Professional Documents
Culture Documents
2007 Mordohai Factors That Affect Individual Tooth Prognosis and Choices in Contemporary Treatment Planning British Dental Journal
Uploaded by
player osamaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
2007 Mordohai Factors That Affect Individual Tooth Prognosis and Choices in Contemporary Treatment Planning British Dental Journal
Uploaded by
player osamaCopyright:
Available Formats
IN BRIEF
PRACTICE
• Attaining an accurate prognosis of periodontally involved teeth is problematic.
• The reporting of success rates in endodontic literature is confused by the definition of
‘success/failure’.
• Heroic attempts to maintain teeth with poor prognosis should be questioned. Implants
should not be ‘the last resort’ and only used when all conventional therapies have failed.
15
Factors that affect individual tooth prognosis and
choices in contemporary treatment planning
N. Mordohai,1 M. Reshad,2 S. Jivraj3 and W. Chee4
A clinician evaluates a tooth for its quality of health. Once accomplished an estimate of longevity and survival is estimated.
With current knowledge about the survival and success of implants a decision is made as to whether to extract or to treat
and maintain the tooth. Questions and doubts abound in the decision making process in regards to the prognosis of an
individual tooth. Unfortunately in dentistry, as in all biologic sciences, there are no straightforward answers to questions. This
article will attempt to review the literature in this area to aid the practitioner in the decision making process with regards to
the compromised tooth. The article will focus on the single tooth or implant restoration. Other factors such as the strategic
value of a tooth and financial limitations in relation to long-term prognosis will also be discussed.
IMPLANTS INTRODUCTION has to be given to prognosis from both a peri-
1. Rationale for dental implants
Periodontally involved teeth receive multiple odontal and an endodontic perspective. Thera-
therapeutic procedures to arrest the disease, peutic decisions need to be made based on this
2. Treatment planning of implants in
posterior quadrants prevent attachment loss and possibly gain prognosis so that success in the long term can
some attachment. Non-surgical and surgical be achieved.
3. Treatment planning of implants in
the aesthetic zone endodontic therapy is performed on teeth with
4. Surgical guidelines for dental
necrotic pulps to seal the tooth or re-seal the Prognosis of periodontally involved teeth
implant placement ‘already sealed’ root canal. On occasion a given Attaining an accurate prognosis of periodon-
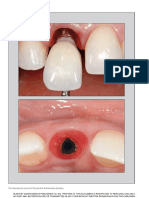
5. Immediate implant placement: tooth may require both periodontal and endo- tally involved teeth is problematic. Hirschfeld
treatment planning and surgical steps dontic procedures followed by restoration to and Wasserman re-examined over 15,000 teeth
for successful outcomes form and function. Today implant dentistry has in 600 patients with advanced periodontitis,
6. Treatment planning of the shifted the treatment planning paradigm; ques- at least 15 years after receiving treatment. The
edentulous maxilla
tionable teeth may be extracted more frequently patients were generally well motivated in their
7. Treatment planning of the in favour of implant placement. ‘Herodontics’ is personal and professional dental care. They also
edentulous mandible
discouraged when the prognosis is poor or fail- had similar periodontal involvement at the onset
8. Impressions techniques for implant ure of treatment may result in inadequate bone and received the same treatment. However, the
dentistry
for implant placement. Considerable thought patients differed markedly in post-treatment
9. Screw versus cemented implant
supported restorations course, with tooth loss ranging from zero to 23
teeth per patient.1 In other words, it is almost
10. Designing abutments for 1,*2Resident Advanced Prosthodontics, USC School of Dentistry,
cement retained implant supported impossible to predict the chance of survival of a
restorations 925 West 34th St, Rm 116, Los Angeles, CA 90089, USA; periodontally compromised tooth.
3Chairman, Section of Fixed Prosthodontics and Operative
11. Connecting implants to teeth Dentistry, University of Southern California School of Dentistry In an attempt to establish clinical parameters
12. Transitioning a patient from teeth / Private Prosthodontics Practitioner, Burbank, California, that would lead to consistently correct prog-
to implants USA; 4Ralph W. and Jean L. Bleak Professor of Restorative noses, McGuire and Nunn published a series of
Dentistry, Director of Implant Dentistry at the University of
13. The role of orthodontics in implant Southern California School of Dentistry / Private Prosthodontics papers. All articles were based on 100 patients
dentistry Practitioner, Pasadena, California, USA with 2,509 teeth under maintenance care for up
14. Interdisciplinary approach to *Correspondence to: Dr Nikitas Mordohai, 73 Ermou Street, to 15 years. It became obvious that ‘projections
implant dentistry Thessaloniki, 54623, Greece
Email: nmordohai@hotmail.com
relying on the commonly taught clinical param-
15. Factors that affect individual eters were ineffective in predicting any outcome
tooth prognosis and choices in other than good’.2 Although the regression
contemporary treatment planning Refereed Paper
© British Dental Journal 2007; 202: 63-72 model formulated predicted accurately 81% of
16. Maintenance and failures
DOI: 10.1038/bdj.2007.23 the time, its accuracy dropped to approximately
BRITISH DENTAL JOURNAL VOLUME 202 NO. 2 JAN 27 2007 63
PRACTICE
Fig. 1 Status before periodontal
treatment reveals mild to moderate
involvement of the incisors.
Fig. 2 Three-year post-operatively
there is evidence of advanced
periodontal destruction.
Fig. 3 Horizontal and vertical root
fractures of mandibular lateral incisor
40% when applied to teeth with an initial prog-
that was endodontically treated and nosis of less than good.3 The same applies to the
restored with a cast dowel. interleukin-1 (IL-1) status of the patient, where
only little correlation existed between clinical
presentation of the tooth (initial prognosis) and
genotype status.4 McGuire and Nunn observed
that substantially greater percentages of teeth
lost had a poor or worse prognosis than surviv-
ing teeth. But the disturbing observation was
that there was great variability in survival time
for teeth lost. For example, teeth lost with an
initial prognosis of good had a survival range
of four months to 12 years. Clearly, initial prog-
nosis did not adequately predict tooth survival5
and especially for posterior teeth, ‘projections
were no more predictable than a coin toss’.2
On the other hand, there is evidence to sup-
port the efficacy of some clinical criteria in
deciding whether to extract or maintain a tooth.
Increasing probing depth, furcation involve-
ment, mobility, percentage of bone loss, hav-
ing a parafunctional habit and not wearing
Fig. 4 Maxillary first bicuspids
are also prone to vertical fractures
an occlusal splint and smoking resulted in an
especially if restored with wide- increased risk of tooth loss.5 Lang et al. found a
diameter dowels. highly significant relationship between increas-
ing probing depth and increasing bleeding on
probing (BOP) incidence and also a highly sig-
nificant relationship between an increasing
BOP and loss of probing attachment. Specifi-
cally, absence of BOP showed an almost 0% risk
for periodontal breakdown, while pockets that
constantly bled during follow-up appointments
had a 30% risk for losing probing attachment.
Although this number is still low, BOP still rep-
resents the most reliable clinical predictor for
disease ‘activity’ during periodontal mainte-
nance.6 Wasserman et al. confirmed the limited
importance of BOP. Patients with periodontal
breakdown had gingival inflammation more
often than patients without breakdown. How-
ever, the teeth with the most inflammation did
not necessarily correspond with the teeth with
64 BRITISH DENTAL JOURNAL VOLUME 202 NO. 2 JAN 27 2007
PRACTICE
the most severe breakdown.7 Fig. 5 Implant supported crown
The smoking habit and the IL-1 genotype of number 7 that presents with aesthetic
problems. It is too long and metal
the patients seemed useful in predicting future display is evident in the cervical area.
risk for disease progress. Patients who smoked or
were positive for IL-1 had a threefold increased
risk of losing their teeth. Patients who were IL-1
positive and heavy smokers were nearly eight
times more likely to lose teeth.4
Success rates of periodontal therapy
The results of most studies on the effectiveness
Fig. 6 Harmonious aesthetics can be
of periodontal therapy are encouraging. Hir- achieved with implant restorations in
schfeld and Wasserman found that 7.1% of the region of tooth number 10.
teeth were lost for periodontal reasons. Fifty per
cent of the patients did not lose any teeth over a
period of 22 years.1 McFall, in a duplicate study,
had very similar results.8 Becker et al. showed
comparable failure rates. When the teeth with
an initial hopeless prognosis were excluded, the
failure rate dropped by half (2.94%).9
Even the tooth type has been shown to be
a factor in the survival of the tooth.1,8,9 The
Fig. 7 Single crown on an implant
tooth loss pattern was almost identical in Hir- replacing number 5, seven years post-
schfeld, Wasserman and McFall’s studies. operatively.
Maxillary molars were the teeth that are most
likely to be lost, followed closely by mandibular
molars. The maxillary and mandibular canines
were the teeth most resistant to periodontal
breakdown.1,8,9
McGuire concluded that it is easier to pre-
dict the prognosis for single-rooted teeth.2 Most
studies seem to agree that anterior teeth respond
better to periodontal treatment and are less like-
ly to be lost due to periodontal reasons. None of
Fig. 8 Poor oral hygiene habits can be
the canines were lost in a well maintained pop- detrimental regardless of the level of
ulation after 22 years of follow-up.1 Maxillary treatment provided and this will be
molars, on the other hand, had the worst prog- the overriding factor when treatment
nosis.1,8 Ramfjord et al. found that the response planning.
of anterior teeth to periodontal treatment was
marginally better than posterior teeth. The
poorest results occurred for the maxillary bicus-
pids and molars, which may in part be related
to furcation involvement10 and the time of the
disease onset. In patients with mild periodonti-
tis, the molar teeth were four times more likely
to be affected than all other teeth combined.7
Fig. 9 Cross-arch splinting
In patients with more advanced disease, 85% of reconstruction due to periodontal
the molar teeth presented with severe destruc- disease.
tion.7 It follows that molars are ‘problem teeth’
and the efficacy of different types of treatment
must be explored.
Success rates of surgical and non-surgical
therapy on molars
In the treatment of molar teeth there are vari-
ous aspects that have to be investigated in order
to evaluate the effectiveness of therapy. Teeth
with and without furcation involvement have
to be studied separately. Additionally, there
Fig. 10 Full mouth radiographs reveal
are different therapeutic approaches for fur- caries on teeth number 7 and 12 and
cated molars. The treatment modalities include very small roots.
either preservation of the furca and strict main-
tenance or elimination of it by root amputation
and hemisection.
Absence of furcation involvement The
treatment outcome even in the absence of
BRITISH DENTAL JOURNAL VOLUME 202 NO. 2 JAN 27 2007 65
PRACTICE
Fig. 11 Implants were placed. The furcation involvement is problematic. However,
central incisors and first molars the results are far more favourable compared to
support a metal-reinforced fixed
provisional restoration.
teeth with destruction in the furca. Sixty-four
per cent of non-furcated teeth with a question-
able prognosis were lost over a course of 19
years.8 When 323 molar teeth without furca
invasion were followed for 6.5 years, 78%
remained unchanged while the remaining 22%
developed a furcation problem.9
Presence of furcation involvement with-
out root resection or amputation Wang et al.
concluded that in the presence of furcation
Fig. 12 CT scan cuts of right and left
first molar areas showing insufficient
involvement, teeth were twice as likely to be
bone volume to house implants. lost.11 Kalkwarf et al. observed that furcation
sites tended to lose probing attachment levels
regardless of the type of therapy provided. This
may be a result of the inability to adequately
instrument these areas during therapy.12
Without any root resection or hemisection
procedure performed, Hirschfeld and Wasser-
man reported loss of nearly one third of the
Fig. 13 Tooth number 5 has a large
diameter post, periapical radiolucency
teeth originally diagnosed as having furcation
and needs a new crown. invasion.1 McFall found that more than half of
furca involved teeth were lost when followed
from 15 to 29 years.8
Conversely, Ross and Thompson reported
acceptable results with non-surgical interven-
tion of maxillary molars with furcation involve-
ment. After five to 24 years, 88% of the teeth
were still functioning comfortably. However,
the significance of these results is limited when
one considers that an additional 11% showed
increased bone loss and that the diagnosis of
all furcations was done solely on radiographs.13
Fig. 14 Implant-supported fixed
partial denture on implants numbers
Becker et al. published very similar results with
4 and 6. the status of 86% of furcated molars remain-
ing stable. Their conclusion was that teeth with
moderate furcation involvement can be treated
successfully and maintained effectively for pro-
longed periods.9
Furcation involved teeth receiving root
resection or amputation Unfortunately, most
studies of surgical intervention with root resec-
tion or hemisection do not present very prom-
ising results either. Langer et al. evaluated 100
patients receiving root resection therapy at least
Fig. 15 Failing endodontic therapy.
10 years prior to the study. Thirty-eight per cent
of these teeth failed, the majority occurring
between the fifth and seventh year. Mandibular
molars failed at a 2:1 ratio compared to maxil-
lary molars. The latter failed primarily because
of progressive periodontal disease, while man-
dibular molars succumbed most frequently to
root fractures.14 Blomlöf et al. reported a very
similar success rate of 68% at 10 years. Smok-
ers seemed to have a threefold risk compared to
non-smokers.15
A study which illustrated more promising
results was conducted by Carnevale et al. They
examined 488 hemisected or root resected teeth.
The possible failure mode could have been peri-
odontal, endodontic or restorative. The failure
rate was 5.7% and only 3.7% of all the teeth
had to be extracted. The highest cause of fail-
ure was dental caries and root fractures, but
not periodontal disease. However, since this is a
66 BRITISH DENTAL JOURNAL VOLUME 202 NO. 2 JAN 27 2007
PRACTICE
retrospective study, the number of furcated teeth Fig. 16 The endodontist decided to
that were initially extracted is not reported and perform apical surgery and retrograde
root filling.
thus conclusions about the efficacy of surgical
treatment of the furcated teeth should be made
with extreme caution. The authors explained the
higher success rates compared to other studies
by the fact that resection therapy is very tech-
nique-sensitive and proper case selection and
restorative expertise are essential.16
Importance of regular maintenance
One aspect that all authors emphasise is the
necessity for frequent recall appointments. The
high success rates of Carnevale et al. are cou-
pled with a three-month recall for 95% of his
patients.16 A frequency of three to four appoint-
ments per year is advocated for the periodon-
tally involved patients.1,2,8,9
Achieving a proper maintenance program is
not an easy task. Although the recall appoint-
ments were sent every three to four months,
patients attended every 5.2 months. Addition-
ally, by the seventh year after treatment, there
Fig. 17 Second apical surgery and
was a 22.1% drop-out rate.9 retrograde root filling.
Becker et al. reported that in a well-main-
tained population after 6.5 years, the annual
tooth loss was 0.11 teeth per patient.9 The
authors also examined another group of patients
who did not return for recall for five years.
Receiving treatment without maintenance had
a negligible effect on reducing probing depths
and 25% of shallow pockets became deeper.
There was worsening of the furcation areas and
statistically significant bone loss. Finally, the
mean annual tooth loss doubled, reaching 0.22
teeth per patient.17
Conclusion on periodontally involved teeth
It is evident that, with the tools available today,
accurate prognosis of periodontally involved
teeth is unreliable. There are some guidelines
that have prognostic value, but they should be
used with caution. Survival rates of anterior
teeth exceed that of posterior teeth. It follows
that anterior teeth can be maintained with lower
Fig. 18 Third apical surgery and
risk. However, in rare circumstances, even teeth retrograde root filling. Despite the
with excellent periodontal status show rapid endodontist’s effort, the tooth was
degradation (Figs 1 and 2). It is the multifacto- still symptomatic.
rial nature of the disease that makes prognosis
and sometimes preservation of the teeth unpre-
dictable.
Success rates of non-surgical endodontic
therapy
When a tooth is fractured, grossly carious or
traumatised, the choice for a patient may be
either endodontic therapy or loss of the tooth.
It is important for the patient and dental profes-
sion to be able to decide on a course of treat-
ment through knowledge of potential success of
various treatment modalities.
In a classical study on rats, Kakehashi et al.
showed that in the absence of bacteria, complete
healing of exposed dental pulps occurred.18 Sjö-
gren et al. showed that when there was a peri-
apical lesion present, endodontic success rates
BRITISH DENTAL JOURNAL VOLUME 202 NO. 2 JAN 27 2007 67
PRACTICE
Fig. 19 After the third surgery failed, dropped by at least 10%.19 They also showed
the tooth was extracted. Remnants that an initial negative culture resulted in a 94%
of the retrograde root filling can be
observed on the radiograph.
endodontic success rate, while an initial positive
culture resulted in significantly reduced success
rates (68%).20 Fouad et al. demonstrated that ‘…
in cases with preoperative periradicular lesions,
a history of diabetes was associated with a signif-
icantly reduced outcome’.21 The data suggest that
patients who are diabetic and have an infected
root canal may have a significantly reduced
chance of healing from an endodontic infection.
Eriksen et al. showed that endodontic spe-
cialists achieve higher success rates when com-
pared to general practitioners. They also showed
that endodontic success rates varied between
54-94%.22 In an investigation of nearly 2,500
teeth, Jonkinen et al. showed that success rates
for endodontic therapy may be as low as 53%.23
However, in this study the protocol for endo-
dontic therapy differed from what is currently
accepted as the norm. This may have had a neg-
Fig. 20 A fifth surgical procedure
was necessary to remove the
ative influence on the success rates.
remnants. The real cause for confusion in survival stud-
ies seems to be the way in which the term ‘suc-
cess’ is defined. If a study has strict criteria for
success, the results are negatively affected. On
the other hand, if the criteria are less strict, the
success rates may be positively affected.
The reporting of success rates in endodontic
literature can be confused by the definition of
‘success/failure, the time period that the out-
come was measured over, the type of endodon-
tic procedure and the unit of measurement.
Much of the literature-cited success rates are
dependent on resolution of the periodontal liga-
ment space with radiographic findings alone
and clinical symptoms are not considered.24-26
Furthermore, study periods are often not ade-
quate to allow classification of teeth displaying
a reduction in periapical radiolucency. Incom-
plete radiographic resolution and success rates
from the longest period of follow-up are extrap-
olated to that of the mean period; measurement
Fig. 21 The root length was
favourable and a narrow diameter
of success is based on roots rather than teeth or
for the dowel was intentionally has not included teeth extracted.19,24
maintained. Friedman and Mor in 2004 defined success
as root canal treatment that ‘has healed’ or ‘is
healing’. They also proposed a new classifica-
tion: ‘functional retention’. Functional retention
is the sum of the healed and the healing sites.
They also suggest that functional retention
includes a tooth with a normal clinical presen-
tation, where radiolucency is present or absent,
newly emerged or persisting.27 In the opinion of
the authors, although functional retention may
Fig. 22 This tooth received root canal
therapy, crown lengthening, cast
result in higher apparent success rates, it may
dowel and core and a new crown. not lead to a predictable endodontic outcome.
Functional retention is a loose criterion for
assessment of endodontic success and may mis-
lead the reader into believing that success rates
are actually higher than they really are.
Success rates of surgical endodontic therapy
Friedman and Mor pooled data from selected
studies and showed that the chance of success
based on selected studies ranged from 37-85%
68 BRITISH DENTAL JOURNAL VOLUME 202 NO. 2 JAN 27 2007
PRACTICE
with an average of 70%. The chance of func- Fig. 23 This tooth requires endodontic
tionality for surgical endodontic procedures re-treatment, crown lengthening,
dowel and core and a crown. It was
was 86-92%.27 Again, functionality increases decided to extract the tooth as the
the numerical value for success rate of surgical patient was a bruxer and the root had
endodontics. But one needs to decide whether unfavourable anatomy.
a functional tooth will result in a predictable
outcome.
Restorability of endodontically treated teeth
Another important issue is the restorability of
endodontically treated teeth. Even if a tooth
has been successfully treated with endodontics,
one still needs to consider the restoration of the
Fig. 24 Advanced periodontal
tooth. Goodacre et al. in a meta-analysis showed disease. The treatment of choice was
that in 12 studies with 2,784 teeth and a six- extraction and implant placement.
year follow-up, 12% of teeth with dowels had
complications.28 Many of these complications
may lead to tooth loss (Figs 3-4). So, the practi-
tioner needs to objectively assess the restorabil-
ity of each endodontically treated tooth prior to
commencement of treatment. The predictability
of the treatment provided will be of benefit both
to the patient and dentist.
Success rates of dental implants
In an attempt to objectively quantify success
with regards to dental implants and their res-
Fig. 25 This patient has implant
torations, many criteria have been defined. The supported restorations in the maxillary
implants should have a minimum of one year of left and mandibular posterior
loading, as most implant failures are detected quadrants. Note failing natural
in the first year of service.29,30 Implant failures dentition.
should also be defined. It is suggested that if an
implant can not be used as support for prosthetic
reconstruction, it should be labelled a ‘sleeping
implant’. These are labelled surviving implants
at best, as they are not usable.31 Lindh et al. sug-
gested that these should really be classed as fail-
ures. If sleeping implants are osseointegrated,
they should be regarded as ‘functional failures’
because they are unrestorable.31
Smith and Zarb have suggested that the aes-
Fig. 26 Panoramic radiograph of
thetic aspect of the implant position should also patient in Figure 25.
be incorporated as factors for a successful result.32
In another meta-analysis Goodacre et al. showed
that 47 out of 493 crowns/prostheses produced
aesthetic problems. They found that aesthetic fail-
ures had a mean of 10%3 (Figs 5 and 6).
Gibbard and Zarb stated that ‘Long-term
success for multiple splinted implants can-
not be extrapolated to single implants’.33 In
a meta-analysis of 66 studies over 10 years,
Lindh et al. included 2,686 dental implants, and
evaluated 570 single crowns and 2,116 implant
fixed partial dentures in partially edentulous
Fig. 27 Same patient as in Figure 25.
jaws. ‘…Although the cumulative survival rate Natural dentition in maxilla has failed.
will decrease if ‘sleeping implants’ are consid- Due to patient health additional
ered as failed, the maximum difference is only implants could not be placed. A
3.7%...’ Implant survival under load after six maxillary denture was fabricated
to seven years was 93.6% for fixed partial den- which was implant retained and
mucosa supported.
tures and 97.5% for single crowns27 (Fig. 7). The
data from the Lindh et al.31 study suggest that
implants and their restorations work extremely
predictably for single teeth or fixed partial den-
tures. It also shows that even with strict inclu-
sion criteria these restorations have excellent
success rates.
BRITISH DENTAL JOURNAL VOLUME 202 NO. 2 JAN 27 2007 69
PRACTICE
Fig. 28 Maxillary denture with the concept of trying to save the tooth by all
Vitallium Palate. means necessary. However, with the inception
of dental implants a completely new avenue has
been opened in the treatment planning proc-
ess. This has created a new topic for debate
within the profession. There appears to be two
schools of thought. One school is advocating the
traditional approach, while the other has adopt-
ed a more aggressive approach with treatment
planning and prefers to extract and replace a
compromised tooth with a dental implant and
restoration.
It is imperative to understand that each
Fig. 29 Panoramic radiograph
showing single implant placement
therapeutic modality has an inherent biologi-
in mandible. Remaining mandibular cal cost. Therefore, a risk analysis should be ini-
teeth are failing. tiated prior to any definitive decisions. In the
authors’ opinion a very stringent approach is
required during this analysis. A treatment with
a poor risk-to-benefit ratio has a greater prob-
ability of biological consequences. In treatment
planning, DeVan’s statement should always be
a cornerstone in the dentist’s mind: ‘…our goal
should be the preservation of what remains
rather than the meticulous restoration of what
Fig. 30 Mandibular teeth have failed
additional implants have been placed.
is missing’.34
Nyman and Lindhe have shown excellent
results with the prosthetic rehabilitation of
patients with advanced periodontal disease with
very few prosthetic complications.35 Figure
9 illustrates a patient that received full mouth
reconstruction in the maxilla due to moderate
periodontal disease. After 25 years the osseous
support did not show significant changes with
regular periodontal maintenance (Fig. 10). Nev-
ertheless, the patient’s medical status changed
and the salivary flow decreased significantly.
Fig. 31 Same patient as in Figures
29-30. There are sufficient implants
The result was caries development on two abut-
placed for a fully implant supported ment teeth (Fig. 10). Considering the medical
restoration history along with the success rates of different
treatment modalities, it was decided to extract
most of the maxillary teeth and place implants
(Fig. 11). Under no circumstances can the pre-
vious periodontal-prosthetic rehabilitation be
considered a failure after 25 years of survival.
An implant-supported restoration was cho-
sen over a tooth-borne cross-arch splint. This
decision was based on the obvious risk associ-
ated with joining numerous teeth in a medically
DISCUSSION compromised patient.
Unfortunately, there are no rules or formulae in The strategic value of the tooth must also be
dentistry that provide straightforward answers. assessed. In the patient shown in Figure 11, the
The practitioner needs to use the knowledge most distal molars were maintained. Extrac-
from the literature along with common sense to tions would have resulted in sinus lifting pro-
derive a treatment plan. The picture is further cedures, which the patient wished to avoid (Fig.
complicated by a multitude of local, systemic 12). Although the teeth had a guarded progno-
and even psychological factors. The patient’s sis, their value as two additional occluding units
medical conditions, the general condition of contradicted their removal. Figure 13 shows
the oral environment and certainly the patient’s tooth number 5 that has a large cast dowel
motivation towards the treatment will influence and needs endodontic re-treatment and a new
the overall success (Fig. 8). Thus, the actual lon- crown. Implants are planned for the mesial and
gevity of a specific treatment modality cannot distal edentulous sites, while the existing teeth
be applied to all patients indiscriminately. on the mesial and distalsites do not need res-
Considering all these parameters, the clini- torations or replacement of restorations. Due to
cian is often faced with a dilemma when decid- the risk involved and the low strategic value of
ing whether or not to extract a tooth with a poor the tooth, a three-unit implant-supported fixed
prognosis. Traditional wisdom was based upon partial denture was fabricated (Fig. 14). It can
70 BRITISH DENTAL JOURNAL VOLUME 202 NO. 2 JAN 27 2007
PRACTICE
be deducted that teeth with higher strategic acquainted with the use of implants in restora-
value will be amenable to more extensive pro- tive dentistry, implants should not be ‘the last
cedures than teeth in less important positions in resort’ and only used when all conventional
the arch. therapies have failed. There is sufficient docu-
mentation today to indicate the use of implants
Clinical recommendations and conclusions as the first choice of treatment in many situ-
Implant placement and restoration is not a ations. With this knowledge the fine line of
technically-demanding procedure.36,37 From whether to maintain a tooth or to replace it with
the results available today, which are based on an implant supported restoration must be made.
follow up studies, it seems that tooth replace- With knowledge of the literature regarding suc-
ment with dental implants is more predictable cess rates of therapies and survival rates of res-
than surgical periodontal and endodontic torations, the clinician has the responsibility
techniques (Figs 15-20). This however should to help patients make the choice. A risk benefit
not automatically preclude these therapeutic and a cost benefit analysis should be carried out
modalities and lead to extraction of the affected each time.
teeth. It does justify, though, a relatively more
aggressive approach, especially in younger The authors would like to thank the Journal of the
California Dental Association for permission to reprint
patients where a significantly long-term prog- parts of this article which were initially published in the
nosis is required. JCDA April 2005 issue.
One needs to decide on the most predictable
strategy for restoring a severely broken-down 1. Hirschfeld A, Wasserman B. A long-term survey of tooth loss
in 600 treated periodontal patients. J Periodontol 1978;
tooth. This may involve the combination of 49: 225-237.
endodontic, periodontal and restorative pro- 2. McGuire M K. Prognosis versus actual outcome: a long-
cedures, in order to save a tooth (Figs 21-22). term survey of 100 treated periodontal patients under
On the other hand, what has been considered maintenance care. J Periodontol 1991; 62: 51-58.
3. McGuire M K, Nunn M E. Prognosis versus actual outcome.
successful prior to the inception of dental II. The effectiveness of clinical parameters in developing an
implants might not be acceptable today. If the accurate prognosis. J Periodontol 1996; 67: 658-665.
tooth has minimal coronal tooth tissue remain- 4. McGuire M K, Nunn M E. Prognosis versus actual outcome.
IV. The effectiveness of clinical parameters and IL-1
ing with unfavourable root structure or if mul- genotype in accurately predicting prognoses and tooth
tiple procedures need to be performed, one survival. J Periodontol 1999; 70: 49-56.
is justified in extracting the tooth in favour 5. McGuire M K, Nunn M E. Prognosis versus actual outcome.
III. The effectiveness of clinical parameters in accurately
of a dental implant (Fig. 23). Multiple proce- predicting tooth survival. J Periodontol 1996; 67: 66-74.
dures, even if independently low-risk, signifi- 6. Lang N P, Joss A, Orsanic T, Gusberti F A, Siegrist B E.
cantly increase the risk of failure. On the other Bleeding on probing. A predictor for the progression of
periodontal disease? J Clin Periodontol 1986; 13: 590-596.
hand, removal of all teeth that do not receive 7. Wasserman B H, Thompson R H Jr, Geiger A M. Relationship
a good prognosis is extremely aggressive and of occlusion and periodontal disease. II. Periodontal status
contraindicated. of the study population. J Periodontol 1971; 42: 371-378.
Heroic attempts to maintain teeth with poor 8. McFall W T Jr. Tooth loss in 100 treated patients with
periodontal disease. A long-term study. J Periodontol 1982;
prognosis should cease. Such attempts increase 53: 539-549.
the risk for failure, as well as the cost for the 9. Becker W, Berg L, Becker B E. The long term evaluation of
patient in the long run. They may also jeopard- periodontal treatment and maintenance in 95 patients.
Int J Periodontics Restorative Dent 1984; 4: 54-71.
ise future treatment outcomes. For example, as 10. Ramfjord S P, Knowles J W, Morrison E C, Burgett F G, Nissle
periodontal destruction progresses, the risk of R R. Results of periodontal therapy related to tooth type.
insufficient bone volume for implant placement J Periodontol 1980; 51: 270-273.
11. Wang H-L, Burgett F G, Shyr Y, Ramfjord S. The influence of
increases. Historically the teeth shown in Figure molar furcation involvement and mobility on future clinical
24 would be maintained until they would exfoli- periodontal attachment loss. J Periodontol 1994; 65: 25-29.
ate from the patient’s mouth. A more aggressive 12. Kalkwarf K L, Kaldahl W B, Patil K D. Evaluation of furcation
region response to periodontal therapy. J Periodontol 1988;
approach, nowadays, will save the patient from 59: 794-804.
the high morbidity and lower predictability of 13. Ross I F, Thompson R H. Long term study of root retention
bone grafting procedures. The authors believe in the treatment of maxillary molars with furcation
that the interpretation of the ‘…preservation of involvement. J Periodontol 1978; 49: 238-273.
14. Langer B, Stein S D, Wagenberg B. An evaluation of root
what remains’34 should be extended to the pre- resections. A ten-year study. J Periodontol 1981;
cious osseous structure of the ridges. 52: 719-722.
Another aspect to consider is that dental 15. Blomlöf L, Jansson L, Appelgren R, Ehnevid H, Lindskog S.
Prognosis and mortality of root-resected molars. Int
caries and periodontal disease do not affect J Periodontics Restorative Dent 1997; 17: 190-201.
implants as there is no calcified tissue and no 16. Carnevale G, Di Febo G, Tonelli M P, Marin C, Fuzzi M.
periodontium. Implants seem to withstand the A retrospective analysis of the periodontal-prosthetic
treatment of molars with interradicular lesions. Int
ravages of the oral cavity better than teeth J Periodontics Restorative Dent 1991; 11: 189-205.
do (Figs 25-28). Implant restorations can also 17. Becker W, Becker B E, Berg L E. Periodontal treatment
be planned for retrievability (Figs 29-31). As without maintenance. A retrospective study in 44 patients.
J Periodontol 1984; 55: 505-509.
teeth are lost, restorations can be modified and 18. Kakehashi S, Stanley H R, Fitzgerald R J. The effects
connected to additional implants. Long term of surgical exposures of dental pulps in germfree and
treatment planning to allow for retrievabil- conventional laboratory rats. J South Calif Dent Assoc 1966;
ity becomes important; once implants integrate 34: 449-451.
19. Sjogren U, Hagglund B, Sundqvist G, Wing K. Factors
they can be almost considered life-time anchor- affecting the long-term results of endodontic treatment.
age units. Clinicians today must become well J Endod 1990; 16: 498-504.
BRITISH DENTAL JOURNAL VOLUME 202 NO. 2 JAN 27 2007 71
PRACTICE
20. Sjogren U, Figdor D, Persson S, Sundqvist G. Influence 29. Goodacre C J, Kan J Y, Rungcharassaeng K. Clinical
of infection at the time of root filling on the outcome of complications of osseointegrated implants. J Prosthet Dent
endodontic treatment of teeth with apical periodontitis. Int 1999; 81: 537-552.
Endod J 1997; 30: 297-306. 30. Goodacre C J, Bernal G, Rungcharassaeng K, Kan J Y. Clinical
21. Fouad A F. Diabetes mellitus as a modulating factor of complications with implants and implant prostheses.
endodontic infections. J Dent Educ 2003; 67: 459-467. J Prosthet Dent 2003; 90: 121-132.
22. Eriksen H M. Endodontology — epidemiologic 31. Lindh T, Gunne J, Tillberg A, Molin M. A meta-analysis of
considerations. Endod Dent Traumatol 1991; 7: 189-195. implants in partial edentulism. Clin Oral Implants Res 1998;
23. Jokinen M A, Kotilainen R, Poikkeus P, Poikkeus R, Sarkki 9: 80-90.
L. Clinical and radiographic study of pulpectomy and root 32. Smith D E, Zarb G A. Criteria for success of osseointegrated
canal therapy. Scand J Dent Res 1978; 86: 366-373. endosseous implants. J Prosthet Dent 1989; 62: 567-570.
24. Morse D, Esposito J V, Pike C, Furst M L. A radiographic 33. Gibbard L L, Zarb G. A 5-year prospective study of implant-
evaluation of the periapical status of teeth treated by the supported single-tooth replacements. J Can Dent Assoc
gutta-percha-eucapercha method: a one-year follow-up 2002; 68: 110-116.
study of 458 root canals — Part III. Oral Surg 1983; 34. DeVan M M. Biological demands of complete dentures.
56: 190-197. J Am Dent Assoc 1952; 45: 524-527.
25. Seltzer S, Bender I B. Factors affecting successful repair after 35. Nyman S, Lindhe J. A longitudinal study of combined
root canal therapy. J Am Dent Assoc 1963; 67: 651-662. periodontal and prosthetic treatment of patients with
26. Heling I, Bialla-Shenkman S, Turetzky A, Horwitz J, Sela J. advanced periodontal disease. J Periodontol 1979;
The outcome of teeth with periapical periodontitis treated 50: 163-169.
with nonsurgical endodontic treatment: a computerized 36. Bell F A, Cavazos E J et al. Four-year experience with the
morphometric study. Quintessence Int 2001; 32: 397-400. placement, restoration, and maintenance of dental implants
27. Friedman S, Mor C. The success of endodontic therapy by dental students. Int J Oral Maxillofac Implants 1994;
— healing and functionality. J Calif Dent Assoc 2004; 9: 725-731.
32: 493-503. 37. Cummings J, Arbree N S. Prosthodontic treatment of
28. Goodacre C J, Bernal G, Rungcharassaeng K, Kan J Y. Clinical patients receiving implants by predoctoral students: five-
complications in fixed prosthodontics. J Prosthet Dent 2003; year follow-up with the IMZ system. J Prosthet Dent 1995;
90: 31-41. 74: 56-59.
72 BRITISH DENTAL JOURNAL VOLUME 202 NO. 2 JAN 27 2007
You might also like
- Periodontal ExaminationDocument40 pagesPeriodontal ExaminationEmad Hussien Haj-Abdulla100% (1)
- Diagnosis and treatment planning for fixed partial denturesDocument16 pagesDiagnosis and treatment planning for fixed partial dentureskaliapreetiNo ratings yet
- PEAK Restoration of The Endodontically Treated Tooth PDFDocument20 pagesPEAK Restoration of The Endodontically Treated Tooth PDFana9025100% (1)
- Managing Furcation InvolvementDocument123 pagesManaging Furcation InvolvementAishaNo ratings yet
- Accidental Root PerforationsDocument57 pagesAccidental Root PerforationsNajla MohammedNo ratings yet
- Furcation Involvement Diagnosis and Treatment FactorsDocument63 pagesFurcation Involvement Diagnosis and Treatment FactorsSamwel EmadNo ratings yet
- Treatment Planning Single Maxillary Anterior Implants for DentistsFrom EverandTreatment Planning Single Maxillary Anterior Implants for DentistsNo ratings yet
- Transitioning Patients From Teeth To ImplantsDocument11 pagesTransitioning Patients From Teeth To ImplantsAlexandra DumitracheNo ratings yet
- #1 Rationale ImplantDocument5 pages#1 Rationale Implantsohaib197No ratings yet
- "Facial Keys To Orthodontic Diagnosis and Treatment Planning Parts IDocument14 pages"Facial Keys To Orthodontic Diagnosis and Treatment Planning Parts ILeonardo Lamim80% (5)
- Decision Making For Tooth Extraction or ConservationDocument16 pagesDecision Making For Tooth Extraction or Conservationavi_sdc100% (1)
- Martinsdarosa 2014Document11 pagesMartinsdarosa 2014Michal Perkowski100% (1)
- Werm Ker 2014Document7 pagesWerm Ker 2014Alice EmailsNo ratings yet
- Periodontics PDFDocument195 pagesPeriodontics PDFدينا حسن نعمة100% (1)
- Pediatric Dental TraumaDocument11 pagesPediatric Dental TraumaDrBhawna AroraNo ratings yet
- Telescopic Overdenture: Perio Prostho Concern For Advanced PeriodontitisDocument4 pagesTelescopic Overdenture: Perio Prostho Concern For Advanced PeriodontitisrekabiNo ratings yet
- Periodontal Regenerative Therapy PDFDocument13 pagesPeriodontal Regenerative Therapy PDFRed Tiger50% (2)
- Failed Root Canals The Case For Extraction and Immediate Implant PlacementDocument3 pagesFailed Root Canals The Case For Extraction and Immediate Implant PlacementKarin Noga VerhagenNo ratings yet
- In The Dental Implant Era, Why Do We Still Bother Saving Teeth?Document8 pagesIn The Dental Implant Era, Why Do We Still Bother Saving Teeth?Gabriela ArgeseanuNo ratings yet
- Outcomes of mandibular Kennedy Class I and II prosthetic rehabilitationDocument7 pagesOutcomes of mandibular Kennedy Class I and II prosthetic rehabilitationsixnaagithaNo ratings yet
- Complete Denture Fabrication For Old Denture Wearer in One DayDocument3 pagesComplete Denture Fabrication For Old Denture Wearer in One DayAsma Akram - ProsthodonticsNo ratings yet
- Practice: Surgical Guidelines For Dental Implant PlacementDocument14 pagesPractice: Surgical Guidelines For Dental Implant PlacementAna94No ratings yet
- Endodoncia Vs ImplantesDocument8 pagesEndodoncia Vs ImplantesSebastián BernalNo ratings yet
- Altered Expectations On Dental Implant Therapy Views of Patients Referred For Treatment of Peri-ImplantitisDocument6 pagesAltered Expectations On Dental Implant Therapy Views of Patients Referred For Treatment of Peri-ImplantitisSantiago Durango HurtadoNo ratings yet
- 3 Badr2016Document22 pages3 Badr2016Daniel Espinoza EspinozaNo ratings yet
- Bilhan 2012Document7 pagesBilhan 2012laur112233No ratings yet
- Article - 1653239529 2Document5 pagesArticle - 1653239529 2Mega AzzahraNo ratings yet
- Success and Survival of Endodotically Treated Cracked Teeth With Radicular ExtensionsDocument8 pagesSuccess and Survival of Endodotically Treated Cracked Teeth With Radicular ExtensionsSayed RustiaNo ratings yet
- Unread - Int Endodontic J - 2022 - Murray - Review of Guidance For The Selection of Regenerative Endodontics ApexogenesisDocument12 pagesUnread - Int Endodontic J - 2022 - Murray - Review of Guidance For The Selection of Regenerative Endodontics ApexogenesisHien TruongNo ratings yet
- Outcomes and Prognostic Factors That Influence The SuccessDocument20 pagesOutcomes and Prognostic Factors That Influence The SuccessdwNo ratings yet
- Surgical Guidelines For Dental Implant Placement: British Dental Journal September 2006Document15 pagesSurgical Guidelines For Dental Implant Placement: British Dental Journal September 2006Louis HutahaeanNo ratings yet
- Kindelan 2008Document11 pagesKindelan 2008DIANA PAOLA FONTECHA GONZÁLEZNo ratings yet
- Prosthetic Rehabilitation and Treatment Outcome of Partially Edentulous Patients With Severe Tooth Wear: 3-Years ResultsDocument21 pagesProsthetic Rehabilitation and Treatment Outcome of Partially Edentulous Patients With Severe Tooth Wear: 3-Years ResultsAlina AlinaNo ratings yet
- Crown Lengthening Vs Forced EruptionDocument4 pagesCrown Lengthening Vs Forced EruptionbarbieNo ratings yet
- Int Endodontic J - 2022 - Fransson - Tooth Survival After Endodontic TreatmentDocument14 pagesInt Endodontic J - 2022 - Fransson - Tooth Survival After Endodontic TreatmentkecasweatNo ratings yet
- Post Removal Techniques Part 1: DentistryDocument7 pagesPost Removal Techniques Part 1: DentistryYessenia SarabiaNo ratings yet
- The Role of Orthodontics in Implant DentistryDocument13 pagesThe Role of Orthodontics in Implant DentistryNeelash KrishnaNo ratings yet
- Introduction To The Course and Rationale For Dental ImplantsDocument34 pagesIntroduction To The Course and Rationale For Dental ImplantsKulashekar ReddyNo ratings yet
- Factors Related To Treatment and Outcomes of Avulsed TeethDocument8 pagesFactors Related To Treatment and Outcomes of Avulsed TeethJessie PcdNo ratings yet
- Oral Diagnosis and Treatment Planning: Part 7. Treatment Planning For Missing TeethDocument11 pagesOral Diagnosis and Treatment Planning: Part 7. Treatment Planning For Missing TeethalfredoibcNo ratings yet
- AvulsiDocument10 pagesAvulsiNirma JerabunNo ratings yet
- Factors Impacting Outcomes of Traumatically Extruded Permanent TeethDocument5 pagesFactors Impacting Outcomes of Traumatically Extruded Permanent Teethkhalisha salsabilaNo ratings yet
- Australian Dental Journal - 2008 - Moule - The Endodontic Management of Traumatized Permanent Anterior Teeth A ReviewDocument16 pagesAustralian Dental Journal - 2008 - Moule - The Endodontic Management of Traumatized Permanent Anterior Teeth A ReviewJamal AfridiNo ratings yet
- Seminar 6 Preventive Prosthodontics in CD WordDocument29 pagesSeminar 6 Preventive Prosthodontics in CD Wordketaki kunteNo ratings yet
- Delayed Replantation of An Avulsed Permanent Incisor Tooth: Case ReportDocument4 pagesDelayed Replantation of An Avulsed Permanent Incisor Tooth: Case ReportadiNo ratings yet
- Endodontic Considerations in The Elderly: ReviewarticleDocument10 pagesEndodontic Considerations in The Elderly: ReviewarticleYasmine SalsabilaNo ratings yet
- Stabilizing Teeth With Non Surgical Treatment: A Case Report of SplintingDocument3 pagesStabilizing Teeth With Non Surgical Treatment: A Case Report of SplintingAgum Nila Sari IINo ratings yet
- Dentalcrowding:The Restorativeapproach: Luis Brea,, Anabella Oquendo,, Steven DavidDocument10 pagesDentalcrowding:The Restorativeapproach: Luis Brea,, Anabella Oquendo,, Steven DavidFRISKA E PANJAITANNo ratings yet
- Practice: Rationale For Dental ImplantsDocument5 pagesPractice: Rationale For Dental Implantsminaxi123No ratings yet
- Dental Trauma - An Overview of Its Influence On The Management of Orthodontic Treatment - Part 1.Document11 pagesDental Trauma - An Overview of Its Influence On The Management of Orthodontic Treatment - Part 1.Djoka DjordjevicNo ratings yet
- Article7 13 4 PDFDocument6 pagesArticle7 13 4 PDFbadar_aqNo ratings yet
- Retention and Relapse 3Document13 pagesRetention and Relapse 3Tara TeraNo ratings yet
- Removable Partial Dentures: ReferencesDocument5 pagesRemovable Partial Dentures: ReferencesKakak AdekNo ratings yet
- Full Mouth Fixed Implant Rehabilitation in A Patient With Generalized Aggressive PeriodontitisDocument6 pagesFull Mouth Fixed Implant Rehabilitation in A Patient With Generalized Aggressive PeriodontitisFernando CursachNo ratings yet
- Prezentare ReabilitareDocument20 pagesPrezentare ReabilitareCenean VladNo ratings yet
- 1 Art 3Document6 pages1 Art 3yaridsantana100% (1)
- Fixed Partial Dentures: Diagnosis and Treatment Planning For Fixed ProsthodonticsDocument6 pagesFixed Partial Dentures: Diagnosis and Treatment Planning For Fixed ProsthodonticspalliNo ratings yet
- 2 Restorative DentistryDocument6 pages2 Restorative DentistryJawad TariqNo ratings yet
- Denture Adhesives Improve Denture PerformanceDocument2 pagesDenture Adhesives Improve Denture PerformancepaulinaNo ratings yet
- OverdentureDocument47 pagesOverdenturemohid sheikhNo ratings yet
- 10 1053@j Sodo 2020 01 007 PDFDocument12 pages10 1053@j Sodo 2020 01 007 PDFFayyaz AhamedNo ratings yet
- Autotransplant of Teeth PDFDocument6 pagesAutotransplant of Teeth PDFErisa BllakajNo ratings yet
- AvulsiDocument5 pagesAvulsiVembri IrawatiNo ratings yet
- Int Endodontic J - 2022 - Murray - Review of Guidance For The Selection of Regenerative Endodontics ApexogenesisDocument12 pagesInt Endodontic J - 2022 - Murray - Review of Guidance For The Selection of Regenerative Endodontics ApexogenesisEdward AbadiaNo ratings yet
- Periodoncia y ProstodonciaDocument5 pagesPeriodoncia y ProstodonciaTpz DiegoNo ratings yet
- Impacted Central Incisors Factors Affecting Prognosis and Treatment Duration 2015 American Journal of Orthodontics and Dentofacial OrthopedicsDocument8 pagesImpacted Central Incisors Factors Affecting Prognosis and Treatment Duration 2015 American Journal of Orthodontics and Dentofacial OrthopedicskjunaidNo ratings yet
- Preventive Prosthodontics: Combination of Tooth Supported BPS Overdenture & Flexible Removable Partial DentureDocument5 pagesPreventive Prosthodontics: Combination of Tooth Supported BPS Overdenture & Flexible Removable Partial DentureInddah NiiNo ratings yet
- Afrand Et Al 2017 AJODODocument11 pagesAfrand Et Al 2017 AJODOplayer osamaNo ratings yet
- 2003.john H. Warford JR - Prediction of Maxillary Canine Impaction UsingDocument5 pages2003.john H. Warford JR - Prediction of Maxillary Canine Impaction UsingLuis HerreraNo ratings yet
- 2000 Ericson Resorption of Incisors AfterDocument9 pages2000 Ericson Resorption of Incisors Afterplayer osamaNo ratings yet
- Delayed Tooth Eruption Pa Tho Genesis, Diagnosis and Treatment.Document14 pagesDelayed Tooth Eruption Pa Tho Genesis, Diagnosis and Treatment.DrFarhana AfzalNo ratings yet
- 2020 Rizell Predictive Factors For Canine Position in Patients With Unilateral Cleft Lip and PalateDocument7 pages2020 Rizell Predictive Factors For Canine Position in Patients With Unilateral Cleft Lip and Palateplayer osamaNo ratings yet
- 2003.john H. Warford JR - Prediction of Maxillary Canine Impaction UsingDocument5 pages2003.john H. Warford JR - Prediction of Maxillary Canine Impaction UsingLuis HerreraNo ratings yet
- 2002 Ericson Does The Canine Dental Follicle Cause Resorption ofDocument10 pages2002 Ericson Does The Canine Dental Follicle Cause Resorption ofplayer osamaNo ratings yet
- Palatally impacted canines assessed in 3DDocument9 pagesPalatally impacted canines assessed in 3Dplayer osamaNo ratings yet
- A New Guide Using CBCT To Identify TheDocument6 pagesA New Guide Using CBCT To Identify Theplayer osamaNo ratings yet
- A Treatment Difficulty Index For Unerupted Maxillary CaninesDocument4 pagesA Treatment Difficulty Index For Unerupted Maxillary Caninesplayer osamaNo ratings yet
- AJODO-2013 143 4 446 UmesanDocument2 pagesAJODO-2013 143 4 446 Umesanplayer osamaNo ratings yet
- 2009 Kau A Novel 3D ClassificationDocument6 pages2009 Kau A Novel 3D Classificationplayer osamaNo ratings yet
- 2000 RichardsonDocument5 pages2000 Richardsonplayer osamaNo ratings yet
- Ectopic Eruption of The Maxillary Canine On CephalometDocument8 pagesEctopic Eruption of The Maxillary Canine On CephalometyeiNo ratings yet
- Letters To The Editor: Bone and Cartilage Changes After Injection of Botulinum ToxinDocument3 pagesLetters To The Editor: Bone and Cartilage Changes After Injection of Botulinum Toxinplayer osamaNo ratings yet
- AJODO-2013 143 4 446 KaramiDocument1 pageAJODO-2013 143 4 446 Karamiplayer osamaNo ratings yet
- Effect of Surgical Exposure Technique, Age, andDocument11 pagesEffect of Surgical Exposure Technique, Age, andplayer osamaNo ratings yet
- Boneceramic Graft Regenerates Alveolar Defects But Slows Orthodontic Tooth Movement With Less Root ResorptionDocument10 pagesBoneceramic Graft Regenerates Alveolar Defects But Slows Orthodontic Tooth Movement With Less Root Resorptionplayer osamaNo ratings yet
- Bone and Cartilage Changes After Injection of Botulinum Toxin - 2016 - American Journal of Orthodontics and Dentofacial OrthopedicsDocument1 pageBone and Cartilage Changes After Injection of Botulinum Toxin - 2016 - American Journal of Orthodontics and Dentofacial Orthopedicsplayer osamaNo ratings yet
- Comparison and Reproducibility of 2 Regions of Reference For Maxillary Regional Registration With Cone-Beam Computed TomographyDocument10 pagesComparison and Reproducibility of 2 Regions of Reference For Maxillary Regional Registration With Cone-Beam Computed Tomographyplayer osamaNo ratings yet
- Corticotomy Assisted Rapid Maxillary Expansion - 2016 - American Journal of Orthodontics and Dentofacial OrthopedicsDocument2 pagesCorticotomy Assisted Rapid Maxillary Expansion - 2016 - American Journal of Orthodontics and Dentofacial Orthopedicsplayer osamaNo ratings yet
- AJODO-2013 (First Author) 143 5 A2Document4 pagesAJODO-2013 (First Author) 143 5 A2player osamaNo ratings yet
- AAO Officers and Organizations DirectoryDocument1 pageAAO Officers and Organizations Directoryplayer osamaNo ratings yet
- Comparison of Three Different Orthodontic Wires For Bonded Lingual Retainer FabricationDocument8 pagesComparison of Three Different Orthodontic Wires For Bonded Lingual Retainer Fabricationosama-alaliNo ratings yet
- AJODO-2013 (First Author) 143 5 A10Document1 pageAJODO-2013 (First Author) 143 5 A10player osamaNo ratings yet
- AJODO-2013 (First Author) 143 5 A14 PDFDocument1 pageAJODO-2013 (First Author) 143 5 A14 PDFplayer osamaNo ratings yet
- PracticalTechforAchiev PDFDocument4 pagesPracticalTechforAchiev PDFosama-alaliNo ratings yet
- Zachrisson Am J Orthod 2011Document9 pagesZachrisson Am J Orthod 2011player osamaNo ratings yet
- SDJ 3 2013Document61 pagesSDJ 3 2013player osamaNo ratings yet
- Radiology in Periodontics PDFDocument7 pagesRadiology in Periodontics PDFIna BogdanNo ratings yet
- Periodontal Osseous Defects A Review PDFDocument8 pagesPeriodontal Osseous Defects A Review PDFLorenaCastanoGarzonNo ratings yet
- Objective Structured Clinical Examination (OSCE) Protocol: MarchDocument16 pagesObjective Structured Clinical Examination (OSCE) Protocol: MarchBhumika SharmaNo ratings yet
- Larato 1970 - Furcation Involvements - Incidence and DistributionDocument3 pagesLarato 1970 - Furcation Involvements - Incidence and DistributionBryan HeeNo ratings yet
- Pre-Implant - Prosthodontics 2Document56 pagesPre-Implant - Prosthodontics 2Ameera RabayahNo ratings yet
- Sanz Et Al 2015Document26 pagesSanz Et Al 2015sidra malikNo ratings yet
- Periodontology 2000 - 2003 - SANZ - Focus On Furcation Defects Guided Tissue RegenerationDocument21 pagesPeriodontology 2000 - 2003 - SANZ - Focus On Furcation Defects Guided Tissue Regenerationcarla lopezNo ratings yet
- DC NH RăngDocument15 pagesDC NH Răngnguyễn quỳnhNo ratings yet
- Preparation and Treatment of Periodontally Compromised DentitionDocument16 pagesPreparation and Treatment of Periodontally Compromised DentitionsankarNo ratings yet
- Orthodontic treatment's greater impact on adolescents' gingivitisDocument8 pagesOrthodontic treatment's greater impact on adolescents' gingivitisMárcio LMSNo ratings yet
- Guided Tissue RegenerationDocument131 pagesGuided Tissue Regenerationt sNo ratings yet
- Periodontal Surgery: Treatment of Multi-Rooted TeethDocument6 pagesPeriodontal Surgery: Treatment of Multi-Rooted TeethYuttapol PimpisonNo ratings yet
- Int Endodontic J - 2014 - Ordinola Zapata - Micro CT Evaluation of C Shaped Mandibular First Premolars in A BrazilianDocument7 pagesInt Endodontic J - 2014 - Ordinola Zapata - Micro CT Evaluation of C Shaped Mandibular First Premolars in A BrazilianRodrigo Cassana RojasNo ratings yet
- Furcation involvement diagnosis and classificationDocument26 pagesFurcation involvement diagnosis and classificationYehya Al KhashabNo ratings yet
- Clinical Reliability of The Furcation Arrow As A Diagnostic MarkerDocument6 pagesClinical Reliability of The Furcation Arrow As A Diagnostic MarkerGabriela GuerraNo ratings yet
- Role of PeriodontistDocument5 pagesRole of PeriodontistNeetha ShenoyNo ratings yet
- Vrushali Bhor Resume 2021Document2 pagesVrushali Bhor Resume 2021Madhu DatarNo ratings yet
- Case SeriesDocument11 pagesCase SeriesLinda Garcia PNo ratings yet
- Furcation Involvement Diagnosis and Treatment OptionsDocument20 pagesFurcation Involvement Diagnosis and Treatment OptionsKarolina DoskoczNo ratings yet
- Furcation Involvement 11Document31 pagesFurcation Involvement 11Sign and Logo ExpertNo ratings yet
- Furcation Diagnosis: Review ArticleDocument14 pagesFurcation Diagnosis: Review ArticleluisNo ratings yet
- PERFORATIONS & MANAGEMENT: A REVIEW OF DIAGNOSIS AND TREATMENTDocument163 pagesPERFORATIONS & MANAGEMENT: A REVIEW OF DIAGNOSIS AND TREATMENTAPARNA AARATHI SREEKUMARNo ratings yet
- McFall 1982 Prognosis SystemsDocument11 pagesMcFall 1982 Prognosis SystemsApril FloresNo ratings yet