Professional Documents
Culture Documents
Osce: Internal Medicine 1. JVP Measurement: © FAAS 3A, 2018
Uploaded by
PatOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Osce: Internal Medicine 1. JVP Measurement: © FAAS 3A, 2018
Uploaded by
PatCopyright:
Available Formats
OSCE: INTERNAL MEDICINE
1. JVP measurement
Raise the head 30°
Turn the patient’s head slightly away from the side you are inspecting
Use tangential lighting
Identify the external jugular vein, then find the internal jugular pulsations
Look for oscillation point of internal jugular venous pulsations in the lower half of the neck
Identify highest point of the pulsation
Extend a long rectangular object horizontally from this point and a ruler vertically from the sternal angle
Measure the vertical distance
Normal: ≤ 3cm from the sternal angle (< 3-4 cm)
High JVP: Right-sided heart failure, constrictive pericarditis, tricuspid stenosis, SVC obsruction
Low JVP: Dehydration, gastrointestinal bleeding
The following features help to distinguish jugular from carotid artery pulsations:
Internal Jugular Pulsations Carotid Pulsations
Rarely palpable Palpable
Soft, rapid, undulating quality, usually A more vigorous thrust with a single
with two elevations and two troughs outward component
per heart beat
Pulsations eliminated by light pressure Pulsations not eliminated by this pressure
on the vein(s) just above the sternal
end of the clavicle
Level of the pulsations changes with Level of the pulsations unchanged by
position, dropping as the patient position
becomes more upright.
Level of the pulsations usually descends Level of the pulsations not affected by
with inspiration. inspiration
2. Blood pressure taking
Center inflatable bladder over the brachial artery. Lower border of the cuff should be 2.5 cm above the
antecubital crease. Position the patient’s arm so that it is slightly flexed at the elbow.
To determine how high to raise the cuff pressure, first estimate the systolic pressure by palpation. As you
feel the radial artery with the fingers of one hand, rapidly inflate the cuff until radial pressure disappears.
Read this pressure on the manometer and add 30 mmHg to it.
Deflate the cuff promptly
Place the bell of a stethoscope lightly over the brachial artery, taking care to make an air seal with its full
rim
Inflate the cuff rapidly again to the level just determined, and then deflate it slowly, at a rate of 2-3 mmHg
per second. Note the level at which you hear the sounds of at least two consecutive beats. This is the
systolic pressure
Continue to lower the pressure slowly. The disappearance point, usually only a few mmHg below the
muffling point, is the best estimate of diastolic pressure
Read both the systolic and diastolic levels to the nearest 2mmHg.
Take blood pressure in both arms atleast once
Blood pressure classification
Systolic (mmHg) Diastolic (mmHg)
Normal < 120 < 80
Prehypertension 120-139 80-89
Stage 1, hypertension 140-159 90-99
Stage 2, hypertension ≥ 160 ≥ 100
Isolated systolic hypertension ≥ 140 < 90
© FAAS 3A, 2018
3. Shifting dullness
Patient on supine
Map the border between areas of tympany and dullness
Percuss from the center outwards
Ask patient to turn on one side, noting borders
No ascites: Borders stay constant between supine and lateral decubitus position
With ascites: Dullness shifts to the more dependent side while tympany shifts to the top
4. Fluid wave test
Press the edges firmly down of the midline of the abdomen, which helps to stop transmission of wave
through fat
Tap one flank with finger tips, feel on the opposite flank for an impulse transmitted through the fluid
Medical conditions associated with ascites:
Kidney failure
Liver cirrhosis
Congestive heart failure
Pleuritis
Colon cancer
Lung cancer
Non-hodgkin’s lymphoma
Ovarian cancer
Pancreatic cancer
Stomach cancer
5. Murphy’s test (for cholecystitis)
Hook left thumb or fingers of right hand under the costal margin at the point where the lateral border of
rectus muscle inserts
Ask patient to take a deep breath
Positive test: sharp increase in tenderness with sudden stop in inspiratory effort
In cholecystitis, the gallbladder becomes inflamed secondary to blockage of the cystic duct, usually by a
gallstone.1,3,4 Subsequently, this inflammation causes the release of prostaglandins, which cause more
inflammation of the gallbladder.1 Patients with acute cholecystitis experience discomfort with the Murphy’s sign
maneuver because the inflamed gallbladder descends toward the examiner’s fingers, which irritates the
peritoneum, thereby causing pain.9 Abdominal examination often elicits voluntary and involuntary guarding in
these patients.
6. Complete CNS exam
Level of consciousness
Alert Patient is awake and aware of self and environment. When spoken to a normal voice, patient
looks at you and responds fully and appropriately to stimuli
Lethargy When spoken to in a loud voice, patient appears drowsy but opens eyes and looks at you,
responds to questions and then falls asleep
Obtundation When shaken gently, patient opens eyes and looks at you but responds slowly and is somewhat
confused. Alertness and interest in environment are decreased
Stupor Patient arouses from sleep only after painful stimuli. Verbal responses are slow or absent. Patient
lapses into unresponsiveness when stimulus stops. Patient has minimal awareness of self or
environment
Coma Despite repeated painful stimuli, patient remains unarousable with eyes closed. No eviden
response to inner need or external stimuli is shown
© FAAS 3A, 2018
Cranial nerves and functions
Cranial nerve Function
I Olfactory Sense of smell
II Optic Vision
III Oculomotor Pupillary constriction, opening of the eye (lid elevation), most EOM movements
IV Trochlear Downward, internal rotation of the eye
V Trigeminal Motor: temporal and masseter muscles (jaw clenching), lateral pterygoid (lateral jaw
movement)
Sensory: facial – 3 divisions (ophthalmic, maxillary, mandibular)
VI Abducens Lateral deviation of the eye
VII Facial Motor: facial movements, facial expression, closing the eye, closing the mouth
Sensory: taste on anterior two third of the tongue
VIII Acoustic Hearing (cochlear division), balance (vestibular division)
IX Glossoharyngeal Motor: Pharynx
Sensory: posterior portion of the eardrum and ear canal, pharynx, posterior tongue
X Vagus Motor: palate, pharynx, larynx
Sensory: pharynx, larynx
XI Spinal accessory Sternocleidomastoid, upper portion of trapezius
XII Hypoglossal Tongue
Cranial Test Elicitation Abnormality
nerve
I Sense of smell on each Let the patient smell a coffee bean/ perfume Frontal lobe lesion
side one nostril at a time
II Visual acuity, visual fields, Visual acuity: Using snellen/ jeager chart Blindness; Hemianopsia; tonic
pupillary reaction to light, Visual field: Confrontation test pupils, Horner’s syndrome;
optic disc Pupillary reaction: Direct and consensual Papilledema, optic atrophy
pupillary light reflex
Optic disc: Use of ophtalmoscope
III, IV, VI Extraocular movements Let the patient look and follow an object (i.e Strabismus, nystagmus,
pen or finger) in an H pattern (areas of gaze intranuclear opthalmoplegia
– up, down, left, right)
V Sensory: pain and light Sensory: Using a blunt object (tip of the Motor or sensory lesions of CN
touch on the face reflex hammer), touch patient’s face (lateral V or its higher motor pahways
(ophthalmic, maxillary, to the eyes, cheeks and mandible)
mandibular zones) Motor: let the patient clench the teeth and
Motor: feel for contractions feel for the contractions of the temporal and
of temporal and masseter masseter muscles
muscles; corneal reflex
VII Make faces Raise both eyebrows, frown, close eyes Weakness from lesion of
tightly, show teeth, smile and puff out cheeks peripheral nerves or of CNS
(Bell’s palsy, stroke)
VIII Assess hearing of Weber test: using a tuning fork, vibrate and Sensoryneural loss: AC > BC
whispered voice. If put it on the forehead Conductive loss: BC > AC
decreased, test for: Rinne test: Using a tuning fork, vibrate and
Leteralization – Weber test put near the patient’s ear and when the
Conduction – Rinne test patient does not hear anymore sound put the
tuning fork on the base of the mastoid bone
IX, X Observe any difficulty of Gag reflex: using a tongue depressor, put it Weakened palate or pharynx;
swallowing; listen to voice; inside the patient’s mouth touching the Hoarseness, nasality; Palatal
watch soft palate rise with posterior pharynx paralysis in CVA
―ah‖; test gag reflex on
each side
XI Trapezius: Assess for bulk, Trapezius: Put your hands on the patient’s Atrophy, fasciculations,
involuntary movements and shoulders and ask patient to raise both weakness
strength of shoulder shrug shoulder against your hands Weakness of SCM when head
Sternocleidomastoid: Sternocleidomastoid: Put your hand on the turns to opposite side
assess strength as head patient’s face and ask patient to move face
turns against your hand against your hand
XII Listen to patient’s Let the patient protrude his tongue Dysarthria; atrophy, fasciculation
articulation; inspect resting (ALS, polio); deviation to weak
tongue; inspect the side in contralateral CVA
protruded tongue
© FAAS 3A, 2018
Motor
Body position – observe the patient’s body position during movement and at rest.
Involuntary movements – if present observe location, quality, rate, rhythm, amplitude, setting
Muscle bulk and tone – inspect muscle contours; assess resistance to passive stretch of arms and legs
Muscle strength – test and grade the major muscle groups, with the examiner providing resistance
Grading Muscle Strength
0 No muscular contraction detected
1 A barely detectable trace of contraction
2 Active movement with gravity eliminated
3 Active movement against gravity
4 Active movement against gravity and some resistance
5 Active movement against full resistance (normal)
Coordination
Check rapid alternating movement in arms and legs: clumsy, slow movements in cerebellar disease
Point-to-point movements:
Gait: ask patient to walk away, turn and come back; walk heel to toe; walk on toes then on heels; hop in
place
Stance: Romerg test – ask patient to stand with feet together and eyes open, then closed for 20-30
seconds, (+) loss of balance when eyes are closed; Pronator drift – ask patient to hold arms forward, with
eyes closed for 20-30 seconds, (+) flexion and pronation at elbow and downward drift
Sensory
Pain: use the sharp end of a pin
Temperature: use test tubes with hot and cold water
Light touch: use fine wisp of cotton
Vibration and position sense
Reflexes
Reflex Elicitation Normal Response
Biceps (C5, C6) The forearm should be supported, either resting on the patient's thighs Flexion of forearm at the elbow
or resting on the forearm of the examiner. The arm is midway between
flexion and extension. Place your thumb firmly over the biceps tendon,
with your fingers curling around the elbow, and tap briskly.
Triceps (C6, C7) Support the patient's forearm by cradling it with yours or by placing it Extension of forearm
on the thigh, with the arm midway between flexion and extension.
Identify the triceps tendon at its insertion on the olecranon, and tap
just above the insertion.
Supinator
(brachioradialis) The patient's arm should be supported. Identify the brachioradialis Brachioradialis reflex: flexion and
(C5, C6) tendon at the wrist. It inserts at the base of the styloid process of the supination of the forearm.
radius, usually about 1 cm lateral to the radial artery. If in doubt, ask
the patient to hold the arm as if in a sling—flexed at the elbow and Biceps reflex: flexion of the forearm. You
halfway between pronation and supination—and then flex the forearm will feel the biceps tendon contract if the
at the elbow against resistance from you. The brachioradialis and its biceps reflex is stimulated by the tap on the
tendon will then stand out. brachioradialis tendon.
Place the thumb of the hand supporting the patient's elbow on the
biceps tendon while tapping the brachioradialis tendon with the other Finger jerk: flexion of the fingers.
hand.
Knee L2, L3, L4) Let the knees swing free by the side of the bed, and place one hand Knee jerk
on the quadriceps so you can feel its contraction. If the patient is in
bed, slightly flex the knee by placing your forearm under both knees
by contraction of the quadriceps with extension of the lower leg
Ankle (S1) With the patient sitting, place one hand underneath the sole and Ankle jerk
dorsiflex the foot slightly. Then tap on the Achilles tendon just above
its insertion on the calcaneus. If the patient is in bed, flex the knee and
invert or evert the foot somewhat, cradling the foot and lower leg in
your arm. Then tap on the tendon
Abdominal reflex Stroke the skin of the abdomen around the umbilicus Brisk contraction of abdominal muscles in
(T8-T12) which the umbilicus moves toward the site
of the stimulus
Plantar response Stroke the skin on the lateral edge of the sole of the foot, starting at Flexion of all the toes
(L5, S1) the heel advancing to the ball of the foot then continuing medially to
the base of the great toe
Anal reflex With a dull object, stroke outward from anus in four quadrants Anal contraction
© FAAS 3A, 2018
Grading of reflexes
4+ Hyperactive
3+ Brisker than average, not necessarily abnormal
2+ Average, normal
1+ Diminished, low normal
0 No response
Meningeal signs
Brudzinski’s sign: with patient supine, flex head and neck toward chest. Note resistance or pain and
watch for flexion of hips and knees
- Meningeal irritation in the subaracnoid space may cause resistance or pain on flexion during both
maneuvers
Kernig’s sign: Flex one of patient’s legs at hip and knee, then straighten knee
- A compressed lumbosacral nerve root also causes pain on straightening the knee of the raised leg
7. Percussion and auscultation of Chest
o Respiratory
Percussion
Hyperextend middle finger of left hand (pleximeter)
Press the interphalangeal joint firmly in chest surface
Partially extend wrist with middle finger partially flexed and relaxed
Strike the dital interphalangeal joint of the pleximeter finger with the right middle finger
Withdraw the striking finger quickly to avoid damping the vibrations created
Normal: resonant (Pathologic: chronic bronchitis, early left-sided heart failure)
Fluid filled: Dull (i.e. pneumonia, atelectasis, pleural effusion)
Hyperinflated: Hyperresonance (i.e Pnemothorax, COPD)
Auscultation
With a stethoscope touching the chest wall, ask patient to take a deep breath (inhalation) and exhale
preferably through the open mouth
Use locations similar to those as percussion
o Cardiovascular
Percussion
Left cardiac border
Percuss the 3rd, 4th and 5th intercostal space stating over the resonant areas near the axillary going
medially
Mark changes from changes from resonant to dullness
rd th th
3 ICS: <4cm, 4 ICS: <7 cm, 5 ICS <9 cm from midsternal line
Right cardiac border
Percuss the 3rd, 4th and 5th intercostal space
No dullness beyond the right edge of the sternum
© FAAS 3A, 2018
Ausculation
Auscultatory areas:
2nd right ICS – Aortic valve
2nd left ICS – Pulmonic valve
Left sternal border from 2nd to 5th ICS – Tricuspid valve
Apex (5th LICS, 7-9 cm from MSL) – Mitral valve
Listen to the precordium with the patient supine
Start auscultation from the base of the heart to the apex or vice-versa
Other two important positions:
o For mitral stenosis: Ask the patient to roll partly onto their left lateral decubitus position, bringing
the left ventricle closer to the chest wall. Place the bell lightly on the apical impulse
o For aortic regurgitation: Ask the patient to sit up, lean forward, exhale completely and stop
breathing in expiration. Pressing the diaphragm of the stethoscope on the chest, listen along the
left sternal border and a the apex
Grading of Murmus
1 Very faint, heard after the clinician has really tuned in
2 Quiet, but heard immediately upon placing stethoscope to chest wall
3 Moderately loud
4 Loud with palpable thrills
5 Very loud with thrill. Maybe heard when the stethoscope is partly off the chest
6 Very loud, with thrill. Maybe heard with stethoscope entirely off the chest
8. Percussion and auscultation of abdomen
Percussion
Percussion helps in assessing the amount and distribution of gas in the abdomen and to identify possible masses
that are solid or fluid filled. It is used in estimating liver and spleen size.
Percuss the abdomen lightly in all four quadrants to assess the distribution of tympany and dullness.
Tympany usually predominates because of gas in the gastrointestinal tract
Liver span
Measure the vertical span of the liver dullness in the midclavicular line
Along the right MCL, at the level of umbilicus, lightly percuss upward towards the liver
Note which level tympany on percussion becomes dullness (lower border of the liver)
At MCL, lightly percuss from the lung resonance down towards the liver
Note the level where resonance is replaced by dullness (upper border of liver)
Normal: From the MCL: 6-12cm
From the MSL: 4-8 cm
Percussion in Traube’s space
Percuss the left lower anterior chest wall between lung resonance above and costal margin below
Percuss going lateral to the anterior axillary line and mid axillary line
Dullness in Traube’s space: Splenomegaly
© FAAS 3A, 2018
Splenic percussion sign
Percuss the lowest intercostal space at the midaxillary line
Change in percussion note from tympany to dullness during deep breathing
9. Sings of appendicitis
Tenderness on palpation in the right iliac fossa over the McBurney’s point
Rebound tenderness
Pain on percussion
Rigidity
Guarding
Rovsing’s sign
Palpate deeply in the left lower quadrant
Quickly withdraw fingers
(+) increased pain in the right lower quadrant during left sided pressure
Referred rebound tenderness – right lower quadrant pain on quick withdrawal
Suggests peritoneal irritation in the right iliac fossa precipitated by palpation at a remote location
Psoas sign
Place hand above patient’s right knee
Ask patient to raise thigh against hand
Ask patient to turn onto left side
Extend patient’s leg at the hip
(+): increased abdominal pain
Flexion of the leg at the hip makes the psoas muscle contract; extension stretches it.
Suggests irritation of the iliopsoas group hip flexors. Positive psoas sign may indicate an inflamed
rectocecal appendix
Obturator sign
Flex patient’s right thigh at the hip with knee bent
Rotae the lf internally at the hip
(+) right hypogastric pain
The maneuver stretches the internal oblique muscle.
Cutaneous hyperesthesia
Pick up a fold of skin between thumb and index finger without pinching it
(+) localized pain
10. Thyroid exam
Ask the patient to flex the neck slightly forward to relax the sternomastoid muscles.
Place the fingers of both hands on the patient’s neck so that your index fingers are just below the cricoid cartilage
Ask the patient to sip and swallow water as before. Feel for the thyroid isthmus rising up under your finger pads. It is
often but not always palpable.
Displace the trachea to the right with the fingers of the left hand; with the right hand fingers, palpate laterally for the
right lobe of the thyroid in the space between the displaced trachea and the relaxed sternomastoid. Find the lateral
margin. In similar fashion, examine the left lobe. The lobes are somewhat harder to feel than the isthmus, so practice
is needed. The anterior surface of a lateral lobe is approximately the size of the distal phalanx of the thumb and feels
somewhat rubbery.
Note the size, shape, and consistency of the gland and identify any nodules or tenderness.
If the thyroid gland is enlarged, listen over the lateral lobes with a stethoscope to detect a bruit, a sound similar to a cardiac
murmur but of noncardiac origin.
© FAAS 3A, 2018
11. Electrocardiography (ECG)
- The standard clinical tool used to measure the electrical activity of the heart
- Recording of the small extracellular signals produced by the movement of action potentials through
cardiac myocytes
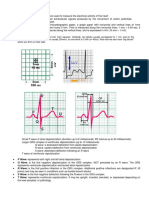
The ECG makes use of electrocardiographic paper, a graph paper with horizontal and vertical lines at 1mm
interval. A heavier line is present every 5 mm. Time is measured along the horizontal lines; 1 mm = 0.04 sec; 5
mm = 0.2 sec. Voltage is ,measured along the vertical lines, and is expressed in mV (10 mm = 1 mV).
ECG paper is traditionally divided into 1mm squares. Vertically, ten blocks usually correspond to 1 mV, and on the
horizontal axis, the paper speed is usually 25mm/s, so one block is 0.04s (or 40ms). Note that we also have "big blocks"
which are 5mm on their side.
Small P wave of atrial depolarization (duration up to 8 milliseconds; PR interval up to 20 milliseconds)
Larger QRS complex of ventricular depolarization (up to 10 milliseconds
Q wave: a downward deflection from septal depolarization
R wave: upward deflection from ventricular depolarization
S wave: downward deflection following an R wave
T wave of ventricular repolarization
P Wave: represents both right and left atrial depolarization
Q Wave: is the first negative depolarization of the QRS complex, NOT preceded by an R wave. The QRS
represents ventricular depolarization and buried atrial repolarization
R Wave: is the first positive inflection in the QRS complex. Additional positive inflections are designated R' (R
prime) and may be seen in conditions such as bundle branch blocks.
S Wave: is the first negative deflection following the R wave in the QRS complex.
T Wave: represents ventricular repolarization. It may be upright, inverted, elevated, or depressed depending on
the lead sampled, or pathology.
© FAAS 3A, 2018
• PR Interval This is the time from the initiation of SA nodal depolarization to the initiation of ventricular
depolarization. It encompasses the time it takes for the action potential to pass through the AV node. The normal
PRI is 120-200 msec. This demonstrates that the electrical impulses are originating from the atria and following
the proper conduction pathways. It is normal for the PRI to shorten slightly during tachycardia, and lengthen
during bradycardia within the limits stated above.
• QRS Duration The normal QRS duration is 60-100 msec. It is measured from the initiation of ventricular
depolarization at the Q or R wave, to the last wave of the complex. This point where the R or S wave returns to
baseline is called the J point. Prolonged QRS indicated conduction problems. This is often caused by bundle
branch blocks.
• QT Interval This interval spans the onset of depolarization of to the completion of repolarization of the ventricules.
Lengthened QT intervals indicated slowed ventricular repolarization. This may be due to hypokalemia, or other
electrolyte imbalances. Shortened QTs are seen with hypercalcemia and digitalis toxicity.
Lead
- One electrode is treated as the positive side of a voltmeter, and one or more electrodes as the negative side
- Records the fluctuation in voltage difference between positive and negative electrodes
The routine ECG consists:
• 12 leads: 6 limb leads and 6 chest leads.
• Frontal plane: 6 limb leads
• Transverse plane: 6 precordial leads
Limb Leads
• Allow us to view the heart in the frontal plane
• Will provide information on how the instantaneous vectors are directed, whether they are directed superiorly or
inferiorly and leftward or rightward
The 3 electrical limb leads represent the difference between 2 of the limb electrodes:
– I (positive connection/electrode to left arm, negative connection/electrode to right arm)
• Defines an axis in the frontal plane at 00
– II (positive to left leg, negative to right arm)
• Defines an axis in the frontal plane at 600
– III (positive to left leg, negative to left arm)
• Defines an axis in the frontal plane at 1200
© FAAS 3A, 2018
The 3 augmented ―unipolar‖ limb leads compare one limb electrode to the average of the other two:
– aVR (positive connection to right arm, negative connection is electronically defined in the middle of the
heart)
• axis defined by this limb lead in the frontal plane is -1500
• the ―a‖ stands for augmented, and the ―V‖ represents unipolar
• exploring electrode is placed at the right arm
– aVL (positive to left arm, negative is middle of the heart)
• axis defined by this limb lead in the frontal plane is -300
• exploring electrode is placed at the left arm
– aVF (positive to left leg [foot], negative is middle of the heart)
• axis defined by this limb lead in the frontal plane is +900
• exploring electrode is placed at the left foot
Chest Leads
• Allow us to view the heart in the horizontal or transverse plane
• Will provide information on how the instantaneous vectors are directed, whether they are directed anteriorly or
posteriorly and leftward or rightward
The Precordial Leads
- Termed chest or precordial leads because the electrodes are arranged on the front wall of the chest, over
the heart or precordium from V1-V6
- Lie in the transverse plane, perpendicular to the plane of the frontal leads
- The ―positive‖ connection is one of the 6 different locations on the chest wall
- The ―negative‖ connection is electronically defined in the middle of the heart by averaging the 3 limb
electrodes
The resultant leads are named V1 through V6 where the ―V‖ stands for unipolar:
V1 : 4th intercostal space to the right of the sternum
V2 : 4th intercostals space to the left of the sternum
V4 : 5th intercostals space at the midclavicular line
V3 : halfway between V2 and V4
V6 : 5th intercostals space at the maxillary line; same level as V4, left midaxillary line
V5 : halfway between V4 and V6; same level as V4, left anterior axillary line
LEAD (-) ELECTRODE (+) ELECTRODE VIEW OF HEART
Lead I RA LA Lateral
Lead II RA LL Inferior
Lead III LA LL Inferior
aVR LA + LL RA None
aVL RA + LL LA Lateral
aVF RA + LA LL Inferior
V1 Septal
V2 Septal
V3 Anterior
V4 Anterior
V5 Lateral
V6 Lateral
© FAAS 3A, 2018
Patient Positioning
Place the patient in a supine or semi-Fowler’s position. If the patient cannot tolerate being flat, you can do the ECG
in a more upright position.
Instruct the patient to place their arms down by their side and to relax their shoulders.
Make sure the patient’s legs are uncrossed.
Move any electrical devices, such as cell phones, away from the patient as they may interfere with the machine.
Skin Preparation
Dry the skin if it’s moist or diaphoretic.
Shave any hair that interferes with electrode placement. This will ensure a better electrode contact with the skin.
Rub an alcohol prep pad or benzoin tincture on the skin to remove any oils and help with electrode adhesion.
Electrode Application
Check the electrodes to make sure the gel is still moist.
Do not place the electrodes over bones.
Do not place the electrodes over areas where there is a lot of muscle movement.
12. Common skin lesions
PRIMARY SKIN LESIONS
Skin Lesion Description Example
Macule Small, flat spot, 1.0 cm in diameter Hemangioma, vitilligo, freckle,
petechiae
Patch Flat spot, ≥ 1-0 cm Café-au-lait spot
Papule Palpable, elevated, 1.0 cm Nevus
Plaque Elevated superficial, ≥ 1.0 cm, often formed by a Psoriasis
coalesce of papules
Nodule Knot-like lesion larger than 0.5 cm, deeper and more Dermatofibroma
firm than a papule
Cyst Nodule filled with expressible material Epidermal inclusion cyst
Wheal Irregular, transient superficial area of localized Mosquito bite, hives
edema
Vesicle Palpable, elevated, filled with serous fluid, up to 1.0 Herpes simplex, Herpes zoster
cm
Bulla ≥ 1.0 cm, filled with serous fluid Insect bite, 2nd degree bite
Pustule Palpable, elevated, filled with pus Acne, impetigo
Burrow Minute, slightly raised tunnel in the epidermis cabies
SECONDARY SKIN LESIONS
Scale A thin flake of dead, exfoliated epidermis Ichthyosis vulgaris, dandruff,
psoriasis, dry skin
Crust Dried residue of skin exudates (serum, pus, blood) Impetigo
Lichenification Visible and palpable thickening of the skin with Neurodermatitis
increased visibility of the normal skin furrows
Scars Increased connective tissue that arises from injury or Hypertrophic scar from steroid
disease injections
Keloids Hypertrophic scarring that extends beyond the
borders of the initiating injury
Erosion Non-scarring loss of the superficial epidermis Apthous stomatitis, moist area after a
surface is moist but does not bleed rupture of a vesicle (chicken pox)
Excoriation Linear, punctuate erosions caused by scratching Cat scratches
Fissure A linear crack in the skin often resulting from excess Athlete’s foot
dryness
Ulcer A deeper loss of epidermis and dermis Stasis ulcer, syphilitic chancre
© FAAS 3A, 2018
You might also like
- Respiratory Examination GuideDocument4 pagesRespiratory Examination Guiderhea100% (2)
- Jarvis Neurological Assessment SummaryDocument11 pagesJarvis Neurological Assessment Summaryaderonke bello100% (2)
- OB - Normal Labor and DeliveryDocument51 pagesOB - Normal Labor and DeliveryJosh Matthew Rosales33% (3)
- Icru Report 62Document62 pagesIcru Report 62Luis Ramirez100% (1)
- Circulatory System QuestionsDocument4 pagesCirculatory System QuestionsJohn Vincent Gonzales50% (2)
- Neurological ExaminationDocument9 pagesNeurological Examinationmohitnet1327No ratings yet
- Child Protection Training ManualDocument229 pagesChild Protection Training Manualbabuin1No ratings yet
- Aromatherapy - 600 Aromatherapy Recipes For Beauty, Health & Home - Plus Advice & Tips On How To Use Essential Oils - Nodrm PDFDocument365 pagesAromatherapy - 600 Aromatherapy Recipes For Beauty, Health & Home - Plus Advice & Tips On How To Use Essential Oils - Nodrm PDFFernanda Rodriguez75% (4)
- Dystolic Dysfunction Ppt. SalmanDocument42 pagesDystolic Dysfunction Ppt. SalmanMustajab MujtabaNo ratings yet
- Cardiovascular AssessmentDocument73 pagesCardiovascular AssessmentmatthewsarfrazbhattiNo ratings yet
- Cardiovascular Assessment (1) - StudentsDocument70 pagesCardiovascular Assessment (1) - Studentsraima ayazNo ratings yet
- Assessment of CvsDocument70 pagesAssessment of CvsTouseeq ManzoorNo ratings yet
- The Precise Neurological ExamDocument30 pagesThe Precise Neurological ExamZīshān FārūqNo ratings yet
- Postural Vital Signs MeasurementRevisedDocument8 pagesPostural Vital Signs MeasurementRevisedumiNo ratings yet
- Emergency 1Document42 pagesEmergency 1Meshari Al- NafisiNo ratings yet
- 8.dx and RPDocument20 pages8.dx and RPkimberlynNo ratings yet
- Pemeriksaan Tanda Vital-Kuliah PengantarDocument22 pagesPemeriksaan Tanda Vital-Kuliah PengantartrisiaNo ratings yet
- Dr.K.sellahewa Cardiovascular System ExaminationDocument8 pagesDr.K.sellahewa Cardiovascular System ExaminationNilaaharan RobinsonNo ratings yet
- Cardio ExaminationDocument7 pagesCardio ExaminationAisha Baniyas??No ratings yet
- Ex - Cerebellar ExamDocument2 pagesEx - Cerebellar ExamssNo ratings yet
- Respiratory Exam (RCT)Document8 pagesRespiratory Exam (RCT)kenners100% (31)
- Vital-Signs 042951Document37 pagesVital-Signs 042951alyssaburgos02No ratings yet
- Bicol University College of NursingDocument71 pagesBicol University College of NursingDanekka TanNo ratings yet
- ABCDE Assessment - Lecturio PDFDocument11 pagesABCDE Assessment - Lecturio PDFjsw03No ratings yet
- 3 - Vital SignDocument27 pages3 - Vital SignBav VAansoqnuaetzNo ratings yet
- Blood PressureDocument18 pagesBlood PressureChelsea BorgoniaNo ratings yet
- Introduction To TraumaDocument27 pagesIntroduction To TraumaFauzi SebunyaNo ratings yet
- SMF Kardiologi Rsud Sidoarjo: Hairudi SugijoDocument87 pagesSMF Kardiologi Rsud Sidoarjo: Hairudi SugijoThambelina Ressita ImoetzNo ratings yet
- PX FISIK Tubuh ManusiaDocument59 pagesPX FISIK Tubuh ManusiaSheila Jessica AndavaniaNo ratings yet
- Anesthetic MonitoringDocument11 pagesAnesthetic Monitoring102022No ratings yet
- DR Sujata: Professor Dept - of Anaesthesiology &critical Care Ucms & GTB HospitalDocument53 pagesDR Sujata: Professor Dept - of Anaesthesiology &critical Care Ucms & GTB HospitalMiniNo ratings yet
- Neuro 1 and 2 LabDocument3 pagesNeuro 1 and 2 LabHardikPatelNo ratings yet
- Vital Signs: Temperature: Respiratory Rate: PulseDocument55 pagesVital Signs: Temperature: Respiratory Rate: PulsemiraNo ratings yet
- Signos VitalesDocument5 pagesSignos VitalesAndrea Correa OrtegaNo ratings yet
- CVS ExaminationDocument10 pagesCVS ExaminationAhmedNo ratings yet
- Assessing The Heart and Neck VesselsDocument6 pagesAssessing The Heart and Neck VesselsA R F I J U LNo ratings yet
- Mrcp-PACES 2023 - Sequence - CVSDocument2 pagesMrcp-PACES 2023 - Sequence - CVSvaranasidineshNo ratings yet
- Clin SkillsDocument6 pagesClin SkillsChristopher MatthewsNo ratings yet
- Cardiovascular (CVS) Examination: Procedure StepsDocument15 pagesCardiovascular (CVS) Examination: Procedure StepsGeorich NarcisoNo ratings yet
- Define Blood Pressure FinalDocument11 pagesDefine Blood Pressure FinalNowshad T 1 8 1 0 2 6No ratings yet
- DRR LessonsDocument8 pagesDRR LessonsKristel Joy BelgicaNo ratings yet
- Blood Regulation: Baroreceptors Are Sensory Neurons That Monitor Arterial BloodDocument20 pagesBlood Regulation: Baroreceptors Are Sensory Neurons That Monitor Arterial BloodSajaratul Syifaa'No ratings yet
- AnestesiDocument11 pagesAnestesiAnonymous 8w9QEGNo ratings yet
- Physical ExaminationDocument32 pagesPhysical ExaminationCaroline AgathaNo ratings yet
- Neuro PEDocument36 pagesNeuro PEkhaderbasha2020No ratings yet
- Baseline Vital Kefah 1ADocument38 pagesBaseline Vital Kefah 1AShahd Abu SnenehNo ratings yet
- General Anesthesia: Compiled By: Asad Arslan Source: Dr. Muhammad Aun SahbDocument21 pagesGeneral Anesthesia: Compiled By: Asad Arslan Source: Dr. Muhammad Aun SahbMr. AlphaNo ratings yet
- Cardiovascular Examination TechniquesDocument36 pagesCardiovascular Examination TechniquesRUTUJA HARISH KSHIRSAGAR100% (1)
- Cned Handbook Single Page1 1Document40 pagesCned Handbook Single Page1 1api-300218860No ratings yet
- Vital SignsDocument10 pagesVital SignsBOSANG Shylla Klaren L.No ratings yet
- Cardiovascular Assessment-1Document60 pagesCardiovascular Assessment-1M Razzaq100% (1)
- Emergency PlanDocument48 pagesEmergency PlansamNo ratings yet
- Cranial Nerve AssessmentDocument5 pagesCranial Nerve AssessmentBAdz TanNo ratings yet
- Hipertensi JNC 7 VS Hipertensi JNC 8Document99 pagesHipertensi JNC 7 VS Hipertensi JNC 8Sarah Riskita MaizaliusNo ratings yet
- FundaDocument5 pagesFundaGreggy Francisco LaraNo ratings yet
- Cardio ResuscitationDocument38 pagesCardio ResuscitationBhakti WashilkarNo ratings yet
- Vital SignsDocument10 pagesVital SignsMuhammad FahmyNo ratings yet
- 4 Abdominal+ExaminationDocument9 pages4 Abdominal+Examinationمرتضى حسين عبدNo ratings yet
- Blood Pressure 01Document23 pagesBlood Pressure 01Fahad MahmoodNo ratings yet
- Vital Sign Na (1) by ZWBDocument52 pagesVital Sign Na (1) by ZWBAshraf Ali100% (1)
- Assessing Blood PressureDocument3 pagesAssessing Blood PressureSean DuayNo ratings yet
- Sensory ExamDocument24 pagesSensory Examsarguss14100% (2)
- Basic Health Care Skills: How To Measure Vital Signs Vital SignsDocument8 pagesBasic Health Care Skills: How To Measure Vital Signs Vital SignsJoan BarcenasNo ratings yet
- Respiratory Exam DetailedDocument12 pagesRespiratory Exam DetailedAshiniNo ratings yet
- Vital SignDocument100 pagesVital SignIbnu FuqonNo ratings yet
- Adult Combined ScheduleDocument13 pagesAdult Combined ScheduleJustin Ng SincoNo ratings yet
- Pathology Practice QuestionsDocument10 pagesPathology Practice QuestionsPatNo ratings yet
- DEPARTMENT OF HEALTH-Medical Officer III-2Document2 pagesDEPARTMENT OF HEALTH-Medical Officer III-2PatNo ratings yet
- Office: of The SecretaryDocument41 pagesOffice: of The SecretaryRachel Caput HortizuelaNo ratings yet
- Canon LawDocument16 pagesCanon LawEmmanuel A. RemolacioNo ratings yet
- Demon Drink GeorgeDocument5 pagesDemon Drink GeorgePatNo ratings yet
- CBC and BMP Fishbone TemplateDocument2 pagesCBC and BMP Fishbone TemplatePatNo ratings yet
- Combined Growth Charts V2 8.4.09 PDFDocument10 pagesCombined Growth Charts V2 8.4.09 PDFKathlyn SunicoNo ratings yet
- Memorandum Circular No. 2005-005Document1 pageMemorandum Circular No. 2005-005PatNo ratings yet
- OMB Certificate SampleDocument1 pageOMB Certificate SamplePatNo ratings yet
- IM Notes 1Document16 pagesIM Notes 1PatNo ratings yet
- Outline of Physical ExaminationDocument6 pagesOutline of Physical ExaminationAnonymous 0WHX7nNo ratings yet
- Monograph On Lung Cancer July14Document48 pagesMonograph On Lung Cancer July14PatNo ratings yet
- Pediatric Medical History: (Approximate Age When Major Developmental Milestones Are Acquired)Document1 pagePediatric Medical History: (Approximate Age When Major Developmental Milestones Are Acquired)PatNo ratings yet
- Pedia Notes PDFDocument10 pagesPedia Notes PDFCarlBuscatoNo ratings yet
- Osce: Pediatrics: Hand WashingDocument11 pagesOsce: Pediatrics: Hand WashingPatNo ratings yet
- Pedia Notes PDFDocument10 pagesPedia Notes PDFCarlBuscatoNo ratings yet
- Mass: Vomiting:: Surgery HISTORY I. Patient'S Profile A. GENERAL DATA (Time: - )Document5 pagesMass: Vomiting:: Surgery HISTORY I. Patient'S Profile A. GENERAL DATA (Time: - )PatNo ratings yet
- Pedia Notes PDFDocument10 pagesPedia Notes PDFCarlBuscatoNo ratings yet
- Abdominal IncisionsDocument9 pagesAbdominal IncisionsSenthilkumar ThiyagarajanNo ratings yet
- Colon CancerDocument1 pageColon CancerPatNo ratings yet
- The Gown Flapping) : Osce: Surgery GowningDocument6 pagesThe Gown Flapping) : Osce: Surgery GowningPatNo ratings yet
- Principles Contact TracingDocument3 pagesPrinciples Contact TracingPatNo ratings yet
- OSCE OB - PDF Version 1Document15 pagesOSCE OB - PDF Version 1FNaF is love FNaF is lifeNo ratings yet
- Osce: Pediatrics: Hand WashingDocument11 pagesOsce: Pediatrics: Hand WashingPatNo ratings yet
- Day 13 REDCOPDocument46 pagesDay 13 REDCOPPrabin ChaudharyNo ratings yet
- LeprosyDocument48 pagesLeprosyPatNo ratings yet
- Childhood Injuries and PoisoningDocument51 pagesChildhood Injuries and PoisoningPatNo ratings yet
- Sandlewood Health BenefitsDocument7 pagesSandlewood Health BenefitskalaimaniNo ratings yet
- Bilirubin Metabolism Jaundice PPP 9Document27 pagesBilirubin Metabolism Jaundice PPP 9Regina Marsha Xaveria100% (1)
- Blood Grouping ReagentsDocument7 pagesBlood Grouping ReagentsDominic EmerencianaNo ratings yet
- AP Lab #6: pGLO Transformation LabDocument4 pagesAP Lab #6: pGLO Transformation Labpointweb85% (20)
- Persistent Prelethal Stress Leads To Cellular AdaptationDocument14 pagesPersistent Prelethal Stress Leads To Cellular AdaptationMalliga SundareshanNo ratings yet
- CCRT Cervix2Document27 pagesCCRT Cervix2Marfu'ah Nik EezamuddeenNo ratings yet
- Winter 2010 Natural FarmerDocument48 pagesWinter 2010 Natural FarmerV1xWqNo ratings yet
- Pyometra in A Cat: A Clinical Case Report: November 2021Document7 pagesPyometra in A Cat: A Clinical Case Report: November 2021Ronny Alberto GallegoNo ratings yet
- Common Mistakes-BiologyDocument8 pagesCommon Mistakes-BiologyteahockNo ratings yet
- Morena E. Dail, RMT, MT (Amt), Mls (Ascpi) : Mors CodeDocument53 pagesMorena E. Dail, RMT, MT (Amt), Mls (Ascpi) : Mors CodemeriiNo ratings yet
- Phytochemical Analysis, Antimicrobial and Antioxidant Activities of Euphorbia Juss.) : An Unexplored Medicinal Herb Reported From CameroonDocument15 pagesPhytochemical Analysis, Antimicrobial and Antioxidant Activities of Euphorbia Juss.) : An Unexplored Medicinal Herb Reported From CameroonClara JamirNo ratings yet
- Pembahasan CBT COMBO 3Document802 pagesPembahasan CBT COMBO 3Sari Dewi WiratsihNo ratings yet
- Important Classifications PDFDocument42 pagesImportant Classifications PDF330 Himank MehtaNo ratings yet
- What Is The DASH Eating Plan - (Printer-Friendly)Document5 pagesWhat Is The DASH Eating Plan - (Printer-Friendly)Are-nim Hanim100% (1)
- Wild and Ancient Fruit - Is It Really Small, Bitter, and Low in Sugar - Raw Food SOSDocument73 pagesWild and Ancient Fruit - Is It Really Small, Bitter, and Low in Sugar - Raw Food SOSVictor ResendizNo ratings yet
- I Notes RETINA PDFDocument251 pagesI Notes RETINA PDFFelipe renquenNo ratings yet
- General Profile: - Pa - 6mos Old - Female - Filipino - Roman Catholic - Alang-Alang Mandaue CityDocument18 pagesGeneral Profile: - Pa - 6mos Old - Female - Filipino - Roman Catholic - Alang-Alang Mandaue CityRj FornollesNo ratings yet
- HPP Neuro Paper GraserDocument12 pagesHPP Neuro Paper GraserCaro ErazoNo ratings yet
- DNA Study GuideDocument2 pagesDNA Study GuideRielle Dela MercedNo ratings yet
- Effect of Nasapana in The Management of Avabahuka A Case StudyDocument5 pagesEffect of Nasapana in The Management of Avabahuka A Case StudyEditor IJTSRDNo ratings yet
- Occupational HealthDocument8 pagesOccupational HealthFemale calm0% (1)
- A Proposed Pediatric Medical Center Research ThesisDocument3 pagesA Proposed Pediatric Medical Center Research ThesisMarielle AbanteNo ratings yet
- CBST LastDocument5 pagesCBST LastMozma AwanNo ratings yet
- 3.ALS Algorithms Advanced Life SupportDocument1 page3.ALS Algorithms Advanced Life SupportLucian Alin DinuNo ratings yet
- Rickey Dixon Letter To The Court On NFL Concussion Settlement FeesDocument9 pagesRickey Dixon Letter To The Court On NFL Concussion Settlement FeesRobert Lee100% (1)