Professional Documents
Culture Documents
C. Liver Function Test (Child Pugh Criteria-To See Albumin and Bilirubin)
C. Liver Function Test (Child Pugh Criteria-To See Albumin and Bilirubin)
Uploaded by
Nadhirah ZulkifliOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
C. Liver Function Test (Child Pugh Criteria-To See Albumin and Bilirubin)
C. Liver Function Test (Child Pugh Criteria-To See Albumin and Bilirubin)
Uploaded by
Nadhirah ZulkifliCopyright:
Available Formats
All EOP medicine 2017/2018
GROUP A
SBAQ
2. 58 years old gentleman came to emergency with low conscius level. Vital
sign shows he is afebrile and normal vital sign. On physical examination, he is
clinically jaundiced, presencse of spider naevi on upper chest, abdomen was
grossly ascites however no hepatosplenomegaly.
What is the appropriate investigation to do at the presentation?
A. ABG
B. Coagulation Profile
C. Liver Function Test (child pugh criteria-to see albumin and bilirubin)
D. Random Blood Glucose
E. Renal Profile
?. 54 yo man with 3 months history of exertional dyspnoea. 9 pck yrs. no other
symptoms.
Physical examination shows bp 116mmhg, pr 86bpm, rr 18 bpm. On chest
examination, there was reduce air entry on lf lower zone which was dull on
percussion. Next best ix to confirm diagnosis.
A) Blood C&S
B) Chest radiograph (suspecting pleural effusion and lung collapse)
C) Pleural fluid cytology
D) Sputum C&S
E) Tumour marker
GENEZENS EOP GROUP A-D 2017/2018 Page 1
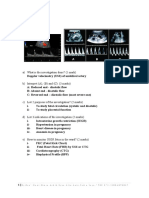
6. Bilaterally in the lower lungs field. cardiovascular system: S3 was heard at
the apex and displaced apex beat. There was pitting oedema of both lower
extremities. State the best management for the patient.
A. ACEis
B. Beta blocker
C. Dopamine
D. Frusemide(fluid overload)
E. Nitroglycerin
7. A 14 years old female presented with a complaint of small mouth since birth.
Patient had history of inability to close mouth but no difficulty in tongue
movement, speech and swallowing. No history of join pain. Past medical, dental
and family history was non-contributory. On examination patient was mildly
pallor. Extra oral examination revealed stiffening (fibrosis) of facial skin in
smooth, taut, and mask like appearance of face. Lips were rigid and
microstomia with fish beak. State the best statement about the presentation
A. Diagnosis is based on clinical manifestations
B. Disease characterized by progressive sin hardening and induration
C. Test and procedure may be used initially to confirm the diagnosis
D. the disease usually involved limited skin involvement
E. Disease in inherited.
8. A 25 years old man was admitted with the chief complaints of generalised
weakness of whole body, easy fatigability, difficulty in speaking, drooping of
both the eyelids for the past 9 months. All his symptoms used to beworse on the
exertion especialy in the evening hours. These complaints were associated with
diplopia on prolonged reading, fatigue on chewing, difficulty in swallowing
solid food and pain in the neck. On examination, his vital sign within normal
limits. There was ptosis and single breath counting up to 16. On systemic
examination the only abnormality detected was grossly reduced power in all the
GENEZENS EOP GROUP A-D 2017/2018 Page 2
muscle of the four limbs with normal reflexed, bilateral flexor planters and
intact sensory system. State the best diagnosis for the patient.
A. Amyotrophic lateral sclerosis
B. Lambert eaton syndrome
C. Multiple sclerosis
D. Myasthenia gravis
E. polymyositis
MEQ
Lan, 32yo gentleman u/l dm type 1 since 14yo
- dizziness, fever, cough, abd. pain, poor oral intake. 2days prior admission,
develop cough n fever. Treat w insulin
Pe: dehydrated, crepitation
Hb 4.3, hct 14.3, wbc 18000
Glucose 25, urea 10.2, creatinine 123, Na 152, K 6.3
Ph 6.5, pO2 98, pCO2 26
1. Investigation
Urine ketone-2+ , serum ketone- 3 mmol/L , VBG-HCO3- <15mmol/l
2. Triggering factor
Infection in this case
3. Causes of unconscious
A diabetic coma is a life-threatening diabetes complication that causes unconsciousness. If you have
diabetes, dangerously high blood sugar (hyperglycemia)
GENEZENS EOP GROUP A-D 2017/2018 Page 3
Causes
Blood sugar that's either too high or too low for too long may cause various serious
conditions, all of which can lead to a diabetic coma.
Diabetic ketoacidosis. If your muscle cells become starved for energy, your body
may respond by breaking down fat stores. This process forms toxic acids known as
ketones. If you have ketones (measured in blood or urine) and high blood sugar, the
condition is called diabetic ketoacidosis. Left untreated, it can lead to a diabetic coma.
Diabetic ketoacidosis is most common in type 1 diabetes but sometimes occurs in type
2 diabetes or gestational diabetes.
Diabetic hyperosmolar syndrome. If your blood sugar level tops 600 milligrams per
deciliter (mg/dL), or 33.3 millimoles per liter (mmol/L), the condition is called diabetic
hyperosmolar syndrome.
Severely high blood sugar turns your blood thick and syrupy. The excess sugar passes
from your blood into your urine, which triggers a filtering process that draws
tremendous amounts of fluid from your body. Left untreated, this can lead to life-
threatening dehydration and a diabetic coma. About 25 to 50 percent of people with
diabetic hyperosmolar syndrome develop a coma.
Hypoglycemia. Your brain needs glucose to function. In severe cases, low blood
sugar may cause you to pass out. Hypoglycemia can be caused by too much insulin or
not enough food. Exercising too vigorously or drinking too much alcohol can have the
same effect.
4. Diagnosis
Diabetic ketoacidosis secondary to infection
5. Management
IV normal saline 100ml/kg, 1 l in 1 hour , 1 l in 2 hour, 1 l in 4 hour , 1 l in 6
hour followed by IV insulin 0.1 unit/kg/hr followed by 1g KCL in 0.5l of
normal saline.
6. Complication
Hypoglycaemia, cerebral oedema, pulmonary oedema, vascular thrombosis,
hypokalemia
GENEZENS EOP GROUP A-D 2017/2018 Page 4
Group B
SBAQ
1. 35 year old , presented to the clinic with chronic productive cough , with
copious sputum . Affected by position . On auscultation, there is coarse
crepetations .
What is the likely diagnosis?
A. Bronchial asthma
B. Bronchiectasis
C. Bronchogenic carcinoma
D. Chronic bronchitis
E. Pulmonary tuberculosis
2. 74 year old man , presented with maneuvering problem since 4 month ago.
He has difficulty to get up from low seat and toilet .
What is the problem?
A. Poor fine finger movement
B. Poor rapid alternative movement
C. Distal muscle weakness
D. Proximal muscle weakness
E. Gait apraxia
GENEZENS EOP GROUP A-D 2017/2018 Page 5
3) 34 yr old gentleman recently travel to myanmar and had hiking activity
presented with fever, generalised body ache n low conscious level. On pe there
was splenomegaly noted. What is the most important appropriate ix?
A) blood culture n sensitvy
B) fbc
C) dengue serology
D) lepto serology
E) thick blood smear
4) a 60s age elrdy women presented with impair heel to toe test. What is the
likely cause of her gait abnormality?
A) cerebellar dysfunction
B) parietal lobe damage
C) temporal lobe damage
D) Ocular motor disturbances
E) Dysesthesias in the feet
5. 55 y/o women is being examined the clinician notices the presence of fine
twitching movement beneath the surface of the tongue and wasting of the one
side of the tongue. Select likely CN involved for this abnormality
A. V
B. VII
C. IX
D. X
E. XII
GENEZENS EOP GROUP A-D 2017/2018 Page 6
6. A 40 y/o lady gave history of weight gain and horseness of voice for the past
3 months. On examination her pulse was 64 b/min and her BMI: 30. Her skin
was pale, coarse and dry. Select most important diagnostic investigation
A. ACTH
B. Cortisol Level
C. Gonadotrophin levels
D. Insulin like growth factor
E. Thyroid function test (suspecting hypothyroidism)
7. A 70 y/o lady presented with history of fever and left sided chest pain for one
month. Her oxygen saturation was 91% under room air and her RR was 20
breaths per minute. Examination of respiratory system shows decreased chest
movements, stony dull percussion note and absence breath sounds on the left
side. select likely finding in her chest x ray.
A. Collapse
B. Consolidation
C. fibrosis
D. Pleural effusion (stony dull percussion)
E. Pneumothorax
GENEZENS EOP GROUP A-D 2017/2018 Page 7
8. 46 year old man with history of fever for the last 3 weeks associated with
cough, night sweats and weight loss. Chest examination was normal.
Abdominal examination revealed hepatosplenomegaly. Chest radiograph
revealed symmetrical fine nodules. Host sputum acid fast bacili was negative.
TB culture is pending. Select most likely diagnosis.
A) Miliary TB
B) Smear positive pulmonary TB
C) Malaria
D) Pneumonia
E) Sarcoidosis
9. A 81 years old gentleman, presented to ED with history of right sided body
weakness (sudden onset) On examination the bp is 180/100 mmHg and right
sided homonymous hemianopia. First line investigation?
A. Cerebral angiography
B. CSF Examination
C. CT Brain
D. Echocardiography
E. Hess Chart
10. An elderly man with history of asthma, CCF, Peptic ulcer admitted with
bronchospasm and rapid AF. He received frequent neb salbutamol and IV
digoxin loading, his regular medication were continued. One day after the
admission, serum potassium noted to be 2.8 mmol/L. Select medciation that
cause this abnormality.
A. Digoxin
B. ACEi (cause hyperkalemia)
C. Salbutamol (can cause hypokalemia)
GENEZENS EOP GROUP A-D 2017/2018 Page 8
D. Ranitidine
E. Spironolactone. (cause hyperkalemia)
OSCE 2
A lady came in with breathlessness. Given abg result.
Ph 7.44
Po2 55
Pco2 normal
Hco3 low
sat 84%
1. Abg technique
Wash your hands, introduce yourself to the patient and clarify their identity.
Explain what you would like to do and obtain consent. Let them know it will be
uncomfortable.
Position the patient’s arm with the wrist extended.
Locate the radial artery with your index and middle fingers.
Insert the needle at 30 degrees to the skin at the point of maximum pulsation of
the radial artery.
2. Interpret table
Normal pH, low PO2, normal PCO2, low HCO3- , low SPO2
3. Severity of aeba and why
??
4. Give 5 principles acute management of AEBA
A-secure airway-ensure patent
GENEZENS EOP GROUP A-D 2017/2018 Page 9
B-breathing-supplement patient oxygen if respi distress or usage of accessory
muscle or SPO2 less than 95% , give nebulized salbutamol 2.5mg with
ipratropium bromide 0.5mg
C-circulaton – draw blood for necessary investigation – do ABG to determine
T1RF or T2RF
Give patient oral prednisolone 30mg or IV hydrocort 200mg if patient cant
tolerate orally
IV MgSO4 2g
Group C
SBAQ
1) A 40 y/o man, non-smoker presented with several months of cough and
lower back pain and an 11kg weight loss. He was treated as pneumonia after a
CXR showed total opacification of the right lung.
Select the next step of investigation for this patient.
A. Bronchoscopy
B. CT Thorax
C. MRI spine
D. Serum calcium
E. Sputum AFB direct smear
2) An 18 y/o woman presented to her GP. She appears anxious and explains
she has been actively practicing for the coming sports game but suffered an
acute severe headache this morning which left her unable to work and she had
vomited several times. The headache is at occipital region and she noticed
some neck stiffness. She denies any recent travelling or fever. She appears
tearful but otherwise well, with no signs following a neurological examination.
The most likely diagnosis is
GENEZENS EOP GROUP A-D 2017/2018 Page 10
A. Tension headache
B. Migraine
C. SAH
D. Meningitis
E. Cervicogenic headache
3) A 56 y/o man presented to the ED for SOB and palpitations that began
acutely one hour ago. On PE, he is afebrile, BP 150/70mmHg, PR 175/min and
RR 30/min. Oxygen saturation is 99% with 5L/min oxygen by face mask. Cardiac
auscultation reveals an irregularly irregular rhythm, tachycardia and some
variability in S1 intensity. ECG demonstrates AF with rapid ventricular rate of
150 beats per min.
Which of the following is the most appropriate acute treatment?
A. Adenosine
B. Amiodarone
C. Cardioversion
D. Diltiazem
E. Metoprolol
4) A 35 y/o woman with NKMI complains of a sharp central chest pain that is
acutely exacerbated each time she moves, breathes in or lie flat. The pain is
mainly at central chest but occasionally radiates towards her neck and
shoulders. The pain is relieved by sitting forward. A pericardial rub is heard on
auscultation. The most appropriate diagnostic investigations is :
A. Cardiac MRI
B. ECG
GENEZENS EOP GROUP A-D 2017/2018 Page 11
C. Serum amylase
D. CXR
E. Echocardiography
5) A 39 y/o man complained of a 6 weeks hx of hemoptysis, night sweats and
LOW. CXR reveals some shadowing in the left upper zone. He is a 20 pack years
smoker and works at the construction site.
Select the most appropriate diagnostic investigation.
A. Blood cultures
B. CTPA
C. ESR
D. Ziehl-Nielson sputum staining
E. Mantoux test
6) A 20 y/o woman is brought into ED after she collapsed at her college. She
had stayed up all night for her friend’s celebration party. She describes sitting
at her desk and seeing multicoloured circles of light in her right visual field
then she woke up in the ambulance feeling confused and drowsy. Her
colleague who witnessed the event saw her collapse and start jerking both
arms and legs for 2 mins.
Select the best classification of the seizure’s semiology.
A. Focal non motor onset to bilateral tonic clonic
B. Focal non motor onset with impaired awareness
C. Focal motor onset with awareness
GENEZENS EOP GROUP A-D 2017/2018 Page 12
D. Generalized motor onset
E. Generalzied non motor onset
7) A 81 y/o man has a 4-day hx of profuse water diarrhea coupled with
abdominal pain. He was seen in the outpt clinic 2 weeks ago and was started
on oral amoxicillin for a lower respiratory tract infection. Stool and blood
cultures were normal. His observation are within normal range and the patient
is apyrexial.
Select the best treatment for this patient.
A. Oral vancomycin
B. Oral metronidazole
C. Oral ciprofloxacin
D. Oral PPI
E. Oral corticosteroids
8) A 69 y/o woman, who had completed 5 cycles of chemotherapy for
metastatic breast CA, presented to the ED complaining of feeling generally
unwell. On examination, she is pyrexia at 38.9℃ and pulse oximetry was 96%
on room air. There are crepitations in the right lung base.
Select the most important investigations.
A. FBC
B. CXR (Suspecting PCP)
C. Sputum acid fast bacilli
D. Blood cultures
E. ABG
GENEZENS EOP GROUP A-D 2017/2018 Page 13
9) A 50 y/o T2DM pt has been taking metformin and sulphonylurea with good
effect for the last 4 years and had maintained good glucose control. In the last
4 months, however, the pt has been persistently hyperglycemic depsite
optimal metformin and sulphonylurea dosage. His HbA1c latest is 9.5% and his
urine protein creatinine indext is increased.
The most appropriate management is
A. Thiazolidinedione
B. DPP-4 inhibitors
C. Rosiglitazones
D. Glucagon-like peptide-1 receptor agonist
E. Insulin
10) A 76 y/o man presents to the ED in a confused state accompanied by his
wife. She states that the pt has become increasingly obtunded in the last 3
days and has not opened his bowels for the same period of time. SHe mentions
he has been suffering from multiple myeloma, but it otherwise healhty. On
examination, the patient has brisk tendon reflexes, dry mucosal membrances,
reduced skin turgor and the eyes appear sunken.
Select the most appropriate management.
A. IV fluid and diuretics
B. Diuretics alone
C. IV calcitonin
D. Psychiatric referral
E. IV fluid resuscitation
GENEZENS EOP GROUP A-D 2017/2018 Page 14
MEQ
A 45 y/o housewife with no previous medical illness, presented with 2 months
hx of painful swelling of the joints asstd with fever and anorexia. This was
followed by rapid onset of swelling of the right elbow, left wrist, knees and IP
joints of both hands. She had lost 5 kg during the illness and started to develop
progressive difficulty to move her joints.
1) State ONE likely diagnosis. [2 marks]
- Rheumatoid arthritis
2) State TWO confirmatory investigations you would do. [4 marks]
ACPA (Anti-citrullinated protein antibody)
RF (Rheumatoid factor)
A GP that she consulted gave her some NSAID and referred her to the hospital.
Pain and swelling of the joint subsided with the tx. However, she only went to
hospital after a week with facial swelling and SOB asstd with reduced urine
output, nausea and vomiting.
Physical examination revealed ill looking lady with tachypnea. Her BP was
150/100mm Hg and pulse rate was 100 beats per min. There was facial
puffiness and gross ankle edema. Massive right sided pleural effusion noted
with the presence of ascites. Kidneys were not ballotable.
Blood investigations results are shown below.
FBC RP ABG UFEME
GENEZENS EOP GROUP A-D 2017/2018 Page 15
Hb - 8.5 g/dl Urea 35 pH - 7.05 Protein 4+
mmol/L
WCC - 9.5×109/L PCO2 - 52 mm Hg Pus cells 20-25
Na 139 mmol/L
Plt - 300×109/L HCO3 - 10 RBC 5-10
K 6.6 mmol/L
PO2 - 93 mm Hg
Cr 400 umol/L
*sPO2 98% on
room air
3) Describe the possible complications that have happened to her after the
visit to her GP. [4 marks]
AKI secondary to NSAID use/ Drug induced nephrotoxicity/acute interstitial
nephritis :
Mechanism - Reduced renal plasma flow caused by a decrease in
prostaglandins, which regulate vasodilation at the glomerular level
AKI result in uremia (reduced excretion of urea) - nausea, vomiting
RAAS is triggered d/t reduced renal perfusion - HPT, edema, reduced urine
output
Intravascular volume increased followed by rise in hydrostatic pressure -
NOTE : Acute interstitial nephritis
Usually caused by an adverse drug reaction
Characterised by small amounts of blood and protein in urine, often with leucocyturia
Kidneys are normal size
Requires cessation of drug and often prednisolone treatment
third space accumulation (ascite, pleural effusion)
GENEZENS EOP GROUP A-D 2017/2018 Page 16
4) List FIVE other important investigations you would do and give reasons for
each. [10 marks]
CXR - confirm pleural effusion, to exclude APO
Renal biopsy - confirm drug induced nephropathy (may show aggressive
glomerular inflammation, usually with crescent formation)
Ultrasound of the kidney- hydronephrosis and kidney size
Coagulation profile before pleural and peritoneal tap
5) Outline FIVE important management strategies for this lady. [5 marks]
- Cessation of the drug + prednisolone
- Correction of K using lytic cocktail
- Chest tube insertion for pleural effusion
- Correct the acidosis by giving HCO3-
- Supportive measures : oxygen therapy …
OSCE 1
A 53 y/o woman has been complaining of having dry cough for the past 3
months. However, for the past 1 week, she had blood stained sputum and right
sided chest pain. She was progressively SOB from mild exertion until at rest.
She had anorexia and LOW. She has been working as a police traffic for the last
20 years and is an ex-smoker (10 pack year).
On examination, she was clubbed and had absent breath sounds on the right
lower zone. There was stony dull to percussion.
Her sputum culture did not yield anything. Below is the CXR.
GENEZENS EOP GROUP A-D 2017/2018 Page 17
1) State TWO (2) abnormalities from the CXR. [2 marks]
Pleural effusion (loss of costophrenic angle and presence of meniscus sign)
Tracheal deviated to the left?
2) State THREE (3) possible causes for the above condition. [3 marks]
Bronchogenic carcinoma
Tuberculosis
Pneumonia
Pulmonary infarction
Scleroderma
3) State THREE (3) investigations for this condition. [3 marks]
Pleural fluid analysis
GENEZENS EOP GROUP A-D 2017/2018 Page 18
CT Thorax
Pleural biopsy
TB workout (Mantoux test, sputum for AFB, sputum culture]
4) State TWO (2) management outlines for this patient. [2 marks]
Therapeutic chest tube insertion
Treat the underlying cause : Anti-TB for TB, antibiotic for pneumonia,
multidisciplinary team management for bronchogenic carcinoma according
to the cell type and CA stage
OSCE 2
A 59 y/o male presented to the ED with non-specific chest discomfort for the
past 6 hours. Asstd sm included mild SOB, occasional palpitation and
abdominal discomfort. He was a smoker, with a past medical hx of T2DM and
HPT. He had no previous hx of heart disease or cardiac arrthythmias.
At the admission, HR was 110 beats/min, BP 114/53 mm Hg and temperature
36.8℃. PE was unremarkable.
The ECG was performed as below :
GENEZENS EOP GROUP A-D 2017/2018 Page 19
1) State TWO (2) ECG findings.[2 marks]
ST elevation at V1 and V2
ST depression at II and aVF , V4,V5,V6
2) State the diagnosis. [2 marks]
- Acute coronary syndrome
3) State TWO (2) further investigations. [3 marks]
Cardiac biomarkers (e.g. Troponin T)
Echocardiography
4) State TWO (2) managements outline. [3 marks]
Initial medical therapy which include : Oxygen, nitrate, antiplatelet, +/-
morphine
GENEZENS EOP GROUP A-D 2017/2018 Page 20
Reperfusion therapy : thrombolysis or PCI
GROUP D
SBAQ
1. 45 years old women was diagnosed with small cell lung cancer 8 weeks ago.
She now had difficulty climbing up stairs and getting off the toilet. On
examination there was bilateral proximal weakness of the upper and lower limb
with normal reflex. Select most likely diagnosis.
A. Brain metastasis
B. Dermatomyositis
C. polymyositis
D. Myasthenia gravis
E. Stroke
2. An 18 years old man had 4 days history of fever, photophobia and headache.
He was brought to the emergency department after he had generalised tonic
clonic seizure. On examination, he was confused and the kernig’s sign was
positive. There were no other focal neurological deficits. Select the best next
step of management for him.
A. intravenous ampicillin and acyclovir
B. Intravenous ceftriaxone and acyclovir
C. Electroencphalography
D. MRI of brain
E. No treatment until lumbar puncture is performed
3. A 60 years old smoker presented with recurrent episode of gastritis that were
not relieved with medication. on examination, he is cachectic and there was
GENEZENS EOP GROUP A-D 2017/2018 Page 21
mild tenderness over the epigastrium. Otherwise there is no other abnormal
finding. What is the most appropriate investigation.
A. Abdominal USS
B. Barium Swallow
C. ERCP
D. upper GI endoscopy
E. Urea breath test
4. A 42 years old women who developed oligomenorrhea, hirsuitism and acne
for 6 months. She subsequently developed back pain and was found to have a
compression fracture of the lumbar spine.what is next step investigation?
A. 24 h urine cortisol
B. Inferior pertrosal sinus sampling
C. MRI of pituitary gland
D. 48 h dexamethasone suppression test
E. CT of adrenal gland
5. a 40 years old smoker had a 12 h history of central chest pain that radiated to
the left arm. On examination he is pale and clammy, PP of 100 b/min and BP of
107/59 mmHg. ECG shows st depression in lead ii, iii, and avf. Select the best
cardiac biomarker in this patient.
A. Aspartate transaminase
B. B- type natriuretic peptide
C. CK MB
D. lactate dehydrogenase
E. Troponin T
GENEZENS EOP GROUP A-D 2017/2018 Page 22
6. A 20 years old college student with previously well controlled asthma came
with persistent symptoms for the past 6 weeks. She was using her short acting
bronchodilator every other days in past 3 weeks. On examination her lungs were
clear and her peak expiratory flow rate was 400 L/min. select best next
treatment option for her.
A. Add theophylline
B. Add inhaled LABA
C. Add inhaled Corticosteroid
D. Add short course of oral corticosteroid
E. switch to combination high dose inhaled corticosteroid long acting
bronchodilator.
7. A 78 years old man had shortness of breath with increase wheezing for the
past 7 days. he had worsening productive cough with chills and rigors. He was a
heavy smoker of 44 packs a years. On examination he was tachypneic and
confused. Other vital signs were normal. state the best empirical intravenous
antibiotic treatment.
A.IV penicillin
B. IV ceftriaxone
C. IV co amoxyclav
D. IV meropenem
E, IV piperacillin/ tazobactam
8. A 25 years old man was admitted for dry cough and SOB for the past 6
weeks. He was diagnosed with HIV 2 years ago but had not been to any follow
up. On examination he was febrile with oxygen saturation on room air of 95 %.
He had shorty cervical LN palpable but other system examination was
GENEZENS EOP GROUP A-D 2017/2018 Page 23
unremarkable. A chest Xray showed right upper lobe fibrotic changes. What is
likely diagnosis?
A. Pneumocytic jirovetcili pneumonia
B. Pulmonary TB
C. CAP
D. penicilliosis
E. Cryptococcosis
9. A 15 years old with previous history of asthma presented with pruritic skin
rash on the limbs. She was otherwise well with no systemic symptoms. Physical
examination showed excoriation and dry skin on flexure of the limbs. Select
most likely diagnosis?
A. Atopic eczema
B. Tinea cruris/corporis
C. Impetigo
D. Pemphigus foliaceous
E. Contact dermatitis
10. A 73 years old women came with acute renal failure. Her serum potassium
was 6.3 mmol/L and serum bicarbonate of 4 mmol/l. her ECG revealed tall
tented T waves. What is the next step in his management?
A. IV calcium gluconate
B. IV sodium Bicarbonate
C. IV Hartmann’s solution
D. IV normal saline
E. Haemodialyis
GENEZENS EOP GROUP A-D 2017/2018 Page 24
MEQ
A 21 years old women was brought to the ED after she was found unconscious
by her roommates. She had been complaining after she was found photophobia
for the last 3 days. Her friends also noticed a changes of behaviour. On
examination she was febrile and confused. Her reflex were brisk throughout.
Her CSF analysis revealed raised cell count predominantly lymphocytes.
However her CSF protein and glucose ratio normal
She developed a generalised Tonic clonic seizure more than 10 minutes upon
arrival to the red zone.
1. Provisional diagnosis
Encephalitis
2. Most likely organism
Herpes simplex virus, Japanese encephalitis virus , CMV,EBV,
autoimmune encephalitis such as anti-NMDA encephalitis, HIV
3. Analyse the immediate complication that had occurred
Status epilepticus (but should be more than 30 minutes?)
4. Explain your immediate management.
A- airway-check patent airway-put patient left lateral position
B- Breathing-supplement patient with oxygen if respi distress
C- Circulation-check the perfusion and put IV cannula and administer IV
lorazepam 2-4mg /IV diazepam 5-10mg or IM Midazolam 10mg if
difficult to set line
If still persists, IV phenytoin 15-20mg/kg / IV sodium valproate 20-
40mg/kg
Osce 1
(Picture of a triple lumens catheter)
1. Name the device. Internal jugular catheter
2. Where can it be inserted? Femoral vein, Right Internal jugular vein, Left
internal jugular vein
3. What are the indications? Haemodialysis, Central Line to administer fluid
and drugs , measurement of CVP, limited vascular access
GENEZENS EOP GROUP A-D 2017/2018 Page 25
4. What are the complications? Infection-catheter related blood stream infection
(CRBSI), bleeding or haematoma, thrombosis , air embolism
Osce 2
65 year old woman, admitted for minor procedure, she had ckd stage 5.
** Picture of tenkoff catheter
1) name this device (2marks)
Tenchkoff’s catheter
2) advantages (2marks)
Reduced risk of hypotension
Lower risk of blood transmitted infection such as Hep B,C,HIV
More independence and mobility
Can be managed at home
3) list 2 contraindications (4 marks)
Absolute contraindication: ileus, adhesion, intra abdominal pathology
Relative contraindication: suspected intra abdominal pathology, respi
distress, intra abdominal vascular graft
4) other alternative (2 marks)
Haemodialysis through arteriovenous fistula
Haemodialysis through internal jugular catheter
GENEZENS EOP GROUP A-D 2017/2018 Page 26
You might also like
- Крок-2 - студ - 18 - англDocument8 pagesКрок-2 - студ - 18 - англAimeeNo ratings yet
- PracticeExam 3 QsDocument17 pagesPracticeExam 3 QsBehrouz YariNo ratings yet
- 02 GRAT - HemodynamicsDocument4 pages02 GRAT - HemodynamicsjuanNo ratings yet
- Paper 1B MedicalDocument22 pagesPaper 1B MedicalAina SakinaNo ratings yet
- Medicine A Supply 2022: Course of Oral Steroids. On Examination There Is Point Tenderness On Upper Lumber SpineDocument8 pagesMedicine A Supply 2022: Course of Oral Steroids. On Examination There Is Point Tenderness On Upper Lumber SpineRabia RabiaNo ratings yet
- (IM) End-Posting Examination Questions (G4)Document13 pages(IM) End-Posting Examination Questions (G4)Hamud RashydNo ratings yet
- KGMC BLOCK L 2023. Revisedd (Follow Yellow)Document29 pagesKGMC BLOCK L 2023. Revisedd (Follow Yellow)noorNo ratings yet
- PracticeExam 2 QsDocument24 pagesPracticeExam 2 QsBehrouz YariNo ratings yet
- EMQs For Medical Students Volume 3 2eDocument16 pagesEMQs For Medical Students Volume 3 2ePasTestBooks50% (2)
- Boron Intrebari Pentru Evaluare enDocument42 pagesBoron Intrebari Pentru Evaluare enAna0% (1)
- Endocrinology Question 1Document16 pagesEndocrinology Question 1BasirQidwai100% (4)
- 2023 MayDocument36 pages2023 MayReshma Shaji PnsNo ratings yet
- Heme QuestionsDocument28 pagesHeme QuestionsChenthanKrishNo ratings yet
- Swammy Plab 1 MockDocument32 pagesSwammy Plab 1 Mockfreelancer08No ratings yet
- Endo QuizDocument3 pagesEndo Quizمصطفى محمد جواد كاظمNo ratings yet
- TBL PaedsDocument10 pagesTBL PaedsHo Yong WaiNo ratings yet
- Medicine/Medicine 4th Year 2016Document25 pagesMedicine/Medicine 4th Year 2016abmad t45No ratings yet
- Plab-1 1700 MCQs Solved With Explanation (Shared by Ussama Maqbool)Document729 pagesPlab-1 1700 MCQs Solved With Explanation (Shared by Ussama Maqbool)Omar Abo el nagaNo ratings yet
- Appeal 2020Document79 pagesAppeal 2020mohammadeidNo ratings yet
- CP PPQsDocument5 pagesCP PPQsJenny LowsleyNo ratings yet
- Asculitis Syndromes: Emily B. Martin, MD Rheumatology Board Review April 9, 2008Document54 pagesAsculitis Syndromes: Emily B. Martin, MD Rheumatology Board Review April 9, 2008Miguel M. Melchor RodríguezNo ratings yet
- High-Yield Endocrine Q&ADocument9 pagesHigh-Yield Endocrine Q&ALillian Bezares100% (1)
- Acute Pancreatitis Case PresDocument29 pagesAcute Pancreatitis Case Preskristine keen buanNo ratings yet
- H مشDocument13 pagesH مشTareq EmadNo ratings yet
- Eng 2006 MedDocument43 pagesEng 2006 MedLucia BogNo ratings yet
- MCQ Maret 2021Document16 pagesMCQ Maret 2021promkes poloNo ratings yet
- Nbme 2 Block 1-4Document112 pagesNbme 2 Block 1-4lk0704No ratings yet
- NBME 1 RatioDocument87 pagesNBME 1 RatioBugs Caslib100% (1)
- NEPHRO Allergo ExamDocument5 pagesNEPHRO Allergo ExamAllison Eunice ServandoNo ratings yet
- MCQ Nas 2 Januari 2020Document13 pagesMCQ Nas 2 Januari 2020OlgHaENo ratings yet
- 2006Document60 pages2006Anatoliy ShchurovskiyNo ratings yet
- Stat Pearls 10 McqsDocument16 pagesStat Pearls 10 McqsFatimaNo ratings yet
- 5th Year 112 PediatricsDocument12 pages5th Year 112 PediatricsAmjad A. Amir100% (2)
- S4 Neuro MCQ 8pgs Jan 2014Document8 pagesS4 Neuro MCQ 8pgs Jan 2014FlowerNo ratings yet
- MCQsDocument21 pagesMCQsZweNo ratings yet
- 7th March 2020 Plab 1 MockDocument32 pages7th March 2020 Plab 1 MockZoha QureshiNo ratings yet
- 2019 Explanation k2Document261 pages2019 Explanation k2berdaderagaNo ratings yet
- Late HIV Stage PresentationDocument29 pagesLate HIV Stage PresentationAdis GudukasaNo ratings yet
- Roru Exoendo - PancreasDocument13 pagesRoru Exoendo - PancreasRitz CelsoNo ratings yet
- MBCHB Year 4 Canvas Resource QuestionsDocument12 pagesMBCHB Year 4 Canvas Resource QuestionsharshaNo ratings yet
- HUEC 2011 Cardio Case StudiesDocument6 pagesHUEC 2011 Cardio Case StudiesShanica Paul-RichardsNo ratings yet
- Mrcs Part-A Online Preparatory Course Mock Exam-1 Paper - 2Document26 pagesMrcs Part-A Online Preparatory Course Mock Exam-1 Paper - 2Rami RaedNo ratings yet
- First Part Exam - Feb 2020Document16 pagesFirst Part Exam - Feb 2020hassan mohamedNo ratings yet
- (IM) End-Posting Examination Questions (G5)Document11 pages(IM) End-Posting Examination Questions (G5)Hamud RashydNo ratings yet
- UVA QuestionsDocument61 pagesUVA QuestionsjhhjjhNo ratings yet
- CASE 25: Acute PancreatitisDocument3 pagesCASE 25: Acute PancreatitisJeanine Angela CuliliNo ratings yet
- Renal PediatricDocument48 pagesRenal PediatricEslam R. Almassri100% (1)
- (IM) End-Posting Examination Questions (G3)Document16 pages(IM) End-Posting Examination Questions (G3)Hamud RashydNo ratings yet
- 2 - Med - Endocrine MCQs - SGDocument33 pages2 - Med - Endocrine MCQs - SGOsman Somi50% (2)
- EndocrinologyDocument15 pagesEndocrinologySafayet HossainNo ratings yet
- Kidney Quiz - Path Exam 3Document15 pagesKidney Quiz - Path Exam 3tatti9990% (1)
- H كدا صارDocument13 pagesH كدا صارTareq EmadNo ratings yet
- MKSAP13-Hematology and OncologyDocument261 pagesMKSAP13-Hematology and OncologyimanNo ratings yet
- RENALDocument10 pagesRENALbhagavan prasadNo ratings yet
- Renal ReviewDocument10 pagesRenal ReviewZen Lenin CaroNo ratings yet
- MRCP - PART ONE - PassMedicine 2020 - EndocrinologyDocument676 pagesMRCP - PART ONE - PassMedicine 2020 - EndocrinologyNadhirah ZulkifliNo ratings yet
- I-Hysterosalpingogram (HSG) /laparoscopic Dye Test Day 2/3 Serum FSH and LH or Day 21 Serum ProgesteroneDocument33 pagesI-Hysterosalpingogram (HSG) /laparoscopic Dye Test Day 2/3 Serum FSH and LH or Day 21 Serum ProgesteroneNadhirah ZulkifliNo ratings yet
- MRCP - PART ONE - PassMedicine 2020 - EndocrinologyDocument676 pagesMRCP - PART ONE - PassMedicine 2020 - EndocrinologyNadhirah ZulkifliNo ratings yet
- 11th Teacher, 2nd EditionDocument213 pages11th Teacher, 2nd EditionNadhirah ZulkifliNo ratings yet
- ST RD ST RD NDDocument13 pagesST RD ST RD NDNadhirah ZulkifliNo ratings yet
- Doing Well: For: Doctor: Date: Doctor's Phone Number: Hospital/Emergency Department Phone NumberDocument2 pagesDoing Well: For: Doctor: Date: Doctor's Phone Number: Hospital/Emergency Department Phone NumberNadhirah ZulkifliNo ratings yet
- Syifaa'.Wani - Shera.Achik - Syaa.Alin - Anis.Fatin - Yaya. THE 9 X-VIBRANT2017Document23 pagesSyifaa'.Wani - Shera.Achik - Syaa.Alin - Anis.Fatin - Yaya. THE 9 X-VIBRANT2017Nadhirah ZulkifliNo ratings yet
- CNS MEQ Part 2Document2 pagesCNS MEQ Part 2Nadhirah ZulkifliNo ratings yet
- PP Teaching RoundDocument2 pagesPP Teaching RoundNadhirah ZulkifliNo ratings yet
- Psy Cwu 1Document18 pagesPsy Cwu 1Nadhirah ZulkifliNo ratings yet
- Approach To Anaemia & HaematuriaDocument2 pagesApproach To Anaemia & HaematuriaNadhirah ZulkifliNo ratings yet
- Psy Cwu 2Document12 pagesPsy Cwu 2Nadhirah ZulkifliNo ratings yet
- Short Cases in Clinical Exams of Internal Medicine (PDFDrive)Document185 pagesShort Cases in Clinical Exams of Internal Medicine (PDFDrive)Nadhirah ZulkifliNo ratings yet
- 5 Obstructive Jaundice EditedDocument33 pages5 Obstructive Jaundice EditedNadhirah ZulkifliNo ratings yet
- Curs 1 2015 DZDocument44 pagesCurs 1 2015 DZIoana DiaconuNo ratings yet
- Diabetes and It's Oral ManifestationsDocument28 pagesDiabetes and It's Oral ManifestationsYashpreetsingh BhatiaNo ratings yet
- DM Report1Document16 pagesDM Report1Wendy EscalanteNo ratings yet
- Diabetes MellitusDocument12 pagesDiabetes MellitusANANo ratings yet
- Stress Hyperglycemia: Anand MosesDocument4 pagesStress Hyperglycemia: Anand MosesDaeng Arya01No ratings yet
- Case Study 2 - DM Type 2Document13 pagesCase Study 2 - DM Type 2Jilkiah Mae Alfoja CampomanesNo ratings yet
- Metabolic Effects of The Consumption of Areca: CatechuDocument8 pagesMetabolic Effects of The Consumption of Areca: CatechuveniNo ratings yet
- DM Egregious ElevenDocument18 pagesDM Egregious ElevendavidtuanandartuaNo ratings yet
- Anti DiabeticDocument132 pagesAnti DiabeticvelangniNo ratings yet
- The Effects of Lifestyle For The Management of Patient With Diabetes Mellitus Type 2Document33 pagesThe Effects of Lifestyle For The Management of Patient With Diabetes Mellitus Type 2EduNo ratings yet
- Group 5 - English - A14-A KeperawatanDocument11 pagesGroup 5 - English - A14-A KeperawatanNi luh ade dwi AntariNo ratings yet
- Diabetes Mellitus: Nhamier M. Jikiri, RN, MD, FPCP Internal MedicineDocument27 pagesDiabetes Mellitus: Nhamier M. Jikiri, RN, MD, FPCP Internal MedicineNursidar Pascual MukattilNo ratings yet
- Treatment Based On: Pathophysiology of HyperglycemiaDocument38 pagesTreatment Based On: Pathophysiology of HyperglycemiaRoby KieranNo ratings yet
- Maintenance and Replacement Fluid Therapy in AdultsDocument10 pagesMaintenance and Replacement Fluid Therapy in AdultsJosé Carlos SantosNo ratings yet
- 2017 Steroid Tapering Guideline Cancer NHS Foundation TrustDocument1 page2017 Steroid Tapering Guideline Cancer NHS Foundation TrustArdan MirazNo ratings yet
- 02 Tatalaksana Terapi Insulin - Prof Tri Murti AndayaniDocument39 pages02 Tatalaksana Terapi Insulin - Prof Tri Murti AndayaniEndang Wulan SariNo ratings yet
- Practice in Clinical BiochemistryDocument112 pagesPractice in Clinical BiochemistryMohamed Magdi100% (1)
- Diabetes Manual - A Guide To Diabetes ManagementDocument243 pagesDiabetes Manual - A Guide To Diabetes ManagementDrsarfaraz SiddiquiNo ratings yet
- Glucose Tolerance TestDocument27 pagesGlucose Tolerance Testsiya sharmaNo ratings yet
- Clinical Chemistry Notes With BlanksDocument34 pagesClinical Chemistry Notes With Blanksepson printerNo ratings yet
- Pediatric Type 1 Diabetes MellitusDocument25 pagesPediatric Type 1 Diabetes MellitusmuhammadferhatNo ratings yet
- Diabetic Pregnancy Outcome ThesisDocument138 pagesDiabetic Pregnancy Outcome ThesisDr. Parvez Hassan0% (1)
- Sps. Flores v. Sps. PinedaDocument7 pagesSps. Flores v. Sps. PinedaRachel CayangaoNo ratings yet
- Insulin and Glucagon: Dr.R.Prameela MD Assistant Professor of PharmacologyDocument31 pagesInsulin and Glucagon: Dr.R.Prameela MD Assistant Professor of PharmacologyRamadi PrameelaNo ratings yet
- Medical-Surgical Nursing Care: Caring For Clients With Diabetes MellitusDocument90 pagesMedical-Surgical Nursing Care: Caring For Clients With Diabetes MellitusJonalynCollodChewacheoNo ratings yet
- REVIEW 2023 AUBF Basics On Chemical Tests For UrineDocument84 pagesREVIEW 2023 AUBF Basics On Chemical Tests For UrineJheshari VinaNo ratings yet
- NCP Diabetes Mellitus Prepregnancy GestationalDocument12 pagesNCP Diabetes Mellitus Prepregnancy GestationalRichson BacayNo ratings yet
- Iron ToxicityDocument35 pagesIron ToxicityMohamed El-sayedNo ratings yet
- Short Guide Clinical NutritionDocument30 pagesShort Guide Clinical Nutritiontopiq100% (1)
- Diabetes in Elderly Adults: Graydon S. Meneilly and Daniel TessierDocument9 pagesDiabetes in Elderly Adults: Graydon S. Meneilly and Daniel Tessierdita prameswariNo ratings yet