Professional Documents
Culture Documents
Financial Support: Necrotic Xanthogranuloma With Disseminated Annular Lesions
Uploaded by
Sango AyraOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Financial Support: Necrotic Xanthogranuloma With Disseminated Annular Lesions
Uploaded by
Sango AyraCopyright:
Available Formats
CASE LETTER 117
Financial support 3. Shah K, Tran AN, Magro CM, Zang JB. Treatment of Kimura dis-
ease with mycophenolate mofetil monotherapy. JAAD Case Rep.
2017;3:416---9.
None declared.
4. Chen Y, Wang J, Xu F, Zeng C, Liu Z. Clinicopathological fea-
tures and prognosis of Kimura’s disease with renal involvement
Author’s contribution in Chinese patients. Clin Nephrol. 2016;85:332---9.
5. Katagiri K, Itami S, Hatano Y, Yamaguchi T, Takayasu S. In vivo
Han Ma: Approval of the final version of the manuscript; expression of IL-4, IL-5 IL-13 and IFN-gamma mRNAs in peripheral
blood mononuclear cells and effect of cyclosporine A in a patient
elaboration and writing of the manuscript.
with Kimura’s disease. Br J Dermatol. 1997;137:972---7.
Conflicts of interest Han Ma
None declared. Department of Dermatology, the Fifth Affiliated Hospital,
Sun Yat-sen University, Zhuhai, Guangdong, China
E-mail: drmahan@sina.com
References
Received 25 February 2018; accepted 1 March 2019
1. Bastos JT, Rocha CRMD, Silva PMCE, Freitas BMP, Cassia FF,
https://doi.org/10.1016/j.abd.2019.03.006
Avelleira JCR. Angiolymphoid hyperplasia with eosinophilia 0365-0596/ © 2019 Sociedade Brasileira de Dermatologia.
versus Kimura’s disease: a case report and a clinical and Published by Elsevier España, S.L.U. This is an open access article
histopathological comparison. An Bras Dermatol. 2017;92:392---4. under the CC BY license (http://creativecommons.org/licenses/
2. Buder K, Ruppert S, Trautmann A, Bröcker EB, Goebeler M, Ker- by/4.0/).
stan A. Angiolymphoid hyperplasia with eosinophilia and Kimura’s
disease --- a clinical and histopathological comparison. J Dtsch
Dermatol Ges. 2014;12:224---8.
Necrotic xanthogranuloma with
disseminated annular lesions夽,夽夽
Dear Editor,
Necrotic xanthogranuloma (NX) is a non-Langerhans histio-
cytosis, initially described in 1980,1 which is characterized
by yellowish plaques and nodules with a tendency to ulcera-
tion, which may infiltrate mainly the periorbital region, the
flexor surface of the extremities, and the trunk. There is no
predilection for gender and it mainly affects middle-aged
patients.
A 73-year-old man, attended the dermatology outpa-
tient clinic, with yellowish lesions on the trunk that had
benn present fortwo years. On physical examination, he
showed infiltrated annular plates with clear centers and
erythematous borders on the thorax and abdomen, and
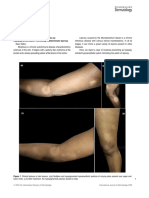
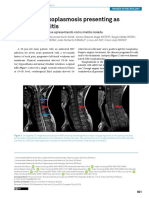
asymptomatic lower limbs (Figs. 1 and 2). One of the lesions
of the abdomen was ulcerated. He reported a previous
diagnosis, about 20 years ago , of annular granuloma. A
biopsy of the abdominal lesion was performed (Fig. 3) with
the diagnostic hypotheses of necrotic xanthogranuloma,
lipoidica necrobiosis, annular granuloma, and xanthoma.
Histopathology showed the dermis completely compromised
by a chronic granulomatous process with numerous Touton
cells, some bizarre, and areas of necrobiosis with nuclear
夽 How to cite this article: Fasciani IA, Valente NYS, Luce MCA,
Kakizaki P. Necrotic xanthogranuloma with disseminated annular
lesions. An Bras Dermatol. 2020;95:117---9. Figure 1 Lesions on the back. Yellowish infiltrated annular
夽夽 Study conducted at the Hospital do Servidor Público Estadual plaques with clear centers and erythematous borders.
de São Paulo (HSPE), São Paulo, SP, Brazil.
118 CASE LETTER
Other changes that may accompany NX are neutrope-
nia, hypocomplementemia, cryoglobulinemia, or hyper-
lipidemia. Associated diseases include multiple myeloma,
chronic lymphocytic leukemia, Hodgkin’s disease, non-
Hodgkin’s lymphoma, asthma, and Quincke’s edema.
The differential diagnoses for NX include lipoid necrobio-
sis, juvenile xanthogranuloma, annular granuloma, foreign
body granuloma, subcutaneous rheumatoid nodules, xan-
thomas (disseminated, normolipemic flat, primary, and
secondary), amyloidosis, and Erdheim---Chester disease.
In histopathology, NX shows typical areas of necrobio-
sis surrounded by granulomas composed of giant Touton
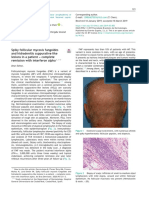
Figure 2 Detail of the lesion on the abdomen. Yellowish cells, foamy histiocytes, and giant foreign-type giant
plaques on the abdomen. cells, as well as lymphocytes, compromising the entire
dermis.
In the pathogenesis of NX, it is suggested that serum
immunoglobulins bind to lipids, depositing in the skin, which
would provoke a foreign body reaction. Another hypothesis
is that paraprotein would bind the Fc portion of IgG by acti-
vating a secondary proliferation of macrophages. It has also
been proposed that the paraprotein in NX has the functional
characteristics of a lipoprotein that can bind to histiocyte
lipoprotein receptors and induce granuloma formation.1
The etiology of this disorder remains obscure despite theo-
ries that attempt to clarify its pathogenesis. Consequently,
treatment is difficult, without a recommended first-line
therapy and a tendency to recurrent skin lesions.
Treatment options include immunomodulatory drugs,
immunosuppressive agents, corticosteroids, alkylating
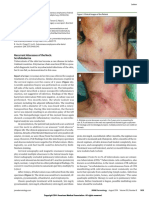
Figure 3 Skin biopsy. Necrotic xanthogranuloma. Presence of agents, plasmapheresis, and radiotherapy.5 However, it
collagen necrobiosis and giant cells. has been found that even with treatment the lesions tend
to be progressive, with recurrence of new lesions. Due to
its rarity, there is no recommended first-line treatment.
Thus, the therapeutic option should be chosen based on the
debris and collagen sclerosis. The findings favored necrobi- hematological conditions associated with the disorder, as
otic xanthogranuloma. In view of this diagnosis, monoclonal well as on the location, extent, and degree of impairment
gammopathy was investigated, and urinary immunofixa- of the patient’s life.
tion revealed a monoclonal band corresponding to the
kappa light chain (Bence Jones) and serum immunofixation, Financial support
detected by the IgG kappa monoclonal band. The patient
was referred to the hematology service, where he under-
None declared.
went bone marrow biopsy, without criteria for hematological
diseases at the time of the work up . The patient is cur-
rently using dapsone and presenting partial improvement Authors’ contribution
of the lesions. He has been followed in conjunction with
hematology. Isaura Azevedo Fasciani: composition of the manuscript.
NX has cutaneous findings, predominantly yellowish Neusa Yuriko Sakai Valente: statistical analysis, approval
plaques in the periorbital area, trunk, and extremities, most of the final version of the manuscript; participation in the
often associated with paraproteinemia, and can coexist with design of the study; critical review of the literature.
systemic involvement of multiple organs, such as the heart, Maria Claudia Alves Luce: conception and planning of the
respiratory system, spleen, kidneys, liver, skeletal muscle, study.
and central nervous system.2 Up to 80% of patients diagnosed Priscila Kakizaki: approval of the final version of the
with NX present or will present monoclonal paraproteine- manuscript; participation in the design of the study; critical
mia, predominantly of the monoclonal gammopathy type IgG review of the manuscript.
kappa or lambda.1
The association between NX and hematological disorders Conflicts of interest
is well documented, with an increased risk of hematological
diseases, malignancies, and lymphoproliferative disorders.3
None declared.
Hematologic disorders may occur up to eight years before
or 11 years after the appearance of cutaneous lesions.4
For this reason, patients diagnosed with NX require lifelong References
care.
CASE LETTER 119
1. Ugurlu S, Bartley GB, Gibson LE. Necrobiotic xanthogranuloma: a,∗
Isaura Azevedo Fasciani , Neusa Yuriko Sakai
long-term outcome of ocular and systemic involvement. Am J Valente a
, Maria Claudia Alves Luce b
,
Ophthalmol. 2000;129:651---7. Priscila Kakizaki b
2. Seastrom S, Bookout A, Hogan DJ. Necrobiotic xanthogran-
uloma without a monoclonal gammopathy. Cutis. 2014;94: a
Department of Dermatology, Hospital do Servidor Público
293---6. Estadual (HSPE), São Paulo, SP, Brazil
3. Spicknall KE, Mehregan DA. Necrobiotic xanthogranuloma. Int J b
Department of Dermatopathology, Hospital do Servidor
Dermatol. 2009;48:1---10. Público Estadual (HSPE), São Paulo, SP, Brazil
4. Wood AJ, Wagner MV, Abbott JJ, Gibson LE. Necrobiotic
xanthogranuloma: a review of 17 cases with emphasis on Corresponding author.
clinical and pathologic correlation. Arch Dermatol. 2009;145:
E-mail: isafasciani@hotmail.com (I.A. Fasciani).
279---84.
5. Miguel D, Lukacs J, Illing T, Elsner P. Treatment of necrobiotic Received 21 November 2018; accepted 13 March 2019
xanthogranuloma --- a systematic review. J Eur Acad Dermatol
Venereol. 2017;31:221---35. https://doi.org/10.1016/j.abd.2019.03.007
0365-0596/ © 2019 Sociedade Brasileira de Dermatologia.
Published by Elsevier España, S.L.U. This is an open access article
under the CC BY license (http://creativecommons.org/licenses/
by/4.0/).
A case of linear atrophoderma lines.1 LAM usually progresses as a linear atrophic lesion in
the first few months; then the lesion ceases to progress and
of Moulin夽,夽夽 persists. The etiology of LAM remains unclear. All reported
cases were so far sporadic. It may be connected with gene
Dear Editor,
mosaicism or autoimmunity. A study of the atrophic compo-
nent of LAM by ultrasonography revealed that subcutaneous
A 15-year-old Chinese girl presented with a 10-year history
volume reduction was the cause of the atrophic appearance,
of asymptomatic, unilateral light brown patches affect-
not dermal atrophy.2 Even though the clinical manifesta-
ing the right arm and right side of the trunk. The lesions
tion of LAM is rather unique, the histopathology of LAM is
were asymptomatic. There were no prior skin lesions or
quite inconspicuous. Hematoxylin and eosin staining usu-
inflammation. There was no significant medical or family
ally shows hyperpigmentation only in basal epidermal layers,
history. Physical examination found linear hyperpigmented
without abnormal collagen or elastic fibers in the dermis or
atrophic patches on the right arm and right trunk following
any obvious inflammation.1 There may be some perivascu-
Blaschko’s lines, involving both the anterior and posterior
lar lymphocytic infiltration, acanthosis, epidermal atrophy,
aspects. The skin was slightly atrophic on palpation. No
altered collagen in the dermis, and decreased or fragmented
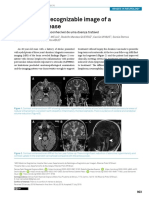
signs of induration or inflammation were noted (Fig. 1A and
elastic tissue.2
B). Laboratory investigations --- including full blood count,
Lopez et al.3 proposed the following diagnostic cri-
erythrocyte sedimentation rate, liver function test, renal
teria for -LAM, including: (1) Onset during childhood or
profile, and antinuclear antibodies --- were all negative or
adolescence; (2) Development of hyperpigmented, slightly
within the normal range. Biopsy of a lesion showed a nor-
atrophic, unilateral lesions following Blaschko lines on the
mal epidermis with increased pigmentation of the basal
trunk or limbs; (3) Absence of prior inflammation or sub-
layer, with more compact dermal collagen and mild upper
sequent scleroderma; (4) A stable, non-progressive clinical
dermal perivascular lymphocytic infiltration (Fig. 2). Der-
course without a pattern of remission; (5) Histologic find-
moscopy found multiple light brown networks with unclear
ings showing hyperpigmentation of the basal epidermis and
margins. The patient was diagnosed with linear atropho-
a normal dermis with unaltered connective tissue and elas-
derma of Moulin (LAM) and started treatment with topical
tic fibers. Up to now, more than 30 cases of LAM have been
halometasone 0.5% cream and hydroquinone 2% cream for
reported in the literature. However, the condition may be
two months, with no improvement.
overestimated. If the diagnostic criteria are strictly adhered
LAM is a rare and distinct clinical entity characterized
to, the diagnosis of LAM cannot be reached in some cases, as
by acquired unilateral, hyperpigmented, and atrophic ban-
these authors reported histologic findings that are compati-
dlike skin lesions following the lines of Blaschko, without
ble with other clinical entities.3
prior inflammation or sclerotic appearance. It is named after
LAM must be differentiated from atrophoderma of Pasini
Moulin, who, in 1992, reported on five patients with pig-
and Pierini (APP), which also presents with similar configura-
mented and more-or-less atrophic bands along Blaschko’s
tion, atrophy, and hyperpigmentation, but does not follow
Blaschko’s lines. In addition, LAM is different from linear
morphea, which usually presents preceding inflammation,
夽 How to cite this article: Zhang L-W, Ma M-S, Chen T, Fu L- induration, or scleroderma.
X. A case of linear atrophoderma of Moulin. An Bras Dermatol. Histopathologically, morphea shows collagen bundles
2020;95:119---21. that are closely packed and oriented horizontally, and der-
夽夽 Study conducted at the Chengdu Second People’s Hospital,
mal appendages and subcutaneous fat are progressively lost.
Sichuan, China.
You might also like
- Gastrointestinal Disorders GuideDocument14 pagesGastrointestinal Disorders GuideAnna Sofia Reyes100% (1)
- Short Atlas in Pediatrics Spot Diagnosis of The Most Common Pediatric Diseases 2nd EditionDocument113 pagesShort Atlas in Pediatrics Spot Diagnosis of The Most Common Pediatric Diseases 2nd Editiondeycallmebud100% (2)
- 5 Tumor Micro EnvironmentDocument33 pages5 Tumor Micro Environmentanon_945728920No ratings yet
- Posttest GeriaDocument7 pagesPosttest GeriaJohn Lyndon SayongNo ratings yet
- M: Elaine Crystine Vieira de Paiva Rua Pedro I, 1.033 Centro 60035-101 - Fortaleza - CE - BrazilDocument2 pagesM: Elaine Crystine Vieira de Paiva Rua Pedro I, 1.033 Centro 60035-101 - Fortaleza - CE - Brazilpruebaprueba321765No ratings yet
- (2017) BELOUSOVA, Irena E. Mycosis Fungoides Manifesting As Giant Cell Lichenoid DermatitisDocument3 pages(2017) BELOUSOVA, Irena E. Mycosis Fungoides Manifesting As Giant Cell Lichenoid DermatitisCassandra VérasNo ratings yet
- Scarisbrook - J Invest Dermatol - 2020 PDFDocument3 pagesScarisbrook - J Invest Dermatol - 2020 PDFOscar MerinoNo ratings yet
- Congenital Scalp Tumor With Ulceration: Jeremy Udkoff MA, MAS - Ralph E. Holmes MD - Magdalene A. Dohil MDDocument2 pagesCongenital Scalp Tumor With Ulceration: Jeremy Udkoff MA, MAS - Ralph E. Holmes MD - Magdalene A. Dohil MDAna MariaNo ratings yet
- Mud I Gonda 2013Document3 pagesMud I Gonda 2013Febyan AbotNo ratings yet
- Topical Rapamycin Solution To Treat Multiple Facial Angiofibromas in A Patient With Tuberous SclerosisDocument3 pagesTopical Rapamycin Solution To Treat Multiple Facial Angiofibromas in A Patient With Tuberous Sclerosisw0rfNo ratings yet
- Cutaneous GranulomasDocument2 pagesCutaneous GranulomasloreagubenjiNo ratings yet
- RARE COMBINATIONDocument4 pagesRARE COMBINATIONYuniita VerayantiiNo ratings yet
- Mikulicz Syndrome Diagnosis in Adolescent Boy via FNACDocument2 pagesMikulicz Syndrome Diagnosis in Adolescent Boy via FNACWasim ShaheenNo ratings yet
- Metastatic Squamous Cell Carcinoma of The ButtockDocument3 pagesMetastatic Squamous Cell Carcinoma of The ButtockApple StarNo ratings yet
- PJSS 66 2 Apr Jun 2011 6Document7 pagesPJSS 66 2 Apr Jun 2011 6Ranielle OngocoNo ratings yet
- Correspondence: Morphea masquerading as leprosyDocument3 pagesCorrespondence: Morphea masquerading as leprosyPriyanka JajuNo ratings yet
- Tsoi 1997Document7 pagesTsoi 1997Araceli Enríquez OvandoNo ratings yet
- Lethal Midline Granuloma-Stewart Nasal Nk/T-Cell Lymphoma-0ur ExperienceDocument9 pagesLethal Midline Granuloma-Stewart Nasal Nk/T-Cell Lymphoma-0ur Experienceopi akbarNo ratings yet
- 2005-Pigmentary Mosaicism and MosaicDocument2 pages2005-Pigmentary Mosaicism and MosaicANo ratings yet
- Management of Pearly Penile Papules: A Review of The LiteratureDocument7 pagesManagement of Pearly Penile Papules: A Review of The LiteratureMeta SakinaNo ratings yet
- Recurrent Abscesses of The Neck: Scrofuloderma: Bacterium Tuberculosis PCR Were Negative. A Culture Was NotDocument2 pagesRecurrent Abscesses of The Neck: Scrofuloderma: Bacterium Tuberculosis PCR Were Negative. A Culture Was NothadriantiNo ratings yet
- Pathophysiology of Meningiomas 2003Document18 pagesPathophysiology of Meningiomas 2003Klinik medan DeliNo ratings yet
- Int J Dermatology - 2022 - Iwasawa - Diagnostic Difficulties in Secondary Syphilis A Case ReportDocument3 pagesInt J Dermatology - 2022 - Iwasawa - Diagnostic Difficulties in Secondary Syphilis A Case ReportArmando NogueraNo ratings yet
- References: Alopecia Areata After Biologic Therapy: Report of A Case Related To AdalimumabDocument2 pagesReferences: Alopecia Areata After Biologic Therapy: Report of A Case Related To AdalimumabMasithaNo ratings yet
- Psoriais PDF NemDocument14 pagesPsoriais PDF NemFabiola VillanuevaNo ratings yet
- Acquired-cutaneous-lymphangiectasias-secondary-to-Document3 pagesAcquired-cutaneous-lymphangiectasias-secondary-to-Andrés WunderwaldNo ratings yet
- Chronic Wound Evaluation and Differential DiagnosisDocument17 pagesChronic Wound Evaluation and Differential DiagnosisVar AndaNo ratings yet
- Basal Cell Carcinoma in ChildhoodDocument2 pagesBasal Cell Carcinoma in ChildhoodAgustina D'AlessandroNo ratings yet
- The Roles of in Ammation in Keloid and Hypertrophic ScarsDocument10 pagesThe Roles of in Ammation in Keloid and Hypertrophic ScarsireneardianiNo ratings yet
- Malignant Myopericytoma: Report of A New Case and Review of The LiteratureDocument6 pagesMalignant Myopericytoma: Report of A New Case and Review of The LiteratureRachel AutranNo ratings yet
- Eritem PolimorfDocument3 pagesEritem PolimorfMădălina ŞerbanNo ratings yet
- Giant Hanging Melanoma of The Eye SkinDocument2 pagesGiant Hanging Melanoma of The Eye SkinRochnald PigaiNo ratings yet
- Granuloma AnnulareDocument9 pagesGranuloma AnnulareMiraNo ratings yet
- Langerhans Cell Histiocytosis in Children: History, Classification, Pathobiology, Clinical Manifestations, and PrognosisDocument10 pagesLangerhans Cell Histiocytosis in Children: History, Classification, Pathobiology, Clinical Manifestations, and PrognosisIchi Celico IzecsonNo ratings yet
- A Case Report of A 55 Year Old Female With Epulis GranulomatosaDocument3 pagesA Case Report of A 55 Year Old Female With Epulis GranulomatosaIsmail YusufNo ratings yet
- Warty Dyskeratoma As A Cutaneous Horn of The Mons PubisDocument3 pagesWarty Dyskeratoma As A Cutaneous Horn of The Mons PubisDomenica BourneNo ratings yet
- Encrucijadas ModelosDocument4 pagesEncrucijadas ModelosArandano L.No ratings yet
- Prurigo Nodularis of HydeDocument12 pagesPrurigo Nodularis of HydeAugusto MonjardimNo ratings yet
- JurnalDocument3 pagesJurnalnurlaras201102No ratings yet
- 9-Traumatic FibromaDocument3 pages9-Traumatic Fibromaasal bakhtyariNo ratings yet
- Keywords: Peripheral Giant Cell Granuloma/giant Cell Epulis, Jaw, ReactiveDocument4 pagesKeywords: Peripheral Giant Cell Granuloma/giant Cell Epulis, Jaw, ReactiveYeni PuspitasariNo ratings yet
- Pitfalls in Predicting Tumor Lysis SyndromeDocument4 pagesPitfalls in Predicting Tumor Lysis SyndromeAndikhaNo ratings yet
- 13 CR Lethal MidlineDocument3 pages13 CR Lethal MidlineSudhir BayyaNo ratings yet
- Molluscum Contagiosum: Report of One Case With OverviewDocument3 pagesMolluscum Contagiosum: Report of One Case With Overviewevitri pasaribuNo ratings yet
- Cytologic Findings of Proliferating Trichilemmal Tumor (PTT) of ScalpDocument4 pagesCytologic Findings of Proliferating Trichilemmal Tumor (PTT) of Scalpma hNo ratings yet
- Document on skin changes associated with hypothyroidismDocument3 pagesDocument on skin changes associated with hypothyroidismKrystal VallesNo ratings yet
- Wjoms v1 Id1009Document4 pagesWjoms v1 Id1009Nexi anessaNo ratings yet
- Case Report: Wouter Meersseman, Patrick Verschueren, Thomas Tousseyn, Rita de Vos, David CassimanDocument1 pageCase Report: Wouter Meersseman, Patrick Verschueren, Thomas Tousseyn, Rita de Vos, David Cassimanmafe alvarezNo ratings yet
- Lipophagic Panniculitis of Childhood: Chronic Actinic DermatitisDocument8 pagesLipophagic Panniculitis of Childhood: Chronic Actinic DermatitisHellgenius SantomauroNo ratings yet
- Segmental Neurofibromatosis: Report of A Rare EntityDocument3 pagesSegmental Neurofibromatosis: Report of A Rare EntityDwi Wahyu AprianiNo ratings yet
- 05Document2 pages05Ahsan JamilNo ratings yet
- Follicular Dendritic Cell Sarcoma of The Tonssilar About A CaseDocument4 pagesFollicular Dendritic Cell Sarcoma of The Tonssilar About A CaseInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Papuloerythroderma Case ReportDocument4 pagesPapuloerythroderma Case ReportLidwina ApyakaNo ratings yet
- Ulcerated Nodule of The FingernailDocument2 pagesUlcerated Nodule of The FingernailMr. LNo ratings yet
- Use of Injectable Platelet-Rich Fibrin in The Treatment of PlasmaDocument4 pagesUse of Injectable Platelet-Rich Fibrin in The Treatment of PlasmaNurul Fajriah YunitaNo ratings yet
- Solitary Fibrous Tumor of Parotid Gland 2022Document6 pagesSolitary Fibrous Tumor of Parotid Gland 2022Reyes Ivan García CuevasNo ratings yet
- Toxic Epidermal Necrolysis: A Paradigm of Critical IllnessDocument10 pagesToxic Epidermal Necrolysis: A Paradigm of Critical IllnessViolett LiebeNo ratings yet
- Hereditary Tumor Syndromes With Skin InvolvementDocument7 pagesHereditary Tumor Syndromes With Skin Involvementghinan jamilahNo ratings yet
- Article - Cytological Features of The Warthin-Like Variant of Salivary Mucoepidermoid CarcinomaDocument5 pagesArticle - Cytological Features of The Warthin-Like Variant of Salivary Mucoepidermoid CarcinomaCandeNo ratings yet
- Juvenile localized scleroderma case reportDocument3 pagesJuvenile localized scleroderma case reportMarisol Susan Poma CastilloNo ratings yet
- 2019 Zebras in Foreskin Dermatopathology (Natural Circumcision)Document6 pages2019 Zebras in Foreskin Dermatopathology (Natural Circumcision)msdsubNo ratings yet
- Stem CellDocument16 pagesStem CellVinnie Juliana YonatanNo ratings yet
- Molecular Mechanisms and Their Clinical Application in MalignanciesFrom EverandMolecular Mechanisms and Their Clinical Application in MalignanciesDaniel E. BergsagelNo ratings yet
- 1806 3713 Jbpneu 46 03 E20180422Document7 pages1806 3713 Jbpneu 46 03 E20180422Sango AyraNo ratings yet
- 1806 3713 Jbpneu 46 03 E20190397 PDFDocument1 page1806 3713 Jbpneu 46 03 E20190397 PDFSango AyraNo ratings yet
- 1980 5918 FM 33 E003321 PDFDocument9 pages1980 5918 FM 33 E003321 PDFSango AyraNo ratings yet
- Angiolymphoid Hyperplasia With Eosinophilia in The Lungs: A Complex Name For An Innocuous Disease?Document2 pagesAngiolymphoid Hyperplasia With Eosinophilia in The Lungs: A Complex Name For An Innocuous Disease?Sango AyraNo ratings yet
- Training With Elastic and Conventional Devices On Body Composition: Systematic Review and Meta-AnalysisDocument9 pagesTraining With Elastic and Conventional Devices On Body Composition: Systematic Review and Meta-AnalysisSango AyraNo ratings yet
- Acute Effect of Partial Body Weight Suspension On The Level of Cocontraction and Gait Biomechanics in Women With Knee OsteoarthritisDocument9 pagesAcute Effect of Partial Body Weight Suspension On The Level of Cocontraction and Gait Biomechanics in Women With Knee OsteoarthritisSango AyraNo ratings yet
- Radiologic and Histologic Findings in Sjögren's Sensory NeuronopathyDocument1 pageRadiologic and Histologic Findings in Sjögren's Sensory NeuronopathySango AyraNo ratings yet
- En - 1806 3713 Jbpneu 46 04 E20180366Document7 pagesEn - 1806 3713 Jbpneu 46 04 E20180366Sango AyraNo ratings yet
- Physical Activity Level Among Older Adultsover 70 Years Old and Very Old AdultsDocument10 pagesPhysical Activity Level Among Older Adultsover 70 Years Old and Very Old AdultsSango AyraNo ratings yet
- Investigation of Chromosomal Alterations in Patients With Alzheimer's Disease in The State of Amazonas, BrazilDocument5 pagesInvestigation of Chromosomal Alterations in Patients With Alzheimer's Disease in The State of Amazonas, BrazilSango AyraNo ratings yet
- 1678 4227 Anp 77 12 0903Document2 pages1678 4227 Anp 77 12 0903Sango AyraNo ratings yet
- Cervical Spine Range of Motion, Posture and Electromyographic Activity of Masticatory Muscles in Temporomandibular DisordersDocument16 pagesCervical Spine Range of Motion, Posture and Electromyographic Activity of Masticatory Muscles in Temporomandibular DisordersSango AyraNo ratings yet
- PKA-pERK Role in ABA AnalgesiaDocument7 pagesPKA-pERK Role in ABA AnalgesiaSango AyraNo ratings yet
- Effects of Intra-Dentate Gyrus Microinjection of Myokine Irisin On Long-Term Potentiation in Male RatsDocument7 pagesEffects of Intra-Dentate Gyrus Microinjection of Myokine Irisin On Long-Term Potentiation in Male RatsSango AyraNo ratings yet
- Origins of Neurology in BrazilDocument8 pagesOrigins of Neurology in BrazilSango AyraNo ratings yet
- Resolution of Headache After Reduction of Prolactin Levels in Hyperprolactinemic PatientsDocument6 pagesResolution of Headache After Reduction of Prolactin Levels in Hyperprolactinemic PatientsSango AyraNo ratings yet
- 1678 4227 Anp 77 12 0848Document7 pages1678 4227 Anp 77 12 0848Sango AyraNo ratings yet
- Con Icts of Interest: Multiple Adult XanthogranulomaDocument3 pagesCon Icts of Interest: Multiple Adult XanthogranulomaSango AyraNo ratings yet
- Francis Rohmer: From The Neurological Ward To Dachau and BackDocument3 pagesFrancis Rohmer: From The Neurological Ward To Dachau and BackSango AyraNo ratings yet
- Dermatologia: Anais Brasileiros deDocument5 pagesDermatologia: Anais Brasileiros deSango AyraNo ratings yet
- Fulminant Toxoplasmosis Presenting As Isolated Myelitis: Toxoplasmose Fulminante Se Apresentando Como Mielite IsoladaDocument2 pagesFulminant Toxoplasmosis Presenting As Isolated Myelitis: Toxoplasmose Fulminante Se Apresentando Como Mielite IsoladaSango AyraNo ratings yet
- Dermatologia: Anais Brasileiros deDocument9 pagesDermatologia: Anais Brasileiros deSango AyraNo ratings yet
- Dermatologia: Anais Brasileiros deDocument2 pagesDermatologia: Anais Brasileiros deSango AyraNo ratings yet
- Spiky Follicular Mycosis Fungoides and Hidradenitis Suppurativa-Like Lesions in A Patient - Complete Remission With Interferon AlphaDocument3 pagesSpiky Follicular Mycosis Fungoides and Hidradenitis Suppurativa-Like Lesions in A Patient - Complete Remission With Interferon AlphaSango AyraNo ratings yet
- Dermatologia: Anais Brasileiros deDocument3 pagesDermatologia: Anais Brasileiros deSango AyraNo ratings yet
- Explosives CompositionDocument9 pagesExplosives Compositionwerdna67No ratings yet
- Ehrlichiosis FDocument1 pageEhrlichiosis Frodrigo lopez jimenezNo ratings yet
- CASE STUDY Peptic Ulcer Disease-1Document6 pagesCASE STUDY Peptic Ulcer Disease-1LintangNAnggraeniNo ratings yet
- Communication DisordersDocument26 pagesCommunication DisordersShainah Marie DichosoNo ratings yet
- NURS FPX 6618 Assessment 1 Planning and Presenting a Care Coordination ProjectDocument5 pagesNURS FPX 6618 Assessment 1 Planning and Presenting a Care Coordination Projectjoohnsmith070No ratings yet
- 1.3 Respiratory DiseasesDocument14 pages1.3 Respiratory DiseasesgalvezchestertimothyNo ratings yet
- Chronic Suppurative Otitis MediaDocument6 pagesChronic Suppurative Otitis MediaSuhas IngaleNo ratings yet
- Case Report 3: Ectopic Pregnancy (Surgical) : Laboratory/Diagnostic FindingsDocument12 pagesCase Report 3: Ectopic Pregnancy (Surgical) : Laboratory/Diagnostic FindingsKM DelantarNo ratings yet
- Thyroid Disorders During PregnancyDocument25 pagesThyroid Disorders During PregnancyA.H.ANo ratings yet
- Transes Anaphy UrinaryDocument6 pagesTranses Anaphy UrinaryPia LouiseNo ratings yet
- Region X RRP PDFDocument142 pagesRegion X RRP PDFGlenn S. GarciaNo ratings yet
- Stones in Galbladder - Pitay Ki Pathri - Homeopathic MedicineDocument4 pagesStones in Galbladder - Pitay Ki Pathri - Homeopathic MedicineParwaz KamalNo ratings yet
- Early Embryology: Somite Stage and Limb Bud DevelopmentDocument21 pagesEarly Embryology: Somite Stage and Limb Bud DevelopmentDavidroy IRITSNo ratings yet
- Gene Environment InteractionDocument26 pagesGene Environment InteractionAwais GulNo ratings yet
- Full Download Ebook Ebook PDF Med Surg Success A Qa Review Applying Critical Thinking To Test Taking Daviss Qa Success 3rd Edition PDFDocument42 pagesFull Download Ebook Ebook PDF Med Surg Success A Qa Review Applying Critical Thinking To Test Taking Daviss Qa Success 3rd Edition PDFlillie.christopher194100% (35)
- Presented By, Dr. Likhit T House Surgeon Medicine D Unit MmcriDocument73 pagesPresented By, Dr. Likhit T House Surgeon Medicine D Unit MmcriVasu LohraNo ratings yet
- Trans Savi Oto Lec 01 Head and Neck History and PE 1st SemesterDocument12 pagesTrans Savi Oto Lec 01 Head and Neck History and PE 1st SemesterJoherNo ratings yet
- Sexually Transmitted Infections or Diseases (Stis or STDS) : Last Updated: July 20, 2021Document28 pagesSexually Transmitted Infections or Diseases (Stis or STDS) : Last Updated: July 20, 2021RiteshNo ratings yet
- Note 1Document30 pagesNote 1Gopika SNo ratings yet
- Thalassemiafinal 111212142013 Phpapp02 130321172427 Phpapp01Document35 pagesThalassemiafinal 111212142013 Phpapp02 130321172427 Phpapp01MUHAMMAD WAQAS TARIQNo ratings yet
- Artikel SaraaaaaDocument8 pagesArtikel SaraaaaaArdiantiWulandariHusenNo ratings yet
- A Public Health Approach To Health and Retirement: What Do We Know About Their Relationship?Document11 pagesA Public Health Approach To Health and Retirement: What Do We Know About Their Relationship?Great PotatosNo ratings yet
- Surgical Instruments: March 2015Document122 pagesSurgical Instruments: March 2015Frida RasyidNo ratings yet
- Is It Psychological, Physical, or Both?: Sue M. Mcdonnell, PHD, CaabDocument8 pagesIs It Psychological, Physical, or Both?: Sue M. Mcdonnell, PHD, CaabSarai Snchz PrietoNo ratings yet
- Overview of The StudyDocument11 pagesOverview of The StudyNaveen rajNo ratings yet
- MLPA Dummy ReportDocument3 pagesMLPA Dummy ReportAakash verma100% (1)
- Nails in Nutritional DefinciesDocument5 pagesNails in Nutritional DefinciesstcerieNo ratings yet