Professional Documents
Culture Documents
Case Study, Chapter 29, Management of Patients With Complications From Heart Disease
Uploaded by
kingOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Case Study, Chapter 29, Management of Patients With Complications From Heart Disease
Uploaded by
kingCopyright:
Available Formats
Case Study, Chapter 29, Management of Patients With Complications From Heart
Disease
1. George Brown, 72 years of age, is a male patient who is admitted with the diagnosis of
acute pulmonary edema secondary to acute left ventricular heart failure. The patient has a
history of coronary artery disease that has been treated medically. The patient is anxious,
pale, cold, clammy, and dyspneic. The vital signs are: blood pressure 88/50 mm Hg, heart
rate 110 bpm, respiratory rate 32 breaths/min, and temperature 97°F. There are bubbling
crackles and wheezing throughout the lung fields and the patient is raising frothy blood-
tinged clear sputum. The patient’s admission weight is 100 kg. (Learning Objective 4)
a. What first actions should the nurse take and what are the rationales for these
actions?
The physician ordered furosemide (Lasix) 40 mg IVP STAT.
b. What are the actions of furosemide that will help the patient?
c. What nursing actions should be implemented when administering a diuretic?
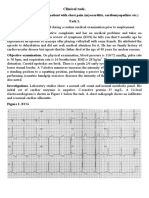
2. Carl Edwards is a 75-year-old man with congestive heart failure. Having sustained
three myocardial infarctions in the last 10 years, he has decreased left ventricular
function. Mr. Edwards takes Digoxin, Capoten, Coreg, and Lasix for management of this
disease. Today he presents to the emergency department with fatigue, generalized
weakness, and feelings of “skipping” heartbeats. Upon arrival, he is placed on the cardiac
monitor, his vital signs are assessed, and an IV is inserted. He currently denies chest pain,
but is experiencing some shortness of breath, and is placed on 2 L of oxygen via nasal
cannula. (Learning Objective 1)
a. Which of his medications might be contributing to his symptoms of generalized
weakness and heart irregularities?
b. For what clinical manifestations should you assess to correlate to his left-sided
heart failure?
c. How do his medications treat his congestive heart failure?
d. How does the hypokalemia affect the effects of Digitalis?
You might also like
- Chronic Heart Failure Case FileDocument2 pagesChronic Heart Failure Case Filehttps://medical-phd.blogspot.comNo ratings yet
- MRCP 1 Last MinDocument10 pagesMRCP 1 Last MinDr.yeasin Arafat100% (1)
- Internal 1 Cardiology QuizzesDocument31 pagesInternal 1 Cardiology QuizzesfabrahamNo ratings yet
- Congestiveheartfailure: Michael C. Scott,, Michael E. WintersDocument10 pagesCongestiveheartfailure: Michael C. Scott,, Michael E. WintersNicolás HonoresNo ratings yet
- PBL PgamboaDocument6 pagesPBL PgamboaLeanne Princess GamboaNo ratings yet
- EXAM PharmDocument40 pagesEXAM PharmJack PopNo ratings yet
- 5 Cardiovascular DisordersDocument4 pages5 Cardiovascular DisordersChristian Joseph OpianaNo ratings yet
- SG001 - Jore, Julianna RheavenDocument9 pagesSG001 - Jore, Julianna RheavenJulianna Rheaven JoreNo ratings yet
- Nursing Care Process Case StudyDocument6 pagesNursing Care Process Case StudyEunice RosalesNo ratings yet
- Cardiovascular Case Study Jan 2 101xDocument4 pagesCardiovascular Case Study Jan 2 101xElizabeth SpokoinyNo ratings yet
- Kuliah Pakar HF FKUMMDocument46 pagesKuliah Pakar HF FKUMMOkta Dwi Kusuma AyuNo ratings yet
- CardiologyDocument102 pagesCardiologyashrafholailNo ratings yet
- Riyadh Ali 4/9/12 MDSC3311Document6 pagesRiyadh Ali 4/9/12 MDSC3311Hugh JacobsNo ratings yet
- MKSAP13-Cardiovascular MedicineDocument102 pagesMKSAP13-Cardiovascular MedicineManisha DesaiNo ratings yet
- Cardiovascular Medicine:Question 1Document101 pagesCardiovascular Medicine:Question 1abdullahmushlihNo ratings yet
- Questions & Answers: CardiologyDocument77 pagesQuestions & Answers: CardiologyDev Yadav100% (1)
- Cast Study 1Document4 pagesCast Study 1Thelda Mae Arteche SablanNo ratings yet
- End-Stage Heart DiseaseDocument44 pagesEnd-Stage Heart DiseaseCyrille AgnesNo ratings yet
- Cardio 8. 4Document3 pagesCardio 8. 4Абдул Насер МохаммадізмаелNo ratings yet
- Incidence Pathophysiology Classification Causes Diagnosis Assessing Cardiovascular Disability Treatment MessagesDocument67 pagesIncidence Pathophysiology Classification Causes Diagnosis Assessing Cardiovascular Disability Treatment MessagesAhmed ElshewiNo ratings yet
- Clin Cardiology CasesDocument34 pagesClin Cardiology CasesSunny Singh0% (1)
- CVS Physio Case Files p1Document4 pagesCVS Physio Case Files p1dawnparkNo ratings yet
- USMLE CompilationDocument101 pagesUSMLE CompilationRendi RafsanjaniNo ratings yet
- Lec 4Document9 pagesLec 4fbbqbcht6yNo ratings yet
- Nur 111 Session 6 Sas 1Document12 pagesNur 111 Session 6 Sas 1Zzimply Tri Sha UmaliNo ratings yet
- Internal Medicine - 1081 ﺔﻠﺌﺳﻷا دﺪﻋ 08-04-2023 ﺔﻠﺌﺳﻷا ﺚﻳﺪﺤﺗ ﺦﻳرﺎﺗ ﻒﻴﻔﻋ ﺪﺠﻣأ .د ﻖﻴﺒﻄﺗ ﰲ ةدﻮﺟﻮﳌا ﺔﻠﺌﺳﻷا ﻊﻴﻤﺟ ﲆﻋ يﻮﺘﺤﻳ ﻊﻴﻤﺠﺘﻟا اﺬﻫDocument2,309 pagesInternal Medicine - 1081 ﺔﻠﺌﺳﻷا دﺪﻋ 08-04-2023 ﺔﻠﺌﺳﻷا ﺚﻳﺪﺤﺗ ﺦﻳرﺎﺗ ﻒﻴﻔﻋ ﺪﺠﻣأ .د ﻖﻴﺒﻄﺗ ﰲ ةدﻮﺟﻮﳌا ﺔﻠﺌﺳﻷا ﻊﻴﻤﺟ ﲆﻋ يﻮﺘﺤﻳ ﻊﻴﻤﺠﺘﻟا اﺬﻫenasNo ratings yet
- PrelimsDocument11 pagesPrelimsJess Fabra100% (1)
- What Symptoms Should Lead The Nurse To Suspect The Pain May Be Angina?Document5 pagesWhat Symptoms Should Lead The Nurse To Suspect The Pain May Be Angina?Dylan Angelo AndresNo ratings yet
- Im CaseDocument7 pagesIm CaserohitNo ratings yet
- PracticeExam 2 AnsDocument51 pagesPracticeExam 2 AnsBehrouz YariNo ratings yet
- Coronary Artery Disease (CAD) NCLEX QuestionsDocument7 pagesCoronary Artery Disease (CAD) NCLEX QuestionsMelodia Turqueza GandezaNo ratings yet
- ThiroidDocument9 pagesThiroidAhmed EmadNo ratings yet
- CCC Practice NBME Questions 1Document4 pagesCCC Practice NBME Questions 1NamarNo ratings yet
- Clinical Pearls CardiologyDocument6 pagesClinical Pearls CardiologyMaritza24No ratings yet
- Topic 4. Clinical CaseDocument4 pagesTopic 4. Clinical CaseSheikhNo ratings yet
- Heart Failure: Abdul Hafiz AliasDocument19 pagesHeart Failure: Abdul Hafiz AliasAbdul Hafiz Alias100% (5)
- Cardiovascular Medicine: QuestionsDocument10 pagesCardiovascular Medicine: QuestionsYuni AryantiNo ratings yet
- QuestionsDocument55 pagesQuestionsInchic MirandaNo ratings yet
- Congestive Heart Failure/Pulmonary Edema Case FileDocument4 pagesCongestive Heart Failure/Pulmonary Edema Case Filehttps://medical-phd.blogspot.comNo ratings yet
- ICC Cronica Fisiopatologia 2014Document11 pagesICC Cronica Fisiopatologia 2014Karen Grissell Serrano RamosNo ratings yet
- Right Side Pleuritic Chest Pain For A Few Hours. On Examination Tachycardia, Respiratory Distress, O Breath Sounds On The Right SideDocument9 pagesRight Side Pleuritic Chest Pain For A Few Hours. On Examination Tachycardia, Respiratory Distress, O Breath Sounds On The Right SideRabia RabiaNo ratings yet
- Ishemic Heart DieaseDocument14 pagesIshemic Heart Dieaseirshad ahmedNo ratings yet
- Anesthesia & Critical Incidents 73Document73 pagesAnesthesia & Critical Incidents 73RaMy “MhMd” ElaRabyNo ratings yet
- 1800 MCQ Revised VersionDocument606 pages1800 MCQ Revised VersionFarah FarahNo ratings yet
- ATI PN Pharmacology Proctored EXAM Review 2021Document77 pagesATI PN Pharmacology Proctored EXAM Review 2021kmills876No ratings yet
- Case Study2Document33 pagesCase Study2Kelly YeowNo ratings yet
- Liza Marie L. Nayre BSN-4: SDL Day 1 - Heart FailureDocument3 pagesLiza Marie L. Nayre BSN-4: SDL Day 1 - Heart FailureSherryle AbilaNo ratings yet
- Tasks:: For StudentDocument3 pagesTasks:: For StudentlalitrajindoliaNo ratings yet
- Ojsadmin, 1034Document5 pagesOjsadmin, 1034杨嘉宜No ratings yet
- Chronic Heart FailureDocument11 pagesChronic Heart FailurelaydyNo ratings yet
- Investigation and Management of Congestive Heart Failure: Clinical ReviewDocument6 pagesInvestigation and Management of Congestive Heart Failure: Clinical ReviewDwiky YuanasikaNo ratings yet
- (Review) Heart FailureDocument7 pages(Review) Heart FailureFreddy PanjaitanNo ratings yet
- Question 1 of 10: AAFP Board Review Clinchers Cardio Quiz 1Document60 pagesQuestion 1 of 10: AAFP Board Review Clinchers Cardio Quiz 1pramesh1No ratings yet
- Hypertension NCLEX Quiz Questions: A. I Will Make Sure I Consume Foods High in PotassiumDocument5 pagesHypertension NCLEX Quiz Questions: A. I Will Make Sure I Consume Foods High in PotassiumMelodia Turqueza GandezaNo ratings yet
- Lemone 6e Chapter 31Document47 pagesLemone 6e Chapter 31Husein Fatih ArafatNo ratings yet
- Dialated CardiologyDocument2 pagesDialated Cardiologyrythem141No ratings yet
- Jibc ADocument19 pagesJibc AttsxxxNo ratings yet
- In ConclusionDocument2 pagesIn ConclusionkingNo ratings yet
- In ConclusionDocument2 pagesIn ConclusionkingNo ratings yet
- In ConclusionDocument2 pagesIn ConclusionkingNo ratings yet
- In ConclusionDocument2 pagesIn ConclusionkingNo ratings yet
- In ConclusionDocument2 pagesIn ConclusionkingNo ratings yet
- Glaucoma: Viviany Taqueti and Scott Vafai HST 150Document15 pagesGlaucoma: Viviany Taqueti and Scott Vafai HST 150Emmanuel B. SahaniNo ratings yet
- In ConclusionDocument2 pagesIn ConclusionkingNo ratings yet
- In ConclusionDocument2 pagesIn ConclusionkingNo ratings yet
- In ConclusionDocument2 pagesIn ConclusionkingNo ratings yet
- OsteoporosisDocument6 pagesOsteoporosiskingNo ratings yet
- In ConclusionDocument2 pagesIn ConclusionkingNo ratings yet
- OsteoporosisDocument6 pagesOsteoporosiskingNo ratings yet
- In ConclusionDocument2 pagesIn ConclusionkingNo ratings yet
- OsteoporosisDocument6 pagesOsteoporosiskingNo ratings yet
- Assignment - Faysal SabraDocument2 pagesAssignment - Faysal SabrakingNo ratings yet
- OsteoporosisDocument6 pagesOsteoporosiskingNo ratings yet
- OsteoporosisDocument6 pagesOsteoporosiskingNo ratings yet
- OsteoporosisDocument6 pagesOsteoporosiskingNo ratings yet
- PNC Chapter 20Document7 pagesPNC Chapter 20kingNo ratings yet
- OsteoporosisDocument6 pagesOsteoporosiskingNo ratings yet
- The Patient With Peripheral Vascular ProblemsDocument6 pagesThe Patient With Peripheral Vascular ProblemskingNo ratings yet
- Assignment - Faysal SabraDocument2 pagesAssignment - Faysal SabrakingNo ratings yet
- Chapter 14: Nursing Management: Patients With Coronary Vascular DisordersDocument13 pagesChapter 14: Nursing Management: Patients With Coronary Vascular DisorderskingNo ratings yet
- PNC Chapter 39Document5 pagesPNC Chapter 39kingNo ratings yet
- Intramuscular Injection: 1-DefinitionDocument11 pagesIntramuscular Injection: 1-DefinitionkingNo ratings yet
- GallstonesDocument2 pagesGallstoneskingNo ratings yet
- Intramuscular Injection: 1-DefinitionDocument11 pagesIntramuscular Injection: 1-DefinitionkingNo ratings yet
- PNC Chapter 11Document20 pagesPNC Chapter 11kingNo ratings yet
- GallstonesDocument2 pagesGallstoneskingNo ratings yet
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (80)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (6)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (1)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeRating: 2 out of 5 stars2/5 (1)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (26)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (404)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (44)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- Gut: the new and revised Sunday Times bestsellerFrom EverandGut: the new and revised Sunday Times bestsellerRating: 4 out of 5 stars4/5 (392)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- The Marshmallow Test: Mastering Self-ControlFrom EverandThe Marshmallow Test: Mastering Self-ControlRating: 4.5 out of 5 stars4.5/5 (58)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingFrom EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingRating: 4 out of 5 stars4/5 (1138)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningFrom EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningRating: 4 out of 5 stars4/5 (3)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)
- A Brief History of Intelligence: Evolution, AI, and the Five Breakthroughs That Made Our BrainsFrom EverandA Brief History of Intelligence: Evolution, AI, and the Five Breakthroughs That Made Our BrainsRating: 4.5 out of 5 stars4.5/5 (6)