Professional Documents
Culture Documents
Management of Soft Tissue Injuries - Case Series
Uploaded by
Anonymous jfqzCfcI4EOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Management of Soft Tissue Injuries - Case Series
Uploaded by
Anonymous jfqzCfcI4ECopyright:
Available Formats
NUJHS Vol. 5, No.
1, March 2015, ISSN 2249-7110
Nitte University Journal of Health Science
Case Report
MANAGEMENT OF SOFT TISSUE INJURIES – CASE SERIES
1 2 3 4 5
Muralee Mohan , B Rajendra Prasad , S M Sharma , Tripthi Shetty & Priyadharsana P S
1
Professor, 2 Professor & Principal, 3Professor & HOD, 4Assistant Professor, 5Post Graduate A.B. Shetty Memorial Institute
of Dental Sciences, Nitte University, Mangalore - 575018.
Correspondence :
Priyadharsana P S
Post Graduate, Department of Oral & Maxillofacial Surgery, A.B Shetty Memorial Institute of Dental Sciences,
Nitte University, Mangalore - 575 018, Karnataka, India.
E-mail : dharsana88@gmail.com
Abstract :
Soft tissue injuries, whether isolated or in combination with other injuries, are amongst the most common traumatic craniofacial
injuries encountered in our day to day practice.
Soft tissue injuries may involve the skin, subcutaneous tissue, underlying muscle or a combination of any of these elements. Although
rarely life-threatening, the treatment of these injuries can be complex and may have significant impact on the patients' facial aesthetics
and function. Hence one should know the “do's and don'ts”.
Disfigurement following trauma, has a detrimental effect on the victim's personality and future. Therefore such cases should be most
appropriately managed with thorough knowledge of applied anatomy, an aesthetic sense and meticulous tissue handling, along with
surgical skills to repair composite structures.
Keywords : Soft tissue injury, Trauma, Management
Introduction : Classification of Wound
Injuries to the head and neck are more common, accounts Centers for Disease Control & Prevention (CDC) 1999 (2)
for more than 70% of road traffic accidents. Of the 613 Ø CLEAN – 75% of surgical wound
maxillofacial injury patients treated in the casualty of Ø CLEAN CONTAMINATED
KSHEMA hospital, Mangalore (2010-2011), 542 patients Ø CONTAMINATED
sustained soft-tissue injuries.(1) Facial soft tissue injuries Ø DIRTY/ INFECTED
vary in severity based on the impact force and type of injury
The aim of managing such complex injury is to achieve
into minor superficial wounds to massive avulsions.
functional and aesthetic recovery in the shortest time
Classification of soft tissue injuries: period. The operating surgeon should understand the
Ø Contusion biomechanics and molecular biology of wound healing and
Ø Abrasion the art of soft tissue repair. Management of complex soft
Ø Laceration tissue injuries are always a challenge to the surgeons.
Simple laceration Since there are a very few literatures on principles of
Stellate laceration managing soft tissue injuries we have attempted to
Flap like laceration highlight the same in this article.
Access this article online
Quick Response Code Ø Avulsion injuries Case Series :
Here we present a series of 3 road traffic accident cases
Ø Bites
who reported to our department with facial soft tissue
Ø Burns injury.
Keywords : Soft tissue injury, Trauma, Management - Priyadharsana P S 79
NUJHS Vol. 5, No.1, March 2015, ISSN 2249-7110
Nitte University Journal of Health Science
Case 1:
A 21 year old male patient reported with severe laceration
soft tissue injury of upper and lower lip following a bike
accident.
Figure 4 : Post Op Day 7
On alternative days chlorhexidine acetate dressing was
changed and the area was kept moist. Wound was allowed
to heal by secondary intention.
Figure 1 : Pre Operative
Wound debridement done with hydrogen peroxide and
povidone – iodine followed by thorough irrigation with
normal saline. Suturing was done in layers. Subcutaneous
layer, orbicularis oris muscle layer closed with 4-0 vicryl and
skin with 4-0 prolene.
Figure 5 : Post Op Day 10
Case 2 :
A 50 year old male patient reported with lacerated nasal
soft tissue injury caused due to a cut by a glass piece.
Patient reported to the department after 9 hours of injury.
Blackish discolouration of the soft tissue noted and patient
Figure 2 : Post Operative
was explained the complications.
Figure 3 : Post Op Day 4
Post operative day 4: patient reported with a complaint of
Figure 1 : Pre Operative
discoloration of lower lip. Patient was placed under
Suturing was done with 5-0 prolene and patient was on
observation. On day 7 sutures were removed and the
regular follow up.
avulsed necrosed portion of soft tissue was removed.
Keywords : Soft tissue injury, Trauma, Management - Priyadharsana P S 80
NUJHS Vol. 5, No.1, March 2015, ISSN 2249-7110
Nitte University Journal of Health Science
Case 3 :
A 45 year old woman reported with severe soft
tissue injury of mid maxillary region following a
fall. Wound was debrided and suturing done in
layers with 4-0 ethilon.
Figure 2 : Post Operative
On post operative day 2 blackish discoloration of soft tissue
noticed. Till post operative day 5 lignocaine without
Figure 1 : Pre Operative Figure 2 : Post Operative
adrenaline was given along the suture line to cause
Post operative day 2 necrosis of the soft tissue noticed.
vasodilation. Noticed colour change from blackish
Daily change of bactigras (chlorhexidine acetate) dressing
discolouration to reddish pink on post operative day 10.
was done as we planned for a wait and watch. On post
Later on patient was prescribed contractubex (R) for better
operative day 3 dehiscence of the wound noted in the both
results.
right and left commisure of the lip. Barrel bandage placed
and patient was adviced to restrict the mouth opening. On
day 4 collagen membrane suturing was done to act as a
scaffold for the wound. Patient is currently on regular
follow up.
Figure 3 : Post Op Day 2 Figure 4 : Post Op Day 10
Figure 3 : Post Op Day 4
Discussion :
Facial soft tissue is more common since the incidence of
road traffic accidents is very high. Facial soft tissue injury is
given maximum attention because the management is
based on both aesthetic and functional aspect. Necrosis of
the soft tissue is one of the major complications of deep or
massive soft tissue injury. Since orofacial region has
Figure 5 : Post Op Day 12 Figure 6 : Post Op Day 15 numerous blood supplies from branches of facial artery,
the end result of treatment is most often positive.
Keywords : Soft tissue injury, Trauma, Management - Priyadharsana P S 81
NUJHS Vol. 5, No.1, March 2015, ISSN 2249-7110
Nitte University Journal of Health Science
Clinical evaluation should be carried out under adequate Wounds in the face should be closed in layers to attain
light source, copious irrigation and hemostasis. Horizontal anatomic alignment and to avoid dead space. The most
injury across the facial region is less likely to damage the common reasons for suture scar or suture mark is closing
facial nerve than the vertical injuries. Ideally facial wounds the wounds under tension and delayed removal. Ideally
without additional injuries should be repaired as soon as facial sutures should be removed between post operative
possible. In major trauma requiring the resuscitative days 4 to 6. Pressure dressing should be avoided in
(3)
measures, the wound can be managed after 4 – 6 hours. devitalised tissues to prevent anaerobic infection. (5)
Local anaesthetics without adrenaline are preferred in Topical antibiotic ointment for post operative use should
such injuries to avoid vasoconstriction which compromises be discontinued after 7 days to prevent tissue reaction. (6)
the blood supply to injured area. According to the literature
Following are the timings for removal of sutures based on
hydrogen peroxide and povidone – iodine should be
different areas of head and neck,
avoided in fresh wounds since they impede with healing
Face / ear – 4 to 6 days
process. The author has quoted that non-ionic detergent
(4) Scalp – 6 to 8 days
minimises inflammatory response. Irrigation removes
Eyelid – 3 to 5 days
enough bacteria if used with 7 pounds of pressure per
Neck – 5 to 7 days.
square inch. This pressure is generated by forcefully
expressing saline from 35 ml syringe with 18 gauge needle. Conclusion: Successful treatment of the patient with
(4)
orofacial soft tissue injury requires regular follow up to
Regeneration of cells occurs from stratum germinatum or ensure proper healing of the wound, in order to prevent
basal layer in the epidermis. Regeneration of cells on the functional & esthetic facial derangement. The surgeon
face results from both basal layer and epidermal pegs. should be familiar with the anatomy of the facial
Epidermal pegs are numerous in the face and hence structures, various treatment modalities and should
significant portion of epidermal layer can be removed closely monitor the patient until optimal healing of the soft
without scarring. tissue had occurred in order to prevent scar formation.
References :
1. Sharma S.M, Gautam, Hardik shah; Characteristics of maxillofacial
soft tissue injuries – 2 years clinical review; Journal of Indian dentist
research & review, dec 2012. 26-32
2. web source; http://www.cdc.gov/nchs/icd9.htm
3. Bhattacharya; management of soft tissue wounds of the face; Indian
journal of plastic surgery. 2012 sep – dec; 45(3): 436 – 443.
4. Raymond J Fonseca; oral and maxillofacial trauma; 2nd edition.
5. Thomas; The Role of the Epidermis and the Mechanism of Action of
Occlusive Dressings in Scarring; wound repair regen 2011 sep (1) s16-
s21.
6. Nicholas J.V Hogg, Bruce B. Horswell; soft tissue pediatric facial
trauma: a review; journal of Canadian Dental Association;july/august
2006, vol. 72(6): 549-552
Keywords : Soft tissue injury, Trauma, Management - Priyadharsana P S 92
You might also like
- Peri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentFrom EverandPeri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentNo ratings yet
- Soft Tissue Management in Facial Trauma: Tara L. Braun, BS Renata S. Maricevich, MDDocument7 pagesSoft Tissue Management in Facial Trauma: Tara L. Braun, BS Renata S. Maricevich, MDoktarinadyaNo ratings yet
- Oculoplastic Surgery: A Practical Guide to Common DisordersFrom EverandOculoplastic Surgery: A Practical Guide to Common DisordersEssam A. El ToukhyNo ratings yet
- 33 Protocolo Biopsia 01Document12 pages33 Protocolo Biopsia 01lauraNo ratings yet
- Facial Soft Tissue TraumaDocument9 pagesFacial Soft Tissue TraumaoktarinadyaNo ratings yet
- Anterior Open Bite With ICR HistoryDocument12 pagesAnterior Open Bite With ICR HistoryKanchit SuwanswadNo ratings yet
- Management of Soft Tissue Wounds of The FaceDocument14 pagesManagement of Soft Tissue Wounds of The FaceHugo HerreraNo ratings yet
- Fracturas Maxilofaciales 2Document11 pagesFracturas Maxilofaciales 2ArturoNo ratings yet
- Open Fractures TTBDocument45 pagesOpen Fractures TTBcromwellopoku42No ratings yet
- Mandible Fractures: Brent B. Pickrell, MD Arman T. Serebrakian, MD, MS Renata S. Maricevich, MDDocument8 pagesMandible Fractures: Brent B. Pickrell, MD Arman T. Serebrakian, MD, MS Renata S. Maricevich, MDmustafasacarNo ratings yet
- 3) Singh2017Document5 pages3) Singh2017joteja8497No ratings yet
- Complications and Pitfalls in Maxillofacial Trauma: 10.5005/jp-Journals-10028-1108Document7 pagesComplications and Pitfalls in Maxillofacial Trauma: 10.5005/jp-Journals-10028-1108Indra D KristionoNo ratings yet
- IntJOralHealthDent 7-2-146 150Document5 pagesIntJOralHealthDent 7-2-146 150Neha MehtaNo ratings yet
- NatlJMaxillofacSurg32152-2112085 055200Document7 pagesNatlJMaxillofacSurg32152-2112085 055200JC QuezadaNo ratings yet
- Accepted Manuscript: 10.1016/j.cjtee.2016.08.002Document18 pagesAccepted Manuscript: 10.1016/j.cjtee.2016.08.002RadenSiwi Bagus HadhiningratNo ratings yet
- Trauma Suturing Techniques: Key PointsDocument10 pagesTrauma Suturing Techniques: Key PointsAstidya MirantiNo ratings yet
- Initial Assessment, Debridement, and Decision Making in The Salvage of Severely Injured Lower ExtremityDocument7 pagesInitial Assessment, Debridement, and Decision Making in The Salvage of Severely Injured Lower ExtremityVigneswaran VaradharajanNo ratings yet
- Soft Tissue Pediatric Facial Trauma: A ReviewDocument5 pagesSoft Tissue Pediatric Facial Trauma: A ReviewGilangIswaraWijayaNo ratings yet
- 2) Neelakandan2014Document14 pages2) Neelakandan2014joteja8497No ratings yet
- Stefan Danilla - Selected Topics in Plastic Reconstructive Surgery (2012, InTech)Document243 pagesStefan Danilla - Selected Topics in Plastic Reconstructive Surgery (2012, InTech)Ramona PaulaNo ratings yet
- Presentasi PABI Pekanbaru 2021Document20 pagesPresentasi PABI Pekanbaru 2021raudhatul muttaqinNo ratings yet
- Management of Facial Fractures, Its Demography and Clinical OutcomeDocument12 pagesManagement of Facial Fractures, Its Demography and Clinical OutcomeIJAR JOURNALNo ratings yet
- Complications of Frontal Sinus Fractures: Stephen E. Metzinger, M.D., F.A.C.S., and Rebecca C. Metzinger, M.DDocument8 pagesComplications of Frontal Sinus Fractures: Stephen E. Metzinger, M.D., F.A.C.S., and Rebecca C. Metzinger, M.DYohana SepthiyaNo ratings yet
- Post Extraction Lingual Mucosal Ulceration With Bone NecrosisDocument4 pagesPost Extraction Lingual Mucosal Ulceration With Bone Necrosisandrianiputri916No ratings yet
- Open Fractures: DR Gourav RamukaDocument30 pagesOpen Fractures: DR Gourav RamukaGaurav Ramuka100% (1)
- Case Report Management Ankyloglossia With Scalpel ElectrosurgeryDocument3 pagesCase Report Management Ankyloglossia With Scalpel ElectrosurgeryDeasireeNo ratings yet
- Neligan Vol 3 Chapter 03 MainDocument55 pagesNeligan Vol 3 Chapter 03 MainisabelNo ratings yet
- 494-Article Text-2090-1-10-20220221Document6 pages494-Article Text-2090-1-10-20220221Hans WinardiNo ratings yet
- "Unilateral Subcondylar Fracture Treated by Close Reduction: A CaseDocument3 pages"Unilateral Subcondylar Fracture Treated by Close Reduction: A CaseAlbertine JaneNo ratings yet
- Zalavras 2017Document14 pagesZalavras 2017alexi.garciaNo ratings yet
- Different Surgical Modalities For Management of Postburn FL Exion Contracture of The ElbowDocument6 pagesDifferent Surgical Modalities For Management of Postburn FL Exion Contracture of The ElbowMadhuchandra HirehalliNo ratings yet
- Surgical Technique For Optimal OutcomesDocument11 pagesSurgical Technique For Optimal OutcomesAndrei EncisoNo ratings yet
- Modes of Failure of Proximal Femoral Nail (PFN) in Unstable Trochanteric FracturesDocument10 pagesModes of Failure of Proximal Femoral Nail (PFN) in Unstable Trochanteric FracturesSrikanthNo ratings yet
- MukokelDocument3 pagesMukokeljulietNo ratings yet
- 137394-Article Text-367387-1-10-20160609Document2 pages137394-Article Text-367387-1-10-20160609Luis GarciaNo ratings yet
- Ravikiran Naalla, 2020Document7 pagesRavikiran Naalla, 2020Ahmed SalahNo ratings yet
- Tibia-Open # MGDocument5 pagesTibia-Open # MGluckyariadneeNo ratings yet
- Bone Repair Using The Masquelet TechniqueDocument13 pagesBone Repair Using The Masquelet TechniqueManny TantorNo ratings yet
- Complicated Facial WoundsDocument5 pagesComplicated Facial WoundsIJAR JOURNALNo ratings yet
- Injury: F. Lavini, C. Dall'Oca, S. Mezzari, T. Maluta, E. Luminari, F. Perusi, E. Vecchini, B. MagnanDocument6 pagesInjury: F. Lavini, C. Dall'Oca, S. Mezzari, T. Maluta, E. Luminari, F. Perusi, E. Vecchini, B. MagnanTefera LeteboNo ratings yet
- Factors Affecting Functional Outcome of Distal Tibia Fractures Treated by Plating Using Minimal Invasive Percutaneous Plate Osteosynthesis TechniqueDocument10 pagesFactors Affecting Functional Outcome of Distal Tibia Fractures Treated by Plating Using Minimal Invasive Percutaneous Plate Osteosynthesis TechniqueIJAR JOURNALNo ratings yet
- Chronic OsteomyelitisDocument6 pagesChronic Osteomyelitisdedyalkarni08No ratings yet
- Amniotic Membrane Transplant in Inflammatory Corneal Ulcers: Interest and Modality of Follow-Up by Anterior Segment OctDocument6 pagesAmniotic Membrane Transplant in Inflammatory Corneal Ulcers: Interest and Modality of Follow-Up by Anterior Segment OctIJAR JOURNALNo ratings yet
- Extraoral DefectsDocument3 pagesExtraoral DefectsRidhoNo ratings yet
- Dentoalveolar Trauma: Ted Fields, DDSDocument26 pagesDentoalveolar Trauma: Ted Fields, DDSCak BasitNo ratings yet
- Prospective Study of Management of Close or CompouDocument5 pagesProspective Study of Management of Close or CompoumaudiaNo ratings yet
- Flaps and GraftsDocument5 pagesFlaps and GraftsmaxfaxNo ratings yet
- Approach To Fingertip Injuries: Patricia Martin-Playa,, Anthony FooDocument9 pagesApproach To Fingertip Injuries: Patricia Martin-Playa,, Anthony FooTeja Laksana NukanaNo ratings yet
- Late Mandible Fracture After Surgical Extraction of Mandibular Third Molar: A Retrospective Data From A Tertiary InstituteDocument5 pagesLate Mandible Fracture After Surgical Extraction of Mandibular Third Molar: A Retrospective Data From A Tertiary InstituteDeividy NespoloNo ratings yet
- Traumatic Wounds of The Upper Extermity Coverage StrategiesDocument14 pagesTraumatic Wounds of The Upper Extermity Coverage Strategiessimohamed3000No ratings yet
- Retentive Aids in Maxillofacial ProsthesisDocument109 pagesRetentive Aids in Maxillofacial ProsthesisEnu KambojNo ratings yet
- Skin ScarringDocument5 pagesSkin ScarringjoshuaNo ratings yet
- Surgical Management of Complex Mandibular Fracture: Case ReportDocument5 pagesSurgical Management of Complex Mandibular Fracture: Case ReportlindaNo ratings yet
- Anaesthesia For Maxillofacial Trauma: Learning ObjectivesDocument7 pagesAnaesthesia For Maxillofacial Trauma: Learning ObjectivesMatthew MarionNo ratings yet
- Ijcmcr CR 00262Document4 pagesIjcmcr CR 00262ayoubNo ratings yet
- Pathophysiology: Laboratory StudiesDocument8 pagesPathophysiology: Laboratory Studiesrahma perwitasariNo ratings yet
- Clinical Case Reports - 2021 - Chybicki - Dental Implant Displacement Complicated by Epulis Fissuratum and ExtraoralDocument5 pagesClinical Case Reports - 2021 - Chybicki - Dental Implant Displacement Complicated by Epulis Fissuratum and ExtraoralMichelle VelezNo ratings yet
- Classification and Management of Acute Wounds and Open FracturesDocument5 pagesClassification and Management of Acute Wounds and Open FracturesRadenSiwi Bagus HadhiningratNo ratings yet
- Contribution of Dehydrated Amniotic Membrane in The Treatment of Recurrent Immunological Corneal Ulcer: Case ReportDocument4 pagesContribution of Dehydrated Amniotic Membrane in The Treatment of Recurrent Immunological Corneal Ulcer: Case ReportIJAR JOURNALNo ratings yet
- 222 PDFDocument2 pages222 PDFsumanth gowdaNo ratings yet
- Surgical Management of Orofacial Extensive Laceration: Case ReportDocument4 pagesSurgical Management of Orofacial Extensive Laceration: Case ReportAnonymous jfqzCfcI4ENo ratings yet
- Nutrition For A Healthy Mouth - Lippincott Williams & Wilkins 2nd Edition (March 27, 2009) PDFDocument370 pagesNutrition For A Healthy Mouth - Lippincott Williams & Wilkins 2nd Edition (March 27, 2009) PDFRishabh KapoorNo ratings yet
- An Unexpected Presentation of A Traumatic Wound On The Lower Lip: A CaseDocument5 pagesAn Unexpected Presentation of A Traumatic Wound On The Lower Lip: A CaseAnonymous jfqzCfcI4ENo ratings yet
- Saluran AkakrDocument8 pagesSaluran AkakranggiliaNo ratings yet
- Odontektomi Penatalaksanaan Gigi Impaksi SummaryDocument56 pagesOdontektomi Penatalaksanaan Gigi Impaksi SummaryAnonymous jfqzCfcI4ENo ratings yet
- Odontektomi Penatalaksanaan Gigi Impaksi SummaryDocument56 pagesOdontektomi Penatalaksanaan Gigi Impaksi SummaryAnonymous jfqzCfcI4ENo ratings yet
- Aleolar Osteitis Concepts and ControversiesDocument10 pagesAleolar Osteitis Concepts and ControversiesKunal Patel100% (1)
- Medoral 19 E467Document6 pagesMedoral 19 E467Anonymous jfqzCfcI4ENo ratings yet
- The Preservation of Alv Bone Ridge During Tooth ExoDocument9 pagesThe Preservation of Alv Bone Ridge During Tooth ExoPutri MortezaNo ratings yet
- Dictation. Fill in The Gaps With A Word From The ListeningDocument1 pageDictation. Fill in The Gaps With A Word From The ListeningNU MaseNo ratings yet
- Test I. True or False. Write TRUE If The Statement Is Correct and FALSE If The Statement Is IncorrectDocument2 pagesTest I. True or False. Write TRUE If The Statement Is Correct and FALSE If The Statement Is IncorrectMariecris Barayuga Duldulao-AbelaNo ratings yet
- 2018 State of The StateDocument26 pages2018 State of The StateRuss LatinoNo ratings yet
- Applying 5S ProceduresDocument70 pagesApplying 5S ProceduresSanta Best100% (3)
- Medicine List With DosageDocument9 pagesMedicine List With DosageonovNo ratings yet
- Public Toilet Awareness and AttitudeDocument24 pagesPublic Toilet Awareness and AttitudeWong Chiok Ling100% (10)
- Ambroxol PDFDocument2 pagesAmbroxol PDFmina zayNo ratings yet
- Health10 - Q4 - Mod1 (Lessons 1-4)Document40 pagesHealth10 - Q4 - Mod1 (Lessons 1-4)Merjie A. NunezNo ratings yet
- E The Real Facts Supporting Jeanne Calment As The Oldest Ever HumanDocument9 pagesE The Real Facts Supporting Jeanne Calment As The Oldest Ever Humanliz201177No ratings yet
- Safety Plan For Chemical PlantDocument7 pagesSafety Plan For Chemical PlantM Amir Haris100% (1)
- MCFP Catalogue 2016Document33 pagesMCFP Catalogue 2016bader_222_jo50% (2)
- Maxicare-Affiliated Providers - DOH-Certified Laboratories For COVID-19 Testing (Jan 22, 2021)Document2 pagesMaxicare-Affiliated Providers - DOH-Certified Laboratories For COVID-19 Testing (Jan 22, 2021)Marites BarnidoNo ratings yet
- A Village Square Lesson PlanDocument4 pagesA Village Square Lesson PlanShivaniNo ratings yet
- Master in Public Administration (MPA)Document106 pagesMaster in Public Administration (MPA)Mg OoNo ratings yet
- Employees' State Insurance Corporation E-Pehchan Card: Insured Person: Insurance No.: Date of RegistrationDocument3 pagesEmployees' State Insurance Corporation E-Pehchan Card: Insured Person: Insurance No.: Date of RegistrationSaikatNo ratings yet
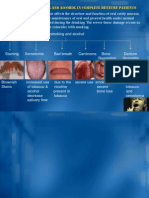
- Effects of Smoking and Alcohol On Complete Denture PatientsDocument2 pagesEffects of Smoking and Alcohol On Complete Denture PatientsAshwin ThejaswiNo ratings yet
- Altitude Diving PhysiologyDocument12 pagesAltitude Diving PhysiologyKarin Gandeswari100% (1)
- Global Safety Manual PDFDocument370 pagesGlobal Safety Manual PDFAdjira SayadNo ratings yet
- Miranda Miracell NewDocument2 pagesMiranda Miracell NewPablo FaldutiNo ratings yet
- Sonographic Evaluation of The DiaphragmDocument1 pageSonographic Evaluation of The DiaphragmAngelo LongoniNo ratings yet
- GayDocument15 pagesGayjulyerwanni100% (2)
- ED Produk KF - KF (Nama Apotek)Document19 pagesED Produk KF - KF (Nama Apotek)Eko FebryandiNo ratings yet
- Caries Risk Assesment: Disha Jandial Mds 1 Year Deptt. of Pediatrics and Preventive DentistryDocument134 pagesCaries Risk Assesment: Disha Jandial Mds 1 Year Deptt. of Pediatrics and Preventive Dentistrydisha 146jandial100% (1)
- REACH - Substances of Very High ConcernDocument3 pagesREACH - Substances of Very High Concerna userNo ratings yet
- PreviewpdfDocument62 pagesPreviewpdfImtiazAhmedNo ratings yet
- BinderDocument13 pagesBinderisabel carreauNo ratings yet
- AsthmaDocument10 pagesAsthmaAcohCChaoNo ratings yet
- Shofa Aji Setyoko (N101 12 051)Document4 pagesShofa Aji Setyoko (N101 12 051)ShofaajiNo ratings yet
- The Intentional Application of Humor With CKD PatientsDocument8 pagesThe Intentional Application of Humor With CKD PatientsKaryn BuxmanNo ratings yet
- US Embassy List of HospitalsDocument4 pagesUS Embassy List of HospitalsJay SorianoNo ratings yet
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (6)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeRating: 2 out of 5 stars2/5 (1)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (24)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (80)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (1)
- Self-Care for Autistic People: 100+ Ways to Recharge, De-Stress, and Unmask!From EverandSelf-Care for Autistic People: 100+ Ways to Recharge, De-Stress, and Unmask!Rating: 5 out of 5 stars5/5 (1)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- Gut: the new and revised Sunday Times bestsellerFrom EverandGut: the new and revised Sunday Times bestsellerRating: 4 out of 5 stars4/5 (392)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (44)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningFrom EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningRating: 4 out of 5 stars4/5 (3)
- Gut: The Inside Story of Our Body's Most Underrated Organ (Revised Edition)From EverandGut: The Inside Story of Our Body's Most Underrated Organ (Revised Edition)Rating: 4 out of 5 stars4/5 (378)
- To Explain the World: The Discovery of Modern ScienceFrom EverandTo Explain the World: The Discovery of Modern ScienceRating: 3.5 out of 5 stars3.5/5 (51)
- The Marshmallow Test: Mastering Self-ControlFrom EverandThe Marshmallow Test: Mastering Self-ControlRating: 4.5 out of 5 stars4.5/5 (58)