Professional Documents
Culture Documents
Exam 2 SG
Uploaded by
Evan0 ratings0% found this document useful (0 votes)
8 views8 pagesExam 2 SG
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentExam 2 SG
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
8 views8 pagesExam 2 SG
Uploaded by
EvanExam 2 SG
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 8
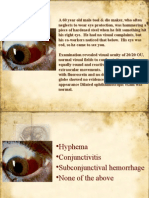
Lecture 9 – The Red Eye
1. External Lid Problems
a. Hordeolum
i. Acute infection/inflammation at the eyelid margin
ii. Sebaceous Zeis or Apocrine Moll
iii. Red and painful
iv. Warm compress, lid antibiotics cream – systemic antibiotics for cellulitis, I&D if persistent
b. Chalazion
i. Chronic, painless, granuloma
ii. Warm compress, lid antibiotics cream – systemic antibiotics for cellulitis, I&D if persistent
c. Dacrocystitis
i. Acute onset, maybe some preceding trauma
ii. Epiphoria – tears down the cheek
iii. URGEN TREATMENT – drain and antibiotics
d. Blepharitis
i. Itching, burning, FB sensation, crusting of eyelids in morning
ii. Anterior = Demodix mites, sleeves of protein on the eyelashes (pilocarpine treatment)
e. Masquerade Conditions
i. BCCA/SCCA – ulcer like, lose eyelashes and glands
ii. Sebaceous – cancer of the Meibomian glands, white creamy
iii. Melanoma – black, dark pigment
2. Cellulitis
a. Preseptal
i. Tenderness, swelling, erythema
ii. Sinusitis, skin abrasion, hordeolum, insect bite
iii. NO PROPTOSIS, NO PAIN ON EOM, NO EOM ABNORMALITES
iv. May not be able to open the lid themselves
b. Orbital
i. Fever, chills, toxic appearing, elevated WBC
ii. PROPTOSIS, DIPLOPIA, PAIN ON EOM
iii. Treatment requires IV antibiotics and possible drainage
3. Conjunctiva
a. Subconjunctival Hemorrhage
i. Blood under the conjunctiva, usually in one sector
ii. Valsalva, trauma, HTN, bleeding problem (disease or anticoagulants), bleeding mass
iii. Exam – look for conjunctival lesion, check EOM, resistance to retropulsion of the globe, BP, CT?
iv. Treatment – nothing, maybe lubricants
b. Algorithm
i. Follicles
1. Preauricular Lymphnode
a. Yes
i. Herpetic Signs
1. Yes = HSV
2. No = Chlamydia
b. No
i. Toxic
ii. Molluscum
iii. Peduculosis
ii. Papillae
1. Severe Purulent = GC
2. Scant Purulent = Bacterial
3. Water = Allergic or Atopic
c. Follicles
i. Lymphocytic aggregates with avascular centers (white in the middle)
ii. Viral – adenoviral, HSV, chlamydia, Molluscum
d. Papillae
i. Response to bacterial or allergic insult
ii. Vascularized red centers to the bumps
e. Acute Viral Conjunctivitis
i. Red eye (conjunctival hyperemia), watery stringy discharge, eyelid crusting in the AM, VA NL
ii. Preauricular lymph node, often asymmetric
iii. May have a membrane/pseudomembrane
iv. Prolonged cases may have the sub epithelial infiltrates
v. DDx – adenoviral, bacterial other than GC, GC, Allergic, Toxic, Atopic
vi. Tx – don’t need to culture, acute lasts 4-7 days, cornea can be 2-3 weeks
vii. Highly contagious for 10-12 days
viii. If membrane or SEI develops refer to ophthalmologist
f. HSK
i. Eye doesn’t improve with conservative treatments
ii. Can affect vision if central lesion
iii. Needs referral to optho
iv. Dendritic lesions with end bulbs on fluor stain
v. Trifluoridine and or Acylcovir/Valtrex
g. Allergic
i. Usually bilateral, itchiness, watery discharge, no crusting
ii. Tx – eliminate agent, cold compress, mild – tears, moderate – allergy drops, severe – steroid IO
h. Vernal
i. Causes – genetics, allergy stuff in the family, asthma, eczema – young males in the spring/sum
ii. Sx – Burning/itching/watery, photophobia, limbus/upper eyelids swollen and rough, white muc.
iii. Often requires steroids or cyclosporine
iv. HORNER TRANTAS DOTS – perilimbal bumps filled with eosinophils, refer to optho
i. Bacterial (Non-GC)
i. Purulent discharge
ii. Staph aureus (blepharitis), Staph epidermidis, H. influ (children), Strep pneumonia
iii. GS and culture ONLY if severe, recurrent, or recalcitrant
iv. Trimeth/polymixin or Cipro QID, if H. influ add systemic amox/clavulanate
j. Gonococcal
i. Severe, purulent discharge, marked chemosis, preauricular nodes
ii. Begins over 12-24 hours
iii. May progress to corneal perforations (examine for ulcers)
iv. Can be seen in neonates
v. GS and Culture – blood and chocolate
vi. Tx – PO/IV antibiotics, consult I&D, topical antibiotics, eye lavages
k. Chronic Chlamydial
i. Symptoms greater than a month, sexually active may have cervicitis or urethritis
ii. Inferior follicles, Giemsa staining for cytoplasmic basophilic inclusion bodies
iii. Azithro or Doxy, topical erythromycin for 2-3 weeks
l. Trachoma
i. Arlt line or scarring of the superior tarsal conjunctiva
ii. Azithro or Doxy, topical erythromycin for 2-3 weeks
m. Molluscum Contagiosum
i. Dome shaped, umbilicated shinny nodules on lid or margin
ii. Chronic follicular conjunctivitis from viral particles
iii. Simple excision or curettage or cryosurgery
4. Sclera
a. Scleritis
i. Serious inflammation of the sclera
ii. Redness/purple of sclera and conjunctiva, severe eye and templ/jaw pain, photophobia,
tearing, decreased VA, maybe blindness
iii. Associated with SLE, RA, Ank spond, arthritises, polyarteritis nodosa, MCTD, wegners, Sjogren,
GCA, IBS, allergic angitis
iv. Differentiate from Episcleritis with pheylephirne or neosynephrine drops (blanches in epi)
v. Diffuse, Nodular, Necrotizing, Posterior
vi. Mild cases = NSAIDs
vii. Oral corticosteroids
viii. Severe = long term immunosuppression
b. Episcleritis
i. Mild eye pain, redness, watery eyes
ii. Benign, self limiting, WORSE IN TOBACCO SMOKERS
iii. Artificial tears if needed
iv. Severe cases oral NSAIDs or topical corticosteroids
c. Pingulecula
i. Yellow/white adjacent to limbus, sup epithelial collagen degrades to elastic like, no excision
d. Pterygium
i. Wedge shaped fibrosis into the cornea, extends onto the cornea, may distort vision, removed
5. Cornea
a. Contact Overwear Syndrome
i. Corneal Inflammation without Ulcer but is an ulcer until proven otherwise
ii. Can be devastating
iii. Acanthomeba – ring
iv. Pseudomonas – central and entire
b. Corneal Ulcer
i. Result of inflammation or infection
ii. Extremely painful due to exposed nerve endings
iii. May also have anterior uveitis symptoms of miosis, aqueous flare, redness
Lecture 10 – Adult Vision Abnormalities
1. Cataracts
a. Opacification of the lens, blurring of vision
b. Normal lens – ectoderm epithelial cells, lens capsule that a=surrounds and is zonular fiber attachement
c. Morgagnian – hypermature liquefied
d. ANteiror polar – pin hole
e. Fetal nuclear – red reflex disturbed, prevent amblyopia, operate at two weeks
f. Nuclear – yellow brownish
g. Cortical – spokes
h. Posterior Sub-Capsular – steroids used, posterior subcapsule is hazy
i. Metabolic – galactosemia
j. Ectopia Lentis – Marfans = up Homocystinuria = down
k. Phaco Emulsification = most common technique
2. Age Related Macular Degeneration
a. ARMD – most common irreversible vision loss over age of 60
b. MOST COMMON IN WHITES, then black/Hispanic/other
c. Risk Factors
i. Aging, smoking, family history, HF1/CFH gene, HTN, UV exposure, female
d. Retinal Pigment Epithelium
i. Maintains photoreceptors, absortion of stray light, outer blood retinal barrier, phag/regen cells
ii. Bruch’s Membrane seperates RPE from choroid
iii. Choroid capillaries prevent overheating and provide O2 and nourishment to RPE
e. Dry ARMD
i. Early stage, less severe, 90% of cases
ii. Blurry or faded vision
iii. Drusen, incipient atrophy, then geographic atrophy
iv. Insufficent nutrition damages photreceptors, with age RPE cant digest photreceptors,
accumulation of metabolic debris (druesen), RPE membrane and cells degenerate and atrophy
v. Lose central vision
vi. Drusen appear as focal areas of eosinophilic material between BM or RPE and Bruch’s
vii. Mild drusen = normal VA, more light
viii. Larger drusen = risk of late form, progression to wet
ix. Geographic atrophy = severest form of Dry without Wet – RPE atrophy and choroid exposed
f. Wet ARMD
i. More severe, 10%
ii. Early symptom is wavy lines
iii. Develop central vision blind spots
iv. Age related Bruch’s changes (thickening, drusen, metabolic deposits) and lose connection RPE
v. Pigment epithelial detachment may occur
vi. Photreceptors and pigment epithelium send distress signal to choriocapillaries to make new
vessels
vii. New vessels grow underneath macula, breakdown Bruch’s, new vessels are fragile
viii. Leak blood, fibrovascular scarring of macula
ix. Potential for rapid and severe vision damage
x. SRNVM or CNVM (NVM = neovascular membrane)
xi. Leakage of blood or serum in CNV develop sudden loss of central vision, often other eye too
g. Diagnostic Tools
i. Visual acuity
ii. Amsler grid test – distorted vision or central irregularities
iii. Ophthalmoscope – direct visualization
iv. Fluroescein and ICG – NVM and location
h. Management
i. Ocuvite – Vitamins C/E, Zinc, Cu, DHA, EPA, Lutein, Zeaxanthin
ii. Wet AMD – VEGF inhibitors, PDT – cold laser, surgery, other laser photocoagulation
i. Rehabilitation
i. Low vision aids – reading lamps, magnifiers, CCTV, Alexa
ii. Don’t smoke, exercise, good diet, sunglasses, take meds, see eye doctor
iii. Q1-2 years for 65+ healthy patients to see eye doctor
3. Viral Keratitis
a. HSV 1&2, VZV 3, EBV 4, CMV – 5, Roseola 6, Pityriasis Rosa 7, Kaposi’s -8
b. HSV, VZV, EBV, and CMV
c. Leading cuse of corneal blindness
d. Atopy = increased risk for bilateral disease
e. Primary infection of epithelial cells, retrograde transport to CN V ganglion, latent, reactivation = eye sxs
f. Primary HSV1
i. Rarely seen, vesicular belpharoconjunctivitis, corneal infolvement, children
ii. Hutchisons Sign – vesicles on the nose before eye problems
g. Recurrent HSK
i. Triggered by – fever, UV, trauma, mensturation, immunosuppression
ii. Cornela ulceration, branching with end bulbs
4. Retinal Detachment
a. General
i. Always occur at the periphery, floaters and flashers first then black curtain
b. Degenerative
i. ARMD
ii. Epiretinal Membrane and Macular Hole
1. Vitreous jelly contracts and activates fibroblasts cracking the central macula
c. Metabolic
i. Diabetic Macular Edema
ii. Proliferative Diabetic Retinopathy and Vitreous Hemorrhage
d. Vascular Occlusive
i. CRVO
1. HTN or DM, can cause the black curtain vision loss but on exam no retinal detachment
ii. CRAO
e. Vitreoretinal Traction
i. Retinal Detachment
f. Trauma
i. Injury, Eye Wall Rupture, IO FB
1. Contraction of the vitreous
2. Flashers and floaters
3. Peripheral retinal tears
4. Scotoma initially in periphery – never isolated central scotoma
ii. Post-surgical
5. Common Retinal Surgeries
a. Macular hole repair, detachment repair, diabetic hemorrhage removal, IO FB, droppec cataract
b. Pars Plana – fixes IO abnormalities and retinal detachment
c. Scleral Buckling for Retinal Detachment – thin silicon band swe in around the eye to give a surface to
reattach retina
d. Retinal Eye Laser
i. Ablation of ischemic tissue – burn away the poorly perfused tissue, thicken leaky vessels
ii. Form adhesions to seal retinal tears
6. Vitreous Substitutes/Eye Gases
a. Temporary, removed at end of operation
i. Perfluron used to flatten tissues
b. Slow absorbing, may be left in
i. Sulfar hexaflorane SF6
ii. Propane octaflurane C3F8
c. Non-absorbing, premant
i. Silicon oil
Lecture 11 – Ocular Manifestations of Systemic Diseases
1. Diabetes
a. Blacks and Mexcans, older than 40s, men>women
b. Age, duration of DM, pregnancy, insulin dependency, diastolic pressure, smoking Type1>2
c. Pathogenesis
i. Endothelial cell damage/prolif + capillary BM thickening, increased plasma viscosity leads to…
ii. Decreased capillary blood flow and perfusion leading to retinal hypoxia
iii. AV shunt IRMA
iv. VEGF leads to neovascularization and fibrovascular proliferation
d. NPDR (Background Retinopathy)
i. Cotton wool spots
ii. Venous beading
iii. Intra-retinal microvascular abnormalities
iv. Intra-retinal hemorrhages
e. PDR
i. Temporarily benefits from anti-VEGF, eventually requires Pan Retinal Photocoagulation laser
ii. Complications – poor perfusion leads to vitreous hemorrhage and fractional membranes to RD
f. Recommended Screen Schedule
i. Type 1 – 3-5 years after diagnosis then yearly
ii. Type 2 – at time of diagnosis, then yearly
iii. Pregnancy – before conception, early in first trimester, then 3-12 months mild/mod or 1-3 sev.
g. Follow Up
i. Normal, mild, mod, severe NPDR, CSME, PDR
ii. 1 year, 9, 6, 4, 2-4, 2-3 months
h. Treatment of DR
i. Laser photocoagulation, anti-VEGF/steroids injections, surgery
ii. Panretinal Photocoagulation
2. Hypertensive Retinopathy
a. Most are asymptomatic, some have HA or blurred vision
b. Exam
i. Arteriolar narrowing, changes in AV crossings, flame hemorrahges, microaneursym, exudates
ii. Cotton wool spots, optic disc swelling
c. Grading
i. 0 = No changes
ii. 1 = Barely detectable arterial narrowing
iii. 2 = Obvious arterial narrowing with focal irregularities
iv. 3 = Retinal hemorrhages = grade 2
v. 4 = Optic disc swelling + grade 3
d. Complications
i. CRVO (complete or hemi)
ii. Blown Capillaries
iii. Ischemia, neovascularization – proliferative retinopathy – will need PRP
3. Increased ICP
a. Normal is 7-15 mmHg, if increased, CPP=MAP-ICP, so CPP decreases
b. ICP of 25-40 has normal alertness, 40-50 LOC, then brain death further
c. Causes – mass effect, brain swelling from liver, HTN, increased venous pressure, CSF production
d. Signs
i. Papilledema or optic disc swelling, usually vision is unaffected
ii. BILATERAL AND SPARES VISION – maybe enlarged blind spot
iii. Neuroretinitis – inflammation of retina and optic nerve – firework appearance
4. Blood Dyscrasias and Embolic Disease
a. Anemia
i. Retinal hemorrhage, CWS, vitreous hemorrhage, CRVO like picture, papilledema
b. Polycythemia
i. Retinal venous dilation and tortuoisity, intraretinal hemorrhages
c. Leukemia
i. Hemorrhages (flame, dot-blot, white Roth spots, boat shaped), microaneurysm, hard exudate
d. Coagulopathies
i. Serous detatchment of retina, retina and choroidal hemorrhage, vitreous hemorrhage
e. Plasma Dyscrasias
i. Retinal venous dialation and trotrousity, sausage like, microanerysus, CRVO, intraretinal hem.
f. Histopathology
i. Flame shaped are in the nerve fiber layer
ii. Dot-blot are in the inner and outer plexiform and inner nuclear layers
g. Hollenhorst Plaque
i. Cholesterol plaque from the carotid breaks off, occasionally after CEA or heart surgery
ii. Vision loss suddenly in the corresponding field to the emboli location
iii. Painless, sudden loss of vision that is not permanent
iv. If no HH plaque seen, then vasculitis is considered
v. Temporal arteritis may cause sudden vision loss
h. Amaurosis Fugax
i. Embolic – carotid or cardiac with afib or valve disease
ii. Hemodynamic – giant cell arteritis, vasospasm, hypercoagulable states
iii. Ocular – angle closure, iritis, severe dry eye
iv. Neurologic – optic neurits, MS, migraine, ICP, psychogenic
v. Idiopathic
i. Sickle Cell
i. Due to sluggish blood flow and occlusion of vessels, most often in the SC disease form
ii. Swelling of the hands and feet is often the first symptom, eye findings are late
iii. Sickle Cell Non-Proliferative Retinopathy
1. Venous tortuosity
2. Salmon patch hemorrhage
3. Schesis cavity
4. Black sunburst
iv. Sickle Cell Proliferative Retinopathy
1. Peripheral arteriolar occlusions
2. AV anastomosis
3. Neovascular proliferation
4. Vitreous Hemorrhage
5. Retinal Detachment
6. Most severe form, progressive, need to treat neovascular tissue with PRP
5. Thyroid Eye Disease
a. 30-50, females
b. TSH receptor antigen in the orbital fat and connective tissue, autoimmune assault
c. Findings
i. Eyelid retraction, lid lag on infraduction (Von Graefe), eye globe lag on supraduction (Kocher’s)
ii. Inability to completely close lids
iii. Chemosis, punctate epithelial erosions, superior limbic keratoconjunctivitis, lacrimal problems
iv. Inferior rectus muscle most commonly affected – diplopia on upgaze and limited elevation
v. Lymphs, plasma, mastocytes on histiology
vi. Deposition of collagen and GAGs causes fibrosis
vii. Lipogenesis by fibroblasts and preadipocytes increase orbital volume
6. Metastatic Carcinoma
a. Breast most frequently, can be bilateral in 20% or so
7. AIDS
a. Early Stage – Kaposis, Zoster, Candida, Lymphoma
i. Kaposi’s HHV 8 - VEGF
b. Middle Stages – Toxoplasma, TB, PCP
c. Late Stage – CMV, MAC
i. CMV retinitis (HHV-5) – intravitreal flame hemorrhages – pizza box, Gancyclovir
8. Occular Inflamations
a. Young people, primary without systemic assocaitong
b. RA, lupus, Sarcoidosis, Wegner, Infections
9. Uveitis
a. Anterior
i. Iris, anterior chamber – 90% of all uveitis
ii. Unilateral/bilateral, pain, photophobia, blurred vision, redness, miosis
iii. Single episode, treated with drops
b. Intermediate
i. Pars plantitis, vitiritis
ii. Macular, less pain or photophobia, floaters, blurred vision
iii. Snowbanking
c. Posterior
i. Chorioretinits
ii. Photopsia
d. Diagnosis
i. Complete visual exam, skin test for TB, toxo, histo – full blood testing CBC, ESR etc
e. Treatment
i. Underlying disease – cycloplegics and steroids to the eye
You might also like
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5795)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1091)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Retinal DetachmentDocument31 pagesRetinal DetachmentEko KunaryagiNo ratings yet
- A. Subjective: 1. Progress NoteDocument3 pagesA. Subjective: 1. Progress NoteEvan100% (1)
- PBL Modul Blindness KLP 14Document25 pagesPBL Modul Blindness KLP 14033010969No ratings yet
- Eye Disorders: Presented by Carmelita Ramos, RNDocument65 pagesEye Disorders: Presented by Carmelita Ramos, RNJayme_Galang_7078100% (1)
- Emergency Eye Care WorkshopDocument21 pagesEmergency Eye Care WorkshopAriani Ratri Dewi100% (1)
- Case Based Ophthalmology GuideDocument12 pagesCase Based Ophthalmology GuideGradestack100% (2)
- MCQ OphthalmologyDocument56 pagesMCQ Ophthalmologypriya00991% (11)
- Quiz - Eye DisordersDocument44 pagesQuiz - Eye DisordersMary Margareth GonzalesNo ratings yet
- Ophthalmology LastDocument28 pagesOphthalmology LastJamal Kadir100% (2)
- Retinal DetachmentDocument10 pagesRetinal DetachmentSilpi HamidiyahNo ratings yet
- Eye MCQDocument21 pagesEye MCQAli SheraziNo ratings yet
- Step by Step VITRECTOMY PDFDocument405 pagesStep by Step VITRECTOMY PDFSzőcs Tímea100% (4)
- Pulm SIM Outline - MineDocument4 pagesPulm SIM Outline - MineEvanNo ratings yet
- Exam 2 Study Guide 2018Document21 pagesExam 2 Study Guide 2018EvanNo ratings yet
- Gestational Trophoblastic DiseaseDocument6 pagesGestational Trophoblastic DiseaseEvan100% (1)
- Genetics Lecture NotesDocument4 pagesGenetics Lecture NotesEvanNo ratings yet
- SDL 14 - CLL:SLLDocument3 pagesSDL 14 - CLL:SLLEvanNo ratings yet
- Cell Bio Exam 4Document53 pagesCell Bio Exam 4EvanNo ratings yet
- Embryo TimelineDocument1 pageEmbryo TimelineEvanNo ratings yet
- Anatomy Exam 2 OutlineDocument23 pagesAnatomy Exam 2 OutlineEvanNo ratings yet
- CM GI Exam 1 SGDocument56 pagesCM GI Exam 1 SGEvanNo ratings yet
- What Are Eye FloatersDocument4 pagesWhat Are Eye FloatersSaravanan ThiruvalathaanNo ratings yet
- Vitreous HemorrhageDocument7 pagesVitreous HemorrhageindahNo ratings yet
- Synthesis of Polydimethylsiloxane and Its Monomer From Hydrolysis of DichlorodimethylsilaneDocument6 pagesSynthesis of Polydimethylsiloxane and Its Monomer From Hydrolysis of Dichlorodimethylsilanecesar orduz zarateNo ratings yet
- Retinal Detachment: DR - Ajai Agrawal Additional Professor Department of Ophthalmology A.I.I.M.S, RishikeshDocument58 pagesRetinal Detachment: DR - Ajai Agrawal Additional Professor Department of Ophthalmology A.I.I.M.S, RishikeshSrishti KhullarNo ratings yet
- Dr. Petty Bpjs Feb 22Document74 pagesDr. Petty Bpjs Feb 22Fariz A NouvalNo ratings yet
- Grodno State Medical University: Assistant Lecturer of The Department of OphthalmologyDocument24 pagesGrodno State Medical University: Assistant Lecturer of The Department of OphthalmologyTeguh Imana NugrahaNo ratings yet
- Ablasio RetinaDocument29 pagesAblasio RetinaTenri AshariNo ratings yet
- Retinal Detachments and The Current Trends of TreatmentDocument10 pagesRetinal Detachments and The Current Trends of Treatmentapi-235387260No ratings yet
- Vitrectomy For Primary Symptomatic Vitreous Opacities: An Evidence-Based ReviewDocument11 pagesVitrectomy For Primary Symptomatic Vitreous Opacities: An Evidence-Based ReviewTasya SylviaNo ratings yet
- Intraocular Gas TemponadDocument15 pagesIntraocular Gas TemponadLoay T. DweikNo ratings yet
- K.15 Ophtalmologic EmergenciesDocument35 pagesK.15 Ophtalmologic EmergenciesZikri Putra Lan Lubis100% (1)
- B06 Posterior SegmentDocument22 pagesB06 Posterior SegmentMigs MedinaNo ratings yet
- 16.retinal Detachment PDFDocument42 pages16.retinal Detachment PDFFrederica MutiaraNo ratings yet
- Concept Map FinaleDocument31 pagesConcept Map FinaleDeVineNo ratings yet
- White Without PressureDocument2 pagesWhite Without PressureGsz Eli WongNo ratings yet
- RetinaDocument57 pagesRetinaRizky PebryanNo ratings yet
- AAO Residents Content OutlineDocument34 pagesAAO Residents Content OutlineNizma PermaisuariNo ratings yet
- Lattice DegenerationDocument3 pagesLattice DegenerationAnumeha JindalNo ratings yet
- Nitrous Oxide Sedation DentistryDocument16 pagesNitrous Oxide Sedation DentistryAnonymous k8rDEsJsU1100% (1)