Professional Documents
Culture Documents
FM5. Hyperthyroidism
Uploaded by
Hello PBJOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
FM5. Hyperthyroidism
Uploaded by
Hello PBJCopyright:
Available Formats
Family Medicine 05: 30-year-old woman with palpitations
User: Hannah Paton
Email: h.paton@mua.edu
Date: April 14, 2019 1:26PM
Learning Objectives
The student should be able to:
Develop a differential diagnosis of palpitations.
Describe the common presentations of hyperthyroidism.
List the common physical findings in hyperthyroidism: lid lag, tremor, and hyperreflexia.
Identify the common causes of hyperthyroidism.
Outline the initial evaluation of a patient with suspected hyperthyroidism.
Discuss the usual course of a patient with Graves disease after radioactive iodine treatment.
Discuss the treatment of hypothyroidism after radioactive iodine treatment.
Knowledge
Signs and Symptoms of Hyperthyroidism
Hyperthyroidism presents with multiple symptoms that vary according to the age of the patient, the duration of the illness, the magnitude of hormone excess, and presence of comorbid conditions. Symptoms are related to the thyroid hormone's
stimulation of catabolism, and enhancement of sensitivity to catecholamines.
In patients under the age of 50, the most common signs and symptoms of hyperthyroidism are:
Heat intolerance (92%)
Tachycardia (96%) due to increased adrenergic tone and heightened conduction
Fatigue (84%)
Weight loss (50%) due to increased calorigenesis and gut motility causing hyperdefecation and malabsorption.
Tremor (84%)
Increased sweating (96%)
Exertional dyspnea caused by O 2 consumption, CO2 production, and respiratory muscle weakness
Depression and hyperreflexia are less common but can be present.
Diarrhea and light periods can also occur with hyperthyroidism.
Many of the typical symptoms of hyperthyroidism are absent in patients older than age 70.
Patients who are older than 70 may present with sinus tachycardia (71%) and/or fatigue (56%), but they can also present with atrial fibrillation or weight loss, and no other symptoms.
Exopthalmos
Exopthalmos (also called proptosis) is the forward projection or bulging of the eye out of the orbit. This is most commonly seen in Graves disease and can be either bilateral or unilateral.
Causes of Enlarged Thyroid (Goiter)
Worldwide, the lack of iodine is the most common cause of goiter. In fact, iodine deficiency is the most common, yet easily preventable cause of developmental delay and intellectual disability in the world. Areas that are the
Lack of iodine
most affected are in northern Africa and Pakistan. Iodized salt is the easiest and least expensive way to supplement iodine.
Hypothyroidism Hashimoto disease, which causes hypothyroidism, is a common cause of goiter.
Hyperthyroidism Graves disease, which causes hyperthyroidism, also causes goiter. In fact, an enlarged thyroid can be seen in patients with too much, normal amounts or not enough thyroid hormone.
Nodules Nodules, either single or multiple, can also cause an enlarged thyroid.
Thyroid cancer Thyroid cancer is usually detected by palpating an enlarged, nodular thyroid.
Pregnancy Pregnancy can occasionally cause a slight enlargement in the thyroid.
Thyroiditis Thyroiditis can also cause an enlarged, often tender, thyroid gland.
Clonus
Clonus: A series of abnormal reflex movements of the foot induced by sudden dorsiflexion causing alternate contraction and relaxation of the gastrocnemius and soleus muscles.
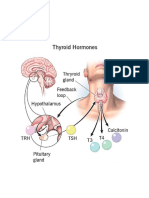
Hypothalamic-Pituitary Axis
The hypothalamus releases thyrotropin releasing hormone (TRH) which stimulates the pituitary to produce and release thyroid stimulating hormone (TSH). TSH stimulates the thyroid to make thyroid hormone (T3 and T4).
When thyroid hormone levels are high: The presence of excess thyroid hormone exerts negative feedback on the hypothalamus and anterior pituitary, and suppresses the release of both TRH from hypothalamus and TSH from
anterior pituitary gland.
When thyroid hormone levels are low: The hypothalamus releases TRH. TRH stimulates the pituitary to produce TSH. The TSH, in turn, stimulates the thyroid to produce thyroid hormone until levels in the blood return to normal.
Therefore, if there are elevated levels of circulating thyroid hormones , suppression of the pituitary gland via a negative feedback loop will result in a low TSH.
Conversely, when there are decreased levels of circulating thyroid hormones , the absence of suppression of the pituitary will result in an increased TSH.
If a primary pituitary problem interferes with the feedback cycle - for example, if a pituitary adenoma develops that is not suppressed by excess thyroid hormone - then TSH may not accurately reflect the levels of circulating thyroid hormone,
and drawing a T4 level helps in the investigation.
Utility of TSH and T4 in evaluation of suspected thyroid disease
TSH LEVEL Serum Free T4 Level Condition indicated
TSH increased Serum Free T4 Decreased Hypothyroidism
TSH mildly elevated (5-10 mIU/L) Serum Free T4 Normal Subclinical Hypothyroidism
TSH inappropriately normal Serum Free T4 Increased Pituitary adenoma (TSH-producing) or Thyroid hormone resistance
TSH decreased Serum Free T4 Increased Hyperthyroidism
TSH decreased (occ. Normal or slightly elevated) Serum Free T4 Decreased Central (or pituitary) hypothyroidism (TSH and/or TRH deficiency)
Serum Free T4 Normal
TSH decreased T3 Toxicosis
Serum T3 Increased
© 2019 Aquifer 1/5
Graves Disease
Autoimmune disease in which thyrotropin receptor antibodies (also called thyroid stimulating immunoglobulins) are produced. These antibodies stimulate the thyroid gland to enlarge and to produce more thyroid hormone.
Causes about 60% to 80% of hyperthyroidism.
Women are five to 10 times more likely than men to get it.
Peak incidence is between ages 40 and 60.
Often occurs with family history of thyroid disease; can also be associated with other autoimmune diseases.
Triggers include stressful life events, high iodine intake, or a recent pregnancy.
Eye Involvement in Graves Disease
The most common manifestations of Graves ophthalmopathy (eye problems) are eyelid retraction and exophthalmos.
Primary symptoms of the eye manifestations of Graves disease are related to corneal irritation from eyelid retraction .
While most of the time the eye signs and symptoms are bilateral, they can be unilateral.
While 50% of patients with Graves have some eye involvement by MRI, only about 20% to 30% of those are clinically relevant. In up to 10% the eye manifestations can happen when the patient is euthyroid or even hypothyroid. Treatment of
hyperthyroidism does not affect the eye manifestations. In fact, some patients who get radioactive iodine will experience worsening symptomatology.
Common Symptoms of Hypothyroidism
Weight gain, cold intolerance, pedal edema, heavy periods, and fatigue all arise from slowed metabolism. Fatigue is common to both hyper- and hypothyroidism.
Clinical Skills
How to Elicit Lid Lag
Ask the patient to follow your finger with their eyes; then move your finger slowly from their upper to lower field of vision. In lid lag, the upper eyelid lags behind the upper edge of the iris as the eye moves downward. Be careful when performing
this maneuver; if your finger is moved too quickly, the diagnosis may be missed.
How to Perform a Thyroid Exam
View the thyroid exam video.
Neurological Exam: How to Elict Deep Tendon Reflexes
Neurological Exam - How to Elicit Deep Tendon Reflexes
Role of Patient Values in Treatment Choice
There is often no one right treatment for a problem. It depends on a patient's social situation and personal beliefs.
Deciding Whether to Trust Patient History
There is an importance to trusting the patient history and not disrupting the doctor-patient relationship.
It is also important to pay attention to the context of the history:
Was it a teenager giving you a history of abstinence in the presence of a parent?
Was the partner in the room?
Was the history taken in private with limited external pressure?
These are some of many factors that will help you individualize this challenging situation.
Management
Treatment of Graves Disease
Medication to suppress thyroid hormone production:
1. Methimazole is the most commonly used medication to suppress thyroid hormone production.
Side effects are rare, but less than 1% of people who take methimazole have a serious side effect known as agranulocytosis in which the bone marrow stops producing white blood cells. This leaves patients vulnerable to serious
infections.
It takes up to three months to suppress thyroid production , although patients usually start to notice improvement in their symptoms after one month.
Patients typically need to stay on medications for several years . More than half of patients return to hyperthyroidism if they try stopping medications.
The appropriate dose of medication fluctuates over time and people on medication need to come in for blood work often for adjustments . People on medication are more likely to have symptoms because fluctuations are hard to
predict.
2. Oral dose of radioactive iodine:
Alternative to thyroid hormone suppressant medication. More commonly used in the United States.
Iodine concentrated in the thyroid and has very few side effects .
During the course of a few months the iodine destroys most of the overactive thyroid cells and the level of thyroid hormone falls and the thyroid gland shrinks in size.
Eventually most people who have this treatment start having too little thyroid in their bloodstream so that they need to start taking small doses of thyroid hormone to replace it.
Low thyroid is relatively easy to manage once you have found a dose where the patient feels normal and the TSH is in the normal range. Blood levels usually need to be drawn once or twice yearly and the dose of thyroid
replacement usually stays about the same.
Patient Values Affect Graves Disease Treatment Choice
Interestingly, in Europe, more people with Graves disease get medication for treatment, while in the US over 70% get radioactive iodine.
Radioactive Iodine Treatment and Follow-Up
Radioactive Iodine Treatment
Obtain a pregnancy test before initiating radioactive iodine treatment.
Advise patients that they should not be near pregnant women or young children for several days following radioactive iodine treatment because the radioactive iodine is excreted in urine and stool. Fetuses or young children exposed to this
could have deleterious effects on their thyroid.
Side effects include transient soreness of the neck or brief worsening of symptoms but they should resolve within a few days. Furthermore, people with ophthalmopathy can have worsening of eye symptoms.
Follow-up for Radioactive Iodine Treatment
The patient needs to be seen within a few months after her radioactive iodine treatment to see when to discontinue propranolol (if prescribed) and to follow her TSH. The patient should have her TSH drawn every two to three months until it has
stabilized. The time frame can be extended after that to six months or longer. Since she will become hypothyroid at some point, it is important to alert the patient to symptoms of hypothyroidism she could expect, so she can be tested earlier if
need be.
Thyroid Replacement Therapy
Starting Thyroid Replacement
A typical starting dose of thyroxine in primary hypothyroidism (such as that which occurs following radioactive iodine treatment) is 1.5 to 1.8 mcg per kilogram.
Increasing the dose slowly is important, especially in elderly patients and in patients like Ms. Waters who are mildly hypothyroid. TSH should be repeated in six weeks .
When a stable TSH level has been achieved in primary hypothyroidism, TSH can be checked once or twice annually.
Some people who have radioactive iodine treatment still have enough thyroid left to relapse. Occasionally they need a second treatment.
© 2019 Aquifer 2/5
Studies
T4 Level for Primary Pituitary Pathology
While the thyroid stimulating hormone (TSH) is usually sufficient to make a diagnosis of both hyperthyroid and hypothyroid, there are some unusual causes of low TSH due to primary pituitary pathology. In those cases the TSH does not reflect
the circulating thyroid level. In those cases, T4 level is low because the pituitary is not stimulating the gland to make thyroxine.
Studies to Determine the Etiology of Hyperthyroidism
Radioactive iodine uptake (RAIU) test and scan measures the amount and pattern of radioactive iodine taken up by the thyroid in the 24 hours following ingestion of a set dose. Normal RAIU uptake is 15% to 30% of the ingested dose.
The various etiologies of hyperthyroidism can be differentiated as conditions that manifest as high RAIU (>30%) or low RAIU (<15%).
For example, excess circulating thyroid hormone which occurs in Graves disease as a result of increased creation of thyroid hormone results in increased radioactive iodine uptake used to synthesize the thyroid hormone.
Conversely, excess circulating thyroid hormone in subacute thyroiditis occurs as a result of the gland leaking excess hormone, so radioactive iodine uptake is low in this case, as more thyroid hormone is not synthesized.
High RAIU (>30%) Low RAIU (<15%)
Graves disease Sub-acute thyroiditis
Multi-nodular goiter Silent thyroiditis
Toxic solitary nodule Iodine induced
TSH-secreting pituitary tumor Exogenous L-Thyroxine
HCG secreting tumor Struma ovarii
Amiodarone
Nodules that cause hyperthyroidism are hyperfunctioning and caused increased radioactive iodine uptake.
"Cold" (non-thyroxine producing) nodules can be caused by cancer although typically in that case hyperthyroidism is not present.
Diffuse increased uptake suggests Graves disease whereas a nodular pattern indicates a single nodule or multi nodular disease.
Example of RAIU scan of a patient with Graves disease
© 2019 Aquifer 3/5
Example of a normal RAIU scan.
Anti-thyrotropin receptor antibodies (TRAb) are the pathologic mechanism for Graves disease and can be detected in the vast majority of patients with this condition. In patients with undiagnosed causes of hyperthyroidism, third-generation
assays for TRAb are 97% sensitive and 99% specific for Graves. These antibodies are to be distinguished from anti-thryroid peroxidase (TPO) antibodies, which are elevated in 90% of patients with Hashimoto thryroiditis and 75% of patients
with Graves.
Studies not used to determine the etiology of hyperthyroidism:
A thyroid ultrasound is used in the evaluation of thyroid nodules and thyroid enlargement but not hyperthyroidism. Ultrasound characteristics of a nodule can be used to stratify risk of malignancy and ultrasound can guide the fine needle
aspiration of nodules that are not easily palpated. Ultrasound is starting to be used to differentiate Graves disease from other causes of hyperthyroidism when RAI scanning is not available or is contraindicated. Some experts predict that color-
flow Doppler ultrasound may replace RAI scanning since it has similar accuracy but is safer, less costly and easier to administer.
An MRI of the thyroid gland is not necessary to diagnose hyperthyroid disease.
Clinical Reasoning
Differential of Palpitations
The following conditions can cause palpitations:
Cardiovascular: Arrhythmia, cardiomyopathy, hypovolemia
Psychiatric: Anxiety, panic attacks
Medications: Caffeine, stimulants, theophylline, and albuterol use
Substances: Tobacco, caffeine, alcohol intoxication or withdrawal, cocaine
Endocrinologic: Hyperthyroidism, pheochromocytoma, hypoglycemia
Hematologic: Anemia
Infectious: Febrile illness
Differential of Palpitations
Likely diagnosis Rationale
Commonly cause palpitations, particularly when the heart rate is fast.
Cardiac arrhythmias Can be associated with dizziness and/or shortness of breath.
Some, like paroxysmal supraventricular tachycardia, are more common in young people.
Commonly cause palpitations and can be associated with shortness of breath.
Anxiety and panic
disorder Anxiety and hyperthyroidism can be difficult to distinguish because tachycardia, tremulousness, irritability, weakness, and fatigue can be present in both disorders. In anxiety, however, systemic symptoms such as
weight loss and changes in stools and menses are rare.
Can be associated with palpitations because of sinus tachycardia due to reduced oxygen carrying capacity in the blood. (Anemia can also cause dyspnea via this mechanism).
Patients with anemia severe enough to cause tachycardia typically report positional dizziness.
Anemia Several causes of anemia are associated with weight loss including nutritional deficiencies (vitamin B12, folate) and malignancy.
A common source of anemia in menstruating women is heavy periods.
In rare cases occult bleeding, for example from the GI tract, can be present and cause anemia.
Increase in thyroid hormone increases the metabolism and may cause weight loss; frequent, loose stools; and light periods.
Hyperthyroidism
Other effects include an increased heart rate.
© 2019 Aquifer 4/5
Can cause palpitations.
Drug/caffeine abuse Intoxication with substances such as cocaine, methamphetamines and even alcohol can cause tachycardia.
Signs such as dilated pupils, increased energy, increased blood pressure, and erratic behavior all suggest intoxication.
Common Causes of Hyperthyroidism
Toxic diffuse goiter (Graves disease) accounts for the majority (60-80%) of hyperthyroidism.
Is an autoimmune disease caused by an antibody that acts at the thyroid-stimulating hormone (TSH) receptor and stimulates the gland to synthesize and secrete excess thyroid hormone.
Toxic diffuse goiter Hypervascularity of the thyroid may result in a bruit or thrill upon auscultation that is not present in other etiologies of hyperthyroidism.
Exophthalmos is characteristic.
Pretibial myxedema, a rare finding, is most common in Graves disease and is caused by the deposition of hyaluronic acid in the dermis and subcutaneous tissues.
Causes about 5% of cases of hyperthyroidism.
Thyroid nodules are common, but most are not symptomatic, and only 4% to 5% are cancerous.
Toxic nodular goiter
Thyroid nodules are more common in patients over 40.
These older patients more often have multi nodular disease, whereas, solitary nodules are seen more often in younger patients and can be associated with iodine deficiency.
Thyroid hormone leaks from an inflamed thyroid.
Thyroiditis
Happens after a viral illness or pregnancy.
Excessive iodine ingestion
Excessive iodine can occur through diet or a medication such as amiodarone, which can induce thyroiditis.
Drug induced hyperthyroidism
References
AACE/AME Task Force on Thyroid Nodules. American Association of Clinical Endocrinologists and Associazione Medici Endocrinologi medical guidelines for clinical practice for the diagnosis and management of thyroid nodules. Endocr Pract.
2006 Jan-Feb;12(1):63-102.
Abbott A. Diagnostic Approach to Palpitations. Am Fam Physician. 2005;71(4):743-50,755-6.
Abbott AV. Diagnostic Approach to Palpitations. Am Fam Physician 2005;71(4):743-56. http://www.aafp.org/afp/20050215/743.html. Accessed April 14, 2017.
American Association of Clinical Endocrinologists. American Association of Clinical Endocrinologists medical guidelines for clinical practice for the evaluation and treatment of hyperthyroidism and hypothyroidism. Endocr Pract. 2002;8:457-69.
Bahn R. Graves' ophthalmopathy. New Engl J Med. 2010;362:726-738.
Bahn RS, Burch HB, Cooper DS, et al. ATA/AACE Taskforce on Hyperthyroidism and Other Causes of Thyrotoxicosis; 2011 Hyperthyroidism and other causes of hyperthyroidism guidelines of the American Association Of Clinical Endocrinologists.
Thyroid 2011;21(6):593-646.
Ballenger JC. Treatment of Panic disorder in the general medical setting. J Psychosom Res. 1998;44:5-15.
Bartalena L, Tanda M. Graves ophthalmopathy. N Engl J Med 2009; 360(10):994-1001
Bindra A, Braunstein G. Thyroiditis. Am Fam Physician. 2006 May 15;73(10):1769-1776. http://www.aafp.org/afp/20060515/1769.html. Accessed April 14, 2017.
Eng C, Quraishi M. Management of thyroid nodules in adult patients. Head and Neck Oncology. 2010;2(11).
Fauci, Anthony S. Chapter 37. In Harrison's Principles of Internal Medicine. United States. McGraw-Hill Professional; 2012.
Hueston WJ. Treatment of hypothyroidism. Am fam physician. 2001;64(10):1717-24. http://www.aafp.org/afp/2001/1115/p1717.html. Accessed April 26, 2017.
Kahaly GJ, Bartalena L, Hegedus, L. The American Thyroid Association/American Association of Clinical Endocrinologists guidelines for hyperthyroidism and other causes of thyrotoxicosis: A European perspective. Thyroid. 2011; 21(6):585-591.
Kroenke K, Spitzer RL, Williams JBW. The Patient Health Questionnaire-2: Validity of a two-item depression screener. Medical Care. 2003;41(11):1284-92.
Okosieme O, Chan D. The utility of radioiodine uptake and thyroid scintography in the diagnosis and management of hyperthyroidism. Clin Endocrine. 2010;72:122-127.
Trivalle C, Doucet J, Cassagne P, et al. Differences in signs and symptoms of hyperthyroidism in older and younger patients. J Am Geriatr Soc. 1996;44:51.
University of Connecticut School of Medicine. DTRs biceps, triceps, knee, ankle. (Video.) Farmington, CT. Used with permission.
University of Connecticut School of Medicine. Thyroid Exam. (Video.) Farmington, CT. Used with permission.
Weetman A. Graves Disease. New Engl J Med. 2000;343(17),236-1248.
Weetman A. Radioiodine treatment for benign thyroid diseases. Clin Endocrinol. 2007;66:757-764.
Weller RK. Outpatient Approach to Palpitations. Am Fam Physician. 2011 Jul 1;84(1):63-69. www.aafp.org/afp/2011/0701/p63.html. Accessed April 14, 2017.
Weller RK. Outpatient Approach to Palpitations. Am Fam Physician. 2011. http://www.aafp.org/afp/2011/0701/p63.html. Accessed December 12, 2016.
Whooley MA, Avins AL, Miranda J, Browner WS. Case-finding instruments for depression. Two questions are as good as many. J Gen Intern Med. 1997;12(7):439-45.
World Health Organization. Iodine Data Status Summary. http://www.who.int/vmnis/iodine/status/summary/iodine_data_status_summary/en/index.html. Accessed April 26, 2017.
© 2019 Aquifer 5/5
You might also like
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (589)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (842)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5806)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1091)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Path Endocrine OutlineDocument46 pagesPath Endocrine Outlineaya derweshNo ratings yet
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- ENDOCRINE SYSTEM OverviewDocument39 pagesENDOCRINE SYSTEM OverviewAnn M. Hinnen Sparks50% (2)
- Diffuse Toxic GoiterDocument64 pagesDiffuse Toxic GoiterMuftihat IsrarNo ratings yet
- Autoimmune Disorders - AgungDocument40 pagesAutoimmune Disorders - AgungalgutNo ratings yet
- Osteoporosis - Sally ChampaDocument18 pagesOsteoporosis - Sally ChampaarunsrlNo ratings yet
- Endocrine Practice TestDocument50 pagesEndocrine Practice TestMonemah Essa Francisco Martinez86% (7)
- SK Singh Lab Report 09042018Document8 pagesSK Singh Lab Report 09042018Iasam Groups'sNo ratings yet
- Nursing Care of at Risk/ High Risk/ Sick ClientDocument256 pagesNursing Care of at Risk/ High Risk/ Sick ClientAaron ConstantinoNo ratings yet
- A Case Study On Graves DiseaseDocument46 pagesA Case Study On Graves DiseaseRenie SerranoNo ratings yet
- Acute Biologic CrisisDocument143 pagesAcute Biologic CrisisAprylL22100% (5)
- Cardiff PacesDocument26 pagesCardiff PacesIvyljn100% (2)
- Benign Diseases of ThyroidDocument70 pagesBenign Diseases of ThyroidMounica MekalaNo ratings yet
- ATA HipertiroidDocument117 pagesATA HipertiroidjordanNo ratings yet
- 1-Good Health Gold Package - PO2257496339-951Document1 page1-Good Health Gold Package - PO2257496339-951Aafaq BhuttoNo ratings yet
- Understanding Thyroid Storm: in Partial Fulfillment of The Requirements For NCM 103 (Medical-Surgical Nursing) RleDocument47 pagesUnderstanding Thyroid Storm: in Partial Fulfillment of The Requirements For NCM 103 (Medical-Surgical Nursing) RleNeirfla Wassabi100% (2)
- Review Plummer DiseaseDocument12 pagesReview Plummer DiseaseNovia ChrisnawatiNo ratings yet
- Types of Thyroid MedicationsDocument3 pagesTypes of Thyroid MedicationsfennarioNo ratings yet
- Hyperthyroidism BrochureDocument2 pagesHyperthyroidism Brochureapi-301861602No ratings yet
- Cosopt PiDocument11 pagesCosopt PiMaria SpatariNo ratings yet
- Endocrine System Disorders Endocrine Disorders - Too Much GigantismDocument4 pagesEndocrine System Disorders Endocrine Disorders - Too Much GigantismDhea Angela A. CapuyanNo ratings yet
- Pathophysiology of Nontoxic Nodular Goiter PDFDocument2 pagesPathophysiology of Nontoxic Nodular Goiter PDFKristine Lou Tan RualloNo ratings yet
- Causes of Endocrine DisordersDocument8 pagesCauses of Endocrine DisordersKrystel Mae GarciaNo ratings yet
- HyperthyroidismDocument6 pagesHyperthyroidismMalena Joy Ferraz VillanuevaNo ratings yet
- Analytical Method For Cleaning Validation of Levothyroxine Sodium inDocument9 pagesAnalytical Method For Cleaning Validation of Levothyroxine Sodium inDidarulNo ratings yet
- DEBOLDocument317 pagesDEBOLalehegn belete100% (5)
- OSPE 4th Yr PathoDocument144 pagesOSPE 4th Yr PathoMuhammadShahzadNo ratings yet
- Kuliah HyperthyroidDocument18 pagesKuliah HyperthyroidFreddyNo ratings yet
- Mail For Uploading The VideoDocument1 pageMail For Uploading The VideoDr Subodh ChaturvediNo ratings yet
- Principles of Temperature MonitoringDocument8 pagesPrinciples of Temperature MonitoringOllie EvansNo ratings yet
- 2007 - A Practical Guide For Clinicians Who Treat Patients With AmiodaroneDocument10 pages2007 - A Practical Guide For Clinicians Who Treat Patients With AmiodaroneXochiquetzal MartinezNo ratings yet