Professional Documents
Culture Documents
Delayed Diagnosis of Duodenal Atresia in An 11 Year Old: Case Report
Uploaded by
Anisa GayatriOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Delayed Diagnosis of Duodenal Atresia in An 11 Year Old: Case Report
Uploaded by
Anisa GayatriCopyright:
Available Formats
Maria E. Tecos et al. Medical Research Archives vol 8 issue 5.
Medical Research Archives
CASE REPORT
Delayed Diagnosis of Duodenal Atresia in an 11 Year Old
Authors
Maria E. Tecos, MD
David F. Mercer, MD
Affiliation
University of Nebraska Medical Center, University of Nebraska Medical Center, Department of General
Surgery
983280 NEBRASKA MEDICAL CTR, OMAHA, NE, 68198
Conflict of Interest:
No author has any professional or financial conflict of interest to report
Support/Funding:
No funding was required for this project
Corresponding Author
Maria E. Tecos
Phone: (402) 559-5510
Email: maria.tecos@unmc.edu
Abstract
Duodenal atresia is a condition typically diagnosed in the neonatal period. Here, we
discuss an 11-year-old patient with a new diagnosis of duodenal atresia, discovered during a lysis
of adhesions. The patient had a history of malrotation and was status-post Ladd’s procedure, but
had continued to experience bilious emesis and symptoms of intestinal obstruction since 1 month
of age, resulting in lifetime total parenteral nutrition (TPN) dependence. She was subsequently
diagnosed with microcolon megacystic hypoperistalsis syndrome (MMHS) and underwent loop
jejunostomy creation that proved unsuccessful in relieving her symptoms. Duodenal atresia was
recognized and repaired intraoperatively during a planned loop jejunostomy revision.
Copyright 2020 KEI Journals. All Rights Reserved
Maria E. Tecos et al. Medical Research Archives vol 8 issue 5. May 2020 Page 2 of 6
Introduction dependence if identified and treated in a
timely manner. Undoubtedly, patients with
Duodenal atresia is found in 1 out of
complex medical histories present
every 5,000-10,000 live births, and is more
challenges when considering the workup of
common in males than females.
a differential diagnosis. It is logical that as a
Approximately 25% of patients with
patient ages, congenital malformations may
duodenal atresia also have Down syndrome.1
be less likely to be considered as the source
It typically presents shortly after birth with
of persistent or refractory symptoms. For
bilious vomiting, and can be diagnosed on
this reason, it is important to revisit these
abdominal x-ray via a characteristic double-
inborn errors as potential sources of
bubble sign. Treatment consists of
dysfunction if they have not been formally
nasogastric tube decompression of the
or adequately ruled out in the diagnostic
stomach, fluid resuscitation, and
process.
duodenoduodenostomy. It is thought to be
the result of intrauterine vascular insult, or Case Report
failure of recanalization during intestinal
Our patient was an 11-year-old
development; as such, pregnancies can often
female with complete TPN dependence
exhibit polyhydramnios.1 It should be
since birth secondary to frequent bilious
considered in the differential for bilious
emesis and longstanding obstructive
emesis in the newborn.
symptoms. She had a diagnosis of MMHS in
As in the case of any complicated or the setting of a history of a Ladd’s procedure
delayed diagnosis, an incompletely and gastrostomy tube (g-tube) placement at
characterized clinical picture has the 1 month old. Despite these interventions,
potential to obscure symptomatology, and she remained unable to tolerate enteral
cloud medical decision making. Patients can feeds, exhibited recurrent episodes of emesis
be subject to debilitating disease sequelae or with abdominal pain, and required frequent
exposed to the risks of additional procedures fecal disimpactions. Small bowel follow
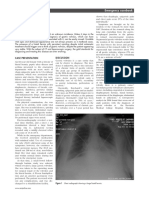
and prolonged treatments. When considering through was attempted in February 2018
duodenal atresia specifically, the clinical without progression of contrast beyond the
course could include fewer surgical duodenum at 5.5 hours, as evidenced in
interventions or a shorter timeframe of TPN Figure 1.
Copyright 2020 KEI Journals. All Rights Reserved http://journals.ke-i.org/index.php/mra
Maria E. Tecos et al. Medical Research Archives vol 8 issue 5. May 2020 Page 3 of 6
Figure 1: Small bowel follow through showing contrast to the level of the duodenum 5.5 hours
into the study
At 10 years old she transferred care duodenum. A foley catheter was inserted
to our facility and underwent loop into the gastrostomy and was unable to be
jejunostomy creation. She continued to have passed across the atretic band. A duodeno-
high-volume bilious output from her g-tube, duodenostomy was then performed, and
and comparatively low-volume clear output patency from portion 2 to portion 3 of the
from her loop jejunostomy. She also duodenum was confirmed by passing the
complained of distension, emesis, foley catheter with the balloon inflated
constipation, and difficulty urinating. across the new anastomosis. We elected to
Because of her persistent symptomatology, a proceed with the original plan of loop
loop jejunostomy revision was scheduled. jejunostomy revision for obstructive relief,
with a future goal of jejunostomy takedown
Extensive lysis of adhesions was
pending symptomatic improvement.
performed. When the duodenum was
isolated, an atretic band appeared to be
present between portions 2 and 3 of the
Copyright 2020 KEI Journals. All Rights Reserved http://journals.ke-i.org/index.php/mra
Maria E. Tecos et al. Medical Research Archives vol 8 issue 5. May 2020 Page 4 of 6
Discussion 70% duodenal stenosis discovered after
foreign body ingestion resulting in
Our patient is an 11-year-old girl
obstruction.2 Another patient was a 5-
without Down syndrome whose medical
month-old male with Down syndrome, who
history of malrotation status-post Ladd’s
presented with hematemesis after previously
procedure complicated her persistent
tolerating breastfeeding without incident.
symptomatology. Her bilious emesis
Duodenal stenosis was diagnosed via a
persisted after her initial loop jejunostomy
combination of upper endoscopy and upper
because her ampulla of Vater was proximal
gastrointestinal series, revealing some
to the atretic duodenal band. The loop
passage of contrast through a stenotic
jejunostomy had scant, non-bilious
duodenum. Malrotation was also discovered
production because it was distal to the
intraoperatively in this patient.3 A more
atretic segment of duodenum. Thus, the
severe case was of duodenal stenosis was
initial loop jejunostomy did not relieve her
discovered in malnourished 18-month-old
symptoms; the true cause of her intestinal
boy, who presented with bilious emesis,
obstruction and bilious emesis (duodenal
failure to thrive, and a scaphoid abdomen.4
atresia) was only discovered after extensive
Lastly, a 9-year-old with persistent vomiting
lysis of adhesions.
was found to have a duodenal diaphragm on
Interestingly, our patient did not endoscopy.5
have the classic double-bubble appearance
The vague clinical picture of
on imaging. This is likely because since
disordered stooling, abdominal pain, bilious
birth, our patient has been intolerant of
emesis, and intolerance of enteral feeding in
enteral feeds, and was TPN dependent. She
a child has a broad differential diagnosis. In
also has had a g-tube in place since 1 month
this case, workup was further complicated
of age. The lack of enteral intake and g-tube
by the patient’s concurrent medical history
gastric decompression likely decreased the
of MMHS. The transfer of patient care
amount of duodenal dilation proximal to the
between multiple facilities provided an
atretic band, preventing the classical double-
additional hurdle to overcome. This delay in
bubble presentation. It is acceptable to
diagnosis was the result of multiple
reason that this patient’s diagnosis of
confounding factors in a challenging case.
duodenal atresia may have been made at an
The true source of the patient’s symptoms
earlier timepoint if it had presented with the
was only elucidated when the diagnostic
typical radiological findings commonly
process was essentially reset, and anatomy
associated with the condition.
was investigated under direct visualizing
Our review of the literature revealed intraoperatively.
several cases of delayed diagnosis of
Conclusion
duodenal anomalies, but no instance of
duodenal atresia in a child as old as our Duodenal anomalies should be
patient. The oldest of these cases was a 16- considered in the differential diagnosis of
year-old male with Down Syndrome, with patients presenting with persistent bilious
Copyright 2020 KEI Journals. All Rights Reserved http://journals.ke-i.org/index.php/mra
Maria E. Tecos et al. Medical Research Archives vol 8 issue 5. May 2020 Page 5 of 6
emesis and obstructive symptoms, especially diagnoses in admitted adult patients. At least
in the setting of inability to tolerate enteral 0.7% of hospitalized adults have been
feeding. Delay in diagnosis of duodenal impacted by errors in diagnosis. As such,
anomalies may severely affect quality of process improvement in the diagnostic
life, as well as commit patients to invasive course can be a point of potential
treatments, such as TPN dependence or intervention to mitigate these errors.6 This
surgical intervention. Missed diagnosis of a concept can be extended to other patient
congenital anomaly should be contemplated populations, including pediatrics, to bolster
in the systematic workup of atypically the efforts of augmenting patient safety by
presenting or refractory patients. encouraging thorough and thoughtful
diagnostic processes.
Systematic review has identified that
even common diseases are among missed
Copyright 2020 KEI Journals. All Rights Reserved http://journals.ke-i.org/index.php/mra
Maria E. Tecos et al. Medical Research Archives vol 8 issue 5. May 2020 Page 6 of 6
References
1. Kimura K & Loening-Baucke V. Bilious 4. Kshirsagar AY, Sulhyan SR, Vasisth G,
vomiting in the newbown: rapid & Nikam YP. Duodenal stenosis in a
diagnosis of intestinal obstruction. Am chil. Afr J Paediatr Surg 2011; 8: 92-94.
Fam Physician 2000; 61 (9): 2791-2798. 5. Barrera AB, Baeza SS, Labra FM, &
2. Gunasekaran SS, Cho ME, & Rodriguez DS. Duodenal diaphragm
Gunasekaran TS. Vomiting in a teenager diagnosis in a school-aged child and
with down syndrome. J Pediatr 2016; minimally invasive treatment: case
174: 272. report. Medwave 2017; 17 (1): e6859.
3. Nicholson MR, Acra SA, Chung DH, & 6. Gunderson CG et al. Prevalence of
Rosen MJ. Endoscopic diagnosis of harmful diagnostic errors in hospitalised
duodenal stenosis in a 5-month-old male adults: a systematic review and meta-
infant. Clin Enosc 2014; 47: 568-570. analysis. BMJ Qual Saf. 2020 Apr 8. Pii:
bmjqs-2019-010822.
Copyright 2020 KEI Journals. All Rights Reserved http://journals.ke-i.org/index.php/mra
You might also like
- Dysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandDysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Apple Peel Small Bowel, A Review of Four Cases: Surgical and Radiographic AspectsDocument8 pagesApple Peel Small Bowel, A Review of Four Cases: Surgical and Radiographic AspectsraecmyNo ratings yet
- Tubular Ileal Duplication Causing Small Bowel Obstruction in A ChildDocument5 pagesTubular Ileal Duplication Causing Small Bowel Obstruction in A ChildDiego Leonardo Herrera OjedaNo ratings yet
- Fecal IncontinenceDocument8 pagesFecal IncontinenceJULIO EDUARDO CENTURION MAGNANNo ratings yet
- Intestinal Malrotation in Neonates With Nonbilious Emesis: Perinatal/Neonatal Case PresentationDocument3 pagesIntestinal Malrotation in Neonates With Nonbilious Emesis: Perinatal/Neonatal Case PresentationSaurav SultaniaNo ratings yet
- Duodenal Stenosis PDFDocument9 pagesDuodenal Stenosis PDFDorcas KafulaNo ratings yet
- Jejunojejunal Intussusception As Initial Presentation of Coeliac Disease: A Case Report and Review of LiteratureDocument6 pagesJejunojejunal Intussusception As Initial Presentation of Coeliac Disease: A Case Report and Review of Literatureellya theresiaNo ratings yet
- 3 Common Pediatric Surgery ContinuedDocument5 pages3 Common Pediatric Surgery ContinuedMohamed Al-zichrawyNo ratings yet
- Intestinal Atresia: A Case ReportDocument3 pagesIntestinal Atresia: A Case ReportOvamelia JulioNo ratings yet
- Subhepatic AppDocument2 pagesSubhepatic AppAgustina TambingNo ratings yet
- Intestinal Obstruction in Paediatrics - James GathogoDocument21 pagesIntestinal Obstruction in Paediatrics - James GathogoMalueth Angui100% (1)
- Neonatal Sigmoid Volvulus A Complication PDFDocument4 pagesNeonatal Sigmoid Volvulus A Complication PDFJimi Kalvin SarareniNo ratings yet
- Focseneanu2015 PDFDocument3 pagesFocseneanu2015 PDFAniydaNo ratings yet
- Complicated Small-Bowel Diverticulosis: A Case Report and Review of The LiteratureDocument3 pagesComplicated Small-Bowel Diverticulosis: A Case Report and Review of The LiteratureYeudiel SuroNo ratings yet
- 6255 24879 1 PBDocument2 pages6255 24879 1 PBSyafatesia nicky pratiwiNo ratings yet
- Management of Jejunoileal Atresia: Our 5 Year ExperienceDocument4 pagesManagement of Jejunoileal Atresia: Our 5 Year ExperienceOvamelia JulioNo ratings yet
- Vitellointestinal Duct Anomalies in InfancyDocument3 pagesVitellointestinal Duct Anomalies in InfancyRonjavafantillanNo ratings yet
- Case Report Duodenal Stenosis in 3 Month Boy: Compiled byDocument15 pagesCase Report Duodenal Stenosis in 3 Month Boy: Compiled byMuhammad Khairuna SyahPutraNo ratings yet
- Laparoscopic Splenectomy For Pediatric Wandering Spleen - A Case ReportDocument11 pagesLaparoscopic Splenectomy For Pediatric Wandering Spleen - A Case ReportAdlyn Bea Albesa-BernaldezNo ratings yet
- Gastric Volvulus: Bang Chau, Susan DufelDocument2 pagesGastric Volvulus: Bang Chau, Susan DufelmustikaarumNo ratings yet
- Case Report: The Combination of Gastroschisis, Jejunal Atresia, and Colonic Atresia in A NewbornDocument5 pagesCase Report: The Combination of Gastroschisis, Jejunal Atresia, and Colonic Atresia in A NewbornAnonymous PmfX227No ratings yet
- Journal of Pediatric Surgery CASE REPORTS: Sonal Nagra, Jitoko K. CamaDocument3 pagesJournal of Pediatric Surgery CASE REPORTS: Sonal Nagra, Jitoko K. CamazuliaahmadNo ratings yet
- Journal of Pediatric Surgery CASE REPORTS: Sonal Nagra, Jitoko K. CamaDocument3 pagesJournal of Pediatric Surgery CASE REPORTS: Sonal Nagra, Jitoko K. CamazuliaahmadNo ratings yet
- The Gentle Touch' Technique in The Treatment of GastroschisisDocument3 pagesThe Gentle Touch' Technique in The Treatment of Gastroschisisansar ahmedNo ratings yet
- Intussusception - A Case ReportDocument3 pagesIntussusception - A Case ReportAgustinus HuangNo ratings yet
- Assessment of The Pediatric PatientDocument12 pagesAssessment of The Pediatric PatientiskoriahNo ratings yet
- Duodenal AtresiaDocument18 pagesDuodenal AtresiaRianto Noviady RamliNo ratings yet
- Acute Appendicitis: Review ArticleDocument6 pagesAcute Appendicitis: Review ArticleAinun Jariah FahayNo ratings yet
- Gastric Perforation in Neonates: Analysis of Five Cases: Case ReportDocument3 pagesGastric Perforation in Neonates: Analysis of Five Cases: Case ReportwineniNo ratings yet
- Document 1Document4 pagesDocument 1arditia dwiNo ratings yet
- J Epsc 2015 05 012Document4 pagesJ Epsc 2015 05 012Hanung PujanggaNo ratings yet
- 20 PediatricDocument31 pages20 PediatricMahmoud AbuAwadNo ratings yet
- Open Access Textbook of General Surgery: Large Bowel Obstruction A BoutallDocument6 pagesOpen Access Textbook of General Surgery: Large Bowel Obstruction A BoutallDian FikriNo ratings yet
- RLQ PainDocument20 pagesRLQ PainBEATRICE SOPHIA PARMANo ratings yet
- Bilious Vomiting in The NewbornDocument6 pagesBilious Vomiting in The NewbornRodrigo Vargas IllescasNo ratings yet
- Total Colonic Aganglionosis (Zuelzer Wilson Syndrome) An EnigmaDocument2 pagesTotal Colonic Aganglionosis (Zuelzer Wilson Syndrome) An EnigmarmysdsNo ratings yet
- Duodenal Duplication, Intestinal Malrotation and Volvulus. An Unusual Cause of Intestinal ObstructionDocument3 pagesDuodenal Duplication, Intestinal Malrotation and Volvulus. An Unusual Cause of Intestinal ObstructionDiego Leonardo Herrera OjedaNo ratings yet
- SigmoidDocument4 pagesSigmoidFKUPR 2017No ratings yet
- Cystic FibrosisDocument3 pagesCystic FibrosisRieza NurdinsyahNo ratings yet
- 1-5 BedahDocument9 pages1-5 BedahHalwia SiruaNo ratings yet
- Association of Duodenal Atresia, Malrotation, Ventricular Septal Defect, Endocardial Cushion Defect, Atrial Septal Defect, and Patent Ductus Arteriosus in A Down Syndrome PatientDocument3 pagesAssociation of Duodenal Atresia, Malrotation, Ventricular Septal Defect, Endocardial Cushion Defect, Atrial Septal Defect, and Patent Ductus Arteriosus in A Down Syndrome PatientasclepiuspdfsNo ratings yet
- The Rapunzel Syndrome - A Case Report: Trichobezoar As A Cause of Intestinal PerforationDocument4 pagesThe Rapunzel Syndrome - A Case Report: Trichobezoar As A Cause of Intestinal PerforationSajag GuptaNo ratings yet
- Gastroschisis: Etiology, Diagnosis, Delivery Options, and CareDocument6 pagesGastroschisis: Etiology, Diagnosis, Delivery Options, and CareCarolina TorresNo ratings yet
- Small Intestine Obstruction in Patients Due To Phytobezoar: Case Report of Four PatientsDocument4 pagesSmall Intestine Obstruction in Patients Due To Phytobezoar: Case Report of Four PatientsInt Journal of Recent Surgical and Medical SciNo ratings yet
- Case Series of Intussusception in Paediatric SurgeryDocument39 pagesCase Series of Intussusception in Paediatric SurgeryRajkiran AmbarapuNo ratings yet
- Medicine: A Newborn Patient With Both Annular Pancreas and Meckel 'S DiverticulumDocument5 pagesMedicine: A Newborn Patient With Both Annular Pancreas and Meckel 'S DiverticulumAdrian UmbriaNo ratings yet
- IntussusceptionDocument4 pagesIntussusceptionBlue TechNo ratings yet
- Case Report Esophageal AtresiaDocument3 pagesCase Report Esophageal Atresiaadriani lawrenciaNo ratings yet
- Hirschsprun G'S Disease: Dr. Manish Kumar Gupta Assistant Professor Department of Paediatric Surgery AIIMS, RishikeshDocument48 pagesHirschsprun G'S Disease: Dr. Manish Kumar Gupta Assistant Professor Department of Paediatric Surgery AIIMS, RishikeshArchana Mahata100% (1)
- Mehu107 U3 T30 Colon CurrentDocument7 pagesMehu107 U3 T30 Colon CurrentRegina PizanNo ratings yet
- Pediatric (S) 2023 Final 7th SemDocument226 pagesPediatric (S) 2023 Final 7th SemSyed NoorNo ratings yet
- Intestinal Obstruction in Neonatal/Pediatric Surgery: by C.A. HajivassiliouDocument13 pagesIntestinal Obstruction in Neonatal/Pediatric Surgery: by C.A. HajivassiliouUlfa LathifaNo ratings yet
- Intestinal Obstruction in Pediatric SurgeryDocument69 pagesIntestinal Obstruction in Pediatric Surgeryabhinay_1712No ratings yet
- Intususcepción: Diagnóstico Y Manejo en Niños Y Adultos: C Ir Ugí ADocument6 pagesIntususcepción: Diagnóstico Y Manejo en Niños Y Adultos: C Ir Ugí ACarlos Angel LiraNo ratings yet
- Child JournalDocument8 pagesChild JournalVijayakanth VijayakumarNo ratings yet
- 6665 PDFDocument4 pages6665 PDFerindah puspowatiNo ratings yet
- Jurnal Kasus Gastrochisis 1Document3 pagesJurnal Kasus Gastrochisis 1ULA HOFINo ratings yet
- PiosalpinxDocument3 pagesPiosalpinxRopiNo ratings yet
- Peritoneal Encapsulation: A Rare Cause of Small Bowel ObstructionDocument3 pagesPeritoneal Encapsulation: A Rare Cause of Small Bowel ObstructionNatalindah Jokiem Woecandra T. D.No ratings yet
- Common Health Problems That Develop During Infancy MPNDocument14 pagesCommon Health Problems That Develop During Infancy MPNShaii Whomewhat GuyguyonNo ratings yet
- New Prognostic Classification and Managements in Infants With Esophageal AtresiaDocument8 pagesNew Prognostic Classification and Managements in Infants With Esophageal AtresiaAnisa GayatriNo ratings yet
- Neonatal Esophageal Perforation With Esophageal Atresia: A Case ReportDocument3 pagesNeonatal Esophageal Perforation With Esophageal Atresia: A Case ReportAnisa GayatriNo ratings yet
- SchollinAsk2019 Article ClinicalPresentationOfIntussusDocument9 pagesSchollinAsk2019 Article ClinicalPresentationOfIntussusAnisa GayatriNo ratings yet
- Allarakia 2019Document4 pagesAllarakia 2019Anisa GayatriNo ratings yet
- Late Complications of Biliary Atresia: Hepatopulmonary Syndrome and Portopulmonary HypertensionDocument6 pagesLate Complications of Biliary Atresia: Hepatopulmonary Syndrome and Portopulmonary HypertensionAnisa GayatriNo ratings yet
- Ishii2020 Article CongenitalMultipleColonicAtresDocument5 pagesIshii2020 Article CongenitalMultipleColonicAtresAnisa GayatriNo ratings yet
- EA Routine Vitamin A Supplementation For The Prevention of Blindness Due To Measles Infection in Children PDFDocument3 pagesEA Routine Vitamin A Supplementation For The Prevention of Blindness Due To Measles Infection in Children PDFAnisa GayatriNo ratings yet
- Areca CatechuDocument8 pagesAreca CatechuAnisa GayatriNo ratings yet
- Review of Related LiteratureDocument5 pagesReview of Related Literaturekeith tambaNo ratings yet
- Stop TB Text Only 2012Document30 pagesStop TB Text Only 2012Ga B B OrlonganNo ratings yet
- Ele Unit5 Revision PDFDocument2 pagesEle Unit5 Revision PDFNatalia ZapataNo ratings yet
- FPSC - Inspector - Custom - Intelligence - Officer - PDF Filename - UTF-8''FPSC Inspector Custom Intelligence OfficerDocument405 pagesFPSC - Inspector - Custom - Intelligence - Officer - PDF Filename - UTF-8''FPSC Inspector Custom Intelligence Officerasimafzal100% (1)
- Barnum Distributors Wants A Projection of Cash Receipts and CashDocument1 pageBarnum Distributors Wants A Projection of Cash Receipts and CashAmit PandeyNo ratings yet
- This Points Are Very Main Part of Self: How To Give Self Introduction in IterviewDocument22 pagesThis Points Are Very Main Part of Self: How To Give Self Introduction in Iterviewvijay kumarNo ratings yet
- Antenatal Assessment of Fetal Well Being FileminimizerDocument40 pagesAntenatal Assessment of Fetal Well Being FileminimizerPranshu Prajyot 67No ratings yet
- Ganendra Art House: 8 Lorong 16/7B, 46350 Petaling Jaya, Selangor, MalaysiaDocument25 pagesGanendra Art House: 8 Lorong 16/7B, 46350 Petaling Jaya, Selangor, MalaysiaFiorela Estrella VentocillaNo ratings yet
- Question 1Document8 pagesQuestion 1daniela222No ratings yet
- Case Study: Political PartiesDocument26 pagesCase Study: Political PartiesChaii100% (1)
- Atty. SungaDocument22 pagesAtty. SungaKris MercadoNo ratings yet
- Outcomes of Democracy: How Do We Assess Democracy?Document7 pagesOutcomes of Democracy: How Do We Assess Democracy?Ankita MondalNo ratings yet
- Chapter 5 Decision TheoryDocument43 pagesChapter 5 Decision TheoryTamiru BeyeneNo ratings yet
- The List of the Korean Companies in the UAE: Company Name 이름 Off. Tel Off. Fax P.O.BoxDocument34 pagesThe List of the Korean Companies in the UAE: Company Name 이름 Off. Tel Off. Fax P.O.Boxnguyen phuong anh100% (1)
- A Room of One's Own EssayDocument3 pagesA Room of One's Own EssayPeter Hadley MahotiereNo ratings yet
- VW Touareg 2 Brake System EngDocument111 pagesVW Touareg 2 Brake System EngCalin GeorgeNo ratings yet
- VMware NSX - SDN Ninja Program DatasheetDocument4 pagesVMware NSX - SDN Ninja Program DatasheetSarah AliNo ratings yet
- Manual BeefDocument82 pagesManual Beefcmukasauk100% (1)
- Based On The 1979 Standards of Professional Practice/ SPPDocument10 pagesBased On The 1979 Standards of Professional Practice/ SPPOwns DialaNo ratings yet
- Kitty GenoveseDocument2 pagesKitty GenoveseRachael BartlettNo ratings yet
- Kentucky National Guard MemorialDocument60 pagesKentucky National Guard MemorialCourier JournalNo ratings yet
- 28-03-2023 Sed TicketsDocument8 pages28-03-2023 Sed TicketssureshhkNo ratings yet
- Sample Thesis of Medical Record SystemDocument8 pagesSample Thesis of Medical Record Systemfj9dbfw4100% (1)
- ACS880 IGBT Supply Control Program: Firmware ManualDocument254 pagesACS880 IGBT Supply Control Program: Firmware ManualGopinath PadhiNo ratings yet
- 2 CSS Word FileDocument12 pages2 CSS Word Fileronak waghelaNo ratings yet
- SAP Manufacturing Implementation Architecture-1Document17 pagesSAP Manufacturing Implementation Architecture-1andriesbuterNo ratings yet
- Legalese and Legal EnglishDocument16 pagesLegalese and Legal English667yhNo ratings yet
- TVM-Excel Function Solved ProblemDocument16 pagesTVM-Excel Function Solved ProblemIdrisNo ratings yet
- Henri Fayol A StrategistDocument13 pagesHenri Fayol A StrategistTerence DeluNo ratings yet
- Accomplishment and Narrative Report OctDocument4 pagesAccomplishment and Narrative Report OctGillian Bollozos-CabuguasNo ratings yet
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (403)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo ratings yet
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (78)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (20)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Gut: the new and revised Sunday Times bestsellerFrom EverandGut: the new and revised Sunday Times bestsellerRating: 4 out of 5 stars4/5 (392)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (5)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- 12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosFrom Everand12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosRating: 4.5 out of 5 stars4.5/5 (207)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (253)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- Algorithms to Live By: The Computer Science of Human DecisionsFrom EverandAlgorithms to Live By: The Computer Science of Human DecisionsRating: 4.5 out of 5 stars4.5/5 (722)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningFrom EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningRating: 4 out of 5 stars4/5 (3)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (1)
- The Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsFrom EverandThe Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsNo ratings yet
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)