Professional Documents
Culture Documents
Mucormycosis Clinical Care Guidelines
Mucormycosis Clinical Care Guidelines
Uploaded by
Juhi Neogi0 ratings0% found this document useful (0 votes)
13 views1 pageThis document provides guidance on organizing clinical services for patients with both COVID-19 infection and rhino-orbito-cerebral mucormycosis at All India Institute of Medical Sciences, New Delhi. It outlines establishing a multidisciplinary mucormycosis team and categorizing patients based on COVID-19 status. It also lists sentinel signs and symptoms to monitor for progression of mucormycosis infection from nose to eyes to brain. Factors contributing to increased mucormycosis cases during the COVID-19 pandemic include diabetes exacerbation by COVID-19, immunosuppressive treatments for COVID-19, and co-infection leading to greater immune compromise. Principles of treatment include controlling underlying conditions,
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document provides guidance on organizing clinical services for patients with both COVID-19 infection and rhino-orbito-cerebral mucormycosis at All India Institute of Medical Sciences, New Delhi. It outlines establishing a multidisciplinary mucormycosis team and categorizing patients based on COVID-19 status. It also lists sentinel signs and symptoms to monitor for progression of mucormycosis infection from nose to eyes to brain. Factors contributing to increased mucormycosis cases during the COVID-19 pandemic include diabetes exacerbation by COVID-19, immunosuppressive treatments for COVID-19, and co-infection leading to greater immune compromise. Principles of treatment include controlling underlying conditions,
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
13 views1 pageMucormycosis Clinical Care Guidelines
Mucormycosis Clinical Care Guidelines
Uploaded by
Juhi NeogiThis document provides guidance on organizing clinical services for patients with both COVID-19 infection and rhino-orbito-cerebral mucormycosis at All India Institute of Medical Sciences, New Delhi. It outlines establishing a multidisciplinary mucormycosis team and categorizing patients based on COVID-19 status. It also lists sentinel signs and symptoms to monitor for progression of mucormycosis infection from nose to eyes to brain. Factors contributing to increased mucormycosis cases during the COVID-19 pandemic include diabetes exacerbation by COVID-19, immunosuppressive treatments for COVID-19, and co-infection leading to greater immune compromise. Principles of treatment include controlling underlying conditions,
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 1
All India Institute of Medical Sciences, New Delhi
Covid-19 Infection and Rhino-orbito-cerebral Mucormycosis
ORGANIZATION OF CLINICAL SERVICES
Treatment Organization & Guidance
• A multispecialty Mucormycosis Clinical team to be in place.
---------------------------------------------------------------------------------
Checklist of sentinel signs/ symptoms to be monitored
• To categorize patients as Covid +ve in patients admitted with Covid-19
& Covid –ve. ➢ Nose and sinuses Mucor infection (relatively early disease)
Admission as per above categorization Early detection at this stage can enable early treatment and minimize complications.
Many patients with Mucor are noted to be Covid RTpcr +ve at >10 • Headache and nasal obstruction- especially if persistent or severe and not responding to pain medicines.
• Nasal crusting and nasal discharge which could be brownish or blood tinged
days from onset • Pain or loss of sensation on face
This may represent immunecompromise related persistence of • Discolouration of skin of face / localised Facial puffiness
Covid infection. • Loosening of teeth/ discoloration or ulceration of palate
➢ Eye / Orbital Mucor infection ( moderately advanced disease
• Eye swelling or redness, double vision, loss of vision, Eye pain, drooping eyelid
Why the surge in Mucormycosis
➢ Intracranial infection (very advanced disease)-
• COVID-19 has tendency to worsen diabetes and also precipitate • II-VI Cranial nerve palsies (Cavernous sinus involvement) ; signs of MCA thrombosis
diabetes in previously normal individuals
Treatment principles-
• The Covid 19 infection itself is associated with leucopenia and
Urgent intervention to minimize progression and mortality/ loss of eye
may lead to immune compromise caused by impaired or
inappropriate immune responses. • Treatment of co-morbid illness/ blood sugar control & of Covid illness
• Immunosuppressive treatments are being widely used for
• To review Covid treatments to minimize immunocompromise
treatment of Covid-19 infection . • Twice daily evaluations as per Mucor Checklist above for progression to orbital/ intracranial involvement.
• Confirmation of Diagnosis by
• The severity of Mucor infection is largely dependent on the • KOH Smear/ Biopsy of involved lesion with appropriate precautions.
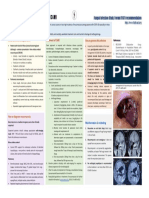
patient’s immunity and general health. • Radiology – CT/ MR for assessment of disease extent.
• Coexistence of Covid – 19 infection with high blood sugar levels, Radiological signs in the initial phase may often be subtle and minimal and may not demonstrate florid sinusitis and bone
erosion. Lack of these signs does not exclude the diagnosis
and immunosuppressive treatments would expectedly increase
incidence and severity of Mucormucosis. • Antifungal treatment with Amphotercin B/ Posaconazole.
• Mucor infection may occur during Covid-19 infection , or after a In situations of high clinical suspicion consider initiation of anti-fungal chemotherapy prior to microbiological confirmation
few weeks of apparent recovery from it. • Early surgical debridement after stabilization of systemic illness and ensuring facilities for post surgical care/ ventilation as anticipated.
For supplementary notes visit : https://drive.google.com/file/d/1Y8ENajpHbqWslZ3g6e60xJNdpf54PbQS/view?usp=sharing
You might also like
- 25 - Vvimp Interview QuestionsDocument14 pages25 - Vvimp Interview QuestionsBala RanganathNo ratings yet
- Jaguar X 350 Workshop ManualDocument6,470 pagesJaguar X 350 Workshop Manualekj100% (2)
- Ccu Del Del Ixj: Booking Reference: MF117JDocument4 pagesCcu Del Del Ixj: Booking Reference: MF117JJuhi NeogiNo ratings yet
- Ocular Manif. of HIVDocument75 pagesOcular Manif. of HIVPrabhjot SinghNo ratings yet
- Beechcraft Super King Air 350Document5 pagesBeechcraft Super King Air 350MikeNo ratings yet
- 1 - KMC-950 Service Manual (Eng) (V1.6)Document160 pages1 - KMC-950 Service Manual (Eng) (V1.6)Widen Carreño67% (3)
- Mini Lesson Lithium Ion Battery SafetyDocument2 pagesMini Lesson Lithium Ion Battery SafetyPRG ARMYNo ratings yet
- Long Covid - The Long Covid Book for Clinicians and Sufferers - Away from Despair and Towards UnderstandingFrom EverandLong Covid - The Long Covid Book for Clinicians and Sufferers - Away from Despair and Towards UnderstandingNo ratings yet
- MEASLESDocument34 pagesMEASLESmanibharathi100% (1)
- Rhino-Orbito-Cerebral Mucormycosis Guidance For Patients: What Are Alarming Symptoms To Watch For?Document1 pageRhino-Orbito-Cerebral Mucormycosis Guidance For Patients: What Are Alarming Symptoms To Watch For?Pappu JaiswalNo ratings yet
- Sars Cov-2 (Covid-19) : Coronavirus Disease (COVID-19) Is An Infectious Disease Caused by A Newly Discovered CoronavirusDocument6 pagesSars Cov-2 (Covid-19) : Coronavirus Disease (COVID-19) Is An Infectious Disease Caused by A Newly Discovered CoronavirusRIZANNEMARIEL BELZANo ratings yet
- COVID 19 Vaccines Training Modules Final Version For Cascading PDFDocument216 pagesCOVID 19 Vaccines Training Modules Final Version For Cascading PDFHerbert OmindeNo ratings yet
- If HP CDC Ipsm Covid 19 Imm OrientationDocument77 pagesIf HP CDC Ipsm Covid 19 Imm OrientationTheFisherman FriasNo ratings yet
- Clinical Management Protocol For Covid-19: (In Adults)Document22 pagesClinical Management Protocol For Covid-19: (In Adults)Ahmed TarigNo ratings yet
- Edited COVID19 HANDOUT Requina SindiongDocument5 pagesEdited COVID19 HANDOUT Requina SindiongJannen CasasNo ratings yet
- COVID-19 in Pediatric PatientsDocument61 pagesCOVID-19 in Pediatric Patientspriyanshu mathurNo ratings yet
- If HP CDC Ipsm Covid 19 Imm OrientationDocument105 pagesIf HP CDC Ipsm Covid 19 Imm OrientationGabrielNo ratings yet
- Neonatal Sepsis, Opthalmia Neonatarum & HIV/AIDSDocument15 pagesNeonatal Sepsis, Opthalmia Neonatarum & HIV/AIDSSAKSHI RANANo ratings yet
- Topic:: Assignment No 1Document8 pagesTopic:: Assignment No 1Adeel AfzalNo ratings yet
- GFDFDFDocument7 pagesGFDFDFRm98No ratings yet
- BinasCuevas InfographicsDocument1 pageBinasCuevas InfographicsRrjer CuevasNo ratings yet
- AJGP 10 2020 Clinical Khan Management Conjunctivitis Covid 19 WEBDocument6 pagesAJGP 10 2020 Clinical Khan Management Conjunctivitis Covid 19 WEByunni anggrainiNo ratings yet
- Ocular Tuberculosis: Lecture For Medical StudentsDocument19 pagesOcular Tuberculosis: Lecture For Medical Studentshenok birukNo ratings yet
- Ocular Manifestations of HIV Power PointDocument33 pagesOcular Manifestations of HIV Power Pointhenok birukNo ratings yet
- Covid 19 Training Tool v7.1 508Document73 pagesCovid 19 Training Tool v7.1 508Shonny Faith Montes OssioNo ratings yet
- Surgery in Covid-19 PandemicDocument49 pagesSurgery in Covid-19 PandemicEmmanuel DanielsNo ratings yet
- COVID-19 Protocol July 2022Document36 pagesCOVID-19 Protocol July 2022Mobile AsdNo ratings yet
- Anterior Segment ManifestationDocument25 pagesAnterior Segment ManifestationNatnaelNo ratings yet
- Pahonmhnvcovid 19200021 EngDocument7 pagesPahonmhnvcovid 19200021 EngBudi AnugrahNo ratings yet
- Covid 19 Training Tool v7.1 508Document73 pagesCovid 19 Training Tool v7.1 508ajNo ratings yet
- Clinical PracticeDocument10 pagesClinical PracticeCarlos AlvarezNo ratings yet
- Mucormycosis ManagementDocument3 pagesMucormycosis Managementparteek bajwaNo ratings yet
- NEJM Severe COVIDDocument10 pagesNEJM Severe COVIDErick Roa GandicaNo ratings yet
- 03NTD 2022 - COVID-19 VS DengueDocument66 pages03NTD 2022 - COVID-19 VS DengueInstitute for Clinical ResearchNo ratings yet
- JR3-Neurological Complications of Coronavirus Disease (COVID-19)Document28 pagesJR3-Neurological Complications of Coronavirus Disease (COVID-19)Riri DaynuriNo ratings yet
- Covid and Dental Care UpdatedDocument49 pagesCovid and Dental Care UpdatedShubham PatelNo ratings yet
- Respiratory Syndrome Coronavirus 2 (Sars-Cov-2) That Can Cause Symptoms From Common Cold ToDocument4 pagesRespiratory Syndrome Coronavirus 2 (Sars-Cov-2) That Can Cause Symptoms From Common Cold ToARISNo ratings yet
- Severe Covid-19: Clinical PracticeDocument10 pagesSevere Covid-19: Clinical Practicemarcelocarvalhoteacher2373No ratings yet
- BY JO1 Anton Steve Lim RN, Pgdip-Ts, Pgdip-SrmDocument49 pagesBY JO1 Anton Steve Lim RN, Pgdip-Ts, Pgdip-SrmDos LimNo ratings yet
- MoHP Protocol For COVID19 November 2020Document28 pagesMoHP Protocol For COVID19 November 2020medya dostorNo ratings yet
- 8.3 Opportunistic Infections in Children Living With HIV Part 2 - Viral & Protozoal OIs and HIV-TB Co-InfectionDocument54 pages8.3 Opportunistic Infections in Children Living With HIV Part 2 - Viral & Protozoal OIs and HIV-TB Co-Infectiondawalgari srivanireddyNo ratings yet
- Diabetes or Endocrinopathy Admitted in The COVID-19 Ward: Katrien Clotman Marcel B. TwicklerDocument5 pagesDiabetes or Endocrinopathy Admitted in The COVID-19 Ward: Katrien Clotman Marcel B. TwicklerElena MandrescuNo ratings yet
- COVID19Document79 pagesCOVID19Mohamad El SharNo ratings yet
- COVID-19 Training Slide Deck Updated 1 March 2020 UpdatedDocument124 pagesCOVID-19 Training Slide Deck Updated 1 March 2020 UpdatedUsama TareenNo ratings yet
- Severe Covid-19Document10 pagesSevere Covid-19Gabriela ArvelaezNo ratings yet
- Covid19 Antigen LectureDocument20 pagesCovid19 Antigen LectureUSI- CAMANO, JAY C.No ratings yet
- Bacterial ConjunctivitisDocument32 pagesBacterial ConjunctivitisYouhengNo ratings yet
- Clinical Case 04-2019 - by SlidesgoDocument103 pagesClinical Case 04-2019 - by SlidesgoJUVIELY PREMACIONo ratings yet
- Common Eye ConditionsDocument35 pagesCommon Eye ConditionsElukoti BhosleNo ratings yet
- Pharmacotherapy Handbook 9th Edition 476 489 INGDocument17 pagesPharmacotherapy Handbook 9th Edition 476 489 INGNyoman WiraNo ratings yet
- 1-Measles (Rubeola) PDFDocument37 pages1-Measles (Rubeola) PDFمصطفى رسول هاديNo ratings yet
- Covid 19 Training Tool v2 For Posting 060220 508Document75 pagesCovid 19 Training Tool v2 For Posting 060220 508bhaskarNo ratings yet
- Diseases of The Conjuctiva IIDocument37 pagesDiseases of The Conjuctiva IILydiah kawiraNo ratings yet
- Session 04 - Covid-19Document29 pagesSession 04 - Covid-19gbunyara100No ratings yet
- Long CovidDocument25 pagesLong CovidaisyarahmaNo ratings yet
- COVID-19 Patient Friendly EbookDocument55 pagesCOVID-19 Patient Friendly EbookYarmand WaqarNo ratings yet
- Measles: Symptoms, Treatment and Prevention: BY: JO1 Harold Jake Arguelles, RN Unit NurseDocument20 pagesMeasles: Symptoms, Treatment and Prevention: BY: JO1 Harold Jake Arguelles, RN Unit NurseTacloban City Jail-MD Health Service UnitNo ratings yet
- Incidence: Specific Types of UveitisDocument15 pagesIncidence: Specific Types of UveitisImatunnisaZiNo ratings yet
- Savira Fadila - Coronavirus Disease 2019 Presenting As ConjunctivitisDocument4 pagesSavira Fadila - Coronavirus Disease 2019 Presenting As Conjunctivitisbudi haryadiNo ratings yet
- Computed Tomographic Features of Pulmonary Mucormycosis Among Covid 19 Survivors A Diagnostic ChallengeDocument9 pagesComputed Tomographic Features of Pulmonary Mucormycosis Among Covid 19 Survivors A Diagnostic ChallengeInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Covid19 - Pathophysiology and ManagementDocument51 pagesCovid19 - Pathophysiology and ManagementMyraflor CaroNo ratings yet
- Viral Infection On HumansDocument29 pagesViral Infection On HumansMashimallowNo ratings yet
- Mucormycosis: Prof. David W. Denning Professor of Infectious Diseases in Global Health The University of Manchester, UKDocument27 pagesMucormycosis: Prof. David W. Denning Professor of Infectious Diseases in Global Health The University of Manchester, UKNarendra N NaruNo ratings yet
- FISF Recommendation MucormycosisDocument1 pageFISF Recommendation MucormycosisShivenra RajNo ratings yet
- Candidates' User Manual For Registration & Choice Filling: WB PG Medical Counselling 2021Document29 pagesCandidates' User Manual For Registration & Choice Filling: WB PG Medical Counselling 2021Juhi NeogiNo ratings yet
- CEE Final PresentationDocument7 pagesCEE Final PresentationJuhi NeogiNo ratings yet
- COMBINED SCREENING TEST - DR JuhiDocument9 pagesCOMBINED SCREENING TEST - DR JuhiJuhi NeogiNo ratings yet
- Part 1 MRCOG Eligibility Application Form: Section 1: Personal DetailsDocument6 pagesPart 1 MRCOG Eligibility Application Form: Section 1: Personal DetailsJuhi NeogiNo ratings yet
- Block Mountains Also Known As Mountain of UpliftmentDocument3 pagesBlock Mountains Also Known As Mountain of UpliftmentJuhi NeogiNo ratings yet
- Final Counselling Result PG 2021Document1,820 pagesFinal Counselling Result PG 2021Juhi NeogiNo ratings yet
- Cee Project-A ReportDocument4 pagesCee Project-A ReportJuhi NeogiNo ratings yet
- Brexit Is TheDocument9 pagesBrexit Is TheJuhi NeogiNo ratings yet
- At KumartuliDocument2 pagesAt KumartuliJuhi NeogiNo ratings yet
- AssignmentDocument2 pagesAssignmentJuhi NeogiNo ratings yet
- BarantiDocument5 pagesBarantiJuhi NeogiNo ratings yet
- As The Name SuggestsDocument2 pagesAs The Name SuggestsJuhi NeogiNo ratings yet
- Assessment (Soils of India)Document3 pagesAssessment (Soils of India)Juhi NeogiNo ratings yet
- 1001987548link of Advt With Inductus WebsiteDocument9 pages1001987548link of Advt With Inductus WebsiteJuhi NeogiNo ratings yet
- A Change of Heart: The Tryst Between Indian Surgeons and Heart TransplantsDocument4 pagesA Change of Heart: The Tryst Between Indian Surgeons and Heart TransplantsJuhi NeogiNo ratings yet
- 5pasteurization - WikipediaDocument12 pages5pasteurization - WikipediaCactusToastNo ratings yet
- BlueLineCatalogue EnglishDocument148 pagesBlueLineCatalogue Englishrohitkb09No ratings yet
- BS 812-118-1988 Testing Aggregates. Methods For Determination of Sulphate ContentDocument17 pagesBS 812-118-1988 Testing Aggregates. Methods For Determination of Sulphate ContentHaris KyriazisNo ratings yet
- Programming With FortranDocument114 pagesProgramming With FortranKalpesh KarkeliNo ratings yet
- The Component Object ModelDocument54 pagesThe Component Object ModelhssarochNo ratings yet
- PDF Yamaha PSR Gx76 CompressDocument39 pagesPDF Yamaha PSR Gx76 Compressdaniel123estradaNo ratings yet
- Sap MMDocument8 pagesSap MMharshali.allenticsNo ratings yet
- 1.1. TS 2Document4 pages1.1. TS 2design mepNo ratings yet
- Document (1) 1Document1 pageDocument (1) 1abdularejNo ratings yet
- Chapter 1 Lesson 1Document10 pagesChapter 1 Lesson 1NathanNo ratings yet
- Macro Economics: Euro Turns 20: Lessons From Two Decades of Single Currency SystemDocument17 pagesMacro Economics: Euro Turns 20: Lessons From Two Decades of Single Currency SystemNishan ShettyNo ratings yet
- OVR T1-T2 4L 12.5-275s P QS Surge Protective DeviceDocument3 pagesOVR T1-T2 4L 12.5-275s P QS Surge Protective DeviceSergio Moreno BarretoNo ratings yet
- Application WindowDocument2 pagesApplication Windowpatriciomaryrose557No ratings yet
- Stw20Nk50Z: N-Channel 500 V, 0.23 Ω, 20 A Supermesh™ Power Mosfet Zener-Protected In To-247 PackageDocument12 pagesStw20Nk50Z: N-Channel 500 V, 0.23 Ω, 20 A Supermesh™ Power Mosfet Zener-Protected In To-247 PackagemonikaNo ratings yet
- Cash Flow Estimation and Risk AnalysisDocument39 pagesCash Flow Estimation and Risk AnalysisRanyDAmandaNo ratings yet
- Front End StrategyDocument3 pagesFront End StrategyYik Tze ChooNo ratings yet
- Europe Vol4 PDFDocument36 pagesEurope Vol4 PDFJosé Antonio CabezaNo ratings yet
- List of Abbreviations: On A/C AllDocument64 pagesList of Abbreviations: On A/C AllDaryl fionnNo ratings yet
- Factorial AnovaDocument65 pagesFactorial AnovaFarhan FaheemNo ratings yet
- Unified Library Application: Laki Reddy Bali Reddy College of EngineeringDocument11 pagesUnified Library Application: Laki Reddy Bali Reddy College of EngineeringKumar GidwaniNo ratings yet
- Chapter+1 +the+Investment+SettingDocument18 pagesChapter+1 +the+Investment+SettingHakdog KaNo ratings yet
- 8.exercise (Ratio Analysis)Document10 pages8.exercise (Ratio Analysis)Fatema TujNo ratings yet
- Pipe Hanger Support Inspection Checklist P055BZOR-0051-Q-677Document1 pagePipe Hanger Support Inspection Checklist P055BZOR-0051-Q-677Thomas SebastianNo ratings yet
- Brazil BubbleDocument1 pageBrazil BubbleDanillo Gabriel NakanoNo ratings yet
- 21612Document3 pages21612Prashant27992No ratings yet