Professional Documents
Culture Documents
DD LEPTOSPIROSIS - Id.en
Uploaded by
Andi Nirwana Widya Ningsih Honre0 ratings0% found this document useful (0 votes)
8 views6 pagesOriginal Title
5. DD LEPTOSPIROSIS.id.en
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
8 views6 pagesDD LEPTOSPIROSIS - Id.en
Uploaded by
Andi Nirwana Widya Ningsih HonreCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 6
Translated from Indonesian to English - www.onlinedoctranslator.
com
5. What are the differential diagnosis related to the scenario ?
A. Leptospirosis
a. Definition
Leptospirosis is a zoonotic disease caused by a spiral-shaped bacterial
infection of the genus Leptospira which is pathogenic, transmitted directly and
indirectly from animals to humans. Leptospira bacteria are spiral-shaped with
hook-like ends, measuring 5-15 micrometers long and 0.1-0.2 micrometers
wide, flexible, thin and flexible. The disease is most commonly transmitted
from animals to humans when people with open skin sores come into contact
with water or soil that has been contaminated with animal urine. Animals that
are the source of leptospirosis transmission are rats, pigs, cows, goats, sheep,
horses, dogs, cats, insects, birds, insectivores (porcupines, bats, squirrels),
while foxes can be carriers of leptospira.
b. Epidemiology
Leptospirosis occurs in various parts of the world but generally in
tropical and subtropical areas with high rainfall. Leptospirosis is an endemic
disease in a number of countries and even in the world. Generally human cases
of Leptospirosis are reported from India, Indonesia, Thailand and Sri Lanka
during the rainy season. Major outbreaks of Leptospirosis in the Southeast
Asian region have been reported in Jakarta (2003), Mumbai (2005) and Sri
Lanka (2008). Based on reports of recent years, the global incidence of
Leptospirosis cases is estimated from 0.1-1 per 100,000 per year in temperate
climates and 10-100 per 100,000 per year in the humid tropics. The incidence
of this disease can reach more than 100 per 100,000 per year in outbreaks and
exposure is high in risk groups.
In 2007 there was an increase in cases of Leptospirosis in humans,
reported as many as 667 cases and 93% confirmed laboratory results with an
8% mortality rate. In 2010 cases of Leptospirosis in Indonesia were reported as
many as 410 cases with 46 deaths (CFR 11.2%). The number of male patients
with leptospirosis is higher than female.
c. Etiology
Leptospirosis is caused by pathogenic organisms of the genus
Leptospira which are included in the order Spirochaeta in the
Trepanometaceae family. This bacterium is spiral-shaped with a tight twist
and the ends are shaped like hooks so that the bacteria are very active in both
rotating movements along their axis, back and forth, or curved. The size of
these bacteria is 0.1 mm x 0.6 mm to 0.1 mm x 20 mm. Leptospira can be
stained with carbolfuchsin stain. However, these bacteria can only be seen
with a dark field microscope. These bacteria are obligate aerobes with optimal
growth at a temperature of 280C-300C and a pH of 7.2 to 8.0.
The genus Leptospira is divided into two serovarians, namely L.
interrogate which is pathogenic (i.e. has the potential to cause disease in
animals and humans) and L. biflexa which is non-pathogenic/saprophytic (i.e.
free-living and generally considered not to cause disease). Pathogenic
leptospires are maintained in nature in the renal tubules and genital tracts of
certain animals.
Various animal species, especially mammals, can act as a source of
human infection, including:
1. Small mammal species, such as wild rats (including mice, porcupine
squirrels)
2. Domestic animals (cows, pigs, dogs, sheep, goats, horses, buffalo)
3. Fur-producing animals (silver fox) in captivity
4. Reptiles and amphibians may also carry leptospires
d. Clinical Manifestations
According to Widoyono (2008), clinical symptoms of leptospirosis in
humans can be divided into three stages, namely:
a. First Stage (leptospiremia)
1. Fever, chills
2. Headache
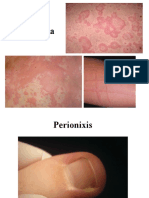
3. Red spots on the skin
4. Malaise and vomiting
Conjunctivitis and redness of the eyes
Pain in the muscles, especially the calf and back muscles.
5. These symptoms will appear between 4-9 days
b. Second Stage
1. At this stage, antibodies are usually formed in the patient's body
2. The symptoms that appear at this stage are more varied than in the first
stage, including jaundice (yellowness)
3. If the fever and other symptoms reappear, meningitis is likely
4. Usually this phase lasts for 4-30 days.
c. Third Stage
According to some clinicians, this disease can also show clinical
symptoms in the third stage (convalescent phase). Complications
Leptospirosis can cause the following symptoms:
1. In the kidneys, renal failure that can cause death
2. In the eyes, closed conjunctiva represents a septicemic phase which is
closely related to photobia and hemorrhagic conjunctiva.
3. In the liver, jaundice (yellowing) that occurs on the fourth and sixth day
with an enlarged liver and soft consistency
4. In the heart, arrhythmias, dilatation of the heart and heart failure that can
cause sudden death
5. In the lungs, hemorrhagic pneumonitis with coughing up blood, chest
pain, respiratory distress and cyanosis
6. Bleeding due to vascular damage from the respiratory tract, digestive
tract, kidneys and genital tract
Infection in pregnancy causes abortion, stillbirth, premature birth and
birth defects.
e. Supporting investigation
Diagnosis can be made by microscopic examination, as well as
by leptospira culture. The clinical sample that should be collected for
examination depends on the phase of the infection. Specimens came
from blood and cerebrospinal fluid (first week of illness) and urine
(after the first week to day 40). The specimens were grown on
Fletcher's media or EMJH media in combination with neomycin or 5-
fluorouracil. On this medium, growth will be seen within a few days to
4 weeks. The presence of leptospires in this medium can be seen using
a dark field microscope or using a fluorescent microscope
(fluorerescent antibody stain). Immunoserological testing is also
important for the diagnosis of leptospirosis. In general, new antibodies
are found after the 7th or 10th day. The titer will increase and will peak
at the 3rd or 4th week of illness. The immunoserological tests
commonly used are: Microscopic Agglutination Test, Enzymelinked
immunosorbent assay (ELISA), polymerase chain reaction (PCR) and
dipstick assays, as well as Leptospira-specific antigen, namely
lipoprotein rLipl32 which can be the gold standard for diagnosis.
The most useful and most frequently collected samples are:
1. Blood with heparin for culture in the first 10 days.
2. Blood or frozen serum for serological examination is taken in
the septicemic phase. The diagnosis is based on a 4-fold
antibody seroconversion between acute and convalescent. A
negative serological result in the early stages of the disease does
not exclude the diagnosis of leptospirosis.
3. Urine for culture is taken in the immune phase.
4. Post mortem samples. It is important to collect specimens from
as many organs as possible for serology. Post mortem samples
should be collected aseptically and inoculated into the culture
medium as soon as possible after death. Samples should be
stored and transported at 4°C. In addition, crust staining,
immunostaining, and immunohisto-chemistry may be helpful.
5. CSF and dialysate for culture were taken in the septicemic
phase. In the case of an-icteric leptospirosis, normal leukocyte
counts with neutrophilia, increased erythrocyte sedimentation
rate (ESR) and protein in the CSF can be found.
f. Management
a) Medicine
Severe cases of leptospirosis should be given high doses of IV
penicillin (IV benzylpenicillin 30 mg/kg, maximum 1.2 g, 6 hours for
5-7 days). Milder cases may be treated with oral antibiotics such as
amoxicillin, ampicillin, doxycycline (2 mg/kg, maximum 100 mg,
every 12 hours for 5-7 days), or erythromycin.
b) Supportive therapy and dialysis
Severe cases require hospitalization with aggressive supportive
care and close monitoring of fluid and electrolyte balance. Peritoneal
dialysis or hemodialysis is indicated in renal failure. Good supportive
care and dialysis have reduced the mortality of this disease in recent
years. If prothrombin is disturbed, vitamin K can be given.
g. Complications
Aseptic meningitis is the most common complication, but encephalitis,
myelitis, radiculitis, peripheral neuritis (unusual) in the second week may
occur due to a hypersensitivity reaction. Severe complications in patients with
severe leptospirosis can be in the form of shock, massive bleeding and ARDS
which is the main cause of death for severe leptospirosis. Shock occurs due to
changes in body homeostasis that play a role in the onset of tissue damage.
Renal failure, liver damage, pulmonary hemorrhage, vasculitis and cardiac
disorders in the form of myocarditis, pericarditis and arrhythmias are rarely
found although they are common causes of death. Although rare, uveitis can
be found after 2 years of symptoms of leptospira.
h. Prognosis
Mortality in severe leptospirosis is about 10%, death is most often due
to kidney failure, massive bleeding or ARDS. Liver and kidney function will
return to normal, despite severe dysfunction, even in patients on dialysis.
About a third of cases with aseptic meningitis may experience periodic
headaches. Some patients with a history of leptospirosis uveitis experience
loss of visual acuity and blurred vision.
i. Prevention
According to Rusmini (2011) in general, the prevention of leptospirosis
that can be done is as follows:
1. Familiarize yourself with Clean and Healthy Life Behavior (PHBS)
2. Wash hands with soap before eating and drinking.
3. Use clean water for bathing and washing.
4. Vegetables and fruit should be washed with clean water.
5. Store food properly and correctly to avoid the reach of rats (closed
tightly, put in the cupboard).
6. Use footwear, especially when activities outside the home.
7. Avoid contact with sewer water or standing water, both in the home
environment and at work.
8. Avoid contact with flood waters.
9. Bathing and washing hands, feet and body parts with soap after work,
especially when in fields/gardens/trash cans/soil/sewers and other
polluted places.
10. Protecting body parts with personal protective equipment (PPE) when
working in a place where there is a risk of contamination.
11. Cover the wound on the skin with a waterproof wound dressing.
12. Avoid the presence of mice in the house or workplace.
13. Avoid pollution and improve rat control.
14. Set a mousetrap.
15. Bury or burn rat carcasses in a safe place.
16. Immediately check with the available health facilities if you experience
symptoms
sick.
Reference :
1. Setadi, B., Setiawan, A., Effendi, D. & Hadinegoro, SRS Practical Instructions for
Leptospirosis. Sari Pediatr. 3, 163–167 (2001).
2. Rampang, NH Leptospirosis Novie H. Rampengan. J. Biomedicine 8, 143–150 (2016).
3. Sitohang, RV, Burni, E., Gasem, MH & Muhadir, A. Instructions for Leptospirosis Control
Techniques. Ministry. health. RI 126 (2017).
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5796)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Modul 2 ImunologiDocument16 pagesModul 2 ImunologiAndi Nirwana Widya Ningsih HonreNo ratings yet
- Faculty of Medicine Makassar, 12 November 2021 Indonesian Muslim University Tropical BlockDocument63 pagesFaculty of Medicine Makassar, 12 November 2021 Indonesian Muslim University Tropical BlockAndi Nirwana Widya Ningsih HonreNo ratings yet
- 12B - Modul 1Document33 pages12B - Modul 1Andi Nirwana Widya Ningsih HonreNo ratings yet
- 12B - Modul 1-1Document62 pages12B - Modul 1-1Andi Nirwana Widya Ningsih HonreNo ratings yet
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (589)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1091)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Female Sexual Dysfunction: Reference: Tog Article 2021Document14 pagesFemale Sexual Dysfunction: Reference: Tog Article 2021Rania AHNo ratings yet
- Amok Syndrome: A Current Reality?Document5 pagesAmok Syndrome: A Current Reality?Sabrina JonesNo ratings yet
- Oral and Maxillofacial Pathology3rd EdDocument986 pagesOral and Maxillofacial Pathology3rd EdPavithra RathinaSwamyNo ratings yet
- PDF Nursing Care PlanDocument16 pagesPDF Nursing Care PlanMichael MabiniNo ratings yet
- FOUNDATIONDocument5 pagesFOUNDATIONKuya RogieNo ratings yet
- Notes On R.A. 11332Document4 pagesNotes On R.A. 11332paolo llegoNo ratings yet
- KROK 1 EXPLANATIONS MicrobiologyDocument18 pagesKROK 1 EXPLANATIONS MicrobiologyAkpene Racheal100% (1)
- Guidelines On Sports Cardiology and - ExerciseDocument80 pagesGuidelines On Sports Cardiology and - ExerciseBruno S. Homem De FariaNo ratings yet
- Margaret A. NewmanDocument21 pagesMargaret A. NewmanLois PabionNo ratings yet
- Sleep Disorder Literature ReviewDocument4 pagesSleep Disorder Literature Reviewea53sm5w100% (1)
- Nursing Case Study Chronic CholecystitisDocument22 pagesNursing Case Study Chronic CholecystitisShairalyn Catada100% (1)
- Recapitulare TestDocument38 pagesRecapitulare TestDana ChitoiNo ratings yet
- ArthritisDocument8 pagesArthritissharon wanjikuNo ratings yet
- The Nature of Suffering and The Goals of NursingDocument140 pagesThe Nature of Suffering and The Goals of NursingGusni FitriNo ratings yet
- Oral Pathology: Dr. Tasnim Hamdan Graduated From University of ValenciaDocument160 pagesOral Pathology: Dr. Tasnim Hamdan Graduated From University of ValenciaMariam Abd ElhadiNo ratings yet
- 100 Item Comprehensive Exam II With Answers and RationaleDocument16 pages100 Item Comprehensive Exam II With Answers and RationaleVJ DeeNo ratings yet
- Acute Cellulitis and Erysipelas in Adults - Treatment - UpToDateDocument34 pagesAcute Cellulitis and Erysipelas in Adults - Treatment - UpToDateBrian VianaNo ratings yet
- General Principles of Bone TumorsDocument6 pagesGeneral Principles of Bone TumorsRonald TejoprayitnoNo ratings yet
- Oncogenic VirusesDocument25 pagesOncogenic VirusesMedicina 19No ratings yet
- 05 Szasz and TorreyDocument14 pages05 Szasz and Torreyscribd4kmhNo ratings yet
- CSF Examination - Najaf Ali Ansari - BSMLS-F20-206Document11 pagesCSF Examination - Najaf Ali Ansari - BSMLS-F20-206Bilal Latif100% (1)
- 3.1 Midwifery & Gynaecology Nursing Papers QPDocument14 pages3.1 Midwifery & Gynaecology Nursing Papers QPTapobrata Sarkar100% (1)
- Unit 4 ReadingDocument4 pagesUnit 4 ReadingElvantNo ratings yet
- Providing Safe Food and The Phillipine Food Safety FrameworkDocument38 pagesProviding Safe Food and The Phillipine Food Safety Frameworkjanelleallab15No ratings yet
- Homeopathy vs. Allopathy vs. AyurvedaDocument30 pagesHomeopathy vs. Allopathy vs. AyurvedaMSKCNo ratings yet
- Hyperthyroidism in Children and Adolescents: What Is The Thyroid Gland?Document3 pagesHyperthyroidism in Children and Adolescents: What Is The Thyroid Gland?Neha ReddyNo ratings yet
- Memo and MinutesDocument3 pagesMemo and MinutesJennifer BeguinwaNo ratings yet
- Buletin Kesehatan Heat StressDocument2 pagesBuletin Kesehatan Heat Stresspaul g doloksaribu100% (1)
- Medical RecordDocument8 pagesMedical RecordKusumadewi WidiarsaNo ratings yet
- Pharmacology Book 2Document63 pagesPharmacology Book 2Ahmed AbdullahNo ratings yet