Professional Documents
Culture Documents
ID 3rd LE PDF
Uploaded by
Jolaine ValloOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
ID 3rd LE PDF
Uploaded by
Jolaine ValloCopyright:
Available Formats
976 (e.g.
(e.g., spinal cord–injured persons) to prevent both infectious and in chronic interstitial nephritis; the primary etiologic factors in this
anatomic complications. condition are analgesic abuse, obstruction, reflux, and toxin expo-
sure. In the presence of underlying renal abnormalities (particularly
CANDIDURIA obstructing stones), infection as a secondary factor can accelerate renal
The appearance of Candida in the urine is an increasingly com- parenchymal damage. In spinal cord–injured patients, use of a long-
mon complication of indwelling catheterization, particularly for term indwelling bladder catheter is a well-documented risk factor for
patients in the intensive care unit, those taking broad-spectrum bladder cancer. Chronic bacteriuria resulting in chronic inflammation
antimicrobial drugs, and those with underlying diabetes mellitus. is one possible explanation for this observation.
In many studies, >50% of urinary Candida isolates have been found
to be non-albicans species. The clinical presentation varies from a ■ FURTHER READING
laboratory finding without symptoms to pyelonephritis and even Bent S et al: Does this woman have acute uncomplicated urinary tract
sepsis. Removal of the urethral catheter results in resolution of can- infection? JAMA 287:2701, 2002.
diduria in more than one-third of asymptomatic cases. Treatment of Grigoryan L et al: Urinary tract infections in young adults. JAMA
asymptomatic patients does not appear to decrease the frequency 312:1677, 2014.
of recurrence of candiduria. Therapy is recommended for patients Gupta K et al: International clinical practice guidelines for the treat-
who have symptomatic cystitis or pyelonephritis and for those who ment of acute uncomplicated cystitis and pyelonephritis in women:
are at high risk for disseminated disease. High-risk patients include A 2010 update by the Infectious Diseases Society of America and
those with neutropenia, those who are undergoing urologic manip- the European Society for Microbiology and Infectious Diseases. Clin
ulation, those who are clinically unstable, and low-birth-weight Infect Dis 52:e103, 2011.
infants. Fluconazole (200–400 mg/d for 7–14 days) reaches high Hooton TM et al: Diagnosis, prevention, and treatment of catheter-
levels in urine and is the first-line regimen for Candida infections associated urinary tract infection in adults: 2009 international clinical
of the urinary tract. Although instances of successful eradication practice guidelines from the Infectious Diseases Society of America.
of candiduria by some of the newer azoles and echinocandins have Clin Infect Dis 50:625, 2010.
been reported, these agents are characterized by only low-level uri- Hooton TM et al: Voided midstream urine culture and acute cystitis in
nary excretion and thus are not recommended. For Candida isolates premenopausal women. N Engl J Med 369; 1883, 2013.
with high levels of resistance to fluconazole, oral flucytosine and/ Nicolle LE et al: Infectious Diseases Society of America guidelines for
or parenteral amphotericin B are options. Bladder irrigation with the diagnosis and treatment of asymptomatic bacteriuria in adults.
amphotericin B generally is not recommended. Clin Infect Dis 40:643, 2005.
PART 5
■ PREVENTION OF RECURRENT UTI IN WOMEN
Recurrence of uncomplicated cystitis in reproductive-age women is
common, and a preventive strategy is indicated if recurrent UTIs are
interfering with a patient’s lifestyle. The threshold of two or more
131 Sexually Transmitted
Infections: Overview
Infectious Diseases
symptomatic episodes per year is not absolute; decisions about inter-
ventions should take the patient’s preferences into account. and Clinical Approach
Three prophylactic strategies are available: continuous, postcoital,
Jeanne M. Marrazzo, King K. Holmes
and patient-initiated therapy. Continuous prophylaxis and postcoital
prophylaxis usually entail low doses of TMP-SMX, a fluoroquinolone,
or nitrofurantoin. These regimens are all highly effective during the
period of active antibiotic intake. Typically, a prophylactic regimen CLASSIFICATION AND EPIDEMIOLOGY
is prescribed for 6 months and then discontinued, at which point the Worldwide, most adults acquire at least one sexually transmitted
rate of recurrent UTI often returns to baseline. If bothersome infections infection (STI), and many remain at risk for complications. Each day,
recur, the prophylactic program can be reinstituted for a longer period. for example, more than 1 million STIs are acquired worldwide, placing
Selection of resistant strains in the fecal flora has been documented in many affected persons at risk for adverse reproductive health outcomes
studies of women taking prophylactic antibiotics for 12 months. and neoplasia. Certain STIs, such as syphilis, gonorrhea, HIV infection,
Patient-initiated therapy involves supplying the patient with materi- hepatitis B, and chancroid, often occur in highly interconnected sexual
als for urine culture and with a course of antibiotics for self-medication networks characterized by high rates of partner change or multiple
at the first symptoms of infection. The urine culture is refrigerated and concurrent partners. Such networks, for example, often include per-
delivered to the physician’s office for confirmation of the diagnosis. sons who engage in transactional sex, men who have sex with men
When an established and reliable patient–provider relationship exists, (MSM), and persons involved in the use of illicit drugs, particularly
the urine culture can be omitted as long as the symptomatic episodes methamphetamine. Other STIs are distributed more evenly throughout
respond completely to short-course therapy and are not followed by populations. For example, chlamydial infections, genital human papil-
relapse. lomavirus (HPV) infections, and genital herpes can spread efficiently
Non-antimicrobial prevention is increasingly being studied. Lacto- even in relatively low-risk populations. Finally, modern technologies
bacillus probiotics are one appealing approach to UTI prevention, but based on detection of nucleic acid have accelerated elucidation of the
there is a paucity of data to support this strategy. Similarly, studies of role of sexual transmission in the spread of some viruses, including
cranberry products for UTI prevention have produced mixed results. Ebola virus and Zika virus, and have provided new evidence of appar-
Varied dosing and product composition between studies remains an ent sexual transmission of several bacteria, including group C Neisseria
issue for providing clinical guidance. meningitidis and anaerobes associated with bacterial vaginosis (BV).
In general, the product of three factors determines the initial rate of
■ PROGNOSIS spread of any STI within a population: rate of sexual exposure of sus-
Cystitis is a risk factor for recurrent cystitis and pyelonephritis. ASB ceptible to infectious people, efficiency of transmission per exposure,
is common among elderly and catheterized patients but does not in and duration of infectivity of those infected. Accordingly, efforts to
itself increase the risk of death. The relationships among recurrent UTI, prevent and control STIs aim to decrease the rate of sexual exposure
chronic pyelonephritis, and renal insufficiency have been widely stud- of susceptible to infected persons (e.g., through education and efforts
ied. In the absence of anatomic abnormalities such as reflux, recurrent to change sexual behavior norms and through control efforts aimed
infection in children and adults does not lead to chronic pyelonephritis at reducing the proportion of the population infected); to decrease
or to renal failure. Moreover, infection does not play a primary role the duration of infectivity (through early diagnosis and curative or
Harrisons_20e_Part5_p0859-p1648.indd 976 6/1/18 12:03 PM
suppressive treatment); and to decrease the efficiency of transmission Organization estimated that 357 million new cases of four curable 977
(through promotion of condom use and safer sexual practices, use of STIs—gonorrhea, chlamydial infection, syphilis, and trichomoniasis—
effective vaccines, and male medical circumcision). occurred annually in recent years. Up to 50% of women of reproductive
In all societies, STIs rank among the most common of all infec- age in developing countries have BV (arguably acquired sexually). All
tious diseases, with at least 40 microorganisms now classified of these curable STIs have been associated with increased risk of HIV
as predominantly sexually transmitted or as frequently sexu- transmission or acquisition.
ally transmissible (Table 131-1). In developing countries, with In the United States, the prevalence of antibody to HSV-2 began to
three-quarters of the world’s population and 90% of the world’s STIs, fall in the late 1990s, especially among adolescents and young adults;
factors such as population growth (especially in adolescent and young- the decline was presumably due to delayed sexual debut, increased
adult age groups), rural-to-urban migration, wars, limited or no provision condom use, and lower rates of multiple (four or more) sex partners—
of reproductive health services for women, and poverty create excep- all well documented by the U.S. Youth Risk Behavior Surveillance
tional vulnerability to disease resulting from unprotected sex. During the System. The estimated annual incidence of HBV infection has also
1990s in China, Russia, the other states of the former Soviet Union, and declined dramatically since the mid-1980s; this decrease is probably
South Africa, internal social structures changed rapidly as borders attributable to now-widespread administration of hepatitis B vaccine
opened to the West, unleashing enormous new epidemics of HIV infec- in infancy. Genital HPV remains the most common sexually transmit-
tion and other STIs. Despite advances in the provision of highly effec- ted pathogen in the United States, infecting 60% of a cohort of initially
tive antiretroviral therapy worldwide, HIV remains the leading cause HPV-negative, sexually active Washington state college women within
of death in some developing countries, and HPV and hepatitis B virus 5 years in a study conducted from 1990 to 2000—i.e., during the pre–
(HBV) remain important causes of cervical and hepatocellular carci- HPV immunization era. The scale-up of HPV vaccine coverage among
noma, respectively—two of the most common (and preventable) malig- young women has already shown promise in reducing the incidence of
nancies in the developing world. Sexually transmitted herpes simplex infection with the HPV types included in the vaccines and of conditions
virus (HSV) infection causes most genital ulcer disease throughout the associated with these viruses.
world, and an increasing proportion of cases of genital herpes occur In industrialized countries, fear of HIV infection in the mid-1980s
in developing countries with generalized HIV epidemics, where the and through the mid-2000s, coupled with widespread behavioral
positive-feedback loop between HSV and HIV transmission remains interventions and better-organized systems of care for the curable
intractable. Despite this consistent link, randomized trials evaluating STIs, initially helped curb the transmission of several STDs. However,
the efficacy of antiviral therapy in suppressing HSV in both HIV- with well-tolerated and highly effective antiretroviral therapy now
uninfected and HIV-infected persons have demonstrated no protective available, HIV has become for many a chronic disease associated with
CHAPTER 131 Sexually Transmitted Infections: Overview and Clinical Approach
effect against acquisition or transmission of HIV. The World Health a normal life span and high quality of life. Rates of gonorrhea and
syphilis remain higher in the United States than in any other Western
industrialized country.
TABLE 131-1 Sexually Transmitted and Sexually Transmissible
Microorganisms In the United States, the Centers for Disease Control and Prevention
(CDC) has compiled reported rates of STIs since 1941. The incidence
BACTERIA VIRUSES OTHERa
of reported gonorrhea peaked at 468 cases per 100,000 population in
Transmitted in Adults Predominantly by Sexual Intercourse the mid-1970s and fell to a low of 98 cases per 100,000 in 2012. With
Neisseria gonorrhoeae HIV (types 1 and 2) Trichomonas vaginalis increased testing and more sensitive tests, the incidence of reported
Chlamydia trachomatis Human T-cell Pthirus pubis Chlamydia trachomatis infection has been increasing steadily since
Treponema pallidum lymphotropic virus reporting began in 1984, reaching an all-time peak of 457.6 cases per
type 1 100,000 in 2011. The incidence of primary and secondary syphilis per
Haemophilus ducreyi
Herpes simplex virus 100,000 peaked at 71 cases in 1946, fell rapidly to 3.9 cases in 1956,
Klebsiella
type 2 ranged from ~10 to 15 cases through 1987 (with markedly increased
(Calymmatobacterium)
granulomatis Human papillomavirus rates among MSM and African Americans), and then fell to a nadir
(multiple genital of 2.1 cases in 2000–2001 (with rates falling most rapidly among
Ureaplasma urealyticum
genotypes)
Mycoplasma genitalium heterosexual African Americans). However, since 1996, with the intro-
Hepatitis B virusb
duction of highly active antiretroviral therapy, gonorrhea, syphilis,
Molluscum contagiosum and chlamydial infection have had a remarkable resurgence among
virus
MSM in North America and Europe, where outbreaks of a rare type
Sexual Transmission Repeatedly Described but Not Well Defined or of chlamydial infection (lymphogranuloma venereum [LGV]) that
Not the Predominant Mode
had virtually disappeared during the AIDS era have occurred. In
Mycoplasma hominis Cytomegalovirus Candida albicans 2014, ~75% of primary and secondary syphilis cases reported to the
Gardnerella vaginalis and Human T-cell Sarcoptes scabiei CDC were in MSM. Moreover, the uptake of daily oral emtricitabine/
other vaginal bacteria lymphotropic virus tenofovir as oral pre-exposure prophylaxis for HIV-1 acquisition has
Group B Streptococcus type 2
increased among MSM since its initial approval for this purpose in 2012
Mobiluncus spp. Hepatitis C virus and has been associated with reports of reduced condom-use frequency
Helicobacter cinaedi (?) Hepatitis D virus and concomitantly increased STI acquisition. These developments have
Helicobacter fennelliae Herpes simplex virus resulted in a soaring incidence of STIs, with increasing co-infection with
type 1 HIV and other sexually transmitted pathogens (particularly Treponema
Anaerobes associated
with bacterial vaginosis Zika virus pallidum, the cause of syphilis; and Neisseria gonorrhoeae, the cause of
Leptotrichia/Sneathia Ebola virus gonorrhea), primarily among MSM.
Group C Neisseria (?) Epstein-Barr virus
meningitidis Human herpesvirus MANAGEMENT OF COMMON SEXUALLY
type 8 TRANSMITTED DISEASE (STD) SYNDROMES
Transmitted by Sexual Contact Involving Oral–Fecal Exposure; of Although other chapters discuss management of specific STIs, most
Declining Importance in Men Who Have Sex with Men patients are managed (at least initially) on the basis of presenting
Shigella spp. Hepatitis A virus Giardia lamblia symptoms and signs and associated risk factors, even in industrialized
Campylobacter spp. Entamoeba histolytica countries. Table 131-2 lists some of the most common clinical STD syn-
dromes and their microbial etiologies. Strategies for their management
a
Includes protozoa, ectoparasites, and fungi. bAmong U.S. patients for whom a
risk factor can be ascertained, most hepatitis B virus infections are transmitted are outlined below. Chapters 196 and 197 address the management of
sexually. infections with human retroviruses.
Harrisons_20e_Part5_p0859-p1648.indd 977 6/1/18 12:03 PM
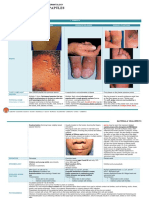
978 TABLE 131-2 Major Sexually Transmitted Disease Syndromes and Consideration of routine demographic data (e.g., gender, age, area of
Sexually Transmitted Microbial Etiologies residence) is a simple first step in this risk assessment. For example,
SEXUALLY TRANSMITTED MICROBIAL national guidelines strongly recommend routine screening of sexually
SYNDROME ETIOLOGIES active females ≤25 years of age for C. trachomatis infection. Table 131-3
AIDS HIV types 1 and 2 provides a set of 11 STD/HIV risk-assessment questions that clinicians
Urethritis: males Neisseria gonorrhoeae, Chlamydia can pose verbally or that health care systems can adapt (with yes/no
trachomatis, Mycoplasma genitalium, responses) into a routine self-administered questionnaire. The initial
Ureaplasma urealyticum (subspecies framing statement gives permission to discuss topics that may be diffi-
urealyticum), Trichomonas vaginalis, HSV, cult for the patient to disclose.
some anaerobic bacteria, Leptotrichia/ Risk assessment is followed by clinical assessment (elicitation of
Sneathia
information on specific current symptoms and signs of STDs). Con-
Epididymitis C. trachomatis, N. gonorrhoeae, and (in firmatory diagnostic tests (for persons with symptoms or signs) or
older men or men who have sex with men)
coliform bacteria
screening tests (for those without symptoms or signs) may involve
microscopic examination, culture, nucleic acid amplification tests
Lower genital tract infections:
females (NAATs), or serology. Initial syndrome-based treatment should cover
the most likely causes. For certain syndromes, results of rapid tests can
Cystitis/urethritis C. trachomatis, N. gonorrhoeae, HSV
narrow the spectrum of this initial therapy (e.g., pH of vaginal fluid
Mucopurulent cervicitis C. trachomatis, N. gonorrhoeae,
M. genitalium
for women with vaginal discharge, Gram’s stain of urethral discharge
for men with urethral discharge, rapid plasma reagin test for genital
Vulvitis Candida albicans, HSV
ulcer to assess the probability of syphilis). After the institution of
Bartholinitis C. albicans, T. vaginalis
treatment, STD management proceeds to the “4 Cs” of prevention and
Vulvovaginitis C. albicans, T. vaginalis control: contact tracing (see “Prevention and Control of STIs,” below),
BV BV-associated bacteria (see text)
Acute pelvic inflammatory N. gonorrhoeae, C. trachomatis,
disease BV-associated bacteria, M. genitalium,
group B streptococci TABLE 131-3 Eleven-Question STD/HIV Risk Assessment
Infertility N. gonorrhoeae, C. trachomatis, Framing Statement
BV-associated bacteria
In order to provide the best care for you today and to understand your risk for
Ulcerative lesions of the genitalia HSV-1, HSV-2, Treponema pallidum,
certain infections, it is necessary for us to talk about your sexual behavior.
Haemophilus ducreyi, C. trachomatis
PART 5
(LGV strains), Klebsiella Screening Questions
(Calymmatobacterium) granulomatis (1) Do you have any reason to think you might have a sexually transmitted
Complications of pregnancy/ Several pathogens implicated infection? If so, what reason?
puerperium (2) For all adolescents <18 years old: Have you begun having any kind of
Intestinal infections
Infectious Diseases
sex yet?
Proctitis C. trachomatis, N. gonorrhoeae, HSV, STD History
T. pallidum
(3) Have you ever had any sexually transmitted infections or any genital
Proctocolitis or enterocolitis Campylobacter spp., Shigella spp., infections? If so, which ones?
Entamoeba histolytica, Helicobacter spp.,
other enteric pathogens Sexual Preference
Enteritis Giardia lamblia (4) Have you had sex with men, women, or both?
Acute arthritis with urogenital N. gonorrhoeae (e.g., DGI), C. trachomatis Injection Drug Use
infection or viremia (e.g., reactive arthritis), HBV (5) Have you ever injected yourself (“shot up”) with drugs? (If yes, have you
Genital and anal warts HPV (30 genital types) ever shared needles or injection equipment?)
Mononucleosis syndrome CMV, HIV, EBV (6) Have you ever had sex with a gay or bisexual man or with anyone who
Hepatitis Hepatitis viruses, T. pallidum, CMV, EBV had ever injected drugs?
Neoplasias Characteristics of Partner(s)
Squamous cell dysplasias and HPV (especially types 16, 18, 31, 45) (7) Has your sex partner had any sexually transmitted infections? If so,
cancers of the cervix, anus, which ones?
vulva, vagina, or penis (8) Has your sex partner had other sex partners during the time you’ve been
Kaposi’s sarcoma, body-cavity HHV-8 together?
lymphomas STD Symptoms Checklist
T cell leukemia HTLV-1 (9) Have you recently developed any of these symptoms?
Hepatocellular carcinoma HBV
For Men For Women
Tropical spastic paraparesis HTLV-1
(a) Discharge of pus (drip) from the (a) Abnormal vaginal discharge
Scabies Sarcoptes scabiei penis (increased amount, abnormal
Pubic lice Pthirus pubis (b) Genital sores (ulcers) or rash odor, abnormal yellow color)
Abbreviations: BV, bacterial vaginosis; CMV, cytomegalovirus; DGI, disseminated (b) Genital sores (ulcers), rash, or
gonococcal infection; EBV, Epstein-Barr virus; HBV, hepatitis B virus; HHV-8, itching
human herpesvirus type 8; HPV, human papillomavirus; HSV, herpes simplex virus;
Sexual Practices, Past 2 Months (for patients answering yes to any of
HTLV, human T-cell lymphotropic virus; LGV, lymphogranuloma venereum.
the above questions, to guide examination and testing)
(10) Now I’d like to ask what parts of your body may have been sexually
STD care and management begin with risk assessment and proceed exposed to an STD (e.g., your penis, mouth, vagina, anus).
to clinical assessment, diagnostic testing or screening, treatment, and Query about Interest in STD Screening Tests (for patients answering
prevention. Risk assessment guides detection and interpretation of no to all of the above questions)
symptoms that could denote an STD; decisions on screening or pro- (11) Would you like to be tested for HIV or any other STDs today? (If yes,
phylactic/preventive treatment; risk reduction counseling and inter- clinician can explore which STD and why.)
vention (e.g., hepatitis B vaccination); treatment of partners of patients Source: Adapted from JR Curtis, KK Holmes, in KK Holmes et al (eds): Sexually
with known infections; and behavioral risk reduction by the patient. Transmitted Diseases, 4th ed. New York, McGraw-Hill, 2008.
Harrisons_20e_Part5_p0859-p1648.indd 978 6/1/18 12:03 PM
ensuring compliance with therapy, and counseling on risk reduction, 979
increasing proportion of men with symptoms and/or signs
including condom promotion and provision as well as motivational of urethritis are simultaneously assessed for infection with
interviewing for risk reduction. N. gonorrhoeae and C. trachomatis by NAATs of first-catch urine.
Consistent with current guidelines, all adults should be screened for The urine specimen tested should consist of the first 10–15 mL of
infection with HIV-1 at least once, and more frequently if they are at the stream, and, if possible, patients should not have voided for
elevated risk for acquisition of this infection. the prior 2 h. Culture or NAAT for N. gonorrhoeae may yield posi-
■ URETHRITIS IN MEN tive results even when Gram’s staining is negative; certain strains
Urethritis in men produces urethral discharge, dysuria, or both, usu- of N. gonorrhoeae can result in negative urethral Gram’s stains in
ally without frequency of urination. Causes include N. gonorrhoeae, up to 30% of cases of urethral infection. Results of tests for gono-
C. trachomatis, Mycoplasma genitalium, Ureaplasma urealyticum, Trichomonas coccal and chlamydial infection predict the patient’s prognosis
vaginalis, HSV, and (rarely) adenovirus. (with greater risk for recurrent NGU if neither chlamydiae nor
Until recently, C. trachomatis caused ~30–40% of cases of nongono- gonococci are found than if either is detected) and can guide both
coccal urethritis (NGU), particularly in heterosexual men; however, the the counseling given to the patient and the management of the
proportion of cases due to this organism has probably declined in some patient’s sexual partner(s).
populations served by effective chlamydial control programs, and older 4. Treat urethritis promptly while test results are pending.
men with urethritis appear less likely to have chlamydial infection.
HSV and T. vaginalis each cause a small proportion of NGU cases in the
United States. Recently, multiple studies have consistently implicated TREATMENT
M. genitalium as a probable cause of many Chlamydia-negative cases.
Fewer studies than in the past have implicated Ureaplasma; the ureaplas- Urethritis in Men
mas have been differentiated into U. urealyticum and Ureaplasma parvum,
Table 131-4 summarizes the steps in management of urethral dis-
and a few studies suggest that U. urealyticum—but not U. parvum—is
charge and/or dysuria in sexually active men.
associated with NGU. Coliform bacteria can cause urethritis in men
In practice, if Gram’s stain does not reveal gonococci, urethritis is
who practice insertive anal intercourse. More recently, anaerobic bac-
treated with a regimen effective for NGU, such as azithromycin or
teria that are characteristically involved in BV, especially Leptotrichia/
doxycycline. Both are effective. Although azithromycin has been more
Sneathia species, have occasionally been associated with urethritis in
effective than doxycycline for M. genitalium infection, the efficacy
heterosexual men. Recommendations for the initial diagnosis of ure-
of azithromycin for treatment of M. genitalium is rapidly declining.
CHAPTER 131 Sexually Transmitted Infections: Overview and Clinical Approach
thritis in men currently include specific tests only for N. gonorrhoeae and
Alternatives include moxifloxacin and pristinamycin, a stretogramin
C. trachomatis; they do not yet include testing for M. genitalium, although
antibiotic available in some countries. If gonococci are demonstrated
a NAAT is now commercially available for the latter.
by Gram’s stain or if no diagnostic tests are performed to exclude
gonorrhea definitively, treatment should include parenteral cepha-
APPROACH TO THE PATIENT losporin therapy for gonorrhea (Chap. 151) plus oral azithromycin,
primarily for additive activity against N. gonorrhoeae given concerns
Urethritis in Men about evolving cephalosporin resistance. Azithromycin is effective for
The following summarizes the approach to the male patient with treating C. trachomatis infection, which can cause urethral co-infection
suspected urethritis: in men with gonococcal urethritis. Sexual partners should also be
tested for gonorrhea and chlamydial infection. Regardless of whether
1. Establish the presence of urethritis. If proximal-to-distal “milking”
of the urethra does not express a purulent or mucopurulent
discharge, even after the patient has not voided for several hours TABLE 131-4 Management of Urethral Discharge in Men
(or preferably overnight), a Gram’s-stained smear of an anterior USUAL CAUSES USUAL INITIAL EVALUATION
urethral specimen obtained by passage of a small urethrogenital Chlamydia trachomatis Demonstration of urethral discharge or
swab 2–3 cm into the urethra usually reveals ≥2 neutrophils Neisseria gonorrhoeae pyuria
per 1000× field when urethritis is present; in gonococcal infec- Mycoplasma genitalium Exclusion of local or systemic
tion, such a smear usually reveals gram-negative intracellular complications
Ureaplasma urealyticum
diplococci as well. Alternatively, the centrifuged sediment of Urethral Gram’s stain to confirm
Trichomonas vaginalis
the first 20–30 mL of voided urine—ideally collected as the first urethritis, detect gram-negative diplococci
Herpes simplex virus
morning specimen—can be examined for inflammatory cells, Test for N. gonorrhoeae, C. trachomatis
either by microscopy showing ≥10 leukocytes per high-power Initial Treatment for Patient and Partners
field or by the leukocyte esterase test. Patients with symptoms Treat gonorrhea (unless excluded):
who lack objective evidence of urethritis generally do not benefit
Ceftriaxone (250 mg IMa) plus azithromycin (1 g PO)
from repeated courses of antibiotics, and other etiologies of such
symptoms may be considered. Management of Recurrence
2. Evaluate for complications or alternative diagnoses. A brief his- Confirm objective evidence of urethritis. If patient was reexposed to untreated
tory and examination can exclude epididymitis and systemic or new partner, repeat treatment of patient and partner.
complications, such as disseminated gonococcal infection (DGI) If patient was not reexposed, consider infection with T. vaginalisb or antibiotic-
and reactive arthritis. Although digital examination of the pros- resistant M. genitaliumc or Ureaplasma, and consider treatment with
metronidazole, azithromycin, or both.
tate gland seldom contributes to the evaluation of sexually active
young men with urethritis, men with dysuria who lack evidence a
Neither oral cephalosporins nor fluoroquinolones are recommended for treatment
of gonorrhea in the United States because of the emergence of increasing
of urethritis as well as sexually inactive men with urethritis fluoroquinolone resistance in N. gonorrhoeae, especially (but not only) among
should undergo prostate palpation, urinalysis, and urine culture men who have sex with men, and the decreasing susceptibility of a still-small
to exclude bacterial prostatitis and cystitis. proportion of gonococci to ceftriaxone (Fig. 131-1). Updates on the emergence of
antimicrobial resistance in N. gonorrhoeae can be obtained from the Centers for
3. Evaluate for gonococcal and chlamydial infection. An absence of Disease Control and Prevention at http://www.cdc.gov/std. bIn men, the diagnosis
typical gram-negative diplococci on Gram’s-stained smear of T. vaginalis infection requires culture, DNA testing, or nucleic acid amplification
of urethral exudate containing inflammatory cells warrants a testing (where available) of early-morning first-voided urine sediment or of a
preliminary diagnosis of NGU, as this test is 98% sensitive for urethral swab specimen obtained before voiding. cM. genitalium is often resistant
to doxycycline and azithromycin but is usually susceptible to the fluoroquinolone
the diagnosis of gonococcal urethral infection. However, an moxifloxacin. Moxifloxacin can be considered for treatment of refractory
nongonococcal, nonchlamydial urethritis.
Harrisons_20e_Part5_p0859-p1648.indd 979 6/1/18 12:03 PM
980 they are tested for these infections, however, they should receive usually caused by urinary pathogens. These older men usually have
the same regimen given to the male index case. Patients with con- no urethritis but do have bacteriuria. Similarly, epididymitis in MSM
firmed persistence or recurrence of urethritis after treatment should who have practiced insertive rectal intercourse is often caused by
be re-treated with the initial regimen if they did not comply with the Enterobacteriaceae.
original treatment or were reexposed to an untreated partner. Most
persistent urethritis is due to M. genitalium, and prompt diagnostic
testing and/or treatment for M. genitalium is recommended.
TREATMENT
National and international guidelines do exist for treatment of Epididymitis
gonococcal urethritis, typically with ceftriaxone plus azithromycin.
However, consensus is still lacking on treatment of urethritis that Ceftriaxone (250 mg as a single dose IM) followed by doxycycline
persists after treatment and cure of gonorrhea. Ideally, the approach (100 mg by mouth twice daily for 10 days) constitutes effective
would involve testing for potential causes of the persistent urethritis treatment for epididymitis caused by N. gonorrhoeae or C. trachomatis.
(e.g., M. genitalium) and antimicrobial susceptibility testing in set- Neither oral cephalosporins nor fluoroquinolones are recommended
tings and populations where antimicrobial resistance is emerging. for treatment of gonorrhea in the United States because of resistance
Currently, assays are available that can detect M. genitalium, and in N. gonorrhoeae, especially (but not only) among MSM (Fig. 131-1).
some experts believe it is time to integrate such testing into STD When infection with Enterobacteriaceae is suspected, oral levofloxa-
care. If M. genitalium is detected, the persistent urethritis can be cin (500 mg once daily for 10 days) or ofloxacin (300 mg twice daily
treated with azithromycin or moxifloxacin in light of local patterns for 10 days) is effective for syndrome-based initial treatment of
of antimicrobial susceptibility. epididymitis; however, because this regimen is not effective against
In heterosexual men with a high likelihood of exposure to tricho- gonococcal or chlamydial infection, it should be combined with
moniasis, an intraurethral swab specimen and a first-voided urine effective therapy for possible gonococcal or chlamydial infection
sample should be tested for T. vaginalis (often by culture, although of the epididymis unless bacteriuria with Enterobacteriaceae is
NAATs are more sensitive and are approved for the diagnosis of tri- confirmed.
chomoniasis in women), and presumptive treatment with metroni-
dazole or tinidazole (2 g by mouth in a single dose) should be given.
For MSM, trichomoniasis is unlikely, and consideration of a course ■ URETHRITIS AND THE URETHRAL SYNDROME IN
of moxifloxacin is warranted. Because MSM also have the highest WOMEN
prevalence rates of antimicrobial-resistant N. gonorrhoeae, this possi- C. trachomatis, N. gonorrhoeae, and occasionally HSV cause symptom-
bility, even if apparently ruled out at the initial presentation, should atic urethritis—known as the urethral syndrome in women—that is
PART 5
be kept in mind. characterized by “internal” dysuria (usually without urinary urgency
or frequency), pyuria, and an absence of Escherichia coli and other uro-
pathogens at counts of ≥102/mL in urine. In contrast, the dysuria asso-
■ EPIDIDYMITIS ciated with vulvar herpes or vulvovaginal candidiasis (and perhaps
Acute epididymitis, almost always unilateral, produces pain, swelling, with trichomoniasis) is often described as “external,” being caused
Infectious Diseases
and tenderness of the epididymis, with or without symptoms or signs by painful contact of urine with the inflamed or ulcerated labia or
of urethritis. This condition must be differentiated from testicular tor- introitus. Acute onset, association with urinary urgency or frequency,
sion, tumor, and trauma. Torsion, a surgical emergency, usually occurs hematuria, or suprapubic bladder tenderness suggests bacterial cysti-
in the second or third decade of life and produces a sudden onset of tis. Among women with symptoms of acute bacterial cystitis, costover-
pain, elevation of the testicle within the scrotal sac, rotation of the epi- tebral pain and tenderness or fever suggest acute pyelonephritis. The
didymis from a posterior to an anterior position, and absence of blood management of bacterial urinary tract infection (UTI) is discussed in
flow on Doppler ultrasound. Persistence of symptoms after a course of Chap. 130.
therapy for epididymitis suggests the possibility of testicular tumor or Signs of vulvovaginitis, coupled with symptoms of external dys-
of a chronic granulomatous disease, such as tuberculosis. In sexually uria, suggest vulvar infection (e.g., with HSV or Candida albicans).
active men under age 35, acute epididymitis is caused most frequently Among dysuric women without signs of vulvovaginitis, bacterial UTI
by C. trachomatis and less commonly by N. gonorrhoeae and is usually must be differentiated from the urethral syndrome by assessment of
associated with overt or subclinical urethritis. Acute epididymitis risk, evaluation of the pattern of symptoms and signs, and specific
occurring in older men or following urinary tract instrumentation is microbiologic testing. An STI etiology of the urethral syndrome is
Percentage
1.5
Elevated cefixime MICs
Elevated ceftriaxone MICs
1.2
0.9
0.6
0.3
0.0
2006 2007* 2008* 2009 2010 2011 2012 2013 2014 2015
Year
*Isolates not tested for cefixime susceptibility in 2007 and 2008.
FIGURE 131-1 Proportion of Neisseria gonorrhoeae isolates with elevated minimal inhibitory concentrations (MICs) of ceftriaxone (≥0.125 μg/mL) and cefixime
(≥0.25 μg/mL), United States, 2006–2015. (From the Centers for Disease Control and Prevention: Gonococcal Isolate Surveillance Project [GISP], 2016.)
Harrisons_20e_Part5_p0859-p1648.indd 980 6/1/18 12:03 PM
1122 have arisen about adverse events and the development of resistance.
For these reasons, prophylaxis is usually restricted to (1) persons at
greatest risk who are intimate and/or household contacts of the index
case and (2) health care workers who have been directly exposed to
respiratory secretions. In most cases, members of wider communities
(e.g., at schools or colleges) are not offered prophylaxis.
The aim of prophylaxis is to eradicate colonization of close
contacts with the strain that has caused invasive disease in the
index case. Prophylaxis should be given to all contacts at the
same time to avoid recolonization by meningococci transmitted from
untreated contacts and should also be used as soon as possible to treat
early disease in secondary cases. If the index patient is treated with an
antibiotic that does not reliably clear colonization (e.g., penicillin), he or
she should be given a prophylactic agent at the end of treatment to
prevent relapse or onward transmission. Although rifampin has been
most widely used and studied, it is not the optimal agent because it
fails to eradicate carriage in 15–20% of cases, rates of adverse events
have been high, compliance is affected by the need for four doses, and
emerging resistance has been reported. Ceftriaxone as a single IM or IV
injection is highly (97%) effective in carriage eradication and can be
used at all ages and in pregnancy. Reduced susceptibility of isolates to
ceftriaxone has occasionally been reported. Ciprofloxacin or ofloxacin
is preferred in some countries; these agents are highly effective and can
be administered by mouth but are not recommended in pregnancy.
Resistance to fluoroquinolones has been reported in some meningo-
FIGURE 150-7 Illustration of meningococcal outer-membrane vesicle containing cocci in North America, Europe, and Asia.
outer-membrane structures. In documented capsular group A, B, C, Y, or W disease, contacts may
be offered immunization (with either the MenACWY conjugate vaccine
or the MenB vaccine, as appropriate) in addition to chemoprophylaxis
PART 5
herd immunity. Rates of capsular group B carriage are higher among to provide protection beyond the duration of antibiotic therapy. Mass
teenagers and young adults. Studies estimating the potential effect of vaccination has been used successfully to control disease during
4CMenB on carriage of capsular group B meningococci among adoles- outbreaks in closed communities (educational and military establish-
cents indicate that there is likely to be some impact. However, because ments) as well as during epidemics in open communities.
these studies lack power, it remains uncertain whether the vaccine
Infectious Diseases
would have the substantial and sustained herd effects in this age group ■ FURTHER READING
that could support widespread routine administration. Christensen H et al: Meningococcal carriage by age: A systematic
An immunogenic vaccine based on two variants of the lipoprotein review and meta-analysis. Lancet Infect Dis 10:853, 2010.
factor H–binding protein (fHbp2) has been developed for use in ado- Cohn AC et al: Prevention and control of meningococcal disease:
lescents and is licensed in the United States and Europe. The vaccine is Recommendations of the Advisory Committee on Immunization
immunogenic against representative indicator strains, inducing four- Practices (ACIP). MMWR Recomm Rep 62(RR-2):1, 2013.
fold rises in bactericidal antibody titer in 50–92% of individuals. fHbp2 Gossger N et al: Immunogenicity and tolerability of recombinant sero-
has an acceptable safety profile, with pain at the injection site, fatigue, group B meningococcal vaccine administered with or without routine
and headache commonly reported. This vaccine can be used with a infant vaccinations according to different immunization schedules: A
range of vaccines routinely administered in adolescence, including randomized controlled trial. JAMA 307:573, 2012.
Tdap (tetanus–diphtheria–acellular pertussis), human papillomavirus, Jafri RZ et al: Global epidemiology of invasive meningococcal disease.
and MenACWY vaccines. fHbp2 has been used to control outbreaks of Popul Health Metr 11:17, 2013.
meningococcal disease in educational institutions in the United States, Pollard AJ et al: Maintaining protection against invasive bacteria
but no formal studies of its effectiveness have yet been undertaken. with protein–polysaccharide conjugate vaccines. Nat Rev Immunol
Both of the new capsular group B meningococcal vaccines are 9:213, 2009.
licensed for use in the United States for persons 10–25 years of age. In Read RC et al: Effect of a quadrivalent meningococcal ACWY glyco-
addition, ACIP recommends their administration to individuals at high conjugate or a serogroup B meningococcal vaccine on meningococcal
risk of capsular group B disease, with 4CMenB administered as two carriage: An observer-blind, phase 3 randomised clinical trial. Lancet
doses (1–2 months apart) and fHbp2 as three doses on a 0/1/6-month 384:2123, 2014.
schedule. Vieusseux M: Memoire sur le maladie qui a regne a Geneva au prin-
temps de 1805. J Med Clin Pharm 11:163, 1805.
■ MANAGEMENT OF CONTACTS
Close (household and kissing) contacts of individuals with meningo-
151 Gonococcal Infections
coccal disease are at increased risk for developing secondary disease
(up to 1000 times the rate for the general population); a secondary
case follows as many as 3% of sporadic cases. About one-fifth of sec-
ondary cases are actually co-primary cases—i.e., cases that occur soon Sanjay Ram, Peter A. Rice
after the primary case and in which transmission is presumed to have
originated from the same third party. The rate of secondary cases is
highest during the week after presentation of the index case. The risk ■ DEFINITION
falls rapidly but remains above baseline for up to 1 year after the index Gonorrhea is a sexually transmitted infection (STI) of epithelium and
case; 30% of secondary cases occur in the first week, 20% in the second commonly manifests as cervicitis, urethritis, proctitis, and conjunctivi-
week, and most of the remainder over the next 6 weeks. In outbreaks tis. If untreated, infections at these sites can lead to local complications
of meningococcal disease, mass prophylaxis has been used; however, such as endometritis, salpingitis, tuboovarian abscess, bartholinitis,
limited data support population intervention, and significant concerns peritonitis, and perihepatitis in female patients; periurethritis and
Harrisons_20e_Part5_p0859-p1648.indd 1122 6/1/18 12:04 PM
epididymitis in male patients; and ophthalmia neonatorum in new- ignored. These persons, unlike symptomatic individuals, may not 1123
borns. Disseminated gonococcemia is an uncommon event whose cease sexual activity and therefore may continue to transmit the infec-
manifestations include skin lesions, tenosynovitis, arthritis, and (in rare tion. This situation underscores the importance of contact tracing and
cases) endocarditis or meningitis. empirical treatment of the sex partners of index cases.
■ MICROBIOLOGY ■ PATHOGENESIS, IMMUNOLOGY, AND
Neisseria gonorrhoeae is a gram-negative, nonmotile, non-spore-forming ANTIMICROBIAL RESISTANCE
organism that grows singly and in pairs (i.e., as monococci and diplo-
cocci, respectively). Exclusively a human pathogen, the gonococcus
Outer-Membrane Proteins PILI Fresh clinical isolates of
N. gonorrhoeae initially form piliated (fimbriated) colonies distinguish-
contains, on average, three genome copies per coccal unit; this poly-
able on translucent agar. Pilus expression is rapidly switched off with
ploidy permits a high level of antigenic variation and the survival of
unselected subculture because of rearrangements in pilus genes. This
the organism in its host. Gonococci, like all other Neisseria species, are
change is a basis for antigenic variation of gonococci. Piliated strains
oxidase positive. They are distinguished from other neisseriae by their
adhere better to cells derived from human mucosal surfaces and are
ability to grow on selective media and to use glucose but not maltose,
more virulent in organ culture models and human inoculation experi-
sucrose, or lactose.
ments than nonpiliated variants. In a fallopian tube explant model, pili
mediate gonococcal attachment to nonciliated columnar epithelial cells.
■ EPIDEMIOLOGY
This event initiates gonococcal phagocytosis and transport through
The incidence of gonorrhea had been declining steadily in the
these cells to intercellular spaces near the basement membrane or
United States, but in 2016 there were ~450,000 newly reported
directly into the subepithelial tissue. Pili are also essential for genetic
cases—up 46% since 2011. With 80 million cases estimated by
competence and transformation of N. gonorrhoeae, which permit
the World Health Organization to have occurred globally in 2014, gon-
horizontal transfer of genetic material between different gonococcal
orrhea remains a major public health problem worldwide, is a signifi-
lineages in vivo.
cant cause of morbidity in developing countries, and may play a role in
enhancing transmission of HIV. OPACITY-ASSOCIATED PROTEIN Another gonococcal surface protein that
Gonorrhea predominantly affects young, nonwhite, unmarried, less is important in adherence to epithelial cells is opacity-associated protein
educated members of urban populations. The number of reported cases (Opa, formerly called protein II). Opa contributes to intergonococcal
probably represents half of the true number of cases—a discrepancy adhesion, which is responsible for the opaque nature of gonococcal
resulting from under-reporting, self-treatment, and nonspecific treat- colonies on translucent agar and the organism’s adherence to a variety
CHAPTER 151 Gonococcal Infections
ment without a laboratory-proven diagnosis. The number of reported of eukaryotic cells, including polymorphonuclear leukocytes (PMNs).
new cases of gonorrhea in the United States rose from ~250,000 in the Certain Opa variants promote invasion of epithelial cells, and this
early 1960s to a high of 1.01 million in 1978. The recorded incidence effect has been linked with the ability of Opa to bind vitronectin,
of gonorrhea in modern times peaked in 1975, with 468 reported glycosaminoglycans, and several members of the carcinoembryonic
new cases per 100,000 population in the United States. This peak was antigen–related cell adhesion molecule (CEACAM) receptor family.
attributable to the interaction of several variables, including improved CEACAM5-binding gonococci prevent exfoliation of epithelium and
accuracy of diagnosis, changes in patterns of contraceptive use, and may interfere with bacterial clearance. N. gonorrhoeae Opa proteins that
changes in sexual behavior. A decline in the overall incidence of gon- bind CEACAM1, which is expressed by primary CD4+ T lymphocytes,
orrhea in the United States over the past quarter-century may reflect suppress the activation and proliferation of these lymphocytes. Select
increased condom use resulting from public health efforts to curtail Opa proteins can engage CEACAM3, which is expressed on neu-
HIV transmission. Nevertheless, in 2016, 146 new cases per 100,000 trophils, with consequent nonopsonic phagocytosis (i.e., phagocytosis
population were reported in this country, representing a 1-year increase independent of antibody and complement) and killing of bacteria.
of 19%; this figure is the highest among industrialized countries. Simul-
PORIN Porin (previously designated protein I) is the most abundant
taneously, antibiotic resistance is increasing in the United States and
gonococcal surface protein. Porin molecules exist as trimers that
other countries, prompting the U.S. Centers for Disease Control and
provide anion-transporting aqueous channels through the other-
Prevention (CDC) to name antibiotic-resistant N. gonorrhoeae as one of
wise hydrophobic outer membrane. Porin exhibits stable interstrain
the three most urgent threats of its kind. At present, the attack rate in
antigenic variation and forms the basis for gonococcal serotyping.
the United States is highest among 15- to 24-year-old women and 20-
Two main serotypes have been identified; PorB.1A strains are often
to 29-year-old men; more than 70% of all reported cases occur in these
associated with disseminated gonococcal infection (DGI), whereas
two groups. From the standpoint of ethnicity, rates are highest among
PorB.1B strains usually cause local genital infections only. DGI strains
African Americans and lowest among persons of Asian descent.
are generally resistant to the killing action of normal human serum
The incidence of gonorrhea is higher in developing countries than
and do not incite a significant local inflammatory response; therefore,
in industrialized nations. The exact incidence of any STI is difficult to
they may not cause symptoms at genital sites. These characteristics
ascertain in developing countries because of limited surveillance and
may be related to the ability of PorB.1A strains to bind to complement-
variable diagnostic criteria. Extremely high rates of gonorrhea have
inhibitory molecules, resulting in a diminished inflammatory response.
been reported among aboriginal populations in Namibia and Australia.
Porin can translocate to the cytoplasmic membrane of host cells—a pro-
Studies in Africa have clearly demonstrated that nonulcerative STIs
cess that could initiate gonococcal endocytosis and invasion.
such as gonorrhea (in addition to ulcerative STIs) are an independent
risk factor for the transmission of HIV (Chap. 197). OTHER OUTER-MEMBRANE PROTEINS Other notable outer-membrane
Gonorrhea is transmitted from males to females more efficiently proteins include H.8, a lipoprotein that is present in high concentration
than in the opposite direction. The rate of transmission to a woman on the surface of all gonococcal strains and is an excellent target for anti-
during a single unprotected sexual encounter with an infected man is body-based diagnostic testing. Transferrin-binding proteins (Tbp1 and
~50–70%. Oropharyngeal gonorrhea occurs in ~20% of women who Tbp2) and lactoferrin-binding protein are required for scavenging iron
practice fellatio with infected partners. Transmission in either direction from transferrin and lactoferrin in vivo. Transferrin and iron have been
by cunnilingus is rare. shown to enhance the attachment of iron-deprived N. gonorrhoeae to
In any population, there exists a small minority of individuals human endometrial cells. IgA1 protease is produced by N. gonorrhoeae
who have high rates of new-partner acquisition. These “core-group and may protect the organism from the action of mucosal IgA.
members” or “high-frequency transmitters” are vital in sustaining STI
transmission at the population level. Another instrumental factor in Lipooligosaccharide Gonococcal lipooligosaccharide (LOS) con-
sustaining gonorrhea in the population is the large number of infected sists of a lipid A and a core oligosaccharide that lacks the repeating
individuals who are asymptomatic or have minor symptoms that are O-carbohydrate antigenic side chain seen in other gram-negative
Harrisons_20e_Part5_p0859-p1648.indd 1123 6/1/18 12:04 PM
1124 bacteria (Chap. 116). Gonococcal LOS possesses marked endotoxic antigenic structure and adapt to changes in the microenvironment,
activity and contributes to the local cytotoxic effect in a fallopian tube has become resistant to numerous antibiotics. The first effective agents
model. LOS core sugars undergo a high degree of phase variation against gonorrhea were the sulfonamides, which were introduced in
under different conditions of growth; this variation reflects genetic the 1930s and became ineffective within a decade. Penicillin was then
regulation and expression of glycotransferase genes that dictate the used as the drug of choice for the treatment of gonorrhea. By 1965, 42%
carbohydrate structure of LOS. These phenotypic changes may affect of gonococcal isolates had developed low-level resistance to penicillin
interactions of N. gonorrhoeae with elements of the humoral immune G. Resistance due to the production of penicillinase arose later.
system (antibodies and complement) and may also influence direct Gonococci become fully resistant to antibiotics either by chromo-
binding of organisms to both professional phagocytes and nonprofes- somal mutations or by acquisition of R factors (plasmids). Two
sional phagocytes (epithelial cells). For example, gonococci that are types of chromosomal mutations have been described. The first
sialylated at their LOS sites inhibit the classic pathway of complement type, which is drug specific, is a single-step mutation leading to high-
by reducing binding of IgG and also bind complement factor H to level resistance. The second type involves mutations at several chromo-
inhibit the alternative pathway of complement. LOS sialylation may somal loci that combine to determine the level as well as the pattern of
also decrease nonopsonic Opa-mediated association with neutrophils resistance. Strains with mutations in chromosomal genes were first
and inhibit the oxidative burst in PMNs. The binding of the unsialy- observed in the late 1950s. As recently as 2007, chromosomal mutations
lated terminal lactosamine residue of LOS to an asialoglycoprotein accounted for resistance to penicillin, tetracycline, or both in ~16% of
receptor on male epithelial cells facilitates adherence and subsequent strains surveyed in the United States.
gonococcal invasion of these cells. Moreover, oligosaccharide struc- β-Lactamase (penicillinase)–producing strains of N. gonorrhoeae
tures in LOS can modulate host immune responses. For example, the (PPNG) carrying β-lactamase plasmids had rapidly spread worldwide
terminal monosaccharide expressed by LOS determines the C-type by the early 1980s. N. gonorrhoeae strains with plasmid-borne tetra-
lectin receptor on dendritic cells that is targeted by the bacteria. In turn, cycline resistance (TRNG) can mobilize some β-lactamase plasmids,
the specific C-type lectin receptor engaged influences whether a TH1- or and PPNG and TRNG occur together, sometimes along with strains
TH2-type response is elicited; the latter response may be less favorable exhibiting chromosomally mediated resistance (CMRNG). Penicillin,
for clearance of gonococcal infection. ampicillin, and tetracycline are no longer reliable for the treatment of
gonorrhea and should not be used.
Host Factors In addition to gonococcal structures that interact
Quinolone-containing regimens also were recommended for
with epithelial cells, host factors seem to be important in mediating
treatment of gonococcal infections; the fluoroquinolones
entry of gonococci into nonphagocytic cells. Activation of phosphati-
offered the advantage of antichlamydial activity when admin-
dylcholine-specific phospholipase C and acidic sphingomyelinase by
istered for 7 days. However, quinolone-resistant N. gonorrhoeae (QRNG)
N. gonorrhoeae, which results in the release of diacylglycerol and cer-
PART 5
appeared soon after these agents were first used to treat gonorrhea.
amide, is a requirement for the entry of N. gonorrhoeae into epithelial
QRNG is particularly common in the Pacific Islands (including Hawaii)
cells. Ceramide accumulation within cells leads to apoptosis, which
and Asia, where, in certain areas, all gonococcal strains are now resis-
may disrupt epithelial integrity and facilitate entry of gonococci into
tant to quinolones. At present, QRNG is also common in parts of
subepithelial tissue. Release of chemotactic factors as a result of com-
Europe and the Middle East. In the United States, QRNG has been
Infectious Diseases
plement activation contributes to inflammation, as does the toxic effect
identified in all areas but predominantly in states on the Pacific coast,
of LOS in provoking the release of inflammatory cytokines.
where resistant strains were first seen. Alterations in DNA gyrase and
The importance of humoral immunity in host defenses against
topoisomerase IV have been implicated as mechanisms of fluoro-
neisserial infections is best illustrated by the predisposition of persons
quinolone resistance.
deficient in terminal complement components (C5 through C9) to
Resistance to spectinomycin, which has been used in the past as an
have recurrent bacteremic gonococcal infections and recurrent menin-
alternative agent, has been reported. Because this agent usually is not
gococcal meningitis or meningococcemia. Gonococcal porin induces
associated with resistance to other antibiotics, spectinomycin can be
T cell–proliferative responses in persons with urogenital gonococcal
reserved for use against multidrug-resistant strains of N. gonorrhoeae.
disease. A significant increase in porin-specific interleukin (IL) 4–
Nevertheless, outbreaks caused by strains resistant to spectinomycin
producing CD4+ as well as CD8+ T lymphocytes is seen in individu-
have been documented in Korea and England when the drug has been
als with mucosal gonococcal disease. A portion of these lymphocytes
used for primary treatment of gonorrhea.
that show a porin-specific TH2-type response could traffic to mucosal
Third-generation cephalosporins have remained highly effective as
surfaces and play a role in immune protection against the disease. Few
single-dose therapy for gonorrhea, but the recent isolation of strains
data clearly indicate that protective immunity is acquired from a previ-
highly resistant to ceftriaxone (minimal inhibitory concentrations [MICs],
ous gonococcal infection, although bactericidal and opsonophagocytic
2 μg/mL) in Japan and some European countries is cause for concern.
antibodies to porin and LOS may offer partial protection. On the other
Even though the MICs of ceftriaxone against certain strains may reach
hand, women who are infected and acquire high levels of antibody
0.015–0.125 μg/mL (higher than the MICs of 0.0001–0.008 μg/mL for
to another outer-membrane protein, Rmp (reduction modifiable pro-
fully susceptible strains), these levels are greatly exceeded in the blood,
tein, formerly called protein III), may be especially likely to become
the urethra, and the cervix when the routinely recommended parenteral
reinfected with N. gonorrhoeae because Rmp antibodies block the effect
dose of ceftriaxone is administered. The rising MICs of oral cefixime (the
of bactericidal antibodies to porin and LOS. Rmp shows little, if any,
previously recommended alternative oral third-generation cephalospo-
interstrain antigenic variation; therefore, Rmp antibodies potentially
rin) against N. gonorrhoeae, combined with this drug’s limited capacity
may block antibody-mediated killing of all gonococci. The mechanism
to reach levels sufficiently higher than MICs in the blood, the urethra,
of blocking has not been fully characterized, but Rmp antibodies may
the cervix, and especially the pharynx, have resulted in the removal of
noncompetitively inhibit binding of porin and LOS antibodies because
cefixime from the list of first-line agents for treatment of uncomplicated
of the proximity of these structures in the gonococcal outer membrane.
gonorrhea. N. gonorrhoeae strains with reduced susceptibility to ceftriax-
In male volunteers who have no history of gonorrhea, the net effect of
one and cefixime (i.e., cephalosporin-intermediate/resistant strains)
these events may influence the outcome of experimental challenge with
contain mutations in (1) the penA allele, which is the principal resistance
N. gonorrhoeae. Because Rmp bears extensive homology to enterobac-
determinant and encodes a penicillin-binding protein (PBP2) whose
terial OmpA and meningococcal class 4 proteins, it is possible that
sequence can differ in up to 60–70 amino acids from that of wild-type
these blocking antibodies result from prior exposure to cross-reacting
PBP2; (2) the multiple transferable resistance regulator (mtrR) gene that
proteins from these species and also play a role in first-time infection
results in increased drug efflux through the MtrCDE efflux pump; and
with N. gonorrhoeae.
(3) penB, which decreases drug influx through PorB.
Gonococcal Resistance to Antimicrobial Agents It is no Resistance to azithromycin can result from alterations of the ribosomal
surprise that N. gonorrhoeae, with its remarkable capacity to alter its binding target by azithromycin and—as with cephalosporins—the
Harrisons_20e_Part5_p0859-p1648.indd 1124 6/1/18 12:04 PM
over- and under-expression of efflux and influx systems. Combined Women infected with N. gonorrhoeae usually develop symptoms. 1125
resistance to cephalosporins and azithromycin could contribute to However, women who either remain asymptomatic or have only
the failure of the currently recommended dual therapy for gonorrhea minor symptoms may delay in seeking medical attention. These minor
with these two antimicrobial agents. Indeed, clinical failures caused by symptoms may include scant vaginal discharge issuing from the
organisms resistant to these agents have been reported on two occa- inflamed cervix (without vaginitis or vaginosis per se) and dysuria
sions in infected heterosexual men treated with both agents. (often without urgency or frequency) that may be associated with
gonococcal urethritis. Although the incubation period of gonorrhea is
■ CLINICAL MANIFESTATIONS less well defined in women than in men, symptoms usually develop
Gonococcal Infections in Men Acute urethritis is the most within 10 days of infection and are more acute and intense than those
common clinical manifestation of gonorrhea in male patients. The of chlamydial cervicitis.
usual incubation period after exposure is 2–7 days, although the The physical examination reveals a mucopurulent discharge
interval can be longer and most men remain asymptomatic. Strains (mucopus) issuing from the cervical os or a reddened (inflamed) cer-
of the PorB.1A serotype tend to cause a greater proportion of cases vix even in the absence of reported symptoms. Because Gram’s stain
of mild and asymptomatic urethritis than do PorB.1B strains. When is not sensitive for the diagnosis of gonorrhea in women, specimens
they occur, urethral discharge and dysuria, usually without urinary should be submitted for culture or a nonculture assay (see “Laboratory
frequency or urgency, are the major symptoms. The discharge initially Diagnosis,” below). Edematous and friable cervical ectopy and endo-
is scant and mucoid but becomes profuse and purulent within a day or cervical bleeding induced by gentle swabbing are more often seen in
two. Gram’s staining of the urethral discharge may reveal PMNs and chlamydial infection. Gonococcal infection may extend deep enough to
gram-negative intracellular monococci and diplococci (Fig. 151-1). The produce dyspareunia and lower abdominal or back pain. In such cases,
clinical manifestations of gonococcal urethritis are usually more severe it is imperative to consider a diagnosis of pelvic inflammatory disease
and overt than those of nongonococcal urethritis, including urethritis (PID) and to administer treatment for that disease (Chaps. 131 and 184).
caused by Chlamydia trachomatis (Chap. 184); however, exceptions N. gonorrhoeae may also be recovered from the urethra and rectum of
are common, and it is often impossible to differentiate the causes of women with cervicitis, but these are rarely the only infected sites. Ure-
urethritis on clinical grounds alone. The majority of cases of urethritis thritis in women may produce symptoms of internal dysuria, which is
seen in the United States today are not caused by N. gonorrhoeae and/or often attributed to “cystitis.” Pyuria in the absence of bacteriuria visible
C. trachomatis. Although a number of other organisms may be responsible, on Gram’s stain of unspun urine, accompanied by urine cultures that
many cases do not have a specific etiologic agent identified. Certain fail to yield >102 colonies of bacteria usually associated with urinary
clones of Neisseria meningitidis, the second member of the pathogenic tract infection, signifies the possibility of urethritis due to C. trachomatis.
CHAPTER 151 Gonococcal Infections
Neisseria species, have been associated with urethritis in men who have Urethral infection with N. gonorrhoeae also may occur in this context,
sex with men (MSM) in Europe and in heterosexual men in the southern but in this instance urethral cultures are usually positive.
and midwestern United States. GONOCOCCAL VAGINITIS The vaginal mucosa of healthy women is
Most symptomatic men with gonorrhea seek treatment and cease lined by stratified squamous epithelium and is rarely infected by
to be infectious. The remaining men, who are largely asymptomatic, N. gonorrhoeae. However, gonococcal vaginitis can occur in anestrogenic
accumulate in number over time and constitute about two-thirds of all women (e.g., prepubertal girls and postmenopausal women), in whom
infected men at any point in time; together with men incubating the the vaginal stratified squamous epithelium is often thinned down to
organism who shed the organism but are asymptomatic, they serve as the basilar layer, which can be infected by N. gonorrhoeae. The intense
the source of spread of infection. Before the antibiotic era, symptoms of inflammation of the vagina makes the physical (speculum and bimanual)
urethritis persisted for ~8 weeks. Epididymitis is now an uncommon examination extremely painful. The vaginal mucosa is red and edema-
complication, and gonococcal prostatitis occurs rarely, if at all. Other tous, and an abundant purulent discharge is often present. Infection in the
unusual local complications of gonococcal urethritis include edema urethra and in Skene’s and Bartholin’s glands often accompanies gono-
of the penis due to dorsal lymphangitis or thrombophlebitis, submu- coccal vaginitis. Inflamed cervical erosion or abscesses in nabothian cysts
cous inflammatory “soft” infiltration of the urethral wall, periurethral may also occur. Coexisting cervicitis may result in pus in the cervical os.
abscess or fistula, inflammation or abscess of Cowper’s gland, and
seminal vesiculitis. Balanitis may develop in uncircumcised men. Anorectal Gonorrhea Because the female anatomy permits the
Gonococcal Infections in Women GONOCOCCAL CERVICITIS
spread of cervical exudate to the rectum, N. gonorrhoeae is sometimes
Mucopurulent cervicitis is a common STI diagnosis in American recovered from the rectum of women with uncomplicated gonococcal
women and may be caused by N. gonorrhoeae, C. trachomatis, and other cervicitis. The rectum is the sole site of infection in only 5% of women
organisms, including Mycoplasma genitalium (Chap. 183). Cervicitis with gonorrhea. Such women are usually asymptomatic but occa-
may coexist with candidal or trichomonal vaginitis. N. gonorrhoeae pri- sionally have acute proctitis manifested by anorectal pain or pruritus,
marily infects the columnar epithelium of the cervical os. Bartholin’s tenesmus, purulent rectal discharge, and rectal bleeding. Among MSM,
glands occasionally become infected. the frequency of gonococcal infection, including rectal infection, fell by
≥90% throughout the United States in the early 1980s, but a resurgence
of gonorrhea among MSM has been documented in several cities since
the 1990s. Gonococcal isolates from the rectum of MSM tend to be
more resistant to antimicrobial agents than are gonococcal isolates from
other sites. Gonococcal isolates with a mutation in mtrR or in the pro-
moter region of the gene that encodes for this transcriptional regulator
develop increased resistance to antimicrobial hydrophobic agents such
as bile acids and fatty acids in feces and thus are found with increased
frequency in MSM. This situation may have been responsible for higher
rates of failure of treatment for rectal gonorrhea with older regimens
consisting of penicillin or tetracyclines.
Pharyngeal Gonorrhea Pharyngeal gonorrhea is usually mild
or asymptomatic, although symptomatic pharyngitis does occasionally
occur with cervical lymphadenitis. The mode of acquisition is oral–
FIGURE 151-1 Gram’s stain of urethral discharge from a male patient with genital sexual exposure, with fellatio being a more efficient means
gonorrhea shows gram-negative intracellular monococci and diplococci. (From the of transmission than cunnilingus. In certain female adolescent pop-
Public Health Agency of Canada.) ulations in the United States, pharyngeal gonorrhea has become as
Harrisons_20e_Part5_p0859-p1648.indd 1125 6/1/18 12:04 PM
1126 common as genital gonorrhea. Most cases resolve spontaneously, and incidence of DGI at present is probably attributable to a decline in
transmission from the pharynx to sexual contacts is rare. Pharyngeal the prevalence of particular strains that are likely to disseminate. DGI
infection almost always coexists with genital infection. Swabs from the strains resist the bactericidal action of human serum and generally do
pharynx should be plated directly onto gonococcal selective media. not incite inflammation at genital sites, probably because of limited
Pharyngeal colonization with N. meningitidis needs to be differentiated generation of chemotactic factors. Strains recovered from DGI cases in
from that with other Neisseria species. the 1970s were often of the PorB.1A serotype, were highly susceptible
to penicillin, and had special growth requirements—including argin-
Ocular Gonorrhea in Adults Ocular gonorrhea in an adult ine, hypoxanthine, and uracil—that made the organism more fastidi-
usually results from autoinoculation of N. gonorrhoeae from an infected ous and more difficult to isolate.
genital site. As in genital infection, the manifestations range from Menstruation is a risk factor for dissemination, and approximately
severe to occasionally mild or asymptomatic disease. The variability in two-thirds of cases of DGI are in women. In about half of affected women,
clinical manifestations may be attributable to differences in the ability symptoms of DGI begin within 7 days of onset of menses. Complement
of the infecting strain to elicit an inflammatory response. Infection may deficiencies, especially of the components involved in the assembly of
result in a markedly swollen eyelid, severe hyperemia and chemosis, the membrane attack complex (C5 through C9), predispose to neisserial
and a profuse purulent discharge. The massively inflamed conjunctiva bacteremia, and persons with more than one episode of DGI should be
may be draped over the cornea and limbus. Lytic enzymes from the screened with an assay for total hemolytic complement activity.
infiltrating PMNs occasionally cause corneal ulceration and rarely The clinical manifestations of DGI have sometimes been classified
cause perforation. into two stages: a bacteremic stage, which is less common today, and a
Prompt recognition and treatment of this condition are of para- joint-localized stage with suppurative arthritis. A clear-cut progression
mount importance. Gram’s stain and culture of the purulent discharge usually is not evident. Patients in the bacteremic stage have higher
establish the diagnosis. Genital cultures also should be performed. temperatures, and chills more frequently accompany their fever. Pain-
Gonorrhea in Pregnant Women, Neonates, and Children ful joints are common and often occur together with tenosynovitis and
Gonorrhea in pregnancy can have serious consequences for both the skin lesions. Polyarthralgias usually include the knees, elbows, and
mother and the infant. Recognition of gonorrhea early in pregnancy more distal joints; the axial skeleton is generally spared. Skin lesions
also identifies a population at risk for other STIs, particularly chlamy- are seen in ~75% of patients and include papules and pustules, often
dial infection, syphilis, and trichomoniasis. The risks of salpingitis and with a hemorrhagic component (Fig. 151-2; see also Fig. A1-43). Other
PID—conditions associated with a high rate of fetal loss—are highest manifestations of noninfectious dermatitis, such as nodular lesions,
during the first trimester. Pharyngeal infection, most often asymptom- urticaria, and erythema multiforme, have been described. These lesions
atic, may be more common during pregnancy because of altered sexual are usually on the extremities and number between 5 and 40. The
PART 5
practices. Prolonged rupture of the membranes, premature delivery, differential diagnosis of the bacteremic stage of DGI includes reactive
chorioamnionitis, funisitis (infection of the umbilical cord stump), and arthritis, acute rheumatoid arthritis, sarcoidosis, erythema nodosum,
sepsis in the infant (with N. gonorrhoeae detected in the newborn’s gastric drug-induced arthritis, and viral infections (e.g., hepatitis B and acute
aspirate during delivery) are common complications of maternal gono- HIV infection). The distribution of joint symptoms in reactive arthritis
coccal infection at term. Other conditions and microorganisms, includ- differs from that in DGI (Fig. 151-3), as do the skin and genital mani-
Infectious Diseases
ing Mycoplasma hominis, Ureaplasma urealyticum, C. trachomatis, and festations (Chap. 355).
bacterial vaginosis (often accompanied by infection with Trichomonas Suppurative arthritis involves one or two joints, most often the
vaginalis), have been associated with similar complications. knees, wrists, ankles, and elbows (in decreasing order of frequency);
The most common form of gonorrhea in neonates is ophthalmia neo- other joints occasionally are involved. Most patients who develop
natorum, which results from exposure to infected cervical secretions gonococcal septic arthritis do so without prior polyarthralgias or skin
during parturition. Ocular neonatal instillation of a prophylactic agent lesions; in the absence of symptomatic genital infection, this disease
(e.g., 1% silver nitrate eye drops or ophthalmic preparations containing cannot be distinguished from septic arthritis caused by other patho-
erythromycin or tetracycline) prevents ophthalmia neonatorum but is gens. The differential diagnosis of acute arthritis in young adults is dis-
not effective for its treatment, which requires systemic antibiotics. The cussed in Chap. 125. Rarely, osteomyelitis complicates septic arthritis
clinical manifestations are acute and usually begin 2–5 days after birth. involving small joints of the hand.
An initial nonspecific conjunctivitis with a serosanguineous discharge Gonococcal endocarditis, although rare today, was a relatively
is followed by tense edema of the eyelids, chemosis, and a profuse, common complication of DGI in the preantibiotic era, accounting for
thick, purulent discharge. Corneal ulcerations that result in nebulae about one-quarter of reported cases of endocarditis. Another unusual
or perforation may lead to anterior synechiae, anterior staphyloma, complication of DGI is meningitis.
panophthalmitis, and blindness. Infections described at other mucosal
Gonococcal Infections in HIV-Infected Persons The associ-
sites in infants, including vaginitis, rhinitis, and anorectal infection, are
ation between gonorrhea and the acquisition of HIV has been demon-
likely to be asymptomatic. Pharyngeal colonization has been demon-
strated in several well-controlled studies, mainly in Kenya and Zaire.
strated in 35% of infants with gonococcal ophthalmia, and coughing is
The nonulcerative STIs enhance the transmission of HIV three- to
the most prominent symptom in these cases. Septic arthritis (see below)
fivefold; transmission of HIV-infected immune cells and increased
is the most common manifestation of systemic infection or DGI in the
viral shedding by persons with urethritis or cervicitis may contribute
newborn. The onset usually comes at 3–21 days of age, and polyartic-
(Chap. 197). HIV has been detected by polymerase chain reaction (PCR)
ular involvement is common. Sepsis, meningitis, and pneumonia are
more commonly in ejaculates from HIV-positive men with gonococcal
seen in rare instances.
urethritis than in those from HIV-positive men with nongonococcal
Any STI in children beyond the neonatal period raises the possi-
urethritis. PCR positivity diminishes twofold after appropriate ther-
bility of sexual abuse. Gonococcal vulvovaginitis is the most common
apy for urethritis. Not only does gonorrhea enhance the transmission
manifestation of gonococcal infection in children beyond infancy. Ano-
of HIV, but it may also increase the individual’s risk for acquisition
rectal and pharyngeal infections are common in these children and are
of HIV. A proposed mechanism is the significantly greater number of
frequently asymptomatic. The urethra, Bartholin’s and Skene’s glands,
CD4+ T lymphocytes and dendritic cells that can be infected by HIV in
and the upper genital tract are rarely involved. All children with
endocervical secretions from women with nonulcerative STIs than in
gonococcal infection should also be evaluated for chlamydial infection,
those from women with ulcerative STIs.
syphilis, and possibly HIV infection.
Gonococcal Arthritis (DGI) DGI (gonococcal arthritis) results ■ LABORATORY DIAGNOSIS
from gonococcal bacteremia. In the 1970s, DGI occurred in ~0.5–3% A rapid diagnosis of gonococcal infection in men may be obtained
of persons with untreated gonococcal mucosal infection. The lower by Gram’s staining of urethral exudates (Fig. 151-1). The detection of
Harrisons_20e_Part5_p0859-p1648.indd 1126 6/1/18 12:04 PM
(e.g., when specimens for culture are 1127
to be mailed), culture media with self-
contained CO2-generating systems (such
as the JEMBEC or Gono-Pak systems)
may be used. Specimens should also be
obtained for the diagnosis of chlamydial
infection (Chap. 184).
PMNs are often seen in the endocer-
vix on a Gram’s stain, and an abnor-
mally increased number (≥30 PMNs per
field in five 1000× oil-immersion micro-
scopic fields) establishes the presence
of an inflammatory discharge. Unfortu-
nately, the presence or absence of gram-
negative intracellular monococci or
diplococci in cervical smears does not
accurately predict which patients have
gonorrhea, and the diagnosis in this set-
ting should be made by culture or another
suitable nonculture diagnostic method.
The sensitivity of a single endocervical
culture is ~80–90%. If a history of rectal
sex is elicited, a rectal wall swab (uncon-
taminated with feces) should be cultured.
A presumptive diagnosis of gonorrhea can-
FIGURE 151-2 Characteristic skin lesions in patients with proven gonococcal bacteremia. The lesions are in not be made on the basis of gram-negative
various stages of evolution. A. Very early petechia on finger. B. Early papular lesion, 7 mm in diameter, on lower leg.
diplococci in smears from the pharynx,
C. Pustule with central eschar resulting from early petechial lesion. D. Pustular lesion on finger. E. Mature lesion
with central necrosis (black) on hemorrhagic base. F. Bullae on anterior tibial surface. (Reprinted with permission where other Neisseria species are compo-
CHAPTER 151 Gonococcal Infections
from KK Holmes et al: Disseminated gonococcal infection. Ann Intern Med 74:979, 1971.) nents of the normal flora.
Several nucleic acid amplification tests
(NAATs), including the Roche COBAS
gram-negative intracellular monococci and diplococci is usually highly AMPLICOR, Gen-Probe Aptima Combo 2, and BD ProbeTec ET, are
specific and sensitive in diagnosing gonococcal urethritis in symp- now widely available on semiautomated or fully automated platforms
tomatic males but is only ~50% sensitive in diagnosing gonococcal and are the most commonly employed diagnostic tests for gonorrhea.
cervicitis. Samples should be collected with Dacron or rayon swabs. These tests also detect C. trachomatis and are more sensitive than cul-
Part of the sample should be inoculated onto a plate of modified ture for identification of either N. gonorrhoeae or C. trachomatis. The
Thayer-Martin or other gonococcal selective medium for culture. It is Gen-Probe and BD tests offer the advantage that urine samples can be
important to process all samples immediately because gonococci do not tested with a sensitivity similar to or greater than that obtained when
tolerate drying. If plates cannot be incubated immediately, they can be urethral or cervical swab samples are assessed by other non-NAATs
held safely for several hours at room temperature in candle extinction or culture, respectively. A disadvantage of non-culture-based assays is
jars prior to incubation. If processing is to occur within 6 h, transport of that N. gonorrhoeae cannot be grown from the transport systems. Thus
specimens may be facilitated by the use of nonnutritive swab transport a culture-confirmatory test and formal antimicrobial susceptibility test-
systems such as Stuart or Amies medium. For longer holding periods ing, if needed, cannot be performed.
Because of the legal implications, the preferred method for the diag-
nosis of gonococcal infection in children is a standardized culture. Two
positive NAATs, each targeting a different nucleic acid sequence, may
Disseminated gonococcal infection Reactive arthritis be substituted for culture of the cervix or the urethra as legal evidence
(N = 102) (N = 173) of infection in children. Although nonculture tests for gonococcal infec-
Hand and fingers tion have not been approved by the U.S. Food and Drug Administra-
tion for use with specimens obtained from the pharynx and rectum of
Wrist infected children, NAATs from these sites are preferred for diagnostic
Elbow evaluation in adult victims of suspected sexual abuse, especially if the
NAATs have been evaluated by the local laboratory and found to be
Shoulder superior. Cultures should be obtained from the pharynx and anus of
Sternal* both girls and boys, the urethra of boys, and the vagina of girls; cervical
specimens are not recommended for prepubertal girls. For boys with a
Spine and SI †
urethral discharge, a meatal specimen of the discharge is adequate for
Hip culture. Presumptive colonies of N. gonorrhoeae should be identified
definitively by at least two independent methods.
Knee
Blood should be cultured in suspected cases of DGI. The use of Isola-
Ankle tor blood culture tubes may enhance the yield. The probability of posi-
tive blood cultures decreases after 48 h of illness. Synovial fluid should
Foot and toes
be inoculated into blood culture broth medium and plated onto choco-
60 50 40 30 20 10 0 10 20 30 40 50 60
late agar rather than selective medium because this fluid is not likely to
be contaminated with commensal bacteria. Gonococci are infrequently
Percent of patients
recovered from early joint effusions containing <20,000 leukocytes/μL
FIGURE 151-3 Distribution of joints with arthritis in 102 patients with but may be recovered from effusions containing >80,000 leukocytes/μL.
disseminated gonococcal infection and 173 patients with reactive arthritis. The organisms are seldom recovered from blood and synovial fluid of
*
Includes the sternoclavicular joints. †SI, sacroiliac joint. the same patient.
Harrisons_20e_Part5_p0859-p1648.indd 1127 6/1/18 12:04 PM
1128 gonorrhea and ease of use. The recommendations for uncomplicated
TREATMENT
gonorrhea apply to HIV-infected as well as HIV-uninfected patients.
Gonococcal Infections The currently recommended regimen for the treatment of uncom-
plicated gonococcal infection of the urethra, cervix, rectum, or
Treatment failure can lead to continued transmission and the emer- pharynx (a single IM dose of ceftriaxone plus a single dose of azith-
gence of antibiotic resistance. The importance of adequate treatment romycin taken orally) almost always results in an effective cure.
with a regimen that the patient will adhere to cannot be overempha- Quinolone-containing regimens are no longer recommended in the
sized. Thus highly effective single-dose regimens have been devel- United States as first-line treatment because of widespread resis-
oped for uncomplicated gonococcal infections. The 2015 treatment tance. A multicenter trial of treatment for uncomplicated gonorrhea
guidelines for gonococcal infections from the CDC are summarized in the United States showed ≥99.5% efficacy of two combination reg-
in Table 151-1. Rising MICs of cefixime worldwide have led the imens: (1) gemifloxacin (320 mg, single oral dose) plus azithromycin
CDC to discontinue its recommendation of this agent as first-line (2 g, single oral dose) or (2) azithromycin (2 g, single oral dose) plus
treatment for uncomplicated gonorrhea. The third-generation cepha- gentamicin (a single IM dose of 240 mg or, in individuals who weigh
losporin ceftriaxone in combination with azithromycin is recom- ≤45 kg, 5 mg/kg). At this time, however, neither of these regimens is
mended as treatment; dual therapy against gonorrhea could slow recommended as first-line treatment.
the development of resistance to either of these antimicrobial Co-infection with C. trachomatis occurs frequently; treatment of
agents. Azithromycin, which also treats nongonococcal urethritis, gonorrhea with ceftriaxone that also includes a single 1-g dose
is preferred to doxycycline because of its superior activity against of azithromycin is effective against chlamydial infection. However,
a 1-g dose of azithromycin used alone as treatment for gonorrhea
TABLE 151-1 Recommended Treatment for Gonococcal Infections: in penicillin-allergic persons results in an unacceptably low cure
Adapted from the 2015 Guidelines of the Centers for Disease Control rate (93%) for gonococcal infections and should not be used. A sin-
and Prevention gle 2-g dose of azithromycin, particularly in the extended-release
DIAGNOSIS TREATMENT OF CHOICEa microsphere formulation, delivers azithromycin to the lower gas-
Uncomplicated gonococcal trointestinal tract, thereby improving tolerability. Azithromycin is
infection of the cervix, urethra, effective against sensitive strains, but this drug is expensive, causes
pharynxb, or rectum gastrointestinal distress, and is not recommended for routine or
First-line regimen Ceftriaxone (250 mg IM, single dose) first-line treatment of gonorrhea. Spectinomycin has been used as
plus an alternative agent for the treatment of uncomplicated gonococcal
Azithromycin (1 g PO, single dose) infections in penicillin-allergic persons outside the United States but
PART 5
Alternative regimensc Cefixime (400 mg PO, single dose) or is not currently available in this country. Of note, the limited effec-
ceftizoxime (500 mg IM, single dose) or tiveness of spectinomycin for the treatment of pharyngeal infection
cefotaxime (500 mg IM, single dose) or reduces its utility in populations among whom such infection is
spectinomycin (2 g IM, single dose)d,e common, such as MSM.
or cefotetan (1 g IM, single dose) plus Persons with uncomplicated infections who receive ceftriaxone
Infectious Diseases
probenecid (1 g PO, single dose)d or
and azithromycin do not need a test of cure; however, cultures for
cefoxitin (2 g IM, single dose) plus
probenecid (1 g PO, single dose)d N. gonorrhoeae should be performed if symptoms persist after therapy
plus
with an established regimen, and any gonococci isolated should
be tested for antimicrobial susceptibility. Persons given an alterna-
Azithromycin (1 g PO, single dose)
tive regimen should return for a test of cure targeting the infected
Epididymitis See Chap. 131
anatomic site. This test ideally should be a culture. If culture is not
Pelvic inflammatory disease See Chap. 131 readily available and NAAT is positive, every effort should be made
Gonococcal conjunctivitis in Ceftriaxone (1 g IM, single dose)f to perform a confirmatory culture. All isolates from test-of-cure cul-
an adult tures should undergo antimicrobial susceptibility testing. Because of
Ophthalmia neonatorumg Ceftriaxone (25–50 mg/kg IV, single high rates of reinfection with N. gonorrhoeae and C. trachomatis within
dose, not to exceed 125 mg)
6 months, repeat testing is recommended 3 months after treatment.
Disseminated gonococcal Symptomatic gonococcal pharyngitis is more difficult to eradicate
infectionh
than genital infection. Persons who cannot tolerate ceftriaxone and
Initial therapyi those in whom quinolones are contraindicated may be treated with
Patient tolerant of β-lactam Ceftriaxone (1 g IM or IV q24h; spectinomycin if it is available, but this agent results in a cure rate of
drugs recommended) or cefotaxime (1 g IV q8h)
≤52%. Persons given spectinomycin should have a pharyngeal sam-
or ceftizoxime (1 g IV q8h)
ple cultured 3–5 days after treatment as a test of cure. A single 2-g
Patients allergic to β-lactam Spectinomycin (2 g IM q12h)d
dose of azithromycin may be used in areas where rates of resistance
drugs
to azithromycin are low.
Continuation therapyi Cefixime (400 mg PO bid)
Treatments for gonococcal epididymitis and PID are discussed in
Meningitis or endocarditis See text for specific recommendationsj Chap. 131. Ocular gonococcal infections in older children and adults
a
True failure of treatment with a recommended regimen is rare and should should be managed with a single dose of ceftriaxone combined
prompt an evaluation for reinfection, infection with a drug-resistant strain, or with saline irrigation of the conjunctivae (both undertaken expe-
an alternative diagnosis. bCeftriaxone and azithromycin are the only agents
recommended for treatment of pharyngeal infection. cSee text for follow-up of ditiously), and patients should undergo a careful ophthalmologic
persons with infection who are treated with alternative regimens. dSpectinomycin, evaluation that includes a slit-lamp examination.
cefotetan, and cefoxitin, which are alternative agents, currently are unavailable DGI may require higher dosages and longer durations of therapy
or in short supply in the United States. eSpectinomycin may be ineffective for the
treatment of pharyngeal gonorrhea. fPlus lavage of the infected eye with saline (Table 151-1). Hospitalization is indicated if the diagnosis is uncer-
solution (once). gProphylactic regimens are discussed in the text. hHospitalization tain, if the patient has localized joint disease that requires aspiration,
is indicated if the diagnosis is uncertain, if the patient has frank arthritis with an or if the patient cannot be relied on to comply with treatment. Open
effusion, or if the patient cannot be relied on to adhere to treatment. iAll initial
regimens should also include azithromycin (1 g PO, single dose) and should be
drainage is necessary only occasionally—e.g., for management of
continued for 24–48 h after clinical improvement begins, at which time the switch hip infections that may be difficult to drain percutaneously. Nonste-
may be made to an oral agent (e.g., cefixime) if antimicrobial susceptibility can be roidal anti-inflammatory agents may be indicated to alleviate pain
documented by culture of the causative organism. If no organism is isolated and
the diagnosis is secure, then treatment with ceftriaxone should be continued for
and hasten clinical improvement of affected joints.
at least 1 week. jHospitalization is indicated to exclude suspected meningitis or Gonococcal meningitis and endocarditis should be treated in the
endocarditis. hospital with high-dose IV ceftriaxone (1–2 g IV every 12–24 h);
Harrisons_20e_Part5_p0859-p1648.indd 1128 6/1/18 12:04 PM
therapy should continue for 10–14 days for meningitis and for at least TABLE 152-1 Characteristics of Type b and Nontypable Strains of 1129
4 weeks for endocarditis. All persons who experience more than Haemophilus influenzae
one episode of DGI should be evaluated for complement deficiency. FEATURE TYPE b STRAINS NONTYPABLE STRAINS
Capsule Ribosyl-ribitol phosphate Unencapsulated
■ PREVENTION AND CONTROL Pathogenesis Invasive infections Mucosal infections due
Condoms, if properly used, provide effective protection against the due to hematogenous to contiguous spread
transmission and acquisition of gonorrhea as well as other infections spread
that are transmitted to and from genital mucosal surfaces. Spermicidal Clinical manifestations Meningitis and Otitis media in infants
preparations used with a diaphragm or cervical sponges impregnated invasive infections in and children; lower
with nonoxynol-9 offer some protection against gonorrhea and chlamy- incompletely immunized respiratory tract
dial infection. However, the frequent use of preparations that contain infants and children infections in adults with
chronic bronchitis
nonoxynol-9 is associated with mucosal disruption that paradoxically
Evolutionary history Basically clonal Genetically diverse
may enhance the risk of HIV infection in the event of exposure. All
patients should be instructed to refer sex partners for evaluation and Vaccine Highly effective Under development
conjugate vaccines
treatment. All sex partners of persons with gonorrhea should be eval-
uated and treated for N. gonorrhoeae and C. trachomatis infections if
their last contact with the patient took place within 60 days before the variable shape; thus, it is often described as a pleomorphic coccobacil-
onset of symptoms or the diagnosis of infection in the patient. If the lus. In clinical specimens such as cerebrospinal fluid (CSF) and sputum,
patient’s last sexual encounter was >60 days before onset of symptoms H. influenzae frequently stains only faintly with safranin and therefore
or diagnosis, the patient’s most recent sex partner should be treated. can easily be overlooked.
Partner-delivered medications or prescriptions for medications to H. influenzae grows both aerobically and anaerobically. Its aerobic
treat gonorrhea and chlamydial infection diminish the likelihood of growth requires two factors: hemin (X factor) and nicotinamide adenine
reinfection (or relapse) in the infected patient. In states where it is dinucleotide (V factor). These requirements are used in the clinical lab-
not prohibited, this approach is an option for partner management. oratory to identify the bacterium. Caution must be used to distinguish
Patients should be instructed to abstain from sexual intercourse until H. influenzae from Haemophilus haemolyticus, a respiratory tract com-
therapy is completed and until they and their sex partners no longer mensal that has identical growth requirements. H. haemolyticus has clas-
have symptoms. Greater emphasis must be placed on prevention by sically been distinguished from H. influenzae by the hemolysis of the
public health education, individual patient counseling, and behavior former species on horse blood agar. However, a significant proportion
CHAPTER 152 Haemophilus and Moraxella Infections
modification, particularly the use of condoms. Sexually active persons, of isolates of H. haemolyticus have now been recognized as nonhemo-
especially adolescents, should be offered screening for STIs. For male lytic. Analysis of various genotypic and phenotypic markers, includ-
patients, NAAT of urine or a urethral swab may be used for screening. ing16S ribosomal sequences, superoxide dismutase, outer-membrane
Preventing the spread of gonorrhea may help reduce the transmission protein P6, protein D, and fuculose kinase, can be used to distinguish
of HIV. No effective vaccine for gonorrhea is yet available, but efforts these two species.
to test several candidates are underway. Six major serotypes of H. influenzae have been identified; designated
■ FURTHER READING a through f, they are based on antigenically distinct polysaccharide cap-
Bolan GA et al: The emerging threat of untreatable gonococcal infec- sules. In addition, some strains lack a polysaccharide capsule and are
tion. N Engl J Med 366:485, 2012. referred to as nontypable strains. Type b and nontypable strains are the
Centers for Disease Control and Prevention: Sexually transmitted most relevant strains clinically (Table 152-1), although encapsulated
disease treatment guidelines, 2015. Morb Mortal Wkly Rep 64(RR3):1, strains other than type b can cause disease. H. influenzae was the first
2015 (www.cdc.gov/mmwr/preview/mmwrhtml/rr6403a1.htm). free-living organism to have its entire genome sequenced.
Golden MR et al: Effect of expedited treatment of sex partners on The antigenically distinct type b capsule is a linear polymer com-
recurrent or persistent gonorrhea or chlamydial infections. N Engl J posed of ribosyl-ribitol phosphate. Strains of H. influenzae type b (Hib)
Med 352:676, 2005. cause disease primarily in infants and children <6 years of age. Nonty-
Rice PA: Gonococcal arthritis (disseminated gonococcal infection). pable strains are primarily mucosal pathogens but occasionally cause
Infect Dis Clin North Am 19:853, 2005. invasive disease.
Unemo M, Shafer WM: Antimicrobial resistance in Neisseria gonor- ■ EPIDEMIOLOGY AND TRANSMISSION
rhoeae in the 21st century: Past, evolution, and future. Clin Microbiol H. influenzae, an exclusively human pathogen, is spread by airborne
Rev 27:587, 2014. droplets or by direct contact with secretions or fomites. Colonization
Wetzler LM et al: Summary and recommendations from the National with nontypable H. influenzae is a dynamic process; new strains are
Institute of Allergy and Infectious Diseases (NIAID) workshop on acquired and other strains are replaced periodically.
“Gonorrhea Vaccines: the Way Forward.” Clin Vaccine Immunol The widespread use of Hib conjugate vaccines in many indus-
23:656, 2016. trialized countries has resulted in striking decreases in the rate
of nasopharyngeal colonization by Hib and in the incidence of
Hib infection (Fig. 152-1). Worldwide, invasive Hib disease occurs pre-
152 Haemophilus
dominantly in unimmunized children and in those who have not com-
and pleted the primary immunization series. Of 194 World Health
Moraxella Infections Organization member countries, 99% have introduced Hib conjugate
vaccination, but a large number of the world’s children remain unim-
munized. Certain groups have a higher incidence of invasive Hib dis-
Timothy F. Murphy ease than the general population, including African-American and
Australian Aboriginal children and Native American groups. Although
this increased incidence has not yet been accounted for, several factors
HAEMOPHILUS INFLUENZAE may be relevant, including age at exposure to the bacterium, socioeco-
nomic conditions, and genetic differences.
■ MICROBIOLOGY
Haemophilus influenzae was first recognized in 1892 by Pfeiffer, who ■ PATHOGENESIS
erroneously concluded that the bacterium was the cause of influ- Hib strains cause systemic disease by invasion and hematogenous
enza. H. influenzae is a small (1- × 0.3-μm) gram-negative organism of spread from the respiratory tract to distant sites such as the meninges,
Harrisons_20e_Part5_p0859-p1648.indd 1129 6/1/18 12:04 PM
1316 These infections are most common among immunocompromised and cause of preventable blindness in the developing world; and urogen-
hypogammaglobulinemic patients. Ureaplasmas and M. hominis can ital infections, which are sexually or neonatally transmitted. The 18
cause septic arthritis in immunodeficient patients. Ureaplasmas proba- serovars of C. trachomatis fall into three groups: the trachoma serovars
bly cause neonatal pneumonitis; their possible causal role in the devel- A, B, Ba, and C; the oculogenital serovars D–K; and the LGV serovars
opment of bronchopulmonary dysplasia—the chronic lung disease L1–L3. Serovars can be distinguished by serologic typing with mono-
of premature infants—has been extensively investigated, with most clonal antibodies or by molecular gene typing. However, serovar
studies indicating at least a significant association. It is unclear whether identification usually is not important clinically, since the antibiotic
ureaplasmas and M. hominis cause infertility, spontaneous abortion, susceptibility pattern is the same for all three groups. The one excep-
premature labor, low birth weight, or chorioamnionitis. tion applies when LGV is suspected on clinical grounds; in this situ-
ation, serovar determination is important because a longer treatment
DIAGNOSIS duration is required for LGV strains.
Culture and PCR are both appropriate methods for the isolation of uro-
genital mycoplasmas. Culture of these organisms, however, requires BIOLOGY, GROWTH CYCLE, AND
special techniques and media that generally are available only at PATHOGENESIS
larger medical centers and reference laboratories. Serologic testing is
not recommended for the clinical diagnosis of urogenital Mycoplasma ■ BIOLOGY
infections. During their intracellular growth, chlamydiae produce characteristic
intracytoplasmic inclusions that can be visualized by direct fluores-
cent antibody or Giemsa staining of infected clinical material, such as
TREATMENT conjunctival scrapings or cervical or urethral epithelial cells. Chlamy-
Urogenital Mycoplasma Infections diae are nonmotile, gram-negative, obligate intracellular bacteria that
replicate within the cytoplasm of host cells, forming the characteristic
Because colonization with urogenital mycoplasmas is common, it membrane-bound inclusions that are the basis for some diagnostic
appears at present that their isolation from the urogenital tract in tests. Originally considered to be large viruses, chlamydiae differ from
the absence of disease generally does not warrant treatment. Mac- viruses in possessing RNA and DNA as well as a cell wall that is quite
rolides and doxycycline are considered the antimicrobial agents of similar in structure to the cell wall of typical gram-negative bacteria.
choice for Ureaplasma infections (Table 183-2). Ureaplasma resistance However, chlamydiae lack peptidoglycan; their structural integrity
to macrolides, doxycycline, quinolones, and chloramphenicol has depends on disulfide binding of outer-membrane proteins.
been reported. M. hominis is resistant to macrolides. Doxycycline
is generally the drug of choice for M. hominis infections, although ■ GROWTH CYCLE
PART 5
resistance has been reported. Clindamycin is generally active against Among the defining characteristics of chlamydiae is a unique growth
M. hominis. Quinolones are active in vitro against M. hominis. For cycle that involves alternation between two highly specialized morpho-
M. genitalium, the initial treatment of choice appears to be azith- logic forms (Figs. 184-1 and 184-2): the elementary body, which is the
romycin; moxifloxacin has been successfully used to treat M. genital- infectious form and is specifically adapted for extracellular survival,
Infectious Diseases
ium resistant to azithromycin.
■ FURTHER READING
Getman D et al: Mycoplasma genitalium prevalence, coinfection, and
macrolide antibiotic resistance frequency in a multicenter clinical
study cohort in the United States. J Clin Microbiol 54:2278, 2016.
Waites KB et al: Mycoplasma pneumoniae from the respiratory tract and
beyond. Clin Microbiol Rev 30:747, 2017.
Workowski KA, Bolan GA: Sexually transmitted diseases treatment
guidelines, 2015. MMWR Recomm Rep 64:1, 2015.
Zheng X et al: Macrolide-resistant Mycoplasma pneumoniae,
United States. Emerg Infect Dis 21:1470, 2015.
184 Chlamydial Infections
Charlotte A. Gaydos, Thomas C. Quinn
Chlamydiae are obligate intracellular bacteria that cause a wide variety
of diseases in humans and animals.
ETIOLOGIC AGENTS
The chlamydiae were originally classified as four species in the genus
Chlamydia: C. trachomatis, C. pneumoniae, C. psittaci, and C. pecorum (the
last species being found in ruminants). The C. psittaci group has been
separated into three species: C. psittaci, C. felis, and C. abortus. The
mouse pneumonitis strain (MoPn) is now classified as C. muridarum,
and the guinea pig inclusion conjunctivitis strain (GPIC) is now des-
ignated C. caviae.
FIGURE 184-1 Chlamydial intracellular inclusions filled with smaller dense
C. trachomatis is divided into two biovars: trachoma and LGV (lym- elementary bodies and larger reticulate bodies. (Reprinted with permission from
phogranuloma venereum). The trachoma biovar causes two major WE Stamm: Chlamydial infections, in Harrison’s Principles of Internal Medicine,
types of disease in humans: ocular trachoma, the leading infectious 17th ed, AS Fauci et al [eds]. New York, McGraw-Hill, 2008, p 1070.)
Harrisons_20e_Part5_p0859-p1648.indd 1316 6/1/18 12:07 PM
2. Initial inclusions The trachoma biovar is essentially a parasite of squamocolumnar 1317
1. Uptake of 3. Fusion of inclusions; epithelial cells; the LGV biovar is more invasive and involves lymphoid
chlamydial EBs appearance of RBs cells. As is typical of chlamydiae, C. trachomatis strains are capable
of causing chronic, clinically inapparent, asymptomatic infections.
Because the duration of the chlamydial growth cycle is ~48–72 h, the
incubation period of sexually transmitted chlamydial infections is
relatively long—generally 1–3 weeks. C. trachomatis causes cell death
Cell cytoplasm as a result of its replicative cycle and can induce cell damage when-
Cell membrane ever it persists. However, few toxic effects are demonstrated, and cell
Cell nucleus death because of chlamydial replication is not sufficient to account for
4. Multiplication of RBs;
6. Release enlargement of inclusion disease manifestations, the majority of which are due to immunopatho-
of EBs logic mechanisms or nonspecific host responses to the organism or its
5. Conversion of by-products.
RBs to EBs In recent years, the entire genomes of various chlamydial species
have been sequenced, the field of proteomics has become estab-
lished, host innate immunity has been more precisely delineated,
and innovative host cell–chlamydial interaction studies have been
conducted. As a result, many insights have been gained into how
8. Return to normal chlamydiae adapt and replicate in their intracellular environment and
cycle with IFN-γ
produce disease. These insights into pathogenesis include information
removal
on the regulation of gene expression, protein localization, the type III
7. Persistence associated secretion system, the roles of CD4+ and CD8+ T lymphocytes in the
with IFN-γ exposure; host response, and T lymphocyte trafficking.
large aberrant RBs The chlamydial heat-shock protein, which shares antigenic epitopes
with similar proteins of other bacteria and with human heat-shock pro-
FIGURE 184-2 Chlamydial life cycle. EBs, elementary bodies; RBs, reticulate tein, may sensitize the host, and repeated infections may cause host cell
bodies; IFN-γ, interferon γ. (Reprinted with permission from WE Stamm: Chlamydial damage. Persistent or recurrent chlamydial infections are associated
infections, in Harrison’s Principles of Internal Medicine, 17th ed, AS Fauci et al with fibrosis, scarring, and complications following simple epithelial
CHAPTER 184 Chlamydial Infections
[eds]. New York, McGraw-Hill, 2008, p 1071.) infections. A common endpoint of these late consequences is scarring
of mucous membranes. Genital complications can lead to pelvic inflam-
and the metabolically active and replicating reticulate body, which is matory disease (PID) and its late consequences of infertility, ectopic
not infectious, is adapted for an intracellular environment, and does pregnancy, and chronic pelvic pain, while ocular infections may lead
not survive well outside the host cell. The biphasic growth cycle begins to blinding trachoma. High levels of antibody to human heat-shock
with attachment of the elementary body (diameter, 0.25–0.35 μm) at protein have been associated with tubal factor infertility and ectopic
specific sites on the surface of the host cell. The elementary body enters pregnancy. Without adequate therapy, chlamydial infections may per-
the cell through a process similar to receptor-mediated endocytosis and sist for several years, although symptoms—if present—usually abate.
resides in an inclusion, where the entire growth cycle is completed. Pathogenic mechanisms of C. pneumoniae have yet to be completely
The chlamydiae prevent phagosome–lysosome fusion. The inclusion elucidated. The same is true for C. psittaci, except that this agent infects
membrane is modified by insertion of chlamydial antigens. Once the cells very efficiently and causes disease that may reflect direct cyto-
elementary body has entered the cell, it reorganizes into a reticulate pathic effects.
body, which is larger (0.5–1 μm) and contains more RNA. After ~8 h,
the reticulate body starts to divide by binary fission. The intracytoplas- C. TRACHOMATIS INFECTIONS
mic, membrane-bound inclusion body containing the reticulate bodies
increases in size as the reticulate bodies multiply. Approximately 18–24 h ■ GENITAL INFECTIONS (SEE ALSO CHAP. 131)
after infection of the cell, these reticulate bodies begin to become ele- Spectrum Although chlamydiae cause a number of human dis-
mentary bodies by a reorganization or condensation process that is eases, localized lower genital tract infections caused by C. trachomatis
poorly understood. After rupture of the inclusion body, the elementary and the sequelae of such infections are the most important in terms
bodies are released to initiate another cycle of infection. of medical and economic impact. Oculogenital infections due to
Chlamydiae are susceptible to many broad-spectrum antibiotics and C. trachomatis serovars D–K are transmitted during sexual contact or
possess a number of enzymes, but they have a very restricted metabolic from mother to baby during childbirth and are associated with many
capacity. None of these metabolic reactions result in the production of syndromes, including cervicitis, salpingitis, acute urethral syndrome,
energy. Chlamydiae have thus been considered to be energy parasites endometritis, ectopic pregnancy, infertility, and PID in female patients;
that use the ATP produced by the host cell for their own metabolic urethritis, proctitis, and epididymitis in male patients; and conjunc-
functions. Many aspects of chlamydial molecular biology are not well tivitis and pneumonia in infants. Women bear the greatest burden of
understood, but the sequencing of several chlamydial genomes and morbidity because of the serious sequelae of these infections. Untreated
new proteomics research have provided researchers with many rele- infections lead to PID, and multiple episodes of PID can lead to tubal
vant tools for elucidating the biology of the life cycle. factor infertility and chronic pelvic pain. Studies estimate that up to
80–90% of women and >50% of men with C. trachomatis genital infec-
■ PATHOGENESIS tions lack symptoms; other patients have very mild symptoms. Thus,
Genital infections are mostly caused by C. trachomatis serovars D–K,
a large reservoir of infected persons continues to transmit infection to
with serovars D, E, and F involved most often. Molecular typing of
sexual partners.
the major outer-membrane protein gene (omp1) from which serovar
As their designations reflect, the LGV serovars (L1, L2, and L3) cause
differences arise has been used to demonstrate that polymorphisms can
LGV, an invasive sexually transmitted disease (STD) characterized by
occur in isolates from patients who are exposed frequently to multiple
acute lymphadenitis with bubo formation and/or acute hemorrhagic
infections, while less variation is observed in isolates from less sexu-
proctitis (see “LGV,” below).
ally active populations. Polymorphisms in the major outer-membrane
protein may provide antigenic variation, and the different forms allow Epidemiology GLOBAL EPIDEMIOLOGY C. trachomatis
persistence in the community because immunity to one is not protec- genital infections are global in distribution. The World Health
tive against the others. Organization (WHO) estimated in 2008 that >106.4 million
Harrisons_20e_Part5_p0859-p1648.indd 1317 6/1/18 12:07 PM
1318 cases occur annually worldwide. This figure makes chlamydial infec- of involvement of C. trachomatis in urethral infection ranges from 3–7%
tion the most prevalent bacterial sexually transmitted infection in the among asymptomatic men to 15–20% among symptomatic men attending
world. The associated morbidity is substantial, and the economic cost STD clinics. One recent multisite study of men in Baltimore, Seattle,
is high. Denver, and San Francisco reported an overall chlamydial prevalence
U.S. EPIDEMIOLOGY In the United States, these infections are the most of 7% in urine samples assessed by nucleic acid amplification tests
commonly reported of all infectious diseases. In 2015, 1,526,658 cases (NAATs)—molecular tests that amplify the nucleic acids in clinical
were reported to the U.S. Centers for Disease Control and Prevention specimens. As in women, infection in men is age related, with young
(CDC); however, the CDC estimates that 2–3 million new cases occur age as the greatest risk factor for chlamydial urethritis. The prevalence
per year, with substantial underreporting due to lack of screening in among men is highest at 20–24 years of age. In STD clinics, urethritis is
some populations. Rates of infection have increased every year; higher usually less prevalent among MSM than among heterosexual men and
rates among women than among men reflect the focus on expansion of is almost always much more common among black men than among
screening programs for women during the past 25 years. Use of increas- white men. One study reported prevalences of 19 and 9% among non-
ingly sensitive diagnostic amplification tests, an increased emphasis on white and white heterosexual men, respectively.
case reporting, and improvements in the information systems used NGU is diagnosed by documentation of a leukocyte urethral exu-
have elevated the number of cases reported every year. The CDC and date and by exclusion of gonorrhea by Gram’s staining or culture. C.
other professional organizations recommend annual screening of all trachomatis urethritis is generally less severe than gonococcal urethritis,
sexually active women <25 years of age as well as rescreening of previ- although in any individual patient these two forms of urethritis cannot
ously infected individuals at 3 months. The case count corresponds to reliably be differentiated solely on clinical grounds. Symptoms include
478.8 cases per 100,000 population, an increase of 5.9% compared with urethral discharge (often whitish and mucoid rather than frankly puru-
the rate in 2014. Young women have the highest infection rates (645.5 lent), dysuria, and urethral itching. Physical examination may reveal
cases per 100,000)—more than twice the rate among men. Interestingly, meatal erythema and tenderness as well as a urethral exudate that is
with the increased availability of urine testing and extragenital testing, often demonstrable only by stripping of the urethra.
men—including gay, bisexual, and other men who have sex with men At least one-third of male patients with C. trachomatis urethral infec-
(MSM)—are increasingly being tested for chlamydial infection. From tion have no evident signs or symptoms of urethritis. The availability
2011 to 2015, rates of chlamydial infection in men increased by 20.0%, of NAATs for first-void urine specimens has facilitated broader-based
whereas rates in women rose by only 0.3% during this period. Chlamy- testing for asymptomatic infection in male patients. As a result,
dial infection rates vary among different racial and ethnic minority asymptomatic chlamydial urethritis has been demonstrated in 5–10%
populations. In 2015, rates among African Americans and American of sexually active male adolescents screened at school-based clinics or
Indians/Alaska Natives were 5.9 and 3.8 times that among Caucasians, community centers. Such patients generally have pyuria (≥15 leuko-
PART 5
respectively. These disparities are important reflections of health ineq- cytes per 400× microscopic field in the sediment of first-void urine), a
uities in the United States. positive leukocyte esterase test, or an increased number of leukocytes
The aforementioned statistics are based on case reporting. Stud- on a Gram-stained smear prepared from a urogenital swab inserted
ies based on screening surveys estimate that the U.S. prevalence of 1–2 cm into the anterior urethra. When specific diagnostic tests for
C. trachomatis cervical infection is 5% among asymptomatic female chlamydiae are not available, the examination of an endourethral
Infectious Diseases
college students and prenatal patients, >10% for women seen in family specimen for increased leukocytes is useful in differentiating between
planning clinics, and >20% for women seen in STD clinics. The prev- true urethritis and functional symptoms in symptomatic patients or in
alence of genital C. trachomatis infections varies substantially by geo- making a presumptive diagnosis of C. trachomatis infection in high-risk
graphic locale, with the highest rates in the southeastern United States. but asymptomatic men (e.g., male patients in STD clinics, sex partners
The prevalence of C. trachomatis in the cervix of pregnant women is of women with nongonococcal salpingitis or mucopurulent cervicitis,
5–10 times higher than that of Neisseria gonorrhoeae. The prevalence fathers of children with inclusion conjunctivitis). Alternatively, urethri-
of genital infection with either agent is highest among women who tis can be assayed noninvasively by examination of a first-void urine
are between the ages of 18 and 24, single, and non-Caucasian. Recur- sample for pyuria, either by microscopy or by the leukocyte esterase
rent infections are common in these same risk groups and are often test. Urine (or a urethral swab) can also be tested directly for chlamy-
acquired from untreated sexual partners. The use of oral contraception diae by DNA amplification methods (NAATs), as described below (see
and the presence of cervical ectopy also confer an increased risk. The “Detection Methods”).
proportion of infections that are asymptomatic appears to be higher for EPIDIDYMITIS Chlamydial urethritis may be followed by acute epi-
C. trachomatis than for N. gonorrhoeae, and symptomatic C. trachomatis didymitis, but this condition is rare, generally occurring in sexually
infections are clinically less severe. Mild or asymptomatic C. trachomatis active patients <35 years of age; in older men, epididymitis is usually
infections of the fallopian tubes nonetheless cause ongoing tubal dam- associated with gram-negative bacterial infection and/or instrumenta-
age and infertility. The costs of C. trachomatis infections and their com- tion procedures. An estimated 50–70% of cases of acute epididymitis
plications to the U.S. health care system have recently been estimated are caused by C. trachomatis. The condition usually presents as unilat-
to be >$516.7 million annually. eral scrotal pain with tenderness, swelling, and fever in a young man,
often occurring in association with chlamydial urethritis. The illness
Clinical Manifestations NONGONOCOCCAL AND POSTGONO-
may be mild enough to treat with oral antibiotics on an outpatient
COCCAL URETHRITIS C. trachomatis is the most common cause of
basis or severe enough to require hospitalization and parenteral ther-
nongonococcal urethritis (NGU) and postgonococcal urethritis (PGU).
apy. Testicular torsion should be excluded promptly by radionuclide
The designation PGU refers to NGU developing in men 2–3 weeks after
scan, Doppler flow study, or surgical exploration in a teenager or
treatment of gonococcal urethritis with single doses of agents such as
young adult who presents with acute unilateral testicular pain with-
penicillin or cephalosporins, which lack antimicrobial activity against
out urethritis. The possibility of testicular tumor or chronic infection
chlamydiae. Current treatment regimens for gonorrhea have evolved
(e.g., tuberculosis) should be excluded when a patient with unilateral
and now include combination therapy with ceftriaxone and azithromy-
intrascrotal pain and swelling does not respond to appropriate antimi-
cin; this current regimen is effective against concomitant chlamydial
crobial therapy.
infection. Thus both the incidence of PGU and the causative role of C.
trachomatis in this syndrome have declined. REACTIVE ARTHRITIS Reactive arthritis consists of conjunctivitis, ure-
In the United States, most of the estimated 2 million cases of acute thritis (or, in female patients, cervicitis), arthritis, and characteristic
urethritis are NGU, and C. trachomatis is implicated in 30–50% of these mucocutaneous lesions. It may develop in 1–2% of cases of NGU and is
cases. The cause of most of the remaining cases of NGU is uncertain, thought to be the most common type of peripheral inflammatory arthri-
but recent evidence suggests that Mycoplasma genitalium, Trichomonas tis in young men. C. trachomatis has been recovered from the urethra of
vaginalis, and herpes simplex virus (HSV) cause some cases. The rate 16–44% of patients with reactive arthritis and 69% of men who have
Harrisons_20e_Part5_p0859-p1648.indd 1318 6/1/18 12:07 PM
signs of urogenital inflammation at the time of examination. Antibodies MUCOPURULENT CERVICITIS Although most women with chlamydial 1319
to C. trachomatis have also been detected in 46–67% of patients with infections of the cervix have no symptoms, almost half generally
reactive arthritis, and Chlamydia-specific cell-mediated immunity has have local signs of infection on examination. Cervicitis is usually
been documented in 72%. In addition, C. trachomatis has been isolated characterized by the presence of a mucopurulent discharge, with >20
from synovial biopsy samples from 15 of 29 patients in a number of neutrophils per microscopic field visible in strands of cervical mucus
small series and from a smaller proportion of synovial fluid specimens. in a thinly smeared, gram-stained preparation of endocervical exudate.
Chlamydial nucleic acids have been identified in synovial membranes Hypertrophic ectopy of the cervix may also be evident as an edematous
and chlamydial elementary bodies in joint fluid. The pathogenesis of area near the cervical os that is congested and bleeds easily on minor
reactive arthritis is unclear, but this condition probably represents an trauma (e.g., when a specimen is collected with a swab). A Papanico-
abnormal host response to a number of infectious agents, including laou smear shows increased numbers of neutrophils as well as a char-
those associated with bacterial gastroenteritis (e.g., Salmonella, Shig- acteristic pattern of mononuclear inflammatory cells, including plasma
ella, Yersinia, or Campylobacter), or to infection with C. trachomatis or cells, transformed lymphocytes, and histiocytes. Cervical biopsy shows
N. gonorrhoeae. Since >80% of affected patients have the HLA-B27 a predominantly mononuclear cell infiltrate of the subepithelial stroma.
phenotype and since other mucosal infections produce an identical Clinical experience and collaborative studies indicate that a cutoff of
syndrome, chlamydial infection is thought to initiate an aberrant >30 polymorphonuclear leukocytes (PMNs)/1000× field in a gram-
hyperreactive immune response that produces inflammation of the stained smear of cervical mucus correlates best with chlamydial or
involved target organs in these genetically predisposed individu- gonococcal cervicitis.
als. Evidence of exaggerated cell-mediated and humoral immune Clinical recognition of chlamydial cervicitis depends on a high index
responses to chlamydial antigens in reactive arthritis supports this of suspicion and careful cervical examination. No genital symptoms
hypothesis. The finding of chlamydial elementary bodies and DNA in are specifically correlated with chlamydial cervical infection. The dif-
joint fluid and synovial tissue from patients with reactive arthritis sug- ferential diagnosis of a mucopurulent discharge from the endocervical
gests that chlamydiae may actually spread from genital to joint tissues canal in a young, sexually active woman includes gonococcal endocer-
in these patients—perhaps in macrophages. vicitis, salpingitis, endometritis, and intrauterine contraceptive device–
NGU is the initial manifestation of reactive arthritis in 80% of induced inflammation. Diagnosis of cervicitis is based on the presence
patients, typically occurring within 14 days after sexual exposure. The of PMNs on a cervical swab as noted above; the presence of chlamydiae
urethritis may be mild and may even go unnoticed by the patient. is confirmed by either culture or NAAT.
Similarly, gonococcal urethritis may precede reactive arthritis, but
PELVIC INFLAMMATORY DISEASE Inflammation of sections of the fallo-
co-infection with an agent of NGU is difficult to rule out. The urethral
pian tube is often referred to as salpingitis or PID. The proportion of
CHAPTER 184 Chlamydial Infections
discharge may be purulent or mucopurulent, and patients may or may
acute salpingitis cases caused by C. trachomatis varies geographically and
not report dysuria. Accompanying prostatitis, usually asymptomatic,
with the population studied. It has been estimated that C. trachomatis
has been described. Arthritis usually begins ~4 weeks after the onset
causes up to 50% of PID cases in the United States. PID occurs via
of urethritis but may develop sooner or, in a small percentage of
ascending intraluminal spread of C. trachomatis or N. gonorrhoeae from
cases, may actually precede urethritis. The knees are most frequently
the lower genital tract. Mucopurulent cervicitis is often followed by
involved; next most commonly affected are the ankles and small joints
endometritis, endosalpingitis, and finally pelvic peritonitis. Evidence
of the feet. Sacroiliitis, either symmetrical or asymmetrical, is docu-
of mucopurulent cervicitis is often found in women with laparoscop-
mented in two-thirds of patients. Mild bilateral conjunctivitis, iritis,
ically verified salpingitis. Similarly, endometritis, demonstrated by an
keratitis, or uveitis is sometimes present but lasts for only a few days.
endometrial biopsy showing plasma cell infiltration of the endometrial
Finally, dermatologic manifestations occur in up to 50% of patients. The
epithelium, is documented in most women with laparoscopy-verified
initial lesions—usually papules with a central yellow spot—most often
chlamydial (or gonococcal) salpingitis. Chlamydial endometritis can
involve the soles and palms and, in ~25% of patients, eventually epithe-
also occur in the absence of clinical evidence of salpingitis. Histologic
lialize and thicken to produce keratoderma blenorrhagicum. Circinate
evidence of endometritis has been correlated with a syndrome consist-
balanitis is usually painless and occurs in fewer than half of patients.
ing of vaginal bleeding, lower abdominal pain, and uterine tenderness
The initial episode of reactive arthritis usually lasts 2–6 months.
in the absence of adnexal tenderness. Chlamydial salpingitis produces
milder symptoms than gonococcal salpingitis and may be associated
PROCTITIS Primary anal or rectal infections with C. trachomatis have
with less marked adnexal tenderness. Thus, mild adnexal or uterine
been described in women and MSM who practice anal intercourse. In
tenderness in a sexually active woman with cervicitis suggests chlamy-
these infections, rectal involvement is initially characterized by severe
dial PID.
anorectal pain, a bloody mucopurulent discharge, and tenesmus.
Chronic untreated endometrial and tubal inflammation can result in
Oculogenital serovars D–K and LGV serovars L1, L2, and L3 have been
tubal scarring, impaired tubal function, tubal occlusion, and infertility
found to cause proctitis. The LGV serovars are far more invasive and
even among women who report no prior treatment for chlamydial
cause much more severely symptomatic disease, including severe
infection. C. trachomatis has been particularly implicated in “subclin-
ulcerative proctocolitis that can be clinically confused with HSV procti-
ical” PID on the basis of a lack of history of PID among Chlamydia-
tis. Histologically, LGV proctitis may resemble Crohn’s disease in that
seropositive women with tubal damage and detection of chlamydial
giant cell formation and granulomas are detected. In the United States
DNA or antigen among asymptomatic women with tubal infertil-
and Europe, cases of LGV proctitis occur almost exclusively in MSM,
ity. These data suggest that the best method to prevent PID and its
many of whom have HIV infection.
sequelae is surveillance and control of lower genital tract infections
The less invasive non-LGV serovars of C. trachomatis cause mild
along with diagnosis and treatment of sex partners and prevention of
proctitis. Many infected individuals are asymptomatic, and in these
reinfections. Promotion of early symptom recognition and health care
cases infection is diagnosed only by routine culture or NAAT of
presentation may reduce the frequency and severity of sequelae of PID.
rectal swabs. The number of fecal leukocytes is usually abnormal
in both asymptomatic and symptomatic cases. Sigmoidoscopy may PERIHEPATITIS The Fitz-Hugh–Curtis syndrome was originally
yield normal findings or may reveal mild inflammatory changes or described as a complication of gonococcal PID. However, studies over
small erosions or follicles in the lower 10 cm of the rectum. Histologic the past several decades have suggested that chlamydial infection is
examination of rectal biopsies generally shows anal crypts and promi- more commonly associated with perihepatitis than is N. gonorrhoeae.
nent follicles as well as neutrophilic infiltration of the lamina propria. Perihepatitis should be suspected in young, sexually active women
Chlamydial proctitis is best diagnosed by isolation of C. trachomatis who develop right-upper-quadrant pain, fever, or nausea. Evidence
from the rectum and documentation of a response to appropriate ther- of salpingitis may or may not be found on examination. Frequently,
apy. NAATs are reportedly more sensitive than culture for diagnosis perihepatitis is strongly associated with extensive tubal scarring, adhe-
and are also specific. sions, and inflammation observed at laparoscopy, and high titers of
Harrisons_20e_Part5_p0859-p1648.indd 1319 6/1/18 12:07 PM
1320 antibody to the 57-kDa chlamydial heat-shock protein have been doc- LGV begins as a small painless papule that tends to ulcerate at the
umented. Culture and/or serologic evidence of C. trachomatis is found site of inoculation, often escaping attention. This primary lesion heals
in three-fourths of women with this syndrome. in a few days without scarring and is usually recognized as LGV only
URETHRAL SYNDROME IN WOMEN In the absence of infection with
in retrospect. LGV strains of C. trachomatis have occasionally been
uropathogens such as coliforms or Staphylococcus saprophyticus, recovered from genital ulcers and from the urethra of men and the
C. trachomatis is the pathogen most commonly isolated from college endocervix of women who present with inguinal adenopathy; these
women with dysuria, frequency, and pyuria. Screening studies can areas may be the primary sites of infection in some cases. Proctitis is
recover C. trachomatis at both the cervix and the urethra; in up to 25% more common among people who practice receptive anal intercourse,
of infected women, the organism is isolated only from the urethra. and an elevated white blood cell count in anorectal smears may predict
The urethral syndrome in women consists of dysuria and frequency LGV in these patients. Ulcer formation may facilitate transmission of
in conjunction with chlamydial urethritis, pyuria, and no bacteriuria HIV infection and other sexually transmitted and blood-borne diseases.
or urinary pathogens. Although symptoms of the urethral syndrome As NAATs for C. trachomatis are being used more often, increasing
may develop in some women with chlamydial infection, the majority numbers of cases of LGV proctitis are being recognized in MSM. Such
of women attending STD clinics for urethral chlamydial infection do patients present with anorectal pain and mucopurulent, bloody rectal
not have dysuria or frequency. Even in women with chlamydial ure- discharge. Sigmoidoscopy reveals ulcerative proctitis or proctocolitis,
thritis causing the acute urethral syndrome, signs of urethritis such as with purulent exudate and mucosal bleeding. Histopathologic find-
urethral discharge, meatal redness, and swelling are uncommon. How- ings in the rectal mucosa include granulomas with giant cells, crypt
ever, mucopurulent cervicitis in a woman presenting with dysuria and abscesses, and extensive inflammation. These clinical, sigmoidoscopic,
frequency strongly suggests C. trachomatis urethritis. Other correlates and histopathologic findings may closely resemble those of Crohn’s
of chlamydial urethral syndrome include a duration of dysuria of disease of the rectum.
>7–10 days, lack of hematuria, and lack of suprapubic tenderness. The most common presenting picture in heterosexual men and
Abnormal urethral Gram’s stains showing >10 PMNs/1000× field in women is the inguinal syndrome, which is characterized by painful
women with dysuria but without coliform bacteriuria support the inguinal lymphadenopathy beginning 2–6 weeks after presumed
diagnosis of chlamydial urethritis. Other possible diagnoses include exposure; in rare instances, the onset comes after a few months. The
gonococcal or trichomonal infection of the urethra. inguinal adenopathy is unilateral in two-thirds of cases, and palpable
enlargement of the iliac and femoral nodes is often evident on the same
INFECTION IN PREGNANCY AND THE NEONATAL PERIOD Infections during side as the enlarged inguinal nodes. The nodes are initially discrete,
pregnancy can be transmitted to infants during delivery. Approxi- but progressive periadenitis results in a matted mass of nodes that
mately 20–30% of infants exposed to C. trachomatis in the birth canal becomes fluctuant and suppurative. The overlying skin becomes fixed,
develop conjunctivitis, and 10–15% subsequently develop pneumonia.
PART 5
inflamed, and thin, and multiple draining fistulas finally develop.
Consequently, all newborn infants receive ocular prophylaxis at birth Extensive enlargement of chains of inguinal nodes above and below
to prevent ophthalmia neonatorum. Without treatment, conjunctivitis the inguinal ligament (“the sign of the groove”) is not specific and,
usually develops at 5–19 days of life and often results in a profuse although not uncommon, is documented in only a minority of cases.
mucopurulent discharge. Roughly half of infected infants develop Spontaneous healing usually takes place after several months; inguinal
Infectious Diseases
clinical evidence of inclusion conjunctivitis. However, it is impossible scars or granulomatous masses of various sizes persist for life. Massive
to differentiate chlamydial conjunctivitis from other forms of neonatal pelvic lymphadenopathy may lead to exploratory laparotomy.
conjunctivitis (e.g., that due to N. gonorrhoeae, Haemophilus influenzae, Constitutional symptoms are common during the stage of regional
Streptococcus pneumoniae, or HSV) on clinical grounds; thus labora- lymphadenopathy and, in cases of proctitis, may include fever, chills,
tory diagnosis is required. Inclusions within epithelial cells are often headache, meningismus, anorexia, myalgias, and arthralgias. Other
detected in Giemsa-stained conjunctival smears, but these smears systemic complications are infrequent but include arthritis with sterile
are considerably less sensitive than cultures or NAATs for chlamy- effusion, aseptic meningitis, meningoencephalitis, conjunctivitis, hepa-
diae. Gram-stained smears may show gonococci or occasional small titis, and erythema nodosum (Fig. A1-39). Complications of untreated
gram-negative coccobacilli in Haemophilus conjunctivitis, but smears anorectal infection include perirectal abscess; anal fistulas; and rec-
should be accompanied by cultures or NAATs for these agents. tovaginal, rectovesical, and ischiorectal fistulas. Secondary bacterial
C. trachomatis has also been isolated frequently and persistently from infection probably contributes to these complications. Rectal stricture is
the nasopharynx, rectum, and vagina of infected infants—occasionally a late complication of anorectal infection and usually develops 2–6 cm
for >1 year in the absence of treatment. In some cases, otitis media from the anal orifice—i.e., at a site within reach on digital rectal exami-
results from perinatally acquired chlamydial infection. Pneumonia nation. A small percentage of cases of LGV in men present as chronic
may develop in infants from 2 weeks to 4 months of age. C. trachomatis progressive infiltrative, ulcerative, or fistular lesions of the penis,
is estimated to cause 20–30% of pneumonia cases in infants <6 months urethra, or scrotum. Associated lymphatic obstruction may produce
of age. Epidemiologic studies have linked chlamydial pulmonary elephantiasis. When urethral stricture occurs, it usually involves the
infection in infants with increased occurrence of subacute lung disease posterior urethra and causes incontinence or difficulty with urination.
(bronchitis, asthma, wheezing) in later childhood.
LYMPHOGRANULOMA VENEREUM C. trachomatis serovars L1, L2,
Diagnosis DETECTION METHODS Historically, chlamydiae were
and L3 cause LGV, an invasive systemic STD. The peak inci- cultivated in the yolk sac of embryonated eggs. The organisms can be
dence of LGV corresponds with the age of greatest sexual grown more easily in tissue culture, but cell culture—once considered
activity: the second and third decades of life. The worldwide incidence the diagnostic gold standard—has been replaced by nonculture assays
of LGV is falling, but the disease is still endemic and a major cause of (Table 184-1). In general, culture for chlamydiae in clinical specimens
morbidity in parts of Asia, Africa, South America, and the Caribbean. is now performed only in specialized laboratories. The first nonculture
LGV is rare in industrialized countries; for more than a decade, the assays, such as direct fluorescent antibody staining of clinical material
reported incidence in the United States has been only 0.1 case per and enzyme immunoassay (EIA), have been replaced by NAATs, which
100,000 population. In the Bahamas, an apparent outbreak of LGV was are currently recommended by the CDC as the diagnostic assays of
described in association with a concurrent increase in heterosexual choice. At present, five NAAT assays cleared by the U.S. Food and Drug
infection with HIV. Reports of outbreaks with the newly identified Administration (FDA) are commercially available, some of which are
variant L2b in Europe, Australia, and the United States indicate that available as high-throughput robotic platforms. Point-of-care diagnos-
LGV is becoming more prevalent among MSM. These cases have usu- tic assays are becoming available; they are of increasing interest since
ally presented as hemorrhagic proctocolitis in HIV-positive men. More patients can potentially be treated before leaving the clinic.
widespread use of NAATs for identification of rectal infections may CHOICE OF SPECIMEN Cervical and urethral swabs have traditionally
have enhanced case recognition. been used for the diagnosis of STDs in female and male patients,
Harrisons_20e_Part5_p0859-p1648.indd 1320 6/1/18 12:07 PM
TABLE 184-1 Diagnostic Tests for Sexually Transmitted and Perinatal Chlamydia trachomatis Infection 1321
INFECTION SUGGESTIVE SIGNS/SYMPTOMS PRESUMPTIVE DIAGNOSIS a
CONFIRMATORY TEST OF CHOICE
Men
NGU, PGU Discharge, dysuria Gram’s stain with >4 neutrophils per Urine or urethral NAAT for C. trachomatis
oil-immersion field; no gonococci
Epididymitis Unilateral intrascrotal swelling, pain, tenderness; Gram’s stain with >4 neutrophils per Urine or urethral NAAT for C. trachomatis
fever; NGU oil-immersion field; no gonococci;
urinalysis with pyuria
Women
Cervicitis Mucopurulent cervical discharge, bleeding and Cervical Gram’s stain with ≥20 Urine, cervical, or vaginal NAAT for C. trachomatis
edema of the zone of cervical ectopy neutrophils per oil-immersion field in
cervical mucus
Salpingitis Lower abdominal pain, cervical motion C. trachomatis always potentially Urine, cervical, or vaginal NAAT for C. trachomatis
tenderness, adnexal tenderness or masses present in salpingitis
Urethritis Dysuria and frequency without hematuria MPC; sterile pyuria; negative routine Urine or urethral NAAT for C. trachomatis
urine culture
Adults of Either Sex
Proctitis Rectal pain, discharge, tenesmus, bleeding; Negative gonococcal culture and Rectal NAAT for C. trachomatis or culture
history of receptive anorectal intercourse Gram’s stain; at least 1 neutrophil per
oil-immersion field in rectal Gram’s
stain
Reactive NGU, arthritis, conjunctivitis, typical skin lesions Gram’s stain with >4 neutrophils per Urine or urethral NAAT for C. trachomatis
arthritis oil-immersion field; lack of gonococci
indicative of NGU
LGV Regional adenopathy, primary lesion, proctitis, None Culture of LGV strain from node or rectum,
systemic symptoms occasionally from urethra or cervix; NAAT for C.
trachomatis from these sites; LGV CF titer, ≥1:64;
MIF titer, ≥1:512
CHAPTER 184 Chlamydial Infections
Neonates
Conjunctivitis Purulent conjunctival discharge 6–18 days after Negative culture and Gram’s stain Conjunctival NAAT for C. trachomatis; FA-stained
delivery for gonococci, Haemophilus spp., scraping of conjunctival material
pneumococci, staphylococci
Infant Afebrile, staccato cough, diffuse rales, bilateral None Chlamydial culture or NAAT of sputum, pharynx, eye,
pneumonia hyperinflation, interstitial infiltrates rectum; MIF antibody to C. trachomatis—fourfold
change in IgG or IgM antibody titer
a
A presumptive diagnosis of chlamydial infection is often made in the syndromes listed when gonococci are not found. A positive test for Neisseria gonorrhoeae does
not exclude the involvement of C. trachomatis, which often is present in patients with gonorrhea.
Abbreviations: CF, complement-fixing; FA, fluorescent antibody; LGV, lymphogranuloma venereum; MIF, microimmunofluorescence; MPC, mucopurulent cervicitis;
NAAT, nucleic acid amplification test; NGU, nongonococcal urethritis; PGU, postgonococcal urethritis.
Source: Reprinted with permission from WE Stamm: Chlamydial infections, in Harrison’s Principles of Internal Medicine, 17th ed, AS Fauci et al (eds). New York,
McGraw-Hill, 2008, p 1075.
respectively. However, given the greatly increased sensitivity and spec- test of cure after treatment for infection with C. trachomatis. However,
ificity of NAATs, less invasive samples (e.g., urine for both sexes and because incidence studies have demonstrated that previous chlamydial
vaginal swabs for women) can be used. For screening of asymptomatic infection increases the probability of becoming reinfected, the CDC
women, the CDC now recommends that self-collected or clinician- does recommend that previously infected individuals be rescreened
collected vaginal swabs, which are slightly more sensitive than urine, 3 months after treatment.
be used. Urine screening tests are often used in outreach screening SEROLOGY Serologic testing may be helpful in the diagnosis of LGV
programs, however. For symptomatic women undergoing a pelvic and neonatal pneumonia caused by C. trachomatis. The serologic test of
examination, cervical swab samples are desirable because they have choice is the microimmunofluorescence (MIF) test, in which high-titer
slightly higher chlamydial counts. For male patients, a urine specimen purified elementary bodies mixed with embryonated chicken yolk sac
is the sample of choice, but self-collected penile-meatal swabs have material are affixed to a glass microscope slide to which dilutions of sera
been explored. are applied. After incubation and washing, fluorescein-conjugated IgG
ALTERNATIVE SPECIMEN TYPES Ocular samples from babies and adults or IgM antibody is applied. The test is read with an epifluorescence
can be assessed by NAATs. However, since commercial NAATs for microscope, with the highest dilution of serum producing visible fluo-
this purpose have not yet been approved by the FDA, laboratories rescence designated as the titer. The MIF test is not widely available
must perform their own verification studies. Samples from rectal and except in research laboratories and is highly labor intensive. Although
pharyngeal sites have been used successfully to detect chlamydiae by the complement fixation (CF) test can also be used, it employs
NAATs, but laboratories must perform validation studies to verify test lipopolysaccharide (LPS) as the antigen and therefore identifies the
performance. pathogen only to the genus level. Single-point titers of >1:64 support
a diagnosis of LGV, in which it is difficult to demonstrate rising anti-
OTHER DIAGNOSTIC ISSUES Because NAATs detect nucleic acids instead body titers—i.e., paired serum samples are difficult to obtain since,
of live organisms, they should be used with caution as test-of-cure by its very nature, the disease results in the patient’s being seen by
assays. Residual nucleic acid from cells rendered noninfective by the physician after the acute stage. Any antibody titer of above 1:16 is
antibiotics may continue to yield a positive result in NAATs for as considered significant evidence of exposure to chlamydiae. However,
long as 3 weeks after therapy when viable organisms have actually serologic testing is never recommended for diagnosis of uncomplicated
been eradicated. Therefore, clinicians should not use NAATs for test genital infections of the cervix, urethra, and lower genital tract or for
of cure until after 3 weeks. The CDC currently does not recommend a C. trachomatis screening of asymptomatic individuals.
Harrisons_20e_Part5_p0859-p1648.indd 1321 6/1/18 12:07 PM
1322
TREATMENT Prevention Since many chlamydial infections are asymptomatic,
effective control and prevention must involve periodic screening of
C. trachomatis Genital Infections individuals at risk. Selective cost-effective screening criteria have been
developed. Among women, young age (generally <25 years) is a critical
A 7-day course of tetracycline (500 mg four times daily), doxycycline
risk factor for chlamydial infections in nearly all studies. Other risk
(100 mg twice daily), erythromycin (500 mg four times daily), or
factors include mucopurulent cervicitis; multiple, new, or symptomatic
a fluoroquinolone (ofloxacin, 300 mg twice daily; or levofloxacin,
male sex partners; and lack of barrier contraceptive use. In some set-
500 mg/d) can be used for treatment of uncomplicated chlamydial
tings, screening based on young age may be as sensitive as criteria that
infections. A single 1-g oral dose of azithromycin is as effective as
incorporate behavioral and clinical measures. Another strategy is uni-
a 7-day course of doxycycline for the treatment of uncomplicated
versal testing of all patients in high-prevalence clinic populations (e.g.,
genital C. trachomatis infections in adults. Azithromycin causes fewer
STD clinics, juvenile detention facilities, and family planning clinics).
adverse gastrointestinal reactions than do older macrolides such as
The effectiveness of selective screening in reducing the prevalence of
erythromycin. The single-dose regimen of azithromycin has great
chlamydial infection among women has been demonstrated in several
appeal for the treatment of patients with uncomplicated chlamydial
studies. In the Pacific Northwest, where extensive screening began in
infection (especially those without symptoms and those with a like-
family planning clinics in 1998 and in STD clinics in 1993, the preva-
lihood of poor compliance) and of the sexual partners of infected
lence declined from 10% in the 1980s to <5% in 2000. Similar trends
patients. These advantages must be weighed against the consider-
have occurred in association with screening programs elsewhere. In
ably greater cost of azithromycin. Whenever possible, the single 1-g
addition, screening can effect a reduction in upper genital tract disease.
dose should be given as directly observed therapy. Although not
In Seattle, women at a large health maintenance organization who
approved by the FDA for use in pregnancy, this regimen appears to
were screened for chlamydial infection on a routine basis had a lower
be safe and effective for this purpose. However, amoxicillin (500 mg
incidence of symptomatic PID than did women who received standard
three times daily for 7 days) can also be given to pregnant women.
care and underwent more selective screening.
The fluoroquinolones are contraindicated in pregnancy. A 2-week
In settings with low to moderate prevalence, the prevalence at
course of treatment is recommended for complicated chlamydial
which selective screening becomes more cost-effective than universal
infections (e.g., PID, epididymitis) and at least a 3-week course of
screening must be defined. Most studies have concluded that univer-
doxycycline (100 mg orally twice daily) or erythromycin base (500 mg
sal screening is preferable in settings with a chlamydial prevalence of
orally four times daily) for LGV. Failure of treatment with a tetra-
>3–7%. Depending on the criteria used, selective screening is likely
cycline in genital infections usually indicates poor compliance or
to be more cost-effective when prevalence falls below 3%. Nearly all
reinfection rather than involvement of a drug-resistant strain. To
regions of the United States have now initiated screening programs,
date, clinically significant drug resistance has not been observed in
PART 5
particularly in family planning and STD clinics. Along with single-
C. trachomatis.
dose therapy, the availability of highly sensitive and specific diagnostic
Treatment or testing for chlamydiae should be considered among
NAATs using urine specimens and self-obtained vaginal swabs makes
N. gonorrhoeae–infected patients because of the frequency of co-
it feasible to mount an effective nationwide Chlamydia control program,
infection. Systemic treatment with erythromycin has been recom-
with screening of high-risk individuals in traditional health-care set-
Infectious Diseases
mended for ophthalmia neonatorum and for C. trachomatis pneumo-
tings and in novel outreach and community-based settings. The U.S.
nia in infants. For the treatment of adult inclusion conjunctivitis, a
Preventive Task Force has named Chlamydia screening as a Grade B
single 1-g dose of azithromycin was as effective as standard 10-day
recommendation, which means that private insurance and Medicare
treatment with doxycycline. Recommended treatment regimens for
will cover the cost of screening under the Affordable Care Act.
both bubonic and anogenital LGV include tetracycline, doxycycline,
or erythromycin for 21 days. ■ TRACHOMA
SEX PARTNERS Epidemiology Trachoma—a sequela of ocular disease in
The continued high prevalence of chlamydial infections in most parts developing countries—continues to be a leading cause of pre-
of the United States is due primarily to the failure to diagnose—and ventable infectious blindness worldwide. The WHO estimates
therefore treat—patients with symptomatic or asymptomatic infec- that ~6 million people have been blinded by trachoma and that
tion and their sex partners. Urethral or cervical infection with ~1.3 million people in developing countries still suffer from preventable
C. trachomatis has been well documented in a high proportion of the blindness due to trachoma; certainly hundreds of millions live in tra-
sex partners of patients with NGU, epididymitis, reactive arthritis, choma-endemic areas. Foci of trachoma persist in Australia, the South
salpingitis, and endocervicitis. If possible, confirmatory laboratory Pacific, and Latin America. C. trachomatis serovars A, B, Ba, and C are iso-
tests for chlamydiae should be undertaken in these individuals, but lated from patients with clinical trachoma in areas of endemicity in devel-
even persons without positive tests or evidence of clinical disease oping countries in Africa, the Middle East, Asia, and South America.
who have recently been exposed to proven or possible chlamydial The trachoma-hyperendemic areas of the world are in northern
infection (e.g., NGU) should be offered therapy. A novel approach is and sub-Saharan Africa, the Middle East, drier regions of the Indian
partner-delivered therapy, in which infected patients receive treat- subcontinent, and Southeast Asia. In hyperendemic areas, the preva-
ment and are also provided with single-dose azithromycin to give lence of trachoma is essentially 100% by the second or third year of
to their sex partner(s). life. Active disease is most common among young children, who are
the reservoir for trachoma. By adulthood, active infection is infrequent
NEONATES AND INFANTS but sequelae result in blindness. In such areas, trachoma constitutes the
In neonates with conjunctivitis or infants with pneumonia, ery- major cause of blindness.
thromycin ethylsuccinate or estolate can be given orally at a dosage Trachoma is transmitted through contact with discharges from the
of 50 mg/kg per day, preferably in four divided doses, for 2 weeks. eyes of infected patients. Transmission is most common under poor
Careful attention must be given to compliance with therapy—a fre- hygienic conditions and most often takes place between family mem-
quent problem. Relapses of eye infection are common after topical bers or between families with shared facilities. Flies can also transfer
treatment with erythromycin or tetracycline ophthalmic ointment the mucopurulent ocular discharges, carrying the organisms on their
and may also follow oral erythromycin therapy. Thus follow-up legs from one person to another. The International Trachoma Initiative
cultures should be performed after treatment. Both parents should founded by the WHO in 1998 aims to eliminate blinding trachoma
be examined for C. trachomatis infection and, if diagnostic testing globally by 2020.
is not readily available, should be treated with doxycycline or
azithromycin. Clinical Manifestations Both endemic trachoma and adult
inclusion conjunctivitis present initially as conjunctivitis characterized
Harrisons_20e_Part5_p0859-p1648.indd 1322 6/1/18 12:07 PM
Drug susceptibility testing is recommended only if the sputum remains interacts with few drugs. Adjustment of the dosage on the basis of renal 1279
culture positive after 3 months of appropriate therapy. function is not necessary.
Rapidly Growing Mycobacteria Rapidly growing mycobac- Cefoxitin Cefoxitin is a second-generation parenteral cephalospo-
teria causing human disease include Mycobacterium abscessus, Myco- rin with activity against rapidly growing NTM, particularly M. absces-
bacterium fortuitum, and Mycobacterium chelonae. Treatment of these sus and M. chelonae. Its mechanism of action against NTM is unknown
mycobacteria is complex and should be undertaken with input from but may involve inactivation of cell-wall synthesis enzymes. High
experienced clinicians. It is important to note that testing rapidly doses are used for treatment of NTM: 200 mg/kg IV three or four times
growing mycobacteria for macrolide resistance is tricky, as an inducible per day, with a maximal daily dose of 12 g. The half-life of cefoxitin is
erm gene may confer in vivo macrolide resistance to isolates that are ~1 h, with primarily renal clearance that requires adjustment in renal
susceptible in vitro. insufficiency. Adverse effects are uncommon but include gastrointesti-
M. abscessus is the third most common NTM pathogen in the nal manifestations, rash, eosinophilia, fever, and neutropenia.
United States. It is endemic in the southeastern states between Texas Newer Drugs Three newer class of drugs—the oxazolidinones,
and Florida. Skin, soft tissue, and bone infections occur, usually after the glycylcyclines, and the ketolides—are currently being evaluated
accidental trauma or surgery. This organism appears to have a pre- for possible use in the treatment of NTM infections, especially those
dilection to cause lung infections in white nonsmoking women aged caused by M. abscessus. Approximately 50% of M. abscessus isolates
>60 who have no preexisting lung disease. M. abscessus isolates are have shown some degree of susceptibility in vitro to linezolid, an
usually resistant to standard anti-TB regimens. Skin and soft tissue oxazolidinone. Tigecycline, which is a glycylcycline and a tetracycline
infections are usually treated for a minimum of 4 months with a mac- derivative, and telithromycin, a ketolide, also appear to have in vitro
rolide (clarithromycin or azithromycin) and a parenteral agent such activity against M. abscessus. These drugs, however, have not yet been
as amikacin, cefoxitin, or imipenem. Bone infections are treated for clinically tested in patients.
at least 6 months. This regimen can be used for the treatment of lung In addition, some anti-TB drugs, including clofazimine and bedaqui-
infections but is often unsuccessful because of drug adverse effects line, are being evaluated as alternative agents for the treatment of
and toxicities. A regimen comprising a combination of parenteral refractory NTM infections. In particular, clofazimine appears to act
drugs is recommended on the basis of in vitro drug susceptibility synergistically in combination with amikacin, bedaquiline, or tigecy-
testing. Surgical resection should be considered in all patients with cline. Inhaled amikacin has a positive symptomatic and microbiologic
good lung reserve and a localized infection. impact, but its toxicity is still a problem. The exact role of these agents
in the treatment of refractory NTM infections remains unclear. Sup-
■ DRUGS FOR THE TREATMENT OF NTM
CHAPTER 177 Syphilis
pressive therapy with periodic parenteral/oral drugs to limit disease
Clarithromycin Clarithromycin is a macrolide antibiotic with progression and control symptoms may be an appropriate alternative
broad activity against many gram-positive and gram-negative bacteria to curative treatment.
as well as NTM. This drug is active against MAC organisms and many
other NTM species, inhibiting protein synthesis by binding to the 50S CONCLUSION
mycobacterial ribosomal subunit. NTM resistance to macrolides is Treatment of mycobacterial infections requires multiple-drug regimens
probably caused by overexpression of the gene ermB, with consequent that often exert significant side effects with the potential to limit tol-
methylation of the binding site. Clarithromycin is well absorbed orally erability. The prolonged duration of treatment has vastly improved
and distributes well to tissues. It is cleared both hepatically and renally; results over those obtained in past decades, but drugs and regimens
the dosage should be reduced in renal insufficiency. Clarithromycin that will shorten treatment duration and limit adverse drug effects and
is a substrate for and inhibits cytochrome 3A4 and should not be interactions are needed.
administered with cisapride, pimozide, or terfenadine because cardiac
■ FURTHER READING
arrhythmias may occur. Numerous drugs interact with clarithromycin
Griffith DE et al: An official ATS/IDSA statement: Diagnosis, treat-
through the CYP3A4 metabolic pathway. Rifampin lowers clarithromy-
ment, and prevention of nontuberculous mycobacterial diseases. Am
cin levels; conversely, rifampin levels are increased by clarithromycin.
J Respir Crit Care Med 175:367, 2007.
However, the clinical relevance of this interaction does not appear to
Nahid P et al: Official American Thoracic Society/Centers for Disease
be great.
Control and Prevention/Infectious Diseases Society of America clin-
For patients with nodular/bronchiectatic MAC infection, the dosage
ical practice guidelines: Treatment of drug-susceptible tuberculosis.
of clarithromycin is 500 mg, given morning and evening three times a
Clin Infect Dis 63:e147, 2016.
week. For the treatment of fibrocavitary or severe nodular/bronchiec-
Pontali E et al: Bedaquiline and multidrug-resistant tuberculosis: A
tatic MAC infection, a dose of 500–1000 mg is given daily. Disseminated
systematic and critical analysis of the evidence. Eur Respir J 47:394,
MAC infection is treated with 1000 mg daily. Clarithromycin is used in
2016.
combination regimens that typically include ethambutol and a rifamy-
cin in order to avoid the development of macrolide resistance. Adverse
effects include frequent gastrointestinal intolerance, hepatotoxicity,
headache, rash, and rare instances of hypoglycemia. Clarithromycin
is contraindicated during pregnancy because of its teratogenicity in Section 9 Spirochetal Diseases
animal models.
177
Azithromycin Azithromycin is a derivative of erythromycin.
Although technically an azalide and not a macrolide, it works similarly Syphilis
to macrolides, inhibiting protein synthesis through binding to the 50S
ribosomal subunit. Resistance to azithromycin is almost always asso- Sheila A. Lukehart
ciated with complete cross-resistance to clarithromycin. Azithromycin
is well absorbed orally, with good tissue penetration and a prolonged
half-life (~48 h). The usual dosage for treatment of MAC infection is DEFINITION
250 mg daily or 500 mg three times per week. Azithromycin is used in Syphilis, a chronic systemic infection caused by Treponema pallidum sub-
combination with other agents to avoid the development of resistance. species pallidum, is usually sexually transmitted and is characterized
For prophylaxis against disseminated MAC infection in immuno- by episodes of active disease interrupted by periods of latency. After
compromised individuals, a dose of 1200 mg once per week is given. an incubation period averaging 2–6 weeks, a primary lesion appears—
Because azithromycin is not metabolized by cytochrome P450, it often associated with regional lymphadenopathy—and then resolves
Harrisons_20e_Part5_p0859-p1648.indd 1279 6/1/18 12:06 PM
1280 without treatment. The secondary stage, with generalized mucosal and 30000
cutaneous lesions and generalized lymphadenopathy, is followed by a
latent period of subclinical infection lasting years or decades. Central Men
nervous system (CNS) involvement may occur early in infection and Women
may be symptomatic or asymptomatic. In the preantibiotic era, one-
Number of cases
third of untreated patients developed tertiary syphilis, characterized by 20000
destructive mucocutaneous, skeletal, or parenchymal lesions; aortitis;
or late CNS manifestations.
ETIOLOGY 10000
The Spirochaetales include four genera that are pathogenic for humans
and for a variety of other animals: Leptospira species (leptospirosis,
Chap. 179); Borrelia species (relapsing fever and Lyme disease, Chaps. 180
and 181); Brachyspira species (gastrointestinal infections); and Treponema
species (syphilis and the endemic treponematoses; see also Chap. 178). 0
The Treponema subspecies include T. pallidum subsp. pallidum (venereal 1990 1995 2000 2005 2010 2015
syphilis); T. pallidum subsp. pertenue (yaws); T. pallidum subsp. endemicum FIGURE 177-1 Primary and secondary syphilis in the United States, 1990–
(endemic syphilis or bejel); and T. carateum (pinta). Until recently, the 2015, by sex. (Data from the Centers for Disease Control and Prevention.)
subspecies were distinguished primarily by the clinical syndromes
they produce, but molecular signatures can now differentiate the three
T. pallidum subspecies when assessed by polymerase chain reaction The incidence of congenital syphilis roughly parallels that of infectious
(PCR) or gene sequencing. The crossing of subspecies boundaries by syphilis in women. In 2015, 487 cases in infants <1 year of age were
some gene sequence “signatures” in certain strains demonstrates a reported, for an increase of 36% in the past 5 years.
genetic “continuum” among strains and subspecies of the pathogenic The populations at highest risk for acquiring syphilis have changed
treponemes. Other Treponema species found in the human mouth, geni- over time, with outbreaks among MSM in the pre-HIV era of the late
tal mucosa, and gastrointestinal tract have been associated with disease 1970s and early 1980s as well as at present. It is speculated that recent
(e.g., periodontitis), but their role as primary etiologic agents is unclear. increases in syphilis and other sexually transmitted infections in MSM
T. pallidum subspecies are thin spiral organisms, with a cell body sur- may be due to unprotected sex between persons who are HIV concor-
rounded by a trilaminar cytoplasmic membrane, a delicate peptidogly- dant and to disinhibition permitted by highly effective antiretroviral
PART 5
can layer, and a lipid-rich outer membrane. Endoflagella wind around therapies. The syphilis epidemic that peaked in 1990, predominantly
the cell body in the periplasmic space and are responsible for motility. among African-American heterosexual men and women, occurred
The T. pallidum subspecies cannot be cultured in vitro. Genome largely in urban areas, where infectious syphilis was correlated with
sequencing revealed severely limited metabolic capabilities, the exchange of sex for crack cocaine. Cases of P&S syphilis among
including a lack of genes required for de novo synthesis of most African Americans increased 3.5-fold between 2003 and 2015, and the
Infectious Diseases
amino acids, nucleotides, and lipids. Genes encoding enzymes of the rate (21.4 per 100,000 population) remains higher than rates for other
Krebs cycle and oxidative phosphorylation are absent. The organisms racial/ethnic groups, even though recent increases have been seen in
contain numerous compensatory genes predicted to encode transport- all racial/ethnic groups.
ers of amino acids, carbohydrates, and lipids. In addition, genome Of individuals named as sexual contacts of persons with infectious
analyses and other studies have revealed the existence of a 12-member syphilis, many have already developed manifestations of syphilis
gene family (tpr) with similarities to variable outer-membrane antigens when they are first seen, and ~30% of asymptomatic contacts examined
of other spirochetes. One member, TprK, has discrete variable regions within 30 days of exposure actually have incubating infection and will
that undergo antigenic variation during infection, providing a mecha- later develop infectious syphilis if not treated. Thus, identification and
nism for immune evasion. treatment of all recently exposed sexual contacts continue to be impor-
The only known natural host for T. pallidum subsp. pallidum (referred tant aspects of syphilis control.
to hereafter as T. pallidum) is the human. T. pallidum can infect many
mammals, but only humans, higher apes, and a few laboratory animals ■ GLOBAL SYPHILIS
regularly develop syphilitic lesions. Rabbits are used to propagate Syphilis remains a significant health problem globally; the
virulent strains of T. pallidum and serve as the animal model that best number of new infections is estimated at 11 million per year.
reflects human disease and immunopathology. The regions that are most affected include sub-Saharan Africa,
South America, China, and Southeast Asia. During the past decade, the
TRANSMISSION AND EPIDEMIOLOGY incidence rate for total syphilis in China reached 30 per 100,000, and
Nearly all cases of syphilis are acquired by sexual contact with infec- rates of infectious syphilis have increased dramatically among MSM in
tious lesions (i.e., the chancre, mucous patch, skin rash, or condylomata many European countries. Worldwide, there are estimated to be
lata; see Fig. A1-20). Less common modes of transmission include 1.4 million cases of syphilis among pregnant women, with 500,000
nonsexual personal contact, infection in utero, blood transfusion, and adverse pregnancy outcomes annually.
organ transplantation.
■ SYPHILIS IN THE UNITED STATES NATURAL COURSE AND PATHOGENESIS OF
With the advent of penicillin therapy in the 1940s, the total number of UNTREATED SYPHILIS
reported cases of syphilis of all stages in the United States declined 95% T. pallidum rapidly penetrates intact mucous membranes or microscopic
from 1943 to a low of 31,575 cases in 2000, with <6000 reported cases abrasions in skin and, within a few hours, enters the lymphatics and
of infectious primary and secondary (P&S) syphilis. (P&S cases are a blood to produce systemic infection and metastatic foci long before the
better indicator of disease activity than total syphilis cases.) Since 2000, appearance of a primary lesion. Blood from a patient with incubating or
the number of P&S cases has quadrupled, with 23,872 cases reported early syphilis is infectious. The generation time of T. pallidum during early
in 2015 (Fig. 177-1). Nationally, ~90% of these cases were in men who active disease in vivo is estimated to be ~30 h, and the incubation period
have sex with men (MSM), ~50% of whom are co-infected with HIV of syphilis is inversely proportional to the number of organisms inocu-
(with exact rates varying by geographic location). From 2014 to 2015, lated. The 50% infectious dose for intradermal inoculation in humans has
P&S cases also rose among all men (19%) and among women (25%), been calculated to be 57 organisms, and the treponeme concentration gen-
and increases were seen in all geographic regions in the United States. erally reaches 107/g of tissue before a clinical lesion appears. The median
Harrisons_20e_Part5_p0859-p1648.indd 1280 6/1/18 12:06 PM
incubation period in humans (~21 days) suggests an average inoculum 1281
of 500–1000 infectious organisms for naturally acquired disease; the
incubation period rarely exceeds 6 weeks.
The primary lesion appears at the site of inoculation, usually persists
for 4–6 weeks, and then heals spontaneously. Histopathologic exami-
nation shows perivascular infiltration, chiefly by CD4+ and CD8+
T lymphocytes, plasma cells, and macrophages, with capillary endo-
thelial proliferation and subsequent obliteration of small blood vessels.
The cellular infiltration produces a TH1-type cytokine profile, consistent
with the activation of macrophages. Phagocytosis of opsonized organ-
isms by activated macrophages ultimately causes their destruction,
resulting in spontaneous resolution of the chancre.
The generalized parenchymal, constitutional, mucosal, and cutane-
ous manifestations of secondary syphilis usually appear ~6–12 weeks
after infection, although primary and secondary manifestations may
occasionally overlap. In contrast, some patients may enter the latent
stage without ever recognizing secondary lesions. The histopathologic
features of secondary maculopapular skin lesions include hyperkerato-
sis of the epidermis, capillary proliferation with endothelial swelling
in the superficial dermis, dermal papillae with transmigration of poly-
morphonuclear leukocytes, and—in the deeper dermis—perivascular
infiltration by CD8+ T lymphocytes, CD4+ T lymphocytes, macro-
phages, and plasma cells. Treponemes are found in many tissues,
including the aqueous humor of the eye and the cerebrospinal fluid
(CSF). T. pallidum disseminates during the first weeks of infection,
invading many tissues, including the CNS; CSF abnormalities are
detected in as many as 40% of patients during the secondary stage.
Clinical hepatitis and immune complex–induced glomerulonephritis
FIGURE 177-2 Primary syphilis with a firm, nontender chancre.
CHAPTER 177 Syphilis
are relatively rare but are recognized manifestations of secondary
syphilis; however, liver function tests reveal the presence of infection
and may yield abnormal results in up to one-quarter of cases of early Consequently, primary syphilis goes unrecognized in women and
syphilis. Generalized nontender lymphadenopathy is noted in 85% MSM more often than in heterosexual men.
of patients with secondary syphilis. The paradoxical appearance of Atypical primary lesions are common. A large inoculum produces
secondary manifestations, even after the development of an immune a dark-field-positive ulcerative lesion in nonimmune volunteers but
response that clears primary lesions, likely results from immune eva- may produce a small dark-field-negative papule, an asymptomatic
sion due to antigenic variation of surface antigens. Secondary lesions but seropositive latent infection, or no response at all in some individ-
generally subside within 2–6 weeks, and the infection enters the latent uals with a history of syphilis. A small inoculum may produce only a
stage, which is detectable only by serologic testing. In the preantibiotic papular lesion, even in nonimmune individuals. Therefore, syphilis
era, up to 25% of untreated patients experienced at least one cutaneous should be considered even in the evaluation of trivial or atypical dark-
relapse of secondary lesions, usually during the first year. Therefore, field-negative genital lesions. The lesions that most commonly must be
identification and examination of sexual contacts are most important differentiated from those of primary syphilis include those caused by
for patients with syphilis of <1 year’s duration. herpes simplex virus infection (Chap. 187), chancroid (Chap. 152), trau-
In the preantibiotic era, about one-third of patients with untreated matic injury, and donovanosis (Chap. 168). Regional (usually inguinal)
latent syphilis developed clinically apparent tertiary disease, the most lymphadenopathy accompanies the primary syphilitic lesion, appear-
common types being the gumma (a usually benign granulomatous ing within 1 week of lesion onset. The nodes are firm, nonsuppurative,
lesion); cardiovascular syphilis (usually involving the vasa vasorum of and painless. Inguinal lymphadenopathy is bilateral and may occur
the ascending aorta and resulting in aneurysm); and late symptomatic with anal as well as with genital chancres. The chancre generally heals
neurosyphilis (tabes dorsalis and paresis). In Western countries today, within 4–6 weeks (range, 2–12 weeks), but lymphadenopathy may
specific treatment for early and latent syphilis and coincidental therapy persist for months.
(i.e., therapy with antibiotics that are given for other conditions but are
active against treponemes) have nearly eliminated tertiary syphilis. ■ SECONDARY SYPHILIS
Asymptomatic CNS involvement, however, is still demonstrable in The protean manifestations of the secondary stage usually include
up to 40% of persons with early syphilis and 25% of patients with late mucocutaneous or cutaneous lesions and generalized nontender
latent syphilis, and modern cases of general paresis and tabes dorsalis lymphadenopathy. The healing primary chancre may still be present in
are being reported from China. The factors that contribute to the devel- ~15% of cases—more frequently in persons with concurrent HIV infec-
opment and progression of tertiary disease are unknown. tion. The skin rash consists of macular, papular, papulosquamous, and
occasionally pustular syphilides; often more than one form is present
CLINICAL MANIFESTATIONS simultaneously. The eruption may be very subtle, and 25% of patients
with a discernible rash may be unaware that they have dermatologic
■ PRIMARY SYPHILIS manifestations. Initial lesions are pale red or pink, nonpruritic, discrete
The typical primary chancre usually begins as a single painless papule macules distributed on the trunk and extremities; these macules prog-
that rapidly becomes eroded and usually becomes indurated, with a ress to papular lesions that are distributed widely and that frequently
characteristic cartilaginous consistency on palpation of the edge and involve the palms and soles (Fig. 177-3; see also Figs. A1-18 and
base of the ulcer. Multiple primary lesions are seen in a minority of A1-19). Rarely, severe necrotic lesions (lues maligna) may appear; they
patients. In heterosexual men the chancre is usually located on the are more commonly reported in HIV-infected individuals. Involvement
penis, where it is readily seen (Fig. 177-2; see also Fig. A1-17), whereas of the hair follicles may result in patchy alopecia of the scalp hair, eye-
in MSM it may also be found in the anal canal or rectum or in the brows, or beard in up to 5% of cases.
mouth. Oral sex has been identified as the source of infection in some In warm, moist, intertriginous areas (commonly the perianal region,
MSM. In women, common primary sites are the cervix and labia. vulva, and scrotum), papules can enlarge to produce broad, moist, pink
Harrisons_20e_Part5_p0859-p1648.indd 1281 6/1/18 12:06 PM
1282 transmitted through blood transfusion
or organ donation from patients with
latent syphilis. It was previously thought
that untreated late latent syphilis had
three possible outcomes: (1) persistent
lifelong infection; (2) development of late
syphilis; or (3) spontaneous cure, with
reversion of serologic tests to negative.
It is now apparent, however, that the
more sensitive treponemal antibody tests
rarely, if ever, become nonreactive with-
out treatment. Although progression to
clinically evident late syphilis is very
rare today, the occurrence of spontaneous
FIGURE 177-3 Secondary syphilis. Left: Maculopapular truncal eruption. Middle: Papules on the palms. Right: microbiologic cure is in doubt.
Papules on the soles. (Courtesy of Jill McKenzie and Christina Marra.)
■ INVOLVEMENT OF THE CNS
or gray-white, highly infectious lesions (condylomata lata; see Fig. A1-20) Traditionally, neurosyphilis has been considered a late manifestation
in 10% of patients with secondary syphilis. Superficial mucosal erosions of syphilis, but this view is inaccurate. CNS syphilis represents a con-
(mucous patches) occur in 10–15% of patients and commonly involve the tinuum encompassing early invasion (usually within the first weeks of
oral or genital mucosa (see Fig. A1-21). The typical mucous patch is a infection), months to years of asymptomatic involvement, and, in some
painless silver-gray erosion surrounded by a red periphery. cases, development of early or late neurologic manifestations.
Constitutional signs and symptoms that may accompany or precede
Asymptomatic Neurosyphilis The diagnosis of asymptomatic
secondary syphilis include sore throat (15–30%), fever (5–8%), weight
neurosyphilis is made in patients who lack neurologic symptoms
loss (2–20%), malaise (25%), anorexia (2–10%), headache (10%), and
and signs but who have CSF abnormalities, including mononuclear
meningismus (5%). Acute meningitis occurs in only 1–2% of cases, but
pleocytosis, increased protein concentrations, or reactivity in the CSF
CSF cell and protein concentrations are increased in up to 40% of early
Venereal Disease Research Laboratory (VDRL) test. CSF abnormalities
syphilis cases, and viable T. pallidum organisms have been recovered
are demonstrated in up to 40% of cases of untreated primary or second-
from CSF during primary and secondary syphilis in 30% of cases;
ary syphilis and in 25% of cases of untreated latent syphilis. T. pallidum
PART 5
the latter finding is often but not always associated with other CSF
has been recovered by inoculation into rabbits of CSF from up to 30%
abnormalities. Ocular findings associated with secondary (or later/
of patients with primary or secondary syphilis but less frequently
unknown-stage) syphilis include pupillary abnormalities and optic
from patients with latent syphilis. The presence of T. pallidum in CSF
neuritis as well as the classic iritis or uveitis. The diagnosis of ocular
is often associated with other CSF abnormalities, but organisms can
syphilis is often considered in affected patients only after they fail to
be recovered from patients with otherwise normal CSF. Although the
Infectious Diseases
respond to topical steroid therapy. Anterior uveitis has been reported
prognostic implications of these findings in early syphilis are uncertain,
in 5–10% of patients with secondary syphilis, and T. pallidum has been
it may be appropriate to conclude that even patients with early syphilis
demonstrated in aqueous humor from such patients. Permanent blind-
who have such findings do indeed have asymptomatic neurosyphilis
ness may result without prompt diagnosis and treatment. The recent
and should be treated for neurosyphilis; such treatment is particu-
publication of a number of reports of ocular syphilis reminds clinicians
larly important in patients with concurrent HIV infection. Before the
to inquire about neurologic manifestations in all stages of syphilis
advent of penicillin, the risk of development of clinical neurosyphilis
infection. In a recent retrospective study, 7.9% of patients with syphilis,
in untreated asymptomatic persons was roughly proportional to the
when asked, reported recent vision or hearing changes, and more than
intensity of CSF changes, with the overall cumulative probability of
half of those reporting these changes had abnormal CSF or ophthalmo-
progression to clinical neurosyphilis ~20% in the first 10 years of infec-
logic findings consistent with syphilis.
tion but increasing with time. Most experts agree that neurosyphilis is
Less common complications of secondary syphilis include hepatitis,
more common among HIV-infected persons, while immunocompetent
nephropathy, gastrointestinal involvement (hypertrophic gastritis,
patients with untreated latent syphilis and normal CSF probably run
patchy proctitis, or a rectosigmoid mass), arthritis, and periostitis.
a very low risk of subsequent neurosyphilis. In several large studies,
Hepatic involvement is common in syphilis; although it is usually
neurosyphilis was associated with a rapid plasma reagin (RPR) titer of
asymptomatic, up to 25% of patients may have abnormal liver function
≥1:32, regardless of clinical stage or HIV infection status.
tests. Frank syphilitic hepatitis may be seen. Renal involvement usually
results from immune complex deposition and produces proteinuria Symptomatic Neurosyphilis The major clinical categories of
associated with an acute nephrotic syndrome. Like those of primary symptomatic neurosyphilis include meningeal, meningovascular, and
syphilis, most manifestations of the secondary stage resolve spontane- parenchymatous syphilis. The last category includes general paresis
ously, usually within 1–6 months. and tabes dorsalis. The onset of symptoms usually occurs <1 year
after infection for meningeal syphilis, up to 10 years after infection for
■ LATENT SYPHILIS meningovascular syphilis, at ~20 years for general paresis, and at 25–30
Positive serologic tests for syphilis, together with a normal CSF exami- years for tabes dorsalis. Neurosyphilis is more frequently symptomatic
nation and the absence of clinical manifestations of syphilis, indicate in patients co-infected with HIV, particularly those with low CD4+ T
a diagnosis of latent syphilis in an untreated person. The diagnosis lymphocyte counts. In addition, evidence suggests that syphilis infec-
is often suspected on the basis of a history of primary or secondary tion worsens the cognitive impairment seen in HIV-infected persons
lesions, a history of exposure to syphilis, or the delivery of an infant and that this effect persists after treatment for syphilis.
with congenital syphilis. A previous nonreactive serologic test or a Meningeal syphilis may present as headache, nausea, vomiting, neck
history of lesions or exposure may help establish the duration of latent stiffness, cranial nerve involvement, seizures, and changes in mental
infection, which is an important factor in the selection of appropriate status. This condition may be concurrent with or may follow the sec-
therapy. Early latent syphilis is limited to the first year after infection, ondary stage. Patients presenting with uveitis, iritis, or hearing loss
whereas late latent syphilis is defined as that of ≥1 year’s duration often have meningeal syphilis, but these clinical findings can also be
(or of unknown duration). T. pallidum may still seed the bloodstream seen in patients with normal CSF.
intermittently during the latent stage, and latent syphilis in a pregnant Meningovascular syphilis reflects meningitis together with inflamma-
woman may infect the fetus in utero. Moreover, syphilis has been tory vasculitis of small, medium, or large vessels. The most common
Harrisons_20e_Part5_p0859-p1648.indd 1282 6/1/18 12:06 PM
presentation is a stroke syndrome involving the middle cerebral artery Routine serologic testing for syphilis in early pregnancy is 1283
of a relatively young adult. However, unlike the usual thrombotic or cost-effective in virtually all populations, even in areas with a
embolic stroke syndrome of sudden onset, meningovascular syphilis low prenatal prevalence of syphilis. Low-tech point-of-care
often becomes manifest after a subacute encephalitic prodrome (with tests have been developed and widely implemented to facilitate ante-
headaches, vertigo, insomnia, and psychological abnormalities), which natal testing in resource-poor settings. Globally, the past 5–8 years have
is followed by a gradually progressive vascular syndrome. seen a 38% reduction in maternal syphilis and a 39% reduction in con-
The manifestations of general paresis reflect widespread late par- genital syphilis. Progress has been uneven, however, with major
enchymal damage and include abnormalities corresponding to the advances in Thailand, Cuba, several Baltic States, and India, but contin-
mnemonic paresis: personality, affect, reflexes (hyperactive), eye (e.g., uing high levels in Africa and China. Periodic lack of penicillin avail-
Argyll Robertson pupils), sensorium (illusions, delusions, hallucina- ability prevents treatment of seropositive women. Integration of
tions), intellect (a decrease in recent memory and in the capacity for ori- programs to prevent congenital syphilis with programs to prevent
entation, calculations, judgment, and insight), and speech. Tabes dorsalis maternal transmission of HIV would be highly cost-effective but is
is a late manifestation of syphilis that presents as symptoms and signs hampered by the restrictions placed on HIV-focused funds. Pregnant
of demyelination of the posterior columns, dorsal roots, and dorsal root women should be screened at their first antenatal visit. Where the prev-
ganglia, including ataxia, foot drop, paresthesia, bladder disturbances, alence of syphilis is high or when the patient is at high risk of reinfec-
impotence, areflexia, and loss of positional, deep-pain, and tempera- tion, serologic testing should be repeated in the third trimester and at
ture sensations. The small, irregular Argyll Robertson pupil, a feature delivery. Neonatal congenital syphilis must be differentiated from
of both tabes dorsalis and paresis, reacts to accommodation but not other generalized congenital infections, including rubella, cytomegalo-
to light. Optic atrophy also occurs frequently in association with tabes. virus or herpes simplex virus infection, and toxoplasmosis, as well as
from erythroblastosis fetalis.
■ OTHER MANIFESTATIONS OF LATE SYPHILIS Manifestations of congenital syphilis may appear early (within the
The slowly progressive inflammatory process leading to tertiary dis- first 2 years of life, often at 2–10 weeks of age) or late (after 2 years).
ease begins early during infection, although these manifestations may The earliest manifestations of congenital syphilis include rhinitis, or
not become clinically apparent for years or decades. Early syphilitic “snuffles” (23%); mucocutaneous lesions (35–41%); bone changes
aortitis first becomes evident soon after secondary lesions subside, and (61%), including periostitis detectable by x-ray examination of long
treponemes that trigger the development of gummas may have seeded bones; hepatosplenomegaly (50%); lymphadenopathy (32%); anemia
the tissue years earlier. (34%); jaundice (30%); thrombocytopenia; and leukocytosis. CNS inva-
sion by T. pallidum is detectable in 22% of infected neonates. Neonatal
Cardiovascular Syphilis Cardiovascular manifestations, usually
CHAPTER 177 Syphilis
death is usually due to pulmonary hemorrhage, secondary bacterial
appearing 10–40 years after infection, are attributable to endarteritis
infection, or severe hepatitis. Late congenital syphilis (untreated after
obliterans of the vasa vasorum, which provide the blood supply to large
2 years of age) is subclinical in 60% of cases; the clinical spectrum
vessels; T. pallidum DNA has been detected by PCR in aortic tissue. Car-
in the remainder of cases may include interstitial keratitis (which
diovascular involvement results in uncomplicated aortitis, aortic regur-
occurs at 5–25 years of age), eighth-nerve deafness, and recurrent
gitation, saccular aneurysm (usually of the ascending aorta), or coronary
arthropathy. Neurosyphilis was documented in about one-quarter of
ostial stenosis. In the preantibiotic era, symptomatic cardiovascular
untreated patients with late congenital syphilis in the preantibiotic
complications developed in ~10% of persons with untreated late syphi-
era. Gummatous periostitis occurs at 5–20 years of age and, as in non-
lis. Today, cardiovascular syphilis is rarely seen in the developed world.
venereal endemic syphilis, tends to cause destructive lesions of the
Late Benign Syphilis (Gumma) Gummas are usually solitary palate and nasal septum. Classic stigmata include Hutchinson’s teeth
lesions ranging from microscopic to several centimeters in diameter. (centrally notched, widely spaced, peg-shaped upper central incisors),
Histologic examination shows a granulomatous inflammation, with a “mulberry” molars (sixth-year molars with multiple, poorly developed
central area of necrosis due to endarteritis obliterans. T. pallidum has cusps), saddle nose, and saber shins.
been detected by PCR in these lesions, and penicillin treatment results
in rapid resolution, confirming the treponemal stimulus for the inflam- LABORATORY EXAMINATIONS
mation. Common sites include the skin and skeletal system; however,
any organ (including the brain) may be involved. Gummas of the skin ■ DEMONSTRATION OF THE ORGANISM
produce indolent, painless, indurated nodular or ulcerative lesions T. pallidum cannot be detected by culture. Historically, dark-field
that may resemble other chronic granulomatous conditions. Skeletal microscopy and immunofluorescence antibody staining have been
gummas may affect any bone or cartilage. Upper respiratory gummas used to identify this spirochete in samples from moist lesions such as
can lead to perforation of the nasal septum or palate. chancres or condylomata lata, but these tests are rarely available out-
side of research laboratories. Sensitive and specific PCR tests have been
■ CONGENITAL SYPHILIS developed but are not commercially available, although a number of
Transmission of T. pallidum across the placenta from a syphilitic woman laboratories perform in-house validated PCR testing.
to her fetus may occur at any stage of pregnancy, but fetal damage T. pallidum can be found in tissue with appropriate silver stains,
generally does not occur until after the fourth month of gestation when but these results should be interpreted with caution because arti-
fetal immunologic competence begins to develop. This timing suggests facts resembling T. pallidum are often seen. Tissue treponemes can be
that the pathogenesis of congenital syphilis, like that of adult syphilis, demonstrated more reliably in research laboratories by PCR or by
depends on the host immune response rather than on a direct toxic immunofluorescence or immunohistochemical methods using specific
effect of T. pallidum. The risk of fetal infection during untreated early monoclonal or polyclonal antibodies to T. pallidum. T. pallidum DNA
maternal syphilis is ~75–95%, decreasing to ~35% for maternal syphilis has been detected by PCR in lesion swabs, tissue samples, blood, CSF,
of >2 years’ duration. Adequate treatment of the woman before the ocular fluid, urine, and oropharyngeal swabs.
16th week of pregnancy should prevent fetal damage, and treatment
before the third trimester should adequately treat the infected fetus.
■ SEROLOGIC TESTS FOR SYPHILIS
Untreated maternal infection may result in a rate of fetal loss of up to
40% with stillbirth (more common than abortion because of the late Treponemal and Lipoidal Tests There are two types of sero-
onset of fetal pathology), prematurity, neonatal death, or nonfatal con- logic tests for syphilis: lipoidal (so-called nontreponemal) and tre-
genital syphilis. Among infants born alive, only fulminant congenital ponemal. Both are reactive in persons with any treponemal infection,
syphilis is clinically apparent at birth, and these babies have a very including syphilis, yaws, pinta, and endemic syphilis.
poor prognosis. The most common clinical problem is the healthy- The most widely used lipoidal antibody tests for syphilis are the
appearing baby born to a mother with a positive serologic test. RPR and VDRL tests, which measure IgG and IgM directed against a
Harrisons_20e_Part5_p0859-p1648.indd 1283 6/1/18 12:06 PM
1284 cardiolipin-lecithin-cholesterol antigen complex. The RPR test is easier positive reactions’ being outnumbered by false-positive reactions,
to perform and uses unheated serum or plasma; it is the test of choice leading to unnecessary treatment. Thus screening with lipoidal tests is
for rapid serologic diagnosis in a clinical setting. The VDRL test remains highly recommended.
the standard for examining CSF and is superior to the RPR for this
purpose. The RPR and VDRL tests are recommended for screening and ■ EVALUATION FOR NEUROSYPHILIS
for quantitation of serum antibody. The titer reflects disease activity, Involvement of the CNS is detected by examination of CSF for mono-
rising during the evolution of early syphilis, often exceeding 1:32 in sec- nuclear pleocytosis (>5 white blood cells/μL), increased protein con-
ondary syphilis, and declining slowly thereafter without therapy. After centration (>45 mg/dL), or CSF VDRL reactivity. Elevated CSF cell
treatment for early syphilis, a persistent fall by fourfold or more (e.g., counts and protein concentrations are not specific for neurosyphilis
a decline from 1:32 to 1:8) is considered an adequate response. VDRL and may be confounded by HIV co-infection. Because CSF pleocy-
titers do not correspond directly to RPR titers, and sequential quantita- tosis may also be due to HIV, some studies have suggested using a
tive testing (as for response to therapy) must employ a single test. CSF white-cell cutoff of 20 cells/μL as diagnostic of neurosyphilis
Treponemal tests measure antibodies to native or recombinant in HIV-infected patients with syphilis. The CSF VDRL test is highly
T. pallidum antigens and include the fluorescent treponemal antibody– specific and, when reactive, is considered diagnostic of neurosyphilis;
absorbed (FTA-ABS) test and the T. pallidum particle agglutination however, this test is insensitive and may be nonreactive even in cases
(TPPA) test, both of which are more sensitive for primary syphilis than of symptomatic neurosyphilis. The RPR test should not be substituted
the lipoidal tests. When used to confirm reactive lipoidal test results, for the VDRL test for CSF examination. The FTA-ABS test on CSF is
treponemal tests have a very high positive predictive value for diag- reactive far more often than the CSF VDRL test in all stages of syphilis,
nosis of syphilis. but reactivity may reflect passive transfer of serum antibody into the
Treponemal enzyme or chemiluminescence immunoassays (EIAs/ CSF. A nonreactive FTA-ABS test on CSF, however, may be used to rule
CIAs), based largely on reactivity to recombinant antigens, are now out asymptomatic neurosyphilis. Measuring CXCL13 in CSF has been
widely used as screening tests by large laboratories. When used for demonstrated to distinguish between neurosyphilis and HIV-related
screening, however, standard treponemal tests give false-positive CSF abnormalities.
results at rates as high as 1–2%, but the rate is much higher with the All T. pallidum–infected patients who have signs or symptoms
EIA/CIA tests. A high proportion of sera that are reactive by EIA/CIA consistent with neurologic disease (e.g., meningitis, hearing loss) or
are nonreactive by lipoidal tests. Such sera should be examined in the ophthalmic disease (e.g., uveitis, iritis) should have a CSF examination,
TPPA test, which includes different antigens and a different platform. regardless of disease stage. The appropriate management of asymp-
If the TPPA test is nonreactive, the patient is unlikely to have syphilis; tomatic persons is less clear. Lumbar puncture on all asymptomatic
if it is reactive, the patient is likely to have current or past syphilis. The patients with untreated syphilis is impractical and unnecessary.
PART 5
rapid immunochromatographic tests described for antenatal screening Because therapy with penicillin G benzathine fails to result in trepone-
in resource-poor settings are largely unavailable in the United States. micidal drug levels in CSF, however, it is important to identify those
Both lipoidal and treponemal tests may be nonreactive in early persons at higher risk for having or developing neurosyphilis so that
primary syphilis, although treponemal tests are slightly more sensitive appropriate therapy may be given. Viable T. pallidum has been isolated
(85–90%) during this stage than lipoidal tests (~80%). All tests are reac- from the CSF of several patients (with and without HIV infection) after
Infectious Diseases
tive during secondary syphilis. (Fewer than 1% of patients with high penicillin G benzathine therapy for early syphilis. Large-scale prospec-
titers have a lipoidal test that is nonreactive or weakly reactive with tive studies have provided evidence-based guidelines for determining
undiluted serum but is reactive with diluted serum—the prozone phe- which syphilis patients may benefit most from CSF examination. Spe-
nomenon.) VDRL and RPR sensitivity and titers may decline in untreated cifically, patients with RPR titers of ≥1:32 are at higher risk of having
persons with late latent syphilis, but treponemal tests remain reactive neurosyphilis (11-fold and 6-fold higher in HIV-infected and HIV-
in late syphilis. After treatment for early syphilis, lipoidal test titers uninfected persons, respectively), as are HIV-infected patients with
will generally decline or the tests will become nonreactive, whereas CD4+ T cell counts of ≤350/μL. Persons with active tertiary syphilis
treponemal tests often remain reactive after therapy and are not helpful and those in whom treatment failure is suspected also should have
in determining the infection status of persons with past syphilis. their CSF examined.
Clinicians need to be familiar with three uses of serologic tests for
syphilis recommended by the Centers for Disease Control and Preven- ■ EVALUATION OF HIV-INFECTED PATIENTS FOR
tion (CDC): (1) screening or diagnosis (RPR or VDRL), (2) quantitative SYPHILIS
measurement of antibody to assess clinical syphilis activity or to Because persons at highest risk for syphilis are also at increased risk for
monitor response to therapy (RPR or VDRL), and (3) confirmation of a HIV infection, these two infections frequently coexist. There is evidence
syphilis diagnosis in a patient with a reactive lipoidal test (FTA-ABS, that syphilis and other genital ulcer diseases are important risk factors
TPPA, EIA/CIA). Whereas IgM titers appear to decline after therapy, for acquisition and transmission of HIV infection. Some manifestations
the presence or absence of specific IgM does not strictly correlate with of syphilis may be altered in patients with concurrent HIV infection,
active T. pallidum infection. Moreover, no commercially available IgM and multiple cases of neurologic relapse after standard therapy have
test is recommended, even for evaluation of infants with suspected been reported in these patients.
congenital syphilis. Persons with newly diagnosed HIV infection should be tested for
syphilis; conversely, all patients with newly diagnosed syphilis should
False-Positive Serologic Tests for Syphilis The lipid anti- be tested for HIV infection. Some authorities, persuaded by reports of
gens of nontreponemal tests are similar to those found in human tis- persistent T. pallidum in CSF of HIV-infected persons after standard
sues, and the tests may be reactive (usually with titers ≤1:8) in persons therapy for early syphilis, recommend CSF examination for evidence
without treponemal infection. Among patients being screened for of neurosyphilis for all co-infected patients, regardless of the stage
syphilis because of risk factors, clinical suspicion, or history of expo- of syphilis, with treatment for neurosyphilis if CSF abnormalities are
sure, ~1% of reactive tests are falsely positive. Modern VDRL and RPR found. Others, on the basis of their own clinical experience, think that
tests are highly specific, and false-positive reactions are largely limited standard therapy—without CSF examination—is sufficient for all cases
to persons with autoimmune conditions or injection drug use. The of early syphilis in HIV-infected patients without neurologic signs or
prevalence of false-positive results increases with advancing age. In a symptoms. As described above, RPR titer and CD4+ T cell count can
patient with a false-positive nontreponemal test, syphilis is excluded be used to identify patients at higher risk of neurosyphilis for lumbar
by a nonreactive treponemal test. puncture, although some cases of neurosyphilis will be missed even
False-positive reactions may also occur with treponemal tests, par- when these criteria are used. Serologic testing after treatment is impor-
ticularly the very sensitive EIA/CIA tests. Screening a low-prevalence tant for all patients with syphilis, particularly for those also infected
population for syphilis with a treponemal test may result in true- with HIV.
Harrisons_20e_Part5_p0859-p1648.indd 1284 6/1/18 12:06 PM
The regimens recommended for prevention are the same as those recom- 1285
TREATMENT
mended for early syphilis. Penicillin G benzathine cures >95% of cases
Syphilis of early syphilis, although clinical relapse can follow treatment,
particularly in patients with concurrent HIV infection. Because the
TREATMENT OF ACQUIRED SYPHILIS risk of neurologic relapse may be higher in HIV-infected patients,
The CDC’s 2015 guidelines for the treatment of syphilis are CSF examination is recommended for HIV-seropositive individuals
summarized in Table 177-1 and are discussed below. Peni- with syphilis of any stage, particularly those with a serum RPR titer
cillin G is the drug of choice for all stages of syphilis. of ≥1:32 or a CD4+ T cell count of ≤350/μL. Therapy appropriate
T. pallidum is killed by very low concentrations of penicillin G, for neurosyphilis should be given if there is any evidence of CNS
although a long period of exposure to penicillin is required because infection.
of the unusually slow rate of multiplication of the organism. The Late Latent Syphilis or Syphilis of Unknown Duration If the CSF is
efficacy of penicillin against syphilis remains undiminished after normal or is not examined, the recommended treatment is penicillin
70 years of use, and there is no evidence of penicillin resistance in G benzathine (7.2 million units total; Table 177-1). If CSF abnormali-
T. pallidum. Other antibiotics effective in syphilis include the tetracy- ties are found, the patient should be treated for neurosyphilis.
clines and the cephalosporins. Aminoglycosides and spectinomycin
inhibit T. pallidum only in very large doses, and the sulfonamides and Tertiary Syphilis CSF examination should be performed. If the
most quinolones are inactive. Azithromycin has shown significant CSF is normal, the recommended treatment is penicillin G benza-
promise as an effective oral agent against T. pallidum; however, strains thine (7.2 million units total; Table 177-1). If CSF is abnormal, the
harboring 23S rDNA mutations that confer macrolide resistance are patient should be treated for neurosyphilis. The clinical response
widespread. Such strains represent >80–90% of recent isolates from to treatment for benign tertiary syphilis is usually impressive,
large U.S., European, and Chinese cities, while rates of 23S mutation but responses in cardiovascular syphilis are not dramatic because
are much lower in some other locations. The prevalence of resistant aortic aneurysm and aortic regurgitation cannot be reversed by
strains varies by geographic location, and routine treatment of syph- antibiotics.
ilis with azithromycin is not recommended. Careful follow-up of any Syphilis in Penicillin-Allergic Patients For penicillin-allergic patients
patient treated for syphilis with azithromycin must be assured. with syphilis, a 2-week (early syphilis) or 4-week (late or late latent
Early Syphilis Patients and Their Contacts Penicillin G benzathine syphilis) course of therapy with doxycycline or tetracycline is rec-
is the most widely used agent for the treatment of early syphilis; ommended (Table 177-1). These regimens appear to be effective in
preventive treatment is also recommended for individuals who have early syphilis but have not been tested for late or late latent syphilis,
CHAPTER 177 Syphilis
been exposed to infectious syphilis within the previous 3 months. and compliance may be problematic. Limited studies suggest that
ceftriaxone (1 g/d, given IM or IV for 8–10 days) is effective for
TABLE 177-1 Recommendations for the Treatment of Syphilisa early syphilis. These nonpenicillin regimens have not been carefully
evaluated in HIV-infected individuals and should be used with
PATIENTS WITH
caution. If compliance and follow-up are not assured, penicillin-
PATIENTS WITHOUT CONFIRMED
STAGE OF SYPHILIS PENICILLIN ALLERGY PENICILLIN ALLERGY allergic HIV-infected persons with late latent or late syphilis should
Primary, secondary, or CSF normal or not CSF normal or not
be desensitized and treated with penicillin.
early latent examined: Penicillin G examined: Tetracycline Neurosyphilis Penicillin G benzathine, even at high doses, does not
benzathine (single dose of HCl (500 mg PO qid) or produce treponemicidal concentrations of penicillin G in CSF and
2.4 mU IM) doxycycline (100 mg PO
bid) for 2 weeks should not be used for treatment of neurosyphilis. Asymptomatic
CSF abnormal: Treat as
neurosyphilis may relapse as symptomatic disease after treatment
neurosyphilis. CSF abnormal: Treat as
neurosyphilis. with benzathine penicillin, and the risk of relapse may be higher in
Late latent (or latent CSF normal or not CSF normal and patient
HIV-infected patients. Both symptomatic and asymptomatic neu-
of unknown duration), examined: Penicillin G not infected with HIV: rosyphilis should be treated with aqueous penicillin (Table 177-1).
cardiovascular, or benzathine (2.4 mU IM Tetracycline HCl (500 mg Administration either of IV aqueous crystalline penicillin G or of
benign tertiary weekly for 3 weeks) PO qid) or doxycycline IM aqueous procaine penicillin G plus oral probenecid in recom-
CSF abnormal: Treat as (100 mg PO bid) for mended doses is thought to ensure treponemicidal concentrations
neurosyphilis. 4 weeks of penicillin G in CSF. The clinical response to penicillin therapy for
CSF normal and meningeal syphilis is dramatic, but treatment of neurosyphilis with
patient infected with existing parenchymal damage may only arrest disease progression.
HIV: Desensitize and
treat with penicillin if No data suggest that additional therapy (e.g., penicillin G benza-
compliance cannot be thine for 3 weeks) is beneficial after treatment for neurosyphilis.
assured. The use of antibiotics other than penicillin G for the treatment
CSF abnormal: Treat as of neurosyphilis has not been studied, although limited data sug-
neurosyphilis. gest that ceftriaxone may be used. In patients with confirmed
Neurosyphilis Aqueous crystalline Desensitize and treat penicillin allergy, desensitization and treatment with penicillin are
(asymptomatic or penicillin G (18–24 mU/d with penicillin. recommended.
symptomatic) IV, given as 3–4 mU q4h
or continuous infusion) for Management of Syphilis in Pregnancy Every pregnant woman
10–14 days should undergo a lipoidal screening test at her first prenatal visit
or and, if at high risk of exposure, again in the third trimester and at
Aqueous procaine penicillin delivery. In the untreated pregnant patient with presumed syph-
G (2.4 mU/d IM) plus oral ilis, expeditious treatment appropriate to the stage of the disease
probenecid (500 mg qid), is essential. Patients should be warned of the risk of a Jarisch-
both for 10–14 days Herxheimer reaction, which may be associated with mild premature
Syphilis in pregnancy According to stage Desensitize and treat contractions but rarely results in premature delivery.
with penicillin. Penicillin is the only recommended agent for the treatment of
See text for indications for CSF examination.
a syphilis in pregnancy. If the patient has a documented penicillin
Abbreviations: CSF, cerebrospinal fluid; mU, million units. allergy, desensitization and penicillin therapy should be undertaken
Source: Adapted from the 2015 Sexually Transmitted Diseases Treatment according to the CDC’s 2015 guidelines. After treatment, a quanti-
Guidelines from the Centers for Disease Control and Prevention. tative nontreponemal test should be repeated monthly throughout
Harrisons_20e_Part5_p0859-p1648.indd 1285 6/1/18 12:06 PM
1286 pregnancy to assess therapeutic efficacy. Treated women whose signs and symptoms of syphilis appear. Because treponemal tests
antibody titers rise by fourfold or whose titers do not decrease by may remain reactive despite treatment for seropositive syphilis,
fourfold over a 3-month period should be re-treated. these tests are not useful in following the response to therapy.
The activity of neurosyphilis (symptomatic or asymptomatic)
EVALUATION AND MANAGEMENT OF CONGENITAL SYPHILIS
correlates best with CSF pleocytosis, and this measure provides the
Whether or not they are infected, newborn infants of women with most sensitive index of response to treatment. Repeat CSF exami-
reactive serologic tests may themselves have reactive tests because nations should be performed every 6 months until the cell count is
of transplacental transfer of maternal IgG antibodies. For asymp- normal. An elevated CSF cell count falls to normal in 3–12 months in
tomatic infants born to women treated adequately with penicillin adequately treated HIV-uninfected patients. The persistence of mild
during the first or second trimester of pregnancy, monthly quanti- pleocytosis in HIV-infected patients may be due to the presence of
tative nontreponemal tests may be performed to monitor for appro- HIV in CSF; this scenario may be difficult to distinguish from treat-
priate reduction in antibody titers. Rising or persistent titers indicate ment failure. Elevated levels of CSF protein fall more slowly, and the
infection, and the infant should be treated. Detection of neonatal CSF VDRL titer declines gradually over several years. In patients
IgM antibody may be useful, but no commercially available test is treated for neurosyphilis, a fourfold reduction in serum RPR titer
currently recommended. has been positively correlated with normalization of CSF abnormal-
An infant should be treated at birth if the treatment status of the ities; this correlation is stronger in HIV-uninfected patients and in
seropositive mother is unknown; if the mother received inadequate HIV-infected patients receiving effective antiretroviral therapy.
or nonpenicillin therapy; if the mother received penicillin therapy in
the third trimester; or if the infant may be difficult to follow. The CSF
should be examined to obtain baseline values before treatment. Pen- IMMUNITY TO SYPHILIS
icillin is the only recommended drug for the treatment of syphilis in The rate of development of acquired resistance to T. pallidum after nat-
infants. Specific recommendations for the treatment of infants and ural or experimental infection depends on both the size of the infecting
older children are included in the CDC’s 2015 treatment guidelines. inoculum and the duration of infection before treatment. Both humoral
and cellular responses are considered to be of major importance in
JARISCH-HERXHEIMER REACTION the healing of early lesions. Cellular infiltration, predominantly by
A dramatic although self-limited reaction consisting of fever, T lymphocytes and macrophages, produces an interferon γ–dominated
chills, myalgia, headache, tachycardia, increased respiratory rate, cytokine milieu and results in the clearance of organisms by activated
increased circulating neutrophil count, and vasodilation with mild macrophages. Specific antibodies to surface antigens enhance phagocy-
hypotension may follow the initiation of treatment for syphilis. This tosis. Antigenic variation of the TprK protein is thought to contribute
reaction is thought to be a response to lipoproteins released by dying to development of subsequent stages of syphilis, persistence of infec-
PART 5
T. pallidum organisms. The Jarisch-Herxheimer reaction occurs in tion, and susceptibility to reinfection with another strain. Comparative
~50% of patients with primary syphilis, 90% of those with secondary genomic studies have revealed genes with sequence variations among
syphilis, and a lower proportion of persons with later-stage disease. T. pallidum strains, leading to development of molecular typing meth-
Defervescence takes place within 12–24 h. In secondary syphilis, ods used to examine syphilis outbreaks. Recent work has demonstrated
erythema and edema of the cutaneous lesions may increase. Patients that immunization with the outer-membrane protein Tp0751 signifi-
Infectious Diseases
should be warned to expect such developments, which can be man- cantly reduces dissemination of T. pallidum during syphilis infection
aged with symptom-based treatment. Steroid therapy is not required in an animal model. Vaccine studies with this and other antigens are
for this mild transient reaction. underway.
FOLLOW-UP EVALUATION OF RESPONSES TO THERAPY ■ FURTHER READING
Efficacy of treatment should be assessed by clinical evaluation and Cameron CE, Lukehart SA: Current status of syphilis vaccine devel-
monitoring of the quantitative VDRL or RPR titer for a fourfold opment: Need, challenges, prospects. Vaccine 32:1602, 2014.
decline (e.g., from 1:32 to 1:8). Patients with primary or secondary Centers for Disease Control and Prevention: Discordant results
syphilis should be examined 6 and 12 months after treatment, and from reverse sequence syphilis screening—five laboratories, United
persons with latent or late syphilis at 6, 12, and 24 months. More fre- States, 2006–2010. MMWR Morb Mortal Wkly Rep 60:133, 2011.
quent clinical and serologic examination (3, 6, 9, 12, and 24 months) Dombrowski JC et al: Prevalence estimates of complicated syphilis. Sex
is recommended for patients concurrently infected with HIV, regard- Transm Dis 42:702, 2015.
less of the stage of syphilis. Hook EW III: Syphilis. Lancet 389:1550, 2017.
After successful treatment of seropositive first-episode primary Workowski KA, Bolan GA: Sexually transmitted diseases treatment
or secondary syphilis, the VDRL or RPR titer progressively declines; guidelines, 2015. MMWR Recomm Rep 64:34, 2015.
the test becomes nonreactive by 12 months in 40–75% of seropositive
primary cases and in 20–40% of secondary cases. In patients with
HIV infection or a history of prior syphilis, VDRL and RPR tests are
178 Endemic Treponematoses
less likely to become nonreactive. Rates of decline of serologic titers
appear to be slower, and serologically defined treatment failures
more common, among HIV-infected patients than among those
without HIV co-infection; however, effective antiretroviral therapy Sheila A. Lukehart
may reduce these differences. Re-treatment should be considered
if serologic responses are not adequate or if clinical signs persist or
recur. Because it is difficult to differentiate treatment failure from The endemic treponematoses are chronic diseases that are transmitted
reinfection, the CSF should be examined, with treatment for neu- by direct contact, usually during childhood, and, like syphilis, can
rosyphilis if CSF is abnormal and treatment for late latent syphilis cause severe late manifestations years after initial infection. These dis-
if CSF is normal. A minority of patients treated for early syphilis eases are caused by very close relatives of Treponema pallidum subspe-
may experience a one-dilution titer increase within 14 days after cies pallidum, the etiologic agent of venereal syphilis (Chap. 177). Yaws,
treatment; however, this early elevation does not significantly affect pinta, and endemic syphilis (bejel) are traditionally distinguished
the serologic outcome at 6 months after treatment. Patients treated from venereal syphilis by mode of transmission, age of acquisition,
for late latent syphilis frequently have low initial VDRL or RPR titers geographic distribution, and clinical features; however, there is some
and may not have a fourfold decline after therapy with penicillin. In overlap for each of these factors. Our “knowledge” about these infec-
such patients, re-treatment is not warranted unless the titer rises or tions is based on observations by health care workers who have visited
Harrisons_20e_Part5_p0859-p1648.indd 1286 6/1/18 12:06 PM
■ DIAGNOSIS In addition to β-lactamase production, alteration of 1131
The most reliable method for establishing a diagnosis of Hib infection penicillin-binding proteins—a second mechanism
is recovery of the organism in culture. The presence of gram-negative of ampicillin resistance—has been detected in isolates of
coccobacilli in Gram-stained CSF is strong evidence for Hib meningitis. H. influenzae. Although rare in the United States, these β-lactamase-
Recovery of the organism from CSF confirms the diagnosis. Cultures negative ampicillin-resistant strains are common in Japan and are
of other normally sterile body fluids, such as blood, joint fluid, pleural increasing in prevalence in Europe. Resistance to macrolides is also
fluid, pericardial fluid, and subdural effusion, are confirmatory in being observed with increasing frequency in many regions of the
other infections. world. Continued monitoring of the evolving antimicrobial suscep-
Detection of PRP is an important adjunct to culture in rapid diag- tibility patterns of H. influenzae will be important.
nosis of Hib meningitis. Immunoelectrophoresis, latex agglutination,
coagglutination, and enzyme-linked immunosorbent assay are effec- ■ PREVENTION
tive in detecting PRP. These assays are particularly helpful when
patients have received prior antimicrobial therapy and thus are espe- Vaccination (See also Chap. 118) Three conjugate vaccines
cially likely to have negative cultures. that prevent invasive infections with Hib in infants and chil-
Because nontypable H. influenzae is primarily a mucosal pathogen, it dren are licensed in the United States. In addition to eliciting
is a component of a mixed flora; thus etiologic diagnosis is challenging. protective antibody, these vaccines prevent disease by reducing rates of
Nontypable H. influenzae infection is strongly suggested by the predom- pharyngeal colonization with Hib. The widespread use of conjugate
inance of gram-negative coccobacilli among abundant polymorphonu- vaccines has dramatically reduced the incidence of Hib disease in
clear leukocytes in a Gram-stained sputum specimen from a patient developed countries. Even though the manufacture of Hib vaccines is
in whom pneumonia is suspected. Although bacteremia is detectable costly, vaccination is cost-effective. The Global Alliance for Vaccines
in a small proportion of patients with pneumonia due to nontypable and Immunizations has recognized the underuse of Hib conjugate
H. influenzae, most such patients have negative blood cultures. vaccines.
A diagnosis of otitis media is based on the detection by pneumatic The disease burden has been reduced in developing countries that
otoscopy of fluid in the middle ear. An etiologic diagnosis requires have implemented routine vaccination (e.g., The Gambia, Chile). An
tympanocentesis but is not routinely sought. An invasive procedure important obstacle to more widespread vaccination is the lack of data
is also required to determine the etiology of sinusitis; thus, treatment on the epidemiology and burden of Hib disease in many developing
is often empirical once the diagnosis is suspected in light of clinical countries.
symptoms and sinus radiographs. All children should be immunized with an Hib conjugate vaccine,
CHAPTER 152 Haemophilus and Moraxella Infections
receiving the first dose at ~2 months of age, the rest of the primary
series at 2–6 months of age, and a booster dose at 12–15 months of age.
TREATMENT Specific recommendations vary for the different conjugate vaccines.
The reader is referred to the recommendations of the American Acad-
Haemophilus influenzae emy of Pediatrics (Chap. 118 and www.cispimmunize.org).
Initial therapy for meningitis due to Hib should consist of a cepha- Currently, no vaccines are available specifically for the prevention
losporin such as ceftriaxone or cefotaxime. For children, the dosage of disease caused by nontypable H. influenzae. However, a vaccine that
of ceftriaxone is 75–100 mg/kg daily given in two doses 12 h apart. contains protein D—a surface protein of H. influenzae—conjugated
The pediatric dosage of cefotaxime is 200 mg/kg daily given in four to pneumococcal polysaccharides is licensed in other countries and
doses 6 h apart. Adult dosages are 2 g every 12 h for ceftriaxone and is used widely throughout the world. The vaccine has shown partial
2 g every 4–6 h for cefotaxime. An alternative regimen for initial efficacy in preventing H. influenzae otitis media in clinical trials. Addi-
therapy is ampicillin (200–300 mg/kg daily in four divided doses) tional progress in the development of vaccines against nontypable
plus chloramphenicol (75–100 mg/kg daily in four divided doses). H. influenzae is anticipated.
Therapy should continue for a total of 1–2 weeks. Chemoprophylaxis The risk of secondary disease is greater than
Administration of glucocorticoids to patients with Hib meningitis normal among household contacts of patients with Hib disease. There-
reduces the incidence of neurologic sequelae. The presumed mecha- fore, all children and adults (except pregnant women) in households
nism is reduction of the inflammation induced by bacterial cell-wall with an index case and at least one incompletely immunized contact
mediators of inflammation when cells are killed by antimicrobial <4 years of age should receive prophylaxis with oral rifampin. When two
agents. Dexamethasone (0.6 mg/kg per day intravenously in four or more cases of invasive Hib disease have occurred within 60 days at a
divided doses for 2 days) is recommended for the treatment of Hib child-care facility attended by incompletely vaccinated children, admin-
meningitis in children >2 months of age. istration of rifampin to all attendees and personnel is indicated, as it is
Invasive infections other than meningitis are treated with the for household contacts. Chemoprophylaxis is not indicated in nursery
same antimicrobial agents. For epiglottitis, the dosage of ceftriax- and child-care contacts of a single index case. The reader is referred to
one is 50 mg/kg daily, and the dosage of cefotaxime is 150 mg/kg the recommendations of the American Academy of Pediatrics.
daily, given in three divided doses 8 h apart. Epiglottitis constitutes
a medical emergency, and maintenance of an airway is critical. The HAEMOPHILUS DUCREYI
duration of therapy is determined by the clinical response. A course Haemophilus ducreyi is the etiologic agent of chancroid (Chap. 131), a
of 1–2 weeks is usually appropriate. sexually transmitted disease characterized by genital ulceration and
Many infections caused by nontypable strains of H. influenzae, inguinal adenitis. In addition to being a cause of morbidity in itself,
such as otitis media, sinusitis, and exacerbations of COPD, can be chancroid is associated with HIV infection because of the role played
treated with oral antimicrobial agents. Approximately 20–35% of by genital ulceration in HIV transmission. Chancroid increases the
nontypable strains produce β-lactamase (with the exact proportion efficiency of transmission of and the degree of susceptibility to HIV
depending on geographic location), and these strains are resistant infection. H. ducreyi has also been recognized as an important cause of
to ampicillin. Several agents have excellent activity against nonty- non-sexually transmitted cutaneous ulcers.
pable H. influenzae, including amoxicillin/clavulanic acid, various
extended-spectrum cephalosporins, and the macrolides azithromy- ■ MICROBIOLOGY
cin and clarithromycin. Fluoroquinolones are highly active against H. ducreyi is a highly fastidious coccobacillary gram-negative bac-
H. influenzae and are useful in adults with exacerbations of COPD. terium whose growth requires X factor (hemin). Although, in light
However, fluoroquinolones are not currently recommended for the of this requirement, the bacterium has been classified in the genus
treatment of children or pregnant women because of possible effects Haemophilus, DNA homology and chemotaxonomic studies have estab-
on articular cartilage. lished substantial differences between H. ducreyi and other Haemophilus
Harrisons_20e_Part5_p0859-p1648.indd 1131 6/1/18 12:04 PM
1132 species. Taxonomic reclassification of the organism is likely in the pertenue, which is endemic in regions where H. ducreyi cutaneous ulcers
future but awaits further study. Ulcers contain predominantly T cells. are seen. Ulcers caused by H. ducreyi are less likely than those of yaws
The fact that patients who have had chancroid may have repeated to show central granulating tissue and less likely to have indurated
infections indicates that infection does not confer protection. edges, but substantial overlap in clinical characteristics exists.
■ EPIDEMIOLOGY AND PREVALENCE ■ DIAGNOSIS
The prevalence of chancroid has declined in the United States Clinical diagnosis of chancroid is often inaccurate, and laboratory
and worldwide. However, prevalence data must be inter- confirmation should be attempted in suspected cases. An accurate
preted with caution because of the difficulty of establishing a diagnosis of chancroid relies on culture of H. ducreyi from the lesion
diagnosis. The infection appears to be more common in developing or from an aspirate of suppurative lymph nodes. Since the organism
countries. Transmission is predominantly heterosexual, and cases in can be difficult to grow, the use of selective and supplemented media
males have outnumbered those in females by ratios of 3:1 to 25:1 during is necessary. No polymerase chain reaction (PCR) assay for H. ducreyi is
outbreaks. Contact with commercial sex workers and illicit drug use commercially available; such tests can be performed by Clinical Labo-
are strongly associated with chancroid. ratory Improvement Amendment (CLIA)–certified clinical laboratories
H. ducreyi has emerged as a major cause of cutaneous ulcers in the that have developed their own assays.
South Pacific and Africa. Strains that cause cutaneous ulcers have A probable diagnosis of chancroid can be made when the following
genome sequences that are nearly identical to class I strains (of two criteria are met: (1) one or more painful genital ulcers; (2) no evidence
related classes) of H. ducreyi that cause genital ulcers. of T. pallidum infection by dark-field examination of ulcer exudate or
by a negative serologic test for syphilis performed at least 7 days after
■ CLINICAL MANIFESTATIONS AND DIFFERENTIAL ulcer onset; (3) a typical clinical presentation for chancroid; and (4) a
DIAGNOSIS negative test for herpes simplex virus in the ulcer exudate.
Infection is acquired as the result of a break in the epithelium during A serologic test for syphilis does not distinguish cutaneous ulcers
sexual contact with an infected individual. After an incubation period due to H. ducreyi from those due to yaws. A PCR assay has been used in
of 4–7 days, the initial lesion—a papule with surrounding erythema— clinical studies to establish an H. ducreyi etiology, but, as stated above,
appears. In 2 or 3 days, the papule evolves into a pustule, which sponta- no such assay is commercially available.
neously ruptures and forms a sharply circumscribed ulcer that generally
is not indurated (Fig. 152-2). The ulcers are painful and bleed easily;
little or no inflammation of the surrounding skin is evident. Approxi- TREATMENT
mately half of patients develop enlarged, tender inguinal lymph nodes, Haemophilus ducreyi
which frequently become fluctuant and spontaneously rupture. Patients
PART 5
usually seek medical care after 1–3 weeks of painful symptoms. Treatment regimens recommended by the Centers for Disease Con-
The presentation of chancroid does not usually include all of the trol and Prevention include (1) a single 1-g oral dose of azithromy-
typical clinical features and is sometimes atypical. Multiple ulcers can cin; (2) ceftriaxone (250 mg intramuscularly in a single dose); (3)
coalesce to form giant ulcers. Ulcers can appear and then resolve, with ciprofloxacin (500 mg by mouth twice a day for 3 days); and (4)
Infectious Diseases
inguinal adenitis (Fig. 152-2) and suppuration following 1–3 weeks erythromycin base (500 mg by mouth three times a day for 7 days).
later; this clinical picture can be confused with that of lymphogranu- Isolates from patients who do not respond promptly to treatment
loma venereum (Chap. 184). Multiple small ulcers can resemble follic- should be tested for antimicrobial resistance. In patients with HIV
ulitis. Other differential diagnostic considerations include the various infection, healing may be slow and longer courses of treatment may
infections causing genital ulceration, such as primary syphilis, second- be necessary. Clinical treatment failure in HIV-seropositive patients
ary syphilis (condyloma latum), genital herpes, and donovanosis. In may reflect co-infection, especially with herpes simplex virus. Con-
rare cases, chancroid lesions become secondarily infected with bacteria; tacts of patients with chancroid should be identified and treated,
the result is extensive inflammation. whether or not symptoms are present, if they have had sexual
Non-sexually transmitted cutaneous ulcers caused by H. ducreyi contact with the patient during the 10 days preceding the patient’s
resemble those of yaws caused by Treponema pallidum subspecies onset of symptoms.
MORAXELLA CATARRHALIS
■ MICROBIOLOGY
M. catarrhalis is an unencapsulated gram-negative diplococcus whose
ecologic niche is the human respiratory tract. The organism was ini-
tially designated Micrococcus catarrhalis. Its name was changed to Neis-
seria catarrhalis in 1970 because of phenotypic similarities to commensal
Neisseria species. On the basis of more rigorous analysis of genetic
relatedness, Moraxella catarrhalis is now the widely accepted name for
this species.
■ EPIDEMIOLOGY
Nasopharyngeal colonization by M. catarrhalis is common in
infancy, with colonization rates ranging between 33% and
100% and depending on geographic location. Several factors
probably account for this geographic variation, including living condi-
tions, day-care attendance, hygiene, household smoking, and popula-
tion genetics. The prevalence of colonization decreases steadily with
age.
The widespread use of pneumococcal conjugate vaccines in some
countries has resulted in alterations in patterns of nasopharyngeal
colonization in resident populations. A relative increase in colonization
FIGURE 152-2 Chancroid with characteristic penile ulcers and associated left by nonvaccine pneumococcal serotypes, nontypable H. influenzae, and
inguinal adenitis (bubo). M. catarrhalis has occurred. These changes in colonization patterns
Harrisons_20e_Part5_p0859-p1648.indd 1132 6/1/18 12:04 PM
medications handled by this pathway. Grazoprevir is used with elbas- recognition and treatment reduce the morbidity and mortality rates 1345
vir (an NS5A inhibitor; see below) in a fixed-dose combination and is associated with HSV infections.
approved by the FDA for treatment of HCV genotypes 1 and 4.
■ ETIOLOGIC AGENT
■ NS5A INHIBITORS The genome of HSV is a 152-kb linear, double-stranded DNA
NS5A is a membrane-associated phosphoprotein that is part of the molecule (molecular weight, ~100 × 106) that encodes >90 tran-
HCV RNA replication complex and is essential for viral replication and scription units with 84 identified proteins. The genomic structures
assembly. Ledipasvir, velpatasvir, daclatasvir, elbasvir, and ombitasvir of the two HSV subtypes are similar. The overall genomic sequence
are all NS5A inhibitors. Each of these agents has largely been developed homology between HSV-1 and HSV-2 is ~50%, whereas the proteome
and studied with specific partner drugs as noted above (Table 186-1). homology is >80%. The homologous sequences are distributed over the
Treatment of HCV has been associated with flaring of chronic HBV entire genome map, and most of the polypeptides specified by one viral
infection. Monitoring for HBV activation in this context is warranted. type are antigenically related to polypeptides of the other viral type.
In the setting of significant renal dysfunction (CrCl, <30 mL/min), few Many type-specific regions unique to HSV-1 and HSV-2 proteins do
data are available to guide use of these newer DAAs. However, studies exist, however, and a number of them appear to be important in host
are ongoing to assess elbasvir/grazoprevir in this context, as these immunity. These type-specific regions have been used to develop sero-
agents are eliminated through the feces and are not renally handled. logic assays that distinguish between the two viral subtypes. Either
Emergence of HCV resistance-associated substitutions to the DAAs restriction endonuclease analysis or sequencing of viral DNA can be
have been documented. The impact on treatment is under active inves- used to distinguish between the two subtypes and among strains of
tigation and at this time is relevant mostly to those patients in whom each subtype. Recombinant viruses (HSV-1/HSV-2) do circulate in
prior treatment has failed. nature. The variability of nucleotide sequences from clinical strains of
These newer DAA regimens allow shorter courses of therapy, HSV-1 and HSV-2 is such that HSV isolates obtained from two individ-
improved tolerability, and reduced resistance. For updated informa- uals can be differentiated by restriction enzyme patterns or genomic
tion, readers should consult http://www.hcvguidelines.org/. sequences. Moreover, epidemiologically related sources, such as sexual
partners, mother–infant pairs, or persons involved in a common-source
ACKNOWLEDGMENT outbreak, can be inferred from such patterns. Deep sequencing of
The author thanks Raphael Dolin, MD, for his contributions to prior versions sequential isolates suggests that more than one variant of HSV-1 or
of this chapter and for years of mentorship. HSV-2 can be found in a single individual.
The viral genome is packaged in a regular icosahedral protein shell
■ FURTHER READING
CHAPTER 187 Herpes Simplex Virus Infections
(capsid) composed of 162 capsomeres (see Fig. 185-1). The outer cover-
American Association for the Study of Liver Disease/Infectious ing of the virus is a lipid-containing membrane (envelope) acquired as
Diseases Society of America: Recommendations for testing, manag- the DNA-containing capsid buds through the inner nuclear membrane
ing, and treating hepatitis C. Available from http://www.hcvguidelines of the host cell. Between the capsid and lipid bilayer of the envelope
.org. Accessed February 2, 2018. is the tegument. Viral replication has both nuclear and cytoplasmic
Crumpacker CS: Ganciclovir. N Engl J Med 335:721, 1996. phases. Initial attachment to the cell membrane involves interactions of
Dienstag JL: Hepatitis B virus infection. N Engl J Med 359:1486, 2008. viral glycoproteins C and B with several cellular heparan sulfate–like
Dobson J et al: Oseltamivir treatment for influenza in adults: A surface receptors. Subsequently, viral glycoprotein D binds to cellular
meta-analysis of randomized controlled trials. Lancet 385:1729, 2015. co-receptors that belong to the tumor necrosis factor receptor family
Dolin R et al: A controlled trial of amantadine and rimantadine in the of proteins, the immunoglobulin superfamily (nectin family), or both.
prophylaxis of influenza A infection. N Engl J Med 307:580, 1982. The ubiquity of these receptors contributes to the wide host range of
Hurt AC et al: Overview of the 3rd isirv-Antiviral Group Conference— herpesviruses. HSV replication is highly regulated. After fusion and
advances in clinical management. Influenza Other Respir Viruses entry, the nucleocapsid enters the cytoplasm and several viral proteins
9:20, 2015. are released from the virion. Some of these viral proteins shut off host
Kamar N et al: Ribavirin for chronic hepatitis E virus infection in trans- protein synthesis (by increasing cellular RNA degradation), whereas
plant recipients. N Engl J Med 370:1111, 2014. others “turn on” the transcription of early genes of HSV replication.
Lai C-L et al: Entecavir versus lamivudine for patients with HBeAg- These early gene products, designated a genes, are required for syn-
negative chronic hepatitis B. N Engl J Med 354:1011, 2006. thesis of the subsequent polypeptide group: the β polypeptides, many
Marty FM et al: Letermovir prophylaxis for cytomegalovirus in of which are regulatory proteins and enzymes required for DNA rep-
hematopoietic-cell transplantation. N Engl J Med 377:2433, 2017. lication. Most current antiviral drugs interfere with β proteins, such as
Whitley RJ et al: Global assessment of resistance to neuraminidase viral DNA polymerase. The third (γ) class of HSV genes requires viral
inhibitors, 2008–2011: The Influenza Resistance Information Study DNA replication for expression and encodes most structural proteins
(IRIS). Clin Infect Dis 58:1197, 2014. specified by the virus. New antiviral drugs directed at viral assembly
and release are under development.
After viral genome replication and structural protein synthesis,
Section 12 Infections Due to DNA Viruses nucleocapsids are assembled in the cell’s nucleus. Envelopment occurs
as the nucleocapsids bud through the inner nuclear membrane into the
perinuclear space. In some cells, viral replication in the nucleus forms
two types of inclusion bodies: type A basophilic Feulgen-positive bod-
187 Herpes Simplex Virus
Infections
ies that contain viral DNA and eosinophilic inclusion bodies that are
devoid of viral nucleic acid or protein and represent a “scar” of viral
infection. Enveloped virions are then transported via the endoplasmic
reticulum and the Golgi apparatus to the cell surface.
Lawrence Corey Viral genomes are maintained by some neuronal cells in a repressed
state called latency. Latency, which is associated with transcription
of only a limited number of virus-encoded RNAs, accounts for the
■ DEFINITION presence of viral DNA and RNA in neural tissue at times when infec-
Herpes simplex viruses (HSV-1, HSV-2; Herpesvirus hominis) produce tious virus cannot be isolated. Maintenance and growth of neural cells
a variety of infections involving mucocutaneous surfaces, the central from latently infected ganglia in tissue culture result in production of
nervous system (CNS), and—on occasion—visceral organs. Prompt infectious virions (explantation) and in subsequent permissive infection
Harrisons_20e_Part5_p0859-p1648.indd 1345 6/1/18 12:07 PM
1346 of susceptible cells (co-cultivation). Activation of the viral genome may demonstrated HSV viremia—another mechanism for extension of
then occur, resulting in reactivation—the normal pattern of regulated infection throughout the body—in ~30–40% of persons with primary
viral gene expression and replication and HSV release. The release HSV-2 infection; latent infection with both viral subtypes in both
of virions from the neuron follows a complex process of anterograde sensory and autonomic ganglia has been demonstrated. For HSV-1
transport down the length of neuronal axons. In experimental animals, infection, trigeminal ganglia are most commonly infected, although
ultraviolet light, systemic and local immunosuppression, and trauma extension to the inferior and superior cervical ganglia also occurs. With
to the skin or ganglia are associated with reactivation. genital infection, sacral nerve root ganglia (S2–S5) are most commonly
Three noncoding RNA latency-associated transcripts (LATs) are affected. Autonomic ganglia, pelvic nerves, and vaginal nerve roots are
found in the nuclei of latently infected neurons. Microdissection plus commonly infected.
real-time polymerase chain reaction (PCR) of individual neurons from After resolution of primary disease, infectious HSV can no longer be
cadaveric trigeminal ganglia explants revealed that many more neu- cultured from the ganglia; however, neuronal infection, as defined by
rons (2–10%) harbor HSV than would be predicted by in situ hybrid- the presence of viral DNA, persists in ganglionic cells in the anatomic
ization studies for LATs. Viral copy number is highly variable between regions of the initial infection. The mechanism of reactivation from
neurons, with extremely high levels in certain neurons, and HSV DNA latency is unknown, although increasingly evidence of limited viral
copy numbers are similar in LAT-positive and LAT-negative neurons. genes or microRNAs is identified in latently infected neurons. Evi-
These findings add to the uncertainty about the role that LATs play in dence exists for viral antigen and activated host T cells at the ganglia
preventing reactivation. Deletion mutants of the LAT region exhibit and periphery, and immune responses in ganglia as well as peripheral
reduced efficiency in their later reactivation. Substitution of HSV-1 tissue appear to influence the frequency and severity of HSV reactiva-
LATs for HSV-2 LATs induces an HSV-1 reactivation pattern. These tion. HSV-specific T cells have been recovered from peripheral-nerve
data indicate that LATs apparently maintain—rather than establish— root ganglia. Many of these resident CD8+ T cells are juxtaposed with
latency. HSV-1 LATs promote the survival of acutely infected neurons, latently HSV-1-infected neurons in the trigeminal ganglia and can
perhaps by inhibiting apoptotic pathways. LAT transcript abundance block reactivation with both interferon (IFN) γ release and granzyme
and low genome-copy number correlate with subnuclear positioning of B–mediated degradation of the immediate-early protein ICP4. In addi-
HSV genomes around the centromere. Indeed, chromatization of HSV tion, there appears to be a latent viral load in the ganglia that correlates
DNA appears to play a vital role in silencing expression of lytic repli- positively with the number of neurons infected and the rate of reacti-
cation genes. While the mechanism of latency and reactivation remains vation but inversely with the number of T cells present. It is not known
elusive, data suggest that viral micro-RNA appears to silence expres- whether reactivating stimuli transiently suppress these immune cells,
sion of the key neurovirulence factor infected-cell protein 34.5 (ICP34.5) independently upregulate transcription of lytic genes, or both. More-
and to bind in an antisense configuration to the immediate-early over, host containment in the mucosa has been demonstrated. Once
PART 5
protein ICP0 messenger RNA to prevent expression, which is vital to virus reaches the dermal–epidermal junction, there are three possible
HSV reactivation. Although certain viral transcripts are known to be outcomes: (1) rapid host containment of infection near the site of reac-
necessary for reactivation from latency, the molecular mechanisms of tivation; (2) spread of small amounts of virus into the epidermis, with
HSV latency are not fully understood, and strategies to interrupt or a micro-ulceration associated with low-titer subclinical shedding; and
maintain latency in neurons are in developmental stages. (3) widespread replication and necrosis of epithelial cells and subse-
Infectious Diseases
While latency is the predominant state of virus on a per-neuron quent clinical recurrence (the latter defined clinically by a skin blister
basis, the high frequency of oral and genital tract reactivation for and ulceration). Histologically, herpetic lesions involve a thin-walled
HSV-1 and HSV-2 suggests that the viruses are rarely quiescent within vesicle or ulceration in the basal region, multinucleated cells that may
the entire biomass of ganglionic tissue. There is increasing recognition include intranuclear inclusions, necrosis, and an acute inflammatory
that HSV infection of the autonomic ganglia plays an important role in infection. Re-epithelialization occurs once viral replication is restricted,
both initial and reactivation infections. In fact, deaths of animals from almost always in the absence of a scar.
HSV-2 infection appear to be related to autonomic dysfunction of the Analysis of the DNA from sequential isolates of HSV or from iso-
bowel. Both HSV-1 and HSV-2 are shed subclinically. Most persons lates from multiple infected ganglia in any one individual has revealed
infected with HSV-2 and HSV-1 have frequent subclinical bursts of similar, if not identical, restriction endonuclease or DNA sequence
reactivation lasting 2–4 h, and the host tissue-based immune system patterns in most persons. As more sensitive genomic technologies
can contain viral reactivation in the tissue before the development of are developed, evidence of multiple strains of the same subtype is
clinical reactivation. increasingly being reported. For example, infection of individual
neurons with multiple strains of drug-susceptible and drug-resistant
■ PATHOGENESIS virus in severely immunosuppressed patients indicates that ganglia
Exposure to HSV at mucosal surfaces or abraded skin sites permits can be reseeded during chronic infection. Because exposure to mucosal
entry of the virus into cells of the epidermis and dermis and initiation shedding is relatively common during a person’s lifetime, current data
of viral replication therein. HSV infections are usually acquired sub- suggest that exogenous infection with different strains of the same
clinically. Whether clinical or subclinical, HSV acquisition is associated subtype does occur.
with sufficient viral replication to permit infection of sensory and/or
autonomic nerve endings. On entry into the neuronal cell, the virus— ■ IMMUNITY
or, more likely, the nucleocapsid—is transported intra-axonally to the Host responses influence the acquisition of HSV disease, the severity of
nerve cell bodies in ganglia. Viral particles tether onto cellular proteins infection, resistance to the development of latency, the maintenance of
that motor along microtubules from axon tips (neurite endings) to latency, and the frequency of recurrences. Both antibody-mediated and
neuronal cell bodies. In humans, the transit interval of spread to the cell-mediated reactions are clinically important. Immunocompromised
ganglia after virus inoculation into peripheral tissue is unknown. patients with defects in cell-mediated immunity experience more
During the initial phase of infection, viral replication occurs in ganglia severe and more extensive HSV infections than those with deficits in
and contiguous neural tissue. Virus then spreads to other mucocuta- humoral immunity, such as agammaglobulinemia. Experimental abla-
neous surfaces through centrifugal migration of infectious virions via tion of lymphocytes indicates that T cells play a major role in prevent-
peripheral sensory nerves. This mode of spread helps explain the large ing lethal disseminated disease, although antibodies help reduce titers
surface area involved, the high frequency of new lesions distant from of virus in neural tissue. Some clinical manifestations of HSV appear to
the initial crop of vesicles that is characteristic in patients with primary be related to the host immune response (e.g., stromal opacities associ-
genital or oral–labial HSV infection, and the ability to recover virus ated with recurrent herpetic keratitis). The surface viral glycoproteins
from neural tissue distant from neurons innervating the inoculation have been shown to be targets of antibodies that mediate neutralization
site. Contiguous spread of locally inoculated virus also may take place and immune-mediated cytolysis (antibody-dependent cell-mediated
and allow further mucosal extension of disease. Recent studies have cytotoxicity). Monoclonal antibodies to HSV viral glycoproteins have,
Harrisons_20e_Part5_p0859-p1648.indd 1346 6/1/18 12:07 PM
in experimental infections, conferred protection against subsequent lesions. As many as 50% of heterosexual adults attending sexually 1347
neurologic disease or ganglionic latency. In humans, however, subunit transmitted disease clinics have antibodies to HSV-2. A wide variety
glycoprotein vaccines have been largely ineffective in reducing acqui- of serologic surveys has catalogued the widespread epidemic of HSV-2
sition of infection. Multiple cell populations, including neutrophils, in Central America, South America, and Africa. In Africa, HSV-2 sero-
macrophages, and a variety of T lymphocytes, play a role in host prevalence has ranged from 40 to 70% in obstetric and other sexually
defenses against HSV infections, as do lymphokines generated by experienced populations. Antibody prevalence rates average ~5–10%
T lymphocytes. In animals, passive transfer of primed lymphocytes higher among women than among men.
confers protection from subsequent HSV challenge. Maximal protec- Many studies continue to show that both incident and—more
tion usually requires the activation of multiple T-cell subpopulations, important—prevalent HSV-2 infection enhances the acquisition rate of
including cytotoxic T cells and T cells responsible for delayed hyper- HIV-1. More specifically, HSV-2 infection is associated on a population
sensitivity. The latter may confer protection by the antigen-stimulated basis with a two- to fourfold increase in HIV-1 acquisition. This association
release of lymphokines (e.g., IFNs), which in turn have a direct antiviral has been amply demonstrated in heterosexual men and women in both
effect and both activate and enhance a variety of specific and nonspe- the developed and the developing worlds. Epidemiologically, regions of
cific effector cells. The HSV virion contains a variety of genes that are the world with high HSV-2 prevalence and selected populations within
directed at the inhibition of host responses. These include gene no. 12 such regions have a higher population-based incidence of HIV-1.
(US-12), which can bind to the cellular transporter-activating protein An important observation is that HSV-2 facilitates the spread of
TAP-1 and reduce the ability of this protein to bind HSV peptides to HIV into low-risk populations; prevalent HSV-2 appears to increase
human leukocyte antigen class I, thereby reducing recognition of viral the risk of HIV infection by seven- to ninefold on a per-coital basis.
proteins by cytotoxic T cells of the host. This effect can be overcome by Mathematical models suggest that ~33–50% of HIV-1 infections may
the addition of IFN-γ, but this reversal requires 24–48 h; thus, the virus be attributable to HSV-2 both in men who have sex with men (MSM)
has time to replicate and invade other host cells. Entry of infectious and in sub-Saharan Africa. In addition, HSV-2 is more frequently
HSV-1 and HSV-2 inhibits several signaling pathways of both CD4+ reactivated in and transmitted by persons co-infected with HIV-1 than
and CD8+ T cells, leading to their functional impairment in killing and in persons not co-infected. Thus, most areas of the world with a high
influencing the spectrum of their cytokine secretion. HIV-1 prevalence also have a high HSV-2 prevalence. The shedding of
HSV-specific CD8+ T-cell responses appear to be an important com- HIV-1 virions from herpetic lesions in the genital region facilitates the
ponent in viral clearance from lesions. Immunosuppressed patients spread of HIV through sexual contact. HSV-2 reactivation is associated
with frequent and prolonged HSV lesions have fewer functional CD8+ with a localized persistent inflammatory response consisting of high
T cells directed at HSV. HSV-specific CD8+ T cells have been shown to concentrations of CCR5-enriched CD4+ T cells as well as inflammatory
CHAPTER 187 Herpes Simplex Virus Infections
persist in the genital skin at the dermal–epidermal junction contiguous dendritic cells in the submucosa of the genital skin. These cells can
to neuronal endings for months after lesion resolution. Even during support HIV infection and replication and thus are likely to account
clinical quiescence, these CD8+ T cells make both antiviral and cyto- for the increased risk of HIV acquisition among persons with genital
toxic proteins indicative of immune surveillance. These resident mem- herpes. Unfortunately, antiviral therapy does not reduce this subclini-
ory CD8+ T cells appear to be “first responders” capable of controlling cal postreactivation inflammation, probably because of the inability of
viral reactivation at the site of viral release into the dermis. This rapid current antiviral agents to prevent the release of small amounts of HSV
“on and off” interplay between the virus and the host helps explain the antigen into the genital mucosa.
variability in clinical disease severity between episodes in any single Several studies suggest that many cases of “asymptomatic” genital
individual. Differences of 30–60 min in host responses can result in HSV-2 infection are, in fact, simply unrecognized or confined to ana-
100- to 1000-fold differences in viral levels and can determine whether tomic regions of the genital tract that are not easily visualized. Asymp-
an episode of disease is subclinical or clinical. tomatic seropositive persons shed virus on mucosal surfaces almost as
There is a strong association between the magnitude of the CD8+ T frequently as do those with symptomatic disease. This large reservoir
lymphocyte response and the clearance of virus from genital lesions. of unidentified carriers of HSV-2 and the frequent asymptomatic reac-
The location, effectiveness, and longevity of the T lymphocytes (and tivation of the virus from the genital tract have fostered the continued
perhaps of other immune effector cells) may be important in the spread of genital herpes throughout the world.
expression of disease and the likelihood of transmission over time. HSV infections occur throughout the year. Transmission can result
from contact with persons who have active ulcerative lesions or with
■ EPIDEMIOLOGY persons who have no clinical manifestations of infection but who are
Seroepidemiologic studies have documented HSV infections shedding HSV from mucocutaneous surfaces. HSV reactivation on gen-
worldwide. The past 15 years have shown that the prevalence of ital skin and mucosal surfaces is common. In fact, recent studies indi-
HSV-2 is even higher in the developing than in the developed cate that most HSV-1 and HSV-2 episodes last <4–6 h; thus, replication
world. In sub-Saharan Africa, HSV-2 seroprevalence among pregnant of the virus and clearance by the host are rapid. Even with once-daily
women may approach 60%, and annual acquisition rates among teenage sampling, HSV DNA can be detected on 20–30% of days by PCR. Corre-
girls may verge on 20%. The global incidence has been estimated at sponding figures for HSV-1 in oral secretions are similar. Rates of shed-
~23.6 million infections per year, with >400 million infected persons ding are highest during the initial years after acquisition, with viral
worldwide. As in the developed world, the rate of HSV-2 coital acquisition shedding occurring on as many as 30–50% of days during this period.
as well as the serologic prevalence is higher among women than among Immunosuppressed patients shed HSV from mucosal sites at an even
men. Most of this HSV-2 acquisition is preceded by acquisition of HSV-1; higher frequency (20–80% of days). These high rates of mucocutaneous
the frequency of genital HSV-1 in the developing world is low at present. reactivation suggest that exposure to HSV from sexual or other close
Infection with HSV-1 is acquired more frequently and earlier in life contact (kissing, sharing of glasses or silverware) is common and help
than infection with HSV-2. More than 90% of adults have antibodies to explain the continuing spread and high seroprevalence of HSV infec-
HSV-1 by the fifth decade of life. In populations of low socioeconomic tions worldwide. Reactivation rates vary widely among individuals.
status, most persons acquire HSV-1 infection before the third decade Among HIV-positive patients, a low CD4+ T-cell count and a high
of life. Antibodies to HSV-2 are not detected routinely until puberty. HIV-1 load are associated with increased rates of HSV reactivation.
Antibody prevalence rates correlate with past sexual activity and vary Daily antiviral chemotherapy for HSV-2 infection can reduce shedding
greatly among different population groups. There is evidence that the rates but does not eliminate shedding, as measured by PCR or culture.
prevalence of HSV-2 has decreased slightly over the past decade or so
in the United States. Serosurveys indicate that 15–20% of the U.S. pop- ■ CLINICAL SPECTRUM
ulation has antibodies to HSV-2. In most routine obstetric and family HSV has been isolated from nearly all visceral and mucocutaneous
planning clinics, 25% of women have HSV-2 antibodies, although only sites. The clinical manifestations and course of HSV infection depend
10% of those who are seropositive for HSV-2 report a history of genital on the anatomic site involved, the age and immune status of the host,
Harrisons_20e_Part5_p0859-p1648.indd 1347 6/1/18 12:07 PM
1348 and the antigenic type of the virus. Primary HSV infections (i.e., first of the facial nerve). Some but not all trials have documented quicker
infections with either HSV-1 or HSV-2 in which the host lacks HSV anti- resolution of facial paralysis with the prompt initiation of antiviral
bodies in acute-phase serum) are frequently accompanied by systemic therapy, with or without glucocorticoids. However, other trials have
signs and symptoms. Compared with recurrent episodes, primary shown little benefit. A recent Cochrane review indicates that there are
infections, which involve both mucosal and extramucosal sites, are advantages to the use of both antiviral drugs and glucocorticoids for
characterized by a longer duration of symptoms and virus isolation moderate to severe Bell’s palsy. Glucocorticoids alone are preferred for
from lesions. The incubation period ranges from 1 to 26 days (median, mild disease.
6–8 days). Both viral subtypes can cause genital and oral–facial infec-
tions, and the infections caused by the two subtypes are clinically
Genital Infections First-episode primary genital herpes is char-
acterized by fever, headache, malaise, and myalgias. Pain, itching,
indistinguishable. However, the frequency of reactivation of infection
dysuria, vaginal and urethral discharge, and tender inguinal lymph-
is influenced by anatomic site and virus type. Genital HSV-2 infection
adenopathy are the predominant local symptoms. Widely spaced
is twice as likely to reactivate and recurs 8–10 times more frequently
bilateral lesions of the external genitalia are characteristic (Fig. 187-1).
than genital HSV-1 infection. Conversely, oral–labial HSV-1 infection
Lesions may be present in varying stages, including vesicles, pustules,
recurs more frequently than oral–labial HSV-2 infection. Asymptomatic
or painful erythematous ulcers. The cervix and urethra are involved in
shedding rates follow the same pattern.
>80% of women with first-episode infections. First episodes of genital
Oral–Facial Infections Gingivostomatitis and pharyngitis are herpes in patients who have had prior HSV-1 infection are associated
the most common clinical manifestations of first-episode HSV-1 infec- with systemic symptoms in a few cases and with faster healing than
tion, whereas recurrent herpes labialis is the most common clinical primary genital herpes. Subclinical DNAemia has been found in ~30%
manifestation of reactivation HSV-1 infection. HSV pharyngitis and of cases of true primary genital herpes. The clinical courses of acute
gingivostomatitis usually result from primary infection and are most first-episode genital herpes are similar for HSV-1 and HSV-2 infection.
common among children and young adults. Clinical symptoms and However, the recurrence rates of genital disease differ with the viral
signs, which include fever, malaise, myalgias, inability to eat, irritabil- subtype: the 12-month recurrence rates among patients with first-
ity, and cervical adenopathy, may last 3–14 days. Lesions may involve episode HSV-2 and HSV-1 infections are ~90 and ~55%, respectively
the hard and soft palate, gingiva, tongue, lip, and facial area. HSV-1 or (median number of recurrences, 4 and <1, respectively). Recurrence
HSV-2 infection of the pharynx usually results in exudative or ulcerative rates for genital HSV-2 infections vary greatly among individuals and
lesions of the posterior pharynx and/or tonsillar pillars. Lesions of the over time within the same individual. HSV has been isolated from
tongue, buccal mucosa, or gingiva may occur later in the course in one- the urethra and urine of men and women without external genital
third of cases. Fever lasting 2–7 days and cervical adenopathy are com- lesions. A clear mucoid discharge and dysuria are characteristics of
symptomatic HSV urethritis. HSV has been isolated from the urethra
PART 5
mon. It can be difficult to differentiate HSV pharyngitis clinically from
bacterial pharyngitis, Mycoplasma pneumoniae infections, and pharyn- of 5% of women with the dysuria–frequency syndrome. Occasionally,
geal ulcerations of noninfectious etiologies (e.g., Stevens-Johnson syn- HSV genital tract disease is manifested by endometritis and salpingitis
drome). No substantial evidence suggests that reactivation of oral–labial in women and by prostatitis in men. About 15% of cases of HSV-2
HSV infection is associated with symptomatic recurrent pharyngitis. acquisition are associated with nonlesional clinical syndromes, such as
Infectious Diseases
Reactivation of HSV from the trigeminal ganglia may be associ- aseptic meningitis, cervicitis, or urethritis. A more complete discussion
ated with asymptomatic virus excretion in the saliva, development of of the differential diagnosis of genital herpes is presented in Chap. 131.
intraoral mucosal ulcerations, or herpetic ulcerations on the vermilion Both HSV-1 and HSV-2 can cause symptomatic or asymptomatic
border of the lip or external facial skin. About 50–70% of seropositive rectal and perianal infections. HSV proctitis is usually associated
patients undergoing trigeminal nerve-root decompression and 10–15% with rectal intercourse. However, subclinical perianal shedding of
of those undergoing dental extraction develop oral–labial HSV infec- HSV is detected in women and men who report no rectal intercourse.
tion a median of 3 days after these procedures. Clinical differentiation This phenomenon is due to the establishment of latency in the sacral
of intraoral mucosal ulcerations due to HSV from aphthous, traumatic,
or drug-induced ulcerations is difficult.
In immunosuppressed patients, HSV infection may extend into
mucosal and deep cutaneous layers. Friability, necrosis, bleeding,
severe pain, and inability to eat or drink may result. The lesions of HSV
mucositis are clinically similar to mucosal lesions caused by cytotoxic
drug therapy, trauma, or fungal or bacterial infections. Persistent ulcer-
ative HSV infections are among the most common infections in patients
with AIDS. HSV and Candida infections often occur concurrently.
Systemic antiviral therapy speeds the rate of healing and relieves the
pain of mucosal HSV infections in immunosuppressed patients. The
frequency of HSV reactivation during the early phases of transplan-
tation or induction chemotherapy is high (50–90%), and prophylactic
systemic antiviral agents such as IV acyclovir and penciclovir or the
oral congeners of these drugs are used to reduce reactivation rates.
Patients with atopic eczema may also develop severe oral–facial HSV
infections (eczema herpeticum), which may rapidly involve extensive
areas of skin and occasionally disseminate to visceral organs. Extensive
eczema herpeticum has resolved promptly with the administration of
IV acyclovir. Erythema multiforme may also be associated with HSV
infections (see Figs. 52-9 and A1-24); some evidence suggests that
HSV infection is the precipitating event in ~75% of cases of cutaneous
erythema multiforme. HSV antigen has been demonstrated both in
circulatory immune complexes and in skin lesion biopsy samples from
FIGURE 187-1 Genital herpes: primary vulvar infection, with multiple, extremely
these cases. Patients with severe HSV-associated erythema multiforme painful, punched-out, confluent, shallow ulcers on the edematous vulva and
are candidates for chronic suppressive oral antiviral therapy. perineum. Micturition is often very painful. Associated inguinal lymphadenopathy
HSV-1 and varicella-zoster virus (VZV) have been implicated in the is common. (Reprinted with permission from K Wolff et al: Fitzpatrick’s Color Atlas
etiology of Bell’s palsy (flaccid paralysis of the mandibular portion & Synopsis of Clinical Dermatology, 5th ed. New York, McGraw-Hill, 2005.)
Harrisons_20e_Part5_p0859-p1648.indd 1348 6/1/18 12:07 PM
dermatome from prior genital tract infection, with subsequent reac- onset of CNS symptoms. In ~25% of the cases examined, the HSV-1 1349
tivation in epithelial cells in the perianal region. Such reactivations strains from the oropharynx and brain tissue of the same patient dif-
are often subclinical. Symptoms of HSV proctitis include anorectal fer; thus some cases may result from reinfection with another strain
pain, anorectal discharge, tenesmus, and constipation. Sigmoidoscopy of HSV-1 that reaches the CNS. Two theories have been proposed to
reveals ulcerative lesions of the distal 10 cm of the rectal mucosa. Rectal explain the development of actively replicating HSV in localized areas
biopsies show mucosal ulceration, necrosis, polymorphonuclear and of the CNS in persons whose ganglionic and CNS isolates are similar.
lymphocytic infiltration of the lamina propria, and (in occasional cases) Reactivation of latent HSV-1 infection in trigeminal or autonomic nerve
multinucleated intranuclear inclusion-bearing cells. Perianal herpetic roots may be associated with extension of virus into the CNS via nerves
lesions are also found in immunosuppressed patients receiving cyto- innervating the middle cranial fossa. HSV DNA has been demonstrated
toxic therapy. Extensive perianal herpetic lesions and/or HSV proctitis by DNA hybridization in brain tissue obtained at autopsy—even from
is common among patients with HIV infection. healthy adults. Thus, reactivation of long-standing latent CNS infection
may be another mechanism for the development of HSV encephalitis.
Herpetic Whitlow Herpetic whitlow—HSV infection of the Recent studies have identified genetic polymorphisms among
finger—may occur as a complication of primary oral or genital herpes families with a high frequency of HSV encephalitis. Peripheral-
by inoculation of virus through a break in the epidermal surface or blood mononuclear cells from these patients (predominantly chil-
by direct introduction of virus into the hand through occupational or dren) appear to secrete reduced levels of IFN in response to HSV.
some other type of exposure. Clinical signs and symptoms include Genetic mutations in TLR3 documented in patients with HSV enceph-
abrupt-onset edema, erythema, and localized tenderness of the infected alitis suggest that some cases of sporadic HSV encephalitis may be
finger. Vesicular or pustular lesions of the fingertip that are indistin- related to host genetic determinants.
guishable from lesions of pyogenic bacterial infection are seen. Fever, The clinical hallmark of HSV encephalitis has been the acute onset of
lymphadenitis, and epitrochlear and axillary lymphadenopathy are fever and focal neurologic symptoms and signs, especially in the tem-
common. The infection may recur. Prompt diagnosis (to avoid unnec- poral lobe (Fig. 187-2). Clinical differentiation of HSV encephalitis from
essary and potentially exacerbating surgical therapy and/or transmis- other viral encephalitides, focal infections, or noninfectious processes is
sion) is essential. Antiviral chemotherapy is usually recommended (see difficult. Elevated cerebrospinal fluid (CSF) protein levels, leukocytosis
below). (predominantly lymphocytes), and red blood cell counts due to hem-
Herpes Gladiatorum HSV may infect almost any area of skin. orrhagic necrosis are common. While brain biopsy has been the gold
Mucocutaneous HSV infections of the thorax, ears, face, and hands standard for defining HSV encephalitis, a highly sensitive and specific
have been described among wrestlers. Transmission of these infections PCR for detection of HSV DNA in CSF has largely replaced biopsy for
CHAPTER 187 Herpes Simplex Virus Infections
is facilitated by trauma to the skin sustained during wrestling. Several defining CNS infection. Although titers of antibody to HSV in CSF
recent outbreaks have illustrated the importance of prompt diagnosis and serum increase in most cases of HSV encephalitis, they rarely do
and therapy to contain the spread of this infection. so earlier than 10 days into the illness and therefore, although useful
in retrospect, generally are not helpful in establishing an early clinical
Eye Infections HSV infection of the eye is the most common diagnosis. In rare cases, demonstration of HSV antigen, HSV DNA, or
cause of corneal blindness in the United States. HSV keratitis presents HSV replication in brain tissue obtained by biopsy is highly sensitive;
as an acute onset of pain, blurred vision, chemosis, conjunctivitis, and examination of such tissue also provides the opportunity to identify
characteristic dendritic lesions of the cornea. Use of topical glucocor- alternative, potentially treatable causes of encephalitis. Antiviral che-
ticoids may exacerbate symptoms and lead to involvement of deep motherapy with acyclovir reduces the rate of death from HSV enceph-
structures of the eye. Debridement, topical antiviral treatment, and/or alitis. Most authorities recommend the administration of IV acyclovir
IFN therapy hastens healing. However, recurrences are common, and to patients with presumed HSV encephalitis until the diagnosis is con-
the deeper structures of the eye may sustain immunopathologic injury. firmed or an alternative diagnosis is made. All confirmed cases should
Stromal keratitis due to HSV appears to be related to T cell–dependent be treated with IV acyclovir (30 mg/kg per day in three divided doses
destruction of deep corneal tissue. An HSV-1 epitope that is autoreac- for 14–21 days). After the completion of therapy, the clinical recurrence
tive with T cell–targeting corneal antigens
has been postulated to be a factor in this
infection. Chorioretinitis, usually a manifes-
tation of disseminated HSV infection, may
occur in neonates or in patients with HIV
infection. HSV and VZV can cause acute
necrotizing retinitis as an uncommon but
severe manifestation.
Central and Peripheral Nervous
System Infections HSV accounts for
10–20% of all cases of sporadic viral enceph-
alitis in the United States. The estimated
incidence is ~2.3 cases per 1 million persons
per year. Cases are distributed throughout
the year, and the age distribution appears to
be biphasic, with peaks at 5–30 and >50 years
of age. HSV-1 causes >95% of cases.
The pathogenesis of HSV encephalitis
varies. In children and young adults, pri-
mary HSV infection may result in enceph-
alitis; presumably, exogenously acquired
virus enters the CNS by neurotropic spread
from the periphery via the olfactory bulb.
However, most adults with HSV encepha-
litis have clinical or serologic evidence of FIGURE 187-2 Computed tomography and diffusion-weighted magnetic resonance imaging scans of the brain
mucocutaneous HSV-1 infection before the of a patient with left-temporal-lobe herpes simplex virus encephalitis.
Harrisons_20e_Part5_p0859-p1648.indd 1349 6/1/18 12:07 PM
1350 of encephalitis requiring more treatment has been reported. For this of lower respiratory tract HSV infection in overall rates of morbidity
reason, some authorities prefer to treat initially for 21 days, and many and mortality associated with these conditions is unclear. HSV is an
continue therapy until HSV DNA has been eliminated from the CSF. uncommon cause of hepatitis in immunocompetent patients. HSV
Even with therapy, neurologic sequelae are common, especially among infection of the liver is associated with fever, abrupt elevations of
persons >50 years of age. bilirubin and serum aminotransferase levels, and leukopenia (<4000
HSV DNA has been detected in CSF from 3 to 15% of persons pre- white blood cells/μL). Disseminated intravascular coagulation may
senting to the hospital with aseptic meningitis. HSV meningitis, which also develop.
is usually seen in association with primary genital HSV infection, is Other reported complications of HSV infection include monarticular
an acute, self-limited disease manifested by headache, fever, and mild arthritis, adrenal necrosis, idiopathic thrombocytopenia, and glomeru-
photophobia and lasting 2–7 days. Lymphocytic pleocytosis in the lonephritis. Disseminated HSV infection in immunocompetent patients
CSF is characteristic. Neurologic sequelae of HSV meningitis are rare. is rare. In immunocompromised patients, burn patients, or malnour-
HSV is the most commonly identified cause of recurrent lymphocytic ished individuals, HSV occasionally disseminates to other visceral
meningitis (Mollaret’s meningitis). Demonstration of HSV antibodies in organs, such as the adrenal glands, pancreas, small and large intestines,
CSF or persistence of HSV DNA in CSF can establish the diagnosis. For and bone marrow. Rarely, primary HSV infection in pregnancy dissem-
persons with frequent recurrences of HSV meningitis, daily antiviral inates and may be associated with the death of both mother and fetus.
therapy has reduced the frequency of recurrent episodes of symptom- This uncommon event is usually related to the acquisition of primary
atic meningitis. infection in the third trimester. Disseminated HSV infection is best
Autonomic nervous system dysfunction, especially of the sacral detected by the presence of HSV DNA in plasma or blood.
region, has been reported in association with both HSV and VZV infec-
tions. Numbness, tingling of the buttocks or perineal areas, urinary Neonatal HSV Infections Of all HSV-infected populations,
retention, constipation, CSF pleocytosis, and (in males) impotence neonates (infants <6 weeks) have the highest frequency of visceral
may occur. Symptoms appear to resolve slowly over days or weeks. and/or CNS infection. Without therapy, the overall rate of death from
Occasionally, hypoesthesia and/or weakness of the lower extremities neonatal herpes is 65%; <10% of neonates with CNS infection develop
persists for many months. Transitory hypoesthesia of the area of skin normally. Although skin lesions are the most commonly recognized
innervated by the trigeminal nerve and vestibular system dysfunction features of disease, many infants do not develop lesions at all or do
(as measured by electronystagmography) are the predominant signs so only well into the course of disease. Neonatal infection is usually
of disease. Whether antiviral chemotherapy can abort these signs or acquired perinatally from contact with infected genital secretions at
reduce their frequency and severity is not yet known. Rarely, transverse delivery. Congenitally infected infants have been reported. Of neonatal
myelitis, manifested by a rapidly progressive symmetric paralysis of HSV infections, 30–50% are due to HSV-1 and 50–70% to HSV-2. The
PART 5
the lower extremities or Guillain-Barré syndrome, follows HSV infec- risk of developing neonatal HSV infection is 10 times higher for an
tion. Similarly, peripheral nervous system involvement (Bell’s palsy) or infant born to a mother who has recently acquired HSV than for other
cranial polyneuritis may be related to reactivation of HSV-1 infection. infants. Neonatal HSV-1 infections may also be acquired through post-
natal contact with immediate family members who have symptomatic
Visceral Infections HSV infection of visceral organs usually or asymptomatic oral–labial HSV-1 infection or through nosocomial
Infectious Diseases
results from viremia, and multiple-organ involvement is common. transmission within the hospital. All neonates with presumed herpes
Occasionally, however, the clinical manifestations of HSV infection should be treated with IV acyclovir and then placed on maintenance
involve only the esophagus, lung, or liver. HSV esophagitis may result oral antiviral therapy for the first 6–12 months of life. Antiviral chemo-
from direct extension of oral–pharyngeal HSV infection into the esoph- therapy with high-dose IV acyclovir (60 mg/kg per day) has reduced
agus or may occur de novo by reactivation and spread of HSV to the the mortality rate from neonatal herpes to ~15%. However, rates of
esophageal mucosa via the vagus nerve. The predominant symptoms morbidity, especially among infants with HSV-2 infection involving the
of HSV esophagitis are odynophagia, dysphagia, substernal pain, and CNS, are still very high.
weight loss. Multiple oval ulcerations appear on an erythematous base
with or without a patchy white pseudomembrane. The distal esopha- HSV in Pregnancy In the United States, 22% of all pregnant
gus is most commonly involved. With extensive disease, diffuse friabil- women and 55% of non-Hispanic black pregnant women are seropos-
ity may spread to the entire esophagus. Neither endoscopic nor barium itive for HSV-2. However, the risk of mother-to-child transmission of
examination can reliably differentiate HSV esophagitis from Candida HSV in the perinatal period is highest when the infection is acquired
esophagitis or from esophageal ulcerations due to thermal injury, radi- near the time of labor—that is, in previously HSV-seronegative women.
ation, or corrosives. Endoscopically obtained secretions—for cytologic The clinical manifestations of recurrent genital herpes—including
examination and culture or DNA detection by PCR—provide the most the frequency of subclinical versus clinical infection, the duration of
useful material for diagnosis. Systemic antiviral chemotherapy usually lesions, pain, and constitutional symptoms—are similar in pregnant
reduces the severity and duration of symptoms and heals esophageal and nonpregnant women. Recurrences increase in frequency over the
ulcerations. course of pregnancy. However, when women are seropositive for HSV-2
HSV pneumonitis is uncommon except in severely immunosup- at the outset of pregnancy, no effect on neonatal outcomes (including
pressed patients and may result from extension of herpetic tracheobron- birth weight and gestational age) is seen. First-episode infections in
chitis into lung parenchyma. Focal necrotizing pneumonitis usually pregnancy have more severe consequences for mother and infant.
ensues. Hematogenous dissemination of virus from sites of oral or Maternal visceral dissemination during the third trimester occasionally
genital mucocutaneous disease may also occur, producing bilateral occurs, as does premature birth or intrauterine growth retardation. The
interstitial pneumonitis. Bacterial, fungal, and parasitic pathogens acquisition of primary disease in pregnancy, whether related to HSV-1
are commonly present in HSV pneumonitis. The mortality rate from or HSV-2, carries the risk of transplacental transmission of virus to the
untreated HSV pneumonia in immunosuppressed patients is high neonate and can result in spontaneous abortion, although this outcome
(>80%). HSV has also been isolated from the lower respiratory tract of is relatively uncommon. For newly acquired genital HSV infection dur-
persons with acute respiratory distress syndrome and prolonged intu- ing pregnancy, most authorities recommend treatment with acyclovir
bation. Most authorities believe that the presence of HSV in tracheal (400 mg three times daily) or valacyclovir (500–1000 mg twice daily)
aspirates in such settings is due to reactivation of HSV in the tracheal for 7–10 days. However, the impact of this intervention on transmission
region and localized tracheitis in persons with long-term intubation. is unknown. The high HSV-2 prevalence rate in pregnancy and the
Such patients should be evaluated for extension of HSV infection into low incidence of neonatal disease (1 case per 6000–20,000 live births)
the lung parenchyma. Controlled trials assessing the role of antiviral indicate that only a few infants are at risk of acquiring HSV. Therefore,
agents used against HSV in morbidity and mortality associated with cesarean section is not warranted for all women with recurrent genital
acute respiratory distress syndrome have not been conducted. The role disease. Because intrapartum transmission of infection accounts for
Harrisons_20e_Part5_p0859-p1648.indd 1350 6/1/18 12:07 PM
the majority of cases, abdominal delivery need be considered only for cytopathic effect in a variety of cell culture systems, and this effect can 1351
women who are shedding HSV at delivery. Several studies have shown be identified within 48–96 h after inoculation. Spin-amplified culture
no correlation between recurrence of viral shedding before delivery with subsequent staining for HSV antigen has shortened the time
and viral shedding at term. Hence, weekly virologic monitoring and needed to identify HSV to <24 h. Culture is indicated when antiviral
amniocentesis are not recommended. sensitivity testing is required. The sensitivity of all detection methods
The frequency of transmission from mother to infant is markedly depends on the stage of the lesions (with higher sensitivity for vesic-
higher among women who acquire HSV near term (30–50%) than ular than for ulcerative lesions), on whether the patient has a first or
among those in whom HSV-2 infection is reactivated at delivery (<1%). a recurrent episode of the disease (with higher sensitivity in first than
Although maternal antibody to HSV-2 is protective, antibody to HSV-1 in recurrent episodes), and on whether the sample is from an immu-
offers little or no protection against neonatal HSV-2 infection. Primary nosuppressed or an immunocompetent patient (with more antigen
genital infection with HSV-1 leads to a particularly high risk of trans- or DNA in immunosuppressed patients). Laboratory confirmation
mission during pregnancy and accounts for an increasing proportion permits subtyping of the virus; information on subtype may be useful
of neonatal HSV cases. Moreover, during reactivation, HSV-1 appears epidemiologically and may help to predict the frequency of reactiva-
more transmissible to the neonate than HSV-2. Only 2% of women who tion after first-episode oral–labial or genital HSV infection.
are seropositive for HSV-2 have HSV-2 isolated from cervical secretions Both type-specific and type-common antibodies to HSV develop
at delivery, and only 1% of infants exposed in this manner develop during the first several weeks after infection and persist indefinitely.
infection, presumably because of the protective effects of maternally Serologic assays with whole-virus antigen preparations, such as com-
transferred antibodies and perhaps lower viral titers during reactiva- plement fixation, neutralization, indirect immunofluorescence, passive
tion. Despite the low frequency of transmission of HSV in this setting, hemagglutination, radioimmunoassay, and enzyme-linked immuno-
30–50% of infants with neonatal HSV are born to mothers with estab- sorbent assay, are useful for differentiating uninfected (seronegative)
lished genital herpes. persons from those with past HSV-1 or HSV-2 infection, but they do
Isolation of HSV by cervicovaginal swab at the time of delivery is the not reliably distinguish between the two viral subtypes. Serologic
greatest risk factor for intrapartum HSV transmission (relative risk = assays that identify antibodies to the type-specific glycoprotein G of
346); however, culture-negative, PCR-positive cases of intrapartum the two viral subtypes (G1 and G2) are available commercially and can
transmission are well described. New acquisition of HSV (odds ratio distinguish reliably between the human antibody responses to HSV-1
[OR] = 49), isolation of HSV-1 versus HSV-2 (OR = 35), cervical versus and HSV-2. Point-of-care assays that provide results from capillary
vulvar HSV detection (OR = 15), use of fetal scalp electrodes (OR = 3.5), blood or serum during a clinic visit are available. A western blot assay
and young maternal age confer further risk of transmission, whereas that can detect several HSV type-specific proteins can also be used.
CHAPTER 187 Herpes Simplex Virus Infections
cesarean delivery is protective (OR = 0.14). Physical examination The presence of type-specific HSV-2 antibody implies past HSV-2
poorly predicts the absence of shedding, and PCR far exceeds culture infection—i.e., latent infection and likely subclinical reactivation.
in terms of sensitivity and speed. Therefore, PCR detection at the onset Acute- and convalescent-phase serum samples can be useful in
of labor should be used to aid clinical decision-making for women with demonstrating seroconversion during primary HSV-1 or HSV-2 infec-
HSV-2 antibody. Because cesarean section appears to be an effective tion. However, few available tests report titers, and increases in index
means of reducing maternal–fetal transmission, patients with recurrent values do not reflect first episodes in all patients. Serologic assays
genital herpes should be encouraged to come to the hospital early at based on type-specific proteins should be used to identify asymptom-
the time of delivery for careful examination of the external genitalia atic carriers of HSV-1 or HSV-2. No reliable IgM method for defining
and cervix as well as collection of a swab sample for viral isolation. acute HSV infection is available.
Women who have no evidence of lesions can have a vaginal delivery. Several studies have shown that persons with previously unrecog-
The presence of active lesions on the cervix or external genitalia is an nized HSV-2 infection can be taught to identify symptomatic reactiva-
indication for cesarean delivery. tions. Individuals seropositive for HSV-2 should be told about the high
If first-episode exposure has occurred (e.g., if HSV serologies show frequency of subclinical reactivation on mucosal surfaces that are not
that the mother is seronegative or if the mother is HSV-1-seropositive visible to the eye (e.g., cervix, urethra, perianal skin) or in microscopic
and the isolate at delivery is found to be HSV-2), many authorities ulcerations that may not be clinically symptomatic. Transmission of
would initiate antiviral therapy for the infant with IV acyclovir. At a infection during such episodes is well established. HSV-2-seropositive
minimum, samples for viral cultures and PCR should be obtained from persons should be educated about the high likelihood of subclinical
the throat, nasopharynx, eyes, and rectum of these infants immediately shedding and the role that condoms (male or female) may play in
and at 5- to 10-day intervals. Lethargy, skin lesions, or fever should be reducing transmission. Antiviral therapy with valacyclovir (500 mg
evaluated promptly. All infants from whom HSV is isolated 24 h after once daily) has been shown to reduce the transmission of HSV-2
delivery should be treated with IV acyclovir at recommended doses. between sexual partners.
■ DIAGNOSIS
Both clinical and laboratory criteria are useful for diagnosing HSV TREATMENT
infections. A clinical diagnosis can be made accurately when charac- Herpes Simplex Virus Infections
teristic multiple vesicular lesions on an erythematous base are present.
However, herpetic ulcerations may resemble skin ulcerations of other eti- Many aspects of mucocutaneous and visceral HSV infections are
ologies. Mucosal HSV infections may also present as urethritis or phar- amenable to antiviral chemotherapy. For mucocutaneous infections,
yngitis without cutaneous lesions. Thus, laboratory studies to confirm acyclovir and its congeners famciclovir and valacyclovir have been
the diagnosis and to guide therapy are recommended. While staining of the mainstays of therapy. Several antiviral agents are available for
scrapings from the base of the lesions with Wright’s, Giemsa’s (Tzanck topical use in HSV eye infections: idoxuridine, trifluorothymidine,
preparation), or Papanicolaou’s stain to detect giant cells or intranu- topical vidarabine, and cidofovir. For HSV encephalitis and neonatal
clear inclusions of Herpesvirus infection is a well-described procedure, herpes, IV acyclovir is the treatment of choice.
few clinicians are skilled in this technique, the sensitivity of staining All licensed antiviral agents for use against HSV inhibit the
is low (<30% for mucosal swabs), and these cytologic methods do not viral DNA polymerase. One class of drugs, typified by the drug
differentiate between HSV and VZV infections. acyclovir, is made up of substrates for the HSV enzyme thymidine
HSV infection is best confirmed in the laboratory by detection of kinase (TK). Acyclovir, ganciclovir, famciclovir, and valacyclovir
virus, viral antigen, or viral DNA in scrapings from lesions. HSV DNA are all selectively phosphorylated to the monophosphate form in
detection by PCR is the most sensitive laboratory technique for detect- virus-infected cells. Cellular enzymes convert the monophosphate
ing mucosal or visceral HSV infections and is the recommended test form of the drug to the triphosphate, which is then incorporated into
for laboratory confirmation of a diagnosis. HSV causes a discernible the viral DNA chain. Acyclovir is the agent most frequently used
Harrisons_20e_Part5_p0859-p1648.indd 1351 6/1/18 12:07 PM
1352 for the treatment of HSV infections and is available in IV, oral, and infections. Anecdotal case reports suggest that ganciclovir may also
topical formulations. Valacyclovir, the valyl ester of acyclovir, offers be less effective than acyclovir for the treatment of HSV infections.
greater bioavailability than acyclovir and thus can be administered All three recommended compounds—acyclovir, valacyclovir, and
less frequently. Famciclovir, the oral formulation of penciclovir, is famciclovir—have proved effective in shortening the duration of
clinically effective in the treatment of a variety of HSV-1 and HSV-2 symptoms and lesions of mucocutaneous HSV infections in both
infections. Ganciclovir is active against both HSV-1 and HSV-2; immunocompromised and immunocompetent patients (Table 187-1).
however, it is more toxic than acyclovir, valacyclovir, and famci- IV and oral formulations prevent reactivation of HSV in seropositive
clovir and generally is not recommended for the treatment of HSV immunocompromised patients during induction chemotherapy or
TABLE 187-1 Antiviral Chemotherapy for Herpes Simplex Virus (HSV) Infection
I. Mucocutaneous HSV infections
A. Infections in immunosuppressed patients
1. Acute symptomatic first or recurrent episodes: IV acyclovir (5 mg/kg q8h) or oral acyclovir (400 mg qid), famciclovir (500 mg bid or tid), or valacyclovir
(500 mg bid) is effective. Treatment duration may vary from 7 to 14 days. IV therapy may be given for 2–7 days until clinical improvement and followed
by oral therapy.
2. Suppression of reactivation disease (genital or oral–labial): IV acyclovir (5 mg/kg q8h) or oral valacyclovir (500 mg bid) or acyclovir (400–800 mg 3–5
times per day) prevents recurrences during the 30-day period immediately after transplantation. Longer-term HSV suppression is often used for
persons with continued immunosuppression. In bone marrow and renal transplant recipients, oral valacyclovir (2 g/d) is also effective in reducing
cytomegalovirus infection. Oral valacyclovir at a dose of 4 g/d has been associated with thrombotic thrombocytopenic purpura after extended use in
HIV-positive persons. In HIV-infected persons, oral acyclovir (400–800 mg bid), valacyclovir (500 mg bid), or famciclovir (500 mg bid) is effective in
reducing clinical and subclinical reactivations of HSV-1 and HSV-2.
B. Infections in immunocompetent patients
1. Genital herpes
a. First episodes: Oral acyclovir (200 mg 5 times per day or 400 mg tid), valacyclovir (1 g bid), or famciclovir (250 mg bid) for 7–14 days is effective. IV
acyclovir (5 mg/kg q8h for 5 days) is given for severe disease or neurologic complications such as aseptic meningitis.
b. Symptomatic recurrent genital herpes: Short-course (1- to 3-day) regimens are preferred because of low cost, likelihood of adherence, and
convenience. Oral acyclovir (800 mg tid for 2 days), valacyclovir (500 mg bid for 3 days), or famciclovir (750 or 1000 mg bid for 1 day, a 1500-mg
single dose, or 500 mg stat followed by 250 mg q12h for 2 days) effectively shortens lesion duration. Other options include oral acyclovir (200 mg 5
times per day), valacyclovir (500 mg bid), and famciclovir (125 mg bid for 5 days).
PART 5
c. Suppression of recurrent genital herpes: Oral acyclovir (400–800 mg bid) or valacyclovir (500 mg daily) is given. Patients with >9 episodes per year
should take oral valacyclovir (1 g daily or 500 mg bid) or famciclovir (250 mg bid or 500 mg bid).
2. Oral–labial HSV infections
a. First episode: Oral acyclovir is given (200 mg 5 times per day or 400 mg tid); an oral acyclovir suspension can be used (600 mg/m2 qid). Oral
Infectious Diseases
famciclovir (250 mg bid) or valacyclovir (1 g bid) has been used clinically. The duration of therapy is 5–10 days.
b. Recurrent episodes: If initiated at the onset of the prodrome, single-dose or 1-day therapy effectively reduces pain and speeds healing. Regimens
include oral famciclovir (a 1500-mg single dose or 750 mg bid for 1 day) or valacyclovir (a 2-g single dose or 2 g bid for 1 day). Self-initiated therapy
with 6-times-daily topical penciclovir cream effectively speeds healing of oral–labial HSV infection. Topical acyclovir cream has also been shown to
speed healing.
c. Suppression of reactivation of oral–labial HSV: If started before exposure and continued for the duration of exposure (usually 5–10 days), oral
acyclovir (400 mg bid) prevents reactivation of recurrent oral–labial HSV infection associated with severe sun exposure.
3. Surgical prophylaxis of oral or genital HSV infection: Several surgical procedures, such as laser skin resurfacing, trigeminal nerve-root decompression,
and lumbar disk surgery, have been associated with HSV reactivation. IV acyclovir (3–5 mg/kg q8h) or oral acyclovir (800 mg bid), valacyclovir (500 mg
bid), or famciclovir (250 mg bid) effectively reduces reactivation. Therapy should be initiated 48 h before surgery and continued for 3–7 days.
4. Herpetic whitlow: Oral acyclovir (200 mg) is given 5 times daily (alternative: 400 mg tid) for 7–10 days.
5. HSV proctitis: Oral acyclovir (400 mg 5 times per day) is useful in shortening the course of infection. In immunosuppressed patients or in patients with
severe infection, IV acyclovir (5 mg/kg q8h) may be useful.
6. Herpetic eye infections: In acute keratitis, topical trifluorothymidine, vidarabine, idoxuridine, acyclovir, penciclovir, and interferon are all beneficial.
Debridement may be required. Topical steroids may worsen disease.
II. Central nervous system HSV infections
A. HSV encephalitis: IV acyclovir (10 mg/kg q8h; 30 mg/kg per day) is given for 10 days or until HSV DNA is no longer detected in cerebrospinal fluid.
B. HSV aseptic meningitis: No studies of systemic antiviral chemotherapy exist. If therapy is to be given, IV acyclovir (15–30 mg/kg per day) should be used.
C. Autonomic radiculopathy: No studies are available. Most authorities recommend a trial of IV acyclovir.
III. Neonatal HSV infections: IV acyclovir (60 mg/kg per day, divided into 3 doses) is given. The recommended duration of IV treatment is 21 days. Monitoring for
relapse should be undertaken. Continued suppression with oral acyclovir suspension should be given for 3–4 months.
IV. Visceral HSV infections
A. HSV esophagitis: IV acyclovir (15 mg/kg per day) is given. In some patients with milder forms of immunosuppression, oral therapy with valacyclovir or
famciclovir is effective.
B. HSV pneumonitis: No controlled studies exist. IV acyclovir (15 mg/kg per day) should be considered.
V. Disseminated HSV infections: No controlled studies exist. IV acyclovir (5 mg/kg q8h) should be tried. Adjustments for renal insufficiency may be needed. No
definite evidence indicates that therapy will decrease the risk of death.
VI. Erythema multiforme associated with HSV: Anecdotal observations suggest that oral acyclovir (400 mg bid or tid) or valacyclovir (500 mg bid) will suppress
erythema multiforme.
VII. Infections due to acyclovir-resistant HSV: IV foscarnet (40 mg/kg IV q8h) should be given until lesions heal. The optimal duration of therapy and the
usefulness of its continuation to suppress lesions are unclear. Some patients may benefit from cutaneous application of trifluorothymidine or 1% cidofovir gel,
both of which must be compounded at a pharmacy. These preparations should be applied once daily for 5–7 days. Topical imiquimod can be considered. The
helicase primase inhibitor pritelivir is being studied for treatment of acyclovir-resistant HSV infection. IV cidofovir (5 mg/kg weekly) may be considered.
VIII. Acyclovir and pregnancy: No adverse effects to the fetus or newborn have been attributable to acyclovir. Acyclovir can be used in all stages of pregnancy
and among women who are breastfeeding (the drug can be found in breast milk). Suppressive acyclovir treatment in late pregnancy reduces the frequency of
cesarean delivery among women with recurrent genital herpes. Such treatment may not protect against transmission to neonates.
Harrisons_20e_Part5_p0859-p1648.indd 1352 6/1/18 12:07 PM
in the period immediately after bone marrow or solid organ trans- detection of such isolates in the past 30 years probably reflects the 1353
plantation. Chronic daily suppressive therapy reduces the frequency reduced transmission of TK-deficient mutants. Isolation of HSV
of reactivation disease among patients with frequent genital or from lesions persisting despite adequate dosages and blood levels of
oral–labial herpes. Only valacyclovir has been subjected to clinical acyclovir should raise the suspicion of acyclovir resistance. Clinical
trials that demonstrated reduced transmission of HSV-2 infection management of acyclovir resistance is challenging. Therapy with
between sexual partners. IV acyclovir (30 mg/kg per day, given as a the antiviral drug foscarnet (40–80 mg/kg IV every 8 h until clinical
10-mg/kg infusion over 1 h at 8-h intervals) is effective in reducing resolution) is useful in acyclovir-resistant cases (Chap. 186). Because
rates of death and morbidity from HSV encephalitis. Early initia- of its toxicity and cost, this drug is usually reserved for patients with
tion of therapy is a critical factor in outcome. The major side effect extensive mucocutaneous infections. Cidofovir is a nucleotide ana-
associated with IV acyclovir is transient renal insufficiency, usually logue and exists as a phosphonate or monophosphate form. Most
due to crystallization of the compound in the renal parenchyma. TK-deficient strains of HSV are sensitive to cidofovir. Cidofovir
This adverse reaction can be avoided if the medication is given ointment speeds healing of acyclovir-resistant lesions. No well-
slowly over 1 h and the patient is well hydrated. Because CSF levels controlled trials of systemic cidofovir have been reported. Occa-
of acyclovir average only 30–50% of plasma levels, the dosage of sional cases may respond to topical imiquimod. True TK-negative
acyclovir used for treatment of CNS infection (30 mg/kg per day) is variants of HSV appear to have a reduced capacity to spread because
double that used for treatment of mucocutaneous or visceral disease of altered neurovirulence—a feature important in the relatively
(15 mg/kg per day). Even higher doses of IV acyclovir are used for infrequent presence of such strains in immunocompetent popula-
neonatal HSV infection (60 mg/kg per day in three divided doses). tions, even with increasing use of antiviral drugs. A new class of
Antiviral drugs neither eradicate latent infection nor affect the risk, drugs that inhibit HSV-specific helicase/primase activity (pritelivir)
frequency, or severity of subclinical or clinical recurrence after the is under clinical investigation and may offer a better toxicity profile
drug is discontinued. for the treatment of acyclovir-resistant strains of HSV.
Increasingly, shorter courses of therapy are being used for recur-
rent mucocutaneous infection with HSV-1 or HSV-2 in immunocom- ACYCLOVIR EFFICACY IN THE DEVELOPING WORLD
petent patients. One-day courses of famciclovir and valacyclovir are Initial studies of acyclovir-like drugs were performed
clinically effective, more convenient, and generally less costly than solely in the developed world. While acyclovir, valacyclo-
longer courses of therapy (Table 187-1). These short-course regimens vir, and famciclovir are effective in the developing world,
should be reserved for immunocompetent hosts. their clinical and virologic benefits, especially in reducing the fre-
quency of genital lesions among patients in Africa, seem reduced
CHAPTER 187 Herpes Simplex Virus Infections
SUPPRESSION OF MUCOCUTANEOUS HERPES from those in European and U.S. populations. The mechanism of
Recognition of the high frequency of subclinical reactivation pro- this phenomenon is uncertain. Acyclovir therapy does not reduce
vides a well-accepted rationale for the use of daily antiviral therapy the rate of HIV acquisition; however, HIV load among MSM in the
to suppress reactivations of HSV, especially in persons with fre- United States decreased by 1.3 log10 in contrast to 0.9 log10 among
quent clinical reactivations (e.g., those with recently acquired genital Peruvian MSM and 0.5 log10 among African women. Curiously, the
HSV infection). Immunosuppressed persons, including those with anti-HIV drug tenofovir reduces HSV-2 acquisition among women
HIV infection, may also benefit from daily antiviral therapy. Daily in Africa although it has no demonstrable clinical benefit or antiviral
acyclovir and valacyclovir reduce the frequency of HSV reactiva- effects among persons with established HSV-2 infection in studies in
tions among HIV-positive persons. Regimens used include acyclovir the United States. The reasons for these disparate results are unclear.
(400–800 mg twice daily), famciclovir (500 mg twice daily), and
valacyclovir (500 mg twice daily); valacyclovir at a dose of 4 g/d
was associated with thrombotic thrombocytopenic purpura in one ■ PREVENTION
study of HIV-infected persons. Daily acyclovir therapy is associated Efforts to control HSV disease on a population basis through suppres-
with a modest reduction in the titer of HIV RNA in plasma (0.5-log10 sive antiviral chemotherapy and/or educational programs have been
reduction) and in the genital mucosa (0.33-log10 reduction). limited. Barrier forms of contraception (especially condoms) decrease
the likelihood of transmission of HSV infection, particularly during
REDUCED HSV TRANSMISSION TO SEXUAL PARTNERS periods of asymptomatic viral excretion. When lesions are present,
Once-daily valacyclovir (500 mg) has been shown to reduce trans- HSV infection may be transmitted by skin-to-skin contact despite the
mission of HSV-2 between sexual partners. Transmission rates are use of a condom. Nevertheless, the available data suggest that consis-
higher from males to females and among persons with frequent tent condom use is an effective means of reducing the risk of genital
HSV-2 reactivation. Serologic screening can be used to identify HSV-2 transmission. Chronic daily antiviral therapy with valacyclovir
at-risk couples. Daily valacyclovir appears to be more effective at can also be partially effective in reducing acquisition of HSV-2, espe-
reducing subclinical shedding than daily famciclovir. cially among susceptible women. There are no comparative efficacy
studies of valacyclovir versus condom use. Most authorities suggest
ACYCLOVIR RESISTANCE both approaches. The need for a vaccine to prevent acquisition of HSV
Clinically relevant acyclovir-resistant strains of HSV do occur. Most infection is great, especially in light of the role HSV-2 plays in enhanc-
of these strains have an altered substrate specificity for phospho- ing the acquisition and transmission of HIV-1.
rylating acyclovir. Thus, cross-resistance to famciclovir and vala- A substantial portion of neonatal HSV cases could be prevented by
cyclovir is usually found. Occasionally, an isolate with altered TK reducing the acquisition of HSV by women in the third trimester of
specificity arises and is sensitive to famciclovir but not to acyclovir. pregnancy. Neonatal HSV infection can result from either the acqui-
In some patients infected with TK-deficient virus, higher doses of sition of maternal infection near term or the reactivation of infection
acyclovir are associated with clearing of lesions. In others, clinical at delivery in the already-infected mother. Women without known
disease progresses despite high-dose therapy. Almost all clinically genital herpes should be counseled to abstain from vaginal intercourse
significant acyclovir resistance has been seen in immunocompro- during the third trimester with partners known to have or suspected of
mised patients, and HSV-2 isolates are more often resistant than having genital herpes. Some authorities have recommended that anti-
HSV-1 strains. A study by the Centers for Disease Control and viral therapy with acyclovir or valacyclovir be given to HSV-2-infected
Prevention indicated that ~5% of HSV-2 isolates from HIV-positive women in late pregnancy as a means of reducing reactivation of HSV-2
persons exhibit some degree of in vitro resistance to acyclovir. Of at term. Data are not available to support the efficacy of this approach,
HSV-2 isolates from immunocompetent patients attending sexually and the high treatment-to-prevention ratio makes this a difficult if not
transmitted disease clinics, <0.5% show reduced in vitro sensitivity dubious public health strategy, even though it can reduce the frequency
to acyclovir. The lack of appreciable change in the frequency of of HSV-associated cesarean delivery.
Harrisons_20e_Part5_p0859-p1648.indd 1353 6/1/18 12:07 PM
2044 must understand the receptor selectivity of various agents and that for stress dose steroids. Cardiogenic shock patients with arrhythmia
some agents the selectivity may be dose-dependent. In patients with may require treatment as outlined in advanced cardiac life support
distributive shock, the aim is to increase the SVR. Norepinephrine is algorithms or placement of an artificial pacemaker. In cases of acute
the first choice vasopressor: with potent α1 and β1 adrenergic effects. ischemic events, consideration must be given to revascularization
The α1 causes vasoconstriction while β1 has positive inotropic and and temporary mechanical supportive measures. In the case of valve
chronotropic effects. At high doses, epinephrine has a similar profile dysfunction, emergency surgery may be considered. Patients with
(at lower doses the β effects predominate), but is associated with tach- hypovolemic shock due to hemorrhage may require surgical interven-
yarrhythmia, myocardial ischemia, decreased splanchnic blood flow, tion in the case of trauma or endoscopic or interventional radiology
pulmonary hypertension, and acidosis. In distributive shock, vaso- procedures in the case of a GI source of blood loss. Among patients
pressin deficiency may be present. Vasopressin acts on the vasopressin with obstructive shock, a tension PTX would necessitate immediate
receptor to reverse vasodilation and redistribute flow to the splanchnic decompression. Proximal pulmonary embolism requires evaluation for
circulation. In a randomized trial in patients with septic shock, the thrombolytic therapy or surgical removal of the clot. Dissection of the
addition of low-dose vasopressin did not reduce all-cause 28-day ascending aorta may require surgical intervention.
mortality compared to norepinephrine. Vasopressin is safe and has a
role as a second agent for hypotension in septic shock. Dopamine does ■ FURTHER READING
not have a role as a first line agent in distributive shock. A random- Mebazaa A et al: Acute heart failure and cardiogenic shock: A multidis-
ized control study in patients with all cause circulatory shock did not ciplinary practical guidance. Intensive Care Med 42:147, 2016.
show a survival benefit, but did reveal an increase in adverse events Monnet X et al: Passive leg raising for predicting fluid responsiveness:
PART 8
(arrhythmia). In this study, the subgroup of patients with cardiogenic A systematic review and meta-analysis. Intensive Care Med 42:1935,
shock had increased mortality. For patients with cardiogenic shock, 2016.
dobutamine is the first line agent; it is a synthetic catecholamine with Pro CI et al: A randomized trial of protocol-based care for early septic
primarily β-mediated effects and minimal α adrenergic effects. The β1 shock. N Engl J Med 370:1683, 2014.
Critical Care Medicine
effect is manifest in increased inotropy and the β2 effect leads to vaso- Rhodes A et al: Surviving sepsis campaign: International guidelines
dilation with decreased afterload; it can be used with norepinephrine in for management of sepsis and septic shock: 2016. Intensive Care Med
patients with mixed distributive and cardiogenic shock. 43:304, 2017.
Vincent JL, De Backer D: Circulatory shock. N Engl J Med 369:1726,
■ OXYGENATION AND VENTILATION SUPPORT 2013.
In addition to the cellular hypoxia caused by the circulatory failure, Vincent JL et al: The value of blood lactate kinetics in critically ill
patients with shock may present with hypoxemia. For patients with patients: A systematic review. Crit Care 20:257, 2016.
distributive shock, this may be related to a primary pulmonary pro-
cess (pneumonia in a patient with septic shock). For patients with
cardiogenic or obstructive shock, the hypoxemia may be related to LV
297 Sepsis and Septic Shock
dysfunction and elevations of PCWP. For patients with all .types . of
shock, there can be development of ARDS and subsequent V/Q mis-
match and shunt. Supplemental oxygen should be initiated and titrated
to maintain SpO2 of 92–95%. This may require intubation and initiation Christopher W. Seymour, Derek C. Angus
of mechanical ventilation. If the patient requires intubation and initia-
tion of mechanical ventilation, this should be provided promptly so as
to minimize the duration of tissue hypoxia. Patients with shock may ■ INTRODUCTION AND DEFINITIONS
have high minute ventilatory needs to compensate for metabolic aci- Sepsis is a common and deadly disease. More than two millennia ago,
dosis. As shock progresses, they may not be able to maintain adequate Hippocrates wrote that sepsis was characterized by rotting flesh and
respiratory compensation, which may be a second indication to initiate festering wounds. Several centuries later, Galen described sepsis as
mechanical ventilator support. If mechanical support is initiated, it a laudable event required for wound healing. Once the germ theory
is important to provide ventilation with lung-protective strategies was proposed by Semmelweis, Pasteur, and others in the nineteenth
focused on low tidal volume ventilation and optimization of positive century, sepsis was recast as a systemic infection referred to as “blood
end-expiratory pressure to minimize ventilator-induced lung injury. In poisoning” and was thought to be due to pathogen invasion and
addition, there should be daily sedation cessation to assess underlying spread in the bloodstream of the host. However, germ theory did
neurologic function and minimize time on mechanical ventilation. not fully explain sepsis: many septic patients died despite successful
There are currently little data to support the use of noninvasive venti- removal of the inciting pathogen. In 1992, Bone and colleagues pro-
lation in the setting of shock. posed that the host, not the germ, was responsible for the pathogenesis
of sepsis. Specifically, they defined sepsis as a systemic inflammatory
Antibiotic Administration Sepsis and septic shock are the most
response to infection. Yet sepsis arose in response to many different
common cause of shock. For patients presenting with undifferentiated
pathogens, and septicemia was neither a necessary condition nor a
shock, if the diagnosis of septic shock is being entertained then broad
helpful term. Thus, these investigators instead proposed the term severe
spectrum antibiotics should be administered after obtaining appropri-
sepsis to describe cases where sepsis was complicated by acute organ
ate cultures. For patients with sepsis, every hour delay in antibiotic
dysfunction and the term septic shock for a subset of sepsis cases that
administration is associated with an increase in mortality. While it is
were complicated by hypotension despite adequate fluid resuscitation
ideal to initiate antibiotics after appropriate cultures, the inability to
along with perfusion abnormalities.
obtain cultures should not delay the start of treatment. When sepsis is
In the past 20 years, research has revealed that many patients develop
excluded as a cause of shock, an important aspect of antibiotic steward-
acute organ dysfunction in response to infection but without a mea-
ship is to stop all antibiotics.
surable inflammatory excess (i.e., without the systemic inflammatory
Specific Causes of Shock Requiring Tailored Intervention response syndrome [SIRS]). In fact, both pro- and anti-inflammatory
The initial evaluation (history, physical examination, and diagnostic responses are present along with significant changes in other path-
testing) may have identified an etiology of shock that requires urgent ways. To clarify terminology and reflect the current understanding of
lifesaving intervention in addition to the initial treatment steps out- the pathobiology of sepsis, the Sepsis Definitions Task Force in 2016
lined above. Patients with distributive shock secondary to anaphylaxis proposed the Third International Consensus Definitions specifying that
require removal of the inciting allergen, administration of epinephrine, sepsis is a dysregulated host response to infection that leads to acute
and vascular support with intravenous fluid resuscitation and vaso- organ dysfunction. This definition distinguishes sepsis from uncompli-
pressors. Adrenal insufficiency requires replacement with intravenous cated infection that does not lead to organ dysfunction, a poor course,
Harrisons_20e_Part8_p2023-p2088.indd 2044 5/30/18 2:23 PM
TABLE 297-1 Definitions and Criteria for Sepsis and Septic Shock 2045
COMMON CLINICAL CRITERIA IN 1991/2003
CONDITION DEFINITION FEATURES (“SEPSIS-1”/”SEPSIS-2”) CRITERIA IN 2016 (“SEPSIS-3”)
Sepsis A life-threatening organ Include signs of infection, Suspected (or documented) infection Suspected (or documented)
dysfunction caused by a with organ dysfunction, plus plus ≥2 systemic inflammatory infection and an acute increase
dysregulated host response to altered mentation; tachypnea; response syndrome (SIRS) criteriaa in ≥2 sepsis-related organ failure
infection hypotension; hepatic, renal, or assessment (SOFA) pointsb
hematologic dysfunction
Septic shock A subset of sepsis in Signs of infection, plus altered Suspected (or documented) infection Suspected (or documented)
which underlying circulatory mentation, oliguria, cool plus persistent arterial hypotension infection plus vasopressor therapy
and cellular/metabolic peripheries, hyperlactemia (systolic arterial pressure, <90 mmHg; needed to maintain mean arterial
abnormalities lead to mean arterial pressure, <60 mmHg; or pressure at ≥65 mmHg and serum
substantially increased change in systolic by >40 mmHg from lactate >2.0 mmol/L despite
mortality risk baseline adequate fluid resuscitation
a
SIRS criteria include 1 point for each of the following (score range, 0–4): fever >38°C (>100.4°F) or <36°C (<96.8°F); tachypnea with >20 breaths per min; tachycardia
with heart rate >90 beats per min; leukocytosis with white blood cell count >12,000/μL; leukopenia (<4000/μL) or >10% bands. bSOFA score is a 24-point measure of
organ dysfunction that uses six organ systems (renal, cardiovascular, pulmonary, hepatic, neurologic, hematologic), where 0–4 points are assigned per organ system.
CHAPTER 297 Sepsis and Septic Shock
or death. In light of the wide variation in the ways that septic shock is provision of supportive therapy, in which case epidemiologic studies
identified in research, clinical, or surveillance settings, the Third Inter- count the “treated,” rather than the actual, incidence. In the United
national Consensus Definitions further specified that septic shock be States, recent cohort studies using administrative data suggest that
defined as a subset of sepsis cases in which underlying circulatory and upwards of 2 million cases of sepsis occur annually. Shock is present in
cellular/metabolic abnormalities are profound enough to substantially ~30% of cases, resulting in an estimated 230,000 cases in a recent sys-
increase mortality risk. tematic review. An analysis of data (both clinical and administrative)
To aid clinicians in identifying sepsis and septic shock at the from 300 hospitals in the United Healthcare Consortium estimated
bedside, new “Sepsis-3” clinical criteria for sepsis include (1) a sus- that septic shock occurred in 19 per 1000 hospitalized encounters. The
pected infection and (2) acute organ dysfunction, defined as an increase incidences of sepsis and septic shock are also reported to be increasing
by two or more points from baseline (if known) on the sequential (or (according to ICD9-CM diagnosis and procedure codes), with a rise of
sepsis-related) organ failure assessment (SOFA) score (Table 297-1). almost 50% in the past decade. However, the stability of objective clin-
Criteria for septic shock include sepsis plus the need for vasopressor ical markers (e.g., provision of organ support, detection of bacteremia)
therapy to elevate mean arterial pressure to ≥65 mmHg with a serum over this period in a two-center validation study suggests that new
lactate concentration >2.0 mmol/L despite adequate fluid resuscitation. ICD-9 coding rules, confusion over semantics (e.g., septicemia versus
severe sepsis), rising capacity to provide intensive care, and increased
■ ETIOLOGY case-finding confound the interpretation of serial trends. Studies from
Sepsis can arise from both community-acquired and hospital-acquired other high-income countries report rates of sepsis in the ICU similar to
infections. Of these infections, pneumonia is the most common source, those in the United States.
accounting for about half of cases; next most common are intraabdom- While the data demonstrate that sepsis is a significant
inal and genitourinary infections. Blood cultures are typically positive public-health burden in high-income countries, its impact on
in only one-third of cases, while many cases are culture negative at all the populations of low- and middle-income countries is prob-
sites. Staphylococcus aureus and Streptococcus pneumoniae are the most ably even more substantial because of the increased incidence of infec-
common gram-positive isolates, while Escherichia coli, Klebsiella species, tious diseases and the high prevalence of HIV in some parts of the
and Pseudomonas aeruginosa are the most common gram-negative iso- developing world. Although there are fewer high-quality studies on
lates. In recent years, gram-positive infections have been reported more sepsis in these countries, the available data support sepsis as a major
often than gram-negative infections, yet a 75-country point-prevalence public-health problem. For example, a study of one cohort in rural
study of 14,000 patients on intensive care units (ICUs) found that 62% Uganda found an incidence of laboratory-confirmed sepsis tenfold that
of positive isolates were gram-negative bacteria, 47% were gram- of current global sepsis estimates; as only a minority of patients with
positive bacteria, and 19% were fungi. sepsis develop bacteremia, the incidence of sepsis in the cohort was
The many risk factors for sepsis are related to both the predisposition probably even higher. Case–fatality rates in low- and middle-income
to develop an infection and, once infection develops, the likelihood countries are also higher than those in high-income countries, as exem-
of developing acute organ dysfunction. Common risk factors for plified by two observational cohorts in Brazil with mortality rates >40%.
increased risk of infection include chronic diseases (e.g., HIV infection,
chronic obstructive pulmonary disease, cancers) and immunosuppres- ■ PATHOGENESIS
sion. Risk factors for progression from infection to organ dysfunction For many years, the clinical features of sepsis were considered the
are less well understood but may include underlying health status, result of an excessive inflammatory host response (SIRS). More
preexisting organ function, and timeliness of treatment. Age, sex, and recently, it has become apparent that infection triggers a much more
race/ethnicity all influence the incidence of sepsis, which is highest complex, variable, and prolonged host response than was previously
at the extremes of age, higher in males than in females, and higher in thought. The specific response of each patient depends on the pathogen
blacks than in whites. The differences in risk of sepsis by race are not (load and virulence) and the host (genetic composition and comor-
fully explained by socioeconomic factors or access to care, raising the bidity), with different responses at local and systemic levels. The host
possibility that other factors, such as genetic differences in suscepti- response evolves over time with the patient’s clinical course. Generally,
bility to infection or in the expression of proteins critical to the host proinflammatory reactions (directed at eliminating pathogens) are
response, may play a role. responsible for “collateral” tissue damage in sepsis, whereas anti-
inflammatory responses are implicated in the enhanced susceptibility
■ EPIDEMIOLOGY to secondary infections that occurs later in the course. These mecha-
The incidences of sepsis and septic shock depend on how acute organ nisms can be characterized as an interplay between two “fitness costs”:
dysfunction and infection are defined as well as on which data sources direct damage to organs by the pathogen and damage to organs stem-
are studied. Disparate estimates come from administrative data, pro- ming from the host’s immune response. The host’s ability to resist as
spective cohorts with manual case identification, and large electronic well as tolerate both direct and immunopathologic damage will deter-
health-record databases. Organ dysfunction is often defined by the mine whether uncomplicated infection becomes sepsis.
Harrisons_20e_Part8_p2023-p2088.indd 2045 5/30/18 2:23 PM
2046
Electron transport chain activity
CELL
Increased ATP
O2 diffusion Lactate/H+
distance
Activated Mitochondrial
leukocyte Tissue edema dysfunction DO2 Tissue
oxygenation
INTERSTITIUM
Endothelial
leak/dysfunction Barrier function
Cytokines DO2
Inflammation Thrombus/
Platelets
DAMPs
MICROCIRCULATION
PART 8
Antithrombin
Tissue Tissue factor
Protein C
Inflammatory damage pathway inhibitor
Activated Lactate/H+
mediators Tissue factor Altered
protein C Hypotension
Fibrinolysis Hypovolemia microvascular
Critical Care Medicine
PAMPs Vasodilation flow
TLR,
NLR, or
CLR
Adhesion
Transmigration
Innate immune Pathogens Activated endothelium
cells ICAM, VCAM-1 expression
FIGURE 297-1 Select mechanisms implicated in the pathogenesis of sepsis-induced organ and cellular dysfunction. The host response to sepsis involves multiple
mechanisms that lead to decreased oxygen delivery (DO2) at the tissue level. The duration, extent, and direction of these interactions are modified by the organ under
threat, host factors (e.g., age, genetic characteristics, medications), and pathogen factors (e.g., microbial load and virulence). The inflammatory response is typically
initiated by an interaction between pathogen-associated molecular patterns (PAMPs) expressed by pathogens and pattern recognition receptors expressed by innate
immune cells on the cell surface (Toll-like receptors [TLRs] and C-type lectin receptors [CLRs]), in the endosome (TLRs), or in the cytoplasm (retinoic acid inducible gene
1–like receptors and nucleotide-binding oligomerization domain–like receptors [NLRs]). The resulting tissue damage and necrotic cell death lead to release of damage-
associated molecular patterns (DAMPs) such as uric acid, high-mobility group protein B1, S100 proteins, and extracellular RNA, DNA, and histones. These molecules
promote the activation of leukocytes, leading to greater endothelial dysfunction, expression of intercellular adhesion molecule (ICAM) and vascular cell adhesion
molecule 1 (VCAM-1) on the activated endothelium, coagulation activation, and complement activation. This cascade is compounded by macrovascular changes such
as vasodilation and hypotension, which are exacerbated by greater endothelial leak tissue edema, and relative intravascular hypovolemia. Subsequent alterations
in cellular bioenergetics lead to greater glycolysis (e.g., lactate production), mitochondrial injury, release of reactive oxygen species, and greater organ dysfunction.
Initiation of Inflammation Over the past decade, our knowl- intravascular coagulation. Abnormalities in coagulation are thought
edge of pathogen recognition has increased tremendously. Pathogens to isolate invading microorganisms and/or to prevent the spread of
activate immune cells by an interaction with pattern recognition infection and inflammation to other tissues and organs. Excess fibrin
receptors (Fig. 297-1), of which four main classes are prominent: Toll- deposition is driven by coagulation via tissue factor, a transmembrane
like receptors (TLRs), RIG-I-like receptors, C-type lectin receptors, and glycoprotein expressed by various cell types; by impaired anticoagu-
NOD-like receptors; the activity of the last group occurs partially in lant mechanisms, including the protein C system and antithrombin;
protein complexes called inflammasomes. The recognition of structures and by compromised fibrin removal due to depression of the fibrino-
conserved across microbial species—so-called pathogen-associated lytic system. Coagulation (and other) proteases further enhance inflam-
molecular patterns (PAMPs)—by all these receptors results in upreg- mation via protease-activated receptors. In infections with endothelial
ulation of inflammatory gene transcription and initiation of innate predominance (e.g., meningococcemia), these mechanisms can be com-
immunity. A common PAMP is the lipid A moiety of lipopolysaccha- mon and deadly.
ride (LPS or endotoxin), which attaches to the LPS-binding protein on
the surface of monocytes, macrophages, and neutrophils. LPS is trans-
Organ Dysfunction Although the mechanisms that underlie
organ failure in sepsis are only partially known, impaired tissue oxy-
ferred to and signals via TLR4 to produce and release cytokines such
genation plays a key role. Several factors contribute to reduced oxygen
as tumor necrosis factor that grow the signal and alert other cells and
delivery in sepsis and septic shock, including hypotension, reduced
tissues. Up to 10 TLRs have been identified in humans.
red-cell deformability, and microvascular thrombosis. Inflammation
At the same time, these receptors also sense endogenous molecules
can cause dysfunction of the vascular endothelium, accompanied by
released from injured cells—so-called damage-associated molecular
cell death and loss of barrier integrity, giving rise to subcutaneous and
patterns (DAMPs), such as high-mobility group protein B1, S100 pro-
body-cavity edema. An excessive and uncontrolled release of nitric
teins, and extracellular RNA, DNA, and histones. The release of DAMPs
oxide causes vasomotor collapse, opening of arteriovenous shunts,
during sterile injuries such as those incurred during trauma gives rise to
and pathologic shunting of oxygenated blood from susceptible tissues.
the concept that the pathogenesis of multiple-organ failure may be sim-
In addition, mitochondrial damage due to oxidative stress and other
ilar in sepsis and noninfectious critical illness. In addition to activating
mechanisms impairs cellular oxygen utilization. The slowing of oxi-
the proinflammatory cytokines, the inflammatory responses implicated
dative metabolism, in parallel with impaired oxygen delivery, reduces
in the pathogenesis of sepsis also activate the complement system,
cellular O2 extraction. Yet energy (i.e., ATP) is still needed to support
platelet-activating factor, arachidonic acid metabolites, and nitric oxide.
basal, vital cellular function, which derives from glycolysis and fer-
Coagulation Abnormalities Sepsis is commonly associated mentation and thus yields H+ and lactate. With severe or prolonged
with coagulation disorders and frequently leads to disseminated insult, ATP levels fall beneath a critical threshold, bioenergetic failure
Harrisons_20e_Part8_p2023-p2088.indd 2046 5/30/18 2:23 PM
ensues, toxic reactive oxygen species are released, and apoptosis leads 2047
emergency. The general manifestations of shock include arterial
to irreversible cell death and organ failure. The actual morphologic hypotension with evidence of tissue hypoperfusion (e.g., oliguria,
changes in sepsis-induced organ failure are also complex. Generally, altered mental status, poor peripheral perfusion, or hyperlactemia).
organs such as the lung undergo extensive microscopic changes, while
other organs may undergo rather few histologic changes. In fact, some
organs (e.g., the kidney) may lack significant structural damage while ■ CLINICAL MANIFESTATIONS
still having significant tubular-cell changes that impair function. The specific clinical manifestations of sepsis are quite variable, depend-
ing on the initial site of infection, the offending pathogen, the pattern
Anti-Inflammatory Mechanisms The immune system harbors of acute organ dysfunction, the underlying health of the patient, and
humoral, cellular, and neural mechanisms that may exacerbate the the delay before initiation of treatment. The signs of both infection and
potentially harmful effects of the proinflammatory response. Phago- organ dysfunction may be subtle. Guidelines provide a long list of
cytes can switch to an anti-inflammatory phenotype that promotes potential warning signs of incipient sepsis (Table 297-1). Once sepsis
tissue repair, while regulatory T cells and myeloid-derived suppressor has been established and the inciting infection is assumed to be under
cells further reduce inflammation. The so-called neuroinflammatory control, the temperature and white blood cell (WBC) count often return
reflex may also contribute: sensory input is relayed through the affer- to normal. However, organ dysfunction typically persists.
ent vagus nerve to the brainstem, from which the efferent vagus nerve
activates the splenic nerve in the celiac plexus, with consequent norepi- Cardiorespiratory Failure Two of the most commonly affected
CHAPTER 297 Sepsis and Septic Shock
nephrine release in the spleen and acetylcholine secretion by a subset of organ systems in sepsis are the respiratory and cardiovascular systems.
CD4+ T cells. The acetylcholine release targets α7 cholinergic receptors Respiratory compromise classically manifests as acute respiratory distress
on macrophages, reducing proinflammatory cytokine release. Disrup- syndrome (ARDS), defined as hypoxemia and bilateral infiltrates of non-
tion of this neural-based system by vagotomy renders animals more cardiac origin that arise within 7 days of the suspected infection. ARDS
vulnerable to endotoxin shock, while stimulation of the efferent vagus can be classified by Berlin criteria as mild (PaO2/FiO2, 201–300 mmHg),
nerve or α7 cholinergic receptors attenuates systemic inflammation in moderate (101–200 mmHg), or severe (≤100 mmHg). A common com-
experimental sepsis. peting diagnosis is hydrostatic edema secondary to cardiac failure or
volume overload. Although traditionally identified by elevated pulmo-
Immune Suppression Patients who survive early sepsis but nary capillary wedge measurements from a pulmonary artery catheter
remain dependent on intensive care occasionally demonstrate evidence (>18 mmHg), cardiac failure can be objectively evaluated on the basis
of a suppressed immune system. These patients may have ongoing of clinical judgment or focused echocardiography.
infectious foci despite antimicrobial therapy or may experience the Cardiovascular compromise typically presents as hypotension. The
reactivation of latent viruses. Multiple investigations have documented cause can be frank hypovolemia, maldistribution of blood flow and
reduced responsiveness of blood leukocytes to pathogens in patients intravascular volume due to diffuse capillary leakage, reduced sys-
with sepsis; these findings were recently corroborated by post-mortem temic vascular resistance, or depressed myocardial function. After ade-
studies revealing strong functional impairments of splenocytes har- quate volume expansion, hypotension frequently persists, requiring
vested from ICU patients who died of sepsis. Immune suppression was the use of vasopressors. In early shock, when volume status is reduced,
evident in the lungs as well as the spleen; in both organs, the expression systemic vascular resistance may be quite high with low cardiac out-
of ligands for T cell–inhibitory receptors on parenchymal cells was put; after volume repletion, however, this picture may rapidly change
increased. Enhanced apoptotic cell death, especially of B cells, CD4+ to low systemic vascular resistance and high cardiac output.
T cells, and follicular dendritic cells, has been implicated in sepsis-
associated immune suppression and death. In a cohort of >1000 ICU Kidney Injury Acute kidney injury (AKI) is documented in >50%
admissions for sepsis, secondary infections developed in 14% of of septic patients, increasing the risk of in-hospital death by six- to
patients, and the associated genomic response at the time of infection eightfold. AKI manifests as oliguria, azotemia, and rising serum crea-
was consistent with immune suppression, including impaired glycolysis tinine levels and frequently requires dialysis. The mechanisms of sepsis-
and cellular gluconeogenesis. The most common secondary infections induced AKI are incompletely understood. AKI may occur in up to 25%
included catheter-related bloodstream infections, ventilator-associated of patients in the absence of overt hypotension. Current mechanistic
infections, and abdominal infections. What is not yet understood is the work suggests that a combination of diffuse microcirculatory blood-
optimal way to identify those sepsis patients who have hyperinflamed flow abnormalities, inflammation, and cellular bioenergetic responses
rather than immunosuppressed phenotypes. Similarly, it is unknown to injury contribute to sepsis-induced AKI beyond just organ ischemia.
whether the dysfunctional immune system is driving organ dysfunc- Neurologic Complications Typical central nervous system dys-
tion and secondary infections or whether the immune system itself is function presents as coma or delirium. Imaging studies typically show
just another dysfunctional organ. no focal lesions, and electroencephalographic findings are usually
consistent with nonfocal encephalopathy. Sepsis-associated delirium is
APPROACH TO THE PATIENT considered a diffuse cerebral dysfunction caused by the inflammatory
Sepsis and Septic Shock response to infection without evidence of a primary central nervous
system infection. Consensus guidelines recommend delirium screening
At the bedside, a clinician begins by asking, “Is this patient septic?” with valid and reliable tools such as the Confusion Assessment Method
Consensus criteria for sepsis and septic shock agree on core diagnostic for the Intensive Care Unit (CAM-ICU) and the Intensive Care Delir-
elements, including suspected or documented infection accompa- ium Screening Checklist (ICDSC). Critical-illness polyneuropathy and
nied by acute, life-threatening organ dysfunction. If infection is myopathy are also common, especially in patients with a prolonged
documented, the clinician must determine the inciting cause and course. For survivors of sepsis, neurologic complications can be severe.
the severity of organ dysfunction, usually by asking: “What just In a national (U.S.) representative prospective cohort of >1000 elderly
happened?” Severe infection can be evident, but it is often quite patients with severe sepsis, moderate to severe cognitive impairment
difficult to recognize. Many infection-specific biomarkers and increased by 10.6 percentage points among patients who survived
molecular diagnostics are under study to help discriminate sterile severe sepsis (odds ratio, 3.34; 95% confidence interval [CI], 1.53–7.25)
inflammation from infection, but these tools are not commonly used. over that among survivors of nonsepsis hospitalizations. Many of these
The clinician’s acumen is still crucial to the diagnosis of infection. limitations persisted for up to 8 years.
Next, the primary physiologic manifestations of organ dysfunction
can be assessed quickly at the bedside with a six-organ framework,
Additional Manifestations Many other abnormalities occur in
sepsis, including ileus, elevated aminotransferase levels, altered glyce-
yielding the SOFA score. Particular focus should then be placed
mic control, thrombocytopenia and disseminated intravascular coag-
on the presence or absence of shock, which constitutes a clinical
ulation, adrenal dysfunction, and sick euthyroid syndrome. Adrenal
Harrisons_20e_Part8_p2023-p2088.indd 2047 5/30/18 2:23 PM
2048 dysfunction in sepsis is widely studied and is Variable Threshold Units
thought to be related more to reversible dys- Heart rate >90 BPM
function of the hypothalamic–pituitary axis or
tissue glucocorticoid resistance than to direct Respiratory rate >20 BPM
damage to the adrenal gland. The diagnosis Temperature <36 C
is difficult to establish. Recent clinical prac- SIRS
White blood cell count >12 k/uL
tice guidelines do not recommend use of the variables
adrenocorticotropic hormone stimulation test Temperature >38 C
or determination of the plasma cortisol level White blood cell count <4 k/uL
to detect relative glucocorticoid insufficiency.
Bands >10 %
■ DIAGNOSIS
Systolic blood pressure ≤100 mmHg
Laboratory and Physiologic Findings
Serum creatinine ≥1.2 mmHg
A variety of laboratory and physiologic changes
are found in patients with suspected infection PaO2/FiO2 ratio ≤300
who are at risk for sepsis. In a 12-hospital cohort Platelets ≤150 k/uL
of electronic health records related to >70,000 SOFA
PART 8
encounters (Fig. 297-2), only tachycardia (heart variables Glasgow coma scale <15
rate, >90 beats per min) was present in >50% of Bilirubin ≥1.2 mg/dL
encounters; the most common accompanying
Mechanical ventilation Present/absent
abnormalities were tachypnea (respiratory rate,
Critical Care Medicine
>20 breaths per min), hypotension (systolic Vasopressors Present/absent
blood pressure, ≤100 mmHg), and hypoxia Vasopressors More than one
(SaO2, ≤90%). Leukocytosis (WBC count,
>12,000/μL) was present in fewer than one- FIGURE 297-2 Distribution of SIRS and SOFA variables among infected patients at risk for sepsis, as
documented in the electronic health record. Dark green bars represent the proportion of such patients
third of patients and leukopenia (WBC count, with abnormal findings; light green bars, the proportion with normal findings; and white bars, the proportion
<4000/μL) in fewer than 5%. Notably, many with missing data. (Adapted from CW Seymour et al: Assessment of clinical criteria for sepsis: For the Third
features that may identify acute organ dys- International Consensus Definitions for Sepsis and Septic Shock [Sepsis-3]. JAMA 315:762, 2016.)
function, such as platelet count, total bilirubin,
or serum lactate level, are measured in only a
small minority of at-risk encounters. If measured, metabolic acidosis similar to that of more complicated measures of organ dysfunction.
with anion gap may be detected, as respiratory muscle fatigue occurs The qSOFA score is undergoing broader evaluation in other cohorts, in
in sepsis-associated respiratory failure. Other, less common findings low-and middle-income settings, and in algorithms linked to clinical
include serum hypoalbuminemia, troponin elevation, hypoglycemia, decision-making. Recent work has also shown that, although SIRS
and hypofibrinogenemia. criteria may be fulfilled in sepsis, they sometimes are not and do not
meaningfully contribute to the identification of patients with suspected
Diagnostic Criteria There is no specific test for sepsis, nor is there infection who are at greater risk of a poor course, ICU admission, or
a gold-standard method for determining whether a patient is septic. In death—outcomes more common among patients with sepsis than
fact, the definition of sepsis can be written as a logic statement: among those without.
As stated above, recent definitions have specified that septic shock
sepsis = f (threat to life | organ dysfunction | dysregulated host response | infection),
is a subset of sepsis in which circulatory and cellular/metabolic abnor-
where sepsis is the dependent variable, which in turn is a function of malities are profound enough to substantially increase mortality risk,
four independent variables linked in a causal pathway, with—from left but the application of this definition as a criterion for enrollment of
to right—one conditional upon the other. There may be uncertainty patients varies significantly in clinical trials, observational studies, and
about whether each variable exists, whether it can be measured, and quality improvement work. For clarity, criteria are proposed for septic
whether the causal and conditional relationships hold. If we assume shock that include (1) sepsis plus (2) the need for vasopressor therapy
that organ dysfunction exists and can be measured, then attributing the to elevate mean arterial pressure to ≥65 mmHg, with (3) a serum lactate
marginal degradation in function to a dysregulated host response is not concentration >2.0 mmol/L after adequate fluid resuscitation.
simple and requires the ability to determine preexisting dysfunction, The new definitions and diagnostic criteria were externally vali-
other noninfectious contributions to organ dysfunction, and—ideally— dated in >1 million encounters stored in electronic health records. Nev-
the mechanism by which the host response to an infection causes organ ertheless, given the uncertainty around the diagnosis of sepsis, Sepsis-3
dysfunction. is undergoing both validation in prospective studies and incorporation
In order to sort through these complex details, clinicians need simple into clinical practice and quality improvement initiatives.
bedside criteria to operationalize the logic statement (Fig. 297-3). With Arterial lactate is a long-studied marker of tissue hypoperfusion,
this mandate, the Sepsis Definitions Task Force recommended that, once and hyperlactemia and delayed lactate clearance are associated with
infection is suspected, clinicians consider whether it has caused organ a greater incidence of organ failure and death in sepsis. In a study of
dysfunction by determining a SOFA score. The SOFA score ranges from >1200 patients with suspected infection, 262 (24%) of 1081 patients
0 to 24 points, with up to 4 points accrued across six organ systems. The exhibited an elevated lactate concentration (≥2.5 mmol/L) even in
SOFA score is widely studied in the ICU among patients with infection, the setting of normal systolic blood pressure (>90 mmHg) and were
sepsis, and shock. With ≥2 new SOFA points, the infected patient is con- at elevated risk of 28-day in-hospital mortality. However, lactic aci-
sidered septic and may be at ≥10% risk of in-hospital death. dosis may occur in the presence of alcohol intoxication, liver disease,
Because the SOFA score requires multiple laboratory tests and may diabetes mellitus, administration of total parenteral nutrition, or
be costly to measure repeatedly, the quick SOFA (qSOFA) score was pro- antiretroviral treatment, among other conditions. Furthermore, in
posed as a clinical prompt to identify patients at high risk of sepsis outside sepsis, an elevated lactate concentration may simply be the manifes-
the ICU, whether on the medical ward or in the emergency department. tation of impaired clearance. These factors may confound the use of
The qSOFA score ranges from 0 to 3 points, with 1 point each for systolic lactate as a stand-alone biomarker for the diagnosis of sepsis; thus it
hypotension (≤100 mmHg), tachypnea (≥22 breaths/min), or altered should be used in the context of other markers of infection and organ
mentation. A qSOFA score of ≥2 points has a predictive value for sepsis dysfunction.
Harrisons_20e_Part8_p2023-p2088.indd 2048 5/30/18 2:23 PM
Health Health 2049
Uncomplicated Uncomplicated
infection Organ infection
Organ
dysfunction
dysfunction
Sepsis Sepsis
CHAPTER 297 Sepsis and Septic Shock
FIGURE 297-3 Schematic of the importance of accurate, easy-to-use criteria for sepsis and its components, infection and organ dysfunction. In the ideal case (left),
criteria clearly distinguish sepsis patients from other patients with uncomplicated infection or organ dysfunction. The reality (right), however, is that existing criteria
fail to make clear distinctions, leaving a significant proportion of patients in areas of uncertainty. (Adapted from DC Angus et al: A framework for the development and
interpretation of different sepsis definitions and clinical criteria. Crit Care Med 44:e113, 2016.)
uncontrolled infection. Early resuscitation requires a structured
TREATMENT
approach including the administration of IV fluids and vasopres-
Sepsis and Septic Shock sors, with oxygen therapy and mechanical ventilation to support
injured organs. The exact components required to optimize resus-
EARLY TREATMENT OF SEPSIS AND SEPTIC SHOCK citation, such as choice and amount of fluid, appropriate type and
Recommendations for sepsis care begin with prompt diagnosis. Rec- intensity of hemodynamic monitoring, and role of adjunctive vaso-
ognition of septic shock by a clinician constitutes an emergency in active agents, all remain controversial, even after the completion and
which immediate treatment can be life-saving. Up-to-date guidelines reporting of recent large randomized trials.
for treatment are derived from international clinical practice guide- Evidence from an older study suggests that protocol-based, early
lines provided by the Surviving Sepsis Campaign. This consortium of goal-directed therapy (EGDT) may confer a greater survival advan-
critical care, infectious disease, and emergency medicine professional tage than clinical assessments of organ perfusion and management
societies has issued three iterations of clinical guidelines for the without a protocol. EGDT included an aggressive resuscitation pro-
management of patients with sepsis and septic shock (Table 297-2). tocol with specific hemodynamic thresholds for fluid administration,
The initial management of infection requires several steps: form- blood transfusion, and use of ionotropes. Given the many controver-
ing a probable diagnosis, obtaining samples for culture, initiating sial features of this older single-center trial, the recent ProCESS trial
empirical antimicrobial therapy, and achieving source control. More compared protocol-based standard care with protocol-based EGDT
than 30% of patients with severe sepsis require source control, mainly and usual care in >31 emergency departments in the United States.
for abdominal, urinary, and soft-tissue infections. The mortality rate Among 1341 patients, the 60-day in-hospital mortality rate for pro-
is lower among patients with source control than among those with- tocol-based standard care (18.2%) was similar to that for usual care
out, although the timing of intervention is debated. For empirical (18.9%) and protocol-based EGDT (21%). The ARISE trial confirmed
antibiotic therapy (Table 297-3), the appropriate choice depends on this finding, showing that, among 1600 patients with early septic
the suspected site of infection, the location of infection onset (i.e., shock at 51 centers in Australia and New Zealand, 90-day mortality
the community, a nursing home, or a hospital), the patient’s medical was similar for EGDT and usual care. Finally, the ProMISe trial,
history, and local microbial susceptibility patterns. In a single-center which enrolled 1260 patients in 56 hospitals in England, found
study of >2000 patients with bacteremia, the number of patients that EGDT offered no mortality benefit in early septic shock but
who needed to receive appropriate antimicrobial therapy in order to did increase treatment intensity and cost. Multiple subsequent
prevent one patient death was 4.0 (95% CI, 3.7–4.3). meta-analyses of the ProCESS, ARISE, and ProMISe trials confirmed
Antibiotic delays may be deadly. For every 1-h delay among patients that EGDT offers no mortality benefit while increasing health care
with sepsis, a 3–7% increase in the odds of in-hospital death is reported. utilization and ICU admission in well-resourced countries. Modified
Although meta-analyses report conflicting results, international clini- versions of EGDT were also tested in lower-resourced settings, with
cal practice guidelines recommend the administration of appropriate no change in outcome. Thus EGDT is no longer recommended as
broad-spectrum antibiotics within 1 h of recognition of severe sepsis the primary strategy for early resuscitation in septic shock. None-
or septic shock. Empirical antifungal therapy should be administered theless, some form of resuscitation is considered essential, and a
only to septic patients at high risk for invasive candidiasis. standardized approach, akin to the use of “trauma teams,” has been
The treatment elements listed above form the basis for two advocated to ensure prompt care. The patient should be moved to an
“bundles” of care: an initial management bundle to be completed appropriate setting, such as the ICU, for ongoing care.
within 3 h of presentation and a management bundle to be completed
SUBSEQUENT TREATMENT OF SEPSIS AND SEPTIC SHOCK
within 6 h. The initial management bundle includes (1) early admin-
istration of appropriate broad-spectrum antibiotics, (2) collection of After initial resuscitation, attention is focused on monitoring and
blood for culture before antibiotic administration, and (3) measure- support of organ function, avoidance of complications, and de-
ment of serum lactate levels. The management bundle includes escalation of care when possible.
(1) an intravenous fluid bolus, (2) treatment with vasopressors for Monitoring Hemodynamic monitoring devices may clarify the
persistent hypotension or shock, and (3) re-measurement of serum primary physiologic manifestations in sepsis and septic shock. The
lactate levels. Implementation of these two bundles has been associ- clinical usefulness of these monitoring devices can be attributable
ated with improved outcome in large multinational studies. to the device itself, the algorithm linked to the device, or the static/
Other elements of the initial management bundle are cardiore- dynamic target of the algorithm. Decades ago, the standard care of
spiratory resuscitation and mitigation of the immediate threats of shock patients included invasive devices like the pulmonary artery
Harrisons_20e_Part8_p2023-p2088.indd 2049 5/30/18 2:23 PM
2050 TABLE 297-2 Elements of Care in Sepsis and Septic Shock: Recommendations Adapted from International Consensus Guidelines
Resuscitation
Sepsis and septic shock constitute an emergency, and treatment should begin right away.
Resuscitation with IV crystalloid fluid (30 mL/kg) should begin within the first 3 h.
Saline or balanced crystalloids are suggested for resuscitation.
If the clinical examination does not clearly identify the diagnosis, hemodynamic assessments (e.g., with focused cardiac ultrasound) can be considered.
In patients with elevated serum lactate levels, resuscitation should be guided towards normalizing these levels when possible.
In patients with septic shock requiring vasopressors, the recommended target mean arterial pressure is 65 mmHg.
Hydroxyethyl starches and gelatins are not recommended.
Norepinephrine is recommended as the first-choice vasopressor.
Vasopressin should be used with the intent of reducing the norepinephrine dose.
The use of dopamine should be avoided except in specific situations—e.g., in those patients at highest risk of tachyarrhythmias or relative bradycardia.
Dobutamine use is suggested when patients show persistent evidence of hypoperfusion despite adequate fluid loading and use of vasopressors.
Red blood cell transfusion is recommended only when the hemoglobin concentration decreases to <7.0 g/dL in the absence of acute myocardial infarction, severe
hypoxemia, or acute hemorrhage.
Infection Control
PART 8
So long as no substantial delay is incurred, appropriate samples for microbiologic cultures should be obtained before antimicrobial therapy is started.
IV antibiotics should be initiated as soon as possible (within 1 h); specifically, empirical broad-spectrum therapy should be used to cover all likely pathogens.
Antibiotic therapy should be narrowed once pathogens are identified and their sensitivities determined and/or once clinical improvement is evident.
If needed, source control should be undertaken as soon as is medically and logistically possible.
Critical Care Medicine
Daily assessment for de-esclation of antimicrobial therapy should be conducted.
Respiratory Support
A target tidal volume of 6 mL/kg of predicted body weight (compared with 12 mL/kg in adult patients) is recommended in sepsis-induced ARDS.
A higher PEEP rather than a lower PEEP is used in moderate to severe sepsis-induced ARDS.
In severe ARDS (PaO2/FIO2, <150 mmHg), prone positioning is recommended, and recruitment maneuvers and/or neuromuscular blocking agents for ≤48 h are
suggested.
A conservative fluid strategy should be used in sepsis-induced ARDS if there is no evidence of tissue hypoperfusion.
Routine use of a pulmonary artery catheter is not recommended.
Spontaneous breathing trials should be used in mechanically ventilated patients who are ready for weaning.
General Supportive Care
Patients requiring a vasopressor should have an arterial catheter placed as soon as is practical.
Hydrocortisone is not suggested in septic shock if adequate fluids and vasopressor therapy can restore hemodynamic stability.
Continuous or intermittent sedation should be minimized in mechanically ventilated sepsis patients, with titration targets used whenever possible.
A protocol-based approach to blood glucose management should be used in ICU patients with sepsis, with insulin dosing initiated when two consecutive blood
glucose levels are >180 mg/dL.
Continuous or intermittent renal replacement therapy should be used in patients with sepsis and acute kidney injury.
Pharmacologic prophylaxis (unfractionated heparin or low-molecular-weight heparin) against venous thromboembolism should be used in the absence of
contraindications.
Stress ulcer prophylaxis should be given to patients with risk factors for gastrointestinal bleeding.
The goals of care and prognosis should be discussed with patients and their families.
Abbreviations: ARDS, acute respiratory distress syndrome; ICU, intensive care unit; PEEP, positive end-expiratory pressure.
Source: Adapted from A Rhodes et al: Surviving Sepsis Campaign: International guidelines for management of sepsis and septic shock: 2016. Crit Care Med 45:486,
2017.
catheter (PAC), also known as the continuous ScvO2 catheter. The may require administration of IV fluids or vasopressors, blood trans-
PAC can estimate cardiac output and measure mixed venous oxygen fusions, or ventilatory support.
saturation, among other parameters, to refine the etiology of shock Many crystalloids can be used in septic shock, including 0.9% nor-
and potentially influence patient outcomes. Recently, a Cochrane mal saline, Ringer’s lactate, Hartmann’s solution, and Plasma-Lyte.
review of 2923 general-ICU patients (among whom the proportion of Because crystalloid solutions vary in tonicity and inorganic/organic
patients in shock was not reported) found no difference in mortality anions, few of these preparations closely resemble plasma. Normal
with or without PAC management, and the PAC therefore is no lon- saline is widely used in the United States. Colloid solutions (e.g.,
ger recommended for routine use. Instead, a variety of noninvasive albumin, dextran, gelatins, or hydroxyethyl starch) are the most
monitoring tools, such as arterial pulse contour analysis (PCA) or widely used fluids in critically ill patients, with variability across
focused echocardiography, can provide continuous estimates of ICUs and countries. A clinician’s choice among colloids is influenced
parameters such as cardiac output, beat-to-beat stroke volume, and by availability, cost, and the desire to minimize interstitial edema.
pulse pressure variation. These tools, along with passive leg-raise Many think that a greater intravascular volume is gained by use of
maneuvers or inferior vena cava collapsibility on ultrasound, can colloids in shock, but the effects of colloids are modified by molec-
help determine a patient’s volume responsiveness but require that a ular weight and concentration as well as by vascular endothelial
variety of clinical conditions be met (e.g., patient on mechanical venti- changes during inflammation. A network meta-analysis using direct
lation, sinus rhythm); in addition, more evidence from larger random- and indirect comparisons in sepsis found evidence of higher mortal-
ized trials on the impact of these tools in daily management is needed. ity with starch than with crystalloids (relative risk [RR], 1.13; 95% CI,
0.99–1.30 [high confidence]) and no difference between albumin (RR,
Support Of Organ Function The primary goal of organ support is 0.83; 95% CI, 0.65, 1.04 [moderate confidence]) or gelatin (RR, 1.24;
to improve delivery of oxygen to the tissues as quickly as possible. 95%CI, 0.61, 2.55 [very low confidence]) and crystalloids. In general,
Depending on the underlying physiologic disturbance, this step crystalloids are recommended on the basis of strong evidence as
Harrisons_20e_Part8_p2023-p2088.indd 2050 5/30/18 2:23 PM
TABLE 297-3 Initial Antimicrobial Therapy for Severe Sepsis with No (pH <7.20) are common indications for mechanical ventilatory 2051
Obvious Source in Adults with Normal Renal Function support. Endotracheal intubation protects the airway, and positive-
CLINICAL CONDITION ANTIMICROBIAL REGIMENSa pressure breathing allows oxygen delivery to metabolically active
Septic shock The many acceptable regimens include (1)
organs in favor of inspiratory muscles of breathing and the dia-
(immunocompetent piperacillin-tazobactam (3.375–4.5 g q6h), (2) phragm. An experiment in dogs showed that the relative proportion
adult) cefepime (2 g q12h), or (3) meropenem (1 g q8h) of cardiac output delivered to respiratory muscles in endotoxic shock
or imipenem-cilastatin (0.5 g q6h). If the patient is decreased by fourfold with spontaneous ventilation over that with
allergic to β-lactam antibiotics, use (1) aztreonam mechanical ventilation. During intubation, patients in shock should
(2 g q8h) or (2) ciprofloxacin (400 mg q12h) or be closely monitored for vasodilatory effects of sedating medica-
levofloxacin (750 mg q24h). Add vancomycin
(loading dose of 25–30 mg/kg, then 15–20 mg/kg
tions or compromised cardiac output due to increased intrathoracic
q8–12h) to each of the above regimens. pressure, both of which may cause hemodynamic collapse. With
Neutropenia Regimens include (1) cefepime (2 g q8h), (2) hemodynamic instability, noninvasive mask ventilation may be less
(<500 neutrophils/μL) meropenem (1 g q8h) or imipenem-cilastatin suitable in patients experiencing sepsis-associated acute respiratory
(0.5 g q6h) or doripenem (500 mg q8h), or failure.
(3) piperacillin-tazobactam (3.375 g q4h). Add
vancomycin (as above) if the patient has a suspected Adjuncts One of the great disappointments in sepsis management
central line–associated bloodstream infection, severe over the past 30 years has been the failure to convert advances in
CHAPTER 297 Sepsis and Septic Shock
mucositis, skin/soft tissue infection, or hypotension. our understanding of the underlying biology into new therapies.
Add tobramycin (5–7 mg/kg q24h) plus vancomycin Researchers have tested both highly specific agents and those with
(as above) plus caspofungin (one dose of 70 mg, more pleotropic effects. The specific agents can be divided into those
then 50 mg q24h) if the patient has severe sepsis/
designed to interrupt the initial cytokine cascade (e.g., anti-LPS or
septic shock.
anti-proinflammatory cytokine strategies) and those that interfere
Splenectomy Use ceftriaxone (2 g q24h, or—in meningitis—2 g
q12h). If the local prevalence of cephalosporin-
with dysregulated coagulation (e.g., antithrombin or activated
resistant pneumococci is high, add vancomycin protein C). Recombinant activated protein C (aPC) was one of the
(as above). If the patient is allergic to β-lactam first agents approved by the U.S. Food and Drug Administration
antibiotics, use levofloxacin (750 mg q24h) or and was the most widely used. A large, randomized, double-blind,
moxifloxacin (400 mg q24h) plus vancomycin (as placebo-controlled, multicenter trial of aPC in severe sepsis (the
above). PROWESS trial) was reported in 2001; the data suggested an abso-
All agents are administered by the intravenous route.
a
lute risk reduction of up to 6% among aPC-treated patients with
Source: Adapted in part from DN Gilbert et al: The Sanford Guide to Antimicrobial severe sepsis. However, subsequent phase 3 trials failed to confirm
Therapy, 47th ed, 2017; and from RS Munford: Sepsis and septic shock, in DL this effect, and the drug was withdrawn from the market. It is no
Kasper et al (eds). Harrison’s Principles of Internal Medicine, 19th ed. New York,
McGraw-Hill, 2015, p 1757. longer recommended in the care of sepsis or septic shock.
Many adjunctive treatments in sepsis and septic shock target
changes in the innate immune response and coagulation cascade.
first-line fluids for sepsis resuscitation, with specific caveats; their Specific adjuncts like glucocorticoids in septic shock have continued
use is guided by resolution of hypotension, oliguria, altered men- to be widely used. A large negative clinical trial and a conflicting
tation, and hyperlactemia. Only weak evidence supports the use systematic review in 2009 extended the debate about whether
of balanced crystalloids, and guidelines recommend against using glucocorticoids lower 28-day mortality or improve shock reversal.
hydroxyethyl starches for intravascular volume replacement. Most meta-analyses report no change in mortality but an increase in
When circulating fluid volume is adequate, vasopressors are rec- shock reversal with glucocorticoid treatment. The recent HYPRESS
ommended to maintain perfusion of vital organs. Vasopressors such trial found no difference between patients with severe sepsis who
as norepinephrine, epinephrine, dopamine, and phenylephrine differ were treated with glucocorticoids and control patients in terms of
in terms of half-life, β- and α-adrenergic stimulation, and dosing reg- the development of shock or the mortality rate. These data and oth-
imens. Recent evidence comes from the SOAP II trial, a double-blind ers led to a suggestion in international clinical practice guidelines
randomized clinical trial at eight centers comparing norepinephrine against using IV hydrocortisone to treat septic shock if adequate
with dopamine in 1679 undifferentiated ICU patients with shock, fluid resuscitation and vasopressor therapy are able to restore hemo-
of whom 63% were septic. Although no difference was observed in dynamic stability. If not, the guidelines suggest the administration of
28-day mortality or in predefined septic-shock subgroup, arrhythmias IV hydrocortisone at a dose of 200 mg per day (weak recommenda-
were significantly greater with dopamine. These findings were con- tion, low quality of evidence).
firmed in a subsequent meta-analysis. As a result, expert opinion and Among other adjuncts, IV immunoglobulin may be associated
consensus guidelines recommend norepinephrine as the first-choice with potential benefit, but significant questions remain and such
vasopressor in septic shock. Levels of the endogenous hormone vaso- treatment is not part of routine practice. Despite a large number
pressin may be low in septic shock, and the administration of vaso- of observational studies suggesting that statin use mitigates the
pressin can reduce the norepinephrine dose. Consensus guidelines incidence or outcome of sepsis and severe infection, there are no
suggest adding vasopressin (up to 0.03 U/min) in patients without confirmatory randomized controlled trials, and statins are not an
a contraindication to norepinephrine, with the intent of raising mean element in routine sepsis care.
arterial pressure or decreasing the norepinephrine dose. There may De-Escalation of Care Once patients with sepsis and septic shock
be select indications for use of alternative vasopressors—e.g., when are stabilized, it is important to consider which therapies are no
tachyarrhythmias from dopamine or norepinephrine, limb ischemia longer required and how care can be minimized. The de-escalation
from vasopressin, or other adverse effects dictate. of initial broad-spectrum therapy, which observational evidence
The transfusion of red blood cells to high thresholds (>10 g/dL) indicates is safe, may reduce the emergence of resistant organisms
had been suggested as part of EGDT in septic shock. However, the as well as potential drug toxicity and costs. The added value of com-
recent Scandinavian TRISS trial in 1005 septic shock patients demon- bination antimicrobial therapy over that of adequate single-agent
strated that a lower threshold (7 g/dL) resulted in 90-day mortality antibiotic therapy in severe sepsis has not been established. Current
rates similar to those with a higher threshold (9 g/dL) and reduced guidelines recommend combination antimicrobial therapy only
transfusions by almost 50%. for neutropenic sepsis and sepsis caused by Pseudomonas. Large
Significant hypoxemia (PaO2, <60 mmHg; or SaO2, <90%), trials are under way in the United States to determine how serum
hypoventilation (rising PaCO2), increased work of breathing, and biomarkers like procalcitonin can assist clinicians in minimizing
inadequate or unsustainable compensation for metabolic acidosis antibiotic exposure, while European trials are indicating that this
Harrisons_20e_Part8_p2023-p2088.indd 2051 5/30/18 2:23 PM
1146 with members at high risk of severe disease (children <1 year of age, Klein NP et al: Waning Tdap effectiveness in adolescents. Pediatrics
pregnant women). Data on the use of the newer macrolides for che- 137:e20153326, 2016.
moprophylaxis are not available, but these drugs are commonly used Skoff TH: Sources of infant pertussis infection in the United States.
because of their increased tolerability and their effectiveness. Pediatrics 136:635, 2015.
World Health Organization: Pertussis vaccines: WHO position
Immunization (See also Chap. 118) The mainstay of pertussis paper—August 2015. Wkly Epidemiol Rec 90:433, 2015.
prevention is active immunization. Pertussis vaccine became widely
used in North America after 1940; the reported number of pertussis
cases subsequently fell by >90%. Whole-cell pertussis vaccines are
prepared through the heating, chemical inactivation, and purification
156 Gram-Negative
of whole B. pertussis organisms. Despite their efficacy (average esti-
mate, 85%; range for different products, 30–100%), whole-cell pertussis Diseases Caused by
vaccines are associated with adverse events—both common (fever;
injection-site pain, erythema, and swelling; irritability) and uncommon Enteric
(febrile seizures, hypotonic-hyporesponsive episodes). Alleged asso- Bacilli
ciations of whole-cell pertussis vaccine with encephalopathy, sudden
infant death syndrome, and autism, although not substantiated, have Thomas A. Russo, James R. Johnson
spawned an active anti-immunization lobby. The development of acel-
lular pertussis vaccines, which are effective and less reactogenic, has
greatly alleviated concerns about the inclusion of pertussis vaccine in
the combined infant immunization series.
GENERAL FEATURES AND PRINCIPLES
The post-antibiotic era has begun. For most people, this is the first time
Although a wide variety of acellular pertussis vaccines were devel-
in their lives that an effective treatment for a bacterial infection may
oped, only a few are still marketed widely; all contain pertussis toxoid
not exist. The Enterobacteriaceae are at the forefront of this evolving
and filamentous hemagglutinin. One acellular pertussis vaccine also
public health crisis. For example, the Centers for Disease Control and
contains pertactin, and another contains pertactin and two types of
Prevention (CDC) and the World Health Organization (WHO) have
fimbriae. In phase 3 efficacy studies, multicomponent acellular per-
designated carbapenem-resistant Enterobacteriaceae as representing
tussis vaccines were more efficacious than one- or two-component
a threat level of “urgent” and “priority one, critical,” respectively.
vaccines. However, epidemiologic studies in countries using one- and
Enterobacteriaceae are responsible for a significant proportion of the
two-component acellular pertussis vaccines demonstrated high vaccine
deaths attributed to resistant bacteria, the number of which has been
effectiveness against pertussis. Adult formulations of acellular pertus-
PART 5
estimated at 23,000 and 25,000 annually in the United States and the
sis vaccines have been shown to be safe, immunogenic, and efficacious
European Union, respectively, with numbers three- to fivefold greater
in clinical trials in adolescents and adults and are now recommended
(per capita) in low- and middle-income countries (e.g., Thailand).
for routine immunization of these groups in several countries.
These pathogens cause a wide variety of infections involving diverse
Although whole-cell vaccines are still used extensively in
anatomic sites in both healthy and compromised hosts. Therefore, a
Infectious Diseases
developing regions of the world, acellular pertussis vaccines
thorough knowledge of clinical presentations and appropriate ther-
are used exclusively for childhood immunization in much of
apeutic choices is necessary for optimal outcomes. Escherichia coli,
the developed world. In light of evidence of early waning of immunity
Klebsiella, Proteus, Enterobacter, Serratia, Citrobacter, Morganella, Provi-
among children who received acellular pertussis vaccine in infancy, the
dencia, Cronobacter, and Edwardsiella are enteric gram-negative bacilli
WHO Strategic Advisory Group of Experts (SAGE) now recommends
(GNB) that are members of the family Enterobacteriaceae. Salmonella,
using whole-cell pertussis vaccine for the primary infant immunization
Shigella, and Yersinia, also in the family Enterobacteriaceae, are dis-
series. In countries using acellular pertussis vaccines in infancy, addi-
cussed in Chaps. 160, 161, and 166, respectively.
tional booster immunizations in older children, adolescents, and adults
are recommended to prevent pertussis in high-risk infants. In North ■ EPIDEMIOLOGY
America, acellular pertussis vaccines for children are given as a three- E. coli, Klebsiella, Proteus, Enterobacter, Serratia, Citrobacter,
dose primary series at 2, 4, and 6 months of age, with a reinforcing dose Morganella, Providencia, Cronobacter, and Edwardsiella are com-
at 15–18 months of age and a booster dose at 4–6 years of age. Adoles- ponents of the normal animal and human colonic microbiota
cents (11–18 years of age) and all unvaccinated adults should receive a and/or the microbiota in various environmental habitats, including
dose of the adult-formulation diphtheria–tetanus–acellular pertussis long-term-care facilities (LTCFs) and hospitals. As a result, except for
vaccine. In addition, several countries, including the United States and certain pathotypes of intestinal pathogenic E. coli, these genera are
the United Kingdom, recommend pertussis immunization specifically global pathogens. The incidence of infection due to these agents is
for health care workers and for women in the third trimester of preg- increasing because of the combination of an aging population and
nancy to increase passive transfer of maternal antibodies to the fetus. In increasing antimicrobial resistance. In healthy humans, E. coli is the
a study from the United Kingdom, immunization of pregnant women predominant species of GNB in the colonic microbiota; Klebsiella and
≥7 days prior to delivery was 91–93% effective at preventing pertussis Proteus are less prevalent. GNB (primarily E. coli, Klebsiella, and Proteus)
in infants ≤3 months of age. Pertussis vaccine coverage among U.S. colonize the oropharynx and skin of healthy individuals only tran-
adolescents was 84.6% in 2012, and coverage among pregnant women siently. By contrast, in LTCFs and hospital settings, a variety of GNB
is increasing (from 12.7% in 2010 to 41.7% in 2013 in a cohort of pri- emerge as the dominant colonizers of both mucosal and skin surfaces,
vately insured women). Nevertheless, coverage among adults remains particularly in association with antimicrobial use, severe illness, and
low (14.2% in 2012). Further improvements in adult vaccine coverage extended length of stay. LTCFs are emerging as an important reservoir
may permit better control of pertussis across the age spectrum, with for resistant GNB. This colonization may lead to subsequent infection;
collateral protection of infants too young to be immunized. However, for example, oropharyngeal colonization may lead to pneumonia, and
more effective vaccines with longer-lasting protection will ultimately colonic/perineal colonization may lead to urinary tract infection (UTI).
be needed to control this disease. The use of ampicillin or amoxicillin was associated with an increased
risk of subsequent infection due to the hypervirulent pathotype of
■ FURTHER READING Klebsiella pneumoniae in Taiwan; this association suggests that changes
De Serres G et al: Morbidity of pertussis in adolescents and adults. J in the quantity or prevalence of colonizing bacteria may significantly
Infect Dis 182:174, 2000. influence the risk of infection. Serratia and Enterobacter infection may be
Kilgore PE et al: Pertussis: Microbiology, disease, treatment, and pre- acquired directly through a variety of infusates (e.g., medications, blood
vention. Clin Microbiol Rev 29:449, 2016. products). Edwardsiella infections are acquired through freshwater
Harrisons_20e_Part5_p0859-p1648.indd 1146 6/1/18 12:05 PM
and marine environment exposures and are most common in phagocytes in the absence of antibody (e.g., as conferred by capsule or 1147
Southeast Asia. the O antigen component of lipopolysaccharide) is one of the defining
traits of an extracellular pathogen. Tissue damage (e.g., as mediated by
■ STRUCTURE AND FUNCTION E. coli hemolysin) may facilitate nutrient acquisition and spread within
Enteric GNB possess an extracytoplasmic outer membrane consisting the host. Without doubt, many important virulence genes await iden-
of a lipid bilayer with associated proteins, lipoproteins, and polysac- tification (Chap. 116).
charides (capsule, lipopolysaccharide). The outer membrane interfaces The ability to induce septic shock is another defining feature of these
with the external environment, including the human host. A variety of genera. GNB are the most common causes of this potentially lethal syn-
components of the outer membrane are critical determinants in patho- drome. Pathogen-associated molecular pattern molecules (PAMPs; e.g.,
genesis (e.g., capsule) and antimicrobial resistance (e.g., permeability the lipid A moiety of lipopolysaccharide) stimulate a proinflammatory
barrier, efflux pumps). In addition, secreted products play an impor- host response via pattern recognition receptors (e.g., Toll-like or C-type
tant role in both host infection (e.g., iron acquisition molecules) and lectin receptors) that activate host defense signaling pathways; if overly
environmental niche survival and colonization (e.g., type VI secretion exuberant, this response results in shock (Chap. 297). Direct bacterial
systems). damage of host tissue (e.g., by toxins) or collateral damage from the
host response can result in the release of damage-associated molecular
■ PATHOGENESIS pattern molecules (DAMPs; e.g., HMGB1) that can propagate a detri-
Multiple bacterial virulence factors are required for the pathogenesis mental proinflammatory host response.
of infections caused by GNB. Possession of specialized virulence genes Many antigenic variants (serotypes) exist in most genera of GNB. For
defines pathogens and enables them to infect the host efficiently. Hosts example, E. coli has more than 150 O (somatic) antigens, 80 K (capsular)
and their cognate pathogens have been co-adapting throughout evo- antigens, and 53 H (flagellar) antigens. This antigenic variability, which
lutionary history. During the host–pathogen “chess match” over time, permits immune evasion and allows recurrent infection by different
various and redundant strategies have emerged in both the pathogens strains of the same species, has impeded vaccine development (Chap. 118).
and their hosts (Table 156-1).
Intestinal pathogenic (diarrheagenic) mechanisms are discussed ■ INFECTIOUS SYNDROMES
below. The members of the Enterobacteriaceae family that cause Depending on both the host and the pathogen, GNB can infect nearly
extraintestinal infections are primarily extracellular pathogens and every organ or body cavity. E. coli can cause either intestinal or extraintes-
therefore share certain pathogenic features. The principal components tinal infection, depending on the particular pathotype, and Edwardsiella
of host defense against Enterobacteriaceae, regardless of species, are tarda can cause both intestinal and extraintestinal infection. Klebsiella
CHAPTER 156 Diseases Caused by Gram-Negative Enteric Bacilli
innate immunity (including intact skin and mucosal barriers; the with- causes primarily extraintestinal infection, but a toxin-producing variant
holding of nutrients; and the activities of complement, antimicrobial of Klebsiella oxytoca has been associated with hemorrhagic colitis.
peptides, and professional phagocytes) and humoral immunity. Both E. coli and—to a lesser degree—Klebsiella account for most extraintes-
susceptibility to and severity of infection are increased with dysfunc- tinal infections due to GNB. These species (for K. pneumoniae, primarily
tion or deficiencies of these host components. By contrast, the virulence its hypervirulent pathotype) are the most virulent pathogens within
traits of intestinal pathogenic E. coli—i.e., the distinctive strains that this group, as demonstrated by their ability to cause severe infections
can cause diarrheal disease—are for the most part different from those in healthy, ambulatory hosts from the community. However, the other
of extraintestinal pathogenic E. coli (ExPEC) and other GNB that cause genera of GNB are also important extraintestinal pathogens, especially
extraintestinal infections. This distinction reflects site-specific differ- among LTCF residents and hospitalized patients, in large part because
ences in host environments and defense mechanisms. of the intrinsic or acquired antimicrobial resistance of these organisms
A given enterobacterial strain usually possesses multiple adhesins and the increasing number of individuals with compromised host
for binding to a variety of host cells (e.g., in E. coli: type 1, S, and F1C defenses. The mortality rate is substantial in many GNB infections and
fimbriae; P pili). Nutrient acquisition (e.g., of iron via siderophores) correlates with severity of illness and underlying host status. Especially
requires many genes that are necessary but not sufficient for pathogen- problematic are pneumonia, sepsis, and septic shock (arising from any
esis. The ability to resist the bactericidal activity of complement and site of infection), for which the associated mortality rates are 20–60%.
■ DIAGNOSIS
TABLE 156-1 Interactions of Extraintestinal Pathogenic Escherichia Isolation of GNB from sterile sites almost always implies infection,
coli with the Human Host: A Paradigm for Extracellular,
Extraintestinal Gram-Negative Bacterial Pathogens whereas their isolation from nonsterile sites, particularly from open
wounds and the respiratory tract, requires clinical correlation to differ-
BACTERIAL GOAL HOST OBSTACLE BACTERIAL SOLUTION
entiate colonization from infection. Clinical microbiology laboratories
Extraintestinal Flow of urine, Multiple adhesins (e.g.,
are increasingly incorporating newer molecular-based methodologies
attachment mucociliary escalator type 1, S, and F1C
fimbriae; P pili) (e.g., matrix-assisted laser desorption–ionization–time-of-flight mass
Nutrient acquisition for Nutrient sequestration Cellular lysis (e.g.,
spectrometry [MALDI-TOF-MS] and polymerase chain reaction [PCR])
growth (e.g., iron via hemolysin), multiple to enhance the sensitivity, accuracy, and rapidity of reporting on
intracellular storage and mechanisms for pathogen identification and resistance genes (e.g., blaKPC, NDM, OXA,
extracellular scavenging competing for iron (e.g., CTX). This information can be used to increase the timeliness of initi-
via lactoferrin and siderophores) and other ation and/or the accurate selection of empirical antimicrobial therapy,
transferrin) nutrients thereby improving outcomes.
Initial avoidance of host Complement, phagocytic Capsular polysaccharide,
bactericidal activity cells, antimicrobial lipopolysaccharide
peptides TREATMENT
Dissemination (within Intact tissue barriers Irritant tissue damage
host and between hosts) resulting in increased Infections Caused by Gram-Negative Enteric Bacilli
excretion (e.g., toxins
such as hemolysin), (See also Chap. 139) Initiation of appropriate empirical
invasion of brain antimicrobial therapy early in the course of GNB infections
endothelium (particularly serious ones) leads to improved outcomes.
Late avoidance of host Acquired immunity (e.g., Cell entry, acquisition of The ever-increasing prevalence of multidrug-resistant (MDR) and
bactericidal activity specific antibodies), antimicrobial resistance extensively drug-resistant (XDR) GNB; the lag between published
treatment with
and current resistance rates; and variations in antimicrobial suscep-
antibiotics
tibility by species, geographic location, regional antimicrobial use,
Harrisons_20e_Part5_p0859-p1648.indd 1147 6/1/18 12:05 PM
1148 and hospital site (e.g., intensive care units [ICUs] versus wards) cephalosporins, β-lactam/β-lactamase inhibitor combinations, and
necessitate familiarity with evolving patterns of antimicrobial resis- carbapenems, thereby further reducing susceptibility to these
tance for the selection of appropriate empirical therapy. Factors β-lactam agents. The prevalence of acquired ESBL production, par-
predictive of resistance in a given isolate include recent antimicro- ticularly of CTX-M-type enzymes, is increasing in GNB worldwide,
bial use, a health care association (e.g., recent or ongoing hospitaliza- in large part as a result of the presence of the corresponding genes
tion, dialysis, residence in an LTCF), or international travel (e.g., to on transferable (conjugal) plasmids variably linked to or associated
Asia, Latin America, Africa, Eastern Europe). Resistance rates will with resistance to fluoroquinolones, trimethoprim-sulfamethoxazole
almost certainly increase over time and will likely be higher than (TMP-SMX), aminoglycosides, tetracyclines, and (more recently)
shown here by the time this chapter is published. Data for 2008–2014 fosfomycin.
from the U.S. National Healthcare Safety Network indicates that the To date, ESBLs are most prevalent in E. coli, K. pneumoniae, and
prevalence of the extended-spectrum β-lactamase (ESBL) phenotype K. oxytoca, but these enzymes can occur in all Enterobacteriaceae.
among Enterobacteriaceae isolates varied by health care setting—i.e., The approximate regional prevalence of ESBL-producing GNB cur-
16% for short-term care, 38.6% for long-term care, and 10.7% for rently follows a descending gradient as follows: China > Eastern
inpatient rehabilitation facilities—as did the prevalence of carba- Europe > other parts of Asia > Latin America and Africa > Western
penem resistance (2.8%, 12%, and 1.9%, respectively). Global ESBL Europe, the United States, Canada, and Australia. International travel
rates for Enterobacteriaceae isolates from hospitalized patients were to high-prevalence regions increases the likelihood of colonization
roughly similar in North America, Western Europe, Australia, and with these strains.
New Zealand and were higher in Latin America, Eastern Europe, ESBL-producing GNB were described initially in hospitals
and Asia. Perhaps even more concerning is the reported isolation of (ICUs > wards) and LTCFs, where outbreaks occurred in association
carbapenem-resistant Enterobacteriaceae (mediated primarily by with extensive use of third-generation cephalosporins. However,
New Delhi metallo-β-lactamase [NDM]) from ambulatory patients over the last decade, the incidence of UTI due to CTX-M ESBL-
without known risk factors. producing E. coli has increased worldwide (including in the United
For appropriately selected patients, it may be prudent initially, States), even among healthy ambulatory women without health care
pending antimicrobial susceptibility results, to use two potentially or antimicrobial exposure. Antimicrobial use in food animals has
active agents as a way to increase the likelihood that at least also been implicated in the rise of ESBLs.
one agent will be active against the patient’s organism. If broad- Carbapenems are the most reliably active β-lactam agents against
spectrum treatment has been initiated, it is important to switch to ESBL-expressing strains. Clinical experience with alternatives is more
the most appropriate narrower-spectrum agent once antimicrobial limited, but, for organisms susceptible to piperacillin-tazobactam
susceptibility results become available. Such responsible antimicro- (minimal inhibitory concentration [MIC], ≤4 μg/mL), this agent—
PART 5
bial stewardship should help disrupt the ever-escalating cycle of dosed at 4.5 g q6h—may offer a carbapenem-sparing alternative, as
selection for increasingly resistant bacteria, decrease the likelihood may ceftazidime-avibactam and ceftolozane-tazobactam.
of Clostridium difficile infection, decrease costs, and maximize the The role of tigecycline is unclear despite its excellent in vitro
useful longevity of available antimicrobial agents. Likewise, it is activity; Proteus, Morganella, and Providencia are inherently resistant,
important to avoid treatment of patients who are colonized but not and attainable serum and urine levels are low. Therefore, caution is
Infectious Diseases
infected (e.g., who have a positive sputum culture without evidence advisable, especially with serious infections, until more clinical data
of pneumonia or a positive urine culture without clinical manifes- become available.
tations of UTI). Oral options for the treatment of strains expressing ESBLs are
At present, the most reliably active antimicrobial agents against limited. Fosfomycin and nitrofurantoin (for E. coli) and perhaps piv-
GNB are the carbapenems (e.g., meropenem); the aminoglycoside mecillinam (not available in the United States) are the most reliably
amikacin; the fourth-generation cephalosporin cefepime; the β- active agents.
lactamase inhibitor combination agents piperacillin-tazobactam, AmpC b-lactamases, when induced or stably derepressed to high
ceftolozane-tazobactam, and ceftazidime-avibactam; and the levels of expression, confer resistance to the same substrates as do
polymyxins (colistin and polymyxin B). However, it should be ESBLs as well as to the cephamycins (e.g., cefoxitin and cefotetan).
noted that Proteus, Serratia, Morganella, and Providencia are intrin- The genes encoding these enzymes are primarily chromosomal and
sically resistant to the polymyxins. The number of antimicrobial therefore may not exhibit the linked or associated resistance to flu-
agents effective against certain Enterobacteriaceae is shrinking, and oroquinolones, TMP-SMX, aminoglycosides, and tetracyclines that
truly pan-resistant GNB exist. Accordingly, the currently available is common with ESBLs. These enzymes are problematic for the cli-
antimicrobial drugs must be used judiciously. nician: resistance may develop during therapy with third-generation
β-Lactamases, which inactivate β-lactam agents, are the most cephalosporins and result in clinical failure, particularly in the set-
important mediators of β-lactam resistance in GNB. Decreased ting of bacteremia.
permeability and/or active efflux of β-lactam agents, although less Although chromosomal AmpC β-lactamases are present in nearly
important and less potent, may occur alone or in combination with all members of the Enterobacteriaceae family, the risk of clinically
β-lactamase-mediated resistance. significant induction of high-level expression or selection of stably
Broad-spectrum β-lactamases (e.g., TEM, SHV), which mediate derepressed mutants with cephalosporin treatment is greatest with
resistance to many penicillins and first-generation cephalospo- Enterobacter cloacae and Enterobacter aerogenes, lower with Serratia
rins, are frequently expressed in enteric GNB. These enzymes are marcescens and Citrobacter freundii, and lowest with Providencia and
inhibited by β-lactamase inhibitors (e.g., clavulanate, sulbactam, Morganella morganii. In addition, rare strains of E. coli, K. pneumoniae,
tazobactam, avibactam). In their wild-type form, they do not hydro- and other Enterobacteriaceae have acquired plasmids containing
lyze third- and fourth-generation cephalosporins or cephamycins inducible AmpC β-lactamase genes.
(e.g., cefoxitin). However, molecular variants of TEM and SHV that For AmpC-expressing strains, carbapenems are an appropri-
have amino acid replacements at certain critical positions in the ate treatment option. Ceftazidime-avibactam and ceftolozane-
peptide do exhibit such hydrolytic capability and thus are referred tazobactam are active in vitro, but clinical data are limited. The
to as ESBLs, as discussed below. fourth-generation cephalosporin cefepime may be an appropriate
ESBLs (e.g., CTX-M, SHV, TEM) are modified broad- option if the concomitant presence of an ESBL can be excluded (a task
spectrum enzymes that hydrolyze third-generation cepha- that currently exceeds the capability of most clinical microbiology
losporins, aztreonam, and (in some instances) fourth- laboratories) and source control is achieved. Although clinical data
generation cephalosporins in addition to the drugs hydrolyzed by are limited, other carbapenem-sparing alternatives to consider if iso-
broad-spectrum β-lactamases. GNB that express ESBLs may also lates are susceptible in vitro include fluoroquinolones, piperacillin-
possess porin mutations that result in decreased uptake of tazobactam, TMP-SMX, tigecycline, and aminoglycosides.
Harrisons_20e_Part5_p0859-p1648.indd 1148 6/1/18 12:05 PM
Carbapenemases—e.g., class A (Klebsiella pneumoniae carba- IV, with or without decreased permeability and active efflux. Flu- 1149
penemase [KPC]); class B (NDM; Verona integron–encoded oroquinolone resistance is increasingly prevalent among GNB and
metallo-β-lactamase [VIM]; and imipenemase metallo-β- is associated with resistance to other antimicrobial classes; for
lactamase [IMP]); and class D [OXA-48])—confer resistance to the example, 20–80% of ESBL-producing enteric GNB are also resistant
same drugs as do ESBLs as well as to cephamycins and carbapenems. to fluoroquinolones. At present, fluoroquinolones should be consid-
As with ESBLs, carbapenemase-encoding genes may be present on ered unreliable as empirical therapy for GNB infections in critically
transferable plasmids, which often encode linked resistance to flu- ill patients.
oroquinolones, TMP-SMX, tetracyclines, and aminoglycosides. In this era of increasing antimicrobial resistance, it is critical to
Transposon-mediated spread (e.g., TN4401 for KPC) is also impor- culture the primary site of infection before initiating antimicrobial
tant. Unfortunately, carbapenemase-producing Enterobacteriaceae therapy and, for systemically ill patients, to obtain blood cultures. In
are becoming increasingly common, particularly in Asia. Asymp- vitro testing may not always detect antimicrobial resistance; there-
tomatic intestinal carriage may facilitate spread. fore, it is important to assess the patient’s clinical response to treat-
Carbapenemase production by Enterobacteriaceae is most prev- ment. Moreover, as discussed above, resistance may emerge during
alent in K. pneumoniae and, secondarily, in E. coli, but has been therapy through the induction or stable derepression of AmpC
described in nearly all members of the family. Carbapenem resis- β-lactamases. In addition, drainage of abscesses, resection of necrotic
tance may also occur in the absence of carbapenemase produc- tissue, and removal of infected foreign bodies, sometimes referred to
tion, mediated by production of an AmpC β-lactamase and/or collectively as “source control,” are often required for cure.
ESBL along with modifications in permeability/efflux. Resistance GNB are commonly involved in polymicrobial infections,
to any carbapenem should prompt assessment for carbapenemase in which the role of each individual pathogen is uncertain
production via either genotypic or phenotypic tests, if available; (Chap. 172). Although some GNB are more pathogenic than others,
the exception to this rule is isolated resistance to imipenem in it is usually prudent, if possible, to design an antimicrobial regimen
M. morganii, Proteus, and Providencia, which exhibit intrinsic low- active against all of the GNB identified, because each is capable of
level resistance. Although the modified Hodge test is used widely pathogenicity in its own right. Lastly, for patients treated initially
for phenotypic confirmation of carbapenemase production, its lim- with a broad-spectrum empirical regimen, the regimen should be
itations include false-positive results with Enterobacter species and de-escalated as expeditiously as possible once susceptibility results
false-negative results with NDM. are known and the patient has responded to therapy.
For treatment of infections due to carbapenem-resistant Enterobac-
teriaceae, tigecycline and colistin are the most reliably active paren- ■ PREVENTION
CHAPTER 156 Diseases Caused by Gram-Negative Enteric Bacilli
teral agents in vitro. However, because tigecycline reaches only low (See also Chap. 137) Certain measures are broadly applicable for
serum and urine concentrations, caution is warranted in using it decreasing infection risk. Antimicrobial stewardship programs should
to treat bacteremia and perhaps UTI, although a few case reports be instituted to facilitate appropriate antimicrobial use, which will
describe some success with tigecycline therapy for UTI. Colistin minimize the development of resistance. Diligent adherence to hand-
has nephrotoxic and neurotoxic potential. The recent emergence hygiene protocols by health care personnel and cleaning/disinfection
of the colistin resistance gene mcr-1 on a stable transferable plas- or single-patient use of objects that come into contact with patients
mid is extremely concerning since polymyxins (polymyxin B and (e.g., stethoscopes and blood pressure cuffs) are essential. Indwelling
polymyxin E [colistin]) currently constitute a last line of defense devices (e.g., urinary and intravascular catheters) should be used
against strains that produce metallo-carbapenemases (e.g., NDM-1). only when necessary and inserted according to an appropriate pro-
In addition, in a recent study, 13% of carbapenem-resistant K. pneu- tocol; protocols for daily-use evaluation and prompt removal should
moniae isolates were co-resistant to colistin independent of mcr-1. be implemented. Multi-use medication vials should be avoided if
Ceftazidime-avibactam is active in vitro against the serine carba- possible. Oral application of chlorhexidine decreases the incidence of
penemases (e.g., KPC, OXA-48) but not the metallo-carbapenemases pneumonia among patients on ventilators. Increasing data support the
(e.g., NDM, VIM, IMP). However, limited clinical data from an implementation of universal decolonization (e.g., chlorhexidine bath-
uncontrolled retrospective study of ceftazidime-avibactam for the ing) to prevent infection in ICU patients. The public health threat from
treatment of infection with carbapenem-resistant Enterobacteriaceae carbapenem-resistant Enterobacteriaceae has resulted in additional
demonstrated suboptimal efficacy and development of resistance recommendations, especially for carbapenemase-producing carbapenem-
in 8% of the cohort. Aminoglycosides may have some utility for resistant Enterobacteriaceae, which are an even greater concern. These
combination therapy if they are active in vitro. Fosfomycin is often recommendations include contact precautions for patients colonized
active in vitro, but clinical data are limited. Furthermore, resis- or infected with carbapenem-resistant Enterobacteriaceae, notification
tance may develop with monotherapy and increased use, plasmid- to the receiving facility from facilities transferring a patient colonized
mediated resistance (via fosA3) has been described (raising concern or infected with these organisms, and daily environmental cleaning.
about rapid dissemination), resistance is generally more prevalent Screening of contacts and active surveillance for these bacteria may
among XDR strains, susceptibility testing may not be readily avail- also be appropriate.
able, and no parenteral formulation is available in the United States.
Aztreonam is active against the problematic metallo-carbapenemases ESCHERICHIA COLI INFECTIONS
but is hydrolyzed by ESBLs and AmpC β-lactamases, which often All E. coli strains share a core genome of ~2000 genes. In contrast,
co-exist in XDR strains. Ongoing studies are assessing aztreonam an E. coli strain’s ability to cause infection and the nature of such
plus avibactam, a promising combination for the treatment of infections are defined largely by accessory (i.e., non-core, non-
pan-drug-resistant strains. essential) genes that encode various virulence factors. The composition
Extensive resistance to available agents may leave the clinician of the E. coli accessory genome is fluid and ongoing, as demonstrated by
with few or no ideal therapeutic options. However, use of a regimen the recent evolution of Shiga toxin–producing enteroaggregative E. coli.
that takes into account the site of infection, achievable drug levels at
that site (e.g., higher concentrations of many agents in urine), and ■ COMMENSAL STRAINS
pharmacodynamic factors (e.g., prolonged infusion of β-lactam agents Commensal E. coli variants are an important constituent of the normal
to maintain drug levels above the MIC) may increase the chance intestinal microbiota that confer benefits to the host (e.g., resistance to
for a successful outcome. Likewise, observational data suggest that colonization with pathogenic organisms). Such strains generally lack
combination therapy may be beneficial against carbapenem-resistant the specialized virulence traits that enable extraintestinal and intesti-
Enterobacteriaceae; randomized controlled trials are in progress. nal pathogenic E. coli strains to cause disease outside and within the
Resistance to fluoroquinolones usually is due to alterations in gastrointestinal tract, respectively. However, even commensal E. coli
or protection of the target sites in DNA gyrase and topoisomerase strains can be involved in extraintestinal infections in the presence of
Harrisons_20e_Part5_p0859-p1648.indd 1149 6/1/18 12:05 PM
1154 When stools are free of mucus and blood, early patient-initiated
treatment of traveler’s diarrhea with a fluoroquinolone or azith-
romycin decreases the duration of illness, and the use of loperamide
may halt symptoms within a few hours. Although dysentery caused
by EIEC is self-limited, treatment hastens the resolution of symp-
toms, particularly in severe cases. In contrast, antimicrobial therapy
for STEC/EHEC/ST-EAEC infection (the presence of which is sug-
gested by grossly bloody diarrhea without fever) should be avoided
because antibiotics may increase the incidence of HUS (possibly
via increased production/release of Stx). In the treatment of HUS,
plasmapheresis has no benefit and the value of inhibition of C5 (via
eculizumab) is unresolved.
KLEBSIELLA INFECTIONS
K. pneumoniae is the most important Klebsiella species from a medical
standpoint, causing community-acquired, LTCF-acquired, and noso-
comial infections. K. oxytoca is primarily a pathogen in LTCFs and
hospitals. Klebsiella species are broadly prevalent in the environment
and colonize the mucosal surfaces of mammals. In healthy humans,
the prevalence of K. pneumoniae colonization is 5–35% in the colon and
1–5% in the oropharynx; skin is usually colonized only transiently.
Most Klebsiella infections in Western countries are caused by
“classic” K. pneumoniae (cKP) and occur in hospitals and
LTCFs. The most common clinical syndromes due to cKP are
pneumonia, UTI, abdominal infection, intravascular device infection,
surgical site infection, soft tissue infection, and secondary bacteremia.
cKP strains have gained notoriety because their propensity for acquir-
ing antimicrobial resistance determinants makes treatment challeng-
PART 5
ing. Clonal group ST258, many members of which produce KPC, is
undergoing international dissemination. The spread of NDM-1-
producing strains from India in association with medical tourism has
captured the attention of physicians and the lay press.
In addition, hypervirulent K. pneumoniae (hvKP) strains that are
Infectious Diseases
phenotypically and clinically distinct from cKP have emerged recently,
having initially been recognized in Taiwan in 1986. Although hvKP
infections have occurred globally in all ethnic groups, most cases have
been reported in individuals of Asian ethnicity, mainly from the Asian
Pacific Rim but also from other locales. Affected individuals often
have diabetes mellitus. These demographics raise the possibility of
a locale-specific distribution of the organism or an increased suscep-
tibility of Asian hosts, especially those who are diabetic. In contrast
to the usual health care–associated context for cKP infections in the
West, hvKP is capable of causing serious life- and organ-threatening
infections in younger, healthy individuals from the community and can
spread metastatically to the eyes, central nervous system, and lungs
from the primary site of infection.
hvKP infection initially was characterized and distinguished from
traditional infections caused by cKP strains by its (1) presentation
as community-acquired pyogenic liver abscess (Fig. 156-1, top ), (2)
occurrence in patients lacking a history of hepatobiliary disease, and
(3) propensity for metastatic spread to distant sites (11–80% of cases).
More recently, the hvKP pathotype has been recognized as the cause
of a variety of serious community-acquired extrahepatic abscesses
and infections without liver involvement, including pneumonia,
meningitis, endophthalmitis (Fig. 156-1, middle), splenic abscess, and
necrotizing fasciitis. Survivors often suffer catastrophic morbidity, such
as vision loss and major neurologic sequelae.
K. pneumoniae subspecies rhinoscleromatis is the causative agent of FIGURE 156-1 Hypervirulent pathotype of K. pneumoniae (hvKP). Top: Abdominal
rhinoscleroma, a granulomatous mucosal upper-respiratory infection CT scan of a previously healthy 24-year-old Vietnamese man shows a primary
liver abscess (red arrow) with metastatic spread to the spleen (black arrow).
that progresses slowly (over months or years) and causes necrosis and (Courtesy of Drs. Chiu-Bin Hsaio and Diana Pomakova.) Middle: A previously healthy
occasionally obstruction of the nasal passages. K. pneumoniae subspecies 33-year-old Chinese man presented with endophthalmitis. (From AS Shon et al:
ozaenae has been implicated as a cause of chronic atrophic rhinitis and Virulence 4:107, 2013.) Bottom: A hypermucoviscous phenotype (which does not
rarely of invasive disease in compromised hosts. K. (Calymmatobacterium) necessarily equate with a mucoid phenotype) has been associated with hvKP
granulomatis is sexually transmitted and is the causative agent of gran- strains. A positive string test is shown. However, this test is not optimally sensitive
uloma inguinale (donovanosis) that results in chronic genital ulcers or specific. A more sensitive and specific marker is needed.
(Chap. 168). These Klebsiella pathotypes are usually isolated from
patients in tropical climates and are genomically distinct from both
cKP and hvKP.
Harrisons_20e_Part5_p0859-p1648.indd 1154 6/1/18 12:05 PM
■ INFECTIOUS SYNDROMES TREATMENT
1155
Pneumonia Although cKP accounts for only a small pro- Klebsiella Infections
portion of cases of community-acquired pneumonia in
Western countries (Chap. 121), cKP and K. oxytoca are com- cKP and K. oxytoca have similar antibiotic resistance pro-
mon causes of pneumonia among LTCF residents and hospitalized files. These species are intrinsically resistant to ampicillin
patients because of increased rates of oropharyngeal colonization in and ticarcillin and are inconsistently susceptible to nitro-
such individuals. Mechanical ventilation is an important risk factor. In furantoin. The prevalence of resistance to amoxicillin-clavulanate,
Asia and South Africa, community-acquired pneumonia due to hvKP fluoroquinolones, and TMP-SMX is generally >20%. Increasing
is becoming increasingly common and often occurs in younger patients resistance is mediated primarily by plasmid-encoded ESBLs (6–70%)
with no underlying disease. Klebsiella is also a common cause of pneu- and carbapenemases (1–18%), with the highest prevalences in
monia in severely malnourished children in developing countries. Eastern Europe and Asia and among health care–associated isolates.
As in all pneumonias due to enteric GNB, typical manifestations Furthermore, isolates of cKP that produce CTX-M ESBLs have been
include production of purulent sputum and evidence of airspace dis- obtained from ambulatory patients with no recent health care con-
ease. Presentation with earlier, less extensive infection is now more tact. Oral treatment for infection due to ESBL-producing Klebsiella is
common than is the classically described lobar infiltrate, bulging fis- more challenging than that for infection due to E. coli because of the
sure, and currant jelly sputum. Pulmonary infection due to hvKP that poor activity of nitrofurantoin, the lesser activity—and perhaps
has spread metastatically (e.g., from a hepatic abscess) usually includes lesser efficacy—of fosfomycin, and limited data on pivmecillinam.
nodular bilateral densities, more commonly in the lower lobes. Pulmo- Empirical treatment of serious cKP and K. oxytoca infections with
nary necrosis, pleural effusion, and empyema can occur with disease amikacin or a carbapenem may be prudent, depending on local
progression. susceptibility patterns and patient-specific risk factors.
Predictably, however, the ESBL-driven use of carbapenems has
UTI cKP accounts for only 1–2% of UTI episodes among otherwise selected for strains of cKP and K. oxytoca that express carbapen-
healthy adults but for 5–17% of episodes of UTI in patients with ana-
emases. The limited treatment options for carbapenem-resistant
tomical and functional abnormalities of the urinary tract, including
Klebsiella are similar to those described for E. coli. Tigecycline,
indwelling urinary catheter use (complicated UTI). UTI due to hvKP
the polymyxins (e.g., colistin), and ceftazidime-avibactam are the
presents more commonly as renal or prostatic abscess due to bacte-
most active agents in vitro. However, ceftazidime-avibactam is not
remic spread than as ascending infection from the urethra and bladder.
active against metallo-carbapenemases (e.g., NDM), and resistance
Abdominal Infection cKP causes a spectrum of abdom- to polymyxins is emerging (e.g., mcr-1-mediated colistin resistance).
CHAPTER 156 Diseases Caused by Gram-Negative Enteric Bacilli
inal infections similar to that caused by E. coli but is less fre- A lethal infection due to a pan-resistant K. pneumoniae isolate has
quently isolated from such infections than is E. coli. hvKP is a already been described in the United States. Combination therapy
common cause of monomicrobial community-acquired pyogenic liver is often used in this setting, and consultation with relevant experts
abscess; in the Asian Pacific Rim, it has been recovered with steadily is advised.
increasing frequency over the past two decades, replacing E. coli as the
most common pathogen causing this syndrome. hvKP also is increas-
ingly described as a cause of spontaneous bacterial peritonitis and PROTEUS INFECTIONS
splenic abscess. Proteus species are part of the colonic flora of a wide variety of mam-
Other Infections When cKP and K. oxytoca cause celluli- mals, birds, fish, and reptiles. The ability of these GNB to generate
tis or soft tissue infection, it most frequently involves devital- histamine from contaminated fish has implicated them in the patho-
ized tissue (e.g., decubitus and diabetic ulcers, burn wounds) genesis of scombroid (fish) poisoning (Chap. 451).
and immunocompromised hosts. cKP and K. oxytoca cause some cases Proteus mirabilis causes 90% of Proteus infections, which occur in the
of surgical site infection and nosocomial sinusitis as well as occasional community, LTCFs, and hospitals. Proteus vulgaris and Proteus penneri
cases of osteomyelitis contiguous to soft tissue infection, nontropical are associated primarily with infections acquired in LTCFs or hospi-
myositis, and meningitis (during the neonatal period and after neuro- tals. P. mirabilis colonizes healthy humans (prevalence, 50%), whereas
surgery). By contrast, hvKP has become an important cause of P. vulgaris and P. penneri are isolated primarily from individuals with
community-acquired monomicrobial necrotizing fasciitis, meningitis, underlying disease. By far the most common site of Proteus infection
endophthalmitis (Fig. 156-1, middle), and abscesses within the brain, is the urinary tract, where the principal known urovirulence factors of
subdural space, and epidural space, particularly in the Asian Pacific Proteus include adhesins, flagella, IgA-IgG protease, iron acquisition
Rim but also globally. Cytotoxin-producing strains of K. oxytoca have systems, and urease. Proteus less commonly causes infection at a vari-
been implicated as a cause of non–C. difficile antibiotic-associated hemor- ety of other extraintestinal sites.
rhagic colitis.
■ INFECTIOUS SYNDROMES
Bacteremia Klebsiella infection at any site can produce bactere-
mia. Infections of the urinary tract, respiratory tract, and abdomen UTI P. mirabilis causes only 1–2% of UTIs in healthy women, and
(especially hepatic abscess) each account for 15–30% of episodes of Proteus species collectively cause only 5% of hospital-acquired UTIs.
Klebsiella bacteremia. Intravascular device–related infections account However, Proteus is responsible for 10–15% of cases of complicated
for another 5–15% of episodes, and surgical site and miscellaneous UTI, primarily those associated with catheterization; indeed, Proteus
infections account for the rest. Klebsiella is an occasional cause of sepsis accounts for 20–45% of urine isolates from chronically catheterized
in neonates and of bacteremia in neutropenic patients. However, like patients. This high prevalence is due in part to bacterial production of
enteric GNB in general, Klebsiella rarely causes endocarditis or other urease, which hydrolyzes urea to ammonia and results in alkalization
endovascular infections. of the urine. Alkalization of urine, in turn, leads to precipitation of
organic and inorganic compounds, which contributes to formation of
■ DIAGNOSIS struvite and carbonate–apatite crystals, formation of biofilms on cathe-
Klebsiellae are readily isolated and identified in the laboratory. These ters, and/or development of frank calculi. Proteus becomes associated
organisms usually ferment lactose, although the subspecies rhinoscle- with the stones and biofilms; thereafter, it usually cannot be eradicated
romatis and ozaenae are nonfermenters and are indole-negative. hvKP without removal of the stones or catheter. Over time, staghorn calculi
usually possesses a hypermucoviscous phenotype (Fig. 156-1, bottom), may form within the renal pelvis and lead to obstruction and renal
although the sensitivity and specificity of the string test is less than failure. Although biologically plausible, clinical support is lacking for
optimal. A better diagnostic test for hvKP is needed. the concept that urine samples exhibiting unexplained alkalinity should
Harrisons_20e_Part5_p0859-p1648.indd 1155 6/1/18 12:05 PM
1156 be cultured, and isolation of a Proteus species (or other urea-splitting and are ICU residents are at greatest risk for infection. Enterobacter
organism) should prompt consideration of an evaluation for urolithiasis. causes a spectrum of extraintestinal infections similar to that described
for other GNB.
Other Infections Proteus occasionally causes pneumonia (primar-
ily in LTCF residents or hospitalized patients), nosocomial sinusitis, ■ INFECTIOUS SYNDROMES
intraabdominal abscesses, biliary tract infection, surgical site infection, Pneumonia, UTI (particularly catheter-related), intravascular device–
soft tissue infection (especially decubitus and diabetic ulcers), and oste- related infection, surgical site infection, and abdominal infection
omyelitis (primarily contiguous); in rare cases, it causes nontropical (primarily postoperative or related to devices such as biliary stents)
myositis. In addition, Proteus uncommonly causes neonatal meningitis, are the most common syndromes encountered. Nosocomial sinusitis,
with the umbilicus frequently implicated as the source; this disease is meningitis related to neurosurgical procedures (including use of intra-
often complicated by development of a cerebral abscess. Otogenic brain cranial pressure monitors), osteomyelitis, and endophthalmitis after
abscess also occurs. eye surgery are less frequent. Neonates (particularly those of low birth
Bacteremia Most episodes of Proteus bacteremia originate from weight) are at risk for C. sakazakii infection, including neonatal bacte-
the urinary tract; however, intravascular devices and any of the less remia, necrotizing enterocolitis, and meningitis (often complicated by
common sites of Proteus infection are also potential sources. Endovas- brain abscess or ventriculitis). Contaminated powdered infant formula
cular infection is rare, but when endocarditis occurs it can be persistent has been implicated as a source for such neonatal infections. The WHO
and destructive. Proteus species are occasional agents of sepsis in neo- recommends that, to reduce the initial number of bacteria, powdered
nates and of bacteremia in neutropenic patients. infant formula should be reconstituted with hot water (>70°C) and, to
limit replication of residual bacteria, the reconstituted formula should
■ DIAGNOSIS be stored at <5°C or its storage time minimized.
Proteus is readily isolated and identified in the laboratory. Most Enterobacter bacteremia can result from primary infection at any
strains are lactose-negative, produce H2S, and demonstrate character- anatomic site. In bacteremia of unclear origin, the contamination of
istic swarming motility on agar plates. P. mirabilis and P. penneri are IV fluids or medications, blood components or plasma derivatives,
indole-negative, whereas P. vulgaris is indole-positive. The inability catheter-flushing fluids, pressure monitors, and dialysis equipment
to produce ornithine decarboxylase differentiates P. penneri from should be considered, particularly in an outbreak setting. Enterobacter
P. mirabilis. can also cause bacteremia in neutropenic patients. Enterobacter endocar-
ditis is rare, occurring primarily in association with illicit IV drug use
or prosthetic valves.
TREATMENT
PART 5
Proteus Infections ■ DIAGNOSIS
Enterobacter is readily isolated and identified in the laboratory. Most
The intrinsic resistance of P. mirabilis to tetracyclines, cefazolin, strains are lactose-positive and indole-negative.
nitrofurantoin, polymyxins, and tigecycline renders treatment of
XDR isolates problematic. Acquired resistance to ampicillin (prev-
Infectious Diseases
alence range, 15–60%), fluoroquinolones (11–55%), and TMP-SMX TREATMENT
(20–50%) is common. Ampicillin-sulbactam tends to be more active,
with resistance prevalences of 6–18%. In the United States and Enterobacter Infections
Canada, the prevalence of ESBL production by P. mirabilis remains Significant antimicrobial resistance exists among Enterobac-
low (generally <5%). However, rates as high as 60% have been ter strains. Ampicillin, ampicillin-sulbactam, and first- and
reported from Asia. Isolates of P. mirabilis that produce CTX-M second-generation cephalosporins have little or no activity.
ESBLs have been recovered from ambulatory patients with no recent Extensive use of third-generation cephalosporins can induce or
health-care contact (see the section on the treatment of extraintestinal select for variants with stable derepression of AmpC β-lactamase,
E. coli infections for treatment considerations). P. vulgaris and P. pen- which confers resistance to these agents, to monobactams (e.g., az-
neri exhibit more extensive drug resistance than does P. mirabilis, and treonam), and—in many cases—to β-lactam/β-lactamase inhibitor
induction or selection of P. vulgaris variants with stable derepres- combinations. Resistance may emerge during therapy; in one study,
sion of chromosomal AmpC β-lactamase may occur. For critically this phenomenon was documented in 20% of clinical isolates. De
ill patients, carbapenems, fourth-generation cephalosporins (e.g., novo resistance should be considered when clinical deterioration
cefepime), ceftazidime-avibactam, ceftolozane-tazobactam, and follows initial improvement, and third-generation cephalosporins
amikacin generally display excellent activity against Proteus species should be avoided in the treatment of serious Enterobacter
(90–100% of isolates susceptible). infections.
Cefepime is stable in the presence of AmpC β-lactamases; thus, it
is a suitable option for treatment of Enterobacter infections so long as
ENTEROBACTER AND CRONOBACTER no coexistent ESBL is present. Detection of ESBLs in Enterobacter is
INFECTIONS difficult because of the presence of AmpC β-lactamase; nonetheless,
E. cloacae and E. aerogenes are responsible for most Enterobacter their prevalence (particularly in E. cloacae) is known to be variable
infections (65–75% and 15–25%, respectively); Cronobacter sakazakii, worldwide but is generally increasing and is now 5–50% overall.
Cronobacter malonaticus (formerly Enterobacter sakazakii), and Enterobacter This increase is evidenced by 2014 data from the National Health-
gergoviae are less commonly isolated (1% for each). Enterobacter spe- care Safety Network, which documented resistance to third- and
cies cause primarily health care–related infections. The organisms are fourth-generation cephalosporins in 36.1% of Enterobacter isolates
widely prevalent in foods, environmental sources (including equip- from central line–associated bloodstream infections in the United
ment at health care facilities), and a variety of animals. States. The prevalence of resistance has ranged from 15 to 40% for
These organisms colonize few healthy humans, but the percentage piperacillin-tazobactam and from 5 to 15% for colistin; it is more
colonized increases significantly with LTCF residence or hospitaliza- variable but generally higher for the fluoroquinolones. Fortunately,
tion. Although colonization is an important prelude to infection, direct carbapenems, ceftazidime-avibactam, ceftolozane-tazobactam, ami-
introduction via IV lines (e.g., contaminated IV fluids or pressure kacin, and tigecycline have generally retained excellent activity
monitors) also occurs. Extensive antibiotic resistance has developed in (90–99% of isolates susceptible). Once susceptibility data for a
Enterobacter species and probably has contributed to the emergence of patient’s isolate become available, it is advisable to de-escalate the
the organisms as prominent nosocomial pathogens. Individuals who antimicrobial regimen whenever possible.
have previously received antibiotic treatment, have comorbid disease,
Harrisons_20e_Part5_p0859-p1648.indd 1156 6/1/18 12:05 PM
SERRATIA INFECTIONS in LTCFs and hospitals—the settings in which nearly all Citrobacter 1157
S. marcescens causes the great majority (>90%) of Serratia infec- infections occur. Citrobacter species account for 1–2% of nosocomial
tions, with other species isolated only occasionally. Serratiae infections. The affected hosts are usually immunocompromised and/
are found primarily in the environment (including in health or have comorbid disease or disruption of skin or mucosal barriers.
care institutions), particularly in moist settings. Serratiae have been Citrobacter causes extraintestinal infections similar to those described
isolated from a variety of animals, insects, and plants but only infre- for other GNB.
quently from healthy humans. In LTCFs or hospitals, reservoirs for the
organisms include the hands and fingernails of health care personnel, ■ INFECTIOUS SYNDROMES
food, milk (on neonatal units), sinks, medical equipment or devices, IV The urinary tract accounts for 40–50% of Citrobacter infections. Less
solutions or parenteral medications (particularly those generated by commonly involved sites include the biliary tree (particularly with
compounding pharmacies), prefilled syringes and multiple-access stones or obstruction), the respiratory tract, surgical sites, soft tissue
medication vials (e.g., heparin, saline), blood products (e.g., platelets), (e.g., decubitus ulcers), the peritoneum, and intravascular devices.
hand soaps and lotions, irrigation solutions, and even disinfectants. Osteomyelitis (usually from a contiguous focus), adult central nervous
Infection results from either direct inoculation (e.g., via contami- system infection (from neurosurgical or other types of meningeal dis-
nated IV fluid or injected medications or recreational drugs) or colo- ruption), and myositis occur rarely. Citrobacter (primarily C. koseri) also
nization (primarily of the respiratory tract). Sporadic infection is most causes 1–2% of neonatal meningitis cases, of which 50–80% are com-
common, but outbreaks (often involving MDR strains in adult and neo- plicated by brain abscess. Further, case reports in adults suggest that
natal ICUs) also occur. Hygiene, medication-compounding standards, C. koseri infection has a predilection for abscess formation. Bacteremia
sterile technique, and infection control programs are critical measures is most often due to UTI, biliary/abdominal infection, or intravascular
to prevent infection. device infection. Citrobacter occasionally causes bacteremia in neutro-
The spectrum of extraintestinal infections caused by Serratia is sim- penic patients. Endocarditis and endovascular infections are rare.
ilar to that for other GNB. Serratia species are usually considered caus-
■ DIAGNOSIS
ative agents of health care–associated infection and account for 1–3%
Citrobacter species are readily isolated and identified; 35–50% of iso-
of hospital-acquired infections. However, population-based laboratory
lates are lactose-positive, and 100% are oxidase-negative. C. freundii is
surveillance studies in Canada and Australia have demonstrated that
indole-negative, whereas C. koseri is indole-positive.
community-acquired Serratia infections occur more commonly than
was previously appreciated. Serratia also is one of the pathogens asso-
ciated with chronic granulomatous disease. TREATMENT
CHAPTER 156 Diseases Caused by Gram-Negative Enteric Bacilli
■ INFECTIOUS SYNDROMES Citrobacter Infections
The respiratory tract, the genitourinary tract, intravascular devices,
C. freundii is more extensively antibiotic-resistant than is C. koseri.
the eye (contact lens–associated keratitis and other ocular infections),
More than 90% of isolates are resistant to ampicillin and to first- and
surgical wounds, and the bloodstream (from contaminated infusions)
second-generation cephalosporins, and >50% of strains are resistant
are the most common sites of Serratia infection; the former five sites are
to ampicillin-sulbactam. Citrobacter species (except C. koseri) possess
the most common sources of Serratia bacteremia. Soft tissue infections
AmpC β-lactamases; induction or selection of variants with stable
(including myositis, fasciitis, mastitis), osteomyelitis, abdominal and
derepression may occur during therapy. The prevalence of resistance
biliary tract infections (postprocedural), and septic arthritis (primar-
generally ranges from 15 to 35% for third-generation cephalospo-
ily from intraarticular injections) occur less commonly. Serratiae are
rins, from 5 to 15% for piperacillin-tazobactam and fluoroquino-
uncommon causes of neonatal or postsurgical meningitis and of bacte-
lones, and from 5 to 20% for TMP-SMX. The prevalence of ESBL
remia in neutropenic patients. Endocarditis is rare.
production is <5%. Carbapenems, amikacin, cefepime, tigecycline,
■ DIAGNOSIS ceftazidime-avibactam, ceftolozane-tazobactam, fosfomycin, and
Serratiae are readily cultured and identified by the laboratory and are colistin are most active (>90% of isolates susceptible).
usually lactose- and indole-negative. The red pigmentation of some
S. marcescens strains and Serratia rubidaea can produce distinctive clin- MORGANELLA AND PROVIDENCIA
ical findings (e.g., pink breast milk or hypopyon; pseudohemoptysis).
INFECTIONS
M. morganii, Providencia stuartii, and (less frequently) Providencia rettgeri
TREATMENT are the members of their respective genera that cause human infections.
The epidemiologic associations, pathogenic properties, and clinical
Serratia Infections manifestations of these organisms resemble those of Proteus species.
Most Serratia strains (>80%) are resistant to ampicillin, Morganella and Providencia occur more commonly among LTCF resi-
amoxicillin-clavulanate, ampicillin-sulbactam, first-generation dents than among hospitalized patients, largely resulting from chronic
cephalosporins, cephamycins, nitrofurantoin, and colistin. urinary-catheter use. In settings with extensive use of polymyxins
Induction or selection of variants with stable derepression of chromo- and tigecycline, these organisms may become increasingly common
somal AmpC β-lactamases may develop during therapy. Both in the because of their intrinsic resistance to these agents.
United States and globally, the prevalence of ESBL-producing isolates
■ INFECTIOUS SYNDROMES
is generally low (<5%), but rates of 20–30% have been reported in
These species are primarily urinary tract pathogens, causing UTIs that
Asia and Latin America. Acquisition of carbapenemase-encoding
are most often associated with long-term (>30-day) catheterization.
genes is uncommon but increasing. For critically ill patients, carbap-
Such infections commonly lead to biofilm formation and catheter
enems, amikacin, ceftazidime-avibactam, and ceftolozane-tazobactam
encrustation (sometimes causing catheter obstruction) or the devel-
are most reliably active (>90% susceptible).
opment of struvite bladder or renal stones (sometimes causing renal
obstruction and serving as foci for relapse). Morganella is also com-
CITROBACTER INFECTIONS monly isolated from snakebite infection.
C. freundii and Citrobacter koseri cause most human Citrobacter infec- Other, less common infectious syndromes include surgical site
tions, which are epidemiologically and clinically similar to Enterobacter infection, soft tissue infection (primarily involving decubitus and
infections. Citrobacter species are commonly present in water, food, soil, diabetic ulcers), burn site infection, pneumonia (particularly ventilator-
and certain animals. Citrobacter is part of the normal fecal microbiota associated), intravascular device infection, and intraabdominal infec-
in a minority of healthy humans, but colonization rates are higher tion. Rarely, the other extraintestinal infections described for GNB also
Harrisons_20e_Part5_p0859-p1648.indd 1157 6/1/18 12:05 PM
1158 occur. Bacteremia is uncommon; when it does occur, any infected site the setting of severe sepsis, fluoroquinolones, third- and fourth-
can serve as the source, but the urinary tract accounts for most cases, generation cephalosporins, carbapenems, and amikacin—either
with the next most common sources being surgical site, soft tissue, and alone or in combination—are the safest choices pending suscepti-
hepatobiliary infections. bility data.
■ DIAGNOSIS
M. morganii and Providencia are readily isolated and identified. Nearly INFECTIONS CAUSED BY MISCELLANEOUS
all isolates are lactose-negative and indole-positive. GENERA
Species of Hafnia, Kluyvera, Cedecea, Pantoea, Ewingella, Leclercia,
TREATMENT Raoultella, and Photorhabdus are occasionally isolated from diverse
clinical specimens, including blood, sputum, urine, cerebrospinal fluid,
Morganella and Providencia Infections joint fluid, bile, and wounds. These organisms are rare and usually
cause infection in compromised hosts or in association with an invasive
Morganella and Providencia may be extensively resistant to procedure or foreign body. Cephalosporinases from Kluyvera have been
antibiotics. Most (or all) isolates are resistant to ampicillin, implicated as the progenitors of CTX-M ESBLs. Kluyvera and Raoultella
ampicillin-sulbactam, first-generation cephalosporins, may produce carbapenemases.
nitrofurantoin, fosfomycin, tigecycline, and the polymyxins; treat-
ment of XDR strains is especially challenging. The β-lactamase ■ FURTHER READING
inhibitor tazobactam increases susceptibility to β-lactam agents, but Boisen N et al: Shiga toxin 2a and enteroaggregative Escherichia coli—A
sulbactam and clavulanic acid do not. Morganella and Providencia deadly combination. Gut Microbes 6:272, 2015.
possess inducible AmpC β-lactamases; clinically significant induc- Chen L et al: Notes from the field: Pan-resistant New Delhi
tion or selection of stably derepressed mutants may develop during metallo-beta-lactamase–producing Klebsiella pneumoniae—Washoe
therapy. The prevalence of resistance generally ranges from 10 to County, Nevada, 2016. MMWR Morb Mortal Wkly Rep 66:33, 2017.
30% for the third-generation cephalosporins, from 10 to 40% for Croxen MA et al: Recent advances in understanding enteric patho-
fluoroquinolones, and from 20 to 40% for TMP-SMX; the prevalence genic Escherichia coli. Clin Microbiol Rev 26:822, 2013.
is more widely variable for piperacillin-tazobactam. The prevalence Dale AP, Woodford N: Extra-intestinal pathogenic Escherichia coli
of ESBL-producing isolates is <5%. Carbapenems, amikacin, cefe- (ExPEC): Disease, carriage and clones. J Infect 71:615, 2015.
pime, ceftazidime-avibactam, and ceftolozane-tazobactam are the Holy O, Forsythe S: Cronobacter spp. as emerging causes of health-
most active agents (>90% of isolates susceptible). Removal of a colo- care-associated infection. J Hosp Infect 86:169, 2014.
nized urinary catheter or stone is critical for eradication of UTI. Khatri A et al: Community-acquired pyelonephritis in pregnancy
PART 5
caused by KPC-producing Klebsiella pneumoniae. Antimicrob Agents
EDWARDSIELLA INFECTIONS Chemother 59:4375, 2015.
E. tarda is the only member of the genus Edwardsiella that is Lim C et al: Epidemiology and burden of multidrug-resistant
associated with human disease. This organism is found pre- bacterial infection in a developing country. Elife Sep 6:5, 2016.
PMCID: PMC5030096.
Infectious Diseases
dominantly in freshwater and marine environments and in
the associated aquatic animal species. Human acquisition occurs pri- Shields RK et al: Clinical outcomes, drug toxicity, and emergence
marily from interaction with these reservoirs or ingestion of inade- of ceftazidime-avibactam resistance among patients treated for
quately cooked aquatic animals. E. tarda infection is rare in the United carbapenem-resistant Enterobacteriaceae infections. Clin Infect Dis
States, where acquisition occurs mainly along the Gulf of Mexico; 63:1615, 2016.
recently reported cases are mostly from Asia. This pathogen shares Shon AS et al: Hypervirulent (hypermucoviscous) Klebsiella pneumo-
clinical features with Salmonella species (as an intestinal pathogen; niae: A new and dangerous breed. Virulence 4:107, 2013.
Chap. 160), Vibrio vulnificus (as an extraintestinal pathogen; Chap. 163), Tamma PD, Rodriguez-Bano J: The use of noncarbapenem β-lactams
and Aeromonas hydrophila (as both an intestinal and an extraintestinal for the treatment of extended-spectrum β-lactamase infections. Clin
pathogen; Chap. 153). Infect Dis 64:942, 2017.
■ INFECTIOUS SYNDROMES
157 Acinetobacter Infections
Gastroenteritis is the predominant infectious syndrome (50–80% of
infections). Self-limiting watery diarrhea is most common, but severe
colitis also occurs. The most common extraintestinal infection is wound
Rossana Rosa, L. Silvia Munoz-Price
infection due to direct inoculation, which is often associated with fresh-
water, marine, or snakebite injuries. Other infectious syndromes result
from invasion of the gastrointestinal tract and subsequent bacteremia.
Most afflicted hosts have comorbidities (e.g., hepatobiliary disease, ■ DEFINITION
iron overload, cancer, or diabetes mellitus). A primary bacteremic syn- Acinetobacter species were first described in 1911 and named Micrococcus
drome, sometimes complicated by meningitis, has a 40% case–fatality calcoaceticus. Thereafter, the genus was renamed multiple times; since
rate. Visceral (primarily hepatic) and intraperitoneal abscesses also 1950, it has been known as Acinetobacter. Acinetobacter species are
occur, as do endocarditis and empyema. gram-negative, oxidase-negative, nonmotile, nonfermenting coccoba-
cilli that are easily recovered on standard culture media. Differentiation
■ DIAGNOSIS among Acinetobacter species on the basis of phenotypic characteristics
Although E. tarda can readily be isolated and identified, most laborato- alone is very difficult. Molecular-based methods such as matrix-
ries do not routinely seek to identify it in stool samples. Production of assisted laser desorption–ionization–time-of-flight mass spectrometry
hydrogen sulfide is a characteristic biochemical property. (MALDI-TOF-MS) and quantitative real-time polymerase chain reac-
tion (PCR) are usually necessary to identify Acinetobacter baumannii, the
most clinically relevant species of the genus.
TREATMENT
Edwardsiella Infections ■ ETIOLOGY AND EPIDEMIOLOGY
Acinetobacter species are naturally encountered in water and soil and
E. tarda is susceptible to most antimicrobial agents appropriate have also been recovered from fruits and vegetables. In humans,
for use against GNB. Gastroenteritis is generally self-limiting, Acinetobacter can be found on the skin and in the respiratory and gas-
but treatment with a fluoroquinolone may hasten resolution. In trointestinal tracts. A. baumannii is capable of surviving environmental
Harrisons_20e_Part5_p0859-p1648.indd 1158 6/1/18 12:05 PM
desiccation for weeks; this characteristic is important from an infection- to this organism include a history of alcohol abuse, diabetes mellitus, 1159
control perspective as it allows this organism to persist in the hospital smoking, and chronic lung disease.
environment and on equipment.
War Zone–Associated Infections Infections caused by
Acinetobacter was historically considered a pathogen of hot
Acinetobacter in war zones include skin and soft tissue infections asso-
and humid climates. In recent years, however, hospital out-
ciated with traumatic injuries and bloodstream infections. Outbreak
breaks caused by A. baumannii have been reported world-
investigations of A. baumannii infections among military personnel
wide, even in temperate climates. In the United States, the Centers for
returning from Iraq and Afghanistan suggested the acquisition of A.
Disease Control and Prevention (CDC) estimates that 12,000 Acineto-
baumannii in field hospitals rather than colonization of the skin before
bacter infections occur every year, 7300 of which are caused by multi-
an injury. This view is supported by the recovery of A. baumannii iso-
drug-resistant strains, with 500 attributable deaths. The increase in the
lates with similar genetic characteristics from inanimate surfaces in
number of infections with A. baumannii is suspected to be due to the
field hospitals and from patients.
rapid spread of certain genetically distinct lineages; of the three inter-
national clonal lineages (ICLs), ICL I and ICL II are multidrug resistant. Disaster Medicine A. baumannii is linked to infections among
The predominance of these lineages remains unexplained, although it victims of trauma during tsunamis, earthquakes, and terrorist attacks.
has been proposed that this population structure is the result of two The types of infections most frequently observed in these settings are
waves of expansion. The first wave followed a bottleneck (possibly soft tissue injuries, but bloodstream infections and pneumonia have
linked to a restricted ecologic niche) that occurred in the distant past. also been reported. In addition, outbreaks of A. baumannii infection in
The second wave is ongoing and is being driven by the rapid expan- ICUs caring for disaster victims have been described.
sion of a limited number of multidrug-resistant clones.
Analysis of the A. baumannii pangenome (the sum of the core and ■ PATHOGENESIS
dispensable genomes) has shown that its organization is charac- Mechanisms of pathogenesis and virulence in Acinetobacter species have
terized by a small core genome and a large accessory or dispos- not been fully elucidated. However, A. baumannii seems to have greater
able genome. This organization reflects A. baumannii’s high plasticity, virulence potential than other Acinetobacter species, as evidenced by its
which enables it to acquire exogenous genetic material. With few ability to grow at 37°C and to resist uptake by macrophages.
exceptions, gene functions associated with virulence are found in the Initial A. baumannii colonization of the host and the environment is
core genome; this observation suggests a limited role for the acquisition facilitated by the organism’s ability to adhere to surfaces and human
of new virulence traits in the recent nosocomial expansion of A. bau- cells and to create biofilms. The ability to form a biofilm is phenotyp-
mannii clones. Genes associated with resistance to antimicrobial agents ically associated with exopolysaccharide production and pilus forma-
CHAPTER 157 Acinetobacter Infections
are found in both the species core genome and the accessory genome. tion. A quorum-sensing molecule encoded by the abaI autoinducer
In the accessory genome, these genes have been found in alien islands, synthase gene has been implicated in A. baumannii biofilm formation
often flanked by integrases, transposases, or insertion sequences. This on abiotic surfaces. Outer-membrane porins appear to mediate cell
pattern suggests possible acquisition by horizontal gene transfer from apoptosis. A. baumannii can survive in harsh environments within the
other Acinetobacter strains or even from different bacterial species pres- host and on inanimate surfaces by modifying the structure of its lipid
ent in the immediate environment. Acquisition of these antimicrobial A, with a consequent decrease in susceptibility to antibiotics and anti-
resistance genes is hypothesized to have led to the recent rapid expan- microbial peptides and an increase in survival upon desiccation.
sion of highly homogeneous clonal lineages, whose main difference Acinetobacter species produce an extracellular capsule that protects
from nonclonal A. baumannii appears to be their antimicrobial the bacteria from external threats, including complement-mediated
resistance. killing. Studies of mouse models showed that Acinetobacter species can
increase capsule production in the presence of subinhibitory levels of
Health Care–Associated Infections Infections caused by
antibiotic—an ability that leads to increased resistance to complement-
A. baumannii occur frequently among patients admitted to intensive
mediated killing and a hypervirulent phenotype.
care units (ICUs). Risk factors for colonization and infection with this
Phospholipase C and phospholipase D have been identified as viru-
pathogen include nursing home residence, prolonged ICU stay, central
lence factors in A. baumannii. These enzymes exert cytotoxic effects on
venous catheterization, tracheostomy, mechanical ventilation, enteral
epithelial cells and facilitate their invasion.
feedings, and treatment with third-generation cephalosporins, fluoro-
Iron-acquisition systems are also important virulence mechanisms in
quinolones, and carbapenems. Acquisition of carbapenem-resistant A.
A. baumannii. Through secretion of siderophores (low-molecular-mass
baumannii is most common among patients exposed to carbapenems.
ferric-binding compounds), A. baumannii is able to grow despite iron
Spread of A. baumannii across different regions is facilitated by the
deficiencies in the surrounding environment (e.g., in the human host).
movement of patients between health care systems and throughout the
Several protein-secretion systems have been identified in A. bau-
continuum of health care. Within the hospital, environmental spread of
mannii. The most recently described is a type II secretion system. The
A. baumannii occurs as a result of inappropriate hand hygiene among
substrate for this system, the LipA lipase, is required for growth on
workers providing health care for infected or colonized patients and the
medium containing lipids as a sole carbon source. Mutants lacking
contamination of hospital equipment, such as respiratory therapy and
the genes for the type II secretion system or its substrate exhibit defec-
ventilation equipment. The air surrounding the patient may also play
tive in vivo growth in a neutropenic murine model of bacteremia.
a role in environmental colonization with A. baumannii, especially in
A. baumannii also has a type VI secretion system whose primary func-
inpatient areas without physical barriers between patients and with an
tion seems to be to secrete antibacterial toxins that kill competing bac-
inadequate number of air exchanges.
teria, including other strains in the same species.
A. baumannii strains identified during hospital outbreaks are typi-
The type V autotransporter system has been characterized in
cally resistant to more antibiotic classes than strains from the commu-
A. baumannii. In a murine systemic model of Acinetobacter infection, the
nity. The prevalence of colonization with A. baumannii at the time of
Acinetobacter trimeric autotransporter mediates biofilm formation and
admission or during a stay in a long-term acute-care hospital (LTACH)
maintenance; adherence to extracellular matrix components such as
or nursing home is variable and depends on regional flora. Outbreaks
collagen I, II, and IV; and virulence.
of A. baumannii in acute-care hospitals and LTACHs that “share”
Outer-membrane vesicles (OMVs) play a special role in protein
patients have been described in Ohio, Michigan, Illinois, and Indiana.
secretion. Many A. baumannii strains secrete OMVs containing vari-
Community-Acquired Infections Community-acquired infec- ous virulence factors, including outer-membrane protein A (OmpA),
tions caused by Acinetobacter have been described in Australia and proteases, and phospholipases. The membrane proteins in OMVs are
Asia. Few cases have been reported in regions with a temperate cli- responsible for eliciting a potent innate immune response. Several
mate, and even those few cases have taken place during warm and studies have shown that A. baumannii OMVs could be used as an acel-
humid months. Risk factors for community-acquired pneumonia due lular vaccine to effectively control A. baumannii infections.
Harrisons_20e_Part5_p0859-p1648.indd 1159 6/1/18 12:05 PM
1160 Nosocomial strains of Acinetobacter can deploy multiple mechanisms their infections as evolving from an edematous peau d’orange appear-
of resistance, including alterations in porins and efflux pumps and ance to a sandpaper appearance with overlying vesicles and then to
expression of β-lactamases. More specifically, Acinetobacter species can a necrotizing process with hemorrhagic bullae. Other case series have
reduce the expression of porins, thus hindering the passage of β-lactam also included necrotizing fasciitis. A. baumannii is an important patho-
antibiotics into the periplasmic space. These species can overexpress gen in burn units worldwide. Large burns provide ideal conditions for
bacterial efflux pumps and decrease the concentration of β-lactam A. baumannii and facilitate patient-to-patient transmission. The pres-
antibiotics in the periplasmic space. Efflux pumps can also actively ence of A. baumannii in wounds contributes to healing delays and graft
remove quinolones, tetracyclines, chloramphenicol, disinfectants, and loss. In addition, wound colonization is a risk factor for bloodstream
tigecycline. Acinetobacter species possess chromosomally encoded infections among patients with extensive burn injuries.
cephalosporinases and are capable of acquiring β-lactamases, including A. baumannii infections resulting from trauma to soft tissues in the
serine and metallo-β-lactamases. AmpC β-lactamases are class C β- setting of natural disasters, such as tsunamis and earthquakes, have
lactamases intrinsic to all A. baumannii strains. Although these enzymes been reported. The implication is that A. baumannii should be con-
are expressed at low levels and are not inducible, the addition of sidered in the differential diagnosis of soft tissue infections following
the insertion sequence ISAba1 next to the AmpC gene increases β- exposure to tropical and subtropical environments.
lactamase production, with resulting resistance to cephalosporins.
Carbapenem resistance in Acinetobacter species is mostly tied to the
Urinary Tract Infections A. baumannii is an infrequent cause
of urinary tract infections. The majority of cases reported are catheter-
emergence of Ambler class D oxacillinases of group 2d, some of which
associated infections, reflecting the ability of A. baumannii to form
are intrinsic and chromosomal (e.g., OXA-51-like) while others are
biofilms on these devices. A few reports have described community-
acquired and are found in plasmids or are chromosomally encoded
acquired infections occurring in the setting of nephrolithiasis and after
(e.g., OXA-23-like, 24 [33-like, 40-like], 58-like, 143-like, and 235-like).
renal transplantation.
■ CLINICAL MANIFESTATIONS Meningitis Central nervous system infections with A. baumannii
have been reported in the context of outbreaks, traumatic injuries,
Pneumonia A. baumannii is a notorious cause of nosocomial pneu-
neurosurgical procedures, and external ventricular drains. One case
monia, most frequently among patients requiring prolonged mechanical
series described a petechial rash in up to 30% of patients. Acinetobacter
ventilation. The onset of disease tends to be later than that caused by
species may look similar to Neisseria meningitidis on a Gram’s stain of
other gram-negative bacilli; however, clinical symptoms of hospital-
cerebrospinal fluid; both appear as gram-negative paired cocci.
acquired or ventilator-associated pneumonia due to A. baumannii are
similar to those of nosocomial or ventilator-associated pneumonia due Other Miscellaneous Infections A few cases of A. baumannii
to other nosocomial pathogens. Thus, the most common indicators of keratitis associated with the use of contact lenses have been reported.
PART 5
infection include fever and increased sputum production. The positiv- Cases of native- and prosthetic-valve endocarditis have also been
ity of respiratory cultures in most cases may present a challenge for the described.
clinician, since airway colonization with A. baumannii is a risk factor
for infection itself. Radiologic findings are nonspecific and can include TREATMENT
Infectious Diseases
lobar consolidations and pleural effusions, but cavitations are rarely
seen. The crude mortality rates associated with nosocomial pneumonia Acinetobacter Infections
due to A. baumannii are reported to be as high as 65%. However, since Treatment of Acinetobacter infections is challenging because Acineto-
these infections occur in debilitated patients, their attributable mortal- bacter can develop resistance to most available antibiotics. Therefore,
ity has been difficult to establish. the choice of empirical therapy should be based on local epidemiol-
Community-acquired pneumonia due to A. baumannii is a relatively ogy and the patient’s colonization status. Definitive therapy should
rare entity. Its clinical presentation is characterized by fever, severe be determined by antimicrobial susceptibility testing. Antimicrobial
respiratory symptoms, and multiple-organ dysfunction. Patients fre- options for the management of infections caused by A. baumannii are
quently have a cough productive of purulent sputum, shortness of displayed in Table 157-1.
breath, and chest pain. Imaging studies usually show lobar consolida- Acinetobacter species possess intrinsic β-lactamases that inactivate
tion. Mortality rates associated with this process are >50%. first- and second-generation cephalosporins. Through acquisition
Bloodstream Infections Bloodstream infections due to of extended-spectrum β-lactamases, the organisms can also become
A. baumannii are most frequent among ICU patients and usually occur resistant to third- and fourth-generation cephalosporins. Neverthe-
in the presence of a central venous catheter or as a secondary complica- less, when the isolate is susceptible, β-lactam agents are the drugs of
tion of hospital-acquired or ventilator-associated pneumonia. Polymi- choice for the treatment of A. baumannii. Among β-lactamase inhib-
crobial growth has been reported in 20–36% of bacteremia episodes. itors, sulbactam is active against A. baumannii and is as effective as
Fever is the most common sign of infection (developing in >95% of carbapenems and polymyxins.
cases), and presentation with septic shock and disseminated intravas- Carbapenems have been the preferred drugs for treatment of
cular coagulopathy has been described in as many as 25 and 30% of invasive or hospital-acquired infections. Unfortunately, surveillance
patients, respectively. A. baumannii bloodstream infections often result data from U.S. hospitals show that up to 50% of A. baumannii isolates
in higher hospitalization costs and longer ICU stays. Crude mortality recovered from ICUs are carbapenem resistant, and rates of carba-
rates from this infection are as high as 40%; however, rates can be as penem resistance are even higher around the world.
high as 70% from infections caused by carbapenem-resistant isolates. Aminoglycosides are of limited utility against A. baumannii
In patients with infections caused by extremely drug-resistant strains, because of toxicity and lack of lung penetration. Inhaled formula-
poor outcomes are thought to be driven by delays in the initiation of tions of tobramycin have been used with variable success.
adequate antimicrobial therapy. Polymyxins are cationic detergents that fell out of use as a result
of nephrotoxicity and neurotoxicity. In vitro, they are the most active
Skin and Soft Tissue Infections Acinetobacter species have been agents against carbapenem-resistant A. baumannii. Colistin has been
described as part of the skin flora, yet the majority of the organisms from used in both intravenous and inhaled formulations, although the
this genus that colonize the skin are not those associated with nosocomial optimal dosage has not yet been determined.
infections. Discerning infection from wound colonization is challeng- Tigecycline is a glycylcycline with clinical activity against A.
ing. Gunshot wounds and the presence of orthopedic external-fixation baumannii. It reaches only low serum concentrations and therefore
devices are common among patients with combat trauma–associated cannot be used for bloodstream infections. The susceptibility of iso-
A. baumannii skin and soft tissue infections. The report on a case series lates is variable, especially in outbreak settings, and the emergence
of eight U.S. military patients described the clinical presentation of of resistance during treatment has been reported.
Harrisons_20e_Part5_p0859-p1648.indd 1160 6/1/18 12:05 PM
TABLE 157-1 Therapeutic Options for the Management of In vitro data favor combination therapy with colistin in many dif- 1161
Multidrug-Resistant Acinetobacter baumannii Infections ferent regimens containing a carbapenem (imipenem, meropenem),
ANTIBIOTIC DOSINGa COMMENTS rifampin, minocycline, ceftazidime, azithromycin, doxycycline,
Sulbactam 3–9 g/d (9–27 g/d if Unavailable as single drug in
trimethoprim-sulfamethoxazole, or ampicillin-sulbactam. However,
given in combination many countries (including the clinical data have not shown such combination therapy to be supe-
with ampicillin) United States) rior to colistin alone.
Meropenem 2 g q8h Prolonged infusion (3–4 h) has
been used; limited data ■ COMPLICATIONS AND PROGNOSIS
Imipenem 500 mg q6h Prolonged infusion (3–4 h) has Infections caused by A. baumannii can be associated with high mortality
been used; limited data rates. Factors contributing to higher mortality are thought to include
Colistin Loading dose of 5 mg/ Optimal dosing regimen unknown severity of the patient’s underlying illness and drug resistance in the
kg followed by 2.5–5.0 Inhaled formulation has been infecting strain.
mg/kg per day of colistin used as adjunct treatment in
base given in 2–4 lung infections. ■ INFECTION CONTROL AND PREVENTION
divided doses
Acinetobacter species are capable of surviving on hospital surfaces for
Polymyxin B 1.5–3 mg/kg q12h prolonged periods. In the hospital environment, A. baumannii has been
Tigecycline 100-mg loading dose Low serum concentrations and associated with establishment of a fecal patina; this term refers to a coat-
followed by 50 mg q12h bacteriostatic activity limit use in
bacteremia.
ing of enteric organisms that can cover the skin of colonized patients
and extend to their surrounding environment. Concentrations of enteric
Minocycline 100 mg q12h Loading dose of 200 mg IV has
been used. organisms are highest in the colonized patient’s rectum, with spread
in a target-like concentric pattern covering the patient’s body and
Amikacin 15 mg/kg qd Inhaled formulation of tobramycin
has been used as adjunct the surrounding environment. High-frequency touch areas in rooms
treatment in lung infections. occupied by patients colonized with A. baumannii are more likely to be
Rifampin 600 mg qd or 600 mg Use in combination therapy contaminated. The hands, gloves, and gowns of health care workers can
q12h be contaminated after entry into the room of a patient colonized with A.
Fosfomycin 4 g q12h PO Use in combination therapy baumannii (Fig. 157-1).
IV formulation not available in Outbreaks caused by A. baumannii are frequently mono- or oligo-
the United States clonal. A common source of infection has been identified in ~50% of
CHAPTER 157 Acinetobacter Infections
outbreaks. These sources include respiratory therapy equipment, the
All drugs are given by the IV route unless otherwise stated.
a
hands of health care workers, bedside humidifiers, warm bathwater,
hospital-prepared distilled water, bedpans, urine jugs, heparinized
Minocycline is a tetracycline that has a bacteriostatic effect on A. saline solution, mattresses, reusable pressure transducers in arterial
baumannii. Synergistic and bactericidal activity has been noted when lines, and fluids used for pressure lavage of wounds.
minocycline is used in combination with colistin or a carbapenem. Control of multidrug-resistant Acinetobacter outbreaks starts with
Fosfomycin is an inhibitor of peptidoglycan synthesis that has early recognition, with subsequent halting of the spread of infec-
no direct activity against A. baumannii but has been observed to tion throughout a facility and prevention of the establishment of an
be synergistic in vitro in combination with colistin or sulbactam. endemic strain. It is important to identify the outbreak strain and
Clinical data have shown higher rates of microbiologic cure, but no differentiate it from non-outbreak strains so that infection control
differences in clinical response, with combinations of fosfomycin activities can be better targeted. Traditionally, the strain was identified
and colistin. with phenotypic typing systems (biotyping) or by determination of
-Hand hygiene
-Contact precautions
Health care worker’s
hands
A. baumannii– A. baumannii–
positive patient Shared equipment
negative patient
Health care
-Physical separation from environment
-Physical separation from
A. baumannii–negative
A. baumannii–positive
patients
-Daily and terminal patients
-Rectal surveillance
disinfection -Cohorting nursing
-Cohorting nursing
personnel
personnel
-Limits on shared equipment -Chlorhexidine baths
-Chlorhexidine baths
-Disinfection of equipment -Antibiotic stewardship
-Antibiotic stewardship
between patients
FIGURE 157-1 Strategies for the prevention of dissemination of Acinetobacter baumannii in health care facilities.
Harrisons_20e_Part5_p0859-p1648.indd 1161 6/1/18 12:05 PM
1162 antimicrobial susceptibility patterns. Molecular typing systems have potentially prevent gastric malignancy and peptic ulceration. In con-
ushered in an era of molecular epidemiology that allows more precise trast, increasing evidence indicates that lifelong H. pylori colonization
identification of outbreak strains through use of techniques such as may offer some protection against complications of gastroesophageal
ribotyping, pulse-field gel electrophoresis, repetitive sequence-based reflux disease (GERD), including esophageal adenocarcinoma. Recent
PCR, and multilocus sequence testing. research has focused on whether H. pylori colonization is also a risk
During outbreaks, the simultaneous introduction of multiple (“bun- factor for some extragastric diseases and whether it is protective against
dled”) measures makes it difficult to assess the impact of each individ- some recently emergent medical problems, such as childhood-onset
ual measure. These interventions include aggressive cleaning of the asthma and other allergic and metabolic conditions.
general environment, active surveillance, contact isolation of colonized
or infected patients, cohorting of medical staff, reinforcement of com- ■ ETIOLOGIC AGENT
pliance with hand hygiene by health care workers, and use of aseptic Helicobacter pylori H. pylori is a gram-negative bacillus that
care devices. has naturally colonized humans for at least 100,000 years, and prob-
Colonization with A. baumannii is a strong predictor of subsequent ably throughout human evolution. It lives in gastric mucus, with a
clinical infection by this organism. Exposure to carbapenems is a risk proportion of the bacteria adherent to the mucosa and possibly a
factor for initial acquisition of this pathogen; therefore, efforts to curtail very small number of the organisms entering cells or penetrating
unnecessary use of antibiotics are fundamental to the prevention of the mucosa; the organism’s distribution is never systemic. Its spiral
A. baumannii colonization of patients and the organism’s establishment shape and flagella render H. pylori motile in the mucus environment.
in health care facilities. The organism has several acid-resistance mechanisms, most notably
■ FURTHER READING a highly expressed urease that catalyzes urea hydrolysis to produce
Adams-Haduch JM et al: Molecular epidemiology of carbapenem- buffering ammonia. H. pylori is microaerophilic (i.e., requires low
nonsusceptible Acinetobacter baumannii in the United States. J Clin levels of oxygen), is slow-growing, and requires complex growth
Microbiol 49:3849, 2011. media in vitro.
Antunes LC et al: Acinetobacter baumannii: evolution of a global Other Helicobacter Species A very small proportion of gastric
pathogen. Pathog Dis 71:292, 2014. Helicobacter infections are due to species other than H. pylori, possibly
Dexter C et al: Community-acquired Acinetobacter baumannii: Clinical acquired as zoonoses. These non-pylori gastric helicobacters are asso-
characteristics, epidemiology and pathogenesis. Expert Rev Anti ciated with low-level inflammation and occasionally with disease. In
Infect Ther 13:567, 2015. immunocompromised hosts, several nongastric (intestinal) Helicobacter
Garnacho-Montero J: Optimum treatment strategies for carbapenem- species can cause disease with clinical features resembling those of
resistant Acinetobacter baumannii: Bacteremia. Expert Rev Anti Infect
PART 5
Campylobacter infections; these species are covered in Chap. 162.
Ther 13:769, 2015.
Lee CR et al: Biology of Acinetobacter baumannii: Pathogenesis, antibi- ■ EPIDEMIOLOGY
otic resistance mechanisms, and prospective treatment options. Front
Cell Infect Microbiol 7:55, 2017. Prevalence and Risk Factors The prevalence of
Infectious Diseases
Munoz-Price LS: Controlling multi-drug resistant gram-negative H. pylori among adults is <30% in most parts of the United
bacilli in your hospital: A transformational journey. J Hosp Infect States and in other developed countries as opposed to >80% in
89:254, 2015. some developing countries. In the United States, prevalence varies with
Munoz-Price LS, Weinstein RA: Acinetobacter infection. N Engl J Med age: up to 50% of 60-year-old persons, ~20% of 30-year-old persons,
358:1271, 2008. and <10% of children are colonized. H. pylori is usually acquired in
Peleg AY et al: Acinetobacter baumannii: Emergence of a successful childhood. The age association is due mostly to a birth-cohort effect
pathogen. Clin Microbiol Rev 21:538, 2008. whereby current 60-year-olds were more commonly colonized as
Tal-Jasper R et al: Clinical and epidemiological significance of car- children than are current children. Spontaneous acquisition or loss of
bapenem resistance in Acinetobacter baumannii infections. Antimicrob H. pylori in adulthood is uncommon. Childhood acquisition explains
Agents Chemother 60:3127, 2016. why the main risk factors for infection are markers of crowding and
Wong D et al: Clinical and pathophysiological overview of social deprivation in childhood.
Acinetobacter infections: A century of challenges. Clin Microbiol Rev Transmission Humans are the only important reservoir
30:409, 2017. of H. pylori. Children may acquire the organism from their
parents (most often the primary caregiver) or from other chil-
dren. The former is more common in developed countries and the latter
in less developed countries. Whether transmission takes place more
158 Infections
often by the fecal–oral or the oral–oral route is unknown, but H. pylori
Helicobacter pylori is easily cultured from vomitus and gastroesophageal refluxate and is
less easily cultured from stool.
■ PATHOLOGY AND PATHOGENESIS
John C. Atherton, Martin J. Blaser H. pylori colonization induces chronic superficial gastritis, a tissue
response in the stomach that includes infiltration of the mucosa by both
mononuclear and polymorphonuclear cells. (The term gastritis should
Helicobacter pylori colonizes the stomach in ~50% of the be used specifically to describe histologic features; it has also been
world’s human population, essentially for life unless eradi- used to describe endoscopic appearances and even symptoms, but
cated by antibiotic treatment. Colonization with this organism these features do not correlate with microscopic findings or even with
is the main risk factor for peptic ulceration (Chap. 317) as well as for the presence of H. pylori.) Although H. pylori is capable of numerous
gastric adenocarcinoma and gastric mucosa-associated lymphoid tis- adaptations that prevent excessive stimulation of the immune system,
sue (MALT) lymphoma (Chap. 76). Treatment for H. pylori has revolu- colonization is accompanied by a considerable persistent local and
tionized the management of peptic ulcer disease, providing a permanent systemic immune response, including the production of antibodies
cure in most cases. Such treatment also represents first-line therapy for and cell-mediated responses. However, these responses are ineffective
patients with low-grade gastric MALT lymphoma. Treatment of in clearing the bacterium. This inefficient clearing appears to be due in
H. pylori is of no benefit in the treatment of gastric adenocarcinoma, but part to H. pylori’s downregulation of the immune system, which fosters
prevention of H. pylori colonization or eradicative treatment could its own persistence.
Harrisons_20e_Part5_p0859-p1648.indd 1162 6/1/18 12:05 PM
114 induced to form bullae with light lateral pressure (Nikolsky’s sign). ■ PURPURIC ERUPTIONS
In a mild form, a scarlatiniform eruption mimics scarlet fever, but the Acute meningococcemia (Chap. 150) classically presents in children as a
patient does not exhibit a strawberry tongue or circumoral pallor. In petechial eruption, but initial lesions may appear as blanchable macules
contrast to the staphylococcal scalded-skin syndrome, in which the or urticaria. Rocky Mountain spotted fever should be considered in the
cleavage plane is superficial in the epidermis, toxic epidermal necrolysis differential diagnosis of acute meningococcemia. Echovirus 9 infection
(Chap. 56), a maximal variant of Stevens-Johnson syndrome, involves (Chap. 199) may mimic acute meningococcemia; patients should be
sloughing of the entire epidermis, resulting in severe disease. Exfoliative treated as if they have bacterial sepsis because prompt differentiation of
erythroderma syndrome (Chaps. 54 and 56) is a serious reaction associ- these conditions may be impossible. Large ecchymotic areas of purpura
ated with systemic toxicity that is often due to eczema, psoriasis, a drug fulminans (Chaps. 150 and 297) reflect severe underlying disseminated
reaction, or mycosis fungoides. Drug rash with eosinophilia and systemic intravascular coagulation, which may be due to infectious or noninfec-
symptoms (DRESS), often due to antiepileptic and antibiotic agents tious causes. The lesions of chronic meningococcemia (Chap. 150) may
(Chap. 56), initially appears similar to an exanthematous drug reaction have a variety of morphologies, including petechial. Purpuric nodules
PART 2
but may progress to exfoliative erythroderma; it is accompanied by may develop on the legs and resemble erythema nodosum but lack its
multiorgan failure and has an associated mortality rate of ~10%. exquisite tenderness. Lesions of disseminated gonococcemia (Chap. 151) are
distinctive, sparse, countable hemorrhagic pustules, usually located
■ VESICULOBULLOUS OR PUSTULAR ERUPTIONS near joints. The lesions of chronic meningococcemia and those of
Cardinal Manifestations and Presentation of Diseases
Varicella (Chap. 188) is highly contagious, often occurring in winter gonococcemia may be indistinguishable in terms of appearance and
or spring, and is characterized by pruritic lesions that, within a given distribution. Viral hemorrhagic fever (Chaps. 204 and 205) should be
region of the body, are in different stages of development at any point considered in patients with an appropriate travel history and a pete-
in time. In immunocompromised hosts, varicella vesicles may lack the chial rash. Thrombotic thrombocytopenic purpura (Chaps. 54, 96, and 111)
characteristic erythematous base or may appear hemorrhagic. Lesions and hemolytic-uremic syndrome (Chaps. 111, 156, and 161) are closely
of Pseudomonas”hot-tub” folliculitis (Chap. 159) are also pruritic and related and are noninfectious causes of fever and petechiae. Cutaneous
may appear similar to those of varicella. However, hot-tub folliculitis small-vessel vasculitis (leukocytoclastic vasculitis) typically manifests as
generally occurs in outbreaks after bathing in hot tubs or swimming palpable purpura and has a wide variety of causes (Chap. 54).
pools, and lesions occur in regions occluded by bathing suits. Lesions
■ ERUPTIONS WITH ULCERS OR ESCHARS
of variola (smallpox) (Chap. S2) also appear similar to those of varicella
The presence of an ulcer or eschar in the setting of a more widespread
but are all at the same stage of development in a given region of the
eruption can provide an important diagnostic clue. For example,
body. Variola lesions are most prominent on the face and extremities,
an eschar may suggest the diagnosis of scrub typhus or rickettsialpox
while varicella lesions are most prominent on the trunk. Herpes simplex
(Chap. 182) in the appropriate setting. In other illnesses (e.g., anthrax)
virus infection (Chap. 187) is characterized by hallmark grouped vesi-
(Chap. S2), an ulcer or eschar may be the only skin manifestation.
cles on an erythematous base. Primary herpes infection is accompanied
by fever and toxicity, while recurrent disease is milder. Rickettsialpox ■ FURTHER READING
(Chap. 182) is often documented in urban settings and is characterized Cherry JD: Cutaneous manifestations of systemic infections, in Feigin
by vesicles followed by pustules. It can be distinguished from varicella and Cherry’s Textbook of Pediatric Infectious Diseases, 7th ed. JD Cherry
by an eschar at the site of the mouse-mite bite and the papule/plaque et al (eds). Houston, Elsevier Saunders, 2014, pp 741–768.
base of each vesicle. Acute generalized exanthematous pustulosis should Weber DJ et al: The acutely ill patient with fever and rash, in Principles
be considered in individuals who are acutely febrile and are taking and Practice of Infectious Diseases, vol 1, 8th ed. JI Bennett et al (eds).
new medications, especially anticonvulsant or antimicrobial agents Philadelphia, Elsevier Saunders, 2015, pp 732–747.
(Chap. 56). Disseminated Vibrio vulnificus infection (Chap. 163) or Wolff K et al: Fitzpatrick’s Color Atlas and Synopsis of Clinical Dermatol-
ecthyma gangrenosum due to Pseudomonas aeruginosa (Chap. 159) should ogy, 7th ed. New York, McGraw-Hill, 2013.
be considered in immunosuppressed individuals with sepsis and hem- Wolff K et al (eds): Fitzpatrick’s Dermatology in General Medicine, 8th ed.
orrhagic bullae. New York, McGraw-Hill, 2012.
■ URTICARIA-LIKE ERUPTIONS
Individuals with classic urticaria (“hives”) usually have a hypersen-
sitivity reaction without associated fever. In the presence of fever,
urticaria-like eruptions are most often due to urticarial vasculitis
(Chap. 356). Unlike individual lesions of classic urticaria, which last
up to 24 h, these lesions may last 3–5 days. Etiologies include serum
17 Fever of Unknown Origin
Chantal P. Bleeker-Rovers,
sickness (often induced by drugs such as penicillins, sulfas, salicylates, Jos W. M. van der Meer
or barbiturates), connective-tissue disease (e.g., systemic lupus eryth-
ematosus or Sjögren’s syndrome), and infection (e.g., with hepatitis B
virus, enteroviruses, or parasites). Malignancy, especially lymphoma, ■ DEFINITION
may be associated with fever and chronic urticaria (Chap. 54). Clinicians commonly refer to any febrile illness without an initially
obvious etiology as fever of unknown origin (FUO). Most febrile illnesses
■ NODULAR ERUPTIONS either resolve before a diagnosis can be made or develop distinguish-
In immunocompromised hosts, nodular lesions often represent dis- ing characteristics that lead to a diagnosis. The term FUO should be
seminated infection. Patients with disseminated candidiasis (often due reserved for prolonged febrile illnesses without an established etiol-
to Candida tropicalis) may have a triad of fever, myalgias, and eruptive ogy despite intensive evaluation and diagnostic testing. This chapter
nodules (Chap. 211). Disseminated cryptococcosis lesions (Chap. 210) focuses on classic FUO in the adult patient.
may resemble molluscum contagiosum (Chap. 191). Necrosis of nod- FUO was originally defined by Petersdorf and Beeson in 1961 as
ules should raise the suspicion of aspergillosis (Chap. 212) or mucormy- an illness of >3 weeks’ duration with fever of ≥38.3°C (≥101°F) on two
cosis (Chap. 213). Erythema nodosum presents with exquisitely tender occasions and an uncertain diagnosis despite 1 week of inpatient evalu-
nodules on the lower extremities. Sweet syndrome (Chap. 54) should be ation. Nowadays, most patients with FUO are hospitalized only if their
considered in individuals with multiple nodules and plaques, often so clinical condition requires it, and not for diagnostic purposes alone;
edematous that they give the appearance of vesicles or bullae. Sweet thus the in-hospital evaluation requirement has been eliminated from
syndrome may occur in individuals with infection, inflammatory the definition. The definition of FUO has been further modified by the
bowel disease, or malignancy and can also be induced by drugs. exclusion of immunocompromised patients, whose workup requires
Harrisons_20e_Part2_p0065-p0418.indd 114 6/1/18 3:14 PM
an entirely different diagnostic and therapeutic approach. For optimal CT and ultrasound. In addition, infective endocarditis is a less frequent 115
comparison of patients with FUO in different geographic areas, it has cause because blood culture and echocardiographic techniques have
been proposed that the quantitative criterion (diagnosis uncertain after improved. Conversely, some diagnoses, such as acute HIV infection,
1 week of evaluation) be changed to a qualitative criterion that requires were unknown four decades ago.
the performance of a specific list of investigations. Accordingly, FUO is Table 17-1 summarizes the findings of large studies on FUO
now defined as follows: conducted over the past 25 years. In general, infection
accounts for about one-fifth of cases of FUO in Western coun-
1. Fever ≥38.3°C (≥101°F) on at least two occasions
tries; next in frequency are noninfectious inflammatory diseases
2. Illness duration of ≥3 weeks
(NIIDs, which include “collagen or rheumatic diseases,” vasculitis
3. No known immunocompromised state
syndromes, granulomatous disorders, and autoinflammatory syn-
4. Diagnosis that remains uncertain after a thorough history-taking,
dromes) and neoplasms. In geographic areas outside the West, infec-
CHAPTER 17
physical examination, and the following obligatory investigations:
tions are a much more common cause of FUO (43% vs 17%), while the
determination of erythrocyte sedimentation rate (ESR) and C-
proportions of cases due to NIIDs and neoplasms are similar. Up to
reactive protein (CRP) level; platelet count; leukocyte count and
50% of cases caused by infections in patients with FUO outside Western
differential; measurement of levels of hemoglobin, electrolytes, crea-
nations are due to tuberculosis, which is a less common cause in the
tinine, total protein, alkaline phosphatase, alanine aminotransferase,
United States and Western Europe. The number of FUO patients diag-
aspartate aminotransferase, lactate dehydrogenase, creatine kinase,
Fever of Unknown Origin
nosed with NIIDs probably will not decrease in the near future, as fever
ferritin, antinuclear antibodies, and rheumatoid factor; protein elec-
may precede more typical manifestations or serologic evidence of these
trophoresis; urinalysis; blood cultures (n = 3); urine culture; chest
diseases by months. Moreover, many NIIDs can be diagnosed only
x-ray; abdominal ultrasonography; and tuberculin skin test (TST) or
after prolonged observation and exclusion of other diseases.
interferon γ release assay (IGRA).
In the West, the proportion of patients who remain undiagnosed
is higher than in non-Western populations and has been increasing
■ ETIOLOGY AND EPIDEMIOLOGY over figures reported in studies before the 1990s. An important factor
The range of FUO etiologies has evolved over time as a result of contributing to the seemingly high diagnostic failure rate is that a
changes in the spectrum of diseases causing FUO, the widespread use diagnosis is more often being established before 3 weeks have elapsed,
of antibiotics, and especially the availability of new diagnostic tech- given that patients with fever tend to seek medical advice earlier and
niques. The proportion of cases caused by intraabdominal abscesses that better diagnostic techniques, such as CT and MRI, are available;
and tumors, for example, has decreased because of earlier detection by therefore, only the cases that are most difficult to diagnose continue to
TABLE 17-1 Etiology of Fever of Unknown Origin (FUO) Over the Past 25 Years: Findings from Large FUO Studies
PERCENTAGE OF CASES DUE TO INDICATED CAUSE
NO. OF PATIENTS NONINFECTIOUS
FIRST AUTHOR (COUNTRY, (RECRUITMENT INFLAMMATORY
YEAR OF PUBLICATION) PERIOD) INFECTIONS DISEASES NEOPLASMS MISCELLANEOUS UNKNOWN
Western Countries
De Kleijn et al. 167 26 24 13 8 30
(Netherlands, 1997) (1992–1994)
Vanderschueren et al. 185 11 18 10 8 53
(Belgium, 2003) (1990–1999)
Hot et al. 280 11 20 27 9 33
(France, 2005) (1995–2005)
Zenone et al. 144 23 26 10 15 26
(France, 2006) (1999–2005)
Bleeker-Rovers 73 16 22 7 4 51
(Netherlands, 2007) (2003–2005)
Mansueto et al. 91 32 12 14 10 32
(Italy, 2008) (1991–2002)
Vanderschueren et al. 114 15 22 13 10 40
(Belgium, 2009) (2003–2007)
Efstathiou et al. 112 30 33 11 5 21
(Greece, 2010) (2001–2007)
Pedersen et al. 52 19 33 8 0 40
(Denmark, 2012) (2005–2010)
Robine et al. 103 12 30 3 5 51
(France, 2014) (2002–2012)
Vanderschueren et al. 436 17 24 11 10 39
(Belgium, 2014) (2000–2010)
Total 1757 19 24 12 8 38
Other Geographic Locations
Tabak et al. 117 34 29 19 4 14
(Turkey, 2003) (1984–2001)
Saltoglu et al. 87 59 18 14 2 7
(Turkey, 2004) (1994–2002)
(Continued)
Harrisons_20e_Part2_p0065-p0418.indd 115 6/1/18 3:14 PM
116
TABLE 17-1 Etiology of Fever of Unknown Origin (FUO) Over the Past 25 Years: Findings from Large FUO Studies (Continued)
PERCENTAGE OF CASES DUE TO INDICATED CAUSE
NO. OF PATIENTS NONINFECTIOUS
FIRST AUTHOR (COUNTRY, (RECRUITMENT INFLAMMATORY
YEAR OF PUBLICATION) PERIOD) INFECTIONS DISEASES NEOPLASMS MISCELLANEOUS UNKNOWN
Ergonul et al. 80 52 16 18 3 11
(Turkey, 2005) (1993–1999)
Brahim et al. 97 36 8 16 5 35
(Turkey, 2005) (1990–2005)
Chin et al. 94 57 7 9 9 18
(Taiwan, 2006) (2001–2002)
PART 2
Colpan et al. 71 45 27 14 6 9
(Turkey, 2007) (2001–2004)
Hu et al. 142 36 32 13 5 14
(China, 2008) (2002–2003)
Cardinal Manifestations and Presentation of Diseases
Kucukardali et al. 154 34 31 14 5 16
(Turkey, 2008) (2003–2004)
Ali-Eldin et al. 93 42 15 30 0 12
(Egypt, 2011) (2009–2010)
Bandyopadhya et al. 164 55 11 22 0 12
(India, 2011) (2008–2009)
Mete et al. 100 26 38 14 2 20
(Turkey, 2012) (2001–2009)
Ma et al. 397 49 18 16 7 10
(China, 2012) (2000–2009)
Ryuko et al. 174 41 27 7 6 19
(Japan, 2013) (2004–2010)
Mahmood et al. 205 49 20 13 2 17
(Pakistan, 2013) (2006–2011)
Alvi et al. 106 44 18 12 10 15
(Iran, 2013) (2007–2011)
Naito et al. 121 23 31 11 12 23
(Japan, 2013) (2011)
Yamanouchi et al. 256 28 18 10 15 29
(Japan, 2014) (1994–2012)
Moawad et al. 98 33 14 18 18 17
(Turkey, 2014) (1995–2008)
Yu et al. 107 30 17 18 14 22
(China, 2014) (2010–2011)
Mir et al. 91 44 12 12 4 27
(India, 2014) (2010–2012)
Kabapy et al. 979 79 17 1 1 2
(Egypt, 2015) (2009–2010)
Montasser et al. 217 66 7 7 12 8
(Egypt, 2015) (unknown)
Popovsa-Jovicic et al. 74 38 26 15 18 4
(Serbia, 2016)
Total 4024 43 20 14 7 16
meet the criteria for FUO. Furthermore, most patients who have FUO presentation of a rather common disease than by a very rare disease.
without a diagnosis currently do well, and thus a less aggressive diag- Table 17-2 presents an overview of possible causes of FUO. Atypical
nostic approach may be used in clinically stable patients once diseases presentations of endocarditis, diverticulitis, vertebral osteomyelitis,
with immediate therapeutic or prognostic consequences have been and extrapulmonary tuberculosis are the more common infectious
ruled out to a reasonable extent. This factor may be especially relevant disease diagnoses. Q fever and Whipple’s disease are quite rare but
to patients with recurrent fever who are asymptomatic between febrile should always be kept in mind as a cause of FUO since the presenting
episodes. In patients with recurrent fever (defined as repeated episodes symptoms can be nonspecific. Serologic testing for Q fever, which
of fever interspersed with fever-free intervals of at least 2 weeks and results from exposure to animals or animal products, should be per-
apparent remission of the underlying disease), the chance of attaining formed when the patient lives in a rural area or has a history of heart
an etiologic diagnosis is <50%. valve disease, an aortic aneurysm, or a vascular prosthesis. In patients
with unexplained symptoms localized to the central nervous system,
■ DIFFERENTIAL DIAGNOSIS gastrointestinal tract, or joints, polymerase chain reaction testing for
The differential diagnosis for FUO is extensive. It is important Tropheryma whipplei should be performed. Travel to or (former) res-
to remember that FUO is far more often caused by an atypical idence in tropical countries or the American Southwest should lead
Harrisons_20e_Part2_p0065-p0418.indd 116 6/1/18 3:14 PM
TABLE 17-2 All Reported Causes of FUOa 117
Infections
Bacterial, nonspecific Abdominal abscess, adnexitis, apical granuloma, appendicitis, cholangitis, cholecystitis, diverticulitis, endocarditis, endometritis,
epidural abscess, infected joint prosthesis, infected vascular catheter, infected vascular prosthesis, infectious arthritis, infective
myonecrosis, intracranial abscess, liver abscess, lung abscess, malakoplakia, mastoiditis, mediastinitis, mycotic aneurysm,
osteomyelitis, pelvic inflammatory disease, prostatitis, pyelonephritis, pylephlebitis, renal abscess, septic phlebitis, sinusitis,
spondylodiscitis, xanthogranulomatous urinary tract infection
Bacterial, specific Actinomycosis, atypical mycobacterial infection, bartonellosis, brucellosis, Campylobacter infection, Chlamydia pneumoniae infection,
chronic meningococcemia, ehrlichiosis, gonococcemia, legionellosis, leptospirosis, listeriosis, louse-borne relapsing fever (Borrelia
recurrentis), Lyme disease, melioidosis (Pseudomonas pseudomallei), Mycoplasma infection, nocardiosis, psittacosis, Q fever (Coxiella
burnetii), rickettsiosis, Spirillum minor infection, Streptobacillus moniliformis infection, syphilis, tick-borne relapsing fever (Borrelia
CHAPTER 17
duttonii), tuberculosis, tularemia, typhoid fever and other salmonelloses, Whipple’s disease (Tropheryma whipplei), yersiniosis
Fungal Aspergillosis, blastomycosis, candidiasis, coccidioidomycosis, cryptococcosis, histoplasmosis, Malassezia furfur infection,
paracoccidioidomycosis, Pneumocystis jirovecii pneumonia, sporotrichosis, zygomycosis
Parasitic Amebiasis, babesiosis, echinococcosis, fascioliasis, malaria, schistosomiasis, strongyloidiasis, toxocariasis, toxoplasmosis,
trichinellosis, trypanosomiasis, visceral leishmaniasis
Viral Colorado tick fever, coxsackievirus infection, cytomegalovirus infection, dengue, Epstein-Barr virus infection, hantavirus infection,
Fever of Unknown Origin
hepatitis (A, B, C, D, E), herpes simplex, HIV infection, human herpesvirus 6 infection, parvovirus infection, West Nile virus infection
Noninfectious Inflammatory Diseases
Systemic rheumatic and Ankylosing spondylitis, antiphospholipid syndrome, autoimmune hemolytic anemia, autoimmune hepatitis, Behçet’s disease,
autoimmune diseases cryoglobulinemia, dermatomyositis, Felty syndrome, gout, mixed connective-tissue disease, polymyositis, pseudogout, reactive arthritis,
relapsing polychondritis, rheumatic fever, rheumatoid arthritis, Sjögren’s syndrome, systemic lupus erythematosus, Vogt-Koyanagi-
Harada syndrome
Vasculitis Allergic vasculitis, eosinophilic granulomatosis with polyangiitis, giant cell vasculitis/polymyalgia rheumatica, granulomatosis with
polyangiitis, hypersensitivity vasculitis, Kawasaki disease, polyarteritis nodosa, Takayasu arteritis, urticarial vasculitis
Granulomatous diseases Idiopathic granulomatous hepatitis, sarcoidosis
Autoinflammatory Adult-onset Still’s disease, Blau syndrome, CAPSb (cryopyrin-associated periodic syndromes), Crohn’s disease, DIRA (deficiency of the
syndromes interleukin 1 receptor antagonist), familial Mediterranean fever, hemophagocytic syndrome, hyper-IgD syndrome (HIDS, also known as
mevalonate kinase deficiency), juvenile idiopathic arthritis, PAPA syndrome (pyogenic sterile arthritis, pyoderma gangrenosum, and
acne), PFAPA syndrome (periodic fever, aphthous stomatitis, pharyngitis, adenitis), recurrent idiopathic pericarditis, SAPHO (synovitis,
acne, pustulosis, hyperostosis, osteomyelitis), Schnitzler syndrome, TRAPS (tumor necrosis factor receptor–associated periodic
syndrome)
Neoplasms
Hematologic Amyloidosis, angioimmunoblastic lymphoma, Castleman’s disease, Hodgkin’s disease, hypereosinophilic syndrome, leukemia,
malignancies lymphomatoid granulomatosis, malignant histiocytosis, multiple myeloma, myelodysplastic syndrome, myelofibrosis, non-Hodgkin’s
lymphoma, plasmacytoma, systemic mastocytosis, vaso-occlusive crisis in sickle cell disease
Solid tumors Most solid tumors and metastases can cause fever. Those most commonly causing FUO are breast, colon, hepatocellular, lung,
pancreatic, and renal cell carcinomas.
Benign tumors Angiomyolipoma, cavernous hemangioma of the liver, craniopharyngioma, necrosis of dermoid tumor in Gardner’s syndrome
Miscellaneous Causes
ADEM (acute disseminated encephalomyelitis), adrenal insufficiency, aneurysms, anomalous thoracic duct, aortic dissection, aortic-
enteral fistula, aseptic meningitis (Mollaret’s syndrome), atrial myxoma, brewer’s yeast ingestion, Caroli disease, cholesterol emboli,
cirrhosis, complex partial status epilepticus, cyclic neutropenia, drug fever, Erdheim-Chester disease, extrinsic allergic alveolitis, Fabry’s
disease, factitious disease, fire-eater’s lung, fraudulent fever, Gaucher disease, Hamman-Rich syndrome (acute interstitial pneumonia),
Hashimoto’s encephalopathy, hematoma, hypersensitivity pneumonitis, hypertriglyceridemia, hypothalamic hypopituitarism, idiopathic
normal-pressure hydrocephalus, inflammatory pseudotumor, Kikuchi’s disease, linear IgA dermatosis, mesenteric fibromatosis,
metal fume fever, milk protein allergy, myotonic dystrophy, nonbacterial osteitis, organic dust toxic syndrome, panniculitis, POEMS
(polyneuropathy, organomegaly, endocrinopathy, monoclonal protein, skin changes), polymer fume fever, post–cardiac injury syndrome,
primary biliary cirrhosis, primary hyperparathyroidism, pulmonary embolism, pyoderma gangrenosum, retroperitoneal fibrosis, Rosai-
Dorfman disease, sclerosing mesenteritis, silicone embolization, subacute thyroiditis (de Quervain’s), Sweet syndrome (acute febrile
neutrophilic dermatosis), thrombosis, tubulointerstitial nephritis and uveitis syndrome (TINU), ulcerative colitis
Thermoregulatory Disorders
Central Brain tumor, cerebrovascular accident, encephalitis, hypothalamic dysfunction
Peripheral Anhidrotic ectodermal dysplasia, exercise-induced hyperthermia, hyperthyroidism, pheochromocytoma
a
This table includes all causes of FUO that have been described in the literature. bCAPS includes chronic infantile neurologic cutaneous and articular syndrome (CINCA,
also known as neonatal-onset multisystem inflammatory disease, or NOMID), familial cold autoinflammatory syndrome (FCAS), and Muckle-Wells syndrome.
to consideration of infectious diseases such as malaria, leishmaniasis, Of the NIIDs, large-vessel vasculitis, polymyalgia rheumatica, sar-
histoplasmosis, or coccidioidomycosis. Fever with signs of endo- coidosis, familial Mediterranean fever, and adult-onset Still’s disease
carditis and negative blood culture results poses a special problem. are rather common diagnoses in patients with FUO. The hereditary
Culture-negative endocarditis may be due to difficult-to-culture bacte- autoinflammatory syndromes are very rare and usually present in
ria such as nutritionally variant bacteria, HACEK organisms (including young patients. Schnitzler syndrome, which can present at any age, is
Haemophilus parainfluenzae, H. paraphrophilus, Aggregatibacter actinomy- uncommon but can often be diagnosed easily in a patient with FUO
cetemcomitans, A. aphrophilus, A. paraphrophilus, Cardiobacterium hominis, who presents with urticaria, bone pain, and monoclonal gammopathy.
C. valvarum, Eikenella corrodens, and Kingella kingae; discussed below), Although most tumors can present with fever, malignant lymphoma
Coxiella burnetii, T. whipplei, and Bartonella species. Marantic endocar- is by far the most common diagnosis of FUO among the neoplasms.
ditis is a sterile thrombotic disease that occurs as a paraneoplastic Sometimes the fever even precedes lymphadenopathy detectable by
phenomenon, especially with adenocarcinomas. Sterile endocarditis is physical examination.
also seen in the context of systemic lupus erythematosus and antiphos- Apart from drug-induced fever and exercise-induced hyperthermia,
pholipid syndrome. none of the miscellaneous causes of fever is found very frequently
Harrisons_20e_Part2_p0065-p0418.indd 117 6/1/18 3:14 PM
118 in patients with FUO. Virtually all drugs can cause fever, even that
relatively low. These tests more often yield false-positive rather than
commencing after long-term use. Drug-induced fever, including DRESS
true-positive results and are of little use without PDCs pointing
(drug reaction with eosinophilia and systemic symptoms; Fig. A1-48),
to specific immunologic disorders. Given the absence of specific
is often accompanied by eosinophilia and also by lymphadenopathy,
symptoms in many patients and the relatively low cost of the test,
which can be extensive. More common causes of drug-induced fever
investigation of cryoglobulins appears to be a valuable screening
are allopurinol, carbamazepine, lamotrigine, phenytoin, sulfasalazine,
test in patients with FUO.
furosemide, antimicrobial drugs (especially sulfonamides, minocycline,
Multiple blood samples should be cultured in the laboratory long
vancomycin, β-lactam antibiotics, and isoniazid), some cardiovascular
enough to ensure ample growth time for any fastidious organisms,
drugs (e.g., quinidine), and some antiretroviral drugs (e.g., nevirapine).
such as HACEK organisms. It is critical to inform the laboratory of
Exercise-induced hyperthermia (Chaps. 15 and 455) is characterized by an
the intent to test for unusual organisms. Specialized media should
elevated body temperature that is associated with moderate to strenu-
be used when the history suggests uncommon microorganisms,
ous exercise lasting from half an hour up to several hours without an
PART 2
such as Histoplasma or Legionella. Performing more than three blood
increase in CRP level or ESR; typically these patients sweat during the
cultures or more than one urine culture is useless in patients with
temperature elevation. Factitious fever (fever artificially induced by the
FUO in the absence of PDCs (e.g., a high level of clinical suspicion of
patient—for example, by IV injection of contaminated water) should be
endocarditis). Repeating blood or urine cultures is useful only when
considered in all patients but is more common among young women
previously cultured samples were collected during antibiotic treat-
Cardinal Manifestations and Presentation of Diseases
in health care professions. In fraudulent fever, the patient is normother-
ment or within 1 week after its discontinuation. FUO with headache
mic but manipulates the thermometer. Simultaneous measurements at
should prompt microbiologic examination of cerebrospinal fluid
different body sites (rectum, ear, mouth) should rapidly identify this
(CSF) for organisms including herpes simplex virus (especially
diagnosis. Another clue to fraudulent fever is a dissociation between
type 2), Cryptococcus neoformans, and Mycobacterium tuberculosis. In
pulse rate and temperature.
central nervous system tuberculosis, the CSF typically has elevated
Previous studies of FUO have shown that a diagnosis is more likely
protein and lowered glucose concentrations, with a mononuclear
in elderly patients than in younger age groups. In many cases, FUO
pleocytosis. CSF protein levels range from 100 to 500 mg/dL in most
in the elderly results from an atypical manifestation of a common dis-
patients, the CSF glucose concentration is <45 mg/dL in 80% of
ease, among which giant cell arteritis and polymyalgia rheumatica are
cases, and the usual CSF cell count is between 100 and 500 cells/μL.
most frequently involved. Tuberculosis is the most common infectious
Microbiologic serology should not be included in the diagnostic
disease associated with FUO in elderly patients, occurring much more
workup of patients without PDCs for specific infections. A TST is
often than in younger patients. As many of these diseases are treatable,
included in the obligatory investigations, but it may yield false-
it is well worth pursuing the cause of fever in elderly patients.
negative results in patients with miliary tuberculosis, malnutrition,
or immunosuppression. Although the IGRA is less influenced by
APPROACH TO THE PATIENT prior vaccination with bacille Calmette-Guérin or by infection with
nontuberculous mycobacteria, its sensitivity is similar to that of the
Fever of Unknown Origin TST; a negative TST or IGRA therefore does not exclude a diag-
nosis of tuberculosis. Miliary tuberculosis is especially difficult to
FIRST-STAGE DIAGNOSTIC TESTS
diagnose. Granulomatous disease in liver or bone marrow biopsy
Figure 17-1 shows a structured approach to patients presenting samples, for example, should always lead to a (re)consideration of
with FUO. The most important step in the diagnostic workup is the this diagnosis. If miliary tuberculosis is suspected, liver biopsy for
search for potentially diagnostic clues (PDCs) through complete and acid-fast smear, culture, and polymerase chain reaction probably still
repeated history-taking and physical examination and the obliga- has the highest diagnostic yield; however, biopsies of bone marrow,
tory investigations listed above and in the figure. PDCs are defined lymph nodes, or other involved organs also can be considered.
as all localizing signs, symptoms, and abnormalities potentially The diagnostic yield of echocardiography, sinus radiography,
pointing toward a diagnosis. Although PDCs are often mislead- radiologic or endoscopic evaluation of the gastrointestinal tract, and
ing, only with their help can a concise list of probable diagnoses bronchoscopy is very low in the absence of PDCs. Therefore, these
be made. The history should include information about the fever tests should not be used as screening procedures.
pattern (continuous or recurrent) and duration, previous medical After identification of all PDCs retrieved from the history, physi-
history, present and recent drug use, family history, sexual history, cal examination, and obligatory tests, a limited list of the most proba-
country of origin, recent and remote travel, unusual environmental ble diagnoses should be made. Since most investigations are helpful
exposures associated with travel or hobbies, and animal contacts. A only for patients who have PDCs for the diagnoses sought, further
complete physical examination should be performed, with special diagnostic procedures should be limited to specific investigations
attention to the eyes, lymph nodes, temporal arteries, liver, spleen, aimed at confirming or excluding diseases on this list. In FUO, the
sites of previous surgery, entire skin surface, and mucous mem- diagnostic pointers are numerous and diverse but may be missed
branes. Before further diagnostic tests are initiated, antibiotic and on initial examination, often being detected only by a very careful
glucocorticoid treatment, which can mask many diseases, should examination performed subsequently. In the absence of PDCs, the
be stopped. For example, blood and other cultures are not reliable history and physical examination should therefore be repeated reg-
when samples are obtained during antibiotic treatment, and the size ularly. One of the first steps should be to rule out factitious or fraud-
of enlarged lymph nodes usually decreases during glucocorticoid ulent fever, particularly in patients without signs of inflammation in
treatment, regardless of the cause of lymphadenopathy. Despite the laboratory tests. All medications, including nonprescription drugs
high percentage of false-positive ultrasounds and the relatively low and nutritional supplements, should be discontinued early in the
sensitivity of chest x-rays, the performance of these simple, low-cost evaluation to exclude drug fever. If fever persists beyond 72 h after
diagnostic tests remains obligatory in all patients with FUO in order discontinuation of the suspected drug, it is unlikely that this drug is
to separate cases that are caused by easily diagnosed diseases from the cause. In patients without PDCs or with only misleading PDCs,
those that are not. Abdominal ultrasound is preferred to abdominal funduscopy by an ophthalmologist may be useful in the early stage
CT as an obligatory test because of relatively low cost, lack of radia- of the diagnostic workup. When the first-stage diagnostic tests do
tion burden, and absence of side effects. not lead to a diagnosis, scintigraphy should be performed, especially
Only rarely do biochemical tests (beyond the obligatory tests when the ESR or the CRP level is elevated.
needed to classify a patient’s fever as FUO) lead directly to a defini-
tive diagnosis in the absence of PDCs. The diagnostic yield of immu- Recurrent Fever In patients with recurrent fever, the diagnos-
nologic serology other than that included in the obligatory tests is tic workup should consist of thorough history-taking, physical
Harrisons_20e_Part2_p0065-p0418.indd 118 6/1/18 3:14 PM
119
Fever ≥38.3° C (≥101° F) and illness lasting ≥3 weeks
and no known immunocompromised state
History and physical examination
Stop antibiotic treatment and glucocorticoids
Obligatory investigations:
CHAPTER 17
ESR or CRP, hemoglobin, platelet count, leukocyte count and differential, electrolytes,
creatinine, total protein, protein electrophoresis, alkaline phosphatase, AST, ALT, LDH,
creatine kinase, antinuclear antibodies, rheumatoid factor, urinalysis, blood cultures (n = 3),
urine culture, chest x-ray, abdominal ultrasonography, and tuberculin skin test or IGRA
Exclude manipulation with thermometer
Fever of Unknown Origin
Stop or replace medication to exclude drug fever
PDCs present PDCs absent or misleading
Guided diagnostic tests Cryoglobulin and funduscopy
FDG-PET/CT (or labeled leukocyte
DIAGNOSIS NO DIAGNOSIS scintigraphy or gallium scan); see Fig. 17-2
Scintigraphy abnormal Scintigraphy normal
Confirmation of abnormality Repeat history and physical examination
(e.g., biopsy, culture) Perform PDC-driven invasive testing
DIAGNOSIS NO DIAGNOSIS DIAGNOSIS NO DIAGNOSIS
Chest and abdominal CT
Temporal artery biopsy (≥55 years)
DIAGNOSIS NO DIAGNOSIS
Stable condition: Deterioration:
Follow-up for new PDCs Further diagnostic tests
Consider NSAID treatment Consider therapeutic trial
FIGURE 17-1 Structured approach to patients with FUO. ALT, alanine aminotransferase; AST, aspartate aminotransferase; CRP, C-reactive protein; ESR, erythrocyte
sedimentation rate; FDG-PET/CT, 18F-fluorodeoxyglucose positron emission tomography combined with low-dose CT; IGRA, interferon γ release assay; LDH, lactate
dehydrogenase; NSAID, nonsteroidal anti-inflammatory drug; PDCs, potentially diagnostic clues (all localizing signs, symptoms, and abnormalities potentially pointing
toward a diagnosis).
examination, and obligatory tests. The search for PDCs should be when PDCs for infections, vasculitis syndromes, or malignancy are
directed toward clues matching known recurrent syndromes (Table present or when the patient’s clinical condition is deteriorating.
17-3). Patients should be asked to return during a febrile episode
so that the history, physical examination, and laboratory tests can Scintigraphy Scintigraphic imaging is a noninvasive method
be repeated during a symptomatic phase. Further diagnostic tests, allowing delineation of foci in all parts of the body on the basis
such as scintigraphic imaging (see below), should be performed of functional changes in tissues. This procedure plays an impor-
only during a febrile episode because abnormalities may be absent tant role in the diagnosis of patients with FUO in clinical practice.
between episodes. In patients with recurrent fever lasting >2 years, Conventional scintigraphic methods used in clinical practice are
it is very unlikely that the fever is caused by infection or malignancy. 67
Ga-citrate scintigraphy and 111In- or 99mTc-labeled leukocyte scin-
Further diagnostic tests in that direction should be considered only tigraphy. Focal infectious and inflammatory processes can also be
Harrisons_20e_Part2_p0065-p0418.indd 119 6/1/18 3:14 PM
120 TABLE 17-3 All Reported Causes of Recurrent Fevera
Infections
Bacterial, nonspecific Apical granuloma, diverticulitis, prostatitis, recurrent bacteremia caused by colonic neoplasia or persistent focal infection, recurrent
cellulitis, recurrent cholangitis or cholecystitis, recurrent pneumonia, recurrent sinusitis, recurrent urinary tract infection
Bacterial, specific Bartonellosis, brucellosis, chronic gonococcemia, chronic meningococcemia, louse-borne relapsing fever (Borrelia recurrentis),
melioidosis (Pseudomonas pseudomallei), Q fever (Coxiella burnetii), salmonellosis, Spirillum minor infection, Streptobacillus
moniliformis infection, syphilis, tick-borne relapsing fever (Borrelia duttonii), tularemia, Whipple’s disease (Tropheryma whipplei),
yersiniosis
Fungal Coccidioidomycosis, histoplasmosis, paracoccidioidomycosis
Parasitic Babesiosis, malaria, toxoplasmosis, trypanosomiasis, visceral leishmaniasis
Viral Cytomegalovirus infection, Epstein-Barr virus infection, herpes simplex
PART 2
Noninfectious Inflammatory Diseases
Systemic rheumatic and Ankylosing spondylitis, antiphospholipid syndrome, autoimmune hemolytic anemia, autoimmune hepatitis, Behçet’s disease,
autoimmune diseases cryoglobulinemia, gout, polymyositis, pseudogout, reactive arthritis, relapsing polychondritis, systemic lupus erythematosus
Vasculitis Churg-Strauss syndrome, giant cell vasculitis/polymyalgia rheumatica, hypersensitivity vasculitis, polyarteritis nodosa, urticarial
vasculitis
Cardinal Manifestations and Presentation of Diseases
Granulomatous diseases Idiopathic granulomatous hepatitis, sarcoidosis
Autoinflammatory syndromes Adult-onset Still’s disease, Blau syndrome, CANDLE (chronic atypical neutrophilic dermatitis with lipodystrophy and elevated
temperature syndrome), CAPSb (cryopyrin-associated periodic syndrome), CRMO (chronic recurrent multifocal osteomyelitis), Crohn’s
disease, DIRA (deficiency of the interleukin 1 receptor antagonist), familial Mediterranean fever, hemophagocytic syndrome, hyper-
IgD syndrome (HIDS, also known as mevalonate kinase deficiency), juvenile idiopathic arthritis, NLRC4-activating mutations, PAPA
syndrome (pyogenic sterile arthritis, pyoderma gangrenosum, and acne), PFAPA syndrome (periodic fever, aphthous stomatitis,
pharyngitis, adenitis), recurrent idiopathic pericarditis, SAPHO (synovitis, acne, pustulosis, hyperostosis, osteomyelitis), SAVI
(stimulator of interferon genes [STING]–associated vasculopathy with onset in infancy), Schnitzler syndrome, TRAPS (tumor
necrosis factor receptor–associated periodic syndrome)
Neoplasms
Angioimmunoblastic lymphoma, Castleman’s disease, colon carcinoma, craniopharyngioma, Hodgkin’s disease, malignant
histiocytosis, mesothelioma, non-Hodgkin’s lymphoma
Miscellaneous Causes
Adrenal insufficiency, aortic-enteral fistula, aseptic meningitis (Mollaret’s syndrome), atrial myxoma, brewer’s yeast ingestion,
cholesterol emboli, cyclic neutropenia, drug fever, extrinsic allergic alveolitis, Fabry’s disease, factitious disease, fraudulent fever,
Gaucher disease, hypersensitivity pneumonitis, hypertriglyceridemia, hypothalamic hypopituitarism, inflammatory pseudotumor,
metal fume fever, milk protein allergy, polymer fume fever, pulmonary embolism, sclerosing mesenteritis
Thermoregulatory Disorders
Central Hypothalamic dysfunction
Peripheral Anhidrotic ectodermal dysplasia, exercise-induced hyperthermia, pheochromocytoma
a
This table includes all causes of recurrent fever that have been described in the literature. bCAPS includes chronic infantile neurologic cutaneous and articular
syndrome (CINCA, also known as neonatal-onset multisystem inflammatory disease, or NOMID), familial cold autoinflammatory syndrome (FCAS), and Muckle-Wells
syndrome.
detected by several radiologic techniques, such as CT, MRI, and allow differentiation among infection, sterile inflammation, and
ultrasound. However, because of the lack of substantial pathologic malignancy. However, since all of these disorders are causes of FUO,
changes in the early phase, infectious and inflammatory foci cannot FDG-PET/CT can be used to guide additional diagnostic tests (e.g.,
be detected at this time. Furthermore, distinguishing active infec- targeted biopsies) that may yield the final diagnosis.
tious or inflammatory lesions from residual changes due to cured In recent years, many cohort studies and several meta-analyses
processes or surgery remains critical. Finally, CT and MRI routinely have focused on the diagnostic yield of PET and PET/CT in FUO.
provide information on only part of the body, while scintigraphy Although these studies are highly variable in terms of the selection
readily allows whole-body imaging. of patients, follow-up, and the selection of a gold-standard reference
point, all meta-analyses report a high diagnostic yield for PET and
Fluorodeoxyglucose Positron Emission Tomography 18F-Fluorodeoxy- PET/CT in the workup of FUO patients, with pooled sensitivity and
glucose (FDG) positron emission tomography (PET) combined specificity figures of ~85% and ~50%, respectively, and a total diag-
with CT has become an established imaging procedure in FUO. nostic yield of ~50% for PET/CT and ~40% for PET. In one study,
FDG accumulates in tissues with a high rate of glycolysis, which FDG-PET was never helpful in diagnosing FUO in patients who had
occurs not only in malignant cells but also in activated leukocytes a normal CRP level and a normal ESR. In a meta-analysis on the
and thus permits the imaging of acute and chronic inflammatory performance, diagnostic yield, and management decision impact of
processes. Normal uptake may obscure pathologic foci in the brain, nuclear imaging tests in patients with FUO, the diagnostic yield of
heart, bowel, kidneys, and bladder. FDG uptake in the heart, which gallium scintigraphy ranged from 21% to 54%, and, on average, the
obscures endocarditis, may be prevented by consumption of a location of a source of fever was correctly localized in approximately
low-carbohydrate diet before the PET investigation. In patients one-third of patients. Moreover, in gallium scintigraphy, results do
with fever, bone marrow uptake is frequently increased in a non- not become available for days, whereas FDG-PET/CT yields results
specific way due to cytokine activation, which upregulates glucose within hours. In this meta-analysis, estimates of the diagnostic
transporters in bone marrow cells. Compared with conventional yield of labeled leukocyte scintigraphy ranged from 8% to 31%, and
scintigraphy, FDG-PET/CT offers the advantages of higher res- overall the cause of FUO was correctly identified on the basis of the
olution, greater sensitivity in chronic low-grade infections, and scan results in only one-fifth of patients. Indirect comparisons of
a high degree of accuracy in the central skeleton. Furthermore, test performance suggested that FDG-PET/CT outperformed stand-
vascular uptake of FDG is increased in patients with vasculitis alone FDG-PET, gallium scintigraphy, and leukocyte scintigraphy.
(Fig. 17-2). The mechanisms responsible for FDG uptake do not Similarly, indirect comparisons of diagnostic yield suggested that
Harrisons_20e_Part2_p0065-p0418.indd 120 6/1/18 3:14 PM
121
CHAPTER 17
Fever of Unknown Origin
FIGURE 17-2 FDG-PET/CT in a patient with FUO. This 72-year-old woman presented with a low-grade fever and severe fatigue of almost 3 months’ duration. An
extensive history was taken, but the patient had no specific complaints and had not traveled recently. Her previous history was unremarkable, and she did not use
any drugs. Physical examination, including palpation of the temporal arteries, yielded completely normal results. Laboratory examination showed normocytic anemia,
a C-reactive protein level of 43 mg/L, an erythrocyte sedimentation rate of 87 mm/h, and mild hypoalbuminemia. Results of the other obligatory tests were all
normal. Since there were no potentially diagnostic clues, FDG-PET/CT was performed. This test showed increased FDG uptake in all major arteries (carotid, jugular,
and subclavian arteries; thoracic and abdominal aorta; iliac, femoral, and popliteal arteries) and in the soft tissue around the shoulders, hips, and knees—findings
compatible with large-vessel vasculitis and polymyalgia rheumatica. Within 1 week after the initiation of treatment with prednisone (60 mg once daily), the patient
completely recovered. After 1 month, the prednisone dose was slowly tapered.
FDG-PET/CT was more likely than alternative tests to correctly diagnostic yield of screening chest and abdominal CT in patients
identify the cause of FUO. with FUO was ~20%. The specificity of chest CT was ~80%, but
Although scintigraphic techniques do not directly provide a defin- that of abdominal CT varied between 63% and 80%. Despite the
itive diagnosis, they often identify the anatomic location of a particu- relatively limited specificity of abdominal CT and the probably lim-
lar ongoing metabolic process and, with the help of other techniques ited additional value of chest CT after normal FDG-PET/CT, chest
such as biopsy and culture, facilitate timely diagnosis and treatment. and abdominal CT may be used as screening procedures at a later
Pathologic FDG uptake is quickly eradicated by treatment with glu- stage of the diagnostic protocol because of their noninvasive nature
cocorticoids in many diseases, including vasculitis and lymphoma; and high sensitivity. Bone marrow aspiration is seldom useful in
therefore, glucocorticoid use should be stopped or postponed until the absence of PDCs for bone marrow disorders. With addition of
after FDG-PET/CT is performed. Results reported in the literature FDG-PET/CT, which is highly sensitive in detecting lymphoma,
and the advantages offered by FDG-PET/CT indicate that conven- carcinoma, and osteomyelitis, the value of bone marrow biopsy as
tional scintigraphic techniques should be replaced by FDG-PET/ a screening procedure is probably further reduced. Several studies
CT in the investigation of patients with FUO at institutions where have shown a high prevalence of giant cell arteritis among patients
this technique is available. FDG-PET/CT is a relatively expensive with FUO, with rates up to 17% among elderly patients. Giant cell
procedure whose availability is still limited compared with that of arteritis often involves large arteries and in most cases can be diag-
CT and conventional scintigraphy. Nevertheless, FDG-PET/CT can nosed by FDG-PET/CT. However, temporal artery biopsy is still
be cost-effective in the FUO diagnostic workup if used at an early recommended for patients ≥55 years of age in a later stage of the
stage, helping to establish an early diagnosis, reducing days of hos- diagnostic protocol: FDG-PET/CT will not be useful in vasculitis
pitalization for diagnostic purposes, and obviating unnecessary and limited to the temporal arteries because of the small diameter of
unhelpful tests. these vessels and the high levels of FDG uptake in the brain. In
the past, liver biopsies have often been performed as a screening
LATER-STAGE DIAGNOSTIC TESTS procedure in patients with FUO. In each of two recent studies, liver
In some cases, more invasive tests are appropriate. Abnormalities biopsy as part of the later stage of a screening diagnostic protocol
found with scintigraphic techniques often need to be confirmed was helpful in only one patient. Moreover, abnormal liver tests are
by pathology and/or culture of biopsy specimens. If lymphade- not predictive of a diagnostic liver biopsy in FUO. Liver biopsy is an
nopathy is found, lymph node biopsy is necessary, even when the invasive procedure that carries the possibility of complications and
affected lymph nodes are hard to reach or when previous biopsies even death. Therefore, it should not be used for screening purposes
were inconclusive. In the case of skin lesions, skin biopsy should in patients with FUO except in those with PDCs for liver disease or
be undertaken. In one study, pulmonary wedge excision, histologic miliary tuberculosis.
examination of an excised tonsil, and biopsy of the peritoneum In patients with unexplained fever after all of the above pro-
were performed in light of PDCs or abnormal FDG-PET results and cedures, the last steps in the diagnostic workup—with only a
yielded a diagnosis. marginal diagnostic yield—come at an extraordinarily high cost in
If no diagnosis is reached despite scintigraphic and PDC-driven terms of both expense and discomfort for the patient. Repetition of
histologic investigations or culture, second-stage screening diag- a thorough history-taking and physical examination and review of
nostic tests should be considered (Fig. 17-1). In three studies, the laboratory results and imaging studies (including those from other
Harrisons_20e_Part2_p0065-p0418.indd 121 6/1/18 3:14 PM
122 chronic inflammatory conditions without a known basis can be con-
hospitals) are recommended. Diagnostic delay often results from
trolled with glucocorticoids, monotherapy with IL-1 blockade can
a failure to recognize PDCs in the available information. In these
provide improved control without the metabolic, immunologic, and
patients with persisting FUO, waiting for new PDCs to appear
gastrointestinal side effects of glucocorticoid administration.
probably is better than ordering more screening investigations.
Only when a patient’s condition deteriorates without providing new
PDCs should a further diagnostic workup be performed. ■ PROGNOSIS
FUO-related mortality rates have continuously declined over recent
decades. The majority of fevers are caused by treatable diseases, and
the risk of death related to FUO is, of course, dependent on the under-
TREATMENT lying disease. In a study by our group (Table 17-1), none of 37 FUO
patients without a diagnosis died during a follow-up period of at least
Fever of Unknown Origin
PART 2
6 months; 4 of 36 patients with a diagnosis died during follow-up as
Empirical therapeutic trials with antibiotics, glucocorticoids, or a result of infection (n = 1) or malignancy (n = 3). A large study on the
antituberculous agents should be avoided in FUO except when a prognosis of FUO (Vanderschueren et al, 2014; Table 17-1) included 436
patient’s condition is rapidly deteriorating after the aforementioned patients and documented a mortality rate of 10%, of which 68% was
diagnostic tests have failed to provide a definite diagnosis. related to the febrile illness—malignancy in most cases. In this study,
Cardinal Manifestations and Presentation of Diseases
only 4 of 168 patients in whom no diagnosis could be made died, all
ANTIBIOTICS AND ANTITUBERCULOUS THERAPY during their first admission. In two of these patients, diagnosis (lym-
Antibiotic or antituberculous therapy may irrevocably diminish phoma and pneumonia) was made during autopsy. Other studies have
the ability to culture fastidious bacteria or mycobacteria. How- also shown that malignancy accounts for most FUO-related deaths.
ever, hemodynamic instability or neutropenia is a good indication Non-Hodgkin’s lymphoma carries a disproportionately high death toll.
for empirical antibiotic therapy. If the TST or IGRA is positive or In nonmalignant FUO, fatality rates are very low. The good outcome
if granulomatous disease is present with anergy and sarcoidosis in patients without a diagnosis confirms that potentially lethal occult
seems unlikely, a trial of therapy for tuberculosis should be started. diseases are very unusual and that empirical therapy with antibiotics,
Especially in miliary tuberculosis, it may be very difficult to obtain antituberculous agents, or glucocorticoids is rarely required in stable
a rapid diagnosis. If the fever does not respond after 6 weeks of patients. In less affluent regions, infectious diseases are still a major
empirical antituberculous treatment, another diagnosis should be cause of FUO, and outcomes may be different.
considered.
COLCHICINE, NONSTEROIDAL ANTI-INFLAMMATORY DRUGS,
■ FURTHER READING
AND GLUCOCORTICOIDS Bleeker-Rovers CP et al: A prospective multicenter study on fever
of unknown origin: The yield of a structured diagnostic protocol.
Colchicine is highly effective in preventing attacks of familial Med- Medicine (Baltimore) 86:26, 2007.
iterranean fever but is not always effective once an attack is well Knockaert DC et al: Fever of unknown origin in adults: 40 years on.
under way. When familial Mediterranean fever is suspected, the J Intern Med 253:263, 2003.
response to colchicine is not a completely reliable diagnostic tool in Mulders-Manders C et al: Fever of unknown origin. Clin Med 15:280,
the acute phase, but with colchicine treatment most patients show 2015.
remarkable improvements in the frequency and severity of subse- Takeuchi M et al: Nuclear imaging for classical fever of unknown ori-
quent febrile episodes within weeks to months. Therefore, colchicine gin: Meta-analysis. J Nucl Med 57:1913, 2016.
may be tried in patients with features compatible with familial Vanderschueren S et al: Mortality in patients presenting with fever of
Mediterranean fever, especially when these patients originate from unknown origin. Acta Clin Belg 69:12, 2014.
a high-prevalence region. If the fever persists and the source remains
elusive after completion of the later-stage investigations, supportive
treatment with nonsteroidal anti-inflammatory drugs (NSAIDs) can
be helpful. The response of adult-onset Still’s disease to NSAIDs is
dramatic in some cases. The effects of glucocorticoids on giant cell Section 3 Nervous System Dysfunction
arteritis and polymyalgia rheumatica are equally impressive. Early
empirical trials with glucocorticoids, however, decrease the chances
of reaching a diagnosis for which more specific and sometimes
life-saving treatment might be more appropriate, such as malignant
lymphoma. The ability of NSAIDs and glucocorticoids to mask fever
18 Syncope
Roy Freeman
while permitting the spread of infection or lymphoma dictates that
their use should be avoided unless infectious diseases and malig-
nant lymphoma have been largely ruled out and inflammatory Syncope is a transient, self-limited loss of consciousness due to acute
disease is probable and is likely to be debilitating or threatening. global impairment of cerebral blood flow. The onset is rapid, duration
ANAKINRA brief, and recovery spontaneous and complete. Other causes of tran-
Interleukin (IL) 1 is a key cytokine in local and systemic inflam- sient loss of consciousness need to be distinguished from syncope;
mation and the febrile response. The availability of specific IL-1- these include seizures, vertebrobasilar ischemia, hypoxemia, and
targeting agents has revealed a pathologic role of IL-1-mediated hypoglycemia. A syncopal prodrome (presyncope) is common, although
inflammation in a growing list of diseases. Anakinra, a recombinant loss of consciousness may occur without any warning symptoms.
form of the naturally occurring IL-1 receptor antagonist (IL-1Ra), Typical presyncopal symptoms include dizziness, lightheadedness or
blocks the activity of both IL-1α and IL-1β. Anakinra is extremely faintness, weakness, fatigue, and visual and auditory disturbances.
effective in the treatment of many autoinflammatory syndromes, The causes of syncope can be divided into three general categories:
such as familial Mediterranean fever, cryopyrin-associated periodic (1) neurally mediated syncope (also called reflex or vasovagal syncope),
syndrome, tumor necrosis factor receptor–associated periodic syn- (2) orthostatic hypotension, and (3) cardiac syncope.
drome, mevalonate kinase deficiency (hyper IgD syndrome), and Neurally mediated syncope comprises a heterogeneous group of
Schnitzler syndrome. There are many other chronic inflammatory functional disorders that are characterized by a transient change in
disorders in which anti-IL-1 therapy is highly effective. A therapeu- the reflexes responsible for maintaining cardiovascular homeostasis.
tic trial with anakinra can be considered in patients whose FUO has Episodic vasodilation (or loss of vasoconstrictor tone) and bradycardia
not been diagnosed after later-stage diagnostic tests. Although most occur in varying combinations, resulting in temporary failure of blood
Harrisons_20e_Part2_p0065-p0418.indd 122 6/1/18 3:14 PM
508 2. In terms of therapy, aggressive debridement of infected tissues may
Physical examination: skin lesions, mucous
be required. However, it is usually difficult to operate on patients membranes, IV catheter sites, perirectal area
who have recently received chemotherapy, both because of a lack Initial Granulocyte count: absolute count < 500/µL; expected
of platelets (which results in bleeding complications) and because evaluation duration of neutropenia
Blood cultures; chest radiogram; other appropriate
of a lack of WBCs (which may lead to secondary infection). A blood studies based on history (sputum, urine, skin biopsy)
culture positive for Clostridium perfringens—an organism commonly
associated with gas gangrene—can have a number of meanings
(Chap. 149). Clostridium septicum bacteremia is associated with the Treat with antibiotic(s) effective
presence of an underlying malignancy. Bloodstream infections with Initial against both gram-negative and
intestinal organisms such as Streptococcus bovis biotype 1 and C. per- therapy gram-positive aerobes.
fringens may arise spontaneously from lower gastrointestinal lesions
(tumor or polyps); alternatively, these lesions may be harbingers of Follow-up Obvious infectious No obvious
site found infectious site
invasive disease. The clinical setting must be considered in order to
define the appropriate treatment for each case.
Subsequent Treat the infection with Afebrile Febrile
therapy
■ RENAL AND URETERAL INFECTIONS the best available
antibiotics. Do not
Infections of the urinary tract are common among patients whose narrow the spectrum
ureteral excretion is compromised (Table 70-1). Candida, which has a unnecessarily. Continue Add a broad-
predilection for the kidney, can invade either from the bloodstream or to treat for both Continue spectrum
gram-positive and regimen. antifungal
in a retrograde manner (via the ureters or bladder) in immunocompro- gram-negative aerobes. agent.
mised patients. The presence of “fungus balls” or persistent candiduria
suggests invasive disease. Persistent funguria (with Aspergillus as
well as Candida) should prompt a search for a nidus of infection in the Continue treatment until neutropenia resolves (granulocyte count > 500/µL).
PART 4
kidney.
Certain viruses are typically seen only in immunosuppressed
patients. BK virus (polyomavirus hominis 1) has been documented in FIGURE 70-2 Algorithm for the diagnosis and treatment of fever and neutropenia.
the urine of bone marrow transplant recipients and, like adenovirus,
may be associated with hemorrhagic cystitis.
Oncology and Hematology
promptly to cover likely pathogens if infection is suspected. Indeed,
early initiation of antibacterial agents is mandatory to prevent deaths.
ABNORMALITIES THAT PREDISPOSE Like most immunocompromised patients, neutropenic patients are
TO INFECTION threatened by their own microbial flora, including gram-positive and
(Table 70-1) gram-negative organisms found commonly on the skin and mucous
membranes and in the bowel (Table 70-4). Because treatment with
■ THE LYMPHOID SYSTEM
narrow-spectrum agents leads to infection with organisms not covered
It is beyond the scope of this chapter to detail how all the immunologic
by the antibiotics used, the initial regimen should target all pathogens
abnormalities that result from cancer or from chemotherapy for cancer
likely to be the initial causes of bacterial infection in neutropenic hosts.
lead to infections. Disorders of the immune system are discussed in
As noted in the algorithm shown in Fig. 70-2, administration of anti-
other sections of this book. As has been noted, patients with antibody
microbial agents is routinely continued until neutropenia resolves—
deficiency are predisposed to overwhelming infection with encapsu-
that is, the granulocyte count is sustained above 500/μL for at least
lated bacteria (including S. pneumoniae, H. influenzae, and N. meningiti-
2 days. Fever may not resolve prior to granulocyte recovery. In some
dis). Infections that result from the lack of a functional cellular immune
cases, patients remain febrile after resolution of neutropenia. In these
system are described in Chap. 197. It is worth mentioning, however,
instances, the risk of sudden death from overwhelming bacteremia is
that patients undergoing intensive chemotherapy for any form of
greatly reduced, and the following diagnoses should be seriously con-
cancer will have not only defects due to granulocytopenia but also lym-
sidered: (1) fungal infection, (2) bacterial abscesses or undrained foci
phocyte dysfunction, which may be profound. Thus, these patients—
of infection, and (3) drug fever (including reactions to antimicrobial
especially those receiving glucocorticoid-containing regimens or drugs
agents as well as to chemotherapy or cytokines). In the proper setting,
that inhibit either T cell activation (calcineurin inhibitors or drugs like
viral infection or graft-versus-host disease should be considered. In
fludarabine, which affect lymphocyte function) or cytokine induc-
clinical practice, antibacterial therapy is usually discontinued when
tion—should be given prophylaxis for Pneumocystis pneumonia.
the patient is no longer neutropenic and all evidence of bacterial dis-
Patients receiving treatment that eliminates B cells (e.g., with
ease has been eliminated. Antifungal agents are then discontinued if
anti-CD20 antibodies or rituximab) are especially vulnerable to inter-
there is no evidence of fungal disease. If the patient remains febrile,
current viral infections. The incidence of progressive multifocal leuko-
a search for viral diseases or unusual pathogens is conducted while
encephalopathy (caused by JC virus) is elevated among these patients.
unnecessary cytokines and other drugs are systematically eliminated
■ THE HEMATOPOIETIC SYSTEM from the regimen.
Initial studies in the 1960s revealed a dramatic increase in the
incidence of infections (fatal and nonfatal) among cancer TREATMENT
patients with a granulocyte count of <500/μL. The use of pro-
phylactic antibacterial agents has reduced the number of bacterial Infections in Cancer Patients
infections, but 35–78% of febrile neutropenic patients being treated for
hematologic malignancies develop infections at some time during che- ANTIBACTERIAL THERAPY
motherapy. Aerobic pathogens (both gram-positive and gram-negative) Hundreds of antibacterial regimens have been tested for use in
predominate in all series, but the exact organisms isolated vary from patients with cancer. The major risk of infection is related to the
center to center. Infections with anaerobic organisms are uncommon. degree of neutropenia seen as a consequence of either the disease
Geographic patterns affect the types of fungi isolated. Tuberculosis and or the therapy. Many of the relevant studies have involved small
malaria are common causes of fever in the developing world and may populations in which the outcomes have generally been good, and
present in this setting as well. most have lacked the statistical power to detect differences among
Neutropenic patients are unusually susceptible to infection with a the regimens studied. Each febrile neutropenic patient should be
wide variety of bacteria; thus, antibiotic therapy should be initiated approached as a unique problem, with particular attention given to
Harrisons_20e_Part4_p0435-p0858.indd 508 6/1/18 5:40 PM
previous infections and recent antibiotic exposures. Several general or microbiologic reason to do so. Planned progressive therapy (the 509
guidelines are useful in the initial treatment of neutropenic patients serial, empirical addition of one drug after another without culture
with fever (Fig. 70-2): data) is not efficacious in most settings and may have unfortunate
consequences. Simply adding another antibiotic for fear that a
1. In the initial regimen, it is necessary to use antibiotics active against
gram-negative infection is present is a dubious practice. The syn-
both gram-negative and gram-positive bacteria (Table 70-4).
ergy exhibited by β-lactams and aminoglycosides against certain
2. Monotherapy with an aminoglycoside or an antibiotic lacking
gram-negative organisms (especially P. aeruginosa) provides the
good activity against gram-positive organisms (e.g., ciprofloxa-
rationale for using two antibiotics in this setting, but recent analyses
cin or aztreonam) is not adequate in this setting.
suggest that efficacy is not enhanced by the addition of aminogly-
3. The agents used should reflect both the epidemiology and the
cosides, while toxicity may be increased. Mere “double coverage,”
antibiotic resistance pattern of the hospital.
with the addition of a quinolone or another antibiotic that is not
4. If the pattern of resistance justifies its use, a single third-generation
likely to exhibit synergy, has not been shown to be of benefit and
cephalosporin constitutes an appropriate initial regimen in
may cause additional toxicities and side effects. Cephalosporins can
many hospitals.
cause bone marrow suppression, and vancomycin is associated with
5. Most standard regimens are designed for patients who have
neutropenia in some healthy individuals. Furthermore, the addition
not previously received prophylactic antibiotics. The develop-
of multiple cephalosporins may induce β-lactamase production by
ment of fever in a patient who has received antibiotics affects
some organisms; cephalosporins and double β-lactam combinations
the choice of subsequent therapy, which should target resistant
should probably be avoided altogether in Enterobacter infections.
organisms and organisms known to cause infections in patients
being treated with the antibiotics already administered. ANTIFUNGAL THERAPY
6. Randomized trials have indicated the safety of oral antibiotic Fungal infections in cancer patients are most often associated with
regimens in the treatment of “low-risk” patients with fever
neutropenia. Neutropenic patients are predisposed to the develop-
and neutropenia. Outpatients who are expected to remain
CHAPTER 70
ment of invasive fungal infections, most commonly those due to Can-
neutropenic for <10 days and who have no concurrent medical
dida and Aspergillus species and occasionally those caused by Mucor,
problems (such as hypotension, pulmonary compromise, or
Rhizopus, Fusarium, Trichosporon, Bipolaris, and others. Cryptococcal
abdominal pain) can be classified as low risk and treated with a
infection, which is common among patients taking immunosup-
broad-spectrum oral regimen.
pressive agents, is uncommon among neutropenic patients receiv-
7. Several large-scale studies indicate that prophylaxis with a
ing chemotherapy for AML. Invasive candidal disease is usually
Infections in Patients with Cancer
fluoroquinolone (ciprofloxacin or levofloxacin) decreases mor-
caused by C. albicans or C. tropicalis but can be caused by C. krusei,
bidity and mortality rates among afebrile patients who are
C. parapsilosis, and C. glabrata.
anticipated to have neutropenia of long duration.
For decades, it has been common clinical practice to add
Commonly used antibiotic regimens for the treatment of febrile amphotericin B to antibacterial regimens if a neutropenic patient
patients in whom prolonged neutropenia (>7 days) is anticipated remains febrile despite 4–7 days of treatment with antibacterial
include (1) ceftazidime or cefepime, (2) piperacillin/tazobactam, agents. The rationale for this empirical addition is that it is difficult
or (3) imipenem/cilastatin or meropenem. All three regimens have to culture fungi before they cause disseminated disease and that
shown equal efficacy in large trials. All three are active against mortality rates from disseminated fungal infections in granulocy-
P. aeruginosa and a broad spectrum of aerobic gram-positive and topenic patients are high. Before the introduction of newer azoles
gram-negative organisms. Imipenem/cilastatin has been associated into clinical practice, amphotericin B was the mainstay of antifun-
with an elevated rate of C. difficile diarrhea, and many centers reserve gal therapy. The insolubility of amphotericin B has resulted in the
carbapenem antibiotics for treatment of gram-negative bacteria that marketing of several lipid formulations that are less toxic than
produce extended-spectrum β-lactamases; these limitations make the amphotericin B deoxycholate complex. Echinocandins (e.g.,
carbapenems less attractive as an initial regimen. Despite the fre- caspofungin) are useful in the treatment of infections caused by
quent involvement of coagulase-negative staphylococci, the initial azole-resistant Candida strains as well as in therapy for aspergillosis
use of vancomycin or its automatic addition to the initial regimen and have been shown to be equivalent to liposomal amphotericin
has not resulted in improved outcomes, and the antibiotic does B for the empirical treatment of patients with prolonged fever and
exert toxic effects. For these reasons, only judicious use of van- neutropenia. Newer azoles have also been demonstrated to be
comycin is recommended—for example, when there is good reason effective in this setting. Although fluconazole is efficacious in the
to suspect the involvement of coagulase-negative staphylococci treatment of infections due to many Candida species, its use against
(e.g., the appearance of erythema at the exit site of a catheter or serious fungal infections in immunocompromised patients is lim-
a positive culture for methicillin-resistant S. aureus or coagulase- ited by its narrow spectrum: it has no activity against Aspergillus or
negative staphylococci). Because the sensitivities of bacteria vary against several non-albicans Candida species. The broad-spectrum
from hospital to hospital, clinicians are advised to check their local azoles (e.g., voriconazole and posaconazole) provide another option
sensitivities and to be aware that resistance patterns can change for the treatment of Aspergillus infections (Chap. 212), including CNS
quickly, necessitating a change in approach to patients with fever infection. Clinicians should be aware that the spectrum of each azole
and neutropenia. Similarly, infection control services should mon- is somewhat different and that no drug can be assumed to be effica-
itor for basic antibiotic resistance and for fungal infections. The cious against all fungi. Aspergillus terreus is resistant to amphotericin
appearance of a large number of Aspergillus infections, in particular, B. Although voriconazole is active against Pseudallescheria boydii,
suggests the possibility of an environmental source that requires amphotericin B is not; however, voriconazole has no activity against
further investigation and remediation. Mucor. Posaconazole, which is administered orally, is useful as a
The initial antibacterial regimen should be refined on the basis prophylactic agent in patients with prolonged neutropenia. Studies
of culture results (Fig. 70-2). Blood cultures are the most relevant in progress are assessing the use of these agents in combinations. For
basis for selection of therapy; surface cultures of skin and mucous a full discussion of antifungal therapy, see Chap. 206.
membranes may be misleading. In the case of gram-positive bac-
teremia or another gram-positive infection, it is important that the ANTIVIRAL THERAPY
antibiotic be optimal for the organism isolated. Once treatment with The availability of a variety of agents active against herpes-group
broad-spectrum antibiotics has begun, it is not desirable to discon- viruses, including some new agents with a broader spectrum of activ-
tinue all antibiotics because of the risk of failing to treat a potentially ity, has heightened focus on the treatment of viral infections, which
fatal bacterial infection; the addition of more and more antibacterial pose a major problem in cancer patients. Viral diseases caused by the
agents to the regimen is not appropriate unless there is a clinical herpes group are prominent. Serious (and sometimes fatal) infections
Harrisons_20e_Part4_p0435-p0858.indd 509 6/1/18 5:40 PM
initial India ink examination (evidence of a heavy fungal burden), high advent of Candida species as common human pathogens dates to the 1529
CSF pressure, low CSF glucose levels, low CSF pleocytosis (<2/μL), introduction of modern therapeutic approaches that suppress normal
recovery of yeast cells from extraneural sites, absence of antibody to host-defense mechanisms. Of these relatively recent advances, the most
capsular polysaccharide, a CSF or serum cryptococcal antigen level of important is the use of antibacterial agents that alter the normal human
≥1:32, and concomitant glucocorticoid therapy or hematologic malig- microbiota and allow nonbacterial species to become more prevalent
nancy. A response to treatment does not guarantee cure since relapse of in the commensal flora. With the introduction of antifungal agents,
cryptococcosis is common even among patients with relatively intact the causes of Candida infections shifted from an almost complete dom-
immune systems. Complications of CNS cryptococcosis include cranial inance of C. albicans to the common involvement of C. glabrata and the
nerve deficits, vision loss, and cognitive impairment. other species listed above. The non-albicans species now account for
approximately half of all cases of candidemia and hematogenously
■ IMMUNE RECONSTITUTION INFLAMMATORY disseminated candidiasis. Recognition of this change is clinically
SYNDROME important, since the various species differ in susceptibility to the newer
The frequent chronicity of cryptococcal infections and their common antifungal agents.
occurrence in settings of changing immunity can result in new clinical Candida is a small, thin-walled, ovoid yeast that measures 4–6 μm in
syndromes, such as the immune reconstitution inflammatory syn- diameter and reproduces by budding. Organisms of this genus occur in
drome (IRIS). IRIS occurs when immunity rebounds in the setting of three forms in tissue: blastospores, pseudohyphae, and hyphae. Candida
treated cryptococcosis (or an undiagnosed asymptomatic infection) grows readily on simple medium; lysis centrifugation enhances its
and the immune response to cryptococcal antigens in tissue triggers recovery from blood. Species are identified by biochemical testing (cur-
an inflammatory response that can be difficult to distinguish from rently with automated devices) or on special agar (e.g., CHROMagar).
a relapsing infection. IRIS can occur when patients with AIDS and
treated cryptococcosis are given antiretroviral therapy that results ■ EPIDEMIOLOGY
in improved immunity. Apart from the difficulties in distinguishing Candida are present in humans as commensals, in animals, in
IRIS from cryptococcal relapse, the management of this syndrome is foods, and on inanimate objects. In developed countries, where
complex because it is caused by the desirable outcome of improving contemporary medical therapeutics are commonly used, Candida
immunity, which is important in controlling cryptococcal infection species are now among the most common nosocomial pathogens. In the
and preventing relapses. The approach to the patient with IRIS must United States, these species are the fourth most common isolates from
attempt to balance resurgent immunity against immune-mediated the blood of hospitalized patients. In a recent point-prevalence study,
damage. Currently, management of IRIS is individualized and can Candida species were the most common organisms infecting the blood-
CHAPTER 211 Candidiasis
involve the use of glucocorticoids to reduce inflammation. stream of hospitalized patients. In regions where advanced medical care
is rarely available, mucocutaneous Candida infections, such as thrush,
■ PREVENTION are more common than deep-organ infections, which rarely occur.
No vaccine is available for cryptococcosis. In patients at high risk (e.g., However, the incidence of deep-organ candidiasis increases steadily as
those with advanced HIV infection and CD4+ T lymphocyte counts of advances in health care—such as therapy with broad-spectrum antibi-
<200/μL), primary prophylaxis with fluconazole (200 mg/d) is effec- otics, more aggressive treatment of cancer, and the use of immunosup-
tive in reducing the prevalence of disease. Since antiretroviral therapy pression for sustaining organ transplants—are implemented. In
raises the CD4+ T lymphocyte count, it constitutes an immunologic aggregate, the global incidence of infections due to Candida species has
form of prophylaxis. risen steadily over the past few decades. Of great recent concern has
■ FURTHER READING been the global emergence of C. auris; certain strains of this organism
Kwon-Chung KJ et al: The case for adopting the “species complex” are resistant to all classes of antifungal agents, and mortality rates from
nomenclature for the etiologic agents of cryptococcosis. mSphere infection have been very high.
2 pii:e00357, 2017.
Maziarz EK, Perfect JR: Cryptococcosis. Infect Dis Clin North Am ■ PATHOGENESIS
30:179, 2016. In the most serious form of Candida infection, the organisms dissem-
Robertson EJ et al: Cryptococcus neoformans ex vivo capsule size is inate hematogenously and form microabscesses and small macroab-
associated with intracranial pressure and host immune response in scesses in major organs. Although the exact mechanism is not known,
HIV-associated cryptococcal meningitis. J Infect Dis 209:74, 2014. Candida probably enters the bloodstream from mucosal surfaces after
Saag MS et al: Practice guidelines for the management of cryptococcal growing to large numbers as a consequence of bacterial suppression
disease. Infectious Diseases Society of America. Clin Infect Dis 30:710, by antibacterial drugs; alternatively, in some instances, the organism
2000. may enter from the skin. A change from the blastospore stage to the
Srichatrapimuk S, Sungkanuparph S: Integrated therapy for HIV pseudohyphal and hyphal stages is generally considered integral to
and cryptococcosis. AIDS Res Ther 13:42, 2016. Candida’s penetration into tissue. However, C. glabrata can cause exten-
sive infection even though it does not transform into pseudohyphae or
hyphae. Adherence to both epithelial and endothelial cells is thought to
be the first step in invasion and infection; several adhesins have been
identified as well as a mucosal toxin, candidalysin. Biofilm formation
211 Candidiasis
also is considered important in pathogenesis. Numerous reviews of
cases of hematogenously disseminated candidiasis have identified
the predisposing factors or conditions associated with disseminated
John E. Edwards, Jr. disease (Table 211-1). Women who receive antibacterial agents may
develop vaginal candidiasis.
Innate immunity is the most important defense mechanism against
The genus Candida encompasses >150 species, only a few of which hematogenously disseminated candidiasis, and the neutrophil is the
cause disease in humans. With rare exceptions (although the excep- most important component of this defense. Macrophages also play an
tions are increasing in number), the human pathogens are C. albicans, important defensive role. STAT1, Dectin-1, CARD9, and TH1 and TH17
C. guilliermondii, C. krusei, C. parapsilosis, C. tropicalis, C. kefyr, C. lusitaniae, lymphocytes contribute significantly to innate defense (see “Clinical Man-
C. dubliniensis, C. glabrata, and C. auris. Ubiquitous in nature, they ifestations,” below). Although many immunocompetent individuals have
inhabit the gastrointestinal tract (including the mouth and orophar- antibodies to Candida, the role of these antibodies in defense against the
ynx), the female genital tract, and the skin. Although cases of candid- organism is not clear. Multiple genetic polymorphisms that predispose to
iasis have been described since antiquity in debilitated patients, the disseminated candidiasis will most likely be identified in future studies.
Harrisons_20e_Part5_p0859-p1648.indd 1529 6/1/18 12:10 PM
1530 TABLE 211-1 Well-Recognized Factors and Conditions Predisposing organs as well as the skin. While the lesions are seen predominantly in
to Hematogenously Disseminated Candidiasis immunocompromised patients treated with cytotoxic drugs, they may
Antibacterial agents Abdominal and thoracic surgery also develop in patients without neutropenia.
Indwelling intravenous catheters Cytotoxic chemotherapy Chronic mucocutaneous candidiasis is a heterogeneous infection of
Hyperalimentation fluids Immunosuppressive agents for organ the hair, nails, skin, and mucous membranes that persists despite
transplantation intermittent therapy. The onset of disease usually comes in infancy or
Indwelling urinary catheters
Respirators within the first two decades of life, but in rare cases comes in later life.
Parenteral glucocorticoids
Neutropenia
The condition may be mild and limited to a specific area of the skin or
Severe burns
nails, or it may take a severely disfiguring form (Candida granuloma)
HIV-associated low CD4+ T-cell counts Low birth weight (neonates)
characterized by exophytic outgrowths on the skin. Chronic mucocu-
Diabetes
taneous candidiasis is usually associated with specific immunologic
dysfunction; most frequently reported is a failure of T lymphocytes to
proliferate or to excrete cytokines in response to stimulation by Candida
■ CLINICAL MANIFESTATIONS
antigens in vitro. A subset of the affected patients have mutations in the
Mucocutaneous Candidiasis Thrush is characterized by white, STAT1 gene resulting in an insufficiency of interferon γ, interleukin 17,
adherent, painless, discrete or confluent patches in the mouth, on the and interleukin 22.
tongue, or in the esophagus, occasionally with fissuring at the corners Approximately half of patients with chronic mucocutaneous
of the mouth. This form of disease caused by Candida can also occur at candidiasis have associated endocrine abnormalities that together
points of contact with dentures. Organisms are identifiable in gram- are designated the autoimmune polyendocrinopathy–candidiasis–
stained scrapings from lesions. The occurrence of thrush in a young, ectodermal dystrophy (APECED) syndrome. This syndrome is due
otherwise healthy-appearing person should prompt an investigation to mutations in the autoimmune regulator (AIRE) gene and is most
for underlying HIV infection. More commonly, thrush is seen as a prevalent among Finns, Iranian Jews, Sardinians, northern Italians,
nonspecific manifestation of severe debilitating illness. Vulvovaginal and Swedes. Conditions that usually follow the onset of the disease
candidiasis is accompanied by pruritus, pain, and vaginal discharge, include hypoparathyroidism, adrenal insufficiency, autoimmune thy-
which is usually thin but may contain whitish “curds” in severe cases. roiditis, Graves’ disease, chronic active hepatitis, alopecia, juvenile-
A subset of patients with recurrent vulvovaginitis have a deficiency onset pernicious anemia, malabsorption, and primary hypogonadism.
in the surface expression of Dectin-1, a major recognition factor for In addition, dental enamel dysplasia, vitiligo, pitted nail dystrophy,
β-glucan on Candida. This deficiency leads to suboptimal functioning and calcification of the tympanic membranes may occur. Patients with
of the CARD9 pathway, which ultimately increases the propensity for chronic mucocutaneous candidiasis rarely develop hematogenously
PART 5
recurrent vaginal infections. disseminated candidiasis, probably because their neutrophil function
Other Candida skin infections include paronychia, a painful swelling remains intact.
at the nail–skin interface; onychomycosis, a fungal nail infection rarely
caused by this genus; intertrigo, an erythematous irritation with red- Deeply Invasive Candidiasis Deeply invasive Candida infec-
ness and pustules in the skin folds; balanitis, an erythematous-pustular tions may or may not be due to hematogenous seeding. Deep esophageal
Infectious Diseases
infection of the glans penis; erosio interdigitalis blastomycetica, an infec- infection may result from penetration by organisms from superficial
tion between the digits of the hands or toes; folliculitis, with pustules esophageal erosions; joint or deep-wound infection from contiguous
developing most frequently in the area of the beard; perianal candidiasis, spread of organisms from the skin; kidney infection from catheter-
a pruritic, erythematous, pustular infection surrounding the anus; initiated spread of organisms through the urinary tract; infection of
and diaper rash, a common erythematous, pustular perineal infection intraabdominal organs and the peritoneum from perforation of the gas-
in infants. Generalized disseminated cutaneous candidiasis, another form trointestinal tract; and gallbladder infection from retrograde migration of
of infection that occurs primarily in infants, is characterized by wide- organisms from the gastrointestinal tract into the biliary drainage system.
spread eruptions over the trunk, thorax, and extremities. The diagnos- However, far more commonly, deeply invasive candidiasis results
tic macronodular lesions of hematogenously disseminated candidiasis from hematogenous seeding of various organs as a complication of can-
(Fig. 211-1) indicate a high probability of dissemination to multiple didemia. Once the organism gains access to the intravascular compart-
ment (either from the gastrointestinal tract or, less often, from the skin
through the site of an indwelling intravascular catheter), it may spread
hematogenously to a variety of deep organs. The brain, chorioretina
(Fig. 211-2), heart, and kidneys are most commonly infected and the
liver and spleen less commonly so (most often in neutropenic patients).
In fact, nearly any organ can become involved, including the endocrine
glands, pancreas, heart valves (native or prosthetic), skeletal muscle,
joints (native or prosthetic), bones, and meninges. Candida organisms can
also spread hematogenously to the skin and cause classic macronodular
lesions (Fig. 211-1). Frequently, painful muscular involvement is evident
beneath the area of affected skin. Chorioretinal involvement and skin
involvement are highly significant, since both findings are associated
with a very high probability of abscess formation in multiple deep
organs as a result of generalized hematogenous seeding. Ocular involve-
ment (Fig. 211-2) may require specific treatment (e.g., partial vitrectomy
or intraocular injection of antifungal agents) to prevent permanent
blindness. An ocular examination is indicated for all patients with can-
didemia, whether or not they have ocular manifestations.
■ DIAGNOSIS
FIGURE 211-1 Macronodular skin lesions associated with hematogenously The diagnosis of Candida infection is established by visualization of pseu-
disseminated candidiasis. Candida organisms are usually but not always visible dohyphae or hyphae on wet mount (saline and 10% KOH), tissue Gram’s
on histopathologic examination. The fungi grow when a portion of the biopsied
specimen is cultured. Therefore, for optimal identification, both histopathology stain, periodic acid–Schiff stain, or methenamine silver stain in the pres-
and culture should be performed. (Image courtesy of Dr. Noah Craft and the Victor ence of inflammation. Absence of organisms on hematoxylin-eosin stain-
Newcomer collection at UCLA, archived by Logical Images, Inc.; with permission.) ing does not reliably exclude Candida infection. The most challenging
Harrisons_20e_Part5_p0859-p1648.indd 1530 6/1/18 12:10 PM
TABLE 211-2 Treatment of Mucocutaneous Candidal Infections 1531
DISEASE PREFERRED TREATMENT ALTERNATIVES
Cutaneous Topical azole Topical nystatin
Vulvovaginal Oral fluconazole (150 mg) or Nystatin suppository
azole cream or suppository
Oral (thrush) Clotrimazole troches Nystatin, fluconazole
Esophageal Fluconazole tablets (100–200 Caspofungin, micafungin,
mg/d) or itraconazole solution or amphotericin B
(200 mg/d)
formulations of amphotericin B, three echinocandins, and the azoles
fluconazole and voriconazole are used; no agent within a given class
has been clearly identified as superior to the others. Most institutions
choose an agent from each class on the basis of their own specific
microbial epidemiology, strategies to minimize toxicities, and cost
considerations. There is a trend to treat with an echinocandin until
FIGURE 211-2 Hematogenous Candida endophthalmitis. A classic off-white lesion sensitivities or speciation is determined. In stable patients, many
projecting from the chorioretina into the vitreous causes the surrounding haze. centers then switch to fluconazole if a sensitive strain is identified
The lesion is composed primarily of inflammatory cells rather than organisms. and there is no evidence of hematogenous disemination. For hemo-
Lesions of this type may progress to cause extensive vitreal inflammation and dynamically unstable or neutropenic patients, initial treatment with
eventual loss of the eye. Partial vitrectomy, combined with IV and possibly
intravitreal antifungal therapy, may be helpful in controlling the lesions. (Image broader-spectrum agents is desirable; these drugs include polyenes,
courtesy of Dr. Gary Holland; with permission.) echinocandins, or later-generation azoles such as voriconazole. Once
the clinical response has been assessed and the pathogen specifically
identified, the regimen can be altered accordingly. At present, the
aspect of diagnosis is determining which patients with Candida isolates vast majority of C. albicans isolates are sensitive to fluconazole. Iso-
have hematogenously disseminated candidiasis. For instance, recovery lates of C. glabrata and C. krusei are less sensitive to fluconazole and
of Candida from sputum, urine, or peritoneal catheters may indicate more sensitive to polyenes and echinocandins. C. parapsilosis is less
CHAPTER 211 Candidiasis
mere colonization rather than deep-seated infection, and Candida isola- sensitive to echinocandins in vitro; however, this lesser sensitivity
tion from the blood of patients with indwelling intravascular catheters is considered insignificant. Posaconazole has been approved for
may reflect inconsequential seeding of the blood from or growth of the prophylaxis, including that against Candida, in neutropenic patients.
organisms on the catheter. Despite extensive research into both antigen Itraconazole is rarely used for Candida, and isavuconazole has not
and antibody detection systems, there is currently no widely available been approved for this indication to date.
and validated diagnostic test to distinguish patients with inconsequen- Some generalizations exist regarding the management of specific
tial seeding of the blood from those whose positive blood cultures rep- Candida infections. Recovery of Candida from sputum is almost never
resent hematogenous dissemination to multiple organs. Many studies indicative of underlying pulmonary candidiasis and does not by
are under way to establish the utility of the β-glucan test; at present, its itself warrant antifungal treatment. Similarly, Candida in the urine
greatest utility is its negative predictive value (~90%). Meanwhile, the of a patient with an indwelling bladder catheter may represent col-
presence of ocular or macronodular skin lesions is highly suggestive onization only rather than bladder or kidney infection; however, the
of widespread infection of multiple deep organs. Despite extensive threshold for systemic treatment is lower in severely ill patients in
tests for hematogenous dissemination, such as polymerase chain reac- this category since it is impossible to distinguish colonization from
tion and T2 technology, no test is fully validated or widely available lower or upper urinary tract infection. If the isolate is C. albicans,
at present. Matrix-assisted laser desorption–ionization–time-of-flight most clinicians use oral fluconazole rather than a bladder washout
mass spectometry (MALDI-TOF MS) will likely be used extensively for with amphotericin B, which was more commonly used in the past.
detection and speciation in the future. Caspofungin has been used with success; although echinocandins
are poorly excreted into the urine, they may be an option, especially
for non-albicans isolates. The doses and duration are the same as
TREATMENT for disseminated candidiasis. The significance of the recovery of
Candida Infections Candida from abdominal drains in postoperative patients is unclear,
but again the threshold for treatment is generally low because most
MUCOCUTANEOUS CANDIDA INFECTION of the affected patients have been subjected to factors predisposing
The treatment of mucocutaneous candidiasis is summarized in to disseminated candidiasis. In addition, there has been a consid-
Table 211-2. erable increase in the recognition and diagnosis of intraabdominal
candidiasis.
CANDIDEMIA AND SUSPECTED HEMATOGENOUSLY Removal of the infected valve and long-term antifungal admin-
DISSEMINATED CANDIDIASIS istration constitute appropriate treatment for Candida endocarditis.
All patients with candidemia are treated with a systemic antifungal Although definitive studies are not available, patients usually are
agent. A certain percentage of patients, including many of those who treated for weeks with a systemic antifungal agent (Table 211-3)
have candidemia associated with an indwelling intravascular cath- and then given chronic suppressive therapy for months or years
eter, probably have “benign” candidemia rather than deep-organ (sometimes indefinitely) with an oral azole (usually fluconazole at
seeding. However, because there is no reliable way to distinguish 400–800 mg/d).
benign candidemia from deep-organ infection, and because antifun- Hematogenous Candida endophthalmitis is a special problem
gal drugs less toxic than amphotericin B are available, antifungal requiring ophthalmologic consultation. When lesions are expanding
treatment for candidemia—with or without clinical evidence of or are threatening the macula, an IV polyene combined with flucyto-
deep-organ involvement—has become the standard of practice. In sine (25 mg/kg four times daily) has been the regimen of choice,
addition, if an indwelling intravascular catheter is present, it is best although comparative studies with other regimens have not yet
to remove or replace the device whenever feasible. been reported. As more data on the azoles (e.g., voriconazole) and
The drugs used for the treatment of candidemia and suspected the echinocandins become available, new strategies involving these
disseminated candidiasis are listed in Table 211-3. Various lipid agents are developing. Of paramount importance is the decision to
Harrisons_20e_Part5_p0859-p1648.indd 1531 6/1/18 12:10 PM
1532 TABLE 211-3 Agents for the Treatment of Disseminated Candidiasis
AGENT ROUTE OF ADMINISTRATION DOSEa COMMENT
Amphotericin B deoxycholate IV only 0.5–1.0 mg/kg daily Being replaced by lipid formulations
Amphotericin B lipid formulations Not approved as primary therapy by the U.S. Food and Drug
Administration, but used commonly because less toxic than
amphotericin B deoxycholate
Liposomal (AmBiSome, Abelcet) IV only 3.0–5.0 mg/kg daily
Lipid complex (ABLC) IV only 3.0–5.0 mg/kg daily
Colloidal dispersion (ABCD) IV only 3.0–5.0 mg/kg daily Associated with frequent infusion reactions
Azolesb
Posaconazole IV and oral 300 mg/d (IV) Approved for prophylaxis
200 mg tid (oral)
Fluconazole IV and oral 400 mg/d Most commonly used
Voriconazole IV and oral 400 mg/d Multiple drug interactions
Approved for candidemia in nonneutropenic patients
Echinocandins Broad spectrum against Candida species; approved for
disseminated candidiasis
Caspofungin IV only 50 mg/d
Anidulafungin IV only 100 mg/d
Micafungin IV only 100 mg/d
a
For loading doses and adjustments in renal failure, see Pappas PG et al: Clinical practice guidelines for the management of candidiasis: 2016 update by the Infectious
Diseases Society of America. Clin Infect Dis 62:e1, 2016. The recommended duration of therapy is 2 weeks beyond the last positive blood culture and the resolution of
signs and symptoms of infection. bAlthough ketoconazole is approved for the treatment of disseminated candidiasis, it has been replaced by the newer agents listed in
this table. Posaconazole has been approved for prophylaxis in neutropenic patients and for oropharyngeal candidiasis.
perform a partial vitrectomy. This procedure debulks the infection ■ FURTHER READING
and can preserve sight, which may otherwise be lost due to vitreal Edwards JE Jr: Candida species, in Mandell, Douglas, and Bennett’s Prin-
scarring. All patients with candidemia should undergo ophthal- ciples of Infectious Diseases, 8th ed. JE Bennett et al (eds). Philadelphia,
PART 5
mologic examination because of the relatively high frequency of Elsevier, 2015, pp 2879–2894.
this ocular complication. Not only can this examination detect a Pappas PG et al: Clinical practice guideline for the management of can-
developing eye lesion early in its course; in addition, identification didiasis. 2016 update by the Infectious Diseases Society of America.
of a lesion signifies a probability of ~90% of deep-organ abscesses Clin Infect Dis 62:e1, 2016.
Infectious Diseases
and may prompt prolongation of therapy for candidemia beyond Uppuluri P et al: Current trends in candidiasis, in Candida albicans: Cellular
the recommended 2 weeks after the last positive blood culture. and Molecular Biology, 2nd ed. R Prasad (ed). Cham, Switzerland,
Although the basis for the consensus is a very small data set, Springer, 2017, pp 5–24.
the recommended treatment for Candida meningitis is a polyene
(Table 211-3) plus flucytosine (25 mg/kg four times daily). Suc-
cessful treatment of Candida-infected prosthetic material (e.g.,
an artificial joint) nearly always requires removal of the infected
material followed by long-term administration of an antifungal
agent selected on the basis of the isolate’s sensitivity and the logistics
of administration. 212 Aspergillosis
David W. Denning
■ PROPHYLAXIS
The use of antifungal agents to prevent Candida infections has been
controversial, but some general principles have emerged. Most centers Aspergillosis is the collective term used to describe all disease enti-
administer prophylactic fluconazole (400 mg/d) to recipients of alloge- ties caused by any one of ~50 pathogenic and allergenic species of
neic stem cell transplants. High-risk liver transplant recipients also are Aspergillus. Only those species that grow at 37°C can cause invasive
given fluconazole prophylaxis in most centers. The use of prophylaxis infection, although some species without this ability can cause allergic
for neutropenic patients has varied considerably from center to center; syndromes. Each common pathogenic species is actually a complex
many centers that elect to give prophylaxis to this population use either of many species (many of them cryptic), but is referred to as a single
fluconazole (200–400 mg/d) or a lipid formulation of amphotericin B species here for simplicity. A. fumigatus is responsible for most cases
(AmBiSome, 1–2 mg/d). Caspofungin (50 mg/d) also has been recom- of invasive aspergillosis, almost all cases of chronic aspergillosis, and
mended. Some centers have used itraconazole suspension (200 mg/d). most allergic syndromes. A. flavus is more prevalent in some hospitals
Posaconazole (200 mg three times daily) has been approved by the U.S. and causes a higher proportion of cases of sinus infections, cutaneous
Food and Drug Administration for prophylaxis in neutropenic patients; infections, and keratitis than A. fumigatus. A. niger can cause invasive
it is gaining in popularity and may replace fluconazole. infection but more commonly colonizes the respiratory tract and causes
Prophylaxis is sometimes given to surgical patients at very high risk. external otitis. A. terreus causes only invasive disease, usually with a
The widespread use of prophylaxis for nearly all patients in general poor prognosis. A. nidulans occasionally causes invasive infection, pri-
surgical or medical intensive care units is not—and should not be—a marily in patients with chronic granulomatous disease.
common practice for three reasons: (1) the incidence of disseminated
candidiasis is relatively low, (2) the cost–benefit ratio is suboptimal, ■ EPIDEMIOLOGY AND ECOLOGY
and (3) increased resistance with widespread prophylaxis is a valid Aspergillus has a worldwide distribution, most commonly growing
concern. in decomposing plant materials (i.e., compost) and in bedding. This
Prophylaxis for oropharyngeal or esophageal candidiasis in hyaline (nonpigmented), septate, branching mold produces vast num-
HIV-infected patients is not recommended unless there are frequent bers of conidia (spores) on stalks above the surface of mycelial growth.
recurrences. Aspergilli are found in indoor and outdoor air, on surfaces, and in
Harrisons_20e_Part5_p0859-p1648.indd 1532 6/1/18 12:10 PM
TABLE 212-1 Disease Frequency and Diagnostic Sensitivity for that, in patients who are not immunocompromised, temporary abroga- 1533
Different Manifestations of Aspergillosis tion of protective responses as a result of glucocorticoid use or a gen-
TYPE OF DISEASE eral anti-inflammatory state is a significant risk factor. Many patients
have some evidence of prior pulmonary disease—typically, a history
PARAMETER INVASIVE CHRONIC ALLERGIC
of pneumonia or chronic obstructive pulmonary disease. Many new
Incidence/100,000a 3.5 10.4 ?b
immunomodulating agents, such as infliximab and ibrutinib, increase
Prevalence/100,000a — 32.8 286c the risk of invasive aspergillosis, as do severe liver disease and high
Global burdena ~250,000 ~3,000,000 ~10,000,000 levels of stored iron in bone marrow. Influenza infection and extracor-
Mortality rate without ~100% ~50% <1% poreal membrane oxygenation therapy have recently been recognized
treatment as risk factors.
Respiratory Diagnostic Sensitivityd Patients with chronic pulmonary aspergillosis have a wide spectrum
Culture ✓ ✓ ✓ of underlying pulmonary disease, including tuberculosis, prior pneu-
Microscopye ✓ ✓ ? mothorax, or chronic obstructive pulmonary disease. These patients are
Antigen ✓✓✓ ✓✓ ✓✓✓ immunocompetent except for some cytokine-regulation defects, most
Real-time PCR
of which are consistent with an inability to mount an inflammatory
✓✓✓ ✓✓✓ ✓✓✓
immune (TH1-like) response or to control it adequately. Glucocorticoids
Blood Diagnostic Sensitivityd accelerate disease progression.
Culture × × × Allergic bronchopulmonary aspergillosis (ABPA) complicates asthma
Antigen ✓✓ ✓ × and cystic fibrosis. Many genetic associations indicate a strong basis for
β-D-glucan ✓✓ ✓ ? the development of a TH2-like and “allergic” response to A. fumigatus.
Real-time PCR ✓✓ × × Remarkably, high-dose glucocorticoid treatment for exacerbations of
IgG antibody ✓ ✓✓✓✓ ✓✓ ABPA almost never leads to invasive aspergillosis. Most patients with
IgE antibody × ✓✓ ✓✓✓✓
Aspergillus bronchitis have bronchiectasis, including those with cystic
fibrosis.
a
http://www.gaffi.org/roadmap/. bAllergic fungal disease can develop at any Different genetic traits are associated with invasive, chronic, and
age, usually in adulthood; the annual frequency with which it occurs is not
known. cAllergic bronchopulmonary aspergillosis and severe asthma with fungal allergic aspergillosis; the majority of people probably are not at
sensitization. dKey for sensitivity: 1 check = limited (as the text indicates, 10–30% risk for aspergillosis. Multiple gene variants appear to be neces-
for culture); 2 checks = higher; 3 checks = >80%; and 4 checks = ~95%. sary for susceptibility to each form of aspergillosis.
High-volume fungal culture increases sensitivity to the same level as PCR.
CHAPTER 212 Aspergillosis
e
Abbreviation: PCR, polymerase chain reaction. ■ CLINICAL FEATURES AND APPROACH TO THE
PATIENT
(Table 212-2)
water from surface reservoirs. Daily exposures vary from a few to
many millions of conidia; high numbers of conidia are encountered in Invasive Pulmonary Aspergillosis Both the frequency of
hay barns and other very dusty environments. The required size of the invasive disease and the pace of its progression increase with greater
infecting inoculum is uncertain; however, only intense exposures (e.g., degrees of immunocompromise. Invasive aspergillosis is arbitrarily
during construction work, handling of moldy bark or hay, or com- classified as acute and subacute, with courses of ≤1 month and
posting) are sufficient to cause disease—acute community-acquired 1–3 months, respectively. More than 80% of cases of invasive asper-
pulmonary aspergillosis—in healthy immunocompetent individuals. gillosis involve the lungs. The most common clinical features are no
Allergic syndromes may be exacerbated by continuous antigenic expo- symptoms at all, fever, cough (sometimes productive), nondescript
sure arising from sinus or airway colonization or from nail infection. chest discomfort, trivial hemoptysis, and shortness of breath. Although
High-efficiency particulate air (HEPA) filtration is often protective the fever often responds to glucocorticoids, the disease progresses. The
against infection; thus HEPA filters should be installed and monitored keys to early diagnosis in at-risk patients are a high index of suspicion,
for efficiency in operating rooms and in areas of the hospital that house screening for circulating antigen (in leukemia), and urgent CT of the
high-risk patients. thorax. Invasive aspergillosis is one of the most common diagnostic
The incubation period of invasive aspergillosis after exposure is errors revealed at autopsy.
highly variable, extending in documented cases from 2 to 90 days.
Thus community acquisition of an infecting strain frequently manifests Invasive Sinusitis The sinuses are involved in 5–10% of cases of
as invasive infection during hospitalization, although nosocomial invasive aspergillosis, especially affecting patients with leukemia and
acquisition is also common. Outbreaks usually are directly related to a recipients of hematopoietic stem cell transplants. In addition to fever,
contaminated air source in the hospital. the most common features are nasal or facial discomfort, blocked nose,
Global aspergillosis incidence and prevalence have been esti- and nasal discharge (sometimes bloody). Endoscopic examination of
mated (Table 212-1). The frequency of different manifestations the nose reveals pale, dusky or necrotic-looking tissue in any location.
of aspergillosis varies considerably with geographic location; CT or MRI of the sinuses is essential but does not distinguish invasive
most notably, chronic granulomatous sinusitis is rare outside the Mid- Aspergillus sinusitis from preexisting allergic or bacterial sinusitis early
dle East and India. Fungal (mycotic) keratitis is particularly common in in the disease process.
Nepal, Myanmar, Bhutan, and India but occurs globally. Chronic pul- Tracheobronchitis Occasionally, only the airways are infected by
monary aspergillosis follows pulmonary tuberculosis in ~6–10% of Aspergillus. The resulting manifestations seen on bronchoscopy range
treated cases and also mimics pulmonary tuberculosis as smear- from acute or chronic bronchitis to ulcerative or pseudomembranous
negative or “clinically diagnosed” tuberculosis. tracheobronchitis. These entities are particularly common among lung
transplant recipients and patients on artificial ventilation. Obstruction
■ RISK FACTORS AND PATHOGENESIS with mucous plugs may occur and is called obstructing bronchial
The primary risk factors for invasive aspergillosis are profound neu- aspergillosis in immunocompromised patients and mucous impaction
tropenia and glucocorticoid use; risk increases with longer duration of in other patients, such as those with ABPA.
these conditions. Higher doses of glucocorticoids increase the risk of
both acquisition of invasive aspergillosis and death from the infection. Aspergillus Bronchitis Recurrent chest infections that only par-
Neutrophil and/or phagocyte dysfunction also is an important risk tially improve with antibiotic treatment and are associated with signifi-
factor, as evidenced by aspergillosis in chronic granulomatous disease, cant breathlessness or coughing up of thick sputum plugs are typical
advanced HIV infection, and relapsed leukemia. An increasing inci- features of Aspergillus bronchitis. Patients are not significantly immu-
dence of invasive aspergillosis in medical intensive-care units suggests nocompromised and usually have bronchiectasis or cystic fibrosis.
Harrisons_20e_Part5_p0859-p1648.indd 1533 6/1/18 12:10 PM
1534 TABLE 212-2 Major Manifestations of Aspergillosis
TYPE OF DISEASE
INVASIVE (ACUTE AND
ORGAN SUBACUTE) CHRONIC SAPROPHYTIC ALLERGIC
Lung Angioinvasive (in neutropenia), non- Chronic cavitary, Aspergillus Aspergilloma (single), airway Allergic bronchopulmonary, severe asthma
angioinvasive, granulomatous nodule, chronic fibrosing colonization with fungal sensitization, extrinsic allergic
alveolitis
Sinus Acute invasive Chronic invasive, chronic Maxillary fungal ball Allergic fungal sinusitis, eosinophilic fungal
granulomatous rhinosinusitis
Brain Abscess, hemorrhagic infarction, Granulomatous, meningitis None None
meningitis
Skin Acute disseminated, locally External otitis, onychomycosis None None
invasive (trauma, burns, IV access)
Heart Endocarditis (native or prosthetic), None None None
pericarditis
Eye Keratitis, endophthalmitis None None None described
Occasional patients present with respiratory failure because of airway may be more prominent than pulmonary symptoms. Cavities may
obstruction with mucus. Concurrent bacterial bronchitis is common. have a fluid level or a well-formed fungal ball, but pericavitary infil-
The diagnosis rests on recurrent detection of Aspergillus in the airway trates and multiple cavities—with or without pleural thickening—are
by microscopy, culture, or polymerase chain reaction (PCR). Aspergillus typical. An irregular internal cavity surface and thickened cavity walls
IgG is usually detectable. are indicative of disease activity. CPA is usually caused by A. fumigatus,
but A. niger has been implicated, particularly in diabetic patients,
Disseminated Aspergillosis In the most severely immunocom- and is linked to oxalosis with renal dysfunction. IgG antibodies to
promised patients, Aspergillus disseminates from the lungs to multiple
Aspergillus are detectable in ~95% of patients with CPA. Some patients
organs—most often to the brain but also to the skin, thyroid, bone, kid-
have concurrent infections—even without a fungal ball—with atypical
ney, liver, gastrointestinal tract, eye (endophthalmitis), and heart valve.
mycobacteria and/or other bacterial pathogens. The most significant
Aside from cutaneous lesions, the most common features are gradual
complication is life-threatening hemoptysis, which may be the present-
clinical deterioration over 1–3 days, with low-grade fever and features
PART 5
ing manifestation.
of mild sepsis, and nonspecific abnormalities in laboratory tests. In
A recently recognized form of chronic pulmonary aspergillosis is the
most cases, at least one localization becomes apparent before death.
Aspergillus nodule, which may resemble early lung carcinoma and may
Blood cultures are almost always negative.
cavitate. Nodules may be single or multiple and 5–50 mm in diameter.
Cerebral Aspergillosis Hematogenous dissemination to the Larger mass lesions are rarely seen. Nodules are usually avid on posi-
Infectious Diseases
brain is a devastating complication of invasive aspergillosis. Single or tron emission tomography. IgG antibodies to Aspergillus are detectable
multiple lesions may develop. In acute disease, hemorrhagic infarction in ~65% of patients with an Aspergillus nodule. If untreated, chronic
is most typical, and cerebral abscess is common. Rarer manifestations cavitary pulmonary aspergillosis typically progresses (sometimes rela-
include meningitis, mycotic aneurysm, and cerebral granuloma (mim- tively rapidly) to unilateral or upper-lobe fibrosis. This end-stage entity
icking a brain tumor). Local spread from cranial sinuses also occurs. is termed chronic fibrosing pulmonary aspergillosis.
Postoperative infection develops rarely and is exacerbated by glucocor- Aspergilloma Aspergilloma (fungal ball) is a late manifestation of
ticoids, which are often given after neurosurgery. The presentation can CPA, but some patients are asymptomatic. The inside of a pulmonary
be either acute or subacute, with mood changes, focal signs, seizures, cavity allows growth that peels off, forming the layers of the fungal ball.
and decline in mental status. MRI is the most useful immediate investi-
gation; unenhanced CT of the brain is usually nonspecific, and contrast
is often contraindicated because of poor renal function.
Endocarditis Most cases of Aspergillus endocarditis are pros-
thetic-valve infections resulting from contamination during surgery.
Native-valve disease is reported, especially as a feature of dissemi-
nated infection and in persons using illicit IV drugs. Culture-negative
endocarditis with large vegetations is the most common presentation;
embolectomy occasionally reveals the diagnosis. C
C
Cutaneous Aspergillosis Dissemination of Aspergillus occasion-
ally results in cutaneous features, usually an erythematous or purplish C
C
nontender area that progresses to a necrotic eschar. Direct invasion of
the skin occurs in neutropenic patients at the site of IV catheter inser- C
tion and in burn patients. Surgical, burn, and trauma wounds may
become infected with Aspergillus (especially A. flavus).
Chronic Pulmonary Aspergillosis The hallmark of chronic
cavitary pulmonary aspergillosis (CPA; also called semi-invasive asper-
gillosis, chronic necrotizing aspergillosis, or complex aspergilloma) FIGURE 212-1 CT scan image of the chest in a patient with long-standing
(Fig. 212-1) is one or more pulmonary cavities expanding over a period bilateral chronic cavitary pulmonary aspergillosis. This patient had a history of
of months or years in association with pulmonary symptoms and sys- several bilateral pneumothoraces and had required bilateral pleurodesis in 1990.
temic manifestations such as fatigue and weight loss. Often mistaken CT then demonstrated multiple bullae, and sputum cultures grew A. fumigatus.
initially for tuberculosis, more than 90% of CPA cases occur in patients The patient had initially weakly and later strongly positive serum IgG Aspergillus
antibody tests. This scan (2003) shows a mixture of thick- and thin-walled
with prior pulmonary disease (e.g., tuberculosis, atypical mycobacte- cavities in both lungs (each marked with C), with a probable fungal ball (black
rial infection, sarcoidosis, rheumatoid lung disease, pneumothorax, arrow) protruding into the large cavity on the patient’s right side (R). There is also
bullae) or lung surgery. The onset is insidious, and systemic features considerable pleural thickening bilaterally.
Harrisons_20e_Part5_p0859-p1648.indd 1534 6/1/18 12:10 PM
Signs and symptoms associated with single (simple) aspergillomas of glucocorticoids, usually leads to resolution. Persistent or recurrent 1535
are minor, including cough (sometimes productive), hemoptysis, signs and symptoms may require more extensive surgery (ethmoidec-
wheezing, and mild fatigue. More significant signs and symptoms are tomy) and possibly antifungal therapy. Recurrence is common, often
associated with chronic cavitary pulmonary aspergillosis and should after another bacterial or viral infection.
be treated as such. About 10% of fungal balls resolve spontaneously (by
being coughed up), but the cavity may still be infected.
Superficial Aspergillosis Aspergillus can cause keratitis and
otitis externa. The former may be difficult to diagnose early enough to
Chronic Aspergillus Sinusitis Three entities are subsumed save the patient’s sight. Treatment requires local surgical debridement
under this broad designation: fungal ball of the sinus, chronic invasive as well as intensive topical antifungal therapy with natamycin (5%).
sinusitis, and chronic granulomatous sinusitis. Fungal ball of the sinus Otitis externa usually resolves with debridement and local application
is limited to the maxillary sinus (except in rare cases involving the of antifungal agents.
sphenoid sinus) and consists of a chronic saprophytic entity in which
the sinus cavity is filled with a fungal ball. Maxillary disease is asso- ■ DIAGNOSIS
ciated with prior upper-jaw root canal work and chronic (bacterial) Several techniques are required to establish the diagnosis of any form
sinusitis. About 90% of CT scans show focal hyperattenuation related of aspergillosis with confidence (Table 212-1).
to concretions; on MRI scans, the T2-weighted signal is decreased, Acute Invasive Aspergillosis Patients with acute invasive
whereas it is increased in bacterial sinusitis. Removal of the fungal aspergillosis have a relatively heavy load of fungus in the affected
ball is curative. No tissue invasion is demonstrable histologically or organ; thus culture, molecular diagnosis, antigen detection, and
radiologically. histopathology usually confirm the diagnosis. However, the pace of
In contrast, chronic invasive sinusitis is a slowly destructive pro- progression leaves only a narrow window for making the diagnosis
cess that most commonly affects the ethmoid and sphenoid sinuses. without losing the patient, and some invasive procedures are not
Patients are usually but not always immunocompromised to some possible because of coagulopathy, respiratory compromise, and other
degree (e.g., as a result of diabetes or HIV infection). Imaging of the factors. Currently, ~40% of cases of invasive aspergillosis are missed
cranial sinuses shows opacification of one or more sinuses, local bone clinically and are diagnosed only at autopsy. Histologic examination of
destruction, and invasion of local structures. The differential diagnosis affected tissue reveals either infarction, with invasion of blood vessels
is wide, including other infections. Apart from a history of chronic by many fungal hyphae, or acute necrosis, with limited inflammation
nasal discharge and blockage, loss of the sense of smell, and persistent and fewer hyphae. Aspergillus hyphae are hyaline, narrow, and septate,
headache, the usual presenting features are related to local involve- with branching at 45°; no yeast forms are present in infected tissue.
ment of critical structures. The orbital apex syndrome (blindness and
CHAPTER 212 Aspergillosis
Hyphae can be seen in cytology or microscopy preparations, which
proptosis) is characteristic. Facial swelling, cavernous sinus thrombo- therefore provide a rapid means of presumptive diagnosis.
sis, carotid artery occlusion, pituitary fossa, and brain and skull-base A positive culture supports the diagnosis, given that multiple other
invasion are complications. (rarer) fungi can mimic Aspergillus species histologically, but only
Chronic granulomatous sinusitis due to Aspergillus is most com- 10–30% of patients with invasive aspergillosis have a positive culture.
monly seen in the Middle East and India and is often caused by A. flavus. Bacterial agar is less sensitive than fungal media for culture; thus, if
It typically presents late, with facial swelling and unilateral proptosis. physicians do not request fungal culture, the diagnosis may be missed.
The prominent granulomatous reaction histologically distinguishes A positive culture may represent noninvasive forms of aspergillosis
this disease from chronic invasive sinusitis, in which tissue necrosis or airway colonization. Both antigen detection and real-time PCR are
with a low-grade mixed-cell infiltrate is typical. IgG antibodies to faster and much more sensitive than culture of respiratory samples
A. flavus are usually detectable. and blood.
Allergic Bronchopulmonary Aspergillosis In almost all The Aspergillus antigen test relies on detection of galactomannan
cases, ABPA represents a hypersensitivity reaction to A. fumigatus; rare release from Aspergillus organisms during growth. Positive serum
cases are due to other aspergilli and other fungi. ABPA occurs in ~2.5% antigen results usually precede clinical or radiologic features by sev-
of patients with asthma who are referred to secondary care and in up to eral days. The sensitivity of antigen detection is reduced by antifungal
15% of teenagers with cystic fibrosis. Episodes of bronchial obstruction prophylaxis and empirical therapy.
with mucous plugs leading to coughing fits, “pneumonia,” consolida- Definitive confirmation of a diagnosis of invasive aspergillosis
tion, and breathlessness are typical. Many patients report coughing up requires (1) a positive culture of a sample taken directly from an
thick sputum casts. Eosinophilia commonly develops before systemic ordinarily sterile site (e.g., a brain abscess) or (2) positive results of
glucocorticoids are given. The cardinal diagnostic test is detection of both histologic testing and culture of a sample taken from an affected
Aspergillus-specific IgE (or a positive skin-prick test in response to organ (e.g., sinuses or skin). Most diagnoses of invasive aspergillosis
A. fumigatus extract) together with an elevated serum level of total IgE are inferred from fewer data, including the presence of the halo sign on
(usually >1000 IU/mL). The presence of hyperattenuated mucus in a high-resolution thoracic CT scan, in which a localized ground-glass
airways is highly specific. Bronchiectasis is characteristic, and some appearance representing hemorrhagic infarction surrounds a nodule
patients develop chronic cavitary pulmonary aspergillosis. or consolidation. Halo signs are present for ~7 days early in the course
of infection in neutropenic patients and are a good prognostic feature,
Severe Asthma with Fungal Sensitization (SAFS) Many reflecting an early diagnosis. Other characteristic radiologic features of
adults with severe asthma do not fulfill the criteria for ABPA and yet
invasive pulmonary aspergillosis include nodules and pleural-based
are allergic to fungi. Although A. fumigatus is a common allergen,
infarction or cavitation, but nonspecific consolidation is common.
numerous other fungi (e.g., Cladosporium and Alternaria species) are
implicated by skin-prick testing and/or specific IgE testing. Serum Chronic Aspergillosis For chronic aspergillosis, Aspergillus anti-
total IgE concentrations are <1000 IU/mL, and bronchial-wall thicken- body testing combined with characteristic imaging is sufficient for the
ing is common. ABPA and SAFS are referred to as fungal asthma. diagnosis. Biopsy of Aspergillus nodules reveals hyphae surrounded by
cells of chronic inflammation and sometimes granulomas. Antibody
Allergic Fungal Rhinosinusitis Like the lungs, the sinuses titers fall slowly with successful therapy. Cultures are infrequently
manifest allergic responses to Aspergillus and other fungi. The affected
positive but are important in checking for azole resistance. Real-time
patients present with chronic (i.e., perennial) sinusitis that is relatively
PCR of sputum is often strongly positive. Some patients with chronic
unresponsive to antibiotics. Many of these patients have nasal polyps,
pulmonary aspergillosis also have elevated titers of total serum IgE and
and all have congested nasal mucosae and sinuses full of mucoid
Aspergillus-specific IgE.
material. The histologic hallmarks of allergic fungal sinusitis are local
eosinophilia and Charcot-Leyden crystals. Removal of abnormal ABPA, SAFS, and Allergic Aspergillus Sinusitis ABPA and
mucus and polyps, with local and occasionally systemic administration SAFS are diagnosed serologically with elevated specific and total
Harrisons_20e_Part5_p0859-p1648.indd 1535 6/1/18 12:10 PM
1536 serum IgE levels or with skin-prick tests. Allergic Aspergillus sinusitis forms of chronic and allergic aspergillosis requires case-by-case
is usually diagnosed histologically, although measurement of IgE anti- evaluation. Glucocorticoids should be used in chronic cavitary
bodies in blood also may be useful. pulmonary aspergillosis only if covered by adequate antifungal
therapy. Antifungal response in Aspergillus bronchitis is gratifying,
but relapse after 4 months of therapy is common.
TREATMENT Resistance in A. fumigatus to one or more azoles, although
Aspergillosis uncommon, is increasingly found globally. Resistance may
be derived from azole fungicide use for crops. In addition,
Antifungal drugs active against Aspergillus include voriconazole, resistance arising from multiple mechanisms may develop during
itraconazole, posaconazole, isavuconazole, caspofungin, micafun- long-term treatment, and a positive culture during antifungal ther-
gin, and amphotericin B (AmB). Possible interactions with other apy is an indication for susceptibility testing.
drugs must be considered before azoles are prescribed. In addition, Surgical treatment is important in several forms of aspergillo-
plasma azole concentrations vary substantially from one patient sis, including fungal ball of the sinus and single aspergillomas, in
to another, and many authorities recommend monitoring levels to which surgery is curative; invasive aspergillosis involving bone,
ensure that drug concentrations are adequate but not excessive, heart valve, sinuses, and proximal areas of the lung; brain abscess;
especially with itraconazole and voriconazole. Initial IV administra- keratitis; and endophthalmitis. In allergic fungal sinusitis, removal
tion is preferred for acute invasive aspergillosis and oral adminis- of abnormal mucus and polyps, with local and occasionally systemic
tration for all other diseases that require antifungal therapy. Current glucocorticoid treatment, usually leads to resolution. Persistent or
recommendations are shown in Table 212-3. recurrent signs and symptoms may require more extensive sur-
Voriconazole and isavuconazole are the preferred agents for gery (ethmoidectomy) and possibly antifungal therapy. Surgery is
invasive aspergillosis; caspofungin, posaconazole, micafungin, and problematic in chronic cavitary pulmonary aspergillosis, usually
lipid-associated AmB are second-line agents. AmB is not active resulting in serious complications. Bronchial artery embolization is
against A. terreus or A. nidulans; multi-azole resistance in A. fumi- preferred for problematic hemoptysis.
gatus is present in <5% of isolates but is increasing; and A. niger is
resistant to itraconazole and isavuconazole. An infectious disease ■ PROPHYLAXIS
consultation is advised for patients with invasive disease, given In situations in which moderate or high risk is predicted (e.g., after induc-
the complexity of management. Immune reconstitution can com- tion therapy for acute myeloid leukemia), the need for antifungal prophy-
plicate recovery. The duration of therapy for invasive aspergillosis laxis for superficial and systemic candidiasis and for invasive aspergillosis
varies from ~3 months to several years, depending on the patient’s is generally accepted. Fluconazole is commonly used in these situations
PART 5
immune status and response to therapy. Relapse occurs if the but has no activity against Aspergillus species. Itraconazole capsules are
response is suboptimal and immune reconstitution is not complete. ineffective, and itraconazole solution offers only modest efficacy. Posa-
Itraconazole is currently the preferred oral agent for chronic and conazole tablets are more effective in reducing infection rates and the
allergic forms of aspergillosis. Voriconazole or posaconazole can be need for empirical antifungal therapy. Some data support the use of IV
substituted when failure, emergence of resistance, or adverse events micafungin. No prophylactic regimen is completely successful.
Infectious Diseases
occur. An itraconazole dose of 200 mg twice daily is recommended,
with monitoring of drug concentrations in the blood. Acute exacer- ■ OUTCOME
bations of ABPA respond well to a short course of glucocorticoids. Invasive aspergillosis is curable if immune reconstitution occurs,
Because chronic cavitary pulmonary aspergillosis responds slowly, whereas allergic and chronic forms are not. The mortality rate for
therapy for >6 months is necessary, and disease control may require invasive aspergillosis is 30–70% if the infection is treated but is 100%
years of treatment, whereas the duration of treatment for other if the diagnosis is missed. Infection with a voriconazole-resistant strain
TABLE 212-3 Treatment of Aspergillosisa
INDICATION PRIMARY TREATMENT PRECAUTIONS SECONDARY TREATMENT COMMENTS
Invasive diseaseb Voriconazole, Drug interactions (especially AmB, caspofungin, As primary therapy, voriconazole and
isavuconazole with rifampin and posaconazole, micafungin isavuconazole have a 20% higher response
carbamazepine)c rate than AmB. Therapeutic drug monitoring is
recommended for voriconazole.
Prophylaxis Posaconazole tablet, Diarrhea and vomiting with Micafungin, aerosolized AmB Some centers monitor plasma levels of
itraconazole solution itraconazole, vincristine itraconazole and posaconazole.
interaction
Single aspergilloma Surgery Multicavity disease: poor Itraconazole, voriconazole, Single large cavities with an aspergilloma are
outcome of surgery, medical intracavity AmB best resected.
therapy preferable
Chronic pulmonary Itraconazole, Poor absorption of itraconazole Posaconazole, IV AmB, IV Resistance may emerge during treatment,
diseaseb voriconazole capsules with proton pump micafungin especially if plasma drug levels are
inhibitors or H2 blockers subtherapeutic.
ABPA/SAFS (“fungal Itraconazole Some glucocorticoid Voriconazole, posaconazole Long-term therapy is helpful in most cases. No
asthma”) interactions, including with evidence indicates whether therapy modifies
inhaled formulations progression to bronchiectasis/fibrosis.
a
For information on duration of therapy and drug resistance in certain Aspergillus species, see text. bAn infectious disease consultation is appropriate for these
patients. cOnline drug-interaction resource: www.aspergillus.org.uk/content/antifungal-drug-interactions.
Note: After loading doses, the oral dose is usually 200 mg bid for voriconazole and itraconazole, 300 mg qd for posaconazole tablets, and 200 mg qd for
isavuconazole. The IV dose of voriconazole for adults is 6 mg/kg twice at 12-h intervals (loading doses) followed by 4 mg/kg q12h; a larger dose is required for
children and teenagers; a lower dose may be safer for persons >70 years of age. Plasma monitoring is helpful in optimizing the dosage. The IV dose of isavuconazole
is 200 mg tid for 2 days (loading dose) followed by 200 mg qd. Caspofungin is given as a single loading dose of 70 mg and then at 50 mg/d; some authorities use
70 mg/d for patients weighing >80 kg, and lower doses are required with hepatic dysfunction. Micafungin is given as 50 mg/d for prophylaxis and as at least 150
mg/d for treatment; this drug has not yet been approved by the U.S. Food and Drug Administration (FDA) for this indication. AmB deoxycholate is given at a daily dose
of 1 mg/kg if tolerated. Several strategies are available for minimizing renal dysfunction. Lipid-associated AmB is given at 3 mg/kg (AmBisome) or 5 mg/kg (Abelcet).
Different regimens are available for aerosolized AmB, but none is FDA approved. Other considerations that may alter dose selection or route include age; concomitant
medications; renal, hepatic, or intestinal dysfunction; and drug tolerability.
Abbreviations: AmB, amphotericin B; ABPA, allergic bronchopulmonary aspergillosis; SAFS, severe asthma with fungal sensitization.
Harrisons_20e_Part5_p0859-p1648.indd 1536 6/1/18 12:10 PM
cases, decreased spasticity in three, and restoration of the ability to 1393
walk after confinement to a wheelchair in two. Antibody to IL-15
receptor β chain has been tested with some promising clinical effects
in small numbers of patients. Physical therapy and rehabilitation are
197 Human Immunodeficiency
Virus Disease: AIDS and
important components of management.
Related Disorders
Anthony S. Fauci, Gregory K. Folkers,
■ FEATURES OF HTLV-2 INFECTION
H. Clifford Lane
Epidemiology HTLV-2 is endemic in certain Native
American tribes and in Africa. It is generally considered to be
a New World virus that was brought from Asia to the Americas AIDS was first recognized in the United States in the summer of 1981,
10,000–40,000 years ago during the migration of infected populations when the U.S. Centers for Disease Control and Prevention (CDC)
across the Bering land bridge. The mode of transmission of HTLV-2 is reported the unexplained occurrence of Pneumocystis jirovecii (formerly
probably the same as that of HTLV-1 (see above). HTLV-2 may be less P. carinii) pneumonia in five previously healthy homosexual men in
readily transmitted sexually than HTLV-1. Los Angeles and of Kaposi’s sarcoma (KS) with or without P. jirovecii
Studies of large cohorts of injection drug users with serologic assays pneumonia and other opportunistic infections in 26 previously healthy
that reliably distinguish HTLV-1 from HTLV-2 indicated that the vast homosexual men in New York, San Francisco, and Los Angeles. The
majority of HTLV-positive cohort members were infected with HTLV-2. disease was soon recognized in male and female injection drug users;
The seroprevalence of HTLV in a cohort of 7841 injection drug users in hemophiliacs and blood transfusion recipients; among female sexual
from drug treatment centers in Baltimore, Chicago, Los Angeles, partners of men with AIDS; and among infants born to mothers with
New Jersey (Asbury Park and Trenton), New York City (Brooklyn and AIDS. In 1983, human immunodeficiency virus (HIV) was isolated
Harlem), Philadelphia, and San Antonio was 20.9%, with >97% of cases from a patient with lymphadenopathy, and by 1984 it was demon-
due to HTLV-2. The seroprevalence of HTLV-2 was higher in the South- strated clearly to be the causative agent of AIDS. In 1985, a sensitive
west and the Midwest than in the Northeast. In contrast, the seroprev- enzyme-linked immunosorbent assay (ELISA) was developed; this led
alence of HIV-1 was higher in the Northeast than in the Southwest or to an appreciation of the scope and evolution of the HIV epidemic at
the Midwest. Approximately 3% of the cohort members were infected first in the United States and other developed nations and ultimately
with both HTLV-2 and HIV-1. The seroprevalence of HTLV-2 increased among developing nations throughout the world (see “HIV Infection
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
linearly with age. Women were significantly more likely than men to and AIDS Worldwide,” below). The staggering worldwide evolution
be infected with HTLV-2; the virus is thought to be more efficiently of the HIV pandemic has been matched by an explosion of information
transmitted from male to female than from female to male. in the areas of HIV virology, pathogenesis (both immunologic and
virologic), treatment of HIV disease, treatment and prophylaxis of the
Associated Diseases Although HTLV-2 was isolated from a opportunistic diseases associated with HIV infection, and prevention
patient with a T-cell variant of hairy-cell leukemia, this virus has of HIV infection. The information flow related to HIV disease is enor-
not been consistently associated with a particular disease and in fact mous and continues to expand, and it has become almost impossible
has been thought of as “a virus searching for a disease.” However, for the health care generalist to stay abreast of the literature. The pur-
evidence is accumulating that HTLV-2 may play a role in certain neu- pose of this chapter is to present the most current information available
rologic, hematologic, and dermatologic diseases. These data require on the scope of the pandemic; on its pathogenesis, treatment, and pre-
confirmation, particularly in light of the previous confusion regarding vention; and on prospects for vaccine development. Above all, the aim
the relative prevalences of HTLV-1 and HTLV-2 among injection drug is to provide a solid scientific basis and practical clinical guidelines for
users. a state-of-the-art approach to the HIV-infected patient.
Prevention Avoidance of needle sharing, adherence to safe-sex
■ DEFINITION
practices, screening of blood (by assays for HTLV-1, which also detect
The current CDC classification system for HIV infection and AIDS
HTLV-2), and avoidance of breast-feeding by infected women are
categorizes patients based on clinical conditions associated with HIV
important principles in the prevention of spread of HTLV-2.
infection together with the level of the CD4+ T lymphocyte count.
A confirmed HIV case can be classified in one of five HIV infection
HUMAN IMMUNODEFICIENCY VIRUS stages (0, 1, 2, 3, or unknown). If there was a negative HIV test within
HIV-1 and HIV-2 are members of the lentivirus subfamily of Retroviri- 6 months of the first HIV infection diagnosis, the stage is 0, and remains
dae and are the only lentiviruses known to infect humans. The lenti- 0 until 6 months after diagnosis. Advanced HIV disease (AIDS) is clas-
viruses are slower-acting than viruses that cause acute infection (e.g., sified as stage 3 if one or more specific opportunistic illness has been
influenza virus) but not than other retroviruses. The features of acute diagnosed (Table 197-1). Otherwise, the stage is determined by CD4+
primary infection with HIV resemble those of more classic acute infec- T lymphocyte test results and immunologic criteria (Table 197-2). If
tions. The characteristic chronicity of HIV disease is consistent with the none of these criteria apply (e.g., because of missing information on
designation lentivirus. For a detailed discussion of HIV, see Chap. 197. CD4+ T lymphocyte test results), the stage is U (unknown).
The definition and staging criteria of AIDS are complex and com-
prehensive and were established for surveillance purposes rather than
■ FURTHER READING for the practical care of patients. Thus, the clinician should not focus
Ishida T et al: Multicenter phase II study of lenalidomide in relapsed on whether the patient fulfills the strict definition of AIDS, but should
or recurrent adult T-cell leukemia-lymphoma: ATLL-002. J Clin Oncol view HIV disease as a spectrum ranging from primary infection, with
34:4086, 2016. or without the acute syndrome, to the relatively asymptomatic
Katsuya H et al: Treatment and survival among 1594 patients with stage, to advanced stages associated with opportunistic diseases
ATL. Blood 126:2570, 2015. (see “Pathophysiology and Pathogenesis,” below).
Ma G et al: Multifaceted functions and roles of HBA in HTLV-1 patho-
genesis. Retrovirology 13:16, 2016.
Moir S et al: Pathogenic mechanisms of HIV disease. Annu Rev Pathol ETIOLOGIC AGENT
6:223, 2011. HIV is the etiologic agent of AIDS; it belongs to the family of human
Panfil AR et al: Human T-cell leukemia virus–associated malignancy. retroviruses (Retroviridae) and the subfamily of lentiviruses
Curr Opin Virol 20:40, 2016. (Chap. 196). Nononcogenic lentiviruses cause disease in other animal
Harrisons_20e_Part5_p0859-p1648.indd 1393 6/1/18 12:08 PM
1394 the HIV-2 groups A through H each are likely derived from a separate
TABLE 197-1 CDC Stage 3 (AIDS)-Defining Opportunistic Illnesses in
HIV Infection transfer to humans from a nonhuman primate reservoir. HIV-1 viruses
Bacterial infections, multiple or recurrenta likely came from chimpanzees and/or gorillas, and HIV-2 from
Candidiasis of bronchi, trachea, or lungs sooty mangabeys. The AIDS pandemic is primarily caused by the
HIV-1 M group viruses. Although HIV-1 group O and HIV-2 viruses
Candidiasis of esophagus
have been found in numerous countries, including those in the
Cervical cancer, invasiveb
developed world, they have caused much more localized epidemics.
Coccidioidomycosis, disseminated or extrapulmonary The taxonomic relationship between primate lentiviruses is shown
Cryptococcosis, extrapulmonary in Fig. 197-1.
Cryptosporidiosis, chronic intestinal (>1 month’s duration)
Cytomegalovirus disease (other than liver, spleen, or nodes), onset at age ■ MORPHOLOGY OF HIV
>1 month Electron microscopy shows that the HIV virion is an icosahedral
Cytomegalovirus retinitis (with loss of vision) structure (Fig. 197-2) containing numerous external spikes formed by
Encephalopathy attributed to HIV the two major envelope proteins, the external gp120 and the trans-
Herpes simplex: chronic ulcers (>1 month’s duration) or bronchitis, membrane gp41. The HIV envelope exists as a trimeric heterodimer.
pneumonitis, or esophagitis (onset at age >1 month) The virion buds from the surface of the infected cell (Fig. 197-2A) and
Histoplasmosis, disseminated or extrapulmonary incorporates a variety of host cellular proteins into its lipid bilayer. The
Isosporiasis, chronic intestinal (>1 month’s duration) structure of HIV-1 is schematically diagrammed in Fig. 197-2B.
Kaposi’s sarcoma
Lymphoma, Burkitt’s (or equivalent term) ■ REPLICATION CYCLE OF HIV
Lymphoma, immunoblastic (or equivalent term) HIV is an RNA virus whose hallmark is the reverse transcription of
Lymphoma, primary, of brain its genomic RNA to DNA by the enzyme reverse transcriptase. The
Mycobacterium avium complex or Mycobacterium kansasii, disseminated or replication cycle of HIV begins with the high-affinity binding via surface-
extrapulmonary exposed residues within the gp120 protein to its receptor on the host
Mycobacterium tuberculosis of any site, pulmonary,b disseminated, or cell surface, the CD4 molecule (Fig. 197-3). The CD4 molecule is a
extrapulmonary 55-kDa protein found predominantly on a subset of T lymphocytes that
Mycobacterium, other species or unidentified species, disseminated or are responsible for helper function in the immune system (Chap. 342).
extrapulmonary Once it binds to CD4, the gp120 protein undergoes a conformational
Pneumocystis jirovecii (previously known as Pneumocystis carinii) pneumonia change that facilitates binding to one of two major co-receptors.
PART 5
Pneumonia, recurrentb The two major co-receptors for HIV-1 are CCR5 and CXCR4. Both
Progressive multifocal leukoencephalopathy receptors belong to the family of seven-transmembrane-domain G
Salmonella septicemia, recurrent protein–coupled cellular receptors, and the use of one or the other
Toxoplasmosis of brain, onset at age >1 month or both receptors by the virus for entry into the cell is an important
Infectious Diseases
determinant of the cellular tropism of the virus. Cell-to-cell spread
Wasting syndrome attributed to HIV
is also facilitated by accessory molecules such as the C-type lectin
a
Only among children age <6 years. bOnly among adults, adolescents, and receptor DC-SIGN expressed on certain dendritic cells (DCs) that
children age ≥6 years.
bind to the HIV gp120 envelope protein, allowing virus captured on
Source: MMWR 63(RR-03), April 11, 2014.
DCs to spread to CD4+ T cells. Following binding of the envelope
protein to the CD4 molecule associated with the above-mentioned
species, including sheep, horses, goats, cattle, cats, and monkeys. The conformational change in the viral envelope gp120, fusion with the
four retroviruses known to cause human disease belong to two distinct host cell membrane occurs via the newly exposed gp41 molecule
groups: the human T lymphotropic viruses (HTLV)-1 and HTLV-2, penetrating the plasma membrane of the target cell and then coiling
which are transforming retroviruses; and the human immunodefi- upon itself to bring the virion and target cell together (Fig. 197-4).
ciency viruses, HIV-1 and HIV-2, which cause cytopathic effects either Following fusion, uncoating of the capsid protein shell is initiated—a
directly or indirectly (Chap. 196). The most common cause of HIV step that facilitates reverse transcription and leads to formation of
disease throughout the world, and certainly in the United States, is the preintegration complex, composed of viral RNA, enzymes, and
HIV-1, which comprises several subtypes with different geographic accessory proteins and surrounded by capsid and matrix proteins
distributions (see “Molecular Heterogeneity of HIV-1,” below). HIV-2 (Fig. 197-3). As the preintegration complex traverses the cytoplasm
was first identified in 1986 in West African patients and was originally to reach the nucleus, the viral reverse transcriptase enzyme catalyzes
confined to West Africa. However, cases traced to West Africa or to the reverse transcription of the genomic RNA into DNA, resulting
sexual contacts with West Africans have been identified throughout in the formation of double-stranded proviral HIV DNA. At several
the world. The currently defined groups of HIV-1 (M, N, O, P) and steps of the replication cycle, the virus is vulnerable to various cellular
factors that can block the progression of infection. The cytoplasmic
tripartite motif-containing protein 5-α (TRIM5-α) is a host restriction
TABLE 197-2 CDC HIV Infection Stages 1–3 Based on Age-Specific
CD4+ T Lymphocyte Count or CD4+ T Lymphocyte Percentage of factor that interacts with retroviral capsids, causing their premature
Total Lymphocytesa disassembly and induction of innate immune responses. While early
AGE ON DATE OF CD4 T+ LYMPHOCYTE TEST studies with laboratory strains found the HIV-1 capsid bound weakly
to the human form of TRIM5-α, capsids of primary isolates appear
<1 YEAR 1–5 YEARS 6 YEARS THROUGH ADULT
to be more susceptible to TRIM5-α-mediated disassembly. The apo-
STAGEa CELLS/µL % CELLS/µL % CELLS/µL % lipoprotein B mRNA editing enzyme (catalytic polypeptide-like 3
1 ≥1500 ≥34 ≥1000 ≥30 ≥500 ≥26 [APOBEC3]) family of cellular proteins also inhibits progression of
2 750–1499 26–33 500–999 22–29 200–499 14–25 virus infection after virus has entered the cell and prior to entering the
3 <750 <26 <500 <22 <200 <14 nucleus. APOBEC3 proteins, which are incorporated into virions and
a
The stage is based primarily on the CD4+ T lymphocyte count; the CD4+
released into the cytoplasm of a newly infected cell, bind to the single
T lymphocyte count takes precedence over the CD4+ T lymphocyte percentage, minus-strand DNA intermediate and deaminate viral cytidine, causing
and the percentage is considered only if the count is missing. hypermutation of retroviral genomes. HIV has evolved a powerful
Source: MMWR 63(RR-03), April 11, 2014. strategy to protect itself from APOBEC. The viral protein Vif targets
Harrisons_20e_Part5_p0859-p1648.indd 1394 6/1/18 12:08 PM
SIV-SYK 1395
HIV-2 and SIV-SMM/MAC SIV-TAL
SIV-MUS
B SIV-GSN
A
SIV-MON
SIV-ASC
SIV-DEN SIV-COL
SIV-DEB
SIV-Ver SIV-MND1
SIV-GRI SIV-SUN
SIV-TAN SIV_LST
SIV-WRC
SIV-OLC
SIV-DRL
SIV-MND2
SIV-RCM
SIV-SAB
SIV-CPZ
Pan troglodytes
schweinfurthii
HIV-1 P and O
groups and
HIV-1 M and N SIV_Gorilla
groups and SIV-CPZ
Pan troglodytes
troglodytes
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
0.25
FIGURE 197-1 A phylogenetic tree based on the nearly complete genomes (gag through nef genes) of primate immunodeficiency viruses. The scale (0.25) indicates
a 25% phylogenetically corrected genetic distance at the nucleotide level. Clades in color represent viruses (HIV-1, HIV-2) identified in humans after relatively recent
transfers from chimpanzee, gorilla, and sooty mangabey reservoirs. (Prepared by Brian Foley, PhD, of the HIV Sequence Database, Theoretical Biology and Biophysics
Group, Los Alamos National Laboratory; additional information at www.hiv.lanl.gov/content/sequence/HelpDocs/subtypes.html.)
APOBEC3 for proteasomal degradation. SAMHD1 is another post- is the point at which the core acquires its external envelope and where
entry host factor that prevents reverse transcription by depleting pools the host restriction factor tetherin can inhibit the release of budding
of deoxynucleotides (dNTPs). The type I interferon (IFN)-induced particles. Tetherin is an IFN-induced type II transmembrane protein
myxovirus resistance protein 2 (MX2) is another restriction factor asso- that interferes with virion detachment, although the HIV accessory
ciated with innate immunity that inhibits HIV-1 nuclear entry. protein Vpu counteracts this effect through direct interactions with
With activation of the cell, the viral DNA accesses the nuclear tetherin. During or soon after budding, the virally encoded protease
pore and is transferred from the cytoplasm to the nucleus, where it catalyzes the cleavage of the gag-pol precursor to yield the mature
is integrated into the host cell chromosomes through the action of virion. Progression through the virus replication cycle is profoundly
another virally encoded enzyme, integrase (Fig. 197-3). HIV proviral influenced by a variety of viral regulatory gene products. Likewise,
DNA integrates into the host genomic DNA preferentially in regions of each point in the replication cycle of HIV is a real or potential target
active transcription and regional hotspots. This provirus may remain for therapeutic intervention. Thus far, the reverse transcriptase, pro-
transcriptionally inactive (latent) or it may manifest varying levels of tease, and integrase enzymes as well as the process of virus–target cell
gene expression, up to active transcription and production of virus binding and fusion have proved to be susceptible to pharmacologic
depending on the metabolic state of the infected cell. disruption.
Cellular activation plays an important role in the replication cycle
of HIV and is critical to the pathogenesis of HIV disease (see “Patho- ■ HIV GENOME
genesis and Pathophysiology,” below). Following initial binding, Figure 197-5 illustrates schematically the arrangement of the HIV
fusion, and internalization of the nucleic acid contents of virions genome. Like other retroviruses, HIV-1 has genes that encode the struc-
into the target cell, incompletely reverse-transcribed DNA intermedi- tural proteins of the virus: gag encodes the proteins that form the core
ates are labile in quiescent cells and do not integrate efficiently into of the virion (including p24 antigen); pol encodes the enzymes respon-
the host cell genome unless cellular activation occurs shortly after sible for protease processing of viral proteins, reverse transcription,
infection. Furthermore, some degree of activation of the host cell is and integration; and env encodes the envelope glycoproteins. However,
required for the initiation of transcription of the integrated proviral HIV-1 is more complex than other retroviruses, particularly those of the
DNA into either genomic RNA or mRNA. This latter process may nonprimate group, in that it also contains at least six other regulatory
not necessarily be associated with the detectable expression of the genes (tat, rev, nef, vif, vpr, and vpu), which code for proteins involved in
classic cell-surface markers of activation. In this regard, activation of the modification of the host cell to enhance virus growth and the regu-
HIV expression from the latent state depends on the interaction of lation of viral gene expression. Several of these proteins are thought to
a number of cellular and viral factors. Following transcription, HIV play a role in the pathogenesis of HIV disease; their various functions
mRNA is translated into proteins that undergo modification through are listed in Fig. 197-5. Flanking these genes are the long terminal
glycosylation, myristoylation, phosphorylation, and cleavage. The repeats (LTRs), which contain regulatory elements involved in gene
viral particle is formed by the assembly of HIV proteins, enzymes, expression (Fig. 197-5). The major difference between the genomes of
and genomic RNA at the plasma membrane of the cells. Budding of HIV-1 and HIV-2 is the fact that HIV-2 lacks the vpu gene and has a vpx
the progeny virion through the lipid bilayer of the host cell membrane gene not contained in HIV-1.
Harrisons_20e_Part5_p0859-p1648.indd 1395 6/1/18 12:08 PM
1396
gp41
Matrix
Capsid Lipid
membrane
RNA
gp120 Reverse
A B transcriptase
PART 5
Infectious Diseases
C
FIGURE 197-2 A. Electron micrograph of HIV. Figure illustrates a typical virion following budding from the surface of a CD4+ T lymphocyte, together with two additional
incomplete virions in the process of budding from the cell membrane. B. Structure of HIV-1, including the gp120 envelope, gp41 transmembrane components of the
envelope, genomic RNA, enzyme reverse transcriptase, p18(17) inner membrane (matrix), and p24 core protein (capsid). (Copyright by George V. Kelvin.) (Adapted
from RC Gallo: Sci Am 256:46, 1987.) C. Scanning electron micrograph of HIV-1 virions infecting a human CD4+ T lymphocyte. The original photograph was imaged at
20,000× magnification. Cell is approximately 10 microns in diameter, and the HIV particles are approximately 120 nanometers. (Courtesy of Elizabeth R. Fischer, Rocky
Mountain Laboratories, National Institute of Allergy and Infectious Diseases; with permission.)
■ MOLECULAR HETEROGENEITY OF HIV-1 and P) transfers. Group M (major), which is responsible for most of the
Molecular analyses of HIV isolates reveal varying levels of infections in the world, has diversified into subtypes and intersubtype
sequence diversity over all regions of the viral genome. For recombinant forms, due to “sub-epidemics” within humans after one
example, the degree of difference in the coding sequences of of those transfers.
the viral envelope protein ranges from a few percent (very close, Among primate lentiviruses, HIV-1 is most closely related to viruses
among isolates from the same infected individual) to more than 50% isolated from chimpanzees and gorillas (Fig. 197-1). The chimpanzee
(extreme diversity, between isolates from the different groups of HIV-1: subspecies Pan troglodytes troglodytes has been established to be the
M, N, O, and P). The changes tend to cluster in hypervariable regions. natural reservoir of the HIV-1 M and N groups. The rare viruses of
HIV can evolve by several means, including simple base substitution, the HIV-1 O and P groups are most closely related to viruses found in
insertions and deletions, recombination, and gain and loss of glycosy- Cameroonian gorillas. The M group comprises nine subtypes, or clades,
lation sites. HIV sequence diversity arises directly from the limited designated A, B, C, D, F, G, H, J, and K, as well as more than 90 known
fidelity of the reverse transcriptase, i.e., a tendency toward copying circulating recombinant forms (CRFs) and numerous unique recom-
errors. The balance of immune pressure and functional constraints on binant forms. Intersubtype recombinants are generated by infection
proteins influences the regional level of variation within proteins. For of an individual with two subtypes that then recombine and create
example, Envelope, which is exposed on the surface of the virion and a virus with a selective advantage. These CRFs range from highly
is under immune selective pressure from both antibodies and cytolytic prevalent forms such as CRF01_AE, common in southeast Asia, and
T lymphocytes, is extremely variable, with clusters of mutations in CRF02_AG from west and central Africa, to a large number of CRFs
hypervariable domains. In contrast, reverse transcriptase, with impor- that are relatively rare, either because they are of a more recent origin
tant enzymatic functions, is relatively conserved, particularly around (newly recombined) or because they have not broken out into a major
the active site. The extraordinary variability of HIV-1 contrasts mark- population. The subtypes and CRFs create the major lineages of the M
edly with the relative stability of HTLV-1 and 2. group of HIV-1. HIV-1 M group subtype C dominates the global pan-
The four groups (M, N, O and P) of HIV-1 are the result of four sepa- demic, and although there is much speculation that it is more transmis-
rate chimpanzee-to-human (or possibly gorilla-to-human for groups O sible than other subtypes, solid data on variations in transmissibility
Harrisons_20e_Part5_p0859-p1648.indd 1396 6/1/18 12:08 PM
1397
2 HIV RNA, reverse
HIV 1 Binding and
transcriptase, integrase,
and other viral proteins
fusion to the
enter the host cell.
host cell
surface.
gp120
CD4
Preintegration
Co-receptor complex
(CCR5 or CXCR4)
Host Cell 3 Viral DNA is
formed by reverse
transcription.
Viral RNA
Reverse
4 transcriptase
Viral DNA is
transported across the
nucleus and integrates
into the host DNA.
Integrase
Viral DNA
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
Host DNA
Mature Virion New viral RNA
5 New viral RNA is
used as genomic RNA
7 and to make viral
The virus matures proteins.
after protease
cleaves long
precursor proteins 6 New viral RNA
and proteins move to
the cell surface and Protease
an immature virion
begins to form.
FIGURE 197-3 The replication cycle of HIV. See text for description. (From the National Institute of Allergy and Infectious Diseases.)
between subtypes are lacking. Human population densities, access to AIDS Worldwide,” below). Subtype B viruses are the overwhelmingly
prevention and treatment, prevalence of genital ulcers, iatrogenic trans- predominant viruses seen in the United States, Canada, certain coun-
missions, and other confounding host factors are all possible reasons tries in South America, western Europe, and Australia. It is thought
why one subtype has spread more than another. that, purely by chance, subtype B was seeded into the United States
Figure 197-6 schematically diagrams the worldwide distribution of and Europe in the late 1970s, thereby establishing an overwhelming
HIV-1 subtypes by region. Nine strains account for the vast majority of founder effect. Many countries have co-circulating viral subtypes that
HIV infections globally: HIV-1 subtypes A, B, C, D, F, G and three of are giving rise to new CRFs. Sequence analyses of HIV-1 isolates from
the CRFs, CRF01_AE, CRF02_AG, and CRF07_BC. Subtype C viruses infected individuals indicate that recombination among viruses of dif-
(of the M group) are by far the most common form worldwide, likely ferent clades likely occurs when an individual is infected with viruses
accounting for ~50% of prevalent infections worldwide. In sub-Saharan of more than one subtype, particularly in geographic areas where sub-
Africa, home to approximately two-thirds of all individuals living with types overlap, and more often in sub-epidemics driven by IV drug use
HIV/AIDS, most infections are caused by subtype C, with smaller than in those driven by sexual transmission.
proportions of infections caused by subtype A, subtype D, CRF02_AG, The extraordinary diversity of HIV, reflected by the presence of
and other subtypes and recombinants. In South Africa, the country multiple subtypes, circulating recombinant forms, and continuous viral
with the largest number of prevalent infections (7.1 million in 2016), evolution, has implications for possible differential rates of transmis-
>98% of the HIV-1 isolates sequenced are of subtype C. In Asia, HIV-1 sion, rates of disease progression, and the development of resistance to
isolates of the CRF01_AE lineage and subtypes B and C predominate. antiretroviral drugs. This diversity may also prove to be a formidable
CRF01_AE accounts for most infections in south and southeast Asia, obstacle to HIV vaccine development, as a broadly useful vaccine
while >95% of infections in India, home to an estimated 2.1 million would need to induce protective responses against a wide range of
HIV-infected individuals, are of subtype C (see “HIV Infection and viral strains.
Harrisons_20e_Part5_p0859-p1648.indd 1397 6/1/18 12:08 PM
1398
CD4+ T cell
CCR5
CD4
gp120
Receptor Membrane
gp41 binding fusion
HIV Virion
FIGURE 197-4 Binding and fusion of HIV-1 with its target cell. HIV-1 binds to its target cell via the CD4 molecule, leading to a conformational change in the gp120
molecule that allows it to bind to the co-receptor CCR5 (for R5-using viruses). The virus then firmly attaches to the host cell membrane in a coiled-spring fashion via
the newly exposed gp41 molecule. Virus-cell fusion occurs as the transitional intermediate of gp41 undergoes further changes to form a hairpin structure that draws
the two membranes into close proximity (see text for details). (Adapted from D Montefiori, JP Moore: Science 283:336, 1999; with permission.)
vif vpu env nef
Long terminal repeat Viral infectivity Viral protein U gp160 envelope protein Negative effector (p27)
factor (p23)
PART 5
Contains control regions Promotes CD4 Cleaved in endoplasmic Promotes down-
that bind host transcription Overcomes inhibitory degratdation and reticulum to gp120 (SU) regulation of surface
factors (NF-κβ, NFAT, effects of APOBEC3, influences virion and gp 41 (TM) CD4 and MHC 1
Sp. 1, TBP) preventing hypermutation release gp120 mediates CD4 expression
Required for the intiation and viral DNA degradation Overcomes and chemokine receptor Blocks apoptosis
of transcription inhibitory effects binding, while gp41 Enhances viron
Infectious Diseases
Contains RNS trans-acting of tetherin mediates fusion activity
response element (TAR) Contains RNA response Alters state of
that binds Tat element (RRE) that cellular activation
binds Rev
Progression to disease
slowed significantly in
absence of Nef
5’ R U5 R U5 3’
gag pol vpr rev tat
Pr55gag Polymerase Viral protein R (p15) Regulator of viral Transcriptional
Polyprotein processed by PR Encodes a variety Promotes G2 gene expression (p19) activator (p14)
of viral enzymes, cell-cycle arrest Binds RRE Binds TAR
MA, matrix (p17) including PR (p10),
Undergoes myristoylation that Facilitates HIV Inhibits viral RNA In presence of host
RT and RNAase H infection of splicing and promotes cyclin T1 and CDK9
helps target gag polyprotein (p66/51), and IN (p32)
to lipid rafts macrophages nuclear export of enhances RNA Pol II
all processed by PR incompletely spliced elongation on the viral
CA capsid (p24) viral RNAs DNA template
Binds cyclophilin A and CPSF6
Target of TRIM5α
NC, nucleocapsid (p7)
Zn finger, RNA-binding protein
p6
Regulates the terminal steps in
virion budding through
interactions with TSG101 and
ALIX 1
Incorporates Vpr into viral
particles
FIGURE 197-5 Organization of the genome of the HIV provirus together with a summary description of its 9 genes encoding 15 proteins. (Adapted from WC Greene,
BM Peterlin: Nat Med 8:673, 2002.)
Harrisons_20e_Part5_p0859-p1648.indd 1398 6/1/18 12:08 PM
1399
CRF01_AE C
CRF02_AG D
CRF07_BC F
A G
B other
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
FIGURE 197-6 Global geographic distribution of HIV-1 subtypes and recombinant forms. Distributions derived from relative frequency of subtypes among >710,000
HIV genomic sequences in the Los Alamos National Laboratory HIV Sequence Database. (Additional information available at www.hiv.lanl.gov/components/sequence/
HIV/geo/geo.comp.)
TRANSMISSION ■ SEXUAL TRANSMISSION
HIV is transmitted primarily by sexual contact (both heterosexual and HIV infection is predominantly a sexually transmitted infection (STI)
male to male); by blood and blood products; and by infected mothers to worldwide. By far the most common mode of infection, particularly
infants intrapartum, perinatally, or via breast milk. After more than in developing countries, is heterosexual transmission, although in
35 years of experience and observations, there is no evidence that HIV many western countries male-to-male sexual transmission dominates.
is transmitted by any other modality. Table 197-3 lists the estimated Although a wide variety of factors including viral load and the pres-
risk of HIV transmission for various types of exposures. ence of ulcerative genital diseases influence the efficiency of hetero-
sexual transmission of HIV, such transmission is generally inefficient.
A recent systemic review found a low per-act risk of heterosexual
TABLE 197-3 Estimated Per-Act Probability of Acquiring HIV From
an Infected Source, By Exposure Act transmission in the absence of antiretrovirals: 0.04% for female-to-male
transmission and 0.08% for male-to-female transmission during vagi-
RISK PER 10,000
TYPE OF EXPOSURE EXPOSURES
nal intercourse in the absence of antiretroviral therapy or condom use
(Table 197-3).
Parenteral
HIV has been demonstrated in seminal fluid both within infected
Blood transfusion 9250 mononuclear cells and in cell-free material. The virus appears to con-
Needle-sharing during injection drug use 63 centrate in the seminal fluid, particularly in situations where there
Percutaneous (needle-stick) 23 are increased numbers of lymphocytes and monocytes in the fluid, as
Sexual seen in genital inflammatory states such as urethritis and epididymitis,
Receptive anal intercourse 138 conditions closely associated with other STIs. The virus has also been
demonstrated in cervical smears and vaginal fluid. There is an elevated
Insertive anal intercourse 11
risk of HIV transmission associated with unprotected receptive anal
Receptive penile-vaginal intercourse 8
intercourse (URAI) among both men and women compared to the risk
Insertive penile-vaginal intercourse 4 associated with unprotected receptive vaginal intercourse. Although
Receptive oral intercourse Low data are limited, the per-act risk for HIV transmission via URAI has
Insertive oral intercourse Low been estimated to be ~1.4% (Table 197-3). The risk of HIV acquisition
Othera associated with URAI is higher than that seen in penile-vaginal inter-
Biting Negligible course probably because only a thin, fragile rectal mucosal membrane
Spitting Negligible separates the deposited semen from potentially susceptible cells in
Throwing body fluids (including semen or saliva) Negligible
and beneath the mucosa, and micro-trauma of the mucosal membrane
has been associated with anal intercourse. Anal douching and sexual
Sharing sex toys Negligible
practices that traumatize the rectal mucosa also increase the likelihood
a
HIV transmission through these exposure routes is technically possible but of infection. It is likely that anal intercourse provides at least two
unlikely and not well documented.
modalities of infection: (1) direct inoculation into blood in cases of
Sources: CDC, www.cdc.gov/hiv/risk/estimates/riskbehaviors.html; P Patel: AIDS
28:1509, 2014.
traumatic tears in the mucosa; and (2) infection of susceptible target
Harrisons_20e_Part5_p0859-p1648.indd 1399 6/1/18 12:08 PM
1400 cells, such as Langerhans cells, in the mucosal layer in the absence of with a dramatic reduction in risk of transmission. In a large study of
trauma. Insertive anal intercourse also confers an increased risk of HIV serodiscordant couples, earlier treatment of the HIV-infected partner
acquisition compared to insertive vaginal intercourse in the receptive with antiretroviral therapy rather than treatment delayed until the
partner since the vaginal mucosa is several layers thicker than the rectal CD4+ T cell counts fell below 250 cells per μL was associated with
mucosa and less likely to be traumatized during intercourse. None- a 96% reduction in HIV transmission to the uninfected partner. This
theless, the virus can be transmitted to either partner through vaginal approach has been widely referred to as treatment as prevention or
intercourse. As noted in Table 197-3, male-to-female HIV transmission TasP. Recent cohort studies have indicated that if the viral load of the
is more efficient than female-to-male transmission. The differences in infected partner is decreased to below detectable levels by antiretrovi-
reported transmission rates between men and women may be due in ral therapy, there is essentially no chance of sexual transmission to the
part to the prolonged exposure to infected seminal fluid of the vagi- uninfected partner.
nal and cervical mucosa, as well as the endometrium (when semen A number of studies including large, randomized, controlled trials
enters through the cervical os). By comparison, the penis and urethral clearly have indicated that male circumcision is associated with a lower
orifice of the uninfected male partner are exposed relatively briefly to risk of acquisition of HIV infection for heterosexual men. Studies also
infected vaginal fluid. Among various cofactors examined in studies suggest that circumcision is protective in those men who have sex
of heterosexual HIV transmission, the presence of other STIs has with men who are insertive only. The benefit of circumcision may be
been strongly associated with HIV transmission. In this regard, there due to increased susceptibility of uncircumcised men to ulcerative
is a close association between genital ulcerations and transmission, STIs, as well as to other factors such as microtrauma to the foreskin
owing to both susceptibility to infection and infectivity. Infections with and glans penis. In addition, the highly vascularized inner layer of
microorganisms such as Treponema pallidum (Chap. 177), Haemophilus foreskin tissue contains a high density of Langerhans cells as well as
ducreyi (Chap. 152), and herpes simplex virus (HSV; Chap. 187) are increased numbers of CD4+ T cells, macrophages, and other cellular
important causes of genital ulcerations linked to transmission of HIV. targets for HIV. Finally, the moist environment under the foreskin may
In addition, pathogens responsible for non-ulcerative inflammatory promote the presence or persistence of microbial flora that, via inflam-
STIs such as those caused by Chlamydia trachomatis (Chap. 184), Neisseria matory changes, may lead to even higher concentrations of target cells
gonorrhoeae (Chap. 151), and Trichomonas vaginalis (Chap. 224) also are for HIV in the foreskin. In addition, randomized clinical trials have
associated with an increased risk of transmission of HIV infection. demonstrated that male circumcision also reduces herpes simplex
Bacterial vaginosis, an infection related to sexual behavior, but not virus (HSV) type 2, human papillomavirus virus (HPV), and genital
strictly an STI, also may be linked to an increased risk of transmission ulcer disease in men as well as HPV, genital ulcer disease, bacterial
of HIV infection. Several studies suggest that treating other STIs and vaginosis, and Trichomonas vaginalis infections among female partners
genital tract syndromes may help prevent transmission of HIV. This of circumcised men. Thus, there may be an added indirect benefit of
PART 5
effect is most prominent in populations in which the prevalence of HIV diminution of risk for HIV acquisition to the female sexual partners of
infection is relatively low. It is noteworthy that this principle may not circumcised men.
apply to the treatment of HSV infections since it has been shown that In some studies the use of oral contraceptives was associated with
even following anti-HSV therapy with resulting healing of HSV-related an increase in incidence of HIV infection over and above that which
genital ulcers, HIV acquisition is not reduced. Biopsy studies revealed might be expected by not using a condom for birth control. This phe-
Infectious Diseases
that the likely explanation is that HIV receptor–positive inflammatory nomenon may be due to drug-induced changes in the cervical mucosa,
cells persisted in the genital tissue despite the healing of ulcers, and so rendering it more vulnerable to penetration by the virus. Adolescent
HIV-susceptible targets remained at the site. girls might also be more susceptible to infection upon exposure due
The quantity of HIV-1 in plasma (viral load) is a primary deter- to the properties of an immature genital tract with increased cervical
minant of the risk of HIV-1 transmission. In a cohort of heterosexual ectopy or exposed columnar epithelium.
couples in Uganda discordant for HIV infection and not receiving Oral sex is a much less efficient mode of transmission of HIV than is
antiretroviral therapy, the mean serum HIV RNA level was signifi- anal intercourse or vaginal intercourse (Table 197-3). A number of stud-
cantly higher among HIV-infected subjects whose partners serocon- ies have reported that the incidence of transmission of infection by oral
verted than among those whose partners did not seroconvert. In fact, sex among couples discordant for HIV was extremely low. However,
transmission was rare when the infected partner had a plasma level of there have been well-documented reports of HIV transmission that
<1700 copies of HIV RNA per milliliter, even when genital ulcer disease likely resulted from fellatio or cunnilingus. Therefore, the assumption
was present (Fig. 197-7). The rate of HIV transmission per coital act was that oral sex is completely safe is not warranted.
highest during the early stage of HIV infection when plasma HIV RNA The association of alcohol consumption and illicit drug use with
levels were high and in advanced disease with high viral set points. unsafe sexual behavior, both homosexual and heterosexual, leads to
Antiretroviral therapy dramatically reduces plasma viremia in most an increased risk of sexual transmission of HIV. Methamphetamine
HIV-infected individuals (see “Treatment,” below) and is associated and other so-called club drugs (e.g., MDMA, ketamine, and gamma
hydroxybutyrate), sometimes taken in conjunction with PDE-5 inhibi-
50 No genital ulcer disease
tors such as sildenafil (Viagra), tadalafil (Cialis), or vardenafil (Levitra),
Genital ulcer disease have been associated with risky sexual practices and increased risk of
Probability of transmission
40
HIV infection, particularly among men who have sex with men.
per 10,000 coital acts
■ TRANSMISSION THROUGH INJECTION DRUG USE
30 HIV can be transmitted to injection drug users (IDUs) who are exposed
to HIV while sharing injection paraphernalia such as needles, syringes,
20 the water in which drugs are mixed, or the cotton through which drugs
are filtered. Parenteral transmission of HIV during injection drug
10 use does not require IV puncture; subcutaneous (“skin popping”) or
intramuscular (“muscling”) injections can transmit HIV as well, even
0 though these behaviors are sometimes erroneously perceived as low-
<1700 <1700– 12,500– ≥38,500 risk. Among IDUs, the risk of HIV infection increases with the duration
12,499 38,499 of injection drug use; the frequency of needle sharing; the number of
HIV load of infected partner, RNA copies/mL partners with whom paraphernalia are shared, particularly in the set-
FIGURE 197-7 Probability of HIV transmission per coital act among monogamous, ting of “shooting galleries” where drugs are sold and large numbers
heterosexual, HIV-serodiscordant couples in Uganda. (From RH Gray et al: Lancet of IDUs may share a limited number of “works”; comorbid psychiatric
357:1149, 2001.) conditions such as antisocial personality disorder; the use of cocaine in
Harrisons_20e_Part5_p0859-p1648.indd 1400 6/1/18 12:08 PM
injectable form or smoked as “crack”; and the use of injection drugs Exposures that place a health care worker at potential risk of HIV 1401
in a geographic location with a high prevalence of HIV infection. As infection are percutaneous injuries (e.g., a needle stick or cut with a
noted in Table 197-3, the per-act risk of transmission from injection sharp object) or contact of mucous membrane or nonintact skin (e.g.,
drug use with a contaminated needle has been estimated to be approx- exposed skin that is chapped, abraded, or afflicted with dermatitis)
imately 0.6%. with blood, tissue, or other potentially infectious body fluids. Large,
multi-institutional studies have indicated that the risk of HIV trans-
■ TRANSMISSION BY TRANSFUSED BLOOD AND mission following skin puncture from a needle or a sharp object that
BLOOD PRODUCTS was contaminated with blood from a person with documented HIV
HIV can be transmitted to individuals who receive HIV-contaminated infection is ~0.23% and after a mucous membrane exposure it is 0.09%
blood transfusions, blood products, or transplanted tissue. The vast (see “HIV and the Health Care Worker,” below) if the injured and/or
majority of HIV infections acquired via contaminated blood transfu- exposed person is not treated within 24 h with antiretroviral drugs.
sions, blood components, or transplanted tissue in resource-rich coun- The risk of hepatitis B virus (HBV) infection following a similar type of
tries occurred prior to the spring of 1985, when mandatory testing of exposure is ~6–30% in nonimmune individuals; if a susceptible worker
donated blood for HIV-1 was initiated. It is estimated that >90% of indi- is exposed to HBV, postexposure prophylaxis with hepatitis B immune
viduals exposed to HIV-contaminated blood products become infected globulin and initiation of HBV vaccine is >90% effective in preventing
(Table 197-3). Transfusions of whole blood, packed red blood cells, HBV infection. The risk of HCV infection following percutaneous
platelets, leukocytes, and plasma are all capable of transmitting HIV injury is ~1.8% (Chap. 332).
infection. In contrast, hyperimmune gamma globulin, hepatitis B immune Rare HIV transmission after nonintact skin exposure has been docu-
globulin, plasma-derived hepatitis B vaccine, and Rho immune globu- mented, but the average risk for transmission by this route has not been
lin have not been associated with transmission of HIV infection. The precisely determined; however, it is estimated to be less than the risk
procedures involved in processing these products either inactivate or for mucous membrane exposure. Transmission of HIV through intact
remove the virus. skin has not been documented. Currently in developed countries, vir-
Currently, in the United States and in most developed countries, tually all puncture wounds and mucous membrane exposures in health
the following measures have made the risk of transmission of HIV care workers involving blood from a patient with documented HIV
infection by transfused blood or blood products extremely small: the infection are treated prophylactically with combination antiretroviral
screening of blood donations for antibodies to HIV-1 and HIV-2 and therapy (cART). This practice, referred to as postexposure prophylaxis
determination of the presence of HIV nucleic acid usually in minipools or PEP, has dramatically reduced the occurrence of puncture-related
of several specimens; the careful selection of potential blood donors transmissions of HIV to health care workers.
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
with health history questionnaires to exclude individuals with risk In addition to blood and visibly bloody body fluids, semen and
behavior; and opportunities for self-deferral and the screening out of vaginal secretions also are considered potentially infectious; however,
HIV-negative individuals with serologic testing for infections that have they have not been implicated in occupational transmission from
shared risk factors with HIV, such as hepatitis B and C and syphilis. patients to health care workers. The following fluids also are consid-
The chance of infection of a hemophiliac via clotting factor concen- ered potentially infectious: cerebrospinal fluid, synovial fluid, pleural
trates has essentially been eliminated because of standard screening fluid, peritoneal fluid, pericardial fluid, and amniotic fluid. The risk for
of blood together with the added layer of safety resulting from heat transmission after exposure to fluids or tissues other than HIV-infected
treatment of the concentrates. It is currently estimated that the risk blood also has not been quantified, but it is probably considerably
of infection with HIV in the United States via transfused screened lower than the risk after blood exposures. Feces, nasal secretions,
blood is approximately 1 in 1.5 million units. Therefore, since nearly saliva, sputum, sweat, tears, urine, and vomitus are not considered
21 million blood components are transfused in the United States each potentially infectious for HIV unless they are visibly bloody. Rare cases
year, despite the best efforts of science, one cannot completely elimi- of HIV transmission via human bites have been reported, but not in the
nate the risk of transfusion-related transmission of HIV. In this regard, setting of occupational exposure.
a case of transfusion-related transmission of HIV was reported in the An increased risk for HIV infection following percutaneous expo-
United States in 2010, which was tracked to a blood donation in 2008; sures to HIV-infected blood is associated with exposures involving
this was the first such reported case since 2002 and only the third in a relatively large quantity of blood, as in the case of a device visibly
that decade. Transmission of HIV (both HIV-1 and HIV-2) by blood or contaminated with the patient’s blood, a procedure that involves
blood products is still an ongoing threat in certain developing countries a hollow-bore needle placed directly in a vein or artery, or a deep
where routine screening of blood is not universally practiced. In 2013, injury. Factors that might be associated with mucocutaneous trans-
108 out of 167 countries (65%) had specific legislation covering the mission of HIV include exposure to an unusually large volume of
safety and quality of blood transfusion, including 79% of high-income blood and prolonged contact. In addition, the risk increases for expo-
countries, 64% of middle-income countries, and 41% of low-income sures to blood from untreated patients with high levels of HIV in the
countries. Furthermore, there have been reports in certain countries of blood. Since the beginning of the HIV epidemic, there have been rare
sporadic breakdowns in routinely available screening procedures in instances where transmission of infection from a health care worker
which contaminated blood was allowed to be transfused, resulting in to patients seemed highly probable. Despite these small number of
small clusters of patients becoming infected. documented cases, the risk of HIV transmission involving health care
workers (infected or not) to patients is extremely low in developed
■ OCCUPATIONAL TRANSMISSION OF HIV: HEALTH countries—in fact, too low to be measured accurately. In this regard,
CARE WORKERS, LABORATORY WORKERS, AND THE several retrospective epidemiologic studies have been performed
HEALTH CARE SETTING tracing thousands of patients of HIV-infected dentists, physicians,
There is a small but definite occupational risk of HIV transmission to surgeons, obstetricians, and gynecologists, and no other cases of HIV
health care workers and laboratory personnel and potentially others transmission that could be linked to the health care providers were
who work with HIV-containing materials, particularly when sharp identified.
objects are used. An estimated 600,000 to 800,000 health care work- Breaches in infection control and the reuse of contaminated syringes,
ers are stuck with needles or other sharp medical instruments in the failure to properly sterilize surgical instruments, and/or hemodialysis
United States each year. The global number of HIV infections among equipment also have resulted rarely in the transmission of HIV from
health care workers attributable to sharps injuries has been estimated patient to patient in hospitals, nursing homes, and outpatient settings.
to be 1000 cases (range, 200–5000) per year. In the United States, 58 Finally, these very rare occurrences of transmission of HIV as well
documented cases of occupational HIV transmission to health care as HBV and HCV to and from health care workers in the workplace
workers, and 150 possible transmissions have been reported by the underscore the importance of the use of universal precautions when
CDC. There have been no confirmed cases reported since 1999. caring for all patients (see below and Chap. 137).
Harrisons_20e_Part5_p0859-p1648.indd 1401 6/1/18 12:08 PM
1402 ■ MOTHER-TO-CHILD TRANSMISSION OF HIV or through other exposures, such as occupationally to health care
HIV infection can be transmitted from an infected mother to her fetus workers. Saliva contains endogenous antiviral factors; among these
during pregnancy, during delivery, or by breast-feeding. This remains factors, HIV-specific immunoglobulins of IgA, IgG, and IgM isotypes
an important form of transmission of HIV infection in some develop- are detected readily in salivary secretions of infected individuals. It has
ing countries. Virologic analyses of aborted fetuses indicate that HIV been suggested that large glycoproteins such as mucins and thrombo-
can be transmitted to the fetus during the first or second trimesters of spondin 1 sequester HIV into aggregates for clearance by the host. In
pregnancy. However, maternal transmission to the fetus occurs most addition, a number of soluble salivary factors inhibit HIV to various
commonly in the perinatal period. Two studies performed in Rwanda degrees in vitro, probably by targeting host cell receptors rather than
and the Democratic Republic of Congo (then called Zaire) indicated the virus itself. Perhaps the best studied of these, secretory leukocyte
that among all mother-to-child transmissions of HIV, the relative pro- protease inhibitor (SLPI), blocks HIV infection in several cell culture
portions were 23–30% before birth, 50–65% during birth, and 12–20% systems, and it is found in saliva at levels that approximate those
via breast-feeding. required for inhibition of HIV in vitro. In this regard, higher salivary
In the absence of antiretroviral therapy for the mother during preg- levels of SLPI in breast-fed infants were associated with a decreased
nancy, labor, and delivery, and for the fetus prophylactically following risk of HIV transmission through breast milk. It has also been sug-
birth, the probability of transmission of HIV from mother to infant/ gested that submandibular saliva reduces HIV infectivity by stripping
fetus ranges from 15% to 25% in industrialized countries and from gp120 from the surface of virions, and that saliva-mediated disruption
25% to 35% in developing countries. These differences may relate to and lysis of HIV-infected cells occurs because of the hypotonicity of
the adequacy of prenatal care as well as to the stage of HIV disease oral secretions. There have been outlier cases of suspected transmission
and the general health of the mother during pregnancy. Higher rates by saliva, but these have probably been blood-to-blood transmissions.
of transmission have been reported to be associated with many Transmission of HIV by a human bite can occur but is a rare event.
factors—the best documented of which is the presence of high mater- Although virus can be identified, if not isolated, from virtually any
nal levels of plasma viremia, with the risk increasing linearly with the body fluid, there is no evidence that HIV transmission can occur as a
level of maternal plasma viremia. It is very unlikely that mother-to- result of exposure to tears, sweat, or urine. However, there have been
child transmission will occur if the mother’s level of plasma viremia is isolated cases of transmission of HIV infection by body fluids that
<1000 copies of HIV RNA/mL of blood and extremely unlikely if the may or may not have been contaminated with blood. Most of these
level is undetectable (i.e., <50 copies/mL). However, there may not be situations occurred in the setting of a close relative providing intensive
a lower “threshold” below which transmission never occurs, since cer- nursing care for an HIV-infected person without observing universal
tain studies have reported rare transmission by women with viral RNA precautions, underscoring the importance of adhering to such pre-
levels <50 copies/mL. Increased mother-to-child transmission is also cautions in the handling of body fluids and wastes from HIV-infected
PART 5
correlated with closer human leukocyte antigen (HLA) match between individuals.
mother and child. A prolonged interval between membrane rupture
and delivery is another well-documented risk factor for transmission. EPIDEMIOLOGY
Other conditions that are potential risk factors, but that have not been
consistently demonstrated, are the presence of chorioamnionitis at ■ HIV INFECTION AND AIDS WORLDWIDE
Infectious Diseases
delivery; STIs during pregnancy; illicit drug use during pregnancy; HIV infection/AIDS is a global pandemic, with cases reported
cigarette smoking; preterm delivery; and obstetric procedures such from virtually every country. At the end of 2016, an estimated
as amniocentesis, amnioscopy, fetal scalp electrodes, and episiotomy. 36.7 million individuals were living with HIV infection,
Today, the rate of mother-to-child transmission has fallen to 1% or less according to the Joint United Nations Programme on HIV/AIDS
in pregnant women who are receiving cART for their HIV infection. (UNAIDS). An estimated 95% of people living with HIV/AIDS reside
Such treatment, combined with cesarean section delivery, has ren- in low- and middle-income countries; ~50% are female, and 2.1 million
dered mother-to-child transmission of HIV an unusual event in the are children <15 years. The regional distribution of these cases is illus-
United States and other developed nations. In this regard, both the trated in Fig. 197-8. The estimated number of people living with
United States Public Health Service and the World Health Organization HIV—i.e., the global prevalence—has increased more than fourfold
guidelines recommend that all pregnant HIV-infected women should since 1990, reflecting the combined effects of continued high rates of
receive life-long cART for the health of the mother and to prevent new HIV infections and the life-prolonging impact of antiretroviral
perinatal transmission regardless of plasma HIV RNA copy number or therapy (Fig. 197-9). In 2016, the global prevalence of HIV infection
CD4+ T cell counts. among people aged 15–49 years was 0.8%, with rates varying widely by
Breast-feeding is an important modality of transmission of HIV country and region as illustrated in Fig. 197-10.
infection in certain developing countries, particularly where moth- In 2016, an estimated 1.8 million new cases of HIV infection occurred
ers continue to breast-feed for prolonged periods. The risk factors worldwide, including 160,000 among children <15 years; about one-
for mother-to-child transmission of HIV via breast-feeding include third of new infections were among people age 15–24 years. Globally,
detectable levels of HIV in breast milk, the presence of mastitis, low the majority of new HIV infections are due to heterosexual transmis-
maternal CD4+ T cell counts, and maternal vitamin A deficiency. The sion. Members of certain high-risk populations are disproportionately
risk of HIV infection via breast-feeding is highest in the early months affected. Sex workers, people who inject drugs, transgender people,
of breast-feeding. In addition, exclusive breast-feeding has been prisoners, gay men, other men who have sex with men, and their
reported to carry a lower risk of HIV transmission than mixed feeding. sexual partners accounted for 34% of all new HIV infections in 2015
In developed countries, breast feeding of babies by an HIV-infected (Fig. 197-11).
mother is contraindicated since alternative forms of adequate nutrition, Between 2000 and 2016, the estimated annual number of new HIV
i.e., formulas, are readily available. In developing countries, where infections globally fell by 40% (Fig. 197-9). These reductions in global
breast-feeding may be essential for the overall health of the infant, HIV incidence likely reflect progress with HIV prevention efforts and
the continuation of cART in the infected mother during the period of the increased provision to HIV-infected people of antiretroviral ther-
breastfeeding markedly diminishes the risk of transmission of HIV to apy, which makes them much less likely to transmit the virus to sexual
the infant. In fact, once cART has been initiated in a pregnant woman, partners. Among adults, the estimated incidence declined by 11%
it should be continued for life. from 2010 to 2016. From 2010 to 2016 there was a ~47% reduction in
HIV infections among children <15 years, progress that is due largely
■ TRANSMISSION OF HIV BY OTHER BODY FLUIDS to the increasing availability of antiretroviral medications to prevent
Although HIV can be isolated typically in low titers from saliva of a the transmission of HIV from mother to infant.
small proportion of infected individuals, there is no convincing evi- In 2016, global AIDS deaths totaled 1.0 million (including 120,000
dence that saliva can transmit HIV infection, either through kissing children <15 years), a 48% decrease since 2005 that coincides with a
Harrisons_20e_Part5_p0859-p1648.indd 1402 6/1/18 12:08 PM
1403
North America and Western and
Central Europe Eastern Europe
2.1 million and Central Asia
1.6 million
Middle East and
North Africa
230,000 Asia and the
Latin America and
the Caribbean Pacific
2.1 million Western and Central 5.1 million
Africa
6.1 million
Eastern and
Southern Africa
19.4 million
FIGURE 197-8 Estimated number of adults and children living with HIV infection as of December, 2016. Total: 36.7 million (30.8 million–42.9 million). (From Joint
United Nations Programme on HIV/AIDS [UNAIDS].)
rapid expansion of access to antiretroviral therapy (Fig. 197-12). Since The 25 countries of West and Central Africa are home to 6.1 million
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
the beginning of the pandemic, an estimated 35 million people have people living with HIV, of whom half a million are children. HIV preva-
died of an AIDS-related illness. lence in most of the countries is relatively low compared with East and
The HIV epidemic has occurred in “waves” in different regions Southern Africa. HIV prevalence among adults across the region over-
of the world, each wave having somewhat different characteristics all stands at 2.2% although there is wide variation between countries,
depending on the demographics of the country and region in ques- ranging from 0.5% in Niger and Senegal to 4.9% in Equatorial Guinea.
tion and the timing of the introduction of HIV into the population. An estimated 60% of new infections in the region in 2015 occurred in
Although the AIDS epidemic was first recognized in the United States Nigeria. As in East and Southern Africa, heterosexual transmission
and shortly thereafter in Western Europe, it very likely began in sub- accounts for most HIV transmission West and Central Africa.
Saharan Africa (see above), which has been particularly devastated The Middle East and North Africa region has one of the lowest HIV
by the epidemic. East and Southern Africa is the region hardest hit prevalence rates in the world (0.1%). In 2016, an estimated 230,000
by HIV. The region is home to 6.2% of the world’s population but has people were living with HIV in the region. Cases are largely concen-
19.4 million people living with HIV, >50% of the global total (Fig. 197-8).
trated among IDUs, men who have sex with men, and sex workers
In eight countries in the region, >10% of the adult population age 15–49
and their clients.
is HIV-infected (Fig. 197-10). South Africa has the highest number of In Asia and the Pacific, an estimated 5.1 million people were living
people living with HIV in the world (7.1 million); Swaziland has the with HIV at the end of 2016. In this region of the world, HIV prevalence
highest adult HIV prevalence in the world (27.2%). Among high-risk is highest in southeast Asian countries, with wide variation in trends
individuals, rates are much higher than in the general population. between different countries. Among countries in Asia, only Thailand
HIV prevalence among sex workers varies between 50% and 70% has an adult seroprevalence rate of >1%. However, the populations
in several countries in the region. Recent data offer promising signs of many Asian nations are so large that even low infection and sero-
of declining HIV incidence and prevalence in many countries in the prevalence rates result in large numbers of people living with HIV. In
region, although frequently at levels that remain high. Heterosexual this regard, three populous countries—China, India and Indonesia—
exposure is the primary mode of HIV transmission in most countries account for around three-quarters of all people living with HIV in the
in sub-Saharan Africa. Women and girls account for ~60 percent of all region. Although the HIV epidemic in Asia has long been concentrated
HIV infections in that region. among specific populations—sex workers and their clients, men who
have sex with men, and IDUs—it is expanding to the
4 40 heterosexual partners of those most at risk.
People living with HIV
Eastern Europe and Central Asia is the only region
New HIV infections and deaths
People living with HIV infection
in the world where the HIV epidemic continues to
expand rapidly, with a >60% increase in annual new
due to AIDS (millions)
3 30
HIV infections between 2010 and 2016. The Russian
New HIV infections Federation and Ukraine account for the majority of
(millions)
2 20 HIV cases in the region, where the epidemic has been
driven by injection drug use and increasingly by het-
erosexual transmission.
1 10 Approximately 2.1 million people were living with
Deaths due to AIDS HIV/AIDS in Latin America and the Caribbean at
the end of 2016. The rate of new HIV infections in the
0 0 region held steady from 2010 to 2016. Brazil is home
1990 1995 2000 2005 2010 2015 to the largest number of HIV-infected persons (830,00)
FIGURE 197-9 Global estimates of HIV incidence, AIDS deaths, and HIV prevalence in the region, and the Bahamas has the region’s high-
1990–2016. (From UNAIDS.) est prevalence (3.3%). Men who have sex with men
Harrisons_20e_Part5_p0859-p1648.indd 1403 6/1/18 12:08 PM
1404
N/A
<1%
1-5%
5-10%
>10%
FIGURE 197-10 Adult HIV prevalence rates by country, 2016. Data are estimates for adults age 15–49 years. (From UNAIDS.)
account for the largest proportion of HIV infections in Central and is ~0.5%. Approximately 2% of Black/African-American adults are
South America. In the Caribbean, heterosexual transmission, often tied HIV-infected in the United States, higher than any other group.
to sex work, is the main driver of transmission. The number of new HIV infections in the United States, HIV inci-
Approximately 2.1 million people were living with HIV/AIDS in dence, peaked at about 130,000 per year in the late 1980s, followed by
North America and western and central Europe at the end of 2016. declines. After remaining stable since the mid-1990s, the estimated
While modes of transmission vary greatly by country, HIV dispropor- number of annual HIV infections in the United States fell ~15%
tionately affects men who have sex with men. Over the past decade, the between 2008 and 2015 (from 45,200 to 38,500). The distribution of inci-
number of HIV diagnoses decreased dramatically in all risk groups in dent HIV cases in 2015 is shown in Fig. 197-14. Gay and bisexual men
western Europe but increased slightly in central Europe. North America account for more than two-thirds of incident infections and were the
PART 5
saw a decrease in HIV diagnoses overall but a small increase among only group that did not experience an overall decline in annual HIV
gay and bisexual men. infections from 2008 to 2015. While infections among white gay and
bisexual men and men age 15–24 years fell during that period, these
■ HIV INFECTION AND AIDS IN THE UNITED STATES declines were offset by increases among 25- to 34-year-old gay and
About 1.8 million people have been infected with HIV in the United States bisexual men, and among Hispanic/Latino gay and bisexual males.
Infectious Diseases
since the beginning of the epidemic, of whom ~693,000 have died. In the United States, the burden of HIV and AIDS is not evenly
Approximately 1.1 million individuals in the United States are living distributed across states and regions. In most areas of the country, HIV
with HIV infection, ~15% of whom are unaware of their infection, is concentrated in urban areas. In the southern United States, larger
according to recent estimates. As illustrated in Fig. 197-13, only about percentages of diagnoses are in smaller metropolitan and nonmetro-
half of HIV-infected people in the United States have been able to nego- politan areas. HIV infection and AIDS have disproportionately affected
tiate the steps in the HIV “care continuum,” from diagnosis, to enter- minority populations in the United States in both urban and rural
ing into care and receiving antiretroviral therapy, and ultimately to areas. Among those diagnosed with HIV (regardless of stage of infec-
achieving a suppressed viral load (see “Treatment,” below). tion) in 2016, 44% percent were Blacks/African Americans, a group that
More than 60% of people living with HIV in the United States are constitutes only 12% of the U.S. population. The estimated rate of new
Black/African American or Hispanic/Latino, and more than half HIV diagnoses in 2016 by race/ethnicity per 100,000 population in the
are men who have sex with men. The estimated HIV seroprevalence United States is shown in Fig. 197-15.
rate among all individuals age 13 years or older in the United States Perinatal HIV transmission, from an HIV-infected mother to her
baby, has declined significantly in the United
Sex workers States, largely due to the implementation of
(5%) guidelines for the universal counseling and
People who inject voluntary HIV testing of pregnant women and
drugs the use of antiretroviral therapy for pregnant
(8%) women and newborn infants to prevent infec-
tion. In 2016, 122 children were newly diag-
Gay men and other men HIV-infected people,
who have sex with men nosed with HIV infection in the United States,
general population
(12%) (56%)
down from a peak of ~1750 in 1991.
The rate of HIV-related deaths in the United
States rose steadily through the 1980s and
peaked in 1995. Since then, the HIV death
Transgender people rate has fallen fourfold (Fig. 197-16). This
(1%) trend is likely due to several factors, includ-
ing improved prophylaxis and treatment of
opportunistic infections, growing experience
among the health professions in caring for
Clients of sex workers HIV-infected individuals, improved access to
and other sexual health care, and a decrease in new infections.
partners of key However, the most influential factor clearly
populations has been the increased use of potent antiret-
(18%) roviral drugs, generally administered in a
FIGURE 197-11 Global distribution of new HIV infections by population. Data for 2015. (From UNAIDS.) combination of three or four agents.
Harrisons_20e_Part5_p0859-p1648.indd 1404 6/1/18 12:08 PM
70 2.5 1405
HIV treatment coverage (all ages) AIDS-related deaths (all ages)
60
Number of AIDS-related deaths (million)
2.0
Antiretroviral therapy coverage (%)
50
1.5
40
30
1.0
20
0.5
10
0 0
2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 2010 2011 2012 2013 2014 2015 2016
FIGURE 197-12 Global antiretroviral therapy coverage and number of AIDS-related deaths, 2000–2016. (From UNAIDS).
PATHOPHYSIOLOGY AND PATHOGENESIS diseases, particularly the infections and neoplasms that are AIDS-
The hallmark of HIV disease is a profound immunodeficiency resulting defining illnesses. Some features of AIDS, such as Kaposi’s sarcoma
primarily from a progressive quantitative and qualitative deficiency and certain neurologic abnormalities, cannot be explained completely
of the subset of T lymphocytes referred to as helper T cells occurring by the immunodeficiency caused by HIV infection, since these com-
in a setting of polyclonal immune activation. The helper subset of T plications may occur prior to the development of severe immunologic
impairment.
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
cells is defined phenotypically by the presence on its surface of the
CD4 molecule (Chap. 342), which serves as the primary cellular recep- The combination of viral pathogenic and immunopathogenic events
tor for HIV. A co-receptor also must be present together with CD4 that occurs during the course of HIV disease from the moment of ini-
for efficient binding, fusion, and entry of HIV-1 into its target cells tial (primary) infection through the development of advanced-stage
(Figs. 197-3 and 197-4). HIV-1 uses two major co-receptors, CCR5 and disease is complex and varied. It is important to appreciate that the
CXCR4, for fusion and entry; these co-receptors are also the primary pathogenic mechanisms of HIV disease are multifactorial and multi-
receptors for certain chemoattractive cytokines termed chemokines and phasic and are different at different stages of the disease. Therefore, it
belong to the seven-transmembrane-domain G protein–coupled family is essential to consider the typical clinical course of an untreated HIV-
of receptors. A number of mechanisms responsible for cellular depletion infected individual in order to more fully appreciate these pathogenic
and/or immune dysfunction of CD4+ T cells have been demonstrated events (Fig. 197-17).
in vitro; these include direct infection and destruction of these cells by
HIV, as well as indirect effects such as immune clearance of infected ■ EARLY EVENTS IN HIV INFECTION: PRIMARY
cells, cell death associated with aberrant immune activation, and INFECTION AND INITIAL DISSEMINATION OF VIRUS
immune exhaustion due to aberrant cellular activation with resulting Using rectal or vaginal mucosal transmission in nonhuman primates
cellular dysfunction. Patients with CD4+ T cell levels below certain as a model, the earliest events (within hours) that occur following
thresholds are at high risk of developing a variety of opportunistic exposure of HIV to the mucosal surface determine whether an infection
will be established or aborted as well as the subsequent
100 course of events following infection. Although the mucosal
barrier is relatively effective in limiting access of HIV to
87%
susceptible targets in the submucosal tissue, the virus
80 can cross the barrier by transport on Langerhans cells, an
75% epidermal type of DC, just beneath the surface or through
microscopic rents in the mucosa. Significant disruptions
in the mucosal barrier as seen in ulcerative genital disease
60 57% facilitate viral entry and increase the efficiency of infection.
55%
Virus then seeks susceptible targets, which are primarily
CD4+ T cells that are spatially dispersed in the mucosa.
40 This spatial dispersion of targets provides a significant
obstacle to the establishment of infection. Such obstacles
account for the low efficiency of sexual transmission of
HIV (see “Sexual Transmission,” above). Both “partially”
20
resting CD4+ T cells and activated CD4+ T cells serve
as early amplifiers of infection. Resting CD4+ T cells are
more abundant; however, activated CD4+ T cells produce
0 larger amounts of virus. In order for infection to become
HIV-infected HIV- Linked to HIV Retained in Suppressed established, the basic reproductive rate (R0) must become
diagnosed care within HIV care for viral load
1 month >3 months (<200 copies/mL equal to or greater than 1, i.e., each infected cell would
on most recent test) infect at least one other cell. Once infection is established,
FIGURE 197-13 Estimated percentage of HIV-infected people engaged at selected stages the virus replicates in lymphoid cells in the mucosa, the
of the continuum of HIV care in the United States. (From Centers for Disease Control and submucosa, and to some extent the lymphoreticular tissues
Prevention [CDC]: HIV Surveillance Supplemental Report 21[No. 7], 2016.) that drain the gut or genital tissues. For a variable period
Harrisons_20e_Part5_p0859-p1648.indd 1405 6/1/18 12:08 PM
1406 Gay and bisexual men who It has been demonstrated that sexual transmission
inject drugs of HIV is the result of a single infectious event and that
People who inject drugs 1200 infections (3%) a viral genetic bottleneck exists for transmission with
2200 infections (6%) selective transmission of certain viruses. In this regard,
certain characteristics of the HIV envelope glycoprotein
have a major influence on transmission, at least in
subtype A and C viruses. Transmitting viruses, often
referred to as “founder viruses,” are usually underrep-
resented in the circulating viremia of the transmitting
partner and are less-diverged viruses with signature
Heterosexuals
sequences including shorter V1–V2 loop sequences and
8800 infections (23%)
fewer predicted N-linked glycosylation sites relative
to the major circulating variants. These viruses are
almost exclusively R5 strains and are usually sensitive
to neutralizing antibody. Once replication proceeds in
the newly infected partner, the founder virus diverges
and accumulates glycosylation sites, becoming pro-
Other gressively more resistant to neutralization (Fig. 197-19).
50 infections (<1%) The acute burst of viremia and wide dissemina-
tion of virus in primary HIV infection may be asso-
Gay and bisexual men ciated with an acute HIV syndrome, which occurs to
26,200 infections (68%)
varying degrees in ~50% of individuals within 2 to
FIGURE 197-14 Estimated distribution of new HIV infections in the United States. Total: 38,500. 4 weeks of initial infection (see below). This syndrome
Incidence estimate for 2015. (From CDC.) is usually associated with high levels of viremia mea-
sured in millions of copies of HIV RNA per milliliter of
of time ranging from a few to several days, the virus cannot yet be plasma that last for several weeks. Acute mononucleosis-like symptoms
detected in the plasma. This period is referred to as the “eclipse” phase are well correlated with the presence of viremia. Virtually all patients
of infection. As more virus is produced within several days to weeks, develop some degree of viremia during primary infection, which
it is disseminated, first to the draining lymph nodes and then to other contributes to virus dissemination throughout the lymphoid tissue,
PART 5
lymphoid compartments where it has easy access to dense concentra- even though they may remain asymptomatic or not recall experiencing
tions of CD4+ T cell targets, allowing for a burst of high-level viremia symptoms. The initial level of plasma viremia in primary HIV infection
that is readily detectable by currently available assays (Fig. 197-18). does not necessarily determine the rate of disease progression; however,
The gut-associated lymphoid tissue (GALT) is a major target of HIV the set point of the level of steady-state plasma viremia after ~1 year
infection and the location where large numbers of CD4+ T cells (usu- seems to correlate with the slope of disease progression in the untreated
Infectious Diseases
ally memory cells) are infected and depleted, both by direct viral effects patient. The strikingly high levels of viremia observed in many patients
and by activation-associated apoptosis. Once virus replication reaches with acute HIV infection is felt to be associated with a higher likelihood
this threshold and virus is widely disseminated, infection is firmly of transmission of the virus to others by a variety of routes including
established throughout the lymphoid tissues of the body and the pro- sexual transmission, shared needles and syringes, and mother-to-child
cess is irreversible. It is important to point out that the initial infection transmission intrapartum, perinatally, or via breast milk.
of susceptible cells may vary somewhat with the route of infection.
Virus that enters directly into the bloodstream via infected blood or ■ ESTABLISHMENT OF CHRONIC AND PERSISTENT
blood products (i.e., transfusions, use of contaminated needles for INFECTION
injection drugs, sharp-object injuries, maternal-to-fetal transmission
either intrapartum or perinatally, or sexual intercourse where there is Persistence of Virus Replication HIV infection is unique
enough trauma to cause bleeding) is likely first cleared from the circu- among human viral infections. Despite the robust cellular and humoral
lation to the spleen and other lymphoid organs, where primary focal immune responses that are mounted following primary infection (see
infections begin, followed by wider dissemination throughout other “Immune Response to HIV,” below), once infection has been estab-
lymphoid tissues as described above. lished the virus succeeds in escaping complete immune-mediated clear-
ance, paradoxically seems to thrive on immune activation, and is never
eliminated completely from the body. Rather, a chronic infection devel-
Black/African American ops and persists with varying degrees of continual virus replication
in the untreated patient for a median of ~10 years before the patient
Hispanic/Latino becomes clinically ill (see “Advanced HIV Disease,” below). It is this
establishment of a chronic, persistent infection that is the hallmark of
Multiple races
HIV disease. Throughout the often-protracted course of chronic infec-
tion, virus replication can invariably be detected in untreated patients
American Indian/
Alaska Native by widely available assays that measure copies of virion-associated
HIV RNA in plasma (copies per milliliter). Levels of virus vary greatly
Native Hawaiian/Other
Pacific Islander in most untreated patients, usually ranging from several thousand to a
few million copies of HIV RNA per milliliter of plasma. Studies using
Asian highly sensitive molecular techniques have demonstrated that even in
certain patients in whom plasma viremia is suppressed to below detec-
White tion (lower limit, 20–50 copies of HIV RNA per milliliter depending
on assay kit manufacturer) by cART, there is a continual low level of
0 10 20 30 40 50 virion production in the majority of infected patients. In other human
Rate/100,000 population viral infections, with very few exceptions, if the host survives, the virus
FIGURE 197-15 Estimated rate of HIV infections (including children) diagnosed is completely cleared from the body and a state of immunity against
during 2016 in the United States, by race/ethnicity (per 100,000 population). subsequent infection develops. HIV infection very rarely kills the host
(From CDC.) during primary infection. Certain viruses, such as HSV (Chap. 187), are
Harrisons_20e_Part5_p0859-p1648.indd 1406 6/1/18 12:08 PM
18 antibodies against the HIV envelope and does 1407
so only after years of persistent virus replication
16 and after the infection is firmly established (see
Deaths per 100,000 population
below). Extensive analyses of sequential HIV iso-
14
lates and host responses have demonstrated that
12 viral escape from B cell and CD8+ T cell responses
occurs early after infection and allows the virus to
10 stay one step ahead of effective immune responses.
Virus-specific CD8+ CTLs expand greatly during
8 primary HIV infection, and they likely represent
6 the high-affinity responses that would be expected
to be most efficient in eliminating virus-infected
4 cells; however, viral control is generally incomplete
as viral replication persists at relatively high levels
2 in the majority of individuals. In addition to viral
escape from CTLs through high rates of mutation,
0
1987 1989 1991 1993 1995 1997 1999 2001 2003 2005 2007 2009 2011 2013 it is thought that the initially strong response
Year of death becomes qualitatively dysfunctional owing to the
overwhelming immune activation associated with
FIGURE 197-16 Trends in annual age-adjusted rates of death due to HIV infection, United States,
1987–2014. Age distribution based on 2000 population. (From CDC.)
persistent viral replication, leading to immune
“exhaustion” that affects both arms of adaptive
immunity. Several studies have indicated that
not completely cleared from the body after infection, but instead enter a exhaustion of HIV-specific CD8+ T cells during prolonged immune
latent state; in these cases, clinical latency is accompanied by microbio- activation is associated with upregulation of several inhibitory recep-
logic latency. This is not the case with HIV infection as described above. tors, such as programmed death (PD) 1 molecule (of the B7-CD28
Chronicity associated with persistent virus replication can also be seen family of molecules), T cell immunoreceptor with Ig and ITIM
in certain cases of HBV and HCV infections (Chap. 334); however, in domains (TIGIT), T cell immunoglobulin and mucin-domain containing
these infections the immune system is not a target of the virus. molecule 3 (Tim-3), and lymphocyte activating gene 3 (Lag-3), collec-
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
tively referred to as immune-checkpoint receptors. Upregulation of these
Escape of HIV from Effective Immune System Control surface proteins restricts polyreactivity and proliferative capacity, func-
Inherent to the establishment of chronicity of HIV infection is the abil- tional attributes of CD8+ T cells that are essential for effective killing of
ity of the virus to evade adequate control and elimination by both the pathogens. Another mechanism contributing to the evasion by HIV of
cellular and humoral immune responses. There are a number of mecha- immune system control is the downregulation of HLA class I molecules
nisms whereby the virus accomplishes this evasion. Paramount among on the surface of HIV-infected cells by the viral proteins Nef, Tat, and
these is the establishment of a sustained level of replication associated Vpu, resulting in the lack of ability of CD8+ CTLs to recognize and kill
with the generation of viral diversity via mutation and recombina- infected target cells. Although this downregulation of HLA class I mol-
tion. The selection of mutants that escape control by CD8+ cytolytic ecules would seem to favor elimination of HIV-infected cells by natural
T lymphocytes (CTLs) is critical to the propagation and progression of killer (NK) cells, this latter mechanism does not remove HIV-infected
HIV infection. The high rate of virus replication associated with inev- cells effectively (see below). Another potential means of escape of
itable mutations also contributes to the inability of antibody to clear HIV-infected cells from elimination by CD8+ CTLs is the sequestration
the autologous virus. Furthermore, for reasons that remain unclear, the of infected cells in immunologically privileged sites such as the central
humoral immune system does not readily produce classic neutralizing nervous system (CNS), as well as the low frequency of virus-specific
±Acute HIV syndrome Death
Wide dissemination of virus
Seeding of lymphoid organs Opportunistic
diseases
Primary Constitutional
infection symptoms
1200 108
HIV RNA Copies per mL Plasma
1100
1000 107
CD4+ T Lymphocyte count (cells/µL)
900 Clinical latency
800 106
700
600 105
500
400 104
300
200 103
100
0 102
0 3 6 9 12 1 2 3 4 5 6 7 8 9 10 11
Weeks Years
FIGURE 197-17 Typical course of an untreated HIV-infected individual. See text for detailed description. (From G Pantaleo et al: N Engl J Med 328:327, 1993. Copyright
1993 Massachusetts Medical Society. All rights reserved.)
Harrisons_20e_Part5_p0859-p1648.indd 1407 6/1/18 12:08 PM
1408 Lamina propria Lymphoid tissue
Infected “resting” Late-responding CTLs
“Resting” CD4+ T cells
CD4+ T cells PD-1+CD8+
HIV T cells
virions
Establishment Partial
Dissemination of lymphoid- control
of virus tissue viral Immune
reservoir activation
Crossing Activated
the CD4+ T cell
barrier
Sustained
HIV
DC Infected production
activated
CD4+ T cell Regulatory
Infected Macrophage
cell T cells
Hours Days Weeks Years
FIGURE 197-18 Summary of early events in HIV infection. See text for detailed description. CTLs, cytolytic T lymphocytes; HIV, human immunodeficiency virus.
(Adapted from AT Haase: Nat Rev Immunol 5:783, 2005.)
CD8+ CTLs in areas of lymphoid tissues, namely germinal centers, profoundly negative consequences for the immunologic control of
where HIV actively replicates. HIV replication. Furthermore, this loss occurs early in the course
The principal targets of neutralizing antibodies against HIV are the of infection, and animal studies indicate that 40–70% of all memory
envelope proteins gp120 and gp41. HIV employs at least three mech- CD4+ T cells in the GALT are eliminated during acute infection. During
PART 5
anisms to evade neutralizing antibody responses: hypervariability in chronic HIV viremia, CD4+ T cells also exhibit evidence of exhaustion,
the primary sequence of the envelope, extensive glycosylation of the including by upregulation of the cytotoxic T-lymphocyte-associated
envelope, and conformational masking of neutralizing epitopes. Sev- antigen 4 (CTLA-4), also a member of the B7-CD28 family.
eral studies that have followed the evolution of the humoral immune Finally, the escape of HIV from immune-mediated elimination dur-
response to HIV from the earliest points after primary infection indi- ing primary infection allows the formation of a pool of latently infected
Infectious Diseases
cate that the virus continually mutates to escape the emerging antibody cells, referred to as the viral reservoir, that may not be recognized or
response such that the sequential antibodies that are induced do not completely eliminated by virus-specific CTLs or by ART (see below).
neutralize the currently autologous virus. Broadly neutralizing antibodies Thus, despite a potent immune response and the marked downregula-
capable of neutralizing a wide range of primary HIV isolates in vitro tion of virus replication following primary HIV infection, HIV succeeds
occur in only about 20% of HIV-infected individuals, and, when they in establishing a state of chronic infection with a variable degree of
do occur, 2 to 3 years of infection with continual virus replication are persistent virus replication. During this period most patients make the
generally required to drive the affinity maturation of the antibodies. clinical transition from acute primary infection to variable periods of
Unfortunately, by the time these broadly neutralizing antibodies are clinical latency or smoldering disease activity (see below).
formed, they are ineffective in containing the virus currently replicat-
ing in the patient. Persistent viremia also results in exhaustion of The HIV Reservoir: Obstacles to the Eradication of
B cells similar to the exhaustion reported for CD8+ T cells, adding to Virus A pool of latently infected, resting CD4+ T cells that serves as
the defects in the humoral response to HIV. at least one component of the persistent reservoir of virus exists in vir-
CD4+ T cell help is essential for the integrity of antigen-specific tually all HIV-infected individuals, including those who are receiving
immune responses, both humoral and cell-mediated. HIV preferen- cART. Such cells carry an integrated form of HIV DNA in the genome
tially infects activated CD4+ T cells including HIV-specific CD4+ of the host and can remain in this state until an activation signal drives
T cells, and so this loss of viral-specific helper T cell responses has the expression of HIV transcripts. Only a small fraction of the latently
infected cells in the viral reservoir contain replication-competent virus
with the overwhelming majority of cells containing defective provi-
ruses incapable of a full replication cycle. However, upon activation of
the reservoir variable degrees of sustained virus replication invariably
Founder
occur. This form of latency is to be distinguished from preintegration
Replicating virus latency, in which HIV enters a resting CD4+ T cell and, in the absence
of an activation signal, reverse transcription of the HIV genome occurs
to a certain extent but the resulting proviral DNA fails to integrate into
the host genome. This period of preintegration latency may last hours
to days, and if no activation signal is delivered to the cell, the proviral
DNA loses its capacity to initiate a productive infection. If these cells do
become activated prior to decay of the preintegration complex, reverse
transcription proceeds to completion and the virus continues along its
replication cycle (see above and Fig. 197-20). The pool of cells that are
in the postintegration state of latency is established early during the
FIGURE 197-19 As HIV diverges from founder to chronically replicating virus,
course of primary HIV infection. Despite the suppression of plasma
it accumulates N-linked glycosylation sites. See text for detailed description. viremia to undetectable levels by potent regimens of cART adminis-
(Adapted from CA Derdeyn et al: Science 303:2019, 2004; B Chohan et al: J Virol tered over several years, this pool of latently infected cells persists and
79:6528, 2005; and BF Keele et al: Proc Natl Acad Sci USA 105:7552, 2008.) can give rise to replication-competent virus upon cellular activation ex
Harrisons_20e_Part5_p0859-p1648.indd 1408 6/1/18 12:08 PM
2 weeks. It was determined on the basis of modeling the kinetics of 1409
viral decline and the emergence of resistant mutants during therapy
Resting CD4+ T cell that 93–99% of the circulating virus originated from recently infected,
rapidly turning over CD4+ T cells and that ~1–7% of circulating virus
originated from longer-lived cells, likely monocytes/macrophages.
A negligible amount of circulating virus originated from the pool of
latently infected cells (Fig. 197-21). It was also determined that the
Preintegration latency
half-life of a circulating virion was ~30–60 min and that of produc-
(unstable)
T cell activation tively infected cells was 1 day. Given the relatively steady level of
(Ag, cytokines) plasma viremia and of infected cells, it appears that extremely large
amounts of virus (~1010–1011 virions) are produced and cleared from
the circulation each day. In addition, data suggest that the minimal
Degradation duration of the HIV-1 replication cycle in vivo is ~2 days. Other studies
of unintegrated have demonstrated that the decrease in plasma viremia that results from
HIV DNA
cART correlates closely with a decrease in virus replication in lymph
T cell activation nodes, further confirming that lymphoid tissue is the main site of HIV
(Ag, cytokines)
replication and the main source of plasma viremia.
CTLs The level of steady-state viremia, called the viral set point, at ~1 year
following acquisition of HIV infection has important prognostic impli-
Resting CD4+ T cell cations for the progression of HIV disease in the untreated patient. It
Postintegration Active Virus Replication has been demonstrated that, as a group, untreated HIV-infected indi-
latency (stable) viduals who have a low set point at 6 months to 1 year following infec-
Cytopathic tion progress to AIDS much more slowly than do individuals whose set
effect of point is very high at that time (Fig. 197-22).
Resting latently infected virus
CD4+ memory T cells
Clinical Latency versus Microbiologic Latency With the
T cell activation exception of certain long-term nonprogressors and “elite controllers”
of HIV replication, the level of CD4+ T cells in the blood inevitably
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
(Ag, cytokines)
decreases progressively in viremic HIV-infected individuals in the
absence of cART. The decline in CD4+ T cells may be gradual or
abrupt, the latter usually reflecting a significant spike in the level of
plasma viremia. Most patients are relatively asymptomatic while this
Virus spread
progressive decline is taking place (see below) and are often described
FIGURE 197-20 Generation of latently infected, resting CD4+ T cells in as being in a state of clinical latency. However, this term is misleading;
HIV-infected individuals. See text for details. Ag, antigen; CTLs, cytolytic it does not mean disease latency, since progression, although slow in
T lymphocytes. (Courtesy of TW Chun; with permission.) many cases and often without symptoms, is generally relentless during
this period. Furthermore, clinical latency should not be confused with
microbiologic latency, since varying levels of virus replication inev-
vivo. Modeling studies built on projections of decay curves have esti- itably occur during this period of clinical latency. Even in those rare
mated that in such a setting of prolonged viral suppression, it would patients who have <50 copies of HIV RNA per milliliter in the absence
require a few to several years for the pool of latently infected cells to be of therapy, there is virtually always some degree of low-level ongoing
completely eliminated. This has not been documented to occur spon- virus replication.
taneously in any patients very likely because the latent viral reservoir
is long-lived and is continually replenished by the low levels of persis-
tent virus replication that may remain below the limits of detection of ■ ADVANCED HIV DISEASE
current assays (see below) as well as by the expansion by proliferation In untreated patients or in patients in whom therapy has not ade-
of the pool of latently infected cells (Fig. 197-20), even in patients who quately controlled virus replication, after a variable period, usually
for the most part are treated successfully. Reservoirs of HIV-infected measured in years, the CD4+ T cell count falls below a critical level
cells, latent or otherwise, can exist in a number of compartments (<200/μL) and the patient becomes highly susceptible to opportunistic
including the lymphoid tissue, peripheral blood, and the
CNS (likely in cells of the monocyte/macrophage lineage) Productively infected Latently infected
as well as in other unidentified locations. Over the past CD4+ lymphocytes CD4+ lymphocytes
several years attempts have been made to eliminate HIV
in the latent viral reservoir using agents that activate ≤1%
resting CD4+ T cells during the course of cART; however,
2 days per generation
93–99%
such attempts, referred to as “shock and kill,” have been
unsuccessful. Thus, this persistent reservoir of infected Uninfected
cells and/or low levels of persistent virus replication t1/2 = 1.0 day CD4+ lymphocytes
remain major obstacles to the goal of eradication of virus
from infected individuals and hence a “cure,” despite the
favorable clinical outcomes that have resulted from cART. t1/2 = 30–60 min
1–7% CD4+ lymphocytes
HIV-1
Viral Dynamics The dynamics of viral production infected with
defective viruses
and turnover have been quantified using mathematical
modeling in the setting of the administration of reverse
transcriptase and protease inhibitors to HIV-infected Uninfected, activated Long-lived
individuals in clinical studies. Treatment with these drugs CD4+ lymphocytes cell populations
resulted in a precipitous decline in the level of plasma FIGURE 197-21 Dynamics of HIV infection in vivo. See text for detailed description. (From AS
viremia, which typically fell by well over 90% within Perelson et al: Science 271:1582, 1996.)
Harrisons_20e_Part5_p0859-p1648.indd 1409 6/1/18 12:08 PM
1410 1 often undetectable by standard assays and normal CD4+ T
cell counts. It is noteworthy that certain of their HIV-specific
0.9 immune responses are robust and clearly superior to those
Proportion surviving without AIDS
0.8 of HIV-infected progressors. In this group of elite controllers
certain HLA class I haplotypes are overrepresented, particu-
0.7 larly HLA-B57-01 and HLA-B27-05. Outside of the subgroup
0.6
of elite controllers, a number of other genetic factors have
been shown to be involved to a greater or lesser degree in
0.5 the control of virus replication and thus in the rate of HIV
disease progression (see “Genetic Factors in HIV-1 and AIDS
0.4 HIV RNA copies/mL
Pathogenesis,” below).
0.3 ≤9060
9,061 to 26,040 ■ LYMPHOID ORGANS AND HIV
0.2 PATHOGENESIS
26,041 to 72,540
0.1 >72,540 Regardless of the portal of entry of HIV, lymphoid tissues
are the major anatomic sites for the establishment and prop-
0 agation of HIV infection. Despite the use of measurements
2 4 6 8 10
of plasma viremia to determine the level of disease activity,
Time, years virus replication occurs mainly in lymphoid tissue and not
FIGURE 197-22 Relationship between levels of virus and rates of disease progression. in blood; indeed, the level of plasma viremia directly reflects
Kaplan-Meier curves for AIDS-free survival stratified by baseline HIV-1 RNA categories (copies virus production in lymphoid tissue.
per milliliter). (From JW Mellors et al: Science 272:1167, 1996.) Some patients experience progressive generalized lymph-
adenopathy early in the course of the infection; others
disease (Fig. 197-17). For this reason, the CDC case definition of AIDS experience varying degrees of transient lymphadenopathy. Lymphade-
includes all HIV-infected individuals >5 years of age with CD4+ T cell nopathy reflects the cellular activation and immune response to the
counts below this level (Table 197-2). Patients may experience consti- virus in the lymphoid tissue, which is generally characterized by follic-
tutional signs and symptoms or may develop an opportunistic disease ular or germinal center hyperplasia. Lymphoid tissue involvement is a
abruptly without any prior symptoms. The depletion of CD4+ T cells common denominator of virtually all patients with HIV infection, even
continues to be progressive and unrelenting in this phase. It is not those without easily detectable lymphadenopathy.
uncommon for CD4+ T cell counts in the untreated patient to drop to as Examinations of lymph tissue and peripheral blood in patients and
PART 5
low as 10/μL or even to zero. In countries where cART and prophylaxis monkeys during various stages of HIV and SIV infection, respectively,
and treatment for opportunistic infections are readily accessible to such have led to substantial insight into the pathogenesis of HIV disease.
patients, survival is increased dramatically even in those patients with In most of the original human studies, peripheral lymph nodes have
advanced HIV disease. In contrast, untreated patients who progress to been used predominantly as the source of lymphoid tissue. More recent
Infectious Diseases
this severest form of immunodeficiency usually succumb to opportu- studies in monkeys and humans have also focused on the GALT, where
nistic infections or neoplasms (see below). the earliest burst of virus replication occurs associated with marked
depletion of CD4+ T cells. In detailed studies of peripheral lymph node
■ LONG-TERM SURVIVORS, LONG-TERM tissue that utilized a variety of molecular techniques to measure the
NONPROGRESSORS, AND ELITE CONTROLLERS level of HIV DNA and RNA and imaging techniques to visualize virus
It is important to distinguish between the terms long-term survivor and and cells, the following picture has emerged. During acute HIV infec-
long-term nonprogressor. Long-term nonprogressors are by definition tion resulting from mucosal transmission, virus replication progres-
long-term survivors; however, the reverse is not always true. Predic- sively amplifies from scattered lymphoid cells in the lamina propria of
tions from one study that antedated the availability of effective cART the gut to draining lymphoid tissue, leading to high levels of plasma
estimated that ~13% of homosexual/bisexual men who were infected viremia. The GALT plays a major role in the amplification of virus
at an early age may remain free of clinical AIDS for >20 years. Many replication, and virus is disseminated from replication in the GALT to
of these individuals may have progressed in their degree of immune peripheral lymphoid tissue. A profound degree of cellular activation
deficiency; however, they certainly survived for a considerable period occurs within lymphoid tissue (see below) and is reflected in follicular
of time. With the advent of effective cART, the survival of HIV- or germinal center hyperplasia. At this time copious amounts of extra-
infected individuals has dramatically increased. Early in the AIDS cellular virions (both infectious and defective) are trapped on the pro-
epidemic, prior to the availability of therapy, if a patient presented cesses of the follicular dendritic cells (FDCs) in the germinal centers of
with a life-threatening opportunistic infection, the median survival the lymph nodes. Virions that have bound complement components
was 26 weeks from the time of presentation. Currently, an HIV-infected on their surfaces attach to the surface of FDCs via interactions with
20-year-old individual in a high-income country who is appropriately complement receptors and likely via Fc receptors that bind to anti-
treated with cART can expect to live at least 50 years according to math- bodies that are attached to the virions. In situ hybridization reveals
ematical model projections. In the face of cART, long-term survival is expression of virus in individual cells of the paracortical area and, to
becoming commonplace. Definitions of long-term nonprogressors have a lesser extent, the germinal center (Fig. 197-23). The persistence of
varied considerably over the years, and so such individuals constitute trapped virus likely reflects a steady state whereby trapped virus turns
a heterogeneous group. Long-term nonprogressors were first described over and is replaced by fresh virions that are continually produced. The
in the 1990s. Originally, individuals were considered to be long-term trapped virus, either as whole virion or shed envelope, serves as a con-
nonprogressors if they had been infected with HIV for a long period tinual activator of CD4+ T cells, thus driving further virus replication.
(≥10 years), their CD4+ T cell counts were in the normal range, and they During the early stages of HIV disease, the architecture of lymphoid
remained stable over years without receiving cART. Approximately tissues is generally preserved and may even be hyperplastic owing to
5–15% of HIV-infected individuals fell into this broader nonprogressor an increased presence of B cells and specialized CD4+ T cells called
category. However, this group was rather heterogenous and over time follicular helper CD4+ T cells (TFH) in prominent germinal centers.
a significant proportion of these individuals progressed and ultimately Extracellular virions can be seen by electron microscopy attached to
required therapy. From this broader group, a much smaller subgroup FDC processes. The trapping of antigen is a physiologically normal
of “elite” controllers or nonprogressors was identified, and they consti- function for the FDCs, which present antigen to B cells and, along with
tuted a fraction of 1% of HIV-infected individuals. These elite control- stimulatory factors produced by TFH cells, contribute to the genera-
lers, by definition, have extremely low levels of plasma viremia that is tion of B cell memory. However, in the case of HIV, persistent cellular
Harrisons_20e_Part5_p0859-p1648.indd 1410 6/1/18 12:08 PM
■ THE ROLE OF IMMUNE ACTIVATION AND 1411
INFLAMMATION IN HIV PATHOGENESIS
Activation of the immune system and variable degrees of inflamma-
tion are essential components of any appropriate immune response
to a foreign antigen. However, immune activation and inflammation,
which can be considered aberrant in HIV-infected individuals, play a
critical role in the pathogenesis of HIV disease as well as other chronic
conditions associated with HIV infection. Immune activation and
inflammation in the HIV-infected individual contribute substantially
to (1) the replication of HIV, (2) the induction of immune dysfunction,
and (3) the increased incidence of chronic conditions such as premature
cardiovascular disease (Table 197-4).
INDUCTION OF HIV REPLICATION BY ABERRANT IMMUNE ACTIVATION The
immune system is normally in a state of homeostasis, awaiting pertur-
bation by foreign antigenic stimuli. Once the immune response deals
with and clears the antigen, the system returns to relative quiescence
(Chap. 342). This is generally not the case in HIV infection where, in
FIGURE 197-23 HIV in the lymph node of an HIV-infected individual. An individual the untreated patient, virus replication is invariably persistent with
cell infected with HIV shown expressing HIV RNA by in situ hybridization using a very few exceptions and immune activation is persistent. HIV rep-
radiolabeled molecular probe. Original ×500. (Adapted from G Pantaleo, AS Fauci licates most efficiently in activated CD4+ T cells; in HIV infection,
et al: Nature 362:355, 1993.)
chronic activation provides the cell substrates necessary for persistent
virus replication throughout the course of HIV disease, particularly
activation, resulting in a shift to secretion of proinflammatory cytok- in the untreated patient. Even in certain patients receiving cART
ines such as interleukin (IL) 1β, tumor necrosis factor (TNF) α, IFN-γ, whose levels of plasma viremia are suppressed to below the level of
and IL-6, can induce viral replication (see below) and diminish the detection by standard assays, there are low but detectable degrees
effectiveness of the immune response against the virus. In addition, the of virus replication that drives persistent immune activation. From a
CD4+ TFH cells that are recruited into the germinal center to provide virologic standpoint, although quiescent CD4+ T cells can be infected,
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
help to B cells in the generation of an HIV-specific immune response albeit inefficiently, with HIV, reverse transcription, integration, and
are highly susceptible to infection and may be an important component virus spread are much more efficient in activated cells. Furthermore,
of the HIV reservoir. Thus, in HIV infection, a normal physiologic func- cellular activation induces expression of virus in cells latently infected
tion of the immune system that contributes to the clearance of virus, as with HIV. In essence, immune activation and inflammation provide
well as to the generation of a specific immune response, can also have the engine that drives HIV replication. In addition to endogenous
deleterious consequences. factors such as cytokines, a number of exogenous factors such as other
As HIV disease progresses, the architecture of lymphoid tissues microbes that are associated with heightened cellular activation can
begins to show disruption. Confocal microscopy reveals destruction enhance HIV replication and thus may play a role in HIV pathogen-
of the fibroblastic reticular cell (FRC) and FDC networks in the T cell esis. Co-infection with a range of viruses, such as HSV types 1 and 2,
zone and B cell follicles, respectively. The mechanisms of destruction cytomegalovirus (CMV), human herpesvirus (HHV) 6, Epstein-Barr
are not completely understood, but they are thought to be associated virus (EBV), HBV, HCV, adenovirus, and HTLV-1 have been shown to
with collagen deposition causing fibrosis and loss of production of upregulate HIV expression. In addition, infestation with nematodes
cytokines such as IL-7 and lymphotoxin-α, which are critical to the has been shown to be associated with a heightened state of immune
maintenance of lymphoid tissues and their lymphocyte constituents. activation that facilitates HIV replication; in certain studies deworm-
As the disease progresses to an advanced stage, there is complete ing of the infected host has resulted in a decrease in plasma viremia.
disruption of the architecture of the lym-
phoid tissues, accompanied by dissolu-
tion of the FRC and FDC networks. At HIV-specific
this point, the lymph nodes are “burnt immune response
out.” This destruction of lymphoid tis-
sue compounds the immunodeficiency
Massive viremia
of HIV disease and contributes both to
the inability to control HIV replication
and to the inability to mount adequate
immune responses against opportunis- Wide dissemination
to lymphoid organs
tic pathogens. The events from primary
infection to the ultimate destruction of Establishment of Trapping of virus and
the immune system are illustrated in Primary infection in GALT establishment of chronic,
Fig. 197-24. More recently, nonhuman pri- infection persistent infection
mate studies and some human studies have Partial immunologic
examined GALT at various stages of HIV control of virus replication
disease. Within the GALT, the basal level
of cellular activation combined with virus- Immune activation
mediated by
mediated activation results in the infec- Destruction of Accelerated virus cytokines and HIV
tion and elimination of an estimated Immune Sy stem replication envelope-mediated
50–90% of CD4+ T cells in the gut. The aberrant cell signaling
extent of this early damage to GALT, which
constitutes a major component of lym- Rapid CD4 + T cell turnover
phoid tissue in the body, may play a role in FIGURE 197-24 Events that transpire from primary HIV infection through the establishment of chronic persistent
determining the potential for immunologic infection to the ultimate destruction of the immune system. See text for details. CTLs, cytolytic T lymphocytes;
recovery of the memory cell subset. GALT, gut-associated lymphoid tissue.
Harrisons_20e_Part5_p0859-p1648.indd 1411 6/1/18 12:08 PM
1412 TABLE 197-4 Conditions Associated with Persistent Immune spectrum of non-HIV antigens may be compromised if immunocom-
Activation and Inflammation in Patients with HIV Infection petent bystander cells are maintained in a state of chronic activation.
Accelerated aging syndrome The deleterious effects of chronic immune activation on the pro-
Bone fragility gression of HIV disease are well established. As in most conditions of
Cancers persistent antigen exposure, the host must maintain sufficient activa-
tion of antigen (HIV)-specific responses but must also prevent exces-
Cardiovascular disease
sive activation and potential immune-mediated damage to tissues.
Diabetes
Certain studies suggest that normal immunoregulatory mechanisms
Kidney disease that act to keep hyperimmune activation in check, particularly CD4+,
Liver disease FoxP3+, and CD25+ regulatory T cells (T-regs), may be dysfunctional
Neurocognitive dysfunction or depleted in the context of advanced HIV disease.
Two diseases of extraordinary global health significance, malaria and Apoptosis Apoptosis is a form of programmed cell death that is a
tuberculosis (TB), have been shown to increase HIV viral load in dually normal mechanism for the elimination of effete cells in organogenesis
infected individuals. Globally, Mycobacterium tuberculosis is the most as well as in the cellular proliferation that occurs during a normal
common opportunistic infection in HIV-infected individuals (Chap. immune response (Chap. 342). Apoptosis can occur by intrinsic or
173). In addition to the fact that HIV-infected individuals are more extrinsic pathways, the latter of which is largely dependent on cellular
likely to develop active TB after exposure and to reactivate latent TB, activation, and the aberrant cellular activation associated with HIV
it has been demonstrated that active TB can accelerate the course of disease is correlated with a heightened state of apoptosis. HIV can
HIV infection. It has also been shown that levels of plasma viremia are trigger activation-induced cell death through the upregulation of the
greatly elevated in HIV-infected individuals with active TB who are death receptors, such as Fas/CD95, TNFR1, or TNF-related apoptosis-
not receiving cART, compared with pre-TB levels and levels of viremia inducing ligand (TRAIL) receptors 1 and 2. Their corresponding
after successful treatment of the active TB. The situation is similar in ligands FasL, TNF, and TRAIL also are upregulated in HIV disease.
the interaction between HIV and malaria parasites (Chap. 219). Acute HIV-induced stress and alterations in homeostasis also can trigger
infection of HIV-infected individuals with Plasmodium falciparum intrinsic apoptosis due to the downregulation of antiapoptotic proteins
increases HIV viral load, and the increased viral load is reversed by such as Bcl-2. Other mechanisms of HIV-induced cell death have been
effective treatment of malaria. described, including autophagy, necrosis, necroptosis, and pyroptosis.
The phenomenon of pyroptosis, an inflammatory form of cell death
MICROBIAL TRANSLOCATION AND PERSISTENT IMMUNE ACTIVATION One
involving the upregulation of the proinflammatory enzyme caspase
proposed mechanism of persistent immune activation involves the
PART 5
1 and release of the proinflammatory cytokines IL-1β and IL-18, has
disruption of the mucosal barrier in the gut due to HIV replication in
been linked to a bystander effect of HIV replication on CD4+ T cells.
submucosal lymphoid tissue. As a result of this disruption, there is an
The process of pyroptosis generates multimeric complexes called
increase in the products, particularly lipopolysaccharide (LPS), of bacte-
inflammasomes, which can also be activated by LPS. Certain viral gene
ria that translocate from the bowel lumen through the damaged mucosa
products have been associated with enhanced susceptibility to apopto-
Infectious Diseases
to the circulation, leading to persistent systemic immune activation and
sis; these include Env, Tat, and Vpr. In contrast, Nef has been shown to
inflammation. This effect can persist even after the HIV viral load is
possess antiapoptotic properties. The intensity of apoptosis correlates
brought to <50 copies/mL by cART. Depletion in the GALT of IL-17–
with the general state of activation of the immune system and not
producing T cells, which are responsible for defense against extracellu-
with the stage of disease or with viral burden. A number of studies,
lar bacteria and fungi, also is thought to contribute to HIV pathogenesis.
including those examining lymphoid tissue, have demonstrated that
PERSISTENT IMMUNE ACTIVATION AND INFLAMMATION INDUCE IMMUNE the rate of apoptosis is elevated in HIV infection and that apoptosis
DYSFUNCTION The immune activated state in HIV infection is reflected is seen in “bystander” cells such as CD8+ T cells and B cells as well as
by hyperactivation of B cells leading to hypergammaglobulinemia; in uninfected CD4+ T cells. It is likely that this bystander apoptosis of
increased lymphocyte turnover; activation of monocytes; expression immunocompetent cells related to immune activation contributes to
of activation markers and immune checkpoint receptors on CD4+ the general immune abnormalities in HIV disease.
and CD8+ T cells; increased activation-associated cellular apoptosis;
lymph node hyperplasia, particularly early in the course of disease; MEDICAL CONDITIONS ASSOCIATED WITH PERSISTENT IMMUNE ACTIVATION
increased secretion of proinflammatory cytokines, particularly IL-6; AND INFLAMMATION IN HIV DISEASE It has become clear, as the sur-
elevated levels of high-sensitivity C-reactive protein, fibrinogen, vival of HIV-infected individuals has increased, that a number of
d-dimer, neopterin, β2-microglobulin, acid-labile interferon, soluble previously unrecognized medical complications are associated with
(s) IL-2 receptors (R), sTNFR, sCD27, and sCD40L; and autoimmune HIV disease—and that these complications relate to chronic immune
phenomena (see “Autoimmune Phenomena,” below). Even in the activation and inflammation (Table 197-4). These complications can
absence of direct infection of a target cell, HIV envelope proteins can appear even after patients have experienced years of adequate control
interact with cellular receptors (CD4 molecules and chemokine recep- of viral replication (plasma viremia below detectable levels) for several
tors) to deliver potent activation signals resulting in calcium flux, the years. Of particular note are endothelial cell dysfunction and its rela-
phosphorylation of certain proteins involved in signal transduction, tionship to cardiovascular disease. Other chronic conditions that have
co-localization of cytoplasmic proteins including those involved in cell been reported include bone fragility, certain cancers, diabetes, kidney
trafficking, immune dysfunction, and, under certain circumstances, and liver disease, and neurocognitive dysfunction, thus presenting an
apoptosis. From an immunologic standpoint, chronic exposure of the overall picture of accelerated aging.
immune system to a particular antigen over an extended period of time
may ultimately lead to an inability to sustain an adequate immune Autoimmune Phenomena Autoimmune phenomena are com-
response to the antigen in question. In many chronic viral infections, monly observed in HIV-infected individuals and they reflect, at least in
including HIV infection, persistent viremia is associated with “func- part, chronic immune activation and the dysregulation of B and T cells.
tional exhaustion” of virus-specific T cells, decreasing their capacity to Although these phenomena usually occur in the absence of autoimmune
proliferate and perform effector functions. It has been demonstrated disease, a wide spectrum of clinical manifestations that may be associ-
that this phenomenon of immune exhaustion may be mediated, at least ated with autoimmunity have been described (see “Immunologic and
in part, by the upregulation of inhibitory receptors on HIV-specific Rheumatologic Diseases,” below). Autoimmune phenomena include
T cells, such as PD-1 and Tim-3 that are shared by both CD4+ and CD8+ antibodies against autoantigens expressed on intact lymphocytes and
T cells, as well as CTLA-4 on CD4+ and 2B4 and CD106 on CD8+ T cells. other cells, or against proteins released from dying cells. Antiplatelet
Furthermore, the ability of the immune system to respond to a broad antibodies have some clinical relevance in that they may contribute to
Harrisons_20e_Part5_p0859-p1648.indd 1412 6/1/18 12:08 PM
the thrombocytopenia of HIV disease (see below). Antibodies to nuclear immune activation include IFN-γ, the CC-chemokine RANTES (CCL5), 1413
and cytoplasmic components of cells have been reported, as have anti- macrophage inflammatory protein (MIP)-1β (CCL4), and IL-18.
bodies to cardiolipin and phospholipids; CD4 molecules; CD43 mole- Several specific cytokines and soluble factors have been associated
cules; C1q-A; variable regions of the T cell receptor α, β, and γ chains; with HIV pathogenesis at various stages of disease, in various tissues or
Fas; denatured collagen; and IL-2. In addition, autoantibodies to a range organs, and in the regulation of HIV replication. Plasma levels of IP-10
of serum proteins, including albumin, immunoglobulin, and thyroglob- are predictive of disease progression, whereas the proinflammatory
ulin, have been reported. Molecular mimicry, either from opportunistic cytokine IL-6, soluble CD14 (sCD14), and coagulation marker d-dimer
pathogens or from HIV itself, also is a trigger or cofactor in autoimmu- are associated with increased risk of all-cause mortality in HIV-infected
nity. Antibodies against the HIV envelope proteins, especially gp41, individuals. In particular, IL-6, sCD14, and d-dimer are associated with
often cross-react with host proteins; the best known examples are increased risk of cardiovascular disease and other causes of death, even
antibodies directed against the membrane-proximal external region in individuals receiving cART. IL-18 has also been shown to play a role
(MPER) of gp41 that also react with phospholipids and cardiolipin. The in the development of the HIV-associated lipodystrophy syndrome,
phenomenon of polyreactive HIV-specific antibodies may be beneficial whereas increased levels of transforming growth factor (TGF)-β are
to the host (see “Immune Response to HIV,” below). associated with the induction of collagen deposition in lymph nodes
The increased occurrence and/or exacerbation of certain autoim- (see above). Elevated levels of TNF-α and IL-6 have been demonstrated
mune diseases have been reported in HIV infection; these diseases in plasma and cerebrospinal fluid (CSF), and increased expression of
include psoriasis, idiopathic thrombocytopenic purpura, Graves’ dis- TNF-α, IL-1β, IFN-γ, and IL-6 has been demonstrated in the lymph
ease, antiphospholipid syndrome, and primary biliary cirrhosis. The nodes of HIV-infected individuals. RANTES, MIP-1α (CCL3), and
majority of these manifestations were described prior to the advent MIP-1β (CCL4) (Chap. 342) inhibit infection by and spread of R5 HIV-1
of cART and have decreased in frequency since its widespread use. strains, while stromal cell–derived factor (SDF) 1 inhibits infection by and
However, with increasing availability of cART, an immune reconstitution spread of X4 strains. The mechanisms whereby the CC-chemokines
inflammatory syndrome (IRIS) has been increasingly observed in infected RANTES (CCL5), MIP-1α (CCL3), and MIP-1β (CCL4) inhibit infection
individuals, particularly those with low CD4+ T cell counts (see below). of R5 strains of HIV, or SDF-1 blocks X4 strains of HIV, involve block-
IRIS is an autoimmune-like phenomenon characterized by a paradoxical ing of the binding of the virus to its co-receptors, the CC-chemokine
deterioration of clinical condition, which is usually compartmentalized receptor CCR5 and the CXC-chemokine receptor CXCR4, respectively.
to a particular organ system, in individuals in whom cART has recently Other soluble factors that have not yet been fully characterized, such as
been initiated. It is associated with a decrease in viral load and at least soluble CD8 antiviral factor (CAF), also have been shown to suppress
partial recovery of immune competence, which is usually associated HIV replication, independent of co-receptor usage.
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
with increases in CD4+ T cell counts. The immunopathogenesis of this
syndrome is felt to be related to an increase in immune response against ■ LYMPHOCYTE TURNOVER IN HIV INFECTION
the presence of residual antigens that are usually microbial and is most The immune systems of patients with HIV infection are characterized
commonly seen with underlying Mycobacterium tuberculosis and crypto- by a profound increase in lymphocyte turnover that is immediately
coccosis. This syndrome is discussed in more detail below. reduced with effective cART. Studies utilizing in vivo or in vitro
labeling of lymphocytes in the S-phase of the cell cycle have demon-
■ CYTOKINES AND OTHER SOLUBLE FACTORS IN HIV strated a tight correlation between the degree of lymphocyte turnover
PATHOGENESIS and plasma levels of HIV RNA. This increase in turnover is seen in
The immune system is homeostatically regulated by a complex net- CD4+ and CD8+ T lymphocytes as well as B lymphocytes and can be
work of immunoregulatory cytokines, which are pleiotropic and observed in peripheral blood and lymphoid tissue. Mathematical mod-
redundant and operate in an autocrine and paracrine manner. They are els derived from these data suggest that one can view the lymphoid
expressed continuously, even during periods of apparent quiescence pool as consisting of dynamically distinct subpopulations of cells that
of the immune system. On perturbation of the immune system by are differentially affected by HIV infection. A major consequence of
antigenic challenge, the expression of cytokines increases to varying HIV infection appears to be a shift in cells from a more quiescent pool
degrees (Chap. 342). Cytokines that are important components of this to a pool with a higher turnover rate. It is likely that a consequence
immunoregulatory network are thought to play major roles in HIV of a higher rate of turnover is a higher rate of cell death. It has been
disease, during both the early and chronic phases of infection. A potent suggested that the more rapid decline in CD4+ compared with CD8+
proinflammatory “cytokine storm” is induced during the acute phase T cells may be linked to alterations in inflammatory and homeostatic
of HIV infection, likely a response by inflammatory cells to virus repli- cytokines that cause increased activation-induced death without
cating at very high levels. Cytokines that are induced during this early replenishment of CD4+ but not CD8+ T cells. (See Table 197-5 for addi-
phase include IFN-α, IL-15, and the CXC chemokine IP-10 (CXCL10), tional mechanisms of depletion.)
followed by IL-6, IL-12, and TNF-α, and a delayed peak of the anti-
inflammatory cytokine IL-10. Soluble factors of innate immunity also ■ THE ROLE OF VIRAL RECEPTORS AND
are induced shortly after infection, including neopterin and β-micro- CO-RECEPTORS IN HIV PATHOGENESIS
globulin. Several of these early-expressed cytokines and factors are CCR5 AND CXCR4 As mentioned above, HIV-1 utilizes two major
not downregulated following the early phase of HIV infection, as seen co-receptors along with CD4 to bind to, fuse with, and enter target
in other self-resolving viral infections, and persist during the chronic cells; these co-receptors are CCR5 and CXCR4, which are also receptors
phase of infection and contribute to maintaining high levels of immune for certain endogenous chemokines. Strains of HIV that utilize CCR5
activation. Among the cytokines and factors associated with early as a co-receptor are referred to as R5 viruses. Strains of HIV that utilize
innate immune responses, they are intended to contain viral replica- CXCR4 are referred to as X4 viruses. Many virus strains are dual tropic
tion, although paradoxically most are potent inducers of HIV expression/ in that they utilize both CCR5 and CXCR4; these are referred to as
replication because of their ability to induce immune activation that R5X4 viruses.
leads to enhanced viral production and an increase in readily available The natural chemokine ligands for the major HIV co-receptors can
target cells for HIV (activated CD4+ T cells). The induction of IFN-α, readily block entry of HIV. For example, the CC-chemokines RANTES
one of the first cytokines induced during primary HIV infection and an (CCL5), MIP-1α (CCL3), and MIP-1β (CCL4), which are the natural
important element of innate immune sensing, is thought to play a par- ligands for CCR5, block entry of R5 viruses, whereas SDF-1, the natural
ticularly important role in HIV pathogenesis by inducing a large num- ligand for CXCR4, blocks entry of X4 viruses. The mechanism of inhibi-
ber of IFN-associated genes that activate the immune system, alter the tion of viral entry is a steric inhibition of binding that is not dependent
homeostasis of CD4+ T cells, and influence the virus variants that are on signal transduction (Fig. 197-25).
selected during the HIV transmission bottleneck. Other cytokines that The transmitting virus is almost invariably an R5 virus that predom-
are elevated during the chronic phase of HIV infection and linked to inates during the early stages of HIV disease. In the absence of cART
Harrisons_20e_Part5_p0859-p1648.indd 1413 6/1/18 12:08 PM
1414 TABLE 197-5 Proposed Mechanisms of CD4+ T Cell Dysfunction and disease. However, the other half of infected individuals progress in
Depletion their disease while maintaining predominance of an R5 virus, and
DIRECT MECHANISMS INDIRECT MECHANISMS individuals infected with subtype C rarely switch from CCR5 tropism
Loss of plasma membrane integrity Aberrant intracellular signaling events
to CXCR4 tropism. The reason for this difference is unclear.
due to viral budding The basis for the tropism of different envelope glycoproteins for
Accumulation of unintegrated viral Autoimmunity either CCR5 or CXCR4 relates to the ability of the HIV envelope,
DNA including the third variable region (V3 loop) of gp120, to interact with
Activation of DNA-dependent protein these co-receptors. In this regard, binding of gp120 to CD4 induces
kinase during viral integration into a conformational change in gp120 that increases its affinity for the
host genome relevant co-receptor. Finally, R5 viruses are more efficient in infecting
Interference with cellular RNA Innocent bystander killing of viral monocytes/macrophages and microglial cells of the brain (see “Neuro-
processing antigen–coated cells pathogenesis in HIV Disease,” below).
Intracellular gp120-CD4 autofusion Apoptosis, pyroptosis (caspase-1
THE INTEGRIN `4a7 The integrin α4β7 is an accessory receptor for HIV.
events associated inflammation), autophagy
It is not essential for the binding and infection of a CD4+ T cell by
Syncytia formation Inhibition of lymphopoiesis from
reduced survival cytokines and HIV; however, it likely plays an important role in the transmission of
lymphoid tissue integrity HIV at mucosal surfaces such as the genital tract and gut and contrib-
Activation-induced cell death utes somewhat to the pathogenesis of HIV disease. The integrin α4β7,
Elimination of HIV-infected cells by
which is the gut homing receptor for peripheral T cells, binds in its
virus-specific immune responses activated form to a specific tripeptide in the V2 loop of gp120, resulting
in rapid activation of leukocyte function–associated antigen 1 (LFA-1),
the central integrin in the establishment of virologic synapses, which
or in cases of therapy failure, there is a transition to a predominantly facilitate efficient cell-to-cell spread of HIV. It has been demonstrated
X4 virus in approximately half of individuals infected with subtype B. that α4β7high CD4+ T cells are more susceptible to productive infection
The transition is often preceded by dual R5X4 strains, and detection than are α4β7low–neg CD4+ T cells because this cellular subset is enriched
of X4 variants is associated with a relatively rapid decline in CD4+ with metabolically active CD4+ T cells that are CCR5high. These cells are
T cell counts, increased HIV plasma viremia, and progression of present at the gut and genital tract mucosal surfaces. Importantly, it
has been demonstrated that the virus that is transmitted during sexual
exposure binds much more efficiently to α4β7 than does the virus that
diversifies from the transmitting virus over time by mutation, partic-
PART 5
ENV ularly involving the accumulation of glycogens on the surface of the
HIV
HIV envelope (see “Early Events in HIV Infection: Primary Infection
HIV and Initial Dissemination of Virus,” above).
Infectious Diseases
■ CELLULAR TARGETS OF HIV
CD4+ T lymphocytes and to a lesser extent CD4+ cells of the myeloid
CD4
lineage are the principal targets of HIV and are the only cells that can
CD4+
be productively infected with HIV. Circulating DCs have been reported
Target Cell
to express low levels of CD4, although high expression of the restriction
factor SAMHD1 in myeloid (mDC) and plasmacytoid (pDC) DCs limits
HIV replication in these cells by depleting intracellular pools of dNTPs
and directly degrading viral RNA. Epidermal Langerhans cells express
SDF-1
CD4 and have been infected by HIV in vivo, although, they too restrict
replication by high expression of the host restriction factor, langerin. As
CXCR4
has been shown in vivo for DCs, FDCs, and B cells, Langerhans cells are
A more likely to bind and transfer virus to activated CD4+ T cells than to
be productively infected themselves.
Of potential clinical relevance is the demonstration that thymic
ENV HIV precursor cells, which were assumed to be negative for CD3, CD4,
and CD8 molecules, actually do express low levels of CD4 and can be
HIV infected with HIV in vitro. In addition, human thymic epithelial cells
transplanted into an immunodeficient mouse can be infected with HIV
by direct inoculation of virus into the thymus. Since these cells may
play a role in the normal regeneration of CD4+ T cells, it is possible
CD4 that their infection and depletion contribute, at least in part, to the
CD4+ impaired ability of the CD4+ T cell pool to completely reconstitute
Target Cell itself in certain infected individuals in whom cART has suppressed
plasma viremia to below the level of detection (see below). In addition,
CD34+ monocyte precursor cells have been shown to be infected in
vivo in patients with advanced HIV disease. It is likely that these cells
CC-Chemokine
express low levels of CD4, and therefore it is not essential to invoke
(RANTES,
CCR5 CD4-independent mechanisms to explain the infection. The clinical
MIP-1 α,
relevance of this finding is unclear.
B MIP-1 β)
FIGURE 197-25 Model for the role of co-receptors CXCR4 and CCR5 in the ■ QUALITATIVE AND QUANTITATIVE ABNORMALITIES
efficient binding and entry of X4 (A) and R5 (B) strains of HIV-1, respectively, OF MONONUCLEAR CELLS
into CD4+ target cells. Blocking of this initial event in the virus life cycle can be
accomplished by inhibition of binding to the co-receptor by the normal ligand for CD4+ T Cells The primary immunopathogenic lesion in HIV
the receptor in question. The ligand for CXCR4 is stromal cell–derived factor (SDF-1); infection involves CD4+ T cells, and the range of CD4+ T cell abnor-
the ligands for CCR5 are RANTES, MIP-1α, and MIP-1β. malities in advanced HIV infection is broad. The defects are both
Harrisons_20e_Part5_p0859-p1648.indd 1414 6/1/18 12:08 PM
quantitative and qualitative and ultimately impact virtually every limb can recognize these bound molecules and potentially collaborate in the 1415
of the immune system, indicating the critical dependence of the integ- elimination of the cells by ADCC. HIV envelope glycoproteins gp120
rity of the immune system on the inducer/helper function of CD4+ T and gp160 manifest high-affinity binding to the CD4 molecule as well
cells. In advanced HIV disease, most of the observed immune defects as to various chemokine receptors. Intracellular signals transduced by
can ultimately be explained by the quantitative depletion of CD4+ T gp120 through both CD4 and CCR5/CXCR4 have been associated with
cells. However, T cell dysfunction can be demonstrated in patients a number of immunopathogenic processes including anergy, apopto-
early in the course of infection, even when the CD4+ T cell count is sis, and abnormalities of cell trafficking. The molecular mechanisms
in the low-normal range. The degree and spectrum of dysfunctions responsible for these abnormalities include dysregulation of the T cell
increase as the disease progresses, reflecting the range of CD4+ T cell receptor–phosphoinositide pathway, p56lck activation, phosphoryla-
functional heterogeneity, especially in lymphoid tissues. One of the tion of focal adhesion kinase, activation of the MAP kinase and ras sig-
first sites of intense HIV replication is in the GALT where CD4+ TH17 naling pathways, and downregulation of the co-stimulatory molecules
cells reside; they are important for host defense against extracellular CD40 ligand and CD80.
pathogens in the intestinal mucosa and help maintain the integrity of The inexorable decline in CD4+ T cell counts that occurs in most
the gut epithelium. In HIV infection, they are depleted by direct and HIV-infected individuals may result in part from the inability of the
indirect effects of viral replication and cause loss of gut homeostasis immune system to regenerate over an extended period of time the
and integrity, as well as a shift toward a TH1 phenotype. Studies have rapidly turning over CD4+ T cell pool efficiently enough to compensate
shown that even after many years of cART, normalization of the CD4+ for both HIV-mediated and naturally occurring attrition of cells. In this
T cells in the GALT remains incomplete. In lymph nodes, HIV perturbs regard, the degree and duration of decline of CD4+ T cells at the time
another important subset of the CD4+ helper T lineage, namely TFH of initiation of therapy is an important predictor of the restoration of
cells (see “Lymphoid Organs and HIV Pathogenesis,” above). TFH these cells. A person who maintains a very low CD4+ T cell count for a
cells, which are derived either directly from naïve CD4+ T cells or from considerable period of time before the initiation of cART almost invari-
other TH precursors, migrate into B follicles during germinal center ably has an incomplete reconstitution of such cells. At least two major
reactions and provide help to antigen-specific B cells through cell–cell mechanisms may contribute to the failure of the CD4+ T cell pool to
interactions and secretion of cytokines to which B cells respond, the reconstitute itself adequately over the course of HIV infection. The first
most important of which is IL-21. As with TH17 cells, TFH cells are is the destruction of lymphoid precursor cells, including thymic and
highly susceptible to HIV infection. However, in contrast to TH17 and bone marrow progenitor cells; the other is the gradual disruption of the
most other CD4+ T cell subsets, the number of TFH cells is increased lymphoid tissue architecture and microenvironment, which is essential
in lymph nodes of HIV-infected individuals, especially those who are for efficient regeneration of immunocompetent cells. Finally, during the
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
viremic. It is unclear whether this increase is helpful to responding B advanced stages of CD4+ T lymphopenia, there are increased serum
cells, although the likely outcome is that the increase in numbers is det- levels of the homeostatic cytokine IL-7. It was initially felt that this
rimental to the quality of the humoral immune response against HIV elevation was a homeostatic response to the lymphopenia; however,
(see “Immune Response to HIV,” below). In addition, defects of central recent findings suggest that the increase in serum IL-7 was a result of
memory cells are a critical component of HIV immunopathogenesis. reduced utilization of the cytokine related to the loss of cells expressing
The progressive loss of antigen-specific CD4+ T cells has important the IL-7 receptor, CD127, which serves as a normal physiologic regula-
implications for the control of HIV infection. In this regard, there is tor of IL-7 production.
a correlation between the maintenance of HIV-specific CD4+ T cell
proliferative responses and improved control of infection. Essentially CD8+ T Cells A relative CD8+ T lymphocytosis is generally asso-
every T cell function has been reported to be abnormal at some stage of ciated with high levels of HIV plasma viremia and likely reflects an
HIV infection. Loss of polyfunctional HIV-specific CD4+ T cells, espe- immune response to the virus as well as dysregulated homeostasis
cially those that produce IL-2, occurs early in disease, whereas IFN- associated with generalized immune activation. During the late stages
producing CD4+ T cells are maintained longer and do not correlate of HIV infection, there may be a significant reduction in the num-
with control of HIV viremia. Other abnormalities include impaired bers of CD8+ T cells despite the presence of high levels of viremia.
expression of IL-2 receptors, defective IL-2 production, reduced expres- HIV-specific CD8+ CTLs have been demonstrated in HIV-infected
sion of the IL-7 receptor (CD127), and a decreased proportion of CD4+ individuals early in the course of disease, and their emergence often
T cells that express CD28, a major co-stimulatory molecule necessary coincides with a decrease in plasma viremia—an observation that is a
for the normal activation of T cells, which is also depleted as a result factor in the proposal that virus-specific CTLs can control HIV disease
of aging. Cells lacking expression of CD28 do not respond normally for a finite period of time in a certain percentage of infected individu-
to activation signals and may express markers of terminal activation als. However, emergence of HIV escape mutants that ultimately evade
including HLA-DR, CD38, and CD45RO. As mentioned above (“The these HIV-specific CD8+ T cells has been described in the majority of
Role of Immune Activation and Inflammation in HIV Pathogenesis”), HIV-infected individuals who are not receiving cART. In addition, as
a subset of CD4+ T cells referred to as T regulatory cells, or T-regs, may the disease progresses, the functional capability of these cells gradually
be involved in damping aberrant immune activation that propagates decreases, at least in part due to the persistent nature of HIV infection
HIV replication. The presence of these T-reg cells correlates with lower that causes functional exhaustion via the upregulation of inhibitory
viral loads and higher CD4+/CD8+ T cell ratios. A loss of this T-reg receptors such as PD-1 and TIGIT on HIV-specific CD8+ T cells (see
capability with advanced disease may be detrimental to the control of “The Role of Immune Activation and Inflammation in HIV Pathogenesis,”
virus replication. above). As chronic immune activation persists, there are also systemic
It is difficult to explain completely the profound immunodeficiency effects on CD8+ T cells, such that as a population they assume an
noted in HIV-infected individuals solely on the basis of direct infection abnormal phenotype characterized by expression of activation markers
and quantitative depletion of CD4+ T cells. This is particularly appar- such as HLA-DR and CD38 with an absence of expression of the IL-2
ent during the early stages of HIV disease, when CD4+ T cell numbers receptor (CD25) and a reduced expression of the IL-7 receptor (CD127).
may be only marginally decreased. In this regard, it is likely that CD4+ In addition, CD8+ T cells lacking CD28 expression are increased in HIV
T cell dysfunction results from a combination of depletion of cells due disease, reflecting a skewed expansion of a less differentiated CD8+
to direct infection of the cell and a number of virus-related but indirect T cell subset. This skewing of subsets is also associated with dimin-
effects on the cell such as elimination of “innocent bystander cells” ished polyfunctionality, a qualitative difference that distinguishes elite
(Table 197-5). Several of these effects have been demonstrated ex vivo controllers from progressors. Elite controllers can also be distinguished
and/or by the analysis of cells isolated from the peripheral blood. Solu- from progressors by the maintenance in the former of a high prolifera-
ble viral proteins, particularly gp120, can bind with high affinity to the tive capacity of their HIV-specific CD8+ T cells coupled to increases in
CD4 molecules on uninfected T cells and monocytes; in addition, virus perforin expression and elimination of infected targets, characteristics
and/or viral proteins can bind to DCs or FDCs. HIV-specific antibody that are markedly diminished in advanced HIV disease. It has been
Harrisons_20e_Part5_p0859-p1648.indd 1415 6/1/18 12:08 PM
1416 reported that the phenotype of CD8+ T cells in HIV-infected indi- a role in the increased morbidity and mortality of HIV-infected children.
viduals may be of prognostic significance. Those individuals whose The absolute number of circulating B cells also may be depressed in HIV
CD8+ T cells developed a phenotype of HLA-DR+/CD38– following infection; this phenomenon likely reflects increased activation-induced
seroconversion had stabilization of their CD4+ T cell counts, whereas apoptosis as well as a redistribution of cells out of the circulation and
those whose CD8+ T cells developed a phenotype of HLA-DR+/ into the lymphoid tissue—phenomena that are associated with ongoing
CD38+ had a more aggressive course and a poorer prognosis. In addi- viral replication.
tion to the defects in HIV-specific CD8+ CTLs, functional defects in
other MHC-restricted CTLs, such as those directed against influenza Monocytes/Macrophages Circulating monocytes are generally
and CMV, have been demonstrated. CD8+ T cells secrete a variety of normal in number in HIV-infected individuals; however, there is evi-
soluble factors that inhibit HIV replication, including the CC-chemokines dence of increased activation within this lineage. The increased level of
RANTES (CCL5), MIP-1α (CCL3), and MIP-1β (CCL4) as well as poten- sCD14 and other biomarkers (see above) reported in HIV-infected indi-
tially a number of as yet unidentified factors. The presence of high lev- viduals is an indirect marker of monocyte activation in vivo. A number
els of HIV viremia in vivo as well as exposure of CD8+ T cells in vitro of other abnormalities of circulating monocytes have been reported in
to HIV envelope, both of which are associated with aberrant immune HIV-infected individuals, many of which may be related directly or indi-
activation, have been shown to be associated with a variety of cellular rectly to aberrant in vivo immune activation. In this regard, increased
functional abnormalities. Furthermore, since the integrity of CD8+ levels of lipopolysaccharide (LPS) are found in the sera of HIV-infected
T cell function depends in part on adequate inductive signals from individuals due, at least in part, to translocation across the gut mucosal
CD4+ T cells, the defect in CD8+ CTLs is likely compounded by the barrier (see above). LPS is a highly inflammatory bacterial product that
quantitative loss and qualitative dysfunction of CD4+ T cells. preferentially binds to macrophages through CD14 and Toll-like recep-
tors, resulting in cellular activation. Functional abnormalities of mono-
B Cells The predominant defect in B cells from HIV-infected indi- cyte/macrophages in HIV disease include decreased secretion of IL-1
viduals is one of aberrant cellular activation, which is reflected by and IL-12; increased secretion of cytokines such as IL-10 and IL-18 and
increased propensity to terminal differentiation and immunoglobulin markers of coagulation such as d-dimer; defects in antigen presentation
secretion, as well as increased expression of markers of activation and and induction of T cell responses due to decreased MHC class II expres-
exhaustion. As a result of activation and differentiation in vivo, B cells sion; and abnormalities of Fc receptor function, C3 receptor–mediated
from HIV viremic patients manifest a decreased capacity to mount clearance, oxidative burst responses, and certain cytotoxic functions
a proliferative response to ligation of the B cell antigen receptor and such as ADCC, possibly related to low levels of expression of Fc and
other B cell stimuli in vitro. B cells from HIV-infected individuals man- complement receptors. Monocytes express the CD4 molecule and several
ifest enhanced spontaneous secretion of immunoglobulins in vitro, a co-receptors for HIV on their surface, and thus are potential targets of
HIV infection. However, in vivo infection of circulating monocytes is
PART 5
process that reflects their highly differentiated state in vivo. There is
also an increased incidence of EBV-related B cell lymphomas in HIV- difficult to demonstrate, although infection of tissue macrophages and
infected individuals that are likely due to combined effects of defective macrophage-lineage cells in the brain (infiltrating macrophages or res-
T cell immune surveillance and increased B cell turnover that increases ident microglial cells) and lung (pulmonary alveolar macrophages) can
the risk of oncogenesis. Untransformed B cells cannot be infected with be demonstrated easily. Tissue macrophages are an important source of
Infectious Diseases
HIV, although HIV or its products can activate B cells directly. B cells HIV during the inflammatory response associated with opportunistic
from patients with high levels of viremia bind virions to their surface infections and can serve as persistent reservoirs of HIV infection, thus
via the CD21 complement receptor. It is likely that in vivo activation representing an obstacle to the eradication of HIV by antiretroviral
of B cells by replication-competent or defective virus as well as viral drugs. Infection of monocyte precursors in the bone marrow may
products during the viremic state accounts at least in part for their acti- directly or indirectly be responsible for certain of the hematologic
vated phenotype. B cell subpopulations from HIV-infected individuals abnormalities in HIV-infected individuals. However, as with DCs,
undergo a number of changes over the course of HIV disease, including monocytes and macrophages express high levels of host restriction fac-
the attrition of resting memory B cells and replacement with several tors that likely help explain the low contribution of myeloid cells to the
aberrant memory and differentiated B cell subpopulations that collec- overall viral burden in HIV-infected individuals.
tively express reduced levels of CD21 and either increased expression Dendritic and Langerhans Cells DCs and Langerhans cells
of activation markers or inhibitory receptors associated with functional are not productively infected with HIV, but they are thought to play an
exhaustion. The more activated and differentiated B cells are also important role in the initiation of HIV infection by virtue of the ability
responsible for increased secretion of immunoglobulins and increased of HIV to bind to cell-surface C-type lectin receptors, particularly DC-
susceptibility to Fas-mediated apoptosis. In more advanced disease, SIGN (see above) and langerin. However, while langerin provides a
there is also the appearance of immature B cells associated with CD4+ host barrier for replication by trafficking HIV to acidic compartments
T cell lymphopenia. Despite increased frequencies of germinal center for degradation, DC-SIGN retains HIV in early endosomal com-
B cells and CD4+ TFH cells, both of which are required for effective partments. This allows efficient presentation of intact virus to CD4+
humoral immunity, cognate B cell–CD4+ T cell interactions in lym- T cell targets that become infected; complexes of infected CD4+ T cells
phoid tissues are perturbed in HIV-infected individuals, especially and DCs provide an optimal microenvironment for virus replication.
those with persistent viremia. In vivo, the aberrant activated state of B Furthermore, pDCs secrete large amounts of IFN-α in response to
cells manifests itself by hypergammaglobulinemia and by the presence viral infections and as such play an important role in innate sensing
of circulating immune complexes and autoantibodies. HIV-infected of HIV during early phase of infection. The numbers of circulating
individuals respond poorly to primary and secondary immunizations pDCs are decreased in HIV infection through mechanisms that remain
with protein and polysaccharide antigens. Using immunization with unclear, although several studies have shown increased lymphoid
influenza vaccine, it has been demonstrated that there is a memory tissue recruitment of DCs associated with lymphoid hyperplasia and
B cell defect in HIV-infected individuals, particularly those with high inflammation. The mDCs or conventional DCs are also involved in
levels of HIV viremia. There is also evidence that responses to HIV the initiation of adaptive immunity in draining lymph nodes by pre-
and non-HIV antigens in infected individuals, especially those who senting antigen to T cells and B cells, as well as by secreting cytokines
remain viremic, are enriched in abnormal subsets of B cells that either such as IL-12, IL-15, and IL-18 that activate other immune cells. There
are highly prone to apoptosis or show signs of functional exhaustion. are also indications that the relatively low infectibility of DCs may be
Taken together, these B cell defects are likely responsible at least in part associated with the expression of host restriction factors, including
for the inadequate humoral response to HIV as well as to decreased APOBEC3G and SAMHD1 (see above).
response to vaccinations and the increase in certain bacterial infections
seen in advanced HIV disease in adults. In addition, they likely contribute Natural Killer Cells The role of NK cells is to provide immu-
to the inadequacy of host defenses against bacterial infections that play nosurveillance against virus-infected cells, certain tumor cells, and
Harrisons_20e_Part5_p0859-p1648.indd 1416 6/1/18 12:08 PM
allogeneic cells (Chap. 342). There are no convincing data that HIV the CCR5 ∆32 allele. Depending on the geographic region in Europe, 1417
productively infects NK cells in vivo; however, functional abnormal- up to 18% of individuals are heterozygous for the CCR5 ∆32 allele. The
ities in NK cells have been observed throughout the course of HIV CCR5 ∆32 allele is rare in other populations. The evolutionary pressure
disease, and the severity of these abnormalities increases as disease that resulted in the emergence of the CCR5 ∆32 allele in the European
progresses. NK cells are part of the innate immune system and act by population remains unknown and has been speculated to be secondary
direct killing of infected cells and secretion of antiviral cytokines and to an ancestral pandemic, such as the plague.
chemokines. In early HIV infection there is an increase in the activation Subsequent studies identified single nucleotide polymorphisms
of NK cells, and the capacity to secrete IFN-γ is maintained, although (SNPs) in the promoter (regulatory) region of CCR5 that influence
they manifest reduced cytotoxic function. During chronic HIV infec- gene expression levels. Alleles bearing specific cassettes of linked
tion, both NK cell cytotoxicity and cytokine secretion become impaired. polymorphisms (haplotypes) were identified and designated as human
Given that HIV infection of target cells downregulates HLA-A and B, haplogroups A to G*2 (HHA to HHG*2) (Fig. 197-26). The CCR5 ∆32
but not HLA-C and D molecules, this may explain in part the relative polymorphism is found on the HHG*2 haplotype. CCR5 haplotypes
inability of NK cells to kill HIV-infected target cells. However, the A–D vs. E–G*2 differ by bearing GT versus AC at polymorphic sites
NK cell impairments, especially in patients with high levels of virus rs1799987 and rs1799988 (Fig. 197-26). CCR5-HHA haplotype rep-
replication, are associated with an expansion of an “anergic” CD56–/ resents the ancestral haplotype (found in chimpanzees) and is asso-
CD16+ NK cell subset. This abnormal subset of NK cells manifests ciated with lower CCR5 gene expression, whereas the CCR5-HHE
an increased expression of inhibitory NK cell receptors (iNKRs) and haplotype is associated with higher CCR5 expression. Methylation of
a substantial decrease in expression of natural cytotoxicity receptors DNA is a common epigenetic signaling mechanism that cells use to
(NCRs) and shows a markedly impaired lytic activity. The overrepre- lock genes in the “off” position, and polymorphisms in CCR5 haplo-
sentation of this abnormal subset of NK cells may explain in part the types may mediate their effects by influencing DNA methylation levels
observed defects in NK cell function in HIV-infected individuals and in the CCR5 locus. The CCR5-HHE and CCR5-HHA haplotypes are
likely begins to occur during primary infection. The relative expression more sensitive and resistant, respectively, to T cell activation–induced
of iNKRs and NCRs—as well as their ligands, which include HLA class I demethylation of the CCR5 locus.
molecules—has an impact on the antiviral functions associated with In worldwide populations, HHE and HHC are more prevalent,
NK cells, including direct killing and ADCC. Polymorphisms in iNKR whereas the ancestral HHA haplotype is more common in persons
and NCR alleles have been linked to HIV-1 disease outcomes. NK cells of African ancestry. The associations of CCR5 haplotypes with HIV
also serve as important sources of HIV-inhibitory CC-chemokines. NK acquisition and/or HIV disease course are largely consistent with their
cells isolated from HIV-infected individuals constitutively produce effects on CCR5 gene expression. For example, homozygosity for the
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
high levels of MIP-1α (CCL3), MIP-1β (CCL4), and RANTES (CCL5), CCR5-HHE haplotype is associated with an increased risk of acquiring
although the impact of these chemokines on HIV replication in vivo HIV, progressing rapidly to AIDS, and reduced immune recovery while
is unclear. Finally, NK cell–DC interactions are important for normal the patient is on ART. The HHA haplotype is associated with slower
immune function. NK cells and DCs reciprocally modulate each other’s disease progression in African populations and has been speculated
activation and maturation. These interactions are markedly impaired in to be a basis for why chimpanzees (who all carry the ancestral CCR5
HIV-infected individuals with high levels of plasma viremia. HHA haplotype) naturally infected with simian immunodeficiency
virus (SIV) may resist disease progression. The pairing of the HHC
■ GENETIC FACTORS IN HIV-1 AND AIDS and CCR5 ∆32-bearing HHG*2 haplotypes (HHC/HHG*2 genotype) is
PATHOGENESIS associated with a lower risk of acquiring HIV infection and slower rate
Candidate gene approaches and genome-wide association studies of HIV disease progression, whereas the pairing of the HHE haplotype
(GWAS) have identified polymorphisms in host genes that contribute with the HHG*2 haplotype is associated with the opposite effects. The
to inter-individual variation in (1) the risk of acquiring HIV, (2) the CCR2-64I-bearing HHF*2 haplotype is associated with a slower HIV
steady-state levels of HIV that are established soon after infection (viro- disease course.
logic set point), (3) the rate at which untreated HIV-infected patients Consistent with these genetic associations, polymorphisms in genes
progress to AIDS as well as risk of developing specific AIDS-defining encoding ligands for CCR5 have also been demonstrated to associate
illnesses (e.g., renal and neurologic diseases), and (4) the level of with variable HIV susceptibility and disease progression rates. Exam-
immune reconstitution (e.g., CD4+ counts) achieved after initiation of ples include copy number variations of CCL3L1 and SNPs in CCL5. The
virally suppressive ART. The key polymorphisms that influence these sum of these studies established a pivotal role of CCR5 and its ligands
four traits are summarized in Table 197-6, and their identification has in HIV-AIDS pathogenesis and, potentially, immune recovery.
greatly advanced our understanding of the genes that influence HIV- The discovery that the CCR5 ∆32/∆32 genotype is associated with
AIDS pathogenesis. Of particular interest are polymorphisms in two strong resistance to HIV infection, and that uninfected Caucasians
chromosomal regions, as they are associated with consistent effects bearing this genotype did not appear to have impaired immunity, led
on HIV acquisition, virologic set point, and/or rates of HIV disease to the development of two kinds of novel therapies. First, it spurred
progression: the region in chromosome 3 that includes the gene that the development of a new class of therapies approved by the U.S. Food
encodes the HIV co-receptor CC chemokine receptor 5 (CCR5) and the and Drug Administration (FDA), i.e., entry inhibitors (e.g., maraviroc)
major histocompatibility locus (MHC) in chromosome 6 (Fig. 197-26). that block the interaction of CCR5 with the HIV envelope. Second, it
led to the evaluation of novel experimental cellular therapies. An
GENETICS OF CCR5: FROM BENCH TO BEDSIDE While the discovery of HIV-infected patient with acute myelogenous leukemia was given an
CCR5 as a major co-receptor for cell entry of HIV-1 was established by allogeneic stem cell transplantation from an HLA-compatible person
in vitro studies, genetic association studies were required to establish whose cells lacked expression of CCR5 due to the ∆32/∆32 genotype.
its seminal role in HIV pathogenesis. Initial in vitro studies revealed There has been no evidence of HIV-1 infection in the patient who
that a 32-bp deletion (∆32) in the coding region of CCR5 contributes underwent the transplant thus far (~10 years). This observation pro-
to resistance to CCR5-using R5 strains of HIV. The CCR5 ∆32 allele vided a “proof of concept” for an HIV cure and led to the development
encodes a truncated protein that is not expressed on the cell surface. of additional novel cellular therapies involving autologous transplan-
Congruently, genotype-phenotype association studies in large cohorts tation of CD4+ T cells in which the CCR5 gene is inactivated ex vivo
demonstrated that individuals homozygous for the CCR5 ∆32 allele using new gene editing procedures.
(∆32/∆32) lack CCR5 surface expression and are highly resistant to
acquiring HIV infection; heterozygosity for the CCR5 ∆32 allele is asso- DISCOVERY OF HLA CLASS I ALLELES THAT ASSOCIATE WITH VIROLOGIC
ciated with a lower risk of acquiring HIV. CONTROL OF HIV INFECTION There is a strong association between
The distribution of the CCR5 ∆32 allele is population specific. Approx- variations within the HLA-B gene with protective (e.g., HLA-B∗57 and
imately 1% of individuals of European ancestry are homozygous for B*27 alleles) or detrimental (e.g., HLA-B∗35 allele) outcomes during
Harrisons_20e_Part5_p0859-p1648.indd 1417 6/1/18 12:08 PM
1418 TABLE 197-6 Host Genetic Factors That Influence Risk of HIV-1 Acquisition and Rates of HIV-1 Disease Progression
GENEa GENETIC VARIATION MECHANISMSb GENETIC EFFECT ON HIV-AIDSc
Genes in MHC Locus
HLA-B B*27 and B*57 Presentation of specific HIV antigens Slower progression to AIDS; lower viral load
B*35 Restriction of specific HIV peptide presentation Faster progression to AIDS; higher viral load
HLA-Bw4 Providing ligands for activating KIR Slower progression to AIDS
HLA class I allele Homozygosity of HLA-class I Reduced repertoire for epitope recognition Faster progression to AIDS; increased risk of
alleles mother-to-child transmission
Shared donor-recipient HLA Preadaptation of HIV strains Faster disease progression to AIDS
alleles
Rare HLA alleles Limited adaptation of HIV strains; less frequent Protection against HIV infection
escape mutants
HLA class II allele HLA-DRB1 alleles Influencing protein specificity of CD4+ T cell HLA-DRB1*15:02—lower viral load
responses to HIV Gag and Nef proteins HLA-DRB1*03:01—higher viral load
HLA extended haplotype A1-B8-DR3-DQ2 (AH 8.1) Increased proinflammatory responses; higher Faster progression to AIDS
TNF-α production
HLA-C 35 kb upstream, rs9264942-C Increased expression of HLA-C Decreased viral load set point
HCP5 rs2395029-G Linkage disequilibrium with HLA-B*57:01 Lower viral load
MICA Noncoding SNP near MICA, May affect HLA class I peptide presentation— Enriched in HIV-1 controllers
rs4418214-T linkage with protective HLA-B alleles
PSORS1C3 rs3131018-A May affect HLA class I peptide presentation Enriched in HIV-1 controllers
ZNRD1 rs9261174-C Possible interference in processing of HIV Slower disease progression to AIDS
transcripts; influencing ZNRD1 expression;
linkage disequilibrium with HLA-A10
Chemokine Receptors
CCR5 32-bp deletion in the ORF (∆32), Truncated CCR5 protein ∆32/∆32: resistance to acquiring HIV
rs333 infection
∆32/wild type: delays AIDS onset; improves
PART 5
immune reconstitution during ART
Promoter SNPs, haplotypes (HHA Altered CCR5 expression, e.g., HHE haplotype HHE/HHE: increased HIV/AIDS susceptibility
to HHG*2) correlates with high CCR5 expression
CCR2 SNP in ORF (64 V→I), Possibly due to linkage with polymorphism in 64I: delayed AIDS onset
rs1799864 CCR5 promoter
Infectious Diseases
CCRL2 Coding SNP (167 Y→F) Possibly due to linkage with CCR5 haplotype 167F is associated with accelerated
rs3204849 progression to AIDS and more rapid
development of PCP
rs1015164 Possibly due to linkage with CCR5 haplotype Associated with high viral load set point
CXCR6 rs2234358 G→T in the 3’UTR Trafficking of effector T cells and activation of NK Prevalence of rs2234358-T was lower in long-
T cells; minor HIV co-receptor term nonprogressors and viremic controllers
CX3CR1 SNPs in ORF (249 V→I, 280M reduces receptor expression and binding of 249I and 280M associated with faster
rs3732379; and 280 T→M, fractalkine, the CX3CR1 ligand AIDS onset in some Caucasian cohorts;
rs3732378) inconsistent effects detected in other cohorts
DARC African-specific promoter SNP –46C/C associates with low neutrophil counts; –46C/C: increased risk of acquiring HIV but
(–46T→C), rs2814778 influences circulating chemokine levels; alters HIV slower HIV disease progression; Duffy-null-
binding to RBCs and transinfection of HIV-1 associated low neutrophil trait associated
with increased HIV risk in persons of African
descent
Chemokines
CCL3L, CCL4L Gene copy number of CCL3L and High numbers of CCL3L and CCL4L gene- Gene copy number lower than population
CCL4L containing segmental duplications correlate with median associated with increased HIV/
high CCL3L and CCL4L levels AIDS susceptibility and reduced immune
reconstitution during ART
CCL5 Promoter SNPs Altered gene expression Altered HIV-AIDS susceptibility
CCL2 Promoter SNP (–2578 T→G), –2578G allele: increased CCL2 expression and –2578G/G associated with increased risk of
rs1024611 monocyte recruitment developing HIV-1-associated dementia and
rapid AIDS onset
Cytokines
IL-6 Promoter SNP (–174 G→C), –174G/G associated with increased IL-6 and CRP –174G/G associated with high risk of KS
rs1800795 levels development and variable recovery of CD4
cells during ART
IL-7RA Coding SNP (244 T→I), 244 I/I associated with increased signal 244 I/I associated with faster CD4+ T cell
rs6897932 transduction and proliferation in response to IL-7 recovery after ART initiation
IL-10 Promoter SNP (–592 C→A), –592A results in decreased IL-10 levels –592A associated with increased HIV-AIDS
rs1800872 susceptibility
(Continued)
Harrisons_20e_Part5_p0859-p1648.indd 1418 6/1/18 12:08 PM
TABLE 197-6 Host Genetic Factors That Influence Risk of HIV-1 Acquisition and Rates of HIV-1 Disease Progression (Continued) 1419
GENE a
GENETIC VARIATION MECHANISMS b
GENETIC EFFECT ON HIV-AIDS c
Innate Immunity Genes
MBL Coding alleles (O) Low plasma concentration and structural variation Slow progression to AIDS in heterozygous
of MBL protein subjects (A/O)
X allele (promoter SNP –221) Decreased levels of MBL protein Faster progression to AIDS in homozygous X/X
subjects
Apobec-3G ORF SNP (186 H→R), Reduced anti-HIV-1 activity 186R associated with rapid AIDS onset in
rs8177832 African Americans
Apobec-3F Haplotype tagged by ORF SNP 231V variant may influence Vif-mediated 231V associated with lower VL, slower
(231 I→V), rs2076101 Apobec-3F degradation progression to AIDS and delayed progression
to PCP
TLR7 ORF SNP (Gln11Leu), rs179008 Decreased expression of TLR7 leading to lack of Leu-containing protein associated with higher
recognition of HIV-infected cells viral load and faster progression to AIDS
PARD3B rs11884476 (C→G), near exon Direct interaction with HIV, signaling through rs11884476-G associated with slower
20 SMAD family of proteins progression to AIDS
IFNL4 Frameshift mutation (TT→∆G), Functional polymorphism in IFNL4 gene, possibly rs368234815-∆G associated with higher
rs368234815 in linkage with IL28B variant and regulates IL-28B prevalence of AIDS-defining illnesses and
levels potentially increased HIV-1 infection risk
Others
ApoE E4 allele E4 enhances HIV cell entry in vitro ApoE4/E4 associated with rapid AIDS onset
and dementia
ApoL1/ MYH9 Several risk haplotypes, Unknown Increased risk for HIV-associated nephropathy
including G1
RYR3 ORF SNP (A →G), rs2229116 Unknown, potential impact on calcium signaling rs2229116-G associated with subclinical
and homeostasis atherosclerosis
PROX1 rs17762192-G, 36kb upstream Unknown, presumably due to its impact on PROX1 rs17762192-G: reduced rate of disease
of PROX1 expression, which is a negative regulator of IFN-γ progression
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
Gene–Gene Interaction
KIR+HLA KIR3DS1 + HLA-Bw4-80Ile Altered NK cell activity required to eliminate HIV- KIR3DS1 associated with HLA-Bw4-80Ile; +:
infected cells delayed AIDS onset
HLA-C1 + KIR2DL3 Reduction of inhibitory KIR likely results in HLA-C1+/KIR2DL3+: better immune recovery
increased immune activation; impaired killing after viral load suppression on ART
of latently infected cells; and a higher proviral
burden
LILRB2+HLA LILRB2 + HLA class I Regulation of dendritic cells by LILRB2-HLA Control of HIV-1
engagement
CCL3L1+ CCR5 Low CCL3L1 gene copies + Low CCL3L1 and high CCR5 expression Increased HIV/AIDS susceptibility and
detrimental CCR5 genotypes reduced immune reconstitution during ART
a
Representative genes and polymorphisms and bpossible mechanisms are listed. cSome of the associations are population specific and may display cohort-specific
effects.
Note: Apobec, apolipoprotein B mRNA editing enzyme, catalytic polypeptide-like; ApoE, apolipoprotein E; ART, antiretroviral therapy; CCL, CC ligand; CCL3L, CCL3-
like; CCR5, CC chemokine receptor 5; CCRL2: CC chemokine receptor like 2; CRP, C-reactive protein; CXCR6, chemokine (C-X-C motif) receptor 6; DARC, Duffy
antigen receptor for chemokines; HCP5, HLA class I histocompatibility antigen protein P5; HHE, human haplogroup E; HLA, human leukocyte antigen; IFN, interferon;
IFNL4, interferon λ4 gene; IL, interleukin; IL-7RA, interleukin 7 receptor-α; KIR, killer cell immunoglobulin-like receptors; KS, Kaposi’s sarcoma; LILRB2, leukocyte
immunoglobulin-like receptor B2; MBL, mannose-binding lectin; MHC, major histocompatibility complex; MICA, MHC class I polypeptide-related sequence A; NK, natural
killer; ORF, open reading frame; PARD3B, par-3 family cell polarity regulator beta; PCP, Pneumocystis pneumonia; PROX1, prospero homeobox 1; PSORS1C3, psoriasis
susceptibility 1 candidate 3; SMAD, Mothers against decapentaplegic homolog; SNP, single nucleotide polymorphism; rs#, SNP identification number; TNF-α, tumor
necrosis factor-α; UTR, untranslated region; VL, viral load; ZNRD1, zinc ribbon domain containing 1; +, present, –, absent.
Sources: Sunil K. Ahuja, MD, Weijing He, MD, Kristen Rogers, MS. Reviews for additional information: P An et al: Trends Genet 26:119, 2010; J Fellay: Antivir Ther
14:731, 2009; RA Kaslow et al: J Infect Dis 191:S68, 2005; D van Manen et al: Retrovirology 9:70, 2012; MP Martin et al: Immunol Rev 254:245, 2013; S Limou
et al: Front Immunol 4:118, 2013; PJ McLaren et al: Curr Opin HIV AIDS 10:110, 2015; PJ McLaren et al: Proc Natl Acad Sci USA 112:14658, 2015; PJ McLaren,
M Carrington: Nat Immunol 16:577, 2015; P An et al: PLoS Genet 12:e1005921, 2016; F Pereyra et al: Science 330:1551, 2010; I Bartha et al: PLoS Comput Biol
13:e1005339, 2017.
HIV infection. Carriage of the HLA-B∗57 and/or HLA-B*27 alleles is underlying the differential effects of the HLA-B alleles on the course
associated with slower disease progression. The beneficial effects of of HIV disease may relate to differences in the ability of antigen-
these alleles may relate in part to their consistent associations with a presenting cells to present immunodominant HIV epitopes to T helper
lower virologic set point as well as to higher cell-mediated immunity or cytotoxic T lymphocytes in the context of MHC-encoded molecules.
in HIV-infected persons. The protective effect of the HLA-B*57 and This may result in differential immune responses that influence viral
B*27 alleles on the HIV disease course is underscored by the finding replication. In this regard, the HLA-B alleles that impact the course
that the prevalence of these alleles is higher among long-term nonpro- of HIV disease differ in their amino acid residues in the HLA-B pep-
gressors and persons who control HIV replication spontaneously (elite tide-binding groove; this may play a critical role in virologic control.
controllers). In contrast, the HLA-B∗35 allele has been associated with Investigators have also examined the influence of extended HLA
faster progression to AIDS and higher viral load. The prevalence of the haplotypes (linked alleles) on the course of HIV disease. The extended
HLA-B alleles differs between populations. HLA-B∗57:01 in Europeans HLA ancestral haplotype (AH) 8.1 is defined by the presence of HLA-
and HLA-B∗57:03 in African Americans are the protective alleles. In A1, HLA-B8, and HLA-DR3 alleles. AH 8.1 is the most common
some populations (e.g., Japanese) where the HLA-B∗57/-B∗27 alleles ancestral haplotype in Caucasians (present in 10%) and is associated
are absent, HLA-B∗51 is associated with a protective phenotype. with multiple autoimmune diseases in HIV-uninfected persons. These
Possession of the protective HLA-B alleles is associated with broader associations of AH 8.1 are thought to be due to a genetically deter-
and stronger CD8+ T cell responses to HIV epitopes. The mechanisms mined hyperresponsiveness characterized by high TNF-α production
Harrisons_20e_Part5_p0859-p1648.indd 1419 6/1/18 12:08 PM
1420 CCR5 promoter
rs 800 351
rs 46 88
rs 34 58
rs 99 48
rs 799 87
rs 000 3
3 4
4
18
42
23 14
9
2
33 2
rs 986
02
HLA-C
41 9
HLA-B
27 7
17 6
1 9
1 9
18 0
10
49
2
Haplo-
rs 856
18
95
79
6
type
31
92
44
allele 304 allele 62 63 67 70 97
2
1
rs
rs
rs
rs
rs
HHA V A G G T C A C wt C M C B*57:01 G E M S V C G
HHB V A T G T C A C wt C M C B*52:01 R E S N T T G
HHC V A T G T C G C wt C V C B*27:05 R E C K N C G
HHD V A T G T T A C wt C M C R E S N T T G
HHE V A G A C C A C wt C Cw*08:02 M C B*14:02 R N C N W T G
HHF*1 V A G A C C A T wt C M C R N S N R T G
HHF*2 I A G A C C A T wt C V T R E S N R T G
HHG*1 V G G A C C A C wt A Cw*07:02 V T B*07:02 R N Y Q S T G
HHG*2 V G G A C C A C ∆32 A V T B*35:01 R N F N R T T
CCR3 CCR2 CCR5 CCRL2 PSORS1C3 HLA-C HLA-B MICA HCP5 MICB
80
– Log10 (P value)
60
Chr. 3p21 Chr. 6p21
CCR5 locus MHC region
20
8
0
Chr. 1 2 3 4 5 6 7 8 9 10 11 12 14 16 18 20 22
13 15 17 19 21
FIGURE 197-26 CCR5 and MHC loci: two key regions that influence HIV-AIDS pathogenesis. Bottom: Manhattan plot of genome-wide association from >6000 HIV-
infected Europeans. (Adapted from PJ McLaren et al: Proc Acad Natl Acad Sci 112:14658, 2015.) ∼8 million common variants were tested for their association with HIV
viral load set point using linear regression. Genome-wide signals of association (p < 5 × 10–8, dotted line) were observed on chromosomes (Chr.) 6p21 in the MHC
region and 3p21 in the CCR5 locus. Upper left: schema depicting composition of CCR5 haplotypes. (Adapted from E Gonzalez et al: Proc Natl Acad Sci USA 96:12004,
1999.) The 9 human haplotypes (HH) designated as HHA to HHG*2 were derived from the coding polymorphism of CCR2 64 V → I; 7 single nucleotide polymorphisms
PART 5
(SNPs) in the CCR5 promoter region as well as the ∆32 coding mutation in CCR5; wt, wild type. Carrington and colleagues refer to the CCR5-HHE haplotype as the P1
haplotype (MP Martin et al: Science 282:1907, 1998). Upper right: Representative haplotypes at Chr. 6p21 MHC region in Europeans. (Adapted from F Pereyra et al:
Science 330:1551, 2010.) Haplotypes defined by the SNPs identified by genome-wide association studies, classic HLA alleles and amino acids in HLA-B and HLA-C that
are associated with HIV viral control. Figure is not to scale and full references are in Table 197-6.
Infectious Diseases
and lack of complement C4A. Strong epidemiologic data indicate that haplotypes. Mathematical modeling revealed that variations in host
carriage of AH 8.1 in HIV-infected persons is associated with a rapid genes may explain about 10% of the observed variability in HIV viral
decline in CD4+ T cells and faster progression to AIDS development. load, whereas viral genetic diversity may explain 29% of the variability.
Gene–gene interactions between HLA alleles and other genes (e.g.,
killer cell immunoglobulin-like receptors) also may influence HIV dis- GENETIC ASSOCIATIONS WITH SPECIFIC AIDS AND NON-AIDS CONDITIONS
ease progression rates. Carotid artery disease Many of the non-AIDS events in HIV-infected
individuals resemble those related to immune senescence and those
POLYMORPHISMS IDENTIFIED BY GWAS THAT ASSOCIATE WITH HIV-1 found in the HIV-uninfected aging population. A functional SNP in
ACQUSITION AND VIROLOGIC CONTROL GWAS have not identified addi- the ryanodine receptor 3 (RYR3) gene was found to be associated with
tional genetic variations that associate with risk of HIV-1 acquisition. an increased risk of common carotid intima–media thickness (cIMT),
By contrast, large-scale GWAS have identified SNPs, especially in the which is a surrogate for subclinical atherosclerosis. Functional studies
MHC, that influence HIV viral load, including in a large group of indi- on RYR3 and its isoforms demonstrate a major role of these receptors in
viduals termed “HIV controllers” who spontaneously (without ART) modulating endothelial function and atherogenesis via calcium signal-
control viral replication. GWAS in HIV-infected persons of European ing pathways, providing a biologically plausible mechanism by which
ancestry identified four SNPs in genes in the HLA class I loci that asso- the SNP in RYR3 may associate with increased cIMT risk.
ciated with virologic control. These SNPs are within or in the vicinity
of PSORS1C3, HLA-C, MICA, and HCP5 genes (Fig. 197-26). As noted in Renal disease HIV-1-associated nephropathy (HIVAN) is a form of
this figure, the individual effects of these alleles are difficult to discern focal sclerosing glomerulonephritis caused by direct infection of kid-
because of linkage disequilibrium. The protective effects of the SNPs ney epithelial cells with HIV. HIVAN is more common in persons of
in HCP5 and MICA may relate to their linkage with known protective African descent. There is evidence that polymorphisms in the MYH9
HLA-B alleles. The protective HCP5 allele is in linkage disequilibrium gene and in the neighboring APOL1 gene are a strong determinant of
with the HLA-B*57:01 allele, and the protective MICA allele tags with susceptibility to HIVAN in African Americans. The effect of carrying
the HLA-B*57:01 and B*27:05 alleles. The protective HLA-C SNP is two APOL1 risk alleles explains nearly 35% of HIVAN. The mecha-
associated with higher HLA-C expression, and this effect is thought nisms by which MYH9/APOL1 variants predispose to HIVAN are
to be due to the altered binding of a microRNA to the HLA-C mRNA. currently unknown.
Higher HLA-C expression has been associated with beneficial HIV HIV-associated neurocognitive
HIV-associated neurocognitive disorder
phenotypes. The mechanism associated with the SNP in PSORS1C3 disorder (HAND) comprises a spectrum of neurocognitive deficits
is unknown. GWAS in African Americans identified a SNP that tags due to HIV infection. Variations in the apolipoprotein E (ApoE)
the HLA-B*57:03 allele that is known to associate with a lower virol- gene have strong associations with Alzheimer’s disease in the
ogic set point and slower disease course. Together, these GWAS data HIV-uninfected population. In HIV-infected persons, possession of
underscore the importance of variations in HLA class I loci in control the ApoE4 allele has been associated with several cognitive out-
of viral replication. A recent GWAS study suggested that an allele in the comes, including dementia, peripheral neuropathy, and impairment
gene encoding CCRL2 influences the HIV viral load set point. CCRL2 in cognition and immediate and delayed verbal memory. Macrophage
is on chromosome 3p21 and resides ~30 kb downstream of the CCR5 recruitment and activation play a central role in the development of
loci; its effect could potentially be due to its linkage with the CCR5 many of the HAND syndromes. Variations in chemokines that play
Harrisons_20e_Part5_p0859-p1648.indd 1420 6/1/18 12:08 PM
an influential role in macrophage activation and recruitment, namely of endogenous neurotoxins from macrophages and to a lesser extent 1421
CCL2 (MCP-1) and CCL3 (MIP-1α), have been shown to alter the risk from astrocytes. In addition, it has been demonstrated that both HIV-1
of developing HAND. Variations in mitochondrial genes also have Nef and Tat can induce chemotaxis of leukocytes, including monocytes,
been associated with risk of AIDS and HAND. A GWAS identified a into the CNS. Neurotoxins can be released from monocytes as a conse-
polymorphism in chromosome 14 in the T cell receptor α locus that quence of infection and/or immune activation. Monocyte-derived
may influence neurocognitive outcomes. neurotoxic factors have been reported to kill neurons via a vari-
HIV-1 associated Pneumocystis pneumonia Human Apobec3 cytidine ety of mechanisms including activation of the N-methyl-d-aspartate
deaminases are intrinsic resistance factors to HIV-1. However, HIV-1 (NMDA) receptors and induction of oxidative stress. In addition, HIV
encodes a viral infectivity factor (Vif) that degrades Apobec3 pro- gp120 shed by virus-infected monocytes could cause neurotoxicity by
teins. Association studies suggest a role of the genetic variation in the antagonizing the function of vasoactive intestinal peptide (VIP), by
Apobec3 family in HIV disease. A common haplotype derived from 6 elevating intracellular calcium levels, and by decreasing neurotrophic
SNPs in the Apobec-3F gene and tagged by a codon-changing variant is factor levels in the cerebral cortex. A variety of monocyte-derived
associated with significantly lower viral load set point, slower rate of cytokines can contribute directly or indirectly to the neurotoxic effects
progression to AIDS, and delayed development of Pneumocystis pneu- in HIV infection; these include TNF-α, IL-1, IL-6, TGF-β, IFN-γ,
monia (PCP). In addition, a coding SNP in the CCRL2 gene is associated platelet-activating factor, and endothelin. Furthermore, among the
with accelerated progression to AIDS and more rapid development of CC-chemokines, elevated levels of monocyte chemotactic protein-1
PCP. (MCP-1 or CCL-2) in the brain and CSF have been shown to correlate
best with the presence and degree of HIV encephalopathy in ART-naïve
ASSOCIATIONS WITH ART-RELATED ADVERSE EVENTS Abacavir, an effec-
patients. In addition, infection and/or activation of monocyte-lineage
tive antiretroviral agent, is associated with significant risk of hypersen-
cells can result in increased production of eicosanoids, quinolinic acid,
sitivity reactions (2–9% of cases). Interestingly, while the HLA-B*57:01
nitric oxide, excitatory amino acids such as l-cysteine and glutamate,
allele is associated with a slower HIV disease course, possession of
arachidonic acid, platelet activating factor, free radicals, TNF-α, and
this allele is associated with a higher risk of abacavir-associated hyper-
TGF-β, which may contribute to neurotoxicity. Astrocytes may play
sensitivity. Pharmacogenetic screening for the HLA-B*57:01 allele is
diverse roles in HIV neuropathogenesis. Reactive gliosis or astrocytosis
recommended before initiation of abacavir treatment.
has been demonstrated in the brains of HIV-infected individuals, and
TNF-α and IL-6 have been shown to induce astrocyte proliferation. In
■ NEUROPATHOGENESIS IN HIV DISEASE addition, astrocyte-derived IL-6 can induce HIV expression in infected
While there has been a remarkable decrease in the incidence of the cells in vitro. Furthermore, it has been suggested that astrocytes may
severe forms of HIV encephalopathy among those with access to
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
downregulate macrophage-produced neurotoxins. Evidence of neu-
treatment in the era of effective cART, HIV-infected individuals can ronal injury can be demonstrated by measuring neurofilament levels
still experience milder forms of neurocognitive impairment despite in CSF. Treatment with cART leads to improvement in neuropsychiatric
adequate cART. Factors that contribute to the neurocognitive decline manifestations and a decrease in these cytokine levels in CSF, suggest-
include lack of complete control of HIV replication in the brain; pro- ing that they are driven by the virus or by its products. However, even
duction of HIV proteins that may be neurotoxic; low CD4+ T cell in patients on long-term cART, there may be evidence of persistently
nadir; chronic immune activation; comorbidities such as drug abuse, activated lymphocytes in the CSF. It is unclear if these lymphocytes
microvascular disease, older age, and diabetes; and the potential for may contribute to neuronal injury in the brain or are critical for control-
neurotoxicity of certain antiretroviral drugs. HIV has been demon- ling the CNS viral reservoir. However, some individuals may develop
strated in the brain and CSF of infected individuals with and without a subacute encephalitis due to an IRIS reaction (see below). This often
neuropsychiatric abnormalities. As opposed to lymphoid tissues, there occurs weeks or a few months after initiation of cART in individuals
are no resident lymphocytes in the brain. The main cell types that are with low CD4+ T cell counts. It is thought that the recovery of CD4+
infected in the brain in vivo are the perivascular macrophages and the T cells causes a lymphocyte response to the CNS HIV reservoir. The
microglial cells, which can sometimes form syncytia resulting in multi- contribution of host genetic factors to development of neuropsychiatric
nucleated giant cells; low-level viral replication is also seen in perivas- manifestations of HIV infection has not been well studied. However,
cular astrocytes. It has been proposed that monocytes that have already evidence supports the role of several genetic factors including the E4
been infected in the blood can migrate into the brain, where they allele for apoE in an increased risk of HIV-associated neurocognitive
then reside as macrophages, or macrophages can be directly infected disorders and peripheral neuropathy.
while residing within the brain. The precise mechanisms whereby It has also been suggested that the CNS may serve as a relatively
HIV enters the brain are unclear; however, they are thought to relate, sequestered site for a reservoir of latently infected cells that might be a
at least in part, to the ability of virus-infected and immune-activated barrier for the eradication of virus by cART (see “The HIV Reservoir:
macrophages to induce adhesion molecules such as E-selectin and vas- Obstacles to the Eradication of Virus,” above).
cular cell adhesion molecule 1 (VCAM-1) on brain endothelium. Other
studies have demonstrated that HIV gp120 enhances the expression of ■ PATHOGENESIS OF KAPOSI’S SARCOMA
intercellular adhesion molecule 1 (ICAM-1) in glial cells and HIV Tat There are at least four distinct epidemiologic forms of KS: (1) the clas-
protein can disrupt the tight junctions of the brain endothelial cells to sic form that occurs in older men of predominantly Mediterranean or
facilitate entry of HIV-infected cells into the CNS. Virus isolates from eastern European Jewish backgrounds with no recognized contributing
the brain are preferentially R5 strains as opposed to X4 strains; in this factors; (2) the equatorial African form that occurs in all ages, also with-
regard, HIV-infected individuals who are heterozygous for CCR5-∆32 out any recognized precipitating factors; (3) the form associated with
appear to be relatively protected against the development of HIV organ transplantation and its attendant iatrogenic immunosuppressed
encephalopathy. Once HIV enters the brain due to pressures of the state; and (4) the form associated with HIV-1 infection. In the latter
local environment, it evolves to develop distinct sequences in the env, two forms, KS is an opportunistic disease; in HIV-infected individuals,
tat, and LTR genes. These unique sequences have been associated with unlike typical opportunistic infections, its occurrence is not strictly
neurocognitive dysfunction; however, it is unclear if they are causal related to the level of depression of CD4+ T cell counts. The pathogen-
(see below). esis of KS is complex; fundamentally, it is an angioproliferative disease
HIV-infected individuals may manifest white matter lesions as well that is not a true neoplastic sarcoma, at least not in its early stages. It
as neuronal loss. The white matter lesions are due to axonal injury and is a manifestation of excessive proliferation of spindle cells that are
a disruption of the blood-brain barrier and not due to demyelination. believed to be of vascular origin and have features in common with
Given the absence of evidence of HIV infection of neurons, HIV- endothelial and smooth-muscle cells. In HIV disease the development
mediated effects on neurons are thought to involve indirect pathways of KS is dependent on the interplay of a variety of factors including
whereby viral proteins, particularly gp120 and Tat, trigger the release HIV-1 itself, human herpes virus 8 (HHV-8), immune activation, and
Harrisons_20e_Part5_p0859-p1648.indd 1421 6/1/18 12:08 PM
1422 cytokine secretion. A number of epidemiologic and virologic stud- TABLE 197-7 Elements of the Immune Response to HIV
ies have clearly linked HHV-8, which is also referred to as Kaposi’s Humoral immunity
sarcoma–associated herpesvirus (KSHV), to KS not only in HIV-infected
Binding antibodies
individuals but also in individuals with the other forms of KS. HHV-8
Neutralizing antibodies
is a γ-herpesvirus related to EBV and herpesvirus saimiri. It encodes a
homologue to human IL-6 and, in addition to KS, has been implicated Type specific
in the pathogenesis of body cavity lymphoma, multiple myeloma, and Group specific
monoclonal gammopathy of undetermined significance. Sequences of Broadly neutralizing
HHV-8 are found universally in the lesions of KS, and patients with KS Antibodies participating in antibody-dependent cellular cytotoxicity (ADCC)
are virtually all seropositive for HHV-8. HHV-8 DNA sequences can be Protective
found in the B cells of 30–50% of patients with KS and 7% of patients Pathogenic (bystander killing)
with AIDS without clinically apparent KS. Enhancing antibodies
Between 1% and 2% of eligible blood donors are positive for anti- Complement
bodies to HHV-8, while the prevalence of HHV-8 seropositivity in Cell-mediated immunity
HIV-infected men is 30–35%. The prevalence of HHV-8 seropositivity in
Helper CD4+ T lymphocytes
HIV-infected women is ~4%. This finding is reflective of the lower inci-
Class I MHC–restricted cytotoxic CD8+ T lymphocytes
dence of KS in women. It has been debated whether HHV-8 is actually
the transforming agent in KS; the bulk of the cells in the tumor lesions CD8+ T cell–mediated inhibition (noncytolytic)
of KS are not neoplastic cells. However, it has been demonstrated that ADCC
endothelial cells can be transformed in vitro by HHV-8. In this regard, Natural killer cells
HHV-8 possesses a number of genes, including homologues of the IL-8 Abbreviation: MHC, major histocompatibility complex.
receptor, Bcl-2, and cyclin D, that can potentially transform the host cell.
Despite the complexity of the pathogenic events associated with the
development of KS in HIV-infected individuals, HHV-8 is the etiologic
agent of this disease. The initiation and/or propagation of KS requires
an activated state and is mediated, at least in part, by cytokines. A num-
ber of factors, including TNF-α, IL-1β, IL-6, granulocyte-macrophage
colony-stimulating factor (GM-CSF), basic fibroblast growth factor, and Neutralizing antibody
oncostatin M, function in an autocrine and paracrine manner to sus-
PART 5
tain the growth and chemotaxis of the KS spindle cells. In this regard, Cytotoxic CD8+
KSHV-derived IL-6 has been demonstrated to induce proliferation of Lysis T lymphocyte
lymphoma cells and to inhibit the cytostatic effects of IFN-α on KSH- Class I MHC
Activation,
V-infected lymphoma cells. proliferation, cytokine
and chemokine release
Infectious Diseases
IMMUNE RESPONSE TO HIV TCR
As detailed above and below, following the initial burst of viremia dur-
Viral antigens
ing primary infection, HIV-infected individuals mount robust immune
responses that in most cases substantially curtail the levels of plasma
viremia and likely contribute to delaying the ultimate development of Fc ADCC
clinically apparent disease for a median of 10 years in untreated indi- receptor
viduals. This immune response contains elements of both humoral and
cell-mediated immunity involving both adaptive and innate immune Free
responses (Table 197-7; Fig. 197-27). It is directed against multiple CD4 gp120
antigenic determinants of the HIV virion as well as against viral pro- Bystander HIV-infected CD4+
teins expressed on the surface of infected cells. Ironically, those CD4+ killing T lymphocyte
T cells with T cell receptors specific for HIV are theoretically those
CD4+ T cells most likely to be activated—and thus to serve as early
targets for productive HIV infection and the cell death or dysfunction Uninfected CD4+
associated with infection. Thus, an early consequence of HIV infection T lymphocyte Helper CD4+ Cytokine
is interference with and decrease of the helper T cell population needed T lymphocytes release
to generate an effective immune response.
Although a great deal of investigation has been directed toward
Activation
delineating and better understanding the components of this immune
response, it remains unclear which immunologic effector mechanisms
are most important in delaying progression of infection and which, if
any, play a role in the pathogenesis of HIV disease. This lack of knowl-
edge has also hampered the ability to develop an effective vaccine for
HIV disease. Class II MHC Lysis
■ HUMORAL IMMUNE RESPONSE
Antibodies to HIV usually appear within 3–6 weeks and almost
HIV-infected CD4+
invariably within 12 weeks of primary infection (Fig. 197-28); rare
T lymphocyte
exceptions are in individuals who have defects in the ability to pro-
duce HIV-specific antibodies. Detection of these antibodies forms
the basis of most diagnostic screening tests for HIV infection. The Natural killer cells
appearance of HIV-binding antibodies detected by ELISA and western
FIGURE 197-27 Schematic representation of the different immunologic effector
blot assays occurs prior to the appearance of neutralizing antibodies; mechanisms thought to be active in the setting of HIV infection. Detailed
the latter generally appear following the initial decreases in plasma descriptions are given in the text. ADCC, antibody-dependent cellular cytotoxicity;
viremia and are more closely related to the appearance of HIV-specific MHC, major histocompatibility complex; TCR, T cell receptor.
Harrisons_20e_Part5_p0859-p1648.indd 1422 6/1/18 12:08 PM
CD8+ T lymphocytes. The first antibodies detected are those directed V1V2 Apex 1423
N332 Glycan
against the immunodominant region of the envelope gp41, followed
Supersite
by the appearance of antibodies to the structural or gag protein p24
and the gag precursor p55. Antibodies to p24 gag are followed by the
appearance of antibodies to the outer envelope glycoprotein (gp120),
the gag protein p17, and the products of the pol gene (p31 and p66). In
addition, one may see antibodies to the low-molecular-weight regula- CD4 Binding
tory proteins encoded by the HIV genes vpr, vpu, vif, rev, tat, and nef. Site
On rare occasion, levels of HIV-specific antibodies may decline during Trimer
interface
treatment of acute HIV infection. gp41 MPER
While antibodies to multiple antigens of HIV are produced, the pre-
cise functional significance of these different antibodies is unclear. The
only viral proteins that elicit neutralizing antibodies are the envelope
proteins gp120 and gp41. Antibodies directed toward the envelope FIGURE 197-29 Known targets of broadly neutralizing antibodies against HIV-1.
proteins of HIV have been characterized both as being protective and (Adapted from PD Kwong, JR Mascola: Immunity 37:412, 2012.)
as possibly contributing to the pathogenesis of HIV disease. Among the
protective antibodies are those that function to neutralize HIV directly
and prevent the spread of infection to additional cells, as well as those The other major class of protective antibodies are those that par-
that participate in ADCC. The first neutralizing antibodies are directed ticipate in ADCC, a form of cell-mediated immunity (Chap. 342) in
against the autologous infecting virus and appear after approximately which NK cells that bear Fc receptors are armed with specific anti-HIV
12 to 24 weeks of infection. Due to its high rate of mutation the virus is antibodies that bind to the NK cells via their Fc portion. These armed
usually able to quickly escape these (and subsequent) neutralizing anti- NK cells then bind to and destroy cells expressing HIV antigens. The
bodies. One important mechanism of immune escape is the addition levels of anti-envelope antibodies capable of mediating ADCC are
of N-linked glycosylation sites, forming a glycan shield that interferes highest in the earlier stages of HIV infection. Antibodies to both gp120
with envelope recognition by these initial antibodies. and gp41 have been shown to participate in ADCC-mediated killing of
A number of broad and potent HIV-neutralizing envelope-specific HIV-infected cells. In vitro, IL-2 can augment ADCC-mediated killing.
antibodies have been isolated from HIV-infected individuals in stud- In addition to playing a role in host defense, HIV-specific antibodies
ies designed to better understand the host response to HIV infection. have also been implicated in disease pathogenesis. Antibodies directed
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
Approximately 20% of patients develop antibodies capable of neu- to gp41, when present in low titer, have been shown in vitro to be capa-
tralizing highly diverse strains. These usually appear 2 or more years ble of facilitating infection of cells through an Fc receptor–mediated
following infection in the face of continual viremia. These studies have mechanism known as antibody enhancement. Thus, the same regions
revealed at least five major sites within the HIV envelope trimer that of the envelope protein of HIV that give rise to antibodies capable
are able to elicit broadly neutralizing antibodies. These sites include of mediating ADCC can also elicit the production of antibodies that
antibodies directed toward the CD4 binding site (CD4bs) of gp120, can facilitate infection of cells in vitro. In addition, it has been postu-
those binding glycan-dependent epitopes in the V1/V2 region of lated that anti-gp120 antibodies that participate in the ADCC killing
gp120, those near the base of the V3 region of gp120, those binding to of HIV-infected cells might also kill uninfected CD4+ T cells if the
the gp120/gp41 bridge, and those binding to the membrane-proximal uninfected cells had bound free gp120, a phenomenon referred to as
region of gp41 (Fig. 197-29). Several of these antibodies contain unique bystander killing.
features including high levels of somatic hypermutation, selective One of the most primitive components of the humoral immune
germline gene usage (especially for CD4bs antibodies), and long heavy system is the complement system (Chap. 342). This element of innate
chain complementary determining regions (especially CDRH3). Of immunity consists of ~30 proteins that are found circulating in blood or
note, while these antibodies are broadly neutralizing in vitro, their associated with cell membranes. While HIV alone is capable of directly
precise in vivo significance is unclear and the patients from whom they activating the complement cascade, the resulting lysis is weak due
were derived demonstrate evidence of ongoing viral replication unless to the presence of host cell regulatory proteins captured in the virion
treated with cART. envelope during budding. It is possible that complement-opsonized
HIV virions have increased infectivity in a manner analogous to antibody-
mediated enhancement.
Initial Seroconversion,
ADCC, CTL
■ CELLULAR IMMUNE RESPONSE
viremia
Given that T cell–mediated immunity is known to play a major role in
host defense against most viral infections (Chap. 342), it is generally
Autologous
thought to be an important component of the host immune response
NAbs to HIV. T cell immunity can be divided into two major categories: that
Broadly reactive mediated by helper/inducer CD4+ T cells and that mediated by cytotoxic/
NAbs
immunoregulatory CD8+ T cells.
HIV-specific CD4+ T cells can be detected in the majority of
HIV-infected patients through the use of flow cytometry to measure
intracellular cytokine production in response to MHC class II tetramers
pulsed with HIV peptides or through lymphocyte proliferation assays
0 1 2 3–10 utilizing HIV antigens such as p24. These cells likely play a critical role
Years infected in the orchestration of the immune response to HIV by providing help
FIGURE 197-28 Relationship between initial HIV viremia and the development to HIV-specific B cells and CD8+ T cells. They may also be capable of
of antibodies to HIV. Within 3 to 6 weeks of initial HIV infection, non-neutralizing directly killing HIV-infected cells. HIV-specific CD4+ T cells may be
antibodies to HIV appear. These antibodies are capable of mediating antibody- preferential targets of HIV infection by HIV-infected antigen-present-
dependent cellular cytotoxicity (ADCC). The decline in plasma viremia generally ing cells during the generation of an immune response to HIV
correlates with the appearance of cytotoxic T lymphocytes (CTL). After (Fig. 197-27). However, they also are likely to undergo clonal expan-
approximately 3 months, autologous neutralizing antibodies (NAbs) capable of
neutralizing prior circulating strains of HIV appear. After 2 or more years, broadly
sions in response to HIV antigens and thus survive as a population of
reactive NAbs appear. (Adapted from JT Mascola, DC Montefiori: Annu Rev Immunol cells. No clear correlations exist between levels of HIV-specific CD4+
28:413, 2010.) T lymphocytes and plasma HIV RNA levels; however, in the setting
Harrisons_20e_Part5_p0859-p1648.indd 1423 6/1/18 12:08 PM
1424 of high viral loads, CD4+ T cell responses to HIV antigens appear to HIV. In 1996, blood banks in the United States added the p24 antigen
shift from one of proliferation and IL-2 production to one of IFN-γ pro- capture assay to the screening process to help identify the rare infected
duction. Thus, while a reverse correlation exists between the level of individuals who were donating blood in the time (up to 3 months)
p24-specific proliferation and levels of plasma HIV viremia, the nature between infection and the development of antibodies. In 2002, the
of the causal relationship between these parameters is unclear. ability to detect early infection with HIV was further enhanced by the
MHC class I–restricted, HIV-specific CD8+ T cells have been identi- licensure of nucleic acid testing (NAT) as a routine part of blood donor
fied in the peripheral blood of patients with HIV-1 infection. These cells screening. These refinements decreased the interval between infection
include CTLs that produce perforins and T cells that can be induced and detection (window period) from 22 days for antibody testing to
by HIV antigens to express an array of cytokines such as IFN-γ, IL-2, 16 days with p24 antigen testing and subsequently to 12 days with
MIP-1β, and TNF-α. CTLs have been identified in the peripheral blood NAT. The development of sensitive assays for monitoring levels of
of patients within weeks of HIV infection and prior to the appearance of plasma viremia ushered in a new era of being able to monitor the pro-
plasma virus. The selective pressure they exert on the evolution of the gression of HIV disease more closely. Utilization of these tests, coupled
population of circulating viruses reflects their potential role in control of with the measurement of levels of CD4+ T lymphocytes in peripheral
HIV infection. These CD8+ T lymphocytes, through their HIV-specific blood, is essential in the management of patients with HIV infection.
antigen receptors, bind to and cause the lytic destruction of target cells
bearing autologous MHC class I molecules presenting HIV antigens. ■ DIAGNOSIS OF HIV INFECTION
Two types of CTL activity can be demonstrated in the peripheral blood The CDC has recommended that screening for HIV infection be
or lymph node mononuclear cells of HIV-infected individuals. The first performed as a matter of routine health care. The diagnosis of HIV
type directly lyses appropriate target cells in culture without prior in infection depends on the demonstration of antibodies to HIV and/or
vitro stimulation (spontaneous CTL activity). The other type of CTL activ- the direct detection of HIV or one of its components. As noted above,
ity reflects the precursor frequency of CTLs (CTLp); this type of CTL activ- antibodies to HIV generally appear in the circulation 3–12 weeks fol-
ity can be demonstrated by stimulation of CD8+ T cells in vitro with a lowing infection.
mitogen such as phytohemagglutinin or anti-CD3 antibody. The standard blood screening tests for HIV infection are based on
In addition to CTLs, CD8+ T cells capable of being induced by HIV the detection of antibodies to HIV. A common platform is the ELISA,
antigens to express cytokines such as IFN-γ also appear in the setting also referred to as an enzyme immunoassay (EIA). This solid-phase assay
of HIV-1 infection. It is not clear whether these are the same or differ- is an extremely good screening test with a sensitivity of >99.5%. Most
ent effector pools compared with those cells mediating cytotoxicity; in diagnostic laboratories use commercial kits that contain antigens from
addition, the relative roles of each in host defense against HIV are not both HIV-1 and HIV-2 and thus are able to detect antibodies to either.
fully understood. It does appear that these CD8+ T cells are driven to These kits use both natural and recombinant antigens and are continu-
PART 5
in vivo expansion by HIV antigen. There is a direct correlation between ously updated to increase their sensitivity to newly discovered species,
levels of CD8+ T cells capable of producing IFN-γ in response to HIV such as group O viruses (Fig. 197-1). The fourth-generation EIA tests
antigens and plasma levels of HIV-1 RNA. Thus, while these cells combine detection of antibodies to HIV with detection of the p24 anti-
are clearly induced by HIV-1 infection, their overall ability to control gen of HIV. EIA tests are generally scored as positive (highly reactive),
infection remains unclear. Multiple HIV antigens, including Gag, Env, negative (nonreactive), or indeterminate (partially reactive). While the
Infectious Diseases
Pol, Tat, Rev, and Nef, can elicit CD8+ T cell responses. Among patients EIA is an extremely sensitive test, it is not optimal with regard to spec-
who control viral replication in the absence of antiretroviral drugs are ificity. This is particularly true in studies of low-risk individuals, such
a subset of patients referred to as elite nonprogressors (see “Long-Term as volunteer blood donors. In this latter population, only 10% of EIA-
Survivors, Long-Term Nonprogressors, and Elite Controllers,” above) positive individuals are subsequently confirmed to have HIV infection.
whose peripheral blood contains a population of CD8+ T cells that Among the factors associated with false-positive EIA tests are antibod-
undergo substantial in vitro proliferation and perforin expression in ies to class II antigens (such as may be seen following pregnancy, blood
response to HIV antigens. It is possible that these cells play an impor- transfusion, or transplantation), autoantibodies, hepatic disease, recent
tant role in HIV-specific host defense. influenza vaccination, and acute viral infections. For these reasons,
At least three other forms of cell-mediated immunity to HIV have anyone suspected of having HIV infection based on a positive or incon-
been described: non-cytolytic CD8+ T cell–mediated suppression of clusive fourth-generation EIA result should have the result confirmed
HIV replication, ADCC, and NK cell activity. Non-cytolytic CD8+ with a more specific assay such as an HIV-1- or HIV-2-specific antibody
T cell–mediated suppression of HIV replication refers to the ability of CD8+ immunoassay, a western blot, or a plasma HIV RNA level. One can
T cells from an HIV-infected patient to inhibit the replication of HIV in estimate whether an individual has a recent infection with HIV-1 by
tissue culture without killing infected targets. There is no requirement comparing the results on a standard EIA test that will score positive
for HLA compatibility between the CD8+ T cells and the HIV-infected for all infected individuals with the results on an assay modified to be
cells. This effector mechanism is thus nonspecific and appears to be less sensitive (“detuned assay”) that will score positive for individuals
mediated by soluble factor(s) including the CC-chemokines RANTES with established HIV infection and negative for individuals with recent
(CCL5), MIP-1α (CCL3), and MIP-1β (CCL4). These CC-chemokines infection. In rare instances, an HIV-infected individual treated early in
are potent suppressors of HIV replication and operate at least in part the course of infection may revert to a negative EIA. This does not indi-
via blockade of the HIV co-receptor (CCR5) for R5 (macrophage-tropic) cate clearing of infection; rather, it signifies levels of ongoing exposure
strains of HIV-1 (see above). ADCC, as described above in relation to to virus or viral proteins insufficient to maintain a measurable antibody
humoral immunity, involves the killing of HIV-expressing cells by NK response. When these individuals have discontinued therapy, viruses
cells armed with specific antibodies directed against HIV antigens. and antibodies have reappeared.
Finally, NK cells alone have been shown to be capable of killing HIV-in- While current CDC recommendations indicate that a positive
fected target cells in tissue culture. This primitive cytotoxic mechanism fourth-generation assay confirmed by a second HIV-1- or HIV-2-specific
of host defense is directed toward nonspecific surveillance for neoplas- immunoassay is adequate for diagnosis, many feel it is prudent to
tic transformation and viral infection through recognition of altered confirm diagnosis with a second platform test such as the western
class I MHC molecules. blot or HIV plasma RNA level. The western blot (Fig. 197-30) assay
takes advantage of the fact that multiple HIV antigens of different,
DIAGNOSIS AND LABORATORY well-characterized molecular weights elicit the production of specific
MONITORING OF HIV INFECTION antibodies. These antigens can be separated on the basis of molec-
The establishment of HIV as the causative agent of AIDS and related ular weight, and antibodies to each component can be detected as
syndromes early in 1984 was followed by the rapid development discrete bands on the western blot. A negative western blot is one in
of sensitive screening tests for HIV infection. By March 1985, blood which no bands are present at molecular weights corresponding to
donors in the United States were routinely screened for antibodies to HIV gene products. In a patient with a positive or indeterminate EIA
Harrisons_20e_Part5_p0859-p1648.indd 1424 6/1/18 12:08 PM
. .. 1425
YYY 160
YYY YYY
120
YYY YYY p66
YYY
. .. env
. ..
YYY p55
YYY YYY
pol 41
. ..
YYY
YYY YYY
. ..
p31
YYY
YYY YYY
. ..
YYY
YYY YYY
p24
gag
. ..
YYY
YYY YYY
p18
. ..
YYY
YYY YYY
1 2 3 4 1 2 3 4 5
A B
1. Virus digested: digest separated into 1. Positive HIV-1 infection
components by molecular weight 2. gp 160 immunization
2. Proteins transferred to filter paper: 3. Indeterminate (HIV-2 infection)
reaction with test serum 4. Indeterminate (cross-reacting antibody to p24)
3. Enzyme-conjugated antihuman antibody added 5. Negative
4. Substrate added and color noted
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
FIGURE 197-30 Western blot assay for detection of antibodies to HIV. A. Schematic representation of how a western blot is performed. B. Examples of patterns
of western blot reactivity. In each instance the western blot strip contains antigens to HIV-1. The serum from the patient immunized to the HIV-1 envelope gp160
contains only antibodies to the HIV-1 envelope proteins. The serum from the patient with HIV-2 infection cross-reacts with both reverse transcriptase and gag gene
products of HIV-1.
and a negative western blot, one can conclude with certainty that the If the result is negative, unless there is strong reason to suspect early
EIA reactivity was a false positive. On the other hand, a western blot HIV infection (as in a patient exposed within the previous 3 months),
demonstrating antibodies to products of all three of the major genes the diagnosis is ruled out and retesting should be performed only as
of HIV (gag, pol, and env) is conclusive evidence of infection with clinically indicated. If the EIA is indeterminate or positive, the test
HIV. Criteria established by the FDA in 1993 state that a western blot should be repeated. If the repeat is negative on two occasions, one can
result is considered positive if antibodies exist to two of the three HIV assume that the initial positive reading was due to a technical error
proteins: p24, gp41, and gp120/160. Using these criteria, ~10% of all in the performance of the assay and that the patient is negative. If the
blood donors deemed positive for HIV-1 infection lacked an antibody repeat is indeterminate or positive, one should proceed to the HIV-1
band to the pol gene product p31. Some 50% of these blood donors western blot. If the western blot is positive, the diagnosis is HIV-1 infec-
were subsequently found to be false positives. Thus, the absence of the tion. If the western blot is negative, the EIA can be assumed to have
p31 band should increase the suspicion that one may be dealing with a been a false positive for HIV-1 and the diagnosis of HIV-1 infection is
false-positive test result. In this setting it is prudent to obtain additional ruled out. It would also be prudent at this point to perform specific
confirmation with an RNA-based test for HIV-1 and/or a follow-up serologic testing for HIV-2 following the same type of algorithm. If
western blot. By definition, western blot patterns of reactivity that do the western blot for HIV-1 is indeterminate, it should be repeated in
not fall into the positive or negative categories are considered “inde- 4–6 weeks; in addition, one may proceed to a specific HIV-1 or HIV-2
terminate.” There are two possible explanations for an indeterminate antibody differentiation assay, HIV-1 RNA assay, or HIV-1 DNA PCR.
western blot result. The most likely explanation in a low-risk individual If the HIV RNA assays are negative and there is no progression in the
is that the patient being tested has antibodies that cross-react with one western blot, a diagnosis of HIV-1 is ruled out. If either HIV-1 RNA
of the proteins of HIV. The most common patterns of cross-reactivity are assay is positive and/or the HIV-1 western blot shows progression, a
antibodies that react with p24 and/or p55. The least likely explanation tentative diagnosis of HIV-1 infection can be made and later confirmed
in this setting is that the individual is infected with HIV and is in the with a follow-up western blot demonstrating a positive pattern. In
process of mounting a classic antibody response. In either instance, the addition to these standard laboratory-based assays for detecting anti-
western blot should be repeated in 1 month to determine whether bodies to HIV, a series of point-of-care tests can provide results in 1–60
the indeterminate pattern is a pattern in evolution. In addition, one may min. Among the most popular of these is the OraQuick Rapid HIV-1
attempt to confirm a diagnosis of HIV infection with one of the tests for antibody test that can be run on blood, plasma, or saliva. The sensi-
HIV RNA (discussed below). While the western blot is an excellent con- tivity and specificity of this test is ~99% when run on whole blood.
firmatory test for HIV infection in patients with a positive or indetermi- Specificity remains the same but sensitivity drops to 98% when the
nate EIA, it is a poor screening test. Among individuals with a negative test is run on saliva. While negative results from this test are adequate
EIA and PCR for HIV, 20–30% may show one or more bands on western to rule out a diagnosis of HIV infection, a positive finding should be
blot. While these bands are usually faint and represent cross-reactivity, considered preliminary and confirmed with standard serologic testing,
their presence creates a situation in which other diagnostic modalities as described above. Two rapid test kits are licensed for home use. They
(such as DNA PCR, RT-PCR, or p24 antigen capture) must be employed are the OraQuick HIV test and the Home Access HIV-1 test system. A
to ensure that the bands do not indicate early HIV infection. positive result with either of these tests should be followed with con-
A guideline for the use of these serologic tests in attempting to make firmatory testing by a healthcare professional.
a diagnosis of HIV infection is depicted in Fig. 197-31. In patients in A variety of laboratory tests are available for the direct detec-
whom HIV infection is suspected, the appropriate initial test is the EIA. tion of HIV or its components (Table 197-8). These tests may be of
Harrisons_20e_Part5_p0859-p1648.indd 1425 6/1/18 12:08 PM
1426
A SEROLOGIC TESTS IN THE DIAGNOSIS OF HIV-1 OR HIV-2 INFECTION
Repeat + HIV-1 + Diagnosis
HIV-1/HIV-2 Western of HIV-1
EIA blot infection
+
– – Indeterminate
Screening
HIV-2
HIV–1/HIV-2
EIA Repeat in 4–6 weeks*
EIA
– + Indeterminate
–
Retest in
– HIV-2 + Diagnosis
3–6 months
Western of HIV-2
if clinically
blot infection
indicated
B HIV-1/2 ANTIGEN/ANTIBODY COMBINATION IMMUNOASSAY
+ –
Negative for HIV-1 and HIV-2
antibodies and p24Ag
HIV-1/HIV-2 antibody
differentiation immunoassay
PART 5
HIV-1 + HIV-1 – HIV-1 + HIV-1 – or indeterminate
HIV-2 – HIV-2 + HIV-2 + HIV-2 –
HIV-1 antibodies HIV-2 antibodies HIV antibodies
Infectious Diseases
detected detected detected HIV-1 NAT
+ indicates reactive test result HIV-1 NAT + HIV-1 NAT –
– indicates nonreactive test result Acute HIV-1 Negative for
infection HIV-1
NAT: nucleic acid test
FIGURE 197-31 Serologic tests for the diagnosis of HIV-1 or HIV-2 infection. A. Algorithm including the use of a western blot. *Stable indeterminate western blot
4–6 weeks later makes HIV infection unlikely. However, it should be repeated twice at 3-month intervals to rule out HIV infection. Alternatively, one may test for HIV-1
p24 antigen or HIV RNA. EIA, enzyme immunoassay. B. CDC algorithm not including the use of a western blot. (Adapted from stacks.cdc.gov/view/cdc/23446.)
considerable help in making a diagnosis of HIV infection when the of HIV. It detects the viral protein p24 in the blood of HIV-infected indi-
antibody determination assays or western blot results are indetermi- viduals where it exists either as free antigen or complexed to anti-p24
nate. In addition, the tests detecting levels of HIV RNA can be used antibodies. Overall, ~30% of individuals with untreated HIV infection
to determine prognosis and to assess the response to antiretroviral have detectable levels of free p24 antigen. This increases to ~50% when
therapies. The simplest, least expensive, and most rarely used of the samples are treated with a weak acid to dissociate antigen-antibody
direct detection tests is the p24 antigen capture assay. This is an EIA-type complexes. Throughout the course of HIV infection, an equilibrium
assay in which the solid phase consists of antibodies to the p24 antigen exists between p24 antigen and anti-p24 antibodies. During the first
TABLE 197-8 Characteristics of Tests for Direct Detection of HIV
TEST TECHNIQUE SENSITIVITYa COST/TESTb
Immune complex–dissociated p24 Measurement of levels of HIV-1 core protein in an EIA-based Positive in 50% of patients; detects $1–2
antigen capture assay format following dissociation of antigen-antibody complexes by down to 15 pg/mL of p24 protein
weak acid treatment
HIV RNA by PCR Target amplification of HIV-1 RNA via reverse transcription Reliable to 40 copies/mL of HIV RNA $75–150
followed by PCR
HIV RNA by bDNA Measurement of levels of particle-associated HIV RNA in a Reliable to 50 copies/mL of HIV RNA $75–150
nucleic acid capture assay employing signal amplification
HIV RNA by TMA Target amplification of HIV-1 RNA via reverse transcription Reliable to 100 copies/mL of HIV RNA $225
followed by T7 RNA polymerase
HIV RNA by NASBA Isothermal nucleic acid amplification with internal controls Reliable to 80 copies/mL of HIV RNA $75–150
Sensitivity figures refer to those approved by the U.S. Food and Drug Administration. Prices may be lower in large-volume settings.
a b
Abbreviations: bDNA, branched DNA; cDNA, complementary DNA; EIA, enzyme immunoassay; NASBA, nucleic acid sequence–based amplification; PCR, polymerase chain
reaction; TMA, transcription-mediated amplification.
Harrisons_20e_Part5_p0859-p1648.indd 1426 6/1/18 12:08 PM
few weeks of infection, before an immune response develops, there or detecting proviral DNA in peripheral blood mononuclear cells are 1427
is a brisk rise in p24 antigen levels. After the development of anti-p24 valuable tools for making a diagnosis of HIV infection; however, they
antibodies, these levels decline. Late in the course of infection, when should be used for diagnosis only when standard serologic testing has
circulating levels of virus are high, p24 antigen levels also increase, failed to provide a definitive result.
particularly when detected by techniques involving dissociation of
antigen-antibody complexes. The p24 antigen capture assay has its ■ LABORATORY MONITORING OF PATIENTS WITH HIV
greatest use as a screening test for HIV infection in patients suspected INFECTION
of having the acute HIV syndrome (see below), as high levels of p24 The epidemic of HIV infection and AIDS has provided the clinician
antigen are present prior to the development of antibodies. Its use as with new challenges for integrating clinical and laboratory data to
a stand-alone test for routine blood donor screening for HIV infection effect optimal patient management. The close relationship between
has been replaced by use of NAT or “fourth-generation” assays that clinical manifestations of HIV infection and CD4+ T cell count has
combine antigen and antibody testing. The ability to measure and mon- made measurement of CD4+ T cell numbers a routine part of the
itor levels of HIV RNA in the plasma of patients with HIV infection evaluation of HIV-infected individuals. The discovery of HIV as the
has been of extraordinary value in furthering our understanding of the cause of AIDS led to the development of sensitive tests that allow one
pathogenesis of HIV infection, in monitoring the response to cART, and to monitor the levels of HIV in the blood. Determinations of peripheral
in providing a diagnostic tool in settings where measurements of anti- blood CD4+ T cell counts and measurements of the plasma levels of
HIV antibodies may be misleading, such as in acute infection and neo- HIV RNA provide a powerful set of tools for determining prognosis
natal infection. Four assays are predominantly used for this purpose. and monitoring response to therapy.
They are reverse transcriptase PCR (RT-PCR; Amplicor and RealTime);
branched DNA (bDNA; VERSANT); transcription-mediated amplifica- CD4+ T Cell Counts The CD4+ T cell count is the laboratory
tion (TMA; APTIMA); and nucleic acid sequence–based amplification test generally accepted as the best indicator of the immediate state
(NASBA; NucliSENS). These tests are of value in making a diagnosis of of immunologic competence of the patient with HIV infection. This
HIV infection, in establishing initial prognosis, and in monitoring the measurement, which can be made directly or calculated as the product
effects of therapy. In addition to the commercially available tests for of the percentage of CD4+ T cells (determined by flow cytometry) and
measuring HIV RNA, DNA PCR assays are also employed by research the total lymphocyte count (determined by the white blood cell count
laboratories for making a diagnosis of HIV infection by amplifying HIV [WBC] multiplied by the lymphocyte differential percentage), has been
proviral DNA from peripheral blood mononuclear cells. The commer- shown to correlate very well with the level of immunologic compe-
cially available RNA detection tests have a sensitivity of 40–80 copies tence. Patients with CD4+ T cell counts <200/μL are at high risk of
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
of HIV RNA per milliliter of plasma. Research laboratory–based RNA disease from P. jirovecii, while patients with CD4+ T cell counts <50/μL
assays can detect as few as one HIV RNA copy per milliliter, while the are also at high risk of disease from CMV, mycobacteria of the M. avium
DNA PCR tests can detect proviral DNA at a frequency of one copy complex (MAC), and/or T. gondii (Fig. 197-32). Once the CD4+ T cell
per 10,000–100,000 cells. Thus, these tests are extremely sensitive. One count is <200/μL, patients should be placed on a regimen for P. jirovecii
frequent consequence of a high degree of sensitivity is some loss of prophylaxis, and once the count is <50/μL, primary prophylaxis for
specificity, and false-positive results have been reported with each of MAC infection is indicated. As with any laboratory measurement,
these techniques. For this reason, a positive EIA with a confirmatory one may wish to obtain two determinations prior to any significant
western blot or HIV RNA assay remains the “gold standard” for a changes in patient management based on CD4+ T cell count alone.
diagnosis of HIV infection, and the interpretation of other test results Patients with HIV infection should have CD4+ T cell measurements
must be done with this in mind. performed at the time of diagnosis and every 3–6 months thereafter.
In the RT-PCR technique, following DNAse treatment, a cDNA More frequent measurements should be made if a declining trend is
copy is made of all RNA species present in plasma. Because HIV is an noted. For patients who have been on cART for at least 2 years with
RNA virus, this will result in the production of DNA copies of the HIV HIV RNA levels persistently <50 copies/mL and CD4 counts >500/μl,
genome in amounts proportional to the amount of HIV RNA present in the monitoring of the CD4 count is felt by many to be optional. There
plasma. This cDNA is then amplified and characterized using standard are a handful of clinical situations in which the CD4+ T cell count
PCR techniques, employing primer pairs that can distinguish genomic may be misleading. Patients with HTLV-1/HIV co-infection may have
cDNA from messenger cDNA. The bDNA assay involves the use of elevated CD4+ T cell counts that do not accurately reflect their degree
a solid-phase nucleic acid capture system and signal amplification of immune competence. In patients with hypersplenism or those who
through successive nucleic acid hybridizations to detect small quanti- have undergone splenectomy, and in patients receiving medications
ties of HIV RNA. Both tests can achieve a tenfold increase in sensitivity that suppress the bone marrow such as IFN-α, the CD4+ T cell per-
to 40–50 copies of HIV RNA per milliliter with a preconcentration centage may be a more reliable indication of immune function than the
step in which plasma undergoes ultracentrifugation to pellet the viral CD4+ T cell count. A CD4+ T cell percentage of 15 is comparable to a
particles. In the TMA assay, a cDNA copy of viral RNA is made using CD4+ T cell count of 200/μL.
primers that contain a promoter sequence for T7 RNA polymerase. T7
polymerase is then added to produce multiple copies of RNA ampli- HIV RNA Determinations Facilitated by highly sensitive tech-
con from the DNA template. It is qualified at 100 copies/mL. The niques for the precise quantitation of small amounts of nucleic acids,
NASBA technique involves the isothermal amplification of a sequence the measurement of serum or plasma levels of HIV RNA has become an
within the gag region of HIV in the presence of internal standards and essential component in the monitoring of patients with HIV infection. As
employs the production of multiple RNA copies through the action discussed in “Diagnosis of HIV Infection,” above, the most commonly
of T7-RNA polymerase. The resulting RNA species are quantitated used technique is the RT-PCR assay. This assay generates data in the
through hybridization with a molecular beacon DNA probe that is form of number of copies of HIV RNA per milliliter of serum or plasma
quenched in the absence of hybridization. The lower limit of detection and can reliably detect as few as 40 copies of HIV RNA per milliliter of
for the NucliSENS assay is 80 copies/mL. plasma. Research-based assays can detect down to one copy per milli-
In addition to being a diagnostic and prognostic tool, RT-PCR and liter. While it is common practice to describe levels of HIV RNA below
DNA-PCR are also useful for amplifying defined areas of the HIV these cut-offs as “undetectable,” this is a term that should be avoided as
genome for sequence analysis and have become an important technique it is imprecise and leaves the false impression that the level of virus is
for studies of sequence diversity and microbial resistance to antiretrovi- 0. By utilizing more sensitive, nested PCR techniques and by studying
ral agents. In patients with a positive or indeterminate EIA test and an tissue levels of virus as well as plasma levels, HIV RNA can be detected
indeterminate western blot, and in patients in whom serologic testing in virtually every patient with HIV infection. The one notable exception
may be unreliable (such as patients with hypogammaglobulinemia or to this is a patient who underwent cytoreductive therapy followed by a
advanced HIV disease), these tests for quantitating HIV RNA in plasma bone marrow transplant from a CCR5∆32 homozygous donor.
Harrisons_20e_Part5_p0859-p1648.indd 1427 6/1/18 12:08 PM
1428
300
CD4 (cells/µL3)
*
200
*
100
* *
* * * * * *
* * * * *
0
HSV HZos Crp KS Cry Ca n PCP NHL DEM PML WS Tox CMV PCP2 MAC
Opportunistic illness
FIGURE 197-32 Relationship between CD4+ T cell counts and the development of opportunistic diseases. Boxplot of the median (line inside the box), first quartile
(bottom of the box), third quartile (top of the box), and mean (asterisk) CD4+ lymphocyte count at the time of the development of opportunistic disease. Can, candidal
esophagitis; CMV, cytomegalovirus infection; Crp, cryptosporidiosis; Cry, cryptococcal meningitis; DEM, AIDS dementia complex; HSV, herpes simplex virus infection;
HZos, herpes zoster; KS, Kaposi’s sarcoma; MAC, Mycobacterium avium complex bacteremia; NHL, non-Hodgkin’s lymphoma; PCP, primary Pneumocystis jirovecii
pneumonia; PCP2, secondary P. jirovecii pneumonia; PML, progressive multifocal leukoencephalopathy; Tox, Toxoplasma gondii encephalitis; WS, wasting syndrome.
(From RD Moore, RE Chaisson: Ann Intern Med 124:633, 1996.)
Measurements of changes in HIV RNA levels over time have been of hands of experts, resistance testing enhances the short-term ability to
great value in delineating the relationship between levels of virus and decrease viral load by ~0.5 log compared with changing drugs merely
rates of disease progression (Fig. 197-22), the rates of viral turnover, the on the basis of drug history. In addition to the use of resistance testing
relationship between immune system activation and viral replication, to help in the selection of new drugs in patients with virologic failure,
and the time to development of drug resistance. HIV RNA measure- it may also be of value in selecting an initial regimen for treatment of
PART 5
ments are greatly influenced by the state of activation of the immune therapy-naïve individuals. This is particularly true in geographic areas
system and may fluctuate greatly in the setting of secondary infections with a high level of background resistance. The patient needs to have
or immunization. For these reasons, decisions based on HIV RNA lev- an HIV-1 RNA level above 500–1000 copies/mL for an accurate resis-
els should never be made on a single determination. Measurements of tance determination. Resistance assays lose their consistency at lower
Infectious Diseases
plasma HIV RNA levels should be made at the time of HIV diagnosis levels of plasma viremia.
and every 3–6 months thereafter in the untreated patient. Following the
initiation of therapy or any change in therapy, plasma HIV RNA levels Co-Receptor Tropism Assays Following the licensure of mara-
should be monitored approximately every 4 weeks until the effective- viroc as the first CCR5 antagonist for the treatment of HIV infection (see
ness of the therapeutic regimen is determined by the development of below), it became necessary to be able to determine whether a patient’s
a new steady-state level of HIV RNA. In most instances of effective virus was likely to respond to this treatment. Patients tend to have CCR5-
antiretroviral therapy the plasma level of HIV RNA will drop to <50 tropic virus early in the course of infection, with a trend toward CXCR4
copies/mL within 6 months of the initiation of treatment. During ther- viruses later in disease. The antiretroviral agent maraviroc is effective
apy, levels of HIV RNA should be monitored every 3–6 months to only against CCR5-tropic viruses. Because the genotypic determinants
evaluate the continuing effectiveness of therapy. of cellular tropism are poorly defined, a phenotypic assay is necessary to
determine this property of HIV. Two commercial assays, the Trofile assay
HIV Resistance Testing The availability of multiple antiretrovi- (Monogram Biosciences) and the Phenoscript assay (VIRalliance), are
ral drugs as treatment options has generated a great deal of interest in available to make this determination. These assays clone the envelope
the potential for measuring the sensitivity of an individual’s HIV viral regions of the patient’s virus into an indicator virus that is then used to
quasispecies to different antiretroviral agents. HIV resistance testing infect target cells expressing either CCR5 or CXCR4 as their co-receptor.
can be done through either genotypic or phenotypic measurements. In These assays take weeks to perform and are expensive. Another, less
the genotypic assays, sequence analyses of the HIV genomes obtained costly option is to obtain a genotypic assay of the V3 region of HIV-1
from patients are compared with sequences of viruses with known and then employ a computer algorithm to predict viral tropism from the
antiretroviral resistance profiles. In the phenotypic assays, the in vivo sequence. While this approach is less expensive than the classic pheno-
growth of viral isolates obtained from the patient is compared with the typic assay, there are fewer data to validate its predictive value.
growth of reference strains of the virus in the presence or absence of dif-
ferent antiretroviral drugs. A modification of this phenotypic approach Other Tests A variety of other laboratory tests have been studied
utilizes a comparison of the enzymatic activities of the reverse tran- as potential markers of HIV disease activity. Among these are quan-
scriptase, protease, or integrase genes obtained by molecular cloning titative culture of replication-competent HIV from plasma, peripheral
of patients’ isolates to the enzymatic activities of genes obtained from blood mononuclear cells, or resting memory CD4+ T cells; circu-
reference strains of HIV in the presence or absence of different drugs lating levels of β2-microglobulin, soluble IL-2 receptor, IgA, acid-labile
targeted to these genes. These tests are quite good in identifying those endogenous IFN, or TNF-α; and the presence or absence of activation
antiretroviral agents that have been utilized in the past and suggesting markers such as CD38, HLA-DR, and PD-1 on CD4+ or CD8+ T cells.
agents that may be of future value in a given patient. Resistance testing Nonspecific serologic markers of inflammation and/or coagulation
is recommended at the time of initial diagnosis and, if therapy is not such as IL-6, d-dimer, and sCD14 have been shown to have a high
initiated at that time, at the time of initiation of cART. Drug resistance correlation with all-cause mortality (Table 197-9). While these mea-
testing is also indicated in the setting of virologic failure and should surements have value as markers of disease activity and help to
be performed while the patient is still on the failing regimen because increase our understanding of the pathogenesis of HIV disease, they
of the propensity for the pool of HIV quasispecies to rapidly revert do not currently play a major role in the monitoring of patients with
to wild-type in the absence of the selective pressures of cART. In the HIV infection.
Harrisons_20e_Part5_p0859-p1648.indd 1428 6/1/18 12:08 PM
TABLE 197-9 Association Between High-Sensitivity CRP, Il-6, and TABLE 197-10 Clinical Findings in the Acute HIV Syndrome 1429
D-Dimer with All-Cause Mortality in Patients with HIV Infection General Neurologic
UNADJUSTED ADJUSTED Fever Meningitis
ODDS RATIO ODDS RATIO Pharyngitis Encephalitis
MARKER (FOURTH/FIRST) P (FOURTH/FIRST) P Lymphadenopathy Peripheral neuropathy
Hs-CRP 2.0 .05 2.8 .03 Headache/retroorbital pain Myelopathy
IL-6 8.3 <.0001 11.8 <.0001 Arthralgias/myalgias Dermatologic
D-dimer 12.4 <.0001 26.5 <.0001 Lethargy/malaise Erythematous maculopapular rash
Abbreviations: Hs-CRP, high-sensitivity C-reactive protein; IL-6, interleukin 6. Anorexia/weight loss Mucocutaneous ulceration
Source: From LH Kuller et al: PLoS Med 5:e203, 2008. Nausea/vomiting/diarrhea
Source: From B Tindall, DA Cooper: AIDS 5:1, 1991.
CLINICAL MANIFESTATIONS
The clinical consequences of HIV infection encompass a spectrum develops and the levels of plasma viremia decrease. Opportunistic
ranging from an acute syndrome associated with primary infection to a infections have been reported during this stage of infection, reflecting
prolonged asymptomatic state to advanced disease. It is best to regard the immunodeficiency that results from reduced numbers of CD4+
HIV disease as beginning at the time of primary infection and progress- T cells and likely also from the dysfunction of CD4+ T cells owing
ing through various stages. As mentioned above, active virus replica- to viral protein and endogenous cytokine-induced perturbations of
tion and progressive immunologic impairment occur throughout the cells (Table 197-5) associated with the extremely high levels of plasma
course of HIV infection in most patients. With the exception of the rare, viremia. The Fiebig staging system has been used to describe the dif-
true, “elite” virus controllers or long-term nonprogressors (see “Long- ferent stages of acute HIV infection, ranging from Stage 1 (HIV RNA
Term Survivors, Long-Term Nonprogressors, and Elite Controllers,” positive alone) to Stage VI (HIV RNA and full western blot positive).
above), HIV disease in untreated patients inexorably progresses even A number of immunologic abnormalities accompany the acute HIV
during the clinically latent stage. Since the mid-1990s, cART has had a syndrome, including multiphasic perturbations of the numbers of
major impact on preventing and reversing the progression of disease circulating lymphocyte subsets. The number of total lymphocytes and
over extended periods of time in a substantial proportion of adequately T cell subsets (CD4+ and CD8+) are initially reduced. An inversion of
treated patients. Today, a person diagnosed with HIV infection and the CD4+/CD8+ T cell ratio occurs later because of a rise in the number
treated with cART has a close to normal life expectancy. of CD8+ T cells. In fact, there may be a selective and transient expan-
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
sion of CD8+ T cell subsets, as determined by T cell receptor analysis
■ ACUTE HIV INFECTION (see above). The total circulating CD8+ T cell count may remain ele-
It is estimated that 50–70% of individuals with HIV infection experi- vated or return to normal; however, CD4+ T cell levels usually remain
ence an acute clinical syndrome ~3–6 weeks after primary infection somewhat depressed, although there may be a slight rebound toward
(Fig. 197-33). Varying degrees of clinical severity have been reported, normal. Lymphadenopathy occurs in ~70% of individuals with pri-
and although it has been suggested that symptomatic seroconversion mary HIV infection. Most patients recover spontaneously from this
leading to the seeking of medical attention indicates an increased syndrome and many are left with only a mildly depressed CD4+ T cell
risk for an accelerated course of disease, there does not appear to be count that remains stable for a variable period before beginning its pro-
a correlation between the level of the initial burst of viremia in acute gressive decline; in some individuals, the CD4+ T cell count returns to
HIV infection and the subsequent course of disease. The typical clin- the normal range. Approximately 10% of patients manifest a fulminant
ical findings in the acute HIV syndrome are listed in Table 197-10; course of immunologic and clinical deterioration after primary infec-
they occur along with a burst of plasma viremia. It has been reported tion, even after the disappearance of initial symptoms. In most patients,
that several symptoms of the acute HIV syndrome (fever, skin rash, primary infection with or without the acute syndrome is followed by a
pharyngitis, and myalgia) occur less frequently in those infected by prolonged period of clinical latency or smoldering low disease activity.
injection drug use compared with those infected by sexual contact. The
syndrome is typical of an acute viral syndrome and has been likened ■ THE ASYMPTOMATIC STAGE—CLINICAL LATENCY
to acute infectious mononucleosis. Symptoms usually persist for one Although the length of time from initial infection to the development of
to several weeks and gradually subside as an immune response to HIV clinical disease varies greatly, the median time for untreated patients is
~10 years. As emphasized above, HIV disease with active virus replica-
tion is ongoing and progressive during this asymptomatic period. The
SUMMARY OF THE ACUTE HIV SYNDROME rate of disease progression is directly correlated with HIV RNA levels.
Patients with high levels of HIV RNA in plasma progress to symptomatic
Primary Infection disease faster than do patients with low levels of HIV RNA (Fig.
3–6 weeks 197-22). Some patients referred to as long-term nonprogressors show little
if any decline in CD4+ T cell counts over extended periods of time.
Plasma viremia Acute Retrafficking of These patients generally have extremely low levels of HIV RNA; a sub-
(wide dissemination syndrome lymphocytes set, referred to as elite nonprogressors, exhibits HIV RNA levels <50 copies/
of virus)
mL. Certain other patients remain entirely asymptomatic despite the
1 week–3 months fact that their CD4+ T cell counts show a steady progressive decline to
extremely low levels. In these patients, the appearance of an opportu-
Immune response to HIV nistic disease may be the first manifestation of HIV infection. During the
asymptomatic period of HIV infection, the average rate of CD4+ T cell
Curtailment Establishment of
of plasma decline is ~50/μL per year in an untreated patient. When the CD4+ T
chronic, persistent
viremia 1–2 weeks cell count falls to <200/μL, the resulting state of immunodeficiency is
infection in
lymphoid tissue severe enough to place the patient at high risk for opportunistic infec-
tions and neoplasms and, hence, for clinically apparent disease.
Clinical latency
■ SYMPTOMATIC DISEASE
FIGURE 197-33 The acute HIV syndrome. See text for detailed description.
Symptoms of HIV disease can appear at any time during the course of
(Adapted from G Pantaleo et al: N Engl J Med 328:327, 1993. Copyright 1993 HIV infection. Generally speaking, the spectrum of illnesses that one
Massachusetts Medical Society. All rights reserved.) observes changes as the CD4+ T cell count declines. The more severe
Harrisons_20e_Part5_p0859-p1648.indd 1429 6/1/18 12:08 PM
1430 and life-threatening complications of HIV infection occur in patients Patients with untreated HIV infection have a sixfold increase in the
with CD4+ T cell counts <200/μL. A diagnosis of AIDS is made in any incidence of pneumococcal pneumonia and a 100-fold increase in the
individual age 6 years and older with HIV infection and a CD4+ T cell incidence of pneumococcal bacteremia. Pneumococcal disease may be
count <200/μL (Stage 3, Table 197-2) and in anyone with HIV infection seen in patients with relatively intact immune systems. In one study,
who develops one of the HIV-associated diseases considered to be the baseline CD4+ T cell count at the time of a first episode of pneumo-
indicative of a severe defect in cell-mediated immunity (Table 197-1). coccal pneumonia was ~300/μL. Of interest is the fact that the inflam-
While the causative agents of the secondary infections are characteristi- matory response to pneumococcal infection appears proportional to
cally opportunistic organisms such as P. jirovecii, atypical mycobacteria, the CD4+ T cell count. Due to this high risk of pneumococcal disease,
CMV, and other organisms that do not ordinarily cause disease in the immunization with the conjugated pneumococcal vaccine followed
absence of a compromised immune system, they also include several by booster immunization with the 23-valent pneumococcal polysac-
common bacterial and mycobacterial pathogens. Following the wide- charide vaccine is one of the generally recommended prophylactic
spread use of cART and implementation of guidelines for the preven- measures for patients with HIV infection. This is likely most effective if
tion of opportunistic infections (Table 197-11), the incidence of these given while the CD4+ T cell count is >200/μL and, if given to patients
secondary infections has decreased dramatically (Fig. 197-34). Overall, with lower CD4+ T cell counts, should be repeated once the count has
the clinical spectrum of HIV disease is constantly changing as patients been above 200 for 6 months. Although clear guidelines do not exist, it
live longer and new and better approaches to treatment and prophy- also makes sense to repeat immunization every 5 years. The incidence
laxis are developed. In addition to the classic AIDS-defining illnesses, of bacterial pneumonia is cut in half when patients quit smoking.
patients with HIV infection also have an increase in several serious Pneumocystis pneumonia (PCP), once the hallmark of AIDS, has
non-AIDS illnesses, including non-AIDS related cancers and cardiovas- dramatically declined in incidence following the development of
cular, renal, and hepatic disease. Non-AIDS events dominate the disease effective prophylactic regimens and the widespread use of cART.
burden for patients with HIV infection receiving cART (Table 197-4). It is, however, still the single most common cause of pneumonia in
In developed countries, AIDS-related illnesses are responsible for only patients with HIV infection in the United States and can be identified
~25% of deaths in patients with HIV infection. A similar percentage of as a likely etiologic agent in 25% of cases of pneumonia in patients
deaths are due to non-AIDS-defining malignancies, with cardiovascu- with HIV infection, with an incidence in the range of 2–3 cases per
lar disease and liver disease each accounting for approximately 15% of 100 person-years. Approximately 30% of cases of HIV-associated PCP
deaths. The physician providing care to a patient with HIV infection occur in patients who are unaware of their HIV status. The risk of
must be well versed in general internal medicine as well as HIV-related PCP is greatest among those who have experienced a previous bout
opportunistic diseases. In general, it should be stressed that a key of PCP and those who have CD4+ T cell counts of <200/μL. Overall,
element of treatment of symptomatic complications of HIV disease, 79% of patients with PCP have CD4+ T cell counts <100/μL and 95%
PART 5
whether they are primary or secondary, is achieving good control of of patients have CD4+ T cell counts <200/μL. Recurrent fever, night
HIV replication through the use of cART and instituting primary and sweats, thrush, and unexplained weight loss also are associated with
secondary prophylaxis for opportunistic infections as indicated. an increased incidence of PCP. For these reasons, it is strongly recom-
mended that all patients with CD4+ T cell counts <200/μL (or a CD4
Diseases of the Respiratory System Acute bronchitis and percentage <15) receive some form of PCP prophylaxis. The incidence
Infectious Diseases
sinusitis are prevalent during all stages of HIV infection. The most of PCP is approaching zero in patients with known HIV infection
severe cases tend to occur in patients with lower CD4+ T cell counts. receiving appropriate cART and prophylaxis. In the United States,
Sinusitis presents as fever, nasal congestion, and headache. The diag- primary PCP is now occurring at a median CD4+ T cell count of 36/μL,
nosis is made by CT or MRI. The maxillary sinuses are most commonly while secondary PCP is occurring at a median CD4+ T cell count of
involved; however, disease is also frequently seen in the ethmoid, 10/μL. Patients with PCP generally present with fever and a cough
sphenoid, and frontal sinuses. While some patients may improve with- that is usually nonproductive or productive of only scant amounts of
out antibiotic therapy, radiographic improvement is quicker and more white sputum. They may complain of a characteristic retrosternal chest
pronounced in patients who have received antimicrobial therapy. It is pain that is worse on inspiration and is described as sharp or burning.
postulated that this high incidence of sinusitis results from an increased HIV-associated PCP may have an indolent course characterized by
frequency of infection with encapsulated organisms such as H. influenzae weeks of vague symptoms and should be included in the differential
and Streptococcus pneumoniae. In patients with low CD4+ T cell counts diagnosis of fever, pulmonary complaints, or unexplained weight loss
one may see mucormycosis infections of the sinuses. In contrast to the in any patient with HIV infection and <200 CD4+ T cells/μL. The most
course of this infection in other patient populations, mucormycosis of common finding on chest x-ray is either a normal film, if the disease
the sinuses in patients with HIV infection may progress more slowly. In is suspected early, or a faint bilateral interstitial infiltrate. The classic
this setting aggressive, frequent local debridement in addition to local finding of a dense perihilar infiltrate is unusual in patients with AIDS.
and systemic amphotericin B may result in effective treatment. In patients with PCP who have been receiving aerosolized pentamidine
Pulmonary disease is one of the most frequent complications of HIV for prophylaxis, one may see an x-ray picture of upper lobe cavitary
infection. The most common manifestation of pulmonary disease is disease, reminiscent of TB. Other less common findings on chest x-ray
pneumonia. Three of the 10 most common AIDS-defining illnesses are include lobar infiltrates and pleural effusions. Thin-section CT may
recurrent bacterial pneumonia, tuberculosis, and pneumonia due to the demonstrate a patchy ground-glass appearance. Routine laboratory
unicellular fungus P. jirovecii. Other major causes of pulmonary infil- evaluation is usually of little help in the differential diagnosis of PCP.
trates include other mycobacterial infections, other fungal infections, A mild leukocytosis is common, although this may not be obvious in
nonspecific interstitial pneumonitis, KS, and lymphoma. patients with prior neutropenia. Elevation of lactate dehydrogenase is
Bacterial pneumonia is seen with an increased frequency in patients common. Arterial blood-gases may indicate hypoxemia with a decline
with HIV infection, with 0.8–2.0 cases per 100 person-years. Patients in Pao2 and an increase in the arterial-alveolar (a–a) gradient. Arterial
with HIV infection are particularly prone to infections with encapsu- blood-gas measurements not only aid in making the diagnosis of PCP
lated organisms. S. pneumoniae (Chap. 141) and H. influenzae (Chap. but also provide important information for staging the severity of the
152) are responsible for most cases of bacterial pneumonia in patients disease and directing treatment (see below). A definitive diagnosis of
with AIDS. This may be a consequence of altered B cell function and/ PCP requires demonstration of the organism in samples obtained from
or defects in neutrophil function that may be secondary to HIV disease induced sputum, bronchoalveolar lavage, transbronchial biopsy, or
(see above). Pneumonias due to S. aureus (Chap. 142) and P. aeruginosa open-lung biopsy. PCR has been used to detect specific DNA sequences
(Chap. 159) also are reported to occur with an increased frequency in for P. jirovecii in clinical specimens where histologic examinations have
patients with HIV infection. S. pneumoniae (pneumococcal) infection failed to make a diagnosis.
may be the earliest serious infection to occur in patients with HIV In addition to pneumonia, a number of other clinical problems
disease. This can present as pneumonia, sinusitis, and/or bacteremia. have been reported in HIV-infected patients as a result of infection
Harrisons_20e_Part5_p0859-p1648.indd 1430 6/1/18 12:08 PM
TABLE 197-11 NIH/CDC/IDSA 2013 Guidelines for the Prevention of Opportunistic Infections in Persons Infected with HIV 1431
PATHOGEN INDICATIONS FIRST CHOICE(S) ALTERNATIVES
Recommended as Standard of Care for Primary and Secondary Prophylaxis
Pneumocystis jirovecii CD4+ T cell count <200/μL Trimethoprim-sulfamethoxazole Dapsone 50 mg bid PO or 100 mg/d PO
or (TMP-SMX), 1 DS tablet qd PO or
Oropharyngeal candidiasis or Dapsone 50 mg/d PO +
or TMP-SMX, 1 SS tablet qd PO Pyrimethamine 50 mg/week PO +
Prior bout of PCP Leucovorin 25 mg/week PO
or
(Dapsone 200 mg PO +
Pyrimethamine 75 mg PO +
Leucovorin 25 mg weekly PO)
or
Aerosolized pentamidine, 300 mg via
Respirgard II nebulizer every month
or
Atovaquone 1500 mg/d PO
or
TMP-SMX 1 DS tablet 3×/week PO
May stop prophylaxis if CD4+ T cell count >200/
μL for ≥3 months
Mycobacterium tuberculosis
Isoniazid sensitive Skin test >5 mm (Isoniazid 300 mg PO + Rifabutin (dose adjusted based on cART
or Pyridoxine 25 mg PO) qd × regimen) or rifampin 600 mg PO qd ×
9 months 4 months
Positive IFN-γ release assay
or or
Isoniazid 900 mg PO twice weekly
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
Prior positive test without treatment
or + Pyridoxine 25 mg PO daily
Close contact with case of active pulmonary TB × 9 months
Same with high probability of exposure to drug-
resistant TB
Drug resistant Consult local public health authorities
Mycobacterium-avium CD4+ T cell count <50/μL Azithromycin 1200 mg weekly PO Rifabutin (dose adjusted based on cART
complex or 600 mg twice weekly PO regimen)
or
Clarithromycin 500 mg bid PO
Prior documented disseminated disease Clarithromycin 500 mg bid PO + Azithromycin 500–600 mg/d PO +
Ethambutol 15 (mg/kg)/d PO Ethambutol 15 (mg/kg)/d PO
May stop prophylaxis if CD4+ T cell count
>100/μL for ≥6 months
Toxoplasma gondii TOXO IgG antibody positive and CD4+ T cell count TMP-SMX 1 DS tablet PO qd TMP-SMX 1 DS 3× weekly PO
<100/μL or
TMP-SMX, 1 SS PO daily
or
Dapsone 50 mg/d PO +
Pyrimethamine 50 mg weekly PO +
Leucovorin 25 mg weekly PO
or
(Dapsone 200 mg PO +
Pyrimethamine 75 mg PO +
Leucovorin 25 mg PO) weekly
or
Atovaquone 1500 mg PO daily ±
(Pyrimethamine 25 mg PO +
Leucovorin 10 mg PO) daily
Prior toxoplasmic encephalitis and CD4+ T cell Sulfadiazine 2000–4000 mg in Clindamycin 600 mg q8h PO +
count <200/μL 2–4 divided doses daily PO + Pyrimethamine 25–50 mg/d PO +
Pyrimethamine 25–50 mg/d PO + Leucovorin 10–25 mg/d PO
Leucovorin 10–25 mg/d PO or
TMP-SMX 1 DS tablet bid
or
Atovaquone 750–1500 mg PO bid ±
(Pyrimethamine 25 mg/d PO +
Leucovorin 10 mg/d PO) or Sulfadiazine
2000–4000 mg/d (in 2–4 divided doses) PO
(Continued)
Harrisons_20e_Part5_p0859-p1648.indd 1431 6/1/18 12:08 PM
1432 TABLE 197-11 NIH/CDC/IDSA 2013 Guidelines for the Prevention of Opportunistic Infections in Persons Infected with HIV (Continued)
PATHOGEN INDICATIONS FIRST CHOICE(S) ALTERNATIVES
Toxoplasma gondii May stop prophylaxis if CD4+ T cell count
>200/μL for ≥3 months
Varicella zoster virus Significant exposure to chickenpox or shingles in Varicella zoster immune globulin, Acyclovir 800 mg PO 5 × day for
a patient with no history of immunization or prior IM, within 10 d of exposure 5–7 days
exposure to either (800-843-7477) or
Valacyclovir 1 g PO tid for 5–7 days
Cryptococcus neoformans Prior documented disease Fluconazole 200 mg/d PO Itraconazole 200 mg/d PO
May stop prophylaxis if CD4+ T cell count >100/
μL, no evidence of active fungal infection, and HIV
RNA levels <500 copies/mL for >3 months
Histoplasma capsulatum Prior documented disease or CD4+ T cell Itraconazole 200 mg bid PO Fluconazole 400 mg/d PO
count <150μL and high risk (endemic area or
occupational exposure)
May stop prophylaxis after 1 year if CD4+ T
cell count >150/μL and patient on cART for ≥6
months
Coccidioides immitis Prior documented disease or positive serology Fluconazole 400 mg/d PO
and CD4+ T cell count <250/μL if from a disease
endemic area. (For this indication prophylaxis can
be stopped if CD4+
T cell count ≥250 for 6 months.)
Penicillium marneffei Prior documented disease Itraconazole 200 mg/d PO Fluconazole 400 mg PO once weekly
Patients with CD4+T cell counts <100 who live
or stay in northern Thailand, Southern China, or
Vietnam
May stop secondary prophylaxis in patients on
ARV therapy with CD4+ T cell count >100/μL for
≥6 months
PART 5
Salmonella species Prior recurrent bacteremia Ciprofloxacin 500 mg bid PO for
≥6 months
Bartonella Prior infection Doxycycline 200 mg/d PO
or
Infectious Diseases
Azithromycin 1200 mg weekly PO
or
Clarithromycin 500 mg bid PO
May stop if CD4+ T cell count >200/μL for
>3 months
Cytomegalovirus Prior end-organ disease Valganciclovir 900 mg bid PO Cidofovir 5 mg/kg every other week IV +
Probenecid
or
Foscarnet 90–120 (mg/kg)/d IV
May stop prophylaxis if CD4+ T cell count
>100/μL for 6 months and no evidence of active
CMV disease
Restart if prior retinitis and CD4+ T cells
<100/μL
Immunizations Generally Recommended
Hepatitis B virus All susceptible (anti-HBc- and anti-HBs-negative) Hepatitis B vaccine: 3 doses
patients
Hepatitis A virus All susceptible (anti-HAV-negative) patients Hepatitis A vaccine: 2 doses
Influenza virus All patients annually Inactivated trivalent influenza Oseltamivir 75 mg PO qd
virus vaccine 1 dose yearly or
Rimantadine or amantadine 100 mg PO bid
(influenza A only)
Streptococcus pneumoniae All patients, preferably before CD4+ T cell count Pneumococcal conjugated
≤200/μL vaccine (13) 0.5 mL IM × 1
followed in 8 weeks or more by
pneumococcal polysaccharide
vaccine (23) if CD4+ T cell count
>200/μL
Patients initially immunized at a CD4+ T cell Reimmunize
count <100/μL whose CD4+ T cell count then
increases to>200/μL
Human papillomavirus All patients 13–26 years of age HPV vaccine; 3 doses
(Continued)
Harrisons_20e_Part5_p0859-p1648.indd 1432 6/1/18 12:08 PM
TABLE 197-11 NIH/CDC/IDSA 2013 Guidelines for the Prevention of Opportunistic Infections in Persons Infected with HIV (Continued) 1433
PATHOGEN INDICATIONS FIRST CHOICE(S) ALTERNATIVES
Recommended for Prevention of Severe or Frequent Recurrences
Herpes simplex Frequent/severe recurrences Valacyclovir 500 mg bid PO
or
Acyclovir 400 mg bid PO
or
Famciclovir 500 mg bid PO
Candida Frequent/severe recurrences Fluconazole 100–200 mg/d PO Posaconazole 400 mg bid PO
Abbreviations: ARV, antiretroviral; bid, twice daily; cART, combination antiretroviral therapy; DS, double-strength; IM, intramuscular; PCP , Pneumocystis jirovecii
pneumonia; PO, by mouth; qd, daily; SS, single-strength; TB, tuberculosis; tid, three times a day.
with P. jirovecii. Otic involvement may be seen as a primary infection, >35 mmHg, adjunct glucocorticoid therapy should be used in addition
presenting as a polypoid mass involving the external auditory canal. to specific antimicrobials. Overall, treatment should be continued for
In patients receiving aerosolized pentamidine for prophylaxis against 21 days and followed by secondary prophylaxis. Prophylaxis for PCP is
PCP, one may see a variety of extrapulmonary manifestations of indicated for any HIV-infected individual who has experienced a prior
P. jirovecii. These include ophthalmic lesions of the choroid, a necrotiz- bout of PCP, any patient with a CD4+ T cell count of <200/μL or a CD4
ing vasculitis that resembles Buerger disease, bone marrow hypopla- percentage <15, any patient with unexplained fever for >2 weeks, and
sia, and intestinal obstruction. Other organs that have been involved any patient with a recent history of oropharyngeal candidiasis. The
include lymph nodes, spleen, liver, kidney, pancreas, pericardium, preferred regimen for prophylaxis is TMP-SMX, one double-strength
heart, thyroid, and adrenals. Organ infection may be associated with tablet daily. This regimen also provides protection against toxoplasmo-
cystic lesions that may appear calcified on CT or ultrasound. sis and some bacterial respiratory pathogens. For patients who cannot
The standard treatment for PCP or disseminated pneumocystosis tolerate TMP-SMX, alternatives for prophylaxis include dapsone plus
is trimethoprim-sulfamethoxazole (TMP-SMX). A high (20–85%) inci- pyrimethamine plus leucovorin, aerosolized pentamidine administered
dence of side effects, particularly skin rash and bone marrow suppres- by the Respirgard II nebulizer, and atovaquone. Primary or secondary
sion, is seen with TMP-SMX in patients with HIV infection. Alternative prophylaxis for PCP can be discontinued in those patients treated with
treatments for mild to moderate PCP include dapsone/trimethoprim, cART who maintain good suppression of HIV (<50 copies/mL) and
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
clindamycin/primaquine, and atovaquone. IV pentamidine is the CD4+ T cell counts >200/μL for at least 3 months.
treatment of choice for severe disease in the patient unable to tolerate M. tuberculosis, once thought to be on its way to extinction in the
TMP-SMX. For patients with a Pao2 <70 mmHg or with an a–a gradient United States, experienced a resurgence associated with the HIV
epidemic (Chap. 173). Worldwide, approximately one-third of all
12 AIDS-related deaths are associated with TB, and TB is the primary
cause of death for 10–15% of patients with HIV infection. In the United
States ~5% of AIDS patients have active TB. Patients with HIV infection
Incidence/100 person-years
10
Pneumocystis carinii pneumonia
are more likely to have active TB by a factor of 100 when compared
8 Disseminated Mycobacterium avium complex with an HIV-negative population. For an asymptomatic HIV-negative
Esophageal candidiasis
person with a positive purified protein derivative (PPD) skin test, the
6 Cytomegalovirus retinitis risk of reactivation TB is around 1% per year. For the patient with
Kaposi’s sarcoma
untreated HIV infection, a positive PPD skin test, and no signs or symp-
4 toms of TB, the rate of reactivation TB is 7–10% per year. Untreated
Cytomegalovirus disease TB can accelerate the course of HIV infection. Levels of plasma HIV
2 Cryptococcosis
RNA increase in the setting of active TB and decline in the setting
Toxoplasmosis of successful TB treatment. Active TB is most common in patients
0 25–44 years of age, in African Americans and Hispanics, in patients in
1992 1993 1994 1995 1996 1997 1998
New York City and Miami, and in patients in developing countries. In
A Year of observation
these demographic groups, 20–70% of the new cases of active TB are
20 in patients with HIV infection. The epidemic of TB embedded in the
epidemic of HIV infection probably represents the greatest health risk
18 to the general public and the health care profession associated with the
No. of opportunistic infections
16 CMV HIV epidemic. In contrast to infection with atypical mycobacteria such
per 100 person-years
14
PCP as MAC, active TB often develops relatively early in the course of HIV
MAC
infection and may be an early clinical sign of HIV disease. In one study,
12 the median CD4+ T cell count at presentation of TB was 326/μL. The
10 clinical manifestations of TB in HIV-infected patients are quite varied
8
and generally show different patterns as a function of the CD4+ T cell
count. In patients with relatively high CD4+ T cell counts, the typical
6 pattern of pulmonary reactivation occurs: patients present with fever,
4 cough, dyspnea on exertion, weight loss, night sweats, and a chest
x-ray revealing cavitary apical disease of the upper lobes. In patients
2
with lower CD4+ T cell counts, disseminated disease is more common.
0 In these patients the chest x-ray may reveal diffuse or lower-lobe bilat-
B 1995 1996 1997 1998 1999 2000 2001
eral reticulonodular infiltrates consistent with miliary spread, pleural
FIGURE 197-34 A. Decrease in the incidence of opportunistic infections and effusions, and hilar and/or mediastinal adenopathy. Infection may be
Kaposi’s sarcoma in HIV-infected individuals with CD4+ T cell counts <100/μL present in bone, brain, meninges, GI tract, lymph nodes (particularly
from 1992 through 1998. (Adapted and updated from FJ Palella et al: N Engl J
Med 338:853, 1998, and JE Kaplan et al: Clin Infect Dis 30[S1]:S5, 2000, with cervical lymph nodes), and viscera. Some patients with advanced HIV
permission.) B. Quarterly incidence rates of cytomegalovirus (CMV), Pneumocystis infection and active TB may have no symptoms of illness, and thus
jirovecii pneumonia (PCP), and Mycobacterium avium complex (MAC) from 1995 screening for TB should be part of the initial evaluation of every patient
to 2001. (From FJ Palella et al: AIDS 16:1617, 2002.) with HIV infection. Approximately 60–80% of HIV-infected patients
Harrisons_20e_Part5_p0859-p1648.indd 1433 6/1/18 12:08 PM
1434 with TB have pulmonary disease, and 30–40% have extrapulmonary infection. Cultures may take 2 weeks to turn positive. Therapy consists
disease. Respiratory isolation and a negative-pressure room should of a macrolide, usually clarithromycin, with ethambutol. Some physi-
be used for patients in whom a diagnosis of pulmonary TB is being cians elect to add a third drug from among rifabutin, ciprofloxacin, or
considered. This approach is critical to limit nosocomial and commu- amikacin in patients with extensive disease. Therapy is continued until
nity spread of infection. Culture of the organism from an involved site resolution of clinical signs and symptoms, negative cultures, and CD4+
provides a definitive diagnosis. Blood cultures are positive in 15% of T cell counts >100/μL for 3–6 months in the setting of cART. Primary
patients. This figure is higher in patients with lower CD4 +T cell counts. prophylaxis for MAC is indicated in patients with HIV infection and
In the setting of fulminant disease one cannot rely on the accuracy of a CD4+ T cell counts <50/μL (Table 197-11). This may be discontinued in
negative PPD skin test to rule out a diagnosis of TB. In addition, IFN-γ patients in whom cART induces a sustained suppression of viral repli-
release assays may be difficult to interpret due to high backgrounds cation and an increase in CD4+ T cell count to >100/μL for ≥6 months.
as a consequence of HIV-associated immune activation. TB is one of Rhodococcus equi is a gram-positive, pleomorphic, acid-fast, non-
the conditions associated with HIV infection for which cure is possible spore-forming bacillus that can cause pulmonary and/or disseminated
with appropriate therapy. Therapy for TB is generally the same in the infection in patients with advanced HIV infection. Fever and cough
HIV-infected patient as in the HIV-negative patient (Chap. 173). Due are the most common presenting signs. Radiographically one may see
to the possibility of multidrug-resistant or extensively drug-resistant cavitary lesions and consolidation. Blood cultures are often positive.
TB, drug susceptibility testing should be performed to guide therapy. Treatment is based on antimicrobial sensitivity testing.
Due to pharmacokinetic interactions, adjusted doses of rifabutin and/ Fungal infections of the lung, in addition to PCP, can be seen in
or changes in cART are required when treating TB in the setting of HIV patients with AIDS. Patients with pulmonary cryptococcal disease pres-
infection. Treatment is most effective in programs that involve directly ent with fever, cough, dyspnea, and, in some cases, hemoptysis. A focal
observed therapy. Initiation of cART and/or anti-TB therapy may be or diffuse interstitial infiltrate is seen on chest x-ray in >90% of patients.
associated with clinical deterioration due to immune reconstitution In addition, one may see lobar disease, cavitary disease, pleural effu-
inflammatory syndrome (IRIS) reactions. These are most common sions, and hilar or mediastinal adenopathy. More than half of patients
in patients initiating both treatments at the same time, may occur as are fungemic, and 90% of patients have concomitant CNS infection.
early as 1 week after initiation of cART therapy, and are seen more Coccidioides immitis is a mold that is endemic in the southwest United
frequently in patients with advanced HIV disease. For these reasons States. It can cause a reactivation pulmonary syndrome in patients
it is recommended that initiation of cART be delayed in antiretrovi- with HIV infection. Most patients with this condition will have CD4+
ral-naïve patients with CD4 counts >50 cells/μL until 2–4 weeks T cell counts <250/μL. Patients present with fever, weight loss, cough,
following the initiation of treatment for TB. For patients with lower and extensive, diffuse reticulonodular infiltrates on chest x-ray. One
CD4 counts the benefits of more immediate cART outweigh the risks of may also see nodules, cavities, pleural effusions, and hilar adenopathy.
PART 5
IRIS, and cART should be started as soon as possible in those patients. While serologic testing is of value in the immunocompetent host, serol-
Effective prevention of active TB can be a reality if the health care ogies are negative in 25% of HIV-infected patients with coccidioidal
professional is aggressive in looking for evidence of latent or active TB infection. Invasive aspergillosis is not an AIDS-defining illness and is
by making sure that all patients with HIV infection receive a PPD skin generally not seen in patients with AIDS in the absence of neutropenia
test or evaluation with an IFN-γ release assay. Anergy testing is not or administration of glucocorticoids. When it does occur, Aspergillus
Infectious Diseases
of value in this setting. Since these tests rely on the host mounting an infection may have an unusual presentation in the respiratory tract of
immune response to M. tuberculosis, patients with CD4+ T cell counts patients with AIDS, where it gives the appearance of a pseudomem-
<200 cells/μL should be retested if their CD4+ T cell counts rise to per- branous tracheobronchitis. Primary pulmonary infection of the lung
sistently above 200. Patients at risk of continued exposure to TB should may be seen with histoplasmosis. The most common pulmonary mani-
be tested annually. HIV-infected individuals with a skin-test reaction of festation of histoplasmosis, however, is in the setting of disseminated
>5 mm, those with a positive IFN-γ release assay, or those who are close disease, presumably due to reactivation. In this setting respiratory
household contacts of persons with active TB should receive treatment symptoms are usually minimal, with cough and dyspnea occurring in
with 9 months of isoniazid and pyridoxine. 10–30% of patients. The chest x-ray is abnormal in ~50% of patients,
Atypical mycobacterial infections are also seen with an increased showing either a diffuse interstitial infiltrate or diffuse small nodules,
frequency in patients with HIV infection. Infections with at least 12 and the urine will often be positive for Histoplasma antigen.
different mycobacteria have been reported, including M. bovis and Two forms of idiopathic interstitial pneumonia have been identified in
representatives of all four Runyon groups. The most common atypical patients with HIV infection: lymphoid interstitial pneumonitis (LIP)
mycobacterial infection is with M. avium or M. intracellulare species— and nonspecific interstitial pneumonitis (NIP). LIP, a common finding
the Mycobacterium avium complex (MAC). Infections with MAC are in children, is seen in about 1% of adult patients with untreated HIV
seen mainly in patients in the United States and are rare in Africa. It infection. This disorder is characterized by a benign infiltrate of the lung
has been suggested that prior infection with M. tuberculosis decreases and is thought to be part of the polyclonal activation of lymphocytes
the risk of MAC infection. MAC infections probably arise from organ- seen in the context of HIV and EBV infections. Transbronchial biopsy
isms that are ubiquitous in the environment, including both soil and is diagnostic in 50% of the cases, with an open-lung biopsy required
water. There is little evidence for person-to-person transmission of for diagnosis in the remainder of cases. This condition is generally
MAC infection. The presumed portals of entry are the respiratory and self-limited and no specific treatment is necessary. Severe cases have
GI tracts. MAC infection is a late complication of HIV infection, occur- been managed with brief courses of glucocorticoids. Although rarely a
ring predominantly in patients with CD4+ T cell counts of <50/μL. clinical problem since the use of cART, evidence of NIP may be seen in
The average CD4+ T cell count at the time of diagnosis is 10/μL. The up to half of all patients with untreated HIV infection. Histologically,
most common presentation is disseminated disease with fever, weight interstitial infiltrates of lymphocytes and plasma cells in a perivascular
loss, and night sweats. At least 85% of patients with MAC infection and peribronchial distribution are present. When symptomatic, patients
are mycobacteremic, and large numbers of organisms can often be present with fever and nonproductive cough occasionally accompanied
demonstrated on bone marrow biopsy. The chest x-ray is abnormal by mild chest discomfort. Chest x-ray is usually normal or may reveal a
in ~25% of patients, with the most common pattern being that of a faint interstitial pattern. Similar to LIP, NIP is a self-limited process for
bilateral, lower-lobe infiltrate suggestive of miliary spread. Alveolar or which no therapy is indicated other than appropriate management of
nodular infiltrates and hilar and/or mediastinal adenopathy also can the underlying HIV infection. HIV-related pulmonary arterial hyperten-
occur. Other clinical findings include endobronchial lesions, abdom- sion (HIV-PAH) is seen in ~0.5% of HIV-infected individuals. Patients
inal pain, diarrhea, and lymphadenopathy. Anemia and elevated may present with an array of symptoms including shortness of breath,
liver alkaline phosphatase are common. The diagnosis is made by the fatigue, syncope, chest pain, and signs of right-sided heart failure. Chest
culture of blood or involved tissue. The finding of two consecutive x-ray reveals dilated pulmonary vessels and right-sided cardiomegaly
sputum samples positive for MAC is highly suggestive of pulmonary with right ventricular hypertrophy seen on electrocardiogram. cART
Harrisons_20e_Part5_p0859-p1648.indd 1434 6/1/18 12:08 PM
does not appear to be of clear benefit, and the prognosis is quite poor immunologic decline; they generally occur in patients with CD4+ 1435
with a median survival in the range of 2 years. T cell counts of <300/μL. In one study, 59% of patients with oral can-
Neoplastic diseases of the lung including KS and lymphoma are dis- didiasis went on to develop AIDS in the next year. Thrush appears
cussed below in the section on neoplastic diseases. as a white, cheesy exudate, often on an erythematous mucosa in the
posterior oropharynx. While most commonly seen on the soft palate,
Diseases of the Cardiovascular System Heart disease is
early lesions are often found along the gingival border. The diagnosis is
a relatively common postmortem finding in HIV-infected patients
made by direct examination of a scraping for pseudohyphal elements.
(25–75% in autopsy series). The most common form of heart disease
Culturing is of no diagnostic value, as patients with HIV infection may
is coronary heart disease. In one large series the overall rate of myo-
have a positive throat culture for Candida in the absence of thrush.
cardial infarction (MI) was 3.5/1000 patient-years, 28% of these events
Oral hairy leukoplakia presents as white, frondlike lesions, generally
were fatal, and MI was responsible for 7% of all deaths in the cohort. In
along the lateral borders of the tongue and sometimes on the adjacent
patients with HIV infection, cardiovascular disease may be associated
buccal mucosa (Fig. 197-35). Despite its name, oral hairy leukoplakia is
with classic risk factors such as smoking, a direct consequence of HIV
not considered a premalignant condition. Lesions are associated with
infection, or a complication of cART. Patients with HIV infection have
florid replication of EBV. While usually more disconcerting as a sign
higher levels of triglycerides, lower levels of high-density lipoprotein
of HIV-associated immunodeficiency than a clinical problem in need
cholesterol, and a higher prevalence of smoking than cohorts of indi-
of treatment, severe cases have been reported to respond to topical
viduals without HIV infection. The finding that the rate of cardiovascu-
podophyllin or systemic therapy with anti-herpesvirus agents. Aph-
lar disease events was lower in patients on antiretroviral therapy than
thous ulcers of the posterior oropharynx also are seen with regularity
in those randomized to undergo a treatment interruption identified a
in patients with untreated HIV infection (Fig. 197-35). These lesions
clear association between HIV replication and risk of cardiovascular
are of unknown etiology and can be quite painful and interfere with
disease. In one study, a baseline CD4+ T cell count of <500/μL was
swallowing. Topical anesthetics provide immediate symptomatic relief
found to be an independent risk factor for cardiovascular disease com-
of short duration. The fact that thalidomide is an effective treatment for
parable in magnitude to that attributable to smoking. While the precise
this condition suggests that the pathogenesis may involve the action
pathogenesis of this association remains unclear, it is likely related to
of tissue-destructive cytokines. Palatal, glossal, or gingival ulcers may
the immune activation and increased propensity for coagulation seen
also result from cryptococcal disease or histoplasmosis.
as a consequence of HIV replication. Exposure to HIV protease inhib-
Esophagitis (Fig. 197-36) may present with odynophagia and retros-
itors and certain reverse transcriptase inhibitors has been associated
ternal pain. Upper endoscopy is generally required to make an accurate
with increases in total cholesterol and/or risk of MI. Any increases in
diagnosis. Esophagitis may be due to Candida, CMV, or HSV. While CMV
the risk of death from MI resulting from the use of certain antiretrovi-
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
tends to be associated with a single large ulcer, HSV infection is more often
rals must be balanced against the marked increases in overall survival
associated with multiple small ulcers. The esophagus may also be the site
brought about by these drugs.
of KS and lymphoma. Like the oral mucosa, the esophageal mucosa may
Another form of heart disease associated with HIV infection is a
have large, painful ulcers of unclear etiology that may respond to thalid-
dilated cardiomyopathy associated with congestive heart failure (CHF)
omide. While achlorhydria is a common problem in patients with HIV
referred to as HIV-associated cardiomyopathy. This generally occurs as a
infection, other gastric problems are generally rare. Among the neoplastic
late complication of HIV infection and, histologically, displays elements
conditions involving the stomach are KS and lymphoma.
of myocarditis. For this reason some have advocated treatment with IV
Infections of the small and large intestine leading to diarrhea,
immunoglobulin (IVIg). HIV can be directly demonstrated in cardiac
abdominal pain, and occasionally fever are among the most significant
tissue in this setting, and there is debate over whether it plays a direct
GI problems in HIV-infected patients. They include infections with
role in this condition. Patients present with typical findings of CHF
bacteria, protozoa, and viruses.
including edema and shortness of breath. Patients with HIV infection
Bacteria may be responsible for secondary infections of the GI tract.
may also develop cardiomyopathy as side effects of IFN-α or nucleo-
Infections with enteric pathogens such as Salmonella, Shigella, and
side analogue therapy. These are reversible once therapy is stopped.
Campylobacter are more common in men who have sex with men and
KS, cryptococcosis, Chagas’ disease, and toxoplasmosis can involve the
are often more severe and more apt to relapse in patients with HIV
myocardium, leading to cardiomyopathy. In one series, most patients
infection. Patients with untreated HIV have approximately a 20-fold
with HIV infection and a treatable myocarditis were found to have
increased risk of infection with S. typhimurium. They may present with
myocarditis associated with toxoplasmosis. Most of these patients
a variety of nonspecific symptoms including fever, anorexia, fatigue,
also had evidence of CNS toxoplasmosis. Thus, MRI or double-dose
and malaise of several weeks’ duration. Diarrhea is common but may
contrast CT scan of the brain should be included in the workup of any
be absent. Diagnosis is made by culture of blood and stool. Long-term
patient with advanced HIV infection and cardiomyopathy.
therapy with ciprofloxacin is the recommended treatment. HIV-infected
A variety of other cardiovascular problems are found in patients
patients also have an increased incidence of S. typhi infection in areas
with HIV infection. Pericardial effusions may be seen in the setting
of the world where typhoid is a problem. Shigella spp., particularly S.
of advanced HIV infection. Predisposing factors include TB, CHF,
flexneri, can cause severe intestinal disease in HIV-infected individuals.
mycobacterial infection, cryptococcal infection, pulmonary infection,
Up to 50% of patients will develop bacteremia. Campylobacter infections
lymphoma, and KS. While pericarditis is quite rare, in one series 5% of
occur with an increased frequency in patients with HIV infection. While
patients with HIV disease had pericardial effusions that were consid-
C. jejuni is the strain most frequently isolated, infections with many
ered to be moderate or severe. Tamponade and death have occurred
other strains have been reported. Patients usually present with crampy
in association with pericardial KS, presumably owing to acute hem-
abdominal pain, fever, and bloody diarrhea. Infection may also present
orrhage. Nonbacterial thrombotic endocarditis has been reported and
as proctitis. Stool examination reveals the presence of fecal leukocytes.
should be considered in patients with unexplained embolic phenom-
Systemic infection can occur, with up to 10% of infected patients exhib-
ena. IV pentamidine, when given rapidly, can result in hypotension as
iting bacteremia. Most strains are sensitive to erythromycin. Abdominal
a consequence of cardiovascular collapse.
pain and diarrhea may be seen with MAC infection.
Diseases of the Oropharynx and Gastrointestinal System Fungal infections may also be a cause of diarrhea in patients with
Oropharyngeal and GI diseases are common features of HIV infection. HIV infection. Histoplasmosis, coccidioidomycosis, and penicilliosis
They are most frequently due to secondary infections. In addition, oral have all been identified as a cause of fever and diarrhea in patients with
and GI lesions may occur with KS and lymphoma. HIV infection. Peritonitis has been seen with C. immitis.
Oral lesions, including thrush, hairy leukoplakia, and aphthous ulcers Cryptosporidia, microsporidia, and Isospora belli (Chap. 224) are
(Fig. 197-35), are particularly common in patients with untreated HIV the most common opportunistic protozoa that infect the GI tract and
infection. Thrush, due to Candida infection, and oral hairy leukopla- cause diarrhea in HIV-infected patients. Cryptosporidial infection may
kia, presumed due to EBV, are usually indicative of fairly advanced present in a variety of ways, ranging from a self-limited or intermittent
Harrisons_20e_Part5_p0859-p1648.indd 1435 6/1/18 12:08 PM
1436
A
B
PART 5
Infectious Diseases
C D
FIGURE 197-35 Various oral lesions in HIV-infected individuals. A. Thrush. B. Hairy leukoplakia. C. Aphthous ulcer. D. Kaposi’s sarcoma.
diarrheal illness in patients in the early stages of HIV infection to a include abdominal pain, malabsorption, diarrhea, and cholangitis. The
severe, life-threatening diarrhea in severely immunodeficient individ- small size of the organism may make it difficult to detect; however,
uals. In patients with untreated HIV infection and CD4+ T cell counts with the use of chromotrope-based stains, organisms can be identified
of <300/μL, the incidence of cryptosporidiosis is ~1% per year. In 75% in stool samples by light microscopy. Definitive diagnosis generally
of cases the diarrhea is accompanied by crampy abdominal pain, and depends on electron-microscopic examination of a stool specimen,
25% of patients have nausea and/or vomiting. Cryptosporidia may intestinal aspirate, or intestinal biopsy specimen. In contrast to crypto-
also cause biliary tract disease in the HIV-infected patient, leading to sporidia, microsporidia have been noted in a variety of extraintestinal
cholecystitis with or without accompanying cholangitis and pancre- locations, including the eye, brain, sinuses, muscle, and liver, and they
atitis secondary to papillary stenosis. The diagnosis of cryptosporidial have been associated with conjunctivitis and hepatitis. The most effec-
diarrhea is made by stool examination or biopsy of the small intestine. tive way to deal with microsporidia in a patient with HIV infection is
The diarrhea is noninflammatory, and the characteristic finding is the to restore the immune system by treating the HIV infection with cART.
presence of oocysts that stain with acid-fast dyes. Therapy is predom- Albendazole, 400 mg bid, has been reported to be of benefit in some
inantly supportive, and marked improvements have been reported patients.
in the setting of effective cART. Treatment with up to 2000 mg/d of I. belli is a coccidian parasite (Chap. 224) most commonly found as a
nitazoxanide (NTZ) is associated with improvement in symptoms or a cause of diarrhea in patients from tropical and subtropical regions. Its
decrease in shedding of organisms in about half of patients. Its overall cysts appear in the stool as large, acid-fast structures that can be differ-
role in the management of this condition remains unclear. Patients entiated from those of cryptosporidia on the basis of size, shape, and
can minimize their risk of developing cryptosporidiosis by avoiding number of sporocysts. The clinical syndromes of Isospora infection are
contact with human and animal feces, by not drinking untreated water identical to those caused by cryptosporidia. The important distinction
from lakes or rivers, and by not eating raw shellfish. is that infection with Isospora is generally relatively easy to treat with
Microsporidia are small, unicellular, obligate intracellular parasites TMP-SMX. While relapses are common, a thrice-weekly regimen of
that reside in the cytoplasm of enteric cells (Chap. 224). The main spe- TMP-SMX appears adequate to prevent recurrence.
cies causing disease in humans is Enterocytozoon bieneusi. The clinical CMV colitis was once seen as a consequence of advanced immuno-
manifestations are similar to those described for cryptosporidia and deficiency in 5–10% of patients with AIDS. It is much less common with
Harrisons_20e_Part5_p0859-p1648.indd 1436 6/1/18 12:08 PM
1437
THE EVALUATION OF DIARRHEA IN A PATIENT
WITH HIV INFECTION
History and physical
Stool culture for enteric pathogens
Stool for ova and parasites x 3
Stool for Clostridium difficile toxin
Diagnosis
No diagnosis
Treat
No suspicion of colitis Suspicion of colitis
Upper endoscopy Diagnosis Colonoscopy
and biopsy and biopsy
Treat
No diagnosis
HIV-Associated Enteropathy
FIGURE 197-36 Barium swallow of a patient with Candida esophagitis. The flow
of barium along the mucosal surface is grossly irregular. FIGURE 197-37 Algorithm for the evaluation of diarrhea in a patient with HIV
infection. HIV-associated enteropathy is a diagnosis of exclusion and can be
made only after other, generally treatable, forms of diarrheal illness have been
the advent of cART. CMV colitis presents as diarrhea, abdominal pain,
ruled out.
weight loss, and anorexia. The diarrhea is usually nonbloody, and the
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
diagnosis is achieved through endoscopy and biopsy. Multiple mucosal
ulcerations are seen at endoscopy, and biopsies reveal characteristic problems encountered in the setting of co-infection with hepatitis B or C,
intranuclear and cytoplasmic inclusion bodies. Secondary bacteremias it is also a reflection of the hepatic injury, ranging from hepatic steatosis
may result as a consequence of thinning of the bowel wall. Treatment to hypersensitivity reactions to immune reconstitution, that can be seen
is with either ganciclovir or foscarnet for 3–6 weeks. Relapses are com- in the context of cART.
mon, and maintenance therapy is typically necessary in patients whose The prevalence of co-infection with HIV and hepatitis viruses
HIV infection is poorly controlled. Patients with CMV disease of the varies by geographic region. In the United States, ~90% of HIV-
GI tract should be carefully monitored for evidence of CMV retinitis. infected individuals have evidence of infection with HBV; 6–14% have
In addition to disease caused by specific secondary infections, chronic HBV infection; 5–50% of patients are co-infected with HCV;
patients with HIV infection may also experience a chronic diarrheal and co-infections with hepatitis D, E, and/or G viruses are common.
syndrome for which no etiologic agent other than HIV can be identi- Among IV drug users with HIV infection, rates of HCV infection
fied. This entity is referred to as AIDS enteropathy or HIV enteropathy. It range from 70% to 95%. HIV infection has a significant impact on the
is most likely a direct result of HIV infection in the GI tract. Histologic course of hepatitis virus infection. It is associated with approximately a
examination of the small bowel in these patients reveals low-grade
mucosal atrophy with a decrease in mitotic figures, suggesting a
hyporegenerative state. Patients often have decreased or absent small-
bowel lactase and malabsorption with accompanying weight loss.
The initial evaluation of a patient with HIV infection and diarrhea
should include a set of stool examinations, including culture, exami-
nation for ova and parasites, and examination for Clostridium difficile
toxin. Approximately 50% of the time this workup will demonstrate
infection with pathogenic bacteria, mycobacteria, or protozoa. If the
initial stool examinations are negative, additional evaluation, including
upper and/or lower endoscopy with biopsy, will yield a diagnosis of
microsporidial or mycobacterial infection of the small intestine ~30% of
the time. In patients for whom this diagnostic evaluation is nonreveal-
ing, a presumptive diagnosis of HIV enteropathy can be made if the
diarrhea has persisted for >1 month. An algorithm for the evaluation of
diarrhea in patients with HIV infection is given in Fig. 197-37.
Rectal lesions are common in HIV-infected patients, particularly
the perirectal ulcers and erosions due to the reactivation of HSV
(Fig. 197-38). These lesions may appear quite atypical, as denuded
skin without vesicles. They typically respond well to treatment with
valacyclovir, famciclovir, or foscarnet. Other rectal lesions encountered
in patients with HIV infection include condylomata acuminata, KS, and
intraepithelial neoplasia (see below).
Hepatobiliary Diseases Diseases of the hepatobiliary system are
a major problem in patients with HIV infection. It has been estimated
that approximately 15% of the deaths of patients with HIV infection are
related to liver disease. While this is predominantly a reflection of the FIGURE 197-38 Severe, erosive perirectal herpes simplex in a patient with AIDS.
Harrisons_20e_Part5_p0859-p1648.indd 1437 6/1/18 12:08 PM
choice in these settings. It is noteworthy that even subclinical reacti- Primary processes related to HIV infection of the nervous system are 1443
vation of herpes simplex may be associated with increases in plasma reminiscent of those seen with other lentiviruses, such as the maedi-
HIV RNA levels. visna virus of sheep.
Diffuse skin eruptions due to Molluscum contagiosum may be seen in Neurologic problems directly attributable to HIV occur throughout
patients with advanced HIV infection. These flesh-colored, umbilicated the course of infection and may be inflammatory, demyelinating, or
lesions resemble those of Penicillium marnefei or Cryptococcosis. They degenerative in nature. The term HIV-associated neurocognitive disorders
tend to regress with effective cART and can also be treated with local (HAND) is used to describe a spectrum of disorders that range from
therapy. Similarly, condyloma acuminatum lesions may be more severe asymptomatic neurocognitive impairment (ANI) to minor neurocog-
and more widely distributed in patients with low CD4+ T cell counts. nitive disorder (MND) to clinically severe dementia. The most severe
Imiquimod cream may be helpful in some cases. Atypical mycobac- form, HIV-associated dementia (HAD), also referred to as the AIDS
terial infections may present as erythematous cutaneous nodules, as dementia complex, or HIV encephalopathy, is considered an AIDS-defining
may fungal infections, Bartonella, Acanthamoeba, and KS. Cutaneous illness. Most HIV-infected patients have some neurologic problem
infections with Aspergillus have been noted at the site of IV catheter during the course of their disease. Even in the setting of suppressive
placement. cART, approximately 50% of HIV-infected individuals can be shown to
The skin of patients with HIV infection is often a target organ for have mild to moderate neurocognitive impairment using sensitive neu-
drug reactions (Chap. 56). Although most skin reactions are mild and ropsychiatric testing. As noted in the section on pathogenesis, damage
not necessarily an indication to discontinue therapy, patients may to the CNS may be a direct result of viral infection of the CNS macro-
have particularly severe cutaneous reactions, including erythroderma, phages or glial cells or may be secondary to the release of neurotoxins
Stevens-Johnson syndrome, and toxic epidermal necrolysis, as a reaction and potentially toxic cytokines such as IL-1β, TNF-α, IL-6, and TGF-β.
to drugs—particularly sulfa drugs, nonnucleoside reverse transcriptase It has been reported that HIV-infected individuals with the E4 allele
inhibitors, abacavir, amprenavir, darunavir, fosamprenavir, and tipra- for apoE are at increased risk for AIDS encephalopathy and peripheral
navir. Similarly, patients with HIV infection are often quite photosen- neuropathy. Virtually all patients with HIV infection have some degree
sitive and burn easily following exposure to sunlight or as a side effect of nervous system involvement with the virus. This is evidenced by
of radiation therapy (Chap. 57). the fact that CSF findings are abnormal in ~90% of untreated patients,
HIV infection and its treatment may be accompanied by cosmetic even during the asymptomatic phase of HIV infection. CSF abnor-
changes of the skin that are not of great clinical importance but may malities include pleocytosis (50–65% of patients), detection of viral
be troubling to patients. Yellowing of the nails and straightening of the RNA (~75%), elevated CSF protein (35%), and evidence of intrathecal
hair, particularly in African-American patients, have been reported as synthesis of anti-HIV antibodies (90%). It is important to point out that
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
a consequence of HIV infection. Zidovudine therapy has been associ- evidence of infection of the CNS with HIV does not imply impairment
ated with elongation of the eyelashes and the development of a bluish of cognitive function. The neurologic function of an HIV-infected indi-
discoloration to the nails, again more common in African-American vidual should be considered normal unless clinical signs and symp-
patients. Therapy with clofazimine may cause a yellow-orange discol- toms suggest otherwise.
oration of the skin and urine. Aseptic meningitis may be seen in any but the very late stages of HIV
infection. In the setting of acute primary infection, patients may experi-
Neurologic Diseases Clinical disease of the nervous system ence a syndrome of headache, photophobia, and meningismus. Rarely,
accounts for a significant degree of morbidity in a high percentage of an acute encephalopathy due to encephalitis may occur. Cranial nerve
patients with HIV infection (Table 197-14). The neurologic problems involvement may be seen, predominantly cranial nerve VII but occa-
that occur in HIV-infected individuals may be either primary to the sionally V and/or VIII. CSF findings include a lymphocytic pleocyto-
pathogenic processes of HIV infection or secondary to opportunistic sis, elevated protein level, and normal glucose level. This syndrome,
infections or neoplasms. Among the more frequent opportunistic dis- which cannot be clinically differentiated from other viral meningiti-
eases that involve the CNS are toxoplasmosis, cryptococcosis, progres- des (Chap. 134), usually resolves spontaneously within 2–4 weeks;
sive multifocal leukoencephalopathy, and primary CNS lymphoma. however, in some patients, signs and symptoms may become chronic.
Other less common problems include mycobacterial infections; syphi- Aseptic meningitis may occur any time in the course of HIV infection;
lis; and infection with CMV, herpes zoster, HTLV-1, Trypanosoma cruzi, however, it is rare following the development of AIDS. This suggests
or Acanthamoeba. Overall, secondary diseases of the CNS have been that clinical aseptic meningitis in the context of HIV infection is an
reported to occur in approximately one-third of patients with AIDS. immune-mediated disease.
These data antedate the widespread use of cART, and this frequency is Cryptococcus is the leading infectious cause of meningitis in patients
considerably lower in patients receiving effective antiretroviral drugs. with AIDS (Chap. 210). While the vast majority of these are due to
C. neoformans, up to 12% may be due to C. gattii. Cryptococcal menin-
TABLE 197-14 Neurologic Diseases in Patients with HIV Infection gitis is the initial AIDS-defining illness in ~2% of patients and generally
Opportunistic infections HIV-1 infection occurs in patients with CD4+ T cell counts <100/μL. Cryptococcal
Toxoplasmosis Aseptic meningitis meningitis is particularly common in untreated patients with AIDS
in Africa, occurring in ~5% of patients. Most patients present with a
Cryptococcosis HIV-associated neurocognitive disorders
(HAND), including HIV encephalopathy/ picture of subacute meningoencephalitis with fever, nausea, vomiting,
Progressive multifocal
leukoencephalopathy AIDS dementia complex altered mental status, headache, and meningeal signs. The incidence
Myelopathy of seizures and focal neurologic deficits is low. The CSF profile may be
Cytomegalovirus
Vacuolar myelopathy normal or may show only modest elevations in WBC or protein levels
Syphilis
and decreases in glucose. The opening pressure in the CSF is usually
Mycobacterium tuberculosis Pure sensory ataxia
elevated. In addition to meningitis, patients may develop cryptococ-
HTLV-1 infection Paresthesia/dysesthesia
comas and cranial nerve involvement. Approximately one-third of
Amebiasis Peripheral neuropathy
patients also have pulmonary disease. Uncommon manifestations of
Neoplasms Acute inflammatory demyelinating cryptococcal infection include skin lesions that resemble molluscum con-
polyneuropathy (Guillain-Barré
Primary CNS lymphoma
syndrome)
tagiosum, lymphadenopathy, palatal and glossal ulcers, arthritis, gas-
Kaposi’s sarcoma troenteritis, myocarditis, and prostatitis. The prostate gland may serve
Chronic inflammatory demyelinating
polyneuropathy (CIDP) as a reservoir for smoldering cryptococcal infection. The diagnosis of
cryptococcal meningitis is made by identification of organisms in spi-
Mononeuritis multiplex
nal fluid with india ink examination or by the detection of cryptococcal
Distal symmetric polyneuropathy
antigen. Blood cultures for fungus are often positive. A biopsy may be
Myopathy
needed to make a diagnosis of CNS cryptococcoma. Treatment is with
Harrisons_20e_Part5_p0859-p1648.indd 1443 6/1/18 12:08 PM
1444 IV amphotericin B 0.7 mg/kg daily, or liposomal amphotericin 4–6 mg/kg The precise cause of HIV-associated dementia remains unclear,
daily, with flucytosine 25 mg/kg qid for at least 2 weeks if possible, although the condition is thought to be a result of a combination of
continuing with amphotericin alone ideally until the CSF culture turns direct effects of HIV on the CNS and associated immune activation.
negative. Decreases in renal function in association with amphotericin HIV has been found in the brains of patients with HIV encephalopathy
can lead to increases in flucytosine levels and subsequent bone mar- by Southern blot, in situ hybridization, PCR, and electron microscopy.
row suppression. Amphotericin is followed by fluconazole 400 mg/d Multinucleated giant cells, macrophages, and microglial cells appear to
PO for 8 weeks, and then fluconazole 200 mg/d until the CD4+ T cell be the main cell types harboring virus in the CNS. Histologically, the
count has increased to >200 cells/μL for 6 months in response to cART. major changes are seen in the subcortical areas of the brain and include
Repeated lumbar puncture may be required to manage increased pallor and gliosis, multinucleated giant cell encephalitis, and vacuolar
intracranial pressure. Symptoms may recur with initiation of cART myelopathy. Less commonly, diffuse or focal spongiform changes occur
as an immune reconstitution syndrome (see above). Other fungi that in the white matter. Areas of the brain involved in motor function, lan-
may cause meningitis in patients with HIV infection are C. immitis guage, and judgment are most severely affected.
and H. capsulatum. Meningoencephalitis has also been reported due to There are no specific criteria for a diagnosis of HIV-associated
Acanthamoeba or Naegleria. dementia, and this syndrome must be differentiated from a number of
HIV-associated dementia consists of a constellation of signs and other diseases that affect the CNS of HIV-infected patients (Table 197-14).
symptoms of CNS disease. While this is generally a late complication The diagnosis of dementia depends on demonstrating a decline in
of HIV infection that progresses slowly over months, it can be seen in cognitive function. This can be accomplished objectively with the use
patients with CD4+ T cell counts >350 cells/μL. A major feature of this of a Mini-Mental Status Examination (MMSE) in patients for whom
entity is the development of dementia, defined as a decline in cogni- prior scores are available. For this reason, it is advisable for all patients
tive ability from a previous level. It may present as impaired ability to with a diagnosis of HIV infection to have a baseline MMSE. However,
concentrate, increased forgetfulness, difficulty reading, or increased changes in MMSE scores may be absent in patients with mild HIV
difficulty performing complex tasks. Initially these symptoms may be encephalopathy. Imaging studies of the CNS, by either MRI or CT,
indistinguishable from findings of situational depression or fatigue. In often demonstrate evidence of cerebral atrophy (Fig. 197-40). MRI may
contrast to “cortical” dementia (such as Alzheimer’s disease), aphasia, also reveal small areas of increased density on T2-weighted images.
apraxia, and agnosia are uncommon, leading some investigators to Lumbar puncture is an important element of the evaluation of patients
classify HIV encephalopathy as a “subcortical dementia” characterized with HIV infection and neurologic abnormalities. It is generally most
by defects in short-term memory and executive function (see below). helpful in ruling out or making a diagnosis of opportunistic infections.
In addition to dementia, patients with HIV encephalopathy may also In HIV encephalopathy, patients may have the nonspecific findings of
have motor and behavioral abnormalities. Among the motor problems an increase in CSF cells and protein level. While HIV RNA can often be
PART 5
are unsteady gait, poor balance, tremor, and difficulty with rapid detected in the spinal fluid and HIV can be cultured from the CSF, this
alternating movements. Increased tone and deep tendon reflexes may finding is not specific for HIV encephalopathy. There appears to be no
be found in patients with spinal cord involvement. Late stages may correlation between the presence of HIV in the CSF and the presence of
be complicated by bowel and/or bladder incontinence. Behavioral HIV encephalopathy. Elevated levels of macrophage chemoattractant
problems include apathy, irritability, and lack of initiative, with pro- protein (MCP-1), β2-microglobulin, neopterin, and quinolinic acid (a
Infectious Diseases
gression to a vegetative state in some instances. Some patients develop metabolite of tryptophan reported to cause CNS injury) have been
a state of agitation or mild mania. These changes usually occur without noted in the CSF of patients with HIV encephalopathy. These findings
significant changes in level of alertness. This is in contrast to the find- suggest that these factors as well as inflammatory cytokines may be
ing of somnolence in patients with dementia due to toxic/metabolic involved in the pathogenesis of this syndrome.
encephalopathies. Combination antiretroviral therapy is of benefit in patients with
HIV-associated dementia is the initial AIDS-defining illness in ~3% HIV-associated dementia. Improvement in neuropsychiatric test scores
of patients with HIV infection and thus only rarely precedes clinical has been noted for both adult and pediatric patients treated with
evidence of immunodeficiency. Clinically significant encephalopathy antiretrovirals. The rapid improvement in cognitive function noted with
eventually develops in ~25% of untreated patients with AIDS. As the initiation of cART suggests that at least some component of this
immunologic function declines, the risk and severity of HIV-associated
dementia increases. Autopsy series suggest that 80–90% of patients
with HIV infection have histologic evidence of CNS involvement.
Several classification schemes have been developed for grading HIV
encephalopathy; a commonly used clinical staging system is outlined
in Table 197-15.
TABLE 197-15 Clinical Staging of Hand According to Frascati Criteria
NEUROCOGNITIVE
STAGE STATUSa FUNCTIONAL STATUSb
Asymptomatic 1 SD below mean in No impairments in
2 cognitive domains activities of daily living
Mild neurocognitive 1 SD below mean in Impairments in activities
disorder 2 cognitive domains of daily living
HIV-associated dementia 2 SD below mean in Notable impairments in
2 cognitive domains activities of daily living
a
Neurocognitive testing should include assessment of at least 5 domains,
including attention-information processing, language, abstraction-executive,
complex perceptual motor skills, memory (including learning and recall), simple
motor skills, or sensory perceptual skills. Appropriate norms must be available to
establish the number of domains in which performance is below 1 SD. bFunctional
status is typically assessed by self-reporting but might be corroborated by a
collateral source. No agreed measures exist for HIV-associated neurocognitive FIGURE 197-40 AIDS dementia complex. Postcontrast CT scan through the
disorder criteria. Note that, for diagnosis of HIV-associated neurocognitive lateral ventricles of a 47-year-old man with AIDS, altered mental status, and
disorder, other causes of dementia must be ruled out and potential confounding dementia. The lateral and third ventricles and the cerebral sulci are abnormally
effects of substance use or psychiatric illness should be considered. prominent. Mild white matter hypodensity is seen adjacent to the frontal horns of
Source: Adapted from A Antinori et al: Neurology 69:1789, 2007. the lateral ventricles.
Harrisons_20e_Part5_p0859-p1648.indd 1444 6/1/18 12:08 PM
TABLE 197-16 Causes of Seizures in Patients with HIV Infection 1445
OVERALL FRACTION OF PATIENTS
CONTRIBUTION TO WHO HAVE SEIZURES,
DISEASE FIRST SEIZURE, % %
HIV encephalopathy 24–47 7–50
Cerebral toxoplasmosis 28 15–40
Cryptococcal meningitis 13 8
Primary central nervous 4 15–30
system lymphoma
Progressive multifocal 1 20
leukoencephalopathy
Source: From DM Holtzman et al: Am J Med 87:173, 1989.
problem is quickly reversible, again supporting at least a partial role of
soluble mediators in the pathogenesis. It should also be noted that these
patients have an increased sensitivity to the side effects of neuroleptic
drugs. The use of these drugs for symptomatic treatment is associated
with an increased risk of extrapyramidal side effects; therefore, patients FIGURE 197-41 Central nervous system toxoplasmosis. A coronal postcontrast
with HIV encephalopathy who receive these agents must be monitored T1-weighted MRI scan demonstrates a peripheral enhancing lesion in the left
carefully. It is felt by many physicians that the decrease in the preva- frontal lobe, associated with an eccentric nodular area of enhancement (arrow);
lence of severe cases of HAND brought about by cART has resulted in this so-called eccentric target sign is typical of toxoplasmosis.
an increase in the prevalence of milder forms of this disorder.
Seizures may be a consequence of opportunistic infections, neo- deficits or with a picture more influenced by the accompanying cere-
plasms, or HIV encephalopathy (Table 197-16). The seizure threshold bral edema and characterized by confusion, dementia, and lethargy,
is often lower than normal in patients with advanced HIV infection due which can progress to coma. The diagnosis is usually suspected on the
in part to the frequent presence of electrolyte abnormalities. Seizures basis of MRI findings of multiple lesions in multiple locations, although
are seen in 15–40% of patients with cerebral toxoplasmosis, 15–35% in some cases only a single lesion is seen. Pathologically, these lesions
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
of patients with primary CNS lymphoma, 8% of patients with cryp- generally exhibit inflammation and central necrosis and, as a result,
tococcal meningitis, and 7–50% of patients with HIV encephalopathy. demonstrate ring enhancement on contrast MRI (Fig. 197-41) or, if MRI
Seizures may also be seen in patients with CNS tuberculosis, aseptic is unavailable or contraindicated, on double-dose contrast CT. There is
meningitis, and progressive multifocal leukoencephalopathy. Seizures usually evidence of surrounding edema. In addition to toxoplasmosis,
may be the presenting clinical symptom of HIV disease. In one study of the differential diagnosis of single or multiple enhancing mass lesions
100 patients with HIV infection presenting with a first seizure, cerebral in the HIV-infected patient includes primary CNS lymphoma and, less
mass lesions were the most common cause, responsible for 32 of the commonly, TB or fungal or bacterial abscesses. The definitive diagnos-
100 new-onset seizures. Of these 32 cases, 28 were due to toxoplasmosis tic procedure is brain biopsy. However, given the morbidity rate that
and 4 to lymphoma. HIV encephalopathy accounted for an additional can accompany this procedure, it is usually reserved for the patient
24 new-onset seizures. Cryptococcal meningitis was the third most who has failed 2–4 weeks of empiric therapy for toxoplasmosis. If the
common diagnosis, responsible for 13 of the 100 seizures. In 23 cases, patient is seronegative for T. gondii, the likelihood that a mass lesion
no cause could be found, and it is possible that these cases represent a is due to toxoplasmosis is <10%. In that setting, one may choose to be
subcategory of HIV encephalopathy. Of these 23 cases, 16 (70%) had 2 more aggressive and perform a brain biopsy sooner. Standard treat-
or more seizures, suggesting that anticonvulsant therapy is indicated in ment is sulfadiazine and pyrimethamine with leucovorin as needed
all patients with HIV infection and seizures unless a rapidly correctable for a minimum of 4–6 weeks. Alternative therapeutic regimens include
cause is found. Due to a variety of drug-drug interactions between clindamycin in combination with pyrimethamine; atovaquone plus
antiseizure medications and antiretrovirals, drug levels need to be pyrimethamine; and azithromycin plus pyrimethamine plus rifabutin.
monitored carefully. Relapses are common, and it is recommended that patients with a
Patients with HIV infection may present with focal neurologic deficits history of prior toxoplasmic encephalitis receive maintenance therapy
from a variety of causes. The most common causes are toxoplasmosis, with sulfadiazine, pyrimethamine, and leucovorin as long as their
progressive multifocal leukoencephalopathy, and CNS lymphoma. CD4+ T cell counts remain <200 cells/μL. Patients with CD4+ T cell
Other causes include cryptococcal infections (discussed above; also counts <100/μL and IgG antibody to Toxoplasma should receive pri-
Chap. 210), stroke, and reactivation of Chagas’ disease. mary prophylaxis for toxoplasmosis. Fortunately, the same daily regi-
Toxoplasmosis has been one of the most common causes of secondary men of a single double-strength tablet of TMP-SMX used for P. jirovecii
CNS infections in patients with AIDS, but its incidence is decreasing in prophylaxis provides adequate primary protection against toxoplas-
the era of cART. It is most common in patients from the Caribbean and mosis. Secondary prophylaxis/maintenance therapy for toxoplasmosis
from France, where the seroprevalence of T. gondii is around 50%. This may be discontinued in the setting of effective cART and increases in
figure is closer to 15% in the United States. Toxoplasmosis is generally CD4+ T cell counts to >200/μL for 6 months.
a late complication of HIV infection and usually occurs in patients JC virus, a human polyomavirus that is the etiologic agent of
with CD4+ T cell counts <200/μL. Cerebral toxoplasmosis is thought progressive multifocal leukoencephalopathy (PML), is an important oppor-
to represent a reactivation of latent tissue cysts. It is 10 times more tunistic pathogen in patients with AIDS (Chap. 133). While ~80% of
common in patients with antibodies to the organism than in patients the general adult population has antibodies to JC virus, indicative of
who are seronegative. Patients diagnosed with HIV infection should be prior infection, <10% of healthy adults show any evidence of ongoing
screened for IgG antibodies to T. gondii during the time of their initial viral replication. PML is the only known clinical manifestation of JC
workup. Those who are seronegative should be counseled about ways virus infection. It is a late manifestation of AIDS and is seen in ~1–4%
to minimize the risk of primary infection including avoiding the con- of patients with AIDS. The lesions of PML begin as small foci of demy-
sumption of undercooked meat and careful hand washing after contact elination in subcortical white matter that eventually coalesce. The
with soil or changing the cat litter box. The most common clinical cerebral hemispheres, cerebellum, and brainstem may all be involved.
presentation of cerebral toxoplasmosis in patients with HIV infection Patients typically have a protracted course with multifocal neurologic
is fever, headache, and focal neurologic deficits. Patients may present deficits, with or without changes in mental status. Approximately
with seizure, hemiparesis, or aphasia as a manifestation of these focal 20% of patients experience seizures. Ataxia, hemiparesis, visual field
Harrisons_20e_Part5_p0859-p1648.indd 1445 6/1/18 12:08 PM
1446 defects, aphasia, and sensory defects may occur. Headache, fever, occurring with pernicious anemia. Although vitamin B12 deficiency can
nausea, and vomiting are rarely seen. Their presence should suggest be seen in patients with AIDS as a primary complication of HIV infec-
another diagnosis. MRI typically reveals multiple, nonenhancing tion, it does not appear to be responsible for the majority of the cases of
white matter lesions that may coalesce and have a predilection for the myelopathy seen in patients with HIV infection. Vacuolar myelopathy
occipital and parietal lobes. The lesions show signal hyperintensity on is characterized by a subacute onset and often presents with gait distur-
T2-weighted images and diminished signal on T1-weighted images. bances, predominantly ataxia and spasticity; it may progress to include
The measurement of JC virus DNA levels in CSF has a diagnostic sen- bladder and bowel dysfunction. Physical findings include evidence of
sitivity of 76% and a specificity of close to 100%. Prior to the availability increased deep tendon reflexes and extensor plantar responses. The
of cART, the majority of patients with PML died within 3–6 months of second form of spinal cord disease involves the dorsal columns and
the onset of symptoms. Paradoxical worsening of PML has been seen presents as a pure sensory ataxia. The third form is also sensory in
with initiation of cART as an immune reconstitution syndrome. There nature and presents with paresthesias and dysesthesias of the lower
is no specific treatment for PML; however, a median survival of 2 years extremities. In contrast to the cognitive problems seen in patients with
and survival of >15 years have been reported in patients with PML HIV encephalopathy, these spinal cord syndromes do not respond well
treated with cART for their HIV disease. Despite having a significant to antiretroviral drugs, and therapy is mainly supportive.
impact on survival, only ~50% of patients with HIV infection and PML One important disease of the spinal cord that also involves the
show neurologic improvement with cART. Studies with other antiviral peripheral nerves is a myelopathy and polyradiculopathy seen in associa-
agents such as cidofovir have failed to show clear benefit. Factors tion with CMV infection. This entity is generally seen late in the course
influencing a favorable prognosis for PML in the setting of HIV infec- of HIV infection and is fulminant in onset, with lower extremity and
tion include a CD4+ T cell count >100/μL at baseline and the ability to sacral paresthesias, difficulty in walking, areflexia, ascending sensory
maintain an HIV viral load of <500 copies/mL. Baseline HIV-1 viral loss, and urinary retention. The clinical course is rapidly progressive
load does not have independent predictive value of survival. PML is over a period of weeks. CSF examination reveals a predominantly
one of the few opportunistic infections that continues to occur with neutrophilic pleocytosis, and CMV DNA can be detected by CSF PCR.
some frequency despite the widespread use of cART. Therapy with ganciclovir or foscarnet can lead to rapid improvement,
Reactivation American trypanosomiasis may present as acute menin- and prompt initiation of foscarnet or ganciclovir therapy is important
goencephalitis with focal neurologic signs, fever, headache, vomiting, in minimizing the degree of permanent neurologic damage. Com-
and seizures. Accompanying cardiac disease in the form of arrhythmias bination therapy with both drugs should be considered in patients
or heart failure should increase the index of suspicion. The presence of who have been previously treated for CMV disease. Other diseases
antibodies to T. cruzi supports the diagnosis. In South America, reacti- involving the spinal cord in patients with HIV infection include
vation of Chagas’ disease is considered to be an AIDS-defining condition HTLV-1-associated myelopathy (HAM) (Chap. 196), neurosyphilis
PART 5
and may be the initial AIDS-defining condition. The majority of cases (Chap. 177), infection with herpes simplex (Chap. 187) or varicella-zoster
occur in patients with CD4+ T cell counts <200 cells/μL. Lesions appear (Chap. 188), TB (Chap. 173), and lymphoma (Chap. 104).
radiographically as single or multiple hypodense areas, typically with Peripheral neuropathies are common in patients with HIV infection.
ring enhancement and edema. They are found predominantly in the They occur at all stages of illness and take a variety of forms. Early
subcortical areas, a feature that differentiates them from the deeper in the course of HIV infection, an acute inflammatory demyelinat-
Infectious Diseases
lesions of toxoplasmosis. T. cruzi amastigotes, or trypanosomes, can be ing polyneuropathy resembling Guillain-Barré syndrome may occur
identified from biopsy specimens or CSF. Other CSF findings include (Chap. 439). In other patients, a progressive or relapsing-remitting
elevated protein and a mild (<100 cells/μL) lymphocytic pleocytosis. inflammatory neuropathy resembling chronic inflammatory demy-
Organisms can also be identified by direct examination of the blood. elinating polyneuropathy (CIDP) has been noted. Patients commonly
Treatment consists of benzimidazole (2.5 mg/kg bid) or nifurtimox present with progressive weakness, areflexia, and minimal sensory
(2 mg/kg qid) for at least 60 days, followed by maintenance therapy changes. CSF examination often reveals a mononuclear pleocytosis,
for the duration of immunodeficiency with either drug at a dose of and peripheral nerve biopsy demonstrates a perivascular infiltrate
5 mg/kg three times a week. As is the case with cerebral toxoplasmosis, suggesting an autoimmune etiology. Plasma exchange or IVIg has been
successful therapy with antiretrovirals may allow discontinuation of tried with variable success. Because of the immunosuppressive effects
therapy for Chagas’ disease. of glucocorticoids, they should be reserved for severe cases of CIDP
Stroke may occur in patients with HIV infection. In contrast to the refractory to other measures. Another autoimmune peripheral neurop-
other causes of focal neurologic deficits in patients with HIV infection, athy seen in patients with AIDS is mononeuritis multiplex (Chaps. 439
the symptoms of a stroke are sudden in onset. Patients with HIV infec- and 356) due to a necrotizing arteritis of peripheral nerves. The most
tion have an increased prevalence of many classic risk factors associ- common peripheral neuropathy in patients with HIV infection is a
ated with stroke, including smoking and diabetes. It has been reported distal sensory polyneuropathy (DSPN) also referred to as painful sensory
that HIV infection itself can lead to an increase in carotid artery stiff- neuropathy (HIV-SN), predominantly sensory neuropathy, or distal
ness. The relative increase in risk for stroke as a consequence of HIV symmetric peripheral neuropathy. This condition may be a direct conse-
infection is more pronounced in women and in individuals between quence of HIV infection or a side effect of dideoxynucleoside therapy. It
the ages of 18 and 29. Among the secondary infectious diseases in is more common in taller individuals, older individuals, and those with
patients with HIV infection that may be associated with stroke are lower CD4 counts. Two-thirds of patients with AIDS may be shown by
vasculitis due to cerebral varicella zoster or neurosyphilis and septic electrophysiologic studies to have some evidence of peripheral nerve
embolism in association with fungal infection. Other elements of the disease. Presenting symptoms are usually painful burning sensations
differential diagnosis of stroke in the patient with HIV infection include in the feet and lower extremities. Findings on examination include a
atherosclerotic cerebral vascular disease, thrombotic thrombocytopenic stocking-type sensory loss to pinprick, temperature, and touch sensa-
purpura, and cocaine or amphetamine use. tion and a loss of ankle reflexes. Motor changes are mild and are usu-
Primary CNS lymphoma is discussed below in the section on neo- ally limited to weakness of the intrinsic foot muscles. Response of this
plastic diseases. condition to antiretrovirals has been variable, perhaps because antiret-
Spinal cord disease, or myelopathy, is present in ~20% of patients rovirals are responsible for the problem in some instances. When due
with AIDS, often as part of HIV-associated neurocognitive disorder. In to dideoxynucleoside therapy, patients with lower extremity peripheral
fact, 90% of the patients with HIV-associated myelopathy have some neuropathy may complain of a sensation that they are walking on ice.
evidence of dementia, suggesting that similar pathologic processes Other entities in the differential diagnosis of peripheral neuropathy
may be responsible for both conditions. Three main types of spinal include diabetes mellitus, vitamin B12 deficiency, and side effects from
cord disease are seen in patients with AIDS. The first of these is a vacu- metronidazole or dapsone. For distal symmetric polyneuropathy that
olar myelopathy, as mentioned above. This condition is pathologically fails to resolve following the discontinuation of dideoxynucleosides,
similar to subacute combined degeneration of the cord, such as that therapy is symptomatic; gabapentin, carbamazepine, tricyclics, or
Harrisons_20e_Part5_p0859-p1648.indd 1446 6/1/18 12:08 PM
analgesics may be effective for dysesthesias. Treatment-naïve patients Ophthalmologic examination reveals widespread pale gray peripheral 1447
may respond to cART. lesions. This condition is often complicated by retinal detachment. It
Myopathy may complicate the course of HIV infection; causes is important to recognize and treat this condition with IV acyclovir as
include HIV infection itself, zidovudine, and the generalized wasting quickly as possible to minimize the loss of vision.
syndrome (discussed below). HIV-associated myopathy may range in Several other secondary infections may cause ocular problems in
severity from an asymptomatic elevation in creatine kinase levels to a HIV-infected patients. P. jirovecii can cause a lesion of the choroid that
subacute syndrome characterized by proximal muscle weakness and may be detected as an incidental finding on ophthalmologic examination.
myalgias. Quite pronounced elevations in creatine kinase may occur These lesions are typically bilateral, are from half to twice the disc diame-
in asymptomatic patients, particularly after exercise. The clinical sig- ter in size, and appear as slightly elevated yellow-white plaques. They are
nificance of this as an isolated laboratory finding is unclear. A variety usually asymptomatic and may be confused with cotton-wool spots. Cho-
of both inflammatory and noninflammatory pathologic processes have rioretinitis due to toxoplasmosis can be seen alone or, more commonly,
been noted in patients with more severe myopathy, including myofiber in association with CNS toxoplasmosis. KS may involve the eyelid or
necrosis with inflammatory cells, nemaline rod bodies, cytoplasmic conjunctiva, while lymphoma may involve the retina. Syphilis may lead
bodies, and mitochondrial abnormalities. Profound muscle wasting, to a uveitis that is highly associated with the presence of neurosyphilis.
often with muscle pain, may be seen after prolonged zidovudine ther-
apy. This toxic side effect of the drug is dose-dependent and is related to Additional Disseminated Infections and Wasting
its ability to interfere with the function of mitochondrial polymerases. Syndrome Infections with species of the small, gram-negative,
It is reversible following discontinuation of the drug. Red ragged fibers Rickettsia-like organism Bartonella (Chap. 167) are seen with increased
are a histologic hallmark of zidovudine-induced myopathy. frequency in patients with HIV infection. While it is not considered an
AIDS-defining illness by the CDC, many experts view infection with
Ophthalmologic Diseases Ophthalmologic problems occur in Bartonella as indicative of a severe defect in cell-mediated immunity. It
~50% of patients with advanced HIV infection. The most common is usually seen in patients with CD4+ T cell counts <100/μL and is a
abnormal findings on funduscopic examination are cotton-wool spots. significant cause of unexplained fever in patients with advanced HIV
These are hard white spots that appear on the surface of the retina and infection. Among the clinical manifestations of Bartonella infection are
often have an irregular edge. They represent areas of retinal ischemia sec- bacillary angiomatosis, cat-scratch disease, and trench fever. Bacillary
ondary to microvascular disease. At times they are associated with small angiomatosis is usually due to infection with B. henselae and is linked to
areas of hemorrhage and thus can be difficult to distinguish from CMV exposure to flea-infested cats. It is characterized by a vascular prolif-
retinitis. In contrast to CMV retinitis, however, these lesions are not asso- eration that leads to a variety of skin lesions that have been confused
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
ciated with visual loss and tend to remain stable or improve over time. with the skin lesions of KS. In contrast to the lesions of KS, the lesions
One of the most devastating consequences of HIV infection is CMV of bacillary angiomatosis generally blanch, are painful, and typically
retinitis. Patients at high risk of CMV retinitis (CD4+ T cell count <100/ occur in the setting of systemic symptoms. Infection can extend to the
μL) should undergo an ophthalmologic examination every 3–6 months. lymph nodes, liver (peliosis hepatis), spleen, bone, heart, CNS, respi-
The majority of cases of CMV retinitis occur in patients with a CD4+ T ratory tract, and GI tract. Cat-scratch disease also is due to B. henselae
cell count <50/μL. Prior to the availability of cART, this CMV reactiva- and generally begins with a papule at the site of inoculation. This is
tion syndrome was seen in 25–30% of patients with AIDS. In the cART followed several weeks later by the development of regional adenop-
era this has dropped to close to 2%. CMV retinitis usually presents athy and malaise. Infection with B. quintana is transmitted by lice and
as a painless, progressive loss of vision. Patients may also complain has been associated with case reports of trench fever, endocarditis,
of blurred vision, “floaters,” and scintillations. The disease is usually adenopathy, and bacillary angiomatosis. The organism is quite difficult
bilateral, although typically it affects one eye more than the other. The to culture, and diagnosis often relies on identifying the organism in
diagnosis is made on clinical grounds by an experienced ophthal- biopsy specimens using the Warthin-Starry or similar stains. Treatment
mologist. The characteristic retinal appearance is that of perivascular is with either doxycycline or erythromycin for at least 3 months.
hemorrhage and exudate. In situations where the diagnosis is in doubt Histoplasmosis is an opportunistic infection that is seen most fre-
due to an atypical presentation or an unexpected lack of response to quently in patients in the Mississippi and Ohio River valleys, Puerto Rico,
therapy, vitreous or aqueous humor sampling with molecular diag- the Dominican Republic, and South America. These are all areas in
nostic techniques may be of value. CMV infection of the retina results which infection with H. capsulatum is endemic (Chap. 207). Because of
in a necrotic inflammatory process, and the visual loss that develops this limited geographic distribution, the percentage of AIDS cases in the
is irreversible. CMV retinitis may be complicated by rhegmatogenous United States with histoplasmosis is only ~0.5. Histoplasmosis is gener-
retinal detachment as a consequence of retinal atrophy in areas of prior ally a late manifestation of HIV infection; however, it may be the initial
inflammation. Therapy for CMV retinitis consists of oral valganciclovir, AIDS-defining condition. In one study, the median CD4+ T cell count
IV ganciclovir, or IV foscarnet, with cidofovir as an alternative. Com- for patients with histoplasmosis and AIDS was 33/μL. While disease
bination therapy with ganciclovir and foscarnet has been shown to due to H. capsulatum may present as a primary infection of the lung, dis-
be slightly more effective than either ganciclovir or foscarnet alone in seminated disease, presumably due to reactivation, is the most common
the patient with relapsed CMV retinitis. A 3-week induction course is presentation in HIV-infected patients. Patients usually present with a
followed by maintenance therapy with oral valganciclovir. If CMV dis- 4- to 8-week history of fever and weight loss. Hepatosplenomegaly and
ease is limited to the eye, intravitreal injections of ganciclovir or foscar- lymphadenopathy are each seen in about 25% of patients. CNS disease,
net may be considered. Intravitreal injections of cidofovir are generally either meningitis or a mass lesion, is seen in 15% of patients. Bone mar-
avoided due to the increased risk of uveitis and hypotony. Maintenance row involvement is common, with thrombocytopenia, neutropenia, and
therapy is continued until the CD4+ T cell count remains >100 μL for >6 anemia occurring in 33% of patients. Approximately 7% of patients have
months. The majority of patients with HIV infection and CMV disease mucocutaneous lesions consisting of a maculopapular rash and skin or
develop some degree of uveitis with the initiation of cART. The etiol- oral ulcers. Respiratory symptoms are usually mild, with chest x-ray
ogy of this is unknown; however, it has been suggested that this may be showing a diffuse infiltrate or diffuse small nodules in ~50% of cases.
due to the generation of an enhanced immune response to CMV as an The gastrointestinal tract may be involved. Diagnosis is made by silver
IRIS (see above). In some instances this has required the use of topical staining of tissue, by culturing the organisms from blood, bone marrow,
glucocorticoids. or tissue, or by detecting antigen in blood or urine. Treatment is typi-
Both HSV and varicella zoster virus can cause a rapidly progressing, cally with liposomal amphotericin B followed by maintenance therapy
bilateral, necrotizing retinitis referred to as the acute retinal necrosis with oral itraconazole until the serum histoplasma antigen is <2 units,
syndrome, or progressive outer retinal necrosis (PORN). This syndrome, the patient has been on antiretrovirals for at least 6 months, and the
in contrast to CMV retinitis, is associated with pain, keratitis, and CD4 count is >150 cells/μL. In the setting of mild infection, it may be
iritis. It is often associated with orolabial HSV or trigeminal zoster. appropriate to initiate therapy with itraconazole alone.
Harrisons_20e_Part5_p0859-p1648.indd 1447 6/1/18 12:08 PM
1448 Following the spread of HIV infection to southeast Asia, dissemi- and mortality in patients with HIV infection than the AIDS-defining
nated infection with the fungus Penicillium marneffei was recognized malignancies and are responsible for approximately 25% of the deaths
as a complication of HIV infection and is considered an AIDS-defining in patients with HIV infection. Rates of non-Hodgkin’s lymphoma
condition in those parts of the world where it occurs. P. marneffei is the have declined; however, this decline has not been as dramatic as the
third most common AIDS-defining illness in Thailand, following TB decline in rates of KS. In contrast, cART has had little effect on human
and cryptococcosis. It is more frequently diagnosed in the rainy than the papillomavirus (HPV)-associated malignancies. As patients with HIV
dry season. Clinical features include fever, generalized lymphadenopa- infection live longer, a wider array of cancers is seen in this population.
thy, hepatosplenomegaly, anemia, thrombocytopenia, and papular skin While some may only reflect known risk factors (e.g., smoking, alcohol
lesions with central umbilication resembling the lesions of Molluscum consumption, co-infection with other viruses such as hepatitis B) that
contagiosum. Treatment is with amphotericin B followed by itraconazole are increased in patients with HIV infection, some may be a direct
until the CD4+ T cell count is >100 cells/μL for at least 6 months. consequence of HIV and are clearly increased in patients with lower
Visceral leishmaniasis (Chap. 221) is recognized with increasing fre- CD4+ T cell counts.
quency in patients with HIV infection who live in or travel to areas Kaposi’s sarcoma is a multicentric neoplasm consisting of multiple
endemic for this protozoal infection transmitted by sandflies. The clin- vascular nodules appearing in the skin, mucous membranes, and
ical presentation is one of hepatosplenomegaly, fever, and hematologic viscera. The clinical course of KS ranges from indolent, with only
abnormalities. Lymphadenopathy and other constitutional symptoms minor skin or lymph node involvement, to fulminant, with extensive
may be present. A chronic, relapsing course is seen in two-thirds of cutaneous and visceral involvement. In the initial period of the AIDS
co-infected patients. Organisms can be isolated from cultures of bone epidemic, KS was a prominent clinical feature of the first cases of AIDS,
marrow aspirates. Histologic stains may be negative, and antibody occurring in 79% of the patients diagnosed in 1981. By 1989 it was seen
titers are of little help. Patients with HIV infection usually respond well in only 25% of cases, by 1992 the number had decreased to 9%, and by
initially to standard therapy with amphotericin B or pentavalent anti- 1997 the number was <1%. HHV-8 (KSHV) has been strongly impli-
mony compounds. Eradication of the organism is difficult, however, cated as a viral cofactor in the pathogenesis of KS.
and relapses are common. Clinically, KS has varied presentations and may be seen at any
Patients with HIV infection are at a slightly increased risk of clinical stage of HIV infection, even in the presence of a normal CD4+ T cell
malaria. This is particularly true for patients from nonendemic areas count. The initial lesion may be a small, raised reddish-purple
and thus at risk for primary infection and in patients with lower CD4+ nodule on the skin (Fig. 197-42), a discoloration on the oral mucosa
T cell counts. HIV-positive individuals with CD4+ T cell counts <300 (Fig. 197-34D), or a swollen lymph node. Lesions often appear in sun-
cells/μL have a poorer response to malaria treatment than others. Co- exposed areas, particularly the tip of the nose, and have a propensity
infection with malaria is associated with a modest increase in HIV viral to occur in areas of trauma (Koebner phenomenon). Because of the
PART 5
load. The risk of malaria may be decreased with TMP-SMX prophylaxis. vascular nature of the tumors and the presence of extravasated red
Generalized wasting is an AIDS-defining condition; it is defined blood cells in the lesions, their colors range from reddish to purple to
as involuntary weight loss of >10% associated with intermittent or brown and often take the appearance of a bruise, with yellowish discol-
constant fever and chronic diarrhea or fatigue lasting >30 days in oration and tattooing. Lesions range in size from a few millimeters to
the absence of a defined cause other than HIV infection. Prior to the several centimeters in diameter and may be either discrete or confluent.
Infectious Diseases
widespread use of cART it was the initial AIDS-defining condition in KS lesions most commonly appear as raised macules; however, they
~10% of patients with AIDS in the United States. Generalized wast- can also be papular, particularly in patients with higher CD4+ T cell
ing is rarely seen today with the earlier initiation of antiretrovirals. counts. Confluent lesions may give rise to surrounding lymphedema
A constant feature of this syndrome is severe muscle wasting with and may be disfiguring when they involve the face and disabling
scattered myofiber degeneration and occasional evidence of myositis. when they involve the lower extremities or the surfaces of joints. Apart
Glucocorticoids may be of some benefit; however, this approach must from skin, the lymph nodes, GI tract, and lung are the organ systems
be carefully weighed against the risk of compounding the immunode- most commonly affected by KS. Lesions have been reported in virtu-
ficiency of HIV infection. Androgenic steroids, growth hormone, and ally every organ, including the heart and the CNS. In contrast to most
total parenteral nutrition have been used as therapeutic interventions malignancies, in which lymph node involvement implies metastatic
with variable success. spread and a poor prognosis, lymph node involvement may be seen
very early in KS and is of no special clinical significance. In fact, some
Neoplastic Diseases The neoplastic diseases considered to be patients may present with disease limited to the lymph nodes. These
AIDS-defining conditions are Kaposi’s sarcoma, non-Hodgkin’s lym- are generally patients with relatively intact immune function and thus
phoma, and invasive cervical carcinoma. In addition, there is also an the patients with the best prognosis. Pulmonary involvement with KS
increase in the incidence of a variety of non-AIDS-defining malig- generally presents with shortness of breath. Some 80% of patients with
nancies including Hodgkin’s disease; multiple myeloma; leukemia; pulmonary KS also have cutaneous lesions. The chest x-ray character-
melanoma; and cervical, brain, testicular, oral, lung, gastric, liver, istically shows bilateral lower lobe infiltrates that obscure the margins
renal, and anal cancers. Since the introduction of potent cART, there of the mediastinum and diaphragm (Fig. 197-43). Pleural effusions are
has been a marked reduction in the incidence of KS (Fig. 197-34). The seen in 70% of cases of pulmonary KS, a fact that is often helpful in the
non-AIDS-defining malignancies now account for more morbidity differential diagnosis. GI involvement is seen in 50% of patients with
A B C
FIGURE 197-42 Kaposi’s sarcoma in three patients with AIDS demonstrating (A) periorbital edema and bruising; (B) classic truncal distribution of lesions; and (C)
upper extremity lesions.
Harrisons_20e_Part5_p0859-p1648.indd 1448 6/1/18 12:08 PM
TABLE 197-18 Management of AIDS-Associated Kaposi’s Sarcoma 1449
Observation and optimization of antiretroviral therapy
Single or limited number of lesions
Radiation
Intralesional vinblastine
Cryotherapy
Extensive disease
Initial therapy
Interferon α (if CD4+ T cells >150/μL)
Liposomal daunorubicin
Subsequent therapy
Liposomal doxorubicin
Paclitaxel
Combination chemotherapy with low-dose doxorubicin, bleomycin, and
vinblastine (ABV)
Targeted radiation
patients in whom tumor persists or is compromising vital functions or
in whom control of HIV replication is not possible, a variety of options
FIGURE 197-43 Chest x-ray of a patient with AIDS and pulmonary Kaposi’s exist. In some cases, lesions remain quite indolent, and many of these
sarcoma. The characteristic findings include dense bilateral lower lobe infiltrates patients can be managed with no specific treatment. Fewer than 10%
obscuring the heart borders and pleural effusions. of AIDS patients with KS die as a consequence of their malignancy,
and death from secondary infections is considerably more common.
KS and usually takes one of two forms: (1) mucosal involvement, which Thus, whenever possible one should avoid treatment regimens that
may lead to bleeding that can be severe; these patients sometimes also may further suppress the immune system and increase susceptibility
develop symptoms of GI obstruction if lesions become large; and (2) to opportunistic infections. Treatment is indicated under two main
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
biliary tract involvement. KS lesions may infiltrate the gallbladder and circumstances. The first is when a single lesion or a limited number of
biliary tree, leading to a clinical picture of obstructive jaundice similar lesions are causing significant discomfort or cosmetic problems, such
to that seen with sclerosing cholangitis. Several staging systems have as with prominent facial lesions, lesions overlying a joint, or lesions
been proposed for KS. One in common use was developed by the in the oropharynx that interfere with swallowing or breathing. Under
National Institute of Allergy and Infectious Diseases AIDS Clinical these circumstances, treatment with localized radiation, intralesional
Trials Group; it distinguishes patients on the basis of tumor extent, vinblastine, topical 9-cis-retinoic acid, or cryotherapy may be helpful.
immunologic function, and presence or absence of systemic disease It should be noted that patients with HIV infection are particularly
(Table 197-17). sensitive to the side effects of radiation therapy. This is especially true
A diagnosis of KS is based on biopsy of a suspicious lesion. Histo- with respect to the development of radiation-induced mucositis; doses
logically one sees a proliferation of spindle cells and endothelial cells, of radiation directed at mucosal surfaces, particularly in the head and
extravasation of red blood cells, hemosiderin-laden macrophages, and, neck region, should be adjusted accordingly. The use of systemic ther-
in early cases, an inflammatory cell infiltrate. Included in the differen- apy, either IFN-α or chemotherapy, should be considered in patients
tial diagnosis are lymphoma (particularly for oral lesions), bacillary with a large number of lesions or in patients with visceral involvement.
angiomatosis, and cutaneous mycobacterial infections. The single most important determinant of response appears to be the
Management of KS (Table 197-18) should be carried out in con- CD4+ T cell count. This relationship between response rate and base-
sultation with an expert since definitive treatment guidelines do not line CD4+ T cell count is particularly true for IFN-α. The response rate
exist. In the majority of cases, effective cART will go a long way in to IFN-α for patients with CD4+ T cell counts >600/μL is ~80%, while
achieving control. Antiretroviral therapy has been associated with the the response rate for patients with counts <150/μL is <10%. In contrast
spontaneous regression of KS lesions. Paradoxically, it has also been to the other systemic therapies, IFN-α provides an added advantage
associated with the initial appearance of KS as a form of IRIS. For of having antiretroviral activity; thus, it may be the appropriate first
choice for single-agent systemic therapy for early patients with dissem-
TABLE 197-17 National Institute of Allergy and Infectious Diseases inated disease. A variety of chemotherapeutic agents also have been
AIDS Clinical Trials Group TIS Staging System For Kaposi’s Sarcoma shown to have activity against KS. Four of them—liposomal daunoru-
GOOD RISK (STAGE 0): POOR RISK (STAGE 1): ANY bicin, liposomal doxorubicin, vinblastine, and paclitaxel—have been
PARAMETER ALL OF THE FOLLOWING OF THE FOLLOWING approved by the FDA for this indication. Liposomal daunorubicin is
Tumor (T) Confined to skin and/ Tumor-associated edema or approved as first-line therapy for patients with advanced KS. It has
or lymph nodes and/or ulceration fewer side effects than conventional chemotherapy. In contrast, liposo-
minimal oral disease Extensive oral lesions mal doxorubicin and paclitaxel are approved only for KS patients who
GI lesions have failed standard chemotherapy. Response rates vary from 23% to
Nonnodal visceral lesions 88%, appear to be comparable to what had been achieved earlier with
Immune system (I) CD4+ T cell count CD4+ T cell count <200/μL combination chemotherapy regimens, and are greatly influenced by
≥200/μL CD4+ T cell count.
Systemic illness (S) No B symptomsa B symptomsa present Lymphomas occur with an increased frequency in patients with con-
Karnofsky performance Karnofsky performance genital or acquired T cell immunodeficiencies (Chap. 344). AIDS is no
status ≥70 status <70 exception; at least 6% of all patients with AIDS develop lymphoma at
No history of History of opportunistic some time during the course of their illness. This is a 120-fold increase
opportunistic infection, infection, neurologic disease, in incidence compared with the general population. In contrast to the
neurologic disease, lymphoma, or thrush situation with KS, primary CNS lymphoma, and most opportunistic
lymphoma, or thrush infections, the incidence of AIDS-associated systemic lymphomas has
a
Defined as unexplained fever, night sweats, >10% involuntary weight loss, or not experienced a dramatic decrease as a consequence of the wide-
diarrhea persisting for more than 2 weeks. spread use of effective cART. Lymphoma occurs in all risk groups,
Harrisons_20e_Part5_p0859-p1648.indd 1449 6/1/18 12:08 PM
1450 with the highest incidence in patients with hemophilia and the lowest
incidence in patients from the Caribbean or Africa with heterosexually
acquired infection. Lymphoma is a late manifestation of HIV infection,
generally occurring in patients with CD4+ T cell counts <200/μL. As
HIV disease progresses, the risk of lymphoma increases. The attack
rate for lymphoma increases exponentially with increasing duration of
HIV infection and decreasing level of immunologic function. At 3 years
following a diagnosis of HIV infection, the risk of lymphoma is 0.8%
per year; by 8 years after infection, it is 2.6% per year. As individuals
with HIV infection live longer as a consequence of improved cART
and better treatment and prophylaxis of opportunistic infections, it is
anticipated that the incidence of lymphomas may increase.
Three main categories of lymphoma are seen in patients with HIV
infection: grade III or IV immunoblastic lymphoma, Burkitt’s lym-
phoma, and primary CNS lymphoma. Approximately 90% of these
lymphomas are B cell in phenotype; more than half contain EBV DNA.
Some are associated with KSHV. These tumors may be either monoclo-
FIGURE 197-44 Immunoblastic lymphoma involving the hard palate of a patient
nal or oligoclonal in nature and are probably in some way related to
with AIDS.
the pronounced polyclonal B cell activation seen in patients with AIDS.
Immunoblastic lymphomas account for ~60% of the cases of lymphoma
in patients with AIDS. The majority of these are diffuse large B cell pronounced than that seen with toxoplasmosis. Locations that are most
lymphomas (DLBCL). They are generally high grade and would have commonly involved with CNS lymphoma are deep in the white matter.
been classified as diffuse histiocytic lymphomas in earlier classification The main diseases in the differential diagnosis are cerebral toxoplasmo-
schemes. This tumor is more common in older patients, increasing in sis and cerebral Chagas’ disease. In addition to the 20% of lymphomas
incidence from 0% in HIV-infected individuals <1 year old to >3% in in HIV-infected individuals that are primary CNS lymphomas, CNS
those >50 years of age. Two variants of immunoblastic lymphoma that disease is also seen in HIV-infected patients with systemic lymphoma.
are seen primarily in HIV-infected patients are primary effusion lym- Approximately 20% of patients with systemic lymphoma have CNS
phoma (PEL) and its solid variant, plasmacytic lymphoma of the oral disease in the form of leptomeningeal involvement. This fact under-
cavity. PEL, also referred to as body cavity lymphoma, presents with scores the importance of lumbar puncture in the staging evaluation of
PART 5
lymphomatous pleural, pericardial, and/or peritoneal effusions in the patients with systemic lymphoma.
absence of discrete nodal or extranodal masses. The tumor cells do not Systemic lymphoma is seen at earlier stages of HIV infection than
express surface markers for B cells or T cells and are felt to represent primary CNS lymphoma. In one series the mean CD4+ T cell count was
a preplasmacytic stage of differentiation. While both HHV-8 and EBV 226/μL. In addition to lymph node involvement, systemic lymphoma
DNA sequences have been found in the genomes of the malignant cells may commonly involve the GI tract, bone marrow, liver, and lung. GI
Infectious Diseases
from patients with body cavity lymphoma, KSHV is felt to be the driv- tract involvement is seen in ~25% of patients. Any site in the GI tract
ing force behind the oncogenesis (see above). may be involved, and patients may complain of difficulty swallowing
Small noncleaved cell lymphoma (Burkitt’s lymphoma) accounts for ~20% or abdominal pain. The diagnosis is usually suspected on the basis of
of the cases of lymphoma in patients with AIDS. It is most frequent in CT or MRI of the abdomen. Bone marrow involvement is seen in ~20%
patients 10–19 years old and usually demonstrates characteristic c-myc of patients and may lead to pancytopenia. Liver and lung involvement
translocations from chromosome 8 to chromosome 14 or 22. Burkitt’s are each seen in ~10% of patients. Pulmonary disease may present as a
lymphoma is not commonly seen in the setting of immunodeficiency mass lesion, multiple nodules, or an interstitial infiltrate.
other than HIV-associated immunodeficiency, and the incidence of this Both conventional and unconventional approaches have been
particular tumor is more than 1000-fold higher in the setting of HIV employed in an attempt to treat HIV-related lymphomas. Systemic
infection than in the general population. In contrast to African Burkitt’s lymphoma is generally treated by the oncologist with combination
lymphoma, where 97% of the cases contain EBV genome, only 50% of chemotherapy. Earlier disappointing figures are being replaced with
HIV-associated Burkitt’s lymphomas are EBV-positive.
Primary CNS lymphoma accounts for ~20% of the cases of lymphoma
in patients with HIV infection. In contrast to HIV-associated Burkitt’s
lymphoma, primary CNS lymphomas are usually positive for EBV.
In one study, the incidence of Epstein-Barr positivity was 100%. This
malignancy does not have a predilection for any particular age group.
The median CD4+ T cell count at the time of diagnosis is ~50/μL. Thus,
CNS lymphoma generally presents at a later stage of HIV infection
than does systemic lymphoma. This may explain, at least in part, the
poorer prognosis for this subset of patients.
The clinical presentation of lymphoma in patients with HIV infec-
tion is quite varied, ranging from focal seizures to rapidly growing
mass lesions in the oral mucosa (Fig. 197-44) to persistent unexplained
fever. At least 80% of patients present with extranodal disease, and a
similar percentage have B-type symptoms of fever, night sweats, or
weight loss. Virtually any site in the body may be involved. The most
common extranodal site is the CNS, which is involved in approxi-
mately one-third of all patients with lymphoma. Approximately 60% of
these cases are primary CNS lymphoma. Primary CNS lymphoma gen-
erally presents with focal neurologic deficits, including cranial nerve
FIGURE 197-45 Central nervous system lymphoma. Postcontrast T1-weighted
findings, headaches, and/or seizures. MRI or CT generally reveals MRI scan in a patient with AIDS, altered mental status, and hemiparesis. Multiple
a limited number (one to three) of 3- to 5-cm lesions (Fig. 197-45). enhancing lesions, some ring-enhancing, are present. The left sylvian lesion
The lesions often show ring enhancement on contrast administration shows gyral and subcortical enhancement, and the lesions in the caudate and
and may occur in any location. Contrast enhancement is usually less splenium (arrowheads) show enhancement of adjacent ependymal surfaces.
Harrisons_20e_Part5_p0859-p1648.indd 1450 6/1/18 12:08 PM
more optimistic results for the treatment of systemic lymphoma follow- other genotypes such as 58 and 53 also are prominent. This raises con- 1451
ing the availability of more effective cART and the use of rituximab in cerns about the level of effectiveness of the current HPV vaccines for
CD20+ tumors. While there is some controversy regarding the use of HIV-infected patients. Despite this, it is recommended that patients
antiretrovirals during chemotherapy, there is no question that their use with HIV infection be vaccinated against HPV.
overall in patients with HIV lymphoma has improved survival. Con-
cerns regarding synergistic bone marrow toxicities with chemotherapy IDIOPATHIC CD4+ T LYMPHOCYTOPENIA
and cART are mitigated with the use of cART regimens that avoid bone A syndrome was recognized in 1992 characterized by an absolute
marrow–toxic antiretrovirals. As in most situations in patients with CD4+ T cell count of <300/μL or <20% of total T cells on a minimum
HIV disease, those with higher CD4+ T cell counts tend to fare better. of two occasions at least 6 weeks apart; no evidence of HIV-1, HIV-2,
Response rates as high as 72% with a median survival of 33 months and HTLV-1, or HTLV-2 on testing; and the absence of any defined immu-
disease-free intervals up to 9 years have been reported. Treatment of nodeficiency or therapy associated with decreased levels of CD4+
primary CNS lymphoma remains a significant challenge. Treatment is T cells. By mid-1993, ~100 patients had been described. After extensive
complicated by the fact that this illness usually occurs in patients with multicenter investigations, a series of reports were published in early
advanced HIV disease. Palliative measures such as radiation therapy 1993, which together allowed a number of conclusions. Idiopathic
provide some relief. The prognosis remains poor in this group, with a CD4+ lymphocytopenia (ICL) is a very rare syndrome, as determined
2-year survival of 29%. by studies of blood donors and cohorts of HIV-seronegative men who
Multicentric Castleman’s disease is a KSHV-associated lymphoprolif- have sex with men. Cases were clearly identified as early as 1983 and
erative disorder that is seen with an increased frequency in patients were remarkably similar to the clinical features of ICL that had been
with HIV infection. While not a true malignancy, it shares many identified decades earlier. The definition of ICL based on CD4+ T cell
features with lymphoma including generalized lymphadenopathy, counts coincided with the ready availability of testing for CD4+ T cells
hepatosplenomegaly, and systemic symptoms of fever, fatigue, and in patients suspected of being immunodeficient. Although, as a result
weight loss. Pulmonary symptoms may be seen in ~50% of patients. of immune deficiency, certain patients with ICL develop some of the
KS is present in 75–82% of cases. Lymph node biopsies reveal a pre- opportunistic diseases (particularly cryptococcosis, nontuberculous
dominance of interfollicular plasma cells and/or germinal centers with mycobacterial infections, and cervical dysplasia) seen in HIV-infected
vascularization and an “onionskin” (hyaline vascular) appearance. patients, the syndrome is demographically, clinically, and immunolog-
Prior to the availability of cART, HIV-infected patients with multicen- ically unlike HIV infection and AIDS. Fewer than half of the reported
tric Castleman’s disease had a 15-fold increased risk of developing ICL patients had risk factors for HIV infection, and there were wide
non-Hodgkin’s lymphoma compared with HIV-infected patients in geographic and age distributions. The fact that a significant propor-
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
general. Treatment typically involves chemotherapy. Anecdotal reports tion of patients did have risk factors probably reflects a selection bias,
of success with rituximab suggest that more specific treatment may be in that physicians who take care of HIV-infected patients are more
successful, although, in one series treatment with rituximab was associ- likely to monitor CD4+ T cells. Approximately half of the patients are
ated with worsening of coexisting KS. The median survival of patients women, compared with approximately one-third among HIV-infected
with treated multicentric Castleman’s disease pre-cART was initially individuals in the United States. Many patients with ICL remained
reported as 14 months. This has increased to a 2-year survival of more clinically stable, and their condition did not deteriorate progressively
than 90% in the era of cART. as is common with seriously immunodeficient HIV-infected patients.
Evidence of infection with human papillomavirus (HPV), associated Approximately 15% of patients with ICL experience spontaneous reversal
with intraepithelial dysplasia of the cervix or anus, is approximately twice of the CD4+ T lymphocytopenia. Immunologic abnormalities in ICL
as common in HIV-infected individuals as in the general population are somewhat different from those of HIV infection. ICL patients often
and can lead to intraepithelial neoplasia and eventually invasive have increases in CD4+ T cell activation with decreases in CD8+ T cells
cancer. In a series of studies, HIV-infected men were examined for evi- and B cells. Furthermore, immunoglobulin levels are either normal or,
dence of anal dysplasia, and Papanicolaou (Pap) smears were found to more commonly, decreased in patients with ICL, compared with the
be abnormal in 20–80%. These changes tend to persist and are generally usual hypergammaglobulinemia of HIV-infected individuals. Virologic
not affected by cART, raising the possibility of a subsequent transition studies of these patients have revealed no evidence of HIV-1, HIV-2,
to a more malignant condition. While the incidence of an abnormal Pap HTLV-1, or HTLV-2 or of any other mononuclear cell–tropic virus. Fur-
smear of the cervix is ~5% in otherwise healthy women, the incidence thermore, there has been no epidemiologic evidence to suggest that a
of abnormal cervical smears in women with HIV infection is 30–60%, transmissible microbe was involved. The cases of ICL have been widely
and invasive cervical cancer is included as an AIDS-defining condition. dispersed, with no clustering. Close contacts and sexual partners who
While only small increases in the absolute numbers of cervical or anal were studied were clinically well and were serologically, immunolog-
cancers have been seen as a consequence of HIV infection, the relative ically, and virologically negative for HIV. ICL is a heterogeneous syn-
risk of these conditions when one compares HIV-infected to nonin- drome, and it is highly likely that there is no common cause; however,
fected men and women is on the order of 10- to 100-fold. Given the high there may be common causes among subgroups of patients that are
rates of dysplasia and relative risks for cervical and anal cancer, a com- currently unrecognized.
prehensive gynecologic and rectal examination, including Pap smear, Patients who present with laboratory data consistent with ICL
is indicated at the initial evaluation and 6 months later for all patients should be worked up for underlying diseases that could be responsi-
with HIV infection. If these examinations are negative at both time ble for the immune deficiency. If no underlying cause is detected, no
points, the patient should be followed with yearly evaluations. If an specific therapy should be initiated. However, if opportunistic diseases
initial or repeat Pap smear shows evidence of severe inflammation with occur, they should be treated appropriately (see above). Depending on
reactive squamous changes, the next Pap smear should be performed the level of the CD4+ T cell count, patients should receive prophylaxis
at 3 months. If, at any time, a Pap smear shows evidence of squamous for the commonly encountered opportunistic infections.
intraepithelial lesions, colposcopic examination with biopsies as indi-
cated should be performed. The 2-year survival rate for HIV-infected
patients with invasive cervical cancer is 64% compared with 79% in
TREATMENT
non-HIV-infected patients. In addition to rectal and cervical lesions, AIDS and Related Disorders
HPV can also lead to head and neck cancers. In one study of men who
have sex with men, 25% were found to have oral HPV; high-risk HPV GENERAL PRINCIPLES OF PATIENT MANAGEMENT
genotypes were three times more common in the HIV-infected men. The CDC guidelines call for the testing for HIV infection to be a
The most common HPV genotypes in the general population and part of routine medical care. It is recommended that the patient be
the genotypes upon which current HPV vaccines are based are 6, 11, informed of the intention to test, as is the case with other routine
16, and 18. This is not the case in the HIV-infected population, where laboratory determinations, and be given the opportunity to “opt
Harrisons_20e_Part5_p0859-p1648.indd 1451 6/1/18 12:08 PM
1452 out.” Such an approach is critical to the goal of identifying as many TABLE 197-19 Initial Evaluation of the Patient with HIV Infection
infected individuals as possible since 15% of the 1.1 million indi- History and physical examination
viduals in the United States who are HIV-infected are not aware of
Routine chemistry and hematology
their status. Under these circumstances of routine testing, although
AST, ALT, alkaline phosphatase, direct and indirect bilirubin
it is desirable, pretest counseling may not always be built into the
testing process. However, no matter how well prepared a patient Lipid profile and fasting glucose
is for adversity, the discovery of a diagnosis of HIV infection is a CD4+ T lymphocyte count
devastating event. Thus, physicians should be sensitive to this fact Plasma HIV RNA level
and, where possible, execute some degree of pretest counseling to at HIV resistance testing
least partially prepare the patient should the results demonstrate the HLA-B5701 screening
presence of HIV infection. Following a diagnosis of HIV infection, RPR or VDRL test
the health care provider should be prepared to immediately activate Anti-Toxoplasma antibody titer
support systems for the newly diagnosed patient and initiate cART Urinalysis
therapy. These supports should include individuals who can spend
PPD skin test or IFN-γ release assay
time talking to the newly diagnosed person and ensuring that he or
Mini-Mental Status Examination
she is emotionally stable and ready to begin therapy. Most commu-
Serologies for hepatitis A, hepatitis B, and hepatitis C
nities have HIV support centers that can be of great help in these
difficult situations. Immunization with pneumococcal polysaccharide; influenza; HPV as indicated
The treatment of patients with HIV infection requires not only Immunization with hepatitis A and hepatitis B if seronegative
a comprehensive knowledge of the possible disease processes that Counseling regarding natural history and transmission
may occur and up-to-date knowledge of and experience with Help contacting others who might be infected
cART, but also the ability to deal with the problems of a chronic, Abbreviations: ALT, alanine aminotransferase; AST, aspartate aminotransferase;
potentially life-threatening illness. A comprehensive knowledge of PPD, purified protein derivative; RPR, rapid plasma reagin; VDRL, Venereal
internal medicine is required to deal with the changing spectrum of Disease Research Laboratory.
illnesses associated with HIV infection, many of which are similar
to a state of accelerated aging. Great advances have been made in HLA-B5701 testing should be done in all patients in whom the drug
the treatment of patients with HIV infection. The appropriate use of abacavir is being considered. Patients should be immunized with
potent cART and other treatment and prophylactic interventions are pneumococcal polysaccharide, with annual influenza shots, and, if
of critical importance in providing each patient with the best oppor- seronegative for these viruses, with HPV, hepatitis A, and hepatitis
PART 5
tunity to live a long and healthy life with HIV infection. In contrast B vaccines. The status of hepatitis C infection should be determined.
to the earlier days of this epidemic, a diagnosis of HIV infection In addition, patients should be counseled with regard to sexual
need no longer be equated with having an inevitably fatal disease. practices and needle sharing, and counseling should be offered to
In addition to medical interventions, the health care provider has a those whom the patient knows or suspects may also be infected.
responsibility to provide each patient with appropriate counseling Once these baseline activities are performed, short- and long-term
Infectious Diseases
and education concerning their disease as part of a comprehensive medical management strategies should be developed based on the
care plan. Patients must be educated about the potential transmis- most recent information available and modified as new information
sibility of their infection and about the fact that while health care becomes available. The field of HIV medicine is changing rapidly,
providers may refer to levels of the virus as “undetectable,” this is and it is difficult to remain fully up-to-date. Fortunately there are a
only a reflection of the sensitivity of the assay being used to measure series of excellent sites on the Internet that are frequently updated,
the virus, rather than a comment on the presence or absence of the and they provide the most recent information on a variety of topics,
virus. It is important for patients to be aware that the virus is still including consensus panel reports on treatment (Table 197-20).
present in virtually all patients who have ever been diagnosed with ANTIRETROVIRAL THERAPY
HIV infection and capable of being transmitted at all stages of HIV
Combination antiretroviral therapy (cART), also referred to as
disease. Thus, there must be frank discussions concerning sexual
highly active antiretroviral therapy (HAART), is the cornerstone of
practices and the sharing of syringes and other paraphernalia used
management of patients with HIV infection. Following the initia-
in illicit drug use. The treating physician not only must be aware of
tion of widespread use of cART in the United States in 1995–1996,
the latest medications available for patients with HIV infection but
marked declines were noted in the incidence of most AIDS-defining
also must educate patients concerning the natural history of their ill-
conditions (Fig. 197-34). Suppression of HIV replication is an
ness and listen and be sensitive to their fears and concerns. As with
important component in prolonging life as well as in improving the
other diseases, therapeutic decisions should be made in consultation
quality of life in patients with HIV infection. Adequate suppression
with the patient, when possible, and with the patient’s proxy if the
requires strict adherence to prescribed regimens of antiretroviral
patient is incapable of making decisions. In this regard, it is recom-
drugs. This has been facilitated by the coformulations of antiretro-
mended that all patients with HIV infection, and in particular those
virals and the development of once-daily regimens. Unfortunately,
with CD4+ T cell counts <200/μL, designate a trusted individual
many of the most important questions related to the treatment of
with durable power of attorney to make medical decisions on their
HIV disease currently lack definitive answers. Among the deci-
behalf, if necessary.
sions that need to be made in the context of prescribing cART
Following a diagnosis of HIV infection, there are several exami-
are when therapy should be started, selection of the best initial
nations and laboratory studies that should be performed to help
regimen, when a given regimen should be changed, and what it
determine the extent of disease and provide baseline standards
for future reference (Table 197-19). In addition to routine chem- TABLE 197-20 HIV Disease Resources Available on the World Wide
istry, fasting lipid profile, aspartate aminotransferase, alanine Web
aminotransferase, total and direct bilirubin, fasting glucose and www.aidsinfo.nih.gov AIDSinfo, a service of the U.S. Department of Health
hematology screening panels, Pap smear, urinalysis, and chest x-ray, and Human Services, posts federally approved
one should also obtain a CD4+ T cell count, a plasma HIV RNA treatment guidelines for HIV and AIDS; provides
level, an HIV resistance test, a rapid plasma reagin or VDRL information on federally funded and privately funded
test, an anti-Toxoplasma antibody titer, and serologies for hepatitis clinical trials and CDC publications and data
A, B, and C. A PPD test or IFN-γ release assay should be done and an www.cdcnpin.org Updates on epidemiologic data and prevention
MMSE performed and recorded. A pregnancy test should be done information from the CDC
in women in whom the drug efavirenz is being considered, and Abbreviation: CDC, Centers for Disease Control and Prevention.
Harrisons_20e_Part5_p0859-p1648.indd 1452 6/1/18 12:08 PM
should be changed to when a change is made. The care provider additional antiretroviral medication. The reverse transcriptase inhib- 1453
and patient must come to a mutually agreeable plan based on the itors block the HIV replication cycle at the point of RNA-dependent
best available data. In an effort to facilitate this process, the U.S. DNA synthesis, the reverse transcription step. While the nonnu-
Department of Health and Human Services makes available on cleoside reverse transcriptase inhibitors are quite selective for the
the Internet (www.aidsinfo.nih.gov) a series of periodically updated HIV-1 reverse transcriptase, the nucleoside and nucleotide analogues
guidelines, including “Guidelines for the Use of Antiretroviral Agents inhibit a variety of DNA polymerases in addition to those of the
in HIV-Infected Adults and Adolescents” and “Guidelines for the Pre- HIV-1 reverse transcriptase. For this reason, serious side effects are
vention of Opportunistic Infections in Persons Infected with Human more varied with the nucleoside analogues and include mitochon-
Immunodeficiency Virus.” At present, an extensive clinical trials net- drial damage that can lead to hepatic steatosis and lactic acidosis as
work, involving both clinical investigators and patient advocates, well as peripheral neuropathy and pancreatitis. The use of either of
is in place attempting to develop improved approaches to therapy. the thymidine analogues zidovudine and stavudine has been associ-
Consortia comprising representatives of academia, industry, inde- ated with a syndrome of hyperlipidemia, glucose intolerance/insulin
pendent foundations, and the federal government are involved in resistance, and fat redistribution often referred to as lipodystrophy syn-
the process of drug development, including a wide-ranging series drome (discussed in “Diseases of the Endocrine System and Metabolic
of clinical trials. As a result, new therapies and new therapeutic Disorders,” above). The reverse transcriptase inhibitors preferred for
strategies are continually emerging. New drugs are often avail- use in combination regimens according to the DHHS Panel on the
able through expanded-access programs prior to official licensure. use of antiretroviral drugs are lamivudine, emtricitabine, abacavir,
Given the complexity of this field, decisions regarding cART are tenofovir disoproxil, and tenofovir alafenamide.
best made in consultation with experts. The HIV-1 protease inhibitors (saquinavir, indinavir, ritonavir,
Currently available drugs for the treatment of HIV infection nelfinavir, amprenavir, fosamprenavir, lopinavir/ritonavir, ataza-
as part of a combination regimen fall into four categories: those navir, tipranavir, and darunavir) are an important part of the
that inhibit the viral reverse transcriptase enzyme (nucleoside and therapeutic armamentarium of antiretrovirals. While possessing
nucleotide reverse transcriptase inhibitors; nonnucleoside reverse antiviral properties of its own, ritonavir is typically used as a phar-
transcriptase inhibitors), those that inhibit the viral protease enzyme macokinetic enhancer due to its high affinity for several isoforms
(protease inhibitors), those that inhibit the viral integrase enzyme of cytochrome P450 (3A4, 2D6) leading to large increases in the
(integrase inhibitors), and those that interfere with viral entry plasma concentrations of co-administered drugs metabolized by
(fusion inhibitors; CCR5 antagonists) (Table 197-21; Fig. 197-46). these pathways As in the case of reverse transcriptase inhibitors,
Numerous formulations combining two or more of these antiretro- resistance to protease inhibitors can develop rapidly in the setting
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
viral drugs have been licensed (Table 197-22). Prior to initiation of of monotherapy, and thus these agents should be used only as
therapy and at any time a change in therapy due to treatment failure part of combination therapeutic regimens. Based upon superior
is being considered, drug resistance testing should be performed efficacy and side-effect profile, ritonavir-boosted darunavir in com-
to help guide the selection of drugs to be used in combination. A bination with emtricitabine and tenofovir disoproxil or tenofovir
summary of known resistance mutations for antiretroviral drugs is alafenamide is the protease inhibitor strategy preferred for initial
shown in Fig. 197-47. therapy according to the DHHS Panel on the use of antiretroviral
The FDA-approved reverse transcriptase inhibitors include the drugs.
nucleoside analogues zidovudine, didanosine, zalcitabine, stavudine, Integrase inhibitors act by blocking the action of the HIV integrase
lamivudine, abacavir, and emtricitabine; the nucleotide analogues enzyme and thus preventing integration of the HIV provirus into the
tenofovir disoproxil and tenofovir alafenamide; and the nonnucleo- host cell genome. They are among the most potent and safest of the
side reverse transcriptase inhibitors nevirapine, delavirdine, efavirenz, antiretroviral drugs and frequently part of initial combination reg-
etravirine, and rilpivirine (Table 197-21). These represent the first imens. The four licensed integrase inhibitors are raltegravir, elvite-
class of drugs licensed for the treatment of HIV infection. They are gravir, dolutegravir, and bictegravir. Elvitegravir is always given in
indicated for this use as part of combination regimens. It should be combination with cobicistat, which acts to boost the concentrations
stressed that none of these drugs should be used as monotherapy of elvitegravir. Cobicistat also inhibits tubular secretion of creatinine,
for HIV infection due to the relative ease with which drug resistance resulting in increases in serum creatinine, and is not recommended
may develop under such circumstances. Thus, when lamivudine, for patients with estimated creatinine clearances <70 mL/min. Bict-
emtricitabine, or tenofovir is used to treat hepatitis B infection in the egravir is available only in combination with tenofovir alafenamide
setting of HIV infection, one should ensure that the patient is also on and emtricitabine.
TABLE 197-21 Antiretroviral Drugs Most Commonly Used in the Treatment of HIV Infection
DOSE IN
DRUG STATUS INDICATION COMBINATION SUPPORTING DATA TOXICITY
Nucleoside or Nucleotide Reverse Transcriptase Inhibitors
Zidovudine (AZT, Licensed Treatment of HIV infection 200 mg q8h or 300 19 vs 1 death in original placebo- Anemia,
azidothymidine, in combination with other mg bid controlled trial in 281 patients with AIDS
granulocytopenia,
*Retrovir, 3’azido-3’- antiretroviral agents or ARC myopathy, lactic
deoxythymidine) acidosis, hepatomegaly
with steatosis,
headache, nausea,
nail pigmentation,
lipid abnormalities,
lipoatrophy,
hyperglycemia
Prevention of maternal-fetal In pregnant women with CD4+ T cell count
HIV transmission ≥200/μL, AZT PO beginning at weeks
14–34 of gestation plus IV drug during
labor and delivery plus PO AZT to infant
for 6 weeks decreased transmission of
HIV by 67.5% (from 25.5% to 8.3%);
n = 363
(Continued)
Harrisons_20e_Part5_p0859-p1648.indd 1453 6/1/18 12:08 PM
1454 TABLE 197-21 Antiretroviral Drugs Most Commonly Used in the Treatment of HIV Infection (Continued)
DOSE IN
DRUG STATUS INDICATION COMBINATION SUPPORTING DATA TOXICITY
Lamivudine (Epivir, Licensed In combination with other 150 mg bid In combination with AZT superior to AZT Flare of hepatitis in HBV-
2’3’-dideoxy-3’- antiretroviral agents for the 300 mg qd alone with respect to changes in CD4+ co-infected patients who
thiacytidine, 3TC) treatment of HIV infection T cell counts in 495 patients who were discontinue drug
zidovudine-naïve and 477 patients who
were zidovudine-experienced; overall
CD4+ T cell counts for the zidovudine
group were at baseline by 24 weeks, while
in the group treated with zidovudine plus
lamivudine, they were 10–50 cells/μL above
baseline; 54% decrease in progression to
AIDS/death compared with AZT alone
Emtricitabine (FTC, Licensed In combination with other 200 mg qd Comparable to lamivudine in combination Hepatotoxicity in HBV-
Emtriva) antiretroviral agents for the with stavudine and nevirapine/efavirenz co-infected patients who
treatment of HIV infection discontinue drug, skin
discoloration
Abacavir (Ziagen) Licensed For treatment of HIV infection 300 mg bid Abacavir + AZT + 3TC equivalent to Hypersensitivity
in combination with other indinavir + AZT + 3TC with regard to viral reaction In HLA-B5701+
antiretroviral agents load suppression (~60% in each group individuals (can be fatal);
with <400 HIV RNA copies/mL plasma) fever, rash, nausea,
and CD4+ T cell increase (~100/μL in vomiting, malaise or
each group) at 24 weeks fatigue, and loss of
appetite
Tenofovir disoproxil Licensed For use in combination with 300 mg qd Reduction of ~0.6 log in HIV-1 RNA levels Renal, osteomalacia,
fumarate (Viread) other antiretroviral agents when added to background regimen in flare of hepatitis in HBV-
when treatment is indicated treatment-experienced patients co-infected patients who
discontinue drug
Tenofovir alafenamide Licensed In combination with 25 mg qd 92% of patients treated in combination Nausea, less renal
(Vemlidy) emtricitabine and other with emtricitabine, elvitegravir, and toxicity than tenofovir
antiretroviral agents for cobicistat had HIV-1 RNA levels <50 disoproxil fumarate
PART 5
treatment of HIV-1 infection copies/mL
Non-Nucleoside Reverse Transcriptase Inhibitors
Nevirapine (Viramune) Licensed In combination with other 200 mg/d × Increase in CD4+ T cell count, decrease Skin rash, hepatotoxicity
antiretroviral agents for 14 days then 200 in HIV RNA when used in combination with
Infectious Diseases
treatment of progressive HIV mg bid nucleosides
infection or
400 mg extended
release qd
Efavirenz (Sustiva) Licensed For treatment of HIV infection 600 mg qhs Efavirenz + AZT + 3TC comparable to Rash, dysphoria,
in combination with other indinavir + AZT + 3TC with regard to viral elevated liver function
antiretroviral agents load suppression (a higher percentage tests, drowsiness,
of the efavirenz group achieved viral load abnormal dreams,
<50 copies/mL, but the discontinuation depression, lipid
rate in the indinavir group was abnormalities, potentially
unexpectedly high, accounting for most teratogenic
treatment “failures”); CD4 cell increase
(~140/μL in each group) at 24 weeks
Etravirine (Intelence) Licensed In combination with other 200 mg bid Higher rates of HIV RNA suppression to Rash, nausea,
antiretroviral agents in <50 copies/mL (56% vs 39%); greater hypersensitivity reactions
treatment-experienced increases in CD4+ T cell count (89 vs
patients whose HIV is 64 cells) compared to placebo when
resistant to nonnucleoside given in combination with an optimized
reverse transcriptase background regimen
inhibitors and other
antiretroviral medications
Rilpivirine (Edurant) Licensed In combination with other 25 mg qd Noninferior to efavirenz with respect Nausea, dizziness,
drugs in previously untreated to suppression at week 48 in 1368 somnolence, vertigo,
patients when treatment is treatment-naive individuals, except in less CNS toxicity and
indicated. patients with pretherapy HIV RNA levels rash than efavirenz
>100,000 where it was inferior
Protease Inhibitors
Ritonavir (Norvir) Licensed In combination with other 600 mg bid (also Reduction in the cumulative incidence Nausea, abdominal
antiretroviral agents for used in lower doses of clinical progression or death from pain, hyperglycemia,
treatment of HIV infection as pharmacokinetic 34% to 17% in patients with CD4+ T cell fat redistribution, lipid
when treatment is warranted booster) count <100/μL treated for a median of abnormalities, may alter
6 months levels of many other
drugs, paresthesias,
hepatitis
(Continued)
Harrisons_20e_Part5_p0859-p1648.indd 1454 6/1/18 12:08 PM
TABLE 197-21 Antiretroviral Drugs Most Commonly Used in the Treatment of HIV Infection (Continued) 1455
DOSE IN
DRUG STATUS INDICATION COMBINATION SUPPORTING DATA TOXICITY
Atazanavir (Reyataz) Licensed For treatment of HIV infection 400 mg qd or Comparable to efavirenz when given in Hyperbilirubinemia, PR
in combination with other 300 mg qd + combination with AZT + 3TC in a study of prolongation, nausea,
antiretroviral agents ritonavir 100 mg 810 treatment-naïve patients; comparable vomiting, hyperglycemia,
qd when given with to nelfinavir when given in combination fat maldistribution, rash
efavirenz with stavudine + 3TC in a study of 467 transaminase elevations,
treatment-naïve patients renal stones
Darunavir (Prezista) Licensed In combination with 600 mg + At 24 weeks, patients with prior extensive Diarrhea, nausea,
100 mg ritonavir for 100 mg ritonavir exposure to antiretrovirals treated with headache, skin
combination therapy in twice daily with food a new combination including darunavir rash, hepatotoxicity,
treatment-experienced adults showed a –1.89-log change in HIV RNA hyperlipidemia,
levels and a 92-cell increase in CD4+ hyperglycemia
T cells compared with –0.48 log and
17 cells in the control arm
Entry Inhibitors
Enfuvirtide (Fuzeon) Licensed In combination with other 90 mg SC bid In treatment of experienced patients, Local injection reactions,
agents in treatment- superior to placebo when added to new hypersensitivity
experienced patients with optimized background (37% vs 16% with reactions, increased rate
evidence of HIV-1 replication <400 HIV RNA copies/mL at 24 weeks; + of bacterial pneumonia
despite ongoing anti- 71 vs + 35 CD4+ T cells at 24 weeks)
retroviral therapy
Maraviroc (Selzentry) Licensed In combination with other 150–600 mg At 24 weeks, among 635 patients with Hepatotoxicity,
antiretroviral agents in adults bid depending CCR5-tropic virus and HIV-1 RNA nasopharyngitis, fever,
infected with only CCR5- on concomitant >5000 copies/mL despite at least cough, rash, abdominal
tropic HIV-1 medications (see 6 months of prior therapy with at least pain, dizziness,
text) 1 agent from 3 of the 4 antiretroviral drug musculoskeletal
classes, 61% of patients randomized symptoms
to maraviroc achieved HIV RNA levels
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
<400 copies/mL compared with 28% of
patients randomized to placebo
Ibalizumab (Trogarzo) Licensed In combination with other Single loading dose At 25 weeks, 50% of patients with Rash, diarrhea, nausea
antiretroviral agents in of 2000 mg followed multi-drug resistant HIV-1 with HIV-1
patients with multidrug- by a maintenance RNA >1000 copies/mL treated with an
resistant HIV-1 dose of 800 mg optimized background of 1 active drug
every 2 weeks and ibalizumab achieved HIV RNA levels
<200 copies/mL
Integrase Inhibitor
Raltegravir (Isentress) Licensed In combination with other 400 mg bid At 24 weeks, among 436 patients with Nausea, headache,
antiretroviral agents 3-class drug resistance, 76% of patients diarrhea, CPK elevation,
randomized to receive raltegravir achieved muscle weakness,
HIV RNA levels <400 copies/mL compared rhabdomyolysis
with 41% of patients randomized to
receive placebo
Elvitegravir Licensed Fixed-dose combination 1 tablet daily Noninferior to raltegravir or atazanavir/ Diarrhea, nausea, upper
(Available only in ritonavir in treatment-experienced respiratory infections,
combination with patients. headache
cobicistat, tenofovir,
and emtricitabine
[Stribild])
Dolutegravir (Tivicay) Licensed In combination with other 50 mg daily for Noninferior to raltegravir, superior to Insomnia, headache,
antiretroviral agents treatment-naïve efavirenz or darunavir/ritonavir hypersensitivity
patients reactions, hepatotoxicity
50 mg twice daily
for treatment-
experienced
patients or those
also receiving
efavirenz or rifampin
Bictegravir Licensed For treatment of HIV infection 50 mg bictegravir/ Non-inferior to dolutegravir/tenofovir/ Nausea, diarrhea,
(Available only in in adults 25 mg tenofovir emtricitabine and non-inferior to headache
combination with alafenamide/ dolutegravir/abacavir/lamivudine
tenofovir alafenamide 200 mg
and emtricitabine emtricitabine qd
[Biktarvy]
*Initial trade names are provided. Generic forms may be available.
Abbreviations: ARC, AIDS-related complex; NRTIs, nonnucleoside reverse transcriptase inhibitors.
Harrisons_20e_Part5_p0859-p1648.indd 1455 6/1/18 12:08 PM
1456 Nucleoside or Nucleotide Reverse Transcriptase Inhibitors
O NH2
CH3 HN HO
HN N N
N N O
NH2 O
N O H2SO4 N
O N
N NH
HN N H2N N N O P OPh
NH O
HOCH2 O
HO O N N HO– N O CH3 O OH 1/2
O H3C
CH2OH 2 O
N3 H H
Zidovudine Didanosine Zalcitabine Abacavir Tenofovir alafenamide
NH2
NH2 N
O N
H CH3 N O O
N N N H CO2H
N O N O OH H2N N O O P O O O C C
O
O N O O O O HO2C H
HO F
S OH CH3
H
H S O
Stavudine Lamivudine Emtricitabine Tenofovir disoproxil fumarate
Nonnucleoside Reverse Transcriptase Inhibitors N
CH3
CH–CH3
H CH3 H O F3C
CH3 SO2 N NH N H3C CH3
Cl H
O O N N
N N N N N N
C N O N
H N
H Br
O N
CH3 SO2 OH N NH2
Delavirdine C N Nevirapine Efavirenz Etravirine
PART 5
HN N NH
Infectious Diseases
Rilpivirine
Protease Inhibitors
H3C CH3
O O S O O CH3
H O O H
N N N O N N O
S N HO N N
H H N H HN N
N CH3 O S H O H
H3 C OH OH H3C
CH3 OH
H
Lopinavir
NH2
N
O
O
NH2 H OH HN O
N OH O S
N O N
N H2SO4 N
O H OH O H
N H O N OCH H2S
NH N H N N N N
NH H3CO
O O OH H H
O OH O NHC(CH3 )3 O O
O
NHC(CH3 )3
×CH3 SO3 H
H
OH H O O
N O H O O
SO2 S
O N H C2 H5 OH
O O N HH H OH N
H3 C NH2
CF3 CH3
Darunavir
FIGURE 197-46 Molecular structures of antiretroviral agents.
Harrisons_20e_Part5_p0859-p1648.indd 1456 6/1/18 12:08 PM
Entry Inhibitors 1457
O NH2 O NH2 O OH
HO
HO HO
O O O O O O O
O H H H H H H H
N N N N N N N N N N N N N N N O
H O H H H H H H H
NH O O O O O O
H2N H2N
HO N HO
O O NH
O HN O OH
OH
O
NH O
O
H 2N
HN
O O
H2 N Ibalizumab
NH
HO
NH2
O
HO
O O
HN O
N H O O O H O O H NH
H N H H H N
N N N N N N N N N
H2N O H H O
H O H O O H O
OH O HN O
OH O
O NH
NH2
HO O HN
F
O
F Me
H N
N N N
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
N N H
Enfuvirtide N
O H O
Me Me NH2
Maraviroc
CI
O F
Integrase Inhibitors H
O O F O
H O F N N
HO H
O
N N N
O F N O O F F
H
N N N H N H
O F O OH
N N N
O OH O
Me OH
Elvitegravir Raltegravir Dolutegravir Bictegravir
FIGURE 197-46 (Continued)
Entry inhibitors act by interfering with the binding of HIV to its initiating antiretroviral therapy must be willing to commit to life-
receptor or co-receptor or by interfering with the process of fusion long treatment and understand the importance of adherence to
(see above). The first drug in this class to be licensed was the fusion their prescribed regimen. The importance of adherence is illustrated
inhibitor enfuvirtide, or T-20, followed by the CCR5 antagonist mara- by the observation that treatment interruption is associated with
viroc. The anti-CD4 monoclonal antibody ibalizumab was licensed in rapid increases in HIV RNA levels, rapid declines in CD4+ T cell
2018, and a variety of additional small molecules that bind to HIV-1 counts, and an increased risk of clinical progression. While it seems
co-receptors are currently in clinical trials. reasonable to assume that the complications associated with cART
could be minimized by intermittent treatment regimens designed to
PRINCIPLES OF THERAPY minimize exposure to the drugs in question, all efforts to do so have
The principles of therapy for HIV infection have been articulated paradoxically been associated with an increase in serious adverse
by a panel sponsored by the U.S. Department of Health and Human events in the patients randomized to intermittent therapy, suggest-
Services as a working group of the NIH Office of AIDS Research ing that some “non-AIDS-associated” serious adverse events such
Advisory Council. These principles are summarized in Table 197-23. as heart attack and stroke may be linked to HIV replication. Thus,
As noted in these guidelines, cART of HIV infection does not lead to unless contraindicated for reasons of toxicity, patients started on
eradication or cure of HIV. The single possible exception to this is cART should remain on cART.
an individual with HIV infection who received an allogeneic stem At present, the U.S. Department of Health and Human Services
cell transplant for treatment of acute myelogenous leukemia. His Guidelines panel recommends that everyone with HIV infection be
conditioning regimen included cytotoxic chemotherapy, total-body treated with cART and that therapy be initiated a soon as possible
irradiation, and antithymocyte immunoglobulin. The donor cells after diagnosis. Therapy has been associated with a decrease in dis-
were homozygous for the CCR5∆32 mutation (see above) and thus ease progression in patients at all stages of HIV infection and leads
resistant to HIV infection. Despite cART being stopped the day of to a decrease in the risk of transmission of infection. In addition, one
the transplant, the patient has exhibited no signs of active HIV infec- may wish to administer a 6-week course of therapy to uninfected
tion for more than 8 years. individuals immediately following a high-risk exposure to HIV.
Treatment decisions must take into account the fact that one is The combination of tenofovir and emtricitabine is also indicated
dealing with a chronic infection that requires daily therapy. Patients for pre-exposure prophylaxis in individuals at high risk of HIV
Harrisons_20e_Part5_p0859-p1648.indd 1457 6/1/18 12:08 PM
1458 TABLE 197-22 Combination Formulations of Antiretroviral Drugs for a change in therapy include a persistently declining CD4+ T
cell count, a consistent increase in HIV RNA levels to >200 copies/
NAME COMBINATION
mL, clinical deterioration, or drug toxicity (Table 197-25). As in the
Atripla* Tenofovir disoproxil fumarate + emtricitabine +
efavirenz
case of initiating therapy, changing therapy may have a lasting
impact on future therapeutic options. When changing therapy
Biktarvy* Tenofovir alafenamide + emtricitabine + bictegravir
because of treatment failure (clinical progression or worsening lab-
Cimduo Tenofovir disoproxil fumarate + lamivudine
oratory parameters), it is important to attempt to provide a regimen
Combivir Zidovudine + lamivudine with at least two new active drugs. This decision can be guided by
Complera* Tenofovir disoproxil fumarate+ emtricitabine + resistance testing (see below). In the patient in whom a change is
rilpivirine
made for reasons of drug toxicity, a simple replacement of one drug
Descovy Tenofovir alafenamide + emtricitabine is reasonable. It should be stressed that in attempting to sort out a
Dutrebis Raltegravir + lamivudine drug toxicity it may be advisable to hold all therapy for a period of
Epzicom Abacavir + lamivudine time to distinguish between drug toxicity and disease progression.
Evotaz Atazanavir + cobicistat Drug toxicity will usually begin to show signs of reversal within
Genvoya* Tenofovir alafenamide + emtricitabine + elvitegravir + 1–2 weeks. Prior to changing a treatment regimen because of drug
cobicistat failure, it is important to ensure that the patient has been adherent to
Juluca Dolutegravir + rilpivirine the prescribed regimen. As in the case of initial therapy, the simpler
Kaletra Lopinavir + ritonavir the new therapeutic regimen, the easier it is for the patient to be
Odefsey* Tenofovir alafenamide +emtricitabine + rilpivirine compliant. Plasma HIV RNA levels should be monitored every 3–6
Prezcobix Darunavir + cobicistat months during therapy and more frequently if one is contemplating
Stribild* Tenofovir disoproxil fumarate + emtricitabine +
a change in regimen due to an increase in viral load or immediately
elvitegravir + cobicistat following a change in regimen.
Symfi* Tenofovir disoproxil fumarate + lamivudine + efavirenz In order to determine an optimal therapeutic regimen for initial
(600 mg) therapy or for a patient on a failing regimen, one may attempt to
Symfi Lo* Tenofovir disoproxil fumarate + lamivudine + efavirenz measure antiretroviral drug susceptibility through genotyping or
(400 mg) phenotyping of HIV quasispecies and to determine adequacy of dos-
Triumeq* Abacavir + lamivudine + dolutegravir ing through measurement of drug levels. Genotyping may be done
Truvada Tenofovir disoproxil fumarate + emtricitabine through cDNA sequencing. Phenotypic assays typically measure
the enzymatic activity of viral enzymes in the presence or absence
Trizivir Zidovudine + lamivudine + abacavir
PART 5
of different concentrations of different drugs and have also been
*Complete, once-daily, single tablet regimens. used to determine co-receptor tropism. These assays will generally
detect quasispecies present at a frequency of ≥10%. Next-generation
infection. For patients diagnosed with an opportunistic infection sequencing may allow detection of quasispecies at frequencies down
to 1%. It is generally recommended that resistance testing be used
Infectious Diseases
and HIV infection at the same time, one may consider a 2- to 4-week
delay in the initiation of antiretroviral therapy during which time in selecting initial therapy in settings where the risk of transmission
treatment is focused on the opportunistic infection. This delay may of resistant virus is high (such as the United States and Europe) and
decrease the severity of any subsequent immune reconstitution in determining new regimens for patients experiencing virologic
inflammatory syndrome by lowering the antigenic burden of the failure while on therapy. Resistance testing may be of particular
opportunistic infection. This is particularly true for patients with value in distinguishing drug-resistant virus from poor patient com-
TB or cryptococcal infections. For patients with advanced HIV pliance. Due to the rapid rate at which drug-resistant viruses revert
infection (CD4+ <50 cells/μL), however, cART should be initiated to wild-type, it is recommended that resistance testing performed
as soon as possible. in the setting of drug failure be carried out while the patient is still
Once the decision has been made to initiate therapy, the health on the failing regimen. Measurement of plasma drug levels can also
care provider must decide which drugs to use as the first regimen. be used to tailor an individual treatment. The inhibitory quotient,
The decision regarding choice of drugs not only will affect the imme- defined as the trough blood level/IC50 of the patient’s virus, is used
diate response to therapy but also will have implications regarding by some to determine the adequacy of dosing of a given treatment
options for future therapeutic regimens. The initial regimen is regimen. Despite the best of efforts there will still be patients with
usually the most effective insofar as the virus has yet to develop sig- ongoing high levels of HIV replication while receiving the best avail-
nificant resistance. HIV is capable of rapidly developing resistance able therapy. These patients will receive benefit from remaining on
to any single agent, and therapy must be given as a multidrug com- antiretroviral therapy even though it is not fully suppressive.
bination. Given that patients can be infected with viruses that harbor In addition to the licensed medications discussed above, a large
drug resistance mutations, it is recommended that a viral genotype number of experimental agents are being evaluated as possible ther-
be done prior to the initiation of therapy to optimize the selection apies for HIV infection. Therapeutic strategies are being developed
of antiretroviral agents. The combination regimens currently recom- to interfere with virtually every step of the replication cycle of the
mended for initial therapy in most treatment-naïve patients are listed virus (Fig. 197-3) and in an attempt to eliminate the reservoir of
in Table 197-24. It is currently debated whether treatment-naïve infected cells to “cure” HIV infection. In addition to directly acting
individuals with <50 copies/mL of HIV RNA benefit from cART. antiviral drugs, other strategies, generically referred to as “immune-
While these individuals are at low risk of disease progression in the based therapies,” are being developed as a complement to antiviral
short term, they do have evidence of persistent immune activation therapy. Among the antiviral agents in early clinical trials are addi-
that may have long-term consequences. Following the initiation of tional nucleoside and nucleotide analogues, protease inhibitors,
therapy one should expect a rapid, at least 1-log (tenfold) reduction fusion inhibitors, receptor and co-receptor antagonists, and integrase
in plasma HIV RNA levels within 1–2 months and then a slower inhibitors—as well as new antiviral strategies including antisense
decline in plasma HIV RNA levels to <50 copies/mL within nucleic acids and maturation inhibitors. Among the immune-based
6 months. During this same time there should be a rise in the CD4+ therapies being evaluated are monoclonal antibodies, IFN-α, bone
T cell count of 100–150/cells μL that is also particularly brisk dur- marrow transplantation, adoptive transfer of lymphocytes geneti-
ing the first month of therapy. Subsequently, one should anticipate cally modified to resist infection or enhance HIV-specific immunity,
a CD4+ T cell count increase of 50–100 cells/year until numbers active immunotherapy with inactivated HIV or its components, IL-7,
approach normal. Many clinicians feel that failure to achieve these and IL-15. Strategies directed toward cure are examining the role of
endpoints is an indication for a change in therapy. Other reasons latency-reversing agents such as histone-deacetylase inhibitors.
Harrisons_20e_Part5_p0859-p1648.indd 1458 6/1/18 12:08 PM
HIV AND THE HEALTH CARE WORKER since 1999. Approximately 85% of the exposures resulting in infection 1459
Health care workers, especially those who deal with large numbers have been due to percutaneous (puncture/cut injury) exposures to
of HIV-infected patients, have a small but definite risk of becoming HIV-infected blood. The individuals with documented seroconversions
infected with HIV as a result of professional activities (see “Occupa- included 19 laboratory workers (16 of whom were clinical laboratory
tional Transmission of HIV: Health Care Workers, Laboratory Workers, workers), 24 nurses, 16 clinical laboratory technicians, 6 physicians, 4
and the Health Care Setting,” above). nonclinical laboratory technicians, 2 housekeepers, 2 surgical technicians,
In the United States 58 health care workers for whom case investi- 1 dialysis technician, 1 respiratory therapist, 1 health aide, 1 embalmer/
gations have been completed have had documented seroconversions to morgue technician, and 1 unknown. In addition, at least 150 possible
HIV following occupational exposures. Only one of these has occurred cases of occupationally acquired HIV infection have been reported among
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
FIGURE 197-47 Amino acid substitutions conferring resistance to antiretroviral drugs. For each amino acid residue, the letter above the bar indicates the amino acid
associated with wild-type virus and the letter(s) below indicate the substitution(s) that confer viral resistance. The number shows the position of the mutation in the
protein. Mutations selected by protease inhibitors in Gag cleavage sites are not listed. HR1, first heptad repeat; NAMs, nRTI-associated mutations; nRTI, nucleoside
reverse transcriptase inhibitor; NNRTI, nonnucleoside reverse transcriptase inhibitor; PI, protease inhibitor. Amino acid abbreviations: A, alanine; C, cysteine; D, aspartate;
E, glutamic acid; F, phenylalanine; G, glycine; H, histidine; I, isoleucine; K, lysine; L, leucine; M, methionine; N, asparagine; P, proline; Q, glutamine; R, arginine; S, serine;
T, threonine; V, valine; W, tryptophan; Y, tyrosine. (Reprinted with permission from the International Antiviral Society—USA. AM Wensing, V Calvez, HR Günthard et al:
2014 Update of the Drug Resistance Mutations in HIV-1. Top Antivir Med 22:642, 2014. Updated information [and thorough explanatory notes] available at www.iasusa.org.)
Harrisons_20e_Part5_p0859-p1648.indd 1459 6/1/18 12:09 PM
1460
PART 5
Infectious Diseases
FIGURE 197-47 (Continued)
health care personnel in the United States. The number of these workers usually through an accident involving a suture needle, failed to reveal
who actually acquired their infection through occupational exposures any cases of possible occupational infection, suggesting that the risk of
is not known. Taken together, data from several large studies suggest infection with a suture needle may be considerably less than that with a
that the risk of HIV infection following a percutaneous exposure to HIV- blood-drawing (hollow-bore) needle.
contaminated blood is ~0.2323%, and after a mucous membrane expo- Most cases of health care worker seroconversion occur as a result
sure, ~0.09%. Although episodes of HIV transmission after nonintact of needle-stick injuries. When one considers the circumstances that
skin exposure have been documented, the average risk for transmission result in needle-stick injuries, it is immediately obvious that adhering
by this route has not been precisely quantified but is estimated to be less to the standard guidelines for dealing with sharp objects would result
than the risk for mucous membrane exposures. The risk for transmission in a significant decrease in this type of accident. In one study, 27% of
after exposure to body fluids or tissues other than HIV-infected blood also needle-stick injuries resulted from improper disposal of the needle
has not been quantified but is probably considerably lower than for blood (over half of these were due to recapping the needle), 23% occurred
exposures. A seroprevalence survey of 3420 orthopedic surgeons, 75% of during attempts to start an IV line, 22% occurred during blood draw-
whom practiced in an area with a relatively high prevalence of HIV infec- ing, 16% were associated with an IM or SC injection, and 12% were
tion and 39% of whom reported percutaneous exposure to patient blood, associated with giving an IV infusion.
Harrisons_20e_Part5_p0859-p1648.indd 1460 6/1/18 12:09 PM
TABLE 197-23 Principles of Therapy of HIV Infection TABLE 197-25 Indications for Changing Antiretroviral Therapy in 1461
1. Ongoing HIV replication leads to immune system damage, progression to Patients with HIV Infectiona
AIDS, and systemic immune activation. Less than a 1-log drop in plasma HIV RNA by 4 weeks following the initiation
2. Plasma HIV RNA levels indicate the magnitude of HIV replication and the of therapy
rate of CD4+ T cell destruction. CD4+ T cell counts indicate the current A reproducible significant increase (defined as threefold or greater) from
level of competence of the immune system. the nadir of plasma HIV RNA level not attributable to intercurrent infection,
3. Maximal suppression of viral replication is a goal of therapy; the vaccination, or test methodology
greater the suppression the less likely the appearance of drug-resistant Persistently declining CD4+ T cell numbers
quasispecies. Clinical deterioration
4. The most effective therapeutic strategies involve the simultaneous Side effects
initiation of combinations of effective anti-HIV drugs with which the patient
has not been previously treated and that are not cross-resistant with a
Generally speaking, a change should involve the initiation of at least two drugs
antiretroviral agents that the patient has already received. felt to be effective in the given patient. The exception to this is when change is
being made to manage toxicity, in which case a single substitution is reasonable.
5. The antiretroviral drugs used in combination regimens should be used
Source: Guidelines for the Use of Antiretroviral Agents in HIV-Infected Adults and
according to optimum schedules and dosages.
Adolescents, USPHS.
6. The number of available drugs is limited. Any decisions on antiretroviral
therapy have a long-term impact on future options for the patient.
7. Women should receive optimal antiretroviral therapy regardless of
antigen-HIV antibody test is utilized for follow-up HIV testing of the
pregnancy status. exposed health care worker, HIV testing may be concluded 4 months
8. The same principles apply to children and adults. The treatment of HIV- after exposure; if a newer testing platform is not available, follow-up
infected children involves unique pharmacologic, virologic, and immunologic HIV testing is typically concluded 6 months after an HIV exposure.
considerations. For consultation on the treatment of occupational exposures to HIV
9. Compliance is an important part of ensuring maximal effect from a given and other bloodborne pathogens, the clinician managing the exposed
regimen. The simpler the regimen, the easier it is for the patient to be patient can call the National Clinicians’ Post-Exposure Prophylaxis
compliant. Hotline (PEPline) at 888-448-4911. This service is available 24 hours a
Source: Modified from Principles of Therapy of HIV Infection, USPHS, and the Henry day at no charge. (Additional information on the Internet is available
J. Kaiser Family Foundation. at www.nccc.ucsf.edu.) PEPline support may be especially useful in
challenging situations, such as when drug-resistant HIV strains are
Occupational exposures to HIV should be considered as a medical suspected or the health care worker is pregnant.
CHAPTER 197 Human Immunodeficiency Virus Disease: AIDS and Related Disorders
emergency to ensure timely postexposure management and admin- Health care workers can minimize their risk of occupational HIV
istration of postexposure antiretroviral prophylaxis (PEP). Recom- infection by following the CDC guidelines of June 2015, which include
mendations regarding PEP must take into account that a variety of adherence to universal precautions, assuming that blood and other
circumstances determine the risk of transmission of HIV following body fluids from all patients are potentially infectious. Therefore, the
occupational exposure. In this regard, several factors have been following infection control precautions should be adhered to at all
associated with an increased risk for occupational transmission of times: (1) routinely use barriers (such as gloves and/or goggles) when
HIV infection, including deep injury, the presence of visible blood on anticipating contact with blood or body fluids; (2) immediately wash
the instrument causing the exposure, injury with a device that had hands and other skin surfaces after contact with blood or body fluids;
been placed in the vein or artery of the source patient, and advanced and (3) carefully handle and dispose of sharp instruments during and
HIV disease in the source patient. Other important considerations after use. For further information contact the CDC at 800-CDC-INFO
when considering PEP in the health care worker include known or (232-4636) or see www.cdc.gov/info. In attempting to put this small but
suspected pregnancy or breast-feeding, the possibility of exposure definite occupational risk of HIV infection to the health care worker in
to drug-resistant virus, and the toxicities of different PEP regimens. perspective, it is important to point out that ~200 health care workers
Regardless of the decision to use PEP, the wound should be cleansed die each year as a result of occupationally acquired hepatitis B infec-
immediately and antiseptic applied. If a decision is made to offer PEP, tion. The tragedy in this instance is that these infections and deaths due
U.S. Public Health Service guidelines recommend that PEP regimens to HBV could be greatly decreased by more extended use of the HBV
contain 3 (or more) antiretroviral drugs administered for a 4-week vaccine. The risk of HBV infection following a needle-stick injury from
duration for all occupational exposures to HIV. Detailed guidelines a hepatitis antigen–positive patient is much higher than the risk of HIV
are available from the Updated U.S. Public Health Service Guidelines infection (see “Transmission,” above). There are multiple examples of
for the Management of Occupational Exposures to HIV and Recommenda- needle-stick injuries where the patient was positive for both HBV and
tions for Postexposure Prophylaxis (CDC, 2013). The report emphasizes HIV and the health care worker became infected only with HBV. For
the importance of adherence to PEP when it is indicated, and close these reasons, it is advisable, given the high prevalence of HBV infec-
follow-up of exposed workers should be provided including coun- tion in HIV-infected individuals, that all health care workers dealing
seling, baseline and follow-up HIV testing, and monitoring for drug with HIV-infected patients be immunized with the HBV vaccine.
toxicity. Follow-up appointments should begin within 72 h of an TB is another infection common to HIV-infected patients that can be
HIV exposure, and if newer fourth-generation combination HIV p24 transmitted to the health care worker. For this reason, all health care
workers should know their PPD status, have it checked yearly, and,
TABLE 197-24 Initial Combination Regimens Recommended for where appropriate, receive 6 months of isoniazid treatment if their skin
Most Treatment-Naïve Patients Regardless of HIV RNA Level or CD4 test converts to positive. In addition, all patients in whom a diagnosis
Count of pulmonary TB is being entertained should be placed immediately
Dolutegravir + tenofovir* + emtricitabine** in respiratory isolation, pending results of the diagnostic evaluation.
Raltegravir + tenofovir* + emtricitabine** The emergence of drug-resistant organisms, including extensively
Bictegravir + tenofovir*+ emtricitabine** drug-resistant TB strains, has made TB an increasingly important prob-
Elvitegravir + cobicistat + tenofovir* + emtricitabine** lem for health care workers. This is particularly true for the health care
Dolutegravir + abacavir + lamivudine** (only for those HLA-B*5701 negative) worker with preexisting HIV infection.
One of the most charged issues ever to come between health
*Tenofovir alafenamide and tenofovir disoproxil fumarate are two forms of
care workers and patients is that of transmission of infection from
tenofovir approved by FDA. Tenofovir alafenamide has fewer bone and renal
toxicities while tenofovir disoproxil fumarate is associated with lower lipid HIV-infected health care workers to their patients. This is discussed in
levels. **Lamivudine may substitute for emtricitabine and vice versa. “Occupational Transmission of HIV: Health Care Workers, Laboratory
Source: Guidelines for the Use of Antiretroviral Agents in HIV-Infected Adults and Workers, and the Health Care Setting,” above. Theoretically, the same
Adolescents, USPHS. universal precautions that are used to protect the health care worker
Harrisons_20e_Part5_p0859-p1648.indd 1461 6/1/18 12:09 PM
1462 from the HIV-infected patient will also protect the patient from the for their affinity maturation and broadly neutralizing capacity. The goal
HIV-infected health care worker. of current efforts is to develop the conformationally correct HIV enve-
lope epitopes that, when used as immunogens, would direct the immune
VACCINE FOR THE PREVENTION OF HIV response of an uninfected individual to the production of broadly neu-
INFECTION tralizing antibodies over a reasonable time frame by sequential immu-
There is currently no safe and effective vaccine that has been approved nizations. It remains to be seen whether this approach will be feasible.
for the prevention of HIV infection. Successful vaccines are predicated
on the assumptions that the body can mount an adequate immune PREVENTION OF HIV ACQUISITION
response to the microbe or virus in question during natural infection Education, counseling, and behavior modification are the cornerstones
and that the vaccine will mimic the natural response to infection. Even of any HIV prevention strategy. A major problem in the United States
with serious diseases, such as smallpox, poliomyelitis, measles, and and elsewhere is that many infections are passed on by those who do
influenza among others, the body in the vast majority of cases clears not know that they are infected. Of the ~1.1 million persons in the United
the infectious agent and provides protection, which is usually life-long States who are HIV-infected, it is estimated that ~15% do not know their
against future exposure against the same pathogen. Unfortunately, this HIV status and approximately 23% of all new infections are transmitted
is not the case with HIV infection since the natural immune response by those people who are not aware that they are infected. In this regard,
to HIV infection is unable to clear the virus from the body and cases of the CDC has recommended that HIV testing become part of routine
superinfection are not uncommon. Some of the factors that contribute medical care and that all individuals between the ages of 13 and 64 years
to the problematic nature of development of a preventive HIV vaccine be tested at least one time. These individuals should be informed of the
are (1) the high mutability of the virus; (2) the fact that the infection testing and be tested without the need for written informed consent.
can be transmitted by cell-free or cell-associated virus; (3) the fact that Each individual can “opt out” of testing, but testing should otherwise
the HIV provirus integrates itself into the genome of the target cell and be routinely administered. Individuals who are practicing high-risk
may remain in a latent form unexposed to the immune system; (4) the behavior should be tested more often. In addition to identifying individ-
likely need for the development of effective mucosal immunity; and uals who might benefit from cART, information gathered from such an
(5) the fact that it has been difficult to establish the precise correlates approach should serve as the basis for behavior-modification programs,
of protective immunity to HIV infection. A fraction of a percent of both for infected individuals who may be unaware of their HIV status
HIV-infected individuals are “elite controllers” in that they maintain and who could infect others and for uninfected individuals practicing
extremely low and even undetectable levels of viremia in the absence high-risk behavior. The practice of “safer sex” is the most effective way
of cART, and a number of individuals have been exposed to HIV mul- for sexually active uninfected individuals to avoid contracting HIV
tiple times but remain uninfected; these facts suggest that there are infection and for infected individuals to avoid spreading infection.
PART 5
elements of host defense or an HIV-specific immune response that have Abstinence from sexual relations is the only absolute way to prevent
the potential to be protective against acquisition of infection. Early sexual transmission of HIV infection. However, for most individuals
attempts to develop a vaccine with the envelope protein gp120 aimed this is not feasible, and there are a number of relatively safe practices
at inducing neutralizing antibodies in humans were unsuccessful; the that can markedly decrease the chances of transmission of HIV infection.
elicited antisera failed to neutralize primary isolates of HIV cultured Partners engaged in monogamous sexual relationships who wish to be
Infectious Diseases
and tested in fresh peripheral blood mononuclear cells. In this regard, assured of safety should both be tested for HIV antibody. If both are
two phase 3 trials were undertaken in the United States and Thailand negative, it must be understood that any divergence from monogamy
using soluble gp120, and the vaccines failed to protect human volun- puts both partners at risk; open discussion of the importance of honesty
teers from HIV infection. In addition, two separate vaccine trials aimed in such relationships should be encouraged. When the HIV status of
at eliciting CD8+ T cell responses to prevent infection and, if unsuc- either partner is not known, or when one partner is positive, there are a
cessful in preventing infection, to control postinfection viremia, also number of options. Use of condoms can markedly decrease the chance of
failed at both goals. In 2009, a vaccine using a poxvirus vector prime HIV transmission. It should be remembered that condoms are not 100%
expressing various viral proteins followed by an envelope protein effective in preventing transmission of HIV infection, and there is a ~10%
boost was tested in a 16,000-person clinical trial (RV144) conducted in failure rate of condoms used for contraceptive purposes. Most condom
Thailand among predominantly low-HIV-prevalence heterosexuals. failures result from breakage or improper usage, such as not wearing the
The vaccine provided the first positive, albeit very modest, signal condom for the entire period of intercourse. Latex condoms are pref-
ever reported in an HIV vaccine trial, showing 31% protection against erable, since virus has been shown to leak through natural skin con-
acquisition of infection. Such a result is certainly not sufficient justifi- doms. Petroleum-based gels should never be used for lubrication
cation for clinical use of the vaccine, but it served as an important first of the condom, since they increase the likelihood of condom rupture.
step in the direction of the development of a safe and effective vaccine Some men who have sex with men practice exclusively fellatio as a “min-
against HIV infection. Follow-up studies of RV144 indicate that non- imal-risk” activity compared with anal intercourse. It should be empha-
neutralizing or weakly neutralizing antibody responses against certain sized that receptive fellatio is not guaranteed safe sex, and although the
constant epitopes in the otherwise highly variable V1-V2 region of the incidence of transmission via fellatio is considerably less than that of
HIV envelope may be associated with the modest degree of protection rectal or vaginal intercourse, there has been documentation of transmis-
observed in that clinical trial. Additional similar studies are being sion of HIV where receptive fellatio was the only sexual act performed
conducted in high-HIV-prevalence countries in sub-Saharan Africa in (see “Transmission,” above). Topical microbicides composed of gels con-
attempts to improve on the results of RV144 by a variety of approaches, taining antiretroviral drugs have been shown to be only modestly and
including increasing the number of vaccine boosts with envelope pro- variably efficacious in preventing acquisition of HIV infection in women
tein and the addition of adjuvant. engaging in vaginal intercourse. The considerable degree of variability
An area of HIV vaccine research that is currently being actively in efficacy relates to the generally poor adherence of participants to
pursued is the attempt to induce broadly neutralizing antibodies by the use of the intervention. Pre-exposure prophylaxis (PrEP) using oral
developing as immunogens for vaccination certain epitopes on the HIV antiretroviral drugs such as Truvada (tenofovir + emtricitabine) as a sin-
envelope that are the targets of naturally occurring broadly neutralizing gle daily pill in uninfected men who have sex with men and transgender
antibodies during HIV infection. It is curious that only about 20% of women is highly efficacious in preventing acquisition of HIV infection.
HIV-infected individuals develop broadly neutralizing antibodies in The degree of efficacy can be greater than 95% if subjects adhere strictly
response to natural infection and they do so only after 2–3 years of ongo- to the regimen. CDC estimates that approximately 1.2 million people in
ing infection. By the time these antibodies appear, they can neutralize a the United States are at “substantial risk” for HIV infection and should
broad range of primary HIV isolates, but they appear to be ineffective be counseled about PrEP. As of 2016, however, fewer than half of primary
against the autologous virus in the infected subject. Upon close exami- physicians and nurses have heard of PrEP.
nation, these broadly neutralizing antibodies manifest a high degree of Adult male circumcision, which has been shown to result in a
somatic mutations that were accumulated over time and are responsible 50–65% reduction in HIV acquisition in the circumcised subject, is
Harrisons_20e_Part5_p0859-p1648.indd 1462 6/1/18 12:09 PM
currently being pursued, particularly in developing nations, as a com- gastroenteritis. Among healthy young adults, acute gastroenteritis is 1463
ponent of HIV prevention. The most effective way to prevent trans- rarely fatal but incurs substantial medical and social costs, including
mission of HIV infection among IDUs is to stop the use of injectable those of time lost from work.
drugs. Unfortunately, that is extremely difficult to accomplish unless Several enteric viruses have been recognized as important etiologic
the individual enters a treatment program. For those who will not or agents of acute infectious gastroenteritis (Table 198-1, Fig. 198-1).
cannot participate in a drug treatment program and who will continue Although most viral gastroenteritis is caused by RNA viruses, the
to inject drugs, the avoidance of sharing of needles and other parapher- DNA viruses that are occasionally involved (e.g., adenovirus types 40
nalia (“works”) is the next best way to avoid transmission of infection. and 41) are included in this chapter. Illness caused by these viruses is
However, the cultural and social factors that contribute to the sharing characterized by the acute onset of vomiting and/or diarrhea, which
of paraphernalia are complex and difficult to overcome. Under these may be accompanied by fever, nausea, abdominal cramps, anorexia,
circumstances, paraphernalia should be cleaned after each usage with and malaise. As shown in Table 198-2, several features can help distin-
a virucidal solution, such as undiluted sodium hypochlorite (house- guish gastroenteritis caused by viruses from that caused by bacterial
hold bleach). Needle exchange programs have been highly successful agents. However, the distinction based on clinical and epidemiologic
in decreasing HIV transmission among injection drug users without parameters alone is often difficult, and laboratory tests are required to
increasing the use of injection drugs. Oral PrEP also is effective in pre- confirm the diagnosis.
venting acquisition of HIV infections among IDUs. It is important for
IDUs to be tested for HIV infection and counseled to avoid transmis- ■ HUMAN CALICIVIRUSES
sion to their sexual partners. Prevention of transmission through blood
or blood products and prevention of mother-to-child transmission are Etiologic Agent The Norwalk virus is the prototype strain of a
discussed in “Transmission,” above. group of small (27–40 nm), nonenveloped, round, icosahedral viruses
with relatively amorphous surface features on visualization by electron
■ FURTHER READING microscopy. Molecular cloning and characterization have demonstrated
Fauci AS, Marston HD: Ending AIDS—is an HIV vaccine necessary? that the viruses have a single, positive-strand RNA genome ~7.5 kb in
N Engl J Med 370:495, 2014. length and possess a single virion-associated protein—similar to that
Fauci AS, Marston HD: Ending the HIV-AIDS pandemic—follow the of typical caliciviruses—with a molecular mass of 60 kDa. On the basis
science. N Engl J Med 373:2197, 2015. of these molecular characteristics, these viruses are presently classified
Gray GE et al: Which new health technologies do we need to achieve into two genera belonging to the family Caliciviridae: the norovi-
an end to HIV/AIDS? PLoS Biol 14:e1002372, 2016. ruses and the sapoviruses (previously called Norwalk-like viruses and
CHAPTER 198 Viral Gastroenteritis
Haase AT: Perils at mucosal front lines for HIV and SIV and their hosts. Sapporo-like viruses, respectively). Human noroviruses can be classi-
Nat Rev Immunol 5:783, 2005. fied into three genogroups: GI, GII, and GIV, which include 9, 22, and
Haynes BF et al: HIV-Host interactions: Implications for vaccine 1 genotype, respectively.
design. Cell Host Microbe 19:292, 2016.
Kanters S et al: Comparative efficacy and safety of first-line antiretro- Epidemiology Infections with the Norwalk and related
viral therapy for the treatment of HIV infection: A systematic review human caliciviruses are common worldwide, and most adults
and network meta-analysis. Lancet HIV 3:e510, 2016. have antibodies to these viruses. Antibody is acquired at an
Kuhar DT et al: Updated US Public Health Service guidelines for the earlier age in developing countries—a pattern consistent with the pre-
management of occupational exposures to human immunodeficiency sumed fecal–oral mode of transmission. Infections occur year-round,
virus and recommendations for postexposure prophylaxis. Infect although, in temperate climates, a distinct increase has been noted in
Control Hosp Epidemiol 34:875, 2013. cold-weather months. Noroviruses may be the most common infec-
Marcus JL et al: Narrowing the gap in life expectancy between tious agents of mild gastroenteritis in the community and affect all age
HIV-infected and HIV-uninfected individuals with access to care. J groups, whereas sapoviruses primarily cause gastroenteritis in chil-
Acquir Immune Defic Syndr 73:39, 2016. dren. Noroviruses also cause traveler’s diarrhea, and outbreaks have
Moir S, Fauci AS: B-cell responses to HIV infection. Immunol Rev occurred among military personnel deployed to various parts of the
275:33, 2017. world. The limited data available indicate that norovirus may be the
Rerks-Ngarm S et al: Vaccination with ALVAC and AIDSVAX to pre- second most common viral agent (after rotavirus) among young chil-
vent HIV-1 infection in Thailand. N Engl J Med 361:2209, 2009. dren and the most common agent among older children and adults. In
UN Joint Programme On HIV/AIDS (UNAIDS): Prevention Gap the United States, with the decline in severe rotavirus disease following
Report, 2016. Available at www.unaids.org/en/resources/documents/2016/ implementation of a rotavirus vaccination program, norovirus has
prevention-gap. become the leading cause of medically attended gastroenteritis in
World Health Organization: Blood safety and availability Fact young children. Noroviruses are also recognized as the major cause of
Sheet. Available at www.who.int/mediacentre/factsheets/fs279/en/. epidemics of gastroenteritis worldwide. In the United States, ~50% of
all reported outbreaks of gastroenteritis are caused by noroviruses.
Virus is transmitted predominantly by the fecal–oral route but is also
present in vomitus. Because an inoculum with very few viruses can be
Section 15 Infections Due to RNA Viruses infectious, transmission can occur by aerosolization, by contact with
contaminated fomites, and by person-to-person contact. Viral shedding
and infectivity are greatest during the acute illness, but challenge stud-
198 Viral Gastroenteritis ies with Norwalk virus in volunteers indicate that viral antigen may be
shed by asymptomatically infected persons and also by symptomatic
Umesh D. Parashar, Roger I. Glass persons before the onset of symptoms and for several weeks after the
resolution of illness. Viral shedding can be prolonged in immunocom-
promised individuals.
Acute infectious gastroenteritis is a common illness that affects persons Pathogenesis The exact sites and cellular receptors for attachment
of all ages worldwide. It is a leading cause of death among children in of viral particles have not been determined. Data suggest that carbo-
developing countries, accounting for an estimated 0.6 million deaths hydrates that are similar to human histo-blood group antigens and
each year, and is responsible for up to 10–12% of all hospitalizations are present on the gastroduodenal epithelium of individuals with the
among children in industrialized countries, including the United secretor phenotype may serve as ligands for the attachment of Norwalk
States. Elderly persons, especially those with debilitating health con- virus. Additional studies must more fully elucidate norovirus–carbohy-
ditions, also are at risk of severe complications and death from acute drate interactions, including potential strain-specific variations. After
Harrisons_20e_Part5_p0859-p1648.indd 1463 6/1/18 12:09 PM
Pneumocystis early in life. It was historically thought that Pneumocystis 1547
215 Pneumocystis Infections
Alison Morris, Henry Masur
developed from reactivation of latent infection, but de novo infections
from environmental sources and person-to-person transmission occur
as well. Outbreaks of PCP suggest that nosocomial transmission can
take place, and studies with rodents show that immunocompetent
animals can serve as reservoirs for transmission of P. carinii (the infect-
ing species in rodents) to immunocompetent and immunosuppressed
■ DEFINITION AND DESCRIPTION animals. However, Pneumocystis organisms are species-specific. Thus,
Pneumocystis is an opportunistic pathogen that is an important cause
humans are infected only by other humans who transmit P. jirovecii;
of pneumonia in immunocompromised hosts, particularly those with
humans cannot be infected with species of Pneumocystis that infect
HIV infection (Chap. 197), organ transplants, or hematologic malignan-
other animals, such as P. carinii (rats), P. murina (mice), or P. oryctolagi
cies and those receiving high-dose glucocorticoids or certain immuno-
(rabbits). The utility of respiratory isolation in preventing transmission
suppressive monoclonal antibodies. Pneumocystis was discovered in
from patients with PCP to other immunosuppressed individuals has
rodents in 1906 and was initially believed to be a protozoan. Because
been debated; no clear evidence exists, although it seems prudent
Pneumocystis cannot be cultured, our understanding of its biology has
to isolate patients with active PCP from other immunosuppressed
been limited, but molecular techniques have demonstrated that the
patients.
organism is actually a fungus. Formerly known as Pneumocystis carinii,
the species infecting humans has been renamed Pneumocystis jirovecii. Role of Immunity Defects in cellular and/or humoral immunity
predispose to development of PCP. Such defects may be congenital,
■ EPIDEMIOLOGY or they may be acquired as a result of HIV infection or of treatment
P. jirovecii pneumonia (PCP) came to medical attention when cases were with immunosuppressive drugs such as glucocorticoids, fludarabine,
reported in malnourished orphans in Europe during World War II. The temozolomide, temsirolimus, cyclophosphamide, rituximab, or alemtu-
disease was later recognized in other immunosuppressed populations zumab. CD4+ T cells are critical in host defense against Pneumocystis.
but was rare in the era before HIV/AIDS and before intensive immu- Among HIV-infected patients, the incidence is inversely related to the
nosuppressive therapy for organ transplantation and autoimmune CD4+ T cell count: at least 80% of cases occur at counts of <200/μL, and
disorders. In 1981, PCP was first reported in men who had sex with most of these cases develop at counts of <100/μL. HIV load is another
men and in IV drug users who had no obvious cause of immunosup- factor that predisposes patients to PCP. CD4+ T cell counts are less spe-
pression. These cases were subsequently recognized as the first cases of cific and thus less useful in predicting the risk of PCP in patients who
what came to be known as the acquired immunodeficiency syndrome are immunosuppressed for reasons other than HIV infection.
CHAPTER 215 Pneumocystis Infections
(AIDS) (Chap. 197).
The incidence of PCP increased dramatically as the AIDS epidemic Lung Pathology Pneumocystis has a unique tropism for the lung.
grew: without chemoprophylaxis or antiretroviral therapy (ART), It is presumably inhaled into the alveolar space. Clinically apparent
80–90% of patients with HIV/AIDS in North America and Western pneumonia occurs only if an individual is immunocompromised.
Europe ultimately develop one or more episodes of PCP. While its Pneumocystis proliferates in the lung, provoking a mononuclear cell
incidence declined with the introduction of anti-Pneumocystis prophy- response. The alveoli become filled with proteinaceous material, and
laxis and combination ART, PCP has continued to be a leading cause of alveolar damage results in increased alveolar-capillary injury and
AIDS-associated morbidity in the United States and Western Europe, surfactant abnormalities. Stained lung sections typically show foamy,
particularly in individuals who do not know they are infected with vacuolated alveolar exudates composed largely of viable and nonviable
HIV until they are profoundly immunosuppressed and in HIV-infected organisms (Fig. 215-1A). Interstitial edema and fibrosis may develop,
patients with CD4+ T lymphocyte counts of <200/μL who are not and organisms can be seen in the alveolar space with silver or other
receiving ART or PCP prophylaxis. stains. Moreover, the organisms can be seen when tissue is subjected to
PCP also develops in HIV-uninfected patients who are immunocom- colorimetric or immunofluorescent staining (Fig. 215-1B–1D).
promised secondary to hematologic or malignant neoplasms, stem cell
or solid organ transplantation, and treatment with immunosuppressive ■ CLINICAL FEATURES
medications. The incidence of PCP depends on the degree and duration
of immunosuppression. PCP is increasingly reported among individ-
Clinical Presentation PCP presents as acute or subacute pneu-
monia that may initially be characterized by a vague sense of dyspnea
uals receiving tumor necrosis factor α inhibitors and antilymphocyte
alone but that subsequently manifests as fever and nonproductive
monoclonal antibodies for rheumatologic or other diseases. While clin-
cough with progressive shortness of breath, ultimately resulting in
ical PCP in immunocompetent hosts has not been clearly documented,
respiratory failure and death. Extrapulmonary manifestations of PCP
studies have shown that Pneumocystis organisms can colonize the air-
are rare but can include involvement of almost any organ, most notably
ways of children and adults who are not overtly immunocompromised.
lymph nodes, spleen, and liver.
The relevance of these organisms to acute or chronic syndromes, such
as chronic obstructive pulmonary disease (COPD), in immunocompe- Physical Examination The physical examination findings in
tent patients is being investigated. PCP are nonspecific. Patients have decreased oxygen saturation—at
In some developing countries, the incidence of PCP among rest or with exertion—that, without treatment, progresses to severe
HIV-infected individuals has been found to be lower than that hypoxemia. Patients may initially have a normal chest examination
in industrialized countries. This lower incidence may be due and no adventitious sounds, but later develop diffuse rales and signs
to competing mortality from infectious diseases such as tuberculosis of consolidation.
and bacterial pneumonia, which typically occur before patients become
immunosuppressed enough to develop PCP. Geographic variations in Laboratory Findings The results of routine laboratory tests are
Pneumocystis exposure and underdiagnosis attributable to lack of diag- nonspecific in PCP. Serum levels of lactate dehydrogenase (LDH) are
nostic resources also may explain the apparent lower frequency of PCP often elevated as a result of pulmonary damage; however, a normal
in some countries. LDH level does not rule out PCP, nor is an elevated LDH value specific
for PCP. The peripheral white blood cell count may be elevated in rela-
■ PATHOGENESIS AND PATHOLOGY tion to the patient’s baseline values, but the increase is usually modest.
Hepatic and renal function are typically normal.
Life Cycle and Transmission The life cycle of Pneumocystis
involves both sexual and asexual reproduction, and the organism exists Radiographic Findings Although the initial chest radiograph
as a trophic form, a cyst, and a precyst at various points. Serologic and may be normal when patients have mild symptoms, the classic radio-
molecular studies have demonstrated that most humans are exposed to graphic appearance of symptomatic PCP consists of diffuse bilateral
Harrisons_20e_Part5_p0859-p1648.indd 1547 6/1/18 12:11 PM
1548
A B
PART 5
Infectious Diseases
C D
FIGURE 215-1 Direct microscopy of Pneumocystis pneumonia. A. Transbronchial lung biopsy stained with hematoxylin and eosin shows eosinophilic alveolar filling. B.
Methenamine silver–stained bronchoalveolar lavage (BAL) fluid. C. Giemsa-stained BAL fluid. D. Immunofluorescent stain of BAL fluid.
interstitial infiltrates that are perihilar and symmetric (Fig. 215-2A)— specific stains indicated above for lung biopsy. While expectorated
yet another finding that is not specific for PCP. The interstitial infiltrates sputum or throat swabs have very low sensitivity, an induced sputum
can progress to alveolar filling (Fig. 215-2B). High-resolution chest CT sample obtained and interpreted by an experienced provider can be
shows diffuse ground-glass opacities in virtually all patients with PCP highly sensitive and specific. The reported sensitivity of induced spu-
(Fig. 215-2C). A normal chest CT essentially rules out the diagnosis tum for PCP is widely variable (55–90%), however, and is dependent on
of PCP. Cysts and pneumothoraces are common chest radiographic both the characteristics of the patient and the experience of the center
findings, especially in patients with HIV infection (Fig. 215-2D). A conducting the test.
wide variety of atypical radiographic findings have been described, Many laboratories now offer polymerase chain reaction (PCR) test-
including asymmetric patterns, upper-lobe infiltrates, mediastinal ade- ing of respiratory specimens for Pneumocystis in preference to direct
nopathy, nodules, cavities, and effusions. microscopy of appropriately stained respiratory secretions. However,
these PCR tests are so sensitive that it is difficult to distinguish patients
■ DIAGNOSIS with colonization (i.e., those whose acute lung disease is due to some
The optimal sample for diagnostic examination depends on how other process but who have low levels of Pneumocystis DNA in the
ill the patient is and what resources are available. Before the 1990s, lungs) from those with acute pneumonia due to Pneumocystis. Such
diagnoses of PCP were usually established by open lung biopsy; later, PCR tests on appropriate samples may be more useful for ruling out a
transbronchial lung biopsy was employed. Hematoxylin and eosin diagnosis of PCP if they are negative than for definitively attributing
staining of pulmonary tissue demonstrates a foamy alveolar infiltrate the disease to Pneumocystis.
and a mononuclear interstitial infiltrate (Fig. 215-1A). This appearance There has been considerable interest in serologic tests such as
is pathognomonic for PCP even though the organisms cannot be spe- assays for (1→3)-β-d-glucan, levels of which are frequently elevated
cifically identified with this stain. The diagnosis is typically established in patients with PCP. However, no serologic assays developed to date
in lung tissue or pulmonary secretions by highly specific staining of the offer both substantial sensitivity and specificity.
cyst—e.g., with methenamine silver (Fig. 215-1B), toluidine blue O, or
Giemsa (Fig. 215-1C)—or by staining with a specific immunofluores- ■ COURSE AND PROGNOSIS
cent antibody (Fig. 215-1D). Untreated, PCP is invariably fatal. Patients with HIV infection often
The demonstration of organisms in bronchoalveolar lavage (BAL) have an indolent course that presents as mild exercise intolerance
fluid is almost 100% sensitive and specific for PCP in patients with or chest tightness without fever or cough and a normal or nearly
HIV infection and is almost as sensitive in patients with immunosup- normal posterior–anterior chest radiograph, with progression over
pression due to other processes. The organisms are identified with the days, weeks, or even a few months to fever, cough, diffuse alveolar
Harrisons_20e_Part5_p0859-p1648.indd 1548 6/1/18 12:11 PM
1549
A B
CHAPTER 215 Pneumocystis Infections
C D
FIGURE 215-2 Radiographs in Pneumocystis pneumonia. A. Posterior–anterior chest radiograph showing symmetric interstitial infiltrates. B. Posterior–anterior chest
radiograph showing symmetric alveolar infiltrates (courtesy of Alison Morris). C. CT image demonstrating symmetric interstitial infiltrates and ground-glass opacities.
D. CT image showing symmetric interstitial infiltrates, ground-glass opacities, and pneumatoceles.
infiltrates, and profound hypoxemia. Some patients with HIV infection TREATMENT
and most patients with other types of immunosuppression have more
acute disease that progresses over a few days to respiratory failure. P. jirovecii Pneumonia
Rare patients also develop distributive shock. A few unusual patients
The treatment of choice for PCP is trimethoprim-sulfamethoxazole
present with extrapulmonary manifestations in the skin or soft tissue,
(TMP-SMX), given either IV or PO for 14 days to non-HIV-infected
retina, brain, liver, kidney, or spleen. Extrapulmonary disease is non-
patients with mild disease and for 21 days to all other patients
specific in presentation and can be diagnosed only by histology.
(Table 215-1). TMP-SMX, which interferes with the organism’s
Factors that influence mortality risk include the patient’s age and
folate metabolism, is at least as effective as alternative agents and
degree of immunosuppression as well as comorbidities, the presence
is better tolerated. TMP-SMX can cause leukopenia, hepatitis, rash,
of preexisting lung disease, a low serum albumin level, the need for
and fever as well as anaphylactic and anaphylactoid reactions, and
mechanical ventilation, and the development of a pneumothorax. With
patients with HIV infection have an unusually high incidence of
advances in supportive critical care, the prognosis for patients with PCP
hypersensitivity to TMP-SMX. Monitoring of serum drug levels
who require intubation and respiratory support has improved and now
is useful if renal function or toxicities are issues. Maintenance of a
depends to a large extent on comorbidities and the prognosis of the
2-h post-dose serum sulfamethoxazole level of 100–150 μg/mL has
underlying disease. Since patients typically do not respond to therapy
been associated with a successful outcome. Resistance to TMP-SMX
for 4–8 days, supportive care for a minimum of 10 days is a reasonable
cannot be measured by organism growth inhibition in the labora-
consideration if such support is compatible with the patient’s wishes and
tory because Pneumocystis cannot be cultured. However, mutations
the prognosis of comorbidities. Patients whose condition continues
in the target gene for sulfamethoxazole that confer in vitro sulfa
to deteriorate after 3 or 4 days or has not improved after 7–10 days
resistance to other organisms have been found in Pneumocystis. The
should be reevaluated to determine whether other infectious processes
clinical relevance of these mutations for the response to therapy is
are present (either having been missed on initial evaluation or having
unknown. Sulfadiazine plus pyrimethamine, an oral regimen more
developed during treatment), whether initial anti-Pneumocystis treat-
often used for treatment of toxoplasmosis, also is highly effective.
ment has failed, or whether noninfectious processes (e.g., congestive
Dapsone plus pyrimethamine or dapsone plus trimethoprim also
heart failure, pulmonary emboli, pulmonary hypertension, drug toxic-
can be used.
ity, or a neoplastic process) are causing pulmonary dysfunction.
Harrisons_20e_Part5_p0859-p1648.indd 1549 6/1/18 12:11 PM
1550 TABLE 215-1 Treatment of Pneumocystosisa glucocorticoid regimen (if any) the patient was receiving when PCP
therapy was begun.
DRUG(S) DOSE, ROUTE ADVERSE EFFECTS
For patients with HIV infection who present with PCP before the
First-Choice Agent initiation of ART, ART should be started within the first 2 weeks of
TMP-SMX TMP (5 mg/kg) plus Fever, rash, cytopenias, therapy for PCP in most situations. Immune reconstitution inflam-
SMX (25 mg/kg) hepatitis, hyperkalemia matory syndrome (IRIS) can occur, however, and the decision to
q6–8h PO or IV (i.e.,
2 double-strength
initiate ART thus requires considerable expertise in optimal timing
tablets tid or qid) relative to PCP recovery as well as in the other factors that are rele-
vant when ART is initiated in any patient.
Alternative Agents
Atovaquone 750 mg bid PO Rash, fever, hepatitis
■ PREVENTION
Clindamycin 300–450 mg q6h PO Hemolysis (G6PD deficiency),
or 600 mg q6–8h IV methemoglobinemia, The most effective method for preventing PCP is to eliminate the cause
plus
15–30 mg qd PO neutropenia, rash of immunosuppression by withdrawing immunosuppressive therapy
Primaquine or treating the underlying cause (e.g., HIV infection). Patients who are
Pentamidine 3–4 mg/kg qd IV Hypotension, azotemia, susceptible to PCP benefit from chemoprophylaxis during the period
cardiac arrhythmias (torsades
of susceptibility. For patients with HIV infection, CD4+ T cell counts
des pointes), pancreatitis,
dysglycemias, hypocalcemia, are a reliable marker of susceptibility, and counts below 200/μL are an
neutropenia, hepatitis indication to start prophylaxis (Table 215-2).
Adjunctive Agent For patients who are immunosuppressed as a result of factors other
than HIV infection, there is no laboratory parameter, including the CD4+
Prednisone or 40 mg bid × 5 d, Peptic ulcer disease,
methylprednisolone 40 mg qd × 5 d, hyperglycemia, mood alteration,
T cell count, that predicts susceptibility to PCP with adequate positive
20 mg qd × 11 d; hypertension and negative accuracy. The period of susceptibility is usually estimated
PO or IV on the basis of experience with the underlying disease and immuno-
suppressive regimen. Premature cessation of prophylaxis has been
a
Treatment can be administered for 14 days to non-HIV-infected patients with mild
disease and for 21 days to all other patients. associated with clusters of cases in certain patient populations, such as
Abbreviations: G6PD, glucose-6-phosphate dehydrogenase; TMP-SMX, solid-organ transplant recipients. Patients receiving a prolonged course
trimethoprim-sulfamethoxazole. of high-dose glucocorticoids appear to be particularly susceptible to PCP.
The glucocorticoid exposure threshold that warrants chemoprophylaxis
is controversial, but such preventive therapy should be strongly consid-
PART 5
Intravenous pentamidine or the combination of clindamycin plus ered for any patient who is receiving more than the equivalent of 20 mg
primaquine is an option for patients who cannot tolerate TMP-SMX of prednisone daily for 30 days or who is receiving glucocorticoids in
and for patients in whose treatment TMP-SMX appears to be failing. conjunction with other immunosuppressive agents. Clinical experience
Pentamidine must be given IV over at least 60 min to avoid potentially also suggests that chemoprophylaxis is useful for patients receiving cer-
lethal hypotension. Adverse effects can be severe and irreversible and tain immunosuppressive agents (e.g., tumor necrosis factor inhibitors,
Infectious Diseases
include renal dysfunction, dysglycemia (life-threatening hypoglyce- antithymocyte globulin, rituximab, and alemtuzumab). The duration of
mia that can occur days or weeks after initial infusion and be followed such chemoprophylaxis is empirically determined by clinical and labo-
by hyperglycemia), neutropenia, and torsades des pointes. Clindamy- ratory indicators of immunologic vulnerability.
cin plus primaquine is effective, but primaquine can be given only
by the oral route—a disadvantage for patients who cannot ingest or
absorb oral drugs. Oral atovaquone is also a reasonable option for TABLE 215-2 Prophylaxis of Pneumocystosis
patients with mild disease who have no impediments to absorbing an DRUG(S) DOSE, ROUTE COMMENTS
oral drug that requires a high-fat meal for optimal absorption.
First-Choice Agent
A major advance in therapy for PCP was the recognition that
glucocorticoids could improve survival rates among HIV-infected TMP-SMX 1 tablet (double- or Incidence of hypersensitivity is
patients with moderate to severe disease (room air PO2, <70 mmHg; single-strength) qd PO high. Rechallenge for non-life-
threatening hypersensitivity;
or alveolar–arterial oxygen gradient, ≥35 mmHg). Glucocorticoids consider dose-escalation
appear to reduce the pulmonary inflammation that occurs after protocol.
specific therapy is started and organisms begin to die, eliciting Alternative Agents
inflammation. Therapy with glucocorticoids should be the standard
Dapsone 50 mg bid or 100 mg Hemolysis is associated with
of care for patients with HIV infection and probably is also effective
qd PO G6PD deficiency.
for patients with other immunodeficiencies. This treatment should
Dapsone 50 mg qd PO Leucovorin ameliorates
be started for moderate or severe disease when therapy for PCP is cytopenias due to
plus
initiated, even if the diagnosis has not yet been confirmed. If HIV- pyrimethamine.
infected or HIV-uninfected patients are receiving high-dose gluco- Pyrimethamine 50 mg weekly PO
corticoids when they develop PCP, there are theoretical advantages plus
to either increasing the steroid dose (to reduce the inflammatory Leucovorin 25 mg weekly PO
response to the dying organisms) or decreasing the steroid dose (to Dapsone 200 mg weekly PO Leucovorin ameliorates
improve immune function), but there is no convincing evidence on plus cytopenias due to
which to base any specific strategy. pyrimethamine.
Pyrimethamine 75 mg weekly PO
No definitive trials have defined the best therapeutic algorithm plus
for patients in whom TMP-SMX treatment for PCP is failing. If no Leucovorin 25 mg weekly PO
other treatable infectious or noninfectious processes are detected Pentamidine 300 mg monthly via Aerosol may cause
and pulmonary dysfunction appears to be due to PCP alone, many Respirgard II nebulizer bronchospasm. Pentamidine is
authorities would switch from TMP-SMX to either IV pentamidine probably less effective than TMP-
or IV clindamycin plus oral primaquine. Some authorities would SMX or dapsone regimens.
add the second drug or drug combination to TMP-SMX rather than Atovaquone 1500 mg qd PO Requires fatty meal for optimal
switching regimens. If patients are not already receiving them, absorption
glucocorticoids should be added to the regimen; the dosage and Abbreviations: G6PD, glucose-6-phosphate dehydrogenase; TMP-SMX,
regimen, which are usually chosen empirically, depend on what trimethoprim-sulfamethoxazole.
Harrisons_20e_Part5_p0859-p1648.indd 1550 6/1/18 12:11 PM
TMP-SMX is the most effective prophylactic drug; few patients experi- helminths and protozoa. These organisms are larger and more complex 1551
ence a PCP breakthrough when they are reliably taking a recommended than bacteria, with a eukaryotic cell structure similar to that of human
TMP-SMX chemoprophylactic regimen. Several TMP-SMX regimens host cells. Historically, this similarity has made it difficult to find
have been used successfully. One double-strength tablet daily is the effective antiparasitic agents that do not cause unacceptable toxicity
regimen with which there is the most experience, but either one single- to human cells. Fortunately, intensive research and modern techniques
strength tablet daily or one double-strength tablet two or three times have now provided suitable agents for safe and effective treatment of
weekly also has been recommended for various populations of patients. most parasitic infections. See Chap. S14 for details on diagnostic pro-
For patients who cannot tolerate TMP-SMX (usually because of cedures and Chap. 217 for details on treatment.
hypersensitivity or bone marrow suppression), alternative drugs Internal parasites of human beings are divided into two types: hel-
include daily dapsone, weekly dapsone-pyrimethamine, atovaquone, minths (worms) and protozoa. Helminths are multicellular organisms
and monthly aerosol pentamidine. Patients who develop hypersen- that can be seen with the naked eye (Chap. 225). There are two phyla:
sitivity to TMP-SMX can sometimes tolerate the drug if a gradual Platyhelminthes (flat worms) and Nemathelminthes (roundworms).
dose-escalation protocol is used. Dapsone cross-reacts with sulfon- Both phyla include some genera that mature in the gastrointestinal
amides in a substantial fraction of patients and therefore is rarely useful tract and others that migrate through the tissue after ingestion or skin
in patients with a history of life-threatening reactions to TMP-SMX. penetration. Tables S14-1 and S14-2 present the helminthic genera,
Aerosolized pentamidine is highly effective, but it is not as effective their definitive and intermediate hosts, geographic distributions, and
as TMP-SMX and may not provide protection in areas of the lung that the parasitic stages in the human body.
are not well ventilated. Atovaquone is also effective and well toler- The key to understanding which helminths use humans as defini-
ated; however, this drug is available only as an oral preparation, and tive hosts is to remember that helminth ova develop into larvae, and
gastrointestinal absorption is unpredictable in patients with abnormal larval stages develop into adults. Humans serve as the definitive host
gastrointestinal motility or function. when they ingest helminth larvae, which develop into adults in the
intestine and usually cause mild disease, often without any symptoms.
■ FURTHER READING (The exception is ingestion of the late-stage larvae of the somatic or
Akgun KM, Miller RF: Critical care in human immunodeficiency tissue flukes, as shown in Table S14-2.) In contrast, if humans ingest
virus–infected patients. Semin Respir Crit Care Med 37:303, 2016. helminth ova and serve as the intermediate host, the ova develop into
Bozzette SA et al: A controlled trial of early adjunctive treatment with larvae, which penetrate the intestine, migrate through the tissue, and
corticosteroids for Pneumocystis carinii pneumonia in the acquired invade organs where they mature into adults. Intermediate hosts with
immunodeficiency syndrome. California Collaborative Treatment parasitic invasion of organs may experience severe disease.
CHAPTER 216 Introduction to Parasitic Infections
Group. N Engl J Med 323:1451, 1990. Protozoa are microscopic single-celled organisms. Among the many
Buchacz K et al: Incidence of AIDS-defining opportunistic infections differences between helminths and protozoans, the most important
in a multicohort analysis of HIV-infected persons in the United States is the ability of protozoa (like bacteria) to multiply within the human
and Canada, 2000–2010. J Infect Dis 214:862, 2016. body and cause overwhelming infections. A major mechanism pro-
Drummond MB et al: Factors associated with abnormal spirometry moting unrestrained growth is evasion of the host immune response
among HIV-infected individuals. AIDS 29:1691, 2015. either by antigenic variation (Trypanosoma brucei) or by survival inside
Kaur N, Mahl TC: Pneumocystis jiroveci (carinii) pneumonia after host cells (e.g., Plasmodium, Babesia, Cryptosporidium, Leishmania, and
infliximab therapy: A review of 84 cases. Dig Dis Sci 52:1481, 2007. Toxoplasma). In contrast, almost all helminths require stages in other
Ma L et al: Genome analysis of three Pneumocystis species reveals hosts to complete their life cycles and multiply. As a result, except
adaptation mechanisms to life exclusively in mammalian hosts. Nat for Strongyloides and Capillaria, which can complete their life cycle in
Commun 7:10740, 2016. humans, increases in the burden of infection with helminths require
Panel on Opportunistic Infections in HIV-Infected Adults and repeated exogenous reinfections. Thus permanent residents of endemic
Adolescents: Guidelines for the prevention and treatment of oppor- countries, who are exposed repeatedly, may have heavy severe infec-
tunistic infections in HIV-infected adults and adolescents: Recom- tions, while most travelers with one or two exposures are unlikely to
mendations from the Centers for Disease Control and Prevention, the experience the full spectrum of chronic helminthic infections.
National Institutes of Health, and the HIV Medicine Association of In contrast to helminthic infections, naïve patients with their first
the Infectious Diseases Society of America. Available at http://aidsinfo protozoal infection usually are the most severely affected because
.nih.gov/contentfiles/lvguidelines/adult_oi.pdf. Accessed January 5, 2018. partial immunity often limits the number of parasites during recurrent
Zolopa A et al: Early antiretroviral therapy reduces AIDS progression/ infections. Protozoan replication to large numbers in the host also pro-
death in individuals with acute opportunistic infections: A multicen- motes the development of drug-resistant forms, especially in malaria
ter randomized strategy trial. PLoS One 4:e5575, 2009. (Chap. 217). Because protozoa belong to many different phyla, it is
easier to understand the pathogenesis and management of protozoal
infections when they are classified by the site of infection (intestinal
protozoans, free-living amebae, and blood and tissue protozoans)
(Table S14-3). Immunocompromised hosts are at risk of disseminated
infection with a number of protozoa, including Leishmania, Toxoplasma,
Section 17 Protozoal and Helminthic Infections: Cryptosporidium, and Trypanosoma cruzi, which are AIDS-defining ill-
General Considerations nesses. In contrast, Strongyloides is the only helminth to disseminate.
HELMINTHIC INFECTIONS
216 Introduction
Infections
to Parasitic The Platyhelminthes (flatworms) are categorized as tapeworms (ces-
todes) and flukes (trematodes). Tapeworms are composed of a head or
scolex bearing the holdfast organs and segments, which become gravid
as they mature. Some tapeworms can reach lengths of many yards; the
Sharon L. Reed, Charles E. Davis longest tapeworms develop in the intestine, where they rarely cause
serious disease. In contrast, flukes are small leaf-shaped organisms
whose size is not a measure of disease severity.
The word parasite comes originally from the Greek parasitos (para, along-
■ FLATWORMS
side of; and sitos, food), meaning someone who eats at another’s table
or lives at another’s expense. Although the same is true of many bacte- Cestodes Tapeworms cause either intestinal or somatic infection,
ria and viruses, the designation parasite is reserved, by convention, for depending on the species. Intestinal infections occur when the human
Harrisons_20e_Part5_p0859-p1648.indd 1551 6/1/18 12:11 PM
cases. Inguinal hernias and chorioretinitis are less common. Laboratory esophagitis, gastritis, and retinitis. CMV disease is an independent risk 1363
abnormalities include elevated alanine aminotransferase levels in factor for both graft loss and death. Without prophylaxis, the period
serum, thrombocytopenia, conjugated hyperbilirubinemia, hemolysis, of maximal risk is between 1 and 4 months after transplantation. Dis-
and elevated protein levels in cerebrospinal fluid. The prognosis for ease likelihood and viral replication levels generally are greater after
severely infected infants is poor, and few survivors escape intellectual primary infection than after reactivation. Molecular studies indicate
or hearing difficulties later in childhood. The differential diagnosis of that seropositive organ transplant recipients are susceptible to infec-
cytomegalic inclusion disease in infants includes syphilis, toxoplasmo- tion with donor-derived, genotypically variant CMV. Reactivation
sis, bacterial sepsis, and infection with a variety of viruses, including infection, although common, is less likely than primary infection to be
rubella, Zika, or herpes simplex virus. clinically significant. The overall risk of clinical disease is related to var-
Most congenital CMV infections are clinically inapparent at birth. ious factors, such as serologic mismatch (donor seropositive, recipient
Of asymptomatically infected infants, 5–25% develop significant psy- seronegative), degree of immunosuppression, use of antilymphocyte
chomotor, hearing, ocular, or dental abnormalities over the next several antibodies, lack of anti-CMV prophylaxis, and co-infection with other
years. pathogens. The transplanted organ is particularly vulnerable as a tar-
get for CMV infection; thus there is a tendency for CMV hepatitis to
Perinatal CMV Infection The newborn may acquire CMV at
follow liver transplantation and for CMV pneumonitis to follow lung
delivery by passage through an infected birth canal or by postnatal
transplantation.
contact with infected breast milk or other maternal secretions. Of
CMV viremia occurs in roughly one-third of hematopoietic stem
infants who are breast-fed for >1 month by seropositive mothers,
cell transplant recipients; the risk of severe disease may be reduced
40–60% become infected. Iatrogenic transmission can result from blood
by prophylaxis or preemptive therapy with antiviral drugs. The risk is
transfusion; use of leukocyte-reduced or CMV-seronegative blood
greatest in the first 100 days after transplantation, and identified risk
products for transfusion into low-birth-weight seronegative infants or
factors include certain types of immunosuppressive therapy, an alloge-
seronegative pregnant women decreases risk.
neic (rather than an autologous) graft, acute graft-versus-host disease,
The great majority of infants infected at or after delivery remain
older age, and pretransplantation recipient seropositivity.
asymptomatic. However, protracted interstitial pneumonitis has been
CMV is an important pathogen in patients with advanced HIV
associated with perinatally acquired CMV infection, particularly in
infection (Chap. 197), in whom it may cause retinitis or disseminated
premature infants, and occasionally has been accompanied by infection
disease, particularly when peripheral-blood CD4+ T cell counts fall
with Chlamydia trachomatis, Pneumocystis, or Ureaplasma urealyticum.
below 50/μL. As treatment for underlying HIV infection has improved,
Poor weight gain, adenopathy, rash, hepatitis, anemia, and atypical
the incidence of serious CMV infections (e.g., retinitis) has decreased.
lymphocytosis may also be found, and CMV excretion often persists
CHAPTER 190 Cytomegalovirus and Human Herpesvirus Types 6, 7, and 8
During the first few weeks after institution of highly active antiret-
for months or years.
roviral therapy, however, acute flare-ups of CMV retinitis may occur
CMV Mononucleosis The most common clinical manifestation secondary to an immune reconstitution inflammatory syndrome.
of CMV infection in immunocompetent hosts beyond the neonatal Syndromes produced by CMV in immunocompromised hosts
period is a heterophile antibody–negative mononucleosis syndrome, (“CMV syndrome”) often begin with fatigue, fever, malaise, anorexia,
which may develop spontaneously or follow transfusion of leukocyte- night sweats, and arthralgias or myalgias. Liver function abnormali-
containing blood products. Although the syndrome occurs at all ages, it ties, leukopenia, thrombocytopenia, and atypical lymphocytosis may
most often involves sexually active young adults. With incubation peri- be observed during these episodes. Without treatment, CMV infection
ods of 20–60 days, the illness generally lasts for 2–6 weeks. Prolonged may progress to more severe end-organ disease. The development of
high fevers, sometimes with chills, profound fatigue, and malaise, tachypnea, hypoxemia, and nonproductive cough signals respiratory
characterize this disorder. Myalgias, headache, and splenomegaly are involvement. Radiologic examination of the lung often shows bilateral
common, but in CMV mononucleosis (as opposed to Epstein-Barr virus interstitial or reticulonodular infiltrates that begin in the periphery of
mononucleosis), exudative pharyngitis and cervical lymphadenopathy the lower lobes and spread centrally and superiorly; localized segmen-
are rare. Occasional patients develop rubelliform rashes, often after tal, nodular, or alveolar patterns are less common. The differential diag-
exposure to ampicillin or certain other antibiotics. Less common are nosis includes Pneumocystis infection; other viral, bacterial, or fungal
interstitial or segmental pneumonia, myocarditis, pleuritis, arthritis, infections; pulmonary hemorrhage; and injury secondary to irradiation
and encephalitis. In rare cases, Guillain-Barré syndrome complicates or to treatment with cytotoxic drugs.
CMV mononucleosis. The characteristic laboratory abnormality of Gastrointestinal CMV involvement may be localized or extensive
CMV mononucleosis is relative lymphocytosis in peripheral blood, and almost exclusively affects immunocompromised hosts. Colitis is
with >10% atypical lymphocytes. Total leukocyte counts may be low, the most common clinical manifestation in organ transplant recipients.
normal, or markedly elevated. Although significant jaundice is uncom- Ulcers of the esophagus, stomach, small intestine, or colon may result
mon, serum aminotransferase and alkaline phosphatase levels are in bleeding or perforation. Clinicians should be aware that blood tests
often moderately elevated. Heterophile antibodies are absent; however, such as CMV antigenemia and viral load testing may yield negative
transient immunologic abnormalities are common and may include results in the setting of intestinal disease. CMV infection may lead
the presence of cryoglobulins, rheumatoid factors, cold agglutinins, to exacerbations of underlying ulcerative colitis. Hepatitis occurs fre-
and antinuclear antibodies. Hemolytic anemia, thrombocytopenia, and quently, particularly after liver transplantation. Acalculous cholecysti-
granulocytopenia complicate recovery in rare instances. tis and adrenalitis also have been described.
Most patients recover without sequelae, although postviral asthe- CMV rarely causes meningoencephalitis in otherwise healthy indi-
nia may persist for months. The excretion of CMV in urine, genital viduals. Two forms of CMV encephalitis are seen in people with HIV.
secretions, and/or saliva often continues for months or years. Rarely, One resembles HIV encephalitis and presents as progressive dementia;
CMV infection is fatal in immunocompetent hosts; survivors can have the other is a ventriculoencephalitis characterized by cranial-nerve
recurrent episodes of fever and malaise, sometimes associated with deficits, nystagmus, disorientation, lethargy, and ventriculomegaly.
autonomic nervous system dysfunction (e.g., attacks of sweating or In immunocompromised patients, CMV can also cause subacute pro-
flushing). gressive polyradiculopathy, which is often reversible if recognized and
treated promptly.
CMV Infection in the Immunocompromised Host CMV retinitis is an important cause of blindness in immunocompro-
(Table 190-1) CMV is the most common viral pathogen complicating mised patients, particularly patients with advanced AIDS (Chap. 197).
organ transplantation (Chap. 138). In recipients of kidney, heart, Early lesions consist of small, opaque, white areas of granular retinal
lung, liver, pancreas, and vascularized composite (hand, face, other) necrosis that spread in a centrifugal manner and are later accompa-
transplants, CMV infection may result in a variety of clinical manifes- nied by hemorrhages, vessel sheathing, and retinal edema (Fig. 190-1).
tations, including fever and leukopenia, hepatitis, colitis, pneumonitis, CMV retinopathy must be distinguished from that due to other
Harrisons_20e_Part5_p0859-p1648.indd 1363 6/1/18 12:07 PM
1364 ■ PREVENTION
Prevention of CMV infection and disease in organ and hematopoietic
stem cell transplant recipients is usually based on one of two meth-
ods: universal prophylaxis or preemptive therapy. With universal
prophylaxis, antiviral drugs are used for a defined period, often 3 or
6 months. One clinical trial demonstrated that, in CMV-seronegative
kidney transplant recipients with seropositive donors, prophylaxis
with (val)ganciclovir was more effective at prevention when given for
200 days rather than 100 days. With preemptive therapy, patients are
monitored weekly for CMV viremia, and antiviral treatment is initiated
once viremia is detected. Because of the bone marrow–suppressive
effects of universal prophylaxis, preemptive therapy has been more
commonly employed in hematopoietic stem cell transplant recipients;
letermovir, which has recently been approved, allows prophylaxis in
higher-risk patients. For patients with HIV infection, CMV end-organ
disease is best prevented by using antiretroviral therapy sufficient to
maintain CD4+ T cell counts above 100/μL. Primary prophylaxis with
FIGURE 190-1 Cytomegalovirus infection in a patient with AIDS may appear as ganciclovir or valganciclovir is not recommended.
an arcuate zone of retinitis with hemorrhages and optic disk swelling. Often CMV Several additional measures are useful for the prevention of
is confined to the retinal periphery, beyond view of the direct ophthalmoscope. CMV transmission to CMV-naïve, high-risk patients. The use of
CMV-seronegative or leukocyte-depleted blood significantly decreases
the rate of transfusion-associated transmission. In a placebo-controlled
conditions, including toxoplasmosis, candidiasis, and herpes simplex
trial, a CMV glycoprotein B vaccine reduced infection rates among
virus infection.
464 CMV-seronegative women; this outcome raises the possibility that
Fatal CMV infections are often associated with persistent viremia
this experimental vaccine will reduce rates of congenital infection, but
and the involvement of multiple organ systems. Progressive pulmo-
further studies must validate this approach. A CMV glycoprotein B
nary infiltrates, pancytopenia, hyperamylasemia, and hypotension are
vaccine with MF59 adjuvant appeared effective in reducing the risk
characteristic features that are frequently found in conjunction with a
and duration of viremia in both seropositive and seronegative renal
terminal bacterial, fungal, or protozoan superinfection. Extensive adre-
transplant recipients at risk for CMV infection. CMV immune globulin
nal necrosis with CMV inclusions is often documented at autopsy, as is
PART 5
has been studied in a variety of clinical situations (primary CMV infec-
CMV involvement of many other organs.
tion in pregnancy, hematopoietic stem cell transplantation, solid organ
transplantation), with conflicting results.
■ DIAGNOSIS Prophylactic acyclovir or valacyclovir at high doses may reduce
CMV infection usually cannot be diagnosed reliably on clinical grounds rates of CMV infection and disease in renal transplant recipients; nei-
Infectious Diseases
alone. Isolation of CMV or detection of its antigens or DNA in appro- ther drug is effective in the treatment of active CMV disease.
priate clinical specimens is the preferred approach. The most common
method of detection is quantitative nucleic acid testing (QNAT) for
CMV by polymerase chain reaction (PCR) technology, for which blood TREATMENT
or other specimens can be used; some centers use a CMV antigenemia Cytomegalovirus Infection
test, an immunofluorescence assay that detects CMV antigens (pp65)
in peripheral-blood leukocytes. Such assays may yield a positive result Ganciclovir is a guanosine derivative that has considerably more
several days earlier than culture methods. QNAT may predict the risk activity against CMV than its congener acyclovir. After intracel-
for disease progression, particularly in immunocompromised hosts. lular conversion by a viral phosphotransferase encoded by CMV
CMV DNA in cerebrospinal fluid is useful in the diagnosis of CMV gene region UL97, ganciclovir triphosphate is a selective inhibitor
encephalitis or polyradiculopathy. Recent introduction of an interna- of CMV DNA polymerase. Several clinical studies have indicated
tional testing standard has helped reduce variation in viral load test response rates of 70–90% among people with HIV who are given
results. ganciclovir for the treatment of CMV retinitis or colitis. In severe
Virus excretion and/or viremia is readily detected by culture of infections (e.g., CMV pneumonia in hematopoietic stem cell trans-
appropriate specimens on human fibroblast monolayers. If CMV titers plant recipients), ganciclovir is sometimes combined with CMV
are high, as is common in congenital disseminated infection and in immune globulin. Prophylactic or suppressive ganciclovir may
AIDS, characteristic cytopathic effects may be detected within a few be useful in high-risk hematopoietic stem cell or organ transplant
days. However, in some situations (e.g., CMV mononucleosis), viral recipients (e.g., those who are CMV-seropositive before transplan-
titers are low, and cytopathic effects may take several weeks to appear. tation). In many people with HIV, persistently low CD4+ T cell
Many laboratories expedite diagnosis with an overnight tissue-culture counts, and CMV disease, clinical and virologic relapses occur
method (shell vial assay) involving centrifugation and an immunocy- promptly if treatment with ganciclovir is discontinued. There-
tochemical detection technique employing monoclonal antibodies to fore, prolonged maintenance regimens are recommended for such
an immediate-early CMV antigen. Isolation of virus from urine, stool, patients. Resistance to ganciclovir is more common among patients
or saliva does not, by itself, constitute proof of acute infection, since treated for >3 months and is usually related to mutations in the
excretion from these sites may continue for months or years after ill- CMV UL97 gene (or, less commonly, the UL54 gene). The advent of
ness. Detection of viremia by QNAT or antigenemia testing is a better CMV genotyping for resistance mutations has made it possible to
predictor of acute infection. rapidly obtain information regarding optimal treatment approaches
A variety of serologic assays detect antibody to CMV. An increased against clinically resistant virus.
level of IgG antibody to CMV may not be detectable for up to 4 weeks Valganciclovir is an orally bioavailable prodrug that is rapidly
after primary infection. Detection of CMV-specific IgM is sometimes metabolized to ganciclovir in intestinal tissues and the liver. Approx-
useful in the diagnosis of recent or active infection; however, circu- imately 60–70% of an oral dose of valganciclovir is absorbed. An
lating rheumatoid factors may result in occasional false-positive IgM oral valganciclovir dose of 900 mg results in ganciclovir blood levels
tests. Serology is more helpful when used to predict risk of CMV similar to those obtained with an IV ganciclovir dose of 5 mg/kg.
infection and disease in transplant recipients rather than to diagnose Valganciclovir appears to be as effective as IV ganciclovir for both
acute disease. CMV induction (treatment) and maintenance regimens, also offering
Harrisons_20e_Part5_p0859-p1648.indd 1364 6/1/18 12:07 PM
the advantage of oral dosing. Furthermore, the adverse-event pro- subsequent rash. In addition, ~10–20% of febrile seizures without rash 1365
files and rates of resistance for the two drugs are similar. during infancy are caused by HHV-6. After initial infection, HHV-6
Ganciclovir or valganciclovir therapy for CMV disease consists of a persists in peripheral-blood mononuclear cells as well as in the central
14- to 21-day induction course (5 mg/kg IV twice daily for ganciclovir nervous system, salivary glands, and female genital tract.
or 900 mg PO twice daily for valganciclovir), sometimes followed In older age groups, HHV-6 has been associated with mononucleosis
by maintenance therapy (e.g., valganciclovir, 900 mg/d). Periph- syndromes; in immunocompromised hosts, encephalitis, pneumonitis,
eral-blood neutropenia develops in roughly one-quarter of treated syncytial giant-cell hepatitis, and disseminated disease are seen. In
patients but may be ameliorated by granulocyte colony-stimulating transplant recipients, HHV-6 infection may also be associated with
factor or granulocyte-macrophage colony-stimulating factor. Whether graft dysfunction. Acute HHV-6-associated limbic encephalitis has
to use maintenance therapy should depend on the overall level of been reported in hematopoietic stem cell transplant recipients and
immunocompromise and the risk of recurrent disease. Discontinua- is characterized by memory loss, confusion, seizures, hyponatremia,
tion of maintenance therapy should be considered in people with HIV and abnormal electroencephalographic and MRI results. High plasma
who, while receiving antiretroviral therapy, have a sustained (3- to loads of HHV-6 DNA in hematopoietic stem cell transplant recipients
6-month) increase in CD4+ T cell counts to >100/μL. Compared with are associated with allelic-mismatched donors, use of glucocorticoids,
shorter (6-week) courses, prolonged (6-month) courses of valganci- delayed monocyte and platelet engraftment, development of limbic
clovir had beneficial effects on hearing and developmental outcomes encephalitis, and increased all-cause mortality rates. Mesial temporal
in infants with congenital CMV infection. lobe epilepsy has been associated with HHV-6 infections, and, like
For treatment of CMV retinitis, some clinicians prefer intravitreal many other viruses, HHV-6 has been implicated in the pathogenesis
injections of ganciclovir or foscarnet (see below) plus oral valgan- of multiple sclerosis, although further study is needed to distinguish
ciclovir to intravenous ganciclovir, although no clinical trials have between association and etiology.
compared these approaches. Foscarnet (sodium phosphonoformate) HHV-7 was isolated in 1990 from T lymphocytes from the peripheral
inhibits CMV DNA polymerase. Because this agent does not require blood of a healthy 26-year-old man. The virus is frequently acquired
phosphorylation to be active, it is also effective against most ganci- during childhood, albeit at a later age than HHV-6. HHV-7 is com-
clovir-resistant isolates. Foscarnet is less well tolerated than ganci- monly present in saliva, which is presumed to be the principal source
clovir and causes considerable toxicity, including renal dysfunction, of infection; breast milk and cervical secretions may also carry the
hypomagnesemia, hypokalemia, hypocalcemia, genital ulcers, dys- virus. Viremia can be associated with either primary or reactivation
uria, nausea, and paresthesia. Moreover, foscarnet administration infection. The most common clinical manifestations of childhood
requires the use of an infusion pump and close clinical monitoring. HHV-7 infections are fever and seizures. Some children present with
CHAPTER 190 Cytomegalovirus and Human Herpesvirus Types 6, 7, and 8
With aggressive hydration and dose adjustments for renal dysfunc- respiratory or gastrointestinal signs and symptoms. An association has
tion, the toxicity of foscarnet can be reduced. The use of foscarnet been made between HHV-7 and pityriasis rosea, but evidence is insuf-
should be avoided when a saline load cannot be tolerated (e.g., in ficient to indicate a causal relationship.
cardiomyopathy). The approved induction regimen is 60 mg/kg Clustering of HHV-6, HHV-7, and CMV infections in transplant
every 8 h for 2 weeks, although 90 mg/kg every 12 h is equally effec- recipients can make it difficult to sort out the roles of the various agents
tive and no more toxic. Maintenance infusions should deliver 90–120 in individual clinical syndromes. HHV-6 and HHV-7 appear to be sus-
mg/kg once daily. No oral preparation is available. Foscarnet- ceptible to ganciclovir and foscarnet, although definitive evidence of
resistant virus may emerge during extended therapy. This drug is clinical response is lacking.
used more frequently after hematopoietic stem cell transplantation
than in other situations to avoid the myelosuppressive effects of ■ HHV-8
ganciclovir; in general, foscarnet is also the first choice for infections Unique herpesvirus-like DNA sequences were reported during 1994
with ganciclovir-resistant CMV. and 1995 in tissues derived from Kaposi’s sarcoma (KS) and body
Cidofovir is a nucleotide analogue with a long intracellular half- cavity–based lymphoma occurring in people with HIV. The virus from
life that allows intermittent IV administration. Induction regimens which these sequences were derived is designated HHV-8 or Kaposi’s
of 5 mg/kg weekly for 2 weeks are followed by maintenance regi- sarcoma–associated herpesvirus (KSHV). HHV-8, which infects B
mens of 3–5 mg/kg every 2 weeks. Cidofovir can cause severe neph- lymphocytes, macrophages, and both endothelial and epithelial cells,
rotoxicity through dose-dependent proximal tubular cell injury; appears to be causally related not only to KS and a subgroup of AIDS-
however, this adverse effect can be tempered somewhat by saline related B cell body cavity–based lymphomas (primary effusion lympho-
hydration and probenecid. Cidofovir is used primarily for ganciclo- mas) but also to multicentric Castleman disease, a lymphoproliferative
vir-resistant virus. disorder of B cells. The association of HHV-8 with several other dis-
eases has been reported but not confirmed.
HHV-8 seropositivity occurs worldwide, with areas of high
HUMAN HERPESVIRUS (HHV) TYPES 6, 7, AND 8 endemicity influencing rates of disease. Unlike other herpes-
virus infections, HHV-8 infection is much more common in
■ HHV-6 AND HHV-7 some geographic areas (e.g., central and southern Africa) than in others
HHV-6 and -7 seropositivity rates are generally high through- (North America, Asia, northern Europe). In high-prevalence areas,
out the world. HHV-6 was first isolated in 1986 from periph- infection occurs in childhood, seropositivity is associated with having
eral-blood leukocytes of six persons with various a seropositive mother or (to a lesser extent) older sibling, and HHV-8
lymphoproliferative disorders. Two genetically distinct variants may be transmitted in saliva. In low-prevalence areas, infections typi-
(HHV-6A and HHV-6B) are now recognized. HHV-6 appears to be cally occur in adults, probably with sexual transmission. Concurrent
transmitted by saliva and possibly by genital secretions. epidemics of HIV-1 and HHV-8 infections among certain populations
Infection with HHV-6 frequently occurs during infancy as maternal (e.g., men who have sex with men) in the late 1970s and early 1980s
antibody wanes. The peak age of acquisition is 9–21 months; by appear to have resulted in the frequent association of AIDS and KS.
24 months, seropositivity rates approach 80%. Older siblings appear to Transmission of HHV-8 may also be associated with organ transplanta-
serve as a source of transmission. In addition, congenital infection may tion, injection drug use, and blood transfusion; however, transmission
occur, and ~1% of newborns are infected with HHV-6; placental infec- via organ transplantation or blood transfusion in the United States
tion with HHV-6 has been described. Congenital infection is generally appears to be quite rare.
asymptomatic, although subtle neurologic defects have been described. Primary HHV-8 infection in immunocompetent children may man-
Most postnatally infected children develop symptoms (fever, fussi- ifest as fever and maculopapular rash. Among individuals with intact
ness, and diarrhea). A minority develop exanthem subitum (roseola immunity, chronic asymptomatic infection is the rule, and neoplastic
infantum; see Fig. A1-5), a common illness characterized by fever with disorders generally develop only after subsequent immunocompromise.
Harrisons_20e_Part5_p0859-p1648.indd 1365 6/1/18 12:07 PM
1526 TABLE 209-1 Treatment of Blastomycosisa ACKNOWLEDGMENT
The authors thank Drs. Stanley W. Chapman and Donna C. Sullivan,
DISEASE PRIMARY THERAPY ALTERNATIVE THERAPY
Professors Emeriti, University of Mississippi, for their continued help and
Immunocompetent Patient/Life-Threatening Disease support and for their contributions to this chapter in an earlier edition.
Pulmonary Lipid AmB, 3–5 mg/kg qd, Itraconazole, 200–400
or mg/d (once patient’s ■ FURTHER READING
condition has stabilized) Richer SM et al: Development of a highly sensitive and specific blas-
AmB deoxycholate,
0.7–1.0 mg/kg qd (total tomycosis antibody enzyme immunoassay using Blastomyces dermati-
dose: 1.5–2.5 g) tidis surface protein BAD-1. Clin Vaccine Immunol 21:143, 2014.
Disseminated Thompson GR 3rd: Isavuconazole treatment of cryptococcosis and
CNS Lipid AmB, 3–5 mg/kg qd, Fluconazole, 800 mg/d (if dimorphic mycoses. Clin Infect Dis 63:356, 2016.
or patient is intolerant to full
course of AmB)
AmB deoxycholate,
0.7–1.0 mg/kg qd (total
Non-CNS
dose: at least 2 g)
Lipid AmB, 3–5 mg/kg qd,
or
Itraconazole, 200–400
mg/d (once patient’s
condition has stabilized)
210 Cryptococcosis
Arturo Casadevall
AmB deoxycholate,
0.7–1.0 mg/kg qd (total
dose: 1.5–2.5 g)
Immunocompetent Patient/Non-Life-Threatening Disease ■ DEFINITION AND ETIOLOGY
Cryptococcus, a genus of yeast-like fungi, is the etiologic agent of
Pulmonary or Itraconazole, 200–400 mg/d, Fluconazole, 400–800
disseminated mg/d,
cryptococcosis. Until recently, cryptococcal strains were separated
or into two species, Cryptococcus neoformans and Cryptococcus gattii, both
(non-CNS) or
Lipid AmB, 3–5 mg/kg qd, of which can cause cryptococcosis in humans. The two varieties of
or Ketoconazole,
400–800 mg/d
C. neoformans—grubii and neoformans—correlate with serotypes A and
AmB deoxycholate, 0.5–0.7 D, respectively. C. gattii, although not divided into varieties, also is
mg/kg qd (in patients antigenically diverse, encompassing serotypes B and C. However,
intolerant to itraconazole or
genome sequencing studies have now revealed tremendous diversity
whose disease progresses
among isolates previously assigned to each species, suggesting that
PART 5
despite therapy)
some may be reclassified as new species. Most clinical microbiology
Immunocompromised Patientb
laboratories do not routinely distinguish between C. neoformans and
All infections Lipid AmB, 3–5 mg/kg qd, Itraconazole, 200–400 C. gattii or among varieties, but rather identify and report all isolates
or mg/d (non-CNS disease,
once clinically improved)
simply as C. neoformans.
Infectious Diseases
AmB deoxycholate, 0.7–1.0
mg/kg qd (total dose:
1.5–2.5 g) ■ EPIDEMIOLOGY
Cryptococcosis was first described in the 1890s but remained relatively
a
Therapy is generally given for 6–12 months. For bone and joint disease, a
12-month course is usually necessary. bSuppressive therapy with itraconazole rare until the mid-twentieth century, when advances in diagnosis and
may be considered for patients whose immunocompromised state continues. increases in the number of immunosuppressed individuals markedly
Fluconazole (800 mg/d) may be useful for patients who have CNS disease or raised its reported prevalence. Although serologic evidence of cryp-
cannot tolerate itraconazole.
tococcal infection is common among immunocompetent individuals,
Abbreviations: AmB, amphotericin B; CNS, central nervous system.
cryptococcal disease (cryptococcosis) is relatively rare in the absence
of impaired immunity. Individuals at high risk for disease due to
Approval of delayed-release tablets and intravenous formulations C. neoformans include patients with hematologic malignancies, recip-
may enhance the role of posazonazole in salvage therapy. ients of solid organ transplants who require ongoing immunosup-
In a recent study including only three patients, isavuconazole, pressive therapy, persons whose medical conditions necessitate
the most recent addition to the azole antifungal class, showed vari- glucocorticoid therapy, and patients with advanced HIV infection and
able clinical efficacy (i.e., a 33% success rate) in the management CD4+ T lymphocyte counts of <200/μL. In contrast, C. gattii–related
of pulmonary and non-CNS disseminated blastomycosis. Its role disease is not associated with specific immune deficits and often occurs
in the management of blastomycosis is uncertain at this time, but in immunocompetent individuals.
its consideration may be warranted for salvage therapy in milder Cryptococcal infection is acquired from the environment.
pulmonary disease. C. neoformans and C. gattii inhabit different ecologic niches. C.
neoformans is frequently found in soils contaminated with
■ PROGNOSIS avian excreta and can easily be recovered from shaded and humid soils
Cure rates are 90–95% among compliant immunocompetent patients contaminated with pigeon droppings. In contrast, C. gattii is not found
given itraconazole for mild to moderate pulmonary and extrapulmo- in bird feces. Instead, it inhabits a variety of arboreal species, including
nary disease without CNS involvement. Bone and joint disease usually several types of eucalyptus tree. C. neoformans strains are found
requires 12 months of therapy. The fewer than 5% of infections that throughout the world; however, var. grubii (serotype A) strains are far
relapse after an initial course of itraconazole usually respond well to a more common than var. neoformans (serotype D) strains among both
second treatment course. clinical and environmental isolates. The geographic distribution of
C. gattii was thought to be largely limited to tropical regions until an
■ GLOBAL CONSIDERATIONS outbreak of cryptococcosis caused by a new serotype B strain began in
Blastomyces remains a prominent cause of dimorphic fungal Vancouver in 1999. This outbreak has extended into the United States,
infections worldwide. In the United States, changes in manda- and C. gattii infections are being encountered increasingly in several
tory reporting requirements have probably blurred estimates states in the Pacific Northwest.
of the current incidence of blastomycosis. Diagnostic delays continue to The global burden of cryptococcosis was recently estimated at
contribute to increased use of health care resources and administration ~1 million cases, with >600,000 deaths annually. Thus cryptococci are
of unnecessary antibacterial courses and probably contribute to global important human pathogens. Since the onset of the HIV pandemic in
resistance as well. the early 1980s, the overwhelming majority of cryptococcosis cases
Harrisons_20e_Part5_p0859-p1648.indd 1526 6/1/18 12:10 PM
have occurred in patients with AIDS (Chap. 197). To comprehend 1527
the impact of HIV infection on the epidemiology of cryptococcosis,
it is instructive to note that in the early 1990s there were >1000 cases
of cryptococcal meningitis each year in New York City—a figure far
exceeding that for all cases of bacterial meningitis. With the advent
of effective antiretroviral therapy, the incidence of AIDS-related cryp-
tococcosis has been sharply reduced among treated individuals.
Therefore, most cases of cryptococcosis now occur in resource-limited
regions of the world. The disease remains distressingly common in
regions where antiretroviral therapy is not readily available (e.g., parts
of Africa and Asia); in these regions, up to one-third of patients with
AIDS have cryptococcosis. Among HIV-infected persons, those with
a decreased percentage of memory B cells expressing IgM may be at
greater risk for cryptococcosis.
■ PATHOGENESIS
Cryptococcal infection is acquired by inhalation of aerosolized infectious
particles. The exact nature of these particles is not known; the two lead-
ing candidate forms are small desiccated yeast cells and basidiospores. FIGURE 210-1 Cryptococcal antigen in human brain tissue, as revealed by
Little is known about the pathogenesis of initial infection. Serologic immunohistochemical staining. Brown areas show polysaccharide deposits in
studies have shown that cryptococcal infection is acquired in child- the midbrain of a patient who died of cryptococcal meningitis. (Reprinted with
hood, but it is not known whether the initial infection is symptomatic. permission from SC Lee et al: Am J Pathol 148; 1267, 1996.)
Given that cryptococcal infection is common while disease is rare, the
consensus is that pulmonary defense mechanisms in immunologically
■ CLINICAL MANIFESTATIONS
intact individuals are highly effective at containing this fungus. It is not
The clinical manifestations of cryptococcosis reflect the site of fungal
clear whether initial infection leads to a state of immunity or whether
infection. The spectrum of disease caused by Cryptococcus species
most individuals are subject throughout life to frequent and recurrent
consists predominantly of meningoencephalitis and pneumonia, but
infections that resolve without clinical disease. However, evidence indi-
skin and soft tissue infections also occur; in fact, cryptococcosis can
cates that some human cryptococcal infections lead to a state of latency
CHAPTER 210 Cryptococcosis
affect any tissue or organ. CNS involvement usually presents as signs
in which viable organisms are harbored for prolonged periods, possibly
and symptoms of chronic meningitis, such as headache, fever, lethargy,
in granulomas. Thus the inhalation of cryptococcal cells and/or spores
sensory deficits, memory deficits, cranial nerve paresis, vision deficits,
can be followed by either clearance or establishment of the latent state.
and meningismus. Cryptococcal meningitis differs from bacterial men-
The consequences of prolonged harboring of cryptococcal cells in the
ingitis in that many Cryptococcus-infected patients present with symp-
lung are not known, but evidence from animal studies indicates that the
toms of several weeks’ duration. In addition, classic characteristics of
organisms’ prolonged presence could alter the immunologic milieu in
meningeal irritation, such as meningismus, may be absent in crypto-
the lung and predispose to allergic airway disease.
coccal meningitis. Indolent cases can present as subacute dementia.
Cryptococcosis usually presents clinically as chronic meningoen-
Meningeal cryptococcosis can lead to sudden catastrophic vision loss.
cephalitis. The mechanisms by which the fungus undergoes extrapul-
Pulmonary cryptococcosis usually presents as cough, increased
monary dissemination and enters the central nervous system (CNS)
sputum production, and chest pain. Patients infected with C. gattii can
remain poorly understood. The mechanism by which cryptococcal cells
present with granulomatous pulmonary masses known as cryptococco-
cross the blood–brain barrier is a subject of intensive study. Current
mas. Fever develops in a minority of cases. Like CNS disease, pulmo-
evidence suggests that both direct fungal-cell migration across the
nary cryptococcosis can follow an indolent course, and the majority of
endothelium and fungal-cell carriage inside macrophages as “Trojan
cases probably do not come to clinical attention. In fact, many cases are
horse” invaders can occur. Cryptococcus species have well-defined
discovered incidentally during the workup of an abnormal chest radio-
virulence factors that include the expression of the polysaccharide cap-
graph obtained for other diagnostic purposes. Pulmonary cryptococ-
sule, the ability to make melanin, and the elaboration of enzymes (e.g.,
cosis can be associated with antecedent diseases such as malignancy,
phospholipase and urease) that enhance the survival of fungal cells in
diabetes, and tuberculosis.
tissue. Among these virulence factors, the capsule and melanin pro-
Skin lesions are common in patients with disseminated cryptococ-
duction have been most extensively studied. The cryptococcal capsule
cosis and can be highly variable, including papules, plaques, purpura,
is antiphagocytic, and the capsular polysaccharide has been associated
vesicles, tumor-like lesions, and rashes. The spectrum of cryptococcosis
with numerous deleterious effects on host immune function. Crypto-
in HIV-infected patients is so varied and has changed so much since the
coccal infections can elicit little or no tissue inflammatory response.
advent of antiretroviral therapy that a distinction between HIV-related
The immune dysfunction seen in cryptococcosis has been attributed to
and HIV-unrelated cryptococcosis is no longer pertinent. In patients
the release of copious amounts of capsular polysaccharide into tissues,
with AIDS and solid organ transplant recipients, the lesions of cuta-
where it probably interferes with local immune responses (Fig. 210-1).
neous cryptococcosis often resemble those of molluscum contagiosum
In clinical practice, the capsular polysaccharide is the antigen that is
(Fig. 210-2; Chap. 191).
measured as a diagnostic marker of cryptococcal infection.
■ DIAGNOSIS
APPROACH TO THE PATIENT A diagnosis of cryptococcosis requires the demonstration of yeast cells
in normally sterile tissues. Visualization of the capsule of fungal cells
Cryptococcosis in cerebrospinal fluid (CSF) mixed with India ink is a useful rapid
Cryptococcosis should be included in the differential diagnosis diagnostic technique. Cryptococcal cells in India ink have a distinctive
when any patient presents with findings suggestive of chronic men- appearance because their capsules exclude ink particles. However,
ingitis. Concern about cryptococcosis is heightened by a history of the CSF India ink examination may yield negative results in patients
headache and neurologic symptoms in a patient with an underlying with a low fungal burden. This examination should be performed
immunosuppressive disorder or state that is associated with an by a trained individual, since leukocytes and fat globules can some-
increased incidence of cryptococcosis, such as advanced HIV infec- times be mistaken for fungal cells. Cultures of CSF and blood that
tion or solid organ transplantation. are positive for cryptococcal cells are diagnostic for cryptococcosis. In
cryptococcal meningitis, CSF examination usually reveals evidence of
Harrisons_20e_Part5_p0859-p1648.indd 1527 6/1/18 12:10 PM
1528 only after careful evaluation of the CSF reveals no evidence of cryp-
tococcal infection. For CNS involvement in a host without AIDS or
obvious immune impairment, most authorities recommend initial
therapy with AmB (0.5–1 mg/kg daily) during an induction phase,
which is followed by prolonged therapy with fluconazole (400 mg/d)
during a consolidation phase. For cryptococcal meningoencephalitis
without a concomitant immunosuppressive condition, the recom-
mended regimen is AmB (0.5–1 mg/kg) plus flucytosine (100 mg/
kg) daily for 6–10 weeks. Alternatively, patients can be treated with
AmB (0.5–1 mg/kg) plus flucytosine (100 mg/kg) daily for 2 weeks
and then with fluconazole (400 mg/d) for at least 10 weeks. Patients
with immunosuppression are treated with the same initial regimens
except that consolidation therapy with fluconazole is given for a
prolonged period to prevent relapse.
Cryptococcosis in patients with HIV infection always requires
aggressive therapy and is considered incurable unless immune func-
tion improves. Consequently, therapy for cryptococcosis in the setting
of AIDS has two phases: induction therapy (intended to reduce the
fungal burden and alleviate symptoms) and lifelong maintenance
FIGURE 210-2 Disseminated fungal infection. A liver transplant recipient therapy (to prevent a symptomatic clinical relapse). Pulmonary and
developed six cutaneous lesions similar to the one shown. Biopsy and serum extrapulmonary cryptococcosis without evidence of CNS involvement
antigen testing demonstrated Cryptococcus. Important features of the lesion can be treated with fluconazole (200–400 mg/d). In patients who
include a benign-appearing fleshy papule with central umbilication resembling have more extensive disease, flucytosine (100 mg/kg per day) may
molluscum contagiosum. (Photo courtesy of Dr. Lindsey Baden; with permission.) be added to the fluconazole regimen for 10 weeks, with lifelong flu-
conazole maintenance therapy thereafter. For HIV-infected patients
chronic meningitis with mononuclear cell pleocytosis and increased with evidence of CNS involvement, most authorities recommend
protein levels. A particularly useful test is cryptococcal antigen (CRAg) induction therapy with AmB. An acceptable regimen is AmB (0.7–1
detection in CSF and blood. The assay is based on serologic detection mg/kg) plus flucytosine (100 mg/kg) daily for 2 weeks followed by
of cryptococcal polysaccharide and is both sensitive and specific. A fluconazole (400 mg/d) for at least 10 weeks and then by lifelong
PART 5
positive CRAg test provides strong presumptive evidence for crypto- maintenance therapy with fluconazole (200 mg/d). Fluconazole
coccosis; however, because the result is often negative in pulmonary (400–800 mg/d) plus flucytosine (100 mg/kg per day) for 6–10 weeks
cryptococcosis, the test is less useful in the diagnosis of pulmonary followed by fluconazole (200 mg/d) as maintenance therapy is an
disease and is of only limited usefulness in monitoring the response alternative. Newer triazoles like voriconazole and posaconazole are
to therapy. highly active against cryptococcal strains and appear to be clinically
Infectious Diseases
In areas of Africa where there is a high prevalence of HIV effective, but clinical experience with these agents in the treatment
infection, routine screening of blood for CRAg in HIV-infected of cryptococcosis is limited. Lipid formulations of AmB can be sub-
patients with low CD4+ T lymphocyte counts may identify stituted for AmB deoxycholate in patients with renal impairment.
individuals at high risk of cryptococcal disease who are candidates for Neither caspofungin nor micafungin is effective against Cryptococcus
antifungal therapy. CRAg screening has shown that a significant pro- species; consequently, neither drug has a role in the treatment of
portion of HIV-infected patients hospitalized with pneumonia in Thai- cryptococcosis. Cryptococcal meningoencephalitis is often associ-
land harbor cryptococcal infection. Inexpensive point-of-care CRAg ated with increased intracranial pressure, which is believed to be
tests are under development and could be of great diagnostic benefit in responsible for damage to the brain and cranial nerves. Appropriate
resource-limited regions. management of CNS cryptococcosis requires careful attention to
the management of intracranial pressure, including the reduction
of pressure by repeated therapeutic lumbar puncture and the place-
TREATMENT ment of shunts. Studies suggest that the addition of a short course
Cryptococcosis of interferon γ to antifungal therapy in patients with HIV infection
increases clearance of cryptococci from the CSF.
Both the site of infection and the immune status of the host must In HIV-infected patients with previously treated cryptococcosis
be considered in the selection of therapy for cryptococcosis. The who are receiving fluconazole maintenance therapy, it may be possi-
disease has two general patterns of manifestation: (1) pulmonary ble to discontinue antifungal drug treatment if antiretroviral therapy
cryptococcosis, with no evidence of extrapulmonary dissemination; results in immunologic improvement.
and (2) extrapulmonary (systemic) cryptococcosis, with or without
meningoencephalitis. Pulmonary cryptococcosis in an immuno-
competent host sometimes resolves without therapy. However, ■ PROGNOSIS AND COMPLICATIONS
given the propensity of Cryptococcus species to disseminate from the Even with antifungal therapy, cryptococcosis is associated with high
lung, the inability to gauge the host’s immune status precisely, and rates of morbidity and death. For the majority of patients with cryp-
the availability of low-toxicity therapy in the form of fluconazole, tococcosis, the most important prognostic factors are the extent and
the current recommendation is for pulmonary cryptococcosis in the duration of the underlying immunologic deficits that predisposed
an immunocompetent individual to be treated with fluconazole them to develop the disease. Therefore, cryptococcosis is often curable
(200–400 mg/d for 3–6 months). Extrapulmonary cryptococcosis with antifungal therapy in individuals with no apparent immunologic
without CNS involvement in an immunocompetent host can be dysfunction, but, in patients with severe immunosuppression (e.g.,
treated with the same regimen, although amphotericin B (AmB; those with AIDS), the best that can be hoped for is that antifungal ther-
0.5–1 mg/kg daily for 4–6 weeks) may be required for more severe apy will induce remission, which can then be maintained with lifelong
cases. In general, extrapulmonary cryptococcosis without CNS suppressive therapy. Before the advent of antiretroviral therapy, the
involvement requires less intensive therapy, with the caveat that median overall survival period for AIDS patients with cryptococcosis
morbidity and death in cryptococcosis are associated with menin- was <1 year. Cryptococcosis in patients with underlying neoplastic
geal involvement. Thus the decision to categorize cryptococcosis disease has a particularly poor prognosis. For CNS cryptococcosis,
as “extrapulmonary without CNS involvement” should be made poor prognostic markers are a CSF assay positive for yeast cells on
Harrisons_20e_Part5_p0859-p1648.indd 1528 6/1/18 12:10 PM
initial India ink examination (evidence of a heavy fungal burden), high advent of Candida species as common human pathogens dates to the 1529
CSF pressure, low CSF glucose levels, low CSF pleocytosis (<2/μL), introduction of modern therapeutic approaches that suppress normal
recovery of yeast cells from extraneural sites, absence of antibody to host-defense mechanisms. Of these relatively recent advances, the most
capsular polysaccharide, a CSF or serum cryptococcal antigen level of important is the use of antibacterial agents that alter the normal human
≥1:32, and concomitant glucocorticoid therapy or hematologic malig- microbiota and allow nonbacterial species to become more prevalent
nancy. A response to treatment does not guarantee cure since relapse of in the commensal flora. With the introduction of antifungal agents,
cryptococcosis is common even among patients with relatively intact the causes of Candida infections shifted from an almost complete dom-
immune systems. Complications of CNS cryptococcosis include cranial inance of C. albicans to the common involvement of C. glabrata and the
nerve deficits, vision loss, and cognitive impairment. other species listed above. The non-albicans species now account for
approximately half of all cases of candidemia and hematogenously
■ IMMUNE RECONSTITUTION INFLAMMATORY disseminated candidiasis. Recognition of this change is clinically
SYNDROME important, since the various species differ in susceptibility to the newer
The frequent chronicity of cryptococcal infections and their common antifungal agents.
occurrence in settings of changing immunity can result in new clinical Candida is a small, thin-walled, ovoid yeast that measures 4–6 μm in
syndromes, such as the immune reconstitution inflammatory syn- diameter and reproduces by budding. Organisms of this genus occur in
drome (IRIS). IRIS occurs when immunity rebounds in the setting of three forms in tissue: blastospores, pseudohyphae, and hyphae. Candida
treated cryptococcosis (or an undiagnosed asymptomatic infection) grows readily on simple medium; lysis centrifugation enhances its
and the immune response to cryptococcal antigens in tissue triggers recovery from blood. Species are identified by biochemical testing (cur-
an inflammatory response that can be difficult to distinguish from rently with automated devices) or on special agar (e.g., CHROMagar).
a relapsing infection. IRIS can occur when patients with AIDS and
treated cryptococcosis are given antiretroviral therapy that results ■ EPIDEMIOLOGY
in improved immunity. Apart from the difficulties in distinguishing Candida are present in humans as commensals, in animals, in
IRIS from cryptococcal relapse, the management of this syndrome is foods, and on inanimate objects. In developed countries, where
complex because it is caused by the desirable outcome of improving contemporary medical therapeutics are commonly used, Candida
immunity, which is important in controlling cryptococcal infection species are now among the most common nosocomial pathogens. In the
and preventing relapses. The approach to the patient with IRIS must United States, these species are the fourth most common isolates from
attempt to balance resurgent immunity against immune-mediated the blood of hospitalized patients. In a recent point-prevalence study,
damage. Currently, management of IRIS is individualized and can Candida species were the most common organisms infecting the blood-
CHAPTER 211 Candidiasis
involve the use of glucocorticoids to reduce inflammation. stream of hospitalized patients. In regions where advanced medical care
is rarely available, mucocutaneous Candida infections, such as thrush,
■ PREVENTION are more common than deep-organ infections, which rarely occur.
No vaccine is available for cryptococcosis. In patients at high risk (e.g., However, the incidence of deep-organ candidiasis increases steadily as
those with advanced HIV infection and CD4+ T lymphocyte counts of advances in health care—such as therapy with broad-spectrum antibi-
<200/μL), primary prophylaxis with fluconazole (200 mg/d) is effec- otics, more aggressive treatment of cancer, and the use of immunosup-
tive in reducing the prevalence of disease. Since antiretroviral therapy pression for sustaining organ transplants—are implemented. In
raises the CD4+ T lymphocyte count, it constitutes an immunologic aggregate, the global incidence of infections due to Candida species has
form of prophylaxis. risen steadily over the past few decades. Of great recent concern has
■ FURTHER READING been the global emergence of C. auris; certain strains of this organism
Kwon-Chung KJ et al: The case for adopting the “species complex” are resistant to all classes of antifungal agents, and mortality rates from
nomenclature for the etiologic agents of cryptococcosis. mSphere infection have been very high.
2 pii:e00357, 2017.
Maziarz EK, Perfect JR: Cryptococcosis. Infect Dis Clin North Am ■ PATHOGENESIS
30:179, 2016. In the most serious form of Candida infection, the organisms dissem-
Robertson EJ et al: Cryptococcus neoformans ex vivo capsule size is inate hematogenously and form microabscesses and small macroab-
associated with intracranial pressure and host immune response in scesses in major organs. Although the exact mechanism is not known,
HIV-associated cryptococcal meningitis. J Infect Dis 209:74, 2014. Candida probably enters the bloodstream from mucosal surfaces after
Saag MS et al: Practice guidelines for the management of cryptococcal growing to large numbers as a consequence of bacterial suppression
disease. Infectious Diseases Society of America. Clin Infect Dis 30:710, by antibacterial drugs; alternatively, in some instances, the organism
2000. may enter from the skin. A change from the blastospore stage to the
Srichatrapimuk S, Sungkanuparph S: Integrated therapy for HIV pseudohyphal and hyphal stages is generally considered integral to
and cryptococcosis. AIDS Res Ther 13:42, 2016. Candida’s penetration into tissue. However, C. glabrata can cause exten-
sive infection even though it does not transform into pseudohyphae or
hyphae. Adherence to both epithelial and endothelial cells is thought to
be the first step in invasion and infection; several adhesins have been
identified as well as a mucosal toxin, candidalysin. Biofilm formation
211 Candidiasis
also is considered important in pathogenesis. Numerous reviews of
cases of hematogenously disseminated candidiasis have identified
the predisposing factors or conditions associated with disseminated
John E. Edwards, Jr. disease (Table 211-1). Women who receive antibacterial agents may
develop vaginal candidiasis.
Innate immunity is the most important defense mechanism against
The genus Candida encompasses >150 species, only a few of which hematogenously disseminated candidiasis, and the neutrophil is the
cause disease in humans. With rare exceptions (although the excep- most important component of this defense. Macrophages also play an
tions are increasing in number), the human pathogens are C. albicans, important defensive role. STAT1, Dectin-1, CARD9, and TH1 and TH17
C. guilliermondii, C. krusei, C. parapsilosis, C. tropicalis, C. kefyr, C. lusitaniae, lymphocytes contribute significantly to innate defense (see “Clinical Man-
C. dubliniensis, C. glabrata, and C. auris. Ubiquitous in nature, they ifestations,” below). Although many immunocompetent individuals have
inhabit the gastrointestinal tract (including the mouth and orophar- antibodies to Candida, the role of these antibodies in defense against the
ynx), the female genital tract, and the skin. Although cases of candid- organism is not clear. Multiple genetic polymorphisms that predispose to
iasis have been described since antiquity in debilitated patients, the disseminated candidiasis will most likely be identified in future studies.
Harrisons_20e_Part5_p0859-p1648.indd 1529 6/1/18 12:10 PM
■ PROGNOSIS vacuole. After the parasites reach a critical mass, intracellular signaling 1609
More than 95% of patients with first-stage and second-stage T. b. gam- within the host and the parasite, including calcium fluxes, results in
biense HAT are definitively cured with pentamidine and nifurtimox– parasite egress from the vacuole. The host cell is destroyed, and the
eflornithine combination therapy, respectively. The overall case–fatality released tachyzoites infect adjoining cells. Parasites can disseminate
rate is <1% except in very advanced cases. As relapses can occur long throughout the body as free tachyzoites or within phagocytic cells in
after completion of treatment, follow-up visits are advised every 6 months the bloodstream or via lymphatics. Tachyzoites actively invade host
for at least 2 years. The relapse rate is very low (<2%) with current cells and can cross epithelial barriers.
first-line therapies; thus blood and CSF examinations during follow-up The tachyzoite replication cycle within an infected organ causes
visits are no longer standard but can be restricted to symptomatic cytopathology and clinical symptoms. Most tachyzoites are elimi-
patients. Patients with second-stage T. b. rhodesiense HAT are at a 5–10% nated by the host’s humoral and cell-mediated immune responses.
risk of dying during or after melarsoprol treatment, but relapses are Tissue cysts containing bradyzoites develop 7–10 days after systemic
very rare. tachyzoite infection. These tissue cysts occur in various host organs
but persist principally within the central nervous system (CNS) and
■ GLOBAL CONSIDERATIONS muscle. The development of this chronic stage completes the asexual
The elimination of sleeping sickness as a public health prob- portion of the life cycle. Active infection in the immunocompromised
lem is in sight, thanks to increased control activities run by host is most likely to be due to the spontaneous release of encysted
national control programs and nongovernmental medical parasites that undergo rapid transformation into tachyzoites within the
organizations, improved funding, and the end of several civil wars CNS and are not contained by the immune system.
(e.g., in Angola) in the last 15 years. Funding for research, develop- The sexual stage in the life cycle takes place in the cat (the definitive
ment, and implementation of improved diagnostic methods (e.g., rapid host) and is defined by the formation of oocysts within the feline host.
diagnostic tests) and therapeutic tools (e.g., oral drugs) remains crucial This enteroepithelial cycle begins with the ingestion of the bradyzoite
to sustain recent achievements. tissue cysts and, after several intermediate stages, culminates in the
production of gametes. Gamete fusion produces a zygote, which envel-
■ FURTHER READING ops itself in a rigid wall and is secreted in the feces as an unsporulated
Brun R et al: Human African trypanosomiasis. Lancet 375:148, 2010.
oocyst. After 2–3 days of exposure to air at ambient temperature, the
Morillo CA et al: Randomized trial of benznidazole for chronic
noninfectious oocyst sporulates to produce eight sporozoite progeny.
Chagas disease cardiomyopathy. N Engl J Med 373:1295, 2015.
The sporulated oocyst can be ingested by an intermediate host, such as
Pérez-Molina JA et al: Old and new challenges in Chagas disease.
a person emptying a cat’s litter box or a pig rummaging in a barnyard.
Lancet Infect Dis 15:1347, 2015.
CHAPTER 223 Toxoplasma Infections
It is in the intermediate host that T. gondii completes its life cycle.
Rassi A Jr et al: Chagas disease. Lancet 375:1388, 2010.
Sporulated oocysts are environmentally hardy and very infec-
Urech K et al: Sleeping sickness in travelers—Do they really sleep?
tious; they are thought to be sources of waterborne outbreaks
PLoS Negl Trop Dis 5:e1358, 2011.
such as those reported in Victoria (British Columbia, Canada)
and in South America. Strains found in South America are more viru-
lent than those from the Northern Hemisphere and are more likely to
be associated with symptomatic disease—usually ocular—in immuno-
223 Toxoplasma Infections
Kami Kim
competent individuals; thus ocular toxoplasmosis should be consid-
ered in a person from South America with ocular symptoms and retinal
abnormalities. Severe disease, including sepsis, fever of unknown ori-
gin, and pneumonia, have been reported and should be considered in
a patient with a history of travel to South America.
■ DEFINITION
Toxoplasmosis is caused by infection with the obligate intracellular ■ EPIDEMIOLOGY
parasite Toxoplasma gondii. Acute infection acquired after birth may be T. gondii infects a wide range of mammals and birds. Its
asymptomatic but is thought to result in the lifelong chronic persistence seroprevalence depends on the locale and the age of the pop-
of cysts in the host’s tissues. In both acute and chronic toxoplasmo- ulation. Generally, hot arid climatic conditions are associated
sis, the parasite is responsible for clinically evident disease, includ- with a low prevalence of infection. In the United States and most Euro-
ing lymphadenopathy, encephalitis, myocarditis, and pneumonitis. pean countries, seroprevalence increases with age and exposure. In the
Congenital toxoplasmosis is an infection of newborns that results from United States, 13.2% of individuals >6 years old had serologic evidence
the transplacental passage of parasites from an infected mother to the of exposure in a 2009–2010 survey, with foreign-born Americans having
fetus. These infants may be asymptomatic at birth, but many later man- a higher rate of seroprevalence. In most other regions of the world, the
ifest a wide range of signs and symptoms, including chorioretinitis, seroprevalence is higher. Perhaps because of increased awareness of
strabismus, epilepsy, and psychomotor retardation. In immunocom- foodborne infections, the prevalence of seropositivity has decreased
petent individuals, toxoplasmosis can also present as acute disease worldwide over the past two decades.
(typically chorioretinitis) associated with food- or waterborne sources.
■ TRANSMISSION
■ ETIOLOGY
T. gondii is an intracellular coccidian that infects both birds and mam- Oral Transmission Most cases of human Toxoplasma infection are
mals. There are two distinct stages in the life cycle that are transmis- thought to be acquired by the oral route. Transmission can be attribut-
sible to humans (Fig. 223-1). Tissue cysts that contain bradyzoites are able to ingestion of sporulated oocysts from contaminated soil, food,
transmitted in undercooked meat. After an intermediate host (e.g., or water. During acute feline infection, a cat may excrete as many as
a human, mouse, sheep, pig, or bird) ingests the cyst, it is rapidly 100 million oocysts per day. These sporozoite-containing oocysts
digested by the acidic-pH gastric secretions. Sporulated oocysts that are highly infectious and may remain viable for many years in soil
contain sporozoites are products of the sexual cycle in feline intestines or water. Humans infected during an oocyst-transmitted infection
and are acquired by ingestion of food or water contaminated with develop stage-specific antibodies to the oocyst/sporozoite.
infected cat feces. Bradyzoites or sporozoites are released, enter the Children and adults also acquire infection from tissue cysts con-
intestinal epithelium, and transform into rapidly dividing tachyzoites. taining bradyzoites. Undercooking or insufficient freezing of meat is
The tachyzoites can infect and replicate in all mammalian cells except an important source of infection in the developed world. More recent
red blood cells. The parasite actively penetrates the cell and forms a epidemiologic studies have associated acute infections with ingestion
parasitophorous vacuole. Parasite replication continues within the of untreated water or shellfish (oysters, mussels, and clams).
Harrisons_20e_Part5_p0859-p1648.indd 1609 6/1/18 12:11 PM
1610 but the disease in the neonate is most
Intermediate host:
birds, mammals, humans severe. If maternal infection occurs dur-
ing the third trimester, the incidence of
Bradyzoites encyst transplacental infection is greatest (65%),
within the CNS but the infant is usually asymptomatic
and muscle of the at birth. Infected infants who are nor-
infected host. mal at birth may have a higher inci-
dence of learning disabilities and chronic
neurologic sequelae than uninfected
children. Only a small proportion (20%)
of women infected with T. gondii develop
Tachyzoites infect
all nucleated cells in
clinical signs of infection. Often the diag-
the host, replicate, nosis is first appreciated when routine
and cause tissue postconception serologic tests show evi-
Oocysts are excreted dence of specific antibody.
damage.
in cat feces.
Contaminated soil is ■ PATHOGENESIS
ingested by birds, Upon the host’s ingestion of either tissue
mammals, and humans.
cysts containing bradyzoites or oocysts
containing sporozoites, the parasites are
Toxoplasmic released from the cysts by the digestive
encephalitis process. Bradyzoites are resistant to the
effect of pepsin and invade the host’s
Definitive host
gastrointestinal tract. Within enterocytes
FIGURE 223-1 Life cycle of Toxoplasma gondii. The cat is the definitive host in which the sexual phase of the cycle is (or other gut-associated cells), the para-
completed. Oocysts shed in cat feces can infect a wide range of animals, including birds, rodents, grazing domestic sites undergo morphologic transforma-
animals, and humans. The bradyzoites found in the muscle of food animals may infect humans who eat insufficiently tion, giving rise to invasive tachyzoites.
cooked meat products, particularly lamb and pork. Although human disease can take many forms, congenital From the gastrointestinal tract, parasites
infection and encephalitis from reactivation of latent infection in the brains of immunosuppressed persons are the disseminate to a variety of organs, partic-
most important manifestations. CNS, central nervous system. (Courtesy of Dominique Buzoni-Gatel, Institut Pasteur, ularly lymphatic tissue, skeletal muscle,
PART 5
Paris; with permission.)
myocardium, retina, placenta, and the
CNS. At these sites, the parasite infects
Transmission via Blood or Organs In addition to being trans- host cells, replicates, and invades the adjoining cells. In this fashion,
mitted orally, T. gondii can be transmitted directly from a seropositive the hallmarks of the infection develop: cell death and focal necrosis
Infectious Diseases
donor to a seronegative recipient in a transplanted heart, heart–lung, surrounded by an acute inflammatory response.
kidney, liver, or pancreas. Viable parasites can be cultured from refrig- In the immunocompetent host, both the humoral and the cellular
erated anticoagulated blood, which may be a source of infection in immune responses control infection; parasite virulence and tissue
individuals receiving blood transfusions. T. gondii reactivation has tropism may be strain specific. Tachyzoites are sequestered by a
been reported in bone marrow, hematopoietic stem cell, and liver variety of immune mechanisms, including induction of parasiticidal
transplant recipients as well as in individuals with AIDS. Although antibody, activation of macrophages with radical intermediates, pro-
antibody titers generally are not useful in monitoring T. gondii infec- duction of interferon γ (IFN-γ), and stimulation of CD8+ cytotoxic
tion, individuals with higher antibody titers may be at relatively high T lymphocytes. These antigen-specific lymphocytes are capable of kill-
risk for reactivation after hematopoietic stem cell transplantation; thus ing both extracellular parasites and target cells infected with parasites.
routine polymerase chain reaction (PCR) screening of blood from these As tachyzoites are cleared from the acutely infected host, tissue cysts
patients may be in order. Screening of Toxoplasma serologies (donor and containing bradyzoites begin to appear, usually within the CNS, the
recipient) before transplantation may identify patients potentially at skeletal muscle, and the retina. Studies indicate that Toxoplasma secretes
risk for reactivated toxoplasmosis. Finally, laboratory personnel can be signaling molecules into infected host cells and that these molecules
infected after contact with contaminated needles or glassware or with modulate host gene expression, host metabolism, and host immune
infected tissue. response. While it was initially thought that cysts with bradyzoites are
not eliminated by the immune system, recent studies in the murine
Transplacental Transmission On average, about one-third model indicate that both CD8+ T cells and alternatively activated mac-
of all women who acquire infection with T. gondii during pregnancy rophages are able to kill cysts in vivo; some cysts persist, however, and
transmit the parasite to the fetus; the remainder give birth to normal, the ability to eliminate cysts may depend on the genetic background of
uninfected babies. Of the various factors that influence fetal outcome, the infected host.
gestational age at the time of infection is the most critical (see below). In the immunocompromised or fetal host, the immune factors nec-
Recrudescent maternal infection is rarely the source of congenital essary to control the spread of tachyzoite infection are lacking. This
disease, although rare cases of transmission by immunocompromised altered immune state allows the persistence of tachyzoites and gives
women (e.g., those infected with HIV or those receiving high-dose rise to progressive focal destruction in affected organs (i.e., necrotizing
glucocorticoids) have been reported. Thus women who are seropositive encephalitis, pneumonia, and myocarditis).
before pregnancy usually are protected against acute infection and do It is thought that all infected individuals have persistent infection
not give birth to congenitally infected neonates. with cysts containing bradyzoites, but this lifelong infection usually
There is essentially no risk of congenital infection if the mother remains subclinical. Although bradyzoites are in a slow metabolic
becomes infected ≥6 months before conception. If infection is acquired phase, cysts do degenerate and rupture within the CNS. This degenera-
<6 months before conception, the likelihood of transplacental infection tive process, with the development of new bradyzoite-containing cysts,
increases as the interval between infection and conception decreases. is the most probable source of recrudescent infection in immunocom-
Women with documented acute toxoplasmosis should be counseled promised individuals and the most likely stimulus for the persistence
to use appropriate measures to prevent pregnancy for 6 months after of antibody titers in the immunocompetent host. Although the concept
infection. In pregnancy, if the mother becomes infected during the first is controversial, the persistence of toxoplasmosis has been hypoth-
trimester, the incidence of transplacental infection is lowest (~15%), esized to be a contributing factor to a variety of neuropsychiatric
Harrisons_20e_Part5_p0859-p1648.indd 1610 6/1/18 12:11 PM
conditions, including schizophrenia and bipolar disease. In rodents, effects from acute infection of these various organs, including pancre- 1611
chronic infection clearly has significant effects on behavior, increasing atitis, myositis, and glomerulonephritis, have been reported.
predation.
■ HOST IMMUNE RESPONSE
■ PATHOLOGY Acute Toxoplasma infection evokes a cascade of protective immune
Cell death and focal necrosis due to replicating tachyzoites induce responses in the immunocompetent host. Toxoplasma enters the host
an intense mononuclear inflammatory response in any tissue or cell at the gut mucosal level and evokes a mucosal immune response that
type infected. Tachyzoites rarely can be visualized by routine histo- includes the production of antigen-specific secretory IgA. Titers of
pathologic staining of these inflammatory lesions. However, immu- serum IgA antibody directed at the tachyzoite surface antigen p30/
nofluorescent staining with parasitic antigen–specific antibodies can SAG1 are a useful marker for congenital and acute toxoplasmosis.
reveal the organism. In contrast to this inflammatory process caused Within the host, T. gondii rapidly induces detectable levels of both
by tachyzoites, bradyzoite-containing cysts cause inflammation only IgM and IgG serum antibodies. Monoclonal gammopathy of the IgG
at the early stages of development. Once the cysts reach maturity, class can occur in congenitally infected infants. IgM levels may be
the inflammatory process can no longer be detected, and the cysts increased in newborns with congenital infection. The polyclonal IgG
remain immunologically quiescent within the brain matrix until they antibodies evoked by infection are parasiticidal in vitro in the presence
rupture. of serum complement and are the basis for the Sabin–Feldman dye
test. However, cell-mediated immunity is the major protective response
Lymph Nodes During acute infection, lymph node biopsy dem-
evoked by the parasite during infection. Macrophages are activated
onstrates characteristic findings, including follicular hyperplasia
after phagocytosis of antibody-opsonized parasites. This activation
and irregular clusters of tissue macrophages with eosinophilic cyto-
can lead to death of the parasite by either an oxygen-dependent or an
plasm. Granulomas rarely are evident in these specimens. Although
oxygen-independent process. If the parasite is not phagocytosed and
tachyzoites are not usually visible, they can be sought either by subin-
enters the macrophage by active penetration, it continues to replicate,
oculation of infected tissue into mice, with resultant disease, or by PCR.
and this replication may represent the mechanism for transport and
PCR amplification of DNA fragments of Toxoplasma genes is effective
dissemination to distant organs. Toxoplasma stimulates a robust inter-
and sensitive in establishing lymph node infection by tachyzoites.
leukin (IL) 12 response by human dendritic cells. The CD4+ and CD8+
Eyes In the eye, infiltrates of monocytes, lymphocytes, and plasma T cell responses are antigen-specific and further stimulate the produc-
cells may produce uni- or multifocal lesions. Granulomatous lesions tion of a variety of important lymphokines that expand the T cell and
and chorioretinitis can be observed in the posterior chamber after acute natural killer cell repertoire. T. gondii is a potent inducer of a TH1 pheno-
CHAPTER 223 Toxoplasma Infections
necrotizing retinitis. Other ocular complications include iridocyclitis, type, with IL-12 and IFN-γ playing an essential role in the control of the
cataracts, and glaucoma. parasites’ growth in the host. Regulation of the inflammatory response
is at least partially under the control of a TH2 response that includes
Central Nervous System During CNS involvement, both focal the production of IL-4 and IL-10 in seropositive individuals. Human
and diffuse meningoencephalitis can be documented, with evidence of T cell clones of both the CD4+ and the CD8+ phenotypes are cytolytic
necrosis and microglial nodules. Necrotizing encephalitis in patients against parasite-infected macrophages. These T cell clones produce
without AIDS is characterized by small diffuse lesions with perivas- cytokines that are “microbistatic.” IL-18, IL-7, and IL-15 upregulate the
cular cuffing in contiguous areas. In the AIDS population, polymor- production of IFN-γ and may be important during acute and chronic
phonuclear leukocytes may be present in addition to monocytes, infection. The effect of IFN-γ may be paradoxical, with stimulation of a
lymphocytes, and plasma cells. Cysts containing bradyzoites frequently host downregulatory response as well.
are found contiguous with the necrotic tissue border. As a consequence Although T. gondii infection is thought to be recrudescent in patients
of combined antiretroviral therapy (cART) for AIDS, the incidence of with AIDS or other immunocompromised states, antibody titers are
toxoplasmosis has decreased in the developed world. Its incidence in not useful in establishing reactivation or in following the activity of
under-resourced settings is not known but is likely to be high. infection. An absence of positive serologic results suggests an alterna-
Lungs and Heart Among patients with AIDS who die of toxo- tive diagnosis, although AIDS patients may have borderline positive
plasmosis, 40–70% have involvement of the lungs and heart. Intersti- or low serologic values. T cells from AIDS patients with reactivation
tial pneumonitis can develop in neonates and immunocompromised of toxoplasmosis fail to secrete both IFN-γ and IL-2. This alteration in
patients. Thickened and edematous alveolar septa infiltrated with the production of these critical immune cytokines contributes to the
mononuclear and plasma cells are apparent. This inflammation may persistence of infection. Toxoplasma infection frequently develops late
extend to the endothelial walls. Tachyzoites and bradyzoite-containing in the course of AIDS (CD4+ T cell count, <100/μL), when the loss of
cysts have been observed within the alveolar membrane. Superim- T cell–dependent protective mechanisms, particularly CD8+ T cells,
posed bronchopneumonia can be caused by other microbial agents. becomes most pronounced.
Cysts and aggregates of parasites in cardiac muscle tissue are evident
in patients with AIDS who die of toxoplasmosis. Focal necrosis sur-
■ CLINICAL MANIFESTATIONS
In persons whose immune systems are intact, acute toxoplasmosis is
rounded by inflammatory cells is associated with hyaline necrosis and
usually asymptomatic and self-limited. This condition can go unrec-
disrupted myocardial cells. Pericarditis is associated with toxoplasmo-
ognized in 80–90% of adults and children with acquired infection.
sis in some patients.
The asymptomatic nature of this infection makes diagnosis difficult
Gastrointestinal Tract Rare cases of human gastrointestinal tract in mothers infected during pregnancy. In contrast, the wide range
infection with T. gondii have presented as ulcerations in the mucosa. of clinical manifestations in congenitally infected children includes
Acute infection in certain strains of inbred mice (C57BL/6) results in severe neurologic complications such as hydrocephalus, microcephaly,
lethal ileitis within 7–9 days. This inflammatory bowel disease has mental retardation, and chorioretinitis. If prenatal infection is severe,
been recognized in several other mammalian species, including pigs multiorgan failure and subsequent intrauterine fetal death can occur. In
and nonhuman primates. children and adults, chronic infection can persist throughout life, with
little consequence to the immunocompetent host.
Other Sites Pathologic changes during disseminated infection
are similar to those described for the lymph nodes, eyes, and CNS. In Toxoplasmosis in Immunocompetent Patients The most
patients with AIDS, the skeletal muscle, pancreas, stomach, and kid- common manifestation of acute toxoplasmosis is cervical lymphade-
neys can be involved, with necrosis, invasion by inflammatory cells, nopathy. The nodes may be single or multiple, are usually nontender,
and (rarely) tachyzoites detectable by routine staining. Large necrotic are discrete, and vary in firmness. Lymphadenopathy also may be
lesions may cause direct tissue destruction. In addition, secondary found in suboccipital, supraclavicular, inguinal, and mediastinal areas.
Harrisons_20e_Part5_p0859-p1648.indd 1611 6/1/18 12:11 PM
1612 Generalized lymphadenopathy occurs in 20–30% of symptomatic visual-field loss, and aphasia. Patients who present with evidence of
patients. Between 20 and 40% of patients with lymphadenopathy diffuse cortical dysfunction develop evidence of focal neurologic dis-
also have headache, malaise, fatigue, and fever (usually with a tem- ease as infection progresses. This altered condition is due not only to
perature of <40°C [<104°F]). A smaller proportion of symptomatic the necrotizing encephalitis caused by direct invasion by the parasite
individuals have myalgia, sore throat, abdominal pain, maculopapular but also to secondary effects, including vasculitis, edema, and hemor-
rash, meningoencephalitis, and confusion. Rare complications associ- rhage. The onset of infection can range from an insidious process over
ated with infection in the normal immune host include pneumonia, several weeks to an acute presentation with fulminant focal deficits,
myocarditis, encephalopathy, pericarditis, and polymyositis. Signs including hemiparesis, hemiplegia, visual-field defects, localized head-
and symptoms associated with acute infection usually resolve within ache, and focal seizures.
several weeks, although the lymphadenopathy may persist for some Although lesions can occur anywhere in the CNS, the areas most
months. In one epidemic, toxoplasmosis was diagnosed correctly in often involved appear to be the brainstem, basal ganglia, pituitary
only 3 of the 25 patients who consulted physicians. If toxoplasmosis gland, and corticomedullary junction. Brainstem involvement gives
is considered in the differential diagnosis, routine laboratory and sero- rise to a variety of neurologic dysfunctions, including cranial nerve
logic screening should precede node biopsy. palsy, dysmetria, and ataxia. With basal ganglion infection, patients
In North America and Europe, there are three predominant may develop hydrocephalus, choreiform movements, and choreo-
genotypes of T. gondii, but strains are more genetically diverse athetosis. Toxoplasma usually causes encephalitis, and meningeal
in South America. Genotypes of T. gondii prevalent in involvement is uncommon. CSF findings may be unremarkable or
South America are more virulent than those typically seen in North may include a modest increase in cell count and in protein—but not
America or Europe. These genotypes may be associated with acute or glucose—concentration.
recurrent ocular disease in immunocompetent individuals and have Cerebral toxoplasmosis must be differentiated from other oppor-
also been associated with pneumonitis and a fulminant sepsis picture tunistic infections or tumors in the CNS of AIDS patients. The differ-
in immunologically normal individuals. Thus a detailed history is crit- ential diagnosis includes herpes simplex encephalitis, cryptococcal
ical for establishing a diagnosis. meningitis, progressive multifocal leukoencephalopathy, and primary
The results of routine laboratory studies are usually unremarkable CNS lymphoma. Involvement of the pituitary gland can give rise to
except for minimal lymphocytosis, an elevated erythrocyte sedimen- panhypopituitarism and hyponatremia from inappropriate secretion
tation rate, and a nominal increase in serum aminotransferase levels. of vasopressin (antidiuretic hormone). HIV-associated neurocognitive
Evaluation of cerebrospinal fluid (CSF) in cases with evidence of disorder (HAND) may present as cognitive impairment, attention loss,
encephalopathy or meningoencephalitis shows an elevation of intra- and altered memory. Brain biopsy in patients who have been treated
cranial pressure, mononuclear pleocytosis (10–50 cells/mL), a slight for TE but who continue to exhibit neurologic dysfunction often fails
PART 5
increase in protein concentration, and (occasionally) an increase in the to identify organisms.
gamma globulin level. PCR amplification of the Toxoplasma DNA target Autopsies of Toxoplasma-infected patients have demonstrated the
sequence in CSF is specific for active toxoplasmosis, but not sensitive. involvement of multiple organs, including the lungs, gastrointestinal
The CSF of chronically infected individuals is normal. tract, pancreas, skin, eyes, heart, and liver. Toxoplasma pneumonia can
be confused with Pneumocystis pneumonia (PcP). Respiratory involve-
Infectious Diseases
Infection of Immunocompromised Patients Patients with ment usually presents as dyspnea, fever, and a nonproductive cough
AIDS and those receiving immunosuppressive therapy for lym-
and may rapidly progress to acute respiratory failure with hemoptysis,
phoproliferative disorders are at greatest risk for developing acute tox-
metabolic acidosis, hypotension, and (occasionally) disseminated intra-
oplasmosis. Toxoplasmosis has also been reported after treatment with
vascular coagulation. Histopathologic studies demonstrate necrosis
antibodies to tumor necrosis factor. The infection may be due either
and a mixed cellular infiltrate. The presence of organisms is a helpful
to reactivation of latent infection or to acquisition of parasites from
diagnostic indicator, but organisms can also be found in healthy tissue.
exogenous sources such as blood or transplanted organs. In individuals
Infection of the heart is usually asymptomatic but can be associated
with AIDS, >95% of cases of Toxoplasma encephalitis (TE) are believed
with cardiac tamponade or biventricular failure. Infections of the gas-
to be due to recrudescent infection. In most of these cases, encephalitis
trointestinal tract and the liver have been documented.
develops when the CD4+ T cell count falls below 100/μL. In immuno-
compromised hosts, the disease may be rapidly fatal if untreated. Thus, Congenital Toxoplasmosis Between 400 and 4000 infants born
accurate diagnosis and initiation of appropriate therapy are necessary each year in the United States are affected by congenital toxoplasmo-
to prevent fulminant infection. sis. Acute infection in mothers acquiring T. gondii during pregnancy is
Toxoplasmosis is a principal opportunistic infection of the CNS usually asymptomatic; most such women are diagnosed via prenatal
in persons with AIDS. Although geographic origin may be related to serologic screening. Infection of the placenta leads to hematogenous
frequency of infection, it has no correlation with the severity of disease infection of the fetus. As gestation proceeds, the proportion of fetuses
in immunocompromised hosts. Individuals with AIDS who are sero- that become infected increases, but the clinical severity of the infection
positive for T. gondii are at high risk for encephalitis. Before the advent declines. Although infected children may initially be asymptomatic,
of current cART, about one-third of the 15–40% of
adult AIDS patients in the United States who were
latently infected with T. gondii developed TE. TE
may still be a presenting infection in individuals
who are unaware of their positive HIV status.
The signs and symptoms of acute toxoplasmo-
sis in immunocompromised patients principally
involve the CNS (Fig. 223-2). More than 50% of
patients with clinical manifestations have intrace-
rebral involvement. Clinical findings at presenta-
tion range from nonfocal to focal dysfunction. CNS
findings include encephalopathy, meningoenceph-
alitis, and mass lesions. Patients may present with
altered mental status (75%), fever (10–72%), sei-
zures (33%), headaches (56%), and focal neurologic FIGURE 223-2 Toxoplasmic encephalitis in a 36-year-old patient with AIDS. The multiple lesions are
findings (60%), including motor deficits, cranial demonstrated by MRI scanning (T1-weighted with gadolinium enhancement). (Courtesy of Clifford Eskey,
nerve palsies, movement disorders, dysmetria, Dartmouth Hitchcock Medical Center, Hanover, NH; with permission.)
Harrisons_20e_Part5_p0859-p1648.indd 1612 6/1/18 12:11 PM
the persistence of T. gondii can result in reactivation and clinical TABLE 223-1 Differential Laboratory Diagnosis of Toxoplasmosis 1613
disease—most frequently chorioretinitis—decades later. Factors associ-
DISTINGUISHING
ated with relatively severe disabilities include delays in diagnosis and CLINICAL SETTING ALTERNATIVE DIAGNOSIS CHARACTERISTICS
in initiation of therapy, neonatal hypoxia and hypoglycemia, profound Mononucleosis Epstein-Barr virus infection Serology/PCR
visual impairment (see “Ocular Infection,” below), uncorrected hydro- syndrome Cytomegalovirus infection Serology/PCR or culture
cephalus, and increased intracranial pressure. If treated appropriately,
HIV infection Serology/viral load
upwards of 70% of children have normal developmental, neurologic,
and ophthalmologic findings at follow-up evaluations. Treatment for Bartonella infection Biopsy (PCR or culture)/
(cat-scratch disease) serology
1 year with pyrimethamine, a sulfonamide, and folinic acid is tolerated
Lymphoma Biopsy
with minimal toxicity (see “Treatment,” below).
Congenital infection Cytomegalovirus infection Viral culture/PCR
Ocular Infection Infection with T. gondii is estimated to Herpes simplex virus Viral culture/PCR
cause 35% of all cases of chorioretinitis in the United States and infection
Europe. It was formerly thought that the majority of cases of Rubella virus infection Serology
ocular disease were due to congenital infection. New ocular toxoplas- Syphilis Serology
mosis in immunocompetent individuals occurs more commonly than Listeriosis Bacterial culture
was previously appreciated and has been associated with outbreaks in Chorioretinitis in Tuberculosis Bacterial culture/PCR
Victoria (British Columbia) and in South America. A variety of ocular immunocompetent Syphilis Serology
manifestations are documented, including blurred vision, scotoma, individual
Histoplasmosis Serology/culture/
photophobia, and eye pain. Macular involvement occurs, with loss of antigen
central vision, and nystagmus is secondary to poor fixation. Involve- Chorioretinitis in Cytomegalovirus infection Viral culture/PCR
ment of the extraocular muscles may lead to disorders of convergence AIDS patient Syphilis Serology
and to strabismus. Ophthalmologic examination should be undertaken Herpes simplex virus Viral culture/PCR
in newborns with suspected congenital infection. As the inflammation infection
resolves, vision improves, but episodic flare-ups of chorioretinitis, Varicella-zoster virus Viral culture/PCR
which progressively destroy retinal tissue and lead to glaucoma, are infection
common. The ophthalmologic examination reveals yellow-white, Fungal infection Culture
cotton-like patches with indistinct margins of hyperemia. As the lesions CNS lesions in AIDS Lymphoma or metastatic Tissue biopsy
CHAPTER 223 Toxoplasma Infections
age, white plaques with distinct borders and black spots within the patient tumor
retinal pigment become more apparent. Lesions usually are located near Brain abscess Biopsy/culture
the posterior pole of the retina; they may be single but are more com-
Progressive multifocal PCR for JC virus
monly multiple. Congenital lesions may be unilateral or bilateral and leukoencephalopathy
show evidence of massive chorioretinal degeneration with extensive Fungal infection Biopsy/culture
fibrosis. Surrounding these areas of involvement are a normal retina
Mycobacterial infection Biopsy/culture/PCR
and vasculature. In patients with AIDS, retinal lesions are often large,
with diffuse retinal necrosis, and include both free tachyzoites and cysts Abbreviations: CNS, central nervous system; PCR, polymerase chain reaction.
containing bradyzoites. Toxoplasmic chorioretinitis may be a prodrome Source: Adapted from JD Schwartzman: Toxoplasmosis, in Principles and Practice
of Clinical Parasitology. Hoboken, Wiley, 2001.
to the development of encephalitis.
■ DIAGNOSIS detected as early as 2–3 weeks after infection. These titers usually peak at
Tissues and Body Fluids The differential diagnosis of acute 6–8 weeks and decline slowly to a new baseline level that persists for life.
toxoplasmosis can be made by appropriate culture, serologic testing, Antibody avidity increases with time and can be useful in difficult cases
and PCR (Table 223-1). Although performed only at specialized labo- during pregnancy for establishing when infection may have occurred.
ratories, the isolation of T. gondii from blood or other body fluids can The serum IgM titer should be measured in concert with the IgG titer to
be accomplished after subinoculation of the sample into the peritoneal better establish the time of infection; either the double-sandwich IgM-
cavity of mice. If no parasites are found in the mouse’s peritoneal ELISA or the IgM-immunosorbent assay (IgM-ISAGA) should be used.
fluid 6–10 days after inoculation, its anti-Toxoplasma serum titer can be Both assays are specific and sensitive, with fewer false-positive results
evaluated 4–6 weeks after inoculation. Isolation of T. gondii from the than other commercial tests. The double-sandwich IgA-ELISA is more
patient’s body fluids reflects acute infection, whereas isolation from sensitive than the IgM-ISAGA for detecting congenital infection in the
biopsied tissue is an indication only of the presence of tissue cysts fetus and newborn. Although a negative IgM result with a positive IgG
and should not be misinterpreted as evidence of acute toxoplasmosis. titer indicates distant infection, IgM can persist for >1 year and should
Persistent parasitemia in patients with latent, asymptomatic infection not necessarily be considered a reflection of acute disease. If acute tox-
is rare. Histologic examination of lymph nodes may suggest the char- oplasmosis is suspected, a more extensive panel of serologic tests can
acteristic changes described above. Demonstration of tachyzoites in be performed. In the United States, testing is available at the Toxoplasma
lymph nodes establishes the diagnosis of acute toxoplasmosis. Like Serology Laboratory at Palo Alto Medical Foundation (http://www.pamf.
subinoculation into mice, histologic demonstration of cysts containing org/serology/clinicianguide.html).
bradyzoites confirms prior infection with T. gondii but is nondiagnostic
for acute infection. Molecular Diagnostics Molecular approaches can directly
detect T. gondii in biologic samples independent of the serologic
Serology Because some diagnostic tests are available only at spe- response. Results obtained with PCR have suggested high sensitivity,
cialty laboratories and are technically challenging, serologic testing has specificity, and clinical utility in the diagnosis of TE, and PCR technol-
become the routine method of diagnosis. Diagnosis of acute infection ogy may be becoming more readily available in resource-poor settings.
with T. gondii can be established by detection of the simultaneous Real-time PCR is a promising technique that can provide quantitative
presence of IgG and IgM antibodies to Toxoplasma in serum. The pres- results. Isolates can be genotyped and polymorphic sequences can be
ence of circulating IgA favors the diagnosis of an acute infection. The obtained, with consequent identification of the precise strain. Molecu-
Sabin–Feldman dye test, the indirect fluorescent antibody test, and the lar epidemiologic studies with polymorphic markers have been useful
enzyme-linked immunosorbent assay (ELISA) all satisfactorily measure in correlating clinical signs and symptoms of disease with different
circulating IgG antibody to Toxoplasma. Positive IgG titers (>1:10) can be T. gondii genotypes.
Harrisons_20e_Part5_p0859-p1648.indd 1613 6/1/18 12:11 PM
1614 The Immunocompetent Adult or Child For the patient who Ocular Toxoplasmosis The serum antibody titer may not cor-
presents with lymphadenopathy only, a positive IgM titer is an indi- relate with the presence of active lesions in the fundus, particularly
cation of acute infection—and an indication for therapy, if clinically in cases of congenital toxoplasmosis. In general, a positive IgG titer
warranted (see “Treatment,” below). The serum IgM titer should be (measured in undiluted serum if necessary) in conjunction with typical
determined again in 3 weeks. An elevation in the IgG titer without an lesions establishes the diagnosis. If lesions are atypical and the serum
increase in the IgM titer suggests that infection is present but is not antibody titer is in the low-positive range, the diagnosis is presump-
acute. If there is a borderline increase in either IgG or IgM, the titers tive. The parasitic antigen–specific polyclonal IgG assay as well as
should be reassessed in 3–4 weeks. parasite-specific PCR may facilitate the diagnosis. Accordingly, the
clinical diagnosis of ocular toxoplasmosis can be supported in 60–90%
The Immunocompromised Host A presumptive clinical diag-
of cases by laboratory tests, depending on the time of anterior chamber
nosis of TE in patients with AIDS is based on clinical presentation,
puncture and the panel of antibody analyses used. In the remaining
history of exposure (as evidenced by positive serology), and radiologic
cases, the possibility of a falsely negative laboratory diagnosis or of an
evaluation. To detect latent infection with T. gondii, HIV-infected per-
incorrect clinical diagnosis cannot be clarified further.
sons should be tested for IgG antibody to Toxoplasma soon after HIV
infection is diagnosed. When these criteria are used, the predictive
value is as high as 80%. More than 97% of patients with AIDS and TREATMENT
toxoplasmosis have IgG antibody to T. gondii in serum. IgM serum
antibody usually is not detectable. Although IgG titers do not correlate Toxoplasmosis
with active infection, serologic evidence of infection virtually always
precedes the development of TE. It is therefore important to determine CONGENITAL INFECTION
the Toxoplasma antibody status of all patients infected with HIV. Anti- Congenitally infected neonates are treated with daily oral
body titers may range from negative to 1:1024 in patients with AIDS pyrimethamine (1 mg/kg) and sulfadiazine (100 mg/kg) along with
and TE. Fewer than 3% of patients have no demonstrable antibody to folinic acid for 1 year. Depending on the signs and symptoms, pred-
Toxoplasma at diagnosis of TE. nisone (1 mg/kg per day) may be used for congenital infection. Some
Patients with TE have focal or multifocal abnormalities demonstra- U.S. states and some countries routinely screen pregnant women
ble by CT or MRI. Neuroradiologic evaluation should include double- (France, Austria) and/or newborns (Denmark, Massachusetts).
dose contrast CT of the head. By this test, single and frequently multiple Management and treatment regimens vary with the country and
contrast-enhancing lesions (<2 cm) may be identified. MRI usually the treatment center. Most experts use spiramycin to treat pregnant
demonstrates multiple lesions located in both hemispheres, with the women who have acute toxoplasmosis early in pregnancy and use
basal ganglia and corticomedullary junction most commonly involved; pyrimethamine/sulfadiazine/folinic acid to treat women who sero-
PART 5
MRI provides a more sensitive evaluation of the efficacy of therapy convert after 18 weeks of pregnancy or in cases of documented fetal
than does CT (Fig. 223-2). These findings are not pathognomonic of infection. This treatment is somewhat controversial: clinical studies,
Toxoplasma infection, because 40% of CNS lymphomas are multifocal which have included few untreated women, have not proven the
and 50% are ring-enhancing. For both MRI and CT scans, the rate of efficacy of such therapy in preventing congenital toxoplasmosis.
Infectious Diseases
false-negative results is ~10%. The finding of a single lesion on an MRI However, studies do suggest that treatment during pregnancy
scan increases the likelihood of primary CNS lymphoma (in which sol- decreases the severity of infection. Many women who are infected
itary lesions are four times more likely than in TE) and strengthens the in the first trimester elect termination of pregnancy. Those who do
argument for the performance of a brain biopsy. A therapeutic trial of not terminate pregnancy are offered prenatal antibiotic therapy to
anti-Toxoplasma medications is frequently used to assess the diagnosis. reduce the frequency and severity of Toxoplasma infection in the
Treatment of presumptive TE with pyrimethamine plus sulfadiazine infant. The optimal duration of treatment for a child with asymp-
or clindamycin results in quantifiable clinical improvement in >50% of tomatic congenital toxoplasmosis is not clear, although most clini-
patients by day 3. Leucovorin is administered to prevent bone marrow cians in the United States would treat the child for 1 year in light
toxicity. By day 7, >90% of treated patients show evidence of improve- of cohort investigations conducted by the National Collaborative
ment. In contrast, if patients fail to respond or have lymphoma, clinical Chicago-Based Congenital Toxoplasmosis Study.
signs and symptoms worsen by day 7. Patients in this category require
INFECTION IN IMMUNOCOMPETENT PATIENTS
brain biopsy with or without a change in therapy. This procedure can
now be performed by a stereotactic CT-guided method that reduces Immunologically competent adults and older children who have
the potential for complications. Brain biopsy for T. gondii identifies only lymphadenopathy do not require specific therapy unless they
organisms in 50–75% of cases. PCR amplification of CSF may also con- have persistent, severe symptoms. Patients with ocular toxoplas-
firm toxoplasmosis or suggest alternative diagnoses (Table 223-1), such mosis are usually treated for 1 month with pyrimethamine plus
as progressive multifocal leukoencephalopathy (JC virus positive) or either sulfadiazine or clindamycin and sometimes with prednisone.
primary CNS lymphoma (Epstein-Barr virus positive). Treatment should be supervised by an ophthalmologist familiar
CT and MRI with contrast are currently the standard diagnostic with Toxoplasma disease. Ocular disease can be self-limited without
imaging tests for TE. As in other conditions, the radiologic response treatment, but therapy is typically considered for lesions that are
may lag behind the clinical response. Resolution of lesions may take severe or close to the fovea or optic disc. Prolonged treatment may
from 3 weeks to 6 months. Some patients show clinical improvement prevent recurrences of ocular toxoplasmosis, but whether treatment
despite worsening radiographic findings. improves long-term visual outcomes is unclear.
Congenital Infection The issue of concern when a pregnant INFECTION IN IMMUNOCOMPROMISED PATIENTS
woman has evidence of recent T. gondii infection is whether the fetus is Primary Prophylaxis Patients with AIDS should be treated for
infected. PCR analysis of the amniotic fluid for the B1 gene of T. gondii acute toxoplasmosis; in immunocompromised patients, toxoplas-
has replaced fetal blood sampling. Serologic diagnosis is based on the mosis is rapidly fatal if untreated. Despite their toxicity, the drugs
persistence of IgG antibody or a positive IgM titer after the first week of used to treat TE were required for survival prior to cART. The
life (a time frame that excludes placental leak). The IgG determination incidence of TE has declined as the survival of patients with HIV
should be repeated every 2 months. An increase in IgM beyond the infection has increased through the use of cART.
first week of life is indicative of acute infection. Up to 25% of infected In Africa, many patients are diagnosed with HIV infection
newborns may be seronegative and have normal routine physical only after developing opportunistic infections. Hence, the
examinations. Thus assessment of the eye and the brain, with ophthal- optimal management of these opportunistic infections is
mologic testing, CSF evaluation, and radiologic studies, is important in important if the benefits of subsequent cART are to be realized. The
establishing the diagnosis. incidence of TE in under-resourced settings is unknown because
Harrisons_20e_Part5_p0859-p1648.indd 1614 6/1/18 12:11 PM
serologic testing and imaging are not available. AIDS patients who meats. Patients need not be advised to part with their cats or to have 1615
are seropositive for T. gondii and who have a CD4+ T lymphocyte their cats tested for toxoplasmosis. Blood intended for transfusion into
count of <100/μL should receive prophylaxis against TE. Toxoplasma-seronegative immunocompromised individuals should be
Of the currently available agents, trimethoprim-sulfamethox- screened for antibody to T. gondii. Although such serologic screening
azole (TMP-SMX) appears to be an effective alternative for treatment is not routinely performed, seronegative women should be screened
of TE in resource-poor settings where the preferred combination of for evidence of infection several times during pregnancy if they are
pyrimethamine plus sulfadiazine is not available. The daily dose of exposed to environmental conditions that put them at risk for infection
TMP-SMX (one double-strength tablet) recommended for prophy- with T. gondii. HIV-positive individuals should adhere closely to these
laxis of PcP is effective against TE. If patients cannot tolerate TMP- preventive measures.
SMX, the recommended alternative is dapsone-pyrimethamine,
which likewise is effective against PcP. Atovaquone with or without ACKNOWLEDGMENT
pyrimethamine also can be considered. Prophylactic monotherapy The author would like to acknowledge Dr. Lloyd Kasper for his numerous
with dapsone, pyrimethamine, azithromycin, clarithromycin, or contributions to our understanding of the pathogenesis of toxoplasmosis and
aerosolized pentamidine is probably insufficient. AIDS patients who his essential role in preparation of this chapter for prior editions.
are seronegative for Toxoplasma and are not receiving prophylaxis for
PcP should be retested for IgG antibody to Toxoplasma if their CD4+ ■ FURTHER READING
T cell count drops to <100/μL. If seroconversion has taken place, Aleixo AL et al: Toxoplasmic retinochoroiditis: Clinical characteris-
then the patient should be given prophylaxis as described above. tics and visual outcome in a prospective study. PLoS Negl Trop Dis
10:e0004685, 2016.
Discontinuing Primary Prophylaxis Current studies indicate that Peyron F et al: Congenital toxoplasmosis in France and the
prophylaxis against TE can be discontinued in patients who have United States: One parasite, two diverging approaches. PLoS Negl
responded to cART and whose CD4+ T lymphocyte count has been Trop Dis 11:e0005222, 2017.
>200/μL for 3 months. Although patients with CD4+ T lymphocyte Wang ZD et al: Prevalence and burden of Toxoplasma gondii infection in
counts of <100/μL are at greatest risk for developing TE, the risk HIV-infected people: A systematic review and meta-analysis. Lancet
that this condition will develop when the count has increased to HIV 4:e177, 2017.
100–200/μL has not been established. Thus, prophylaxis should
be discontinued when the count has increased to >200/μL. Dis-
continuation of therapy reduces the pill burden; the potential for
drug toxicity, drug interaction, or selection of drug-resistant patho-
CHAPTER 224 Protozoal Intestinal Infections and Trichomoniasis
224 Protozoal
gens; and cost. Prophylaxis should be recommenced if the CD4+
T lymphocyte count again decreases to <100–200/μL. Intestinal
Individuals who have completed initial therapy for TE should
receive treatment indefinitely unless immune reconstitution, with
Infections and
a CD4+ T cell count of >200/μL, occurs as a consequence of cART. Trichomoniasis
Combination therapy with pyrimethamine plus sulfadiazine plus
leucovorin is effective for this purpose. An alternative to sulfadi- Peter F. Weller
azine in this regimen is clindamycin.
Discontinuing Secondary Prophylaxis (Long-Term Maintenance
Therapy) Patients receiving secondary prophylaxis for TE are at PROTOZOAL INFECTIONS
low risk for recurrence when they have completed initial therapy for
TE, remain asymptomatic, and have evidence of restored immune ■ GIARDIASIS
function. Individuals with HIV infection should have a CD4+ T Giardia intestinalis (also known as G. lamblia or G. duodenalis) is
lymphocyte count of >200/μL for at least 6 months after cART. a cosmopolitan protozoal parasite that inhabits the small
This recommendation is consistent with more extensive data indi- intestines of humans and other mammals. Giardiasis is one of
cating the safety of discontinuing secondary prophylaxis for other the most common parasitic diseases in both developed and developing
opportunistic infections during advanced HIV disease. A repeat countries worldwide, causing both endemic and epidemic intestinal
MRI brain scan is recommended. Secondary prophylaxis should be disease and diarrhea.
reintroduced if the CD4+ T lymphocyte count decreases to <200/μL. Life Cycle and Epidemiology (Fig. 224-1) Infection follows
the ingestion of environmentally hardy cysts, which excyst in the small
■ PREVENTION intestine, releasing flagellated trophozoites (Fig. 224-2) that multiply by
All HIV-infected persons should be counseled regarding sources of Tox- binary fission. Giardia remains a pathogen of the proximal small bowel
oplasma infection. The chances of primary infection with Toxoplasma can and does not disseminate hematogenously. Trophozoites remain free in
be reduced by not eating undercooked meat and by avoiding oocyst- the lumen or attach to the mucosal epithelium by means of a ventral
contaminated material (i.e., a cat’s litter box). Specifically, lamb, beef, sucking disk. As a trophozoite encounters altered conditions, it forms a
and pork should be cooked to an internal temperature of 165–170°F morphologically distinct cyst, which is the stage of the parasite usually
(74–77°C); from a more practical perspective, meat cooked until it is no found in the feces. Trophozoites may be present and even predominate
longer pink inside usually satisfies this requirement. Hands should be in loose or watery stools, but it is the resistant cyst that survives outside
washed thoroughly after work in the garden, and all fruits and vege- the body and is responsible for transmission. Cysts do not tolerate heat-
tables should be washed. Ingestion of raw shellfish is a risk factor for ing or desiccation, but they do remain viable for months in cold fresh
toxoplasmosis, given that the filter-feeding mechanism of clams and water. The number of cysts excreted varies widely but can approach
mussels concentrates oocysts. 107 per gram of stool.
If the patient owns a cat, the litter box should be cleaned or changed Ingestion of as few as 10 cysts is sufficient to cause infection in
daily, preferably by an HIV-negative, nonpregnant person; alterna- humans. Because cysts are infectious when excreted, person-to-person
tively, patients should wash their hands thoroughly after changing the transmission occurs where fecal hygiene is poor. Giardiasis is especially
litter box. Litter boxes should be changed daily if possible, as freshly prevalent in day-care centers; person-to-person spread also takes place
excreted oocysts will not have sporulated and will not be infectious. in other institutional settings with poor fecal hygiene and during anal–
Patients should be encouraged to keep their cats inside and not to oral contact. If food is contaminated with Giardia cysts after cooking or
adopt or handle stray cats. Cats should be fed only canned or dried preparation, food-borne transmission can occur. Waterborne transmis-
commercial food or well-cooked table food, not raw or undercooked sion accounts for episodic infections (e.g., in campers and travelers)
Harrisons_20e_Part5_p0859-p1648.indd 1615 6/1/18 12:11 PM
You might also like
- Infections in Cancer Chemotherapy: A Symposium Held at the Institute Jules Bordet, Brussels, BelgiumFrom EverandInfections in Cancer Chemotherapy: A Symposium Held at the Institute Jules Bordet, Brussels, BelgiumNo ratings yet
- 131 - StiDocument16 pages131 - Sti4g8psyr2qfNo ratings yet
- Fast Facts: Complex Perianal Fistulas in Crohn's Disease: A multidisciplinary approach to a clinical challengeFrom EverandFast Facts: Complex Perianal Fistulas in Crohn's Disease: A multidisciplinary approach to a clinical challengeNo ratings yet
- AsedrffgvChapter QwescDocument16 pagesAsedrffgvChapter Qwesch68wqhk9nnNo ratings yet
- Sexually Transmitted Diseases: Vaccines, Prevention, and ControlFrom EverandSexually Transmitted Diseases: Vaccines, Prevention, and ControlRating: 5 out of 5 stars5/5 (19)
- Nonantibiotic Prevention andDocument27 pagesNonantibiotic Prevention andGheorghe SecuNo ratings yet
- Urinary Tract Infections Guide for Diagnosis and TreatmentDocument22 pagesUrinary Tract Infections Guide for Diagnosis and TreatmentpupuayuwandiraNo ratings yet
- Gonorrhea: Treatment Update For An Increasingly Resistant OrganismDocument8 pagesGonorrhea: Treatment Update For An Increasingly Resistant OrganismRadhiatul AdillahNo ratings yet
- Reviews: Epidemiology, Definition and Treatment of Complicated Urinary Tract InfectionsDocument15 pagesReviews: Epidemiology, Definition and Treatment of Complicated Urinary Tract InfectionsPutu AdiNo ratings yet
- 10.1515 - Labmed 2021 0085Document13 pages10.1515 - Labmed 2021 0085Tony ZhangNo ratings yet
- Pharmacotherapeutic Advances For Recurrent Urinary Tract Infections in WomenDocument16 pagesPharmacotherapeutic Advances For Recurrent Urinary Tract Infections in Womentravel doctorNo ratings yet
- Tandogdu 2016Document6 pagesTandogdu 2016Elena CuibanNo ratings yet
- 546-Texto Del Artículo-2262-1-10-20200124Document14 pages546-Texto Del Artículo-2262-1-10-20200124Paul Coacalla JuaresNo ratings yet
- Uti - HarriDocument9 pagesUti - HarrilololoNo ratings yet
- Manajemen UTI Pada ElderlyDocument4 pagesManajemen UTI Pada ElderlyTrismi IstianaNo ratings yet
- 1 s2.0 S1569905616300495 MainDocument7 pages1 s2.0 S1569905616300495 MainCris FischerNo ratings yet
- IVU AdultosDocument16 pagesIVU AdultosJorge Luis German BecerraNo ratings yet
- The Challenge of Urinary Tract Infections in Renal Transplant RecipientsDocument14 pagesThe Challenge of Urinary Tract Infections in Renal Transplant RecipientsdevinaNo ratings yet
- Infeccion Tracto UrinarioDocument16 pagesInfeccion Tracto UrinarioGloria Milena VeraNo ratings yet
- Hematology 2013Document5 pagesHematology 2013Jonathanj RomerorNo ratings yet
- Guía de Práctica Clínica Europea ITUDocument7 pagesGuía de Práctica Clínica Europea ITUVICTORIA GONZALEZ VEGANo ratings yet
- 11 - Recurrent UTI TOG 2020Document7 pages11 - Recurrent UTI TOG 2020Anna JuniedNo ratings yet
- Management of Urinary Tract Infection in Women A Practical Approach For Everyday PracticeDocument23 pagesManagement of Urinary Tract Infection in Women A Practical Approach For Everyday PracticeKeysha AbigailNo ratings yet
- Infectious Spondylodiscitis Diagnosis and TreatmentDocument12 pagesInfectious Spondylodiscitis Diagnosis and TreatmentRoxana StanciuNo ratings yet
- Systematic Review: Tuberculous Peritonitis - Presenting Features, Diagnostic Strategies and TreatmentDocument16 pagesSystematic Review: Tuberculous Peritonitis - Presenting Features, Diagnostic Strategies and TreatmenthendraNo ratings yet
- Management of The Urologic Sepsis SyndromeDocument10 pagesManagement of The Urologic Sepsis SyndromeNur Syamsiah MNo ratings yet
- Ets SexualDocument18 pagesEts SexualwilliamNo ratings yet
- Contents IdcDocument3 pagesContents IdcJono TurnerNo ratings yet
- Urethritis in FemaleDocument7 pagesUrethritis in FemaleRika SuryanaNo ratings yet
- Hepatitis CDocument12 pagesHepatitis CCristian Giraldo GuzmànNo ratings yet
- IVU in The ClinicDocument16 pagesIVU in The ClinicDaniela LSNo ratings yet
- proktitisDocument13 pagesproktitisRENTI NOVITANo ratings yet
- Case Study HIV With DiarrheaDocument29 pagesCase Study HIV With DiarrheaMatin Ahmad Khan100% (1)
- Urinary Tract Infection in Patients With Diabetes MellitusDocument10 pagesUrinary Tract Infection in Patients With Diabetes MellitusMistic 1948No ratings yet
- Uti PDFDocument10 pagesUti PDFmahmoud EltoukhyNo ratings yet
- Approach To Urinary Tract InfectionsDocument17 pagesApproach To Urinary Tract InfectionsManusama HasanNo ratings yet
- Gyne - (Section B) PID-STI-1Document45 pagesGyne - (Section B) PID-STI-1Kailash KhatriNo ratings yet
- GetahunLTBINEJM2015 PDFDocument9 pagesGetahunLTBINEJM2015 PDFSharah Stephanie IINo ratings yet
- tmp5D6 TMPDocument2 pagestmp5D6 TMPFrontiersNo ratings yet
- Bmjopen 2016 015233Document7 pagesBmjopen 2016 015233SEPTIANA SAPUTRINo ratings yet
- HHS Public Access: Urinary Tract Infections and Asymptomatic Bacteriuria in Older AdultsDocument18 pagesHHS Public Access: Urinary Tract Infections and Asymptomatic Bacteriuria in Older AdultsichaNo ratings yet
- Uti and Asymptomatic BacteriuriaDocument18 pagesUti and Asymptomatic Bacteriurianabella cholidatunNo ratings yet
- Special Considerations of Antibiotic Prescription in The Geriatric PopulationDocument7 pagesSpecial Considerations of Antibiotic Prescription in The Geriatric PopulationLydiaphNo ratings yet
- Gonorrhea Infection in Women: Prevalence, Effects, Screening, and ManagementDocument14 pagesGonorrhea Infection in Women: Prevalence, Effects, Screening, and ManagementMaulana MalikibrahimNo ratings yet
- Evaluation and Management UTI in Emergency-1-10Document10 pagesEvaluation and Management UTI in Emergency-1-10Ade PrawiraNo ratings yet
- Acog Practice BulletinDocument10 pagesAcog Practice BulletinCristian AranibarNo ratings yet
- Mycoplasma genitalium infections guidelinesDocument14 pagesMycoplasma genitalium infections guidelinesfaridahakimlNo ratings yet
- Abstract: Gonorrhea Is A Set of Clinical Conditions Resulting From Infection WithDocument5 pagesAbstract: Gonorrhea Is A Set of Clinical Conditions Resulting From Infection WithLaili Firda RusdianaNo ratings yet
- Management of Vaginal Discharge Syndrome: How Effective Is Our Strategy?Document4 pagesManagement of Vaginal Discharge Syndrome: How Effective Is Our Strategy?Epi PanjaitanNo ratings yet
- workowski2015Document4 pagesworkowski2015Sharif KavumaNo ratings yet
- 2920 2925 D Mannose A Promising Support For Acute Urinary Tract Infections in Women. A Pilot StudyDocument6 pages2920 2925 D Mannose A Promising Support For Acute Urinary Tract Infections in Women. A Pilot StudyRafaela FriasNo ratings yet
- Prevalence of UTIs Among Female HostellersDocument17 pagesPrevalence of UTIs Among Female HostellerspromiseNo ratings yet
- Bader2 PDFDocument10 pagesBader2 PDFMuhammad YousufNo ratings yet
- Bacteriuria in Individuals Who Become Delirious: CommentaryDocument3 pagesBacteriuria in Individuals Who Become Delirious: CommentaryGabreilla HanochNo ratings yet
- Seminar: Joana Torres, Saurabh Mehandru, Jean-Frédéric Colombel, Laurent Peyrin-BirouletDocument15 pagesSeminar: Joana Torres, Saurabh Mehandru, Jean-Frédéric Colombel, Laurent Peyrin-BirouletKaren ojedaNo ratings yet
- Nejmra1315399invasive Candidiasisoct8-2015Document12 pagesNejmra1315399invasive Candidiasisoct8-2015kendyNo ratings yet
- Ascitits BKDocument16 pagesAscitits BKAjengNo ratings yet
- Fungal Infections in The IcuDocument23 pagesFungal Infections in The IcuVemuri SrinivasNo ratings yet
- Clinical Presentations and Epidemiology of Urinary Tract InfectionsDocument11 pagesClinical Presentations and Epidemiology of Urinary Tract InfectionsdimasNo ratings yet
- Aetiology and Frequency of Cervico-Vaginal Infections Among Mexican WomenDocument8 pagesAetiology and Frequency of Cervico-Vaginal Infections Among Mexican WomenMiriam SuarezNo ratings yet
- Preoperative Evaluation and PreparationDocument7 pagesPreoperative Evaluation and PreparationJolaine ValloNo ratings yet
- February 2024 NewsletterDocument1 pageFebruary 2024 NewsletterJolaine ValloNo ratings yet
- Pathoma RuntimesDocument6 pagesPathoma RuntimesaloverofdanceNo ratings yet
- PhysicianDocument204 pagesPhysicianTrisNo ratings yet
- (ANES) Fri Asynchronous - Discussion - Principles of Palliative Care and End of Life CareDocument8 pages(ANES) Fri Asynchronous - Discussion - Principles of Palliative Care and End of Life CareJolaine ValloNo ratings yet
- CL Psychiatry Case Vignettes, 2022: July 1Document2 pagesCL Psychiatry Case Vignettes, 2022: July 1Jolaine ValloNo ratings yet
- (GYN) 05 Pelvic PainDocument5 pages(GYN) 05 Pelvic PainJolaine ValloNo ratings yet
- (ANES) Fri Asynchronous Discussion - Basic Principles of Palliative Care and End of Life Care (Group 3) 10-23-2020Document12 pages(ANES) Fri Asynchronous Discussion - Basic Principles of Palliative Care and End of Life Care (Group 3) 10-23-2020Jolaine ValloNo ratings yet
- Structure-Function Correlation of Juxtapapillary Choroidal Thickness With Visual Field Analysis of Patients Suspected With GlaucomaDocument9 pagesStructure-Function Correlation of Juxtapapillary Choroidal Thickness With Visual Field Analysis of Patients Suspected With GlaucomaJolaine ValloNo ratings yet
- (DERMA) 01 Introduction To Dermatology (History and PE)Document8 pages(DERMA) 01 Introduction To Dermatology (History and PE)Jolaine ValloNo ratings yet
- Effect of Internet-Based Vs Face-to-Face Cognitive Behavioral Therapy For Adults With Obsessive-Compulsive Disorder A Randomized Clinical TrialDocument15 pagesEffect of Internet-Based Vs Face-to-Face Cognitive Behavioral Therapy For Adults With Obsessive-Compulsive Disorder A Randomized Clinical TrialJolaine ValloNo ratings yet
- Effects of Music As An Adjunctive Therapy On Severity of Symptoms in Patients With Obsessive-Compulsive Disorder: Randomized Controlled TrialDocument15 pagesEffects of Music As An Adjunctive Therapy On Severity of Symptoms in Patients With Obsessive-Compulsive Disorder: Randomized Controlled TrialJolaine ValloNo ratings yet
- RhythmsDocument59 pagesRhythmsJolaine ValloNo ratings yet
- Student Guide Clerkship Revised AY2021-2022 Sept - OctDocument12 pagesStudent Guide Clerkship Revised AY2021-2022 Sept - OctJolaine ValloNo ratings yet
- Advocacy Proposal - Group 3-3Document6 pagesAdvocacy Proposal - Group 3-3Jolaine ValloNo ratings yet
- (DERMA) 06 Asymptomatic Skin Colored PapulesDocument12 pages(DERMA) 06 Asymptomatic Skin Colored PapulesJolaine ValloNo ratings yet
- (DERMA) 03 TineasDocument9 pages(DERMA) 03 TineasJolaine ValloNo ratings yet
- Data Management MCCODDocument48 pagesData Management MCCODJolaine ValloNo ratings yet
- Derma Quiz 5 NotesDocument6 pagesDerma Quiz 5 NotesJolaine ValloNo ratings yet
- Rheuma Prestests CompiledDocument13 pagesRheuma Prestests CompiledJolaine ValloNo ratings yet
- Med-Rheuma-Patient Write Up - Valeriano and ValloDocument10 pagesMed-Rheuma-Patient Write Up - Valeriano and ValloJolaine ValloNo ratings yet
- Pgi To Do List: As of October 22, 2020 - Please Do Steps 1-3:)Document2 pagesPgi To Do List: As of October 22, 2020 - Please Do Steps 1-3:)Jolaine ValloNo ratings yet
- Hema Pretests CompiledDocument6 pagesHema Pretests CompiledJolaine ValloNo ratings yet
- Onco Pretests CompiledDocument6 pagesOnco Pretests CompiledJolaine ValloNo ratings yet
- 12 Clin Path Exocrine and Endocrine Functions of The PancreasDocument13 pages12 Clin Path Exocrine and Endocrine Functions of The PancreasJolaine ValloNo ratings yet
- Data Management 'Birth Certificate'Document22 pagesData Management 'Birth Certificate'Jolaine Vallo100% (1)
- Gi Pretests CompiledDocument7 pagesGi Pretests CompiledJolaine ValloNo ratings yet
- D2 Grp1 CLIN PATH Case Discussion 1Document11 pagesD2 Grp1 CLIN PATH Case Discussion 1Jolaine ValloNo ratings yet
- 03 C2022 ClinPath 1.03 Hemostasis and ThrombosisDocument7 pages03 C2022 ClinPath 1.03 Hemostasis and ThrombosisJolaine ValloNo ratings yet
- 01 CLIN PTH S01 T01 Red Blood Cell DisordersDocument8 pages01 CLIN PTH S01 T01 Red Blood Cell DisordersJolaine ValloNo ratings yet
- Inbound 6622251263463521221Document2 pagesInbound 6622251263463521221Haji Ehsan Ullah EhsanNo ratings yet
- Immunohematology Handouts UpdatedDocument15 pagesImmunohematology Handouts UpdateddmclmllNo ratings yet
- BIONAIDDocument16 pagesBIONAIDAnonymous Wie6lbepNo ratings yet
- Pertussis (Whooping Cough) : University of BuroaDocument42 pagesPertussis (Whooping Cough) : University of BuroaMumin Alamin AllaminNo ratings yet
- Package Insert Leaflet HbsAg Abbott QuantitativeDocument7 pagesPackage Insert Leaflet HbsAg Abbott QuantitativeirdinamarchsyaNo ratings yet
- Care, Compassion, Excellence Mount Lockyer Primary School A Place To Learn and GrowDocument4 pagesCare, Compassion, Excellence Mount Lockyer Primary School A Place To Learn and GrowMountLockyerNo ratings yet
- BT102-Microbiology Current Paper Solved Question Final Term February 2020Document11 pagesBT102-Microbiology Current Paper Solved Question Final Term February 2020Awais Bhutta100% (1)
- 79 Elisa Automation Application Ebook FINALDocument35 pages79 Elisa Automation Application Ebook FINALbotond77No ratings yet
- Artikel JurnalDocument10 pagesArtikel JurnalUmmuNo ratings yet
- Operator Loadout for Arid EnvironmentsDocument11 pagesOperator Loadout for Arid EnvironmentsJustus WeißeNo ratings yet
- Introduction To BiotechnologyDocument335 pagesIntroduction To BiotechnologySamson TizazuNo ratings yet
- NVI Product Catalog 4 1Document40 pagesNVI Product Catalog 4 1Ayele Bizuneh100% (4)
- SchistosomiasisDocument33 pagesSchistosomiasishendra ari100% (1)
- Hepatitis BDocument12 pagesHepatitis BEmicar TecNo ratings yet
- Jurnal Pencegahan KecacinganDocument5 pagesJurnal Pencegahan KecacinganBinterBarapadangNo ratings yet
- Lecture 2Document3 pagesLecture 2Athena Thessa van VlotenNo ratings yet
- Ampiginosa 1Document5 pagesAmpiginosa 1Juan BianchiNo ratings yet
- Myocarditis NEJM 2022Document13 pagesMyocarditis NEJM 2022Πάνος ΣταγήςNo ratings yet
- Corp Other 005024 2 LIAISON CLIA Family Collection Menu LowDocument2 pagesCorp Other 005024 2 LIAISON CLIA Family Collection Menu LowYaser MNo ratings yet
- Measles (Case Presentation)Document19 pagesMeasles (Case Presentation)Zam Pamate100% (3)
- Stefan Hall - Fast Chicken Pox Cure EbookDocument29 pagesStefan Hall - Fast Chicken Pox Cure Ebookjijimin130% (1)
- New Case - Firza Humaira RespiDocument21 pagesNew Case - Firza Humaira RespiHardiyanti HermanNo ratings yet
- Result: Call Center: 01756963308Document2 pagesResult: Call Center: 01756963308Activity ManagerNo ratings yet
- Herpes Simplex Genitalia: Pante, Jaselle Paronable, Ana MurielDocument18 pagesHerpes Simplex Genitalia: Pante, Jaselle Paronable, Ana MurielThea MallariNo ratings yet
- Inflammation and WOund HealingDocument122 pagesInflammation and WOund HealingDeb SNo ratings yet
- CDC - Overuse of Antibiotics Is Killing AmericansDocument4 pagesCDC - Overuse of Antibiotics Is Killing AmericansjohntandraNo ratings yet
- What Is LeptospirosisDocument9 pagesWhat Is LeptospirosisRotessa Joyce Diaz OngNo ratings yet
- PCV 13Document2 pagesPCV 13api-237098034No ratings yet
- Mkpdp1035 : Name Lab No. Refby: Gender: Report Status Collected Mkpdp1035 Male DR - Veena BoraDocument2 pagesMkpdp1035 : Name Lab No. Refby: Gender: Report Status Collected Mkpdp1035 Male DR - Veena Borachetan bhagatNo ratings yet
- Limfadenopati LimfadenitisDocument45 pagesLimfadenopati LimfadenitisM Fiqih ArrachmanNo ratings yet
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (402)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (13)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 3.5 out of 5 stars3.5/5 (2)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (78)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo ratings yet
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- Techniques Exercises And Tricks For Memory ImprovementFrom EverandTechniques Exercises And Tricks For Memory ImprovementRating: 4.5 out of 5 stars4.5/5 (40)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 5 out of 5 stars5/5 (4)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (41)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingFrom EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingRating: 5 out of 5 stars5/5 (5)
- The Ultimate Guide To Memory Improvement TechniquesFrom EverandThe Ultimate Guide To Memory Improvement TechniquesRating: 5 out of 5 stars5/5 (34)
- The Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsFrom EverandThe Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsNo ratings yet
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingFrom EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingRating: 3.5 out of 5 stars3.5/5 (33)
- The Happiness Trap: How to Stop Struggling and Start LivingFrom EverandThe Happiness Trap: How to Stop Struggling and Start LivingRating: 4 out of 5 stars4/5 (1)
- The Tennis Partner: A Doctor's Story of Friendship and LossFrom EverandThe Tennis Partner: A Doctor's Story of Friendship and LossRating: 4.5 out of 5 stars4.5/5 (4)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (44)