Professional Documents
Culture Documents
9 Suppl - 1 S58
Uploaded by
ChristopherLawrenceOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
9 Suppl - 1 S58
Uploaded by
ChristopherLawrenceCopyright:
Available Formats
PAIN MEDICINE
Volume 9 • Number S1 • 2008
Vertebroplasty and Kyphoplasty: Case Presentation,
Complications, and Their Prevention
Downloaded from https://academic.oup.com/painmedicine/article-abstract/9/suppl_1/S58/1825158 by KERIS National Access user on 28 January 2020
Allen W. Burton, MD
Departments of Anesthesiology and Pain Medicine, University of Texas MD Anderson Cancer Center, Houston, Texas,
USA
ABSTRACT
Objective. To describe vertebroplasty and kyphoplasty, which are relatively new techniques used to
treat painful vertebral compression fractures.
Design Setting Patients. This article briefly reviews the procedural indications, technical aspects of
the procedure, and strategies for complication avoidance.
Results. Percutaneous vertebroplasty is the injection of a vertebral body with bone cement, generally
polymethylmethacrylate. Kyphoplasty is the placement of balloons (called “tamps”) into the verte-
bral body with an inflation/deflation sequence to create a cavity prior to the cement injection. These
procedures are most often performed in a percutaneous fashion on an outpatient (or short stay)
basis. The mechanism of action is unknown, but it is postulated that stabilization of the fracture
leads to analgesia. The procedure is indicated for painful vertebral compression fractures due to
osteoporosis or malignancy, and painful hemangiomas. The procedure has efficacy in painful
vertebral metastasis and traumatic compression fractures. Much evidence favors the use of this
procedure for pain associated with these disorders. The overall risks of the procedure are low but
serious complications can occur. The serious complications include spinal cord compression, nerve
root compression, venous embolism, pulmonary embolism including cardiovascular collapse, and
others. With good patient selection and careful technique, these complications are avoidable,
making the risk-to-benefit ratio highly favorable.
Conclusions. Vertebroplasty and kyphoplasty are effective and safe techniques used to treat painful
spinal fractures.
Key Words. Kyphoplasty; Vertebroplasty; Vertebral Compression Fracture; Osteoporosis; Spinal
Metastasis; Spine Fractures; Spine Interventional Procedures
Case Report was located in the thoracolumbar spine. It was
described as nonradiating, worse with movement,
A 43-year-old physician presented with a
2-month history of severe low back pain after
a fall while playing with his children. The pain
with numerical pain scores ranging from 1–10/10
over the previous 24 hours. The patient was taking
oxycodone-CR 80 mg orally every 8 hours, plus
hydromorphone 8–16 mg orally up to six times
Reprint requests to: Allen W. Burton, MD, Departments of
Anesthesiology and Pain Medicine, UT MD Anderson
daily for breakthrough pain. The patient was
Cancer Center, 1400 Holcombe Blvd.-409, Houston TX diagnosed with vertebral compression fractures
77030, USA. Tel: 713-745-7246; Fax: 713-745-0177; (VCFs) at T-11, L1, L2, L3, L4, and L5. He was
E-mail: awburton@mdanderson.org. diagnosed with multiple myeloma and begun on
Disclosure: AWB is the principal investigator on a Kyphon, chemotherapy 2 weeks prior to consultation. His
Inc.-supported research protocol. magnetic resonance imaging (MRI) scan revealed
© American Academy of Pain Medicine 1526-2375/08/$15.00/S58 S58–S64 doi:10.1111/j.1526-4637.2008.00440.x
Vertebroplasty and Kyphoplasty: Complications and Prevention S59
Downloaded from https://academic.oup.com/painmedicine/article-abstract/9/suppl_1/S58/1825158 by KERIS National Access user on 28 January 2020
Figure 1 Anterior-posterior/lateral ra-
diographs after six-level vertebro-
plasty. Large cement extrusion is seen
at T-11 anteriorly, extrusion into a
small vein at L-1, and into the disk at
L-2.
T-2 signal enhancement at the fractured levels injection. Percutaneous kyphoplasty (PK) may
without canal compromise. The patient was restore vertebral body height and reduce the
offered the option of percutaneous vertebroplasty kyphotic angulation of the compression fracture
(PV). The patient underwent PV at L3, L4, and prior to PMMA injection [5].
L5 with slight reduction in pain. Two weeks later Ideal candidates for PV or PK have activity-
the patient underwent PV at T-11, L1, and L2 related axial pain corresponding to the level of a
with near complete pain relief. The patient had a recent compression fracture. This pain lessens or
polymethylmethacrylate (PMMA) leak anteriorly goes away completely with recumbency and/or
from his T-11 and L1, and into the disk at L1–2 sitting still. A complete neurologic exam and
during the procedure, but this was asymptomatic. recent radiographic imaging is mandatory to rule
(Figures 1 and 2). Over the next 4 weeks, the out spinal cord compromise and/or retropulsed
patient was gradually reconditioned with a low- bony fragments in the canal. MRI should show an
impact exercise program, having only mild back
discomfort eased with tramadol on an as-needed
basis. He has undergone bone marrow transplant
and his myeloma is in remission. Thus, although
this patient had a minor PMMA leak, it was
asymptomatic and the clinical outcome was good.
Procedural Overview
Vertebroplasty and kyphoplasty are relatively new
techniques used to treat painful VCFs. Vertebro-
plasty is the percutaneous injection of a vertebral
body with bone cement, generally PMMA.
PMMA has been used in orthopedics since the late
1960s [1]. PV was first reported by a French group
in 1987 for the treatment of painful hemangiomas
[2]. Since then, the indications for PV have
expanded to include osteoporotic compression
fractures, traumatic compression fractures, and
painful vertebral metastasis [3,4]. Kyphoplasty is a
modification of PV. It involves the percutaneous
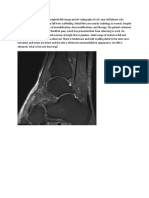
placement of balloons (called “tamps”) into the Figure 2 Axial computed tomography of T-11 showing
vertebral body with an inflation/deflation polymethylmethacrylate anterior to the vertebral body
sequence to create a cavity prior to the cement adjacent to the vascular structures in the area.
S60 Burton
increased T-2-weighted signal due to bone edema with a review of Food and Drug Administration
at the level with a recent fracture. Bone scan has safety data revealing 58 reported complications
also been used to target the most recent fracture(s) from 1999 through 2003 out of approximately
in patients with multiple fractures [6]. Cord com- 200,000 procedures performed. These were
Downloaded from https://academic.oup.com/painmedicine/article-abstract/9/suppl_1/S58/1825158 by KERIS National Access user on 28 January 2020
pression on MRI (in the absence of neurologic approximately evenly divided among PV and PK,
findings) is a relative contraindication. If on MRI with more cases of pedicle fracture and cord
there is a suspicion of a posterior cortical fracture, compression from PK than PV [17]. It must be
a computed tomography (CT) scan will reveal the noted that this voluntary reporting system is
bony architecture more precisely. almost certainly flawed and most likely underre-
ports the overall incidence of complications. As
further studies are completed, a more complete
Potential Complications
risk–benefit ratio can be defined.
Complications are rare, but can be serious. The
exact incidence is unknown. Most case series
Procedural Technical
report asymptomatic PMMA extravasation rates of Aspects/Complication Avoidance
around 10–15% [5,7]. The Society for Interven-
tional Radiology (SIR) divides up complications Standards for the safe practice of these techniques
for these techniques into minor and major. Minor have been published by the Society of Interven-
complications are those considered to require no tional Radiologists in 2003 and recently updated
therapy and having no consequence, such as by the Cardiovascular and Interventional Radio-
PMMA extravasation into the disk. Major compli- logical Society of Europe; the highlights of this
cations are those requiring therapy, including an document are in Table 1 [18,19].
unplanned increase in the level of care needed, or Prior to the procedure, the patient should be off
having ongoing permanent sequelae (i.e., PMMA of all anticoagulants and his/her coagulation
into the spinal canal with neurological deficit). SIR profile should be normal. Platelet count should be
noted published complication rates for major com- at least 50,000 at the time of the procedure,
plications to be less than 1%, except in those with although no data exists to clearly define a “cut-off”
neoplastic involvement of the vertebrae, where the platelet count. There may be instances when the
reported level of major complications is less than
5% [8]. Table 1 Overview of guidelines from Society of Interven-
PMMA can flow out of the vertebral body pos- tional Radiologists and Cardiovascular and Interventional
teriorly into the spinal canal and neural foramina, Radiological Society of Europe. Please see the refer-
or anteriorly into the paraspinous veins with sys- ences for the complete documents (modified from [17]
temic consequences. There are case reports of and [18])
nerve root and spinal cord compression from Indications
extravertebral PMMA [9,10]. Several minimally Painful osteoporotic VCF refractory to 3 weeks of analgesic
therapy
symptomatic pulmonary emboli—one case of car- Painful vertebrae due to benign or malignant primary or
diovascular collapse requiring pulmonary embo- secondary bone tumors
lectomy, one case of lethal pulmonary embolus, Painful VCF with osteonecrosis (Kummel’s disease)
Reinforcement of vertebral body prior to surgical procedure*
and one case of paradoxical cerebral arterial Chronic traumatic VCF with nonunion*
PMMA emboli—have been reported [11–14]. Absolute contraindications
There is a suggestion in the literature of less Asymptomatic VCF
PMMA leak with PK vs PV [15]. Patient improving on medical therapy
Ongoing infection
Infectious complications are rare, but reported. Prophylaxis in steoporotic patient
There are several reports of osteomyelitis requir- Uncorrectable coagulopathy
ing corpectomy [16]. Meticulous attention to Myelopathy due to retropulsion of bone/canal compromise
Allergy to PMMA or opacification agent
sterile technique is warranted, including preopera-
Relative contraindications
tive intravenous antibiotic administration. Most Radicular pain
have abandoned the older technique of adding VCF >70% height loss*
tobramycin powder to the PMMA due to uncer- Severe spinal stenosis, asymptomatic retropulsion of bony
fragment
tainty over both the efficacy and potential impact Tumor extension into canal/epidural space
on the PMMA properties. Lack of surgical backup*
Complications have been reported with both * Recommendations from the more recent update [18].
procedures (vertebroplasty and kyphoplasty), PMMA = polymethylmethacrylate; VCF = vertebral compression fracture.
Vertebroplasty and Kyphoplasty: Complications and Prevention S61
risk–benefit ratio favors doing these procedures in
patients with lower platelet counts. Active infec-
tion and sepsis are contraindications. The author
recommends waiting at least 2 weeks after treat-
Downloaded from https://academic.oup.com/painmedicine/article-abstract/9/suppl_1/S58/1825158 by KERIS National Access user on 28 January 2020
ment of an infection to minimize infectious risks.
Informed consent should include lack of pain
relief, osteomyelitis, fracture of the vertebra or
pedicle, extravasation of cement into the spinal
canal or neural foramen, paralysis or nerve root
damage, and venous embolism. Rare but fatal ana-
phylaxis to PMMA has been reported in four cases
[17]. Also, the rare but potential need for open
surgery should be discussed with the patient.
Vertebroplasty and kyphoplasty require the
clinician to be trained in spinal anatomy, fluoro-
scopic imaging, and the use of these techniques
to perform interventional procedures. The pro-
cedure should be performed in a sterile operating
room suite that will allow fluoroscopic imaging
of the thoracolumbar spine. Biplanar or C-arm Figure 3 Anterior-posterior radiograph of lumbar vertebro-
fluoroscopy of good quality is mandatory for plasty after polymethylmethacrylate injection.
maximal procedural safety. A radiolucent table is
mandatory, as is appropriate padding for prone, trochar. This information is used to more carefully
slightly flexed positioning. Other procedural inject the PMMA. For example, if a small amount
materials needed include local anesthetic solution of contrast injection reveals a direct spread into a
(the author uses a 50:50 mixture of 1% lidocaine venous channel, the operator may move the
with 0.25% bupivacaine), PMMA material, and trochar prior to injection or carefully inject rela-
barium or other radioopacification material. tively solidified PMMA to embolize the large vein
Eleven-gauge or 13-gauge bone biopsy needles prior to injecting more PMMA into the vertebral
with connection tubing and cement injection body. The literature reveals variable efficacy of the
syringes are needed; numerous commercial “kits” use of venography [20,21]. The author no longer
are available. uses venography.
General anesthesia or monitored anesthesia PMMA injection into the vertebral body is
care (MAC) can be utilized. If MAC is used, the undertaken after careful imaging confirming loca-
surgeon must use generous amounts of local anes- tion of the trochar or trochars into the anterome-
thetic, especially onto the periosteum, where dial portion of the vertebral body (Figure 3). The
much nociception occurs. Some patients experi- PMMA should be opacified and beginning to
ence discomfort with advancement of the trochars harden to the consistency of toothpaste prior to
across the posterior cortical margin, with balloon injection. Injection can be done by small syringes
inflation (in the case of kyphoplasty), and with filled with PMMA or by one of several commer-
PMMA injection. The anesthesiologist must be cially available kits. The injection must be done
prepared to “deepen” the MAC during these under live lateral or biplanar fluoroscopic guid-
phases of the procedure. Patient selection is ance. If PMMA begins to go into a blood vessel or
important with consideration to the anesthesia toward the posterior cortical margin, it must be
choice. Very anxious or nervous patients may have halted immediately. The authors halt cement
a better experience with a general anesthetic. injection when it spreads to the posterior one-
Careful consideration must be given to padding third of the vertebral body. In order to minimize
the pressure points of this fragile group of PMMA leakage, several groups recommend the
patients. After uni- or bipedicular vertebral body use of high-viscosity cement and relatively small
access has been obtained, some clinicians proceed volume injection [22–24].
directly with injection of PMMA, whereas others
prefer to do venography prior to cement injection. Outcomes in Special Circumstances
In theory, venography provides anatomic knowl- As experience grows with these techniques,
edge of large venous channels’ proximity to the various groups are pushing the envelope on indi-
S62 Burton
cations for the procedure, with the possibility of Table 2 Vertebroplasty vs kyphoplasty (see text section
seeing more complications in this patient group. for further details and references)
There is some preliminary data/case series on effi- Vertebroplasty
cacy in patients with radicular pain, traumatic Less expensive
Faster for the operator and patient
Downloaded from https://academic.oup.com/painmedicine/article-abstract/9/suppl_1/S58/1825158 by KERIS National Access user on 28 January 2020
burst fractures, severe VCF/vertebral plana, cervi- Indicated to treat even older fractures
cal spine pathology, and intra-operative PMMA Kyphoplasty
augmentation of pedicle screw fixation spinal sta- More anatomic correction of spinal deformity than
bilization [25–29]. In our center, we have pushed vertebroplasty
Greater height restoration in recent fractures, less than 3
“relative” contraindications in cancer patients months old
without increased morbidity, even in those with Indicated for patients with extensive kyphosis due to multiple
very advanced cancers [30,31]. recent VCFs
Less PMMA extravasation
Adjacent-Level Fractures PMMA = polymethylmethacrylate; VCF = vertebral compression fracture.
Cortet and colleagues first noted a small increase
in adjacent-level fractures with long-term tive trials have been done to date, but one is in the
follow-up [23]. This phenomenon is similar with planning stages. Currently, we favor the use of PK
both PV and PK [32]. Subsequent VCFs may in circumstances where the patient has a collapse
occur at adjacent or remote levels (compared with of more than 20% of vertebral height and a frac-
the treated “vertebroplastied” level). The reported ture age of less than 3 months in hopes of restoring
rate of new fractures varies from 7% to 20% over vertebral height and maintaining functional
a 1-year follow-up, with sooner refracture occur- anatomy when possible. Deramond and colleagues
ring at the adjacent levels [33]. This suggests a have stated that PK may be preferrable over PV in
local unfavorable biomechanical situation in some patients with severe or multiple wedge deformity
patients who suffer adjacent-level fracturing and that has developed in the last 3 weeks. They do
ongoing disease process (usually osteoporosis) in caution that this is speculative until direct com-
the nonadjacent fracture group. A recent large parison trials are done [38] (see Table 2).
database of 106 patients having undergone 212 PV
procedures was evaluated over a 3-year follow-up
period of time by Kim and colleagues [34]. They Key Points
noted 72 new fractures over the 3-year follow-up • PV and PK are safe and effective procedures
(7.9%). One-year fracture-free rate was 93% by used in the treatment of painful VCFs.
Kaplan–Meier analysis. The mean fracture-free • Osteoporotic patients need careful positioning
interval was 32 months, with adjacent fractures and padding to avoid injury.
being predicted by location in the thoracolumbar • During the performance of PV/PK, careful
junction and greater height restoration. There needle placement is critical with the use of
may be certain anatomical configurations in the omni-planar fluoroscopic imaging.
fracture that predispose to adjacent-level fracture, • Injection of PMMA must be done slowly and
such as intra-osseous clefts [35]. Also, certain carefully using a viscous opacified cement mixture
patient populations may be at higher risk for to avoid extravasation or halt injection promptly
future fractures, including those with osteoporo- upon extravasation.
sis, previous vertebral fracture, and organ trans- • Over-injection of PMMA should be avoided,
plant recipients. [36,37]. It must be noted that in particularly with respect to the posterior corti-
all series examining this phenomenon (including cal wall/spinal canal region.
our own), outcomes of pain relief following PV or • Any neurologic abnormality postprocedurally
PK for the adjacent level fracture are excellent mandates a careful evaluation, including consid-
(data in submission). eration of prompt CT to define the PMMA
injection in three dimensions and guide poten-
Vertebroplasty vs Kyphoplasty tial therapeutic options including surgical
Both PV and PK have been shown to be effective decompression.
to reduce the pain associated with VCFs. These
procedures both have low complication rates and
Conclusions
tend to have islands of supporters, i.e., clinicians
who always favor one over the other regardless of PV and PK are minimally invasive techniques used
clinical circumstances. No head-to-head compara- to treat painful VCFs. There is a growing body of
Vertebroplasty and Kyphoplasty: Complications and Prevention S63
evidence, albeit of limited quality—predominately vertebroplasty with acrylic cement. Neurochirurgie
open case series—which indicates that these pro- 1987;33:166–8.
cedures are efficacious in alleviating the pain asso- 3 Jensen ME, Evans AJ, Mathis JM, et al. Percutane-
ciated with VCF. The results of the procedures ous polymethylmethacrylate vertebroplasty in the
treatment of osteoporotic vertebral body compres-
Downloaded from https://academic.oup.com/painmedicine/article-abstract/9/suppl_1/S58/1825158 by KERIS National Access user on 28 January 2020
in these numerous reports are uniformly good.
sion fractures: Technical aspects. Am J Neuroradiol
There are, however, a growing number of case 1997;18(10):1897–904.
reports of serious complications. 4 Kaemmerlen P, Thiesse P, Jonas P, et al. Percuta-
Recent reviews and editorials have called for a neous injection of orthopedic cement in meta-
more critical evaluation of these procedures. Watts static vertebral lesions. N Engl J Med 1989;321(2):
and colleagues reviewed the literature, concluding 121.
that controlled multicenter trials are needed to 5 Lieberman IH, Dudeney S, Reinhardt MK, Bell G.
determine the short- and long-term safety [39]. Initial outcome and efficacy of “kyphoplasty” in the
Garfin and colleagues concluded that there is treatment of painful osteoporotic vertebral com-
a 95% improvement in pain and significant pression fractures. Spine 2001;26(14):1631–8.
improvement in function following these proce- 6 Maynard AS, Jensen ME, Schweickert PA, et al.
Value of bone scan imaging in predicting pain relief
dures [40]. They emphasized that the procedure is
from percutaneous vertebroplasty in oseoporotic
technically demanding, with the potential for sig- vertebral fractures. Am J Neuroradiol 2000;21(10):
nificant complications. They recommended 1807–12.
further efficacy and safety studies. Jarvik and Deyo 7 McKiernan F, Faciewski T, Jensen R. Quality of life
called for randomized controlled trials (RCTs) or following vertebroplasty. J Bone Joint Surg 2004;
some type of control cohort to compare long term 86:2600–6.
outcomes carefully [41]. Einhorn calls for careful 8 McGraw JK, Cardella J, Barr JD, et al. Society of
monitoring of outcomes and minimal training Interventional Radiology quality improvement
standards [42]. Birkmeyer calls for randomized guidelines for percutaneous vertebroplasty. J Vasc
clinical trials, citing insufficient evidence via Interv Radiol 2003;14(9):s311–5.
case series to prove safety, efficacy, and cost- 9 Lee BJ, Lee SR, Yoo TY. Paraplegia as a complica-
tion of percutaneous vertebroplasty with polymeth-
effectiveness [43].
ylmethacryalte: A case report. Spine 2002;27(19):
It will be difficult to conduct the RCTs needed to E419–22.
compare short- and long-term outcomes of PV 10 Ratliff J, Nguyen T, Heiss J. Root and spinal cord
and/or PK vs more conservative therapies. These compression from methymethacrylate vertebro-
procedures have gained such widespread popularity plasty. Spine 2001;26(13):E300–2.
that patients would undoubtedly resist being ran- 11 Jang JS, Lee SH, Jung SK. Pulmonary embolism of
domized to the conservative treatment group, and polymethymethacrylate after percutanous vertebro-
recent attempts at RCTs for PV have been plagued plasty: A report of three cases. Spine 2002;27(19):
by low enrollment. Blinding would be impossible, E416–8.
as pain relief is usually dramatic and prompt. Other 12 Tozzi P, Abdelmoumene Y, Corno AF, et al. Man-
studies need to be done to compare PV and PK in agement of pulmonary embolism during acrylic ver-
tebroplasty. Ann Thorac Surg 2002;74(5):1706–8.
various disease states in a randomized fashion.
13 Chen HL, Wong CS, Ho ST, et al. lethal pulmo-
Early studies are underway to evaluate biologic nary embolism during percutaneous vertebroplasty.
materials for spinal injection rather than acrylic Anesth Analg 2002;95(4):1060–2.
(PMMA). In spite of the need for more research, 14 Scroop R, Eskridge J, Britz GW. Paradoxical
PV and PK have shown great promise in the treat- cerebral arterial embolization of cement during
ment of painful VCFs due to a variety of different intraoperative vertebroplasty: Case report. Am J
pathologic states. With careful patient selection, Neuroradiol 2002;23(5):868–70.
adequate training, and attention to detail during 15 Phillips FM, Wetzel FT, Lieberman I, Campbell-
the procedure, serious complications are rare. Hupp M. An in vivo comparison of the potential for
extravertebral cement leak after vertebroplasty and
kyphoplasty. Spine 2002;27(19):2173–8.
References
16 Walker DH, Mummaneni P, Rodts GE. Infected
1 Charnley J. The reaction of bone to self-curing vertebroplasty report of two cases and review of
acrylic cement. A long-term histological study in the literature. Neurosurg Focus 2004;17(6):E6.
man. J Bone Surg Br 1970;52:340–53. 17 Nussbaum DA, Gailloud P, Murphy K. A review of
2 Gailbert P, Deramond H, Rosat P, Le Gars D. A complications associated with vertebroplasty and
method for certain spinal angiomas: Percutaneous kyphoplasty as reported to the food and drug
S64 Burton
administration medical device web site. J Vasc Interv kyphoplasty performed at a cancer center: Refuting
Radiol 2004;15:1185–92. proposed contraindications. J Neurosurg Spine
18 McGraw JK, Cardella J, Barr JD, et al. Society of 2005;2(4):436–40.
Interventional Radiology quality improvement 31 Burton AW, Reddy SK, Shah HN, Tremont-Lukats
guidelines for percutaneous vertebroplasty. J Vasc I, Mendel E. Percutaneous vertebroplasty—a tech-
Downloaded from https://academic.oup.com/painmedicine/article-abstract/9/suppl_1/S58/1825158 by KERIS National Access user on 28 January 2020
Interv Radiol 2003;14:827–31. nique to treat refractory spinal pain in the setting of
19 Gangi A, Sabharwal T, Irani FG, et al. Guidelines advanced metastatic cancer: A case series. J Pain
for percutaneous vertebroplasty. Cardiovasc Inter- Symptom Manag 2005;30(1):87–95.
vent Radiol 2006;29:173–8. 32 Fribourg D, Tang C, Sra P, Delamarter R, Bae H.
20 Gaughen JR, Jensen ME, Schweikert PA, et al. Rel- Incidence of subsequent vertebral fracture after
evance of antecedent venography in percutaneous kyphoplasty. Spine 2004;29(20):2270–6.
vertebroplasty for the treatment of osteoporotic 33 Trout AT, Kallmes DF, Kaufmann TJ. New frac-
compression fractures. Am J Neuroradiol 2002; tures after vertebroplasty: adjacent fractures occur
23(4):594–600. significantly sooner. Am J Neuroradiol 2006;27(1):
21 Vasconcelos C, Gailloud P, Beauchamp NJ, Heck 217–23.
DV, Murphy KJ. Is percutaneous vertebroplasty 34 Kim SH, Kang HS, Choi JA, Ahn JM. Risk factors
without pretreatment venography safe? Evaluation of new compression fractures in adjacent vertebrae
of 205 consecutive procedures. Am J Neuroradiol after percutaneous vertebroplasty. Acta Radiol
2002;23(6):913–7. 2004;45:440–5.
22 Fourney DR, Schomer DF, Nader R, et al. Percute- 35 Trout AT, Kallmes DF, Lane JI, Layton KF, Marx
neous vertebroplasty and kyphoplasty for painful WF. Subsequent vertebral fractures after vertebro-
vertebral body fractures in cancer patients. J Neu- plasty: association with intraosseous clefts. Am J
rosurg Spine 2003;98:21–30. Neuroradiol 2006;27(7):1586–91.
23 Laredo JD, Hamze B. Complications of percutane- 36 Lindsay R, Silverman SL, Cooper C, et al. Risk of
ous vertebroplasty and their prevention. Semin vertebral compression fracture in the year following
Ultrasound CT MR 2005;26(2):65–80. a fracture. JAMA 2001;285(3):320–3.
24 Burton AW, Rhines LD, Mendel E. Vertebroplasty 37 Deen HG, Aranda-Michel J, Reimer R, Miller DA,
and kyphoplasty: A comprehensive review. Neuro- Putzke JD. Balloon kyphoplasty for vertebral com-
surg Focus 2005;18(3):e1. pression fractures in solid organ transplant recipi-
25 Chung SK, Lee SH, Kim DY, Lee HY. Treatment ents: results of treatment and comparison with
of lower lumbar radiculopathy caused by primary vertebral compression fractures. Spine J
osteoporotic compression fracture: The role of ver- 2006;6(5):494–9.
tebroplasty. J Spinal Disord Tech 2002;15(6):461–8. 38 Deramond H, Saliou G, Aveillan M, Lehmann P,
26 Nakano M, Hirano N, Matsuura K, et al. Percuta- Vallee JN. Respective contributions of vertebro-
neous transpedicular vertebroplasty with calcium plasty and kyphoplasty to the management of
phosphate cement in the treatment of osteoporotic osteoporotic vertebral fractures. Joint Bone Spine
vertebral compression and burst fractures. J Neuro- 2006;73(6):610–3.
surg 2002;97(3):287–93. 39 Watts NB, Harris ST, Genant HK. Treatment of
27 Peh WCG, Gilula LA, Peck DD. Percutaneous painful osteoporotic vertebral compression fractures
vertebroplasty for severe osteoporootic vertebral with percutaneous vertebroplasty or kyphoplasty.
body compression fractures. Radiology 2002;223(1): Osteoporos Int 2001;12(6):429–37.
121–6. 40 Garfin SR, Yuan HA, Reiley MA. Kyphoplasty and
28 Wetzel SG, Martin JB, Somon T, Wilhelm K, vertebroplasty for the treatment of painful osteopo-
Rufenacht DA. Painful osteolytic matastasis of the rotic compression fractures. Spine 2001;26:1511–5.
atlas: Treatment with percutenous vertebroplasty. 41 Jarvik JG Deyo RA. Cementing the evidence: Time
Spine 2002;27(22):e493–5. for a randomized trial of vertebroplasty. Am J
29 Sarzier JS, Evans AJ, Cahill DW. Increased pedicle Neuroradiol 2000;21:1373–4.
screw pullout strength with vertebroplasty augmen- 42 Einhorn TA. Vertebroplasty: An opportunity to do
tation in osteoporotic spines. J Neurosurg 2002; something really good for patients. Spine 2000;
96(suppl. 3):309–12. 25(9):1051–2.
30 Hentschel SJ, Burton AW, Fourney DR, Rhines 43 Birkmeyer N. Point of view. Spine 2001;26:
LD, Mendel E. Percutaneous vertebroplasty and 1637–8.
You might also like
- J Neurol Sci (Turk)Document9 pagesJ Neurol Sci (Turk)nulaeli Siti ANo ratings yet
- Lessons Learned: Trapeziectomy and Suture Suspension Arthroplasty For Thumb Carpometacarpal OsteoarthritisDocument7 pagesLessons Learned: Trapeziectomy and Suture Suspension Arthroplasty For Thumb Carpometacarpal Osteoarthritiszakaria ramdaniNo ratings yet
- Raval PDFDocument5 pagesRaval PDFdebby claudiNo ratings yet
- Treatment of Pathological Fractures Due To Simple Bone Cysts by Extended Curettage Grafting and Intramedullary DecompressionDocument9 pagesTreatment of Pathological Fractures Due To Simple Bone Cysts by Extended Curettage Grafting and Intramedullary DecompressionHendra AjahNo ratings yet
- Case Series of All-Arthroscopic Treatment For Terrible Triad of The Elbow: Indications and Clinical OutcomesDocument10 pagesCase Series of All-Arthroscopic Treatment For Terrible Triad of The Elbow: Indications and Clinical OutcomesdorfynatorNo ratings yet
- Case Report Traumatic Fracture: Dislocation of Cervicothoracic Junction - Grand Round Presentation of C7-T1 Instabilities and Different Instrumentation TechniquesDocument6 pagesCase Report Traumatic Fracture: Dislocation of Cervicothoracic Junction - Grand Round Presentation of C7-T1 Instabilities and Different Instrumentation TechniquesMohammad Al-SofyaniNo ratings yet
- Sicotj160057 PDFDocument6 pagesSicotj160057 PDFDr'Dinesh MishraNo ratings yet
- Moderator:Dr Vijay Kumar Co-Moderator:Dr Venketish All India Institute of Medical Sciences New DelhiDocument58 pagesModerator:Dr Vijay Kumar Co-Moderator:Dr Venketish All India Institute of Medical Sciences New DelhiWasim R. IssaNo ratings yet
- Pi Is 0363502317302241Document5 pagesPi Is 0363502317302241ashik MohamedNo ratings yet
- Atraumatic Cuff TearsDocument7 pagesAtraumatic Cuff Tearschandan noelNo ratings yet
- MontotenniselbowDocument7 pagesMontotenniselbowPURVA THAKURNo ratings yet
- External Fixation of Tibia Fractures: RequireDocument1 pageExternal Fixation of Tibia Fractures: RequireCraciun Ana-MariaNo ratings yet
- Bone Healing Induced by ESWTDocument4 pagesBone Healing Induced by ESWTDyah SafitriNo ratings yet
- Accepted Manuscript: Current Problems in Diagnostic RadiologyDocument54 pagesAccepted Manuscript: Current Problems in Diagnostic RadiologyMur murNo ratings yet
- Clinical Case Reports - 2020 - Thompson - Superior Gluteal Nerve Injury Following Landmark Guided Corticosteroid InjectionDocument3 pagesClinical Case Reports - 2020 - Thompson - Superior Gluteal Nerve Injury Following Landmark Guided Corticosteroid InjectionGunnar LarssonNo ratings yet
- Posterior Surgical Approach For Thoracic Burst Fracture And Spinal Cord InjuryDocument11 pagesPosterior Surgical Approach For Thoracic Burst Fracture And Spinal Cord Injurybosnia agusNo ratings yet
- Ankle Arthrodesis After Severe InfectionDocument5 pagesAnkle Arthrodesis After Severe InfectionSeagate PramonoNo ratings yet
- New Trends and Techniques in Open Reduction and Internal Fixation of Fractures of The Tibial PlateauDocument8 pagesNew Trends and Techniques in Open Reduction and Internal Fixation of Fractures of The Tibial PlateauCosmina BribanNo ratings yet
- Comparing Erector Spinae Plane Block With Serratus Anterio - 2020 - British JourDocument9 pagesComparing Erector Spinae Plane Block With Serratus Anterio - 2020 - British JourtasyadelizaNo ratings yet
- Intertan Nail Vs PFN ADocument7 pagesIntertan Nail Vs PFN AzubayetarkoNo ratings yet
- CT Scan Sacrum & CoccyxDocument6 pagesCT Scan Sacrum & CoccyxFaisal Akbar Asaristiwa100% (1)
- Boissonneault2019 PDFDocument17 pagesBoissonneault2019 PDFBangkit PrimayudhaNo ratings yet
- Management of The Mangled ExtremityDocument10 pagesManagement of The Mangled ExtremityosteonectinNo ratings yet
- Kneemliinjuries: Common Problems and SolutionsDocument11 pagesKneemliinjuries: Common Problems and SolutionsHenry CollazosNo ratings yet
- Semiconstrained Total Elbow Arthroplasty-1Document6 pagesSemiconstrained Total Elbow Arthroplasty-1Ευαγγελια ΚιμπαρηNo ratings yet
- Spinal Cord Compression Due To Undiagnosed Thoracic Meningioma Following Lumbar Surgery in An Elderly Patient: A CaseDocument4 pagesSpinal Cord Compression Due To Undiagnosed Thoracic Meningioma Following Lumbar Surgery in An Elderly Patient: A CaseLuwiNo ratings yet
- 1005-04eDocument6 pages1005-04eHitham El ShahatNo ratings yet
- Analysis of Risk Factors For New Vertebral Fracture After Percutaneous VertebroplastyDocument7 pagesAnalysis of Risk Factors For New Vertebral Fracture After Percutaneous VertebroplastyCecilia Suarez HerreraNo ratings yet
- 10 The Use of Tecartherapy in Ankle Sprain TraumasDocument5 pages10 The Use of Tecartherapy in Ankle Sprain TraumasSilvia PluisNo ratings yet
- Fraktur FemurDocument11 pagesFraktur FemurYusuf BrilliantNo ratings yet
- ET 7. Predictors of Compartment Syndrome After Tibial Fracture. JOT. 2015Document5 pagesET 7. Predictors of Compartment Syndrome After Tibial Fracture. JOT. 2015Flavia Rodríguez BracamonteNo ratings yet
- Fraktur FrakDocument11 pagesFraktur FrakRirin SeptianiNo ratings yet
- Anterior Cervicothoracic Corpectomy Via Cervical ApproachDocument6 pagesAnterior Cervicothoracic Corpectomy Via Cervical ApproachSadashivayya SoppimathNo ratings yet
- ESWT - Current Evidence Bone 2010Document5 pagesESWT - Current Evidence Bone 2010eredaronline1No ratings yet
- Treatment of Tibial Plateau Fractures Dual Plating Dual IncisionDocument6 pagesTreatment of Tibial Plateau Fractures Dual Plating Dual IncisionAnnie JoNo ratings yet
- Morbidity and Total Knee Arthroplasty As A Long Term Sequela of Tibial Plateau FracturesDocument8 pagesMorbidity and Total Knee Arthroplasty As A Long Term Sequela of Tibial Plateau FracturesAthenaeum Scientific PublishersNo ratings yet
- Distal Humeral Fractures-Current Concepts PDFDocument11 pagesDistal Humeral Fractures-Current Concepts PDFRina AlvionitaNo ratings yet
- Treatment of Thoracolumbar FractureDocument14 pagesTreatment of Thoracolumbar FractureLaela LathifatunNo ratings yet
- Oncologi NursingDocument15 pagesOncologi NursingKogilla VaniNo ratings yet
- Effectiveness of Arthroscopic Decompression in The Treatment of Anterolateral Ankle Impingement Syndrome A Systematic Literature ReviewDocument5 pagesEffectiveness of Arthroscopic Decompression in The Treatment of Anterolateral Ankle Impingement Syndrome A Systematic Literature ReviewInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Acta 88 118Document11 pagesActa 88 118darshan tatiaNo ratings yet
- Clinical Analysis of The Frosch Approach in The Treatment of Posterolateral Tibial Plateau Fractures Combined With Lateral Tibial Plateau FracturesDocument11 pagesClinical Analysis of The Frosch Approach in The Treatment of Posterolateral Tibial Plateau Fractures Combined With Lateral Tibial Plateau FracturesraynaldidjohariofcNo ratings yet
- 2019 Article 2632analisis TomograficoDocument6 pages2019 Article 2632analisis TomograficoLenin EstrellaNo ratings yet
- Clinical Outcome of A Precontoured Symphysis Pubis Plate With Tension Band Wiring For Traumatic Symphysis Pubis Rupture in Pelvic FracturesDocument6 pagesClinical Outcome of A Precontoured Symphysis Pubis Plate With Tension Band Wiring For Traumatic Symphysis Pubis Rupture in Pelvic FracturesodyNo ratings yet
- Articulo Publicado 3 Karina PortilloDocument4 pagesArticulo Publicado 3 Karina PortilloKarina PortilloNo ratings yet
- Jain Extrapleural ApproachDocument5 pagesJain Extrapleural ApproachOj AlimbuyuguenNo ratings yet
- Surgical Management of Posterior Ligament Complex Stri 2024 International JoDocument5 pagesSurgical Management of Posterior Ligament Complex Stri 2024 International JoRonald QuezadaNo ratings yet
- J Surneu 2005 04 039Document7 pagesJ Surneu 2005 04 039MohitNo ratings yet
- Talar Body Fracture Case in 10-Year-Old BoyDocument6 pagesTalar Body Fracture Case in 10-Year-Old BoyPoliceNo ratings yet
- The Effectiveness and Safety of General and Spinal Anesthesia On Systemic Inflammatory Response in Patients With Tumor-Type Total Knee ArthroplastyDocument6 pagesThe Effectiveness and Safety of General and Spinal Anesthesia On Systemic Inflammatory Response in Patients With Tumor-Type Total Knee Arthroplastyjean carlo ulloa velaNo ratings yet
- Stabilization of Distal Humerus Fractures by Precontoured Bi-Condylar Plating in A 90-90 PatternDocument5 pagesStabilization of Distal Humerus Fractures by Precontoured Bi-Condylar Plating in A 90-90 PatternmayNo ratings yet
- Trauma Case Reports: Jugert Bango, Evan Zhang, Daniel L. Aaron, Amna DiwanDocument4 pagesTrauma Case Reports: Jugert Bango, Evan Zhang, Daniel L. Aaron, Amna DiwanCristhian Jover CastroNo ratings yet
- Fuchs 2005Document5 pagesFuchs 2005BudhiNo ratings yet
- TotalHip PDFDocument11 pagesTotalHip PDFLoredanaNovacNo ratings yet
- 2023 TrungluDocument9 pages2023 Trungludr.speleologNo ratings yet
- ELECTROACUPUNCTURE FOR ALLEVIATION OF PHANTOM LIMB PAIN : Case ReportDocument5 pagesELECTROACUPUNCTURE FOR ALLEVIATION OF PHANTOM LIMB PAIN : Case ReportrezteevicNo ratings yet
- Pathophysiology: Laboratory StudiesDocument8 pagesPathophysiology: Laboratory Studiesrahma perwitasariNo ratings yet
- Posterolateral Approach For Posterior Malleolus FiDocument12 pagesPosterolateral Approach For Posterior Malleolus FiorlanquisNo ratings yet
- Metastase Bone DiseaseDocument20 pagesMetastase Bone DiseasedrkurniatiNo ratings yet
- Metastatic Spine Disease: A Guide to Diagnosis and ManagementFrom EverandMetastatic Spine Disease: A Guide to Diagnosis and ManagementRex A. W. MarcoNo ratings yet
- Soil-Transmitted Helminth Infection and Eosinophil Level Among Waste Collectors in Banda AcehDocument8 pagesSoil-Transmitted Helminth Infection and Eosinophil Level Among Waste Collectors in Banda AcehChristopherLawrenceNo ratings yet
- Soil-Transmitted Helminth Infection and Eosinophil Level Among Waste Collectors in Banda AcehDocument8 pagesSoil-Transmitted Helminth Infection and Eosinophil Level Among Waste Collectors in Banda AcehChristopherLawrenceNo ratings yet
- Quick Reference Guide: Ws4U Back FrontDocument2 pagesQuick Reference Guide: Ws4U Back FrontChristopherLawrenceNo ratings yet
- Volume 9 No 1Document94 pagesVolume 9 No 1ChristopherLawrenceNo ratings yet
- Deteksi Dini Skoliosis Di Tingkat Sekolah Dasar Katolik Santo Yoseph 2Document5 pagesDeteksi Dini Skoliosis Di Tingkat Sekolah Dasar Katolik Santo Yoseph 2Baguus Setya AditamaNo ratings yet
- Osteoporotic Vertebral Compression Fracture - TreaDocument4 pagesOsteoporotic Vertebral Compression Fracture - TreaChristopherLawrenceNo ratings yet
- 12 Week Stair Jumping Program Mar 2010Document18 pages12 Week Stair Jumping Program Mar 2010Brito KevinNo ratings yet
- Osteoporotic Vertebral Compression Fractures and VDocument13 pagesOsteoporotic Vertebral Compression Fractures and VChristopherLawrenceNo ratings yet
- FrontDocument3 pagesFrontChristopherLawrenceNo ratings yet
- Surgery:: A Case Report For A Mortality Following Kyphoplasty: Suggested Method of PreventionDocument3 pagesSurgery:: A Case Report For A Mortality Following Kyphoplasty: Suggested Method of PreventionChristopherLawrenceNo ratings yet
- 12 Week Stair Jumping Program Mar 2010Document18 pages12 Week Stair Jumping Program Mar 2010Brito KevinNo ratings yet
- The NBA and Youth Basketball Recommendations For PDocument13 pagesThe NBA and Youth Basketball Recommendations For PChristopherLawrenceNo ratings yet
- AAOS 2018 Foot and Ankle - by KhawajaDocument108 pagesAAOS 2018 Foot and Ankle - by KhawajaChristopherLawrenceNo ratings yet
- 12 Week Stair Jumping Program Mar 2010Document18 pages12 Week Stair Jumping Program Mar 2010Brito KevinNo ratings yet
- AAOS 2018 Basic Science - by KhawajaDocument75 pagesAAOS 2018 Basic Science - by KhawajaChristopherLawrenceNo ratings yet
- Knee Injury and Osteoarthritis Outcome Score Koos PDFDocument4 pagesKnee Injury and Osteoarthritis Outcome Score Koos PDFNuruel Thamie PoethreeNo ratings yet
- DASH Questionnaire Disability Arm Shoulder HandDocument3 pagesDASH Questionnaire Disability Arm Shoulder HandChristopherLawrenceNo ratings yet
- DASH Questionnaire Disability Arm Shoulder HandDocument3 pagesDASH Questionnaire Disability Arm Shoulder HandChristopherLawrenceNo ratings yet
- Soal TO 1 Padi November 2017 PDFDocument41 pagesSoal TO 1 Padi November 2017 PDFChristopherLawrenceNo ratings yet
- Reverensi Kuisioner Oswestry PDFDocument3 pagesReverensi Kuisioner Oswestry PDFagungary95No ratings yet
- (Journal PDFDocument8 pages(Journal PDFChristopherLawrenceNo ratings yet
- DASH Questionnaire Disability Arm Shoulder HandDocument3 pagesDASH Questionnaire Disability Arm Shoulder HandChristopherLawrenceNo ratings yet
- Abstracts of The 2018 AANS/CNS Joint Section On Disorders of The Spine and Peripheral Nerves Annual MeetingDocument109 pagesAbstracts of The 2018 AANS/CNS Joint Section On Disorders of The Spine and Peripheral Nerves Annual MeetingEka Wahyu HerdiyantiNo ratings yet
- Solomon, Olivia Feriña N. Osmak Ortho Rota8On March 9,2021: Compression FractureDocument3 pagesSolomon, Olivia Feriña N. Osmak Ortho Rota8On March 9,2021: Compression FractureOlivia SolomonNo ratings yet
- Management of Metastatic Spinal Cord Compression: Southern Medical Journal September 2017Document9 pagesManagement of Metastatic Spinal Cord Compression: Southern Medical Journal September 2017Rudy Arindra WijayaNo ratings yet
- PMMA - An Essential Material in Medicine and DentistryDocument12 pagesPMMA - An Essential Material in Medicine and Dentistryr2201cNo ratings yet
- New Symptomatic Compression Fracture After Percutaneous Vertebroplasty at The Thoracolumbar JunctionDocument4 pagesNew Symptomatic Compression Fracture After Percutaneous Vertebroplasty at The Thoracolumbar JunctionRamy ElmasryNo ratings yet
- Effects On Inadvertent Endplate Fracture Following Lateral Cage Placement On Range of Motion and Indirect Spine Decompression in Lumbar Spine Fusion Constructs: A Cadaveric StudyDocument8 pagesEffects On Inadvertent Endplate Fracture Following Lateral Cage Placement On Range of Motion and Indirect Spine Decompression in Lumbar Spine Fusion Constructs: A Cadaveric Studysiti hanifahNo ratings yet
- Comfort nursing relieves pain and improves ability after spine surgeryDocument8 pagesComfort nursing relieves pain and improves ability after spine surgeryBella FebriantiNo ratings yet
- Osteoporotic Vertebral Compression Fracture - TreaDocument4 pagesOsteoporotic Vertebral Compression Fracture - TreaChristopherLawrenceNo ratings yet
- 9 - Sacral Insufficiency Fracture Repair-SacroplastyDocument7 pages9 - Sacral Insufficiency Fracture Repair-SacroplastySoumabho DasNo ratings yet
- Fajo 990Document238 pagesFajo 990Mohamed A SalehNo ratings yet
- Osteoporosis and Fragility Fractures Surgical PerpspectiveDocument54 pagesOsteoporosis and Fragility Fractures Surgical PerpspectiveSonal DudaniNo ratings yet
- Surgical Treatment of Severe Osteoporosis Includin-DikonversiDocument6 pagesSurgical Treatment of Severe Osteoporosis Includin-DikonversikhairaniNo ratings yet
- Height of The Anterior Wall. Normal Trabecular Structure.: Fig. 1 Osteoporotic Fracture by Compression With Loss ofDocument9 pagesHeight of The Anterior Wall. Normal Trabecular Structure.: Fig. 1 Osteoporotic Fracture by Compression With Loss ofNyoman InsanNo ratings yet
- Osteoporosis Diagnosis & Management: DR Aditya Kundu JR1 Department of Orthopedics, CNMC&HDocument53 pagesOsteoporosis Diagnosis & Management: DR Aditya Kundu JR1 Department of Orthopedics, CNMC&HAditya KunduNo ratings yet
- Classification of Compression FracturesDocument6 pagesClassification of Compression FracturesKaustubh KeskarNo ratings yet
- Lsrs Meeting Program 2017-2018 PDFDocument265 pagesLsrs Meeting Program 2017-2018 PDFSulaiman SomaniNo ratings yet
- SPINE EU ENG ITA REV 07 31 05 2022 - Compressed 1Document32 pagesSPINE EU ENG ITA REV 07 31 05 2022 - Compressed 1Guo KangNo ratings yet
- Injectable Functional Biomaterials For Minimally Invasive SurgeryDocument20 pagesInjectable Functional Biomaterials For Minimally Invasive Surgery서지영No ratings yet
- Multiple Choice Questions on Abdominal Pain, Awake Intubation, and Airway TrainingDocument7 pagesMultiple Choice Questions on Abdominal Pain, Awake Intubation, and Airway TrainingAhmed Ben BellaNo ratings yet
- C4 AuthDocument3 pagesC4 AuthijustwanawriteNo ratings yet
- Assessing Bias The Importance of Considering ConfoundingDocument4 pagesAssessing Bias The Importance of Considering ConfoundingAndrieli TodescatoNo ratings yet
- Occipitocervical Instability & DislocationDocument205 pagesOccipitocervical Instability & DislocationM Ivan Pratama ZebuaNo ratings yet
- Most Common CPT CodesDocument5 pagesMost Common CPT CodesKrishna KumarNo ratings yet
- Musculoskeletal 20,000 Series CPT Questions With Answers-CpcDocument16 pagesMusculoskeletal 20,000 Series CPT Questions With Answers-Cpcanchalnigam25100% (7)
- Is Calcium Phosphate Augmentation A Viable Option For Osteoporotic Hip Fractures?Document8 pagesIs Calcium Phosphate Augmentation A Viable Option For Osteoporotic Hip Fractures?Santiago MartinezNo ratings yet
- Patient Escort Program Goals: ObjectivesDocument4 pagesPatient Escort Program Goals: ObjectivesKhafidzul Fiqih Reviyant TohaNo ratings yet
- Osteoporosis 2020Document46 pagesOsteoporosis 2020Angélica Montañez Robledo100% (1)
- VertoCure PDFDocument16 pagesVertoCure PDFMostafa ElgendyNo ratings yet
- Spinal SurgeryDocument19 pagesSpinal SurgerySalomeSibashviliNo ratings yet
- Advanced Cancer. Pain and Quality of LifeDocument356 pagesAdvanced Cancer. Pain and Quality of Lifestrahiltodorov100% (1)