Professional Documents
Culture Documents
Assessmentofhearing
Uploaded by
Nitin Sharma0 ratings0% found this document useful (0 votes)
33 views85 pagesThis document summarizes key aspects of hearing assessment:
1. It describes the structures of the auditory system including the organ of Corti and its components like hair cells and supporting cells.
2. It outlines clinical tests used to assess hearing like tuning fork tests, Rinne test, Weber test, and bone conduction tests.
3. It explains audiometric tests including pure tone audiometry where air and bone conduction thresholds are measured to create an audiogram.
4. Common types of hearing loss and their characteristics are defined such as conductive, sensorineural, and mixed hearing loss.
Original Description:
;LDFMGK;LESGJMISTJ
Original Title
assessmentofhearing
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document summarizes key aspects of hearing assessment:
1. It describes the structures of the auditory system including the organ of Corti and its components like hair cells and supporting cells.
2. It outlines clinical tests used to assess hearing like tuning fork tests, Rinne test, Weber test, and bone conduction tests.
3. It explains audiometric tests including pure tone audiometry where air and bone conduction thresholds are measured to create an audiogram.
4. Common types of hearing loss and their characteristics are defined such as conductive, sensorineural, and mixed hearing loss.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
33 views85 pagesAssessmentofhearing
Uploaded by
Nitin SharmaThis document summarizes key aspects of hearing assessment:
1. It describes the structures of the auditory system including the organ of Corti and its components like hair cells and supporting cells.
2. It outlines clinical tests used to assess hearing like tuning fork tests, Rinne test, Weber test, and bone conduction tests.
3. It explains audiometric tests including pure tone audiometry where air and bone conduction thresholds are measured to create an audiogram.
4. Common types of hearing loss and their characteristics are defined such as conductive, sensorineural, and mixed hearing loss.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 85
Assessment of Hearing
Dr. Maria Sajjad
AUDITORY SYSTEM
Organ of Corti
o Sense organ of hearing, It is situated on the basilar
membrane.
o Important components:
• Tunnel of Corti: Formed by inner and outer rods.
• Hair cells: Receptor cells of Hearing
Transfers sound energy into electrical energy.
Inner hair cells are supplied by afferent cochlear
fibres.
Outer hair cells receive efferent innervation from
olivary complex.
• Supporting Cells:
Dieters` cells: provide support to outer hair
cells.
Cells of Hensen: lie outside Dieters` cells.
• Tectorial Membrane: Overlies the organ of
corti. Shearing force between the hair cells
and tectorial membrane produces the
stimulus to hair cells.
Structure of organ of corti
Nerve supply of Hair cells
• 95% of Afferent fibres of spiral ganglion supply
the inner hair cells, while 5% supply the outer
hair cells.
• Efferent fibres to the hair cells come from
olivocochlear bundle whose cell bodies are
situated in superior olivary complex.
Auditory Pathway
Hair cells
Dendrites of bipolar cells
of spiral ganglion
Axons of bipolar cells form
cochlear division of CN VIII
Cochlear Nuclei
Superior olivary complex
Lateral lemniscus
Nucleus of lateral lemniscus
Inferior colliculus
Medial geniculate body
Auditory radiations
Auditory cortex (area 41)
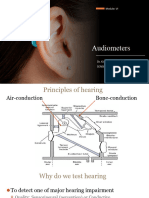
Mechanism of Hearing
• Mechanical conduction of sound
Pinna EAC Tympanic Memberane
• Chain of Ossicles Stapes Foot Plate
Pressure changes in inner ear fluid
Movement of basilar membrane
Stimulation of hair cells.
• Tranduction of mechanical energy to electrical
impulses:
Movement of basilar membrane sets up
shearing force between tectorial membrane
and hair cells.
Distortion of hair cells gives rise to cochlear
microphonics which trigger the nerve impulse.
• Neural Pathways.
Frequently used terms
• Frequency: Number of cycles per second
• Pure tone: Single frequency sound
• Complex sound: Sound with more than one
frequency.
• Decibel (dB): Unit to determine intensity of
sound. It is 1/10th of a bel, and named after
Graham Bell.
• Masking: Phenomenon to produce inaudibility
of one sound by the presentation of the other.
Types of Hearing Loss
• Conductive hearing loss: caused by
interference of sound conduction from
external ear to stapediovestibular joint.
• Sensorineural hearing loss: results from either
lesion of cochlea (sensory type) or from lesion
of VIIIth nerve and its connections (neural
type). Neural can be further divide as:
Retrocochlear: lesion of VIIIth nerve,
Central: Lesion of central auditory
connections
• Mixed Hearing loss:
Elements of both conductive and
sensorineural deafness are present in the
same ear.
• NOHL:
No organic lesion present. It is either
psychogenic or due to malingering (usually
involved in litigation)
Assessment of Hearing
Clinical tests:
Tuning Fork tests:
• Performed with tuning forks of different
frequencies (128,256,512,1024,2048,4096)
• Most Commonly used tuning fork has a
frequency of 512Hz.
• AC measures both the conducting mechanism
and cochlea.
• BC measures cochlear function only.
Tuning forks
Rinne Test
• AC is compared with BC
• Vibrating tuning fork is placed on patient`s
mastoid and when he stops hearing, it is
placed erect and in line with the EAC, about
2cm from the orifice.
• If he still hears AC is more than BC.
• It is called positive when AC is longer and
louder than BC. It is seen in normal persons or
those having sensorineural deafness.
• Negative Rinne ( BC > AC) is seen in
conductive deafness.
• False negative Rinne test:
• patient has no hearing in test ear.
• BC stimulus may be perceived by contralateral
ear.
• No hearing by AC the result is labeled as Rinne
negative.
• This mistaken impression of function in a non
functioning ear is called false negative Rinne
test.
Weber Test
• Tuning fork is struck and base placed on either
the forehead, vertex or upper incisor teeth.
• Patient is asked where the sound is heard the
loudest.
• Normal hearing person: Sound is heard
equally in both ears.
• Conductive deafness: Lateralized to worse ear.
• SN deafness: Lateralized to better ear.
• Lateralized weber in conductive deafness may
indicate a hearing loss of 10-15 dB.
Modified Schawabach Test(ABC test)
• Compares the bone conduction of patient
with that of a normal hearing
person(examiner).
• Tuning fork is placed on the patients mastoid
with the meatus blocked and when the
patient no longer hears it, it is placed on the
normal hearing person`s mastoid.
• Conductive deafness + Normal hearing
person: Patient and examiner hear the fork for
the same duration.
• SN deafness: Patient hears the fork for a
shorter duration.
Bing Test
• Test of BC, and examines the effect of occlusion
of ear canal on hearing.
• Vibrating tuning fork is placed on the mastoid
while the examiner alternately closes and opens
the ear canal by pressing tragus inward.
• Normal person+ SN hearing loss: Hears louder
when ear canal is occluded and softer when canal
is open. (Bing +)
• Conductive hearing loss: No change appreciated
( Bing -).
Gelle`s test
• Test of BC and examines the effect of
increased air pressure in ear canal on hearing.
• Vibrating tuning fork is placed on the mastoid
while air pressure in ear canal is changed by
Siegle`s speculum.
• Normal person + SN hearing loss: Hearing is
decreased ( Gelle`s +).
• Conductive deafness: No change (as ossicular
chain is fixed or disconnected) (Gelle`s -).
Audiometric Tests
Pure Tone Audiometry
PTA
• An audiometer is an electronic device which
produces pure tones, intensity of which can be
increased or decreased in 5 dB steps.
• AC thresholds are measured for tones of
125,250,500,1K,2K,4K,8K Hz.
• BC thresholds are measured for tones of
250,500,1K,2K,4K Hz.
• It is charted in the form of a graph called
audiogram.
Precautions
• Patient should be visible to the tester, and
respond by signaling.
• No visible or tactile clues should be available
to the patient regarding the hearing stimulus.
• Test should be conducted in a sound proof
room.
• Duration of presentation should be 1-3 sec.
• The head phones should be properly seated
over the external auditory canal.
• The audiometer should be properly checked
before performing the test.
• Before placing the ear phones on the patient,
the patient's ear should be examined for the
presence of wax. If present it should be
cleaned.
Procedure
• Pure tone air conduction threshold is tested using
head phones.
• “Up 5-down 10" method of threshold estimation:
This technique is based on Hughson - Westlake
ascending technique.
• Tones of short duration is used for threshold
estimation. This method of threshold estimation
involves the following steps:
• Step I : The better ear is tested first in order to
determine the need for masking.
• Step II : Start with a 1000 Hz tone at a level above
the threshold to allow easy identification of the
tone. If the patient is suspected to be having a
profound hearing loss then the testing should be
started with 250Hz frequency. This is because of
the fact that the individuals with profound
hearing loss often have testable hearing only in
the low frequency range.
• Step III : The patient's understanding of the
listening task should be checked by using both
short and long duration test tones. The patient
should be instructed to raise the index finger as
soon as the sound is heard.
Step IV : During testing, the examiner should vary
the interval between tone presentations to avoid
telegraphing the stimulus.
• Step V : The starting intensity of the test tone is
reduced in 10 dB steps following each positive
response, until a hearing threshold level is
reached at which the subject fails to respond.
Then, the tone is raised by 5 dB until tone is
heard.The threshold is defined as the faintest
tone that can be heard 50% or more of the
time, and is established after several threshold
crossings.
• Second ear is then test in the same way with
the retest beginning at 1K Hz.
• If there is difference in AC threshold exceeding
40dB at any frequency masking should be
used.
• Bone Conduction level are measured between
250Hz and 4K Hz.
• BC is tested using a bone vibrator.
• The auditory threshold is assessed as
described for air conduction assessment. The
only difference is that the better hearing ear
should be masked using a masking tone
delivered via a head phone.
Scale of hearing threshold estimation in
audiometry:
dB loss Description
- 10 to 15 Normal limits
16 - 19 Mild hearing loss
30 - 44 Moderate hearing loss
45 - 59 Moderately severe hearing loss
60 - 79 Severe hearing loss
80 and above Profound hearing loss
Nomenclature on the pure tone
audiogram
• O right air conduction
• X left air conduction
• [ masked right bone conduction
• ] masked left bone conduction
Conductive hearing
loss, low tone
Otitis media with
effusion:
A conductive loss
maximal in the low
frequencies with now
sensorineural element.
Conductive hearing loss
Conductive hearing loss
across the audiometric
range with an increase in
the BC threshold
(caharts`notch) at 2kHZ.
Caharts` notch reflects a
loss in the inertial
component of stapes
footplate.
Sensorineural hearing loss, low tone
(meinere’s disease)
Sensorineural hearing loss with a
notch at 6 kHz (noise induced hearing
loss)
Speech Audiometry
• Patient`s ability to hear and understand
speech is measured.
• Two parameters are studied:
a. Speech Reception threshold
b. Discrimination score
Speech Reception Threshold(SRT)
• Minimum Intensity at which 50% words are
repeated correctly by the patient.
• Set of spondee words is delivered to each ear.
• Intensity is varied in 5dB steps till half of them are
correctly heard.
• Normally SRT is within 10dB of the average of
pure tone threshold of 3 speech
freqeuncies(500, 1K, 2K Hz).
• SRT better than pure tone average by more than
10db suggests a functional hearing loss.
Discrimination score
• Measure of patient`s ability to understand
speech.
• List of phonetically balanced (PB) words
(single syllable) is delivered to each ear
separately at 30 to 40 dB above his SRT and %
of words correctly heard is recorded.
• In normal persons and with CHL score of 90 to
100% can be obtained.
Bekesy Audiometry
• Self recording audiometry where various pure
tone frequencies automatically move from low to
high while patient controls intensity through a
button.
• Two tracings one with continuous and other with
pulsed tone are obtained.
• They help to differentiate a cochlear from
retrocochlear and organic from functional
hearing loss.
• It is rarely done these days.
Impedence audiometry
• The primary purpose of impedence
audiometry is to determine the status of the
tympanic membrane and the middle ear.
• It is divided into 2 parts:
a. Tympanometry
b. Acoustic reflex measurements.
Tympanometry
• Altering the pressure in the EAC results in
changes in compliance because the TM is tense
and ossicular chain stiffened.
• Point of maximum compliance occurs when the
pressure in the meatus is equal to that in the
middle ear.
• If the pressure exceeds or falls below the middle
ear pressure, compliance will be reduced.
• Indirectly middle ear pressure can be calculated
from point of maximum complaince.
Procedure
• Probe is inserted into the external auditory canal till a air
tight seal is obtained. Probe tone is presented typically at
226Hz into the ear canal while the air pressure of the
canal is altered between +200 and - 400 decapascals. The
maximum compliance occurs when the pressure of the
external auditory canal and the middle ear becomes
equal.
• The compliance peak indicates the pressure of the
middle ear.
• The height of the compliance peak indicates the mobility
/ stiffness of the tympanic membrane or the middle ear
cavity.
• By charting the compliance of tympanoossicular system
various pressure changes different types of
tympanograms are obtained.
Types of tympanograms:
• Type A: Normal Tympanogram
• Type As: Reduced compliance at or near
ambient air pressure, seen in fixation of
ossicles.
• Type Ad: Increased compliance at or near
ambient pressure seen in ossicular
discontinuity or thin or lax TM.
• Type B: Flat or dome shaped graph. No change
in compliance with pressure changes. Seen in
middle ear fluid or thick TM.
• Type C: Maximum compliance at pressures
more than -100mmH2O (negative pressure in
middle ear).
Acoustic(Stapedial) reflex
Measurements
• A loud sound, 70-100dB above the threshold
of hearing of a particular ear causes bilateral
contraction of the stapedial muscle which can
be detected by Tympanometry.
• Reflex arc is the VIIIth nerve, cochlear nucleus
and complex brainstem internuclear
connections to the ipsilateral and contralateral
facial nuclei, facial nerve and the nerve to
stapedius.
• Minimal auditory stimulus that produces a
contraction of stapedius muscle is known as
acoustic reflex threshold and indicated on an
audiogram by the letter ‘Z’.
Physical volume of ear canal
• Acoustic immitance can measure the phsyical
volume of air between probe tip and TM.
• Normally it is upto 1ml in children and 2ml in
adults.
• If > 2ml in children and > 2.5ml in adults,
indicates perforation of TM.
Special Tests
Short Increment Sensitivity Index
(SISI Test)
• The SISI test is still widely used to determine
whether the patient is having cochlear
pathology. This test is based on a
phenomenon known as recruitment
(abnormal loudness growth).
• Recruitment: The ear which does not hear low
intensity sounds begins to hear greater
intensity sounds as loud or even louder than
normal hearing ear.
• A continous tone is presented 20dB above the
threshold and sustained for two minutes.
• Every 5 sec tone is increased by 1dB and 20
such blips are presented. Patient indicates the
blips heard.
• In conductive deafness SISI score is more than
15%, 70-100% in cochlear deafness, 0-20% in
nerve deafness.
Evoked Response Audiometry
• It measures electrical activity in the auditory
pathways in response to auditory stimuli.
• Two most important component of evoked
electrical response are:
a. Electrocochleography
b. Auditory brainstem response (ABR).
Electrocochleography
• It measures electrical potential arising in the
cochlea and CN VIIIth in response to auditory
stimuli within first 5 milliseconds.
• There are three classes of potentials that can be
recorded .They are compound action potential of
auditory nerve (AP), Summating potential
(SP), and cochlear potential (CP) also known as
cochlear microphonic.
• Recording electrode is usually a thin needle
passed through the TM onto the promontory.
• In Adults it can be done under LA, but in
children or anxious individuals sedation or GA
is required.
• It is useful:
a. To find threshold of hearing in young infants
and children.
b. To differentiate lesions of the cochlea from
those of CN VIII.
Auditory brainstem response (ABR)
• Also known as Brain stem evoked response
audiometry.
• BERA is resistant to the effects of
sleep, sedation, sleep and anesthesia.
• BERA is an objective way of eliciting brain
stem potentials in response to audiological
click stimuli. These waves are recorded by
electrodes placed over the scalp.
• Since the electrodes should be placed over
the head, the hair must be oil free.
• The standard electrode configuration for BERA
involves placing a non inverting electrode over
the vertex of the head, and inverting
electrodes placed over the ear lobe or mastoid
prominence.
• One more earthing electrode is placed over
the forehead.
• In brain stem evoked response audiometry,
the impulses are generated by the brain stem.
• These impulses when recorded contains a
series of peaks and troughs.
• The positive peaks (vortex positive) are
referred to by the Roman numerals I - VII.
• These peaks are considered to originate from
the following anatomical sites:
1. Cochlear nerves - waves I and II
2. Cochlear nucleus - wave III
3. Superior olivary complex - wave IV
4. Nulclei of lateral lemniscus - wave V
5. Inferior colliculus - waves VI and VII
• Uses of BERA:
I. As a screening procedure for infants.
II. To determine the threshold of hearing in children and
adults who do not cooperate and in malingerers.
III. To diagnose retrocochlear pathology particularly
acoustic neuroma.
IV. To diagnose brainstem pathology e.g multiole
sclerosis or pontine tumors.
V. To monitor CN VIII intraoperatively in surgery of
acoustic neuroma.
Otoacoustic emissions (OAE)
• Sounds produced by motile elements of
cochlear outer hair cells.
• Can be elicited by a very sensitive microphone
placed in EAC.
• Sounds produced by outer hair cells travel in a
reverse direction: outer hair cells Basilar
Memberane perilymph oval window
ossicles TM EAC.
• OAEs are present when outer hair cells are
healthy and absent when they are damaged, thus
help test function of cochlea.
• Uses:
1. To screen children and neonates for hearing
disabilities
2. Estimate hearing sensitivity within a limited
range of frequencies
3. To differentiate sensory and neural components
in sensorineural hearing loss
4. To rule out malingering (functional hearing loss).
Hearing assessment in Infants and
Children
Screening Procedures
• They are employed to test hearing in high risk
infants and are based on infants behavioral
response to sound stimuli.
• Arousal test: High frequency noise is
presented for 2 secs to the infant when he is
in light sleep. Normal hearing infant can be
aroused twice when 3 such stimuli are
presented.
• Auditory response cradle: screening device for
newborns where baby is placed in a cradle
and his behaviour in response to auditory
stimulation are monitored by transducers.
Behaviour Observation Audiometry
• Auditory signal presented to an infant produces a
change in behaviour e.g alerting, cessation of an
activity or widening of eyes.
• Moro`s reflex: sudden movement of limbs and
extension of head in response to sound of 80-90
dB.
• Cochleopalpebral reflex: Child responds by a blink
to aloud sound.
• Cessation reflex: Infant stops activity or starts
crying in response to a sound of 90 dB.
Behaviour Observation Audiometry
Visual Reinforcement
Audiometry(VRA)
• This test technique is suited to infants aged 7 or 8
months to 3 years developmentally.
• The child is taught (i.e., conditioned) to turn their head
when a sound is heard.
• Initial conditioning is achieved by the introduction of
stimuli at moderately high levels
• When child looks for source of sound they are shown a
colourful, moving puppet or toy under illumination as a
reward.
• This puppet or toy "reinforces" the child's
turning behaviour or orientation and gives rise
to the term Visual Reinforcement Orientation
Audiometry. Once this conditioned response is
reliably observed, the stimuli can be
presented at ever decreasing levels until
auditory threshold or minimum audible levels
have been reached.
Visual Reinforcement
Audiometry(VRA)
Play Audiometry
• Play audiometry is suited to children aged around 3 to
7 years developmentally.
• The child is taught to respond, using a pre-determined
task, whenever they hear tonal stimuli that are
introduced through headphones or through a bone
conductor placed behind the ear on the mastoid.
• Given sufficient cooperation from the child it is usually
possible to produce a complete and accurate
"audiogram" that illustrates their threshold of hearing
for a pre-determined frequency range.
Play Audiometry
Speech Audiometry
• Child is asked to repeat the names of certain
objects or to point them out on the pictures.
• Voice can be gradually lowered.
• In this way hearing level and speech
discrimination can be tested.
Objective Tests
• Evoked Response Audiometry:
a. Electrocochleography.
b. Brainstem Evoked Response Audiometry
(BERA).
• Otoacoustic Emmisions.
• Impedance Audiometry.
THANK YOu
You might also like
- GRBASDocument4 pagesGRBASNitin Sharma100% (1)
- Radiology SpottersDocument58 pagesRadiology SpottersPartha Ganesan33% (3)
- Pathophysiology of Migraine.5Document11 pagesPathophysiology of Migraine.5Bryan100% (1)
- Audiology: DR Humra ShamimDocument69 pagesAudiology: DR Humra ShamimNitin SharmaNo ratings yet
- Auditory Tests With Disease Specific SignificanceDocument60 pagesAuditory Tests With Disease Specific SignificanceSonal SharmaNo ratings yet
- Test of Hearing and Pure Tone AudiometryDocument35 pagesTest of Hearing and Pure Tone AudiometryarjumandNo ratings yet
- Hearing EvaluationDocument151 pagesHearing EvaluationDr Sravya M VNo ratings yet
- Assessment of HearingDocument51 pagesAssessment of HearingSwetha PasupuletiNo ratings yet
- Audiometric Testing: Presented By: Azmat TahiraDocument31 pagesAudiometric Testing: Presented By: Azmat Tahiraayesha badarNo ratings yet
- Audiometric Testing: Presented By: Azmat TahiraDocument31 pagesAudiometric Testing: Presented By: Azmat Tahiraayesha badarNo ratings yet
- Assessment of HearingDocument114 pagesAssessment of Hearinghonda matiz100% (2)
- Tes Garpu TalaDocument13 pagesTes Garpu TalaSamuel ChristianNo ratings yet
- Assessment of HearingDocument30 pagesAssessment of HearingNitin SharmaNo ratings yet
- Hearing AssessmentDocument30 pagesHearing AssessmentRitesh SuranaNo ratings yet
- Noise Induce Hearing LossDocument8 pagesNoise Induce Hearing LossGunawan AliNo ratings yet
- Tuning Fork TestDocument56 pagesTuning Fork TestAbdur RaqibNo ratings yet
- 9 Audiometer 03 07 2023Document30 pages9 Audiometer 03 07 2023Kushagra Narang 21BML0031No ratings yet
- Yilkal Zemene, M.D., ENT, Head and Neck Surgeon Mekelle University, MekelleDocument34 pagesYilkal Zemene, M.D., ENT, Head and Neck Surgeon Mekelle University, MekelleruthNo ratings yet
- BeraDocument34 pagesBeramrabhilekhNo ratings yet
- Assessment of HearingDocument45 pagesAssessment of HearingRachanaNo ratings yet
- Lecture 2 - Audiometry PracticalDocument42 pagesLecture 2 - Audiometry PracticalSaera Hafiz Nikita100% (1)
- Biomedical Inst. Lec 4 PDFDocument25 pagesBiomedical Inst. Lec 4 PDFLari EvergardenNo ratings yet
- Emailing AudiologyDocument42 pagesEmailing AudiologyIsabel CastilloNo ratings yet
- Tuning Fork TestDocument24 pagesTuning Fork Testazadut100% (1)
- Tuning Fork Test PDFDocument24 pagesTuning Fork Test PDFazadutNo ratings yet
- Pemeriksaan PendengaranDocument63 pagesPemeriksaan PendengaranHeather PorterNo ratings yet
- Pure Tone AudiometryDocument13 pagesPure Tone AudiometryDanishyana DhiwaneoNo ratings yet
- 1 PB AnatomyDocument27 pages1 PB AnatomyMuhammad AdhaNo ratings yet
- 4 PTA and TympanometryDocument22 pages4 PTA and TympanometryMariam QaisNo ratings yet
- Weber TestDocument5 pagesWeber TestSuranewNo ratings yet
- FlashcardsDocument140 pagesFlashcardsDoodNo ratings yet
- Sense of Hearing: Exercise 9Document4 pagesSense of Hearing: Exercise 9Stephen YorNo ratings yet
- EENT NotesDocument12 pagesEENT Noteslsdmode100% (1)
- The Acoustic Analyzer. Methods of Examination.Document69 pagesThe Acoustic Analyzer. Methods of Examination.waqar khanNo ratings yet
- Tests To Diagnose Dead Regions in Cochlea-AgDocument37 pagesTests To Diagnose Dead Regions in Cochlea-AgVenkat NandhuNo ratings yet
- Auditory Brainstem Evoked Response (Abr)Document37 pagesAuditory Brainstem Evoked Response (Abr)Nitin Sharma100% (2)
- Prof. Dr. Mohamed Talaat EL - Ghonemy Facebook/O6UentDocument33 pagesProf. Dr. Mohamed Talaat EL - Ghonemy Facebook/O6Uentadel madanyNo ratings yet
- HearingDocument3 pagesHearingAnnabelle ArtiagaNo ratings yet
- Cochlear ImplantDocument33 pagesCochlear ImplantNithiyah DevarajuNo ratings yet
- Reflex Measurements: Quick GuideDocument10 pagesReflex Measurements: Quick GuidefilippobNo ratings yet
- MPEG AudioDocument68 pagesMPEG Audiocsivaranjani69No ratings yet
- Audio BaileyDocument7 pagesAudio BaileyMonisa HiraNo ratings yet
- Hearing LossDocument19 pagesHearing LossGuna ChaitanyaNo ratings yet
- Pendekatan Klinis Penurunan PendengaranDocument29 pagesPendekatan Klinis Penurunan PendengaranHeather PorterNo ratings yet
- Bera TestDocument34 pagesBera Testassumpta0% (1)
- IE464 - T6 - Auditory, Tactile, and Vestibular SystemDocument23 pagesIE464 - T6 - Auditory, Tactile, and Vestibular SystemIbrahem AbdulrahmanNo ratings yet
- Physiology of Special SenseDocument101 pagesPhysiology of Special SenseRefqueensasNo ratings yet
- Manual Lab Audiology - For StudentDocument12 pagesManual Lab Audiology - For StudentAnnisa Alifia AksaniNo ratings yet
- Aud4001 Lecture NotesDocument13 pagesAud4001 Lecture NotesjazmashNo ratings yet
- Clinical Tests For HearingDocument23 pagesClinical Tests For HearingAnindya NandiNo ratings yet
- Principles of Audiologic EvaluationDocument42 pagesPrinciples of Audiologic EvaluationJohnson JayarajNo ratings yet
- A Story About The Ear: Mrs. JamesonDocument40 pagesA Story About The Ear: Mrs. JamesonDito TrunogatiNo ratings yet
- Second DayDocument47 pagesSecond DayMeryville JacildoNo ratings yet
- Tuning Fork Tests: Name: Roll No: Assignment: Submitted ToDocument3 pagesTuning Fork Tests: Name: Roll No: Assignment: Submitted ToFizza AliNo ratings yet
- 2.0 Information Sources 2.1 Audio Signals: Dr. Ing. Saviour ZammitDocument12 pages2.0 Information Sources 2.1 Audio Signals: Dr. Ing. Saviour ZammitwarrengauciNo ratings yet
- Signal Processing For Auditory SystemsDocument108 pagesSignal Processing For Auditory SystemsKarthikeya SharmaNo ratings yet
- Dr. Ashman's ENT Notes PDFDocument56 pagesDr. Ashman's ENT Notes PDFJulian GordonNo ratings yet
- Mechanism of HearingDocument203 pagesMechanism of HearingMythily VedhagiriNo ratings yet
- Tuning Fork TestsDocument3 pagesTuning Fork TestsClarissa YudakusumaNo ratings yet
- Assessment and Management of Patients With Hearing and Balance DisordersDocument9 pagesAssessment and Management of Patients With Hearing and Balance Disordersxhemhae100% (1)
- Otic Preparations: Compounding & Manufacturing II Presentation of Luisabel NoveloDocument10 pagesOtic Preparations: Compounding & Manufacturing II Presentation of Luisabel NoveloNitin SharmaNo ratings yet
- Vestibular Appratus: BY: Harshita YadavDocument49 pagesVestibular Appratus: BY: Harshita YadavNitin SharmaNo ratings yet
- Complication of Neck Dissection & Its Management.: Dr. Sanjay Maharjan 1 Yr Resident, Ent-Hns, MTH, PokharaDocument37 pagesComplication of Neck Dissection & Its Management.: Dr. Sanjay Maharjan 1 Yr Resident, Ent-Hns, MTH, PokharaNitin SharmaNo ratings yet
- Deep Cervical Fascia - Investing Layer - Prevertebral Layer - Pretracheal Layer - Carotid Sheath - AnatomyQADocument9 pagesDeep Cervical Fascia - Investing Layer - Prevertebral Layer - Pretracheal Layer - Carotid Sheath - AnatomyQANitin SharmaNo ratings yet
- ENT EXAMINATIONGOOD-instrumentspdfDocument38 pagesENT EXAMINATIONGOOD-instrumentspdfNitin SharmaNo ratings yet
- Assessment of HearingDocument30 pagesAssessment of HearingNitin SharmaNo ratings yet
- Otorhinolaryngology (Ent) Dec11Document4 pagesOtorhinolaryngology (Ent) Dec11Nitin SharmaNo ratings yet
- Pta SymbolsDocument1 pagePta SymbolsNitin SharmaNo ratings yet
- Diseasesofexternalear 1Document86 pagesDiseasesofexternalear 1Nitin Sharma100% (1)
- DD of Hearing LossDocument1 pageDD of Hearing LossNitin SharmaNo ratings yet
- Grbas ScaleDocument1 pageGrbas ScaleNitin SharmaNo ratings yet
- Anatomy of Paranasal SinusesDocument49 pagesAnatomy of Paranasal SinusesNitin SharmaNo ratings yet
- Endoscopic Sinus Surgery ConsentDocument3 pagesEndoscopic Sinus Surgery ConsentNitin SharmaNo ratings yet
- Sty ConsentDocument3 pagesSty ConsentNitin SharmaNo ratings yet
- Assessment of The Pediatric PatientDocument7 pagesAssessment of The Pediatric Patienttantalizin marieNo ratings yet
- Human ReproductionDocument16 pagesHuman ReproductionNajeela khaleelNo ratings yet
- Homonymous Hemianopia - UpToDateDocument6 pagesHomonymous Hemianopia - UpToDateSonali GuptaNo ratings yet
- DONGEN Hugo Robert VanDocument116 pagesDONGEN Hugo Robert Vanayuk prihatinNo ratings yet
- Department of Education: Semi-Detailed Lesson Plan in Advanced BiologyDocument11 pagesDepartment of Education: Semi-Detailed Lesson Plan in Advanced BiologysydleorNo ratings yet
- Acute Epiglottitis (Syn. Supraglottic Laryngitis)Document4 pagesAcute Epiglottitis (Syn. Supraglottic Laryngitis)mahmoud azmyNo ratings yet
- AnalgesicDocument47 pagesAnalgesicMOHAMAD ZULFIKRIE ABASNo ratings yet
- Chapter30 NecropsyMethodsandProceduresDocument9 pagesChapter30 NecropsyMethodsandProceduresFernanda MenezesNo ratings yet
- Test 1 All NotesDocument41 pagesTest 1 All NotesLizethNo ratings yet
- Screenshot 2023-03-07 at 8.07.32 PM PDFDocument52 pagesScreenshot 2023-03-07 at 8.07.32 PM PDFirfanNo ratings yet
- Sibs With Anencephaly, Anophthalmia, Clefts, Omphalocele, and Polydactyly: Hydrolethalus orDocument4 pagesSibs With Anencephaly, Anophthalmia, Clefts, Omphalocele, and Polydactyly: Hydrolethalus orSarly FebrianaNo ratings yet
- Anatomy and PhysiologyDocument4 pagesAnatomy and PhysiologyMhica B. PrestozaNo ratings yet
- OSCE Cerebellar Examination PDFDocument6 pagesOSCE Cerebellar Examination PDFriczen vilaNo ratings yet
- SAS - Session 7 - PSY079 - Intro To PsychologyDocument8 pagesSAS - Session 7 - PSY079 - Intro To PsychologyLordelee Mae N PamaylaonNo ratings yet
- DR Fadel Naim Ass. Prof. Faculty of Medicine IUGDocument65 pagesDR Fadel Naim Ass. Prof. Faculty of Medicine IUGأمال داودNo ratings yet
- Embryolog Y By: Dr. Thaaer Mohammed Daher Alsaad M.B.Ch.B. (MBBS) F.I.B.M.S. (PHD) Senior Lecturer ISM MSUDocument97 pagesEmbryolog Y By: Dr. Thaaer Mohammed Daher Alsaad M.B.Ch.B. (MBBS) F.I.B.M.S. (PHD) Senior Lecturer ISM MSUSandipan MandalNo ratings yet
- Case Study CHF Final Output Group 2Document83 pagesCase Study CHF Final Output Group 2SHEILA MAE SACLOTNo ratings yet
- Cytokines, Inflammation and PainDocument13 pagesCytokines, Inflammation and PainFitriNo ratings yet
- AntitumoralesDocument19 pagesAntitumoralesMaira BianchiniNo ratings yet
- Hydrocephalus AND Spina Bifida: MR - Sachin T.Gadade M.SC (N) PediatricsDocument61 pagesHydrocephalus AND Spina Bifida: MR - Sachin T.Gadade M.SC (N) PediatricsAbdirahman Abdillahi FarahNo ratings yet
- Quiz 1 - 4Document32 pagesQuiz 1 - 4Akash PatelNo ratings yet
- Update On Neuroimaging For Categorization of Parkinson's Disease and Atypical ParkinsonismDocument11 pagesUpdate On Neuroimaging For Categorization of Parkinson's Disease and Atypical ParkinsonismYo MismoNo ratings yet
- Report On "Neuropsychoanalysis Around The World," An Online Meeting Hosted by The International Neuropsychoanalysis Society, July 2020Document12 pagesReport On "Neuropsychoanalysis Around The World," An Online Meeting Hosted by The International Neuropsychoanalysis Society, July 2020Lucas CarroNo ratings yet
- Nursing CS Endocrine SystemDocument1 pageNursing CS Endocrine SystemLia neNo ratings yet
- MorphogenesisDocument25 pagesMorphogenesisDrAbhilasha SharmaNo ratings yet
- Medicine Viva Notes by Dr. VaidyaDocument57 pagesMedicine Viva Notes by Dr. VaidyaFariha AnsariNo ratings yet
- Socio-Psycholinguistics (June 2021)Document5 pagesSocio-Psycholinguistics (June 2021)Gul HassanNo ratings yet
- Core CH 15 Detecting The EnvironmentDocument9 pagesCore CH 15 Detecting The EnvironmentKa yan SoNo ratings yet