missed home on postoperative days 7 and 13; deaths oc-
transfusion requirement, or overall morbidity. The pan- curred on postoperative days 14 and 15 while the patients
creatic leak rate was 9.7% for LDP. This study may not were at home. Both patients received subcutaneous un-
be directly comparable to published Western series, fractionated heparin and mechanical compression for deep
however, due to the ambiguous definition of pancreatic venous thrombosis prophylaxis during hospitalization, had
(REPRINTED) ARCH SURG/ VOL 145 (NO. 7), JULY 2010 WWW.ARCHSURG.COM
619
©2010 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ on 08/09/2019
no history of venous thromboembolic disease, and did not nant stump was sutured closed (80%). Inevitably, the
demonstrate postsplenectomy thrombocytosis. Both pa- search continues for a better technique of pancreatic di-
tients had a 3- to 4-hour drive home after discharge. It has vision and stump treatment to significantly reduce or ame-
been suggested that increased intra-abdominal pressure en- liorate the complication of pancreatic fistula.
hances venous stasis, reduces intraoperative portal ve- Tumor size was statistically different between the 2
nous blood flow, and enhances the activation of coagula- groups in this study, albeit the mean difference was only 7
tion and fibrinolysis13-15; however, appropriate deep venous mm (4.0 mm for the ODP group vs 3.3 mm for the LDP
thrombosis prophylaxis as was used in these patients should group). We did not match for tumor size but rather chose
minimize this risk.16 Both of these patients had been diag- to match for factors we felt would directly affect operative
nosed as having malignancy and 1 had obesity (BMI of 38), time and outcome such as indication (benign or malig-
which are known risk factors for postoperative thrombo- nant) and extent of operation (pancreatic specimen length).
embolism. It remains unclear and unlikely that these deaths Although we attempted to circumvent selection bias
were directly attributable to the laparoscopic approach. In through cohort matching, a certain degree of bias is in-
the ODP group, the single death was also in a patient un- herent with any study outside of a randomized con-
dergoing ODP for pancreatic ductal adenocarcinoma. Ad- trolled design. However, it is our opinion that some se-
ditionally, 3 other patients in the ODP group had throm- lection bias is necessary and appropriate when evaluating
boembolic complications, suggesting that these patients are a new approach or technology to improve the likeli-
at high risk irrespective of the approach used. The third hood of success and reduce patient risk for such novel
patient who died in the LDP group had undergone a spleen- advances. While this study confirms the advantages and
preserving pancreatectomy for intraductal papillary mu- success of the laparoscopic approach for distal pancre-
cinous neoplasm. The patient was dismissed on postop- atectomy in these matched patients, it does not imply that
erative day 4 when clinically well. On postoperative day all patients will achieve superior results; such a broad state-
7, he called with abdominal pain and was referred to his ment will require a randomized controlled trial.
local hospital for initial evaluation and potential transfer. The laparoscopic approach to distal pancreatectomy ap-
Unfortunately, contact with the patient was lost and the pears to provide advantages of less blood loss and shorter
patient was admitted with a presumed bowel obstruction. length of hospital stay in selected patients compared with
After several days of observation, a computed tomo- the open approach. Overall complication rates, however,
graphic scan identified a fluid collection in the pancreatic appear similar between the 2 groups. Patient selection bias
resection bed and a decision was made for laparotomy on and limits of a retrospective analysis warrant prospective
postoperative day 12. The fluid collection was evacuated controlled trials to validate the advantages of the laparo-
and, by report, the pancreatic stump was débrided. The pro- scopic approach in distal pancreatectomy.
cedure was complicated by a portal vein injury and the pa-
tient died of massive hemorrhage with exsanguination. Accepted for Publication: February 19, 2010.
The overall morbidity in our study was not different Correspondence: Michael L. Kendrick, MD, Division of
between LDP and ODP. The incidence of postoperative Gastroenterologic and General Surgery, Mayo Clinic,
pancreatic leak, the most common major morbidity af- MA-W12, 200 First St SW, Rochester, MN 55905
ter distal pancreatectomy, was not different. Encompass- (kendrick.michael@mayo.edu).
ing all grades of leak, we observed a leak rate of 17%, Author Contributions: Study concept and design: Vijan,
which is comparable or favorable to that reported by oth- Reid-Lombardo, and Kendrick. Acquisition of data: Vi-
ers.3,17 When excluding clinically insignificant leaks (grade jan, Ahmed, and Kendrick. Analysis and interpretation of
A), the leak rate was also similar between groups. The data: Vijan, Harmsen, Que, Nagorney, Donohue, Far-
use of prophylactic surgical drains was more common nell, and Kendrick. Drafting of the manuscript: Vijan,
in the ODP group (82%) than in the LDP group (36%). Ahmed, Harmsen, Reid-Lombardo, and Kendrick. Criti-
This difference is largely attributed to a single surgeon’s cal revision of the manuscript for important intellectual con-
preference (M.L.K.), where drains are rarely used. Be- tent: Harmsen, Que, Reid-Lombardo, Nagorney, Dono-
cause grade A leaks may be based solely on the level of hue, Farnell, and Kendrick. Statistical analysis: Vijan and
amylase from drain effluent, undetection of some grade Harmsen. Administrative, technical, and material sup-
A leaks may have occurred in patients without prophy- port: Vijan, Ahmed, Reid-Lombardo, and Kendrick. Study
lactic drains. It is our impression, however, that clini- supervision: Que, Farnell, and Kendrick.
cally significant leaks will not be missed as it is our prac- Financial Disclosure: None reported.
tice to image patients with any clinical suspicion of Previous Presentation: This paper was presented at the
pancreatic stump leak. Several methods of transecting the 117th Scientific Session of the Western Surgical Asso-
pancreas and treating the pancreatic stump have been re- ciation; November 9, 2009; San Antonio, Texas; and is
ported in an effort to reduce this serious complication published after peer review and revision. The discus-
after pancreatic resection. The method of pancreatic tran- sions that follow this article are based on the originally
section varied between the LDP and ODP groups. In most submitted manuscript and not the revised manuscript.
patients in the LDP group, the pancreas was transected
by harmonic scalpel (75%) or Endo GIA stapler (25%) REFERENCES
and the remnant stump was treated with TissueLink
(75%), whereas in the ODP group, pancreatic transec- 1. Katkhouda N, Hurwitz MB, Rivera RT, et al. Laparoscopic splenectomy: out-
tion was performed with electrocautery (60%) or Endo come and efficacy in 103 consecutive patients. Ann Surg. 1998;228(4):568-
GIA stapler (40%) and, when deemed necessary, the rem- 578.
(REPRINTED) ARCH SURG/ VOL 145 (NO. 7), JULY 2010 WWW.ARCHSURG.COM
620
©2010 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ on 08/09/2019
2. Kaneko H. Laparoscopic hepatectomy: indications and outcomes. J Hepatobili- postoperative day 7, was early discharge a factor and does this
ary Pancreat Surg. 2005;12(6):438-443. imply that patients should stay close at hand for a few days af-
3. Kooby DA, Gillespie T, Bentrem D, et al. Left-sided pancreatectomy: a multi- ter discharge before heading home? Should the pancreatic duct
center comparison of laparoscopic and open approaches. Ann Surg. 2008;
be handled differently from a technical standpoint to mini-
248(3):438-446.
4. Eom BW, Jang JY, Lee SE, Han HS, Yoon YS, Kim SW. Clinical outcomes com-
mize the risk of leak? Could venous thromboembolism be pre-
pared between laparoscopic and open distal pancreatectomy. Surg Endosc. 2008; vented by continuing Lovenox through a long car ride home?
22(5):1334-1338. Third, the authors performed a laparoscopic spleen-
5. Mabrut JY, Fernandez-Cruz L, Azagra JS, et al; Hepatobiliary and Pancreatic Sec- preserving procedure in 25% of patients. How often was lapa-
tion (HBPS) of the Royal Belgian Society of Surgery; Belgian Group for Endo- roscopic splenic preservation attempted unsuccessfully? How
scopic Surgery (BGES); Club Coelio. Laparoscopic pancreatic resection: results common is spleen preservation at the authors’ institution when
of a multicenter European study of 127 patients. Surgery. 2005;137(6):597- the operation is done open? What are the current indications
605. at the Mayo Clinic in adults for considering splenic preserva-
6. Melotti G, Butturini G, Piccoli M, et al. Laparoscopic distal pancreatectomy: re-
tion (for example, IPMN [intraductal papillary mucinous neo-
sults on a consecutive series of 58 patients. Ann Surg. 2007;246(1):77-82.
7. Nakamura Y, Uchida E, Aimoto T, Matsumoto S, Yoshida H, Tajiri T. Clinical out-
plasm], small mucinous or neuroendocrine tumors, antici-
come of laparoscopic distal pancreatectomy. J Hepatobiliary Pancreat Surg. 2009; pated benign histology)?
16(1):35-41. Dr Kendrick: First, with respect to the 4 patients who were
8. Pryor A, Means JR, Pappas TN. Laparoscopic distal pancreatectomy with splenic excluded from the laparoscopic group, 3 of those patients were
preservation. Surg Endosc. 2007;21(12):2326-2330. converted to an open procedure for adhesions; they all had sig-
9. Laxa BU, Carbonell AM II, Cobb WS, et al. Laparoscopic and hand-assisted dis- nificant prior abdominal operations. One patient was con-
tal pancreatectomy. Am Surg. 2008;74(6):481-487. verted for bleeding from the splenic vein during the proce-
10. Bassi C, Dervenis C, Butturini G, et al; International Study Group on Pancreatic dure. As far as intention to treat, to my knowledge none of them
Fistula Definition. Postoperative pancreatic fistula: an international study group
developed a pancreatic leak or prolonged hospital stay.
(ISGPF) definition. Surgery. 2005;138(1):8-13.
11. Velanovich V. Case-control comparison of laparoscopic vs open distal
Your second question was regarding our change in manage-
pancreatectomy. J Gastrointest Surg. 2006;10(1):95-98. ment based on our experience with thromboembolic complica-
12. Teh SH, Tseng D, Sheppard BC. Laparoscopic and open distal pancreatic resec- tions. As mentioned, we had 2 deaths that were directly attrib-
tion for benign pancreatic disease. J Gastrointest Surg. 2007;11(9):1120-1125. uted to pulmonary embolism. In both of these patients, this
13. Milic DJ, Pejcic VD, Zivic SS, et al. Coagulation status and the presence of post- complication occurred 2 weeks postoperatively and these pa-
operative deep vein thrombosis in patients undergoing laparoscopic tients had no other evidence of complications during their hos-
cholecystectomy. Surg Endosc. 2007;21(9):1588-1592. pital stay or afterwards. Because of these events, we also looked
14. Lord RV, Ling JJ, Hugh TB, Coleman MJ, Doust BD, Nivison-Smith I. Incidence at the open group, and interestingly 4 of those patients had sig-
of deep vein thrombosis after laparoscopic vs minilaparotomy cholecystectomy.
nificant thromboembolic complications, 3 of them with pulmo-
Arch Surg. 1998;133(9):967-973.
15. Garg PK, Teckchandani N, Hadke NS, Chander J, Nigam S, Puri SK. Alteration in
nary embolus. The 1 death that occurred in the open group was
coagulation profile and incidence of DVT in laparoscopic cholecystectomy. Int J also a patient who died of a pulmonary embolus after resection
Surg. 2009;7(2):130-135. for adenocarcinoma. This has raised our concern with respect
16. Richardson W, Apelgren K, Earle D, Fanelli R. Guidelines for deep venous throm- to patients who undergo pancreatectomy for ductal adenocar-
bosis prophylaxis during laparoscopic surgery. Surg Endosc. 2007;21(12): cinoma irrespective of whether it is performed laparoscopically
2331-2334. or open. These patients had routine perioperative DVT [deep ve-
17. Alexakis N, Sutton R, Neoptolemos JP. Surgical treatment of pancreatic fistula. nous thrombosis] prophylaxis and we feel that consideration
Dig Surg. 2004;21(4):262-274. should be given to prophylaxis or full anticoagulation for up to
1 month postoperatively in these selected patients.
You had asked whether early discharge may be a factor in
DISCUSSION
the perioperative deaths. Pulmonary embolus occurred in asymp-
tomatic patients 2 weeks postoperatively without any other com-
Jeffrey E. Lee, MD, Houston, Texas: Drs Vijan, Kendrick, and plications noted during their hospital stay or after discharge.
their colleagues from the Mayo Clinic emphasize that mini- Because of this, it is not clear whether the timing of discharge
mally invasive distal pancreatectomy is being increasingly per- is a significant factor in these patients. The third death oc-
formed, yet randomized trials of this procedure have not been curred in a patient who was dismissed on postoperative day 4
done and there have been relatively few high-quality compari- who remained asymptomatic until day 7. This patient was man-
son studies published. The results presented here confirm that aged elsewhere for a leak and unfortunately underwent surgi-
laparoscopic distal pancreatectomy can generally be per- cal débridement complicated by hemorrhage that caused his
formed safely in selected patients and that one can anticipate death. Although we see or contact our patients routinely after
benefits similar to those achieved in patients who undergo other discharge to avoid this type of problem, this patient under-
minimally invasive abdominal operations, including a shorter scores the importance of close follow-up and communication
hospital stay. I have 3 questions. with their local health care providers.
First, the authors report that they excluded 4 patients who Finally, in terms of indications for spleen-preserving distal
required conversion from a laparoscopic to an open proce- pancreatectomy, we feel that any patient without an invasive
dure. From the intent-to-treat standpoint, it would be prefer- malignancy is a potential candidate for spleen preservation. Mu-
able to describe the outcomes of these patients. Did any of these cinous cyst adenomas and side-branch IPMNs are the most fre-
patients suffer a postoperative complication? quent indications for spleen preservation in our experience. In
Second, is there any change in management recommended our laparoscopic experience, we have had 1 patient who was
as a result of the deaths that occurred in 3 patients who un- intended to undergo a spleen-preserving procedure where bleed-
derwent laparoscopic distal pancreatectomy? Since the only ing from the splenic vein necessitated splenectomy.
deaths in this series occurred following discharge and since a
pancreatic leak often does not manifest itself until on or after Financial Disclosure: None reported.
(REPRINTED) ARCH SURG/ VOL 145 (NO. 7), JULY 2010 WWW.ARCHSURG.COM
621
©2010 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ on 08/09/2019
You might also like
- Huber 2011 How Should We Define Health PDFDocument3 pagesHuber 2011 How Should We Define Health PDFLeidy Bueno Arias100% (1)
- Legislator Email on Safe Patient HandlingDocument5 pagesLegislator Email on Safe Patient HandlingAnonymous dcpGmD60% (5)
- Urinary Catheter Core Care Plan September 2015 PDFDocument2 pagesUrinary Catheter Core Care Plan September 2015 PDFAsh Staley Delvin SparkNo ratings yet
- Short-Term Surgical and Long-Term Survival Outcomes After Laparoscopic Distal Gastrectomy With D Lymphadenectomy For Gastric CancerDocument7 pagesShort-Term Surgical and Long-Term Survival Outcomes After Laparoscopic Distal Gastrectomy With D Lymphadenectomy For Gastric CancerThế VũNo ratings yet
- Fonc 09 00597Document13 pagesFonc 09 00597Giann PersonaNo ratings yet
- Laparoscopia Versus Laparotomía para El Manejo Del Traumatismo Abdominal - Revisión Sistemática y MetanálisisDocument13 pagesLaparoscopia Versus Laparotomía para El Manejo Del Traumatismo Abdominal - Revisión Sistemática y MetanálisisLuis Miguel Díaz VegaNo ratings yet
- Distal Pancreatectomy Outcomes: Perspectives From A Community-Based Teaching InstitutionDocument6 pagesDistal Pancreatectomy Outcomes: Perspectives From A Community-Based Teaching InstitutionmfachrezaaNo ratings yet
- WarshawDocument11 pagesWarshawJuan RamirezNo ratings yet
- Gastrectomía LaparoscópicaDocument7 pagesGastrectomía LaparoscópicaGreyza VelazcoNo ratings yet
- Bun V34N3p223Document6 pagesBun V34N3p223pingusNo ratings yet
- 10.1016@S1470 20451930318 3Document10 pages10.1016@S1470 20451930318 3FistiNo ratings yet
- Versus: Laparoscopic Open Appendectomy: Which Way To Go?Document6 pagesVersus: Laparoscopic Open Appendectomy: Which Way To Go?Claudiu Ungureanu ClauNo ratings yet
- Long-Term Outcomes of Primary Endoscopic Resection Vs Surgery For T1Document16 pagesLong-Term Outcomes of Primary Endoscopic Resection Vs Surgery For T1ellya zalfaNo ratings yet
- 1 Bjs 10662Document8 pages1 Bjs 10662Vu Duy KienNo ratings yet
- A Randomized Trial of Laparoscopic Versus Open Surgery For Rectal CancerDocument9 pagesA Randomized Trial of Laparoscopic Versus Open Surgery For Rectal CancerFarizka Dwinda HNo ratings yet
- armijo2020Document7 pagesarmijo2020Yeudiel SuroNo ratings yet
- 1 s2.0 S1743919116308421 MainDocument10 pages1 s2.0 S1743919116308421 MainRony RonyNo ratings yet
- 10 Carcinomatoza PeritonealaDocument9 pages10 Carcinomatoza PeritonealaGabriela MilitaruNo ratings yet
- Ramirez 2013Document10 pagesRamirez 2013Nadia Farah FadhilaNo ratings yet
- Simultaneous Versus Delayed Resection For Initially Resectable Synchronous Colorectal Cancer Liver MetastasesDocument8 pagesSimultaneous Versus Delayed Resection For Initially Resectable Synchronous Colorectal Cancer Liver MetastasesDr Shiv ChopraNo ratings yet
- Efficacy of EUS-RFA in Pancreatic Tumors: Is It Ready For Prime Time? A Systematic Review and Meta-AnalysisDocument9 pagesEfficacy of EUS-RFA in Pancreatic Tumors: Is It Ready For Prime Time? A Systematic Review and Meta-AnalysisRadinal MauludiNo ratings yet
- Laparaskopi PeritonitisDocument5 pagesLaparaskopi PeritonitisPutri RiszaNo ratings yet
- Goh 2019Document5 pagesGoh 2019Maya RafidaNo ratings yet
- The Incidence and Risk of Early Postoperative Small Bowel Obstruction After Laparoscopic Resection For Colorectal Cancer 2014Document7 pagesThe Incidence and Risk of Early Postoperative Small Bowel Obstruction After Laparoscopic Resection For Colorectal Cancer 2014alemago90No ratings yet
- 268 2011 Article 1088 PDFDocument6 pages268 2011 Article 1088 PDFIoel Tovar TrovaNo ratings yet
- Laparoscopic Versus Open Surgery For Gastric Gastrointestinal Stromal Tumors: A Propensity Score Matching AnalysisDocument10 pagesLaparoscopic Versus Open Surgery For Gastric Gastrointestinal Stromal Tumors: A Propensity Score Matching AnalysisFerdian PriantoNo ratings yet
- Open Versus Laparoscopic Cholecystectomy A ComparaDocument5 pagesOpen Versus Laparoscopic Cholecystectomy A ComparaChintya EltaNo ratings yet
- JCM 10 01853Document16 pagesJCM 10 01853Katrina Mae FajardoNo ratings yet
- Comparison of Perioperative Outcomes Between Laparoscopic and Open Approach For PancreatoduodenectomyDocument9 pagesComparison of Perioperative Outcomes Between Laparoscopic and Open Approach For PancreatoduodenectomyVu Duy KienNo ratings yet
- Appendicitis NaddlerDocument6 pagesAppendicitis NaddlerMedardo ApoloNo ratings yet
- Percutaneous Needle Aspiration Versus Catheter Drainage in Treating Hepatic AbscessDocument8 pagesPercutaneous Needle Aspiration Versus Catheter Drainage in Treating Hepatic AbscessRatna TriasnawatiNo ratings yet
- MOC IV 2014 Laparoscopy and Elective Colon Resection June 2012Document18 pagesMOC IV 2014 Laparoscopy and Elective Colon Resection June 2012pingusNo ratings yet
- A Randomized Trial of Laparoscopic Versus Open Surgery For Rectal CancerDocument9 pagesA Randomized Trial of Laparoscopic Versus Open Surgery For Rectal CancerOtoyGethuNo ratings yet
- Loop Vs DividedDocument8 pagesLoop Vs DividedNatalindah Jokiem Woecandra T. D.No ratings yet
- Kumar Et Al. - 2016 - International Myeloma Working Group Consensus CritDocument19 pagesKumar Et Al. - 2016 - International Myeloma Working Group Consensus CritCarina MoitaNo ratings yet
- Laparoscopic Versus Open Cholecystectomy For Patients With Symptomatic CholecystolithiasisDocument2 pagesLaparoscopic Versus Open Cholecystectomy For Patients With Symptomatic CholecystolithiasisNad-Ya KatherineNo ratings yet
- Anastomosis After LaparoscopicDocument16 pagesAnastomosis After LaparoscopicDuratul FahliaNo ratings yet
- European Journal of Surgical Oncology: Review ArticleDocument12 pagesEuropean Journal of Surgical Oncology: Review ArticleWarren SeowNo ratings yet
- Eras SystectomyDocument9 pagesEras Systectomymehmet kabaaliNo ratings yet
- ESMO Recommendations For NGSDocument15 pagesESMO Recommendations For NGSsagarkarvandeNo ratings yet
- Laparoscopic Versus Open Transhiatal Esophagectomy For Distal and Junction CancerDocument6 pagesLaparoscopic Versus Open Transhiatal Esophagectomy For Distal and Junction CancerDea Melinda SabilaNo ratings yet
- Meta-Analysis of Prophylactic Abdominal Drainage in Pancreatic SurgeryDocument9 pagesMeta-Analysis of Prophylactic Abdominal Drainage in Pancreatic SurgeryMauro MorelNo ratings yet
- 702 1383 1 PB PDFDocument7 pages702 1383 1 PB PDFEko RistiyantoNo ratings yet
- Laparoscopic Versus Open Appendicectomy: A Comparative StudyDocument7 pagesLaparoscopic Versus Open Appendicectomy: A Comparative StudyChristianWicaksonoNo ratings yet
- Article - Laparoscopic Versus Open Surgery For Rectal Cancer (COLOR II) - Short-Term Outcomes of A Randomised, Phase 3 Trial - 2013Document9 pagesArticle - Laparoscopic Versus Open Surgery For Rectal Cancer (COLOR II) - Short-Term Outcomes of A Randomised, Phase 3 Trial - 2013Trí Cương NguyễnNo ratings yet
- 5 Shabanzadeh2012Document12 pages5 Shabanzadeh2012dw21541No ratings yet
- Tobert 2023Document8 pagesTobert 2023Will CKNo ratings yet
- Timing of Surgical Resection For Curative Colorectal Cancer With Liver MetastasisDocument6 pagesTiming of Surgical Resection For Curative Colorectal Cancer With Liver MetastasisdorissjbNo ratings yet
- Reoperative Antireflux Surgery For Failed Fundoplication: An Analysis of Outcomes in 275 PatientsDocument8 pagesReoperative Antireflux Surgery For Failed Fundoplication: An Analysis of Outcomes in 275 PatientsDiego Andres VasquezNo ratings yet
- Cytoreductive Surgery and IntraperitonealDocument11 pagesCytoreductive Surgery and IntraperitonealJorge FallasNo ratings yet
- Meta 1 - Zheng X - 2018Document9 pagesMeta 1 - Zheng X - 2018matheus.verasNo ratings yet
- Brachytherapy For The Palliation of Dysphagia Owing To Esop - 2017 - RadiotherapDocument8 pagesBrachytherapy For The Palliation of Dysphagia Owing To Esop - 2017 - RadiotherapFlorin AchimNo ratings yet
- Assessment of Enhanced Recovery After Surgery (Erasâ®) Protocol in Colorectal Cancer SurgeryDocument8 pagesAssessment of Enhanced Recovery After Surgery (Erasâ®) Protocol in Colorectal Cancer SurgeryIJAR JOURNALNo ratings yet
- Locoregional Treatments Obsolete For Patients With Cancer With Liver MetastasesDocument18 pagesLocoregional Treatments Obsolete For Patients With Cancer With Liver MetastasesDR. SUMANTRA RAYNo ratings yet
- 1-s2.0-S0022480417303529-mainDocument6 pages1-s2.0-S0022480417303529-mainEva ArdianahNo ratings yet
- Tratamiento Esofago Cervical Lu, 2021Document9 pagesTratamiento Esofago Cervical Lu, 2021Carlos N. Rojas PuyolNo ratings yet
- Baratti. Peritoneal sarcomatosis. Ann surg Oncol 2010Document9 pagesBaratti. Peritoneal sarcomatosis. Ann surg Oncol 2010Juan Torres MeleroNo ratings yet
- A Prospective Treatment Protocol For Outpatient Laparoscopic Appendectomy For Acute AppendicitisDocument5 pagesA Prospective Treatment Protocol For Outpatient Laparoscopic Appendectomy For Acute AppendicitisBenjamin PaulinNo ratings yet
- OutDocument9 pagesOutMaria PalNo ratings yet
- Comparison of Laparoscopic vs. Open Surgery For Rectal CancerDocument7 pagesComparison of Laparoscopic vs. Open Surgery For Rectal Cancermohammed askarNo ratings yet
- Clinical Outcomes of Laparoscopic Surgery For Transverse and Descending Colon Cancers in A Community SettingDocument6 pagesClinical Outcomes of Laparoscopic Surgery For Transverse and Descending Colon Cancers in A Community SettingpingusNo ratings yet
- Lung Cancer Current Therapies and New Targeted TreatmentsDocument13 pagesLung Cancer Current Therapies and New Targeted TreatmentsWlad PaCaNo ratings yet
- The SAGES Manual of Flexible EndoscopyFrom EverandThe SAGES Manual of Flexible EndoscopyPeter NauNo ratings yet
- BAB I PancreatoblastomaDocument5 pagesBAB I PancreatoblastomaHana YunikoNo ratings yet
- What Is Language TestingDocument2 pagesWhat Is Language TestingHana YunikoNo ratings yet
- What Is Language TestingDocument2 pagesWhat Is Language TestingHana YunikoNo ratings yet
- Attendant E.CDocument2 pagesAttendant E.CHana YunikoNo ratings yet
- Vocab AnimalsDocument2 pagesVocab AnimalsHana YunikoNo ratings yet
- AbstractDocument1 pageAbstractHana YunikoNo ratings yet
- AbstractDocument1 pageAbstractHana YunikoNo ratings yet
- AbstractDocument1 pageAbstractHana YunikoNo ratings yet
- Epidemiology of Sport-Related Spinal Cord Injuries: A Systematic ReviewDocument10 pagesEpidemiology of Sport-Related Spinal Cord Injuries: A Systematic Reviewanna widiaNo ratings yet
- Young InfantDocument69 pagesYoung InfantAurora Doris BatagaNo ratings yet
- ACCP Standards of PracticeDocument4 pagesACCP Standards of Practiceryuurecca0% (1)
- Factors Affecting The Outcomes of Direct Pulp Capping Using BiodentineDocument9 pagesFactors Affecting The Outcomes of Direct Pulp Capping Using BiodentineyesikaichaaNo ratings yet
- Type of Hospital AdmissionDocument2 pagesType of Hospital AdmissionPenugasan PerpanjanganNo ratings yet
- FLEP ScoreDocument6 pagesFLEP ScoreSaravanan SuthanthiranathanNo ratings yet
- Optima Health 2023 2024 Cova - Benefits Brochure FinalDocument8 pagesOptima Health 2023 2024 Cova - Benefits Brochure FinalKobusNo ratings yet
- Prevalence of and Factors Associated With Nurse Burnout in The USDocument11 pagesPrevalence of and Factors Associated With Nurse Burnout in The USSMA N 1 TOROHNo ratings yet
- Guideline On The Treatment of Premenstrual Dysphoric Disorder (PMDD)Document14 pagesGuideline On The Treatment of Premenstrual Dysphoric Disorder (PMDD)Detya PertiwiNo ratings yet
- Clinical Presentation On AppendicectomyDocument30 pagesClinical Presentation On AppendicectomyValarmathiNo ratings yet
- Lymphedema BrochureDocument8 pagesLymphedema BrochureJose MiaNo ratings yet
- PDGMDocument39 pagesPDGMLaluMohan KcNo ratings yet
- Add (Acute Diarrhoeal Disease)Document46 pagesAdd (Acute Diarrhoeal Disease)Mohamed Mahroof100% (1)
- 2.standards of Midwifery PracticeDocument22 pages2.standards of Midwifery PracticeVeena DalmeidaNo ratings yet
- SEXUAL HEALTH AND HYGIENE LESSON 6Document9 pagesSEXUAL HEALTH AND HYGIENE LESSON 6Nikka GoenettNo ratings yet
- Association & Causation 6Document13 pagesAssociation & Causation 6Mongolian MutuNo ratings yet
- Hvac WorksDocument4 pagesHvac WorksSaleem BashaNo ratings yet
- Invigilation Time Table 2022Document3 pagesInvigilation Time Table 2022ThomasNo ratings yet
- Walaa SNC Network List Mar 2021Document9 pagesWalaa SNC Network List Mar 2021ning yangNo ratings yet
- Medicaid Medical Record DocumentationDocument3 pagesMedicaid Medical Record DocumentationRam KumarNo ratings yet
- Vietfair - Lịch triển lãm 2022 - EDocument3 pagesVietfair - Lịch triển lãm 2022 - EThao NguyenNo ratings yet
- Sorbion SachetsDocument3 pagesSorbion SachetsReil_InsulaNo ratings yet
- Safe Patient HandlingDocument2 pagesSafe Patient Handlingapi-3697326No ratings yet
- Hafizuddin Azfar (Els 1265)Document46 pagesHafizuddin Azfar (Els 1265)Mohd hafiz AzmiNo ratings yet
- Potent Antioxidant Acacia catechu ExtractDocument1 pagePotent Antioxidant Acacia catechu ExtractmdibashaNo ratings yet
- The Journal of Contemporary Dental PracticeDocument7 pagesThe Journal of Contemporary Dental Practicegone goneNo ratings yet
- Niple PainDocument13 pagesNiple PainPUPUT NUGRAHANo ratings yet