Professional Documents
Culture Documents
Elastography in The Evaluation of Thyroid Nodules in Children - Expanding The Field of Ultrasound To Reduce The Need For Invasive Procedures
Uploaded by
Paulo E M SouzaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Elastography in The Evaluation of Thyroid Nodules in Children - Expanding The Field of Ultrasound To Reduce The Need For Invasive Procedures
Uploaded by
Paulo E M SouzaCopyright:
Available Formats
Original
Cunha GB et al. Article
/ Elastography of thyroid nodules in children http://dx.doi.org/10.1590/0100-3984.2018.0034
Elastography for the evaluation of thyroid nodules in pediatric
patients
A elastografia na avaliação de nódulos tireoidianos em pacientes pediátricos
Gustavo Bittar Cunha1,a, Luciana Cristante Izar Marino1,b, André Yamaya1,c, Cristiane Kochi1,d, Osmar Monte1,e,
Carlos Alberto Longui1,f, Adriano Namo Cury1,g, Eduardo de Faria Castro Fleury1,h
1. Irmandade da Santa Casa de Misericórdia de São Paulo, São Paulo, SP, Brazil.
Correspondence: Dr. Gustavo Bittar Cunha. Irmandade da Santa Casa de Misericórdia de São Paulo. Rua Doutor Cesário Mota Júnior, 112,
Vila Buarque. São Paulo, SP, Brazil, 01221-020. Email: gbittarcunha@gmail.com.
a. https://orcid.org/0000-0001-8014-1409; b. https://orcid.org/0000-0002-8257-3691; c. https://orcid.org/0000-0002-4454-6465;
d. https://orcid.org/0000-0003-2727-8646; e. https://orcid.org/0000-0002-2549-9237; f. https://orcid.org/0000-0002-6361-5235;
g. https://orcid.org/0000-0002-9777-8366; h. https://orcid.org/0000-0002-5334-7134.
Received 9 March 2018. Accepted after revision 28 May 2018.
How to cite this article:
Cunha GB, Marino LCI, Yamaya A, Kochi C, Monte O, Longui CA, Cury AN, Fleury EFC. Elastography for the evaluation of thyroid nodules in pediatric
patients. Radiol Bras. 2019 Mai/Jun;52(3):141–147.
Abstract Objective: To evaluate the usefulness of elastography (using manual compression) as an additional diagnostic tool for children and
adolescents with thyroid nodules.
Materials and Methods: This was a prospective study conducted between September 2012 and August 2013 at a hospital in Brazil.
We performed elastography, ultrasound, and fine-needle aspiration biopsy in 32 patients between 6 and 18 years of age who had,
in total, 38 thyroid nodules.
Results: The elastography findings correlated with the histopathological diagnosis in 78.5% of cases. In three patients, an unneces-
sary thyroidectomy could have been avoided if the elastography results had been prioritized. Only one malignant thyroid nodule was
found to show high elasticity.
Conclusion: Our results suggest that high elasticity of a nodule on elastography is associated with a low risk of thyroid cancer. If
further confirmed in other studies, elastography may prove useful as a complementary test for screening thyroid nodules in children.
Keywords: Thyroid neoplasms; Child; Thyroid nodule/diagnostic imaging; Elasticity imaging techniques; Ultrasonography.
Resumo Objetivo: Avaliar a utilidade da elastografia (usando compressão manual) como uma ferramenta adicional de diagnóstico em crian-
ças e adolescentes com nódulos da tireoide.
Materiais e Métodos: Este foi um estudo prospectivo realizado entre setembro de 2012 e agosto de 2013 em um hospital no
Brasil. Realizamos elastografia, ultrassonografia e biópsia por aspiração com agulha fina em 32 pacientes com idade entre 6 e 18
anos que tinham, no total, 38 nódulos tireoidianos.
Resultados: Os achados da elastografia em relação ao histopatológico foram corretos em 78,5% dos casos. A elastografia poderia
ter evitado a tireoidectomia desnecessária de três pacientes. Apenas um nódulo maligno da tireoide foi classificado como E1.
Conclusão: Nossos resultados sugeriram que a alta elasticidade de um nódulo na elastografia está associada a um baixo risco
de câncer de tireoide. Caso se confirme em outros estudos, a elastografia pode ser útil como teste de triagem complementar de
nódulos tireoidianos em crianças.
Unitermos: Neoplasias da tireoide; Criança; Nódulo da tireoide/diagnóstico por imagem; Técnicas de imagem por elasticidade;
Ultrassonografia.
INTRODUCTION more likely to have thyroid cancer than are boys, whereas
Thyroid nodules are rare in children, with an incidence the female:male ratio is 1:1 in the prepubertal period(5).
of 1.0–1.5%, although they are seen in up to 13% of adoles- Children are often diagnosed with advanced thyroid
cents and young adults(1,2). However, the risk of malignancy cancer, 40–90% of cases presenting with lymph node in-
among children and adolescents with thyroid nodules is volvement and 20–30% presenting with distant metasta-
high, the incidence of thyroid carcinomas in pediatric pa- ses(6). A recent study of children with suspicious nodules
tients being 18.0–26.7%(3), with a risk of recurrence as high showed rates of malignancy and metastasis of 25% and
as 39%(4). The incidence of thyroid cancer is 1:1,000,000 44%, respectively(7). Thorough investigation of suspicious
among children under 10 years of age, 1:200,000 among in- nodules that might require surgery is recommended to en-
dividuals 10–14 years of age and 1:75,000 among individu- sure early identification of malignancy and to avoid unnec-
als 15–19 years of age. After puberty, girls are four times essary thyroidectomy in those with benign nodules(8).
Radiol Bras. 2019 Mai/Jun;52(3):141–147 141
0100-3984 © Colégio Brasileiro de Radiologia e Diagnóstico por Imagem
Cunha GB et al. / Elastography of thyroid nodules in children
The protocol for the diagnosis of thyroid nodules in- Elastography acquires information on the movement
cludes physical examination, laboratory testing, fine-nee- of the tissue in response to the application of a small
dle aspiration biopsy (FNAB), and thyroid ultrasound(2). amount of pressure(15). In softer tissues, the applied pres-
However, the most appropriate investigations of thyroid sure causes the tissue to compress more, whereas harder
nodules are still debated. Ultrasound is considered more tissues compress less(15). This compressibility of the tissue
sensitive than physical examination for the detection of (its stiffness) is known as strain and is presented as a color
thyroid nodules, although the former has low specificity for map called an “elastogram”(15). Colors around and within
differentiating between malignant and benign nodules(9). the nodules are evaluated and visually scored according to
The ultrasound criteria for malignant thyroid nodules in- the 4–5-scale scoring system, the regions of interest being
clude marked hypoechogenicity, indistinct or spiculated specified as the target region and the adjacent reference
margins, microcalcifications, intranodular vascularity, and region. A score of 4 indicates no elasticity in the target re-
a taller-than-wide shape, although those criteria have a gion (the nodule), and a score of 5 indicates no elasticity
wide range of sensitivities (55–95%) and specificities (52– in the target region or in the adjacent reference region (the
81%) for identifying and differentiating between malignant area showing posterior shadowing). The strain ratio is cal-
or benign(10). culated automatically, and a higher strain ratio translates
Although FNAB is thought to be the most accurate to a higher probability of malignancy(18). Another form of
method for diagnosing thyroid nodules, it is particularly dif- evaluating the elastography data is by calculating the thy-
ficult to perform the procedure in children because of the roid strain ratio to perform an objective, semiquantitative
discomfort associated with the biopsy. In addition, in 20– analysis of the tissue stiffness(19).
40% of cases, the cytological findings following FNAB are Although many ultrasound elastography reports have
indeterminate or the specimen is insufficient for a definite referred to “cytologically indeterminate” thyroid nodules,
diagnosis. An accurate diagnosis is often made only after it is practical to define the ultrasound indications for the
histological evaluation(11). The nodule size that warrants a application of elastography during ultrasound scanning of
biopsy is still debated. In adults, biopsy is recommended for thyroid nodules(20). Elastography can be easily used as an
nodules ≥ 1.0 cm, whereas it is advisable to perform biopsy adjunctive noninvasive tool for B-mode ultrasound of inde-
on smaller nodules (those ≥ 0.5 cm) in children(2), because terminate nodules, which are common(20,21). However, it is
of the high incidence of malignancy among children. not yet known whether this approach is suitable for the risk
Elastography is a promising new technique for the stratification of such nodules(20,21).
ultrasound evaluation of thyroid nodules(12,13). The tech- In general, there are two ultrasound methods used
nique relies on software that is available for conventional for determining thyroid nodule stiffness(22): strain elastog-
ultrasound devices, and it evaluates the different types of raphy, in which force is applied to the tissue by manual
tissue, according to variations in their stiffness. It is based compression and the tissue deformation is parallel to the
on the principle that benign lesions are usually more elas- direction of the force; and shear-wave elastography (SWE),
tic than are malignant lesions, and elastography data can in which a push beam is created and the tissue deforma-
facilitate the differential diagnosis of clinical pathologies, tion is perpendicular to the direction of the force.
such as thyroid nodules(14). In children and adolescents with thyroid nodules, dif-
Ultrasound elastography is a noninvasive, painless ferentiating between benign and malignant nodules is vi-
imaging tool, based on the estimation of the mechanical tally important. We evaluated the usefulness of strain elas-
properties (elasticity) of the tissue, that provides additional tography as an additional diagnostic tool for children who
and clinically relevant information(15). One recent study present with thyroid nodules.
showed that elastography can increase the accuracy of ul-
trasound in thyroid nodule differentiation and suggested MATERIALS AND METHODS
that it is the best noninvasive procedure available, com- This was a prospective study conducted between Sep-
parable to FNAB for the evaluation of thyroid nodules, tember 2012 and August 2013 at a hospital in Brazil. The
regardless of the nodule size, provided that the nodule is research ethics committee of the institution approved the
solid and without calcification(16). study (Authorization no. 01687412200005479). The par-
Ultrasound elastography can be useful to distinguish ents or legal guardian of each participant gave written in-
between benign and malignant thyroid nodules(16). Be- formed consent, and all of the participants provided assent.
cause malignant nodules exhibit stiffness on elastography, We evaluated 35 patients with thyroid nodules who had
this approach is also believed to have diagnostic value in been treated in the pediatric endocrinology department of
the identification of malignant lesions. In addition, re- our hospital. In total, 42 thyroid nodules were identified on
fined elastography approaches can provide an objective physical examination or cervical ultrasound. We excluded
ratio (or index) as a quantitative indicator to compare the three patients with a total of four nodules: in one patient
stiffness of a lesion with that of normal tissue or with a (with two nodules), the FNAB results were inconclusive;
direct power unit(17). in another patient, the initial evaluation showed that the
142 Radiol Bras. 2019 Mai/Jun;52(3):141–147
Cunha GB et al. / Elastography of thyroid nodules in children
nodule had invaded the muscle but subsequent evaluations probe. The operator highlighted a box (region of interest)
showed that it had regressed; and one patient withdrew that included the nodule to be evaluated.
from the study. Therefore, the final sample comprised 32 The patient was placed in the supine position with the
patients with a total of 38 thyroid nodules. neck in hyperextension, and the ultrasound transducer was
Laboratory evaluations of thyroid function (to deter- held perpendicular to the region of interest. For elastogra-
mine circulating levels of thyroid-stimulating hormone, phy, slight, continuous manual compression was exerted
free thyroxine, thyroid peroxidase antibody, antithyroglobu- with the transducer on the thyroid nodules until resistance
lin antibody, and calcitonin) were conducted. Patients with could be felt. When resistance was sensed, the operator
euthyroidism were referred for ultrasound, elastography, relaxed the hand holding the transducer so as to provide
and FNAB. All examinations were conducted by the same spontaneous decompression of the thyroid nodule. It is im-
radiologist who, at the time of the study, had nine years portant that the pressure level remains constant through-
of experience in thyroid imaging. The specimen obtained out the examination. The operator knows that the degree of
by FNAB was evaluated by a cytologist with more than 30 manual compression is correct when a green light appears
years of experience in cytological analysis. to the left of the ultrasound image, as shown in Figure 1.
The Bethesda System for Reporting Thyroid Cytopa- The possibility to select the region of interest for the elas-
thology was used in order to categorize the biopsy findings tography analysis allowed accurate screening, even of small
as nondiagnostic (category I), benign (category II), atypia nodules, regardless of the position of the nodule within the
of undetermined significance (category III), suspicious for thyroid gland.
follicular neoplasm (category IV), suspicious for malig- The principle of elastography is to acquire two ultra-
nancy (category V), or malignant (category VI). Thyroidec- sound images (one before tissue compression and one af-
tomy was recommended for patients in whom the cytology ter) and track tissue displacement by assessing the propa-
was potentially non-benign (thyroid nodules classified as gation of the imaging beam. The use of dedicated software
Bethesda category IV, V, or VI). allows tissue distortion to be measured accurately. This
Ultrasound and elastography were performed on an technique is easy to perform. In the present study, exami-
ultrasound system with a 5–14 MHz multifrequency trans- nation times ranged from 30 s to 2 min. All examinations
ducer (Sonix SP; Ultrasonix Medical Corporation, Vancou- were performed by the same operator, who was blinded to
ver, Canada). For the elastography study, we used special the cytology results. The elastography software provides
software developed for the Ultrasonix system (version 3.0.2 elasticity information in various colors. In descending or-
[beta 1]; Ultrasonix Medical Corporation). The radiologist der of elasticity, the colors are blue, green, yellow, and red.
in charge of the study obtained the rights to use the soft- In this study, elastography data were evaluated with a
ware for experimental research during the study period. scoring system, modified from the Azizi et al.(23) classifica-
Elastography was performed during the ultrasound exami- tion, in which each thyroid nodule was given a score of E1
nation, with the same real-time instrument and the same or E2. As illustrated in Figures 2, 3, and 4, if < 50% of a
Figure 1. Green light appears to the
left of the ultrasound image when
the degree of manual compression
is correct.
Radiol Bras. 2019 Mai/Jun;52(3):141–147 143
Cunha GB et al. / Elastography of thyroid nodules in children
nodule appeared in red, it was classified as E1 (elastic),
whereas a nodule in which > 50% of the area appeared in
red was classified as E2 (stiff).
The Bethesda cytology classification was used, and
thyroidectomy was recommended for patients with thyroid
nodules classified as Bethesda IV, V, or VI. McNemar’s test
was used in order to determine the level of agreement be-
tween the elastography findings (benign or malignant) and
the histological diagnosis.
RESULTS
Overview
Figure 2. Classification of thyroid nodules by elastography. A classification
of E1 indicated an elastic (probably benign) lesion, and a classification of E2 We enrolled 32 patients with one or more nodules,
indicated a hard (probably malignant) lesion. referred for suspicious nodules detected by palpation
Figure 3. Elastography image
of a thyroid nodule classified
as E1.
Figure 4. Elastography image
of a thyroid nodule classified
as E2.
144 Radiol Bras. 2019 Mai/Jun;52(3):141–147
Cunha GB et al. / Elastography of thyroid nodules in children
or as incidental radiographic findings. The mean age of high level of calcitonin, as well as another thyroid nodule,
the patients was 12.9 years (range, 6–18 years) and the which was classified as Bethesda V. Of the five thyroid
female:male ratio was 2.5:1. The sample comprised 23 fe- nodules characterized as benign by histology, three were
male patients and 9 male patients, with mean ages of 13.5 classified as E1.
and 11.0 years, respectively. As in studies involving much larger samples (of
The nodules ranged in size from 0.5 cm to 4.3 cm, and adults), the fact that the vast majority of patients with be-
all were submitted to FNAB. Of the 32 patients, 12 had nign cytology do not undergo surgery precludes an abso-
cytological abnormalities concerning for cancer and were lute assessment of the accuracy of biopsy. However, of the
referred for total thyroidectomy. Overall, seven patients 24 thyroid nodules characterized as benign after FNAB,
were diagnosed with thyroid cancer, corresponding to an the elastography result was classified as E1 in 22 (92%).
incidence of 22%. The histological diagnosis was papillary Among the six patients referred for surgery after FNAB
thyroid carcinoma in six of those patients and medullary findings suspicious for follicular neoplasm (Bethesda IV),
thyroid carcinoma in one. the elastography result was classified as E1 in three, and
The patients with cytologically benign nodules agreed the histology confirmed the thyroid nodules to be benign
to long-term surveillance with annual cervical ultrasound in all three cases.
examinations. If there were changes in the ultrasound fea-
tures of a nodule, FNAB was again performed. At this writ- DISCUSSION
ing, there have been no changes in the diagnosis of any of Although this study was carried out between Septem-
the benign nodules. ber 2012 and August 2013, it is still of great importance
The mean age of the seven patients diagnosed with because there is a lack of articles evaluating the use of elas-
thyroid cancer was 12 years (range, 7–18 years). Six were tography in thyroid nodules with a focus on children and
female and one was male. In the sample as a whole, the adolescents. Using elastography in real time, we observed
test for antibodies was positive in 11 patients, only one of that thyroid nodules with greater elasticity are at a lower
whom was among those diagnosed with thyroid cancer. risk of malignancy, as evidenced by the fact that three of
The patient who was diagnosed with medullary thyroid car- the five nodules with benign histology were classified as
cinoma had elevated calcitonin levels: 3770 pg/mL (refer- E1. In addition, elastography classified only one malignant
ence value: < 8.4 pg/mL). nodule as E1. However, that patient had a final diagnosis
of medullary thyroid carcinoma, and it is known that up to
Thyroid nodules 50% of such nodules exhibit greater elasticity(24).
On the basis of the FNAB results, 24 (63%) of the 38 Of the six patients with FNAB findings suspicious for
thyroid nodules were classified as Bethesda II, 6 (16%) follicular neoplasm (Bethesda IV thyroid nodules), three
were classified as Bethesda IV, 7 (18%) were classified as had elastography results classified as E1 and a histologi-
Bethesda V, and 1 (3%) was classified as Bethesda VI. All cal diagnosis of benign nodules. Therefore, those three pa-
thyroid nodules classified as Bethesda V and VI were found tients were referred for thyroidectomy unnecessarily.
to be malignant in the postoperative pathology. Of the six Although there have been a number of scientific re-
thyroid nodules classified as Bethesda IV, five were benign ports about the diagnostic value of elastography in adults,
and one was malignant. Of the 38 thyroid nodules evalu- only one study has addressed its use in children with thy-
ated, 18 (47%) were located in the right lobe; 17 (45%) roid nodules. In one recent study, Borysewicz-Sanczyk et
were located in the left lobe; 2 (5%) were located in the al.(25) employed elastography in their analysis of a total of
isthmus; and 1 (3%) was diffuse. The two nodules in the 62 thyroid nodules in 47 children and adolescents: 37 fe-
isthmus were both benign, whereas the nodule with a dif- males (age range, 9–18 years) and 10 males (age range,
fuse appearance was malignant. Four of the nodules in the 7–17 years). The authors found elastography to have a high
right lobe were malignant, as were four of those in the left negative predictive value for a benign diagnosis. The first
lobe. All of the thyroid nodules (whether malignant or be- study to assess the role of elastography in the analysis of
nign) ranged in size from 1.3 cm to 1.6 cm. thyroid nodules was conducted in 2007 by Rago et al.(16).
The authors reported a positive predictive value of 100%
Elastography features and a negative predictive value of 98%. They concluded
Of the 14 thyroid nodules evaluated by histology, that elastography is a useful adjunctive tool for the diagno-
5 (35.7%) were benign and 9 (64.3%) were malignant. sis of thyroid cancer.
McNemar’s test showed that the elastography findings If larger studies confirm our results, elastography might
correlated with the histopathological diagnosis in 78.5% allow children with elastic thyroid nodules to be placed
of the cases—in 21.4% of the benign nodules and 57.1% in follow-up without invasive procedures or unnecessary
of the malignant nodules. Only one malignant nodule thyroidectomies. However, the accuracy of elastography is
(the one diagnosed as medullary thyroid carcinoma) was limited by intra- and inter-operator variability(26,27), which
classified as E1. In that particular case, the patient had a could be minimized by using SWE techniques(28). Unlike
Radiol Bras. 2019 Mai/Jun;52(3):141–147 145
Cunha GB et al. / Elastography of thyroid nodules in children
strain elastography, SWE is a quantitative technique that Acknowledgments
is not operator-dependent, which avoids the limitations of We are indebted to the patients and families evaluated,
strain elastography in evaluations of the head and neck, as well as to Dr. Maria do Carmo Assunção Queiroz for her
including the thyroid. Therefore, it is expected that SWE expertise and assistance in the cytological analyses.
can provide more information(28). However, to date, there
have been few studies aimed at standardizing specific val- REFERENCES
ues for the various SWE techniques used in the evaluation 1. National Cancer Institute. SEER Cancer Statistics Review. Inter-
net. [cited 2018 Feb 15]. Available from: https://seer.cancer.gov/
of thyroid tissue(24).
archive/csr/1975_2015/results_merged/sect_26_thyroid.pdf.
In a recent study, Duan et al.(28) used two-dimensional 2. Francis GL, Waguespack SG, Bauer AJ, et al. Management guide-
SWE ultrasound in the evaluation of 137 nodules smaller lines for children with thyroid nodules and differentiated thyroid
than 10 mm, showing that SWE values were significantly cancer. Thyroid. 2015;25:716–59.
higher in malignant lesions than in benign lesions. The 3. Gupta A, Ly S, Castroneves LA, et al. A standardized assessment of
thyroid nodules in children confirms higher cancer prevalence than
SWE technique proved to be better than conventional
in adults. J Clin Endocrinol Metab. 2013;98:3238–45.
ultrasound in differentiating between malignant and be-
4. Welch Dinauer CA, Tuttle RM, Robie DK, et al. Clinical features
nign lesions. The combination of the two techniques had associated with metastasis and recurrence of differentiated thyroid
a specificity of 94.5%, sensitivity of 95.7%, positive pre- cancer in children, adolescents and young adults. Clin Endocrinol
dictive value of 89.8%, and negative predictive value of (Oxf). 1998;49:619–28.
97.7%. 5. Hogan AR, Zhuge Y, Perez EA, et al. Pediatric thyroid carcinoma: in-
cidence and outcomes in 1753 patients. J Surg Res. 2009;156:167–
Fukuhara et al.(29), evaluating thyroid nodules with 72.
SWE, showed that the “shear-wave velocity” was signifi- 6. Chaukar DA, Rangarajan V, Nair N, et al. Pediatric thyroid cancer.
cantly higher in papillary thyroid cancer than in normal J Surg Oncol. 2005;92:130–3.
tissues and benign tumors, and there was no significant 7. Divarci E, Çeltik Ü, Dökümcü Z, et al. Management of childhood
difference between normal thyroid tissue and benign nod- thyroid nodules: surgical and endocrinological findings in a large
group of cases. J Clin Res Pediatr Endocrinol. 2017;9:222–8.
ules. The authors also found that the results were most
8. O’Gorman CS, Hamilton J, Rachmiel M, et al. Thyroid cancer in
consistent for nodules larger than 20 mm. childhood: a retrospective review of childhood course. Thyroid.
In a large prospective study that evaluated 4550 nod- 2010;20:375–80.
ules, of which 1305 were evaluated with strain elastogra- 9. Niedziela M, Korman E. Thyroid carcinoma in a fourteen-year-old
phy, the method showed a sensitivity of 74.2%, specificity boy with Graves disease. Med Pediatr Oncol. 2002;38:290–1.
of 91.1%, negative predictive value of 98%, positive pre- 10. Haugen BR, Alexander EK, Bible KC, et al. 2015 American Thyroid
Association management guidelines for adult patients with thyroid
dictive value of 37.4%, and accuracy of 90% to differenti-
nodules and differentiated thyroid cancer: The American Thyroid
ate between malignant and benign nodules. In the present Association Guidelines Task Force on Thyroid Nodules and Differ-
study, we concluded that hard nodules should always be entiated Thyroid Cancer. Thyroid. 2016;26:1–133.
considered suspicious for malignancy. However, nodules 11. Redman R, Zalaznick H, Mazzaferri EL, et al. The impact of assess-
that are “less stiff” are also frequently diagnosed as carci- ing specimen adequacy and number of needle passes for fine-nee-
dle aspiration biopsy of thyroid nodules. Thyroid. 2006;16:55–60.
nomas(30).
12. Ophir J, Alam SK, Garra B, et al. Elastography: ultrasonic estima-
tion and imaging of the elastic properties of tissues. Proc Inst Mech
CONCLUSION Eng H. 1999;213:203–33.
Given the conflicts related to the small number of 13. Cochlin DL, Ganatra RH, Griffiths DF. Elastography in the detec-
studies addressing thyroid cancer in the pediatric popula- tion of prostatic cancer. Clin Radiol. 2002;57:1014–20.
tion, we thought it important to improve the investigation 14. Fleury EFC, Fleury JCV, Oliveira VM, et al. Proposal for the sys-
tematization of the elastographic study of mammary lesions through
of thyroid nodules in young patients. In the present study, ultrasound scan. Rev Assoc Med Bras. (1992). 2009;55:192–6.
the low number of false-negative elastography results im- 15. Cantisani V, Lodise P, Grazhdani H, et al. Ultrasound elastography
plies that high elasticity of thyroid nodules is associated in the evaluation of thyroid pathology. Current status. Eur J Radiol.
with benign histology. 2014;83:420–8.
Although markers such as microRNAs and somatic 16. Rago T, Vitti P. Role of thyroid ultrasound in the diagnostic evalu-
ation of thyroid nodules. Best Pract Res Clin Endocrinol Metab.
mutations of differentiated carcinomas have recently
2008;22:913–28.
shown accuracy in the evaluation of thyroid nodules, ul- 17. Kim DW, Jung SJ, Eom JW, et al. Color Doppler features of solid,
trasound elastography could be incorporated into the rou- round, isoechoic thyroid nodules without malignant sonographic
tine evaluation of thyroid nodules, with greater ease and features: a prospective cytopathological study. Thyroid. 2013;23:
at a lower cost. However, further studies are needed in 472–6.
order to strengthen the role of elastography in the pedi- 18. Kwak JY, Kim EK. Ultrasound elastography for thyroid nodules: re-
cent advances. Ultrasonography. 2014;33:75–82.
atric population, with a focus on FNAB cytology results
19. Carneiro-Pla D. Ultrasound elastography in the evaluation of thy-
classified as Bethesda III or IV, because those categories roid nodules for thyroid cancer. Curr Opin Oncol. 2013;25:1–5.
are responsible for the largest number of unnecessary thy- 20. Zhao CK, Xu HX, Xu JM, et al. Risk stratification of thyroid nod-
roidectomies. ules with Bethesda category III results on fine-needle aspiration
146 Radiol Bras. 2019 Mai/Jun;52(3):141–147
Cunha GB et al. / Elastography of thyroid nodules in children
cytology: the additional value of acoustic radiation force impulse 26. Moon WJ, Baek JH, Jung SL, et al. Ultrasonography and the ultra-
elastography. Oncotarget. 2017;8:1580–92. sound-based management of thyroid nodules: consensus statement
21. Seong M, Shin JH, Hahn SY. Ultrasound strain elastography for cir- and recommendations. Korean J Radiol. 2011;12:1–14.
cumscribed solid thyroid nodules without malignant features cat- 27. Magri F, Chytiris S, Capelli V, et al. Shear wave elastography in
egorized as indeterminate by b-mode ultrasound. Ultrasound Med the diagnosis of thyroid nodules: feasibility in the case of coexis-
Biol. 2016;42:2383–90. tent chronic autoimmune Hashimoto’s thyroiditis. Clin Endocrinol
22. Barr RG, Memo R, Schaub CR. Shear wave ultrasound elastogra- (Oxf). 2012;76:137–41.
phy of the prostate: initial results. Ultrasound Q. 2012;28:13–20. 28. Duan SB, Yu J, Li X, et al. Diagnostic value of two-dimensional
23. Azizi G, Keller J, Lewis M, et al. Performance of elastography for shear wave elastography in papillary thyroid microcarcinoma. Onco
the evaluation of thyroid nodules: a prospective study. Thyroid. Targets Ther. 2016;9:1311–7.
2013;23:734–40. 29. Fukuhara T, Matsuda E, Fujiwara K, et al. Phantom experiment and
24. Dudea SM, Botar-Jid C. Ultrasound elastography in thyroid disease. clinical utility of quantitative shear wave elastography for differenti-
Med Ultrason. 2015;17:74–96. ating thyroid nodules. Endocr J. 2014;61:615–21.
25. Borysewicz-Sanczyk H, Dzieciol J, Sawicka B, et al. Practical ap- 30. Russ G, Royer B, Bigorgne C, et al. Prospective evaluation of thy-
plication of elastography in the diagnosis of thyroid nodules in chil- roid imaging reporting and data system on 4550 nodules with and
dren and adolescents. Horm Res Paediatr. 2016;86:39–44. without elastography. Eur J Endocrinol. 2013;168:649–55.
Radiol Bras. 2019 Mai/Jun;52(3):141–147 147
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5795)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
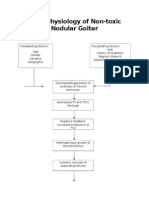
- Pathophysiology of Nontoxic Nodular GoiterDocument2 pagesPathophysiology of Nontoxic Nodular GoiterJan Jewey80% (10)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Bayesian Hypothesis Testing and Hierarchical Modelling of Ivermectin Effectiveness in Treating Covid-19Document14 pagesBayesian Hypothesis Testing and Hierarchical Modelling of Ivermectin Effectiveness in Treating Covid-19Paulo E M SouzaNo ratings yet
- Higher Frequency of Hepatic Steatosis at CT Among COVID 19 Positive PatientsDocument7 pagesHigher Frequency of Hepatic Steatosis at CT Among COVID 19 Positive PatientsPaulo E M SouzaNo ratings yet
- Necessidade de Vacinação COVID-19 em Indivíduos Previamente Infectados Um Estudo de Coorte RetrospectivoDocument19 pagesNecessidade de Vacinação COVID-19 em Indivíduos Previamente Infectados Um Estudo de Coorte RetrospectivoPaulo E M SouzaNo ratings yet
- Esteatose HepaticaDocument15 pagesEsteatose HepaticaPaulo E M SouzaNo ratings yet
- Differentiation of Hepatic Cysts From Hemangiomas: Contribution of "Inversion Recovery" Single-Shot Fast Spin-Echo SequenceDocument8 pagesDifferentiation of Hepatic Cysts From Hemangiomas: Contribution of "Inversion Recovery" Single-Shot Fast Spin-Echo SequencePaulo E M SouzaNo ratings yet
- Down Syndrome and Thyroid Disorders: A Review: 25 V. P. PrasherDocument18 pagesDown Syndrome and Thyroid Disorders: A Review: 25 V. P. PrasherErNi CiewekwekcrewetNo ratings yet
- Labreportnew - 2023-08-15T114659.034Document1 pageLabreportnew - 2023-08-15T114659.034Yashi GuptaNo ratings yet
- Chapter 10 Hormones and Hormone Antagonists Complete PDF NotesDocument12 pagesChapter 10 Hormones and Hormone Antagonists Complete PDF NotesJio InNo ratings yet
- Clinical Scoring Scales in ThyroidologyDocument16 pagesClinical Scoring Scales in ThyroidologyafadurNo ratings yet
- Anti TGDocument24 pagesAnti TGFlorea RodicaNo ratings yet
- Goitre - Wikipedia PDFDocument7 pagesGoitre - Wikipedia PDFrameshNo ratings yet
- Presentation (Final)Document32 pagesPresentation (Final)Sarah Rose FeccoNo ratings yet
- Thy 2010 0417Document66 pagesThy 2010 0417priskavkNo ratings yet
- Hashimoto ThyroiditisDocument19 pagesHashimoto ThyroiditisPaulina Maria PaciejNo ratings yet
- Deepthashree K - 642153000020249 2Document1 pageDeepthashree K - 642153000020249 2Deeptha AravamudhanNo ratings yet
- Thyroid Disease Anesthetic ConsiderationsDocument30 pagesThyroid Disease Anesthetic ConsiderationsmirzaoctaNo ratings yet
- Global Epidemiology of Hyperthyroidism and Hypothyroidism: Nature Reviews Endocrinology March 2018Document17 pagesGlobal Epidemiology of Hyperthyroidism and Hypothyroidism: Nature Reviews Endocrinology March 2018yenny handayani sihiteNo ratings yet
- Daftar PustakaDocument2 pagesDaftar PustakaJalalludin AnNo ratings yet
- Guias Thyroid 2012Document43 pagesGuias Thyroid 2012JoseAbdalaNo ratings yet
- FunctionTests Brochure PDFDocument2 pagesFunctionTests Brochure PDFArslan SaleemNo ratings yet
- S60 - LPL - Noida 3 N-27, Sec-18, Commercial Complex, Near. Atta Market, Noida.120-3029866/3142530 NoidaDocument2 pagesS60 - LPL - Noida 3 N-27, Sec-18, Commercial Complex, Near. Atta Market, Noida.120-3029866/3142530 NoidaGaurav singhNo ratings yet
- Foods To Avoid If You Have Thyroid Problems 1Document7 pagesFoods To Avoid If You Have Thyroid Problems 1Arinda PatriciaNo ratings yet
- SampleDocument2 pagesSamplesatyajeetNo ratings yet
- Pharmacotherapy of Thyroid DisordersDocument6 pagesPharmacotherapy of Thyroid DisordersShaden -No ratings yet
- Thyroid FunctionDocument12 pagesThyroid Functionسلطان القلحNo ratings yet
- Diagnosis of HyperthyroidismDocument25 pagesDiagnosis of HyperthyroidismGuardito PequeñoNo ratings yet
- Interpretation: A06 - Raj Hospital - Cash (Cghs - 20) Main Road Ranchi Jharkhand 834001Document4 pagesInterpretation: A06 - Raj Hospital - Cash (Cghs - 20) Main Road Ranchi Jharkhand 834001AlokNo ratings yet
- MethimazoleDocument5 pagesMethimazoleapi-300595323No ratings yet
- Guidelines For Laboratory Practice 2012 PDFDocument81 pagesGuidelines For Laboratory Practice 2012 PDFMauricio Vanessa Juliana Koury PalmeiraNo ratings yet
- Thyroid Disease (Chan)Document29 pagesThyroid Disease (Chan)Sidiq AboobakerNo ratings yet
- Xrug7152 1 PDFDocument2 pagesXrug7152 1 PDFSarah ArpithaNo ratings yet
- HypothyroidismDocument15 pagesHypothyroidismfachrulmirzaNo ratings yet
- Thyroid by Dr. Shyam Kalavalapalli, Endocrinologist, HyderabadDocument87 pagesThyroid by Dr. Shyam Kalavalapalli, Endocrinologist, HyderabadSherman BellNo ratings yet
- Thyroid DisorderDocument16 pagesThyroid DisorderKen TokkNo ratings yet