Professional Documents
Culture Documents
en Papilla Vaters Tumor in Elderly An Inter
Uploaded by
Ayip Bahsan AlBantaniOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
en Papilla Vaters Tumor in Elderly An Inter
Uploaded by
Ayip Bahsan AlBantaniCopyright:
Available Formats
CASE REPORT
Papilla Vater’s Tumor in Elderly: an Interdisciplinary Issue
Eric Daniel Tenda*, Murdani Abdullah **, Kuntjoro Harimurti***,
Edy Rizal Wahyudi ***, Czeresna Heriawan Soejono***
* Department of Internal Medicine, Faculty of Medicine University of Indonesia
Dr. Cipto Mangunkusumo General National Hospital, Jakarta
** Division of Gastroenterology, Department of Internal Medicine, Faculty of Medicine
University of Indonesia/Dr. Cipto Mangunkusumo General National Hospital, Jakarta
*** Division of Geriatric, Department of Internal Medicine, Faculty of Medicine
University of Indonesia/Dr. Cipto Mangunkusumo General National Hospital, Jakarta
ABSTRACT
Tumors of the papilla Vater are very rare. Papilla Vater’s tumors are benign or malignant tumors in
the ampulla of Vater and periampullary region. Blockage of ampulla leads to the development of obstructive
jaundice; intermittent cholangitis, epigastric discomfort and weight loss. Treatment possibilities include
endoscopic ampulectomy, surgical transduodenal excision of tumors of the ampulla and pancreatoduodenectomy
(PDE). Prognosis depends on histological typing of the tumor and their clinical stage. We report a case of papilla
Vater’s tumor in elderly with comorbidities based on literature review.
A 68-year-old female patient was referred for evaluation of intra and extra hepatic bile duct dilatation noted
on abdominal ultrasonography. She complained of intermittent epigastric and right upper abdominal pain, with
yellowish skin for two months. The laboratory findings showed leukocytosis, hyperbilirubinemia, abnormal liver
function test, and high Ca 19-9. An endoscopic retrograde cholangiopancreatography (ERCP) revealed a distal
obstruction caused by papilla Vater’s tumor. Abdominal computed tomography (CT) with contrast, revealed
a dilated common bile duct and pancreatic duct. The histologic evaluation was highly suggestive for dysplasia.
She is now on a schedule for a Whipple procedure.
To make a true diagnosis and optimal treatment of papilla Vater’s tumor is multimodal. By doing
a comprehensive geriatric assessment, with a careful modality selection, a Whipple procedure can be performed
in elderly (65 years) safely. The post operative morbidity and mortality depends on their multi morbidity. Surgical,
endoscopic, or radiologic biliary decompression; relief of gastric outlet obstruction; and adequate pain control
may improve the quality of life but do not affect overall survival rate. By building a great interdisciplinary
teamwork, the quality of life increased as follows.
Keywords: papilla Vater tumor, elderly, Whipple procedure
INTRODUCTION duodenum are neuroendocrine tumors (NETs), such
Papilla Vater’s tumors are benign or malignant as somatostatinomas and carcinoid tumors. Carcinoid
tumors in the ampulla of Vater and periampullary tumors arise from enterochromaffin cells, and
region. These represent 1.5% of gastrointestinal gastrointestinal carcinoids are usually located in the
(GI) tract tumors with incidence about 6 million/ appendix, ileum, stomach, and rectum; only 8 cases
year.1 Tumors of the papilla Vater are very rare; have been reported in the literature.2
the majority of tumors of the minor papilla of the Blockage of ampulla leads to the development
of obstructive jaundice; intermittent cholangitis,
epigastric discomfort and weight loss. Frequently
Correspondence: the patient underwent an endoscopy, endosonography,
Murdani Abdullah contrast enhanced computed tomography (CT) and
Division of Gastroenterology, Department of Internal Medicine
Dr. Cipto Mangunkusumo General National Hospital endoscopic retrograde cholangiopancreatography
Jl. Diponegoro No. 71 Jakarta 10430 Indonesia (ERCP).2
Phone: +62-21-3153957 Fax: +62-21-3142454
E-mail: murdani@hotmail.com
Volume 11, Number 3, December 2010 155
Eric Daniel Tenda, Murdani Abdullah , Kuntjoro Harimurti, Edy Rizal Wahyudi , Czeresna Heriawan Soejono
Treatment possibilities include endoscopic prominent with a tumor, cholangiogram showed an
ampulectomy, surgical transduodenal excision of enlargement of CBD, intra and extra hepatic duct. From
tumors of the ampulla and pancreatoduodenectomy pancreatogram, the main pancreatic duct (MPD) was
(PDE). Tumors arising from the papilla of Vater have nonvisualized. The conclusion for this ERCP was, there
a better prognosis than carcinomas of the pancreas and is a distal obstruction of CBD at causa papilla Vater’s
bile duct, and it has quite a different pathological nature tumor (figure 2). Multiple deep biopsies taken from this
from these tumors.3 Prognosis depends on histological nodule during ERCP. The pathologic findings revealed
typing of the tumor and their clinical stage and maybe highly suggestive dysplasia duodenum mucosal. Under
associated with an excellent prognosis, and if the the diagnosis of a tumor of the papilla Vater, the patient
tumor is limited to the duodenal mucosa without any underwent double pigtail 10 Fr stenting procedure at
invasion into the adjacent pancreas then the five-year the CBD (figure 3).
survival may be as high as 90%. Prognosis for patients
with carcinoma of papilla Vater is better than other
periampullary tumors. The overall survival after the
Whipple operation for pancreatic adenocarcinoma is
about 20 percent at five years after surgery. Patients
without spread of cancer into their lymph nodes may
have up to 40% survival.1-3
CASE ILLUSTRATION
A 68-year-old female was referred to our department
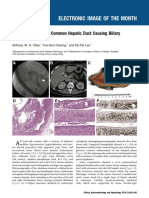
for evaluation of dilatation of the main pancreatic duct, Figure 1. Abdominal ultrasonography showed enlargement of intra
intra and extra hepatic biliary duct, with a double hepatic, extra hepatic and common bile duct
duct sign, noted on abdominal ultrasonography (US).
She complained of intermittent right upper quadrant
and epigastric pain 2 months prior to admissions,
followed by yellowish skin, and dark brown colored
urine. She also complained about nausea, vomiting
and low dietary intake during 2 weeks prior to referral.
The patient had a history of hepatic abscess. She did not
drink alcohol or smoking or any particular medications
and denied sweating and diarrhea. Laboratory data on
admission were as follows: total bilirubin 31.6 mg/
dL, aspartate aminotransferase (AST) 97 U/L, alanine
transaminase (ALT) 39 U/L, alkaline phosphatase
(ALP) 1,014 U/L, and gamma glutamyl transpeptidase
(GGT) 806 U/L. The complete blood count showed
leukocytosis 12,100/mm3, neutrophil segment 85,
Figure 2. ERCP showed distal obstruction of CBD at causa papilla
and hypoalbuminemia 2.5 mg/dL. Serum electrolytes Vater’s tumor
were within normal limits. On the fourth days of
hospitalization, the patient underwent ERCP that
showed a distal obstruction of the biliary duct. The CA
19-9 was 8,378 U/mL. On the CT scan, the pancreatic
duct was diffusely dilated without a definite mass and
the common bile duct was dilated.
The abdominal US revealed a dilatation at intra and
extra hepatic biliary and common bile duct (CBD);
sludge in gall bladder. There was no sign of pancreatic
duct enlargement. The summary from this examination
was enlargement of intra and extra hepatic biliary duct
and CBD (figure 1). On the CT scan, the pancreatic
duct was diffusely dilated without a definite mass
and the common bile duct was slightly dilated, with
a non specific hepatomegaly, and no sign of lymph
Figure 3. ERCP showed double pigtails stenting 10 Fr at common
nodes enlargement. Endoscopy showed papilla Vater’s bile duct
156 The Indonesian Journal of Gastroenterology, Hepatology, and Digestive Endoscopy
Papilla Vater’s Tumor in Elderly: an Interdisciplinary Issue
DISCUSSION (TNF-alpha) due to local infections. Treatment for pain
A classical carcinoid tumor is usually still referred to and dyspepsia has to commence at once.
as a carcinoid tumor. The incidence of gastrointestinal From the laboratory studies, blood biochemistry,
carcinoids is 1.6-2.0 cases per 100,000 persons/ test for anemia caused by occult bleeding from
year, but the prevalence maybe higher.2 Qiao et the ampullary mass. Hyperbilirubinemia conjugated
al reported ampullary carcinomas accounting for type, rise in serum ALT, AST, and alkaline phosphatase
approximately 0.2% of all tumors in GI tract types can level due to blockage of the biliary outflow and biliary
be found in this area originating from the duodenal obstructions. As seen in this patient, we found there
mucosa or from the bile duct or the pancreatic duct.3 is a slight anemia, hyperbilirubinemia, rise in AST
The etiology of the disease is poorly understood. and ALT. Currently, no tumor marker is sensitive or
Patients with familial adenomatous polyposis (FAP) specific enough to serve as a reliable screening tools
have an increased risk of both benign and malignant for this case. Carbohydrate antigen (CA) 19-9 is
papilla Vater’s tumor. Most of these tumors are the most studied and sensitive marker for
resectable for cure at diagnosis; however, the 5-years pancreatobiliary neoplasms at present. In this case
survival rate is only approximately 40-67% at best. the CA 19-9 is 8,378 U/mL.
Operative mortality rates have decreased significantly Abdominal US is the most useful noninvasive initial
over the last decade because of increased surgical investigations for distinguishing medical from surgical
experience, improved anesthesia, better preoperative causes of jaundice and we can identify dilated ducts,
imaging and interdisciplinary pre and post operative liver metastasis (in almost 90% cases), ascites and nodal
management. Post operative mortality rates in our metastasis. The level of obstruction can be assessed in
hospital are 20% and at the best centers are 1-2%. 90% patient, as seen in this case. The limitation of
A higher rate of ampullary tumor is observed in male. abdominal ultrasound is the effectiveness related to the
Ampullary tumor or cancer most often seen in the fifth skill of the user, very superficial lesions and very deep
through the seventh decades of life.4 In this case, our lesions may be missed. Distinguishing a metastasis
patient is a 68 years old female. from a hemangioma may be difficult, sensitivity is
The tumor or carcinoma of the ampulla of Vater 80-90%, and information is inferior to that obtained
is part of the spectrum of periampullary carcinomas, by CT scan or magnetic resonance imaging (MRI).
usually present with jaundice, and abdominal pain.1,2 Poor bowel preparation may obscure the important
Jaundice is the presenting symptom in 73% of pathology. It has been found to be a diagnostic tools
resected patients and in 80% of unresected patients of ampulla of Vater carcinoma only in 23.8% cases.
in the 28-year experience published by Talamini In this case, the cause of distal obstruction at CBD
et al.4 Jaundice may intermittently wax and wane are not seen in this modalities. CT is a noninvasive
because of central necrosis and sloughing or pressure procedure. CT scan is superior to US but inferior to
opening of an obstructed duct. Other clinical features endoscopic ultrasound (EUS) for tumor or carcinoma
include progressive weight loss in 61% cases, as seen of the ampulla of Vater unless extensive tumor is
in this case. Abdominal pain and back pain were present. CT scan is better in evaluating resectability
present in 46% and it is usually dull, aching mid and preoperative staging. It gives better assessment of
epigastric pain or right hypochondric pain, and back invasion, encasement, or compression of vessels and
pain may be a sign of advanced stage. In this case, adjacent organs. CT-guided biopsy may be obtained
there is an abdominal pain and radiating back pain. when mass lesions are present, but endoscopic biopsy
At the third day of hospitalization, the patient was taking is preferred. In this case, CT revealed an enlargement
a nonsteroidal anti-inflammatory drugs to relieve of CBD and no sign of mass or space occupying lesions
the pain. There is a significant progress from the visual in pancreas, metastasis and lymph nodes enlargement.
analog score, from 7 to 1. Pruritus associated with ERCP allows diagnostic and therapeutic access
jaundice in 13-38% cases. Dyspepsia and vomiting to both the common bile duct and pancreatic duct.
may be present if compromise of the duodenal lumen The procedure displays the details of ductal anatomy
leads to gastric outlet obstructions, and can contribute and accurately demonstrates the level and nature of
to loss of appetite. In this case, there is a dyspepsia and the obstruction. Anatomical variations in ducts can
loss of appetite.4 At the first day of hospitalizations, be evaluated carefully4. In this case, the side viewing
with good collaborations with nutritionist, we give endoscopy revealed the papila Vater’s tumor that
blenderized diet through nasogastric tube. Proton pump cause the obstruction of distal CBD. ERCP allows
inhibitors and pro kinetic drugs were also be given to therapeutic procedures, such as sphincterotomy,
the patient. As we know there is an interaction between stenting, and nasobiliary drainage. In this case, stent
pain and dyspepsia, because of the pro inflammatory double pigtails was placed and it reveals a good
reactions that enhance tumor necrosis factor alpha progression for hyperbilirubinemia. Endoscopic
Volume 11, Number 3, December 2010 157
Eric Daniel Tenda, Murdani Abdullah , Kuntjoro Harimurti, Edy Rizal Wahyudi , Czeresna Heriawan Soejono
excision of small periampullary tumors is gaining in survival rate of patients who underwent radical
popularity. It permits sampling of pancreatic juice, bile, resection was 49%. They concluded that local resection
and brush/grasp biopsy. The ERCP disadvantage is an is recommended only for small, benign tumors and
invasive procedure that requires an expert endoscopist for patients who may be unfit for radical surgery;
or radiologist and a cooperative patient. Very small otherwise, pylorus-preserving PDE is safe and the most
tumors (< 1 cm) can be missed. ERCP is not possible effective procedure.7
if access to the duodenal papilla is difficult to obtain Interdisciplinary management including: (1)
because of diverticula, anatomical ductal variations, Assessment of nutritional status and supplementation.
or prior surgical bypass.4 Consultations with nutritionist to provide patient
The surveillance epidemiology and end result education regarding postgastrectomy diet; (2)
(SEER) database indicates adenocarcinoma is Intravenous antibiotic prophylaxis; (3) Fluid and
the most frequently identified histology for papilla electrolyte correction; (4) Assessment of coagulation
Vater’s cancer. Adenocarcinoma not otherwise specific profile and correction of decreased prothrombin time by
(NOS) was reported in 65% of cases. Carcinoma administration of vitamin K in patients with advanced
NOS was reported in 8.1%; adenocarcinoma arising jaundice; (5) Preoperative biliary drainage in jaundiced
from adenoma (adenocarcinoma in villous adenoma, patients is indicated in patients with cholangitis
in tubulovillous adenoma, in adenomatous polyp and and those with profound hyperbilirubinemia as this
villous adenocarcinoma) was third most common, may impact coagulation status and wound healing.
reported in 7.5%. Other pathologic diagnosis reported Preoperative stenting may be associated with increased
included papillary adenocarcinoma (5.6%), mucinous postoperative infectious complications; (6) Standard
adenocarcinoma (4.7%), and signet ring cell carcinoma treatment for dyspepsia and loss of appetite with
(2%). In this case the specimen from papilla Vater’s a comprehensive management of pain; (7) Assessment
tumor was taken during ERCP. The conclusion from of cardiac, renal, and pulmonary status; (8) Medical
histologic finding is high grade dysplasia of duodenum rehabilitations interventions usually, for patients
mucosa.4 experiencing pre or postoperative deconditioning, most
Surgical resection of an ampullary carcinoma commonly experienced postoperative complications or
is the primary modality of treatment. The highest had preexisting conditions e.g. pain; (9) Assessment of
cure rates are achieved if the tumor is localized to the patient mental status and supportive psychotherapy
the ampullary region and complete resection is especially for patient with adjustment disorders or
achieved. Diagnostic staging laparoscopy may be depressions.
indicated to avoid laparotomy in the setting of advanced Carcinoid tumors of the papilla Vater’s are very
disease with distant occult metastasis. PDE Whipple rarely found, but the true incidence might be much
is the standard procedure. Pylorus preserving PDE or higher, and the tumors frequently have aggressive
classic Whipple can be performed depending on extent behavior. Carcinoid tumors of the papilla Vater’s
of tumor and surgeon preference. With improvement should be included in the differential diagnosis of
in interdisciplinary postoperative management and recurrent abdominal pain, cholangitis or pancreatitis
surgical technique, operative mortality rates are as of unknown cause. By doing a comprehensive geriatric
low as 1% in experienced centers. 5 Resectability assessment, with a careful modality selection, this case
rates for ampullary carcinoma was up to 96% in can have a good prognostic future.
the 1990s.6 Local resection (ampullectomy) may be PDE is the treatment of choice not only for
considered for patients with an ampullary adenoma ampullary carcinoma but also for adenoma with
with absence of dysplasia on preoperative biopsies high grade dysplasia also for elderly persons in good
who are inappropriate candidates for PDE. Recurrence somatical status;1 for frail unfit persons with distant
rate is high in this population; therefore, surveillance metastases or miscellaneous contraindications for
endoscopy is indicated. Extensive preoperative surgery remains endoscopic sphincterotomy and
assessment of cardiac, respiratory, renal, and cerebral stenting a valid alternative of palliative treatment.
functions should be performed in older patients or With good teamwork and interdisciplinary
those with comorbid conditions. Toh et al reported 25 management with comprehensive geriatric assessment,
patients (13 male, 12 female) with a median age of 65 the treatment or palliative care and quality of life can
years who had an ampullary tumor. The resectability increase.
rate was 88%, with no operative mortality. The 5-years
158 The Indonesian Journal of Gastroenterology, Hepatology, and Digestive Endoscopy
Papilla Vater’s Tumor in Elderly: an Interdisciplinary Issue
REFERENCES Lillemoe KD, et al. Adenocarcinoma of the ampulla of Vater.
1. Kala Z, Weber P, Hemmelová B, Marek F, Hlavsa J, Sobotka A 28-year experience. Ann Surg 1997;225:590-600.
M. Ampullary tumours (ampullomas) in the elderly-an 5. Nafisa KK, Pankaj C, Ronald SC, Venkata SK, Uma C,
interdisciplinary problem. Indian J Med Res 2010;131:418-21. Gunateet G, et al. Carcinoma of the ampulla of Vater.
2. Kim YG, Kim TN, Kim KO. Carcinoid tumor of the minor Emedicine online: Carcinoma of the gastrointestinal tract
papilla in complete pancreas divisum presenting as recurrent (cited 2010 Nov 01). Available from URL: http://www.
abdominal pain. BMC Gastroenterology 2010;10:7. emedicine.medscape.com/article/282920-overview.
3. Qiao QL, Zhao YG, Ye ML, Yang YM, Zhao JX, Huang YT, 6. Cameron JL. One thousand consecutive pancreatico-
et al. Carcinoma of the ampulla of Vater: factors influencing duodenectomies and beyond: a personal series. Am J Surg
long-term survival of 127 patients with resection. World J 2007;194:S11-5.
Surg 2007;31:137-46. 7. Toh SK, Davies N, Dolan P, Worthley C, Townsend N,
4. Talamini MA, Moesinger RC, Pitt HA, Sohn TA, Hruban RH, Williams JA. Good outcome from surgery for ampullary
tumour. Aust N Z J Surg 1999;69:195-8.
Volume 11, Number 3, December 2010 159
You might also like
- Endoscopic Ultrasound Management of Pancreatic Lesions: From Diagnosis to TherapyFrom EverandEndoscopic Ultrasound Management of Pancreatic Lesions: From Diagnosis to TherapyAntonio FacciorussoNo ratings yet
- Diagnosis and Management of Klatskin Tumor: April 2010Document6 pagesDiagnosis and Management of Klatskin Tumor: April 2010Feby Kurnia PutriNo ratings yet
- Colitis: A Practical Approach to Colon and Ileum Biopsy InterpretationFrom EverandColitis: A Practical Approach to Colon and Ileum Biopsy InterpretationAnne Jouret-MourinNo ratings yet
- Primary Congenital Choledochal Cyst With Squamous Cell Carcinoma: A Case ReportDocument6 pagesPrimary Congenital Choledochal Cyst With Squamous Cell Carcinoma: A Case ReportRais KhairuddinNo ratings yet
- It Is Not Always A Cholangiocarcinoma: Unusual Peritoneal Carcinomatosis Revealing Gastric AdenocarcinomaDocument5 pagesIt Is Not Always A Cholangiocarcinoma: Unusual Peritoneal Carcinomatosis Revealing Gastric AdenocarcinomaIJAR JOURNALNo ratings yet
- 492 568 1 SMnjsjsdjsDocument4 pages492 568 1 SMnjsjsdjsZidna MazayatulNo ratings yet
- Gallbladder Carcinoma Presenting As Right Upper Quadrant Pain: A Case ReportDocument19 pagesGallbladder Carcinoma Presenting As Right Upper Quadrant Pain: A Case ReportMacky YongcoNo ratings yet
- (Final Edit) Ventral Onlay Buccal Graft For Urethrorectal FistulaDocument13 pages(Final Edit) Ventral Onlay Buccal Graft For Urethrorectal FistulaNadia Rezky ElizaNo ratings yet
- Problems in Diagnosis Approach For Carcinoma of Pancreatic HeadDocument6 pagesProblems in Diagnosis Approach For Carcinoma of Pancreatic HeadfikriafisNo ratings yet
- Case 101Document14 pagesCase 101Marj MendezNo ratings yet
- Case Presentation:: DR - Amra Farrukh PG.T Su.IDocument75 pagesCase Presentation:: DR - Amra Farrukh PG.T Su.IpeeconNo ratings yet
- 70564-EN-diagnostic-approach-and-treatment-of-choDocument5 pages70564-EN-diagnostic-approach-and-treatment-of-choFatricia SolissaNo ratings yet
- A Rare Case of Colon Cancer in A Young Patient: A Case Report and Literature ReviewDocument5 pagesA Rare Case of Colon Cancer in A Young Patient: A Case Report and Literature ReviewIJAR JOURNALNo ratings yet
- Brunner's Gland Adenoma: Case ReportDocument3 pagesBrunner's Gland Adenoma: Case ReportasclepiuspdfsNo ratings yet
- s40792 018 0489 1Document7 pagess40792 018 0489 1Laura PredescuNo ratings yet
- Modern imaging in patients with obstructive jaundiceDocument4 pagesModern imaging in patients with obstructive jaundicedanaogreanuNo ratings yet
- Liver Abscess DissertationDocument4 pagesLiver Abscess DissertationPayForAPaperAtlanta100% (1)
- Calcagno 2018Document10 pagesCalcagno 2018cut normaya putriNo ratings yet
- Fibrolamellar Variant of Hepatocellular Carcinoma in A Young FemaleDocument3 pagesFibrolamellar Variant of Hepatocellular Carcinoma in A Young FemaleIKIKIKIKIKI999999No ratings yet
- International Journal of Infectious Diseases: Anshuman Pandey, Shakeel Masood, Namrata P. AwasthiDocument3 pagesInternational Journal of Infectious Diseases: Anshuman Pandey, Shakeel Masood, Namrata P. Awasthijohanna monsalveNo ratings yet
- Tubular Ileal Duplication Causing Small Bowel Obstruction in A ChildDocument5 pagesTubular Ileal Duplication Causing Small Bowel Obstruction in A ChildDiego Leonardo Herrera OjedaNo ratings yet
- 17-09-2019 Lower GI FINALDocument32 pages17-09-2019 Lower GI FINALNaima HabibNo ratings yet
- A Rare and Fatal Case of Nasogastric Tube.492Document1 pageA Rare and Fatal Case of Nasogastric Tube.492Stefania Szeibert-KerekesNo ratings yet
- Akiyama Case ReportDocument3 pagesAkiyama Case ReportApmc SchwartzNo ratings yet
- 2007-03 - Intestinal Autotransplantation For Adenocarcinoma of Pancreas Involving The Mesenteric Root - Our Experience and Literature Review PDFDocument3 pages2007-03 - Intestinal Autotransplantation For Adenocarcinoma of Pancreas Involving The Mesenteric Root - Our Experience and Literature Review PDFNawzad SulayvaniNo ratings yet
- Coledocolitiasis CurrentDocument6 pagesColedocolitiasis CurrentvalNo ratings yet
- A Giant Simple Hepatic Cyst With Chronic ConstipationDocument2 pagesA Giant Simple Hepatic Cyst With Chronic ConstipationJapanese Journal of Gastroenterology and HepatologyNo ratings yet
- Jejunojejunal Intussusception As Initial Presentation of Coeliac Disease: A Case Report and Review of LiteratureDocument6 pagesJejunojejunal Intussusception As Initial Presentation of Coeliac Disease: A Case Report and Review of Literatureellya theresiaNo ratings yet
- Urological Science: Haoping Tai, Jue-Hawn Yin, Zhon-Min Huang, Tang-Yi TsaoDocument3 pagesUrological Science: Haoping Tai, Jue-Hawn Yin, Zhon-Min Huang, Tang-Yi TsaorendyjiwonoNo ratings yet
- Materi DR Budi WidodoDocument44 pagesMateri DR Budi WidodoAnna Maria UlfaNo ratings yet
- KlatskinDocument24 pagesKlatskinArian WawolumajaNo ratings yet
- Recurrent Pancreatitis Caused by Groove PancreatitisDocument7 pagesRecurrent Pancreatitis Caused by Groove PancreatitisroxxanaNo ratings yet
- Pancreatic Head Mass: What Can Be Done ? Diagnosis: UltrasonographyDocument4 pagesPancreatic Head Mass: What Can Be Done ? Diagnosis: UltrasonographyMolla WariNo ratings yet
- Hepatic Computed Tomography and Cholangiography by Use of Gadoxetic Acid in Healthy CatsDocument11 pagesHepatic Computed Tomography and Cholangiography by Use of Gadoxetic Acid in Healthy CatsAlejandro Estrada RiosNo ratings yet
- Recurrent Acute Pancreatitis and Massive Hemorrhagic Ascites Secondary To A Duodenal Duplication in A Child: A Case ReportDocument4 pagesRecurrent Acute Pancreatitis and Massive Hemorrhagic Ascites Secondary To A Duodenal Duplication in A Child: A Case ReportHarnadi WonogiriNo ratings yet
- Recurrent pancreatitis and sphincter of Oddi dysfunctionDocument4 pagesRecurrent pancreatitis and sphincter of Oddi dysfunctionDimas ArdaniNo ratings yet
- Ictericia Obstructiva, Tratamiento EndoscópicoDocument6 pagesIctericia Obstructiva, Tratamiento EndoscópicoGeraldine RuizNo ratings yet
- JournalDocument5 pagesJournalMuhammad SyariefNo ratings yet
- Jurnal IkterusDocument3 pagesJurnal IkterusTututWidyaNurAnggrainiNo ratings yet
- EN Acute Pancreatitis As A Complication ofDocument5 pagesEN Acute Pancreatitis As A Complication ofShandy JonnerNo ratings yet
- Purbadi-Peritoneal tuberculosis mimicking advanced ovarian cancer case report- Laparoscopy as diagnostic modality-2021-International Journal of Surgery Case ReportsDocument4 pagesPurbadi-Peritoneal tuberculosis mimicking advanced ovarian cancer case report- Laparoscopy as diagnostic modality-2021-International Journal of Surgery Case ReportsSulaeman Andrianto SusiloNo ratings yet
- 260-Article Text-875-1-10-20220728Document4 pages260-Article Text-875-1-10-20220728hasan andrianNo ratings yet
- Electronic Image of The Month: A Rare Tumor of The Common Hepatic Duct Causing Biliary ObstructionDocument2 pagesElectronic Image of The Month: A Rare Tumor of The Common Hepatic Duct Causing Biliary ObstructionDeborah Anasthasia PakpahanNo ratings yet
- Primary Pure Squamous Cell Carcinoma of The Duodenum: A Case ReportDocument4 pagesPrimary Pure Squamous Cell Carcinoma of The Duodenum: A Case ReportGeorge CiorogarNo ratings yet
- Jurnal 7Document3 pagesJurnal 7rahayuNo ratings yet
- dejesus-et-al-2020-ultrasonographic-evaluation-of-cholecystoduodenostomy-sites-in-six-catsDocument9 pagesdejesus-et-al-2020-ultrasonographic-evaluation-of-cholecystoduodenostomy-sites-in-six-catscitratomNo ratings yet
- Amma 2018 0026Document4 pagesAmma 2018 0026Dan CretuNo ratings yet
- Adenocarcinoma at Angle of Treitz: A Report of Two Cases With Review of LiteratureDocument3 pagesAdenocarcinoma at Angle of Treitz: A Report of Two Cases With Review of LiteratureRijal SaputroNo ratings yet
- 2020 Paper SplenicDocument5 pages2020 Paper SplenicLauburu CrossNo ratings yet
- Choledochal Cyst: SymposiumDocument3 pagesCholedochal Cyst: SymposiumRegi Anastasya MangiriNo ratings yet
- Metastatic Spread of Primary Lung Adenocarcino - 2024 - International Journal ofDocument5 pagesMetastatic Spread of Primary Lung Adenocarcino - 2024 - International Journal ofRonald QuezadaNo ratings yet
- Recurrent Adenocarcinoma of Colon Presenting As Duo-Denal Metastasis With Partial Gastric Outlet Obstruction: A Case Report With Review of LiteratureDocument5 pagesRecurrent Adenocarcinoma of Colon Presenting As Duo-Denal Metastasis With Partial Gastric Outlet Obstruction: A Case Report With Review of LiteratureVika RatuNo ratings yet
- 1 s2.0 S2210261221009731 MainDocument4 pages1 s2.0 S2210261221009731 Maintarmohamed.muradNo ratings yet
- Imaging in Chronic PancreatitisDocument7 pagesImaging in Chronic Pancreatitisdesy 102017135No ratings yet
- General Surgery: Ruptured Liver Abscess: A Novel Surgical TechniqueDocument3 pagesGeneral Surgery: Ruptured Liver Abscess: A Novel Surgical TechniqueRahul SinghNo ratings yet
- A Case Report On Hilar Cholangiocarcinoma With Duodenal WhipwormsDocument5 pagesA Case Report On Hilar Cholangiocarcinoma With Duodenal WhipwormsIJAR JOURNALNo ratings yet
- T5 Pancreas PDFDocument19 pagesT5 Pancreas PDFAmin ZahariNo ratings yet
- Groove Pancreatitis: A Rare Case SeriesDocument4 pagesGroove Pancreatitis: A Rare Case SeriesJothiprasad VenkatesanNo ratings yet
- Synchronous Pancreatic Neuroendocrine Tumor and Pancreatic Cyst A Case ReportDocument4 pagesSynchronous Pancreatic Neuroendocrine Tumor and Pancreatic Cyst A Case ReportWorld Journal of Clinical SurgeryNo ratings yet
- Revisión Del Carcinoma de Vesicula: Poster No.: Congress: Type: AuthorsDocument26 pagesRevisión Del Carcinoma de Vesicula: Poster No.: Congress: Type: AuthorsArturo García MarquezNo ratings yet
- Assessment of Dysphagia in Acute Stroke Patients by The Gugging Swallowing ScreenDocument8 pagesAssessment of Dysphagia in Acute Stroke Patients by The Gugging Swallowing ScreenAyip Bahsan AlBantaniNo ratings yet
- Does Ethics Really Matter To The Sustainability of New Ventures The Relationship Between Entrepreneurial Ethics, Firm Visibility and Entrepreneurial PerformanceDocument23 pagesDoes Ethics Really Matter To The Sustainability of New Ventures The Relationship Between Entrepreneurial Ethics, Firm Visibility and Entrepreneurial PerformanceAyip Bahsan AlBantaniNo ratings yet
- Effect of Dietary Omega-3 Fatty Acid Supplementation On Frailty-Related Phenotypes in Older Adults: A Systematic Review and Meta-Analysis ProtocolDocument5 pagesEffect of Dietary Omega-3 Fatty Acid Supplementation On Frailty-Related Phenotypes in Older Adults: A Systematic Review and Meta-Analysis ProtocolAyip Bahsan AlBantaniNo ratings yet
- How Much and What Type of Protein Should A Critically Ill Patient Receive?Document9 pagesHow Much and What Type of Protein Should A Critically Ill Patient Receive?Ayip Bahsan AlBantaniNo ratings yet
- Non-Protein Calorie: Nitrogen Ratio (NPC/N) As An Indicator of Nitrogen Balance in Clinical SettingsDocument3 pagesNon-Protein Calorie: Nitrogen Ratio (NPC/N) As An Indicator of Nitrogen Balance in Clinical SettingsAyip Bahsan AlBantaniNo ratings yet
- Curroncol 28 00293Document10 pagesCurroncol 28 00293Ayip Bahsan AlBantaniNo ratings yet
- Trends in Incidence and Management of Cancer of THDocument9 pagesTrends in Incidence and Management of Cancer of THAyip Bahsan AlBantaniNo ratings yet
- Updates in Management of Ampullary CarcinomasDocument5 pagesUpdates in Management of Ampullary CarcinomasAyip Bahsan AlBantaniNo ratings yet
- KasaiDocument7 pagesKasaishalukiriNo ratings yet
- Anatomi Topografi Kepala-ParotisDocument12 pagesAnatomi Topografi Kepala-ParotisFeri IrawanNo ratings yet
- Biliary AtresiaDocument25 pagesBiliary Atresiajulius billiNo ratings yet
- Clinical Exam QuestionsDocument32 pagesClinical Exam QuestionsAtiqah ShahNo ratings yet
- Enteric Contrast MediaDocument25 pagesEnteric Contrast MediaNoraini Raimi Sajari100% (1)
- Avian Digestive SystemDocument9 pagesAvian Digestive SystemChaudhary Ahmed RazaNo ratings yet
- Upper Gastrointestinal BleedingDocument3 pagesUpper Gastrointestinal BleedingcheyzerrlNo ratings yet
- Case Write Up SURGERYDocument14 pagesCase Write Up SURGERYRahul Audenesen50% (2)
- Reviewerenema and Oxygen MarieDocument4 pagesReviewerenema and Oxygen MarieIrish EspinosaNo ratings yet
- RLE CLD Secondary To BADocument45 pagesRLE CLD Secondary To BACatherine Kate GulengNo ratings yet
- Unit 4 Taste PDFDocument4 pagesUnit 4 Taste PDFMonica Garcia RamisNo ratings yet
- Cholecystectomy 4 PrintingDocument19 pagesCholecystectomy 4 PrintingKyle Punzalan100% (2)
- Digestive System SS2Document19 pagesDigestive System SS2Oluwatoniloba TellaNo ratings yet
- A Case Study On Urinalysis and Body FluidsDocument17 pagesA Case Study On Urinalysis and Body Fluidsrakish16No ratings yet
- Journey Through DigestionDocument4 pagesJourney Through DigestionJoy JonesNo ratings yet
- Characterized: Heterotrophs or Organisms That Cannot Make Their OwnDocument5 pagesCharacterized: Heterotrophs or Organisms That Cannot Make Their OwnKyungsoo DoNo ratings yet
- What's The Difference Between Gastric and Duodenal Ulcers?Document6 pagesWhat's The Difference Between Gastric and Duodenal Ulcers?Anonymous cDy4bZMMNo ratings yet
- Nutrition in Animals NotesDocument5 pagesNutrition in Animals NotesGowri YadavNo ratings yet
- Types of EnemaDocument6 pagesTypes of EnemaOmprakash Saini100% (2)
- Case Study For Diagnosis of DiseaseDocument29 pagesCase Study For Diagnosis of DiseaseFirifan DiribaNo ratings yet
- The Small Intestine: Anatomy and RelationsDocument5 pagesThe Small Intestine: Anatomy and RelationsaoifeoxNo ratings yet
- Histology of The Esophagus and Stomach-1Document34 pagesHistology of The Esophagus and Stomach-1kuchipuchi12No ratings yet
- Zollinger EllisonDocument2 pagesZollinger EllisonFrama Intan MiguelNo ratings yet
- Functions of Bile Salts: Emulsification, Absorption of Fats and Fat-Soluble VitaminsDocument24 pagesFunctions of Bile Salts: Emulsification, Absorption of Fats and Fat-Soluble VitaminsAyeshaNo ratings yet
- Defecation ReflexDocument31 pagesDefecation ReflexNayyer Khan100% (1)
- Chapter 45 Lewis Med SurgeDocument14 pagesChapter 45 Lewis Med SurgeZeppKFwNo ratings yet
- Colonoscopy For DummiesDocument79 pagesColonoscopy For Dummiesmike.krawulski9224100% (3)
- Rectal ProlapseDocument6 pagesRectal ProlapseAnjani Putri RetnaninggalihNo ratings yet
- GastrointestinalDocument39 pagesGastrointestinalالمسوول الاعلاميNo ratings yet
- Bile Duct InjuryDocument62 pagesBile Duct InjuryShashidhara Puttaraj100% (1)